Access the Manage Office tab and locate Eligibility Settings in the Company Settings section
|
|
|
- Amber Green
- 6 years ago
- Views:
Transcription
1 Eligibility Verification Instructions for Use Once you have completed the Eligibility Verification User Agreement and Office Ally has linked your account you must complete the Eligibility Settings in Manage Office. To complete the set-ups: Access the Manage Office tab and locate Eligibility Settings in the Company Settings section From the Eligibility Settings link you may designate the default settings for the program to automatically process the eligibility verifications for your office. They are as follows: Activate Eligibility for all Patients: Click Activate to set the flag for all patients in your program. Through the Manage Patient record, you may deselect patients you do not want to verify eligibility on. If you do not wish to activate all patients, you may individually select the patients through their Manage Patient record. Deactivate Eligibility for all Patients: Click Deactivate to remove the flag for all patients in your program. Through the Manage Patient record, you may select patients you do want to verify eligibility on. If you do not wish to deactivate all patients, you may individually select the patients through their Manage Patient record. Time Zone: Click the drop down and select the time zone for your office location. Eligibility Check Frequency: Allows you to select how often you check eligibility for each patient. Currently you may only choose to have eligibility verified for each appointment set. In the future you will have the ability to select to have eligibility verified for each calendar month for a patient versus each appointment. Once you have completed the settings for your office click Update to save them.
2 Insurances The next step is to link the Insurance record in Manage Office to the Health Plan Eligibility Name. To Begin, access Manage Office/List Maintenance/Insurances. Edit each insurance record you would like eligibility verified for. Locate the Health Plan Eligibility Name field Click the Browse button to access the list of Health Plans available for eligibility verification. Search the list and click select to link the Health Plan. Click update to save the information. This action will need to be completed for each insurance company you want the system to verify eligibility for. NOTE: MEDICARE (coming soon) NOTE: MEDICARE (coming soon) NPI validation and approvalis required prior to submitting eligibility verifications for Medicare patients. If Office Ally identifies your NPI as not registered when you attempt to schedule appointments for your Medicare patients, Office Ally will attempt to automatically register your NPI for you through Ability (Vision Share). If the validation request comes back approved, you will be able to submit eligibility requests for Medicare patients within 2-3 days. If the validation request comes back denied, you will need to follow steps to verify your provider information is correct with the Medicare NPI Crosswalk / NPPES. Provider Record Verify you have correctly entered the provider s National Provider Identifier (NPI) in the provider record in Manage Office / List Maintenance / Providers The NPI is required and is submitted with the Eligibility Verification request submitted to the Health Plan.
3 Manage Patients The Insurance Eligibility section will have the setting reflected in the Manage Office, Eligibility section in the Insurance tab. Note: If the Health Plan Elig. Name is blank but the Health Plan is linked to the Insurance Co. record in Manage Office you do not have to link it. The first time you schedule an appointment for the patient, the system will update the record in the Manage Patients record. The following fields are required elements for Eligibility Verification checking: Patient Data Patient s First Name Patient Last Name Date of Birth Gender Special Note: Patients linked to an IPA or Medical Group as the Payer, you must link their actual health plan in the Health Plan Elig. section in order to verify eligibility. Insurance Health Plan Elig. Benefit Co. Name (defaults from link in Insurance Co. record) Patient Relationship to Primary Insured Subscriber ID You may elect to exclude a patient from the Eligibility Verification process by unchecking the Elig. Activation box. View Details review the last eligibility verification status received on the patient. Scheduling Appointments When you select the patient Health Plan Eligibility Name will populate from the Patient s record. If this field has not been linked to the patient in Manage Patients you may select the Health Plan from the search list. When you update the appointment the Health Plan Eligibility Name will be updated in the patient s record. To exclude a patient from Eligibility Verification checking for this specific appointment uncheck the Check Eligibility box. NPI validation and approval is required prior to submitting eligibility verifications for Medicare patients. If Office Ally identifies your NPI as not registered when you attempt to schedule appointments for your Medicare patients, Office Ally will attempt to automatically register your NPI for you through Ability (Vision Share). If the validation request comes back approved, you will be able to submit eligibility requests for Medicare patients within 2-3 days. If the validation request comes back denied, you will need to follow steps to verify your provider information is correct with the Medicare NPI Crosswalk / NPPES.
4 Appointments On the appointments tab you will see: Provider/Staff Provider/Staff/Resources Weekly View Elig. Status will display the status of the verification By clicking the status you will be able to see further details related to the verification. There are five possible responses. o Do Not Check User elected not to check eligibility for the patient o Eligible Response returned indicating the patient is eligible o Invalid Response returned indicating either the patient information submitted is invalid (transaction fee will apply) or the request failed to reach the insurance company, a total of three attempts are made at no additional fee (transaction fee will not apply. For failed to reach the insurance company, up to 3 attempts will be made at no additional fee) View the returned status for further details. o Not Eligible Response returned indicating the patient is not eligible o Pending Response pending from the insurance company Elig. Copay Amount of the copay indicated for the patient by the insurance company Check Now For newly added appointments, to recheck invalid responses or for any appointment you want to check eligibility NOW, simply click the Check Now link located within the status page.
5 Examples of Elig. Status and Elig. Copay Responses To view responses click on the status or $ sign within the appointment record. Elig Status (Eligible) Elig. Status (Not Eligible) Elig. Copay ($)
6 Special Notes Time Zone It is important you select the appropriate time zone for your office location. This is to ensure requests are submitted and responses returned within the appropriate time lines for your office hours. IPA/Medical Groups If the patient is linked to an IPA or Medical Group as the Payer in the Insurance Co. field, you must link their actual health plan in the Health Plan Elig. Co. ID field in the Insurance Eligibility section of the patient record in Manage Patients / Insurance tab. Invalid Verification Requests There are various types of invalid verification requests. If the invalid request is due to inaccurate or missing patient/insurance information you will receive a transaction fee for the request. However, if the invalid request is due to a failure of the request to reach the Health Plan to verify the submission you will not receive a transaction fee. Up to three submissions will be made to complete the transaction. If all 3 attempts fail you will not receive the transaction fee. If one of three attempts is successful, you will receive one transaction fee. Insurance to Health Plan links - Office Ally will map the current available health plans to the insurance records in Manage Office. In the event Office Ally miss-mapped an insurance to a health plan simply access the Eligibility Settings section in Manage Office. Click on the Deactivate button to remove all patient settings. Coming Soon!!!!!! MEDICARE NPI validation and approval is required prior to submitting eligibility verifications for Medicare patients. If Office Ally identifies your NPI as not registered when you attempt to schedule appointments for your Medicare patients, Office Ally will attempt to automatically register your NPI for you through Ability (Vision Share). If the validation request comes back approved, you will be able to submit eligibility requests for Medicare patients within 2-3 days. If the validation request comes back denied, you will need to follow steps to verify your provider information is correct with the Medicare NPI Crosswalk / NPPES.
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Member Access Manual. Contents. Registration Process Logging In Making a Donation Donation History Account Information
 Manual Contents Registration Process Logging In Making a Donation Donation History Account Information This is the first screen you will see as a new user, and for future logins. First time users must
Manual Contents Registration Process Logging In Making a Donation Donation History Account Information This is the first screen you will see as a new user, and for future logins. First time users must
Availity TM Eligibility and Benefits Inquiry
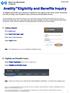 October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
Prescriber Web Prior Authorization
 Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Claims Claim Submission QUICK REFERENCE
 Claims Claim Submission QUICK REFERENCE This will review the process of how to submit a claim online and check the status of a previously submitted claim. Get Started 1. From, click Link and sign in NOTE:
Claims Claim Submission QUICK REFERENCE This will review the process of how to submit a claim online and check the status of a previously submitted claim. Get Started 1. From, click Link and sign in NOTE:
Research and Resolve UB-04 Claim Denials. HP Provider Relations/October 2014
 Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Physical Therapy. Contact your Primary Access Administrator (PAA) if Eligibility and Benefits is not listed in the navigation menu.
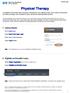 October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
Network Health Claims Editing Portal
 Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Amazing Charts PM Billing & Clearinghouse Portal
 Amazing Charts PM Billing & Clearinghouse Portal Agenda Charge Review Charge Entry Applying Patient Payments Claims Management Claim Batches Claim Reports Resubmitting Claims Reviewing claim batches in
Amazing Charts PM Billing & Clearinghouse Portal Agenda Charge Review Charge Entry Applying Patient Payments Claims Management Claim Batches Claim Reports Resubmitting Claims Reviewing claim batches in
edispense Vaccine Manager Coverage Inquiry
 edispense Coverage Inquiry 1 Getting Started To perform a Coverage Inquiry, open your browser, go to www.edispense5.com Click on Menu,, Coverage Inquiry 2 Enter Patient Information/Check Eligibility Select
edispense Coverage Inquiry 1 Getting Started To perform a Coverage Inquiry, open your browser, go to www.edispense5.com Click on Menu,, Coverage Inquiry 2 Enter Patient Information/Check Eligibility Select
Rev 7/20/2015. ClaimsConnect Rejection Guide
 ClaimsConnect Rejection Guide Helper Client, The purpose of this document is to assist you in accelerating the resolution of claim rejections. We have identified the most frequent rejection messages, and
ClaimsConnect Rejection Guide Helper Client, The purpose of this document is to assist you in accelerating the resolution of claim rejections. We have identified the most frequent rejection messages, and
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
EHR Go Guide: Claims and Ledgers
 EHR Go Guide: Claims and Ledgers Introduction Understanding how to submit patient claims and work with patient ledgers is a vital skill. This guide will provide an overview of how to enter and edit new
EHR Go Guide: Claims and Ledgers Introduction Understanding how to submit patient claims and work with patient ledgers is a vital skill. This guide will provide an overview of how to enter and edit new
The following Key Features describe important functions in the Account and Loan Transfer service.
 Account and Loan Transfer The Account Transfer service makes moving funds between accounts secure and simple. The user will find processing Multi-Entry Transfers and defining Recurring Transfers as easy
Account and Loan Transfer The Account Transfer service makes moving funds between accounts secure and simple. The user will find processing Multi-Entry Transfers and defining Recurring Transfers as easy
Version 1/Revision 18 Page 1 of 36. epaces Professional Claim REFERENCE GUIDE
 Version 1/Revision 18 Page 1 of 36 Table of Contents GENERAL CLAIM INFORMATION TAB... 3 PROFESSIONAL CLAIM INFORMATION TAB... 5 PROVIDER INFORMATION TAB... 10 DIAGNOSIS TAB... 12 OTHER PAYERS TAB... 13
Version 1/Revision 18 Page 1 of 36 Table of Contents GENERAL CLAIM INFORMATION TAB... 3 PROFESSIONAL CLAIM INFORMATION TAB... 5 PROVIDER INFORMATION TAB... 10 DIAGNOSIS TAB... 12 OTHER PAYERS TAB... 13
Axium: Entering Insurance
 Axium: Entering Insurance To enter insurance in Axium follow the directions below: Is the Patient the Policy Holder? If so, we need to indicate this! (Front Desk Primary Responsibility) 1. Select the Patient.
Axium: Entering Insurance To enter insurance in Axium follow the directions below: Is the Patient the Policy Holder? If so, we need to indicate this! (Front Desk Primary Responsibility) 1. Select the Patient.
Getting Started. Enter Patient Information/Check Eligibility. To perform a Coverage Inquiry, open your browser, go to
 Medicare part D Coverage Inquiry Manual Getting Started To perform a Coverage Inquiry, open your browser, go to www.mytransactrx.com Click on Menu, Part D Coverage Inquiry Enter Patient Information/Check
Medicare part D Coverage Inquiry Manual Getting Started To perform a Coverage Inquiry, open your browser, go to www.mytransactrx.com Click on Menu, Part D Coverage Inquiry Enter Patient Information/Check
Maintaining Budget Change Requests
 Maintaining Budget Change Requests This document describes the functions used in TEAMS to enter and approve requests to move funds from one General Ledger account to another. In this document: Request
Maintaining Budget Change Requests This document describes the functions used in TEAMS to enter and approve requests to move funds from one General Ledger account to another. In this document: Request
To add a new profile to the database, click on the Add New Patient link in the Manage Patients Tab.
 MANAGE PATIENTS TAB P r a c t i c e M a t e M a n u a l 89 OVERVIEW The Manage Patients Tab is where you manage all the information pertaining to new and existing patients. The information entered here
MANAGE PATIENTS TAB P r a c t i c e M a t e M a n u a l 89 OVERVIEW The Manage Patients Tab is where you manage all the information pertaining to new and existing patients. The information entered here
Claim Investigation Submission Guide
 Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Provider Healthcare Portal Demonstration:
 Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
ProSuite and Stewart Title NextSTEPS
 ProSuite and Stewart Title NextSTEPS Do you order Title Insurance from Stewart Title NextSTEPS? Do you order online and find yourself manually completing much of the same information that you have already
ProSuite and Stewart Title NextSTEPS Do you order Title Insurance from Stewart Title NextSTEPS? Do you order online and find yourself manually completing much of the same information that you have already
Entering Payments in Aprima PRM
 Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
The claims will appear on the list in order of Date Created. The search criteria at the top of the list will assist you in locating past claims.
 P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
Online Evidence of Insurability (EOI) Submission Process: A Guide for Employers
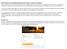 Online Evidence of Insurability (EOI) Submission Process: A Guide for Employers Securian is pleased to offer a new way to submit evidence of insurability online. With minimal set up and changes to your
Online Evidence of Insurability (EOI) Submission Process: A Guide for Employers Securian is pleased to offer a new way to submit evidence of insurability online. With minimal set up and changes to your
Employer/TPA Role to Assign Wage Audit Forms
 Employer/TPA Role to Assign Wage Audit Forms 1. TABLE OF CONTENTS 1. Table of Contents... 2 2. Introduction... 3 3. New UCO-2/UCO-2C Role Process... 4 Version Date: July 11, 2018 Page 2 2. INTRODUCTION
Employer/TPA Role to Assign Wage Audit Forms 1. TABLE OF CONTENTS 1. Table of Contents... 2 2. Introduction... 3 3. New UCO-2/UCO-2C Role Process... 4 Version Date: July 11, 2018 Page 2 2. INTRODUCTION
Associated Connect. Reference Guide: Quick Payments
 Associated Connect Reference Guide: Quick Payments Page 2 of 14 Quick Payments Use the Quick Payments service to send, save and manage your ACH payments. Depending on your configuration, you can use Quick
Associated Connect Reference Guide: Quick Payments Page 2 of 14 Quick Payments Use the Quick Payments service to send, save and manage your ACH payments. Depending on your configuration, you can use Quick
Availity ' Eligibility and Benefits SM'
 Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
Eligibility Troubleshooting 101
 Eligibility Troubleshooting 101 Reference Guide Contents Introduction... 3 Invalid/Missing Search Criteria... 3 Invalid/Missing Subscriber/Insured Name... 3 Resubmit... 5 Patient vs. Subscriber... 7 Invalid
Eligibility Troubleshooting 101 Reference Guide Contents Introduction... 3 Invalid/Missing Search Criteria... 3 Invalid/Missing Subscriber/Insured Name... 3 Resubmit... 5 Patient vs. Subscriber... 7 Invalid
Ambetter and Allwell 1 st Quarterly Webinar April 12 th, 2018
 Ambetter and Allwell 1 st Quarterly Webinar April 12 th, 2018 Conference Number: (855) 351-5537 Conference Code: 741 390 3784 If you haven t already, please call into the webinar to hear us speak. Your
Ambetter and Allwell 1 st Quarterly Webinar April 12 th, 2018 Conference Number: (855) 351-5537 Conference Code: 741 390 3784 If you haven t already, please call into the webinar to hear us speak. Your
Creating and Assigning Targets
 Creating and Assigning Targets Targets are a powerful reporting tool in PortfolioCenter that allow you to mix index returns for several indexes, based on the portfolio s asset class allocation. For example,
Creating and Assigning Targets Targets are a powerful reporting tool in PortfolioCenter that allow you to mix index returns for several indexes, based on the portfolio s asset class allocation. For example,
CABS New Employee Benefits Enrollment Guide. Coventry Corporate Benefits
 CABS New Employee Benefits Enrollment Guide Coventry Corporate Benefits Table of Contents Overview Initial Login Screen Welcome Screen Personal Information screen (Adding Dependents and Beneficiaries)
CABS New Employee Benefits Enrollment Guide Coventry Corporate Benefits Table of Contents Overview Initial Login Screen Welcome Screen Personal Information screen (Adding Dependents and Beneficiaries)
The benefits of using ExpressPAth for your practice include: Easy access. With 24/7 access, you can submit requests and get answers at any time.
 Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Kuali Research User Guide: Create a new Budget document for a Child Award
 Kuali Research User Guide: Create a new Budget document for a Child Award Version 6.0: November 206 Purpose: To create a detailed or modular budget for a child award. Trigger / Timing / Frequency: Once
Kuali Research User Guide: Create a new Budget document for a Child Award Version 6.0: November 206 Purpose: To create a detailed or modular budget for a child award. Trigger / Timing / Frequency: Once
New MN ITS Direct Data Entry (DDE) Screens Professional (837P)
 New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
Recurring Payments CitiDirect BE SM
 Recurring Payments CitiDirect BE SM A Simple, Easy Way to Schedule Recurring Payments User Guide Treasury and Trade Solutions Recurring Payments CitiDirect BE Table of Contents Table of Contents 1. Overview
Recurring Payments CitiDirect BE SM A Simple, Easy Way to Schedule Recurring Payments User Guide Treasury and Trade Solutions Recurring Payments CitiDirect BE Table of Contents Table of Contents 1. Overview
Kentucky Health Net Access With My Rewards Panel Overview
 Kentucky Health Net Access With My Rewards Panel Overview 2019 1 Agenda - Part 1 First Time KY Health Net access Secure Log In Member Eligibility Verification Check Benefits 2 KY Health Net Access Pin
Kentucky Health Net Access With My Rewards Panel Overview 2019 1 Agenda - Part 1 First Time KY Health Net access Secure Log In Member Eligibility Verification Check Benefits 2 KY Health Net Access Pin
Using ERAs with Helper
 Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
University of Wisconsin System SFS Business Process AP Working with 1099 Transactions. Contents
 Contents Instructions for 1099 Process Overview... 2 I. 1099 Voucher Clean Up... 3 II. Run Update Withholdings Process (This will be Run Centrally by UWSA)... 14 III. Run Queries for Validation and to
Contents Instructions for 1099 Process Overview... 2 I. 1099 Voucher Clean Up... 3 II. Run Update Withholdings Process (This will be Run Centrally by UWSA)... 14 III. Run Queries for Validation and to
Medical Billing Assistant - Program Options
 Medical Billing Assistant - Program Options Program Options allows you to control the behavior of MBA in situations where making a permanent change in the program wasn t possible. You may find this option
Medical Billing Assistant - Program Options Program Options allows you to control the behavior of MBA in situations where making a permanent change in the program wasn t possible. You may find this option
PC-ACE Pro32 Reference Guide for Railroad Medicare Claims
 A RRB-Contracted Medicare Administrative Contractor RRB Provider Contact Center 888-355-9165 PC-ACE Pro32 Reference Guide for Railroad Medicare Claims This Reference Guide is intended for use in conjunction
A RRB-Contracted Medicare Administrative Contractor RRB Provider Contact Center 888-355-9165 PC-ACE Pro32 Reference Guide for Railroad Medicare Claims This Reference Guide is intended for use in conjunction
eclinicalworks Training Eligibility Tool
 eclinicalworks Training Eligibility Tool The ADI eclinicalworks database utilizes the Navicure clearinghouse for all eligibility and benefits queries. Eligibility is scheduled to run each night for the
eclinicalworks Training Eligibility Tool The ADI eclinicalworks database utilizes the Navicure clearinghouse for all eligibility and benefits queries. Eligibility is scheduled to run each night for the
Customer Communication Document Scheduled: 02.12
 ANZ Transactive ENHANCEMENT Release 7.1 Customer Communication Document Scheduled: 02.12 CONTENTS FX CROSS RATES 3 What will change? 3 Why is it changing? 3 What does this mean for me? 3 What will it look
ANZ Transactive ENHANCEMENT Release 7.1 Customer Communication Document Scheduled: 02.12 CONTENTS FX CROSS RATES 3 What will change? 3 Why is it changing? 3 What does this mean for me? 3 What will it look
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions
 WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
OVERVIEW GUIDE TO HOME COUNSELOR ONLINE NATIONAL FORECLOSURE MITIGATION COUNSELING (NFMC) FEATURES
 OVERVIEW GUIDE TO HOME COUNSELOR ONLINE NATIONAL FORECLOSURE MITIGATION COUNSELING (NFMC) FEATURES WHO SHOULD USE THIS OVERVIEW GUIDE? WHAT IS NFMC? This overview guide contains information for Home Counselor
OVERVIEW GUIDE TO HOME COUNSELOR ONLINE NATIONAL FORECLOSURE MITIGATION COUNSELING (NFMC) FEATURES WHO SHOULD USE THIS OVERVIEW GUIDE? WHAT IS NFMC? This overview guide contains information for Home Counselor
Prior Authorizations with InterQual Integration
 Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
My ACCESS Account Provider View
 My ACCESS Account Provider View November 7, 2010 Table of Contents Table of Contents... 2 Overview... 3 Provider View Process Flow... 4 Florida Medicaid Home... 5 Customer Search... 6 My Account Status...
My ACCESS Account Provider View November 7, 2010 Table of Contents Table of Contents... 2 Overview... 3 Provider View Process Flow... 4 Florida Medicaid Home... 5 Customer Search... 6 My Account Status...
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Claim Investigation Submission Guide
 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Kuali Coeus Research Management (KCRM) User Guide: Create a new Budget document for a Child Award
 Kuali Coeus Research Management (KCRM) User Guide: Create a new Budget document for a Child Award Version 5.0: August 2014 Purpose: To create detailed or modular budget for a child (or grandchild) award.
Kuali Coeus Research Management (KCRM) User Guide: Create a new Budget document for a Child Award Version 5.0: August 2014 Purpose: To create detailed or modular budget for a child (or grandchild) award.
The Budgets file is a robust feature in DPHS, offering the following functions:
 Budgets Overview: The Budgets file is a robust feature in DPHS, offering the following functions: Create New Budgets Copy Budgets from one year to another View and Modify Existing Budgets Delete a Budget
Budgets Overview: The Budgets file is a robust feature in DPHS, offering the following functions: Create New Budgets Copy Budgets from one year to another View and Modify Existing Budgets Delete a Budget
Renewing your Health Coverage Through DC Health Link
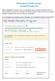 Who is this guide for? Employers who are renewing their group coverage through DC Health Link. These employers currently offer coverage to their group through DC Health Link. The renewal benefit package
Who is this guide for? Employers who are renewing their group coverage through DC Health Link. These employers currently offer coverage to their group through DC Health Link. The renewal benefit package
Work with Guarantor Accounts
 Work with Guarantor Accounts Update guarantor information... 2 Demand a statement for a guarantor... 2 Change the guarantor for a hospital account... 2 Change the guarantor for a minor's hospital account...
Work with Guarantor Accounts Update guarantor information... 2 Demand a statement for a guarantor... 2 Change the guarantor for a hospital account... 2 Change the guarantor for a minor's hospital account...
How to Order an Employment Verification
 How to Order an Employment Verification To order an Employment verification, do the following: Some employers require using an alternate Employee ID rather than using a SSN. If this is a requirement for
How to Order an Employment Verification To order an Employment verification, do the following: Some employers require using an alternate Employee ID rather than using a SSN. If this is a requirement for
Connecticut Medical Assistance Program Workshop Web Claim Submission
 Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
REFUND OVERVIEW. Here s an overview on how refunds should be handled:
 1 REFUND OVERVIEW Here s an overview on how refunds should be handled: 1. Agree with the customer on how the product(s) will be returned Verify with the customer that you have their correct email address.
1 REFUND OVERVIEW Here s an overview on how refunds should be handled: 1. Agree with the customer on how the product(s) will be returned Verify with the customer that you have their correct email address.
MMF Investment Policy Management
 MMF Investment Policy Management Citibank Online Investments Transaction Services MMF Investment Policy Management Table of Contents Table of Contents Money Market Funds Investment Policy Management...2
MMF Investment Policy Management Citibank Online Investments Transaction Services MMF Investment Policy Management Table of Contents Table of Contents Money Market Funds Investment Policy Management...2
Finance Manager: Payroll
 : Payroll W2 Processing The W2 Processing routine prepares the employee payroll information that is necessary for completing the W-2s. The routine encompasses five steps: Generate W2 History File, Edit
: Payroll W2 Processing The W2 Processing routine prepares the employee payroll information that is necessary for completing the W-2s. The routine encompasses five steps: Generate W2 History File, Edit
FINANCE TRAINING CAPITAL PROJECTS Capital Budget Amendment and Create Captial Project
 FINANCE TRAINING CAPITAL PROJECTS Capital Budget Amendment and Create Captial Project CONTENTS: CREATING A CAPITAL PROJECT BUDGET AMENDMENT CREATING A CAPITAL PROJECT Creating a Capital Project Budget
FINANCE TRAINING CAPITAL PROJECTS Capital Budget Amendment and Create Captial Project CONTENTS: CREATING A CAPITAL PROJECT BUDGET AMENDMENT CREATING A CAPITAL PROJECT Creating a Capital Project Budget
Quick Guide. Election Entry
 Election Entry 1. Click the Benefits link. 2. Click the Manage Automated Enrollment link. 3. Click the Events link. 4. Click the On-Demand Event Maintenance link. 5. Enter the desired information into
Election Entry 1. Click the Benefits link. 2. Click the Manage Automated Enrollment link. 3. Click the Events link. 4. Click the On-Demand Event Maintenance link. 5. Enter the desired information into
Prior Authorizations on the Provider Portal. July 2017
 Prior Authorizations on the Provider Portal July 2017 2 Disclaimer The information provided is current as of June 2017 and is subject to change. Stay current with up-to-date information on the OHCA public
Prior Authorizations on the Provider Portal July 2017 2 Disclaimer The information provided is current as of June 2017 and is subject to change. Stay current with up-to-date information on the OHCA public
29 September The following topics will be covered.
 Combat Tax Exclusion Purpose This guide provides the procedures for Starting, Stopping, Deleting and Approving Combat Tax Exclusion transactions in Direct Access. Before you begin Review the Combat Tax
Combat Tax Exclusion Purpose This guide provides the procedures for Starting, Stopping, Deleting and Approving Combat Tax Exclusion transactions in Direct Access. Before you begin Review the Combat Tax
Workday Benefits Training
 Workday Benefits Training Reporting and Processing Leslie Ruth Sr Consultant June 15, 2016 Reflection Always have eyes that see the best in people, a heart that forgives the worst, a mind that forgets
Workday Benefits Training Reporting and Processing Leslie Ruth Sr Consultant June 15, 2016 Reflection Always have eyes that see the best in people, a heart that forgives the worst, a mind that forgets
Lender Connect Collaboration
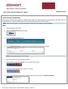 Lender Connect Collaboration When working in files that were originated via RealEC/Closing Insight, the Lender will send over a Closing product with Event Code 431 - Closing Instructions. Below provides
Lender Connect Collaboration When working in files that were originated via RealEC/Closing Insight, the Lender will send over a Closing product with Event Code 431 - Closing Instructions. Below provides
CMS-1500 (02/12) AND UBO4 PAPER CLAIMS REJECT CRITERIA
 To: First Choice VIP Care Plus Participating Providers and Facilities Date: September, 2015 Subject: UPDATED LIST OF COMMON ERRORS ON CLAIMS SUBMISSIONS. Summary: Earlier this year, we distributed a list
To: First Choice VIP Care Plus Participating Providers and Facilities Date: September, 2015 Subject: UPDATED LIST OF COMMON ERRORS ON CLAIMS SUBMISSIONS. Summary: Earlier this year, we distributed a list
Illinois Institute of Technology/TouchNet Payment Plan User Guide
 Students desiring to enroll in IIT s convenient payment plan can follow the step below utilizing TouchNet s Bill & Payment Suite. You can access your account via the Manage Account section on the Finance
Students desiring to enroll in IIT s convenient payment plan can follow the step below utilizing TouchNet s Bill & Payment Suite. You can access your account via the Manage Account section on the Finance
Kansas Medical Assistance Program. Vertical Perspective. Other Insurance/Medicare Training Packet - Professional
 Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
MYOB Exo Employer Services
 MYOB Exo Employer Services Single Touch Payroll Last modified: 15 June 2018 Contents Single Touch Payroll 1 Setting up Single Touch Payroll 1 Configuring System Settings... 1 General Settings... 2 Payer
MYOB Exo Employer Services Single Touch Payroll Last modified: 15 June 2018 Contents Single Touch Payroll 1 Setting up Single Touch Payroll 1 Configuring System Settings... 1 General Settings... 2 Payer
INVESTOR360 : ADDITIONAL ASSETS
 INVESTOR360 : ADDITIONAL ASSETS The Additional Assets section displays a list of outside assets associated with the account, such as bank accounts, loans, and credit cards, as well as assets manually entered
INVESTOR360 : ADDITIONAL ASSETS The Additional Assets section displays a list of outside assets associated with the account, such as bank accounts, loans, and credit cards, as well as assets manually entered
Life of a Claim. HP Provider Relations/August 2014
 Life of a Claim HP Provider Relations/August 2014 Agenda General requirements for reimbursement by the Indiana Health Coverage Programs (IHCP) System edits System audits Pricing methodologies Suspended
Life of a Claim HP Provider Relations/August 2014 Agenda General requirements for reimbursement by the Indiana Health Coverage Programs (IHCP) System edits System audits Pricing methodologies Suspended
MASTER SCHEDULING GUIDE TO CREATING CREDIT RECOVERY SECTIONS IN PERIODS 50-75
 MASTER SCHEDULING GUIDE TO CREATING CREDIT RECOVERY SECTIONS IN PERIODS 50-75 USER GUIDE ON CREATING CREDIT RECOVERY SECTIONS IN MISIS Per LAUSD MEM-6733.1 Credit Recovery Program Opportunities, all schools
MASTER SCHEDULING GUIDE TO CREATING CREDIT RECOVERY SECTIONS IN PERIODS 50-75 USER GUIDE ON CREATING CREDIT RECOVERY SECTIONS IN MISIS Per LAUSD MEM-6733.1 Credit Recovery Program Opportunities, all schools
New MN ITS Direct Data Entry (DDE) Screens Dental (837D)
 New MN ITS Direct Data Entry (DDE) Screens Dental (837D) This handout is intended to accompany the MN ITS DDE Dental 837D Training Webinar. It is not intended to replace the MN-ITS User Guides or specific
New MN ITS Direct Data Entry (DDE) Screens Dental (837D) This handout is intended to accompany the MN ITS DDE Dental 837D Training Webinar. It is not intended to replace the MN-ITS User Guides or specific
New Employees How to Enroll in Health Coverage
 New Employees How to Enroll in Health Coverage through DC Health Link Who is this guide for? This guide will walk employees without a DC Health Link account through setting up their employee account, selecting
New Employees How to Enroll in Health Coverage through DC Health Link Who is this guide for? This guide will walk employees without a DC Health Link account through setting up their employee account, selecting
Chapter 6. Cash Control
 Chapter 6 Cash Control This Page Left Blank Intentionally CTAS User Manual 6-1 Cash Control: Introduction The Cash Control section allows you to enter the beginning balances for the fiscal year. This section
Chapter 6 Cash Control This Page Left Blank Intentionally CTAS User Manual 6-1 Cash Control: Introduction The Cash Control section allows you to enter the beginning balances for the fiscal year. This section
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
1. Plan. Objective: Figure 1. The above form is available for HOD/BCO. Click on Plan -> Data Entry > Annual Plan as shown in Figure 1.
 1. Plan Open Internet explorer. Write http:ifms.raj.nic.in in the address bar. IFMS login page will be displayed. Click on Budget. Enter user Id and password. User Id and password is same as that of budget.
1. Plan Open Internet explorer. Write http:ifms.raj.nic.in in the address bar. IFMS login page will be displayed. Click on Budget. Enter user Id and password. User Id and password is same as that of budget.
Benefits Enrollment Procedure
 Contents Procedure Overview Step 1: Create Family Member/Dependents (IT 0021) Step 2: Enroll an Employee in the Health/Insurance Plans Procedure Overview Overview To gain an understanding on how to process
Contents Procedure Overview Step 1: Create Family Member/Dependents (IT 0021) Step 2: Enroll an Employee in the Health/Insurance Plans Procedure Overview Overview To gain an understanding on how to process
Chapter 18. Indebtedness
 Chapter 18 Indebtedness This Page Left Blank Intentionally CTAS User Manual 18-1 Indebtedness: Introduction The Indebtedness Module is designed to track an entity s indebtedness. By entering the principal
Chapter 18 Indebtedness This Page Left Blank Intentionally CTAS User Manual 18-1 Indebtedness: Introduction The Indebtedness Module is designed to track an entity s indebtedness. By entering the principal
Exception Report Guide. August 2018
 Exception Report Guide August 2018 Quick Payroll Exception Error Guides We understand your day-to-day challenges; this is why we want to try to make your business life easier. We have prepared this guide
Exception Report Guide August 2018 Quick Payroll Exception Error Guides We understand your day-to-day challenges; this is why we want to try to make your business life easier. We have prepared this guide
Claims INFO Adjustment Submission Guide
 Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
IRA FMV and Contribution Report Wizard Instructions for Tax Reporting Service Clients
 IRA FMV and Contribution Report Wizard Instructions for Tax Reporting Service Clients Wizard Purpose The IRA FMV and Contribution Report Wizard must be completed by financial organizations with a 5498
IRA FMV and Contribution Report Wizard Instructions for Tax Reporting Service Clients Wizard Purpose The IRA FMV and Contribution Report Wizard must be completed by financial organizations with a 5498
Frequently asked questions and answers for pharmacy providers
 Frequently asked questions and answers for pharmacy providers The purpose of Medicare s Limited Income Newly Eligible Transition (NET) Program is to ensure individuals with Medicare s low-income subsidy
Frequently asked questions and answers for pharmacy providers The purpose of Medicare s Limited Income Newly Eligible Transition (NET) Program is to ensure individuals with Medicare s low-income subsidy
Provider Healthcare Portal Overview. Indiana Health Coverage Programs DXC Technology October 2017
 Provider Healthcare Portal Overview Indiana Health Coverage Programs DXC Technology October 2017 Session Objectives Provider Enrollment transactions Home Page Member Eligibility Prior Authorization Claims
Provider Healthcare Portal Overview Indiana Health Coverage Programs DXC Technology October 2017 Session Objectives Provider Enrollment transactions Home Page Member Eligibility Prior Authorization Claims
Filing Secondary Claims on Provider Express
 Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Chapter 6 DRAWDOWNS ACCESSING THE DRAWDOWN FUNCTIONS
 Chapter 6 DRAWDOWNS Drawdowns may be made for an activity after it has been funded and, except for PI, may only be made from the funding sources (or grant years) from which the activity was funded. The
Chapter 6 DRAWDOWNS Drawdowns may be made for an activity after it has been funded and, except for PI, may only be made from the funding sources (or grant years) from which the activity was funded. The
Claim Form Billing Instructions: CMS-1500 Claim Form
 Claim Form Billing Instructions: CMS-1500 Claim Form Item Required Field? Description and Instructions number N/A Situational When submitting a Medicare Replacement Plan claim, write or stamp Medicare
Claim Form Billing Instructions: CMS-1500 Claim Form Item Required Field? Description and Instructions number N/A Situational When submitting a Medicare Replacement Plan claim, write or stamp Medicare
Instructions on how to complete Enrollment/Change for: I divorced my spouse
 Instructions on how to complete Enrollment/Change for: I divorced my spouse 1. Log into the enrollment site at: https://trustmark.benselect.com/enroll Employee ID or SSN PIN: Last 4 of SSN and last 2 of
Instructions on how to complete Enrollment/Change for: I divorced my spouse 1. Log into the enrollment site at: https://trustmark.benselect.com/enroll Employee ID or SSN PIN: Last 4 of SSN and last 2 of
RESIDENTIAL HEALTH CARE. [Type text] [Type text] [Type text] Version
![RESIDENTIAL HEALTH CARE. [Type text] [Type text] [Type text] Version RESIDENTIAL HEALTH CARE. [Type text] [Type text] [Type text] Version](/thumbs/77/75761243.jpg) New York State UB04 Billing Guidelines [Type text] [Type text] [Type text] Version 2013-01 2/11/2013 E M E D N Y I N F O R M A T I O N emedny is the name of the electronic New York State Medicaid system.
New York State UB04 Billing Guidelines [Type text] [Type text] [Type text] Version 2013-01 2/11/2013 E M E D N Y I N F O R M A T I O N emedny is the name of the electronic New York State Medicaid system.
How do I bill patient co-pays?
 How do I bill patient co-pays? To bill patient co-pays, the Patient Pay (Self Pay) insurance must be first entered in the Patient insurance file or the System File must have the default Self Pay insurance
How do I bill patient co-pays? To bill patient co-pays, the Patient Pay (Self Pay) insurance must be first entered in the Patient insurance file or the System File must have the default Self Pay insurance
MERCER SPECTRUM A SIMPLE SOLUTION FOR EMPLOYERS (WITH MORE THAN 20 EMPLOYEES)
 MERCER SPECTRUM A SIMPLE SOLUTION FOR EMPLOYERS (WITH MORE THAN 20 EMPLOYEES) MERCERSPECTRUM OVERVIEW This guide provides an overview of MercerSpectrum, one of our two online options used for providing
MERCER SPECTRUM A SIMPLE SOLUTION FOR EMPLOYERS (WITH MORE THAN 20 EMPLOYEES) MERCERSPECTRUM OVERVIEW This guide provides an overview of MercerSpectrum, one of our two online options used for providing
Claims Validation Process for Providers (Alpha MCS)
 Providers have requested to know the validation sequence their claims go through in the AlphaMCS system. Below is the documentation that the MCO staff use for this purpose. Validation Sequence Clean claims
Providers have requested to know the validation sequence their claims go through in the AlphaMCS system. Below is the documentation that the MCO staff use for this purpose. Validation Sequence Clean claims
Processing Customer Credit Memos and Refunds
 Processing Customer Credit Memos and Refunds If a job completed for a customer requires the processing of a refund or credit you can create a credit memo for the customer that will be reflected on the
Processing Customer Credit Memos and Refunds If a job completed for a customer requires the processing of a refund or credit you can create a credit memo for the customer that will be reflected on the
AlphaMCS CLAIMS GUIDE. Written by: Ross Inman, AlphaCM Support Douglas Vann, AlphaCM Software Developer Cheryl Mason, AlphaCM Customer
 AlphaMCS CLAIMS GUIDE Written by: Ross Inman, AlphaCM Support Douglas Vann, AlphaCM Software Developer Cheryl Mason, AlphaCM Customer Overview... 5 Validation Sequence... 6 ED Claims... 13 1 Adjusted Above
AlphaMCS CLAIMS GUIDE Written by: Ross Inman, AlphaCM Support Douglas Vann, AlphaCM Software Developer Cheryl Mason, AlphaCM Customer Overview... 5 Validation Sequence... 6 ED Claims... 13 1 Adjusted Above
Bill Registration Process through IDBI Net Banking. 1. Login to IDBI Bank net Banking from IDBI Bank website - https://www.idbi.
 Bill Registration Process through IDBI Net Banking 1. Login to IDBI Bank net Banking from IDBI Bank website - https://www.idbi.com 2. Post login click on "Bills" Tab to check the sub options available
Bill Registration Process through IDBI Net Banking 1. Login to IDBI Bank net Banking from IDBI Bank website - https://www.idbi.com 2. Post login click on "Bills" Tab to check the sub options available
OPEN ENROLLMENT INSTRUCTIONS
 OPEN ENROLLMENT INSTRUCTIONS These instructions will help you navigate through BenefitBridge in making your elections for Open Enrollment For benefits effective in 2018 Start by navigating to the website
OPEN ENROLLMENT INSTRUCTIONS These instructions will help you navigate through BenefitBridge in making your elections for Open Enrollment For benefits effective in 2018 Start by navigating to the website
Store Credit Magento Extension User Guide Official extension page: Store Credit
 Store Credit Magento Extension User Guide Official extension page: Store Credit Page 1 Table of contents: 1. General Settings.....3 2. Store Credit Product Creation.. 5 3. Product Price Settings..6 4.
Store Credit Magento Extension User Guide Official extension page: Store Credit Page 1 Table of contents: 1. General Settings.....3 2. Store Credit Product Creation.. 5 3. Product Price Settings..6 4.
CareCentrix Claim Rejection Code Guide
 Document intent: This document describes the reasons and codes that contracted providers receive when a claim is rejeted. REJECTION CODE CATEGORY CODE DESCRIPTION STATUS CODE DESCRIPTION This column contains
Document intent: This document describes the reasons and codes that contracted providers receive when a claim is rejeted. REJECTION CODE CATEGORY CODE DESCRIPTION STATUS CODE DESCRIPTION This column contains
Mybenefits.illinois.gov. Enrolling in Benefits
 Mybenefits.illinois.gov Enrolling in Benefits Benefit Choice Enrollment Once you know which plan is best for you, you can begin the enrollment process. On the MyBenefits home page, click Enroll Now to
Mybenefits.illinois.gov Enrolling in Benefits Benefit Choice Enrollment Once you know which plan is best for you, you can begin the enrollment process. On the MyBenefits home page, click Enroll Now to
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
Pension Procedures. Setting up a Pension E/D on the employee
 Pension Procedures Setting up a Pension E/D on the employee The Evolution system has been programmed to know what the Federal Limits are for the various Pension Plan types. If you have an employee who
Pension Procedures Setting up a Pension E/D on the employee The Evolution system has been programmed to know what the Federal Limits are for the various Pension Plan types. If you have an employee who
