Inter-Plan Operations (BlueCard )
|
|
|
- Eleanore Beatrice Scott
- 6 years ago
- Views:
Transcription
1 Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association
2 Agenda History of BlueCard Claim reminders Program performance Claim tips On the horizon What improvements are coming? Contacting us 2
3 Add title for transition slide BlueCard history 3
4 BlueCard history The BlueCard Program began in 1994 and was designed to enable members traveling or living in another Plan s service area to receive their at home benefits while away. BlueCard allows members to receive the same provider discounts negotiated by the Host Plan (i.e., BCBSNC). BlueCard links participating providers and independent BCBS Plans across the country electronically for claims processing and reimbursement. 4
5 BlueCard history (continued) Who do we service? From 1994 through 2007 BlueCard enrollment has grown from 64 million members to 100,200,000 in 2008 network wide 910,000 Hosted members reside in North Carolina, making Blue Cross and Blue Shield of North Carolina (BCBSNC) the 3rd largest Host Plan 10,363,974 Host claims processed 3,337,785 Home claims processed 5
6 Inter-Plan Programs The BCBSNC department that services BlueCard members has other responsibilities related to the communications & activities between the BCBS Plans The department changed its name to Inter-Plan Programs during July 2006 to accommodate the functions of all Plan-to-Plan programs 6
7 Add title for transition slide Claim reminders 7
8 Claim reminders (members) Utilize a participating provider Carry and ensure that the provider has a copy of their most current ID card Ensure any pre-certifications are obtained Member appeals must be initiated to the member s benefit plan 8
9 Claim reminders (providers) Review the ID card to ensure that the card is current Validate the member s eligibility and benefits Submit claims with correct patient information, which includes: Correct ID number, submit as listed on the card File claim with all pertinent information required to enable BCBSNC to price the claim, e.g., modifiers, CPT codes 9
10 Claim reminders (BCBSNC) Accept claims from all NC participating providers Price and submit all claims to the member s benefit plan for adjudication Administer any request for information between the member s benefit plan and the provider Process the payment and/or denial received from the member s benefit plan to the NC provider Be a liaison for all claim status between our NC providers and the member s benefit plan 10
11 Claim reminders (member s benefit plan) The member s benefit plan is accountable for: Membership validation Applying benefits Adjudicating or denying the claim Eligibility related inquires The buck stops here!!! 11
12 Add title for transition slide 2007 Inter-Plan Program Performance 12
13 Inter-Plan Performance During 2007 IPP received 10,963,974 Host claims, representing $2,091,951, of processed dollars. Implementing programs to pay 99% of original claims within 30 calendar days 100% 80% 60% 40% 20% 0% 1st Qtr 2nd Qtr 3rd Qtr 4th Qtr < 90 days < 60 days < 30 days 13
14 Inter-Plan Performance (continued) In addition, during 2007 Inter-Plan Operations handled: 301,315 Inquires and phone calls were received and resolved through regular customer service 32,383 Inquires were handled through the Plan to Plan Unit 28,103 Callbacks were made on follow up inquires 14
15 Add title for transition slide Claim tips 15
16 How can you help reduce the cycle time on aged claims? Correct claims filing: Make sure that all patient ID # s and prefix s are current and correct, and submit this information as it appears on the ID card Make sure that all pertinent information is included on the claim that will allow BCBSNC to price the claim appropriately For NOC procedures, provide a description of the services. This information can be documented electronically on : For 837 professional claims at the line level, this information can be found at loop 2400, this is in the NTE segment. For 837 institutional claims there is no specific loop or element, however to report at the claim level, this information can be provided at loop 2300, this is for in the NTE segment. For unlisted DME procedures, including the invoice with the claim will help expedite processing. 16
17 Claim tips (continued) Solicited Medical Records Currently there are 3 methods to request and receive solicited medical records USPS, Fax, and Online (Provider Link) The most preferred method is online or fax 17
18 Claim tips (continued) Consider your costs of not responding to solicited medical records requests: Provider Not submitting the information within 10 days Submitting without the BCBSNC cover sheet Not sending the requested information This results in aged provider A/R and potential loss of revenue. Additional administrative expenses BCBSNC Additional administrative expenses Delays in processing claims due to multiple requests being sent to the provider Increases member dissatisfaction 18
19 Claim tips (continued) It is extremely important that the medical record request is read in its entirety to ensure that the BCBS home-plan receives what they need the first time This reduces multiple record submissions and or phone calls to the call centers, which results in delays in determining BCBSNC liability on the claim 19
20 Other opportunities Please ensure that all unsolicited refund request submitted to BCBSNC are printed in black ink and legible File claims electronically as much as possible!!! 20
21 Add title for transition slide Making things easier What we ve done! 21
22 Preauthorizations Scenario: If the provider had acquired preauthorization prior to treating the member and the member s BCBS home-plan denies the claim because records stating that preauthorization was requested cannot be located What is new BCBSNC can now validate that the preauthorization was received over the phone 22
23 Benefit plan requiring member information Scenario To minimize claim denials due to lack of member s COB information What is new The COB questionnaire is now available online Providers can access and provide a copy to the member to capture COB information Providers can use supplied information on the claim Member can forward the completed form to their benefit plan 23
24 Medicare primary Scenario: A provider wishes to research the status of a Medicare cross-over claim What is new The provider can contact BCBSNC s BlueCard Customer Service directly BCBSNC will connect the provider (soft transfer) to the member s benefit plan, or facilitate a conference call for the provider to obtain status 24
25 Add title for transition slide Coming soon! 25
26 Coming soon! End to end New claim adjudication performance metrics Drives host and benefit plan collaboration Blue 2 November 2008 Simplify the preexistence information requests COB January 2009 Providers can be proactive if acquiring COB information from the member BlueCard Member and/or Provider Appeals 26
27 Add title for transition slide Resources 27
28 Resources Blue e SM BlueCard Customer Service Submit general written inquiries to: BCBSNC Inter-Plan Correspondence P.O. Box 2291 Durham, NC Submit Unsolicited Refunds inquiries to (before sending a check): BCBSNC Inter-Plan Correspondence ATTN: Host Refund Inquiries P.O. Box 2291 Durham, NC
29 Add title for transition slide Questions??? 29
30 Acronyms BCBS BCBSNC COB CPT DME ID IG IPP NC NOC USPS Blue Cross and Blue Shield Blue Cross and Blue Shield of North Carolina Coordination of Benefit Current Procedural Terminology Durable Medical Equipment Identification Implementation Guide Inter-Plan Programs North Carolina Not Otherwise Classified United States Postal Service Definitions Benefit Plan Home Plan. The Plan that houses the member s benefits and eligibility 30
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Arkansas Blue Cross and Blue Shield
 Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Precertification requirements for FEP members for BRCA testing and outpatient services
 2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM
 HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Clinical Policies and Procedures for Major Joint and Lower Extremity Services Overview and FAQs for BCBSNC In-Network Providers.
 Clinical Policies and Procedures for Major Joint and Lower Extremity Services Overview and FAQs for BCBSNC In-Network Providers October 17, 2016 Overview Blue Cross and Blue Shield of North Carolina (BCBSNC)
Clinical Policies and Procedures for Major Joint and Lower Extremity Services Overview and FAQs for BCBSNC In-Network Providers October 17, 2016 Overview Blue Cross and Blue Shield of North Carolina (BCBSNC)
Claims Operations. An End to End Overview. An independent licensee of the Blue Cross and Blue Shield Association
 Claims Operations An End to End Overview An independent licensee of the Blue Cross and Blue Shield Association Agenda Let s cover today. End to end Claims Flow From receipt to payment Great Successes in
Claims Operations An End to End Overview An independent licensee of the Blue Cross and Blue Shield Association Agenda Let s cover today. End to end Claims Flow From receipt to payment Great Successes in
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Secondary Professional Claims on the HCFA-1500
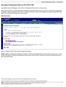 Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
OTHER PARTY LIABILITY PHONE BLUE CROSS AND BLUE SHIELD OF KANSAS TOLL FREE PO BOX 239 FAX TOPEKA, KS
 OTHER PARTY LIABILITY PHONE 785-291-4013 BLUE CROSS AND BLUE SHIELD OF KANSAS TOLL FREE 800-430-1274 PO BOX 239 FAX 785-291-8981 TOPEKA, KS 66601-9913 OTHER PARTY LIABILITY (OPL) is the area within Blue
OTHER PARTY LIABILITY PHONE 785-291-4013 BLUE CROSS AND BLUE SHIELD OF KANSAS TOLL FREE 800-430-1274 PO BOX 239 FAX 785-291-8981 TOPEKA, KS 66601-9913 OTHER PARTY LIABILITY (OPL) is the area within Blue
The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
 Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
I. Claim submission instructions
 Humboldt Del Norte Independent Practice Association And Humboldt Del Norte Foundation for Medical Care Claims Settlement Practices and Dispute Resolutions Mechanism As required by Assembly Bill 1455, the
Humboldt Del Norte Independent Practice Association And Humboldt Del Norte Foundation for Medical Care Claims Settlement Practices and Dispute Resolutions Mechanism As required by Assembly Bill 1455, the
Medical Policy Guidelines and Procedures
 Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Quick guide to Blue member ID cards
 Quick guide to Blue member ID cards A guide for providers who treat out-of-area Blue Cross Blue Shield members Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity
Quick guide to Blue member ID cards A guide for providers who treat out-of-area Blue Cross Blue Shield members Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity
Blue Medicare HMO Blue Medicare PPO
 Blue Medicare HMO Blue Medicare PPO Medicare Fast Track Appeals Medicare Fast Track Appeals An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and BlueShield
Blue Medicare HMO Blue Medicare PPO Medicare Fast Track Appeals Medicare Fast Track Appeals An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and BlueShield
Preferred IPA of California Claims Settlement Practices Provider Notification
 Preferred IPA of California Claims Settlement Practices Provider Notification As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth regulations establishing
Preferred IPA of California Claims Settlement Practices Provider Notification As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth regulations establishing
Ambulance and Emergency Medical Transport Services
 Ambulance and Emergency Medical Transport Services Understanding the basics of BCBSNC processes An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Agenda + Enrollment +
Ambulance and Emergency Medical Transport Services Understanding the basics of BCBSNC processes An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Agenda + Enrollment +
A. Telephone... 2 B. Mail... 2 C. Fax... 3 D. Internet... 3
 Contents For Information Regarding: Refer to Page: I. Communicating with Us A. Telephone... 2 B. Mail... 2 C. Fax... 3 D. Internet... 3 II. Communicating with Affiliated Companies A. Dental Services...
Contents For Information Regarding: Refer to Page: I. Communicating with Us A. Telephone... 2 B. Mail... 2 C. Fax... 3 D. Internet... 3 II. Communicating with Affiliated Companies A. Dental Services...
CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM
 CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM The California Department of Managed Health Care has set forth regulations establishing certain claim settlement practices and a process for resolving
CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM The California Department of Managed Health Care has set forth regulations establishing certain claim settlement practices and a process for resolving
Blue cross of california claims address
 Blue cross of california claims address D Self D Spouse D Son D Daughter. Sex. D M D F. Date of birth (MM/DD/YYYY). Name of other health insurance company Group no. Employer name. Policy no. Section B.
Blue cross of california claims address D Self D Spouse D Son D Daughter. Sex. D M D F. Date of birth (MM/DD/YYYY). Name of other health insurance company Group no. Employer name. Policy no. Section B.
HEALTHCARE REVIEW PROGRAM
 HEALTHCARE REVIEW PROGRAM ANNUAL REPORT 2008 North Carolina Department of Insurance Wayne Goodwin, Commissioner A REPORT ON EXTERNAL REVIEW REQUESTS IN NORTH CAROLINA Healthcare Review Program North Carolina
HEALTHCARE REVIEW PROGRAM ANNUAL REPORT 2008 North Carolina Department of Insurance Wayne Goodwin, Commissioner A REPORT ON EXTERNAL REVIEW REQUESTS IN NORTH CAROLINA Healthcare Review Program North Carolina
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Best Practice Recommendation for
 Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
HOST CLAIM VOLUMES 2009
 1 CLAIMS Claims HOST CLAIM VOLUMES 2009 2 Mountain State Host/Par Claims 3 Medical Policy and Pre-Certification/Pre-Auth Router 4 Medical Policy and Pre-certification/ Pre-Authorization Router Effective
1 CLAIMS Claims HOST CLAIM VOLUMES 2009 2 Mountain State Host/Par Claims 3 Medical Policy and Pre-Certification/Pre-Auth Router 4 Medical Policy and Pre-certification/ Pre-Authorization Router Effective
6. Provider Dispute Resolution Process
 6. Provider Dispute KP actively encourages our contracted Providers to utilize MSCC staff to resolve billing and payment issues. If you remain unable to resolve your billing and payment issues, KP makes
6. Provider Dispute KP actively encourages our contracted Providers to utilize MSCC staff to resolve billing and payment issues. If you remain unable to resolve your billing and payment issues, KP makes
For Participating Rehabilitation Therapists May 2006
 For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
State Employees and Teachers Indemnity Plan. Summer Provider Conferences 2007
 State Employees and Teachers Indemnity Plan Summer Provider Conferences 2007 The North Carolina General Assembly The NC General Assembly is currently in its long session scheduled through mid to late summer
State Employees and Teachers Indemnity Plan Summer Provider Conferences 2007 The North Carolina General Assembly The NC General Assembly is currently in its long session scheduled through mid to late summer
Electronic Claims Submission (EDI) Training
 Electronic Claims Submission (EDI) Training Part 1 How to complete the CMS-1500 form Contact Information: EDI@I-AHC.net 866-374-9558 770-455-0040 1 Two parts of Training Part 1: How to complete CMS-1500
Electronic Claims Submission (EDI) Training Part 1 How to complete the CMS-1500 form Contact Information: EDI@I-AHC.net 866-374-9558 770-455-0040 1 Two parts of Training Part 1: How to complete CMS-1500
WHAT IF YOU DISAGREE WITH OUR DECISION?
 WHAT IF YOU DISAGREE WITH OUR DECISION? In addition to the UM program, BCBSNC offers an appeals process for our MEMBERS. If you want to appeal an ADVERSE BENEFIT DETERMINATION or have a GRIEVANCE, you
WHAT IF YOU DISAGREE WITH OUR DECISION? In addition to the UM program, BCBSNC offers an appeals process for our MEMBERS. If you want to appeal an ADVERSE BENEFIT DETERMINATION or have a GRIEVANCE, you
Medicare Secondary Payer (MSP) Chapter 11
 Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
Medicare Secondary Payer (MSP) Chapter 11
 Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
INDIVIDUAL PRACTICE ASSOCIATION MEDICAL GROUP OF SANTA CLARA COUNTY (SCCIPA)
 INDIVIDUAL PRACTICE ASSOCIATION MEDICAL GROUP OF SANTA CLARA COUNTY (SCCIPA) AB 1455 Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455,
INDIVIDUAL PRACTICE ASSOCIATION MEDICAL GROUP OF SANTA CLARA COUNTY (SCCIPA) AB 1455 Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455,
All Providers. Provider Network Operations. Date: June 22, 2001
 To: From: All Providers Provider Network Operations Date: June 22, 2001 Please te: This newsletter contains information pertaining to Arkansas Blue Cross Blue Shield, a mutual insurance company, it s wholly
To: From: All Providers Provider Network Operations Date: June 22, 2001 Please te: This newsletter contains information pertaining to Arkansas Blue Cross Blue Shield, a mutual insurance company, it s wholly
Provider Appeals Submission Best Practices
 Provider Appeals Submission Best Practices Objective As a result of this session, you should: Be familiar with Harvard Pilgrim s Provider Appeals Policies Understand the most common reasons for submitting
Provider Appeals Submission Best Practices Objective As a result of this session, you should: Be familiar with Harvard Pilgrim s Provider Appeals Policies Understand the most common reasons for submitting
The BlueCard Program Provider Manual. March 2018
 M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
Provider Manual. The BlueCard Program
 The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
HSA-Compatible Health Plans!
 HSA-Compatible Health Plans! Blue Cross and Blue Shield of Illinois offers high deductible health plans that are designed to be used with Health Savings Accounts (HSAs) Two plans: BlueEdgeSM Individual
HSA-Compatible Health Plans! Blue Cross and Blue Shield of Illinois offers high deductible health plans that are designed to be used with Health Savings Accounts (HSAs) Two plans: BlueEdgeSM Individual
Montgomery County Medical Society
 Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
CHAPTER 3: MEMBER INFORMATION
 CHAPTER 3: MEMBER INFORMATION UNIT 4: COORDINATION OF BENEFITS IN THIS UNIT TOPIC SEE PAGE 3.4 COORDINATION OF BENEFITS (COB) 2 3.4 COB: TWO AND THREE PAYER CLAIMS Updated! 4 3.4 FREQUENTLY ASKED QUESTIONS
CHAPTER 3: MEMBER INFORMATION UNIT 4: COORDINATION OF BENEFITS IN THIS UNIT TOPIC SEE PAGE 3.4 COORDINATION OF BENEFITS (COB) 2 3.4 COB: TWO AND THREE PAYER CLAIMS Updated! 4 3.4 FREQUENTLY ASKED QUESTIONS
Kaiser Foundation Health Plan, Inc. CLAIMS SETTLEMENT PRACTICES PROVIDER DISPUTE RESOLUTION MECHANISMS Northern California Region
 Kaiser Foundation Health Plan, Inc. CLAIMS SETTLEMENT PRACTICES PROVIDER DISPUTE RESOLUTION MECHANISMS Northern California Region Kaiser Permanente ( KP ) values its relationship with the contracted community
Kaiser Foundation Health Plan, Inc. CLAIMS SETTLEMENT PRACTICES PROVIDER DISPUTE RESOLUTION MECHANISMS Northern California Region Kaiser Permanente ( KP ) values its relationship with the contracted community
Specialty Drug Medical Benefit Management
 Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
HEALTHCARE REVIEW PROGRAM
 HEALTHCARE REVIEW PROGRAM ANNUAL REPORT 2009 North Carolina Department of Insurance Wayne Goodwin, Commissioner A REPORT ON EXTERNAL REVIEW REQUESTS IN NORTH CAROLINA Healthcare Review Program North Carolina
HEALTHCARE REVIEW PROGRAM ANNUAL REPORT 2009 North Carolina Department of Insurance Wayne Goodwin, Commissioner A REPORT ON EXTERNAL REVIEW REQUESTS IN NORTH CAROLINA Healthcare Review Program North Carolina
Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates
 Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION
 CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
Provider Training Tool & Quick Reference Guide
 Provider Training Tool & Quick Reference Guide Table of Contents I. Coastal Introduction II. Services III. Obtaining Authorization a. Coastal Intake Flow Chart b. Referral/Authorization Form (Sample) IV.
Provider Training Tool & Quick Reference Guide Table of Contents I. Coastal Introduction II. Services III. Obtaining Authorization a. Coastal Intake Flow Chart b. Referral/Authorization Form (Sample) IV.
Veterans Choice Program and Patient-Centered Community Care Claims and Billing Tips Webinar
 Veterans Choice Program and Patient-Centered Community Care Claims and Billing Tips Webinar August 2018 Introduction The U.S. Department of Veterans Affairs (VA) Veterans Choice Program (VCP) and Patient-Centered
Veterans Choice Program and Patient-Centered Community Care Claims and Billing Tips Webinar August 2018 Introduction The U.S. Department of Veterans Affairs (VA) Veterans Choice Program (VCP) and Patient-Centered
Dental Office Implementation Guide
 Dental Office Implementation Guide 9/29/2017 Identification Card FEP BlueDental Announcement The Blue Cross Blue Shield Association (BCBSA) has partnered with the GRID Dental Corporation (GDC) to administer
Dental Office Implementation Guide 9/29/2017 Identification Card FEP BlueDental Announcement The Blue Cross Blue Shield Association (BCBSA) has partnered with the GRID Dental Corporation (GDC) to administer
Transparency Claim Payment Policies & Other Information URL
 Transparency Claim Payment Policies & Other Information URL s a. Out of network liability and balance billing Balance billing occurs when an out-of-network provider bills an enrollee for charges other
Transparency Claim Payment Policies & Other Information URL s a. Out of network liability and balance billing Balance billing occurs when an out-of-network provider bills an enrollee for charges other
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Electronic Claim Adjustments User Guide
 Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
Management: A Guide To Optimizing. Market
 Best Practices In Revenue Cycle Management: A Guide To Optimizing Your Revenue Cycle In A Value-Based Market T h e 2 0 1 8 O P E N M I N D S M a n a g e m e n t B e s t P r a c t i c e s I n s t i t u
Best Practices In Revenue Cycle Management: A Guide To Optimizing Your Revenue Cycle In A Value-Based Market T h e 2 0 1 8 O P E N M I N D S M a n a g e m e n t B e s t P r a c t i c e s I n s t i t u
ancillary claims filing requirements: specialty pharmacy
 ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
HEALTH INSURANCE UTILIZATION REVIEW, APPEALS AND GRIEVANCES AND EXTERNAL REVIEW
 A CONSUMER S GUIDE TO HEALTH INSURANCE UTILIZATION REVIEW, APPEALS AND GRIEVANCES AND EXTERNAL REVIEW If you are a health care consumer and have a complaint about your insurer s denial of a claim or some
A CONSUMER S GUIDE TO HEALTH INSURANCE UTILIZATION REVIEW, APPEALS AND GRIEVANCES AND EXTERNAL REVIEW If you are a health care consumer and have a complaint about your insurer s denial of a claim or some
Coordination of Benefits Reference Guide. WellCare of Georgia. GA022149_PRO_GDE_ENG State Approved WellCare 2013 GA_04_13
 Coordination of Benefits Reference Guide WellCare of Georgia Table of Contents Page 1: Definitions Page 2: Coordination of Benefits Page 3: Basis of Reimbursement Coordination of Benefits Reference Guide
Coordination of Benefits Reference Guide WellCare of Georgia Table of Contents Page 1: Definitions Page 2: Coordination of Benefits Page 3: Basis of Reimbursement Coordination of Benefits Reference Guide
Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.
 Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.* Revised effective Nov. 15, 2016 *Human Affairs International
Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.* Revised effective Nov. 15, 2016 *Human Affairs International
Instructions for Completing the Blue Medicare Supplement SM
 Instructions for Completing the Blue Medicare Supplement SM 1. Page 1; Section 1: Complete your Personal Information. 2. Page 1; Section 2: Select your desired plan. and effective date. Application 3.
Instructions for Completing the Blue Medicare Supplement SM 1. Page 1; Section 1: Complete your Personal Information. 2. Page 1; Section 2: Select your desired plan. and effective date. Application 3.
North Carolina Department of Insurance
 North Carolina Department of Insurance Healthcare Review Program Semiannual Report for the period of James E. Long Commissioner of Insurance A REPORT ON EXTERNAL REVIEW REQUESTS IN NORTH CAROLINA Healthcare
North Carolina Department of Insurance Healthcare Review Program Semiannual Report for the period of James E. Long Commissioner of Insurance A REPORT ON EXTERNAL REVIEW REQUESTS IN NORTH CAROLINA Healthcare
Excellus BlueCross BlueShield Provider Relations Fall Seminar
 Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
Provider Dispute Mechanism
 This information is intended to inform you of your rights, responsibilities, and related procedures as they relate to claim practices and provider disputes for commercial HMO, POS, and PPO products where
This information is intended to inform you of your rights, responsibilities, and related procedures as they relate to claim practices and provider disputes for commercial HMO, POS, and PPO products where
NATIONAL ELEVATOR INDUSTRY HEALTH BENEFIT PLAN 19 Campus Boulevard Suite 200 Newtown Square, PA
 NATIONAL ELEVATOR INDUSTRY HEALTH BENEFIT PLAN 19 Campus Boulevard Suite 200 Newtown Square, PA 19073-3288 800-523-4702 www.neibenefits.org Summary of Material Modifications February 2018 New Option for
NATIONAL ELEVATOR INDUSTRY HEALTH BENEFIT PLAN 19 Campus Boulevard Suite 200 Newtown Square, PA 19073-3288 800-523-4702 www.neibenefits.org Summary of Material Modifications February 2018 New Option for
Appeals for providers
 This section contains information about the processes for the following types of provider appeals and disputes: Dental Provider Appeals and Disputes Medical Provider Appeals and Disputes Hospital/Facility
This section contains information about the processes for the following types of provider appeals and disputes: Dental Provider Appeals and Disputes Medical Provider Appeals and Disputes Hospital/Facility
Instructions To Complete The Highmark Blue Shield Billing Dispute Form For MDs and DOs
 As of September 5, 2008, the Billing Dispute External Review Process is available to physicians who are class members of the Love Settlement Agreement ( the Settlement Agreement ) and the physician groups
As of September 5, 2008, the Billing Dispute External Review Process is available to physicians who are class members of the Love Settlement Agreement ( the Settlement Agreement ) and the physician groups
Filing Secondary Claims on Provider Express
 Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
TRANSPORTATION. [Type text] [Type text] [Type text] Version
![TRANSPORTATION. [Type text] [Type text] [Type text] Version TRANSPORTATION. [Type text] [Type text] [Type text] Version](/thumbs/89/101159249.jpg) New York State Billing Guidelines [Type text] [Type text] [Type text] Version 2016-01 5/26/2016 EMEDNY INFORMATION emedny is the name of the New York State Medicaid system. The emedny system allows New
New York State Billing Guidelines [Type text] [Type text] [Type text] Version 2016-01 5/26/2016 EMEDNY INFORMATION emedny is the name of the New York State Medicaid system. The emedny system allows New
Medicare Advantage Private Fee-for-service Plan Model Terms and Conditions of Payment
 Medicare Advantage Private Fee-for-service Plan Model Terms and Conditions of Payment Table of Contents 1. Introduction 2. When a provider is deemed to accept Humana Gold Choice PFFS terms and conditions
Medicare Advantage Private Fee-for-service Plan Model Terms and Conditions of Payment Table of Contents 1. Introduction 2. When a provider is deemed to accept Humana Gold Choice PFFS terms and conditions
CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM
 As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth regulations establishing certain claim settlement practices and the process for resolving claims disputes
As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth regulations establishing certain claim settlement practices and the process for resolving claims disputes
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
CHOC Health Alliance Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM
 CHOC Health Alliance Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
CHOC Health Alliance Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
UnitedHealthcare Community Plan of Iowa. Annual Provider Training
 UnitedHealthcare Community Plan of Iowa Annual Provider Training Agenda Communication Prior Authorization Appeals Claims and Billing Doc #: PCA-1-003045-08182016_0822016 Communication Communication Where
UnitedHealthcare Community Plan of Iowa Annual Provider Training Agenda Communication Prior Authorization Appeals Claims and Billing Doc #: PCA-1-003045-08182016_0822016 Communication Communication Where
Anthem Blue Cross and Blue Shield. Serving Hoosier Healthwise and Healthy Indiana Plan
 Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Provider Reconsideration and Appeals. BlueCross BlueShield of Tennessee, Inc. an Independent Licensee of the BlueCross BlueShield Association
 Provider Reconsideration and Appeals BlueCross BlueShield of Tennessee, Inc. an Independent Licensee of the BlueCross BlueShield Association What is a Provider Claim Reconsideration? A claim reconsideration
Provider Reconsideration and Appeals BlueCross BlueShield of Tennessee, Inc. an Independent Licensee of the BlueCross BlueShield Association What is a Provider Claim Reconsideration? A claim reconsideration
Avenues of Resolution for Indiana Health Coverage Programs
 Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Cedars-Sinai Medical Group Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM
 Cedars-Sinai Medical Group Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has
Cedars-Sinai Medical Group Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has
Cenpatico South Carolina Frequently Asked Questions (FAQ)
 Cenpatico South Carolina Frequently Asked Questions (FAQ) GENERAL Who is Cenpatico? Cenpatico, a division of Centene Corporation, is one of the nation s most experienced behavioral health companies providing
Cenpatico South Carolina Frequently Asked Questions (FAQ) GENERAL Who is Cenpatico? Cenpatico, a division of Centene Corporation, is one of the nation s most experienced behavioral health companies providing
Living Choices Assisted Living September 2016 HP Fiscal Agent for the Arkansas Division of Medical Services
 Living Choices Assisted Living September 2016 HP Fiscal Agent for the Arkansas Division of Medical Services 1 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and
Living Choices Assisted Living September 2016 HP Fiscal Agent for the Arkansas Division of Medical Services 1 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and
Section 7 Billing Guidelines
 Section 7 Billing Guidelines Billing, Reimbursement, and Claims Submission 7-1 Submitting a Claim 7-1 Corrected Claims 7-2 Claim Adjustments/Requests for Review 7-2 Behavioral Health Services Claims 7-3
Section 7 Billing Guidelines Billing, Reimbursement, and Claims Submission 7-1 Submitting a Claim 7-1 Corrected Claims 7-2 Claim Adjustments/Requests for Review 7-2 Behavioral Health Services Claims 7-3
IDAHO INDIVIDUAL APPLICATION COVER SHEET FOR ENROLLMENT OUTSIDE OF THE IDAHO EXCHANGE
 IDAHO INDIVIDUAL APPLICATION COVER SHEET FOR ENROLLMENT OUTSIDE OF THE IDAHO EXCHANGE Welcome to Blue Cross of Idaho To apply for medical and/or dental coverage for 2016, complete this cover sheet and
IDAHO INDIVIDUAL APPLICATION COVER SHEET FOR ENROLLMENT OUTSIDE OF THE IDAHO EXCHANGE Welcome to Blue Cross of Idaho To apply for medical and/or dental coverage for 2016, complete this cover sheet and
Evidence of Coverage: Your Medicare Health Benefits and Services as a Member of Aetna Medicare SM Plan (PPO).
 January 1 December 31, 2018 Evidence of Coverage: Your Medicare Health Benefits and Services as a Member of Aetna Medicare SM Plan (PPO). This booklet gives you the details about your Medicare health care
January 1 December 31, 2018 Evidence of Coverage: Your Medicare Health Benefits and Services as a Member of Aetna Medicare SM Plan (PPO). This booklet gives you the details about your Medicare health care
Provider Manual. Section 5: Billing and Payment
 Provider Manual TABLE OF CONTENTS SECTION 5 SECTION 5: BILLING AND PAYMENT... 1 INTRODUCTION... 6 CLAIMS SUBMISSION GUIDE HIGHLIGHTS... 7 WHO TO CALL WITH QUESTIONS... 7 NATIONAL PROVIDER IDENTIFIER (NPI)...
Provider Manual TABLE OF CONTENTS SECTION 5 SECTION 5: BILLING AND PAYMENT... 1 INTRODUCTION... 6 CLAIMS SUBMISSION GUIDE HIGHLIGHTS... 7 WHO TO CALL WITH QUESTIONS... 7 NATIONAL PROVIDER IDENTIFIER (NPI)...
Please submit claims and encounters electronically via Office Ally at
 Claim Submission All claims must be submitted within 90 calendar days from the date of service for contracted providers unless otherwise stated in the provider service agreement. Please submit claims and
Claim Submission All claims must be submitted within 90 calendar days from the date of service for contracted providers unless otherwise stated in the provider service agreement. Please submit claims and
Coordination of Benefits (COB)
 Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more Plans providing benefits or services for medical treatment.
Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more Plans providing benefits or services for medical treatment.
Other Coverage Questionnaire
 PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
MDwise Healthy Indiana Plan (HIP)
 MDwise Healthy Indiana Plan (HIP) Annual IHCP Seminar October 2012 Exclusively serving Indiana families since 1994. HIPP0080 (10/11) Topics Comparison between Hoosier Healthwise and Healthy Indiana Plan
MDwise Healthy Indiana Plan (HIP) Annual IHCP Seminar October 2012 Exclusively serving Indiana families since 1994. HIPP0080 (10/11) Topics Comparison between Hoosier Healthwise and Healthy Indiana Plan
Claims and Appeals Process for the Self-Funded Medical Plans Administered by UnitedHealthcare
 SUPPLEMENT TO SUMMARY OF BENEFITS HANDBOOK FOR RETIREES AND SURVIVING DEPENDENTS Claims and Appeals Process for the Self-Funded Medical Plans Administered by UnitedHealthcare Filing a Claim for Benefits
SUPPLEMENT TO SUMMARY OF BENEFITS HANDBOOK FOR RETIREES AND SURVIVING DEPENDENTS Claims and Appeals Process for the Self-Funded Medical Plans Administered by UnitedHealthcare Filing a Claim for Benefits
Billing and Payment. To register, call UHC-FAST ( ) or your local Evercare provider representative.
 Billing and Payment Billing and Claims On the Web www.unitedhealthcareonline.com Register for UnitedHealthcare Online SM, our free Web site for network physicians and health care professionals. At UnitedHealthcare
Billing and Payment Billing and Claims On the Web www.unitedhealthcareonline.com Register for UnitedHealthcare Online SM, our free Web site for network physicians and health care professionals. At UnitedHealthcare
Claim Reconsideration Requests Reference Guide
 Claim Reconsideration Requests Reference Guide This reference tool provides instruction regarding the submission of a Claim Reconsideration Request form and details the supporting information required
Claim Reconsideration Requests Reference Guide This reference tool provides instruction regarding the submission of a Claim Reconsideration Request form and details the supporting information required
LEARNING WHAT IT TAKES TO BILL MANAGED CARE INSURANCES
 home health LEARNING WHAT IT TAKES TO BILL MANAGED CARE INSURANCES Lynn Labarta, CEO, Imark Billing 1 home health LYNN LABARTA CEO, Imark Billing Founder of Imark Billing with over 15 years experience
home health LEARNING WHAT IT TAKES TO BILL MANAGED CARE INSURANCES Lynn Labarta, CEO, Imark Billing 1 home health LYNN LABARTA CEO, Imark Billing Founder of Imark Billing with over 15 years experience
PPO PLANS DISCLOSURE FORM Blue Cross and Blue Shield of Arizona Effective on and after January 1, 2012
 PPO PLANS DISCLOSURE FORM Blue Cross and Blue Shield of Arizona Effective on and after January 1, 2012 This form applies to the following plans: BluePreferred 100/50, BluePreferred 90/70, BluePreferred
PPO PLANS DISCLOSURE FORM Blue Cross and Blue Shield of Arizona Effective on and after January 1, 2012 This form applies to the following plans: BluePreferred 100/50, BluePreferred 90/70, BluePreferred
AETNA BETTER HEALTH OF FLORIDA Claims Adjustment Request & Provider Claim Reconsideration Form
 Aetna Better Health of Florida 1340 Concord Terrace Sunrise, FL 33323 AETNA BETTER HEALTH OF FLORIDA Claims Adjustment Request & Provider Claim Reconsideration Form Aetna Better Health of Florida is committed
Aetna Better Health of Florida 1340 Concord Terrace Sunrise, FL 33323 AETNA BETTER HEALTH OF FLORIDA Claims Adjustment Request & Provider Claim Reconsideration Form Aetna Better Health of Florida is committed
********IMPORTANT NOTICE********
 ********IMPRTANT NTICE******** Subscriber (and/or Spouse) Name Address 1 Address 2 City, State, Zip Date of Notice: Benefits Termination Date: Election Rights Expire on: Subscriber or Member ID Number:
********IMPRTANT NTICE******** Subscriber (and/or Spouse) Name Address 1 Address 2 City, State, Zip Date of Notice: Benefits Termination Date: Election Rights Expire on: Subscriber or Member ID Number:
Forms & Publications: Manuals, Bulletins, Quick Points, Provider Press. Administrative Updates: Forms for Demographic Changes
 MMGMA DAY WITH THE PAYERS May 19, 2016 Janet Benton, Director Provider Relations Kate Mikonowicz, Network Management Consultant, Pr. Shannon Hoskin, Network Management Consultant, Sr. Blue Cross and Blue
MMGMA DAY WITH THE PAYERS May 19, 2016 Janet Benton, Director Provider Relations Kate Mikonowicz, Network Management Consultant, Pr. Shannon Hoskin, Network Management Consultant, Sr. Blue Cross and Blue
Chapter 7. Billing and Claims Processing
 Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
ASO. BlueCross BlueShield of Oregon. Core Offerings SELF-FUNDED GROUPS, SIZED 100+ Crater Lake
 BlueCross BlueShield of Oregon ASO Core Offerings SELF-FUNDED GROUPS, SIZED 100+ Regence BlueCross BlueShield of Oregon is an Independent Licensee of the Blue Cross and Blue Shield Association Crater Lake
BlueCross BlueShield of Oregon ASO Core Offerings SELF-FUNDED GROUPS, SIZED 100+ Regence BlueCross BlueShield of Oregon is an Independent Licensee of the Blue Cross and Blue Shield Association Crater Lake
AMENDMENT 5 TO THE ADMINISTRATIVE SERVICES AGREEMENT WITH SAN JOAQUIN VALLEY INSURANCE AUTHORITY
 AMENDMENT 5 TO THE ADMINISTRATIVE SERVICES AGREEMENT WITH SAN JOAQUIN VALLEY INSURANCE AUTHORITY This is an Amendment to the Administrative Services Agreement as of January 1, 2015. This Amendment shall
AMENDMENT 5 TO THE ADMINISTRATIVE SERVICES AGREEMENT WITH SAN JOAQUIN VALLEY INSURANCE AUTHORITY This is an Amendment to the Administrative Services Agreement as of January 1, 2015. This Amendment shall
Administrative Guide. Physician, Health Care Professional, Facility and Ancillary Provider. UHCCommunityPlan.com KanCare Program
 Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide UHCCommunityPlan.com 2013 KanCare Program Community Plan Welcome to UnitedHealthcare This administrative guide
Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide UHCCommunityPlan.com 2013 KanCare Program Community Plan Welcome to UnitedHealthcare This administrative guide
Provider Dispute/Appeal Procedures
 Provider Dispute/Appeal Procedures Providers have the opportunity to request resolution of Disputes or Formal Provider Appeals that have been submitted to the appropriate internal Keystone First department.
Provider Dispute/Appeal Procedures Providers have the opportunity to request resolution of Disputes or Formal Provider Appeals that have been submitted to the appropriate internal Keystone First department.
