Secondary Professional Claims on the HCFA-1500
|
|
|
- Meryl Simmons
- 6 years ago
- Views:
Transcription
1 Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry section with your profile, a Claims Entry Agreement will appear. Read the agreement and click on Accept to continue. (If you do not accept, you will be returned to the main page.) You only need to accept once for the profile. Welcome screen Click on Submit a HCFA-500 Claim to begin the process. Please note: Only healthcare professionals located in the BlueCross BlueShield of South Carolina service area, or with offices in contiguous counties to the BlueCross service area, may file online. All others must file to the BlueCross plan in their local service area. SM My Insurance Manager is a Service Mark of BlueCross BlueShield of South Carolina. BlueCross BlueShield of South Carolina is an independent licensee of the Blue Cross and Blue Shield Association.
2 To file a secondary claim, answer No to the question, Is this plan the primary payer? 3. First, choose the Tax ID Number Type Employer s Identification Number (EIN) or Social Security Number (SSN).. Second, choose the health plan from the menu. Important: To avoid claim processing delays or denials, be sure to choose the correct health plan. 3. To file a secondary claim, answer No to the question, Is this plan the primary payer? Complete information on the Billing Location Selection, Patient Information, General Claim Information and other screens as you would a primary claim until you get to the Other Payer screen.
3 Other Payer Screen HCFA Other Payer s Name You may type in any entry, from the name of the other insurance company to the name of the kind of insurance. Example: For a Medicare claim, select Medicare in the Other Payer box, then type in Medicare in the Other Payer s Name, and then choose Medicare under the Insurance Type menu.. Claim Type Choose the type from the menu. If you have chosen Medicare in the Other Payer s Name box, you must choose Medicare. 3. Member and Patient Information Member Type can be confusing. HIPAA requires us to report whether or not the insured is a person. For example, in the case of worker s compensation, the insured may be a company. From the Relationship to Member menu, choose the patient s relationship to the member. In the Last or Organization Name, enter the name of the insured (or the insured company). 3
4 Line Selection for Adjustments This screen appears after you have filled in the claim lines and passed the base claim validation screen. Click on the blue line number to adjust a line. If you have more than one line to adjust, you will be directed back to this screen for the next selection after you finish adjusting each line. 4
5 Line Level Adjustments Screen HCFA-500 Most common claims adjustments 3a 3b 4 Please see the next page for an explanation of the red numbers on this example. 5
6 . You may read a list of Claim Adjustment Reason Codes by choosing this link (see page 7). The most common ones are listed in blue above the link.. You must fill in the Procedure Code, Units, Paid Amount and Prior Adjudication Date. 3. Information for COB is found on the remit. In this example, you ll see an adjustment to the patient responsibility group code recorded in claim adjustment group code (3a). You could fill up to five different reason codes in claim adjustment group code. Below, in claim adjustment group code, one reason code is entered for the contractual obligations group code (3b). 4. Choose this link to read detailed information on how to report bundled or unbundled procedures. 6
7 You must choose Continue and validate the information for one line before adjusting another. When you are adjusting multiple lines of a claim, the total of the Paid Amounts on each line s adjustment screen should add up to the total found in the Payer Paid field on the Other Payer screen (seen on page 3). Please note: You must enter an amount beside each reason code you enter. Claim Adjustment Reason Code Table This screen shows part of the table available when you select the link for this table. 7
8 Claim Submission Screen HCFA-500 If you wish to submit the claim now, you may. You can submit additional information on either the () entire claim or () individual lines, but this is NOT required for BlueCross adjudication. HIPAA requires us to give you the opportunity to add additional information. 8
9 Receipt Confirmation Screen After submitting the claim, you will receive a claim number. Please print this page for your records. The print option is in the top right corner. 9
CREATING SECONDARY CLAIMS IN SERVICE CENTER
 CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
Secondary Claims 07/10/2017 1
 Secondary Claims 07/10/2017 1 Example of an MSP Claim (Professional-Processed at Service Line Level) The LOB selected will be the line of business you are submitting to for this claim. Must select Y for
Secondary Claims 07/10/2017 1 Example of an MSP Claim (Professional-Processed at Service Line Level) The LOB selected will be the line of business you are submitting to for this claim. Must select Y for
Medical Eligibility & Benefits Lookup Tips
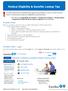 Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
This Member Health Statement reflects medical and pharmacy claims finalized within the preceding 28 days. Member Health Statement THIS IS NOT A BILL
 PO BOX 1798 532 RIVERSIDE AVENUE JACKSONVILLE, FL 32231-0014 GARY J. BLUE 2121 BLUECROSS WAY JACKSONVILLE, FL 32246-0023 HOW CAN BLUE HELP YOU? If you have any questions about your claims activity, please
PO BOX 1798 532 RIVERSIDE AVENUE JACKSONVILLE, FL 32231-0014 GARY J. BLUE 2121 BLUECROSS WAY JACKSONVILLE, FL 32246-0023 HOW CAN BLUE HELP YOU? If you have any questions about your claims activity, please
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Using ERAs with Helper
 Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
Specialty Drug Medical Benefit Management
 Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Understanding your ChiroTouch-Generated CMS 1500 Health Insurance Claim Form
 Understanding your ChiroTouch-Generated CMS 1500 Health Insurance Claim Form Click on any box on the claim form below for a guide to entering this information into ChiroTouch. ChiroTouch cannot advise
Understanding your ChiroTouch-Generated CMS 1500 Health Insurance Claim Form Click on any box on the claim form below for a guide to entering this information into ChiroTouch. ChiroTouch cannot advise
My Benefits: Standard Enrollment HELP MENU MANUAL
 My Benefits: Standard Enrollment HELP MENU MANUAL TABLE OF CONTENTS Page Numbers Access Employee Self-Service... 2 Enroll in Benefits... 3 Additional Information... 8 Add Qualifying Event... 8 Add Dependents
My Benefits: Standard Enrollment HELP MENU MANUAL TABLE OF CONTENTS Page Numbers Access Employee Self-Service... 2 Enroll in Benefits... 3 Additional Information... 8 Add Qualifying Event... 8 Add Dependents
Self-Service Enrollment Instructions. Courtesy of
 Self-Service Enrollment Instructions Courtesy of Self-service Enrollment BenAware s convenient self-service portal is available for use anytime during the open enrollment period. STEP 1: VISIT ENROLLMENT
Self-Service Enrollment Instructions Courtesy of Self-service Enrollment BenAware s convenient self-service portal is available for use anytime during the open enrollment period. STEP 1: VISIT ENROLLMENT
Guide to Fill Out the Enrollment Information Form
 Guide to Fill Out the Enrollment Information Form The Trust will need to know your monthly premium information to update your benefits on your Benefit Convenience Card or send you a Benefit Convenience
Guide to Fill Out the Enrollment Information Form The Trust will need to know your monthly premium information to update your benefits on your Benefit Convenience Card or send you a Benefit Convenience
Quick Guide to Secondary Claims
 Quick Guide to Secondary Claims Would you like to: Please click below what you would like help with to be directed to that specific section in this guide. Convert your primary claim to a secondary claims
Quick Guide to Secondary Claims Would you like to: Please click below what you would like help with to be directed to that specific section in this guide. Convert your primary claim to a secondary claims
Blue care network pre authorization. Blue care network pre authorization
 Paieška Paieška Paieška Blue care network pre authorization Blue care network pre authorization > > Blue Cross Complete (Medicaid) BCN Advantage HMO-POS Formulary Custom Formulary Prior Authorization and
Paieška Paieška Paieška Blue care network pre authorization Blue care network pre authorization > > Blue Cross Complete (Medicaid) BCN Advantage HMO-POS Formulary Custom Formulary Prior Authorization and
COB Smart. Council on Affordable Quality Healthcare (CAQH) Coordination of Benefits (COB) Data Now Included with Our Eligibility Response
 COB Smart Council on Affordable Quality Healthcare (CAQH) Coordination of Benefits (COB) Data Now Included with Our Eligibility Response Experian and the marks used herein are service marks or registered
COB Smart Council on Affordable Quality Healthcare (CAQH) Coordination of Benefits (COB) Data Now Included with Our Eligibility Response Experian and the marks used herein are service marks or registered
Montgomery County Medical Society
 Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
E-Commerce Enrollment
 Electronic Claims Submission HCIQ will electronically submit your primary carrier, professional claims. Please refer to our payer list to view the insurance companies that we currently submit to. Electronic
Electronic Claims Submission HCIQ will electronically submit your primary carrier, professional claims. Please refer to our payer list to view the insurance companies that we currently submit to. Electronic
Inter-Plan Operations (BlueCard )
 Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
BenefitSolver. Employee. Manual
 BenefitSolver Employee Manual 1 TABLE OF CONTENTS New Hire Enrollment Page 3 Life Event Changes Page 8 Change in Beneficiary Page 13 Note: The system will time out after 10 minutes of inactivity. 2 New
BenefitSolver Employee Manual 1 TABLE OF CONTENTS New Hire Enrollment Page 3 Life Event Changes Page 8 Change in Beneficiary Page 13 Note: The system will time out after 10 minutes of inactivity. 2 New
HealthyBlue Simple Steps to a Healthy Reward
 HealthyBlue Simple Steps to a Healthy Reward Taking control of your health has its rewards. With HealthyBlue, all you need to do is complete 3 steps within 180 days of your effective date to earn a Healthy
HealthyBlue Simple Steps to a Healthy Reward Taking control of your health has its rewards. With HealthyBlue, all you need to do is complete 3 steps within 180 days of your effective date to earn a Healthy
Claim Reconsideration Requests Reference Guide
 Claim Reconsideration Requests Reference Guide This reference tool provides instruction regarding the submission of a Claim Reconsideration Request form and details the supporting information required
Claim Reconsideration Requests Reference Guide This reference tool provides instruction regarding the submission of a Claim Reconsideration Request form and details the supporting information required
Best Practice Recommendation for
 Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
OPEN ENROLLMENT DIRECTIONS
 OPEN ENROLLMENT DIRECTIONS EMPLOYEE ONLINE LOG-IN PAGE: emponline.rps205.com https://emponline.rps205.com/ifas7/login/login.aspx?returnurl=%2fifas7%2femponline%2f Use your current Employee Online user
OPEN ENROLLMENT DIRECTIONS EMPLOYEE ONLINE LOG-IN PAGE: emponline.rps205.com https://emponline.rps205.com/ifas7/login/login.aspx?returnurl=%2fifas7%2femponline%2f Use your current Employee Online user
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
MERCER SPECTRUM A SIMPLE SOLUTION FOR EMPLOYERS (WITH MORE THAN 20 EMPLOYEES)
 MERCER SPECTRUM A SIMPLE SOLUTION FOR EMPLOYERS (WITH MORE THAN 20 EMPLOYEES) MERCERSPECTRUM OVERVIEW This guide provides an overview of MercerSpectrum, one of our two online options used for providing
MERCER SPECTRUM A SIMPLE SOLUTION FOR EMPLOYERS (WITH MORE THAN 20 EMPLOYEES) MERCERSPECTRUM OVERVIEW This guide provides an overview of MercerSpectrum, one of our two online options used for providing
CMS 1500 Online Claims Entry. Conduent Government Healthcare Solutions
 CMS 1500 Online Claims Entry Conduent Government Healthcare Solutions Resources When online use: Ask Service Representative HIPAA.Desk.NM@Conduent.com NMProviderSupport@Conduent.com Call Center 505-246-0710
CMS 1500 Online Claims Entry Conduent Government Healthcare Solutions Resources When online use: Ask Service Representative HIPAA.Desk.NM@Conduent.com NMProviderSupport@Conduent.com Call Center 505-246-0710
for employers Quick Reference Guide for Plan Administrators of Personal Funding Accounts inside:
 for employers Quick Reference Guide for Plan Administrators of Personal Funding Accounts inside: Welcome... 2 Implementation of Personal Funding Accounts... 4 Steps for Employers... 4 Steps for Employees...
for employers Quick Reference Guide for Plan Administrators of Personal Funding Accounts inside: Welcome... 2 Implementation of Personal Funding Accounts... 4 Steps for Employers... 4 Steps for Employees...
Let s Get Started Today!
 The Hy-Vee Part-Time Smart Choices Markeplace brought to you by Midwest Heritage Shop and Enroll in 6 Easy Steps Let s Get Started Today! Hy-Vee wants to help you get the insurance coverage you need. You
The Hy-Vee Part-Time Smart Choices Markeplace brought to you by Midwest Heritage Shop and Enroll in 6 Easy Steps Let s Get Started Today! Hy-Vee wants to help you get the insurance coverage you need. You
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims
 Medicare Advantage Provider s Frequently Asked Questions Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims Generally, as a healthcare provider you should file claims for your Blue Cross and
Medicare Advantage Provider s Frequently Asked Questions Empire BlueCross Lab, DME, and Specialty Pharmacy Blue Claims Generally, as a healthcare provider you should file claims for your Blue Cross and
Coordination of Benefits (COB) Professional
 Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Provider Healthcare Portal Demonstration:
 Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
SECTION 9 1 CLAIMS PROCEDURES
 SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
NYIT Self-Service Application Instructions Benefits Open Enrollment AAUP, Faculty and Staff
 NYIT Self-Service Application Instructions Benefits Open Enrollment AAUP, Faculty and Staff The NYIT Self-Service Application gives employees access to view and change certain Benefits data. Benefits which
NYIT Self-Service Application Instructions Benefits Open Enrollment AAUP, Faculty and Staff The NYIT Self-Service Application gives employees access to view and change certain Benefits data. Benefits which
2019 Member Identification Card Guide
 2019 Member Identification Card Guide Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service Revised: Dec. 2018 In the event of any inconsistency between
2019 Member Identification Card Guide Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service Revised: Dec. 2018 In the event of any inconsistency between
All Providers Billing Medicare Crossover Claims. Medical and Institutional Crossover Claim Forms Update
 P R O V I D E R B U L L E T I N BT200143 NOVEMBER 7, 2001 To: Subject: All Providers Billing Medicare Crossover Claims Medical and Institutional Crossover Claim Forms Update Overview This bulletin includes
P R O V I D E R B U L L E T I N BT200143 NOVEMBER 7, 2001 To: Subject: All Providers Billing Medicare Crossover Claims Medical and Institutional Crossover Claim Forms Update Overview This bulletin includes
HIPAA 5010 Webinar Questions and Answer Session
 HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
PC-ACE Secondary Insurance Setup
 This document is intended as a help guide for entering secondary insurance information in the PC-ACE software. It is not intended to replace the general help (accessible by the F1 key) or specific item
This document is intended as a help guide for entering secondary insurance information in the PC-ACE software. It is not intended to replace the general help (accessible by the F1 key) or specific item
2014 Excellus BlueCross BlueShield Medicare PPO Individual Enrollment Request Form
 2014 Excellus BlueCross BlueShield Medicare PPO Individual Enrollment Request Form Excellus BlueCross BlueShield contracts with the federal government and is a PPO plan with a Medicare contract. Enrollment
2014 Excellus BlueCross BlueShield Medicare PPO Individual Enrollment Request Form Excellus BlueCross BlueShield contracts with the federal government and is a PPO plan with a Medicare contract. Enrollment
Other Coverage Questionnaire
 PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
Billing Medicare Secondary Payer (MSP) Claims
 Billing Medicare Secondary Payer (MSP) Claims Per CR8486 effective 1/1/2016 MSP claims for Medicare Part A will be accepted via DDE. Review MM8486 for detailed instructions (https://www.cms.gov/outreach-and-education/medicare-learning-network-
Billing Medicare Secondary Payer (MSP) Claims Per CR8486 effective 1/1/2016 MSP claims for Medicare Part A will be accepted via DDE. Review MM8486 for detailed instructions (https://www.cms.gov/outreach-and-education/medicare-learning-network-
Facility Instruction Manual:
 Facility Instruction Manual: Submitting Secondary Claims with COB Data Elements Overview This supplement to the billing section of the Passport Health Plan (PHP) Provider Manual provides specific coding
Facility Instruction Manual: Submitting Secondary Claims with COB Data Elements Overview This supplement to the billing section of the Passport Health Plan (PHP) Provider Manual provides specific coding
New MN ITS Direct Data Entry (DDE) Screens Professional (837P)
 New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
Go! Guide: Insurance in the EHR
 Go! Guide: Insurance in the EHR Introduction The Insurance tab of the patient chart is where the patient s insurance information is stored and kept up-to-date. It is important that the insurance information
Go! Guide: Insurance in the EHR Introduction The Insurance tab of the patient chart is where the patient s insurance information is stored and kept up-to-date. It is important that the insurance information
14. Roster Processing
 14. Roster Processing Plan processing Roster processing Roster processing roster list You can create rosters by entering data manually or by using the file import capability. If you want to create the
14. Roster Processing Plan processing Roster processing Roster processing roster list You can create rosters by entering data manually or by using the file import capability. If you want to create the
FIND A DOCTOR Page 1 of 22
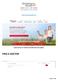 www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
Medicare Advantage Public Provider Portal
 Medicare Advantage Public Provider Portal Assisting Providers in Navigating Anthem s Medicare Advantage Provider Sites www.anthem.com/medicareprovider Updated September 2013 Introduction Providers may
Medicare Advantage Public Provider Portal Assisting Providers in Navigating Anthem s Medicare Advantage Provider Sites www.anthem.com/medicareprovider Updated September 2013 Introduction Providers may
Electronic Claim Adjustments User Guide
 Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
Manage Your Account. User Guide. Retirement planning made easier by Legal & General
 Manage Your Account User Guide Retirement planning made easier by Legal & General Contents What is Manage Your Account (MYA)? 2 How does it work? 3 Why use MYA? 3 Manage Your Account step by step 4 Starting
Manage Your Account User Guide Retirement planning made easier by Legal & General Contents What is Manage Your Account (MYA)? 2 How does it work? 3 Why use MYA? 3 Manage Your Account step by step 4 Starting
Patient Billing and Financial Services
 Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
NOTE: the $50,000 gross receipt threshold is calculated by the average of the current tax year s gross receipts and its two prior years.
 PURDUE UNIVERSITY COOPERATIVE EXTENSION SERVICE Dubois County February 28 th, 2017 Dear 4-H Volunteer, This letter provides information to help your 4-H Club or 4-H Affiliate meet the Internal Revenue
PURDUE UNIVERSITY COOPERATIVE EXTENSION SERVICE Dubois County February 28 th, 2017 Dear 4-H Volunteer, This letter provides information to help your 4-H Club or 4-H Affiliate meet the Internal Revenue
Getting Paid: Master the ABN Advance Beneficiary Notice
 Getting Paid: Master the ABN Advance Beneficiary Notice One of the most popular topics I ve written about over the past 10 years, and the one I get the most email on, is the ins and outs of using the Medicare
Getting Paid: Master the ABN Advance Beneficiary Notice One of the most popular topics I ve written about over the past 10 years, and the one I get the most email on, is the ins and outs of using the Medicare
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request.
 Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request www.providerexpress.com Updated: June 2016 Important Note: Any specific member/provider
Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request www.providerexpress.com Updated: June 2016 Important Note: Any specific member/provider
MedBlue sm Rx (PDP) MedBlue sm Rx Plus (PDP)
 MedBlue sm Rx (PDP) MedBlue sm Rx Plus (PDP) P.O. Box 100191, Columbia, SC 29202-3191 Medicare Prescription Drug Plan Individual Enrollment Form Please contact MedBlue Rx or MedBlue Rx Plus if you need
MedBlue sm Rx (PDP) MedBlue sm Rx Plus (PDP) P.O. Box 100191, Columbia, SC 29202-3191 Medicare Prescription Drug Plan Individual Enrollment Form Please contact MedBlue Rx or MedBlue Rx Plus if you need
MyOEBB Benefits New Hire Enrollment Guide
 MyOEBB Benefits New Hire Enrollment Guide Once you enroll, no plan changes can be made until the next Open Enrollment period unless you experience a Qualified Status Change (QSC)*. *Please see your educational
MyOEBB Benefits New Hire Enrollment Guide Once you enroll, no plan changes can be made until the next Open Enrollment period unless you experience a Qualified Status Change (QSC)*. *Please see your educational
The claims will appear on the list in order of Date Created. The search criteria at the top of the list will assist you in locating past claims.
 P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
Kansas Medical Assistance Program. Vertical Perspective. Other Insurance/Medicare Training Packet - Professional
 Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
Filing Secondary Claims on Provider Express
 Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
RETAIL PREMIUM PAYMENT GUIDE for Producers Processes & Options for Submitting Initial & Ongoing Premiums
 Over 65 RETAIL PREMIUM PAYMENT GUIDE for Producers Processes & Options for Submitting Initial & Ongoing Premiums Making the First Month s Premium... 2 Overview of Payment Options for Paying the First Month
Over 65 RETAIL PREMIUM PAYMENT GUIDE for Producers Processes & Options for Submitting Initial & Ongoing Premiums Making the First Month s Premium... 2 Overview of Payment Options for Paying the First Month
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
Quick Start Guide To Report 401k Contributions Online
 Northern California Carpenters 401k Plan Quick Start Guide To Report 401k Contributions Online Employer Services v1.4 1 Dear Employer, Effective January 1, 2019, contributions to the Northern California
Northern California Carpenters 401k Plan Quick Start Guide To Report 401k Contributions Online Employer Services v1.4 1 Dear Employer, Effective January 1, 2019, contributions to the Northern California
Access to Care. BlueEdge HSA with HSA Bank
 Access to Care SM BlueEdge HSA with HSA Bank Welcome to your BlueEdge HSA, offered by Blue Cross and Blue Shield of Texas (BCBSTX). The BlueEdge HSA combines a high deductible health plan (HDHP) with a
Access to Care SM BlueEdge HSA with HSA Bank Welcome to your BlueEdge HSA, offered by Blue Cross and Blue Shield of Texas (BCBSTX). The BlueEdge HSA combines a high deductible health plan (HDHP) with a
Step 3: To assist us in determining the available list of pharmacy plans to be contracted, please complete the enclosed Insurance Payer List.
 BillingScripts Rx Initial Enrollment Packet Thank you for choosing BillingScripts Rx for your pharmaceutical billing and funding services. This Initial Enrollment Packet contains instructions and forms
BillingScripts Rx Initial Enrollment Packet Thank you for choosing BillingScripts Rx for your pharmaceutical billing and funding services. This Initial Enrollment Packet contains instructions and forms
Claims adjustments Adjustment codes and coordination of benefits (COB)
 Claims adjustments Adjustment codes and coordination of benefits (COB) 23.03.522.1 H (9/17) aetna.com Electronic submission of adjustment group codes and claims adjustment reason codes Aetna is the brand
Claims adjustments Adjustment codes and coordination of benefits (COB) 23.03.522.1 H (9/17) aetna.com Electronic submission of adjustment group codes and claims adjustment reason codes Aetna is the brand
Benefits (ESS): Make Benefit Elections
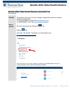 Using BearTrax All Employees Introduction Purpose: The purpose of this task is for you to manage, change and/or submit your benefit elections using BearTrax. To request a password, you ll email beartrax@shawnee.edu.
Using BearTrax All Employees Introduction Purpose: The purpose of this task is for you to manage, change and/or submit your benefit elections using BearTrax. To request a password, you ll email beartrax@shawnee.edu.
Evidence of Coverage:
 January 1 December 31, 2018 Evidence of Coverage: Your Medicare Health Benefits and Services and Prescription Drug Coverage as a Member of Regence MedAdvantage + Rx Enhanced (PPO) This booklet gives you
January 1 December 31, 2018 Evidence of Coverage: Your Medicare Health Benefits and Services and Prescription Drug Coverage as a Member of Regence MedAdvantage + Rx Enhanced (PPO) This booklet gives you
Provider Healthcare Portal Overview. Indiana Health Coverage Programs DXC Technology October 2017
 Provider Healthcare Portal Overview Indiana Health Coverage Programs DXC Technology October 2017 Session Objectives Provider Enrollment transactions Home Page Member Eligibility Prior Authorization Claims
Provider Healthcare Portal Overview Indiana Health Coverage Programs DXC Technology October 2017 Session Objectives Provider Enrollment transactions Home Page Member Eligibility Prior Authorization Claims
Availity TM Eligibility and Benefits Inquiry
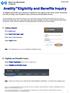 October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
What You Need to Know About
 What You Need to Know About Medical Specialty Drug Prior Authorizations 2016 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service OVERVIEW
What You Need to Know About Medical Specialty Drug Prior Authorizations 2016 Edition Published by Provider Relations and Education Your Partners in Outstanding Quality, Satisfaction and Service OVERVIEW
Electronic Claims Guide
 Electronic Claims Guide Arizona Computer Services, Inc th ARIZONA COMPUTER SERVICES, INC. 5727 N 7 Street Suite 640 Phoenix, Arizona 85014 (602) 263-8958 www.acsmb.com Table of Contents Table of Contents...
Electronic Claims Guide Arizona Computer Services, Inc th ARIZONA COMPUTER SERVICES, INC. 5727 N 7 Street Suite 640 Phoenix, Arizona 85014 (602) 263-8958 www.acsmb.com Table of Contents Table of Contents...
Performance Evaluation System. Recourse: Reviewing a Ratings Recourse Request. Quick-Start Guide for Evaluators
 Performance Evaluation System Ratings D, Recourse: Reviewing a Ratings Recourse Request Quick-Start Guide for Evaluators NOTE: This Quick-Start Guide provides you basic information on navigating through
Performance Evaluation System Ratings D, Recourse: Reviewing a Ratings Recourse Request Quick-Start Guide for Evaluators NOTE: This Quick-Start Guide provides you basic information on navigating through
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers
 Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
Healthy Indiana Plan POWER Account Debit Card
 Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
New MN ITS Direct Data Entry (DDE) Screens Institutional (837I)
 New MN ITS Direct Data Entry (DDE) Screens Institutional (837I) This handout is intended to accompany the MN ITS DDE Institutional (837I) Training Webinar session. It is not intended to replace the MN-ITS
New MN ITS Direct Data Entry (DDE) Screens Institutional (837I) This handout is intended to accompany the MN ITS DDE Institutional (837I) Training Webinar session. It is not intended to replace the MN-ITS
How-To Guide for Calculating Your Annual Healthcare Expenses with mybluecross and OptumRx
 How-To Guide for Calculating Your Annual Healthcare Expenses with mybluecross and OptumRx The guide is only intended to provide a reasonable estimate of out-of-pocket expenses for employees considering
How-To Guide for Calculating Your Annual Healthcare Expenses with mybluecross and OptumRx The guide is only intended to provide a reasonable estimate of out-of-pocket expenses for employees considering
Coordination of Benefits (COB)
 Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
W2/W3 Reporting: Submitting wage and tax information to the Social Security Administration (SSA) This guide will walk you through:
 W2/W3 Reporting: Submitting wage and tax information to the Social Security Administration (SSA) This guide will walk you through: Generating WinStabs reports for rail and bus members Completing electronic
W2/W3 Reporting: Submitting wage and tax information to the Social Security Administration (SSA) This guide will walk you through: Generating WinStabs reports for rail and bus members Completing electronic
Chapter 7. Billing and Claims Processing
 Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Paying and Reporting Form 941 Quarterly T ax
 Paying and Reporting Form 941 Quarterly T ax This guide will walk you through: Documenting tax payments in WinStabs Making tax payments through EFTPS Filing 941 tax return with the IRS Who must file Form
Paying and Reporting Form 941 Quarterly T ax This guide will walk you through: Documenting tax payments in WinStabs Making tax payments through EFTPS Filing 941 tax return with the IRS Who must file Form
Blue Shield. CCHCA Physician Handbook
 Part II Section C Blue Shield Introduction 1 Verifying Blue Shield Member Eligibility and Benefits 1 Blue Shield Sample Member ID Card 2 Pharmacy Benefit 5 Member Grievance Forms 9 CCHCA Physician Handbook
Part II Section C Blue Shield Introduction 1 Verifying Blue Shield Member Eligibility and Benefits 1 Blue Shield Sample Member ID Card 2 Pharmacy Benefit 5 Member Grievance Forms 9 CCHCA Physician Handbook
Anthem Blue Cross and Blue Shield. Serving Hoosier Healthwise and Healthy Indiana Plan
 Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Mybenefits.illinois.gov. Enrolling in Benefits
 Mybenefits.illinois.gov Enrolling in Benefits Benefit Choice Enrollment Once you know which plan is best for you, you can begin the enrollment process. On the MyBenefits home page, click Enroll Now to
Mybenefits.illinois.gov Enrolling in Benefits Benefit Choice Enrollment Once you know which plan is best for you, you can begin the enrollment process. On the MyBenefits home page, click Enroll Now to
Let s Get Started Today!
 The Hy-Vee Part-Time Smart Choices Marketplace brought to you by Midwest Heritage Shop and Enroll in 6 Easy Steps Let s Get Started Today! Hy-Vee wants to help you get the insurance coverage you need.
The Hy-Vee Part-Time Smart Choices Marketplace brought to you by Midwest Heritage Shop and Enroll in 6 Easy Steps Let s Get Started Today! Hy-Vee wants to help you get the insurance coverage you need.
The BlueCard Program Provider Manual. March 2018
 M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
Gilsbar 360 Alliance PROVIDER MANUAL. Gilsbar.
 Gilsbar 360 Alliance PROVIDER MANUAL Gilsbar www.gilsbar360alliance.com Dear Provider: Gilsbar is building a PPO network that gives providers and employers the opportunity to truly work together. We ve
Gilsbar 360 Alliance PROVIDER MANUAL Gilsbar www.gilsbar360alliance.com Dear Provider: Gilsbar is building a PPO network that gives providers and employers the opportunity to truly work together. We ve
Submitting Secondary Claims with COB Data Elements - Facilities
 Overview Submitting Secondary Claims with COB Data Elements - Facilities This supplement to the billing section of the AmeriHealth Caritas Pennsylvania Claims Filing Instruction Manual provides specific
Overview Submitting Secondary Claims with COB Data Elements - Facilities This supplement to the billing section of the AmeriHealth Caritas Pennsylvania Claims Filing Instruction Manual provides specific
ISMA Coalition Meeting September 13, 2013
 ISMA Coalition Meeting September 13, 2013 Questions and Answers 1. For OMPP and each MCE: When will all the Medicaid payers be able to accept electronic claims (837 files) for secondary claims with Primary
ISMA Coalition Meeting September 13, 2013 Questions and Answers 1. For OMPP and each MCE: When will all the Medicaid payers be able to accept electronic claims (837 files) for secondary claims with Primary
State Employee Health Plan and Fully Insured Episodes of Care BlueCross BlueShield of Tennessee Blue Network S Frequently Asked Questions
 The Initiative State Employee Health Plan and Fully Insured Episodes of Care BlueCross BlueShield of Tennessee Blue Network S Frequently Asked Questions 1. What is the Tennessee Healthcare Innovation Initiative?
The Initiative State Employee Health Plan and Fully Insured Episodes of Care BlueCross BlueShield of Tennessee Blue Network S Frequently Asked Questions 1. What is the Tennessee Healthcare Innovation Initiative?
Entering Payments in Aprima PRM
 Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
2018 BlueCross Rx Value SM (PDP) BlueCross Rx Plus SM (PDP)
 P.O. Box 100191, Columbia, SC 29202-3191 2018 BlueCross Rx Value SM (PDP) BlueCross Rx Plus SM (PDP) BlueCross Rx Value/BlueCross Rx Plus Medicare Prescription Drug Plan Individual Enrollment Form Please
P.O. Box 100191, Columbia, SC 29202-3191 2018 BlueCross Rx Value SM (PDP) BlueCross Rx Plus SM (PDP) BlueCross Rx Value/BlueCross Rx Plus Medicare Prescription Drug Plan Individual Enrollment Form Please
County of San Bernardino Retirement Medical Trust (RMT) Plan
 County of San Bernardino Retirement Medical Trust (RMT) Plan One of the benefits offered to eligible employees by the County of San Bernardino is the Retirement Medical Trust (RMT) plan. This is an account
County of San Bernardino Retirement Medical Trust (RMT) Plan One of the benefits offered to eligible employees by the County of San Bernardino is the Retirement Medical Trust (RMT) plan. This is an account
Research and Resolve UB-04 Claim Denials. HP Provider Relations/October 2014
 Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Provider Manual. The BlueCard Program
 The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
Medicaid MCO Complaints
 Medicaid MCO Complaints Medicaid Prompt Payment Compliance Branch Department of Insurance Presentation at the Fall Provider Workshops sponsored by the Department for Medicaid Services and HP Enterprises
Medicaid MCO Complaints Medicaid Prompt Payment Compliance Branch Department of Insurance Presentation at the Fall Provider Workshops sponsored by the Department for Medicaid Services and HP Enterprises
