Clear Coverage Online Authorizations Community Health Network of CT, Inc.
|
|
|
- Austin McCoy
- 6 years ago
- Views:
Transcription
1 Clear Coverage Online Authorizations Community Health Network of CT, Inc.
2 Overview Clear coverage is an online authorization tool which: Lowers authorization turn around time Improves workflow by decreasing administrative tasks Automates clinical evaluation processes 2
3 Clear Coverage Functionality Provides a web based hosted solution for authorization requests. Allows providers to search authorization request for up to 365 days. Enables providers to review eligibility of members in real time. Creates an authorization request. Allows view of only CMAP Providers Allows providers to attach the supporting clinical documentation to their authorization request. 3
4 Minimum Computer Requirements An Internet browser An Internet browser An Internet browser Adobe Reader An Internet browser Standard Screen Resolution An Internet browser Reliable High Speed Internet Access 4
5 5
6 Public Web Portal: Clear Coverage Inpatient Authorization Admission: Clear Coverage is a web-based decision tool that will give providers the ability to submit an Authorization Request/Prior Authorization electronically, at the point of care, and receive an immediate, realtime response to their request. Sign in or create an account here. 6
7 Log in Screen The Log in Screen for Clear Coverage CHNCT Help Desk:
8 Changing your password 8
9 Home Tab 9
10 Authorization Search 10
11 New Authorization 11
12 Patient Eligibility This eligibility lookup does not replace the DSS s AVES system, please continue to use the DSS s AVES system if a record of the transaction is required. 12
13 Administration 13
14 Authorization Request Overview Clear Coverage offers six steps to successful completion of an Authorization Request: Select the member Select the clinician (Admitting provider) Add the diagnosis (Up to four codes) Select the service (Inpatient) Select the service information (Admitting facility) Add additional notes/information 14
15 Step One Select the Member 15
16 Authorization Panes Clear Coverage Authorization Panes The pane on the left side of the screen allows the user to select the information required for the authorization. The pane on the right side of the screen displays all of the information selected. 16
17 Step Two Select the Clinician (Admitting Provider) 17
18 Default Inpatient Provider CT Medical Assistance Program 18
19 Step Three Add the Diagnosis Code (Up to Four) 19
20 Step Four Select the Service (Inpatient) 20
21 Step Five Select the Service Information (Admitting Facility) 21
22 Step Six Adding Notes or Attachments Use this section to provide: Facility contact information Campus where member is located Clinical documentation attachment Medical Recor Number Click here to attach documents 22
23 Clear Coverage Printing 23
24 Faxing from Clear Coverage From the Print tab, a selection is available for a Fax Coversheet. Cover sheet is member and authorization specific and cannot be used for other members or authorizations. 24
25 Home Tab 25
26 Clear Coverage An authorization number is generated as a reference number and is not an indication of approval. Providers can be notified of the approval status of their authorization request via letter, phone or web. 26
27 Questions before the live demonstration 27
28 Inpatient Authorization Process 28
29 Inpatient Authorization Process Admission notification may be submitted via web portal (Clear Coverage) as of April 1st, and/or phone, fax. If the provider chooses to use phone or fax: Phone: and follow prompts for authorization Fax: for initial notification Fax: for submission of clinical information 29
30 Clear Coverage is not used for the following Routine maternity deliveries. (Authorization not required) NICU babies at the facility of their birth. (Authorization not required) Newborns without an ID number transferred to another facility or readmitted should be faxed to CHNCT. (Authorization is required) Behavioral health admissions. Submit to CT Behavioral Health Partnership. (phone ) Elective admissions. Providers to submit requests via fax to CHNCT. Medicare Part A admissions. 30
31 Inpatient Authorization Process Notification must be submitted within 2 business days of admission. If clinical review is not submitted upon notification, it must be submitted within 2 business days or it will result in a denial. To accommodate holiday weekends, the system will allow for notification up to 5 days from the date of admission. Admission notification greater than 5 days from the date of admission cannot be entered into Clear Coverage. 31
32 CDH Authorization Process At this time, Chronic Disease Hospitals (CDH) may submit initial notification only into Clear Coverage. Continued stay review should be phoned or faxed to CHNCT. In the future, continued stay requests may be made through Clear Coverage. CDH facilities will be notified when this feature is available. 32
33 Determinations During this transition period, determination letters will continue to be mailed upon initial determination. Hospitals will be notified when determination letters are available in Clear Coverage. Authorization status may continue to be viewed in the HP portal. There is a one day lag in file transfer from Clear Coverage to the HP system. 33
34 Admission Dates Admission notification must include the admission date to be billed. If the admission date does not match what is billed, the claim will deny. Hospital must notify CHNCT for any correction of admission in order for the authorization to be cancelled and re-entered. 34
35 Retro Processes: Retro Eligible (Prepay) The following process applies when eligibility is granted retrospectively. These retro reviews are submitted by fax and are not in Clear Coverage: Notification must be submitted within 10 days of eligibility being granted. Notification must be submitted with Verification of Eligibility (VOE) and clinical information. Retro reviews will not be performed onsite. If authorization was given for a newborn, there is no need to re-submit once an ID is assigned. 35
36 Retro Processes: Special Retros The following process relates to failure to obtain authorization for emergency admissions. These special retro reviews are submitted by mail and are not in Clear Coverage: Submit a copy of the medical record and a check for $100 made out to: State of CT Department of Social Services Special retros submitted after 30 days must include a good cause exception. The number of special retros allowed is determined by DSS each State fiscal year. Retros will be completed within 60 days of receipt of the request. 36
37 Thank You 37
Community Health Network of CT, Inc.
 PRPRE0024-0712 Clear Coverage Online Authorizations Outpatient Surgery Community Health Network of CT, Inc. A New Way to Request Authorizations As of July 31, 2012, there are now three options for requesting
PRPRE0024-0712 Clear Coverage Online Authorizations Outpatient Surgery Community Health Network of CT, Inc. A New Way to Request Authorizations As of July 31, 2012, there are now three options for requesting
Hospital Modernization Implementation/ APR DRG Workshop. Presented by The Department of Social Services & HP Enterprise Services
 Hospital Modernization Implementation/ APR DRG Workshop Presented by The Department of Social Services & HP Enterprise Services 1 Training Topics Hospital Modernization Overview Inpatient Payment Methodology
Hospital Modernization Implementation/ APR DRG Workshop Presented by The Department of Social Services & HP Enterprise Services 1 Training Topics Hospital Modernization Overview Inpatient Payment Methodology
Professional Refresher Workshop. Presented by The Department of Social Services & HP
 Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility SAGA Becomes Medicaid for Low Income Adults Automated Voice Response System (AVRS)
Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility SAGA Becomes Medicaid for Low Income Adults Automated Voice Response System (AVRS)
Behavioral Health Professional Refresher Workshop. Presented by The Department of Social Services & HP
 Behavioral Health Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility Verification Policy Review Fee Schedule Updates Provider Bulletins
Behavioral Health Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility Verification Policy Review Fee Schedule Updates Provider Bulletins
Claim Investigation Submission Guide
 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Network Health Claims Editing Portal
 Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Portal User Guide. Submitting Inpatient Notifications and Prior Authorization Requests. Tufts Health Together and Tufts Health Direct
 MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
Connecticut Medical Assistance Program Workshop Web Claim Submission
 Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
 www.mydentalcoverage.com 1 2 3 Complete the Fields as indicated 4 Complete the Fields as indicated click submit 5 6 Security Questions 7 Email sent to Activate Account 8 Close out previous browser and
www.mydentalcoverage.com 1 2 3 Complete the Fields as indicated 4 Complete the Fields as indicated click submit 5 6 Security Questions 7 Email sent to Activate Account 8 Close out previous browser and
Arise Health Insurance Fully Insured Groups 51+ and Self-Funded Groups. Choose It and Use It.
 Arise Health Insurance Fully Insured Groups 51+ and Self-Funded Groups Choose It and Use It. What can you count on from Arise Health Plan? Personal service, plus top-quality coverage You get health coverage
Arise Health Insurance Fully Insured Groups 51+ and Self-Funded Groups Choose It and Use It. What can you count on from Arise Health Plan? Personal service, plus top-quality coverage You get health coverage
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 09/14/2016 *all red text is new for 09/14/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Hospital Monthly Important Message Updated as of 09/14/2016 *all red text is new for 09/14/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
How to Take a Withdrawal
 How to Take a Withdrawal Table of Contents Important Information Read This First! 2 Can I Withdraw Funds from My Account? What Should I Consider Before Taking a Withdrawal? Taking a Withdrawal 3 Step 1:
How to Take a Withdrawal Table of Contents Important Information Read This First! 2 Can I Withdraw Funds from My Account? What Should I Consider Before Taking a Withdrawal? Taking a Withdrawal 3 Step 1:
SUBMITTING AND REVIEWING A CLAIM
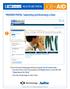 PROVIDER PORTAL: Submitting and Reviewing a Claim ➊ ➊ Go to the portal landing page and log in using your User ID and password. If you do not have a User ID and password, click Register Now or see the
PROVIDER PORTAL: Submitting and Reviewing a Claim ➊ ➊ Go to the portal landing page and log in using your User ID and password. If you do not have a User ID and password, click Register Now or see the
Medical Eligibility & Benefits Lookup Tips
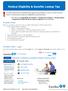 Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Claims INFO Adjustment Submission Guide
 Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Electronic Prior Authorization - Provider Guide. July 2017
 Electronic Prior Authorization - Provider Guide July 2017 Table of Contents Getting Started 3 Registration 4 Logging In 5 System Configurations (Post Office Settings) 6 Prior Request Form 7 General 7 Patient
Electronic Prior Authorization - Provider Guide July 2017 Table of Contents Getting Started 3 Registration 4 Logging In 5 System Configurations (Post Office Settings) 6 Prior Request Form 7 General 7 Patient
Electronic Prior Authorization - Provider Guide
 Electronic Prior Authorization - Provider Guide Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient and
Electronic Prior Authorization - Provider Guide Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient and
Viewing and Updating W-4 Information in Drexel One
 Please Note: These instructions are intended to provide employees with basic information required to access and update W-4 federal tax withholding setup. The screen shots are provided for general reference
Please Note: These instructions are intended to provide employees with basic information required to access and update W-4 federal tax withholding setup. The screen shots are provided for general reference
eauthorization Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with
 Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop
 CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
Electronic PriorAuthorization - Provider Guide. July 2017
 Electronic PriorAuthorization - Provider Guide July 2017 Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient
Electronic PriorAuthorization - Provider Guide July 2017 Table of Contents Getting Started 4 Registration 5 Logging In 6 System Configurations (Post Office Settings) 7 Prior Request Form 8 General 8 Patient
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
NIA Magellan 1 Frequently Asked Questions (FAQ s) For HealthAmerica Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For HealthAmerica Providers Question GENERAL Why is Health America implementing an outpatient imaging program? Answer To improve quality and manage the
NIA Magellan 1 Frequently Asked Questions (FAQ s) For HealthAmerica Providers Question GENERAL Why is Health America implementing an outpatient imaging program? Answer To improve quality and manage the
Connecticut Medical Assistance Program Long Term Care Refresher Workshop. Presented by: The Department of Social Services & HP for Billing Providers
 Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers
 Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers Question GENERAL Why is CareSource implementing an outpatient imaging program? Answer To improve quality and manage the
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers Question GENERAL Why is CareSource implementing an outpatient imaging program? Answer To improve quality and manage the
CareCore National Musculoskeletal Management Program Physical Medicine and Therapy Frequently Asked Questions
 EVIDENCE-BASED HEALTHCARE SOLUTIONS CareCore National Physical Medicine and Therapy Prepared for December 2, 2014 Table of Contents Introduction to CareCore National... 3 Who is CareCore National?... 3
EVIDENCE-BASED HEALTHCARE SOLUTIONS CareCore National Physical Medicine and Therapy Prepared for December 2, 2014 Table of Contents Introduction to CareCore National... 3 Who is CareCore National?... 3
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
NIA Frequently Asked Questions (FAQ s) For Kentucky Spirit Health Plan Providers
 Question GENERAL Why is Kentucky Spirit Health Plan implementing an outpatient imaging program? NIA Frequently Asked Questions (FAQ s) For Providers Answer To improve quality and manage the utilization
Question GENERAL Why is Kentucky Spirit Health Plan implementing an outpatient imaging program? NIA Frequently Asked Questions (FAQ s) For Providers Answer To improve quality and manage the utilization
Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona
 Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Home Health Provider Billing Workshop Review 2013
 Connecticut Medical Assistance Program (CMAP) Home Health Provider Billing Workshop Review 2013 Presented by The Department of Social Services & HP Enterprise Services 1 WORKSHOP AGENDA CHC Program Changes
Connecticut Medical Assistance Program (CMAP) Home Health Provider Billing Workshop Review 2013 Presented by The Department of Social Services & HP Enterprise Services 1 WORKSHOP AGENDA CHC Program Changes
Individual Claim Entry
 Individual Claim Entry User Guide Individual Claim Entry User Guide WCPSOnline Individual Claim Entry User Guide 02.09.09 1 Individual Claim Entry User Guide This material and the information contained
Individual Claim Entry User Guide Individual Claim Entry User Guide WCPSOnline Individual Claim Entry User Guide 02.09.09 1 Individual Claim Entry User Guide This material and the information contained
MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18
 MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18 Agenda Save Time by Utilizing the MHS Secure Web Portal: Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims
MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18 Agenda Save Time by Utilizing the MHS Secure Web Portal: Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims
Frequently Asked Questions Cardiology Prior Authorization Program Applies to UnitedHealthcare Community Plan Members.
 Frequently Asked Cardiology Prior Authorization Program Applies to UnitedHealthcare Community Plan Members. Overview Prior authorization is required for select cardiology procedures provided to certain
Frequently Asked Cardiology Prior Authorization Program Applies to UnitedHealthcare Community Plan Members. Overview Prior authorization is required for select cardiology procedures provided to certain
Claim Investigation Submission Guide
 Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Prior Authorizations with InterQual Integration
 Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
Eligibility and Benefits Inquiry Guide
 Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
HOW TO SUBMIT OWCP-04 BILLS TO ACS
 HOW TO SUBMIT OWCP-04 BILLS TO ACS OFFICE OF WORKERS COMPENSATION PROGRAMS DIVISION OF ENERGY EMPLOYEES OCCUPATIONAL ILLNESS COMPENSATION The following services should be billed on the OWCP-04 Form: General
HOW TO SUBMIT OWCP-04 BILLS TO ACS OFFICE OF WORKERS COMPENSATION PROGRAMS DIVISION OF ENERGY EMPLOYEES OCCUPATIONAL ILLNESS COMPENSATION The following services should be billed on the OWCP-04 Form: General
evicore healthcare Utilization management programs Frequently asked questions
 evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
User Guide for Pricing Engine
 User Guide for Pricing Engine Version 1.2 Effective Date: 02/27/2019 Contents 1.0 STEPS TO ACCESS SEEMYLOANSTATUS... 2 2.0 SUBMITTING LOCK REQUEST... 4 2.1 STEPS TO REQUEST LOCK ON A NEW LOAN... 4 2.2
User Guide for Pricing Engine Version 1.2 Effective Date: 02/27/2019 Contents 1.0 STEPS TO ACCESS SEEMYLOANSTATUS... 2 2.0 SUBMITTING LOCK REQUEST... 4 2.1 STEPS TO REQUEST LOCK ON A NEW LOAN... 4 2.2
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions
 WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Sunflower Health Plan Providers
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Plan Providers Question GENERAL Why is Sunflower Health Plan implementing an outpatient imaging program? Answer To improve
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Plan Providers Question GENERAL Why is Sunflower Health Plan implementing an outpatient imaging program? Answer To improve
Intensive Case Management Primary Care Provider Training
 Intensive Case Management Primary Care Provider Training NaviNet Enhancements Kelley Royer-Marek Manager, Risk Adjustment Programs kroyer-marek@amerihealthcaritas.com December, 2017 What is the purpose
Intensive Case Management Primary Care Provider Training NaviNet Enhancements Kelley Royer-Marek Manager, Risk Adjustment Programs kroyer-marek@amerihealthcaritas.com December, 2017 What is the purpose
Blue Cross OGB-dedicated Customer Service:
 Blue Cross OGB-dedicated Customer Service: 1.800.392.4089 Frequently Asked uestions Blue Cross and Blue Shield of Louisiana administers benefits for the Office of Group Benefits (OGB) for their PPO, HMO
Blue Cross OGB-dedicated Customer Service: 1.800.392.4089 Frequently Asked uestions Blue Cross and Blue Shield of Louisiana administers benefits for the Office of Group Benefits (OGB) for their PPO, HMO
Finance Data Mart. Student Guide
 Student Guide TABLE OF CONTENTS OBJECTIVE... 3 DATA MART... 3 ACTIVITY REPORTS... 8 Ambulatory Care Activity Report... 8 Average Hours Per Discharge... 12 Census Reports... 12 Charges and Usage... 13 DEPARTMENTAL
Student Guide TABLE OF CONTENTS OBJECTIVE... 3 DATA MART... 3 ACTIVITY REPORTS... 8 Ambulatory Care Activity Report... 8 Average Hours Per Discharge... 12 Census Reports... 12 Charges and Usage... 13 DEPARTMENTAL
CoventryCares of Kentucky Provider Training Program
 CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
Prior Authorizations on the Provider Portal. July 2017
 Prior Authorizations on the Provider Portal July 2017 2 Disclaimer The information provided is current as of June 2017 and is subject to change. Stay current with up-to-date information on the OHCA public
Prior Authorizations on the Provider Portal July 2017 2 Disclaimer The information provided is current as of June 2017 and is subject to change. Stay current with up-to-date information on the OHCA public
Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017
 Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017 Key Points Starting Nov. 1, 2017, notification/prior authorization is required
Genetic and Molecular Lab Testing Notification/Prior Authorization Process Frequently Asked Questions Effective Nov. 1, 2017 Key Points Starting Nov. 1, 2017, notification/prior authorization is required
(FAQ s) For Florida Aetna Medicare HMO Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Florida Aetna Medicare HMO Providers Question GENERAL Why did Aetna implement an outpatient imaging program? Answer To improve quality and manage the
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Florida Aetna Medicare HMO Providers Question GENERAL Why did Aetna implement an outpatient imaging program? Answer To improve quality and manage the
NIA Magellan 1 Frequently Asked Questions (FAQ s) For CareSource Just4Me Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did CareSource Just4Me implement an outpatient imaging program? Answer To improve quality and manage the utilization
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did CareSource Just4Me implement an outpatient imaging program? Answer To improve quality and manage the utilization
DTE Energy retirees: Welcome to PayFlex
 DTE Energy retirees: Welcome to PayFlex You are enrolled in a Retiree Reimbursement Account (RRA). Your new RRA comes with some great tools to help you manage your account. Through the PayFlex member website,
DTE Energy retirees: Welcome to PayFlex You are enrolled in a Retiree Reimbursement Account (RRA). Your new RRA comes with some great tools to help you manage your account. Through the PayFlex member website,
Pamela Ballou-Nelson, RN, MSPH, CMPE, PhD, Principal, MGMA Consulting April 10, , Telligen, Inc.
 MIPS 2018 Cost Reporting and Your QRUR Pamela Ballou-Nelson, RN, MSPH, CMPE, PhD, Principal, MGMA Consulting April 10, 2018 2016, Telligen, Inc. Quality Payment Program Cost Reporting Quality Payment Program
MIPS 2018 Cost Reporting and Your QRUR Pamela Ballou-Nelson, RN, MSPH, CMPE, PhD, Principal, MGMA Consulting April 10, 2018 2016, Telligen, Inc. Quality Payment Program Cost Reporting Quality Payment Program
Personal Care Attendant (PCA) Waiver. Billing Provider Workshop for Personal Care Service Providers
 Personal Care Attendant (PCA) Waiver Billing Provider Workshop for Personal Care Service Providers Presented by The Department of Social Services & Hewlett Packard Enterprise 1 PCA Waiver Workshop Introduction
Personal Care Attendant (PCA) Waiver Billing Provider Workshop for Personal Care Service Providers Presented by The Department of Social Services & Hewlett Packard Enterprise 1 PCA Waiver Workshop Introduction
Post Payment Documentation Request Portal
 Post Payment Documentation Request Portal Responding to an Expense Reimbursement Post Payment Document Request Fannie Mae s Post Payment Documentation Request portal provides an efficient and simple way
Post Payment Documentation Request Portal Responding to an Expense Reimbursement Post Payment Document Request Fannie Mae s Post Payment Documentation Request portal provides an efficient and simple way
Patient Billing and Financial Services
 Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Adviser Guide: MPPM Website Accessing client portfolios & resources pages
 Macquarie Private Portfolio Management Adviser Guide: MPPM Website Accessing client portfolios & resources pages Prepared: September 2012 Contact: Ph: 1800 501 180 Email: mppm@macquarie.com Landing Page
Macquarie Private Portfolio Management Adviser Guide: MPPM Website Accessing client portfolios & resources pages Prepared: September 2012 Contact: Ph: 1800 501 180 Email: mppm@macquarie.com Landing Page
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Arkansas BlueCross BlueShield
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For BlueShield Question GENERAL Why is Arkansas Plan implementing an outpatient imaging program? Answer To improve quality and manage the utilization of
NIA Magellan 1 Frequently Asked Questions (FAQ s) For BlueShield Question GENERAL Why is Arkansas Plan implementing an outpatient imaging program? Answer To improve quality and manage the utilization of
4/29/2014. April 30, 2014
 April 30, 2014 Rachel Peura, RN Educated in PA; worked in a variety of settings in PA including: Acute care In and outpatient medical rehab Office settings Clinical trials House supervisor positions Employed
April 30, 2014 Rachel Peura, RN Educated in PA; worked in a variety of settings in PA including: Acute care In and outpatient medical rehab Office settings Clinical trials House supervisor positions Employed
Employee Retirement System of Texas (ERS)
 Employee Retirement System of Texas (ERS) HealthSelect SM of Texas & Consumer Directed HealthSelect SM Blue Cross and Blue Shield of Texas, a Division of Health Care Service Corporation, a Mutual Legal
Employee Retirement System of Texas (ERS) HealthSelect SM of Texas & Consumer Directed HealthSelect SM Blue Cross and Blue Shield of Texas, a Division of Health Care Service Corporation, a Mutual Legal
NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers
 NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers Question GENERAL Why is Home State Health Plan implementing an outpatient imaging program? Answer To improve quality and manage
NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers Question GENERAL Why is Home State Health Plan implementing an outpatient imaging program? Answer To improve quality and manage
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) BlueCross BlueShield of South Carolina Providers
 Magellan Healthcare 1 Frequently Asked Questions (FAQ s) BlueCross BlueShield of South Carolina Providers Question Answer GENERAL Why did BlueCross implement an outpatient imaging program? Why did BlueCross
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) BlueCross BlueShield of South Carolina Providers Question Answer GENERAL Why did BlueCross implement an outpatient imaging program? Why did BlueCross
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Ambetter from Sunshine Health Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did Ambetter from implement an outpatient imaging program? Answer To improve quality and manage the utilization of nonemergent
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did Ambetter from implement an outpatient imaging program? Answer To improve quality and manage the utilization of nonemergent
Housekeeping. Link Participant ID with Audio. Mute your line UNMUTED. Raise your hand with questions
 Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
RISD 2018 Voluntary Insurance Open Enrollment Dec-01 Dec-15, Benefit Enrollment Instructions
 2018 Benefit Enrollment Instructions Contents Quick Reference... 3 Access and log in to the Online Enrollment Portal (OEP)... 6 Password Reset and Login Instructions... 7 Enrolling in 2018 Supplemental
2018 Benefit Enrollment Instructions Contents Quick Reference... 3 Access and log in to the Online Enrollment Portal (OEP)... 6 Password Reset and Login Instructions... 7 Enrolling in 2018 Supplemental
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Gateway Health Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging program? Why did Gateway Health select NIA Magellan to manage its
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging program? Why did Gateway Health select NIA Magellan to manage its
Accessing your payslip from DMUhub
 Accessing your payslip from DMUhub To gain access to DMUhub, type dmuhub.dmu.ac.uk into your internet address field. You will be taken to the Single Sign-on page. Input your staff username and password.
Accessing your payslip from DMUhub To gain access to DMUhub, type dmuhub.dmu.ac.uk into your internet address field. You will be taken to the Single Sign-on page. Input your staff username and password.
Connecticut interchange MMIS
 Connecticut interchange MMIS Provider Manual Chapter 7 Licensed Behavioral Health Clinicians in Independent Practice February 1, 2013 Connecticut Department of Social Services (DSS) 55 Farmington Ave Hartford,
Connecticut interchange MMIS Provider Manual Chapter 7 Licensed Behavioral Health Clinicians in Independent Practice February 1, 2013 Connecticut Department of Social Services (DSS) 55 Farmington Ave Hartford,
A GUIDE TO MY AMERICORPS
 A GUIDE TO MY AMERICORPS IN MY AMERICORPS, YOU CAN.. Search AmeriCorps program opportunities, create an AmeriCorps application, and apply for positions Manage your education award Request Forbearance on
A GUIDE TO MY AMERICORPS IN MY AMERICORPS, YOU CAN.. Search AmeriCorps program opportunities, create an AmeriCorps application, and apply for positions Manage your education award Request Forbearance on
Financial Edge (FE) Instructions
 Financial Edge (FE) Instructions Welcome to the CU Foundation s accounting system! Please report any issues or make suggestions to accounting@cufund.org. Step 1: Password Set up and Change at the Manage
Financial Edge (FE) Instructions Welcome to the CU Foundation s accounting system! Please report any issues or make suggestions to accounting@cufund.org. Step 1: Password Set up and Change at the Manage
NIA Frequently Asked Questions (FAQ s) For Sunshine State Health Plan Providers
 Question GENERAL Why is Sunshine State Health Plan implementing an outpatient imaging program? NIA Frequently Asked Questions (FAQ s) For Providers Answer To improve quality and manage the utilization
Question GENERAL Why is Sunshine State Health Plan implementing an outpatient imaging program? NIA Frequently Asked Questions (FAQ s) For Providers Answer To improve quality and manage the utilization
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Coventry Health Care of Virginia, Inc. Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Coventry Health Care of Providers Question GENERAL Why did Coventry Health Care of implementing an outpatient imaging program? Answer To improve quality
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Coventry Health Care of Providers Question GENERAL Why did Coventry Health Care of implementing an outpatient imaging program? Answer To improve quality
2019 FAQs Medical plan. Frequently Asked Questions from employees
 2019 FAQs Medical plan Frequently Asked Questions from employees September 2018 Medical plan benefits Here are some commonly asked questions about the Medical Plan Benefits that our employees have raised.
2019 FAQs Medical plan Frequently Asked Questions from employees September 2018 Medical plan benefits Here are some commonly asked questions about the Medical Plan Benefits that our employees have raised.
Blackbaud Merchant Services TM Portal Features Overview Transaction Management Through the Blackbaud Merchant Services Web Portal
 Blackbaud Merchant Services TM Portal Features Overview Transaction Management Through the Blackbaud Merchant Services Web Portal From the web portal, you can use many features to manage transactions and
Blackbaud Merchant Services TM Portal Features Overview Transaction Management Through the Blackbaud Merchant Services Web Portal From the web portal, you can use many features to manage transactions and
NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers
 gat NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers Question GENERAL Why is West Virginia Family Health implementing an outpatient imaging program? Why did West
gat NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers Question GENERAL Why is West Virginia Family Health implementing an outpatient imaging program? Why did West
FAIRFIELD PUBLIC SCHOOLS. Munis Self Service
 FAIRFIELD PUBLIC SCHOOLS Munis Self Service Employee Self Service User Guide Version 10.5 https://fairfieldboe.munisselfservice.com/default.aspx LOG IN: Username: first initial, last name, last 4 of your
FAIRFIELD PUBLIC SCHOOLS Munis Self Service Employee Self Service User Guide Version 10.5 https://fairfieldboe.munisselfservice.com/default.aspx LOG IN: Username: first initial, last name, last 4 of your
GENERAL BENEFIT INFORMATION
 Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Healthy Indiana Plan (HIP) Provider Orientation
 Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
University of Cincinnati Medical Plan Summary and Comparison Effective January 1- December 31, 2018-AAUP only
 Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/2018 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/2018
Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/2018 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/2018
MHS Prior Authorization 0317.PR.P.PP
 MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
MHS Prior Authorization 0317.PR.P.PP Prior Authorization (PA) PA requirements Recent Updates Helpful Tips Web Telephone Fax Referrals Appeals Process Need to Know Questions and Answers Agenda MHS Prior
Referral and Prior Authorization Tool Guide
 Referral and Prior Authorization Tool Guide An Independent 1 Licensee of the Blue Cross Blue Shield Association 044509 (2-1-2018) Referral & Prior Authorization Please check the prior authorization code
Referral and Prior Authorization Tool Guide An Independent 1 Licensee of the Blue Cross Blue Shield Association 044509 (2-1-2018) Referral & Prior Authorization Please check the prior authorization code
PROVIDER MANUAL. In the Colorado Access Provider Manual, you will find information about:
 In the Colorado Access Provider Manual, you will find information about: Section 1. Colorado Access General Information Section 2. Colorado Access Policies Section 3. Quality Management Section 4. Provider
In the Colorado Access Provider Manual, you will find information about: Section 1. Colorado Access General Information Section 2. Colorado Access Policies Section 3. Quality Management Section 4. Provider
Provider Manual. ChoiceBenefits. BayCare Health System Medical Plan
 2019 Provider Manual ChoiceBenefits BayCare Health System Medical Plan 1 Table of Contents BayCare... 2 BayCare Exclusive Network... 2 Rules unique to Cigna BayCare Members... 2 Provider Relations Representative...
2019 Provider Manual ChoiceBenefits BayCare Health System Medical Plan 1 Table of Contents BayCare... 2 BayCare Exclusive Network... 2 Rules unique to Cigna BayCare Members... 2 Provider Relations Representative...
2 General Information RE DRG Implementation Where can we get information about how the Agency is implementing DRGs in Florida FFS Medicaid?
 1 Capitated Health Plan Provider Reimbursement As I understand it the managed care organizations are not required to change their inpatient reimbursement method but could do so. If Medica implements this
1 Capitated Health Plan Provider Reimbursement As I understand it the managed care organizations are not required to change their inpatient reimbursement method but could do so. If Medica implements this
When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective?
 GENERAL When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective? The bill has been signed into law by the Governor and will be effective July 1, 2008. However, DCH
GENERAL When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective? The bill has been signed into law by the Governor and will be effective July 1, 2008. However, DCH
MHS CMS 1500 Tips and Billing Guidelines
 MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
User Guide. Healthcode E Practice Suite biller - 1 -
 User Guide Healthcode E Practice Suite biller - 1 - Index Introduction... 3 PC / Internet Explorer Set-Up... 4 Logging onto E Practice biller... 8 Status Page... 10 Patients Tab... 11 Adding New Patients...
User Guide Healthcode E Practice Suite biller - 1 - Index Introduction... 3 PC / Internet Explorer Set-Up... 4 Logging onto E Practice biller... 8 Status Page... 10 Patients Tab... 11 Adding New Patients...
Ambetter from Superior HealthPlan
 Ambetter from Superior HealthPlan 1/14/2016 This document does not meet accessibility standards. If you have questions about the information contained within, please contact Provider Services at 1-877-687-1196
Ambetter from Superior HealthPlan 1/14/2016 This document does not meet accessibility standards. If you have questions about the information contained within, please contact Provider Services at 1-877-687-1196
Expedited Psychiatric Inpatient Admission Policy
 The Commonwealth of Massachusetts Executive Office of Health and Human Services Department of Mental Health Department of Public Health Office of MassHealth Executive Office of Housing and Economic Development
The Commonwealth of Massachusetts Executive Office of Health and Human Services Department of Mental Health Department of Public Health Office of MassHealth Executive Office of Housing and Economic Development
eclaims - Overview FOR THE FOLLOWING CLAIMS: DENTAL OPTICAL CLINIC HEALTH SCREENING SPECIALIST PEDIATRICIAN MATERNITY
 eclaims - Overview FOR THE FOLLOWING CLAIMS: DENTAL OPTICAL CLINIC HEALTH SCREENING SPECIALIST PEDIATRICIAN MATERNITY Member submit reimbursement claims via My AIA portal / app Member upload supporting
eclaims - Overview FOR THE FOLLOWING CLAIMS: DENTAL OPTICAL CLINIC HEALTH SCREENING SPECIALIST PEDIATRICIAN MATERNITY Member submit reimbursement claims via My AIA portal / app Member upload supporting
NIA Magellan 1 Frequently Asked Questions (FAQs) for Highmark Health Options Providers
 gat Question GENERAL NIA Magellan 1 Frequently Asked Questions (FAQs) for Providers Why is Highmark Health Options implementing an outpatient imaging program? Why did Highmark Health Options select NIA
gat Question GENERAL NIA Magellan 1 Frequently Asked Questions (FAQs) for Providers Why is Highmark Health Options implementing an outpatient imaging program? Why did Highmark Health Options select NIA
SECTION 9 1 CLAIMS PROCEDURES
 SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
NIA Frequently Asked Questions (FAQ s) For CoventryCares of Kentucky Providers
 Question GENERAL Do Kentucky Members have any copay responsibilities? NIA Frequently Asked Questions (FAQ s) For Providers Answer Members do not have copays for outpatient imaging procedures. PRIOR AUTHORIZATION
Question GENERAL Do Kentucky Members have any copay responsibilities? NIA Frequently Asked Questions (FAQ s) For Providers Answer Members do not have copays for outpatient imaging procedures. PRIOR AUTHORIZATION
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
Infinite Campus Portal Parents Quick Reference
 Infinite Campus Portal Parents Quick Reference I n f i n i t e C a m p u s P o r t a l i s a w a y f o r p a r e n t s / g u a r d i a n s t o a c c e s s s t u d e n t i n f o r m a t i o n, r e g i s
Infinite Campus Portal Parents Quick Reference I n f i n i t e C a m p u s P o r t a l i s a w a y f o r p a r e n t s / g u a r d i a n s t o a c c e s s s t u d e n t i n f o r m a t i o n, r e g i s
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
INTERMEDIATE ADMINISTRATIVE SIMPLIFICATION CENTERS FOR MEDICARE & MEDICAID SERVICES. Online Guide to: ADMINISTRATIVE SIMPLIFICATION
 02 INTERMEDIATE» Online Guide to: CENTERS FOR MEDICARE & MEDICAID SERVICES Last Updated: February 2014 TABLE OF CONTENTS INTRODUCTION: ABOUT THIS GUIDE... i About Administrative Simplification... 2 Why
02 INTERMEDIATE» Online Guide to: CENTERS FOR MEDICARE & MEDICAID SERVICES Last Updated: February 2014 TABLE OF CONTENTS INTRODUCTION: ABOUT THIS GUIDE... i About Administrative Simplification... 2 Why
University of Cincinnati Medical Plan Summary and Comparison Non AAUP - Effective January 1- December 31, 2018
 Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
My ACCESS Account Provider View
 My ACCESS Account Provider View November 7, 2010 Table of Contents Table of Contents... 2 Overview... 3 Provider View Process Flow... 4 Florida Medicaid Home... 5 Customer Search... 6 My Account Status...
My ACCESS Account Provider View November 7, 2010 Table of Contents Table of Contents... 2 Overview... 3 Provider View Process Flow... 4 Florida Medicaid Home... 5 Customer Search... 6 My Account Status...
