Healthy Indiana Plan (HIP) Provider Orientation
|
|
|
- Hubert Lee
- 6 years ago
- Views:
Transcription
1 Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation
2 Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories POWER account and copay Provider reimbursement Hospital assessment fee Hospital presumptive eligibility Coordination of benefits/ third-party liability (TPL) Contacts Questions and answers 2
3 HIP plans and coverage HIP Plus plan Includes: o Physician services o Inpatient and outpatient services o Prescription drugs o Routine dental, vision and chiropractic services o Pregnancy-related services Copays apply to nonemergent emergency room (ER) visits only POWER account contributions HIP Basic plan Includes: o Physician services o Inpatient and outpatient services o Prescription drugs o No routine dental, vision or chiropractic o Pregnancy-related services Copays apply to outpatient and inpatient services, preferred and nonpreferred drugs, and nonemergent ER visits 3
4 HIP plans and coverage (cont.) HIP State Plus plan Mirrors current Medicaid-covered services, including: o Chiropractic care o Nonemergent transportation o Routine dental and vision o Short-term skilled nursing facility stays (SNF) Copays apply to nonemergent ER visits POWER account contributions HIP State Basic plan Mirrors current Medicaid-covered services, including: o Chiropractic o Nonemergent transportation o Routine dental and vision o Short-term SNF stays Copays apply to outpatient and inpatient services, preferred and nonpreferred drugs, and nonemergent ER visits 4
5 Additional covered benefits Pharmacy Pharmacy services will be carved-in. Express Scripts, Inc. will provide pharmacy benefit management. Maternity coverage Maternity coverage will be added. If member is pregnant at enrollment or redetermination, they will be enrolled in HIP Maternity. Members who begin a new benefit year while pregnant on HIP will move to HIP Maternity. During pregnancy, members do not have copays, POWER Account contributions and POWER accounts are frozen. 5
6 Additional covered benefits (cont.) Dental Members in the HIP Plus plan and HIP State plans receive dental benefits. Plus product benefits are limited. Basic products do not include dental (except for members ages 19 and 20 and pregnant women). DentaQuest is the contracted administrator of HIP dental benefits. Vision Members in the HIP Plus plan and HIP State plans receive vision benefits: o One exam per year and one pair of glasses and lenses or contacts, if medically necessary, every two years. The HIP Basic plan does not include vision benefits (except for members under the age of 21 and pregnant women). VSP is the contracted administrator of vision benefits. 6
7 Eligibility Those 19 to 64 years old with income up to 138% of the federal poverty line (FPL) are eligible for HIP. There is no asset test. Eligibility is not impacted by availability of employer coverage. There is no waiting period for HIP, and coverage lasts for one year; then the member has to reapply. 7
8 Eligibility (cont.) Eligibility verification can be done using Availity at or the Provider Healthcare Portal at You can: Verify a member s HIP eligibility on date of service. Identify the HIP plan of the member. o The member s HIP product type and pregnancy status drives their benefit coverage. Verify member s medical care evaluation (MCE) for claim submission purposes. Confirm the reimbursement to be expected based on HIP eligibility (for example, Indiana Health Coverage Programs [IHCP] Medicaid fee-for-service FFS rates vs. Medicare rates). 8
9 Eligibility (cont.) HIP member ID card: Copays are not listed on the ID card; check the Availity Portal or call Provider Services to verify copay. Members will not receive new cards when they change products within the same benefit period. 9
10 Preferred medical provider (PMP) All members enrolled in HIP must have a PMP once a plan is selected. Availity identifies the member s PMP information, or provider s can call the Provider Helpline to obtain the member s PMP. Referrals are required the same as for HHW: o When a referral has been obtained, providers should enter the NPI of the member s PMP in box 17b of the CMS-1500 form (see the Provider Operations Manual for exceptions and complete instructions). For HIP PMPs, rosters are available through the provider website
11 HIP Plus HIP Plus is the best value and the preferred HIP plan. HIP Plus requires monthly affordable POWER account contributions. Copays apply to nonemergent ER visits only. HIP Plus covers all services currently covered under HIP Basic
12 HIP Plus (cont.) Additional covered services include: o Bariatric surgery. o Temporomandibular joint syndrome (under medical benefits). o 75 therapy visits per benefit period. o Dental. o Vision. o Chiropractic. o Transportation (as a value-added benefit) up to 20 one-way trips/unlimited for pregnant members
13 HIP Basic HIP Basic does not require monthly POWER account contributions. Required copays include: o Outpatient services (physicians/hospital): $4 per visit o Outpatient services (dental): $4 per service o Inpatient: $75 per admission o Preferred drugs: $4 per prescription o Nonpreferred drugs: $8 per prescription o ER for nonemergency visit: $
14 HIP Basic (cont.) HIP Basic includes essential health benefits and pregnancy coverage. HIP Basic does not include coverage for dental, vision, treatment of TMJ or bariatric surgery. o Exception includes coverage for pregnant members and 19- and 20-year-old members. There is a limit of 60 combined therapy visits per benefit period. Transportation is covered (as a value-added benefit) up to 20 one-way trips/unlimited for pregnant members
15 HIP State plan The HIP State plans are different from the HIP Plus and HIP Basic products. Members receive the same benefits as HHW. Pregnancy-related services are covered. Members designated as medically frail include: o Low-income parents or caretakers who previously would have been in HHW. o 19- and 20-year-old noncaretakers with the lowest income level. Pregnant members and Native American members do not have cost-sharing responsibilities, such as POWER account contributions and copays
16 HIP State plan products cost sharing HIP State Plus attributes: o Plus plan is the best value and the preferred HIP o Affordable monthly POWER account contributions o Monthly contributions the same as HIP Plus o ER copays only HIP State Basic attributes: o Copays the same as the regular HIP Basic o More services require copays o No POWER account contribution o Low-income parents/caretaker members 16 16
17 HIP State plan benefits There are no therapy limits. Bariatric surgery and TMJ are covered. Dental and vision coverage is the same as HHW: o HIP members receive two dental cleanings per year. o HIP members receive one vision exam per year and glasses every two years. Nonemergent transportation coverage is the same as HHW: o There is no limit on the number of trips, and coverage includes transport to health classes (Women, Infants, and Children, etc.)
18 Medically frail Medically frail includes those with a serious health condition/ situation, such as: Cancer, AIDS, aplastic anemia, diabetes with a comorbidity, coagulation defect, lipid storage disease or other primary immune deficiency. A disabling mental disorder. A chronic substance abuse disorder. A physical, intellectual or developmental disability that significantly impairs the individual s ability to perform one or more activities of daily living. Being disabled based on Social Security Administration criteria. Requiring an organ transplant
19 Medically frail guidelines Milliman Underwriting Guidelines (MUG) are used to quantify the seriousness of a member s condition. MUG utilizes a point system based on diagnosis, key medical indicators and medications. The rating is intended to project the level-of-care the member is likely to require for the next 12 months. Members are validated as medically frail when their MUG total meets one of the following criteria: o 150 points for physical condition o 75 points for behavioral or substance abuse condition 19 19
20 Member categories Pregnant women: Pregnant women will not have cost sharing in either HIP Plus or HIP Basic once their pregnancy is reported, and they will receive additional benefits available only to pregnant women. Native Americans: By federal law, Native Americans are exempt from cost sharing; they can receive HIP benefits without required contributions or ER copays
21 Pregnant members and HIP Maternity Pregnant HIP members move to HIP Maternity. At their annual HIP redetermination, HIP members due for redetermination during their pregnancy will move to HIP Maternity until they complete their two-month postpartum period. HIP Maternity allows the member to continue with the same experience as if eligible for HIP. Members will have State plan benefits. HIP Maternity members will receive new member ID cards
22 POWER account HIP Plus and HIP State Plus members have a $2,500 POWER account. Pregnant members will have their POWER account frozen, and no services will be charged during their pregnancy. Preventive services are exempt from being paid from the POWER account and are paid by the health plan. The new Presumptive Eligibility plan does not have a POWER account. Dental, vision and pharmacy services must be paid from POWER accounts
23 POWER account (cont.) HIP Plus and HIP State Plus members are required to pay monthly contributions in one of five PAC tiers based on income (except during pregnancy). Members who use tobacco products will be assessed and additional surcharge of 50% on their POWER Account. Initial payment must be made within 60 days of enrollment. No benefits are paid during conditional status. members cannot access health care until they make their first POWER account payment. Note: HIP Basic plan members also have POWER accounts but are not required to make contributions
24 POWER account (cont.) POWER account tiers Tiers Monthly PAC single person Tier 1 Tier 2 Tier 3 Tier 4 Tier 5 Monthly PAC spouses PAC with tobacco surcharge Spouse PAC when one has tobacco surcharge $1 $1 $1.50 $1 and $1.50 $1.50 $5 $2.50 $7.50 $2.50 and $3.75 $3.75 $10 $5 $15 $5 and $7.50 $7.50 $15 $7.50 $22.50 $7.50 and $11.25 $11.25 $20 $10 $30 $10 and $15 $15 Spouse PAC when both have tobacco surcharge 24 24
25 POWER account (cont.) Members whose income is greater than 100% of the FPL and become more than 60 days delinquent will be termed and must wait six months to reapply. Members whose income is equal to or less than 100% of the FPL are moved to HIP Basic benefits if they become more than 60 days delinquent
26 HIP Plus POWER account rollover At the end of the 12-month benefit period, a portion of unused POWER account funds may be rolled over to the next benefit year; this determination is done 120 days into the next benefit period. HIP Plus members receive rollover credit for the unused balance of their POWER account funds that they contributed. Members who have had their required preventive service(s) receive double credit; the total credit can t be more than the 12-month total of their required contribution for the new benefit year
27 HIP Basic POWER account rollover At the end of the 12-month benefit year, a portion of unused POWER account funds may be rolled over to the next year; this determination is done 120 days into the next benefit year. HIP Basic members receive rollover credit only if they have had their required preventive service(s). Members can use the credit to reduce the amount they need to contribute if they move to HIP Plus for the next benefit year. The amount of credit is the percentage of the remaining POWER account balance; the total reduction can t be more than 50% of their required annual contribution
28 Copays HIP products require ER copays for nonemergent use of the ER. The copay is $8. The copay is waived if a prudent lay person judges the visit as emergent or the member is admitted from the ER. The ER copay is also waived if the member calls our 24/7 NurseLine first and is advised to go to the ER
29 Copays (cont.) HIP Basic requires additional copays: o Inpatient: $75 per admission o Outpatient services (physicians/hospital): $4 per visit o Outpatient services (dental for members who are pregnant or years of age): $4 per service o Preferred drugs: $4 per prescription o Nonpreferred drugs: $8 per prescription 29 29
30 Copays (cont.) Copays are due at the time of service. No copays are required for preventive care, family planning, maternity services and any service when the member is pregnant (through 60 days postpartum). HIP members can t use their POWER account to pay any copay
31 Assessing HIP Basic copays Example A: Member has an office visit and is then sent to the hospital for CT scan and to the lab for multiple tests. Total copay: $12 member has $4 copay for office visit, $4 copay for hospital CT scan and a single $4 copay for lab services
32 Assessing HIP Basic copays (cont.) Example B: Member has an office visit, and an X-ray and three lab tests are done in the physician s office. Total copay: $4 office visit and services by a single provider at a single location are treated as a single visit
33 Assessing HIP Basic copays (cont.) Example C: Member has a dental visit with screening X-rays, teeth cleaning and three fillings. Total copay: $4 screening X-rays and cleanings are preventive and do not have copays; single $4 copay for the three fillings
34 Assessing HIP Basic copays (cont.) Example D: Member has dental visit for three fillings and a crown fitting. Total copay: $8 dental services require $4 for each type of service rendered
35 Assessing HIP Basic copays (cont.) Example E: Member has three preferred prescriptions filled at pharmacy. Total copay: $12 member has $4 copay for each preferred prescription
36 Provider reimbursement HIP medical claims are paid at Medicare rates.* When an HIP service is covered, and there is no Medicare rate, Anthem will pay 130% of the Medicaid rate (see the Medicaid fee schedule on the IHCP website). * Hospital claims (inpatient and outpatient) for members in the low-income parent/caretaker plans are paid at Medicaid rates, and hospitals also receive hospital assessment fee (HAF) payments
37 Hospital assessment fee The Indiana Family and Social Services Administration (FSSA) implemented an HAF in accordance with Public Law , Section 281, as enacted by the 2011 session of the Indiana General Assembly. HAF permits inpatient and outpatient aggregate claims payment at the upper Medicare payment limits without exceeding them
38 Hospital assessment fee (cont.) In-state acute care hospitals licensed under IC and freestanding psychiatric hospitals licensed under IC are subject to HAF. Outpatient laboratory services (codes listed on the Medicare clinical laboratory fee schedule) are not subject to the HAF increase
39 Hospital assessment fee (cont.) Per IHCP Bulletin BT201608, dated January 26, 2016, HAF adjustments will be applied to reimbursements for HIP member services. IHCP modified HAF payment distributions to include increased reimbursement to eligible hospitals for services provided to all HIP members, including presumptive eligibility HIP members. HIP managed care entities (MCEs) will apply HAF adjustment factors accordingly when adjudicating claims. Non-HAF eligible hospitals will continue to be reimbursed applying current rates and methodologies
40 Hospital presumptive eligibility What benefits do presumptively eligible individuals receive? Presumptively eligible individuals receive Presumptive Eligibility Basic, which is equivalent to HIP Basic and has no vision or dental services. Presumptively eligible individuals are placed into MCE. Presumptively eligible individuals must apply for full coverage within 60 days
41 Hospital presumptive eligibility (cont.) What costs will hospital presumptive eligibility adult members need to pay? Copays are the same as HIP Basic. Copay is due at time of service. Note, these individuals do not have a POWER account
42 Hospital presumptive eligibility (cont.) When does coverage begin? The coverage period for hospital presumptive eligibility begins on the date the qualified provider makes determination the individual is presumptively eligible. The effective date is not the date individual first receives care
43 Hospital presumptive eligibility (cont.) Hospital staff asks individual questions to complete hospital presumptive eligibility application. If found eligible for hospital presumptive eligibility, individual determined presumptively eligible for up to 60 days. Individual receives a recipient identification number (RID) to use on Indiana Application for Health Coverage. If not found eligible for hospital presumptive eligibility, health plan Web application will deny eligibility and denial letter will be printed for applicant. If over 65 years of age and a parent/caretaker of a child under the age of 18, individual will be placed in MAHP (presumptive eligibility for parent/caretakers). If hospital presumptive eligibility adult, individual placed in MAHA (hospital presumptive eligibility for adults) and approval notice printed for applicant to use as proof of eligibility. Individual selects MCE or is auto-assigned. They must submit Indiana Application for Health Coverage to maintain benefits. No POWER account contribution required. Individual may reapply at any time. No appeal rights
44 Hospital presumptive eligibility (cont.) Why is hospital presumptive eligibility important? Hospital presumptive eligibility allows individuals to obtain health care while the Indiana Application for Health Coverage is being processed. Hospital presumptive eligibility allows providers to be reimbursed for services provided immediately after hospital presumptive eligibility approval. During the presumptive eligibility period, the individual will be able to receive treatment from other IHCP providers after they leave the hospital
45 Hospital presumptive eligibility (cont.) To qualify for adult hospital presumptive eligibility, applicant must: Be a U.S. citizen, a permanent resident in the U.S. for at least five years or a qualified alien. Be an Indiana resident. Not be incarcerated. Not be covered under presumptive eligibility for pregnant women. Not a hospital presumptive eligibility recipient in the previous 12 months. Not enrolled in the IHCP. Be under 138% of the FPL
46 Coordination of benefits/tpl Members enrolled in HIP may have other insurance at the time of service that Anthem and the state are not aware of; coordination of benefits must take place, and there will continue to be coordination of TPL for accidents. Anthem will recoup claims paid if a member had other insurance, and providers have six months from the date of the recoupment notification to submit claims. Providers may not pursue reimbursement from the member for any reason
47 HIP contacts HIP Provider Services: Member Services: (TTY 711) 24/7 NurseLine: (TTY 711) Submit claims to: Mailstop: IN999 P.O. Box Indianapolis, IN
48 HIP contacts (cont.) Medical and pharmacy precertification: VSP (vision): DentaQuest (dental): Transportation:
49 Thank you is the trade name of Anthem Insurance Companies, Inc., independent licensee of the Blue Cross and Blue Shield Association. ANTHEM is a registered trademark of Anthem Insurance Companies, Inc. The Blue Cross and Blue Shield names and symbols are registered marks of the Blue Cross and Blue Shield Association. Express Scripts, Inc. is a separate company that provides pharmacy services and pharmacy benefit management services on behalf of health plan members. AINPEC December
Healthy Indiana Plan 2.0 Special Populations
 Healthy Indiana Plan 2.0 Special Populations Objectives After reviewing this presentation you will understand: HIP 2.0 features, options, benefits, and cost sharing Different options, enrollment, benefits,
Healthy Indiana Plan 2.0 Special Populations Objectives After reviewing this presentation you will understand: HIP 2.0 features, options, benefits, and cost sharing Different options, enrollment, benefits,
The value of Healthy Indiana Plan (HIP) Plus Getting the most value from HIP
 Serving Hoosier Healthwise, Healthy Indiana Plan The value of Healthy Indiana Plan (HIP) Plus Getting the most value from HIP The value of HIP Plus HIP Plus gives members more bang for their buck! (Anthem)
Serving Hoosier Healthwise, Healthy Indiana Plan The value of Healthy Indiana Plan (HIP) Plus Getting the most value from HIP The value of HIP Plus HIP Plus gives members more bang for their buck! (Anthem)
Presumptive Eligibility. Last Updated: February 20, 2018
 Presumptive Eligibility Last Updated: February 20, 2018 Agenda Presumptive Eligibility Overview Covered Benefits Qualified Providers (QPs) How to Become a QP Completing the PE Application Other Resources
Presumptive Eligibility Last Updated: February 20, 2018 Agenda Presumptive Eligibility Overview Covered Benefits Qualified Providers (QPs) How to Become a QP Completing the PE Application Other Resources
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates
 Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
Emergency Services INDIANA HEALTH COVERAGE PROGRAMS. Copyright 2017 DXC Technology Company. All rights reserved.
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Emergency Services L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 2 5 P U B L I S H E D : N O V E M B E R 1 6, 2 0 1 7 P O L
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Emergency Services L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 2 5 P U B L I S H E D : N O V E M B E R 1 6, 2 0 1 7 P O L
Cost if you use a Non-Network Provider. Cost if you use an In-Network Provider. Covered Medical Benefits
 Anthem Blue Cross Life and Health Insurance Company Student Health Plan: Samuel Merritt University Your Plan: Custom PPO 300/20/40/20 Your Network: Prudent Buyer PPO This summary of benefits is a brief
Anthem Blue Cross Life and Health Insurance Company Student Health Plan: Samuel Merritt University Your Plan: Custom PPO 300/20/40/20 Your Network: Prudent Buyer PPO This summary of benefits is a brief
MDwise Annual IHCP Seminar. Exclusively serving Indiana families since 1994.
 MDwise 101 2016 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda MDwise history IHCP Overview MDwise Delivery System Model IHCP Program Overview Hoosier Healthwise Healthy Indiana
MDwise 101 2016 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda MDwise history IHCP Overview MDwise Delivery System Model IHCP Program Overview Hoosier Healthwise Healthy Indiana
Anthem Blue Cross Your Plan: Anthem Elements Choice PPO 6500 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Anthem Elements Choice PPO 6500 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage,
Anthem Blue Cross Your Plan: Anthem Elements Choice PPO 6500 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage,
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Anthem Blue Cross Your Plan: Classic PPO 250/20/20 (Essential Formulary $5/$15/$30/$50/30%) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Classic PPO 250/20/20 (Essential Formulary $5/$15/$30/$50/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you
Anthem Blue Cross Your Plan: Classic PPO 250/20/20 (Essential Formulary $5/$15/$30/$50/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you
Cost if you use an In-Network Provider. Cost if you use a Non-Network Provider. Covered Medical Benefits. $18,000 single / $36,000 family
 Anthem Blue Cross Your Plan: Anthem Elements Choice EQ PPO 6000 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage,
Anthem Blue Cross Your Plan: Anthem Elements Choice EQ PPO 6000 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage,
California State University Risk Management Authority
 Anthem Blue Cross Your Plan: Custom Premier PPO 500/20/80/60 Your Network: Prudent Buyer PPO California State University Risk Management Authority This summary of benefits is a brief outline of coverage,
Anthem Blue Cross Your Plan: Custom Premier PPO 500/20/80/60 Your Network: Prudent Buyer PPO California State University Risk Management Authority This summary of benefits is a brief outline of coverage,
Division of Family Resources
 Our mission is to develop, finance and compassionately administer programs to provide health care and other social services to Hoosiers in need in order to enable them to achieve healthy, self-sufficient
Our mission is to develop, finance and compassionately administer programs to provide health care and other social services to Hoosiers in need in order to enable them to achieve healthy, self-sufficient
Anthem Blue Cross Your Plan: Classic PPO 1000/35/20 (Essential Formulary $5/$20/$30/$50/30%) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Classic PPO 1000/35/20 (Essential Formulary $5/$20/$30/$50/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you
Anthem Blue Cross Your Plan: Classic PPO 1000/35/20 (Essential Formulary $5/$20/$30/$50/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you
Your Plan: Anthem Preferred DirectAccess gpaf Your Network: BlueCare
 Your Plan: Anthem Preferred DirectAccess gpaf Your Network: BlueCare This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
Your Plan: Anthem Preferred DirectAccess gpaf Your Network: BlueCare This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
Anthem Blue Cross Your Plan: Custom Classic PPO 500/20/20 (RX $5/$10/$25/30%) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Custom Classic PPO 500/20/20 (RX $5/$10/$25/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Custom Classic PPO 500/20/20 (RX $5/$10/$25/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection
IHCP Annual Workshop October 2017
 IHCP Annual Workshop October 2017 MDwise 101 HHW-HIPP0519( 10/17) Exclusively serving Indiana families since 1994. Agenda MDwise History IHCP Overview MDwise Delivery System Model IHCP Program Overview
IHCP Annual Workshop October 2017 MDwise 101 HHW-HIPP0519( 10/17) Exclusively serving Indiana families since 1994. Agenda MDwise History IHCP Overview MDwise Delivery System Model IHCP Program Overview
Anthem Blue Cross Your Plan: Modified Classic PPO 250/20/20 Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Modified Classic PPO 250/20/20 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Modified Classic PPO 250/20/20 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Your Plan: 2018 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO
 Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2018 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2018 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
Your Plan: 2017 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO
 Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2017 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2017 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
Your Plan: Custom Premier PPO 300/20/20 (Medicare) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Custom Premier PPO 300/20/20 (Medicare) Your Network: Prudent Buyer PPO City of Santa Rosa This summary of benefits is a brief outline of coverage, designed to help you with
Anthem Blue Cross Your Plan: Custom Premier PPO 300/20/20 (Medicare) Your Network: Prudent Buyer PPO City of Santa Rosa This summary of benefits is a brief outline of coverage, designed to help you with
Anthem Blue Cross Your Plan: Modified Classic PPO 500/30/20 (PHBP CLASSIC PLUS PPO) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Modified Classic PPO 500/30/20 (PHBP CLASSIC PLUS PPO) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the
Anthem Blue Cross Your Plan: Modified Classic PPO 500/30/20 (PHBP CLASSIC PLUS PPO) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the
Auxiliary Organizations Association
 Auxiliary Organizations Association Your Plan: Modified Premier PPO 500/20/80/60 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Auxiliary Organizations Association Your Plan: Modified Premier PPO 500/20/80/60 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Cost if you use an In-Network Provider. Cost if you use a Non-Network Provider. Covered Medical Benefits
 Anthem Blue Cross Life and Health Insurance Company Your Plan: Solution PPO 1500/15/20 (Essential Formulary $5/$20/$40/$60/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline
Anthem Blue Cross Life and Health Insurance Company Your Plan: Solution PPO 1500/15/20 (Essential Formulary $5/$20/$40/$60/30%) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline
Anthem Blue Cross Your Plan: Classic PPO - Active Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Classic PPO - Active Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Classic PPO - Active Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Your Plan: 2017 Classic PPO Plan (1VYV) - Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO
 Page 1 of 6 Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2017 Classic PPO Plan (1VYV) - Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits
Page 1 of 6 Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2017 Classic PPO Plan (1VYV) - Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits
Your Plan: 2018 Advantage PPO Plan (S828 and Z0KC) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: 2018 Advantage PPO Plan (S828 and Z0KC) Your : Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: 2018 Advantage PPO Plan (S828 and Z0KC) Your : Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection
HealthKeepers, Inc. Your Plan: Anthem HealthKeepers Platinum OAPOS 10/0%/3000 Your Network: HealthKeepers
 HealthKeepers, Inc. Your Plan: Anthem HealthKeepers Platinum OAPOS 10/0%/3000 Your Network: HealthKeepers This summary of benefits is a brief outline of coverage, designed to help you with the selection
HealthKeepers, Inc. Your Plan: Anthem HealthKeepers Platinum OAPOS 10/0%/3000 Your Network: HealthKeepers This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Custom Classic HMO 20/250 Admit (Rx $15/$30/$45/$45) Your Network: Select HMO
 Anthem Blue Cross Your Plan: Custom Classic HMO 20/250 Admit (Rx $15/$30/$45/$45) Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Custom Classic HMO 20/250 Admit (Rx $15/$30/$45/$45) Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Custom Value Deductible HMO $100 30/40/10% Your Network: Select HMO
 Anthem Blue Cross Your Plan: Custom Value Deductible HMO $100 30/40/10% Your : Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Custom Value Deductible HMO $100 30/40/10% Your : Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Modified Anthem PPO HSA-H 2000/ /40 Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Modified Anthem PPO HSA-H 2000/6000 20/40 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Modified Anthem PPO HSA-H 2000/6000 20/40 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
OVERVIEW OF YOUR BENEFITS
 OVERVIEW OF YOUR BENEFITS 9 IMPORTANT PHONE NUMBERS Rochester Benefit Fund Office (585) 244-0830 For questions about eligibility, Coordination of Benefits, your 1199SEIU Health Benefits ID card, prescription
OVERVIEW OF YOUR BENEFITS 9 IMPORTANT PHONE NUMBERS Rochester Benefit Fund Office (585) 244-0830 For questions about eligibility, Coordination of Benefits, your 1199SEIU Health Benefits ID card, prescription
Cost if you use a Non-Network Provider. Cost if you use an In-Network Provider. Covered Medical Benefits
 Anthem Blue Cross California State University Risk Management Authority Your Plan: Custom Premier HMO 20/200 admit/100 OP (Custom Rx $5/$20/$60/20%) Your Network: California Care HMO This summary of benefits
Anthem Blue Cross California State University Risk Management Authority Your Plan: Custom Premier HMO 20/200 admit/100 OP (Custom Rx $5/$20/$60/20%) Your Network: California Care HMO This summary of benefits
Your Plan: 2019 Classic PPO Plan (1122 and ZOJZ) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: 2019 Classic PPO Plan (1122 and ZOJZ) Your Network: Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the
Anthem Blue Cross Your Plan: 2019 Classic PPO Plan (1122 and ZOJZ) Your Network: Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the
Your Plan: 2019 Classic PPO Plan (1122 and ZOJZ) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: 2019 Classic PPO Plan (1122 and ZOJZ) Your Network: Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the
Anthem Blue Cross Your Plan: 2019 Classic PPO Plan (1122 and ZOJZ) Your Network: Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the
Your Plan: Anthem HealthKeepers Essential Guided Access Plus w/dental gcpa Your Network: HealthKeepers
 Your Plan: Anthem HealthKeepers Essential Guided Access Plus w/dental gcpa Your Network: HealthKeepers This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Your Plan: Anthem HealthKeepers Essential Guided Access Plus w/dental gcpa Your Network: HealthKeepers This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Modified Premier HMO 15/100% (Essential formulary $5/$15/$25/$45/30%) Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Modified Premier HMO 15/100% (Essential formulary $5/$15/$25/$45/30%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to
Anthem Blue Cross Your Plan: Modified Premier HMO 15/100% (Essential formulary $5/$15/$25/$45/30%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to
Program Update. October 26, 2017
 Program Update October 26, 2017 HIP Waiver Extension Submitted extension request in January 2017 Amendment filed in July 2017. State is in negotiations with CMS for waiver changes. Waiver content is subject
Program Update October 26, 2017 HIP Waiver Extension Submitted extension request in January 2017 Amendment filed in July 2017. State is in negotiations with CMS for waiver changes. Waiver content is subject
Anthem Blue Cross Your Plan: Classic HMO 20/40/250 Admit /125 OP ($5/$15/$30/$50/30%) Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Classic HMO 20/40/250 Admit /125 OP ($5/$15/$30/$50/30%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with
Anthem Blue Cross Your Plan: Classic HMO 20/40/250 Admit /125 OP ($5/$15/$30/$50/30%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with
RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER COVERKIDS TABLE OF CONTENTS
 RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER 1200-13-21 COVERKIDS TABLE OF CONTENTS 1200-13-21-.01 Scope and Authority 1200-13-21-.02 Definitions 1200-13-21-.03
RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER 1200-13-21 COVERKIDS TABLE OF CONTENTS 1200-13-21-.01 Scope and Authority 1200-13-21-.02 Definitions 1200-13-21-.03
Anthem Blue Cross Your Plan: Anthem PPO HSA 2700/0 Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Anthem PPO HSA 2700/0 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Anthem PPO HSA 2700/0 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Value HMO 30/40/30% Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Value HMO 30/40/30% Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Anthem Blue Cross Your Plan: Value HMO 30/40/30% Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Anthem Blue Cross Your Plan: Value HMO 30/40/30% Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Value HMO 30/40/30% Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Anthem Blue Cross Your Plan: Value HMO 30/40/30% Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Anthem Blue Cross Your Plan: Custom Anthem HSA /40 Embedded (HSA291) - Actives Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Custom Anthem HSA 2700 20/40 Embedded (HSA291) - Actives Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with
Anthem Blue Cross Your Plan: Custom Anthem HSA 2700 20/40 Embedded (HSA291) - Actives Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with
Your Plan: 2018 Classic PPO Plan (1122 and ZOJZ) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: 2018 Classic PPO Plan (1122 and ZOJZ) Your : Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: 2018 Classic PPO Plan (1122 and ZOJZ) Your : Prudent Buyer PPO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Modified Anthem Elements Choice HMO 5900 Your Network: Select HMO
 Anthem Blue Cross Your Plan: Modified Anthem Elements Choice HMO 5900 Your : Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Modified Anthem Elements Choice HMO 5900 Your : Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Modified Value HMO 30/40/30% Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Modified Value HMO 30/40/30% Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Modified Value HMO 30/40/30% Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Lumenos HSA 2000/ /40 (LHSA2153) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Lumenos HSA 2000/4000 20/40 (LHSA2153) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Lumenos HSA 2000/4000 20/40 (LHSA2153) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Your Plan: 2018 HMO Plan (2940) Your Network: California Care HMO
 Anthem Blue Cross Your Plan: 2018 HMO Plan (2940) Your : California Care HMO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: 2018 HMO Plan (2940) Your : California Care HMO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Anthem Elements Choice HMO 1500 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Select HMO
 Anthem Blue Cross Your Plan: Anthem Elements Choice HMO 1500 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed
Anthem Blue Cross Your Plan: Anthem Elements Choice HMO 1500 (Essential Formulary $5/$20/$50/$65/30% $500 Deductible) Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed
Your Guide to Kentucky HEALTH
 Your Guide to Kentucky HEALTH Your Guide to Kentucky HEALTH Kentucky has changed the way Medicaid works for some people. The state s new program is called Kentucky HEALTH. Kentucky HEALTH offers health
Your Guide to Kentucky HEALTH Your Guide to Kentucky HEALTH Kentucky has changed the way Medicaid works for some people. The state s new program is called Kentucky HEALTH. Kentucky HEALTH offers health
Anthem Blue Cross Your Plan: Custom Premier HMO 25/100% (Custom $5/$20/$30/$50/30%) Your Network: Select HMO
 Anthem Blue Cross Your Plan: Custom Premier HMO 25/100% (Custom $5/$20/$30/$50/30%) Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: Custom Premier HMO 25/100% (Custom $5/$20/$30/$50/30%) Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: ALADS Custom Classic PPO Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: ALADS Custom Classic PPO Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: ALADS Custom Classic PPO Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Classic HMO 20/40/250 Admit /125 OP Your Network: Select HMO
 Anthem Blue Cross Your Plan: Classic HMO 20/40/250 Admit /125 OP Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Classic HMO 20/40/250 Admit /125 OP Your Network: Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
LVAIC-Muhlenberg College: Lehigh Valley Flex Blue PPO Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkblueshield.com or by calling 1-800-345-3806.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkblueshield.com or by calling 1-800-345-3806.
Anthem Blue Cross Your Plan: Premier HMO 20/200 admit/100 OP (Essential Formulary $10/$25/$45/30%) Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Premier HMO 20/200 admit/100 OP (Essential Formulary $10/$25/$45/30%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to
Anthem Blue Cross Your Plan: Premier HMO 20/200 admit/100 OP (Essential Formulary $10/$25/$45/30%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to
Anthem Blue Cross of California Your Contract Code: 302G Your Plan: Anthem Gold PPO 20/30%/6500 Your Network: Prudent Buyer PPO
 Anthem Blue Cross of California Your Contract Code: 302G Your Plan: Anthem Gold PPO 20/30%/6500 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help
Anthem Blue Cross of California Your Contract Code: 302G Your Plan: Anthem Gold PPO 20/30%/6500 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help
Auxiliary Organizations Association
 Auxiliary Organizations Association Your Plan: Modified Premier HMO 20/200 admit/100 OP (Modified RX $5/$20/$60/20%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage,
Auxiliary Organizations Association Your Plan: Modified Premier HMO 20/200 admit/100 OP (Modified RX $5/$20/$60/20%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage,
MHS Updates Summer PR.P.PP
 MHS Updates Summer 2017 0517.PR.P.PP Updates Important to You Prior Authorization (PA) Updates DME Changes Therapy Authorization Process MHS Prior Authorization 101 Home Health MHS Occurrence Prior Authorization
MHS Updates Summer 2017 0517.PR.P.PP Updates Important to You Prior Authorization (PA) Updates DME Changes Therapy Authorization Process MHS Prior Authorization 101 Home Health MHS Occurrence Prior Authorization
Anthem Blue Cross Effective: January 1, 2018 Your Plan: University of California UC Care Plan Your Network: UC Select and Anthem Preferred
 Anthem Blue Cross Effective: January 1, 2018 Your Plan: University of California UC Care Plan Your Network: UC Select and Anthem Preferred This summary of benefits is a brief outline of coverage, designed
Anthem Blue Cross Effective: January 1, 2018 Your Plan: University of California UC Care Plan Your Network: UC Select and Anthem Preferred This summary of benefits is a brief outline of coverage, designed
Anthem Blue Cross Your Plan: Premier HMO 10/100% - MUST Trust Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Premier HMO 10/100% - MUST Trust Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Premier HMO 10/100% - MUST Trust Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Lumenos HSA 1500/ /30 (LHSA497H) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Lumenos HSA 1500/4500 10/30 (LHSA497H) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Lumenos HSA 1500/4500 10/30 (LHSA497H) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
$200 individual/$400 family combined network and out-of-network.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 New Castle County Government : Blue Choice PPO Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 New Castle County Government : Blue Choice PPO Coverage for: Individual/Family
Your Plan: Anthem Silver Blue Access Choice 5000/20%/6600 Your Network: Blue Access Choice
 Your Plan: Anthem Silver Blue Access Choice 5000/20%/6600 Your Network: Blue Access Choice This summary of benefits is a brief outline of coverage, designed to help y ou with the selection process. This
Your Plan: Anthem Silver Blue Access Choice 5000/20%/6600 Your Network: Blue Access Choice This summary of benefits is a brief outline of coverage, designed to help y ou with the selection process. This
Anthem Blue Cross Your Plan: CSEBO HMO 10 (Custom Premier HMO 10/100%) Your Network: California Care HMO
 Anthem Blue Cross Your Plan: CSEBO HMO 10 (Custom Premier HMO 10/100%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross Your Plan: CSEBO HMO 10 (Custom Premier HMO 10/100%) Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Important Questions. Why this Matters:
 Important Questions What is the overall deductible? This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/calpers
Important Questions What is the overall deductible? This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/calpers
What is the overall deductible?
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/2018 6/30/2019 WEA Trust Essential Health Plan: Kenosha School District Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/2018 6/30/2019 WEA Trust Essential Health Plan: Kenosha School District Coverage for: Individual/Family
OPERATING ENGINEERS HEALTH & WELFARE FUND BENEFIT PLANS SUMMARY COMPARISON FOR ACTIVES and EARLY RETIREES
 PPO Plan For Non-PPO Providers Employee Premium None None None None None Explanation of Plans and Options Available to You Deductible Annual Out-of-Pocket Maximum Medical and ¹Pediatric Dental & Vision
PPO Plan For Non-PPO Providers Employee Premium None None None None None Explanation of Plans and Options Available to You Deductible Annual Out-of-Pocket Maximum Medical and ¹Pediatric Dental & Vision
Your Plan: Lumenos HSA Embedded Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Lumenos HSA Embedded Your Network: Prudent Buyer PPO City of Chico This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Lumenos HSA Embedded Your Network: Prudent Buyer PPO City of Chico This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Your Plan: BCBSHP Preferred DirectAccess Plus groayour Network: Blue Open Access POS 10PK G-OAP2F 500/20 5K
 Your Plan: BCBSHP Preferred DirectAccess Plus groayour Network: Blue Open Access POS 10PK G-OAP2F 500/20 5K This summary of benefits is a brief outline of coverage, designed to help you with the selection
Your Plan: BCBSHP Preferred DirectAccess Plus groayour Network: Blue Open Access POS 10PK G-OAP2F 500/20 5K This summary of benefits is a brief outline of coverage, designed to help you with the selection
1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs
 1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Rochester Area Employers
1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Rochester Area Employers
John J. Wernert, MD FSSA Secretary
 John J. Wernert, MD FSSA Secretary Healthy Indiana Plan True Medicaid Reform First Medicaid plan with strong consumerdirected features (2008) HDHP POWER Account Consumer choice + Provider engagement Proven
John J. Wernert, MD FSSA Secretary Healthy Indiana Plan True Medicaid Reform First Medicaid plan with strong consumerdirected features (2008) HDHP POWER Account Consumer choice + Provider engagement Proven
Your Plan: Anthem Silver PPO 3400/0%/3400 w/hsa Your Network: Anthem PPO
 Your Plan: Anthem Silver PPO 3400/0%/3400 w/hsa Your Network: Anthem PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Your Plan: Anthem Silver PPO 3400/0%/3400 w/hsa Your Network: Anthem PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Your Plan: Anthem HealthKeepers Preferred DirectAccess gqqa Your Network: HealthKeepers Open Access
 Your Plan: Anthem HealthKeepers Preferred DirectAccess gqqa Your Network: HealthKeepers Open Access This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Your Plan: Anthem HealthKeepers Preferred DirectAccess gqqa Your Network: HealthKeepers Open Access This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem BlueCross BlueShield Christian Care Communities Blue Access PPO Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Anthem Blue Cross of California Your Plan: Anthem Gold HMO 40/20%/6500 Your Network: California Care HMO
 Anthem Blue Cross of California Your Plan: Anthem Gold HMO 40/20%/6500 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross of California Your Plan: Anthem Gold HMO 40/20%/6500 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
SDMGMA Third Party Payer Day. Chelsea King, Policy Analyst
 SDMGMA Third Party Payer Day Chelsea King, Policy Analyst Agenda Medicaid Overview Third Party Liability Common TPL Errors NDC Claims Processing Anesthesia Claims Online Portal Q & A Medicaid Overview
SDMGMA Third Party Payer Day Chelsea King, Policy Analyst Agenda Medicaid Overview Third Party Liability Common TPL Errors NDC Claims Processing Anesthesia Claims Online Portal Q & A Medicaid Overview
Anthem Blue Cross Your Plan: Premier HMO 15/100% (RX $10/$20/$35) Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Premier HMO 15/100% (RX $10/$20/$35) Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross Your Plan: Premier HMO 15/100% (RX $10/$20/$35) Your : California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Your Plan: Anthem Premier DirectAccess gwaa Your Network: KeyCare
 Your Plan: Anthem Premier DirectAccess gwaa Your Network: KeyCare This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
Your Plan: Anthem Premier DirectAccess gwaa Your Network: KeyCare This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
Anthem Blue Cross Your Plan: Value HMO 30/40/500/3 day Your Network: Priority Select HMO
 Anthem Blue Cross Your Plan: Value HMO 30/40/500/3 day Your : Priority Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Value HMO 30/40/500/3 day Your : Priority Select HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
2018 Medical Comparison Guide
 2018 Medical Comparison Guide This and the following pages contain a limited description of the benefit coverage available through this group plan. Coverage is governed at all times by the complete terms
2018 Medical Comparison Guide This and the following pages contain a limited description of the benefit coverage available through this group plan. Coverage is governed at all times by the complete terms
1199SEIU Greater New York Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs
 1199SEIU Greater New York Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 09/01/2015 Coverage for: Medicare-Eligible Retirees with 25 Years
1199SEIU Greater New York Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 09/01/2015 Coverage for: Medicare-Eligible Retirees with 25 Years
Your Summary of Benefits
 Your Summary of Benefits Producers Health Benefits Plan Classic PPO Modified Classic PPO 500/25/20 This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for
Your Summary of Benefits Producers Health Benefits Plan Classic PPO Modified Classic PPO 500/25/20 This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for
Your Guide to Kentucky HEALTH
 Your Guide to Kentucky HEALTH Updated August 2018 Your Guide to Kentucky HEALTH Kentucky has changed the way Medicaid works for some people. The state s new program is called Kentucky HEALTH. Kentucky
Your Guide to Kentucky HEALTH Updated August 2018 Your Guide to Kentucky HEALTH Kentucky has changed the way Medicaid works for some people. The state s new program is called Kentucky HEALTH. Kentucky
Anthem Blue Cross and Blue Shield Your Plan: Anthem Gold PPO 2000/20%/4000 Your Network: PPO
 Anthem Blue Cross and Blue Shield Your Plan: Anthem Gold PPO 2000/20%/4000 Your Network: PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Anthem Blue Cross and Blue Shield Your Plan: Anthem Gold PPO 2000/20%/4000 Your Network: PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
PE Process Guide. Qualified Provider Responsibilities
 PE Process Guide The purpose of this document is to provide Qualified Providers (QP) participating in the Presumptive Eligibility (PE) program guidance on eligibility requirements and the QP s role in
PE Process Guide The purpose of this document is to provide Qualified Providers (QP) participating in the Presumptive Eligibility (PE) program guidance on eligibility requirements and the QP s role in
Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage
 Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage Effective January 1, 2008 through December 31, 2008 1-800-645-3965 TTY/TDD: 1-888-857-4816 Seven days a week 8 a.m. 8
Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage Effective January 1, 2008 through December 31, 2008 1-800-645-3965 TTY/TDD: 1-888-857-4816 Seven days a week 8 a.m. 8
Your Plan: Anthem Bronze PPO 6350/30%/6850 Plus Your Network: Anthem PPO
 Your Plan: Anthem Bronze PPO 6350/30%/6850 Plus Your Network: Anthem PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Your Plan: Anthem Bronze PPO 6350/30%/6850 Plus Your Network: Anthem PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Your Plan: Bronze Pathway X HMO Plus w/hsa Your Network: Pathway X HMO
 Your Plan: Bronze Pathway X HMO Plus w/hsa Your Network: Pathway X HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
Your Plan: Bronze Pathway X HMO Plus w/hsa Your Network: Pathway X HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
Anthem Blue Cross: Anthem Silver DirectAccess, a Multi-State Plan Coverage Period: 01/01/ /31/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
Important Questions Answers Why this Matters:
 Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
Important Questions Answers Why this Matters:
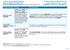 Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
Anthem Blue Cross of California Your Plan: Anthem Gold HMO 25/20%/6600 Your Network: California Care HMO
 Anthem Blue Cross of California Your Plan: Anthem Gold HMO 25/20%/6600 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross of California Your Plan: Anthem Gold HMO 25/20%/6600 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Your Plan: 2017 HMO Value Plan (0KGJ) Your Network: California Care HMO
 Anthem Blue Cross Your Plan: 2017 HMO Value Plan (0KGJ) Your : California Care HMO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: 2017 HMO Value Plan (0KGJ) Your : California Care HMO ACWA JPIA C00361 This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Your Plan: Anthem HealthKeepers Silver OAPOS 3500/0%/3500 w/hsa Your Network: HealthKeepers
 Your Plan: Anthem HealthKeepers Silver OAPOS 3500/0%/3500 w/hsa Your Network: HealthKeepers This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Your Plan: Anthem HealthKeepers Silver OAPOS 3500/0%/3500 w/hsa Your Network: HealthKeepers This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This
Important Questions. Why this Matters:
 Important Questions This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/calpers or by calling
Important Questions This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/calpers or by calling
Anthem Blue Cross and Blue Shield Your Plan: Anthem Bronze Pathway PPO 5000/30%/7150 Your Network: Pathway PPO
 Anthem Blue Cross and Blue Shield Your Plan: Anthem Bronze Pathway PPO 5000/30%/7150 Your Network: Pathway PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Anthem Blue Cross and Blue Shield Your Plan: Anthem Bronze Pathway PPO 5000/30%/7150 Your Network: Pathway PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-800-342-9816. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-800-342-9816. Important
1199SEIU National Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs
 1199SEIU National Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Wage Classes I & II and Early Retirees with
1199SEIU National Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Wage Classes I & II and Early Retirees with
