Consumer s Right to Know About Health Plans in Rhode Island
|
|
|
- Blake Wilcox
- 6 years ago
- Views:
Transcription
1 Consumer s Right to Know bout Health Plans in Rhode Island etna Life Insurance Company (etna) January, 2012 Consumer Disclosure Safe and Healthy Lives In Safe and Healthy Communities 1
2 Consumer Disclosure etna Life Insurance Company Medical PPO Plan with Pharmacy CONSUMER'S RIGHT TO KNOW BOUT HELTH PLNS THE HELTH CRE CCESSIBILITY ND QULITY SSURNCE CT Knowing how Health Plans work helps you to be a better consumer. This Health Plan is regulated by the Rhode Island Department of Health and is required by law to disclose the information contained in this document, routinely, to all prospective subscribers and to current subscribers upon request. Official Plan Documents give complete information about this Health Plan, in sample or final form, and are available upon request. Health Plans must also provide a comprehensive list of all participating providers, updated annually. This Consumer Disclosure has been reviewed and approved for single service Health Plans by the Rhode Island Department of Health in accordance with R (Rules and Regulations for Certifying Health Plans). Requests for more information about Health Plan certification or consumer rights may be addressed to: Rhode Island Department of Health, Division of Health Services Regulation, 3 Capitol Hill, Providence, RI , Phone: Q Who can I contact at the Health Plan for information? Representatives of this Health Plan are available to help you get the information you need. You can contact a Health Plan representative at: Member Services Representative 151 Farmington venue, Hartford, Connecticut Toll Free: TDD Number: Para contractor a un representante que hable Espanol, llame a: Nombre del Represtante de Plan:
3 3
4 Q How does the Health Plan review and approve covered services? Health Plan may review covered services that are recommended by providers to decide if the services are medically necessary. If the plan decides the service is not medically necessary, it will not pay. You and your provider can appeal the Health Plan's decision. The plan only pays for covered medical expenses that are medically necessary and are not considered experimental or investigational. Some expenses may require prior authorization by the Plan before they will be covered. ll inpatient services extending beyond the initial certification period require concurrent review, (assesses the need for continued stay, level of care and quality of care). ll expenses not requiring precertification are reviewed retrospectively, (post-service review). The criteria for medically necessity determinations of service or supply include, but are not limited to: appropriateness for diagnosis, care or treatment; reports in peer reviewed medical literature; reports and guidelines published by nationally recognized health care organizations (including scientific data); meeting generally recognized professional standards of safety and effectiveness in the United States for diagnosis, care or treatment; the setting or technical skills to safely and adequately provide the services or supplies. Written policies and criteria are available from the Member Services Representative. Q What if I have an emergency? n emergency is a problem that needs to be seen by a provider "right-away" to prevent permanent damage or death. Here's what this Health Plan wants you to do when you have an emergency health care problem, at home or out of state. If you need emergency care, you are covered 24 hours a day, 7 days a week, anywhere in the world. Call your primary care physician first, if possible. Your primary care physician is required to provide emergency coverage 24 hours a day, including weekends and holidays. However, if a delay would be detrimental to your health, see the nearest emergency facility. Nonemergency treatment in hospital emergency rooms, however, is not a covered benefit. Q What if I refuse referral to a participating provider? When a specific covered service is recommended. Health Plans may send you to certain participating providers. If you refuse the referral and get the service from another provider, the Health Plan must tell you effect if will have on payment. s a PPO member, you also have the option of obtaining nonreferred care from participating and nonparticipating providers (including primary care physicians), subject to the annual deductible, coinsurance and maximum benefit limitation as outlined in your plan summary. 4
5 Q Does the Health Plan require that I get a second opinion for any services? What if I want a second opinion? In some cases the Health Plan may require a second opinion before it will pay for a covered service. Or you may just want a second opinion on a plan for diagnosis or treatment. etna does not require that you obtain a second opinion before it will pay for covered services. However, if you elect to obtain a second opinion and obtain a referral from a primary care physician or the Plan, etna will pay a portion of the charge for the physician services as well as any x-ray and laboratory tests, but only if the surgical procedure is covered under the plan. Q How does the Health Plan make sure that my personal health information is protected and kept confidential? In general, personal health information must be kept confidential (private) by a Health Plan, its employees and agencies it contracts with. Here's how the Health Plan makes sure that personal health information is protected. Disclosure of personal health information cannot be made to others without your authorization. However, disclosure may be made without consent where it is necessary for the conduct of etna s business, to regulators of etna s business when required by law, or to law enforcement authorities when needed to prevent or prosecute fraud or other illegal activities. Such disclosure cannot be contrary to any state or federal law which applies. The actions of etna s own confidentiality requirement contained in it s Code of Conduct. In addition, all providers must agree to comply with all applicable state and federal laws regarding confidentiality of patient information and keep member information confidential. Q How am I protected from discrimination? You have the right to be treated fairly and equally. Health Plans may not discriminate against you due to age, sex, religion, race or ethnic origin, disability, occupational status or any other characteristics protected by law. This plan does not discriminate against members or prospective members due to age, sex, religion, race, ethic origin, disability, occupational status, or any other characteristic protected by state or federal law. Q If I refuse treatment, will it affect my future treatment? Health Plan must tell you what effect it will have on future coverage if you refuse to be treated for any condition. If you refuse treatment it will not affect coverage for any future treatment you may receive. 5
6 Q How does the health plan pay providers? Your Health Plan must tell you about the kinds of financial arrangements it has with providers. This health plan may include a capitated reimbursement arrangement or other similar risk sharing arrangement and other financial arrangements with providers. Q How is coverage renewed or canceled? etna will renew your coverage on its calendar year anniversary date unless you choose another plan offered by your employer. Some provisions may change, including out-of-pocket costs. Your coverage may be canceled only as allowed by law, e.g. if your employer fails to pay the premiums for your group. Q If I am covered by two or more health plans, what should I do? If you or a family member are covered by two or more Health Plans, you may have to give information on your coverage to each Health Plan. This helps the Health Plans to arrange payments between the plans when you or a family member receive a service. Here's what this plan will ask you to tell them. If you are covered by two or more health plans, benefits under the other plans may be taken into consideration when determining the benefits payable under this plan. This may mean a reduction in benefits under this plan. You must inform etna of the other coverage(s) that your have so that it can be determined whether or not and to what extent this plan can coordinate benefits with the other plan(s).. 6
7 Medical PPO etna Life Insurance Company COVERED SERVICES T--GLNCE Information Shown is Based on Health Insurance Plans That Meet the Requirements of Federal Health Care Reform Legislation nnual Deductible: In-Network: Indiv-$0 - $5,000/Family- 2x or 3x Indiv; Max Lifetime Cap: Unlimited. Out-of-Network: Indiv-$100 - $10,000/Family- 2x or 3x Indiv Type of Service (Not ll Services are Listed Is Prior uthorization Required *(Yes/No) What Out-of-Pocket Expenses Will I Have to Pay? Call plan or check Official Plan Documents for Details mbulance No 0-30% of the negotiated charge after deductible Chiropractic Treatment No 0-30% of the negotiated charge after deductible; or Specialist copay of $5 - $65, or 0-30% after Specialist copay of $5 - $65 Dental Care No Office copay: None - $25 Inpatient: None - 20% of the negotiated charge after deductible and/or per confinement deductible, ($0 - $400). Diagnostic X-rays, Imaging and Laboratory Tests No $5 - $60 copay or 0-30% or 0-30% after $5 - $60 copay Emergency Services No $25 - $150 copay or 0-30% or 0-30% after $25 - $150 copay after deductible Summary for consumer information only. This is not a contract. What Other Limitations pply? Ground ambulance cannot have copay greater than $50. None Coverage is limited to services that are medical in nature, and to dental services to repair sound natural teeth damaged due to injury. No other coverage for dental services. If performed as a part of a physician office visit and billed by the physician, expenses are covered subject to the applicable physician's office visit member cost sharing Non-emergency use of the emergency room covered at 50%. If I Choose a Non- Participating Provider Will the Service be Covered? Yes, 0-50% of the the deductible. the deductible. Yes, 20% - 40% of the the deductible and/or per confinement deductible, ($0 - $400). Prior authorization penalty applies, (up to $500). the deductible. Yes, Same as preferred care. 7
8 Medical PPO COVERED SERVICES T--GLNCE Information Shown is Based on Health Insurance Plans That Meet the Requirements of Federal Health Care Reform Legislation nnual Deductible: In-Network: Indiv-$0 - $5,000/Family- 2x or 3x Indiv. limit; Max Lifetime Cap: Unlimited. Out-of-Network: Indiv-$100 - $10,000/Family- 2x or 3x Indiv. limit Type of Service (Not ll Services are Listed Is Prior uthorization Required *(Yes/No) What Out-of-Pocket Expenses Will I Have to Pay? Call plan or check Official Plan Documents for Details Experimental Treatments Yes Office copay: None - $25 Inpatient: None - 20% of the negotiated charge after deductible and/or per confinement deductible, ($0 - $400). Eye Care No Routine Eye Exam: 0-30% of the negotiated charge after deductible; or Specialist copay of $5 - $65, or 0-30% after Specialist copay of $5 - $65 Foot Care No Same as Specialist: 0-30% of the negotiated charge after deductible; or Specialist copay of $5 - $65, or 0-30% after Specialist copay of $5 - $65 Health Education & Wellness No Preventive Care: PCP $5 - $60 copay; or 0-30%; or 0-30% after $5- $60 copay Home Health Care Yes No charge, or same as specialist cost share of 0-30% of the What Other Limitations pply? Coverage limited to new cancer therapies in accordance with Rhode Island mandate. Coverage limited to Rhode Island mandate for Diabetic Education. Limited to (60, 100, 120) visits per calendar year If I Choose a Non- Participating Provider Will the Service be Covered? Yes, 20% - 40% of the the deductible and/or per confinement deductible, ($0 - $400). Prior authorization penalty applies, (up to $500). the deductible. the deductible. the deductible. 8
9 Summary for consumer information only. This is not a contract. negotiated charge after deductible; or Specialist copay of $5 - $65, or 0-30% after Specialist copay of $5 - $65 Each visit by a nurse or therapist is one visit. Each visit up to 4 hours by a home health care aide is one visit. the deductible. 9
10 Medical PPO COVERED SERVICES T--GLNCE Information Shown is Based on Health Insurance Plans That Meet the Requirements of Federal Health Care Reform Legislation nnual Deductible: In-Network: Indiv-$0 - $5,000/Family- 2x or 3x Indiv. limit; Max Lifetime Cap: Unlimited. Out-of-Network: Indiv-$100 - $10,000/Family- 2x or 3x Indiv. limit Type of Service (Not ll Services are Listed Is Prior uthorization Required *(Yes/No) What Out-of-Pocket Expenses Will I Have to Pay? Call plan or check Official Plan Documents for Details Hospice Care Yes Inpatient: 0-30% or Same as Preferred Inpatient Hospital Coverage. Deductible and/or day values may be lower. Outpatient: 0-30% or same as Specialist Office visit cost sharing of 0 - $65 Hospitalization and Inpatient Services Yes 0-30% or 0-30% after a $50 -$500 per confinement deductible, or $50 - $500 per day for 1-5 days per confinement; thereafter covered 100% or $50 - $500 per day plus 0-30% for the first 1-5 days per confinement; thereafter Covered 100%, 10%, 20%, 30% What Other Limitations pply? Inpatient: Limited to 30 days per lifetime. The member cost sharing applies to all covered benefits incurred during a member's inpatient stay. Outpatient: Up to a maximum benefit of $5,000 The member cost sharing applies to all covered benefits incurred during a member's outpatient visit The member cost sharing applies to all covered benefits incurred during a member's inpatient stay If I Choose a Non- Participating Provider Will the Service be Covered? Yes, inpatient 0% - 50% of the the deductible or Same as Non-Preferred Inpatient Hospital Coverage. Deductible and/or day values may be lower. Outpatient 0-50% Yes, 0% - 50% of the the deductible and/or per confinement deductible, Maternity Yes Same as inpatient hospital Same as inpatient hospital Same as inpatient hospital Medical Equipment and Supplies No Durable Medical Equipment: 0, 10%, 20%, 30%, 50% or 100% Durable Medical Equipment: 0, 10%, 20%, 30%, 50% or 100% Yes, 20% - 100% of the 10
11 the deductible. Maximum annual benefit of (No limit, $1,250, $2,500, $5,000, $7,500, $10,000, $20,000) per member per calendar year. 11
12 Medical PPO COVERED SERVICES T--GLNCE Information Shown is Based on Health Insurance Plans That Meet the Requirements of Federal Health Care Reform Legislation nnual Deductible: In-Network: Indiv-$0 - $5,000/Family- 2x or 3x Indiv. limit; Max Lifetime Cap: Unlimited. Out-of-Network: Indiv-$100 - $10,000/Family- 2x or 3x Indiv. limit Type of Service (Not ll Services are Listed Is Prior uthorization Required *(Yes/No) What Out-of-Pocket Expenses Will I Have to Pay? Call plan or check Official Plan Documents for Details Mental Health, Inpatient Yes Same as IP Hospital (complies with RI MH mandate) Mental Health, Outpatient No Same as OP Hospital (complies with RI MH mandate) Nursing Home Care Yes 0-30% of the negotiated charge after deductible and/or per confinement deductible Nutritional Support No, however must obtain prescription from physician. Same as prescription drug or INN medical supplies (for such items as feeding tubes) cost sharing, depending on type of nutritional support obtained. Physician Office Visits No Office Visits to Non-Specialist (nonsurgical): $50 - $60 copay; or 0% - 30% 0% - 30% after $5 - $60 copay What Other Limitations pply? Same as IP Hospital (complies with RI MH mandate) Same as OP Hospital (complies with RI MH mandate) Limited to (60, 90, 100, 120) days per calendar year The member cost sharing applies to all covered benefits incurring during a member's inpatient stay Only for diagnosis and treatment of illness or injury, except for mandated If I Choose a Non- Participating Provider Will the Service be Covered? Same as Non-Par IP Hospital Same as Non-Par IP Hospital the deductible and/or per confinement deductible. Prior authorization penalty applies, (up to $500). Same as prescription drug or OON medical supplies (for such items as feeding tubes) cost sharing, depending on type of nutritional support obtained. 12
13 preventive services. the deductible. 13
14 Type of Service (Not ll Services are Listed Is Prior uthorization Required *(Yes/No) What Out-of-Pocket Expenses Will I Have to Pay? Call plan or check Official Plan Documents for Details Prescription Drugs Yes Single Tier Copays : $5 - $70 or Two Tier Copays: $5/$15, $10/$20, $15/$25, $20/$30, $30/$40, $30/$50 or Prescription llowance amounts : $10/$75, $10/$70, $15/$65, $15/$60 with member out-of-pocket maximum of None/$150, None/$200, None/$250, None/$300 respectively. or Three Tier Copays : $5/$10/$25, $5/$15/$30, $5/$20/$40, $5/$30/$50, $5/$40/$60, $10/$15/$30, $10/$20/$35, $10/$25/$50, $10/$30/$45, $10/$30/$50, $10/$30/$60, $15/$20/$35, $15/$25/$40, $15/$30/$50, $15/$35/$50, $15/$35/$60, $20/$30/$45, $20/$30/$50, $20/$40/$70, $5/$10/50%, $5/$15/50%, $10/$15/50%, $15/$20/50%, $10/$20/50%, 30%/30%/50%, $10/30%/50%; Mail Order Drug: Covered 100% after combined medical/rx plan deductible and $10 copay for generic drugs, $20 copay for formulary brand-name drugs, and $50 copay for nonformulary brand-name drugs up to a day supply from etna Rx Home Delivery. Self-Injectibles: "4th Tier 10%, 15%, 20%, 25%, 30%, 35%, 40%, 45%, 50% for formulary and non formulary drugs 4th and 5th Tier (10%, 20%, 30%, 40%) for formulary and What Other Limitations pply? The full cost of the drug is applied to the deductible before benefits are considered for payment under the pharmacy plan. Prior authorization required for certain outpatient prescription drugs. Limited to a 30 day supply from drugs received from a community pharmacy. Limited to a 90 day supply from drugs received from a mail order pharmacy. "Pharmacy Managed Self Injectables (PMSI) First prescription fill at any retail or mail order drug facility. Subsequent fills must be through etna Specialty Pharmacy " No Mandatory Generic (NO MG) - Member is responsible to pay the applicable copay only. Prescription drug plan year deductible (must be satisfied before any drug benefits are paid) Individual None, $100, $200 Individual If I Choose a Non- Participating Provider Will the Service be Covered? Yes,Not Covered or 20% - 50% or 20% - 50% after applicable preferred RxDrug copay or For Prescription llowance only: 30% - 50%. Mail Order Drug not covered. Self-Injectibles not covered. 14
15 20%, 25%, 30%, 35%, 40%, 45%, 50% for non formulary drugs" None, $100, $200 Family (None, 3x) Individual amount Family (None, 3x) Individual amount Rehabilitation (PT/OT/Speech Therapy) Yes (inpatient) No (outpatient) PT/OT/ST combined: Covered 100%, 10%, 20%, 30%, or Covered same as Specialist Office visit cost sharing; Or Separate ST Covered 100%, 10%, 20%, 30% or same as Specialist Office visit cost sharing with the PT/OT covered 100%, 10%, 20%, 30% or Covered same as Specialist Office visit cost sharing Prescription drug plan year maximum (combined maximum for drugs received at a preferred or non-preferred pharmcy (None, $2,500, $3,000, $3,500, $4,000, $5,000, $6,000, $7,000) per member (None, $2,500, $3,000, $3,500, $4,000, $5,000, $6,000, $7,000) per member Prescription Drug nnual Out of Pocket Maximum Individual: None, $2,000, $3,000, $4,000, $5,000, $6,000, $7,000, $8,000, $9,000, $10,000 Family: (2x, 3x) Individual amount" or Not Covered When ST is separate from PT/OT, PT/OT is Limited to 20, 25, or 30 visits per calendar year combined the deductible and/or per confinement deductible, ($0 - $400). Prior authorization penalty applies, (up to $500). Substance buse, Inpatient Yes Same as Inpatient Hospital Limited to 30, 45, or 60 days Same as Non-Preferred 15
16 Substance buse, Outpatient No Covered 100%, 10%, 20%, 30%, or same as Specialist Office visit cost sharing Surgery, Outpatient Yes Covered 100%, 10%, 20%, 30% or same as Specialist Office visit cost sharing Smoking Cessation Treatment No, however must obtain prescription from physician for prescription nicotine replacement therapy. Summary for consumer information only. This is not a contract. Same as prescription drug cost sharing for nicotine replacement therapy. 100% coinsurance, no deductible, no copay for physician or specialist office visit for smoking cessation counseling sessions. 10 per calendar year. The member cost sharing applies to all covered benefits incurred during a member's inpatient stay Limited to visits per calendar year. The member cost sharing applies to all Covered Benefits incurred during a member's outpatient visit. Maximums are a combined limit for preferred and non-preferred services. Member cost sharing applies to all Covered Benefits incurred during a member's outpatient visit Mandate originally applied visit limits, but those limits were subsequently removed. Currently, no visit limits may be applied INN or OON. Inpatient Hospital coverage 20% - 50% 20% - 50% Same as prescription drug cost sharing for nicotine replacement therapy. Same as OON physician or specialist office visit cost sharing for smoking cessation counseling sessions. 16
Consumer s Right to Know About Health Plans in Rhode Island
 Consumer s Right to Know bout Health Plans in Rhode Island Vision Service Plan Effective March 17, 2016 Consumer Disclosure Safe and Healthy Lives in Safe and Healthy Communities Consumer Disclosure CONSUMER'S
Consumer s Right to Know bout Health Plans in Rhode Island Vision Service Plan Effective March 17, 2016 Consumer Disclosure Safe and Healthy Lives in Safe and Healthy Communities Consumer Disclosure CONSUMER'S
Consumer s Right to Know About Health Plans in Rhode Island
 Consumer s Right to Know bout Health Plans in Rhode Island UnitedHealthcare of New England, Inc. Choice dvanced January 1, 2016 Consumer Disclosure Safe and Healthy Lives in Safe and Healthy Communities
Consumer s Right to Know bout Health Plans in Rhode Island UnitedHealthcare of New England, Inc. Choice dvanced January 1, 2016 Consumer Disclosure Safe and Healthy Lives in Safe and Healthy Communities
Not applicable. Immunizations 1 exam per 12 months for members age 18 to age 65; 1 exam per 12 months for adults age 65 and older.
 PLAN FEATURES NON- Deductible (per calendar year) $300 Employee $600 Employee $900 Family $1,800 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
PLAN FEATURES NON- Deductible (per calendar year) $300 Employee $600 Employee $900 Family $1,800 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
CA HMO Deductible $1,500 70%
 Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18 12/31/18
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18 12/31/18 Wood County Employee Health Benefits Plan: Health & RX only Coverage for: Single/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18 12/31/18 Wood County Employee Health Benefits Plan: Health & RX only Coverage for: Single/Family
Plan changes are in red In-Network 2015 Out-of-Network
 General Information Lifetime Maximum Benefit Unlimited Unlimited Annual Maximum Benefit Unlimited Unlimited Coinsurance Percentage 80.00% 50.00% Precertification Requirements Precertification Penalty Covered
General Information Lifetime Maximum Benefit Unlimited Unlimited Annual Maximum Benefit Unlimited Unlimited Coinsurance Percentage 80.00% 50.00% Precertification Requirements Precertification Penalty Covered
PLAN DESIGN & BENEFITS. $100 Individual/$200 Family $500 Individual/$1000 Family
 PLAN FEATURES Deductible (per calendar year) Provider None $1000 Individual/$2000 Family Deductible (per calendar year) Facility Level A: Level B: $100 Individual/$200 Family $500 Individual/$1000 Family
PLAN FEATURES Deductible (per calendar year) Provider None $1000 Individual/$2000 Family Deductible (per calendar year) Facility Level A: Level B: $100 Individual/$200 Family $500 Individual/$1000 Family
PLAN DESIGN AND BENEFITS - NYC Community Plan SM 6-11 PARTICIPATING PROVIDER REFERRED*
 Aetna Health Inc. for Referred Benefits Plan Effective Date: 10/1/2011 PLAN FEATURES Deductible (per calendar ) $5,000 Individual $15,000 Family Unless otherwise indicated, the Deductible must be met prior
Aetna Health Inc. for Referred Benefits Plan Effective Date: 10/1/2011 PLAN FEATURES Deductible (per calendar ) $5,000 Individual $15,000 Family Unless otherwise indicated, the Deductible must be met prior
PARTICIPATING PROVIDERS / REFERRED Deductible (per calendar year)
 Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Unlimited/ $1,000,000 per lifetime Primary Care Physician Selection
 PLAN FEATURES Deductible (per calendar year) None Individual None Family Member Coinsurance Out-of-Pocket Maximum $1,500 $3,000 Individual (per calendar year) $3,000 $6,000 Family Member cost sharing for
PLAN FEATURES Deductible (per calendar year) None Individual None Family Member Coinsurance Out-of-Pocket Maximum $1,500 $3,000 Individual (per calendar year) $3,000 $6,000 Family Member cost sharing for
Covered 100% 20% 1 exam per 12 months for members age 18 and older.
 PLAN FEATURES NON- Deductible (per calendar year) $1,200 Individual $2,000 Individual $3,600 Family $6,000 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred
PLAN FEATURES NON- Deductible (per calendar year) $1,200 Individual $2,000 Individual $3,600 Family $6,000 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING NO-REFERRAL 4.4 ($2,000 DED) $2,000 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING 3.4 ($1,500 DED) PARTICIPATING PROVIDERS. $1,500 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
Premium, balance-billed charges, penalties for not obtaining pre-authorization (pre-auth) for services, and health care this plan doesn't cover.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.assuranthealth.com or by calling 1-800-553-7654. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.assuranthealth.com or by calling 1-800-553-7654. Important
What is the overall deductible? Are there other deductibles for specific services? Is there an out-ofpocket
 Regence BlueShield: Regence Direct Silver with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers &
Regence BlueShield: Regence Direct Silver with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers &
In-network: $5,000 single / $10,000 family per calendar year. Out-of-network: $10,000 per insured per
 Regence BlueShield: Regence Direct Bronze HSA Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
Regence BlueShield: Regence Direct Bronze HSA Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
PLAN DESIGNS AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY INC
 Aetna Pharmacy Management Custom RX PLAN FEATURES Deductible (per calendar year) $250 Deductible Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member Coinsurance
Aetna Pharmacy Management Custom RX PLAN FEATURES Deductible (per calendar year) $250 Deductible Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member Coinsurance
Florida Health Network Only (HMO Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012
 Florida 2-100 Health Network Only (HMO Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOnly Plan 12-1500-80 HSA PLAN FEATURES Deductible (per calendar
Florida 2-100 Health Network Only (HMO Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOnly Plan 12-1500-80 HSA PLAN FEATURES Deductible (per calendar
Florida - EPO Aetna Select - ASC PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY PLAN FEATURES
 PLAN FEATURES Deductible (per calendar year) $100 Individual $200 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Pharmacy expenses do not apply towards the
PLAN FEATURES Deductible (per calendar year) $100 Individual $200 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Pharmacy expenses do not apply towards the
BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Coverage Period: 01/01/2015
 BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015 01/01/2015 12/31/2015-12/31/2015 Coverage
BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015 01/01/2015 12/31/2015-12/31/2015 Coverage
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by calling 1-585-343-0055 ext. 6415. Important Questions Answers
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by calling 1-585-343-0055 ext. 6415. Important Questions Answers
PARTICIPATING PROVIDERS / REFERRED Deductible (per calendar year)
 Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Value PPO
 BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Value PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at www.bridgespanhealth.com.
BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Value PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at www.bridgespanhealth.com.
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mylahc.org or by calling 1-855-475-3702. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mylahc.org or by calling 1-855-475-3702. Important Questions
Florida Health Network Only (HMO Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012
 Florida 2-100 Health Network Only (HMO Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOnly Plan 12-1500-Compass PLAN FEATURES Deductible (per calendar
Florida 2-100 Health Network Only (HMO Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOnly Plan 12-1500-Compass PLAN FEATURES Deductible (per calendar
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summacare.com or by calling 1-800-996-8701. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summacare.com or by calling 1-800-996-8701. Important
$300 Individual; $ 800 Family. Applies to out-of-network services only. What is the overall deductible?
 What is the overall deductible? This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.indecscorp.com or by
What is the overall deductible? This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.indecscorp.com or by
Not applicable Optional. CHE PREFERRED CARE (Home Host) Covered 100%
 PLAN FEATURES Catholic Health East PROVIDED BY LIFE INSURANCE COMPANY Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
PLAN FEATURES Catholic Health East PROVIDED BY LIFE INSURANCE COMPANY Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
Sigma-Aldrich Corporation Healthcare Plans MEDIUM Option Coverage Period: 01/01/ /31/2016 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mysialbenefits.com or by calling 1-877-335-7515, option
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mysialbenefits.com or by calling 1-877-335-7515, option
California Natural Products: EPO Option Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.deltahealthsystems.com or by calling 1-209-858-2525 Ext
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.deltahealthsystems.com or by calling 1-209-858-2525 Ext
PLAN DESIGN AND BENEFITS - New York Open Access MC 3-11 HSA Compatible
 PLAN FEATURES Deductible (per plan year) $3,000 Individual $6,000 Individual $6,000 Family $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered
PLAN FEATURES Deductible (per plan year) $3,000 Individual $6,000 Individual $6,000 Family $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered
01/01/ /31/2019 UMR: PALO PINTO GENERAL HOSPITAL:
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 UMR: PALO PINTO GENERAL HOSPITAL: 7670-00-160036 001 Coverage for: Individual
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 UMR: PALO PINTO GENERAL HOSPITAL: 7670-00-160036 001 Coverage for: Individual
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org/go/state or by calling 1-888-762-8633 Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org/go/state or by calling 1-888-762-8633 Important
PPO HSA HDHP $2,500 90/50
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $2,500 Individual $5,000 Family $5,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $2,500 Individual $5,000 Family $5,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member
Aetna Choice POS II Medical Plan PLAN FEATURES NETWORK OUT-OF-NETWORK. Individual Deductible* $1,000 $2,000. Family Deductible* $2,000 $4,000
 Schedule of Benefits Employer: Adobe Systems Incorporated ASC: 660819 Effective Date: January 1, 2012 Schedule: 2B Booklet Base: 1 For: Aetna Choice POS II 80/60 Plan This is an ERISA plan, and you have
Schedule of Benefits Employer: Adobe Systems Incorporated ASC: 660819 Effective Date: January 1, 2012 Schedule: 2B Booklet Base: 1 For: Aetna Choice POS II 80/60 Plan This is an ERISA plan, and you have
Coverage for: Individual + Family Plan Type: PPO
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 09/01/2018-12/31/2018 Venezia Transport Service: High Plan Coverage for: Individual + Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 09/01/2018-12/31/2018 Venezia Transport Service: High Plan Coverage for: Individual + Family
PLAN DESIGN AND BENEFITS AETNA LIFE INSURANCE COMPANY - Insured
 PLAN FEATURES Deductible (per calendar year) Individual $1,500 Family $3,000 All covered expenses accumulate simultaneously toward both the preferred and non-preferred Deductible. Unless otherwise indicated,
PLAN FEATURES Deductible (per calendar year) Individual $1,500 Family $3,000 All covered expenses accumulate simultaneously toward both the preferred and non-preferred Deductible. Unless otherwise indicated,
PLAN DESIGN AND BENEFITS - PA POS HSA COMPATIBLE NO-REFERRAL 2.4 ($2,500 Ded) PARTICIPATING PROVIDERS
 PLAN FEATURES Deductible (per plan year) $2,500 Individual NON- $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All
PLAN FEATURES Deductible (per plan year) $2,500 Individual NON- $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All
Important Questions Answers Why this Matters: For in-network providers: $11,000 Individual $22,000 Family of 2 or more
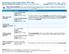 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/burton-lumber/or by calling 1-888-271-5870.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/burton-lumber/or by calling 1-888-271-5870.
Regence BlueCross BlueShield of Oregon: Preferred Coverage Period: 07/01/ /31/2016
 Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
Choice Easy Tier PPO Plus %/35% Coverage Period: On or after 1/1/2019. You don t have to meet deductibles for specific services.
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
(30- to 34-day supply) 100% after $40 copay; significant or new therapeutic class drugs: 50%
 C O U N T Y S I N T R A N E T S I T E : H T T P : / / I N T R A N E T. C O. R I V E R S I D E. C A. U S 25 Exclusive Care Select Medicare Coordination Plan Tier 1: Exclusive Care Network Tier 2: Any Provider
C O U N T Y S I N T R A N E T S I T E : H T T P : / / I N T R A N E T. C O. R I V E R S I D E. C A. U S 25 Exclusive Care Select Medicare Coordination Plan Tier 1: Exclusive Care Network Tier 2: Any Provider
In-Network (IN): $2,000/Individual, $4,000/Family per benefit period. Out-of-Network (OON): $4,000/Individual, $8,000/Family per benefit period.
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
PLAN DESIGN AND BENEFITS - IN MANAGED CHOICE POS OPEN ACCESS 90/60/60 $1,000 PREFERRED CARE
 PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
VA Aetna Coastal VA HP Silver $10 Copay
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
Marsh and McLennan: Anthem Blue Cross and Blue Shield $2,850 Deductible Plan Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
PLAN DESIGN AND BENEFITS MC Open Access Plan 1913
 PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year) $1,500 Individual $4,500 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior
PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year) $1,500 Individual $4,500 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior
$ 400 person/ $1,200 family; Waived for inpatient and outpatient hospital charges at Centers of Excellence and Hospitals of Distinction.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mbpet.net or by calling 1-888-742-3380. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mbpet.net or by calling 1-888-742-3380. Important Questions
DE Aetna Silver $5 Copay 2750 PPO
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
VA Aetna Whole Health Catastrophic 100%
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
Quote Effective: 04/01/ /30/2019 Version Updated: 01/07/2019
 Quote Effective: 04/01/2019-06/30/2019 Version Updated: 01/07/2019 Print Package: HIOS ID (Enrollment Code) 78124NY1000265-00 (SON5) Plan Name: Rating Region: Rate Rochester For the Benefits described
Quote Effective: 04/01/2019-06/30/2019 Version Updated: 01/07/2019 Print Package: HIOS ID (Enrollment Code) 78124NY1000265-00 (SON5) Plan Name: Rating Region: Rate Rochester For the Benefits described
Participating MEMBER RESPONSIBILITY
 Deductible 80% $500 Preferred Provider Organization Underwritten by Coventry Health and Life Insurance Company (d.b.a. HealthAmerica) DEDUCTIBLES AND MAXIMUMS Annual Deductible Individual $500 $1,000 Family
Deductible 80% $500 Preferred Provider Organization Underwritten by Coventry Health and Life Insurance Company (d.b.a. HealthAmerica) DEDUCTIBLES AND MAXIMUMS Annual Deductible Individual $500 $1,000 Family
$8,300 $24,900 Maximum Lifetime Benefit
 PPO Schedule of Health Plus 2 C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive
PPO Schedule of Health Plus 2 C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive
Important Questions. Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cnichs.com or http://secure.healthx.com/cnic_new.aspx
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cnichs.com or http://secure.healthx.com/cnic_new.aspx
Important Questions Answers Why this Matters: Network: $500 Individual / $1,000 Family Non-Network: $1,000 Individual / $2,000 Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-262-4772.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-262-4772.
OH Aetna Gold $5 Copay
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
15% 30% $7,350 Individual Unlimited Individual (per calendar year) Out-Of-Pocket Maximum
 PLAN FEATURES Deductible (per calendar year) $1,750 Individual $20,000 Individual $3,500 Family $40,000 Family All covered expenses accumulate toward both the preferred and non-preferred Deductible. Unless
PLAN FEATURES Deductible (per calendar year) $1,750 Individual $20,000 Individual $3,500 Family $40,000 Family All covered expenses accumulate toward both the preferred and non-preferred Deductible. Unless
2018 Summary of Benefits
 2018 Summary of Benefits Barry, Christian, Greene, Jasper, Lawrence, and Newton Counties, MO H1664--001 Benefits effective January 1, 2018 H1664_18_2916SB Accepted 09302017 This booklet provides you with
2018 Summary of Benefits Barry, Christian, Greene, Jasper, Lawrence, and Newton Counties, MO H1664--001 Benefits effective January 1, 2018 H1664_18_2916SB Accepted 09302017 This booklet provides you with
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.empireblue.com/eocdps/fi or by calling 1-855-220-3341.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.empireblue.com/eocdps/fi or by calling 1-855-220-3341.
PLAN DESIGN AND BENEFITS - New York Open Access EPO 4-10/10 HSA Compatible
 PLAN FEATURES Deductible (per plan year) $3,500 Individual $7,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. The Individual Deductible can only be met
PLAN FEATURES Deductible (per plan year) $3,500 Individual $7,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. The Individual Deductible can only be met
Aetna Select Medical Plan PLAN FEATURES NETWORK OUT-OF-NETWORK. Plan Maximum Out of Pocket Limit excludes precertification penalties.
 Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 25, 2016 Effective Date: January 1, 2016 Schedule: 12D Booklet Base: 12 For: Aetna Select - Security Staff (Outside CT) Electing
Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 25, 2016 Effective Date: January 1, 2016 Schedule: 12D Booklet Base: 12 For: Aetna Select - Security Staff (Outside CT) Electing
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.careconnect.com or by calling 1-855-706-7545. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.careconnect.com or by calling 1-855-706-7545. Important
Important Questions Answers Why this Matters:
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
BridgeSpan Health Company: BridgeSpan Silver HDHP 2000 MyChoice Northwest
 BridgeSpan Health Company: BridgeSpan Silver HDHP 2000 MyChoice Northwest Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Individual
BridgeSpan Health Company: BridgeSpan Silver HDHP 2000 MyChoice Northwest Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Individual
What is the overall deductible? Are there services covered before you meet your deductible?
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
Florida Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012
 Florida 2-100 Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOption Plan 12-2000-70 PLAN FEATURES PARTICIPATING PROVIDERS
Florida 2-100 Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOption Plan 12-2000-70 PLAN FEATURES PARTICIPATING PROVIDERS
BridgeSpan Health Company: BridgeSpan Bronze Essential 6850 Value PPO
 BridgeSpan Health Company: BridgeSpan Bronze Essential 6850 Value PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at www.bridgespanhealth.com.
BridgeSpan Health Company: BridgeSpan Bronze Essential 6850 Value PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at www.bridgespanhealth.com.
Student Health Insurance Plan Insurance Company Coverage Period: 08/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.studentplanscenter.com or by calling 1-800-756-3702.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.studentplanscenter.com or by calling 1-800-756-3702.
AvMed In-Network Tier A Providers: $1,500 individual / $3,000 family AvMed In-Network Tier B Providers: What is the overall deductible?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
Medical Plan Options - Retirees Age 65 or Over/ Disabled Participants with Medicare Coverage
 l Plan Options - Retirees Age 65 or Over/ Disabled Participants with re Program Name Group Prime Solution Group Prime Solution for Seniors for Seniors Type of Policy re Cost Plan with re Prescription Drug
l Plan Options - Retirees Age 65 or Over/ Disabled Participants with re Program Name Group Prime Solution Group Prime Solution for Seniors for Seniors Type of Policy re Cost Plan with re Prescription Drug
What is the overall deductible? Are there other deductibles for specific services? Is there an out-of-pocket limit on my expenses?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nhp.org or by calling Customer Service at 1-866-414-5533
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nhp.org or by calling Customer Service at 1-866-414-5533
Florida Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012
 Florida 2-100 Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN FEATURES PREFERRED PROVIDERS NON-PREFERRED PROVIDERS Deductible (per calendar year) PLAN DESIGN
Florida 2-100 Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN FEATURES PREFERRED PROVIDERS NON-PREFERRED PROVIDERS Deductible (per calendar year) PLAN DESIGN
PLAN COMPARISON (Blue Cross Blue Shield of Massachusetts) For Members Who Are Eligible For Medicare
 Quarterly Premium Rate * Per Person $2,215.08 $1,789.50 $618.99 $890.70 Rates effective: 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 Eligibility Service
Quarterly Premium Rate * Per Person $2,215.08 $1,789.50 $618.99 $890.70 Rates effective: 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 Eligibility Service
PLAN COMPARISON (Blue Cross Blue Shield of Massachusetts) For Members Who Are Eligible For Medicare
 Quarterly Premium Rate * Per Person $2,358.60 $1,905.33 $658.74 $1,165.11 Rates effective: 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 Eligibility Service
Quarterly Premium Rate * Per Person $2,358.60 $1,905.33 $658.74 $1,165.11 Rates effective: 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 Eligibility Service
California Small Group MC Aetna Life Insurance Company NETWORK CARE
 PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
Even though you pay these expenses, they don t count toward the outof-pocket limit.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summit-inc.net or www.yctrust.net or by calling Summit
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summit-inc.net or www.yctrust.net or by calling Summit
Regence BlueShield: Choice HSA 1500 Coverage Period: 01/01/ /31/2016
 Regence BlueShield: Choice HSA 1500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual & Eligible Family Plan Type:
Regence BlueShield: Choice HSA 1500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual & Eligible Family Plan Type:
SUPPLEMENT TO BROWN UNIVERSITY STUDENT HEALTH INSURANCE PROGRAM SUMMARY BROCHURE
 SUPPLEMENT TO 2017-2018 BROWN UNIVERSITY STUDENT HEALTH INSURANCE PROGRAM SUMMARY BROCHURE This Supplement is designed to clarify additional specific benefits outlined in the Summary Brochure while the
SUPPLEMENT TO 2017-2018 BROWN UNIVERSITY STUDENT HEALTH INSURANCE PROGRAM SUMMARY BROCHURE This Supplement is designed to clarify additional specific benefits outlined in the Summary Brochure while the
Summary of Benefits. Allwell Medicare (HMO) Bexar County, TX H Benefits effective January 1, 2018 H0062_18_2962SB_Accepted
 2018 Summary of Benefits Bexar County, TX H0062 -- 001 Benefits effective January 1, 2018 H0062_18_2962SB_Accepted 09102017 This booklet provides you with a summary of what we cover and your cost-sharing.
2018 Summary of Benefits Bexar County, TX H0062 -- 001 Benefits effective January 1, 2018 H0062_18_2962SB_Accepted 09102017 This booklet provides you with a summary of what we cover and your cost-sharing.
What is the overall deductible?
 Regence BlueShield of Idaho: Evolve Core Coverage Period: 07/01/2013 06/30/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible Family Plan Type:
Regence BlueShield of Idaho: Evolve Core Coverage Period: 07/01/2013 06/30/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible Family Plan Type:
2018 Summary of Benefits
 2018 Summary of Benefits Benton, Crawford, Sebastian, Washington Counties, AR H9630--001 Benefits effective January 1, 2018 H9630_18_2913SB Accepted 09302017 This booklet provides you with a summary of
2018 Summary of Benefits Benton, Crawford, Sebastian, Washington Counties, AR H9630--001 Benefits effective January 1, 2018 H9630_18_2913SB Accepted 09302017 This booklet provides you with a summary of
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summacare.com or by calling 1-800-996-8701. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summacare.com or by calling 1-800-996-8701. Important
PLAN DESIGN AND BENEFITS Standard PPO Plan
 North Carolina PPO (Mandated 1 Life Plan) PLAN DESIGN AND BENEFITS Standard PPO Plan PLAN FEATURES PARTICIPATING Deductible (per plan year) $500 Individual $1,000 Individual $1,500 Family $3,000 Family
North Carolina PPO (Mandated 1 Life Plan) PLAN DESIGN AND BENEFITS Standard PPO Plan PLAN FEATURES PARTICIPATING Deductible (per plan year) $500 Individual $1,000 Individual $1,500 Family $3,000 Family
$4,800 $9,600 Maximum Lifetime Benefit
 PPO Schedule of PPO Medical C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive months
PPO Schedule of PPO Medical C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive months
Summary of Benefits. Allwell Medicare (HMO) Palm Beach, Manatee, Marion and Seminole Counties, Florida H
 2018 Summary of Benefits Palm Beach, Manatee, Marion and Seminole Counties, Florida H9276-003 Benefits effective January 1, 2018 H9276_18_2860SB_A Accepted 09172017 This booklet provides you with a summary
2018 Summary of Benefits Palm Beach, Manatee, Marion and Seminole Counties, Florida H9276-003 Benefits effective January 1, 2018 H9276_18_2860SB_A Accepted 09172017 This booklet provides you with a summary
For non-preferred providers: $14,300 Person/$28,600 Family. Doesn t apply to preventive care services or glasses for children.
 WPS Preferred Plan: Bronze 7150 Coverage Period: 1/1/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: PPO This is only a summary.
WPS Preferred Plan: Bronze 7150 Coverage Period: 1/1/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: PPO This is only a summary.
Coverage Period: Beginning on or after 01/01/2018 Coverage for: Individual + Family Plan Type: PPO
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services S.PIC.7350.100.50 (Silver) Coverage Period: Beginning on or after 01/01/2018 Coverage for: Individual + Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services S.PIC.7350.100.50 (Silver) Coverage Period: Beginning on or after 01/01/2018 Coverage for: Individual + Family
Schedule of Benefits (GR-9N-S DE)
 Schedule of Benefits (GR-9N-S-01-001-01 DE) Plan Sponsor: The Church of Jesus Christ of Latter-Day Saints-Senior Missionaries Group Policy Number: 840232 Issue Date: June 3, 2013 Effective Date: August
Schedule of Benefits (GR-9N-S-01-001-01 DE) Plan Sponsor: The Church of Jesus Christ of Latter-Day Saints-Senior Missionaries Group Policy Number: 840232 Issue Date: June 3, 2013 Effective Date: August
Heavy & General 472/172 of NJ Welfare Fund: Class 1 & 2 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 Heavy & General 472/172 of NJ Welfare Fund: Class 1 & 2 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 04/01/2014-03/31/2015 Coverage for: Individual + Family
Heavy & General 472/172 of NJ Welfare Fund: Class 1 & 2 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 04/01/2014-03/31/2015 Coverage for: Individual + Family
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
2018 Summary of Benefits
 2018 Summary of Benefits Allwell Medicare Select (HMO) Benton, Washington counties, AR H9630--003 Benefits effective January 1, 2018 H9630_18_2915SB Accepted 09302017 This booklet provides you with a summary
2018 Summary of Benefits Allwell Medicare Select (HMO) Benton, Washington counties, AR H9630--003 Benefits effective January 1, 2018 H9630_18_2915SB Accepted 09302017 This booklet provides you with a summary
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-855-333-5734. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-855-333-5734. Important
Community Core PPO Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mycmc.com to log onto the Community Medical Centers Forum
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mycmc.com to log onto the Community Medical Centers Forum
Deductible Per Calendar Year In-network Out-of-network
 PSGBS.ID.SG.MED.HMO.0119 F3927435 Medical Benefit Summary BrightIdea Gold 1000 Provider Network: BrightPath Deductible Per Calendar Year In-network Out-of-network Individual/Family $1,000/$2,000 $10,000/$20,000
PSGBS.ID.SG.MED.HMO.0119 F3927435 Medical Benefit Summary BrightIdea Gold 1000 Provider Network: BrightPath Deductible Per Calendar Year In-network Out-of-network Individual/Family $1,000/$2,000 $10,000/$20,000
For: Choice POS II - Clerical & Technical and Service & Maintenance Employees Choice POS II (Base Rx) Plan
 Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: June 23, 2016 Effective Date: January 1, 2016 Schedule: 2A Booklet Base: 2 For: Choice POS II - Clerical & Technical and Service &
Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: June 23, 2016 Effective Date: January 1, 2016 Schedule: 2A Booklet Base: 2 For: Choice POS II - Clerical & Technical and Service &
What is the overall deductible? Are there other deductibles for specific services?
 Regence BlueShield: Innova Coverage Period: 08/01/2016 07/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Eligible Family Plan Type: PPO This
Regence BlueShield: Innova Coverage Period: 08/01/2016 07/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Eligible Family Plan Type: PPO This
OH Aetna Silver $5 Copay 2750 NA CSR $0
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-855-586-6960.
Lourdes Health System Proposed Effective Date: Aetna Helathfund Aetna Choice POS ll - ASC Salary Band: Less than $21,000 to $41,999
 PROVIDED BY LIFE INSURANCE COMPANY FUND FEATURES HealthFund Amount $750 Employee $1,500 Employee + Spouse $1,500 Employee + Child(ren) $1,500 Family Amount contributed to the Fund by the employer Fund
PROVIDED BY LIFE INSURANCE COMPANY FUND FEATURES HealthFund Amount $750 Employee $1,500 Employee + Spouse $1,500 Employee + Child(ren) $1,500 Family Amount contributed to the Fund by the employer Fund
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-398-6177.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-398-6177.
