Behavioral Health Professional Refresher Workshop. Presented by The Department of Social Services & HP
|
|
|
- Lenard Haynes
- 6 years ago
- Views:
Transcription
1 Behavioral Health Professional Refresher Workshop Presented by The Department of Social Services & HP 1
2 Training Topics Client Eligibility Verification Policy Review Fee Schedule Updates Provider Bulletins Re-Enrollment Web Claim Inquiry / Submission Third Party Liability Frequent Claim Denials Claim Resolution Guide ICD-10 Time for Questions 2
3 Client Eligibility Verification DSS recommends that providers verify a client s eligibility on the date of service prior to providing services. To verify a client s eligibility through the secure Web site click on the Eligibility tab on the main menu. 3
4 Client Eligibility Verification Enter enough data to satisfy at least one of the valid search combinations; click search When entering a full name as part of your search, a middle initial is required if present in his/her Connecticut Medical Assistance Program (CMAP) profile. 4
5 Web Eligibility Screen Enhancements Search by Service Type Codes Providers will now be able to search by up to five (5) different service type codes. The service type codes allow providers to verify the client s eligibility benefit coverage for specific services. The first service type code field defaults to 30 Health Benefit Plan Coverage. If the provider searches by that default selection, it will return with all the service type codes that are covered for the client s benefit plan. The specific service type codes for behavioral health providers is A6 Psychotherapy. 5
6 Web Eligibility Screen Enhancements Search by Service Type Codes 6
7 Web Eligibility Screen Enhancements Search by Service Type Codes A6 Psychotherapy 7
8 Web Eligibility Screen Enhancements The eligibility verification request screen has been enhanced to verify eligibility to the end of the current month. The eligibility response is based on current eligibility and is subject to change. Please validate again on the actual date of service. 8
9 Web Eligibility Screen Enhancements HUSKY B client eligibility search response HUSKY B copay amounts will not show on the eligibility screen. 9
10 Web Eligibility Screen Enhancements HUSKY B copay amounts Provider should refer to the CTBHP Web site for HUSKY B co-pay amounts. From Web site, select For Providers, then Covered Services then click on the link for New: HUSKY B Client Cost-Share Services. 10
11 Web Eligibility Screen Enhancements HUSKY C client eligibility search response 11
12 Policy Review Provider Bulletin Behavioral Health Clinician Coverage for Individuals Under Age 21 in Fee-For-Service Medicaid (HUSKY C) and Medicaid for Low Income Adults (HUSKY D). Effective January 1, 2012 behavioral health assessment and treatment services provided by the following independent practitioners to individuals covered by HUSKY C and HUSKY D who are under twenty-one (21) years of age will be reimbursed as optional services by Connecticut Medicaid. Licensed Clinical Social Workers (LCSWs) Licensed Marital and Family Therapists (LMFTs) Licensed Professional Counselors (LPCs) Licensed Alcohol and Drug Counselors (LADCs) Certified Alcohol and Drug Counselors (CADCs) 12
13 Policy Review Behavioral Health Clinicians and Psychologists cannot see HUSKY C & D clients that are over 21. Prior Authorization (PA) from the Connecticut Behavioral Health Partnership is required for these services. Refer to the Web site for providers and select covered services. Under Authorization Schedule select your provider type based on Independent Group Practitioners. Prior Authorization does not guarantee benefits. Behavioral Health Clinicians and Psychologists can see HUSKY A, HUSKY B and Charter Oak clients regardless of age. 13
14 Policy Review Provider Bulletin Requirements for Payment of Services Provided by Licensed Behavioral Health Clinicians in Independent Practice. Policy regulations for payment are posted on the Web site, go to publications, then to Provider manuals to chapter 7 and from the drop down box choose Behavioral Health Clinicians Services. These regulations: (1) define licensed behavioral health clinicians ; (2) identify the individuals to whom licensed behavioral health clinicians may provide reimbursable services; (3) identify the services covered, service limitations and services not covered; (4) describe the prior authorization and registration requirements; (5) identify the rules for billing procedures and payments; and (6) describe documentation requirements. 14
15 Fee Schedule Updates Behavioral Health Clinicians fee schedules have been updated for claims with dates of service January 1, 2013 and forward. Accessing Behavioral Health Clinicians fee schedule: From Web site, go to Provider, then to Provider Fee Schedule Download, click on I Accept scroll to Behavioral Health Clinicians and click on the PDF link. From Web site, select For Providers, then Covered Services then click on the link for CT BHP Proposed Fees/Rates. Behavioral health clinicians can only bill for those services that are on their fee schedule and which they personally provide. 15
16 Fee Schedule Updates Behavioral Health Clinicians fee schedules 16
17 Fee Schedule Updates Psychologists have been updated for claims with dates of service January 1, 2013 and forward. Accessing Psychologists fee schedule: From Web site, go to Provider, then to Provider Fee Schedule Download, click on I Accept scroll to Behavioral Health Psychologist and click on the PDF link. From Web site, select For Providers, then Covered Services then click on the link for CT BHP Proposed Fees/Rates. 17
18 Fee Schedule Updates Behavioral Health Psychologists fee schedules 18
19 Fee Schedule Updates screen shot 19
20 Provider Bulletins Provider Bulletins Access the Publications page via our Web site and select Publications from either the Information box on the left hand side of the home page or from the Information drop-down menu. The Bulletin Search menu allows you to search for specific bulletins (by year, number, or title) as well as for all bulletins relevant to your provider type. When searching by title, you can search by any word as long as that word is in the title of the bulletin. 20
21 Provider Bulletins Provider bulletin search by Year 12 and Number 04 to pull up a specific bulletin. Provider bulletins numbers are located on the actual document. 21
22 Provider Bulletins Provider bulletin search by Year 13 and Provider Type Behavioral Health Clinician to pull up all the bulletins for 2013 pertaining to Behavioral Health Clinicians and Psychologists. 22
23 Provider Bulletins Provider Bulletin Elimination of Paper Re-enrollment Applications As of March 1, 2013, paper provider re-enrollment applications submitted to HP will no longer be accepted. If a paper application is received from a provider who is required to submit their re-enrollment application via the Wizard, the paper application will not be processed and will be returned to the provider with instructions to use the online Wizard. Behavioral Health providers must submit their provider reenrollment application via the online Wizard located on the Web site. 23
24 Provider Re-enrollment Re-enrollment Period Behavioral Health Clinicians and Groups, Psychologists and Groups, who complete their re-enrollment on or after January 1, 2012 will be required to re-enroll every five years. Providers will receive a reminder letter when the provider is due for re-enrollment (30 days prior to the end of their previous enrollment contract). This letter contains the Application Tracking Number (ATN). The ATN and NPI or AVRS ID are required to access re-enrollment application. 24
25 Provider Re-Enrollment Select Provider Re-Enrollment from the Provider dropdown menu To log-in to your Re-Enrollment Application, enter the ATN and NPI or AVRS ID 25
26 Web Claim Inquiry At the claims menu select claims inquiry to view claims processed regardless of the submission method. Search by: Internal Control Number (ICN) Client ID and date of service (no greater range than 93 days) Date of payment (no greater range than 93 days) Pending claims 26
27 Web Claim Inquiry Web Claim function buttons Paid claim Denied claim Suspended claim 27
28 Web Claim Submission Claim submission Professional 28
29 Web Claim Submission Claim submission Professional (Cont.) 29
30 Web Claim Submission Claim submission Professional (Cont.) 30
31 Third Party Liability Medicaid is the Payer of last resort. The three digit Carrier Code of the Other Insurance (OI) is required to be submitted on the claim when OI is primary. The three digit code can be found on the client eligibility verification screen under TPL. It can also be found on the claim submission screen under the TPL panel in the Client Carriers field. Other Insurance and Medicare Billing Guides are located Web site under publications, scroll to provider manual chapter 11 and select Professional Other Insurance/Medicare Billing Guide. 31
32 Third Party Liability Update To correct or update Third Party Liability (TPL) information: Obtain TPL forms Print out form located on Web site at under Information Publications Forms Other Forms TPL Information Form. Call Health Management System, Inc. (HMS) HMS staff will mail or fax the form to the provider. request to and form will be e- mailed back to provider. Submit completed forms Fax to HMS with HIPAA compliant letter to Scan completed forms and submit through to * Provider Manual Chapter 5 - Claim Submission Information 32
33 Dual Eligible / Medicare Prime Dual Eligible is when a client is eligible for Medicare and Medicaid. Medicaid is always the payer of last resort and claims must be submitted to Medicare first for Medicare eligible services. At this time for behavioral health clinician claims we will only cover claims if the provider has already received payment from Medicare. If Medicare is prime and makes a payment we will pay coinsurance and/or deductible up to your Medicaid rate. If Medicare s payment is greater than or equal to your Medicaid rate, Medicaid will pay zero. Medicare Billing Guides are located under Provider Manual chapter 11 on the Web site. 33
34 Web Claim Submission 34
35 Claim Resolution Guide Provider Manual Chapter 12 Claim Resolution Guide This guide lists commonly posted Explanation of Benefit (EOB) codes and provides a brief explanation of the reason why claims were either suspended or denied. This guide provides a detailed description of the cause of each EOB and more importantly, the necessary correction to the claim, if appropriate, in order to resolve the error condition. This guide also provides tips by identifying where providers can go to find additional information to assist with correcting their claims. 35
36 Claim Resolution Guide EOB 4801 Procedure not covered. Check: Prior Authorization, FTC, Referring Provider, Quantity Restrictions. Cause The procedure billed is not permitted to be paid to the billing provider on the date of service. Resolution If the procedure billed is not a covered procedure on the provider's fee schedule for the date of service, the service is not payable. If the procedure billed is present on the provider's fee schedule, contact the Provider Assistance Center to request an update to the procedure code in question. 36
37 Most Frequent Claim Denials EOB 4140 The Services Submitted are not Covered Under the Client s Benefit Plan and EOB 4250 No Reimbursement Rule for the Associated Provider Type/Provider Specialty. The provider should verify client eligibility to determine if services are covered for provider type and specialty. If the services are covered under client s benefit plan, client eligibility could have been updated at some point. Providers should re-submit the claim for processing or verify by calling the Provider Assistance Center (PAC). 37
38 ICD-10 Changes ICD (International Statistical Classification of Diseases and Related Health Problems)-10 Changes On October 1, 2014 the ICD-9 code set used to report medical diagnosis and inpatient procedures will be replaced by ICD-10 code sets. The transition to ICD-10 is required for all providers, payers and vendors. Please start paying attention to information about ICD-10 and that we will use that coding instead of the DSM-5 codes on Medicaid claims. 38
39 Training Session Wrap Up Where to go for more information: For questions on authorizations and the authorization processing contact: Value Options For questions on claim and enrollment questions you can contact: HP Provider Assistance Center (PAC) Monday through Friday, 8 a.m. to 5 p.m. (EST), excluding holidays. 39
40 Time for Questions Questions & Answers 40
Professional Refresher Workshop. Presented by The Department of Social Services & HP
 Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility SAGA Becomes Medicaid for Low Income Adults Automated Voice Response System (AVRS)
Professional Refresher Workshop Presented by The Department of Social Services & HP 1 Training Topics Client Eligibility SAGA Becomes Medicaid for Low Income Adults Automated Voice Response System (AVRS)
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop
 CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
Home Health Provider Billing Workshop Review 2013
 Connecticut Medical Assistance Program (CMAP) Home Health Provider Billing Workshop Review 2013 Presented by The Department of Social Services & HP Enterprise Services 1 WORKSHOP AGENDA CHC Program Changes
Connecticut Medical Assistance Program (CMAP) Home Health Provider Billing Workshop Review 2013 Presented by The Department of Social Services & HP Enterprise Services 1 WORKSHOP AGENDA CHC Program Changes
Connecticut Medical Assistance Program Workshop Web Claim Submission
 Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Connecticut Medical Assistance Program Long Term Care Refresher Workshop. Presented by: The Department of Social Services & HP for Billing Providers
 Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
Hospital Modernization Implementation/ APR DRG Workshop. Presented by The Department of Social Services & HP Enterprise Services
 Hospital Modernization Implementation/ APR DRG Workshop Presented by The Department of Social Services & HP Enterprise Services 1 Training Topics Hospital Modernization Overview Inpatient Payment Methodology
Hospital Modernization Implementation/ APR DRG Workshop Presented by The Department of Social Services & HP Enterprise Services 1 Training Topics Hospital Modernization Overview Inpatient Payment Methodology
Personal Care Attendant (PCA) Waiver. Billing Provider Workshop for Personal Care Service Providers
 Personal Care Attendant (PCA) Waiver Billing Provider Workshop for Personal Care Service Providers Presented by The Department of Social Services & Hewlett Packard Enterprise 1 PCA Waiver Workshop Introduction
Personal Care Attendant (PCA) Waiver Billing Provider Workshop for Personal Care Service Providers Presented by The Department of Social Services & Hewlett Packard Enterprise 1 PCA Waiver Workshop Introduction
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 04/11/2018 *all red text is new for 04/11/2018 The following documents were recently updated: CMAP Addendum B Connecticut Medical Assistance Program s (CMAP
Hospital Monthly Important Message Updated as of 04/11/2018 *all red text is new for 04/11/2018 The following documents were recently updated: CMAP Addendum B Connecticut Medical Assistance Program s (CMAP
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 09/14/2016 *all red text is new for 09/14/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Hospital Monthly Important Message Updated as of 09/14/2016 *all red text is new for 09/14/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 11/09/2016 *all red text is new for 11/09/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Hospital Monthly Important Message Updated as of 11/09/2016 *all red text is new for 11/09/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Community Health Network of CT, Inc.
 PRPRE0024-0712 Clear Coverage Online Authorizations Outpatient Surgery Community Health Network of CT, Inc. A New Way to Request Authorizations As of July 31, 2012, there are now three options for requesting
PRPRE0024-0712 Clear Coverage Online Authorizations Outpatient Surgery Community Health Network of CT, Inc. A New Way to Request Authorizations As of July 31, 2012, there are now three options for requesting
Connecticut interchange MMIS
 Connecticut interchange MMIS Provider Manual Claim Submission Information Chapter 5 Connecticut Department of Social Services (DSS) 25 Sigourney Street Hartford, CT 06106 EDS US Government Solutions 195
Connecticut interchange MMIS Provider Manual Claim Submission Information Chapter 5 Connecticut Department of Social Services (DSS) 25 Sigourney Street Hartford, CT 06106 EDS US Government Solutions 195
Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide
 Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide Version 5.0 February 26, 2007 Revision History Document Version Date Name Comments 1.0 12/27/2006 Patti George Created. 2.0
Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide Version 5.0 February 26, 2007 Revision History Document Version Date Name Comments 1.0 12/27/2006 Patti George Created. 2.0
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
REINSTATEMENT And IMPLEMENTATION Of LAHIPP THIRD PARTY LIABILITY (TPL) CLAIMS PAYMENT
 REINSTATEMENT And IMPLEMENTATION Of LAHIPP THIRD PARTY LIABILITY (TPL) CLAIMS PAYMENT April 7, 2017 LOUISIANA MEDICAID PROGRAM DEPARTMENT OF HEALTH BUREAU OF HEALTH SERVICES FINANCING TABLE OF CONTENTS
REINSTATEMENT And IMPLEMENTATION Of LAHIPP THIRD PARTY LIABILITY (TPL) CLAIMS PAYMENT April 7, 2017 LOUISIANA MEDICAID PROGRAM DEPARTMENT OF HEALTH BUREAU OF HEALTH SERVICES FINANCING TABLE OF CONTENTS
Clear Coverage Online Authorizations Community Health Network of CT, Inc.
 Clear Coverage Online Authorizations Community Health Network of CT, Inc. Overview Clear coverage is an online authorization tool which: Lowers authorization turn around time Improves workflow by decreasing
Clear Coverage Online Authorizations Community Health Network of CT, Inc. Overview Clear coverage is an online authorization tool which: Lowers authorization turn around time Improves workflow by decreasing
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Connecticut interchange MMIS
 Connecticut interchange MMIS Provider Manual Chapter 7 Licensed Behavioral Health Clinicians in Independent Practice February 1, 2013 Connecticut Department of Social Services (DSS) 55 Farmington Ave Hartford,
Connecticut interchange MMIS Provider Manual Chapter 7 Licensed Behavioral Health Clinicians in Independent Practice February 1, 2013 Connecticut Department of Social Services (DSS) 55 Farmington Ave Hartford,
Living Choices Assisted Living September 2016 HP Fiscal Agent for the Arkansas Division of Medical Services
 Living Choices Assisted Living September 2016 HP Fiscal Agent for the Arkansas Division of Medical Services 1 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and
Living Choices Assisted Living September 2016 HP Fiscal Agent for the Arkansas Division of Medical Services 1 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and
UB-04 Medicare Crossover and Replacement Plans. HP Provider Relations October 2012
 UB-04 Medicare Crossover and Replacement Plans HP Provider Relations October 2012 Agenda Objectives Medicare crossover claim defined Medicare replacement plan claims Electronic billing of crossovers Paper
UB-04 Medicare Crossover and Replacement Plans HP Provider Relations October 2012 Agenda Objectives Medicare crossover claim defined Medicare replacement plan claims Electronic billing of crossovers Paper
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
Research and Resolve UB-04 Claim Denials. HP Provider Relations/October 2014
 Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise.
 Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
MHS CMS 1500 Tips and Billing Guidelines
 MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
Claims Management. February 2016
 Claims Management February 2016 Overview Claim Submission Remittance Advice (RA) Exception Codes Exception Resolution Claim Status Inquiry Additional Information 2 Claim Submission 3 4 Life of a Claim
Claims Management February 2016 Overview Claim Submission Remittance Advice (RA) Exception Codes Exception Resolution Claim Status Inquiry Additional Information 2 Claim Submission 3 4 Life of a Claim
CMS 1500 Online Claims Entry. Conduent Government Healthcare Solutions
 CMS 1500 Online Claims Entry Conduent Government Healthcare Solutions Resources When online use: Ask Service Representative HIPAA.Desk.NM@Conduent.com NMProviderSupport@Conduent.com Call Center 505-246-0710
CMS 1500 Online Claims Entry Conduent Government Healthcare Solutions Resources When online use: Ask Service Representative HIPAA.Desk.NM@Conduent.com NMProviderSupport@Conduent.com Call Center 505-246-0710
How to Order an Employment Verification
 How to Order an Employment Verification To order an Employment verification, do the following: Some employers require using an alternate Employee ID rather than using a SSN. If this is a requirement for
How to Order an Employment Verification To order an Employment verification, do the following: Some employers require using an alternate Employee ID rather than using a SSN. If this is a requirement for
Kansas Medical Assistance Program. Vertical Perspective. Other Insurance/Medicare Training Packet - Professional
 Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
SutterSelect Administrative Manual. June 2017
 SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
Kentucky Medicaid. Spring 2009 Billing Workshop UB04
 Kentucky Medicaid Spring 2009 Billing Workshop UB04 Agenda Representative List Reference List UB Claim Form Detailed Billing Instructions NDC (Hospitals and Renal Dialysis) Forms Timely Filing FAQ S Did
Kentucky Medicaid Spring 2009 Billing Workshop UB04 Agenda Representative List Reference List UB Claim Form Detailed Billing Instructions NDC (Hospitals and Renal Dialysis) Forms Timely Filing FAQ S Did
Goals. Reflection. The 3 Ps: Marcus Lemonis. Private Practice Management: From Intake to Billing 9/18/16
 Private Practice Management: From Intake to Billing Christian J. Dean, Ph.D., LPC-S, LMFT, NCC And Sola Kippers, Ph.D., LPC-S, LMFT Goals O Have an understanding of overall practice components (brief overview)
Private Practice Management: From Intake to Billing Christian J. Dean, Ph.D., LPC-S, LMFT, NCC And Sola Kippers, Ph.D., LPC-S, LMFT Goals O Have an understanding of overall practice components (brief overview)
Avenues of Resolution for Indiana Health Coverage Programs
 Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Claim Adjustment Process. HP Provider Relations/October 2015
 Claim Adjustment Process HP Provider Relations/October 2015 Agenda Types of adjustments System-initiated adjustments Web interchange adjustment process Void feature Paper adjustment process Timely filing
Claim Adjustment Process HP Provider Relations/October 2015 Agenda Types of adjustments System-initiated adjustments Web interchange adjustment process Void feature Paper adjustment process Timely filing
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Life of a Claim. HP Provider Relations/August 2014
 Life of a Claim HP Provider Relations/August 2014 Agenda General requirements for reimbursement by the Indiana Health Coverage Programs (IHCP) System edits System audits Pricing methodologies Suspended
Life of a Claim HP Provider Relations/August 2014 Agenda General requirements for reimbursement by the Indiana Health Coverage Programs (IHCP) System edits System audits Pricing methodologies Suspended
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
Behavioral Health FAQs
 Behavioral Health FAQs Authorizations & Notifications Q: The behavioral health prior authorization forms do not indicate what documentation to submit. What clinical information should I send with a prior
Behavioral Health FAQs Authorizations & Notifications Q: The behavioral health prior authorization forms do not indicate what documentation to submit. What clinical information should I send with a prior
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers
 Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
Claim Submission Process Training For Individual Consumer-Directed Attendant Care Providers Topics Overview Accessing Online Self-Service Tools Billing the Member Claim Submission Forms Claim Submission
Network Health Claims Editing Portal
 Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Housekeeping. Link Participant ID with Audio. Mute your line UNMUTED. Raise your hand with questions
 Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
TRANSACTION STANDARD TRADING PARTNER AGREEMENT/ADDENDUM
 TRANSACTION STANDARD TRADING PARTNER AGREEMENT/ADDENDUM This Trading Partner Agreement ( TPA ) is entered into between DXC Technology Services LLC ( DXC Services ), as an agent for the Connecticut Department
TRANSACTION STANDARD TRADING PARTNER AGREEMENT/ADDENDUM This Trading Partner Agreement ( TPA ) is entered into between DXC Technology Services LLC ( DXC Services ), as an agent for the Connecticut Department
Insert photo here. Common Denials. Presented by EDS Provider Field Consultants
 Insert photo here Common Denials Presented by EDS Provider Field Consultants October 2007 Common Denials Agenda Session Objectives Edits and Audits Defined Edit Grouping Denial Overview Questions 2 October
Insert photo here Common Denials Presented by EDS Provider Field Consultants October 2007 Common Denials Agenda Session Objectives Edits and Audits Defined Edit Grouping Denial Overview Questions 2 October
Availity TM Eligibility and Benefits Inquiry
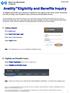 October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
Summary of Changes - New Enrollment and Claims Payment System Effective June 1, 2017
 Overview Starting June 1, 2017, UnitedHealthcare Community Plan in Florida will change to a new enrollment and claims payment system. This Summary of Changes is a guide to help answer questions you may
Overview Starting June 1, 2017, UnitedHealthcare Community Plan in Florida will change to a new enrollment and claims payment system. This Summary of Changes is a guide to help answer questions you may
Dual Special Needs Plans, Behavioral Benefit
 Dual Special Needs Plans, Behavioral Benefit Offered by UnitedHealthcare Dual Complete Launch Date January 1, 2019 Contents What are Dual Special Needs Plans (DSNPs)? UnitedHealthcare Dual Complete Behavioral
Dual Special Needs Plans, Behavioral Benefit Offered by UnitedHealthcare Dual Complete Launch Date January 1, 2019 Contents What are Dual Special Needs Plans (DSNPs)? UnitedHealthcare Dual Complete Behavioral
CoreMMIS bulletin Core benefits Core enhancements Core communications
 CoreMMIS bulletin Core benefits Core enhancements Core communications INDIANA HEALTH COVERAGE PROGRAMS BT201667 OCTOBER 20, 2016 CoreMMIS billing guidance: Part I On December 5, 2016, the Indiana Health
CoreMMIS bulletin Core benefits Core enhancements Core communications INDIANA HEALTH COVERAGE PROGRAMS BT201667 OCTOBER 20, 2016 CoreMMIS billing guidance: Part I On December 5, 2016, the Indiana Health
Indiana Health Coverage Program Seminar Presented by MDwise UB-04 October 22-24, 2007
 Indiana Health Coverage Program Seminar Presented by MDwise UB-04 October 22-24, 2007 Topics for today Who is MDwise MDwise Delivery Systems UB-04 Claims submission and Inquiries Referrals and Prior Authorization
Indiana Health Coverage Program Seminar Presented by MDwise UB-04 October 22-24, 2007 Topics for today Who is MDwise MDwise Delivery Systems UB-04 Claims submission and Inquiries Referrals and Prior Authorization
The benefits of using ExpressPAth for your practice include: Easy access. With 24/7 access, you can submit requests and get answers at any time.
 Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
KALAMAZOO COMMUNITY MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES ADMINISTRATIVE PROCEDURE 08.08
 KALAMAZOO COMMUNITY MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES ADMINISTRATIVE PROCEDURE 08.08 Subject: Claims Management Section: Financial Management Applies To: Page: KCMHSAS Staff KCMHSAS Contract Providers
KALAMAZOO COMMUNITY MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES ADMINISTRATIVE PROCEDURE 08.08 Subject: Claims Management Section: Financial Management Applies To: Page: KCMHSAS Staff KCMHSAS Contract Providers
New MN ITS Direct Data Entry (DDE) Screens Professional (837P)
 New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
Third Party Liability. Presented by EDS Provider Field Consultants
 Third Party Liability Presented by EDS Provider Field Consultants OCTOBER 2007 Agenda Session Objectives TPL Responsibilities Identifying TPL Resources Updating TPL Information Reporting Casualty Cases
Third Party Liability Presented by EDS Provider Field Consultants OCTOBER 2007 Agenda Session Objectives TPL Responsibilities Identifying TPL Resources Updating TPL Information Reporting Casualty Cases
0518.PR.P.PP.2 7/18. The Ins and Outs of CMS 1500 Billing
 0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
DTE Energy retirees: Welcome to PayFlex
 DTE Energy retirees: Welcome to PayFlex You are enrolled in a Retiree Reimbursement Account (RRA). Your new RRA comes with some great tools to help you manage your account. Through the PayFlex member website,
DTE Energy retirees: Welcome to PayFlex You are enrolled in a Retiree Reimbursement Account (RRA). Your new RRA comes with some great tools to help you manage your account. Through the PayFlex member website,
Your. Getting Reimbursed Guide
 Your Getting Reimbursed Guide Table of Contents Introduction to Getting Reimbursed........... 4 Managing your HRA online................ 5 The Reimbursement Process............... 8 Getting Started with
Your Getting Reimbursed Guide Table of Contents Introduction to Getting Reimbursed........... 4 Managing your HRA online................ 5 The Reimbursement Process............... 8 Getting Started with
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise.
 Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents
 Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Transportation.. the right way. HP Provider Relations/October 2013
 Transportation.. the right way HP Provider Relations/October 2013 Agenda Session objectives Transportation services Provider enrollment Member eligibility Billing guidelines Copayment amounts and exemptions
Transportation.. the right way HP Provider Relations/October 2013 Agenda Session objectives Transportation services Provider enrollment Member eligibility Billing guidelines Copayment amounts and exemptions
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Arise Health Insurance Fully Insured Groups 51+ and Self-Funded Groups. Choose It and Use It.
 Arise Health Insurance Fully Insured Groups 51+ and Self-Funded Groups Choose It and Use It. What can you count on from Arise Health Plan? Personal service, plus top-quality coverage You get health coverage
Arise Health Insurance Fully Insured Groups 51+ and Self-Funded Groups Choose It and Use It. What can you count on from Arise Health Plan? Personal service, plus top-quality coverage You get health coverage
Claim Adjustment Process. HP Provider Relations/October 2013
 Claim Adjustment Process HP Provider Relations/October 2013 Agenda Session Objectives Types of Adjustments Adjustment Criteria Adjustment Process Web interchange Replacement Process Paper Adjustment Process
Claim Adjustment Process HP Provider Relations/October 2013 Agenda Session Objectives Types of Adjustments Adjustment Criteria Adjustment Process Web interchange Replacement Process Paper Adjustment Process
Molina/BMS 2012 Provider Workshops IRG d/b/a APS Healthcare, Inc. Updates. Presented by: Helen C. Snyder, Associate Director
 Molina/BMS 2012 Provider Workshops IRG d/b/a APS Healthcare, Inc. Updates Presented by: Helen C. Snyder, Associate Director Updates Provider Registration with APS v. Molina Medicaid enrollment Eligibility/Provider
Molina/BMS 2012 Provider Workshops IRG d/b/a APS Healthcare, Inc. Updates Presented by: Helen C. Snyder, Associate Director Updates Provider Registration with APS v. Molina Medicaid enrollment Eligibility/Provider
FlexChoice. Reimbursement Account Overview. Sentinel Benefits. Custom Solutio ns for Life and Wealth
 FlexChoice Reimbursement Account Overview Sentinel Benefits & F I NA N CI A L GRO U P Custom Solutio ns for Life and Wealth Welcome to Your F SA We have put together this guide to help you get the most
FlexChoice Reimbursement Account Overview Sentinel Benefits & F I NA N CI A L GRO U P Custom Solutio ns for Life and Wealth Welcome to Your F SA We have put together this guide to help you get the most
Basic Billing 2013 Ohio Medicaid Home Care Agencies
 Basic Billing 2013 Ohio Medicaid Home Care Agencies Ombudsman Kathy Frye Laura Gipson Dwayne Knowles Kenneth Morgan Jamie Speakes Meagan Lyle, Manager Office of Ohio Health Plans External Business Relations
Basic Billing 2013 Ohio Medicaid Home Care Agencies Ombudsman Kathy Frye Laura Gipson Dwayne Knowles Kenneth Morgan Jamie Speakes Meagan Lyle, Manager Office of Ohio Health Plans External Business Relations
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
Archived SECTION 17 - CLAIMS DISPOSITION. Section 17 - Claims Disposition
 SECTION 17 - CLAIMS DISPOSITION 17.1 ACCESS TO REMITTANCE ADVICES...2 17.2 INTERNET AUTHORIZATION...3 17.3 ON-LINE HELP...3 17.4 REMITTANCE ADVICE...3 17.5 CLAIM STATUS MESSAGE CODES...7 17.5.A FREQUENTLY
SECTION 17 - CLAIMS DISPOSITION 17.1 ACCESS TO REMITTANCE ADVICES...2 17.2 INTERNET AUTHORIZATION...3 17.3 ON-LINE HELP...3 17.4 REMITTANCE ADVICE...3 17.5 CLAIM STATUS MESSAGE CODES...7 17.5.A FREQUENTLY
UB-04 Workshop. Presented by: Xerox State Healthcare, LLC Provider Relations
 UB-04 Workshop Presented by: Xerox State Healthcare, LLC Provider Relations Resources When online use: Ask Service Representative HIPAA.Desk.NM@xerox.com NMPRSupport@xerox.com Call Center 505-246-0710
UB-04 Workshop Presented by: Xerox State Healthcare, LLC Provider Relations Resources When online use: Ask Service Representative HIPAA.Desk.NM@xerox.com NMPRSupport@xerox.com Call Center 505-246-0710
PARTNERS HEALTH PLAN PHP CARE COMPLETE FIDA-IDD. TRAINING FOR DEVELOPMENTAL DISABILITIES PROVIDER NETWORK June 16, 2017
 PARTNERS HEALTH PLAN PHP CARE COMPLETE FIDA-IDD TRAINING FOR DEVELOPMENTAL DISABILITIES PROVIDER NETWORK June 16, 2017 AGENDA Welcome & Introduction Care Management/Interdisciplinary Teams (IDT)/Life Plans
PARTNERS HEALTH PLAN PHP CARE COMPLETE FIDA-IDD TRAINING FOR DEVELOPMENTAL DISABILITIES PROVIDER NETWORK June 16, 2017 AGENDA Welcome & Introduction Care Management/Interdisciplinary Teams (IDT)/Life Plans
HP Provider Electronic Solutions. Billing Instructions. Long Term Care Claims
 HP Provider Electronic Solutions Billing Instructions Long Term Care Claims TABLE OF CONTENTS INTRODUCTION... 3 CLIENT SCREEN... 5 CLIENT ENTRY INSTRUCTIONS... 5 BILLING PROVIDER SCREEN... 7 BILLING PROVIDER
HP Provider Electronic Solutions Billing Instructions Long Term Care Claims TABLE OF CONTENTS INTRODUCTION... 3 CLIENT SCREEN... 5 CLIENT ENTRY INSTRUCTIONS... 5 BILLING PROVIDER SCREEN... 7 BILLING PROVIDER
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
ALABAMA MEDICAID AGENCY ADMINISTRATIVE CODE CHAPTER 560-X-20 THIRD PARTY TABLE OF CONTENTS
 Medicaid Chapter 560-X-20 ALABAMA MEDICAID AGENCY ADMINISTRATIVE CODE CHAPTER 560-X-20 THIRD PARTY TABLE OF CONTENTS 560-X-20-.01 560-X-20-.02 560-X-20-.03 560-X-20-.04 560-X-20-.05 560-X-20-.06 560-X-20-.07
Medicaid Chapter 560-X-20 ALABAMA MEDICAID AGENCY ADMINISTRATIVE CODE CHAPTER 560-X-20 THIRD PARTY TABLE OF CONTENTS 560-X-20-.01 560-X-20-.02 560-X-20-.03 560-X-20-.04 560-X-20-.05 560-X-20-.06 560-X-20-.07
Section 65 Children s Behavioral Health Day Treatment. KEPRO Mapping Document
 Section 65 Children s Behavioral Health Day Treatment KEPRO Mapping Document Initiating Requests in KEPRO Login to KEPRO Care Connection (must be done using Internet Explorer, IE Tab for Chrome, or using
Section 65 Children s Behavioral Health Day Treatment KEPRO Mapping Document Initiating Requests in KEPRO Login to KEPRO Care Connection (must be done using Internet Explorer, IE Tab for Chrome, or using
Pfizer encompass Co-Pay Assistance Program for INFLECTRA :
 Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Patient Resource Guide
 Access Services Patient Resource Guide AstraZeneca Access 360 is committed to helping you access our medicines. This guide will provide you with information and resources to help you understand how to
Access Services Patient Resource Guide AstraZeneca Access 360 is committed to helping you access our medicines. This guide will provide you with information and resources to help you understand how to
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Physical Therapy. Contact your Primary Access Administrator (PAA) if Eligibility and Benefits is not listed in the navigation menu.
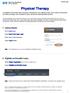 October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
QUICK TIP: Download a Quick Reference Guide from the Resource Center to help you use the PayFlex member website.
 [Date] Dear DTE Energy Retiree, It s our pleasure to welcome you to PayFlex! You re enrolled in a Retiree Reimbursement Account (RRA). Your RRA comes with some great tools to help you manage your account.
[Date] Dear DTE Energy Retiree, It s our pleasure to welcome you to PayFlex! You re enrolled in a Retiree Reimbursement Account (RRA). Your RRA comes with some great tools to help you manage your account.
Rural Health Clinics Mississippi Medicaid
 O f f i c e o f t h e G o v e r n o r M i s s i s s i p p i D i v i s i o n o f M e d i c a i d Rural Health Clinics Mississippi Medicaid Mary Katherine Ulmer, M.S. O F F I C E O F T H E G O V E R N O
O f f i c e o f t h e G o v e r n o r M i s s i s s i p p i D i v i s i o n o f M e d i c a i d Rural Health Clinics Mississippi Medicaid Mary Katherine Ulmer, M.S. O F F I C E O F T H E G O V E R N O
Health Share Treatment Authorization Request for PA (HSTAR_PA) Form
 Health Share Treatment Authorization Request for PA (HSTAR_PA) Form Instructions for Completing the HSTAR General Information This form is for use by providers contracted with Health Share of Oregon as
Health Share Treatment Authorization Request for PA (HSTAR_PA) Form Instructions for Completing the HSTAR General Information This form is for use by providers contracted with Health Share of Oregon as
RULES OF DEPARTMENT OF COMMERCE AND INSURANCE DIVISION OF INSURANCE AND DIVISION OF TENNCARE
 RULES OF DEPARTMENT OF COMMERCE AND INSURANCE DIVISION OF INSURANCE AND DIVISION OF TENNCARE CHAPTER 0780-1-73 UNIFORM CLAIMS PROCESS FOR TENNCARE PARTICIPATING TABLE OF CONTENTS 0780-1-73-.01 Authority
RULES OF DEPARTMENT OF COMMERCE AND INSURANCE DIVISION OF INSURANCE AND DIVISION OF TENNCARE CHAPTER 0780-1-73 UNIFORM CLAIMS PROCESS FOR TENNCARE PARTICIPATING TABLE OF CONTENTS 0780-1-73-.01 Authority
IHCP Annual Workshop October 2016
 IHCP Annual Workshop October 2016 MDwise CMS-1500 Billing and Claim Processing Exclusively serving Indiana families since 1994. Agenda Who is MDwise? Provider Enrollment: Are you a contracted MDwise Provider?
IHCP Annual Workshop October 2016 MDwise CMS-1500 Billing and Claim Processing Exclusively serving Indiana families since 1994. Agenda Who is MDwise? Provider Enrollment: Are you a contracted MDwise Provider?
FIND A DOCTOR Page 1 of 22
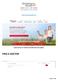 www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
www.hometownhealth.com FIND A DOCTOR Page 1 of 22 Type in Name of Doctor OR ADVANCED SEARCH You can filter your results by: Provider Last OR Group Name Provider Type City County Specialty Plan Zip Code
Access to Care. BlueEdge HSA with HSA Bank
 Access to Care SM BlueEdge HSA with HSA Bank Welcome to your BlueEdge HSA, offered by Blue Cross and Blue Shield of Texas (BCBSTX). The BlueEdge HSA combines a high deductible health plan (HDHP) with a
Access to Care SM BlueEdge HSA with HSA Bank Welcome to your BlueEdge HSA, offered by Blue Cross and Blue Shield of Texas (BCBSTX). The BlueEdge HSA combines a high deductible health plan (HDHP) with a
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Unit 14 Radiology Management
 Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Utilization Management Request for Services Process. October 21, 2015
 Utilization Management Request for Services Process October 21, 2015 Illinois Mental Health Collaborative PRESENTERS Brent Sparlin Clinical Quality Assurance Analyst and Lauren Kelbus Clinical Care Manager
Utilization Management Request for Services Process October 21, 2015 Illinois Mental Health Collaborative PRESENTERS Brent Sparlin Clinical Quality Assurance Analyst and Lauren Kelbus Clinical Care Manager
Tellus EVV Claims Portal TRAINING REFERENCE GUIDE
 Tellus EVV Claims Portal TRAINING REFERENCE GUIDE REV: 11/17 Sponsored by Centric Consulting, LLC, and the State of Florida, AHCA Table of Contents... 3 5.1 Overview... 3 5.2 Claims Home Page... 4 5.3
Tellus EVV Claims Portal TRAINING REFERENCE GUIDE REV: 11/17 Sponsored by Centric Consulting, LLC, and the State of Florida, AHCA Table of Contents... 3 5.1 Overview... 3 5.2 Claims Home Page... 4 5.3
Billing and Claims Overview. January February 2018
 Billing and Claims Overview January 2018 - February 2018 BH1182-012018 Claims Submission option 1 Online Entry through www.unitedhealthcareonline.com Submitting claims closely mirrors the process of manually
Billing and Claims Overview January 2018 - February 2018 BH1182-012018 Claims Submission option 1 Online Entry through www.unitedhealthcareonline.com Submitting claims closely mirrors the process of manually
Managed Health Services
 Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
SDMGMA Third Party Payer Day. Lori Lawson, Deputy Medicaid Director
 SDMGMA Third Party Payer Day Lori Lawson, Deputy Medicaid Director 1 Agenda Medicaid Overview TPL ARSD How to report TPL on 1500 form How to report TPL on UB form Common TPL Errors ICD-10 update a. Readiness
SDMGMA Third Party Payer Day Lori Lawson, Deputy Medicaid Director 1 Agenda Medicaid Overview TPL ARSD How to report TPL on 1500 form How to report TPL on UB form Common TPL Errors ICD-10 update a. Readiness
NEW YORK STATE MEDICAID PROGRAM INFORMATION FOR ALL PROVIDERS GENERAL BILLING
 NEW YORK STATE MEDICAID PROGRAM INFORMATION FOR ALL PROVIDERS GENERAL BILLING Table of Contents COMMON BENEFIT IDENTIFICATION CARD...2 VOICE INTERACTIVE PHONE SYSTEM...3 PRIOR APPROVAL ROSTERS...4 ELECTRONIC
NEW YORK STATE MEDICAID PROGRAM INFORMATION FOR ALL PROVIDERS GENERAL BILLING Table of Contents COMMON BENEFIT IDENTIFICATION CARD...2 VOICE INTERACTIVE PHONE SYSTEM...3 PRIOR APPROVAL ROSTERS...4 ELECTRONIC
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT
 CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
Claim Investigation Submission Guide
 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
SECTION 9 1 CLAIMS PROCEDURES
 SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
How to Journalize using Data Entry
 Steps Essential to Success 1. Print a copy of the Problem you intend to complete. To do so, go to the software log-in page and click on Download Student Manual button, click on the Problem to open it.
Steps Essential to Success 1. Print a copy of the Problem you intend to complete. To do so, go to the software log-in page and click on Download Student Manual button, click on the Problem to open it.
Applied Behavior Analysis (ABA) Proper Billing Guidelines & Authorization Updates. January 2016
 Applied Behavior Analysis (ABA) Proper Billing Guidelines & Authorization Updates January 2016 The Way Forward 2 Objectives Overview of Claims-Proper Billing Procedures NPI Registration Authorization Updates
Applied Behavior Analysis (ABA) Proper Billing Guidelines & Authorization Updates January 2016 The Way Forward 2 Objectives Overview of Claims-Proper Billing Procedures NPI Registration Authorization Updates
TO: Merchants Insurance Group Commercial Lines Agents [EXCEPT NEW YORK]
![TO: Merchants Insurance Group Commercial Lines Agents [EXCEPT NEW YORK] TO: Merchants Insurance Group Commercial Lines Agents [EXCEPT NEW YORK]](/thumbs/76/73744052.jpg) February 13, 2017 BULLETIN NO. 5622 TO: Merchants Insurance Group Commercial Lines Agents [EXCEPT NEW YORK] SUBJECT: Introduction of New Credit Card Payment Vendor Agency Bulletin Effective February 13,
February 13, 2017 BULLETIN NO. 5622 TO: Merchants Insurance Group Commercial Lines Agents [EXCEPT NEW YORK] SUBJECT: Introduction of New Credit Card Payment Vendor Agency Bulletin Effective February 13,
