RECONTRACTING 10/31/2016. Aetna Medicare Advantage. Aetna Behavioral Health
|
|
|
- Jordan Watson
- 5 years ago
- Views:
Transcription
1 DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan. - PPO Product. - Physician Services Based on Medicare Reimbursement. - Follows Aetna coding and guidelines. Aetna Behavioral Health -Separate agreements. -Separate networks. - Adding a new Behavioral Health Provider, visit / Health Care Providers / Join the Network / Select Behavioral Health Applications - Aetna Behavioral Health Customer Service:
2 MERITAIN HEALTH, AN AETNA COMPANY QUICK OVERVIEW A guide for doing business with Meritain Health Contracts Since Meritain Health is a fully owned Aetna subsidiary, if contract includes PPO or Choice POS II products, then your contract also applies to Meritain Health patients who have elected the Aetna network. Please note that Meritain is no longer a part of Aetna Signature Administrators. Sample ID card Recognizing a Meritain member To identify a patient who is using the Aetna network through Meritain, look for the Meritain logo and network by Aetna on the patient s member ID card. Meritain does work with other networks. If an employer selects a network other than Aetna for their employees, Meritain will follow the rules governing those network contracts. Aetna s responsibility Handle claims pricing Provide network access services and management Resolve provider contract issues Meritain s responsibility Handle claims processing Provide customer service Conduct utilization review to determine medical necessity based upon Aetna Clinical Policy Bulletins (criteria) If you don t have access to the website or ID card, call AETNA S HEALTH CARE PROFESSIONALS WEBSITE OPTIONS AVAILABLE WITHOUT LOGIN 5 PROVIDER DEMOGRAPHIC REQUESTS INCLUDE: New Provider Enrollments Is your new Provider already participating in the Aetna/Cofinity Network? Find out at: Aetna Provider Services Cofinity Customer Service If not, contact Aetna Credentialing at to determine the provider s Aetna credentialing status. Updates to Current Providers Do you have changes to your Practice address, Tax ID, or New Patient Status? Need to submit a Provider Termination from your Practice? 6 2
3 SUBMIT DEMOGRAPHIC CHANGES Aetna: Via below form at aetna.com (under Healthcare Professionals and then Helpful Links ) or via NaviNet by Security Officer Cofinity: Via website or send directly to ProviderRelations@Cofinity.net Please allow days for Aetna s and Cofinity s Provider Data Service Teams to process Provider maintenance requests. 7 NEW PROVIDER ENROLLMENTS Provider IS credentialed by Aetna to participate but is not currently tied to your Practice Tax ID. Aetna Direct Groups >NaviNet NaviNet Security Officer transaction or > Health Care Professionals Update Provider Demographic Data Submit or >Fax Letter to Provider Data Maintenance at Provider is NOT currently credentialed by Aetna to participate. Aetna performs credentialing for Aetna and Cofinity Network Participation. > Health Care Professionals Join the Network Submit or >Contact Aetna Credentialing by Phone at Cofinity Network Groups > Find by Customer Provider Contact Us or > Provider Add request to ProviderRelations@cofinity.net or >Contact Cofinity Customer Service by phone at You will need to select: Medical, Dental, or Behavioral If Medical then 2 options: Mid-level (Non-credentialed) or All Other (Credentialed) Provide all Demographic Details: including CAQH #, TIN (if joining a par tin must use group tin), , NPI, License #, if PCP/Spec and more 9 3
4 AETNA CREDENTIALING FAQs 1. I've heard of an organization called the Council for Affordable Quality Healthcare or CAQH. Can you tell me more about this organization? Answer: Yes, CAQH is a nonprofit alliance of America s leading health plans allowing providers to submit one application to meet the needs of all of the health plans and hospitals. 2. If I am already registered with CAQH, what are my next steps? Answer: Please ensure that you have granted Aetna authorization to review your information. 3. If I have not yet registered with CAQH, what are my next steps? Answer: If you have not completed CAQH s online registration, you will receive a registration kit from CAQH within 7-10 business days after submitting your online application. 4. How long does the credentialing process take? Answer: The credentialing process takes approximately 90-days post application submission date. You may check status of your application by contacting our Aetna Credentialing Department at # PROVIDER SERVICE CENTER: Aetna Medicare Service Center: Aetna Credentialing:
5 # # ENTER AETNA HEALTH PLAN Look for Access / Security Officer FAQs and Tips 15 5
6 # AETNA PLAN CENTRAL Left: Aetna Secure Options Center: Check Important Announcements Right: Links to Provider Resources 17 CONTACT AETNA PROVIDER SERVICES DIRECTLY ONLINE Example: Select Support Center / Doing Business With Us see many informational links At Bottom of most screens in Grey Box Under Tools Select Contact 18 6
7 19 20 CONTACT US FEATURE NaviNet Look for a gray shaded Contact link in the lower portion of the screen. Benefits of using the Contact feature include: Dedicated staff committed solely to managing requests directed to Aetna through the Contact feature. Estimated Turnaround Time for response varies by the complexity of your inquiry but you WILL get a response. Reconsideration option drives the claim back through the auto-adjudication process. Eliminates the need to contact the Aetna Service Center via phone. You will provide your own direct name, TIN or NPI, and phone for response. For member type inquires (options 1-5) will need to select Traditional plan (W ID# s) or HMO for Aetna Medicare, also will need Member ID number and Group number. Currently there is an inability to upload attachments with this feature, i.e. medical records, clinical notes, etc. Aetna is researching enhancements. 21 7
8 ELIGIBILITY 22 ELIGIBILITY DETAILS This box shows Product & COB Details Click here to view & Print ID Card 23 WHAT S NEW? ACCESSING ONLINE MEMBER ID CARDS Digital Member IDs Please remember - if an Aetna Patient shows you a digital or printed copy of their ID, you should accept it as valid proof of coverage. 24 8
9 PAYMENT ESTIMATOR / REQUEST SCREEN Type of estimate Billing provider Place of service Diagnosis code(s) Procedure code(s) Billed Charge Choose one 25 SEE ALLOWED FEES, PT. RESP., REDUCTIONS 26 REFERRALS 27 9
10 REFERRAL FORM 28 REFERRAL INQUIRY 29 PRECERTIFICATION 30 10
11 PRECERTIFICATION 31 PRECERTIFICATION FORM 32 PRECERTIFICATION 33 11
12 PRECERTIFICATION CODE SEARCH TOOL 34 ACCESS CLAIM PAYMENT & CODING POLICIES SELECT SUPPORT CENTER / CLAIMS 35 ACCESS WRITTEN PRICING POLICIES 36 12
13 ALPHABETICAL LIST 37 CLICK TO REVIEW AND PRINT 38 ACCESS EOB S RECOMMEND SEARCHING BY PATIENT 39 13
14 SUBMIT CLAIMS FOR RECONSIDERATION ONLINE GO TO CLIAM EOB TOOL / EOB SEARCH POPULATES CLAIM DATA ONLY RUNS BACK THROUGH SYSTEM (I.E. USE WHEN PROVIDER PAR STATUS UPDATED, OR LEVEL 1 APPEAL/RECON) GENERATES TRACKING NUMBER RESOLUTION GENERATES NEW EOB CANNOT SUBMIT NOTES APPROX. 2-3 WEEK TURNAROUND TIN Level Access 40 SUBMIT PROJECT REQUESTS (OVER 25 CLAIMS SAME ISSUE) Select Account Management Tools / Multiple Claim Reconsiderations Specialized Rep. to identify root cause and correct Can submit with just 2 examples, or list all claims Can also first request claim history report to get all claim IDs to copy 41 PROJECTS: APPROX. 45 DAY TURN AROUND WILL PROVIDE REPORT IF REQUESTED AND NEW FINANCIAL DETAILS 42 14
15 MEDICARE ATTESTATION Currently must be completed via NaviNet. If PHO / IPA NaviNet currently does not grant access (working on solution hopefully by end of year) For now this year only, these groups can send attest form with a roster / list of all Tax IDs. Send signed form and tin list to: MedicareFDR@aetna.com 43 WILL SHOW IF EXPIRED Check boxes for steps completed, fill in signature of person attesting and submit. 44 AETNA DISPUTE AND APPEALS PROCESS Mail Appeal letter and records or supporting documents to: Aetna Provider Resolution Team P.O. Box Lexington, KY Fax: Aetna Dispute/Appeals process is summarized on aetna.com First: Claim Reconsideration (or Level 1 appeal) o Submit within 180 days from initial claim decision. o Aetna has up to 60 days to review and respond. Next: Level II appeal must by filed within 60 days of the reconsideration or Level 1 response for HMO-based benefits plans for Indemnity and PPO-based benefits plans 45 15
16 RADIOLOGY PRE-AUTHORIZATION Med Solutions (DBA evicore Healthcare or MSI) is responsible for the preauthorization of high-tech outpatient diagnostic imaging procedures for Aetna members. Preauthorization is required for CT scans, Nuclear cardiology, MRI/MRA, PET scans, Sleep Studies and select cardiac imaging services. Preauthorization can be completed by calling MSI at (888) or online at or FAX (888) AETNA EFT/ERA -Paper-free. The EFT/ERA enrollment is now standard for Aetna -Complete EFT/ERA forms Sign Up for EFT Notification s on NaviNet under Options 47 AETNA OFFICELINK NEWSLETTER -Quarterly updates. -Signup on Navinet under Communications / Newsletters or -National Precertification List. -Clinical Payment, coding and policy changes. -Changes to preferred drug list. -Learning opportunities and more
17 LABORATORY Quest Diagnostics is our national preferred laboratory. It provides tests and services to all Aetna members. Find a convenient location, schedule an appointment and get testing reminders by visiting Quest Diagnostics or calling Your market may also have contracted with local laboratory providers such as: Michigan Joint Venture Hospital Laboratories 49 AETNA STUDENT HEALTH (ASH) NaviNet support eligibility & benefits, claims status inquiry, precertification and referral transactions for members covered under Aetna Student Health plans. AETNA SIGNATURE ADMINISTRATORS (ASA) Providers should direct all ASA claim questions to the appropriate payer on the members card. ASA determines benefits and eligibility. See logo on ID cards below 50 Cofinity Customer Service
18 USING COFINITY S WEBSITE Cofinity s website has many features: Make claims inquiries See repriced amounts Get payer information Access specialty billing rules Find in-network providers Access GH / WC / Auto Participating Payer Lists Updated Quarterly 52 COFINITY WEBSITE View Cofinity s updated website at: for member & claim inquiry, claim activity reports, access payer information, update provider demographic information and other tools. 53 COFINITY WEBSITE 54 18
19 MEMBER CLAIM INQUIRY 55 CLAIMS ACTIVITY REPORT 56 PROVIDER SEARCH FUNCTION 57 19
20 COFINITY BILLING RULES 58 GET CURRENT PRODUCT PAYER LISTS UPDATED QUARTERLY 59 You can also escalate to Cofinity on the website: Go to Cofinity.net / click on a link at the bottom of the page that says Contact Us Select Customer Service option There is a dedicated team of people that work that mailbox on a daily basis
21 CONTACT INFORMATION Aetna Credentialing Aetna Provider Service Navinet Customer Service Cofinity Customer Service Aetna Better Health Secure Provider Web Portal: Aetna Better Health Provider Relations: fax: THANK YOU! QUESTIONS? 62 21
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions October 2016 AAHAM Updates
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions October 2016 AAHAM Updates Debby Synowicki Sr. Provider Relations Representative Aetna s Values Wheel 2 Aetna
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions October 2016 AAHAM Updates Debby Synowicki Sr. Provider Relations Representative Aetna s Values Wheel 2 Aetna
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
UnitedHealthcare IMGMA 2017
 UnitedHealthcare IMGMA 2017 Indiana Advocates 2 Exciting changes are forthcoming! 3 eligibilitylink Voluntary usage deployed on 1-18-17, forced usage deployed on 2-8-17 Patient Eligibility & Benefits removed
UnitedHealthcare IMGMA 2017 Indiana Advocates 2 Exciting changes are forthcoming! 3 eligibilitylink Voluntary usage deployed on 1-18-17, forced usage deployed on 2-8-17 Patient Eligibility & Benefits removed
Housekeeping. Link Participant ID with Audio. Mute your line UNMUTED. Raise your hand with questions
 Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
CoventryCares of Kentucky Provider Training Program
 CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona
 Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
NIA Frequently Asked Questions for Select Health of South Carolina Providers
 NIA Frequently Asked Questions for Select Health of South Carolina Providers Question GENERAL Why is Select Health implementing an outpatient imaging program? Why did Select Health choose National Imaging
NIA Frequently Asked Questions for Select Health of South Carolina Providers Question GENERAL Why is Select Health implementing an outpatient imaging program? Why did Select Health choose National Imaging
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal
 Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
General Who is National Imaging Associates, Inc. (NIA)?
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry West Virginia Providers Performing Physical Medicine Services Question General Who is National Imaging Associates,
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry West Virginia Providers Performing Physical Medicine Services Question General Who is National Imaging Associates,
EXCHANGE NETWORK. First Choice Health Network (FCHN) is excited to be a part of Assurant s initial offering on the Montana Exchange.
 Fall 2014 - FCH Big Sky Region Provider Newsletter EXCHANGE NETWORK First Choice Health Network (FCHN) is excited to be a part of Assurant s initial offering on the Montana Exchange. You may remember that
Fall 2014 - FCH Big Sky Region Provider Newsletter EXCHANGE NETWORK First Choice Health Network (FCHN) is excited to be a part of Assurant s initial offering on the Montana Exchange. You may remember that
GENERAL BENEFIT INFORMATION
 Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers
 NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
Medical Eligibility & Benefits Lookup Tips
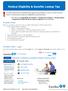 Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
NIA Frequently Asked Questions (FAQ s) For Dean Health Plan Providers
 Question GENERAL Why does Dean Health Plan utilize an outpatient imaging program? Why did select National Imaging Associates, Inc. (NIA) to manage its outpatient advanced imaging NIA Frequently Asked Questions
Question GENERAL Why does Dean Health Plan utilize an outpatient imaging program? Why did select National Imaging Associates, Inc. (NIA) to manage its outpatient advanced imaging NIA Frequently Asked Questions
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For AmeriHealth Caritas District of Columbia (DC) Providers
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For AmeriHealth Caritas District of Columbia (DC) Providers Question GENERAL Why is AmeriHealth Caritas DC implementing an outpatient
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For AmeriHealth Caritas District of Columbia (DC) Providers Question GENERAL Why is AmeriHealth Caritas DC implementing an outpatient
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
Unit 14 Radiology Management
 Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
HealthPlus Amerigroup Provider Training Program
 HealthPlus Amerigroup Provider Training Program Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components How the Program Works: The Authorization
HealthPlus Amerigroup Provider Training Program Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components How the Program Works: The Authorization
Specialty Drug Medical Benefit Management
 Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
HIPAA 5010 Webinar Questions and Answer Session
 HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
PROVIDER MANUAL. Revised January Page 1
 PROVIDER MANUAL Revised January 2018 Page 1 Table of Contents Introduction 3 General Information 4 Who Do I Call? 5 ID Card Logos 6 Credentialing/Recredentialing 7 Provider Changes 8 Referral and Authorization
PROVIDER MANUAL Revised January 2018 Page 1 Table of Contents Introduction 3 General Information 4 Who Do I Call? 5 ID Card Logos 6 Credentialing/Recredentialing 7 Provider Changes 8 Referral and Authorization
Eligibility and Benefits Inquiry Guide
 Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
New Hampshire Healthy Families Quick Reference Guide for Rendering Providers
 New Hampshire Healthy Families Quick Reference Guide for Rendering Providers December 1, 2013 New Hampshire Healthy Families has selected NIA Magellan 1 to implement a radiology benefit management program
New Hampshire Healthy Families Quick Reference Guide for Rendering Providers December 1, 2013 New Hampshire Healthy Families has selected NIA Magellan 1 to implement a radiology benefit management program
Gilsbar 360 Alliance PROVIDER MANUAL. Gilsbar.
 Gilsbar 360 Alliance PROVIDER MANUAL Gilsbar www.gilsbar360alliance.com Dear Provider: Gilsbar is building a PPO network that gives providers and employers the opportunity to truly work together. We ve
Gilsbar 360 Alliance PROVIDER MANUAL Gilsbar www.gilsbar360alliance.com Dear Provider: Gilsbar is building a PPO network that gives providers and employers the opportunity to truly work together. We ve
HealthChoice Illinois
 HealthChoice Illinois November 2017 Presented by: Matt Wolf and Lori Lomahan Meeting Agenda Introductions Credentialing Update Billing Instructions Claims Adjudication Reimbursement Methodology MCO Website
HealthChoice Illinois November 2017 Presented by: Matt Wolf and Lori Lomahan Meeting Agenda Introductions Credentialing Update Billing Instructions Claims Adjudication Reimbursement Methodology MCO Website
1 Buckeye Community Health Plan. Quick Reference Guide for Rendering Providers November 1, 2014
 Buckeye Community Health Plan Quick Reference Guide for Rendering Providers November 1, 2014 Buckeye Community Health Plan has selected NIA Magellan to implement a radiology benefit management program
Buckeye Community Health Plan Quick Reference Guide for Rendering Providers November 1, 2014 Buckeye Community Health Plan has selected NIA Magellan to implement a radiology benefit management program
Avenues of Resolution for Indiana Health Coverage Programs
 Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
(FAQ s) For Florida Aetna Medicare HMO Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Florida Aetna Medicare HMO Providers Question GENERAL Why did Aetna implement an outpatient imaging program? Answer To improve quality and manage the
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Florida Aetna Medicare HMO Providers Question GENERAL Why did Aetna implement an outpatient imaging program? Answer To improve quality and manage the
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Gateway Health Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging program? Why did Gateway Health select NIA Magellan to manage its
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging program? Why did Gateway Health select NIA Magellan to manage its
Cenpatico South Carolina Frequently Asked Questions (FAQ)
 Cenpatico South Carolina Frequently Asked Questions (FAQ) GENERAL Who is Cenpatico? Cenpatico, a division of Centene Corporation, is one of the nation s most experienced behavioral health companies providing
Cenpatico South Carolina Frequently Asked Questions (FAQ) GENERAL Who is Cenpatico? Cenpatico, a division of Centene Corporation, is one of the nation s most experienced behavioral health companies providing
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2012-2013 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 1 of 8 Year 2012-2013 Summary
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2012-2013 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 1 of 8 Year 2012-2013 Summary
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
10/30/2017. Third Party Payer Day: Medicare Plus Blue Claims & System Issue Resolution. Provider contacts Provider Inquiry Service Center
 Third Party Payer Day: Medicare Plus Blue Claims & System Issue Resolution November 10, 2017 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee of the Blue Cross and
Third Party Payer Day: Medicare Plus Blue Claims & System Issue Resolution November 10, 2017 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee of the Blue Cross and
Frequently Asked Questions Radiology Management Program
 Frequently Asked Questions Radiology Management Program Neighborhood Health Plan of Rhode Island (Neighborhood) has implemented a prior authorization program with MedSolutions. This will include clinical
Frequently Asked Questions Radiology Management Program Neighborhood Health Plan of Rhode Island (Neighborhood) has implemented a prior authorization program with MedSolutions. This will include clinical
A Quick Look at Your Health Plan
 A Quick Look at Your Health Plan Memorial Community Hospital Group #14693 When you enroll with Meritain Health, you re taking the next step towards a healthier, more balanced you. It s important for you
A Quick Look at Your Health Plan Memorial Community Hospital Group #14693 When you enroll with Meritain Health, you re taking the next step towards a healthier, more balanced you. It s important for you
Monthly Premiums for Employees/TRS Members working at least 20 hours per week
 2016-17 TRS-ActiveCare Medical Plans Monthly Premiums for Employees/TRS Members working at least 20 hours per week Premiums valid from September 1, 2016 until August 31, 2017 PISD Contribution for full-time
2016-17 TRS-ActiveCare Medical Plans Monthly Premiums for Employees/TRS Members working at least 20 hours per week Premiums valid from September 1, 2016 until August 31, 2017 PISD Contribution for full-time
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna Delaware Providers Performing Physical Medicine Services
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna Delaware Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna Delaware Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
General Who is National Imaging Associates, Inc. (NIA)?
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
General Who is National Imaging Associates, Inc. (NIA)?
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna/Coventry Pennsylvania Providers Performing Physical Medicine Services Question Answer General Who is National Imaging
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES MENTAL HEALTH AND SUBSTANCE ABUSE PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES MENTAL HEALTH AND SUBSTANCE ABUSE PLAN 2010-2011 Call APS Healthcare, Inc. Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES MENTAL HEALTH AND SUBSTANCE ABUSE PLAN 2010-2011 Call APS Healthcare, Inc. Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Medical Policy Guidelines and Procedures
 Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Chapter 7. Billing and Claims Processing
 Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
evicore healthcare Utilization management programs Frequently asked questions
 evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers
 NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers Question GENERAL Why is Home State Health Plan implementing an outpatient imaging program? Answer To improve quality and manage
NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers Question GENERAL Why is Home State Health Plan implementing an outpatient imaging program? Answer To improve quality and manage
A Quick Look at Your Health Plan Citizens Memorial Hospital. Group #16533
 A Quick Look at Your Health Plan Citizens Memorial Hospital Group #16533 When you enroll with, you re taking the next step towards a healthier, more balanced you. It s important for you to understand how
A Quick Look at Your Health Plan Citizens Memorial Hospital Group #16533 When you enroll with, you re taking the next step towards a healthier, more balanced you. It s important for you to understand how
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For Gateway Health Medicare Assured Providers
 Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For Gateway Health Medicare Assured Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging Why did Gateway Health select
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For Gateway Health Medicare Assured Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging Why did Gateway Health select
NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers
 gat NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers Question GENERAL Why is West Virginia Family Health implementing an outpatient imaging program? Why did West
gat NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers Question GENERAL Why is West Virginia Family Health implementing an outpatient imaging program? Why did West
NIA Magellan 1 Frequently Asked Questions (FAQs) for Highmark Health Options Providers
 gat Question GENERAL NIA Magellan 1 Frequently Asked Questions (FAQs) for Providers Why is Highmark Health Options implementing an outpatient imaging program? Why did Highmark Health Options select NIA
gat Question GENERAL NIA Magellan 1 Frequently Asked Questions (FAQs) for Providers Why is Highmark Health Options implementing an outpatient imaging program? Why did Highmark Health Options select NIA
Prior Authorization for Outpatient Injectable Chemotherapy Frequently Asked Questions
 Prior Authorization for Outpatient Injectable Chemotherapy Frequently Asked Questions Key Points We require prior authorization for injectable chemotherapy given in an outpatient setting to a member who
Prior Authorization for Outpatient Injectable Chemotherapy Frequently Asked Questions Key Points We require prior authorization for injectable chemotherapy given in an outpatient setting to a member who
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2011-2012 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year 2011-2012 Summary of
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2011-2012 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year 2011-2012 Summary of
Annual Notice of Changes for 2017
 HAP Senior Plus Option 2 (PPO) offered by Alliance Health and Life Insurance Co. Annual Notice of Changes for 2017 You are currently enrolled as a member of Alliance Medicare PPO. Next year, there will
HAP Senior Plus Option 2 (PPO) offered by Alliance Health and Life Insurance Co. Annual Notice of Changes for 2017 You are currently enrolled as a member of Alliance Medicare PPO. Next year, there will
Consolidated Credentialing Verification Organization (CVO) Initiative
 Consolidated Credentialing Verification Organization (CVO) Initiative The Texas Association of Health Plans (TAHP) in collaboration with the Texas Medical Association (TMA) and Medicaid Managed Care Organizations
Consolidated Credentialing Verification Organization (CVO) Initiative The Texas Association of Health Plans (TAHP) in collaboration with the Texas Medical Association (TMA) and Medicaid Managed Care Organizations
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
NIA Magellan 1 Frequently Asked Questions (FAQ s) For HealthAmerica Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For HealthAmerica Providers Question GENERAL Why is Health America implementing an outpatient imaging program? Answer To improve quality and manage the
NIA Magellan 1 Frequently Asked Questions (FAQ s) For HealthAmerica Providers Question GENERAL Why is Health America implementing an outpatient imaging program? Answer To improve quality and manage the
Louisiana Healthcare Connections Quick Reference Guide for Rendering Providers
 Louisiana Healthcare Connections Quick Reference Guide for Rendering Providers February 1, 2012 Louisiana Healthcare Connections selected NIA Magellan 1 to implement a radiology benefit management program
Louisiana Healthcare Connections Quick Reference Guide for Rendering Providers February 1, 2012 Louisiana Healthcare Connections selected NIA Magellan 1 to implement a radiology benefit management program
Getting started with and using electronic remittance advice (ERA) and electronic funds transfer (EFT)
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Getting started with and using electronic remittance advice (ERA) and electronic funds transfer (EFT) www.aetna.com
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Getting started with and using electronic remittance advice (ERA) and electronic funds transfer (EFT) www.aetna.com
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
2018 Quick Reference Guide
 Effective: 01-01-2018 AARP MedicareComplete (HMO): H1045-030 & H1045-043 AARP MedicareComplete Choice Plan 2 (Regional PPO): R7444-003 AARP Medicare Complete Choice Essential (Regional PPO): R7444-004
Effective: 01-01-2018 AARP MedicareComplete (HMO): H1045-030 & H1045-043 AARP MedicareComplete Choice Plan 2 (Regional PPO): R7444-003 AARP Medicare Complete Choice Essential (Regional PPO): R7444-004
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers
 Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers Question GENERAL Why is CareSource implementing an outpatient imaging program? Answer To improve quality and manage the
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers Question GENERAL Why is CareSource implementing an outpatient imaging program? Answer To improve quality and manage the
LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH
 LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to:
LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to:
Claims. A Quick Guide on the Importance and Process of Handling Claims and Encounter Submissions
 Claims A Quick Guide on the Importance and Process of Handling Claims and Encounter Submissions Claims Benefits of Using Electronic Claims, EFT, & ERA Electronic claim submission has been proven to significantly
Claims A Quick Guide on the Importance and Process of Handling Claims and Encounter Submissions Claims Benefits of Using Electronic Claims, EFT, & ERA Electronic claim submission has been proven to significantly
Provider/Payer Enrollment Tips and Tricks
 Provider/Payer Enrollment Tips and Tricks Thea Hensley Provider Enrollment Coordinator Cody Regional Health 307-578-2498 ahensley@codyregionalhealth.org Vocabulary Provider/Payer Enrollment-Refers to the
Provider/Payer Enrollment Tips and Tricks Thea Hensley Provider Enrollment Coordinator Cody Regional Health 307-578-2498 ahensley@codyregionalhealth.org Vocabulary Provider/Payer Enrollment-Refers to the
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Sunshine Health Quick Reference Guide for Rendering Providers
 Sunshine Health Quick Reference Guide for Rendering Providers Effective June 1, 2011 Revised May 2, 2014 Sunshine Health selected NIA Magellan 1 to implement a radiology benefit management program for
Sunshine Health Quick Reference Guide for Rendering Providers Effective June 1, 2011 Revised May 2, 2014 Sunshine Health selected NIA Magellan 1 to implement a radiology benefit management program for
Glossary of Terms. Adjudication: The way a health plan decides how much it will pay for certain expenses.
 Page 1 Glossary of Terms Adjudication: The way a health plan decides how much it will pay for certain expenses. Affordable Care Act (ACA): The comprehensive health care reform law enacted in March 2010.
Page 1 Glossary of Terms Adjudication: The way a health plan decides how much it will pay for certain expenses. Affordable Care Act (ACA): The comprehensive health care reform law enacted in March 2010.
Calendar Year Medical Deductible Calendar Year Out-of-Pocket Maximum $2,000 per individual / $4,000 per family Lifetime Benefit Maximum
 An independent member of the Blue Shield Association Access+HMO Per Admit 20-500 Benefit Summary (For groups of 101 and above) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California
An independent member of the Blue Shield Association Access+HMO Per Admit 20-500 Benefit Summary (For groups of 101 and above) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Participating Provider Network Orientation. Provider Experience
 Participating Provider Network Orientation Provider Experience Introduction Kaiser Permanente is an integrated healthcare delivery system. We are a healthcare provider and we offer medical services at
Participating Provider Network Orientation Provider Experience Introduction Kaiser Permanente is an integrated healthcare delivery system. We are a healthcare provider and we offer medical services at
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
MHS CMS 1500 Tips and Billing Guidelines
 MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
Maine Chapter of the Healthcare Financial Management Association. MaineCare Provider Relations
 Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
AETNA BETTER HEALTH OF FLORIDA Claims Adjustment Request & Provider Claim Reconsideration Form
 Aetna Better Health of Florida 1340 Concord Terrace Sunrise, FL 33323 AETNA BETTER HEALTH OF FLORIDA Claims Adjustment Request & Provider Claim Reconsideration Form Aetna Better Health of Florida is committed
Aetna Better Health of Florida 1340 Concord Terrace Sunrise, FL 33323 AETNA BETTER HEALTH OF FLORIDA Claims Adjustment Request & Provider Claim Reconsideration Form Aetna Better Health of Florida is committed
Summary of Changes - New Enrollment and Claims Payment System Effective June 1, 2017
 Overview Starting June 1, 2017, UnitedHealthcare Community Plan in Florida will change to a new enrollment and claims payment system. This Summary of Changes is a guide to help answer questions you may
Overview Starting June 1, 2017, UnitedHealthcare Community Plan in Florida will change to a new enrollment and claims payment system. This Summary of Changes is a guide to help answer questions you may
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise.
 Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Northern Arizona Provider Town Hall
 Northern Arizona Provider Town Hall 1 Agenda 01 02 03 04 Welcome Remarks and Introductions Ron Haase Chief Human Resources Officer Northern Arizona Healthcare About UMR Washington Covena / Marisa Aragon
Northern Arizona Provider Town Hall 1 Agenda 01 02 03 04 Welcome Remarks and Introductions Ron Haase Chief Human Resources Officer Northern Arizona Healthcare About UMR Washington Covena / Marisa Aragon
MHS Prior Authorization 0317.PR.P.PP
 MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
Aetna Better Health of Kansas
 Aetna Better Health of Kansas FAQ s from 8/16/18 Webinar General 1. We understand that the injunction and protest by Amerigroup as well as the protests by Wellcare and AmeriHealth will delay some of the
Aetna Better Health of Kansas FAQ s from 8/16/18 Webinar General 1. We understand that the injunction and protest by Amerigroup as well as the protests by Wellcare and AmeriHealth will delay some of the
Section 7. Claims Procedures
 Section 7 Claims Procedures Timely Filing Guidelines 1 Claim Submissions 1 Claims for Referred Services 1 Claims for Authorized Services 2 Filing Electronic Claims 2 Filing Paper Claims 2 Claims Resubmission
Section 7 Claims Procedures Timely Filing Guidelines 1 Claim Submissions 1 Claims for Referred Services 1 Claims for Authorized Services 2 Filing Electronic Claims 2 Filing Paper Claims 2 Claims Resubmission
Overcoming to Become a Provider 3 REIMBURSEMENT RELUCTANCE
 1 Learning Objectives Assess if accepting reimbursement is appropriate for business. Establish Tax ID, NPI number, and CAQH log-in to start credentialing process. Outline process for benefits verification
1 Learning Objectives Assess if accepting reimbursement is appropriate for business. Establish Tax ID, NPI number, and CAQH log-in to start credentialing process. Outline process for benefits verification
KanCare All MCO Training FQHC s & RHC s Spring 2018
 KanCare All MCO Training FQHC s & RHC s Spring 2018 Welcome Introductions Welcome, Introductions & Agenda Agenda Encounter Rates Place of Service (POS) Secondary Claims Credentialing Issues How to avoid
KanCare All MCO Training FQHC s & RHC s Spring 2018 Welcome Introductions Welcome, Introductions & Agenda Agenda Encounter Rates Place of Service (POS) Secondary Claims Credentialing Issues How to avoid
NIA Frequently Asked Questions (FAQ s) For CoventryCares of Kentucky Providers
 Question GENERAL Do Kentucky Members have any copay responsibilities? NIA Frequently Asked Questions (FAQ s) For Providers Answer Members do not have copays for outpatient imaging procedures. PRIOR AUTHORIZATION
Question GENERAL Do Kentucky Members have any copay responsibilities? NIA Frequently Asked Questions (FAQ s) For Providers Answer Members do not have copays for outpatient imaging procedures. PRIOR AUTHORIZATION
New Provider Forms. If you have any questions, please us.
 New Provider Forms Thanks for your interest in becoming a HAP provider. Following this page are three forms we ll need you to complete and return back to us at Providers_Recruitment@hap.org: Physician
New Provider Forms Thanks for your interest in becoming a HAP provider. Following this page are three forms we ll need you to complete and return back to us at Providers_Recruitment@hap.org: Physician
The benefits of using ExpressPAth for your practice include: Easy access. With 24/7 access, you can submit requests and get answers at any time.
 Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
FIND A DOCTOR Page 1 of 22
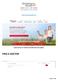 www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
Provider Manual. ChoiceBenefits. BayCare Health System Medical Plan
 2019 Provider Manual ChoiceBenefits BayCare Health System Medical Plan 1 Table of Contents BayCare... 2 BayCare Exclusive Network... 2 Rules unique to Cigna BayCare Members... 2 Provider Relations Representative...
2019 Provider Manual ChoiceBenefits BayCare Health System Medical Plan 1 Table of Contents BayCare... 2 BayCare Exclusive Network... 2 Rules unique to Cigna BayCare Members... 2 Provider Relations Representative...
Aetna Required Clean Claim Elements UB92
 Texas Hospitals and Facilities DISCLOSURE OF CLEAN CLAIM ELEMENTS; DISCLOSURE OF NECESSARY ATTACHMENTS; DISCLOSURE OF ADDITIONAL CLEAN CLAIM ELEMENTS; DISCLOSURE OF REVISION OF DATA ELEMENTS, ATTACHMENTS
Texas Hospitals and Facilities DISCLOSURE OF CLEAN CLAIM ELEMENTS; DISCLOSURE OF NECESSARY ATTACHMENTS; DISCLOSURE OF ADDITIONAL CLEAN CLAIM ELEMENTS; DISCLOSURE OF REVISION OF DATA ELEMENTS, ATTACHMENTS
Excellus BlueCross BlueShield Provider Relations Fall Seminar
 Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Ambetter from Sunshine Health Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did Ambetter from implement an outpatient imaging program? Answer To improve quality and manage the utilization of nonemergent
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did Ambetter from implement an outpatient imaging program? Answer To improve quality and manage the utilization of nonemergent
SECTION 9 1 CLAIMS PROCEDURES
 SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
Ambetter from Sunshine Health Quick Reference Guide for Rendering Providers
 Ambetter from Sunshine Health Quick Reference Guide for Rendering Providers Effective January 1, 2014 Ambetter from Sunshine Health selected NIA Magellan 1 to implement a radiology benefit management program
Ambetter from Sunshine Health Quick Reference Guide for Rendering Providers Effective January 1, 2014 Ambetter from Sunshine Health selected NIA Magellan 1 to implement a radiology benefit management program
Cigna PPO Network. National network. Competitive discounts. Flexible for your business and members.
 Cigna PPO Network National network. Competitive discounts. Flexible for your business and members. Group Benefit Services, Inc. Healthy Advantage Clients CIGNA Preferred Provider Organization (PPO) National
Cigna PPO Network National network. Competitive discounts. Flexible for your business and members. Group Benefit Services, Inc. Healthy Advantage Clients CIGNA Preferred Provider Organization (PPO) National
