Working with Anthem Subject Specific Webinar Series
|
|
|
- Laurel Townsend
- 5 years ago
- Views:
Transcription
1 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: Conference Code: # Please Mute Your Phone Use the mute button or press *6 This presentation contains proprietary information of Anthem Blue Cross and Blue Shield. It is intended for Anthem providers. Any redistribution or other use is strictly forbidden.
2 Provider Claim Submission & Adjustment Requests Tips and Tools Agenda Housekeeping and Announcements Claim Submission Medical Policy and Clinical UM Guidelines Clinical Claim Edits Reimbursement Policies Claim Processing Remittance Advice Claim Adjustments Complaints and Appeals Helpful Links and Handouts 2
3 Working with Anthem Subject Specific Webinar Series Housekeeping & Announcements Navigation and Handouts Click here for handouts 1. Select items by checking the boxes 2. Select a destination on your computer 3. Press OK to download Control your view Full Screen 3
4 Claim Submission - Initial Claims should be submitted in the same manner as you would to any other payer following national correct coding guidelines Complete member ID number including alpha prefix NPI and Tax Identification Numbers required Referring provider name in box 17 with type 1 NPI box 17b Rendering provider NPI should be present in box 24j on professional claim forms Billing (Organizational/Billing Type 2) NPI should be present in box 33a 4
5 Claim Submission - Initial Claims should be submitted in the same manner as you would to any other payer following national correct coding guidelines Billing address under 5010 must be a physical location not a PO Box o Submit PO Box in the Pay To Loop on electronic claims Submit with Taxonomy codes for practitioners with dual specialties Facility claim requirements o Present on admission (POA) indicators 5
6 Claim Submission - Initial Ancillary Provider Claim Submission Reminder Independent Clinical Lab o File to the Plan whose service area where the specimen was drawn. o Determined by the zip code associated with NPI Durable/Home Medical Equipment o File to the Plan in whose service area the equipment and/or supplies were delivered, shipped to, or o the location of the retail store where the equipment and/or supplies were purchased or rented. 6
7 Claim Submission - Initial Ancillary Provider Claim Submission Reminder Specialty Pharmacy o File to Plan in service area ordering provider located (ordering physician address) o Determined by the zip code associated with NPI Applies to all Commercial and Medicare Advantage Blue Plans Does not apply to Federal Employee Program (FEP) members More Information Answers@Anthem, Ancillary Claim Filing Requirements FAQs September, 2012 link: pdf?refer=ahpprovider&state=wi 7
8 Claim Submission Medicare Crossover Claims Submitted directly to the secondary payer electronically by Medicare Indicated on the Medicare EOMB Payment made directly by the secondary payer Submitting a paper claim before or immediately upon receiving your Medicare EOMB may cause: Rejected claims Delayed payments Duplicate denials Double work for your payment posters 8
9 Claim Submission Medicare Crossover Claims continued When a Medicare claim has crossed over, providers are to wait 30 calendar days from the Medicare remittance date before submitting the claim to the local Blue Plan to avoid claim returns. Providers should continue to submit services that are covered by Medicare directly to Medicare. Even if Medicare may exhaust or has exhausted its benefits, continue to submit claims to Medicare to allow for the crossover process to occur and for the member s benefit policy to be applied. Local Blue Plans will reject provider submitted claims received within 30 calendar days of the Medicare remittance date or any claims received without a Medicare remittance date on the claim.. 9
10 Claim Submission Medicare Crossover Claims continued Submitted directly to the secondary payer electronically by Medicare Indicated on the Medicare EOMB MA18 Alert: The claim information is also being forwarded to the patient's supplemental insurer. Send any questions regarding supplemental benefits to them. N89 Alert: Payment information for this claim has been forwarded to more than one other payer, but format limitations permit only one of the secondary payers to be identified in this remittance advice Payment made directly by the secondary payer 10 10
11 Claim Submission Medicare Crossover Claims 11 11
12 Claim Submission Medicare Crossover Claims 12 12
13 Claim Submission Medicare Crossover Claims continued Anthem will reject Medicare primary provider-submitted claims with the following conditions Medicare advice remark codes MA18 or N89 that indicate Medicare crossover has occurred Received by provider s local Blue Plan within 30 calendar days of Medicare remittance date Received by provider s local Blue Plan with no Medicare remittance data 13 13
14 Claim Submission Medicare Statutorily Excluded Services Providers who render statutorily excluded services should indicate these services by using GY modifier at the line level at the service line level of the claim. Providers required to submit only statutorily excluded service lines on a claim (cannot combine with other services like Medicare exhaust services or other Medicare covered services) Provider s local plan will not require Medicare EOMB If providers submit combined line claims (some lines with GY, some without) to their local plan, the provider s local plan will deny the claims, instructing provider to split the claim and resubmit. More information: August 2013 Network Update Newsletter - BCBSA initiative addresses secondary payer Medicare claims beginning on page
15 Claim Submission Claim Submission - Electronic Why submit claims electronically? No postal delays Transmit claims 24 hours a day, seven days a week Electronic claims are faster and more accurate Electronic claims are acknowledged by Anthem through notification and error reports that are placed in your electronic mailbox Accepted directly from providers (direct submitters) or through billing services, vendors and clearinghouses
16 Claim Submission Claim Submission - Electronic Submit in 5010 format Initial Claims Secondary Claims Corrected Claims Wisconsin Payer IDs: Professional Institutional (facility) Anthem EDI Help Desk Telephone: Website: Live Chat 16 16
17 Claim Submission Claim Submission An Anthem Difference Ambulatory Surgery Centers (ASC) facility services submitted on a professional claim form consistent with Medicare o Do not include a rendering physician as these charges should be submitted separately by the physician Guidelines Public provider website o Anthem Medical Policies and Clinical UM Guidelines o Clinical Claim Edits Secure Provider Portal MyAnthem SM via Availity o On Availity select MyPayer Portals Anthem Payer Portal Administrative Support\Policies & Procedures o Reimbursement Policies 17 17
18 Medical Policy & Clinical UM Guidelines Accessed through the Medical Policy, Clinical UM and Precertification Guideline router Information available for local and out-of-state Blue plans Precertification requirements Medical policies o Searchable by term and code 18 18
19 Clinical Claim Edits Accessed through the Anthem Customized Claim Edits link under Self Service and Support on the Provider Home page of our website Edits contain, the subject, the edit number, the rationale and if available the reference for the claims edit Google search by term or by code Default includes Medical Policies, Medical Coverage Guidelines and 10 results 19 19
20 Reimbursement Policies Accessed through Availity to MyAnthem Payer Portal Select Administrative Support Policies & Programs o Procedures for Professional Reimbursement o Recommended for immediate review List of Payment Policy Indicators Bundled Services and Supplies Policy 0008 Frequency Editing Policy
21 Reimbursement Policies Accessing MyAnthem via Availity To access MyAnthem, click on My Payer Portals on Availity s left navigation menu. Then click Anthem Provider Portal and I Agree to be navigated to MyAnthem without entering an additional log in and password
22 Reimbursement Policies Accessing MyAnthem via Availity 22 22
23 Claim Processing A Picture Paper Claim Received Claim Imaged Claim keyed Data submitted to Claim Processing System Is Member Local? Yes Member Eligibility & Benefits Medical Policy Clinical UM Guidelines Provider Indentification Provider Pricing Including Reimbursement Policies, Clinical Claim Edits Claim Adjudicated Electronic Claim Received No Provider Indentification Provider Pricing Including Reimbursement Policies, Clinical Claim Edits Provider Remittance Advice Data sent to member s (home) plan Member Eligibility & Benefits Medical Policy Clinical UM Guidelines Claim Adjudicated Data sent to provider s (host) plan 23 23
24 Claim Processing Status Electronically 276/277 Transactions (5010 format) Availity Multi-payer portal All lines of business Telephonically Ready Reference Guide o Found under Contact Us on the public provider website Availity is an independent company providing a wide variety of online tools that allow providers to access real-time information from multiple payers via one secure sign-on 24 24
25 Claim Processing Status Availity Inquiry Recommendations Start with Member Eligibility Inquiry Under Claims Management, select Claim Status Inquiry o Change the provider if not the same as organizational (billing) o Enter date of service range 25 25
26 Claim Processing Status Availity Inquiry Recommendations continued o Click on From-To Date of Service to expand 26 26
27 Remittance Advice Paper and Electronic Electronically 835 ERA Electronic Funds Transfer (EFT) Payments EFT and EFT+ERA Enrollment via CAQH EnrollHub ERA only Anthem EDI at On Paper In the Mail Online copies via Availity link to MyAnthem SM Hand-Out: Provider Remittance Advice Example 27 27
28 Remittance Advice Paper and Electronic Availity link to MyAnthem SM 28 28
29 Remittance Advice MyAnthem SM 29 29
30 Remittance Advice MyAnthem SM Anthem Remittance Inquiry Tool Selections 30 30
31 Remittance Advice MyAnthem SM 31 31
32 Remittance Advice MyAnthem SM Opens a PDF file of the actual remit File can be: Searched Printed Saved to disk 32 32
33 Remittance Advice Healthcare Exchange Members Grace Period Grace period for individual health plans purchased on Exchange that are eligible for a governmental premium subsidy. 3 month grace period applies after the individual has paid at least one month s premium Premium non-payment Anthem will process claims for services received during the first month Anthem will pend claims for services received during the second and third months of the grace period, until the full premium is received After the third month, if the premium is not received, the member s health plan will be terminated and the claims for services received during the second and third month will be denied Providers will be notified of denied claims on their remittance advice The member will be responsible for payment of services 33 33
34 Remittance Advice Healthcare Exchange Members Grace Period Grace period for individual health plans purchased on Exchange that are eligible for a governmental premium subsidy. Premium non-payment continued Providers notified on their remittance advice that the claim cannot be paid until the premium is received Members displayed with a status of "Health Insurance Exchange - HIX GRACE PERIOD." on Availity and ICR Providers notified on 271 transactions (enhanced detail) Health Exchange Information Page Link 34 34
35 Remittance Advice Healthcare Exchange Members Grace Period 271 Eligibility Transactional Response Enhanced Detail 2100C/D DTP: DTP01 ="343" (Premium Paid to Date End) DTP03 = This message provides the date for which the premium is paid through (the last day of coverage for which a premium payment has been received).this is the last day of the month before the beginning of the grace period. 2110C/D DTP (1 st iteration): DTP01 = "193" (Period Start) DTP03 = This message provides the date that represents the first day of the first month of the grace period. 2110C/D DTP (2 nd iteration): DTP01 = "194" (Period End) DTP03 = This message provides the date that is the last day of the third month of the grace period. 2110C/D MSG: MSG01 = "Health Insurance Exchange - HIX GRACE PERIOD." This message indicates that a member is in the second or third month of a grace period, and that claims for this member will pend until premium is paid
36 Remittance Advice Healthcare Exchange Members Grace Period Grace period for individual health plans purchased on Exchange that are eligible for a governmental premium subsidy Premium non-payment continued After the third month, if the premium is not received, the member s health plan will be terminated and the claims for services received during the second and third months will be denied. Providers will be notified of denied claims on their remittance advice The members will be responsible for payment of services 36 36
37 Remittance Advice Healthcare Exchange Members Grace Period Grace period for individual health plans purchased on Exchange that are eligible for a governmental premium subsidy Premium non-payment continued ANSI 835 Codes passed on 835 Electronic Remittance Advice o Claim Adjustment Reason Code (CARC) 133 The disposition of the claim service is pending further review (Use only with Group Code OA) Start: 02/28/1997 Last modified : 01/20/2013 o Remittance Advice Remark Code (RARC) N617 This enrollee is in the second or third month of the advanced premium tax credit grace period Start: 07/15/2013 Paper Remittance Advice remark code information o See our Grace period for individual health plans purchased on the Exchange article on our Health Exchange Information Page 37 37
38 Claim Adjustments Appeal vs. Complaint Guide to Provider Complaints and Appeals accessed under o Appeal A formal request to change a decision upheld through the complaint process or reverse an adverse Utilization Management decision. o Complaint any expression of dissatisfaction submitted by a provider concerning claim payments or member benefits Link: Guide to Provider Complaints and Appeals 38 38
39 Claim Adjustments Complaints Administrative or operational in nature Your local Anthem plan is responsible for these decision o Claim processing, benefit interpretation and reimbursement o Not related to medical necessary, experimental or investigational or precertification decisions Send a Provider Adjustment Request Form o Under Answers@Anthem, choose Provider Forms, Provider Adjustment Request Form Send a Secure Message 39 39
40 Claim Adjustments Complaints Administrative or operational in nature o Provider Requests for Adjustment Local, BlueCard, Anthem Medicare Advantage PPO & FEP PO Box , Atlanta, GA
41 Claim Adjustments Complaints Secure Message via Availity o Under Claims Management Select Secure Messaging o From Claim Status Inquiry Select Send a Secure Message 41 41
42 Claim Adjustments Complaints and Appeals Complaints Secure Message via Availity o Immediate confirmation that inquiry was delivered successfully o Sent to Anthem Customer Service based on line of business o Tracking in Anthem Customer Service Call System o Response sent to your Secure Message Mail box o Average Response Time FEP 10 days Local (Facets) 3 days National (Nasco) 3 days BlueCard 30 days 42 42
43 Claim Adjustments Complaints and Appeals Complaints Telephonic Service o Call the service numbers indicated on the Ready Reference Guide or printed on your remittance advice. o If you do not feel your question or issue was adequately addressed Ask to speak to a supervisor If this does not resolve your issue Contact your Network Relations Consultant Provide the call reference numbers given by the telephonic service associates you spoke with 43 43
44 Claim Adjustments Complaints and Appeals Issue Escalation Secure Messaging o If you do not feel your question or issue was adequately addressed send another secure message requesting escalation to a supervisor Telephonic Service o If you do not feel your question or issue was adequately addressed, ask to speak to a supervisor Network Relations o If supervisor escalation does not resolve your issue Contact your Network Relations Consultant Provide the call reference numbers given by the telephonic service associates you spoke with 44 44
45 Claim Adjustments Complaints and Appeals Appeals Requests to change clinical decisions based on whether a service or supplies are medically necessary or experimental or investigational Always submitted secondarily to a reconsideration request or complaint. Applicable to o Local Anthem Members o BlueCard Members o Other Programs Federal Employee Program (FEP) Medicare Advantage 45 45
46 Claim Adjustments Complaints and Appeals Appeals Local Anthem Members Submit a complaint first Submit appeals in writing with a copy of our response to your complaint Use the Provider Appeal Checklist to ensure all information needed is included Mail the information to: Anthem Blue Cross and Blue Shield Attn: Appeals Department PO Box Atlanta, GA For additional information see the Provider Complaints and Appeals Process under the Answers@Anthem menu 46 46
47 Claim Adjustments Appeals BlueCard Program Members Clinical and benefit decisions are made by the members Home plan Your local Wisconsin plan is your single point of contact Use the Provider Adjustment Request Form Send to the local claims and correspondence address Anthem Blue Cross and Blue Shield Attn: Appeals Department PO Box Atlanta, GA Your local plan will facilitate the process with the on your behalf 47 47
48 Claim Adjustments Appeals Other Program Members Federal Employee Plan (FEP) o o o o o Follow specified directions Submit a verbal or written complaint first Submit appeals in writing within 180-days of initial adverse action Use the Provider Adjustment Request Form Send to the local claims and correspondence address Anthem Blue Cross and Blue Shield Attn: Appeals Department PO Box Atlanta, GA o Appeals routed directly to FEP who will respond o Questions Contact FEP in Wisconsin at
49 Claim Adjustments Appeals Other Program Members Anthem Medicare Advantage o Requirements and Process defined by Medicare o Access at o Includes all Anthem Medicare Advantage plans Information found in the Medicare Advantage HMO and PPO Provider Guidebook Provider Service Anthem Medicare Advantage Appeals* Fax: Mail Information to: Medicare Advantage Appeals and Grievance 4361 Irwin Simpson Road Mason, OH
50 Links and Handouts Guide to Provider Complaints and Appeals Contact Us Page Provider Forms EDI Solutions EDI Registration-Forms CAQH EnrollHub Handout - Provider Remittance Advice Example Handout - Anthem EFT ERA Brochure 50 50
51 Provider Claim Submission & Adjustment Requests Tips and Tools 51 51
52 Working with Anthem Subject Specific Webinar Series Please complete the Webinar Evaluation Survey Individuals completing the evaluation survey within 2 business days will be eligible for a Blue Prize package. Winner will be notified by within 3 business days Thank you for attending Anthem Blue Cross and Blue Shield is the trade name of Blue Cross Blue Shield of Wisconsin ("BCBSWi") which underwrites or administers the PPO and indemnity policies; Compcare Health Services Insurance Corporation ("Compcare") which underwrites or administers the HMO policies; and Compcare and BCBSWi collectively which underwrite or administer the POS policies. Independent licensees of the Blue Cross and Blue Shield Association. ANTHEM is a registered trademark of Anthem Insurance Companies, Inc. The Blue Cross and Blue Shield names and symbols are registered marks of the Blue Cross and Blue Shield Association
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
 Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Montgomery County Medical Society
 Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Provider Manual. The BlueCard Program
 The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
Chapter 7. Billing and Claims Processing
 Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
ancillary claims filing requirements: specialty pharmacy
 ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
Arkansas Blue Cross and Blue Shield
 Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
Housekeeping. Link Participant ID with Audio. Mute your line UNMUTED. Raise your hand with questions
 Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Medicare Advantage Public Provider Portal
 Medicare Advantage Public Provider Portal Assisting Providers in Navigating Anthem s Medicare Advantage Provider Sites www.anthem.com/medicareprovider Updated September 2013 Introduction Providers may
Medicare Advantage Public Provider Portal Assisting Providers in Navigating Anthem s Medicare Advantage Provider Sites www.anthem.com/medicareprovider Updated September 2013 Introduction Providers may
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Specialty Drug Medical Benefit Management
 Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Medicare Advantage: tools and strategies to collecting
 Medicare Advantage: tools and strategies to collecting 5343 North 118 th Court Milwaukee WI 53225 414 476 1112 fax 414 476 6118 www.specializedmed.com Medicare Advantage WHCA Fall 2017 Presenter: Medicare
Medicare Advantage: tools and strategies to collecting 5343 North 118 th Court Milwaukee WI 53225 414 476 1112 fax 414 476 6118 www.specializedmed.com Medicare Advantage WHCA Fall 2017 Presenter: Medicare
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
Anthem Blue Cross and Blue Shield. Serving Hoosier Healthwise and Healthy Indiana Plan
 Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Pfizer encompass Co-Pay Assistance Program for INFLECTRA :
 Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Eligibility and Benefits Inquiry Guide
 Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Coordination of Benefits (COB)
 Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Precertification requirements for FEP members for BRCA testing and outpatient services
 2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Maine Chapter of the Healthcare Financial Management Association. MaineCare Provider Relations
 Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
Claim Investigation Submission Guide
 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Excellus BlueCross BlueShield Provider Relations Fall Seminar
 Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Veterans Choice Program and Patient-Centered Community Care Claims and Billing Tips Webinar
 Veterans Choice Program and Patient-Centered Community Care Claims and Billing Tips Webinar August 2018 Introduction The U.S. Department of Veterans Affairs (VA) Veterans Choice Program (VCP) and Patient-Centered
Veterans Choice Program and Patient-Centered Community Care Claims and Billing Tips Webinar August 2018 Introduction The U.S. Department of Veterans Affairs (VA) Veterans Choice Program (VCP) and Patient-Centered
The BlueCard Program Provider Manual. March 2018
 M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
Inter-Plan Operations (BlueCard )
 Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
MHS CMS 1500 Tips and Billing Guidelines
 MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
Best Practice Recommendation for. Processing & Reporting Remittance Information ( v) Version 3.93
 Best Practice Recommendation for Processing & Reporting Remittance Information (835 5010v) Version 3.93 For use with ANSI ASC X12N 835 (005010X222) Health Care Claim Payment/Advice Technical Report Type
Best Practice Recommendation for Processing & Reporting Remittance Information (835 5010v) Version 3.93 For use with ANSI ASC X12N 835 (005010X222) Health Care Claim Payment/Advice Technical Report Type
(MO HealthNet) Text Telephone Medical Claims Reimbursement Rate Dispute Medical Necessity Appeal. Attn: Claim Disputes
 KEY CONTACTS The following chart includes several important telephone and fax numbers available to your office. When calling, please have the following information available: NPI (National Provider Identifier)
KEY CONTACTS The following chart includes several important telephone and fax numbers available to your office. When calling, please have the following information available: NPI (National Provider Identifier)
Coordination of Benefits (COB) Professional
 Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
RECONTRACTING 10/31/2016. Aetna Medicare Advantage. Aetna Behavioral Health
 DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
835 Health Care Claim Payment/Advice
 Companion Document 835 835 Health Care Claim Payment/Advice Basic Instructions This section provides information to help you prepare for the ANSI ASC X12 Health Care Claim Payment/Advice (835) transaction.
Companion Document 835 835 Health Care Claim Payment/Advice Basic Instructions This section provides information to help you prepare for the ANSI ASC X12 Health Care Claim Payment/Advice (835) transaction.
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
The benefits of using ExpressPAth for your practice include: Easy access. With 24/7 access, you can submit requests and get answers at any time.
 Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM
 HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
I. Claim submission instructions
 Humboldt Del Norte Independent Practice Association And Humboldt Del Norte Foundation for Medical Care Claims Settlement Practices and Dispute Resolutions Mechanism As required by Assembly Bill 1455, the
Humboldt Del Norte Independent Practice Association And Humboldt Del Norte Foundation for Medical Care Claims Settlement Practices and Dispute Resolutions Mechanism As required by Assembly Bill 1455, the
HIPAA 5010 Webinar Questions and Answer Session
 HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
Update. If the provider is serving: Then: The provider should: The information in this communication applies.
 Update CONTRACTUAL OCTOBER 24, 2017 UPDATE 17-906 5 PAGES Individual Medicare Advantage and IFP Claims Changes Effective January 1, 2018 After Health Net of California, Inc., Health Net Community Solutions,
Update CONTRACTUAL OCTOBER 24, 2017 UPDATE 17-906 5 PAGES Individual Medicare Advantage and IFP Claims Changes Effective January 1, 2018 After Health Net of California, Inc., Health Net Community Solutions,
A more efficient you.
 A more efficient you. Introducing EmployerAccess Anthem s easy-to-use online benefits management system Anthem Blue Cross and Blue Shield is the trade name of: In Colorado: Rocky Mountain Hospital and
A more efficient you. Introducing EmployerAccess Anthem s easy-to-use online benefits management system Anthem Blue Cross and Blue Shield is the trade name of: In Colorado: Rocky Mountain Hospital and
New 2019 Health Care Plan information for all Colorado PERA Retirees Updated
 New 2019 Health Care Plan information for all Colorado PERA Retirees Updated Anthem Blue Cross and Blue Shield (Anthem) would like to provide new 2019 health plan information for Colorado Public Employee
New 2019 Health Care Plan information for all Colorado PERA Retirees Updated Anthem Blue Cross and Blue Shield (Anthem) would like to provide new 2019 health plan information for Colorado Public Employee
Availity TM Eligibility and Benefits Inquiry
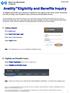 October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
Wright State University. Managing Your Medical Plan
 Wright State University Managing Your Medical Plan 2016 Medical Plans Benefit Year: 1/1/2016 12/31/2016 In-Network 90/10 Plan 80/20 Plan HDHP Calendar Year Deductible Co-Insurance Out-of Pocket Maxi $125/$250
Wright State University Managing Your Medical Plan 2016 Medical Plans Benefit Year: 1/1/2016 12/31/2016 In-Network 90/10 Plan 80/20 Plan HDHP Calendar Year Deductible Co-Insurance Out-of Pocket Maxi $125/$250
835 Payment Advice NPI Dual Receipt
 Chapter 5 NPI Dual Receipt This Companion Document explains the from Anthem Blue Cross and Blue Shield (Anthem) during the 835 National Provider Identifier (NPI) Dual Receipt period. The ANSI ASC X12N,
Chapter 5 NPI Dual Receipt This Companion Document explains the from Anthem Blue Cross and Blue Shield (Anthem) during the 835 National Provider Identifier (NPI) Dual Receipt period. The ANSI ASC X12N,
Claims Management. February 2016
 Claims Management February 2016 Overview Claim Submission Remittance Advice (RA) Exception Codes Exception Resolution Claim Status Inquiry Additional Information 2 Claim Submission 3 4 Life of a Claim
Claims Management February 2016 Overview Claim Submission Remittance Advice (RA) Exception Codes Exception Resolution Claim Status Inquiry Additional Information 2 Claim Submission 3 4 Life of a Claim
Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates
 Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal
 Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
UB-04 Medicare Crossover and Replacement Plans. HP Provider Relations October 2012
 UB-04 Medicare Crossover and Replacement Plans HP Provider Relations October 2012 Agenda Objectives Medicare crossover claim defined Medicare replacement plan claims Electronic billing of crossovers Paper
UB-04 Medicare Crossover and Replacement Plans HP Provider Relations October 2012 Agenda Objectives Medicare crossover claim defined Medicare replacement plan claims Electronic billing of crossovers Paper
835 Health Care Claim Payment / Advice
 Companion Document 835 835 Health Care Claim Payment / Advice This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not
Companion Document 835 835 Health Care Claim Payment / Advice This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not
Welcome to Blue Cross Commercial Risk Adjustment Webinar
 Welcome to Blue Cross Commercial Risk Adjustment Webinar For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background
Welcome to Blue Cross Commercial Risk Adjustment Webinar For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background
Getting started with and using electronic remittance advice (ERA) and electronic funds transfer (EFT)
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Getting started with and using electronic remittance advice (ERA) and electronic funds transfer (EFT) www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Getting started with and using electronic remittance advice (ERA) and electronic funds transfer (EFT) www.aetna.com
National Electronic Data Interchange Transaction Set Companion Guide Health Care Claims Institutional & Professional 837 ASC X12N 837 (005010)
 National Electronic Data Interchange Transaction Set Companion Guide Health Care Claims Institutional & Professional 837 ASC X12N 837 (005010) DMC Managed Care Claims - Electronic Data Interchange Strategy
National Electronic Data Interchange Transaction Set Companion Guide Health Care Claims Institutional & Professional 837 ASC X12N 837 (005010) DMC Managed Care Claims - Electronic Data Interchange Strategy
Secondary Professional Claims on the HCFA-1500
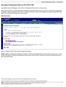 Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
Frequently Asked Questions
 Corrected Claims Submissions 1. What is a corrected claim? If a claim was submitted to and accepted by Healthfirst but was later found to have incorrect information, certain data elements on the claim
Corrected Claims Submissions 1. What is a corrected claim? If a claim was submitted to and accepted by Healthfirst but was later found to have incorrect information, certain data elements on the claim
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION
 CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
Healthy Indiana Plan POWER Account Debit Card
 Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
Essential Drug Formulary
 Essential Drug Formulary January 1, 2017 Benefit Update 51502MUMENABS 01/15 Prescription Drug Plan Anthem s pharmacy program includes 64,000 pharmacies across the country, plus a convenient mail order
Essential Drug Formulary January 1, 2017 Benefit Update 51502MUMENABS 01/15 Prescription Drug Plan Anthem s pharmacy program includes 64,000 pharmacies across the country, plus a convenient mail order
Electronic Claim Adjustments User Guide
 Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
CAQH CORE Training Session
 CAQH CORE Training Session 2016 Marketbased Adjustments Survey Thursday, December 8, 2016 2:00 3:00 PM ET Logistics Presentation Slides & How to Participate in Today s Session Download a copy of today
CAQH CORE Training Session 2016 Marketbased Adjustments Survey Thursday, December 8, 2016 2:00 3:00 PM ET Logistics Presentation Slides & How to Participate in Today s Session Download a copy of today
Provider Dispute Mechanism
 This information is intended to inform you of your rights, responsibilities, and related procedures as they relate to claim practices and provider disputes for commercial HMO, POS, and PPO products where
This information is intended to inform you of your rights, responsibilities, and related procedures as they relate to claim practices and provider disputes for commercial HMO, POS, and PPO products where
PROVIDER VOUCHER OTHER INSURANCE
 00435 9875667 000522 0000961 00001/00002 k00425 1351 WILLIAM HOWARD TAFTROAD FOR RELATED INQUIRES PLEASE CALL OR WRITE: ANTHEM BLUE CROSS AND BLUE SHIELD P.O. BOX 105557 ATLANTA, GA 30348 XXX-XXX-XXXX
00435 9875667 000522 0000961 00001/00002 k00425 1351 WILLIAM HOWARD TAFTROAD FOR RELATED INQUIRES PLEASE CALL OR WRITE: ANTHEM BLUE CROSS AND BLUE SHIELD P.O. BOX 105557 ATLANTA, GA 30348 XXX-XXX-XXXX
Physical Therapy. Contact your Primary Access Administrator (PAA) if Eligibility and Benefits is not listed in the navigation menu.
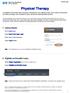 October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
Ambetter 101. Quarterly Provider Webinar February 23, 2017
 Ambetter 101 Quarterly Provider Webinar February 23, 2017 AGENDA 1. What is Ambetter? 2. The Health Insurance Marketplace 3. Public Website and Secure Portal 4. Verification of Eligibility, Benefits and
Ambetter 101 Quarterly Provider Webinar February 23, 2017 AGENDA 1. What is Ambetter? 2. The Health Insurance Marketplace 3. Public Website and Secure Portal 4. Verification of Eligibility, Benefits and
Elite Visa Benefit Card Frequently Asked Questions
 What is the Elite Visa Benefit Card? The Elite Benefit Card is a stored-value card that simplifies the process of paying for qualified health flexible spending account (FSA) expenses. As an alternative
What is the Elite Visa Benefit Card? The Elite Benefit Card is a stored-value card that simplifies the process of paying for qualified health flexible spending account (FSA) expenses. As an alternative
835 Health Care Claim Payment / Advice
 Companion Document 835 835 Health Care Claim Payment / Advice This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not
Companion Document 835 835 Health Care Claim Payment / Advice This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not
A Reference Manual for Group Administrators. Kentucky. with Prime and Complete Dental Programs.
 A Reference Manual for Group Administrators with Prime and Complete Dental Programs Kentucky www.anthem.com TABLE OF CONTENTS WELCOME TO ANTHEM BLUE CROSS AND BLUE SHIELD DENTAL PROGRAM / EMPLOYER SERVICES...1
A Reference Manual for Group Administrators with Prime and Complete Dental Programs Kentucky www.anthem.com TABLE OF CONTENTS WELCOME TO ANTHEM BLUE CROSS AND BLUE SHIELD DENTAL PROGRAM / EMPLOYER SERVICES...1
The Alignment of Financial Services and Healthcare:
 The Alignment of Financial Services and Healthcare: The Electronic Funds Transfer (EFT) Standard And Healthcare Operating Rules for EFT and Electronic Remittance Advice (ERA) Thursday, November 29, 2012
The Alignment of Financial Services and Healthcare: The Electronic Funds Transfer (EFT) Standard And Healthcare Operating Rules for EFT and Electronic Remittance Advice (ERA) Thursday, November 29, 2012
0518.PR.P.PP.2 7/18. The Ins and Outs of CMS 1500 Billing
 0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
835 Health Care Claim Payment / Advice
 Companion Document 835 835 Health Care Claim Payment / Advice This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not
Companion Document 835 835 Health Care Claim Payment / Advice This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not
Effective June 3rd, 2019, Virginia Premier will reject paper claims submitted with incomplete information for required fields.
 April 1, 2019 Provider Billing Guidelines Policy Dear Provider, Per the Centers for Medicaid and Medicare Services (CMS) and Department of Medical Assistance (DMAS), it is the provider's responsibility
April 1, 2019 Provider Billing Guidelines Policy Dear Provider, Per the Centers for Medicaid and Medicare Services (CMS) and Department of Medical Assistance (DMAS), it is the provider's responsibility
eauthorization Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with
 Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
Ambetter of Arkansas. Arkansas Medical Society 12 th Annual Insurance Conference October 1, /5/2015
 Ambetter of Arkansas Arkansas Medical Society 12 th Annual Insurance Conference October 1, 2015 AGENDA 1. Verification of Eligibility 2. Prior Authorization 3. Claims Submission 4. PaySpan 5. Ambetter
Ambetter of Arkansas Arkansas Medical Society 12 th Annual Insurance Conference October 1, 2015 AGENDA 1. Verification of Eligibility 2. Prior Authorization 3. Claims Submission 4. PaySpan 5. Ambetter
Claim Reconsideration Requests Reference Guide
 Claim Reconsideration Requests Reference Guide This reference tool provides instruction regarding the submission of a Claim Reconsideration Request form and details the supporting information required
Claim Reconsideration Requests Reference Guide This reference tool provides instruction regarding the submission of a Claim Reconsideration Request form and details the supporting information required
Northern Arizona Provider Town Hall
 Northern Arizona Provider Town Hall 1 Agenda 01 02 03 04 Welcome Remarks and Introductions Ron Haase Chief Human Resources Officer Northern Arizona Healthcare About UMR Washington Covena / Marisa Aragon
Northern Arizona Provider Town Hall 1 Agenda 01 02 03 04 Welcome Remarks and Introductions Ron Haase Chief Human Resources Officer Northern Arizona Healthcare About UMR Washington Covena / Marisa Aragon
Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims
 Medicare Advantage Provider s Frequently Asked Questions Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims Generally, as a healthcare provider you should file claims for your Blue Cross and
Medicare Advantage Provider s Frequently Asked Questions Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims Generally, as a healthcare provider you should file claims for your Blue Cross and
Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.
 Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.* Revised effective Nov. 15, 2016 *Human Affairs International
Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.* Revised effective Nov. 15, 2016 *Human Affairs International
Best Practice Recommendation for
 Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers
 Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
Medical Policy Guidelines and Procedures
 Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
Research and Resolve UB-04 Claim Denials. HP Provider Relations/October 2014
 Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Electronic Prior Authorization - Provider Guide
 Electronic Prior Authorization - Provider Guide Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient and
Electronic Prior Authorization - Provider Guide Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient and
Provider Healthcare Portal Demonstration:
 Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop
 CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
Electronic PriorAuthorization - Provider Guide. July 2017
 Electronic PriorAuthorization - Provider Guide July 2017 Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient
Electronic PriorAuthorization - Provider Guide July 2017 Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient
Answers to Frequently Asked Questions Comprehensive Quality & Risk Program
 Answers to Frequently Asked Questions Comprehensive Quality & Risk Program What is the Comprehensive Quality & Risk Program? The Comprehensive Quality & Risk Program is a chronic conditions quality of
Answers to Frequently Asked Questions Comprehensive Quality & Risk Program What is the Comprehensive Quality & Risk Program? The Comprehensive Quality & Risk Program is a chronic conditions quality of
Connecticut Medical Assistance Program Long Term Care Refresher Workshop. Presented by: The Department of Social Services & HP for Billing Providers
 Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
For Participating Rehabilitation Therapists May 2006
 For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
