Incontinence Supplies Policy
|
|
|
- Randolph Henry
- 6 years ago
- Views:
Transcription
1 Policy Number 2018R7111C Incontinence Supplies Policy Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible for submission of accurate claims. This reimbursement policy is intended to ensure that you are reimbursed based on the code or codes that correctly describe the health care services provided. UnitedHealthcare Community Plan reimbursement policies uses Current Procedural Terminology (CPT *), Centers for Medicare and Medicaid Services (CMS) or other coding guidelines. References to CPT or other sources are for definitional purposes only and do not imply any right to reimbursement. This reimbursement policy applies to all health care services billed on CMS 1500 forms and, when specified, to those billed on UB04 forms. Coding methodology, industry-standard reimbursement logic, regulatory requirements, benefits design and other factors are considered in developing reimbursement policy. This information is intended to serve only as a general reference resource regarding UnitedHealthcare Community Plan s reimbursement policy for the services described and is not intended to address every aspect of a reimbursement situation. Accordingly, UnitedHealthcare Community Plan may use reasonable discretion in interpreting and applying this policy to health care services provided in a particular case. Further, the policy does not address all issues related to reimbursement for health care services provided to UnitedHealthcare Community Plan enrollees. Other factors affecting reimbursement supplement, modify or, in some cases, supersede this policy. These factors include, but are not limited to: federal &/or state regulatory requirements, the physician or other provider contracts, the enrollee s benefit coverage documents, and/or other reimbursement, medical or drug policies. Finally, this policy may not be implemented exactly the same way on the different electronic claims processing systems used by UnitedHealthcare Community Plan due to programming or other constraints; however, UnitedHealthcare Community Plan strives to minimize these variations. UnitedHealthcare Community Plan may modify this reimbursement policy at any time by publishing a new version of the policy on this Website. However, the information presented in this policy is accurate and current as of the date of publication. CPT Copyright American Medical Association. All rights reserved. CPT is a registered trademark of the American Medical Association. Application This reimbursement policy applies to UnitedHealthcare Community Plan Medicaid Product This reimbursement policy applies to services reported using the 1500 Health Insurance Claim Form (a/k/a ) or its electronic equivalent or its successor form. This policy applies to all products and all network and non-network physicians and other qualified health care professionals, including, but not limited to, non-network authorized and percent of charge contract physicians and other qualified health care professionals. Payment Policies for Medicare & Retirement, UnitedHealthcare Community Plan Medicare and Employer & Individual please use this link. Medicare & Retirement and UnitedHealthcare Community Plan Medicare Policies are listed under Medicare Advantage Reimbursement Policies. Employer & Individual are listed under Reimbursement Policies-Commercial.
2 Policy Overview This policy identifies circumstances in which UnitedHealthcare Community Plan will reimburse suppliers for incontinence supplies and the maximum amount of supplies that will be reimbursed per month. Reimbursement Guidelines For the purposes of this policy, incontinence supplies have been split into two subgroups. Group 1 includes disposable diapers, briefs, protective underwear, pull-ons, liners, etc. Group 2 includes Disposable underpads (commonly called chux). The HCPCS codes for each supply within a group that is addressed in this policy are listed in the Codes section below. Washable (non-disposable) items are not addressed in this policy. Claims for incontinence supplies must contain more than one ICD-10 diagnosis code. An ICD-10 diagnosis code from the Incontinence Supplies ICD-10 List and an ICD-10 diagnosis code reflecting the condition causing the incontinence must both be present on the claim. If one or more of the ICD-10 diagnoses on the Incontinence Supplies ICD-10 List are the ONLY diagnosis code(s) on the claim all incontinence supplies will be denied. For a list of acceptable ICD-10 diagnosis codes, refer to the Attachment Section Claims for incontinence supplies must meet state specific age requirements. For a list of state specific age requirements, refer to the Attachment Section. Unless a different amount is outlined in the State Maximums Section, a maximum of 300 individual units/items from the Group 1 supplies will be allowed per member per month. This equates to 9-10 disposable incontinent supply items per day or one every 2 ¼ - 2 ½ hours. All Group 1 codes are monthly aggregates, regardless of a member requiring a change in size during the month. The maximum amount of each size per member per month is not allowed. Once the maximum unit/item count of Group 1 has been met, documentation showing medical necessity for exceeding the limit must be submitted before payment for any exceeding the maximum will be considered. Orders for all supplies must be submitted with the appropriate HCPCS code for the size provided. If a member does not require incontinence supplies in Group 1, then no supplies in Group 2 will be reimbursable. If the member does require supplies from Group 1, then the Group 2 supplies will be allowed. Unless a different amount is outlined in the State Maximums Section, a maximum of 300 individual units/items from the Group 2 supplies will be allowed per member per month. For a list of acceptable HCPCS Group 1 and Group 2 Supplies codes, refer to the Attachment Section Vendors are not to schedule automatic shipment of incontinence supplies. Prior to each shipment, the vendor should contact the member or caregiver to determine the quantity of supplies on hand and the appropriate size and date for shipment. The delivery date should not be prior to the member having 15 days of supplies available. An order should not contain more than 30 day s worth of supplies. Delivering items where standard packaging exceeds 45 days or more supply is not permitted. Stockpiling of supplies is not allowed. State Maximums for Group 1/Group 2 HCPCS Codes based on State (authorization may be required based on benefits and provider manual). 360/month MS CAN 300/month HI, MI, OH, PA, WI, RI, NE (Group 1) NY (Group 2)
3 250/month DE, MA, MD, NY (Group 1), TX, LA 200/month NJ, NM (Group 1), WA, FL, TN 186/month KS, MO 150/month NM, RI (Group 2) REIMBURSEMENT POLICY State Exceptions Arizona Arizona is exempt from this policy as their incontinence supplies are handled via capitation thru a specified vendor For Arizona Long Term Care (AZ LTC) only: AZ LTC has a combined quantity limit for incontinence supplies: Max combined quantity limit of 180 per month for members age 21 and older AZ LTC is exempt from remainder of the policy Max combined quantity limit of 240 per month for members under age 21 California Per California Medicaid, only codes from the Incontinence Supplies ICD-10 Diagnosis Codes List are acceptable as a secondary diagnosis For a list of acceptable California secondary ICD-10 diagnosis codes, refer to the Attachment Section. Per State Regulations Codes T4525, T4526, T4527, T4528, T4541, T4542 and T4544 are limited to 120 units in a 27 day period Codes T4522 and T4524 are limited to no more than 192 units in a 27 day period Codes T4521, T4529, T4530, T4531, T4532, T4533, T4534 and T4543 are limited to no more than 200 units in a 27 day period Code T4523 is limited to no more than 216 units in a 27 day period Florida Incontinence Supplies may be reimbursed up to a combined total of 200 units Florida Long Term Care (LTC), Home and Community Based Services (HCBS) are excluded from this policy due to state requirements Iowa Per State Regulation, Iowa incontinence supply codes can be billed separately or in a combination between groups. For a list of acceptable Iowa Medicaid Maximum Unit Limits and Timeframes, refer to the Attachment Section Iowa Medicaid must submit a diagnosis from the Iowa Incontinence Supplies Codes List and an ICD-10 diagnosis code reflecting the condition causing incontinence. For a list of acceptable ICD-10 diagnosis codes refer to the Attachment Section. Iowa requires documentation to be submitted for supplies that exceed the expected maximum
4 Kansas REIMBURSEMENT POLICY Per State Regulation, codes A4553 and A4554 is exempt from this policy for Medicaid because they are not considered to be incontinence supplies. CodesT4541 and T4542 are not covered Per State Regulation, Home Health Care Providers are required to submit one diagnosis and it must be one of these diagnosis codes F98.0, F98.1, N39.42, N39.45, R15.9 or R39.81 and covered for member s age 21 and over Louisiana Michigan Missouri New Mexico Louisiana requires documentation to be submitted for supplies that exceed the expected maximum Per State Regulation, Michigan is excluded from the Group 2 denials if there are no Group 1 supplies received Incontinence Supplies may be reimbursed up to a combined total of 186 units and requires documentation to be submitted for supplies that exceed the maximum units New Mexico is excluded from the Group 2 denials if there are no Group 1 supplies received New Mexico Medicaid is limited to either 200 diapers (Group 1) per month or 150 underpads (Group 2) per month, but not both New York New York Medicaid providers are required to submit one diagnosis and it must be from the New York Incontinence Supplies List. For a list of acceptable ICD-10 diagnosis codes refer to the Attachment Section. Per State Regulation, code A4554 allows a maximum of 300 units per month Pennsylvania Tennessee Virginia Per State Regulation, Pennsylvania Medicaid is excluded from the Group 2 denials if there are no Group 1 supplies received and the diagnosis requirement Tennessee requires documentation to be submitted for supplies that exceed the expected maximum Virginia is excluded from the Group 2 denials if there are no Group 1 supplies received Per State Regulations, there are no state maximums for Group 1 and Group 2 supplies Questions and Answers 1 2 Q: Why are incontinence supplies not reimbursed when only one diagnosis code is submitted? A: A valid incontinence diagnosis and condition causing the incontinence must be listed on the claim along with any symptoms. A claim that list codes based on symptoms alone will not pay. Therefore a diagnosis code causing the incontinence should be billed along with the symptom diagnosis code indicating the cause of the symptoms. So, it is not that the diagnosis is not covered, but that another code must be billed along with the diagnosis code for the symptoms that shows the condition causing the symptoms. Q: Why are Group 2 supplies not reimbursed? A: Group 2 supplies are covered, but only if the member is also receiving Group 1 supplies. Group 2 products are used to maintain sanitary conditions for the member. The primary use is not to protect furniture and bedding. If the member does not require the use of the Group 1 products in order to maintain sanitary conditions, then there should be no need for the Group 2 products.
5 Attachments: Please right-click on the icon to open the file Incontinence Supplies State Specific Age Requirements List of State Specific Age Requirements UnitedHealthcare Community Plan Incontinence Supplies ICD-10 List of Required ICD-10 Incontinence Supplies Diagnosis Codes California Medicaid Incontinence Supplies ICD-10 List of Required California ICD-10 Incontinence Supplies Iowa Medicaid Incontinence Supplies ICD-10 List of Required Iowa ICD-10 Incontinence Supplies New York Medicaid Incontinence Supplies ICD-10 List of Required New York ICD-10 Incontinence Supplies UnitedHealthcare Community Plan HCPCS Group (1) Codes List of Group (1) Incontinence Supplies Codes UnitedHealthcare Community Plan HCPCS Group (2) Codes List of Group (2) Incontinence Supplies Codes Iowa Medicaid Incontinence Supplies Category and Combination Category Maximum Limits and Timeframes List of Iowa Category and Combination Category Maximum Limits and Timeframes Resources Individual state Medicaid regulations, manuals & fee schedules American Medical Association, Current Procedural Terminology ( CPT ) Professional Edition and associated publications and services Centers for Medicare and Medicaid Services, CMS Manual System and other CMS publications and services
6 Centers for Medicare and Medicaid Services, Healthcare Common Procedure Coding System, HCPCS Release and Code Sets History 2/18/2018 State Exceptions Section: added exception for Virginia state maximums 1/8/2018 Attachment Section: updated Iowa Category and Combination Category Maximum Limits and Timeframes to provider more clarity around the submission of combination codes B or C with D. 1/1/2018 1/1/2018: Annual Version Change History Section: Entries prior to 1/1/2015 were archived 11/15/2017 State Exceptions Section: Added max units exception for AZ LTC 11/12/2017 State Exceptions Section: Removed verbiage for Florida regarding documentation requirements that exceed the max units Attachment Section: Updated the state specific age requirements list (Texas from beginning age of 4 to beginning age of 3) 11/1/2017 Attachment Section: added Florida LTC and HCBS exclusions 10/12/2017 State Exceptions Section: Kansas diagnosis and age requirements added regarding Home Health Care Providers 10/4/2017 State Exceptions Section: Kansas exception updated for codes T4541 and T4542 8/27/2017 State Exceptions Section: Added exception for Virginia 7/21/2017 State Exceptions Section: Removed language regarding T4543 for New Mexico 7/15/2017 Application Section: Removed UnitedHealthcare Community Plan Medicare products as applying to this policy. Added location for UnitedHealthcare Community Plan Medicare reimbursement policies 7/2/2017 State Maximums updated for Kansas. State Exceptions Section: Added A4553 exception for Kansas 6/18/2017 State Exceptions Section: Added verbiage for Florida and Iowa regarding documentation requirements that exceed the max. Added HCPCS and limits for California Medicaid Attachment Section: Updated the California Medicaid Incontinence Supplies ICD-10 List 5/28/2017 Attachment Section: Updated state specific age requirements list for FL MMA (comprehensive) 5/20/2017 Reimbursement Guidelines Section: Added State specific age requirements language State Exceptions Section: Removed Florida and Missouri allowed ages Attachment Section: Added state specific age requirements list 4/9/2017 State Maximums Section: Updated Nebraska max units to 300 3/12/2017 Policy Approval Date Change (no new version) State Exceptions Section: Age requirements removed for Florida Long-Term Care (LTC) 2/28/2017 State Exceptions Section: Added documentation regarding age requirements and combined total units for Florida and Missouri. 2/11/2017 State Maximums for Group1/Group 2 HCPCS codes based on State: Added Maximum limit for Missouri
7 State Exceptions Section: Added exception for Florida and Missouri REIMBURSEMENT POLICY 1/1/2017 Annual Version Change Policy Verbiage Changes: Overview section updated to remove reference to ICD 9 CM State Exceptions Section: New Mexico Medicaid monthly limit language but not both was updated for Group (1) and Group (2) supplies. Attachments Section: Updated to remove Incontinence Supplies ICD-9-CM Codes List Added code A4553 to the UnitedHealthcare Community Plan HCPCS Group (2) Codes List History Section: Entries prior to 1/1/2015 archived. 11/13/2016 State Maximums Section: Updated New York Group 2 max units State Exceptions Section: Iowa Medicaid Diagnosis verbiage added. New York, updated max units for code A4554 Attachment Section: Added the Iowa Medicaid Incontinence Supplies ICD-10 Diagnosis Codes Lists. 10/2/2016 Attachment Section: Updated the Incontinence Supplies ICD-10 List 8/20/2016 Reimbursement Guidelines: ICD-10 Diagnosis Requirements Revised. State Exceptions Section: Added diagnosis verbiage for New York. Added exception for Pennsylvania. Attachment Section: Updated the Incontinence Supplies ICD-10 List, added the New York Medicaid Incontinence Supplies ICD-10 List. 5/21/2016 State Exceptions Section: Added secondary diagnosis requirement for California Added HCPCS Maximum and Combination Unit Limits for Arizona Attachment Section: Added Incontinence Supply ICD-9 List, Incontinence Supply ICD-10 List, California Incontinence Supply ICD-10 Diagnosis Codes List, Iowa Maximum and Combination Unit Limits Supplies List, HCPCS Incontinence Supply Group (1) and HCPCS Group (2) List Codes Section: Removed 4/7/2016 State Exceptions Section: Exception for Iowa Removed 3/14/2016 Annual Approval Date Change State Exception Section: Exception added for Pennsylvania 2/19/2016 State Exceptions Section Updated: Added the word Medicaid for Pennsylvania Codes ICD-10-CM Section Updated: Added the diagnosis descriptions 1/1/2016 Annual Policy Version Change State Exception: Added exception for California Entries Prior to 1/1/2014 archived 2/16/2013 Policy implemented by UnitedHealthcare Community & State Back to the top
Incontinence Supplies Policy, Professional
 Policy Number 2018R7111D Incontinence Supplies Policy, Professional Annual Approval Date 3/14/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for
Policy Number 2018R7111D Incontinence Supplies Policy, Professional Annual Approval Date 3/14/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for
Medically Unlikely Edits (MUE) Policy
 Medically Unlikely Edits (MUE) Policy Policy Number 2018R7117L Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Medically Unlikely Edits (MUE) Policy Policy Number 2018R7117L Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Co-Surgeon / Team Surgeon Policy
 Co-Surgeon / Team Surgeon Policy Policy Number 2018R0052C Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Co-Surgeon / Team Surgeon Policy Policy Number 2018R0052C Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Procedure to Place of Service Policy
 Procedure to Place of Service Policy REIMBURSEMENT POLICY Policy Number 2017R7108N Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
Procedure to Place of Service Policy REIMBURSEMENT POLICY Policy Number 2017R7108N Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
Procedure to Place of Service Policy, Professional
 Procedure to Place of Service Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R7108Q Annual Approval Date 3/8/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT
Procedure to Place of Service Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R7108Q Annual Approval Date 3/8/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT
Age to Diagnosis Code & Procedure Code Policy
 Age to Diagnosis Code & Procedure Code Policy Policy Number 2017R0086C Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee You are responsible for submission of accurate
Age to Diagnosis Code & Procedure Code Policy Policy Number 2017R0086C Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee You are responsible for submission of accurate
National Drug Code (NDC) Requirement Policy, Facility and Professional
 National Drug Code (NDC) Requirement Policy, Facility and Professional IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible for submission of accurate claims. This reimbursement policy is
National Drug Code (NDC) Requirement Policy, Facility and Professional IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible for submission of accurate claims. This reimbursement policy is
Unlisted Services Policy
 Policy Number 2018R7101G Annual Approval Date Unlisted Services Policy 11/11/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Policy Number 2018R7101G Annual Approval Date Unlisted Services Policy 11/11/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Procedure to Modifier Policy
 Policy Number 2018R0119D Annual Approval Date Procedure to Modifier Policy 3/08/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Policy Number 2018R0119D Annual Approval Date Procedure to Modifier Policy 3/08/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Physical Medicine & Rehabilitation: Multiple Therapy Procedure Reduction Policy
 Policy Number 2018R0121B Physical Medicine & Rehabilitation: Procedure Reduction Policy Annual Approval Date 3/08/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
Policy Number 2018R0121B Physical Medicine & Rehabilitation: Procedure Reduction Policy Annual Approval Date 3/08/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
Time Span Codes Policy, Professional
 Time Span Codes Policy, Professional Policy Number 2018R0102G Annual Approval Date 11/14/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are
Time Span Codes Policy, Professional Policy Number 2018R0102G Annual Approval Date 11/14/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are
Vaccines For Children Policy, Professional
 Policy Number 2018R7109L Vaccines For Children Policy, Professional Annual Approval Date 11/09/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for
Policy Number 2018R7109L Vaccines For Children Policy, Professional Annual Approval Date 11/09/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for
Facility Billing Policy
 Policy Number 2018F7007A Annual Approval Date Facility Billing Policy 3/8/2018 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible for submission
Policy Number 2018F7007A Annual Approval Date Facility Billing Policy 3/8/2018 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible for submission
Vaccines For Children Policy
 Policy Number 2017R7109P Annual Approval Date Vaccines For Children Policy 11/09/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of
Policy Number 2017R7109P Annual Approval Date Vaccines For Children Policy 11/09/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of
Adjunct Professional Services Policy
 Policy Number 2017R7114K Adjunct Professional Services Policy Annual Approval Date 11/9/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Policy Number 2017R7114K Adjunct Professional Services Policy Annual Approval Date 11/9/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Add-On Codes Policy. Approved By 7/12/2017
 Policy Number 2018R0071B Annual Approval Date Add-On Codes Policy 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate
Policy Number 2018R0071B Annual Approval Date Add-On Codes Policy 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate
One or More Sessions Policy
 One or More Sessions Policy Policy Number 2017R0118B Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
One or More Sessions Policy Policy Number 2017R0118B Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Adjunct Professional Services Policy
 Policy Number 2017R7114C Adjunct Professional Services Policy Annual Approval Date 11/9/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Policy Number 2017R7114C Adjunct Professional Services Policy Annual Approval Date 11/9/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Ambulance Policy. Approved By 7/12/2017
 Ambulance Policy Policy Number 2018R0123A Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate claims.
Ambulance Policy Policy Number 2018R0123A Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate claims.
Add-on Policy 7/13/2016
 Policy Number 2017R0071B Annual Approval Date Add-on Policy 7/13/2016 Approved By REIMBURSEMENT POLICY CMS-1500 Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are
Policy Number 2017R0071B Annual Approval Date Add-on Policy 7/13/2016 Approved By REIMBURSEMENT POLICY CMS-1500 Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are
Ambulance Policy, Professional
 Policy Number 2018R0123G Annual Approval Date Ambulance Policy, Professional 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Policy Number 2018R0123G Annual Approval Date Ambulance Policy, Professional 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are responsible
Durable Medical Equipment, Orthotics and Prosthetics Multiple Frequency Policy
 Durable Medical Equipment, Orthotics and Prosthetics Multiple Frequency Policy Policy Number 2018R0109H Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE
Durable Medical Equipment, Orthotics and Prosthetics Multiple Frequency Policy Policy Number 2018R0109H Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE
Multiple Procedure Payment Reduction (MPPR) for Diagnostic Imaging Policy, Professional
 Multiple Procedure Payment Reduction (MPPR) for Diagnostic Imaging Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R0085F Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight
Multiple Procedure Payment Reduction (MPPR) for Diagnostic Imaging Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R0085F Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight
Durable Medical Equipment, Orthotics and Prosthetics Multiple Frequency Policy
 Durable Medical Equipment, Orthotics and Prosthetics Multiple Frequency Policy Policy Number 2018R0109B Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE
Durable Medical Equipment, Orthotics and Prosthetics Multiple Frequency Policy Policy Number 2018R0109B Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE
Reimbursement Policy Subject: Emergency Services: Nonparticipating Providers and Facilities 07/29/13 05/01/17 Administration Policy
 Reimbursement Policy Subject: Emergency Services: Nonparticipating Providers and Facilities Committee Approval Obtained: Section: Effective Date: 07/29/13 05/01/17 Administration *****The most current
Reimbursement Policy Subject: Emergency Services: Nonparticipating Providers and Facilities Committee Approval Obtained: Section: Effective Date: 07/29/13 05/01/17 Administration *****The most current
Injection and Infusion Services Policy
 REIMBURSEMENT POLICY CMS-1500 Injection and Infusion Services Policy Policy Number 2018R0009A Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS
REIMBURSEMENT POLICY CMS-1500 Injection and Infusion Services Policy Policy Number 2018R0009A Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS
Multiple Procedure Policy
 Policy Policy Number 2018R0034C Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate claims. This
Policy Policy Number 2018R0034C Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate claims. This
Contrast and Radiopharmaceutical Materials Policy
 Contrast and Radiopharmaceutical Materials Policy Policy Number 2018R0104B Annual Approval Date 3/14/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible
Contrast and Radiopharmaceutical Materials Policy Policy Number 2018R0104B Annual Approval Date 3/14/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible
Contrast and Radiopharmaceutical Materials Policy
 Policy Number Contrast and Radiopharmaceutical Materials Policy 2017R0104B Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY
Policy Number Contrast and Radiopharmaceutical Materials Policy 2017R0104B Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY
Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy
 Policy Number Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy 2017R0125B Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight
Policy Number Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy 2017R0125B Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight
Bilateral Procedures Policy
 Bilateral Procedures Policy Policy Number 2018R0023B Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of
Bilateral Procedures Policy Policy Number 2018R0023B Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of
Maximum Frequency Per Day Policy
 Maximum Frequency Per Day Policy Policy Number 2018R0060H Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Maximum Frequency Per Day Policy Policy Number 2018R0060H Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
36 Million Without Health Insurance in 2014; Decreases in Uninsurance Between 2013 and 2014 Varied by State
 36 Million Without Health Insurance in 2014; Decreases in Uninsurance Between 2013 and 2014 Varied by State An estimated 36 million people in the United States had no health insurance in 2014, approximately
36 Million Without Health Insurance in 2014; Decreases in Uninsurance Between 2013 and 2014 Varied by State An estimated 36 million people in the United States had no health insurance in 2014, approximately
Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy Policy Number
 REIMBURSEMENT POLICY CMS-1500 Multiple Procedure Payment Reduction (MPPR) for and Ophthalmology Procedures Policy Policy Number 2018R0125B Annual Approval Date 3/14/2018 Approved By Reimbursement Policy
REIMBURSEMENT POLICY CMS-1500 Multiple Procedure Payment Reduction (MPPR) for and Ophthalmology Procedures Policy Policy Number 2018R0125B Annual Approval Date 3/14/2018 Approved By Reimbursement Policy
Multiple Procedure Payment Reduction (MPPR) for Diagnostic Imaging Policy, Professional
 Reimbursement Policy CMS 1500 Multiple Procedure Payment Reduction (MPPR) for Diagnostic Imaging Policy, Professional Policy Number 2019R0085A Annual Approval Date 7/11/2018 Approved By Reimbursement Policy
Reimbursement Policy CMS 1500 Multiple Procedure Payment Reduction (MPPR) for Diagnostic Imaging Policy, Professional Policy Number 2019R0085A Annual Approval Date 7/11/2018 Approved By Reimbursement Policy
IMPORTANT TAX INFORMATION
 IMPORTANT TAX INFORMATION To set up and maintain your account with WestconGroup, we require you to provide us valid Resale Certificates for all states that you are located in, as well as for any other
IMPORTANT TAX INFORMATION To set up and maintain your account with WestconGroup, we require you to provide us valid Resale Certificates for all states that you are located in, as well as for any other
STATE TAX WITHHOLDING GUIDELINES
 STATE TAX WITHHOLDING GUIDELINES ( Guardian Insurance & Annuity Company, Inc. and Guardian Life Insurance Company of America (hereafter collectively referred to as Company )) (Last Updated 11/2/215) state
STATE TAX WITHHOLDING GUIDELINES ( Guardian Insurance & Annuity Company, Inc. and Guardian Life Insurance Company of America (hereafter collectively referred to as Company )) (Last Updated 11/2/215) state
UnitedHealthcare Medicare Advantage Reimbursement Policy CMS 1500 Multiple Procedure Payment Reduction (MPPR) for Therapy Services Policy
 Multiple Procedure Payment Reduction (MPPR) for Therapy Services Policy Policy Number Annual Approval Date 3/14/2018 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This
Multiple Procedure Payment Reduction (MPPR) for Therapy Services Policy Policy Number Annual Approval Date 3/14/2018 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This
Age of Insured Discount
 A discount may apply based on the age of the insured. The age of each insured shall be calculated as the policyholder s age as of the last day of the calendar year. The age of the named insured in the
A discount may apply based on the age of the insured. The age of each insured shall be calculated as the policyholder s age as of the last day of the calendar year. The age of the named insured in the
Global Days Policy, Professional
 REIMBURSEMENT POLICY Global Days Policy, Professional Policy Number 2018R0005D Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
REIMBURSEMENT POLICY Global Days Policy, Professional Policy Number 2018R0005D Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
Aetna Medicare 2013 Benefits at a Glance
 Aetna Medicare 2013 Benefits at a Glance 58.40.366.1-CVSP A Aetna Medicare Rx (PDP) Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Hawaii, Illinois, Indiana,
Aetna Medicare 2013 Benefits at a Glance 58.40.366.1-CVSP A Aetna Medicare Rx (PDP) Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Hawaii, Illinois, Indiana,
medicaid a n d t h e How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief
 on medicaid a n d t h e uninsured July 2012 How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief Effective January 2014, the ACA establishes a new minimum Medicaid
on medicaid a n d t h e uninsured July 2012 How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief Effective January 2014, the ACA establishes a new minimum Medicaid
Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy Policy Number
 REIMBURSEMENT POLICY CMS-1500 Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy Policy Number 2018R0125A Annual Approval Date 3/14/2018 Approved
REIMBURSEMENT POLICY CMS-1500 Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy Policy Number 2018R0125A Annual Approval Date 3/14/2018 Approved
ACORD Forms Updated in AMS R1
 ACORD Forms Updated in AMS360 2017 R1 The following forms will use the ACORD form viewer, also new in this release. Forms with an indicate they were added because of requests in the Product Enhancement
ACORD Forms Updated in AMS360 2017 R1 The following forms will use the ACORD form viewer, also new in this release. Forms with an indicate they were added because of requests in the Product Enhancement
Installment Loans CHARTS. No cap other than unconscionability:
 NCLC NATIONAL CONSUMER LAW CENTER Installment Loans WILL STATES PROTECT BORROWERS FROM A NEW WAVE OF PREDATORY LENDING? Copyright 2015, National Consumer Law Center, Inc. CHARTS CHART 1 Full APRs Allowed
NCLC NATIONAL CONSUMER LAW CENTER Installment Loans WILL STATES PROTECT BORROWERS FROM A NEW WAVE OF PREDATORY LENDING? Copyright 2015, National Consumer Law Center, Inc. CHARTS CHART 1 Full APRs Allowed
Long-Term Care Partnership Overview & Training Requirements Guide
 Long-Term Care Insurance Mutual of Omaha Insurance Company SM Long-Term Care Partnership Overview & Training Requirements Guide 75014 Version November 16, 2015 For producer use only. Not for use with the
Long-Term Care Insurance Mutual of Omaha Insurance Company SM Long-Term Care Partnership Overview & Training Requirements Guide 75014 Version November 16, 2015 For producer use only. Not for use with the
Data Note: What if Per Enrollee Medicaid Spending Growth Had Been Limited to CPI-M from ?
 Data Note: What if Per Enrollee Medicaid Spending Growth Had Been Limited to CPI-M from 2001-2011? Rachel Garfield, Robin Rudowitz, and Katherine Young Congress is currently debating the American Health
Data Note: What if Per Enrollee Medicaid Spending Growth Had Been Limited to CPI-M from 2001-2011? Rachel Garfield, Robin Rudowitz, and Katherine Young Congress is currently debating the American Health
Long-Term Care Partnership Overview & Training Requirements Guide
 Long-Term Care Partnership Overview & Training Requirements Guide Version Sept. 12, 2012 M28108 Contents LONG-TERM CARE PARTNERSHIP OVERVIEW & TRAINING REQUIREMENTS GUIDE Long-Term Care Partnership Overview...4
Long-Term Care Partnership Overview & Training Requirements Guide Version Sept. 12, 2012 M28108 Contents LONG-TERM CARE PARTNERSHIP OVERVIEW & TRAINING REQUIREMENTS GUIDE Long-Term Care Partnership Overview...4
Multiple Procedure Payment Reduction (MPPR) for Medical and Surgical Services Policy, Professional
 REIMBURSEMENT POLICY CMS-1500 Multiple Payment Reduction (MPPR) for Medical and Surgical Services Policy, Professional Policy Number 2019R0034B Annual Approval Date 7/11/2018 Approved By Reimbursement
REIMBURSEMENT POLICY CMS-1500 Multiple Payment Reduction (MPPR) for Medical and Surgical Services Policy, Professional Policy Number 2019R0034B Annual Approval Date 7/11/2018 Approved By Reimbursement
CAH Financial Indicators Report: Summary of Indicator Medians by State
 Flex Monitoring Team Data Summary Report No. 26: CAH Financial Indicators Report: Summary of Indicator Medians by State March 2018 The Flex Monitoring Team is a consortium of the Rural Health Research
Flex Monitoring Team Data Summary Report No. 26: CAH Financial Indicators Report: Summary of Indicator Medians by State March 2018 The Flex Monitoring Team is a consortium of the Rural Health Research
WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES CLASSIC PLAN WITH LOWER PLAN PREMIUMS
 PR Contact: IR Contact: H. Patel Jeff Potter CKPR WellCare Health Plans, Inc. (312) 616-2471 (813) 290-6313 hpatel@ckpr.biz jeff.potter@wellcare.com WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES
PR Contact: IR Contact: H. Patel Jeff Potter CKPR WellCare Health Plans, Inc. (312) 616-2471 (813) 290-6313 hpatel@ckpr.biz jeff.potter@wellcare.com WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES
Comparative Revenues and Revenue Forecasts Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas
 Comparative Revenues and Revenue Forecasts 2010-2014 Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas Comparative Revenues and Revenue Forecasts This data shows tax
Comparative Revenues and Revenue Forecasts 2010-2014 Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas Comparative Revenues and Revenue Forecasts This data shows tax
ACORD Forms in ebixasp (03/2004)
 ACORD Forms in ebixasp (03/2004) Form number Form Name Edition Date 1 Property Loss Notice 2002/1 2 Automobile Loss Notice 2002/1 3 General Liability Notice of Occurrence/Claim 2002/1 4 Workers Compensation
ACORD Forms in ebixasp (03/2004) Form number Form Name Edition Date 1 Property Loss Notice 2002/1 2 Automobile Loss Notice 2002/1 3 General Liability Notice of Occurrence/Claim 2002/1 4 Workers Compensation
CAH Financial Indicators Report: Summary of Indicator Medians by State
 Flex Monitoring Team Data Summary Report No. 18: : Summary of Indicator Medians by State March 2016 The Flex Monitoring Team is a consortium of the Rural Health Research Centers located at the Universities
Flex Monitoring Team Data Summary Report No. 18: : Summary of Indicator Medians by State March 2016 The Flex Monitoring Team is a consortium of the Rural Health Research Centers located at the Universities
Multiple Procedure Payment Reduction (MPPR) for Surgical Procedures
 Policy Number MPS04242013RP Approved By UnitedHealthcare Medicare Committee Current Approval Date 03/26/2014 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare
Policy Number MPS04242013RP Approved By UnitedHealthcare Medicare Committee Current Approval Date 03/26/2014 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare
NCSL Midwest States Fiscal Leaders Forum. March 10, 2017
 NCSL Midwest States Fiscal Leaders Forum March 10, 2017 Public Pensions: 50-State Overview David Draine, Senior Officer Public Sector Retirement Systems Project The Pew Charitable Trusts More than 40 active,
NCSL Midwest States Fiscal Leaders Forum March 10, 2017 Public Pensions: 50-State Overview David Draine, Senior Officer Public Sector Retirement Systems Project The Pew Charitable Trusts More than 40 active,
Bilateral Procedures Policy Annual Approval Date
 Reimbursement Policy CMS 1500 Policy Number 2018R0023A Bilateral Procedures Policy Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
Reimbursement Policy CMS 1500 Policy Number 2018R0023A Bilateral Procedures Policy Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
2014 SUMMARY OF BENEFITS
 2014 SUMMARY OF BENEFITS First Health Part D Value Plus (PDP) Prescription Drug Plan S5569, S5768 Y0022_PDP_2014_S5569_S5768_SB accepted SECTION I INTRODUCTION TO SUMMARY OF BENEFITS Thank you for your
2014 SUMMARY OF BENEFITS First Health Part D Value Plus (PDP) Prescription Drug Plan S5569, S5768 Y0022_PDP_2014_S5569_S5768_SB accepted SECTION I INTRODUCTION TO SUMMARY OF BENEFITS Thank you for your
Household Income for States: 2010 and 2011
 Household Income for States: 2010 and 2011 American Community Survey Briefs By Amanda Noss Issued September 2012 ACSBR/11-02 INTRODUCTION Estimates from the 2010 American Community Survey (ACS) and the
Household Income for States: 2010 and 2011 American Community Survey Briefs By Amanda Noss Issued September 2012 ACSBR/11-02 INTRODUCTION Estimates from the 2010 American Community Survey (ACS) and the
2017 WORKBOOK. Mandatory LTC Training
 2017 WORKBOOK Mandatory LTC Training ABOUT THE AUTHOR EDUCATION CREDIT AND YOUR CERTIFICATE OF COMPLETION LTC Connection specializes exclusively in LTC insurance training and education and has been working
2017 WORKBOOK Mandatory LTC Training ABOUT THE AUTHOR EDUCATION CREDIT AND YOUR CERTIFICATE OF COMPLETION LTC Connection specializes exclusively in LTC insurance training and education and has been working
NCCI Research Workers Compensation and Prescription Drugs 2016 Update
 NCCI Research Workers Compensation and Prescription Drugs 2016 Update By Barry Lipton, FCAS, MAAA, Practice Leader and Senior Actuary, NCCI David Colón, ACAS, MAAA, Associate Actuary, NCCI Introduction
NCCI Research Workers Compensation and Prescription Drugs 2016 Update By Barry Lipton, FCAS, MAAA, Practice Leader and Senior Actuary, NCCI David Colón, ACAS, MAAA, Associate Actuary, NCCI Introduction
Medically Unlikely Edits Policy
 Medically Unlikely Edits Policy Policy Number Annual Approval Date 1/13/2017 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare
Medically Unlikely Edits Policy Policy Number Annual Approval Date 1/13/2017 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare
Reimbursement Policy Subject: Claims Timely Filing 07/01/13 06/05/17 Administration Policy
 Reimbursement Policy Subject: Claims Timely Filing Committee Approval Obtained: Section: Effective Date: 07/01/13 06/05/17 Administration *****The most current version of the Reimbursement Policies can
Reimbursement Policy Subject: Claims Timely Filing Committee Approval Obtained: Section: Effective Date: 07/01/13 06/05/17 Administration *****The most current version of the Reimbursement Policies can
JH Insurance Licensing Guide
 JH Insurance Licensing Guide Insurance policies and/or associated riders and features may not be available in all states. Life insurance is underwritten by John Hancock Life Insurance Company (U.S.A.),
JH Insurance Licensing Guide Insurance policies and/or associated riders and features may not be available in all states. Life insurance is underwritten by John Hancock Life Insurance Company (U.S.A.),
Highlights. Percent of States with a Decrease in MH Expenditures from Prior Year: FY2001 to 2010
 FY 2010 State Mental Health Revenues and Expenditures Information from the National Association of State Mental Health Program Directors Research Institute, Inc (NRI) Sept 2012 Highlights SMHA Funding
FY 2010 State Mental Health Revenues and Expenditures Information from the National Association of State Mental Health Program Directors Research Institute, Inc (NRI) Sept 2012 Highlights SMHA Funding
Long-Term Care Education Requirements Prior to Selling
 for Training AK All Health 8 hrs 4 hrs 24 months AL All Accident & Health 8 hrs 4 hrs Renewal deadline is the date the license expires. s are renewed biennially based on agent's birth month and year. AR
for Training AK All Health 8 hrs 4 hrs 24 months AL All Accident & Health 8 hrs 4 hrs Renewal deadline is the date the license expires. s are renewed biennially based on agent's birth month and year. AR
Health Insurance Price Index for October-December February 2014
 Health Insurance Price Index for October-December 2013 February 2014 ehealth 2.2014 Table of Contents Introduction... 3 Executive Summary and Highlights... 4 Nationwide Health Insurance Costs National
Health Insurance Price Index for October-December 2013 February 2014 ehealth 2.2014 Table of Contents Introduction... 3 Executive Summary and Highlights... 4 Nationwide Health Insurance Costs National
Long-Term Care Education Requirements Prior to Selling
 for AK All Health 8 hrs 4 hrs 24 months AL All Accident & Health 8 hrs 4 hrs Renewal deadline is the date the license expires. s are renewed biennially based on agent's birth month and year. AR All Accident,
for AK All Health 8 hrs 4 hrs 24 months AL All Accident & Health 8 hrs 4 hrs Renewal deadline is the date the license expires. s are renewed biennially based on agent's birth month and year. AR All Accident,
kaiser medicaid and the uninsured commission on The Cost and Coverage Implications of the ACA Medicaid Expansion: National and State-by-State Analysis
 kaiser commission on medicaid and the uninsured The Cost and Coverage Implications of the ACA Expansion: National and State-by-State Analysis Executive Summary John Holahan, Matthew Buettgens, Caitlin
kaiser commission on medicaid and the uninsured The Cost and Coverage Implications of the ACA Expansion: National and State-by-State Analysis Executive Summary John Holahan, Matthew Buettgens, Caitlin
Continuing Education
 Continuing Education FROM: PGI PHONE: (800) 829-7247 FAX: (317) 549-9470 Thanks for your interest in continuing education through Pentera Group, Inc. (PGI). Attached please find information on PGI courses
Continuing Education FROM: PGI PHONE: (800) 829-7247 FAX: (317) 549-9470 Thanks for your interest in continuing education through Pentera Group, Inc. (PGI). Attached please find information on PGI courses
Update: 50-State Survey of Retiree Health Care Liabilities Most recent data show changes to benefits, funding policies could help manage rising costs
 A fact sheet from Dec 2018 Update: 50-State Survey of Retiree Health Care Liabilities Most recent data show changes to benefits, funding policies could help manage rising costs Getty Images Overview States
A fact sheet from Dec 2018 Update: 50-State Survey of Retiree Health Care Liabilities Most recent data show changes to benefits, funding policies could help manage rising costs Getty Images Overview States
BY THE NUMBERS 2016: Another Lackluster Year for State Tax Revenue
 BY THE NUMBERS 2016: Another Lackluster Year for State Tax Revenue Jim Malatras May 2017 Lucy Dadayan and Donald J. Boyd 2016: Another Lackluster Year for State Tax Revenue Lucy Dadayan and Donald J. Boyd
BY THE NUMBERS 2016: Another Lackluster Year for State Tax Revenue Jim Malatras May 2017 Lucy Dadayan and Donald J. Boyd 2016: Another Lackluster Year for State Tax Revenue Lucy Dadayan and Donald J. Boyd
Rebundling and NCCI Editing
 Policy Number CCR10082014RP Rebundling and NCCI Editing Approved By UnitedHealthcare Medicare Committee Current Approval Date 10/08/2014 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable
Policy Number CCR10082014RP Rebundling and NCCI Editing Approved By UnitedHealthcare Medicare Committee Current Approval Date 10/08/2014 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable
Table PDENT-CH (continued) This measure identifies the percentage of children ages 1 to 20 who are covered by Medicaid or CHIP Medicaid Expansion
 Table PDENT-CH. Percentage of Eligibles Ages 1 to 20 who Received Preventive Dental Services, as Submitted by States for the FFY 2016 Form CMS-416 Report (n = 50 states) State Denominator Rate State Mean
Table PDENT-CH. Percentage of Eligibles Ages 1 to 20 who Received Preventive Dental Services, as Submitted by States for the FFY 2016 Form CMS-416 Report (n = 50 states) State Denominator Rate State Mean
American Memorial Contract
 American Memorial Contract Please complete all pages of the contract and send it back to Stephens- Matthews with a copy of each state license you choose to appoint in. You are required to submit with the
American Memorial Contract Please complete all pages of the contract and send it back to Stephens- Matthews with a copy of each state license you choose to appoint in. You are required to submit with the
Application Trade Credit Insurance Multi Buyer
 Chubb Global Markets Political Risk & Credit 1133 Avenue of the Americas New York, NY 10036 (212) 835-3138 (NY) (312) 612-8827 (Chicago) (213) 612-5512 (Los Angeles) Application Trade Credit Insurance
Chubb Global Markets Political Risk & Credit 1133 Avenue of the Americas New York, NY 10036 (212) 835-3138 (NY) (312) 612-8827 (Chicago) (213) 612-5512 (Los Angeles) Application Trade Credit Insurance
How Quickly are States Connecting Applicants to Medicaid and CHIP Coverage?
 January 019 Issue Brief How Quickly are States Connecting Applicants to Medicaid and CHIP Coverage? Samantha Artiga and Maria Diaz Summary In November 018, the Centers for Medicare and Medicaid Services
January 019 Issue Brief How Quickly are States Connecting Applicants to Medicaid and CHIP Coverage? Samantha Artiga and Maria Diaz Summary In November 018, the Centers for Medicare and Medicaid Services
Frequently Asked Questions on Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS) 2015 Medicare Payment Final Rules (CMS-1614-F)
 Frequently Asked Questions on Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS) 2015 Medicare Payment Final Rules (CMS-1614-F) Adjusting DMEPOS Payment Amounts Using Competitive
Frequently Asked Questions on Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS) 2015 Medicare Payment Final Rules (CMS-1614-F) Adjusting DMEPOS Payment Amounts Using Competitive
Required Minimum Distribution Election Form for IRA s, 403(b)/TSA and other Qualified Plans
 Required Minimum Distribution Election Form for IRA s, 403(b)/TSA and other Qualified Plans For Policyholders who have not annuitized their deferred annuity contracts Zurich American Life Insurance Company
Required Minimum Distribution Election Form for IRA s, 403(b)/TSA and other Qualified Plans For Policyholders who have not annuitized their deferred annuity contracts Zurich American Life Insurance Company
Professional/Technical Component Policy, Professional
 Professional/Technical Component Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R0012F Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT
Professional/Technical Component Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R0012F Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT
Medically Unlikely Edits (MUE)
 Policy Number MUE10012009RP Medically Unlikely Edits (MUE) Approved By UnitedHealthcare Medicare Committee Current Approval Date 09/11/2013 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is
Policy Number MUE10012009RP Medically Unlikely Edits (MUE) Approved By UnitedHealthcare Medicare Committee Current Approval Date 09/11/2013 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is
Other Payer Advanced APMs in the Quality Payment Program for Performance Year 2019
 Other Payer Advanced APMs in the Quality Payment Program for Performance Year 2019 Under the Quality Payment Program s All-Payer Combination Option, State Medicaid Agencies, Medicare Advantage and other
Other Payer Advanced APMs in the Quality Payment Program for Performance Year 2019 Under the Quality Payment Program s All-Payer Combination Option, State Medicaid Agencies, Medicare Advantage and other
State, Local and Net Tuition Revenue Supporting General Operating Expenses of Higher Education, U.S., Fiscal Year 2010, Current (unadjusted) Dollars
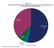 State, Local and Net Tuition Revenue Supporting General Operating Expenses of Higher Education, U.S., Fiscal Year 2010, Current (unadjusted) Dollars Net Tuition $51.3 Billion 37% All State Support $73.7
State, Local and Net Tuition Revenue Supporting General Operating Expenses of Higher Education, U.S., Fiscal Year 2010, Current (unadjusted) Dollars Net Tuition $51.3 Billion 37% All State Support $73.7
Non-Financial Change Form
 Non-Financial Change Form Please Print All Information Below Section 1. Contract Owner s Information Administrative Offices: PO BOX 19097 Greenville, SC 29602-9097 Phone number (800) 449-0523 Overnight
Non-Financial Change Form Please Print All Information Below Section 1. Contract Owner s Information Administrative Offices: PO BOX 19097 Greenville, SC 29602-9097 Phone number (800) 449-0523 Overnight
Final Paycheck Laws by State
 ALABAMA AL No Provision No Provision ALASKA AK 23.05.140(b) ARIZONA AZ Ariz. Rev. Stat. 23-350, 23-353 ARKANSAS AR Ark. Code Ann. 11-4-405 CALIFORNIA CA Cal. Lab. Code 201 to 202, 227.3 COLORADO CO Colo.
ALABAMA AL No Provision No Provision ALASKA AK 23.05.140(b) ARIZONA AZ Ariz. Rev. Stat. 23-350, 23-353 ARKANSAS AR Ark. Code Ann. 11-4-405 CALIFORNIA CA Cal. Lab. Code 201 to 202, 227.3 COLORADO CO Colo.
Basics of Medical Data Call Reporting Requirements. Objectives
 Basics of Medical Data Call Reporting Requirements Presented by: Grace Arrieche, Kristin Champagne, and Bob Vaughan 1 Objectives Review the basic business and reporting rules for reporting medical data
Basics of Medical Data Call Reporting Requirements Presented by: Grace Arrieche, Kristin Champagne, and Bob Vaughan 1 Objectives Review the basic business and reporting rules for reporting medical data
Health Reform & Immuniza3ons in 2014
 Health Reform & Immuniza3ons in 2014 Associa(on of Immuniza(on Managers Atlanta, Georgia Alexandra Stewart stewarta@gwu.edu Milken Ins(tute, School of Public Health, Department of Health Policy, GWU July
Health Reform & Immuniza3ons in 2014 Associa(on of Immuniza(on Managers Atlanta, Georgia Alexandra Stewart stewarta@gwu.edu Milken Ins(tute, School of Public Health, Department of Health Policy, GWU July
Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications
 Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications June 28, 2012 Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy In a 5-4 Decision,
Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications June 28, 2012 Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy In a 5-4 Decision,
Medicaid & CHIP: February 2014 Monthly Applications, Eligibility Determinations, and Enrollment Report April 4, 2014
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-26-12 Baltimore, Maryland 21244-1850 Medicaid & CHIP: February 2014 Monthly Applications,
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-26-12 Baltimore, Maryland 21244-1850 Medicaid & CHIP: February 2014 Monthly Applications,
Durable Medical Equipment, Orthotics and Prosthetics Policy, Professional
 Reimbursement Policy CMS 1500 Durable Medical Equipment, Orthotics and Prosthetics Policy, Professional Policy Number 2018R0109C Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight
Reimbursement Policy CMS 1500 Durable Medical Equipment, Orthotics and Prosthetics Policy, Professional Policy Number 2018R0109C Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight
State Retiree Health Care Liabilities: An Update Increased obligations in 2015 mirrored rise in overall health care costs
 A brief from Sept 207 State Retiree Health Care Liabilities: An Update Increased obligations in 205 mirrored rise in overall health care costs Overview States paid a total of $20.8 billion in 205 for nonpension
A brief from Sept 207 State Retiree Health Care Liabilities: An Update Increased obligations in 205 mirrored rise in overall health care costs Overview States paid a total of $20.8 billion in 205 for nonpension
Intensity Modulated Radiation Therapy Policy
 Policy Number 2017R0130D Intensity Modulated Radiation Therapy Policy Annual Approval Date 2/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You
Policy Number 2017R0130D Intensity Modulated Radiation Therapy Policy Annual Approval Date 2/8/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You
Insufficient and Negative Equity
 Insufficient and Negative Equity Lack Of Equity Impedes The Real Estate Market Mark Fleming Chief Economist December, 2011 70% 60% 50% 40% 30% Negative Equity Highly Concentrated Negative Equity Share,
Insufficient and Negative Equity Lack Of Equity Impedes The Real Estate Market Mark Fleming Chief Economist December, 2011 70% 60% 50% 40% 30% Negative Equity Highly Concentrated Negative Equity Share,
Medically Unlikely Edits (MUE)
 Policy Number MUE10012009RP Medically Unlikely Edits (MUE) Approved By UnitedHealthcare Medicare Committee Current Approval Date 04/13/2016 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is
Policy Number MUE10012009RP Medically Unlikely Edits (MUE) Approved By UnitedHealthcare Medicare Committee Current Approval Date 04/13/2016 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is
Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
MARKET TRENDS: MEDICARE SUPPLEMENT. Gorman Health Group, LLC
 MARKET TRENDS: MEDICARE SUPPLEMENT Gorman Health Group, LLC Issued: December 1, 2016 TABLE OF CONTENTS EXECUTIVE SUMMARY... 3 OVERALL TRENDS IN MEDICARE SUPPLEMENT ENROLLMENT... 4 NATIONWIDE ENROLLMENT...
MARKET TRENDS: MEDICARE SUPPLEMENT Gorman Health Group, LLC Issued: December 1, 2016 TABLE OF CONTENTS EXECUTIVE SUMMARY... 3 OVERALL TRENDS IN MEDICARE SUPPLEMENT ENROLLMENT... 4 NATIONWIDE ENROLLMENT...
LIFE AND ACCIDENT AND HEALTH
 201 FOR THE YEAR ENDED DECEMBER 1, 201 LIFE AND ACCIDENT AND HEALTH 201 Schedule A - Part 1 - Real Estate Owned Schedule A - Part 2 - Real Estate Acquired and Additions Made Schedule A - Part - Real Estate
201 FOR THE YEAR ENDED DECEMBER 1, 201 LIFE AND ACCIDENT AND HEALTH 201 Schedule A - Part 1 - Real Estate Owned Schedule A - Part 2 - Real Estate Acquired and Additions Made Schedule A - Part - Real Estate
Systematic Distribution Form
 Systematic Distribution Form (To be used for all Qualified Plans, IRA s and Non-Qualified Plans) (This form is not applicable to a Required Minimum Distribution ( RMD ). If you are older than 70 ½, refer
Systematic Distribution Form (To be used for all Qualified Plans, IRA s and Non-Qualified Plans) (This form is not applicable to a Required Minimum Distribution ( RMD ). If you are older than 70 ½, refer
Projected Savings of Medicaid Capitated Care: National and State-by-State. October 2015
 Projected Savings of Medicaid Capitated Care: National and State-by-State October 2015 I. Executive Summary We were asked by the Association for Community Affiliated Plans (ACAP) to estimate the Medicaid
Projected Savings of Medicaid Capitated Care: National and State-by-State October 2015 I. Executive Summary We were asked by the Association for Community Affiliated Plans (ACAP) to estimate the Medicaid
University of Wisconsin System SFS Business Process AP /1042s/Tax Bolt-On
 Contents 1099/1042-S Tax Bolt-On Process Overview... 1 Process Detail... 2 I. Search/Update for Existing Value 1099 / 1042 Records on the Bolt-On table... 2 II. Enter a New 1099/1042s records into the
Contents 1099/1042-S Tax Bolt-On Process Overview... 1 Process Detail... 2 I. Search/Update for Existing Value 1099 / 1042 Records on the Bolt-On table... 2 II. Enter a New 1099/1042s records into the
