Population Health: Moving Beyond ACOs
|
|
|
- Maud Patterson
- 5 years ago
- Views:
Transcription
1 Population Health: Moving Beyond ACOs Martin Hickey Michael Nugent Robert Henkle March 2, 2015 Executive Summit 1
2 Just what is Population Health The health outcomes of a group of individuals Health accountability for a defined group What defines the group? The group Geography The payor The hospital / system Defined borders In and out freedoms A group of providers / physicians Primary Care Specialty A disease or procedure 2
3 What happened to the Individual? including the distribution of such outcomes within the group Doctor / Patient relationship We all die Outcomes add significance to accountabilities 3
4 IHI Population Health Composite Model 4
5 Its not about the Money!... IT S ABOUT THE MONEY!!! 5
6 Healthcare Reform: Jumping the S Curves A Value Heads in Beds B Tough to go from Volume/ FFS to Capitation/Value 6
7 ACA Health Care reform Insurance reform? Health Cost reform? 7
8 Healthcare The Blood on the floor is yours! PAIN CHANGE OR No change without changing incentives! 8
9 Taking Risk for Population Health (Group) Reverses volume incentives Focus on health, not volume Results in Improved Health Status Reduces hospital admissions / readmissions / ER visits Reduced Costs = Increased Margins EBITDA can double under risk 9
10 Key Population Health Actions Group definition and premium portion at risk Physicians on salaries Primary care base Data analytics on outcomes, cost, physicians, episode treatment groups patients Predictive modeling Case / care management Focus on Behavioral Health Community Health Workers Transitions in care 10
11 New Mexico Health Connections ACA Health Plan Cooperative Fully at risk Analytics and Medical Management double down Behavioral Health Community Health Workers Full physician practice cost and outcomes internally transparent to physicians 11
12 NMHC 2014 Results Robin Hood Admissions / 1, vs 54 benchmark Readmissions 5.2 vs 12 benchmark MLR 73% Mount Auburn Cambridge IPA Primary Care Shared Savings to large group full risk delegation Primary Care W-2 goal in 2018 is $350,000 12
13 Ascension s Journey to Value-Based Care and Population Health Robert J. Henkel, FACHE President and Chief Executive Officer, Ascension Health Executive Vice President, Ascension
14 OUR VISION CALLS US TO STRENGTHEN THE CATHOLIC HEALTH MINISTRY OUR MISSION Rooted in the loving ministry of Jesus as healer, we commit ourselves to serving all persons with special attention to those who are poor and vulnerable. Our Catholic health ministry is dedicated to spiritually centered, holistic care which sustains and improves the health of individuals and communities. We are advocates for a compassionate and just society through our actions and our words. OUR VISION We envision a strong, vibrant Catholic health ministry in the United States which will lead to the transformation of healthcare. We will ensure service that is committed to health and well-being for our communities and that responds to the needs of individuals throughout the life cycle. We will expand the role of the laity, in both leadership and sponsorship, to ensure a Catholic health ministry of the future. OUR VALUES Service of the Poor Generosity of spirit, especially for persons most in need Reverence Respect and compassion for the dignity of diversity of life Integrity Inspiring trust through personal leadership Wisdom Integrating excellence and stewardship Creativity Courageous innovation Dedication Affirming the hope and joy of our ministry 14
15 ASCENSION HEALTH FOOTPRINT Ascension is the largest Catholic health system, the largest private nonprofit system and the second largest system (based on revenues) in the United States, operating in 23 states and the District of Columbia. 1515
16 Approach to Population Health A key strategic priority for Ascension is to create clinically integrated systems of care in our markets that enable us to deliver on the Quadruple Aim improved health outcomes, improved experience for those we serve, and improved experience for providers, at a lower overall cost of care Ascension is building the internal capabilities to enable value-based care in order to manage the health and well being of the populations we serve. Building regionally-based clinically integrated systems of care to manage Medicare, Medicaid, Exchange, and Commercial populations, as well as our associates Assembling capabilities in network development/management and innovative approaches to care management Developing a central risk function to manage and pool risk Creating a System-wide enterprise architecture to support delivery of fee-for-value models Ascension markets are moving at different paces to population health business models and risk-based contracting - this provides Ascension with an opportunity to rapidly test capabilities/approaches in certain markets, learn from these pilots and replicate best practices across the System 16
17 Ascension is Developing Capabilities to Take on Greater Risk Spectrum of Risk Increasing coordination, commitment, and provider risk Provider Payer Provide care to population as part of a broader provider network Create a narrow network product with a health plan Partner with a plan using a shared savings approach Enter a capitated risk arrangement with a plan partner Form a JV and private label a plan with a health plan partner Own/operate a health plan Required Capabilities Network Development / Management Capabilities Care / Medical Management Capabilities Risk Management & Reimbursement Optimization Capabilities Back Office Capabilities Sales and Marketing Capabilities IT Capabilities 17
18 MissionPoint Health Partners Innovative Model for Network Development and Care Management MissionPoint directly designs, and builds provider networks, deploys health partners who call on patients in the hospital or in their homes, and further supports any additional needs members have to live well and flourish in their community. MissionPoint s clients include integrated health systems, payers and large employers (i.e. entities that have historically organized and taken risk for populations). In addition to care management solutions and narrow network development, MissionPoint provides a unique set of products and services directly to employers and payers such as complex case management, onsite clinics, and a suite of wellness services. 18
19 MissionPoint Custom Network Design Per Member Per Month Payment Shared Savings Pool Additional Physician Incentives Extended Weekday Hours Open Saturdays Open Sundays with Patients Comprehensive Medication Review Medical Home Internal Medicine Family Practice Pediatrics Specialists Outpatient Facilities Inpatient Facilities MissionPoint Provider Network MissionPoint Member Population Identification and Stratification Care at a Distance Personal Care Team Wellness Partners and Services MissionPoint Health Partners 19
20 Creating Value for the Ecosystem Payer TPA Pays Claims and Network Service Fee Provides Shared Savings Option Self- Insured Employer Options During Open Enrollment Employee Preferred Network (MPHP) Clinically Integrated Network Open Access Dedicated Medical Home Low Co-Pay Levels Leveling Monthly Premiums Coordinated Patient Record Deep Wellness Support Employee Selects Medical Home Primary Care Physician Specialty C Specialty A Specialty B Specialty Care In-Network Narrow Network Higher Co-Pay Levels Rising Monthly Premiums Wellness Support Employee/ Member MissionPoint Health Partner Out-of-Network Open Network Highest Co-Pay/Co-Insurance Levels High Monthly Premiums Low Coordination Little Wellness Support Partner B Partner C Partner A Alliance Network 20 20
21 21 MissionPoint Strategic Approach
22 MissionPoint Approach to Managing Patient Risk Patient Data Maximized to Guide Effective Interactions Benefit Design Steers Members Towards Optimal Use of MissionPoint Network High-Cost Patients Rising-Risk Patients Prioritize Highest Risk Members: Immediately deploy Health Partners to patients during trigger events At-Risk Patients Target Members Showing Warning Signs: Track future risk scores and population trends for pro-active Health Partner engagement Healthy Patients Create Opportunities Across Members: Leverage highly effective, low cost screenings and preventative care for optimal health outcomes across members 22
23 MissionPoint Health Partner Solutions Diverse Focus Areas Addressed on Three Health Partner Teams Patient Connects to Health Partner: Physician Referral Self Referral Hospital Discharge ED Visit Transitional Hospital Discharge Long-term Care Skilled Care Home Visits Ambulatory ED Disease Management Wellness Office Based Presence Integrated Care Psychosocial Needs Life Resources Family Resources Behavioral Adaptation 23
24 24 MissionPoint Performance: Self-Insured Population
25 MissionPoint Performance: MSSP MSSP Comparison of Calendar Year 2012 to Calendar Year 2013 Inpatient Cost per Beneficiary Outpatient Cost per Beneficiary Post-Acute Cost per Beneficiary* 32.33% of Total Spend {2013} 16.71% of Total Spend {2013} 17.48% of Total Spend {2013} $3, $2, $1, $1, $2, $1, % % decrease from 2012 to 2013 All MSSP ACO Average Change: +0.19% % % increase from 2012 to 2013 All MSSP ACO Average Change: +7.37% % % decrease from 2012 to 2013 All MSSP ACO Average Change: +2.35% The remainder of spend is comprised of Part B Physician/ Supplier (30.59%) and Durable Medical Equipment (2.89%). * Post-Acute Cost includes Skilled Nursing Facility, Home Health, and Hospice 25
26 MissionPoint Performance: MSSP (continued) MSSP Comparison of Calendar Year 2012 to Calendar Year 2013 Hospitalizations per 1, % % decrease from 2012 to 2013 All MSSP ACO Average Change: -3.69% ED Visits per 1, % % decrease from 2012 to 2013 All MSSP ACO Average Change: 0.00% Primary Care Visits per 1,000 8, , % % increase from 2012 to 2013 All MSSP ACO Average Change: +3.24% 30-Day All-Cause Readmissions 15.99% % % % decrease from 2012 to 2013 All MSSP ACO Average Change: -3.23% 30-Day Post-Discharge Provider Visits Per 1,000 Discharges % % decrease from 2012 to 2013 All MSSP ACO Average Change: +1.79% 26
27 Ascension Risk Services DEGREE OF INSURANCE RISK ASSUMED CURRENT PROGRAMS Professional and General Liability (PGL) Program Workers Compensation and Associate Safety Certitude Independent Physician Program Commercially insured auto, property, Directors & Officers (D&O) OPPORTUNITIES / AREAS OF EXPERTISE Claims Management Loss Prevention Accountable Care Organization (ACO) Management Risk Employer/Provider Stop Loss INSURE NEW RISKS New Ascension business risk (e.g. Ascension Investment Management, The Resource Group, SmartHealth) Additional coverage lines (e.g. Catastrophic Medical Risk, ACO Management Risk, D&O, Technology) 3rd party health system risks SCOPE OF SERVICES / SOLUTIONS OFFERED 27
28 Ascension Clinical Holdings: Provision of Services to Support a Clinician Alignment Strategy Provide physician services that offer a compelling value proposition for employed and strategic partners. Offer a portfolio of needed services to physician practices to enable more cost effective practice management while better positioning them to participate as a preferred network. Initial offering includes Practice Management and Electronic Medical Record Additional offerings include Certitude (medical malpractice coverage) and The Resource Group (GPO) Ascension Employed Physicians Affiliated Providers 28
29 Improving Physician Practice Quality & Financial Performance Alignment with a national physician group, focused on high quality, patient centric care - Seamless integration with an existing, installed base in-market - Connection to networked ecosystem - Participation in care networks More time to care for patients - Reduced administrative burden - Less time managing vendors Improved bottom line - Improve the rate of collection - Avoid costly software implementation - Expenses incurred in administrative tasks Retained independence 29
30 Ascension Provider Enterprise A high performing medical group which unites a community of providers employed across Ascension through a common culture that fosters personcentered care as the central principle. The Ascension Provider Organization develops physician leaders and communities of providers and empowers them to assure a focus on the quadruple aim of: 1. Improved health outcomes 2. Enhanced patient experience 3. Excellent provider experience 4. The lowest overall cost of care We envision: Every regional medical group is a corporation that is a subsidiary of Ascension Provider Organization or Ascension Medical Group. Regional groups are each governed by an interdisciplinary management board focused on quality, service, the provider experience, the cost of care and the sustainability of the provider organization. 30
31 AESA Conceptual View Interaction Services and Business Core Capabilities Business Services Data Services and Master Data Sources Attributes A delivery framework Platform Agnostic Technology Agnostic Application Agnostic Vendor Agnostic Scalable Supports Current and Future Business Needs Enabled By Enterprise Architecture Framework Application Architecture & Portfolio Management Service Management & Governance Data Management & Governance 31
32 Financial Models 32
33 Introduction Martin defined population health and its velocity Bob provided deep insights into population health operating model/capabilities Now I will focus what makes a successful population health financial model Financial formula Financial operations Biography Actuarial roots, evolved into advisor to payer & provider executives committed to operationalizing the decisions/changes necessary to succeed Co-author of industry s top selling ACO book published by American College of Healthcare Executives 33
34 Thesis There are 2 primary financial decisions required to create a successful financial model Financial formula, defined in terms of sources and uses of shared savings and shared risk proceeds Ongoing financial management people & process model But there is one CEO/Executive Team decision that even the best financial model/cfo cannot fix without the help of clinicians and operators Organizational structure & operating model design 34
35 Organizational Structure & Operating Model Design The organizational structure and operating model need to be designed to minimize barriers/politics that physicians, hospitals and insurers encounter when operating under a shared savings or shared risk payment model Symptoms of potential problems Managed care team signs $750M risk contract and the health system loses $75M in 12 months Medical management resources / costs quadruple among the hospital, medical group, clinically integrated network and payer(s), without a common Care Model Blueprint, frustrating patients and physicians Bonuses never get to those that do the work The Population Health team has 5 people on it; the other 25,000 employees don t know what Population Health is 35
36 Consider 2 Organizational Structures A Thin Governance & Management Layer Independent PCP Group 1 EMR, EDW Culture Governance Comp Model Referral Relationships % Medicare Care models Independent PCP Group 2 EMR, EDW Culture Governance Comp Model Referral Relationships % Medicare Care models Health System 1 EMR, EDW Culture Governance Comp Model Referral Relationships % Medicare Care models Health System 2 EMR, EDW Culture Governance Comp Model Referral Relationships % Medicare Care models Various Sub- Specialty Groups EMR, EDW Culture Governance Comp Model Referral Relationships % Medicare Care models In this model, the PCPs, hospitals, specialists in the network all hold different contracts with different payers with different incentives Each of the parties have their own EMRs, EDWs, clinical models, contractual relationships that a thin Governance layer and small management team cannot harmonize Executive team opportunity to establish common identity, expectations and operating model that finance can help capitalize, reward, contract, budget for 36
37 Consider 2 Organizational Structures B Payers, Employers Health System 1 EMR, EDW Culture Governance Comp Model Referral Relationships % Medicare Care models Health System 1 s Clinically & Financially Integrated Provider Network Independent PCP Group 1 Independent PCP Group 2 Health System 2 Independent Specialty Group Preferred Post Acute Network Wrap Network Jointly Owned Population Health Support NewCo Single EDW Coordinated recruitment & contracting functional support Common care model blueprint (people, process, technology) In this model, the market leader forms a Clinically & Financially Integrated Network (with or without other co-owners) CFIN participants and even payer partners can co-own the Population Health Support Newco, or contract with it for services 37
38 Why is An Integrated Financial Model Important? Your organization has likely spent millions on population health Your organization may be just one bad deal away from scrapping its population health plans It s difficult to take substantive capitated risk AND still manage fee for service payment model, particularly without enough skin in the game for providers, payers and consumers. So we owe a serious conversation to your action plan to evolve your financial model from a FFS model to a mixed model of capitated payments AND fee for service payments. The action plan needs to address 2 key sets of choices/decisions: Financial formula, defined in terms of sources of funds and uses of funds Ongoing financial management people & process model 38
39 Key Financial Management Choices Your sources of shared risk & shared savings funds Which of your system s patients do you target for a performance based reimbursement model AND/OR narrow network by when? What providers and services will be included in the financial budget our organization will be responsible to achieve, over time? What level of direct investment from payers & providers? Sidebar: What will your system do to mitigate competitive responses, particularly in a slow-growth market? Your uses of shared savings & shared risk funds Minimum and maximum distribution amounts? Group vs. individual performance weighting and distribution? Improvement vs. achievement impact on distribution? Quality vs. cost vs. citizenship metrics/performance? Hardwiring financial management / operations Budgeting best practices Monthly operating report best practices Transparency 39
40 Key Financial Management Choices Common Straw Model Template 40
41 Sources of Funds Decisions Which of your system s patients do you target for a performance based reimbursement model AND/OR narrow network by when? What providers and services will be included in the financial budget our organization will be responsible to achieve, over time? What level of direct investment from payers & providers? Sidebar: What will your system do to mitigate competitive responses, particularly in a slow-growth market? 41
42 Which Patients? Which of your system s patients do you target for a performance based reimbursement model AND/OR narrow network day 1 vs. day 1000? Most systems have 1-5% of their admissions and/or revenue tied to performance based contracts and/or narrow networks Some systems had 10-50% in the 1980s and early 1990s It s imperative to understand the savings profile of the populations you plan to cover, before you sign risk deals Medicare major post acute savings opportunities Medicaid variety of socioeconomic issues, behavioral health Commercial site of service, avoidable ED, Rx, ancillary and specialty utilization opportunities So anticipate a mixed financial model ; with some lives under narrow network/risk based payment models; and what that means to your operating and compensation models 42
43 Which Providers & Services? Many hospital-based provider systems are signing shared savings (no risk) arrangements worth 1-3% of revenue Fewer are signing full risk based deals, where if the provider incurs more expense than expected, then the provider owes the payer money Payers are increasingly seeking large primary care groups to take on financial risk on primary care & specialty professional expenses and facility expenses over time So, once you ve picked a population (e.g. Medicare Advantage vs. patients in need of hip surgery), you face several different options Take primary care professional expense risk; and/or Take specialty care professional expense risk; and/or Take facility expense risk; and/or Take pharmacy expense risk 43
44 Which Direct Investments? Typically $0 Changing as payers & providers recognize the significant operating model changes necessary to achieve sustainable savings Joint investment in analytics and hardwiring people, process & technology into care model on highest cost, highest risk patients 44
45 Case Study How a Bad Financial Deal Can Kill a Great Start Modestly growing market, with 4 competitors (including 1 AMC) ABC CIN recruited 12 key sub-specialists from AMC and gets an exclusive arrangement with BCBS to care for 25,000 HIX lives, 25,000 MA lives and 25,000 POS lives, at risk and under a 10-20% discount relative to current PPO fee schedule AMC competitor creates its own CIN and is excluded from HIX, MA and POS populations (except for emergency and super subspecialty services) For profit competitor creates its own CIN, and takes a 15% discount across all populations to keep beds full, without enhancements to its network Payer, reeling from MA losses because of under-priced products, aggressively markets for-profit competitor s network/product where the payer s margins are the greatest Commercial fee schedules decline ~15% across the market and ABC CIN loses 4 commercial market share points in 2 years 45
46 Case Study How a Bad Financial Deal Can Kill a Great Start What went wrong? Payers could exclude 1 (or more) from a network So competitors matched/extended your price discounts given short term pressure to fill beds Undifferentiated value proposition to independent physicians, let alone consumers, further fragmented the market to the point that physicians terminated their employment agreements and formed a large multispecialty practice aligned with the payers with the most lives Pacing the operational, competitive and financial transformation is a critical executive decision. Anticipate strategic moves particularly in fragmented provider markets with significant payer power Establish a clear operational plan that will achieve both market essentiality and value creation within specific populations (e.g., Medicaid managed care vs. commercial vs. chronically ill) in partnership with community providers 46
47 Uses of Funds Decisions How will you distribute and/or invest shared savings & shared risk proceeds with physicians, hospitals, payers and consumers? Minimum and maximum distribution amounts? Group vs. individual performance weighting and distribution? PCP vs. specialist distribution? Improvement vs. achievement impact on distribution? Quality vs. cost vs. citizenship metrics/performance? 47
48 Uses of Funds Decisions General Template for Revision Minimum and maximum distribution amounts? Group vs. individual performance weighting and distribution? PCP vs. specialist distribution? Improvement vs. achievement impact on distribution? Quality vs. cost vs. citizenship metrics/performance? 48
49 Minimum & Maximum Distribution Amounts Physician practices aiming for 10-20% of total compensation But employers aren t willing to pre-fund bonus accounts worth 10-20% of medical costs So providers need to revise their internal funds flow formulas/accounting accordingly, mindful of fair market value rules 49
50 Group vs. Individual Performance, PCP vs. Specialty Typically skewed towards individual, when group-wide coordination is the key to unlocking significant savings Result is more pod-level arrangements, that respect how far, how fast a particular group can change their behaviors Generally, more of the shared savings and risk flow to PCPs rather than specialists 50
51 Improvement vs. Achievement Typically skewed towards achievement, when improvement is typically the priority, out of the gate Result is an important message from leadership that overall group-level improvement will be the priority, over the next several years, recognizing some may leave 51
52 Metrics & Thresholds Typically underweighted in cost and citizenship, which are essential to short-term success Typically groups specify a minimum performance threshold to justify any shared savings/bonus payout Few groups assess specific financial penalties for underperformance 52
53 Case Study Slow Down to Speed Up person employed medical group and affiliated network, under significant pressure from CEO to move from volume to value Assessed their readiness to generate savings (e.g., readmissions, ED, Rx, post-acute, etc.); which only amounted to only $ /physician Decided to slow down to speed up in its quest from volume to value Instead, engaged core group of physicians in significant care model redesign blueprint exercise for populations payers indicated were in most need of management Subsequently entered into MSSP and variety of commercial ACOs with a multi-payer operating model and ~300 core physicians capable of sustainable cross-continuum quality improvements and cost savings (vs. all physicians & all populations at once) 53
54 Financial Management Best Practices for Population Health Budgeting process best practice Is the Population Health initiative a cost center, revenue center or profit center? What comprises the Population Health s revenue line over time? Expense items? Will population health-related capital investments be given higher priority during start-up phase? Ongoing monthly operating review best practice What s in your CMO s job description and KPIs? Design & deployment of a cross-continuum care model that specifies people, process & technologies required to manage to a lower cost, higher quality outcome What s in your Medical Group leader s job description and KPIs? Medical group operational excellence (i.e., staffing, productivity, compensation, procurement, etc.) What s in your CFO s job description and KPIs? Budgeting for shared savings & risk Measuring success and fixing problems Allocating capital Managing risk What s your managed care leader s job description and KPIs? Negotiator? Analyst? Product developer? Population health leader? 54
55 Summary 55
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business?
 Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Approved Models to Align Incentives between Hospitals and their Physicians
 Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
The Case For Value ACA to MACRA to MIPS
 The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
Population-Based Healthcare: Structural Models and Options
 Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Session 75 OF, Advantages & Challenges for Provider Led Health Plans. Moderator: LuCretia Leola Hydell, ASA, MAAA
 Session 75 OF, Advantages & Challenges for Provider Led Health Plans Moderator: LuCretia Leola Hydell, ASA, MAAA Presenters: Jerry Clark, MD, FACP Josh Martin Mark Rishell SOA Antitrust Disclaimer SOA
Session 75 OF, Advantages & Challenges for Provider Led Health Plans Moderator: LuCretia Leola Hydell, ASA, MAAA Presenters: Jerry Clark, MD, FACP Josh Martin Mark Rishell SOA Antitrust Disclaimer SOA
The Emergence of Value-Based Care: Present and Future Tense
 The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
The Health Insurance Market in Virginia. Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017
 The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS
 CENTER FOR INDUSTRY TRANSFORMATION MAY 2015 FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS Authors Amy Bibby Partner, DHG Healthcare amy.bibby@dhgllp.com Matthew Fadel Manager, DHG Healthcare matt.fadel@dhgllp.com
CENTER FOR INDUSTRY TRANSFORMATION MAY 2015 FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS Authors Amy Bibby Partner, DHG Healthcare amy.bibby@dhgllp.com Matthew Fadel Manager, DHG Healthcare matt.fadel@dhgllp.com
11/16/2015. Valence Health Solutions To Support. Vision. 20 years of Serving ~100 Hospital & Health System Clients Nationally.
 Valence Health Solutions To Support Prepared for First Illinois HFMA Optimize risk contracts Analyze and improve in-network utilization Improve quality November 2015 2015 Valence Health. All rights reserved.
Valence Health Solutions To Support Prepared for First Illinois HFMA Optimize risk contracts Analyze and improve in-network utilization Improve quality November 2015 2015 Valence Health. All rights reserved.
9/23/2016. Our Services. Transitioning from Fee-for-Service to Value-based Reimbursement. Key Trends and Strategies for Rural Health Providers
 Transitioning from Fee-for-Service to Value-based Reimbursement Key Trends and Strategies for Rural Health Providers Paul MacLellan, CEO >> Health care consulting company >> Wholly owned subsidiary of
Transitioning from Fee-for-Service to Value-based Reimbursement Key Trends and Strategies for Rural Health Providers Paul MacLellan, CEO >> Health care consulting company >> Wholly owned subsidiary of
A Practical Discussion of Value and Quality Based Payments What Do I Do Now?
 Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
than value. infrastructure for value-based payment, it is apparent that greater assumption of
 EXECUTIVE BRIEFING Value-Based Contracting: How to Think Like a Payer It is widely recognized that the rate of healthcare spending in the U.S. is unsustainable. In recent years, experts of all types, from
EXECUTIVE BRIEFING Value-Based Contracting: How to Think Like a Payer It is widely recognized that the rate of healthcare spending in the U.S. is unsustainable. In recent years, experts of all types, from
Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models
 Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models Kristina Rollings Product Director, Emerging Solutions March 24, 2014 Agenda 1. State of the
Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models Kristina Rollings Product Director, Emerging Solutions March 24, 2014 Agenda 1. State of the
The Road to Value. Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017
 The Road to Value Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017 1,500 Physicians UnityPoint Clinic 17 hospitals + 15 rural network hospitals 35,000
The Road to Value Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017 1,500 Physicians UnityPoint Clinic 17 hospitals + 15 rural network hospitals 35,000
Clinically Integrated Networks and Population Health The next chapter in healthcare
 Clinically Integrated Networks and Population Health The next chapter in healthcare M A T T H E W M A T U S I A K, D H S C, F R I P H ( UK) M T ( A S C P ) Health System Challenges While the Uninsured
Clinically Integrated Networks and Population Health The next chapter in healthcare M A T T H E W M A T U S I A K, D H S C, F R I P H ( UK) M T ( A S C P ) Health System Challenges While the Uninsured
Rewarding High Quality: Practical Models for Value- Based Physician Payment
 Rewarding High Quality: Practical Models for Value- Based Physician Payment Introduction In its 2013 report, Moving Beyond Fee-for-Service, the Alliance of Community Health Plans (ACHP) addressed the increasing
Rewarding High Quality: Practical Models for Value- Based Physician Payment Introduction In its 2013 report, Moving Beyond Fee-for-Service, the Alliance of Community Health Plans (ACHP) addressed the increasing
How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments?
 How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments? 1:10 PM 2:10 PM Steering Toward Success: Achieving Value in Whole Person Care September 25 and
How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments? 1:10 PM 2:10 PM Steering Toward Success: Achieving Value in Whole Person Care September 25 and
MANAGEMENT S DISCUSSION AND ANALYSIS OF FINANCIAL CONDITION AND RESULTS OF OPERATIONS FOR ASCENSION
 MANAGEMENT S DISCUSSION AND ANALYSIS OF FINANCIAL CONDITION AND RESULTS OF OPERATIONS FOR ASCENSION As of and for the six months ended December 31, 2014 and 2013 The following information should be read
MANAGEMENT S DISCUSSION AND ANALYSIS OF FINANCIAL CONDITION AND RESULTS OF OPERATIONS FOR ASCENSION As of and for the six months ended December 31, 2014 and 2013 The following information should be read
Achieving Value-based Care in Rural Populations through Provider-Sponsored Health Plans. February 11, 2014
 Achieving Value-based Care in Rural Populations through Provider-Sponsored Health Plans February 11, 2014 1 Value-Based Care is No Joke 2 What is Value-Based or Accountable Care? Value- Based Care = (Access
Achieving Value-based Care in Rural Populations through Provider-Sponsored Health Plans February 11, 2014 1 Value-Based Care is No Joke 2 What is Value-Based or Accountable Care? Value- Based Care = (Access
Using Analytics To Transform Your ACO
 Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION
 THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION HFMA First Illinois Chapter August 12, 2014 Stu Schaff Manager, DGA Partners Agenda > Background & Context > Measures
THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION HFMA First Illinois Chapter August 12, 2014 Stu Schaff Manager, DGA Partners Agenda > Background & Context > Measures
Retrospective Denials Management
 Retrospective Denials Management Weaving together the Clinical, Technical, and Legal Components Glen Reiner, RN, MBA, Western Region President Goals for our time together today Present an overview of effective
Retrospective Denials Management Weaving together the Clinical, Technical, and Legal Components Glen Reiner, RN, MBA, Western Region President Goals for our time together today Present an overview of effective
IT TAKES THREE TO TANGO
 IT TAKES THREE TO TANGO Structural Collaboration Between Carriers, Providers and Consumers A HEALTHSCAPE ADVISORS EXECUTIVE BRIEFING This HealthScape Advisors Executive Brief discusses a more comprehensive
IT TAKES THREE TO TANGO Structural Collaboration Between Carriers, Providers and Consumers A HEALTHSCAPE ADVISORS EXECUTIVE BRIEFING This HealthScape Advisors Executive Brief discusses a more comprehensive
White Paper. AMGA Advocacy. Taking Risk, 3.0: Medical Groups Are Moving to Risk Is Anyone Else? AMGA s Third Annual Survey on Taking Risk
 White Paper AMGA Advocacy Taking Risk, 3.0: Medical Groups Are Moving to Risk Is Anyone Else? AMGA s Third Annual Survey on Taking Risk AMGA Advocacy Taking Risk, 3.0: Medical Groups Are Moving to Risk
White Paper AMGA Advocacy Taking Risk, 3.0: Medical Groups Are Moving to Risk Is Anyone Else? AMGA s Third Annual Survey on Taking Risk AMGA Advocacy Taking Risk, 3.0: Medical Groups Are Moving to Risk
Physician groups what goes wrong, how do we avoid it? Subtitle: Physicians, Change, and Maximizing Employed Physician Performance
 Physician groups what goes wrong, how do we avoid it? Subtitle: Physicians, Change, and Maximizing Employed Physician Performance Thomas Ferkovic Managing Partner SS&G Healthcare Chicago tferkovic@ssandg.com
Physician groups what goes wrong, how do we avoid it? Subtitle: Physicians, Change, and Maximizing Employed Physician Performance Thomas Ferkovic Managing Partner SS&G Healthcare Chicago tferkovic@ssandg.com
CVS HEALTH/AETNA INVESTOR CALL SCRIPT
 MIKE McGUIRE, CVS HEALTH IRO Good morning, everyone. Thanks so much for joining us this morning to hear about the definitive merger agreement we announced yesterday to acquire Aetna, one of the nation
MIKE McGUIRE, CVS HEALTH IRO Good morning, everyone. Thanks so much for joining us this morning to hear about the definitive merger agreement we announced yesterday to acquire Aetna, one of the nation
MANAGEMENT S DISCUSSION CONDITION AND RESULTS OF OPERATIONS FOR ASCENSION AS OF AND FOR THE SIX MONTHS ENDED DECEMBER 31, 2013 AND 2012
 MANAGEMENT S DISCUSSION AND ANALYSIS OF FINANCIAL CONDITION AND RESULTS OF OPERATIONS FOR ASCENSION AS OF AND FOR THE SIX MONTHS ENDED DECEMBER 31, 2013 AND 2012 The following information should be read
MANAGEMENT S DISCUSSION AND ANALYSIS OF FINANCIAL CONDITION AND RESULTS OF OPERATIONS FOR ASCENSION AS OF AND FOR THE SIX MONTHS ENDED DECEMBER 31, 2013 AND 2012 The following information should be read
Problems with Current Health Plans
 Problems with Current Health Plans Poor Integration, Coordination and Collaboration - Current plans offer limited coordination between the health plan, Providers, and the Members, as well as limited mobile
Problems with Current Health Plans Poor Integration, Coordination and Collaboration - Current plans offer limited coordination between the health plan, Providers, and the Members, as well as limited mobile
MEDICARE ADVANTAGE MA Plans. to $28 per month 46% HOW HEALTH SYSTEMS CAN THRIVE WITH. Developing Your Medicare Advantage Strategy PRODUCT
 HOW HEALTH SYSTEMS CAN THRIVE WITH MEDICARE ADVANTAGE The 2019 Medicare Advantage (MA) plan year began on January 1st and once again more Americans enrolled in MA plans than the year before. Fueled by
HOW HEALTH SYSTEMS CAN THRIVE WITH MEDICARE ADVANTAGE The 2019 Medicare Advantage (MA) plan year began on January 1st and once again more Americans enrolled in MA plans than the year before. Fueled by
An Introduction to Value Based Care. Evan Richards Product Leader Value Based Care Solutions May 2016
 An Introduction to Value Based Care Evan Richards Product Leader Value Based Care Solutions May 2016 2016 General Electric Company All rights reserved. This does not constitute a representation or warranty
An Introduction to Value Based Care Evan Richards Product Leader Value Based Care Solutions May 2016 2016 General Electric Company All rights reserved. This does not constitute a representation or warranty
CLINICALLY INTEGRATED REGIONAL CONSORTIA
 CLINICALLY INTEGRATED REGIONAL CONSORTIA How Providers Are Coming Together in New Partnership Models and Implications for Payors Fall Managed Care Forum November 13, 2014 The Chartis Group, LLC The Proliferation
CLINICALLY INTEGRATED REGIONAL CONSORTIA How Providers Are Coming Together in New Partnership Models and Implications for Payors Fall Managed Care Forum November 13, 2014 The Chartis Group, LLC The Proliferation
2017 EMPLOYER SERIES. 6 Things Employers Need to Know About Rising Health Care Costs. Cost Management Key Findings
 2017 EMPLOYER SERIES 6 Things Employers Need to Know About Rising Health Care Costs Cost Management 2017 Key Findings It s one of the biggest challenges employers face today: keeping health care costs
2017 EMPLOYER SERIES 6 Things Employers Need to Know About Rising Health Care Costs Cost Management 2017 Key Findings It s one of the biggest challenges employers face today: keeping health care costs
79th OREGON LEGISLATIVE ASSEMBLY Regular Session. Enrolled. Senate Bill 934 CHAPTER... AN ACT
 79th OREGON LEGISLATIVE ASSEMBLY--2017 Regular Session Enrolled Senate Bill 934 Sponsored by Senator STEINER HAYWARD, Representative BUEHLER CHAPTER... AN ACT Relating to payments for primary care; creating
79th OREGON LEGISLATIVE ASSEMBLY--2017 Regular Session Enrolled Senate Bill 934 Sponsored by Senator STEINER HAYWARD, Representative BUEHLER CHAPTER... AN ACT Relating to payments for primary care; creating
Payment Reform in Support of Population Health Management
 Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
J.P. Morgan 35 th Annual Healthcare Conference. DRAFT 01/04/17 1p
 J.P. Morgan 35 th Annual Healthcare Conference DRAFT 01/04/17 1p Forward-Looking Statements This presentation includes forward-looking statements within the meaning of Section 27A of the Securities Act
J.P. Morgan 35 th Annual Healthcare Conference DRAFT 01/04/17 1p Forward-Looking Statements This presentation includes forward-looking statements within the meaning of Section 27A of the Securities Act
aligning managed care contracts, compensation plans, and incentive models
 REPRINT NOVEMBER 2011 Michael E. Nugent healthcare financial management association www.hfma.org aligning managed care contracts, compensation plans, and incentive models Providers should take the lead
REPRINT NOVEMBER 2011 Michael E. Nugent healthcare financial management association www.hfma.org aligning managed care contracts, compensation plans, and incentive models Providers should take the lead
partnering with payers? key lessons to keep in mind
 REPRINT January 2014 Bill Eggbeer Kevin Sears Kenneth Homer healthcare financial management association hfma.org partnering with payers? key lessons to keep in mind As providers enter into risk-sharing
REPRINT January 2014 Bill Eggbeer Kevin Sears Kenneth Homer healthcare financial management association hfma.org partnering with payers? key lessons to keep in mind As providers enter into risk-sharing
Delivering Value-Based Care:
 Discussion Summary Delivering Value-Based Care: Episodes of Care Analytics for Health Care Providers, Payers and ACOs July 2015 Interview Featuring: J. Peter Chingos, Senior Industry Consultant, Health
Discussion Summary Delivering Value-Based Care: Episodes of Care Analytics for Health Care Providers, Payers and ACOs July 2015 Interview Featuring: J. Peter Chingos, Senior Industry Consultant, Health
2.05 Predictive Modeling P4P and Physician Engagement. Pay for Performance Summit February 7, 2006
 2.05 Predictive Modeling P4P and Physician Engagement Pay for Performance Summit February 7, 2006 1 Agenda Three Key Healthcare Trends About Predictive Modeling About Reporting Business and Clinical Outcomes
2.05 Predictive Modeling P4P and Physician Engagement Pay for Performance Summit February 7, 2006 1 Agenda Three Key Healthcare Trends About Predictive Modeling About Reporting Business and Clinical Outcomes
C - Suite Transformation Management Training: Finance and Operations Overview. May 17, 2017
 C - Suite Transformation Management Training: Finance and Operations Overview Presented by: Peter R. Epp, CPA May 17, 2017 Overview Summary of Value Based Payment (VBP) Initiatives Underlying VBP Payment
C - Suite Transformation Management Training: Finance and Operations Overview Presented by: Peter R. Epp, CPA May 17, 2017 Overview Summary of Value Based Payment (VBP) Initiatives Underlying VBP Payment
FMV Considerations for Bundled Payment Arrangements
 FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
Is There a Role for the Orthopaedic Surgeon in ACOs?
 Is There a Role for the Orthopaedic Surgeon in ACOs? Michael R. Redler, MD Head Team Physician Sacred Heart University Visiting Assistant Clinical Professor University of Virginia Orthopaedic Consultant
Is There a Role for the Orthopaedic Surgeon in ACOs? Michael R. Redler, MD Head Team Physician Sacred Heart University Visiting Assistant Clinical Professor University of Virginia Orthopaedic Consultant
March 28, Dear Administrator Slavitt:
 20555 Victor Parkway Livonia, MI 48152 tel 734-343-1000 trinity-health.org March 28, 2016 Andy Slavitt Administrator Center for Medicare and Medicaid Services U.S. Department of Health and Human Services
20555 Victor Parkway Livonia, MI 48152 tel 734-343-1000 trinity-health.org March 28, 2016 Andy Slavitt Administrator Center for Medicare and Medicaid Services U.S. Department of Health and Human Services
March 1, Chairman Lamar Alexander United States Senate Committee on Health, Education, Labor, and Pensions Washington, DC 20510
 March 1, 2019 Chairman Lamar Alexander United States Senate Committee on Health, Education, Labor, and Pensions Washington, DC 20510 Dear Chairman Alexander: On behalf of AMGA and our members, I appreciate
March 1, 2019 Chairman Lamar Alexander United States Senate Committee on Health, Education, Labor, and Pensions Washington, DC 20510 Dear Chairman Alexander: On behalf of AMGA and our members, I appreciate
Delivering Value for All Health Care Stakeholders. Larry Merlo President & Chief Executive Officer
 Delivering Value for All Health Care Stakeholders Larry Merlo President & Chief Executive Officer Agenda Our Value Proposition Has Never Been Stronger We See Compelling Opportunities in a Robust Health
Delivering Value for All Health Care Stakeholders Larry Merlo President & Chief Executive Officer Agenda Our Value Proposition Has Never Been Stronger We See Compelling Opportunities in a Robust Health
Succeeding with APMs: Structuring Relationships Between Payers and Providers
 Succeeding with APMs: Structuring Relationships Between Payers and Providers OCTOBER 30, 2017 Crystal Gateway Marriott Hotel Arlington, VA Enhance your Summit experience with Log in at: glsr.it/lansummit
Succeeding with APMs: Structuring Relationships Between Payers and Providers OCTOBER 30, 2017 Crystal Gateway Marriott Hotel Arlington, VA Enhance your Summit experience with Log in at: glsr.it/lansummit
AFFORDABILITY REVIEW. Mysteries of the Medical Loss Ratio
 AFFORDABILITY REVIEW Mysteries of the Medical Loss Ratio NANCY DJORDJEVIC DIRECTOR, HEALTHCARE ANALYTICS APRIL 2016 WHO IS GORMAN HEALTH GROUP? Gorman Health Group is the leading solutions and consulting
AFFORDABILITY REVIEW Mysteries of the Medical Loss Ratio NANCY DJORDJEVIC DIRECTOR, HEALTHCARE ANALYTICS APRIL 2016 WHO IS GORMAN HEALTH GROUP? Gorman Health Group is the leading solutions and consulting
Avalere Health 2015 Industry Outlook
 2015 Industry Outlook 2 Introduction Industry Outlook 2015 Changes in healthcare financing, delivery, and organization are transforming the sector. Health plans and providers are revising their business
2015 Industry Outlook 2 Introduction Industry Outlook 2015 Changes in healthcare financing, delivery, and organization are transforming the sector. Health plans and providers are revising their business
35th Annual J.P. Morgan Healthcare Conference. January 12, 2017
 35th Annual J.P. Morgan Healthcare Conference January 12, 2017 Safe Harbor Statement and Non-GAAP Financial Measures This presentation contains forward-looking statements, including statements regarding
35th Annual J.P. Morgan Healthcare Conference January 12, 2017 Safe Harbor Statement and Non-GAAP Financial Measures This presentation contains forward-looking statements, including statements regarding
JP Morgan Healthcare Conference January 13, 2016
 JP Morgan Healthcare Conference January 13, 2016 FORWARD-LOOKING STATEMENTS Certain statements and information in this presentation may be deemed to be forward-looking statements within the meaning of
JP Morgan Healthcare Conference January 13, 2016 FORWARD-LOOKING STATEMENTS Certain statements and information in this presentation may be deemed to be forward-looking statements within the meaning of
No change from proposed rule. healthcare providers and suppliers of services (e.g.,
 American College of Physicians Medicare Shared Savings/Accountable Care Organization (ACO) Final Rule Summary Analysis Category Final Rule Summary Change from Proposed Rule and Comments ACO refers to a
American College of Physicians Medicare Shared Savings/Accountable Care Organization (ACO) Final Rule Summary Analysis Category Final Rule Summary Change from Proposed Rule and Comments ACO refers to a
Session 115IF, Provider Risk-Sharing Arrangements in Medicaid. Presenters: Puneet Budhiraja, ASA, MAAA Michael Minor Sudha Shenoy, FSA, MAAA, CERA
 Session 115IF, Provider Risk-Sharing Arrangements in Medicaid Presenters: Puneet Budhiraja, ASA, MAAA Michael Minor Sudha Shenoy, FSA, MAAA, CERA SOA Antitrust Disclaimer SOA Presentation Disclaimer 2018
Session 115IF, Provider Risk-Sharing Arrangements in Medicaid Presenters: Puneet Budhiraja, ASA, MAAA Michael Minor Sudha Shenoy, FSA, MAAA, CERA SOA Antitrust Disclaimer SOA Presentation Disclaimer 2018
JP Morgan 27th Annual Healthcare Conference Angela F. Braly President & Chief Executive Officer January 12, 2009
 JP Morgan 27th Annual Healthcare Conference Angela F. Braly President & Chief Executive Officer January 12, 2009 Safe Harbor Statement Under The Private Securities Litigation Reform Act of 1995 The statements
JP Morgan 27th Annual Healthcare Conference Angela F. Braly President & Chief Executive Officer January 12, 2009 Safe Harbor Statement Under The Private Securities Litigation Reform Act of 1995 The statements
Cowen and Company 37 th Annual Health Care Conference. March 6, 2017
 Cowen and Company 37 th Annual Health Care Conference March 6, 2017 Safe Harbor Statement and Non-GAAP Financial Measures This presentation contains forward-looking statements, including statements regarding
Cowen and Company 37 th Annual Health Care Conference March 6, 2017 Safe Harbor Statement and Non-GAAP Financial Measures This presentation contains forward-looking statements, including statements regarding
OBLIGATED GROUP MANAGEMENT S DISCUSSION AND ANALYSIS OF RESULTS FOR THE FISCAL YEAR ENDED JUNE 30, 2018
 OBLIGATED GROUP MANAGEMENT S DISCUSSION AND ANALYSIS OF RESULTS FOR THE FISCAL YEAR ENDED JUNE 30, 2018 For additional information please visit www.essentiahealth.org. For past quarterly and annual disclosures
OBLIGATED GROUP MANAGEMENT S DISCUSSION AND ANALYSIS OF RESULTS FOR THE FISCAL YEAR ENDED JUNE 30, 2018 For additional information please visit www.essentiahealth.org. For past quarterly and annual disclosures
Lessons Learned from the Financial Front Lines of Population Health Management
 Lessons Learned from the Financial Front Lines of Population Health Management Presenters Deborah Bloomfield, PhD, CPA Central Markets CFO for Catholic Health Partners and CFO for Mercy Health Charles
Lessons Learned from the Financial Front Lines of Population Health Management Presenters Deborah Bloomfield, PhD, CPA Central Markets CFO for Catholic Health Partners and CFO for Mercy Health Charles
PATH TOWARD PAYMENTS THAT REWARD VALUE
 PATH TOWARD PAYMENTS THAT REWARD VALUE David Muhlestein, PhD JD Chief Research Officer Leavitt Partners @DavidMuhlestein December 18, 2017 1 PRESENTATION OVERVIEW 1. Current Trends 2. Are ACOs Delivering
PATH TOWARD PAYMENTS THAT REWARD VALUE David Muhlestein, PhD JD Chief Research Officer Leavitt Partners @DavidMuhlestein December 18, 2017 1 PRESENTATION OVERVIEW 1. Current Trends 2. Are ACOs Delivering
Risky Business: Crystal Run Health Plans. Michelle A. Koury, MD Jonathan Nasser, MD Crystal Run Healthcare
 Risky Business: Crystal Run Health Plans Michelle A. Koury, MD Jonathan Nasser, MD Crystal Run Healthcare About Crystal Run Healthcare Physician owned MSG in NY State, founded 1996 >350 providers, >30
Risky Business: Crystal Run Health Plans Michelle A. Koury, MD Jonathan Nasser, MD Crystal Run Healthcare About Crystal Run Healthcare Physician owned MSG in NY State, founded 1996 >350 providers, >30
Sutter Medical Network
 Sutter Medical Network Sutter Care Pattern Analyzer making the case for affordability Fifth National Pay for Performance Summit March 9, 2010 Michael van Duren, M.D., CMO Sutter Physician Services Colleen
Sutter Medical Network Sutter Care Pattern Analyzer making the case for affordability Fifth National Pay for Performance Summit March 9, 2010 Michael van Duren, M.D., CMO Sutter Physician Services Colleen
ACO Essentials Series
 ACO Essentials Series How to Use Health Endeavors Technology January, 2017 1/11/2017 1 Agenda Day 1&2 Interactive Analytic Tools Define ACO Goals- Success Plan Organizational Structure Executive TIN and
ACO Essentials Series How to Use Health Endeavors Technology January, 2017 1/11/2017 1 Agenda Day 1&2 Interactive Analytic Tools Define ACO Goals- Success Plan Organizational Structure Executive TIN and
Figure 1: Original APM Framework
 Contents Overview... 2 This Year s APM Measurement Effort... 3 Scope... 3 Data Source... 4 The LAN Survey... 4 The Blue Cross Blue Shield Association Survey... 8 The America s Health Insurance Plans Survey...
Contents Overview... 2 This Year s APM Measurement Effort... 3 Scope... 3 Data Source... 4 The LAN Survey... 4 The Blue Cross Blue Shield Association Survey... 8 The America s Health Insurance Plans Survey...
Medicare Advantage Explained 2008
 Medicare Advantage Explained 2008 Getting More from Your Medicare Benefits An educational resource from 4 Medicare Basics 7 About Medicare Advantage 9 Medicare Advantage Options 12 Reviewing Your Choices
Medicare Advantage Explained 2008 Getting More from Your Medicare Benefits An educational resource from 4 Medicare Basics 7 About Medicare Advantage 9 Medicare Advantage Options 12 Reviewing Your Choices
Public sector employers already face growing financial. How Public Sector Employers Can Manage Retiree Health Liabilities. Retirement Strategies
 Retirement Strategies How Public Sector Employers Can Manage Retiree Health Liabilities Changes in the Governmental Accounting Standards Board (GASB) reporting requirements will increase the liabilities
Retirement Strategies How Public Sector Employers Can Manage Retiree Health Liabilities Changes in the Governmental Accounting Standards Board (GASB) reporting requirements will increase the liabilities
Embracing the Future of Care Delivery: What have we learned?
 Embracing the Future of Care Delivery: What have we learned? Robert Nesse, M.D. Senior Advisor for Healthcare Policy and Payment Reform CEO, Mayo Clinic Health System 2010-2015 2014 MFMER slide-1 Fundamental
Embracing the Future of Care Delivery: What have we learned? Robert Nesse, M.D. Senior Advisor for Healthcare Policy and Payment Reform CEO, Mayo Clinic Health System 2010-2015 2014 MFMER slide-1 Fundamental
AAOS MACRA Proposed Rule Summary (Short)
 AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
Critical Access Hospital (CAH) ND Critical Access Hospital Board Boot Camp April 13, 2018
 Critical Access Hospital (CAH) Financial Analysis 2016, ND CAH ACO Experiences, Plans and Possibilities ND Critical Access Hospital Board Boot Camp April 13, 2018 1 Support for the Financial Analysis The
Critical Access Hospital (CAH) Financial Analysis 2016, ND CAH ACO Experiences, Plans and Possibilities ND Critical Access Hospital Board Boot Camp April 13, 2018 1 Support for the Financial Analysis The
MassHealth Section 1115 Waiver Summary. Key provisions:
 MassHealth Section 1115 Waiver Summary With unsustainable spending growth that accounts for nearly 40 percent of the overall state budget, MassHealth released a draft federal waiver touted as an opportunity
MassHealth Section 1115 Waiver Summary With unsustainable spending growth that accounts for nearly 40 percent of the overall state budget, MassHealth released a draft federal waiver touted as an opportunity
Health care affordability VBC transformation
 Health care affordability VBC transformation What s at stake? The cost of health care in the United States has been on an unsustainable rise for some time, driven by fundamental delivery and financing
Health care affordability VBC transformation What s at stake? The cost of health care in the United States has been on an unsustainable rise for some time, driven by fundamental delivery and financing
Integrating Population Health Analytics and the EHR Environment Session 87, March 6, 2018
 Integrating Population Health Analytics and the EHR Environment Session 87, March 6, 2018 Nina M. Taggart, MD, Senior Medical Director, Population Health and Payer Relations, Lehigh Valley Health Network
Integrating Population Health Analytics and the EHR Environment Session 87, March 6, 2018 Nina M. Taggart, MD, Senior Medical Director, Population Health and Payer Relations, Lehigh Valley Health Network
MACRA: APPLICATIONS & IMPLICATIONS September 13, /13/2016. Mark Blessing, CPA, FHFMA Partner
 MACRA: APPLICATIONS & IMPLICATIONS September 13, 2016 Mark Blessing, CPA, FHFMA Partner mblessing@bkd.com Zach Remmich Managing Consultant zremmich@bkd.com 1 TO RECEIVE CPE CREDIT Participate in entire
MACRA: APPLICATIONS & IMPLICATIONS September 13, 2016 Mark Blessing, CPA, FHFMA Partner mblessing@bkd.com Zach Remmich Managing Consultant zremmich@bkd.com 1 TO RECEIVE CPE CREDIT Participate in entire
Opportunities on the Horizon. CCWJC/CCPN Provider Meeting Update November 2 nd, 2017
 Opportunities on the Horizon CCWJC/CCPN Provider Meeting Update November 2 nd, 2017 CCPN is physician-led and will: Increase quality and efficiency of health care Support independent, rural and/or small
Opportunities on the Horizon CCWJC/CCPN Provider Meeting Update November 2 nd, 2017 CCPN is physician-led and will: Increase quality and efficiency of health care Support independent, rural and/or small
Common Managed Care Terms & Definitions
 Contact Us: Email: info@emedbiz.com Phone: 561-430-2090 Fax: 561-430-2091 Website: www.emedbiz.com Common Managed Care Terms & Definitions Balance billing: The practice of billing a patient for the amount
Contact Us: Email: info@emedbiz.com Phone: 561-430-2090 Fax: 561-430-2091 Website: www.emedbiz.com Common Managed Care Terms & Definitions Balance billing: The practice of billing a patient for the amount
37 th Annual J.P. Morgan Healthcare Conference January 9, 2019
 37 th Annual J.P. Morgan Healthcare Conference January 9, 2019 1 Disclaimer Statement This presentation contains forward-looking statements within the meaning of Section 27A of the Securities Act of 1933,
37 th Annual J.P. Morgan Healthcare Conference January 9, 2019 1 Disclaimer Statement This presentation contains forward-looking statements within the meaning of Section 27A of the Securities Act of 1933,
Assessing ACO Performance
 Assessing ACO Performance David V. Axene, FSA, FCA, CERA, MAAA As more health plans utilize Accountable Care Organizations (i.e., ACOs) as part of their network operations, ACO performance assessment is
Assessing ACO Performance David V. Axene, FSA, FCA, CERA, MAAA As more health plans utilize Accountable Care Organizations (i.e., ACOs) as part of their network operations, ACO performance assessment is
Re: Comments on proposed rule for the Medicare Shared Savings Program: Accountable Care Organizations
 June 6, 2011 Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1345-P PO Box 8013 Baltimore, MD 21244-8013 Re: Comments on proposed rule for the Medicare Shared
June 6, 2011 Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1345-P PO Box 8013 Baltimore, MD 21244-8013 Re: Comments on proposed rule for the Medicare Shared
Will Health Plans Kill the Laboratory Outreach Program?
 Will Health Plans Kill the Laboratory Outreach Program? Jane M. Hermansen MBA, MT(ASCP) Mayo Clinic Rochester, Minnesota Learning Objectives Describe emerging payer trends in today s healthcare environment
Will Health Plans Kill the Laboratory Outreach Program? Jane M. Hermansen MBA, MT(ASCP) Mayo Clinic Rochester, Minnesota Learning Objectives Describe emerging payer trends in today s healthcare environment
The Future Of Medicare Physician Reimbursement
 Portfolio Media. Inc. 111 West 19 th Street, 5th Floor New York, NY 10011 www.law360.com Phone: +1 646 783 7100 Fax: +1 646 783 7161 customerservice@law360.com The Future Of Medicare Physician Reimbursement
Portfolio Media. Inc. 111 West 19 th Street, 5th Floor New York, NY 10011 www.law360.com Phone: +1 646 783 7100 Fax: +1 646 783 7161 customerservice@law360.com The Future Of Medicare Physician Reimbursement
Providers Contracting Directly With Employers
 Providers Contracting Directly With Employers NOVEMBER 14, 2018 1 The Current Model 2 Direct-to-Employer (DTE) Health Plan Aligned Incentives Gain Share Direct Relationship At The Table Integrated Data
Providers Contracting Directly With Employers NOVEMBER 14, 2018 1 The Current Model 2 Direct-to-Employer (DTE) Health Plan Aligned Incentives Gain Share Direct Relationship At The Table Integrated Data
MACRAnomics. Patient-Level Economics and Strategic Implications for Providers. Presented to: NW Ohio HFMA October 20, 2016
 MACRAnomics Patient-Level Economics and Strategic Implications for Providers Presented to: NW Ohio HFMA October 20, 2016 Property of HealthScape Advisors Strictly Confidential 2 MACRAnomics: Objectives
MACRAnomics Patient-Level Economics and Strategic Implications for Providers Presented to: NW Ohio HFMA October 20, 2016 Property of HealthScape Advisors Strictly Confidential 2 MACRAnomics: Objectives
October 6, Re: Notice of Benefit and Payment Parameters for 2018; CMS-9934-P. Submitted electronically via
 20555 Victor Parkway Livonia, MI 48152 tel 734-343-1000 trinity-health.org October 6, 2016 Andrew M. Slavitt Acting Administrator Centers for Medicare & Medicaid Services Department of Health and Human
20555 Victor Parkway Livonia, MI 48152 tel 734-343-1000 trinity-health.org October 6, 2016 Andrew M. Slavitt Acting Administrator Centers for Medicare & Medicaid Services Department of Health and Human
10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD. AccountableCareInstitute.com
 10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD FQHCs Bridge the Gap in Care Bridge Built and Maintained by FFS Dollars 2 CMMI View of FFS Medicine 3 Accountability High
10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD FQHCs Bridge the Gap in Care Bridge Built and Maintained by FFS Dollars 2 CMMI View of FFS Medicine 3 Accountability High
Managing the risk and unpredictable costs of transplants
 Managing the risk and unpredictable costs of transplants Executive summary While payers understand that transplants will be a part of their medical expense, they may be unprepared for the financial volatility
Managing the risk and unpredictable costs of transplants Executive summary While payers understand that transplants will be a part of their medical expense, they may be unprepared for the financial volatility
To Acquire. Creating the first and only global, comprehensive virtual healthcare delivery platform. June 19, 2017
 To Acquire Creating the first and only global, comprehensive virtual healthcare delivery platform June 19, 2017 1 Today s Presenters Jason Gorevic President & CEO Mark Hirschhorn COO & CFO Peter McClennen
To Acquire Creating the first and only global, comprehensive virtual healthcare delivery platform June 19, 2017 1 Today s Presenters Jason Gorevic President & CEO Mark Hirschhorn COO & CFO Peter McClennen
Presented by: Steven Flores. Prepared for: The Predictive Modeling Summit
 Presented by: Steven Flores Prepared for: The Predictive Modeling Summit November 13, 2014 Disease Management Introduction A multidisciplinary, systematic approach to health care delivery that: Includes
Presented by: Steven Flores Prepared for: The Predictive Modeling Summit November 13, 2014 Disease Management Introduction A multidisciplinary, systematic approach to health care delivery that: Includes
Valuation of Alternative Payment Models
 Valuation of Alternative Payment Models No portion of this white paper may be used or duplicated by any person or entity for any purpose without the express written permission of PYA. I. Introduction:
Valuation of Alternative Payment Models No portion of this white paper may be used or duplicated by any person or entity for any purpose without the express written permission of PYA. I. Introduction:
Value Based Contracting
 Value Based Contracting CONCEPTS FOR THE MEDICAL PRACTICE dhgllp.com/healthcare 225 Peachtree Street NE, Suite 600 Atlanta, GA 30303 Bill Hannah PRINCIPAL Bill.Hannah@dhgllp.com 404.575.8921 Doral Davis-Jacobsen
Value Based Contracting CONCEPTS FOR THE MEDICAL PRACTICE dhgllp.com/healthcare 225 Peachtree Street NE, Suite 600 Atlanta, GA 30303 Bill Hannah PRINCIPAL Bill.Hannah@dhgllp.com 404.575.8921 Doral Davis-Jacobsen
Volume to Value The Great Transformation of American Medicine
 Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
Building an Effective Reimbursement System. Population Based Reimbursement: Introduction. The Challenge. David Axene, FSA, FCA, CERA, MAAA
 Population Based Reimbursement: Building an Effective Reimbursement System David Axene, FSA, FCA, CERA, MAAA Introduction As more and more health systems consider population based reimbursement, pursue
Population Based Reimbursement: Building an Effective Reimbursement System David Axene, FSA, FCA, CERA, MAAA Introduction As more and more health systems consider population based reimbursement, pursue
Healthcare Reform and Its Impact on the Care Delivery System
 Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Case Study Background Reading Strategic Management - Banks
 Case Study Background Reading Strategic Management - Banks The CEO of St. Sebastian Health System, a moderate-sized hospital system in a mid-sized, Midwest city has hired you to help turn things around.
Case Study Background Reading Strategic Management - Banks The CEO of St. Sebastian Health System, a moderate-sized hospital system in a mid-sized, Midwest city has hired you to help turn things around.
Elevate by Denver Health Medical Plan
 Quality Overview by Denver Health Medical Plan Accreditation Exchange Product Accrediting Organization: Accreditation Status: NCQA Health Plan Accreditation (Marketplace HMO) Accredited* Excellent: Organization
Quality Overview by Denver Health Medical Plan Accreditation Exchange Product Accrediting Organization: Accreditation Status: NCQA Health Plan Accreditation (Marketplace HMO) Accredited* Excellent: Organization
Health Service Board Rates and Benefits Committee Meeting
 Health Service Board Rates and Benefits Committee Meeting Blue Shield Medical Group ACO Review April 10, 2014 Prepared by Aon Hewitt Health and Benefits Contents History ACO Overview Evaluation Framework
Health Service Board Rates and Benefits Committee Meeting Blue Shield Medical Group ACO Review April 10, 2014 Prepared by Aon Hewitt Health and Benefits Contents History ACO Overview Evaluation Framework
Provider-Sponsored Health Plans for ACOs
 Provider-Sponsored Health Plans for ACOs Phil Kamp, CEO November 5, 2013 Change is Coming Or is Here in Some Cases Massive Shift in Payment Models Likelihood of Hospitals Gaining Payer Capabilities in
Provider-Sponsored Health Plans for ACOs Phil Kamp, CEO November 5, 2013 Change is Coming Or is Here in Some Cases Massive Shift in Payment Models Likelihood of Hospitals Gaining Payer Capabilities in
The Health Management Academy Strategic Survey Q1 2019: Defining Risk. March 2019
 The Health Management Academy Strategic Survey Q1 2019: Defining Risk March 2019 1 Defining Risk In 2019, the U.S. healthcare market is poised to continue its march towards value-based care. In the context
The Health Management Academy Strategic Survey Q1 2019: Defining Risk March 2019 1 Defining Risk In 2019, the U.S. healthcare market is poised to continue its march towards value-based care. In the context
Fee for Service: Paying for Volume, Not Value
 Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
Changes to Medicare under the Affordable Care Act
 January, 2017 siepr.stanford.edu Stanford Institute for Policy Brief Changes to Medicare under the Affordable Care Act By Jack Davidson and Jonathan Levin The Affordable Care Act (ACA) made substantial
January, 2017 siepr.stanford.edu Stanford Institute for Policy Brief Changes to Medicare under the Affordable Care Act By Jack Davidson and Jonathan Levin The Affordable Care Act (ACA) made substantial
Today s Payers and Providers
 Today s Payers and Providers Strategies for Success Emad Rizk, MD President and Chief Executive Officer Accretive Health Session Objectives Description of value based models in the market Data elements
Today s Payers and Providers Strategies for Success Emad Rizk, MD President and Chief Executive Officer Accretive Health Session Objectives Description of value based models in the market Data elements
Initiative Options for Simulation Scenarios
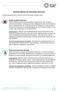 Initiative Options for Simulation Scenarios The following options are in version 2h of the ReThink Health simulation model. Enable healthier behaviors Promote healthy behavior and help people to stop behaviors
Initiative Options for Simulation Scenarios The following options are in version 2h of the ReThink Health simulation model. Enable healthier behaviors Promote healthy behavior and help people to stop behaviors
Lehigh Valley Health Network
 Lehigh Valley Health Network Journey to Accountable Care November 19, 2014 Powered by Populytics Lehigh Valley Health Network Fast Facts In Allentown/Bethlehem area, north of Philadelphia Recognized by
Lehigh Valley Health Network Journey to Accountable Care November 19, 2014 Powered by Populytics Lehigh Valley Health Network Fast Facts In Allentown/Bethlehem area, north of Philadelphia Recognized by
MGMA BUSINESS PLAN COMPETITION. Team 2
 MGMA BUSINESS PLAN COMPETITION Team 2 IDS HOSPITAL, LAREDO, TX (Team 2) Executive Summary Integrated Delivery Systems (IDS) is a 200 bed, medium-sized comprehensive service provider hospital in Laredo,
MGMA BUSINESS PLAN COMPETITION Team 2 IDS HOSPITAL, LAREDO, TX (Team 2) Executive Summary Integrated Delivery Systems (IDS) is a 200 bed, medium-sized comprehensive service provider hospital in Laredo,
