MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18
|
|
|
- Andrea Short
- 5 years ago
- Views:
Transcription
1 MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18
2 Agenda Save Time by Utilizing the MHS Secure Web Portal: Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims o Review Claims Secure Messaging
3 Administration
4 Secure Web Portal Login or Registration Login/Register is the same for MHS, Ambetter from MHS, Allwell from MHS and Behavioral Health Providers.
5 Web Portal Training Documents Documents Include: Registration Guide MHS Web Portal User Guides. How To Complete Specific Tasks on the MHS Web Portal.
6 Complete Registration or Login The Registration is complete and the Secure Portal homepage will be visible! An will be sent to the provider when they have access to specific tools.
7 Dashboard Change User has the ability to change between Tax ID Numbers added along with choices for: Medicaid, Ambetter from MHS, Allwell from MHS and Behavioral Health IN Medicaid.
8 Homepage MHS (Medicaid)
9 MHS Welcome and Quick Links Welcome: Multiple TINs can be managed from a single account. Account Managers can oversee the secure portal accounts of their staff/office. User can be added, disabled, and have their permissions changed. Reports are available here. Patient and Provider Analytics Quick Links: Public link to Provider Resources: o Demographic Update Tool o Preferred Drug Lists o Provider Education Member Management Forms IHCP Provider Healthcare Portal link Pharmacy Information Go Paperless
10 MHS Member Management Forms Click on Member Management Forms under Quick Links. Choose between: Member Disenrollment Form Panel Management Form
11 Account Details To view your Account Details: 1. Select the drop-down arrow next to user name in the upper right corner on the dashboard. 2. Click Account Details. *Note: Under Your TINs you see the Current Primary Default TIN for the account, and can select another TIN to Mark As Default or Remove a TIN.
12 Account Manager User Management For Account Managers to manage their office staff/users associated to their practice: When using this feature you can disable/enable users, and manage permissions for your account. 1. Select the drop-down arrow next to your name in the upper right corner. 2. Select User Management. 3. Click Update User next to the user name.
13 Quality Reports
14 Reports To view Quality Reports: Click Reports on the homepage.
15 Reports View P4P Reports including: Members Needing Services Group Scorecard Individual Scorecard If you have questions or find any issues with your scorecard, please
16 Reports View Members Needing Services.
17 Reports View Group Scorecard.
18 Reports View Individual Scorecard.
19 Reports Patient Analytics Click on Patient Analytics from Homepage.
20 Reports Patient Analytics Functionalities of the Patient Tab.
21 Reports Patient Analytics Each member has a detailed Patient Profile.
22 Reports Patient Analytics Quality Measure Report by selected groups and filters.
23 Reports Patient Analytics Creating Saved Reports for frequent use.
24 Reports Provider Analytics The tool designed to support patient care and help improve performance in value-based programs. Provider Analytics has multiple tabs, including a Quality tab which provides care gap information, and the Value-based Contracting tab.
25 Eligibility
26 Check Eligibility The Eligibility tab offers an Eligibility Check tool designed to quickly check the status of any member. Update the Date of Service, if necessary. Enter the Member ID or Last Name and DOB (Date of Birth). Click Check Eligibility.
27 Check Eligibility Eligibility status is indicated by a Green Thumbs-Up for Eligible and an Orange Thumbs-Down for Ineligible. Details for any member can be viewed by clicking on the Member s Name. Care Gaps can also be seen within the search results. By clicking Emergency Room Visit?, an ER visit will be indicated. Right Choice Program indicator labeled Yes
28 Add Emergency Room Visit Update with specific details regarding the Reason for Visit and Facility.
29 Member Record
30 Member Record Details Member Overview Cost Sharing Assessments Health Record Visits, Medications, Immunizations, Labs, and Allergies Care Plan Authorizations Referrals Coordination of Benefits Claims Power Account Service Estimate *only HIP Members Document Resource Center Notes
31 Member Overview Overview Tab: 1. Patient Information 2. Eligibility History 3. PCP Information and PMP History 4. EPSDT 5. Care Gaps 6. Allergies
32 View Clinical Information Clinical Information: Three Most Recent ER Visits Three Most Recent Inpatient Admissions Three Most Recent Office Visits Top 5 Most Occurring Diagnosis Recent Pharmacy Activity
33 Cost Sharing Cost Sharing shows if a member has any co-payments.
34 Assessments Types of Assessments: 1. Link to Notification of Pregnancy. 2. HIP Preventative Services Assessment submission. 3. View completion of Previous Assessments.
35 Health Record - Visits Visits show a listing of the member s Primary Diagnosis, Date, Visit Type, Claim Type and Facility/Provider. Including: Medical, Dental, Vision and Behavioral.
36 Health Record - Medications Member s most recent Pharmacy Claims.
37 Health Record - Immunizations Member s most recent Immunizations and Schedule.
38 Health Record - Labs Member s most recent Labs.
39 Health Record - Allergies Member list of Allergies.
40 Care Plan Displays if a member has a Care Plan.
41 Authorizations View previously submitted or Create A New Authorization.
42 Referrals Refer a member to Case Management or Behavioral Health.
43 Coordination of Benefits This screen shows if a member has other insurance.
44 Claims Claims screen shows the members most recent claims and create a new claim: Clicking on the Claim No. shows additional details.
45 Document Resource Center Medical Necessity or Quality Management Document Upload.
46 Notes Click on Write Note and see previous Notes.
47 Patient List
48 View Patient List Click Patients tab at the top of the screen. The Patient List appears displaying Eligibility Status, Preferred Language, Member Name, Medicaid ID, Date of Birth, Phone Number, Alerts and Right Choices Program. To download the patient list to Excel, click Download. This allows for you to manage your patient information as desired in Excel.
49 Filter Patient List Filter By: Provider NPI Provider Medicaid Number Member Last Name Care Gaps (CG) Case Management (CM) Emergency Department (ED) Preferred Language Disease Management (DM) New Member (NM) No HRA
50 Download to Excel Filter Excel: Download date and disclaimer will appear.
51 Authorizations
52 Authorizations View, create and filter group Authorizations: Click on the AUTH ID to see additional information.
53 Authorizations Filter Authorizations by: Date Range, Member, Authorization#, Confirmation#, Status or Auth Type.
54 Create a New Authorization New Authorization: Click Create Authorization. Enter Member ID or Last Name and Birthdate.
55 Creating a New Authorization Select a Service Type.
56 Creating a New Authorization Select Provider NPI Add Primary Diagnosis
57 Creating a New Authorization If required Add Additional Procedures.
58 Creating a New Authorization Service Line Details: Provider Request will appear on the left side of the screen Update Servicing Provider - Check box if same as Requesting Provider - Update Servicing Provider information if not the same Update Start Date and End Date Update Total Units/Visits/Days Update Primary Procedure - Code lookup provided Add any additional procedures Add additional Service Line if applicable - All service lines added will appear on the left side of the screen
59 Creating a New Authorization Submit a new Authorization: Confirmation number
60 Authorization for Durable & Home Medical Equipment Requests should be initiated via MHS Secure portal: 1. Select Authorizations tab and click on Create Authorization. 2. Enter Member ID or Last Name and Date of Birth. 3. Choose DME and you will be directed to the Medline portal for order entry.
61 Claims
62 Claims Web Portal Claims Functionalities: Submit new claim. Review claims information on file for a patient. Correct claims. View payment history. Submit a New Claim: Click Create Claim and enter Member ID and Birthdate.
63 Claim Submission Choose the Claim Type: Professional or Institutional claim submission.
64 Professional Claim Submission: Step 1 In the General Info section, populate the Patient s Account Number and other information related to the patient s condition by typing into the appropriate fields. Click Next.
65 Professional Claim Submission: Step 2 Add the Diagnosis Codes for the patient in Box 21. Click the Add button to save. Click Add Coordination of Benefits to include any payments made by another insurance carrier (if applicable).
66 Professional Claim Submission: Step 3 Add Service Lines.
67 Professional Claim Submission: Step 4-5 Enter Referring and Billing provider information. Enter Service Facility Location. Click Next. In the Attachments section you can Browse and Attach any documents to the claim as desired. (Note: If you have no attachments, skip this section.) Click Next.
68 Professional Claim Submission: Step 6 In the Review section, you can see if the claim is eligible for Real Time Editing and Pricing. Click Validate for RTEP Claims and Click Submit for regular processed claims.
69 RTEP Claim Pricing View RTEP Overview: On the final screen each procedure code will receive a reimbursement estimate, pended claim explanation or denial reason. Claims with a reimbursement estimate or pend explanation, may be impacted by final adjudication including a change to the reimbursement amount or a denial. Adjudication status may be affected by Code Editing or other payment rules.
70 Submitted Claims The Submitted tab will show only claims created via the MHS portal: Paid is a green thumbs up Denied is a orange thumbs down Pending is a clock RTEP claims also show if eligible (i.e. line 2 was submitted, but was not eligible for RTEP).
71 Reviewing Claims
72 Individual Claims On the Individual tab, submitted using paper, portal or clearing house: View the Claim Number, Claim Type, Member Name, Service Dates, Billed/Paid, and Claim Status. Paid is a green thumbs up, Denied is a orange thumbs down and a clock is Pending.
73 Saved Claims To view Saved claims: Drafts, Professional or Institutional: 1.Select Saved 2.Click Edit to view a claim 3.Fix any errors or complete before submitting Or 4. Click Delete to delete saved claim that is no longer necessary 5. Click OK to confirm the deletion
74 Correcting Claims After clicking on a Claim # link: 1. Click Correct Claim. 2. Proceed through the claims screens correcting the information that you may have omitted when the claim was originally submitted. 3. Continue clicking Next to move through the screens required to resubmit 4. Review the claim information. 5. Click Submit. Only claims with a status of PAID or DENIED can be corrected online.
75 Payment History Click on Payment History to view Check Date, Check Number, Check Clear Date, Mailing Address and Payment Amount. Click on Check Date to view Explanation of Payment.
76 Payment History Click on View Service Line Details.
77 Payment History View Service Line Details: The Explanation of Payment details displays the Date and Check Number This view shows each patient payment by service line detail made on the check
78 Tips to Remember Clicking on items (claim numbers, check numbers, dates) that are highlighted blue will reveal additional information. When filtering to find a claim or payment, only a 1 month span can be used. Click on the Saved Claims tab to view claims that have been Created but not Submitted. Claims in this queue can be edited for submission or deleted from this tab. In order to utilize the Correct Claim feature, the claim needs to be in a Paid or Denied status. When managing multiple tax id numbers, change to a new tax id number and view the dashboard associated with that TIN from any screen. When filtering Payment History the span is limited to 1 month.
79 Claims Audit Tool The Clear Claim Connection screen appears, allowing you to enter the Procedure, Quantity, Modifiers, Date and Place of Service, and Diagnosis for a claim proactively before you submit or retroactively after you submit.
80 Secure Messaging
81 Secure Messaging Create a New Secure Message: Click Messaging tab from the Dashboard. Click Create Message.
82 Secure Messaging Contents of a Secure Message: Select Subject and if applicable Member ID and Date of Birth along with your message then click Send. A confirmation message appears that your message successfully sent.
83 MHS Provider Relations Team Candace Ervin Envolve Dental Indiana Provider Relations ext m Chad Pratt Provider Relations Specialist Northeast Region ext Tawanna Danzie Provider Relations Specialist Northwest Region ext Jennifer Garner Provider Relations Specialist Southeast Region ext Taneya Wagaman Provider Relations Specialist Central Region ext Katherine Gibson Provider Relations Specialist North Central Region ext Esther Cervantes Provider Relations Specialist South West Region ext mhsindiana.com LaKisha Browder Candace Ervin Behavioral Health Provider Relations Specialist - East Region Envolve Dental Indiana Provider Relations ext lakisha.j.browder@mhsindiana.co m ext Candace.Ervin@envolvehealth.co m
84 Questions? Thank you for being our partner in care.
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
MHS Prior Authorization 0317.PR.P.PP
 MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
MHS CMS 1500 Tips and Billing Guidelines
 MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
0518.PR.P.PP.2 7/18. The Ins and Outs of CMS 1500 Billing
 0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
MHS UB Tips and Billing Guidelines 0418.PR.P.PP 5/18
 MHS UB 04 2018 Tips and Billing Guidelines 0418.PR.P.PP 5/18 Agenda Claim Process Claim Process Common Claim Rejections Common Claim Denials Claim Adjustments Claims Dispute Resolution Prior Authorization
MHS UB 04 2018 Tips and Billing Guidelines 0418.PR.P.PP 5/18 Agenda Claim Process Claim Process Common Claim Rejections Common Claim Denials Claim Adjustments Claims Dispute Resolution Prior Authorization
MHS UB-04 Billing and Claim Processing Tips and Billing Guidelines
 MHS UB-04 Billing and Claim Processing Tips and Billing Guidelines 1 1015.PR.P.PP 10/15 Agenda Who is MHS? Claim Process Filing Process Common Claim Rejections Common Claim Denials Claim Adjustments Claims
MHS UB-04 Billing and Claim Processing Tips and Billing Guidelines 1 1015.PR.P.PP 10/15 Agenda Who is MHS? Claim Process Filing Process Common Claim Rejections Common Claim Denials Claim Adjustments Claims
Welcome to Managed Health Services (MHS) 0717.PR.P.PP 10/17
 Welcome to Managed Health Services (MHS) 0717.PR.P.PP 10/17 Agenda MHS Overview Health Programs Claim Process Prior Authorization Process HEDIS Coordinated Care Programs MHS Partnership Ambetter Questions
Welcome to Managed Health Services (MHS) 0717.PR.P.PP 10/17 Agenda MHS Overview Health Programs Claim Process Prior Authorization Process HEDIS Coordinated Care Programs MHS Partnership Ambetter Questions
Ambetter and Allwell 1 st Quarterly Webinar April 12 th, 2018
 Ambetter and Allwell 1 st Quarterly Webinar April 12 th, 2018 Conference Number: (855) 351-5537 Conference Code: 741 390 3784 If you haven t already, please call into the webinar to hear us speak. Your
Ambetter and Allwell 1 st Quarterly Webinar April 12 th, 2018 Conference Number: (855) 351-5537 Conference Code: 741 390 3784 If you haven t already, please call into the webinar to hear us speak. Your
Maintaining Budget Change Requests
 Maintaining Budget Change Requests This document describes the functions used in TEAMS to enter and approve requests to move funds from one General Ledger account to another. In this document: Request
Maintaining Budget Change Requests This document describes the functions used in TEAMS to enter and approve requests to move funds from one General Ledger account to another. In this document: Request
The benefits of using ExpressPAth for your practice include: Easy access. With 24/7 access, you can submit requests and get answers at any time.
 Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
eauthorization Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with
 Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Tellus EVV Claims Portal TRAINING REFERENCE GUIDE
 Tellus EVV Claims Portal TRAINING REFERENCE GUIDE REV: 11/17 Sponsored by Centric Consulting, LLC, and the State of Florida, AHCA Table of Contents... 3 5.1 Overview... 3 5.2 Claims Home Page... 4 5.3
Tellus EVV Claims Portal TRAINING REFERENCE GUIDE REV: 11/17 Sponsored by Centric Consulting, LLC, and the State of Florida, AHCA Table of Contents... 3 5.1 Overview... 3 5.2 Claims Home Page... 4 5.3
MDwise Annual IHCP Seminar. Exclusively serving Indiana families since 1994.
 MDwise 101 2016 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda MDwise history IHCP Overview MDwise Delivery System Model IHCP Program Overview Hoosier Healthwise Healthy Indiana
MDwise 101 2016 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda MDwise history IHCP Overview MDwise Delivery System Model IHCP Program Overview Hoosier Healthwise Healthy Indiana
Avenues of Resolution for Indiana Health Coverage Programs
 Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
LTC/MMA Monthly Claims Training Prior Authorization Submission
 LTC/MMA Monthly Claims Training Prior Authorization Submission Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to: Molina
LTC/MMA Monthly Claims Training Prior Authorization Submission Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to: Molina
Eligibility and Benefits Inquiry Guide
 Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Prescriber Web Prior Authorization
 Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Electronic Prior Authorization - Provider Guide. July 2017
 Electronic Prior Authorization - Provider Guide July 2017 Table of Contents Getting Started 3 Registration 4 Logging In 5 System Configurations (Post Office Settings) 6 Prior Request Form 7 General 7 Patient
Electronic Prior Authorization - Provider Guide July 2017 Table of Contents Getting Started 3 Registration 4 Logging In 5 System Configurations (Post Office Settings) 6 Prior Request Form 7 General 7 Patient
Managed Health Services
 Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
Claim Investigation Submission Guide
 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
MHS Updates Summer PR.P.PP
 MHS Updates Summer 2017 0517.PR.P.PP Updates Important to You Prior Authorization (PA) Updates DME Changes Therapy Authorization Process MHS Prior Authorization 101 Home Health MHS Occurrence Prior Authorization
MHS Updates Summer 2017 0517.PR.P.PP Updates Important to You Prior Authorization (PA) Updates DME Changes Therapy Authorization Process MHS Prior Authorization 101 Home Health MHS Occurrence Prior Authorization
Ambetter 101. Quarterly Provider Webinar February 23, 2017
 Ambetter 101 Quarterly Provider Webinar February 23, 2017 AGENDA 1. What is Ambetter? 2. The Health Insurance Marketplace 3. Public Website and Secure Portal 4. Verification of Eligibility, Benefits and
Ambetter 101 Quarterly Provider Webinar February 23, 2017 AGENDA 1. What is Ambetter? 2. The Health Insurance Marketplace 3. Public Website and Secure Portal 4. Verification of Eligibility, Benefits and
Healthy Indiana Plan POWER Account Debit Card
 Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
Electronic Prior Authorization - Provider Guide
 Electronic Prior Authorization - Provider Guide Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient and
Electronic Prior Authorization - Provider Guide Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient and
Electronic PriorAuthorization - Provider Guide. July 2017
 Electronic PriorAuthorization - Provider Guide July 2017 Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient
Electronic PriorAuthorization - Provider Guide July 2017 Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient
Network Health Claims Editing Portal
 Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Provider Healthcare Portal Demonstration:
 Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Claim Preparation and Filing Overview for U.S.
 Claim Preparation and Filing Overview for U.S. During the course of a patient visit, invoices will be created by various staff within the office. It is recommended that when an insurance invoice is created
Claim Preparation and Filing Overview for U.S. During the course of a patient visit, invoices will be created by various staff within the office. It is recommended that when an insurance invoice is created
DUS DocWay TM Loan Documents User Guide. January 2019
 DUS DocWay TM Loan Documents User Guide January 2019 Table of Contents Getting Started with DUS DocWay... 1 Welcome Page Navigation... 3 Loan Documents Navigation... 6 Update Document Category and Type...
DUS DocWay TM Loan Documents User Guide January 2019 Table of Contents Getting Started with DUS DocWay... 1 Welcome Page Navigation... 3 Loan Documents Navigation... 6 Update Document Category and Type...
Specialty Drug Medical Benefit Management
 Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH
 LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to:
LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to:
Version 1/Revision 18 Page 1 of 36. epaces Professional Claim REFERENCE GUIDE
 Version 1/Revision 18 Page 1 of 36 Table of Contents GENERAL CLAIM INFORMATION TAB... 3 PROFESSIONAL CLAIM INFORMATION TAB... 5 PROVIDER INFORMATION TAB... 10 DIAGNOSIS TAB... 12 OTHER PAYERS TAB... 13
Version 1/Revision 18 Page 1 of 36 Table of Contents GENERAL CLAIM INFORMATION TAB... 3 PROFESSIONAL CLAIM INFORMATION TAB... 5 PROVIDER INFORMATION TAB... 10 DIAGNOSIS TAB... 12 OTHER PAYERS TAB... 13
Healthy Indiana Plan (HIP) Provider Orientation
 Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
For Lenders. Accessing LOS: LOS is a web based program that can be accessed at the following URL address: https://los.chfa.org/los
 Accessing LOS: LOS is a web based program that can be accessed at the following URL address: https://los.chfa.org/los A User ID and Password will be assigned to all users by the designated account administrator
Accessing LOS: LOS is a web based program that can be accessed at the following URL address: https://los.chfa.org/los A User ID and Password will be assigned to all users by the designated account administrator
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Post Payment Documentation Request Portal
 Post Payment Documentation Request Portal Responding to an Expense Reimbursement Post Payment Document Request Fannie Mae s Post Payment Documentation Request portal provides an efficient and simple way
Post Payment Documentation Request Portal Responding to an Expense Reimbursement Post Payment Document Request Fannie Mae s Post Payment Documentation Request portal provides an efficient and simple way
What You Need to Know About
 What You Need to Know About Medical Specialty Drug Prior Authorizations 2016 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service OVERVIEW
What You Need to Know About Medical Specialty Drug Prior Authorizations 2016 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service OVERVIEW
Medical Eligibility & Benefits Lookup Tips
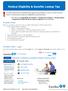 Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Web Benefits Admin User Guide
 Web Benefits Admin User Guide. Table of Contents Navigate to Web Benefits... 3 Accessing Employee User Accounts... 4 Employee profile... 4 Active coverage... 5 Event history... 6 Family... 6 Adding a New
Web Benefits Admin User Guide. Table of Contents Navigate to Web Benefits... 3 Accessing Employee User Accounts... 4 Employee profile... 4 Active coverage... 5 Event history... 6 Family... 6 Adding a New
When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective?
 GENERAL When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective? The bill has been signed into law by the Governor and will be effective July 1, 2008. However, DCH
GENERAL When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective? The bill has been signed into law by the Governor and will be effective July 1, 2008. However, DCH
HealthChoice Illinois
 HealthChoice Illinois November 2017 Presented by: Matt Wolf and Lori Lomahan Meeting Agenda Introductions Credentialing Update Billing Instructions Claims Adjudication Reimbursement Methodology MCO Website
HealthChoice Illinois November 2017 Presented by: Matt Wolf and Lori Lomahan Meeting Agenda Introductions Credentialing Update Billing Instructions Claims Adjudication Reimbursement Methodology MCO Website
Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide
 Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide Version 5.0 February 26, 2007 Revision History Document Version Date Name Comments 1.0 12/27/2006 Patti George Created. 2.0
Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide Version 5.0 February 26, 2007 Revision History Document Version Date Name Comments 1.0 12/27/2006 Patti George Created. 2.0
MDwise, Inc. MDwise Updates 2017 IHCP First-Quarter Workshop. Exclusively serving Indiana families since 1994.
 MDwise, Inc. MDwise Updates 2017 IHCP First-Quarter Workshop Exclusively serving Indiana families since 1994. Agenda MDwise History Meet your Provider Relations Team IHCP Managed Care Overview MDwise Delivery
MDwise, Inc. MDwise Updates 2017 IHCP First-Quarter Workshop Exclusively serving Indiana families since 1994. Agenda MDwise History Meet your Provider Relations Team IHCP Managed Care Overview MDwise Delivery
IHCP Annual Workshop October 2017
 IHCP Annual Workshop October 2017 MDwise 101 HHW-HIPP0519( 10/17) Exclusively serving Indiana families since 1994. Agenda MDwise History IHCP Overview MDwise Delivery System Model IHCP Program Overview
IHCP Annual Workshop October 2017 MDwise 101 HHW-HIPP0519( 10/17) Exclusively serving Indiana families since 1994. Agenda MDwise History IHCP Overview MDwise Delivery System Model IHCP Program Overview
FlexChoice. Reimbursement Account Overview. Sentinel Benefits. Custom Solutio ns for Life and Wealth
 FlexChoice Reimbursement Account Overview Sentinel Benefits & F I NA N CI A L GRO U P Custom Solutio ns for Life and Wealth Welcome to Your F SA We have put together this guide to help you get the most
FlexChoice Reimbursement Account Overview Sentinel Benefits & F I NA N CI A L GRO U P Custom Solutio ns for Life and Wealth Welcome to Your F SA We have put together this guide to help you get the most
Prior Authorizations with InterQual Integration
 Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
Maine Chapter of the Healthcare Financial Management Association. MaineCare Provider Relations
 Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
DTE Energy retirees: Welcome to PayFlex
 DTE Energy retirees: Welcome to PayFlex You are enrolled in a Retiree Reimbursement Account (RRA). Your new RRA comes with some great tools to help you manage your account. Through the PayFlex member website,
DTE Energy retirees: Welcome to PayFlex You are enrolled in a Retiree Reimbursement Account (RRA). Your new RRA comes with some great tools to help you manage your account. Through the PayFlex member website,
Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017
 Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017 Key Points Starting Nov. 1, 2017, notification/prior authorization is required
Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017 Key Points Starting Nov. 1, 2017, notification/prior authorization is required
Portal User Guide. Submitting Inpatient Notifications and Prior Authorization Requests. Tufts Health Together and Tufts Health Direct
 MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Do not include a Social Security Number in your .
 Member Guide Table of Contents Introduction... 3 System Requirements... 3 Accessing CoreLink II... 4 Menu Components... 5 Log-in Screen... 5 Log-in Instructions... 5 Forgot Your Password... 6 Main Menu...
Member Guide Table of Contents Introduction... 3 System Requirements... 3 Accessing CoreLink II... 4 Menu Components... 5 Log-in Screen... 5 Log-in Instructions... 5 Forgot Your Password... 6 Main Menu...
VetXML - eclaims. New Feature Documentation
 VetXML - eclaims New Feature Documentation P a g e 1 What does it do? VetXML is now fully integrated with Voyager. VetXML is a communication standard to make it easier for the veterinary profession to
VetXML - eclaims New Feature Documentation P a g e 1 What does it do? VetXML is now fully integrated with Voyager. VetXML is a communication standard to make it easier for the veterinary profession to
Insurer User Manual Chapter 4: Insurer Home Page
 Insurer User Manual Chapter 4: Insurer Home Page 2018 HCAI Communications Table of Contents Navigating the Insurer Page... 2 Primary Navigation Bar... 3 Dashboard... 3 Plans and Invoices... 4 Claims...
Insurer User Manual Chapter 4: Insurer Home Page 2018 HCAI Communications Table of Contents Navigating the Insurer Page... 2 Primary Navigation Bar... 3 Dashboard... 3 Plans and Invoices... 4 Claims...
Flexible Spending Accounts (FSA)
 FSA Member Guide London Health Administrators.. 0 Commercial Way, East Providence, RI 09. P# 0- -700. 700. F# 0--97. 97. Email: customerservice@londonhealthusa.com FSA Overview Thank you for enrolling
FSA Member Guide London Health Administrators.. 0 Commercial Way, East Providence, RI 09. P# 0- -700. 700. F# 0--97. 97. Email: customerservice@londonhealthusa.com FSA Overview Thank you for enrolling
Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates
 Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
BBPadmin s WebCOBRA On Demand Employer User s Guide. BBPadmin s Employer User s Guide to
 BBPadmin s Employer User s Guide to 1 Table of Contents Introduction to Employers... 5 Chapter 1: Getting Started... 6 Purpose of WebCOBRA... 6 For Employers... 6 For Participants... 6 Getting Started
BBPadmin s Employer User s Guide to 1 Table of Contents Introduction to Employers... 5 Chapter 1: Getting Started... 6 Purpose of WebCOBRA... 6 For Employers... 6 For Participants... 6 Getting Started
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
The Budgets file is a robust feature in DPHS, offering the following functions:
 Budgets Overview: The Budgets file is a robust feature in DPHS, offering the following functions: Create New Budgets Copy Budgets from one year to another View and Modify Existing Budgets Delete a Budget
Budgets Overview: The Budgets file is a robust feature in DPHS, offering the following functions: Create New Budgets Copy Budgets from one year to another View and Modify Existing Budgets Delete a Budget
Housekeeping. Link Participant ID with Audio. Mute your line UNMUTED. Raise your hand with questions
 Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
Atradius Atrium. July version 3.0. Atradius Atrium. User manual. Atradius Atrium - User Manual Version 3.0
 July 2018 - version 3.0 User manual 1 - User Manual Version 3.0 Drive your business forward with powerful, easy-to-use credit management tools is the Atradius online platform, which offers you one place
July 2018 - version 3.0 User manual 1 - User Manual Version 3.0 Drive your business forward with powerful, easy-to-use credit management tools is the Atradius online platform, which offers you one place
CASH ADVANCES TABLE OF CONTENTS
 CASH ADVANCES TABLE OF CONTENTS Overview... 2 Responsibilities... 2 Delegate Entry Authority to Other Users... 2 Cash Advance Tips and Reminders... 4 Create and Manage... 5 Create a Cash Advance for Yourself...
CASH ADVANCES TABLE OF CONTENTS Overview... 2 Responsibilities... 2 Delegate Entry Authority to Other Users... 2 Cash Advance Tips and Reminders... 4 Create and Manage... 5 Create a Cash Advance for Yourself...
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Claims Management. February 2016
 Claims Management February 2016 Overview Claim Submission Remittance Advice (RA) Exception Codes Exception Resolution Claim Status Inquiry Additional Information 2 Claim Submission 3 4 Life of a Claim
Claims Management February 2016 Overview Claim Submission Remittance Advice (RA) Exception Codes Exception Resolution Claim Status Inquiry Additional Information 2 Claim Submission 3 4 Life of a Claim
The claims will appear on the list in order of Date Created. The search criteria at the top of the list will assist you in locating past claims.
 P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
Next Year Budget Entry Monroe County, WI
 2014 Next Year Budget Entry Departments are responsible for submitting budget requests. This document outlines the entry of Next Year Budget Requests using Budget Detail entry and the submission of these
2014 Next Year Budget Entry Departments are responsible for submitting budget requests. This document outlines the entry of Next Year Budget Requests using Budget Detail entry and the submission of these
BT JUNE 20, 2002
 P R O V I D E R B U L L E T I N BT200231 JUNE 20, 2002 To: All Providers Subject: Overview This bulletin contains information from the Hoosier Healthwise Managed Care Program about how managed care entities
P R O V I D E R B U L L E T I N BT200231 JUNE 20, 2002 To: All Providers Subject: Overview This bulletin contains information from the Hoosier Healthwise Managed Care Program about how managed care entities
Your health savings account. User Guide
 Your health savings account User Guide UPMC Consumer Advantage health savings account Thank you for choosing the UPMC Consumer Advantage health savings account (HSA). We want to make it easy for you to
Your health savings account User Guide UPMC Consumer Advantage health savings account Thank you for choosing the UPMC Consumer Advantage health savings account (HSA). We want to make it easy for you to
Ambetter from Superior HealthPlan
 Ambetter from Superior HealthPlan 1/14/2016 This document does not meet accessibility standards. If you have questions about the information contained within, please contact Provider Services at 1-877-687-1196
Ambetter from Superior HealthPlan 1/14/2016 This document does not meet accessibility standards. If you have questions about the information contained within, please contact Provider Services at 1-877-687-1196
Product Eligibility and Pricing Services. Loan Originator User Guide
 Product Eligibility and Pricing Services Loan Originator User Guide Table of Contents Table of Contents Log In... 1 Enter New Loan Data... 1 Evaluate Products... 6 Analyze Search Results... 6 Update Search
Product Eligibility and Pricing Services Loan Originator User Guide Table of Contents Table of Contents Log In... 1 Enter New Loan Data... 1 Evaluate Products... 6 Analyze Search Results... 6 Update Search
Provider Orientation. style. Click to edit Master subtitle style. December, 2017
 Click EMHS to Employee edit Master Health title Plan Provider Orientation Click to edit Master subtitle December, 2017 Pam Hageny Director of Health Plan Operations & Provider Network Beacon Health EMHS
Click EMHS to Employee edit Master Health title Plan Provider Orientation Click to edit Master subtitle December, 2017 Pam Hageny Director of Health Plan Operations & Provider Network Beacon Health EMHS
Claims Claim Submission QUICK REFERENCE
 Claims Claim Submission QUICK REFERENCE This will review the process of how to submit a claim online and check the status of a previously submitted claim. Get Started 1. From, click Link and sign in NOTE:
Claims Claim Submission QUICK REFERENCE This will review the process of how to submit a claim online and check the status of a previously submitted claim. Get Started 1. From, click Link and sign in NOTE:
(MO HealthNet) Text Telephone Medical Claims Reimbursement Rate Dispute Medical Necessity Appeal. Attn: Claim Disputes
 KEY CONTACTS The following chart includes several important telephone and fax numbers available to your office. When calling, please have the following information available: NPI (National Provider Identifier)
KEY CONTACTS The following chart includes several important telephone and fax numbers available to your office. When calling, please have the following information available: NPI (National Provider Identifier)
Plan Overview 11/12/2014. Indiana QHP Marketplace Basics Ambetter from MHS. Ambetter from MHS Highlights 10/3/2014. Local and Experienced
 Indiana QHP Marketplace Basics 10/3/2014 Jo Nahod-Carlin Director, Marketing & Communications About MHS has been proudly serving Indiana residents for nearly two decades through Hoosier Healthwise and
Indiana QHP Marketplace Basics 10/3/2014 Jo Nahod-Carlin Director, Marketing & Communications About MHS has been proudly serving Indiana residents for nearly two decades through Hoosier Healthwise and
Section Eleven. Referrals and Prior Authorization REFERRAL PROCESS. Physician Referrals within Plan Network
 REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
Ambetter of Arkansas. Arkansas Medical Society 12 th Annual Insurance Conference October 1, /5/2015
 Ambetter of Arkansas Arkansas Medical Society 12 th Annual Insurance Conference October 1, 2015 AGENDA 1. Verification of Eligibility 2. Prior Authorization 3. Claims Submission 4. PaySpan 5. Ambetter
Ambetter of Arkansas Arkansas Medical Society 12 th Annual Insurance Conference October 1, 2015 AGENDA 1. Verification of Eligibility 2. Prior Authorization 3. Claims Submission 4. PaySpan 5. Ambetter
Claim Investigation Submission Guide
 Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Master User Manual. Last Updated: August, Released concurrently with CDM v.1.0
 Master User Manual Last Updated: August, 2010 Released concurrently with CDM v.1.0 All information in this manual referring to individuals or organizations (names, addresses, company names, telephone numbers,
Master User Manual Last Updated: August, 2010 Released concurrently with CDM v.1.0 All information in this manual referring to individuals or organizations (names, addresses, company names, telephone numbers,
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise.
 Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
1. Welcome to BenefitBridge. To access the BenefitBridge portal, login to BenefitBridge from the internet. 2. In the internet address bar, type:
 1. Welcome to BenefitBridge. To access the BenefitBridge portal, login to BenefitBridge from the internet. 2. In the internet address bar, type: www.benefitbridge.com/egusd 1 1. If you are a returning
1. Welcome to BenefitBridge. To access the BenefitBridge portal, login to BenefitBridge from the internet. 2. In the internet address bar, type: www.benefitbridge.com/egusd 1 1. If you are a returning
Published May Following these questions and answers, please find a guide to abbreviations and special terms.
 Frequently Asked Questions for Indiana FQHCs and RHCs: Working with Managed Care Entities / Health Plans Indiana Health Coverage Programs, Hoosier Healthwise and HIP Published May 2011 The Indiana Federally
Frequently Asked Questions for Indiana FQHCs and RHCs: Working with Managed Care Entities / Health Plans Indiana Health Coverage Programs, Hoosier Healthwise and HIP Published May 2011 The Indiana Federally
Prior Authorizations on the Provider Portal. July 2017
 Prior Authorizations on the Provider Portal July 2017 2 Disclaimer The information provided is current as of June 2017 and is subject to change. Stay current with up-to-date information on the OHCA public
Prior Authorizations on the Provider Portal July 2017 2 Disclaimer The information provided is current as of June 2017 and is subject to change. Stay current with up-to-date information on the OHCA public
During this section we will discuss: Washington Healthplanfinder Homepage Individual and Family Application Flow Household
 1 2 3 During this section we will discuss: Washington Healthplanfinder Homepage www.wahealthplanfinder.org Individual and Family Application Flow Household Composition and Tax Filing Status Premium Payments
1 2 3 During this section we will discuss: Washington Healthplanfinder Homepage www.wahealthplanfinder.org Individual and Family Application Flow Household Composition and Tax Filing Status Premium Payments
Claims Packaging Tool Servicer Support User Manual Version 1.0 Effective Date : 07/11/2018
 Claims Packaging Tool Servicer Support User Manual Version 1.0 Effective Date : 07/11/2018 Table of Contents Claims Packaging Tool (CPT) Overview...3 CPT Servicer Use... 3 Flow Chart and Timeline...4 Claims
Claims Packaging Tool Servicer Support User Manual Version 1.0 Effective Date : 07/11/2018 Table of Contents Claims Packaging Tool (CPT) Overview...3 CPT Servicer Use... 3 Flow Chart and Timeline...4 Claims
*This document is searchable.
 CCHP Prior Authorization List and Toll Free Phone Number 877-227-1142 Fax Number 414-266-4726 www. Childrenschp.com(childrenscommunityhealthplan.org) Utilization Provider Portal: provider.childrenscommunityhealthplan.org
CCHP Prior Authorization List and Toll Free Phone Number 877-227-1142 Fax Number 414-266-4726 www. Childrenschp.com(childrenscommunityhealthplan.org) Utilization Provider Portal: provider.childrenscommunityhealthplan.org
Clear Coverage Online Authorizations Community Health Network of CT, Inc.
 Clear Coverage Online Authorizations Community Health Network of CT, Inc. Overview Clear coverage is an online authorization tool which: Lowers authorization turn around time Improves workflow by decreasing
Clear Coverage Online Authorizations Community Health Network of CT, Inc. Overview Clear coverage is an online authorization tool which: Lowers authorization turn around time Improves workflow by decreasing
LZS PORTAL USER MANUAL BUDGET TRANSFER. MS Dynamic Portal Budget Transfer P a g e
 LZS BUDGET TRANSFER PORTAL USER MANUAL 1 P a g e REQUESTOR GUIDE 1. Open URL https://portalgp.zakatselangor.com.my/gpdbtportal/login.aspx 2. Choose Company and Login to portal using Email Id and given
LZS BUDGET TRANSFER PORTAL USER MANUAL 1 P a g e REQUESTOR GUIDE 1. Open URL https://portalgp.zakatselangor.com.my/gpdbtportal/login.aspx 2. Choose Company and Login to portal using Email Id and given
Seller Procedures Delegated. Seller Portal
 Seller Procedures Delegated 1 Seller Portal Summary 2 Introduction to the Seller Portal (EZCLD.LHFS.com) and review of the Loan Submission phases. TOOLS AND FUNCTIONALITY LeftNav Menu Loan Actions Menu
Seller Procedures Delegated 1 Seller Portal Summary 2 Introduction to the Seller Portal (EZCLD.LHFS.com) and review of the Loan Submission phases. TOOLS AND FUNCTIONALITY LeftNav Menu Loan Actions Menu
Seller Procedures Non-Delegated. Seller Portal
 Seller Procedures Non-Delegated 1 Seller Portal Summary 2 Introduction to the Seller Portal (EZCLD.LHFS.com) and review of the Loan Submission phases. TOOLS AND FUNCTIONALITY LeftNav Menu Loan Actions
Seller Procedures Non-Delegated 1 Seller Portal Summary 2 Introduction to the Seller Portal (EZCLD.LHFS.com) and review of the Loan Submission phases. TOOLS AND FUNCTIONALITY LeftNav Menu Loan Actions
Johns Hopkins HealthCare LLC
 Johns Hopkins HealthCare LLC Johns Hopkins Employer Health Programs (EHP) Presented by: by: Johns Hopkins HealthCare Provider Relations Department 11/14/2018 Agenda Welcome About JHHC Provider Website
Johns Hopkins HealthCare LLC Johns Hopkins Employer Health Programs (EHP) Presented by: by: Johns Hopkins HealthCare Provider Relations Department 11/14/2018 Agenda Welcome About JHHC Provider Website
Claim Adjustment Process. HP Provider Relations/October 2015
 Claim Adjustment Process HP Provider Relations/October 2015 Agenda Types of adjustments System-initiated adjustments Web interchange adjustment process Void feature Paper adjustment process Timely filing
Claim Adjustment Process HP Provider Relations/October 2015 Agenda Types of adjustments System-initiated adjustments Web interchange adjustment process Void feature Paper adjustment process Timely filing
FIND A DOCTOR Page 1 of 22
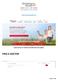 www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
Second quarter provider updates. July 2016
 Second quarter provider updates July 2016 Agenda Introductions Healthy Indiana Plan (HIP) debit card Claim disputes Behavioral health Updated Network Relations representatives map 2 HIP debit card - Background
Second quarter provider updates July 2016 Agenda Introductions Healthy Indiana Plan (HIP) debit card Claim disputes Behavioral health Updated Network Relations representatives map 2 HIP debit card - Background
QUICK TIP: Download a Quick Reference Guide from the Resource Center to help you use the PayFlex member website.
 [Date] Dear DTE Energy Retiree, It s our pleasure to welcome you to PayFlex! You re enrolled in a Retiree Reimbursement Account (RRA). Your RRA comes with some great tools to help you manage your account.
[Date] Dear DTE Energy Retiree, It s our pleasure to welcome you to PayFlex! You re enrolled in a Retiree Reimbursement Account (RRA). Your RRA comes with some great tools to help you manage your account.
ISMA Coalition Meeting September 13, 2013
 ISMA Coalition Meeting September 13, 2013 Questions and Answers 1. For OMPP and each MCE: When will all the Medicaid payers be able to accept electronic claims (837 files) for secondary claims with Primary
ISMA Coalition Meeting September 13, 2013 Questions and Answers 1. For OMPP and each MCE: When will all the Medicaid payers be able to accept electronic claims (837 files) for secondary claims with Primary
Medicaid Waiver Management Application. CDO Budget and Plan of Care Process Quick Reference Guide
 Medicaid Waiver Management Application CDO Budget and Plan of Care Process Quick Reference Guide Once an Individual has chosen the Consumer Directed Option (CDO), the Case Manager will need to complete
Medicaid Waiver Management Application CDO Budget and Plan of Care Process Quick Reference Guide Once an Individual has chosen the Consumer Directed Option (CDO), the Case Manager will need to complete
IHCP Annual Workshop October 2016
 IHCP Annual Workshop October 2016 MDwise CMS-1500 Billing and Claim Processing Exclusively serving Indiana families since 1994. Agenda Who is MDwise? Provider Enrollment: Are you a contracted MDwise Provider?
IHCP Annual Workshop October 2016 MDwise CMS-1500 Billing and Claim Processing Exclusively serving Indiana families since 1994. Agenda Who is MDwise? Provider Enrollment: Are you a contracted MDwise Provider?
