Specialty Drug Medical Benefit Management
|
|
|
- Elmer Farmer
- 6 years ago
- Views:
Transcription
1 Specialty Drug Medical Benefit Management
2 Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations Contact Information NovoLogix Prior Authorization Process
3 Introduction Specialty Drug Medical Benefit Management Drug costs continue to rise and specialty drugs contribute significantly to that trend. We adopted some practices to manage specialty drugs billed under the medical benefit when the specialty drug is administered at: Outpatient hospitals Infusion suites Physician offices Patient homes
4 Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations Contact Information NovoLogix Prior Authorization Process
5 SMBM Strategy Three components: 1. National Drug Code (NDC) required and validated In 2016, this became a requirement. We will reject claims for drugs that do not include a valid NDC code. 2. Self-administered specialty drugs blocked under medical Certain self-administered drugs the medical benefit covered are now only be covered under the pharmacy benefit.
6 SMBM Strategy Three components (cont d): 3. Prior authorization (PA) required for certain medical specialty drugs (injectable/infusible drugs) billed under the medical benefit BlueChoice has been requiring prior authorizations for some of these specialty drugs for many years. Effective June 1, 2016, get the PA from CVS/caremark using NovoLogix medical prior authorization system, Pharmacy specialty drugs billed under the pharmacy benefit continue to get prior authorizations through CVS/caremark. Important: BlueChoice providers no longer contact Utilization Management, contact NovoLogix for prior authorizations.
7 SMBM Strategy Participating Plans BlueCross and BlueChoice Plans: Fully insured Exchange plans BlueChoice self-funded plans BlueCross self-funded plans beginning Jan. 1, 2017
8 SMBM Strategy Nonparticipating Plans BlueCross and BlueChoice plans not participating with the program include: Federal Employees Program (FEP) State Health Plan Out-of-state members (BlueCard )
9 Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations Contact Information NovoLogix Prior Authorization Process
10 Prior Authorization Process How to Submit Authorization Requests Initiate requests using My Insurance Manager (via or the preferred method: 1. Identify patient, physician and treatment facility 2. Complete the online authorization request form 3. Answer protocol questions, if applicable 4. Confirm the information 5. Submit the request
11 Prior Authorization Process Gather necessary patient and therapy information GENERAL CLINICAL INFORMATION PROTOCOLS/NOTES Name and NPI of provider delivering the drug Member name and ID number Place of service that will perform the procedures Anticipated dates of service Primary diagnosis Authorization priority NDC code Quantity Complete any applicable protocol questions to complete the authorization request After creation you will be able to add Notes and/or upload supporting documentation NovoLogix may need additional information to complete the authorization request. Those requests will show in the Provider Action section of your homepage.
12 Prior Authorization Process Provider Online via Single Sign-on through My Insurance Manager SM or NovoLogix phone NovoLogix Clinical Review* Claims are Paid Services are Performed Approval/Denial of Request * If not auto-approved, NovoLogix makes determinations within two days for most requests BlueCross 12 BlueShield of South Carolina is an independent licensee of the Blue Cross and Blue Shield Association.
13 Prior Authorization Process Prior Authorization Request Example Place of Service Date(s) of Service NDC and Quantity (*) Indicates required fields
14 Prior Authorization Process Additional Clinical Information Authorizations requiring additional information will be in the Provider Action queue. Provide the clinical information as quickly as possible for a timely determination.
15 Prior Authorization Process Prior Authorization Review 1 Intake Level 2 Initial Review 3 Requests are evaluated using NovoLogix s clinical algorithm At this point, authorizations can: 1. Approve 2. Deny Additional Clinical Review Requests can: 1. Approve 2. Require additional clinical review 3. Pend for clinical validation of medical records NovoLogix will review request and can: 1. Approve 2. Send on for additional clinical review 3. Deny A peer-to-peer discussion is always available! Note: Refer to your authorization number for updated information regarding the submitted request.
16 Prior Authorization Process Notification of Determination Written and electronic provider notification Member will receive a separate notification
17 Prior Authorization Process Notification of Determination Approval Notification Electronic and written notice to provider and member. Provider can view approval on NovoLogix tool. Denial Notification Electronic and written notice to ordering physician. Member will receive written notice. Authorization Validity Period Most drug authorizations are good for one year from approval date. Provider Reconsideration Review Instructions Instructions are included in written communications. BlueCross will handle the reviews.
18 Prior Authorization Process Retrospective Review Process Within 30 calendar days of date of service, NovoLogix will review requests based on medical necessity. Authorization determinations are listed in the provider s queue.
19 Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Contracted IVT Providers Prior Authorization Process Other Important Information Provider Tools Provider Relations Contact Information NovoLogix Prior Authorization Process
20 Other Important Information Claims Process Claim Submission Submit claims to BlueCross and BlueChoice. File claims using Electronic Media Claims (EMC) or online using My Insurance Manager available at or Check claim status through My Insurance Manager. Provider Reconsideration Review Process Submit Provider Reconsideration Review requests to BlueCross for review of prior authorization or claim payment denials. Follow the instructions on the non-authorization letter or remittance notification.
21 Other Important Information Reminders Effective June 1, 2016, prior authorizations for specialty medical drugs should be obtained from NovoLogix. BlueChoice providers do not contact the Utilization Management department for prior authorizations, contact NovoLogix. Medical Specialty Drug Lists are available on the BlueCross and BlueChoice websites. Contracted IVT providers must follow the two-step prior authorization process.
22 Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Contracted IVT Providers Prior Authorization Process Other Important Information Provider Tools Provider Relations Contact Information NovoLogix Prior Authorization Process
23 Provider Tools My Insurance Manager Available 24 hours a day, seven days a week Check patient eligibility and if drug requires prior authorization Single sign-on to NovoLogix to complete the authorization Upload additional clinical information
24 Provider Tools Resources and NovoLogix provider training video SMBM FAQs Guide: What You Need to Know About Medical Specialty Drug Prior Authorizations Drug Lists» Medical Specialty Drugs» Self-administered Drugs Bulletins BlueNews SM
25 Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Contracted IVT Providers Prior Authorization Process Other Important Information Provider Tools Provider Relations Contact Information NovoLogix Prior Authorization Process
26 Provider Relations Contact Information NovoLogix Help: Available Monday through Friday, 7 a.m. 6 p.m. Central Time Call: helpdesk@novologix.net BlueCross and BlueChoice Provider Relations and Education: Phone: Use the Provider Advocate Contact Form Go to Contact Us on the websites
27 SMBM Strategy Questions? Provider Advocate Contact Form in Contact Us or
28 Questions What was the Actual Date Providers Began Getting Prior Authorizations from NovoLogix? The date to begin date to getting prior authorizations through NovoLogix was June 1, Where are the Medical Specialty Drugs and Selfadministered Drugs Lists Located? The drug lists are available on our websites, or in the Education Center on the Precertification page.
29 Questions How Do I Check the Status of a Prior Authorization? Go through My Insurance Manager to verify the status of a prior authorization on the NovoLogix system. Who can I contact if I have not received a response to my prior authorization request? If you have a question about the status of a prior authorization request, call NovoLogix at
30 Questions How do I submit a Prior Authorization? Log on to My Insurance Manager, then go to Patient Care and select Precertification/Referral. A message may appear advising that prior authorization is required. You may call or click the link to initiate the request.
31 Questions Questions? Provider Advocate Contact Form in Contact Us or
32 Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy NovoLogix Authorization Process Other Important Information Provider Tools Provider Relations Contact Information NovoLogix Prior Authorization Process
33 NovoLogix Prior Authorization Process PA request submitted By Mail, Fax, or via online portal PA request is received Eligibility verified, PA criteria applied NO Denied Meets guidelines YES PA approved Medication is administered Prescriber or pharmacy sends drug claim to health plan Appeals submitted to BCBSSC Claim adjudication and payment
34 NovoLogix Prior Authorization Process Create an Authorization #1 Get Started
35 NovoLogix Prior Authorization Process #2 - Enter Patient Detail Choose an option to start the prior authorization: Quick Start New Patient Existing Patient
36 NovoLogix Prior Authorization Process #2 - Enter Patient Detail (cont d) The asterisk indicates required fields: Name Date of Birth Member ID Relationship to Insured
37 NovoLogix Prior Authorization Process #3 - Enter Authorization Detail Complete all required fields and any other required or applicable authorization detail fields.
38 NovoLogix Prior Authorization Process #4 - Enter Authorization Lines Enter the applicable: Date(s) of Service Drug Name or NDC Quantity Any Additional Information
39 NovoLogix Prior Authorization Process #4 - Enter Authorization Lines (cont d) Review the information entered on the Authorization Detail screen.
40 NovoLogix Prior Authorization Process #5 Protocols and Submitting Request Complete any protocol questions.
41 NovoLogix Prior Authorization Process #5 Protocols and Submitting Request The status and authorization number will be displayed at the top of the screen.
42 NovoLogix Prior Authorization Process Add a Note Add a note from the Authorization Detail Screen
43 NovoLogix Prior Authorization Process Add a Document Add a document from the Authorization Detail Screen
44 NovoLogix Prior Authorization Process Resources and NovoLogix provider training video SMBM FAQs Guide: What You Need to Know About Medical Specialty Drug Prior Authorizations Drug Lists» Medical Specialty Drugs» Self-administered Drugs
45 SMBM Strategy Questions? Send to: Subject: Webinar SMBM - IVT
46 SMBM Strategy
Specialty Drug Medical Benefit Management. Note! Contents are subject to change and are not a guarantee of payment.
 Specialty Drug Medical Benefit Management Note! Contents are subject to change and are not a guarantee of payment. Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Authorization
Specialty Drug Medical Benefit Management Note! Contents are subject to change and are not a guarantee of payment. Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Authorization
What You Need to Know About
 What You Need to Know About Medical Specialty Drug Prior Authorizations 2016 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service OVERVIEW
What You Need to Know About Medical Specialty Drug Prior Authorizations 2016 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service OVERVIEW
GENERAL Why is BlueCross and BlueChoice implementing an MSK Program focused on interventional pain management procedures?
 Musculoskeletal Care Management (MSK) Program Interventional Pain Management (IPM) Frequently Asked Questions (FAQ s) For BlueCross BlueShield of South Carolina 1 and BlueChoice HealthPlan of South Carolina
Musculoskeletal Care Management (MSK) Program Interventional Pain Management (IPM) Frequently Asked Questions (FAQ s) For BlueCross BlueShield of South Carolina 1 and BlueChoice HealthPlan of South Carolina
Montgomery County Medical Society
 Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
CLAIM EDITOR FREQUENTLY ASKED QUESTIONS
 1. What is the Avalon Claim Editor? The Avalon Claim Editor is designed to provide consistent application of BlueCross BlueShield of South Carolina medical policy to laboratory claims. The medical policies
1. What is the Avalon Claim Editor? The Avalon Claim Editor is designed to provide consistent application of BlueCross BlueShield of South Carolina medical policy to laboratory claims. The medical policies
The benefits of using ExpressPAth for your practice include: Easy access. With 24/7 access, you can submit requests and get answers at any time.
 Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Prescriber Web Prior Authorization
 Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Durable Medical Equipment. Note! Contents are subject to change and are not a guarantee of payment.
 Durable Medical Equipment Note! Contents are subject to change and are not a guarantee of payment. General Information Durable Medical Equipment (DME) Eligibility and Benefits Filing DME Claims Group Updates
Durable Medical Equipment Note! Contents are subject to change and are not a guarantee of payment. General Information Durable Medical Equipment (DME) Eligibility and Benefits Filing DME Claims Group Updates
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
ancillary claims filing requirements: specialty pharmacy
 ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
 Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
2017 Affordable Care Act (ACA)/Exchange Plans. Note! Contents are subject to change and are not a guarantee of payment.
 2017 Affordable Care Act (ACA)/Exchange Plans Note! Contents are subject to change and are not a guarantee of payment. Agenda Essential Health Benefits BlueCross BlueShield of South Carolina ACA/Exchange
2017 Affordable Care Act (ACA)/Exchange Plans Note! Contents are subject to change and are not a guarantee of payment. Agenda Essential Health Benefits BlueCross BlueShield of South Carolina ACA/Exchange
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) BlueCross BlueShield of South Carolina Providers
 Magellan Healthcare 1 Frequently Asked Questions (FAQ s) BlueCross BlueShield of South Carolina Providers Question Answer GENERAL Why did BlueCross implement an outpatient imaging program? Why did BlueCross
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) BlueCross BlueShield of South Carolina Providers Question Answer GENERAL Why did BlueCross implement an outpatient imaging program? Why did BlueCross
General Who is National Imaging Associates, Inc. (NIA)?
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry West Virginia Providers Performing Physical Medicine Services Question General Who is National Imaging Associates,
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry West Virginia Providers Performing Physical Medicine Services Question General Who is National Imaging Associates,
General Who is National Imaging Associates, Inc. (NIA)?
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
Prior Authorization and Medical Necessity Determination Processes
 Prior Authorization and Medical Necessity Determination Processes Prior authorizations (PAs) are required for inpatient admissions, various procedures, prescription medications and physical and occupational
Prior Authorization and Medical Necessity Determination Processes Prior authorizations (PAs) are required for inpatient admissions, various procedures, prescription medications and physical and occupational
Health Insurance Marketplaces (Exchanges)
 Health Insurance Marketplaces (Exchanges) Essential Health Benefits Starting in 2014, non-grandfathered health plans in the individual and small group markets, within the Health Insurance Marketplace (exchanges),
Health Insurance Marketplaces (Exchanges) Essential Health Benefits Starting in 2014, non-grandfathered health plans in the individual and small group markets, within the Health Insurance Marketplace (exchanges),
Section Eleven. Referrals and Prior Authorization REFERRAL PROCESS. Physician Referrals within Plan Network
 REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
General Who is National Imaging Associates, Inc. (NIA)?
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna Delaware Providers Performing Physical Medicine Services
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna Delaware Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna Delaware Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
Questions and Answers
 Questions and Answers Radiation Oncology Utilization Management Program Why did Florida Blue implement a radiation oncology utilization management program? The purpose of the program is to ensure radiation
Questions and Answers Radiation Oncology Utilization Management Program Why did Florida Blue implement a radiation oncology utilization management program? The purpose of the program is to ensure radiation
Secondary Professional Claims on the HCFA-1500
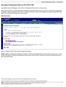 Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
KanCare All MCO Training. Fall 2018
 KanCare All MCO Training Fall 2018 Welcome, Introductions & Agenda Welcome Introductions United HealthCare Agenda for the day Provider Specific afternoon Session 1:00 p.m. to 4:30 p.m. Break out tables
KanCare All MCO Training Fall 2018 Welcome, Introductions & Agenda Welcome Introductions United HealthCare Agenda for the day Provider Specific afternoon Session 1:00 p.m. to 4:30 p.m. Break out tables
Blue Shield. CCHCA Physician Handbook
 Part II Section C Blue Shield Introduction 1 Verifying Blue Shield Member Eligibility and Benefits 1 Blue Shield Sample Member ID Card 2 Pharmacy Benefit 5 Member Grievance Forms 9 CCHCA Physician Handbook
Part II Section C Blue Shield Introduction 1 Verifying Blue Shield Member Eligibility and Benefits 1 Blue Shield Sample Member ID Card 2 Pharmacy Benefit 5 Member Grievance Forms 9 CCHCA Physician Handbook
Interventional Pain Management (IPM) Frequently Asked Questions
 Interventional Pain Management (IPM) Frequently Asked Questions Question GENERAL Why did HMSA implement a process to review pain management? Answer To improve quality and manage the utilization of nonemergent
Interventional Pain Management (IPM) Frequently Asked Questions Question GENERAL Why did HMSA implement a process to review pain management? Answer To improve quality and manage the utilization of nonemergent
Claim Investigation Submission Guide
 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Clinical Policies and Procedures for Major Joint and Lower Extremity Services Overview and FAQs for BCBSNC In-Network Providers.
 Clinical Policies and Procedures for Major Joint and Lower Extremity Services Overview and FAQs for BCBSNC In-Network Providers October 17, 2016 Overview Blue Cross and Blue Shield of North Carolina (BCBSNC)
Clinical Policies and Procedures for Major Joint and Lower Extremity Services Overview and FAQs for BCBSNC In-Network Providers October 17, 2016 Overview Blue Cross and Blue Shield of North Carolina (BCBSNC)
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal
 Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
MHS Prior Authorization 0317.PR.P.PP
 MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Frequently Asked Questions Cardiology Prior Authorization Program Applies to UnitedHealthcare Community Plan Members.
 Frequently Asked Cardiology Prior Authorization Program Applies to UnitedHealthcare Community Plan Members. Overview Prior authorization is required for select cardiology procedures provided to certain
Frequently Asked Cardiology Prior Authorization Program Applies to UnitedHealthcare Community Plan Members. Overview Prior authorization is required for select cardiology procedures provided to certain
PHARMACY COVERAGE GUIDELINES ORIGINAL EFFECTIVE DATE: 1/18/18 SECTION: DRUGS LAST REVIEW DATE: 8/13/18 LAST CRITERIA REVISION DATE: ARCHIVE DATE:
 STEP THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage Guideline must
STEP THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage Guideline must
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
MHS CMS 1500 Tips and Billing Guidelines
 MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
Anthem Blue Cross and Blue Shield. Serving Hoosier Healthwise and Healthy Indiana Plan
 Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Avenues of Resolution for Indiana Health Coverage Programs
 Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Prior Authorizations with InterQual Integration
 Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona
 Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) NH Healthy Families Prior Authorization Program Physical Medicine Services
 Question General When does the Physical Medicine Services program transition to a Prior Authorization program for NH Healthy Families? National Imaging Associates, Inc. (NIA) Frequently Asked Questions
Question General When does the Physical Medicine Services program transition to a Prior Authorization program for NH Healthy Families? National Imaging Associates, Inc. (NIA) Frequently Asked Questions
Precertification requirements for FEP members for BRCA testing and outpatient services
 2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
evicore healthcare Utilization management programs Frequently asked questions
 evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
Webinar Schedule Join us for our next webinar! Are you a newly contracted Provider? Existing Provider who has new staff? Would your office like to lea
 Fall 2018 Provider Newsletter What s New? Provider Services Phone Number 888-243-3312 We are excited to share a change with you! Our dedicated Provider Services telephone number launched on November 1
Fall 2018 Provider Newsletter What s New? Provider Services Phone Number 888-243-3312 We are excited to share a change with you! Our dedicated Provider Services telephone number launched on November 1
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18
 MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18 Agenda Save Time by Utilizing the MHS Secure Web Portal: Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims
MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18 Agenda Save Time by Utilizing the MHS Secure Web Portal: Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims
Maryland Medical Group Management Association CareFirst Updates & Reminders
 Maryland Medical Group Management Association CareFirst Updates & Reminders May 11, 2018 Agenda Enhance Security for Provider Portal National Drug Code Requirement Medication Management and Electronic
Maryland Medical Group Management Association CareFirst Updates & Reminders May 11, 2018 Agenda Enhance Security for Provider Portal National Drug Code Requirement Medication Management and Electronic
Blue Exclusive SM Upstate 1 BusinessADVANTAGE Select Upstate Small Group Narrow Network Products
 Blue Exclusive SM Upstate 1 BusinessADVANTAGE Select Upstate 1 2016 Small Group Narrow Network Products MyHealth First Network is an independent company that offers a provider network on behalf of BlueCross
Blue Exclusive SM Upstate 1 BusinessADVANTAGE Select Upstate 1 2016 Small Group Narrow Network Products MyHealth First Network is an independent company that offers a provider network on behalf of BlueCross
Provider Reconsideration and Appeals. BlueCross BlueShield of Tennessee, Inc. an Independent Licensee of the BlueCross BlueShield Association
 Provider Reconsideration and Appeals BlueCross BlueShield of Tennessee, Inc. an Independent Licensee of the BlueCross BlueShield Association What is a Provider Claim Reconsideration? A claim reconsideration
Provider Reconsideration and Appeals BlueCross BlueShield of Tennessee, Inc. an Independent Licensee of the BlueCross BlueShield Association What is a Provider Claim Reconsideration? A claim reconsideration
Patient Services and Support
 Patient Services and Support BENLYSTA Gateway: Providing resources and information to meet changing access needs 1-877-4-BENLYSTA (1-877-423-6597) Select option 1 for BENLYSTA Gateway Monday-Friday, 8
Patient Services and Support BENLYSTA Gateway: Providing resources and information to meet changing access needs 1-877-4-BENLYSTA (1-877-423-6597) Select option 1 for BENLYSTA Gateway Monday-Friday, 8
2016 Health Insurance Marketplaces (Exchanges) Note! Contents are subject to change and are not a guarantee of payment.
 2016 Health Insurance Marketplaces (Exchanges) Note! Contents are subject to change and are not a guarantee of payment. Essential Health Benefits 10 Categories of Benefits 1. Ambulatory patient services
2016 Health Insurance Marketplaces (Exchanges) Note! Contents are subject to change and are not a guarantee of payment. Essential Health Benefits 10 Categories of Benefits 1. Ambulatory patient services
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers
 Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
RECONTRACTING 10/31/2016. Aetna Medicare Advantage. Aetna Behavioral Health
 DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
CareCore National Musculoskeletal Management Program Physical Medicine and Therapy Frequently Asked Questions
 EVIDENCE-BASED HEALTHCARE SOLUTIONS CareCore National Physical Medicine and Therapy Prepared for December 2, 2014 Table of Contents Introduction to CareCore National... 3 Who is CareCore National?... 3
EVIDENCE-BASED HEALTHCARE SOLUTIONS CareCore National Physical Medicine and Therapy Prepared for December 2, 2014 Table of Contents Introduction to CareCore National... 3 Who is CareCore National?... 3
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
21 - Pharmacy Services
 21 - Pharmacy Services The role of Health Plan of Nevada s (HPN) Pharmacy Services is to evaluate and determine the appropriateness of quality drug therapy while maintaining and improving therapeutic outcomes.
21 - Pharmacy Services The role of Health Plan of Nevada s (HPN) Pharmacy Services is to evaluate and determine the appropriateness of quality drug therapy while maintaining and improving therapeutic outcomes.
Chapter 7. Billing and Claims Processing
 Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
GENERAL Why did Magellan Complete Care implement an MSK Program focused on IPM procedures?
 Magellan Healthcare 1 Musculoskeletal Care Management (MSK) Program Interventional Pain Management (IPM) Frequently Asked Questions (FAQ s) For Magellan Complete Care of Florida Providers Question GENERAL
Magellan Healthcare 1 Musculoskeletal Care Management (MSK) Program Interventional Pain Management (IPM) Frequently Asked Questions (FAQ s) For Magellan Complete Care of Florida Providers Question GENERAL
SutterSelect Administrative Manual. June 2017
 SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
Electronic Prior Authorization Initiatives at the Point of Care: Moving the Industry Forward
 Electronic Prior Authorization Initiatives at the Point of Care: Moving the Industry Forward Friday, April 20 th from 11:45am to 12:45am Marc Nyarko, Humana Bruce Wilkinson, CVS Caremark Roger Pinsonneault,
Electronic Prior Authorization Initiatives at the Point of Care: Moving the Industry Forward Friday, April 20 th from 11:45am to 12:45am Marc Nyarko, Humana Bruce Wilkinson, CVS Caremark Roger Pinsonneault,
Unit 14 Radiology Management
 Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Medication Limitation of Non Coverage for Prevention Benefit Coverage with Waived Cost Share
 Cost Share Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage Guideline must be
Cost Share Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage Guideline must be
Welcome to the BlueChoice Network
 Welcome to the BlueChoice Network BlueChoice Network Objective The BlueChoice network is composed of hospitals, physicians, health care professionals, and ancillary providers that have contracted with
Welcome to the BlueChoice Network BlueChoice Network Objective The BlueChoice network is composed of hospitals, physicians, health care professionals, and ancillary providers that have contracted with
Medicare Part D Transition Policy CY 2018 HCSC Medicare Part D
 Contract: H0107, H0927, H1666, H3251, H3822, H3979, H8133, H8634, H8554, S5715 Policy Name: Medicare Formulary Transition Purpose: This procedure describes the standard process Health Care Service Corporation
Contract: H0107, H0927, H1666, H3251, H3822, H3979, H8133, H8634, H8554, S5715 Policy Name: Medicare Formulary Transition Purpose: This procedure describes the standard process Health Care Service Corporation
For Participating Rehabilitation Therapists May 2006
 For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
CoventryCares of Kentucky Provider Training Program
 CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Ambetter 101. Quarterly Provider Webinar February 23, 2017
 Ambetter 101 Quarterly Provider Webinar February 23, 2017 AGENDA 1. What is Ambetter? 2. The Health Insurance Marketplace 3. Public Website and Secure Portal 4. Verification of Eligibility, Benefits and
Ambetter 101 Quarterly Provider Webinar February 23, 2017 AGENDA 1. What is Ambetter? 2. The Health Insurance Marketplace 3. Public Website and Secure Portal 4. Verification of Eligibility, Benefits and
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims
 Medicare Advantage Provider s Frequently Asked Questions Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims Generally, as a healthcare provider you should file claims for your Blue Cross and
Medicare Advantage Provider s Frequently Asked Questions Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims Generally, as a healthcare provider you should file claims for your Blue Cross and
Training Documentation
 Training Documentation Durable Medical Equipment 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital Advantage
Training Documentation Durable Medical Equipment 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital Advantage
10/30/2017. Third Party Payer Day: Medicare Plus Blue Claims & System Issue Resolution. Provider contacts Provider Inquiry Service Center
 Third Party Payer Day: Medicare Plus Blue Claims & System Issue Resolution November 10, 2017 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee of the Blue Cross and
Third Party Payer Day: Medicare Plus Blue Claims & System Issue Resolution November 10, 2017 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee of the Blue Cross and
Welcome to Blue Cross Commercial Risk Adjustment Webinar
 Welcome to Blue Cross Commercial Risk Adjustment Webinar For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background
Welcome to Blue Cross Commercial Risk Adjustment Webinar For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions
 WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
Portal User Guide. Submitting Inpatient Notifications and Prior Authorization Requests. Tufts Health Together and Tufts Health Direct
 MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
2019 Member Identification Card Guide
 2019 Member Identification Card Guide Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service Revised: Dec. 2018 In the event of any inconsistency between
2019 Member Identification Card Guide Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service Revised: Dec. 2018 In the event of any inconsistency between
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Arkansas State University System Prescription Drug Program
 Arkansas State University System Prescription Drug Program The Arkansas State University (ASU) prescription drug program involves a partnership with the University of Arkansas for Medical Sciences (UAMS)
Arkansas State University System Prescription Drug Program The Arkansas State University (ASU) prescription drug program involves a partnership with the University of Arkansas for Medical Sciences (UAMS)
Professional Refresher Workshop. Presented by The Department of Social Services & HP
 Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility SAGA Becomes Medicaid for Low Income Adults Automated Voice Response System (AVRS)
Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility SAGA Becomes Medicaid for Low Income Adults Automated Voice Response System (AVRS)
Authorization and appeals kit: Moderate to severe plaque psoriasis
 1 Authorization and appeals kit: Moderate to severe plaque psoriasis Resources for healthcare providers INDICATIONS COSENTYX is indicated for the treatment of moderate to severe plaque psoriasis in adult
1 Authorization and appeals kit: Moderate to severe plaque psoriasis Resources for healthcare providers INDICATIONS COSENTYX is indicated for the treatment of moderate to severe plaque psoriasis in adult
CMS 1500 Paper Claim Billing Instructions Form number
 CMS 1500 Paper Claim Billing Instructions Form number 0938-1197 Please refer to the National Uniform Claim Committee official 1500 Health Insurance Claim Reference Instruction Manual for definition, field
CMS 1500 Paper Claim Billing Instructions Form number 0938-1197 Please refer to the National Uniform Claim Committee official 1500 Health Insurance Claim Reference Instruction Manual for definition, field
Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017
 Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017 Key Points Starting Nov. 1, 2017, notification/prior authorization is required
Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017 Key Points Starting Nov. 1, 2017, notification/prior authorization is required
NIA Frequently Asked Questions (FAQ s) For CoventryCares of Kentucky Providers
 Question GENERAL Do Kentucky Members have any copay responsibilities? NIA Frequently Asked Questions (FAQ s) For Providers Answer Members do not have copays for outpatient imaging procedures. PRIOR AUTHORIZATION
Question GENERAL Do Kentucky Members have any copay responsibilities? NIA Frequently Asked Questions (FAQ s) For Providers Answer Members do not have copays for outpatient imaging procedures. PRIOR AUTHORIZATION
Claims and Appeals Procedures
 Dear Participant: December 2002 The Department of Labor s Pension and Welfare Benefits Administration has issued new claims and appeals regulations that will be applicable to the Connecticut Carpenters
Dear Participant: December 2002 The Department of Labor s Pension and Welfare Benefits Administration has issued new claims and appeals regulations that will be applicable to the Connecticut Carpenters
Connecticut Medical Assistance Program Workshop Web Claim Submission
 Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Medical Eligibility & Benefits Lookup Tips
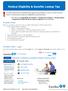 Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Maine Chapter of the Healthcare Financial Management Association. MaineCare Provider Relations
 Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop
 CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
Pharmacy/Prescriber Medicaid Managed Care Network & Medicaid Provider Enrollment. February 14, 2018
 Pharmacy/Prescriber Medicaid Managed Care Network & Medicaid Provider Enrollment February 14, 2018 2 Pharmacy/ Prescriber Enrollment Enrollment Effective Date Pharmacy/Prescriber FAQ s Contract Amendment
Pharmacy/Prescriber Medicaid Managed Care Network & Medicaid Provider Enrollment February 14, 2018 2 Pharmacy/ Prescriber Enrollment Enrollment Effective Date Pharmacy/Prescriber FAQ s Contract Amendment
2017 Benefit Update Meeting Columbia, South Carolina. Meeting Handbook for Providers
 2017 Benefit Update Meeting Columbia, South Carolina Meeting Handbook for Providers In the event of any inconsistency between information contained in this handbook and the agreement(s) between you and
2017 Benefit Update Meeting Columbia, South Carolina Meeting Handbook for Providers In the event of any inconsistency between information contained in this handbook and the agreement(s) between you and
Network Health Claims Editing Portal
 Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers
 NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
ASO. BlueCross BlueShield of Oregon. Core Offerings SELF-FUNDED GROUPS, SIZED 100+ Crater Lake
 BlueCross BlueShield of Oregon ASO Core Offerings SELF-FUNDED GROUPS, SIZED 100+ Regence BlueCross BlueShield of Oregon is an Independent Licensee of the Blue Cross and Blue Shield Association Crater Lake
BlueCross BlueShield of Oregon ASO Core Offerings SELF-FUNDED GROUPS, SIZED 100+ Regence BlueCross BlueShield of Oregon is an Independent Licensee of the Blue Cross and Blue Shield Association Crater Lake
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
