Delivering Value-Based Care:
|
|
|
- Sharon King
- 5 years ago
- Views:
Transcription
1 Discussion Summary Delivering Value-Based Care: Episodes of Care Analytics for Health Care Providers, Payers and ACOs July 2015 Interview Featuring: J. Peter Chingos, Senior Industry Consultant, Health Analytics Practice, Health & Life Sciences, SAS Institute Inc.
2 Introduction Episodes of care (EOC) is redefining the way health care organizations manage patient care and connect outcomes and value to payment. By leveraging insights from EOC, both providers and payers can clearly understand the quality and total cost of care and make adjustments to optimize resources, drive towards better health outcomes, reduce costs, and generate higher patient satisfaction. IIA spoke with Peter Chingos, a Senior Industry Consultant with the Health Analytics Practice, Health & Life Sciences at SAS Institute Inc. to discuss the various benefits and opportunities EOC analytics provides, as well as some of the challenges associated with implementation. What are episodes of care and why are they important? Episodes of care (EOC) offer a critical way to measure and manage within the context of valuebased payment for medical services. An EOC is a group of clinically related services delivered to a patient over a period of time. Examples might be the term of a pregnancy culminating in the delivery, a knee replacement and rehab, management of a chronic condition such as diabetes or hypertension for a specific period, or treatment of an acute condition such as a stroke or heart attack. EOCs represent why patients interact with the health care system. They are the ultimate product upon which to measure value and organize resources to deliver that value. Under fee-for-service, health care providers measure and manage around the individual services they provide. The focus is on volume, revenue, cost, and efficiency of delivery in essence, a factory mentality. Service quality and customer satisfaction are important for a host of market and regulatory reasons. However, until recent value-based payment approaches were introduced, quality didn t hit the bottom line. In fact, under fee-for-service, additional services needed to compensate for poor quality, including readmissions, just create more revenue. The individual service or interaction is not the right way to measure value. EOC which looks at complete sequences of services and their outcome is the right way. EOC covers the intersection of care over time. If you really want to make changes and have a great health care system, you can t look at patients, diseases, and services piecemeal. EOC is a much better way to detail and analyze at how care is managed. July 2015 p. 2
3 How is the shift to value-based payment driving the use of EOC? As the name suggests, with value-based payment (VBP) models the payer reimburses the provider based on patient outcomes and value delivered, not on the services and resources expended. The shift is in direct response to market demand for lower health care costs, which have been on an unsustainable upward trajectory, while at the same time quality of care is still compromised by unnecessary variation, medical error, and readmissions. Quality care at reasonable cost is a major issue for the U.S. government, employers, and individual patients. Private and government insurers are responding by increasing the proportion of payment tied to quality, and while the cost of production is still important, the focus shifts to total cost of care and bending the cost curve for the population served. There are different approaches emerging for connecting payment to value: Bundled payment, where there is a flat fee for a given outcome (e.g., a hip replacement). Shared savings, where the payer and provider share the savings when a quality outcome is produced below estimated cost. Fully capitated accountable care, where the provider is paid for providing medical services to populations of patients. In all three cases, you need EOC to measure and analyze the quality and cost of outcomes. If a provider wants to assess its readiness for bundled payment or shared savings contracts, or determine how to price them, it needs EOC as the foundation of analysis. If a provider is managing an ACO population and wants to drive out unwarranted waste, it needs the clinically actionable insights from EOC analysis that take you beyond the baseline performance measures that everyone uses. July 2015 p. 3
4 How much momentum is there behind the shift to value-based payments? Many progressive providers have VBP pilots around specific treatments such as oncology care. In 2015, 20 major health systems and payers pledged to convert 75 percent of their business to value-based arrangements by Over 700 public and private Accountable Care Organizations (ACO) have been created since 2011 covering an estimated 23.5 million people, 7.8 million via Medicare. Those ACOs have saved Medicare $417 million and distributed shared savings payments to providers of $460 million. There are over 6,900 participants in the voluntary Bundled Payments for Care Improvement (BPCI) program, and CMS estimates that its proposed mandatory Comprehensive Care for Joint Replacement (CCJR) program will save $153 million over five years and impact 800 hospitals. We re getting close to critical mass. Medicare is helping drive the change in other ways as well. For example, the Kaiser Family Foundation estimates that CMS s Hospital Readmission Reduction Program will reduce payments by $428 million nationwide in 2015 on just five clinical conditions. As a result, all hospitals are measuring their quality in terms of readmission rates and are mobilizing resources to manage readmission risk so they don t get penalized financially. EOCs can help them do that. What specific kinds of insights are derived from EOC analysis? EOCs provide a better understanding and accounting for the products of the health care. Once you have EOC as a standard for analyzing care, you gain deeper insight into both cost and quality: How much variation is there in episode cost? What component and utilization costs drive the variation? Are there opportunities to shift patients to a better price point? How much variation is there in quality and outcomes? What care processes produce the best results? What are the opportunities to improve patient care pathways? July 2015 p. 4
5 With more actionable clinical information, providers can better engage clinicians and support staff in performance improvement activities. It s a lot easier to engage a clinician on quality than cost. EOCs also give providers a new lens for looking across a population of patients and understanding which clinical conditions are driving costs. As they manage and optimize the delivery of episodes, providers tend to standardize resources, reduce variation, and have more predictable operations. With greater stability and predictability, they can plan with greater confidence, whether for budgeting, facilities, resources, contract negotiations, or partnerships. Meanwhile, payers have the opportunity to gain insight into how care is being delivered across providers. Which providers have better cost and quality? Payers can share the feedback with providers and can reward providers based on comparative results. What are some specific use cases? Here are three examples: Analysis reveals that post-acute care is being delivered in inpatient rehabilitation facilities at a much higher rate than regional benchmarks and driving up cost. By implementing care pathways and protocols, providers can appropriately redirect patients requiring less intensive services to less expensive skilled nursing facilities. Another example is how EOC provides a standard for assessing variation and determining what amount of any particular service is warranted. Less variation in testing, imaging, doctor visits, inpatient stays, and so on will ultimately lead to less spending and a more stable process. When providers reduce unnecessary testing and treatment that also improves the experience and satisfaction of patients. Health care providers have scarce resources and must prioritize which clinical and operational projects to invest in. Opportunities identified by EOC analytics can help providers select projects with the greatest return. July 2015 p. 5
6 How is EOC enabling more predictive analytics? Once you have data within the context of EOC, you can look ahead in a variety of ways, for example: Risk scoring can be enhanced by assessing episode as well as patient risk. If you can identify a patient s likelihood of incurring adverse events and high costs across the entire episode, you can take preventive measures. Risk adjustment models can better predict patient cost given their unique conditions, severity of illness, and comorbidities. Aggregate forecasting can become more accurate: What s likely to happen with the population being managed? Treatment plans can be optimized: What would be the best course of action given various care options and patient condition and preferences? What are some of the implementation challenges? While payers are pushing for value-based payment, many providers are holding back for two main reasons. One, even among sophisticated providers, managing patients across the care continuum is still new. There is a significant amount of enabling organizational and administrative infrastructure required. For example, bundled payments look like a simplification, but in the short term they can complicate the transaction flow between provider and payer. Two, and perhaps most importantly, health systems run on narrow margins, and many prefer to take their chances under the status quo rather than risk losing money under new payment methods. That said, analyzing your clinical product line with EOC would be the first step to understanding exposure to financial risk and finding ways to increase market share and margins while July 2015 p. 6
7 avoiding risk. So providers should be using EOC both to make direct improvements to cost and care, and to prepare for and make the transition to value-based payment. What then are the challenges in implementing EOC? Lack of data and analytic infrastructure. If clinical and operational data are fragmented, you can t pull together the end-to-end view of EOC. And if you don t have the analytical tools and skills, you can t put the data to work. How should organizations go about putting EOC analytics capability in place? For starters, there are several key capabilities to consider: Episode definitions. What event triggers an episode? What services and diagnoses are included? What cost categories are used? What concludes an episode? You can use existing definitions (e.g., CMS BPCI, PROMETHEUS ECR) or create your own, but you ll want to maintain the flexibility to modify rules for defining an episode. Attribution rules. How will you assign ownership of the episode? What provider specifically will be held accountable for the case? Concurrent episodes. A patient may have multiple concurrent episodes (e.g., comes in for a hip replacement and develops gastric problems). You need to account for what s included in each episode. Output detail. EOC analysis can generate a lot of questions. It s helpful to have as much detail as possible to drill down into. Risk adjustment. EOC provides a more complete view of clinical activity, but it can t tell the whole story. For example, the severity of a patient s illness may impact cost and quality. Consider ways of risk adjusting your data and output. Then you need to understand the key steps for adopting EOC: Form an EOC analytics planning team aligned with key stakeholders. Define the scope of what you need to measure population, episodes, providers, time periods together with the data sources and analytic requirements. July 2015 p. 7
8 Plan the data and analytic infrastructure to implement EOC, with special attention to scalability you ll need computing power and an analytic solution that can grow with your business needs. Detail your implementation plan and roadmap. Then start piloting. You might begin with procedures or conditions in stronger clinically integrated programs (e.g., cardiology, orthopedics or oncology) where there s an opportunity to learn and improve, and where much of the needed data is available. What are the top things that provider organizations really need to know about EOC? First, the measures that you re currently using don t adequately capture how your clinical enterprise works. You really need to understand what s driving costs from a clinical perspective, and then use that information to engage providers, align resources, increase efficiencies, and optimize care. You need EOC to develop that capability it s a better unit of measure and analysis. Second, you need EOC to succeed in a market with value-based payments. You need the insight into your clinical costs and quality. Third-parties may aggregate a lot of useful comparative data for you, but you still need the means to learn and improve your operations, as well as to price services and negotiate contracts. Third, adopting EOC is a strategic business decision. Whether it s to support bundled payment, manage an ACO, or identify improvement opportunities, you re leveraging EOC to change how you measure and manage. July 2015 p. 8
9 What do analysts working on EOC applications need to know? Analysts need to appreciate the complexity. They are going to need to work very closely with their business partners as they work through the definitions of episodes and the analytics based on them. There are many decision points and clinical considerations. The analysts can t think of this as a one-time modeling project; it s an ongoing team effort with the business. Finally, what do payers need to keep in mind? Payers are pushing for value-based payment because that transfers financial risk to the providers. But they re not always making it easy for the providers. Some are partnering, while others are perceived to be using bundled payment as another way to drive down payment. Payers should recognize that they are sitting on an enormous amount of data that their provider partners have not seen before or have had limited access to. There is a real opportunity for payers to reach out to provide partners in support of care delivery as well as encouraging value-based payment. July 2015 p. 9
10 Additional Information To learn more about this topic, please visit sas.com/episodeanalytics. About the Interviewee J. Peter Chingos has over 25 years of experience in health care management, consulting and business analytics. Throughout his career, Peter has focused on large-scale, strategic initiatives to improve quality and efficiency in health care delivery. Prior to working at SAS, Peter managed an analytic consulting group at Health Dialog focused on provider opportunities under payment reform. He also managed a business intelligence team at Maine Medical Center responsible for clinical quality measurement. Peter has implemented decision support/cost accounting systems in hospitals nationwide and started his career at Massachusetts General Hospital coordinating clinical operations and managing performance improvement teams. Peter holds a BA from McGill University and an MBA in Health Care Management from Boston University. SAS and all other SAS Institute Inc. product or service names are registered trademarks or trademarks of SAS Institute Inc. in the USA and other countries. indicates USA registration. Other brand and product names are trademarks of their respective companies _S July 2015 p. 10
Healthcare Reform and Its Impact on the Care Delivery System
 Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
The Emergence of Value-Based Care: Present and Future Tense
 The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
White Paper. The Road to Value-Based Health Care. Revolutionizing Payment and Delivery Through Episode Analytics
 White Paper The Road to Value-Based Health Care Revolutionizing Payment and Delivery Through Episode Analytics Contents Executive Summary... 1 Value-Based Care: The Shifting Incentive and Its Adoption...
White Paper The Road to Value-Based Health Care Revolutionizing Payment and Delivery Through Episode Analytics Contents Executive Summary... 1 Value-Based Care: The Shifting Incentive and Its Adoption...
Using Analytics To Transform Your ACO
 Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
FMV Considerations for Bundled Payment Arrangements
 FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
Best Practices Value-Based Bundled Programs
 Best Practices Value-Based Bundled Programs From Strategy through Execution June 27, 2017 Value-based payments end-to-end impacts Strategy and governance Care delivery innovation and collaboration Unit
Best Practices Value-Based Bundled Programs From Strategy through Execution June 27, 2017 Value-based payments end-to-end impacts Strategy and governance Care delivery innovation and collaboration Unit
Payment Reform in Support of Population Health Management
 Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
In This Issue (click to jump):
 May 7, 2014 In This Issue (click to jump): Analysis of Trends in Health Spending 2013 2014 Spotlight on Medicare Advantage Enrollment Oncology Drug Trend Report S&P Predicts Shift from Job-Based Coverage
May 7, 2014 In This Issue (click to jump): Analysis of Trends in Health Spending 2013 2014 Spotlight on Medicare Advantage Enrollment Oncology Drug Trend Report S&P Predicts Shift from Job-Based Coverage
Stuart H. Altman. The Changing Health Care System: Economic Forces Pushing States To Become More Involved
 The Changing Health Care System: Economic Forces Pushing States To Become More Involved Stuart H. Altman Sol Chaikin Professor of Health Policy The Heller School for Social Policy and Management Brandeis
The Changing Health Care System: Economic Forces Pushing States To Become More Involved Stuart H. Altman Sol Chaikin Professor of Health Policy The Heller School for Social Policy and Management Brandeis
Value Based Contracting
 Value Based Contracting CONCEPTS FOR THE MEDICAL PRACTICE dhgllp.com/healthcare 225 Peachtree Street NE, Suite 600 Atlanta, GA 30303 Bill Hannah PRINCIPAL Bill.Hannah@dhgllp.com 404.575.8921 Doral Davis-Jacobsen
Value Based Contracting CONCEPTS FOR THE MEDICAL PRACTICE dhgllp.com/healthcare 225 Peachtree Street NE, Suite 600 Atlanta, GA 30303 Bill Hannah PRINCIPAL Bill.Hannah@dhgllp.com 404.575.8921 Doral Davis-Jacobsen
HEALTH POLICY & EDUCATION SERIES
 HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
CNYCC Joint Board and Finance Committee Forum
 1 CNYCC Joint Board and Finance Committee Forum December 1, 2015 Michael Bailit Bailit Health 2 Meeting Agenda 1. Value-Based Payment Overview Environmental Context New York State Roadmap DSRIP Payment
1 CNYCC Joint Board and Finance Committee Forum December 1, 2015 Michael Bailit Bailit Health 2 Meeting Agenda 1. Value-Based Payment Overview Environmental Context New York State Roadmap DSRIP Payment
DELIVERING HIGHER-VALUE MATERNITY CARE
 DELIVERING HIGHER-VALUE MATERNITY CARE Designing Alternative Payment Models for Better Care, Lower Spending, and Financially Viable Maternity Care Providers Harold D. Miller President and CEO Center for
DELIVERING HIGHER-VALUE MATERNITY CARE Designing Alternative Payment Models for Better Care, Lower Spending, and Financially Viable Maternity Care Providers Harold D. Miller President and CEO Center for
The Case For Value ACA to MACRA to MIPS
 The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
A Practical Discussion of Value and Quality Based Payments What Do I Do Now?
 Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
CF Health Advisors: Partner Biographies
 The Evolving Healthcare Landscape C F H E A LT H A D V I S O R S S E P T E M B E R, 2 0 1 6 CF Health Advisors: Partner Biographies CHARLENE FRIZZERA President and CEO JEREMY BROWN Managing Partner Former
The Evolving Healthcare Landscape C F H E A LT H A D V I S O R S S E P T E M B E R, 2 0 1 6 CF Health Advisors: Partner Biographies CHARLENE FRIZZERA President and CEO JEREMY BROWN Managing Partner Former
Demystifying Hospital Readmissions Penalties
 Financial Leadership Council Research Note August 1, 2016 Demystifying Hospital Readmissions Penalties Commonly Asked Questions from Hospital CFOs Highlights Readmissions penalties will likely get larger
Financial Leadership Council Research Note August 1, 2016 Demystifying Hospital Readmissions Penalties Commonly Asked Questions from Hospital CFOs Highlights Readmissions penalties will likely get larger
Health care affordability VBC transformation
 Health care affordability VBC transformation What s at stake? The cost of health care in the United States has been on an unsustainable rise for some time, driven by fundamental delivery and financing
Health care affordability VBC transformation What s at stake? The cost of health care in the United States has been on an unsustainable rise for some time, driven by fundamental delivery and financing
Considerations for a Hospital-Based ACO. Insurance Premium Construction: Tim Smith, ASA, MAAA, MS
 Insurance Premium Construction: Considerations for a Hospital-Based ACO Tim Smith, ASA, MAAA, MS I once saw a billboard advertising a new insurance product co-branded by the local hospital system and a
Insurance Premium Construction: Considerations for a Hospital-Based ACO Tim Smith, ASA, MAAA, MS I once saw a billboard advertising a new insurance product co-branded by the local hospital system and a
Initiative Options for Simulation Scenarios
 Initiative Options for Simulation Scenarios The following options are in version 2h of the ReThink Health simulation model. Enable healthier behaviors Promote healthy behavior and help people to stop behaviors
Initiative Options for Simulation Scenarios The following options are in version 2h of the ReThink Health simulation model. Enable healthier behaviors Promote healthy behavior and help people to stop behaviors
Avalere Health 2015 Industry Outlook
 2015 Industry Outlook 2 Introduction Industry Outlook 2015 Changes in healthcare financing, delivery, and organization are transforming the sector. Health plans and providers are revising their business
2015 Industry Outlook 2 Introduction Industry Outlook 2015 Changes in healthcare financing, delivery, and organization are transforming the sector. Health plans and providers are revising their business
Advanced Analytics. The key to unlocking the Triple Aim and Value-Based Purchasing. Ines Vigil MD, MPH, MBA
 Advanced Analytics The key to unlocking the Triple Aim and Value-Based Purchasing Ines Vigil MD, MPH, MBA Advanced Analytics: The key to unlocking the Triple Aim and Value-Based Purchasing Current State
Advanced Analytics The key to unlocking the Triple Aim and Value-Based Purchasing Ines Vigil MD, MPH, MBA Advanced Analytics: The key to unlocking the Triple Aim and Value-Based Purchasing Current State
Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]
![Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701] Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]](/thumbs/87/96500790.jpg) Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
Eight Indispensable Financial Considerations of Shifting from Volume to Value Reimbursement
 Eight Indispensable Financial Considerations of Shifting from Volume to Value Reimbursement September 25-26, 2017 Max Reiboldt, CPA President CEO Learning Objectives This session will provide you with
Eight Indispensable Financial Considerations of Shifting from Volume to Value Reimbursement September 25-26, 2017 Max Reiboldt, CPA President CEO Learning Objectives This session will provide you with
MN DEPARTMENT OF HEALTH PROVIDER PEER GROUPING (PPG) ADVISORY GROUP DEFINING PARAMETERS ANN ROBINOW
 MN DEPARTMENT OF HEALTH PROVIDER PEER GROUPING (PPG) ADVISORY GROUP DEFINING PARAMETERS ANN ROBINOW MEETING 2: JUNE 26, 2009 Introduction Comments and changes to meeting summary? Review of questions or
MN DEPARTMENT OF HEALTH PROVIDER PEER GROUPING (PPG) ADVISORY GROUP DEFINING PARAMETERS ANN ROBINOW MEETING 2: JUNE 26, 2009 Introduction Comments and changes to meeting summary? Review of questions or
than value. infrastructure for value-based payment, it is apparent that greater assumption of
 EXECUTIVE BRIEFING Value-Based Contracting: How to Think Like a Payer It is widely recognized that the rate of healthcare spending in the U.S. is unsustainable. In recent years, experts of all types, from
EXECUTIVE BRIEFING Value-Based Contracting: How to Think Like a Payer It is widely recognized that the rate of healthcare spending in the U.S. is unsustainable. In recent years, experts of all types, from
The Health Insurance Market in Virginia. Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017
 The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
Integrating Population Health Analytics and the EHR Environment Session 87, March 6, 2018
 Integrating Population Health Analytics and the EHR Environment Session 87, March 6, 2018 Nina M. Taggart, MD, Senior Medical Director, Population Health and Payer Relations, Lehigh Valley Health Network
Integrating Population Health Analytics and the EHR Environment Session 87, March 6, 2018 Nina M. Taggart, MD, Senior Medical Director, Population Health and Payer Relations, Lehigh Valley Health Network
Rewarding High Quality: Practical Models for Value- Based Physician Payment
 Rewarding High Quality: Practical Models for Value- Based Physician Payment Introduction In its 2013 report, Moving Beyond Fee-for-Service, the Alliance of Community Health Plans (ACHP) addressed the increasing
Rewarding High Quality: Practical Models for Value- Based Physician Payment Introduction In its 2013 report, Moving Beyond Fee-for-Service, the Alliance of Community Health Plans (ACHP) addressed the increasing
FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS
 CENTER FOR INDUSTRY TRANSFORMATION MAY 2015 FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS Authors Amy Bibby Partner, DHG Healthcare amy.bibby@dhgllp.com Matthew Fadel Manager, DHG Healthcare matt.fadel@dhgllp.com
CENTER FOR INDUSTRY TRANSFORMATION MAY 2015 FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS Authors Amy Bibby Partner, DHG Healthcare amy.bibby@dhgllp.com Matthew Fadel Manager, DHG Healthcare matt.fadel@dhgllp.com
Journey To Value: The State of Value-Based Reimbursement
 White Paper Journey To Value: The State of Value-Based Reimbursement Second in a series of national research studies on healthcare s transition from volume to value, conducted by ORC International and
White Paper Journey To Value: The State of Value-Based Reimbursement Second in a series of national research studies on healthcare s transition from volume to value, conducted by ORC International and
Population-Based Healthcare: Structural Models and Options
 Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Prospective vs. Retrospective. Will Bundled Payment Really Be.. Fee For Service
 Fee For Service Episode Based Payment: Are You Ready For Medicare s Next Wave of Provider Payment Reform? Payer Robert Mechanic, MBA The Estes Park Institute January 30, 2012 Hospital Surgeon Specialist
Fee For Service Episode Based Payment: Are You Ready For Medicare s Next Wave of Provider Payment Reform? Payer Robert Mechanic, MBA The Estes Park Institute January 30, 2012 Hospital Surgeon Specialist
THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION
 THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION HFMA First Illinois Chapter August 12, 2014 Stu Schaff Manager, DGA Partners Agenda > Background & Context > Measures
THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION HFMA First Illinois Chapter August 12, 2014 Stu Schaff Manager, DGA Partners Agenda > Background & Context > Measures
21% Total Medicare Beneficiaries (2017): 58 million
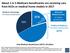 About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
Medicare Advantage Value-Based Insurance Design: Considerations and implications
 White paper Medicare Advantage Value-Based Insurance Design: Considerations and implications Health plans and providers are slowly moving away from traditional provider payment systems to a more innovative
White paper Medicare Advantage Value-Based Insurance Design: Considerations and implications Health plans and providers are slowly moving away from traditional provider payment systems to a more innovative
Building the Healthcare System of the Future O R A C L E W H I T E P A P E R F E B R U A R Y
 Building the Healthcare System of the Future O R A C L E W H I T E P A P E R F E B R U A R Y 2 0 1 7 Introduction Healthcare in the United States is changing rapidly. An aging population has increased
Building the Healthcare System of the Future O R A C L E W H I T E P A P E R F E B R U A R Y 2 0 1 7 Introduction Healthcare in the United States is changing rapidly. An aging population has increased
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business?
 Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
AAOS MACRA Proposed Rule Summary (Short)
 AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
Healthcare Finance Trends and Perspectives
 Healthcare Finance Trends and Perspectives AONE Annual Conference, Fort Worth, TX April 2 nd, 2016 Chuck Alsdurf, MAcc, CPA Director, Healthcare Finance Policy, Operational Initiatives Healthcare Financial
Healthcare Finance Trends and Perspectives AONE Annual Conference, Fort Worth, TX April 2 nd, 2016 Chuck Alsdurf, MAcc, CPA Director, Healthcare Finance Policy, Operational Initiatives Healthcare Financial
A.J. Yates, Jr., MD Chief of Orthopaedic Surgery UPMC Shadyside Associate Professor Vice Chairman for Quality Management UPMC Department of
 Creation of Value The CJR: Bundled Care in Arthroplasty A.J. Yates, Jr., MD Chief of Orthopaedic Surgery UPMC Shadyside Associate Professor Vice Chairman for Quality Management UPMC Department of Orthopaedic
Creation of Value The CJR: Bundled Care in Arthroplasty A.J. Yates, Jr., MD Chief of Orthopaedic Surgery UPMC Shadyside Associate Professor Vice Chairman for Quality Management UPMC Department of Orthopaedic
Affordable Care Act Update: Implementing Medicare Costs Savings
 Affordable Care Act Update: Implementing Medicare Costs Savings This new law recognizes that Medicare isn t just something that you re entitled to when you reach 65; it s something that you ve earned.
Affordable Care Act Update: Implementing Medicare Costs Savings This new law recognizes that Medicare isn t just something that you re entitled to when you reach 65; it s something that you ve earned.
Value-Based Payments (VBP)
 Value-Based Payments (VBP) Overview September 27, 2016 September 27, 2016 2 NYS What is Value Based Payment? NYS Timeline VBP Outcomes and Levels P4P vs. VBP VBP Overview Agenda MCTAC VBP Arrangements
Value-Based Payments (VBP) Overview September 27, 2016 September 27, 2016 2 NYS What is Value Based Payment? NYS Timeline VBP Outcomes and Levels P4P vs. VBP VBP Overview Agenda MCTAC VBP Arrangements
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making. Introduction. William Bednar, FSA, FCA, MAAA
 Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
Catalyzing Payment Innovation. Suzanne Delbanco, Ph.D. Executive Director September 20, 2012
 Catalyzing Payment Innovation Suzanne Delbanco, Ph.D. Executive Director September 20, 2012 Payment Reform: Why Should We Care? The health care payment systems of the status quo continue to drain the value
Catalyzing Payment Innovation Suzanne Delbanco, Ph.D. Executive Director September 20, 2012 Payment Reform: Why Should We Care? The health care payment systems of the status quo continue to drain the value
CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives
 CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives Presented by: Peter R. Epp, CPA S e p t e m b e r 2 9, 2 0 1 6 HMA I n t r o d u c t i o n One of the overarching objectives
CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives Presented by: Peter R. Epp, CPA S e p t e m b e r 2 9, 2 0 1 6 HMA I n t r o d u c t i o n One of the overarching objectives
Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models
 Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models Kristina Rollings Product Director, Emerging Solutions March 24, 2014 Agenda 1. State of the
Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models Kristina Rollings Product Director, Emerging Solutions March 24, 2014 Agenda 1. State of the
Global Payments to Improve Quality and Efficiency in Medicaid:
 Global Payments to Improve Quality and Efficiency in Medicaid: Concepts and Considerations November 2009 Prepared for the Massachusetts Medicaid Policy Institute by Mark Heit and Kip Piper Sellers Dorsey
Global Payments to Improve Quality and Efficiency in Medicaid: Concepts and Considerations November 2009 Prepared for the Massachusetts Medicaid Policy Institute by Mark Heit and Kip Piper Sellers Dorsey
10 Best Practices For Payer Contracting:
 10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. 2016 NHIA Annual Conference & Exposition 1 Speaker Disclosures Steve Selbst is employed by
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. 2016 NHIA Annual Conference & Exposition 1 Speaker Disclosures Steve Selbst is employed by
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations
 10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. Speaker Disclosures Steve Selbst is employed by a business firm that provides services related
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. Speaker Disclosures Steve Selbst is employed by a business firm that provides services related
What s Next for MSSP ACOs? The Case for Moving to Medicare Risk
 What s Next for MSSP ACOs? The Case for Moving to Medicare Risk Picking Your Path on a Journey Towards Value-Based Care Participants in one of Medicare s boldest attempts to overhaul how doctors and physicians
What s Next for MSSP ACOs? The Case for Moving to Medicare Risk Picking Your Path on a Journey Towards Value-Based Care Participants in one of Medicare s boldest attempts to overhaul how doctors and physicians
Value Based Purchasing. RHP 9 Learning Collaborative February 22, 2017
 Value Based Purchasing RHP 9 Learning Collaborative February 22, 2017 Purpose Dialogue with RHP stakeholders on the following topics: What Value Based Purchasing (VBP) is and why HHSC is promoting it VBP
Value Based Purchasing RHP 9 Learning Collaborative February 22, 2017 Purpose Dialogue with RHP stakeholders on the following topics: What Value Based Purchasing (VBP) is and why HHSC is promoting it VBP
Providers involved in the Centers for Medicare & Medicaid Services ACE demonstration project share
 Pursuing Bundled Payments Lessons from the ACE Demonstration Providers involved in the Centers for Medicare & Medicaid Services ACE demonstration project share lessons learned from their experiences in
Pursuing Bundled Payments Lessons from the ACE Demonstration Providers involved in the Centers for Medicare & Medicaid Services ACE demonstration project share lessons learned from their experiences in
Summary of proposed rule provisions for Accountable Care Organizations under the Medicare Shared Savings Program
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
From Silos to Services for Value-Based Care
 White Paper From Silos to Services for Value-Based Care Author Amy Larsson, RN, BSN, MBA Vice President, Clinical Claims Management, Change Healthcare A bundled payment program built by hand 25 years ago
White Paper From Silos to Services for Value-Based Care Author Amy Larsson, RN, BSN, MBA Vice President, Clinical Claims Management, Change Healthcare A bundled payment program built by hand 25 years ago
aligning managed care contracts, compensation plans, and incentive models
 REPRINT NOVEMBER 2011 Michael E. Nugent healthcare financial management association www.hfma.org aligning managed care contracts, compensation plans, and incentive models Providers should take the lead
REPRINT NOVEMBER 2011 Michael E. Nugent healthcare financial management association www.hfma.org aligning managed care contracts, compensation plans, and incentive models Providers should take the lead
This is a sample of the instructor materials for The Core Elements of Value in Healthcare, by Paveljit S. Bindra.
 This is a sample of the instructor materials for The Core Elements of Value in Healthcare, by Paveljit S. Bindra. The complete instructor materials include the following: Test bank PowerPoint slides for
This is a sample of the instructor materials for The Core Elements of Value in Healthcare, by Paveljit S. Bindra. The complete instructor materials include the following: Test bank PowerPoint slides for
Note: This is an authorized excerpt from 2015 Healthcare Benchmarks: Value-Based Reimbursement. To download the entire report, go to
 Note: This is an authorized excerpt from 2015 Healthcare Benchmarks: Value-Based Reimbursement. To download the entire report, go to http://store.hin.com/product.asp?itemid=5088 or call 888-446-3530. 2015
Note: This is an authorized excerpt from 2015 Healthcare Benchmarks: Value-Based Reimbursement. To download the entire report, go to http://store.hin.com/product.asp?itemid=5088 or call 888-446-3530. 2015
PREPARING FOR THE NEXT GENERATION OF MANAGED CARE CONTRACTING
 PREPARING FOR THE NEXT GENERATION OF MANAGED CARE CONTRACTING Nanci Robertson, RN BSN President - Robertson Consulting, Inc. Doral Jacobsen, MBA FACMPE CEO - Prosper Beyond, Inc. DORAL JACOBSEN AND NANCI
PREPARING FOR THE NEXT GENERATION OF MANAGED CARE CONTRACTING Nanci Robertson, RN BSN President - Robertson Consulting, Inc. Doral Jacobsen, MBA FACMPE CEO - Prosper Beyond, Inc. DORAL JACOBSEN AND NANCI
Predictive Analytics and Technology Session
 Predictive Analytics and Technology Session Eric Widen, CEO HBI Solutions Population Health Colloquium March 28 th, 2017 HBI Solutions Session Agenda Introductions and Overview Eric Widen Session 1: Michael
Predictive Analytics and Technology Session Eric Widen, CEO HBI Solutions Population Health Colloquium March 28 th, 2017 HBI Solutions Session Agenda Introductions and Overview Eric Widen Session 1: Michael
The Health Management Academy Strategic Survey Q1 2019: Defining Risk. March 2019
 The Health Management Academy Strategic Survey Q1 2019: Defining Risk March 2019 1 Defining Risk In 2019, the U.S. healthcare market is poised to continue its march towards value-based care. In the context
The Health Management Academy Strategic Survey Q1 2019: Defining Risk March 2019 1 Defining Risk In 2019, the U.S. healthcare market is poised to continue its march towards value-based care. In the context
Volume to Value The Great Transformation of American Medicine
 Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers
 Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers Montana Chamber of Commerce Healthcare Forum November 29-30, 2016 Shane Wolverton SVP CORPORATE DEVELOPMENT, QUANTROS
Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers Montana Chamber of Commerce Healthcare Forum November 29-30, 2016 Shane Wolverton SVP CORPORATE DEVELOPMENT, QUANTROS
The New York State Value-Based Payment (VBP) Roadmap. Behavioral Health Providers January 30, 2018
 The New York State Value-Based Payment (VBP) Roadmap Behavioral Health Providers January 30, 2018 1 Housekeeping All lines have been muted To ask a question at any time, use the Chat feature in WebEx We
The New York State Value-Based Payment (VBP) Roadmap Behavioral Health Providers January 30, 2018 1 Housekeeping All lines have been muted To ask a question at any time, use the Chat feature in WebEx We
Vertical Integration Trends and Impacts: (a) Physicians & Hospitals (b) Payers & Providers
 Vertical Integration Trends and Impacts: (a) Physicians & Hospitals (b) Payers & Providers Lawton Robert Burns, Ph.D., MBA The James Joo-Jin Kim Professor Department of Health Care Management The Wharton
Vertical Integration Trends and Impacts: (a) Physicians & Hospitals (b) Payers & Providers Lawton Robert Burns, Ph.D., MBA The James Joo-Jin Kim Professor Department of Health Care Management The Wharton
How the Affordable Care Act Is Changing Healthcare What You Can Do to Thrive in the New Environment
 How the Affordable Care Act Is Changing Healthcare What You Can Do to Thrive in the New Environment David N. Gans MSHA, FACMPE, Senior Fellow, Industry Affairs MGMA-ACMPE Disclosure No financial relationships
How the Affordable Care Act Is Changing Healthcare What You Can Do to Thrive in the New Environment David N. Gans MSHA, FACMPE, Senior Fellow, Industry Affairs MGMA-ACMPE Disclosure No financial relationships
How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments?
 How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments? 1:10 PM 2:10 PM Steering Toward Success: Achieving Value in Whole Person Care September 25 and
How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments? 1:10 PM 2:10 PM Steering Toward Success: Achieving Value in Whole Person Care September 25 and
BUNDLED PAYMENTS IN RADIATION ONCOLOGY
 BUNDLED PAYMENTS IN RADIATION ONCOLOGY CASE STUDIES IN INNOVATIVE SPECIALIST VALUE-BASED PAYMENT INITIATIVES: SPECIALTY PAYMENT REFORMS THAT REDUCE THE COSTS OF PROCEDURES Constantine Mantz MD Chief Medical
BUNDLED PAYMENTS IN RADIATION ONCOLOGY CASE STUDIES IN INNOVATIVE SPECIALIST VALUE-BASED PAYMENT INITIATIVES: SPECIALTY PAYMENT REFORMS THAT REDUCE THE COSTS OF PROCEDURES Constantine Mantz MD Chief Medical
Improving health care affordability Helping health plans bend the cost curve
 Improving health care affordability Helping health plans bend the cost curve What s at stake? After years of escalating costs, US health care has become unaffordable for many. Industry stakeholders, including
Improving health care affordability Helping health plans bend the cost curve What s at stake? After years of escalating costs, US health care has become unaffordable for many. Industry stakeholders, including
MedTech Innovation Amid Changing Dynamics for Insurers, Hospitals, and Consumers
 MedTech Innovation Amid Changing Dynamics for Insurers, Hospitals, and Consumers Deutsche Bank Medtech Boot Camp March 21, 2016 James C. Robinson Leonard D. Schaeffer Professor of Health Economics Director,
MedTech Innovation Amid Changing Dynamics for Insurers, Hospitals, and Consumers Deutsche Bank Medtech Boot Camp March 21, 2016 James C. Robinson Leonard D. Schaeffer Professor of Health Economics Director,
Risky Business: Capitated Financing in the Dual Eligible Demonstration Projects
 Risky Business: Capitated Financing in the Dual Eligible Demonstration Projects Ellen Breslin Davidson and Tony Dreyfus BD Group Community Catalyst, Inc. 30 Winter St. 10 th Floor Boston, MA 02108 617.338.6035
Risky Business: Capitated Financing in the Dual Eligible Demonstration Projects Ellen Breslin Davidson and Tony Dreyfus BD Group Community Catalyst, Inc. 30 Winter St. 10 th Floor Boston, MA 02108 617.338.6035
Journal of Pharmaceutical Care & Health Systems
 Journal of Pharmaceutical Care & Health Systems Sheiman, 2016, 3:2 http://dx.doi.org/10.4172/2376-0419.1000154 Review Article Open Access Payment Methods for Integration: Typology, Evidence and Pre-conditions
Journal of Pharmaceutical Care & Health Systems Sheiman, 2016, 3:2 http://dx.doi.org/10.4172/2376-0419.1000154 Review Article Open Access Payment Methods for Integration: Typology, Evidence and Pre-conditions
Lehigh Valley Health Network
 Lehigh Valley Health Network Journey to Accountable Care November 19, 2014 Powered by Populytics Lehigh Valley Health Network Fast Facts In Allentown/Bethlehem area, north of Philadelphia Recognized by
Lehigh Valley Health Network Journey to Accountable Care November 19, 2014 Powered by Populytics Lehigh Valley Health Network Fast Facts In Allentown/Bethlehem area, north of Philadelphia Recognized by
AMGA MIPS Collaborative. June 21, 2017
 AMGA MIPS Collaborative June 21, 2017 Calculating the MIPS score The MIPS composite performance score will include four weighted categories: MIPS Composite Performance Score Quality Cost Improvement activities
AMGA MIPS Collaborative June 21, 2017 Calculating the MIPS score The MIPS composite performance score will include four weighted categories: MIPS Composite Performance Score Quality Cost Improvement activities
Today s Payers and Providers
 Today s Payers and Providers Strategies for Success Emad Rizk, MD President and Chief Executive Officer Accretive Health Session Objectives Description of value based models in the market Data elements
Today s Payers and Providers Strategies for Success Emad Rizk, MD President and Chief Executive Officer Accretive Health Session Objectives Description of value based models in the market Data elements
FROM SILOS TO SERVICES FOR VALUE-BASED CARE
 White Paper FROM SILOS TO SERVICES FOR VALUE-BASED CARE A bundled payment program built by hand 25 years ago is still delivering lessons for HIT today By Amy Larsson RN, BSN, MBA, Vice President, Clinical
White Paper FROM SILOS TO SERVICES FOR VALUE-BASED CARE A bundled payment program built by hand 25 years ago is still delivering lessons for HIT today By Amy Larsson RN, BSN, MBA, Vice President, Clinical
Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study
 Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study Presented by Bill O Brien, FSA, MAAA Consulting Actuary Milliman Houston, TX (832) 878-4078 Preconference I Agenda
Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study Presented by Bill O Brien, FSA, MAAA Consulting Actuary Milliman Houston, TX (832) 878-4078 Preconference I Agenda
How Bundled Payments Create Value in New Product Designs Cognizant
 How Bundled Payments Create Value in New Product Designs 1 About Cognizant 2 This Will Not Take Long. 3 What is a Health Insurance Product? 4 Understanding Product Design Commercial Insurance One specific
How Bundled Payments Create Value in New Product Designs 1 About Cognizant 2 This Will Not Take Long. 3 What is a Health Insurance Product? 4 Understanding Product Design Commercial Insurance One specific
THE FUTURE OF HEALTHCARE: TRENDS THAT WILL AFFECT YOUR PROFESSIONAL AND PERSONAL LIFE
 THE FUTURE OF HEALTHCARE: TRENDS THAT WILL AFFECT YOUR PROFESSIONAL AND PERSONAL LIFE Dr. Keith Hornberger, BSRT, MBA, DHA, FACHE 1 The Future Direction of Healthcare Healthcare Reform will catalyze a
THE FUTURE OF HEALTHCARE: TRENDS THAT WILL AFFECT YOUR PROFESSIONAL AND PERSONAL LIFE Dr. Keith Hornberger, BSRT, MBA, DHA, FACHE 1 The Future Direction of Healthcare Healthcare Reform will catalyze a
BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities
 BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities A Presentation for the ACC April 3, 2018 Christopher J. Donovan Partner Foley & Lardner LLP C. Frederick (Fred) Geilfuss
BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities A Presentation for the ACC April 3, 2018 Christopher J. Donovan Partner Foley & Lardner LLP C. Frederick (Fred) Geilfuss
2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet
 2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet
 2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
Point of View: Medicare Profitability in a Reform Market
 Point of View: Profitability in a Reform Market Bill Eggbeer, Managing Director, & Krista Bowers, Director, BDC Advisors, LLC Introduction Overall, accounts for approximately 20% of the total domestic
Point of View: Profitability in a Reform Market Bill Eggbeer, Managing Director, & Krista Bowers, Director, BDC Advisors, LLC Introduction Overall, accounts for approximately 20% of the total domestic
Fee for Service: Paying for Volume, Not Value
 Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
March 28, Dear Administrator Slavitt:
 20555 Victor Parkway Livonia, MI 48152 tel 734-343-1000 trinity-health.org March 28, 2016 Andy Slavitt Administrator Center for Medicare and Medicaid Services U.S. Department of Health and Human Services
20555 Victor Parkway Livonia, MI 48152 tel 734-343-1000 trinity-health.org March 28, 2016 Andy Slavitt Administrator Center for Medicare and Medicaid Services U.S. Department of Health and Human Services
How Health Reform Saves Consumers and Taxpayers Money
 How Health Reform Saves Consumers and Taxpayers Money The Affordable Care Act Lowers Costs and Improves Quality June Health reform s three major goals insurance reform, affordable coverage, and slower
How Health Reform Saves Consumers and Taxpayers Money The Affordable Care Act Lowers Costs and Improves Quality June Health reform s three major goals insurance reform, affordable coverage, and slower
Changes to Medicare under the Affordable Care Act
 January, 2017 siepr.stanford.edu Stanford Institute for Policy Brief Changes to Medicare under the Affordable Care Act By Jack Davidson and Jonathan Levin The Affordable Care Act (ACA) made substantial
January, 2017 siepr.stanford.edu Stanford Institute for Policy Brief Changes to Medicare under the Affordable Care Act By Jack Davidson and Jonathan Levin The Affordable Care Act (ACA) made substantial
Ready, Risk, Reward: Aligning for Success with the Second Generation of Clinically Integrated Networks
 Consulting Ready, Risk, Reward: Aligning for Success with the Second Generation of Clinically Integrated Networks This white paper provides an in-depth look at the future of clinically integrated networks
Consulting Ready, Risk, Reward: Aligning for Success with the Second Generation of Clinically Integrated Networks This white paper provides an in-depth look at the future of clinically integrated networks
5 critical issues for BPCI-A
 REPRINT June 2018 John M. Harris Molly Johnson Amanda Brown healthcare financial management association hfma.org 5 critical issues for BPCI-A Many hospitals and health systems may benefit from participation
REPRINT June 2018 John M. Harris Molly Johnson Amanda Brown healthcare financial management association hfma.org 5 critical issues for BPCI-A Many hospitals and health systems may benefit from participation
MGMA National MGMA18 The Annual Conference September, 2018 Attendee Form
 MGMA National MGMA18 The Annual Conference September, 2018 Attendee Form Title CEU Code CEUs Specialty MGMA18 The Annual Conference-PRE102 Designing and Building Processes for Value-based Healthcare 5
MGMA National MGMA18 The Annual Conference September, 2018 Attendee Form Title CEU Code CEUs Specialty MGMA18 The Annual Conference-PRE102 Designing and Building Processes for Value-based Healthcare 5
Healthcare Financial Management Association Certification Program. Module I: The Business of Health Care Learner s Guide
 Healthcare Financial Management Association Certification Program Module I: The Business of Health Care Learner s Guide For examination period beginning June 2015 1 Course 1 - The Big Picture Learning
Healthcare Financial Management Association Certification Program Module I: The Business of Health Care Learner s Guide For examination period beginning June 2015 1 Course 1 - The Big Picture Learning
MACRA: APPLICATIONS & IMPLICATIONS September 13, /13/2016. Mark Blessing, CPA, FHFMA Partner
 MACRA: APPLICATIONS & IMPLICATIONS September 13, 2016 Mark Blessing, CPA, FHFMA Partner mblessing@bkd.com Zach Remmich Managing Consultant zremmich@bkd.com 1 TO RECEIVE CPE CREDIT Participate in entire
MACRA: APPLICATIONS & IMPLICATIONS September 13, 2016 Mark Blessing, CPA, FHFMA Partner mblessing@bkd.com Zach Remmich Managing Consultant zremmich@bkd.com 1 TO RECEIVE CPE CREDIT Participate in entire
Insight to Value-Based Care and A Joint Venture Case Study. Whitney Courser SVP, Sales and Marketing
 Insight to Value-Based Care and A Joint Venture Case Study Whitney Courser SVP, Sales and Marketing WCourser@nuehealth.com Meet NueHealth 22-year-old, privately held, nationally trusted healthcare partner
Insight to Value-Based Care and A Joint Venture Case Study Whitney Courser SVP, Sales and Marketing WCourser@nuehealth.com Meet NueHealth 22-year-old, privately held, nationally trusted healthcare partner
When the Dust Settles-What s Next?
 When the Dust Settles-What s Next? AMA IPPS Conference Robert Nesse M.D. Senior Director of Payment Reform Mayo Clinic nesse.robert@mayo.edu What is Driving the Change in Healthcare? Common Belief: The
When the Dust Settles-What s Next? AMA IPPS Conference Robert Nesse M.D. Senior Director of Payment Reform Mayo Clinic nesse.robert@mayo.edu What is Driving the Change in Healthcare? Common Belief: The
Milliman Healthcare Services
 Milliman Healthcare Services Milliman Introduction About Milliman Milliman is the leader in providing actuarial consulting services to the health industry. We also develop and maintain sophisticated healthcare
Milliman Healthcare Services Milliman Introduction About Milliman Milliman is the leader in providing actuarial consulting services to the health industry. We also develop and maintain sophisticated healthcare
MACRAnomics. Patient-Level Economics and Strategic Implications for Providers. Presented to: NW Ohio HFMA October 20, 2016
 MACRAnomics Patient-Level Economics and Strategic Implications for Providers Presented to: NW Ohio HFMA October 20, 2016 Property of HealthScape Advisors Strictly Confidential 2 MACRAnomics: Objectives
MACRAnomics Patient-Level Economics and Strategic Implications for Providers Presented to: NW Ohio HFMA October 20, 2016 Property of HealthScape Advisors Strictly Confidential 2 MACRAnomics: Objectives
2017 EMPLOYER SERIES. 6 Things Employers Need to Know About Rising Health Care Costs. Cost Management Key Findings
 2017 EMPLOYER SERIES 6 Things Employers Need to Know About Rising Health Care Costs Cost Management 2017 Key Findings It s one of the biggest challenges employers face today: keeping health care costs
2017 EMPLOYER SERIES 6 Things Employers Need to Know About Rising Health Care Costs Cost Management 2017 Key Findings It s one of the biggest challenges employers face today: keeping health care costs
December COMMUNITY CHECKUP CHART PACK
 December 2017 2017 COMMUNITY CHECKUP CHART PACK 2 Washington State Performance for Commercially Insured as Compared to NCQA National Benchmarks 3 Washington State Performance for Medicaid Insured as Compared
December 2017 2017 COMMUNITY CHECKUP CHART PACK 2 Washington State Performance for Commercially Insured as Compared to NCQA National Benchmarks 3 Washington State Performance for Medicaid Insured as Compared
Final Rule Summary. Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, December 31, 2021
 Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
Accountable Care Organizations and Alternative Payment Methods Opportunities for Community Health Workers
 Accountable Care Organizations and Alternative Payment Methods Opportunities for Community Health Workers May 11, 2017 The 8 th Annual Community Health Worker/Patient Navigator Conference Katharine London,
Accountable Care Organizations and Alternative Payment Methods Opportunities for Community Health Workers May 11, 2017 The 8 th Annual Community Health Worker/Patient Navigator Conference Katharine London,
