BPCI Advanced: Updates from CMS and Details on the New Pricing Methodology. April 26, MedAxiom Consulting, LLC. All rights reserved.
|
|
|
- Augustine Elliott
- 5 years ago
- Views:
Transcription
1 BPCI Advanced: Updates from CMS and Details on the New Pricing Methodology April 26,
2 Attendee Control Panel Grab Tab Click arrow to open/close Control Panel. Audio pane Select audio format. Select Telephone or Mic & Speakers devices. When using telephone, be sure to use your pin number. Raise Hand When vocal questions/comments are allowed, please select the hand icon to get the presenter s attention. A red arrow means your hand is raised. Handouts when available, you are now able to download handout materials from this pane. Questions pane If turned on by an organizer, attendees can submit questions and review answers. Broadcast messages to attendees will also show here. Type your question and click Send to submit it to the organizer 2
3 Keely Macmillan GM BPCI Advanced Archway Health Joel Sauer Vice President MedAxiom Consulting Ginger Biesbrock Vice President MedAxiom Consulting 3
4 THE SOLUTION Add slide about MedAxiom / Archway relationship EDUCATION DATA READINESS & OPTIMIZATION TOOLS & SOLUTIONS The MedAxiom & Archway Health partnership is intended to make design and implementation of bundled payment programs as simple as possible for heart programs. The team combines the expertise of CV consultants, proven healthcare operators, big data analysts, and technology entrepreneurs. 4 4
5 Introduction CMS announced the voluntary Bundled Payment for Care Improvement (BPCI) Advanced program on Tuesday Jan 9 th Non-binding application due March 12, 2018 for Oct 1 st, 2018 start date Open window period in 2019 for Jan 1, 2020 start date Goals of today s webinar: BPCI Advanced Application Timeline & Updates from CMS Details on the New Pricing Model Address questions from the group
6 BPCI Advanced Application Timeline & Updates from CMS 01 6
7 BPCI Advanced Timeline Providers must decide by Aug 1 st whether to participate in BPCI Advanced starting Oct 1 st Updates from CMS CMS received great interest in BPCI Advanced; are continuing to work through the program s high volume of inquiries Data and target prices to be released in May Further Details on Pricing Methodology: CMS currently working on specifications and plan to make them available soon File formats for the historical claims files: CMS is still finalizing the data file layouts and variables and will provide sample file layouts to Applicants prior to the release of the historical data Archway has asked CMS to provide more specificity Applicants should expect to review their data and target prices in June
8 Details on the new Pricing Methodology 02 8
9 Archway s Pricing Experts MAH-JABEEN SOOBADER, PH.D, MPH, CHIEF ANALYTICS OFFICER JUN WANG, PHD, MD PRINCIPAL DATA SCIENTIST BONGANI MNGOMEZULU, VP OF ANALYTICS
10 CMS Goals Informing BPCI-A Pricing Methodology Encourage both high and low cost providers to participate Reward participants improvement over time Adjust for patient case mix that is not under the providers control Allow for trends in regional and other relevant provider characteristics Induce Medicare savings while maintaining high quality care
11 Overview of Episode-Specific Price Setting Start with 4 years of historical baseline data: Standardize payments to remove variations caused by geography (e.g. Area Wage) and Payment Policy (e.g. IME) Apply Index Price Trending to standardize year to year variation in pricing (e.g. inflation, changes in DRG weight, etc) Apply Patient Case Mix Adjustment to account for varying levels of patient severity Apply Peer Adjusted Trend (PAT) Factor to account for differences in peer hospitals
12 Overview of Episode-Specific Price Setting Start with 4 years of historical baseline data: Standardize payments to remove variations caused by geography (e.g. Area Wage) and Payment Policy (e.g. IME) Apply Index Price Trending to standardize year to year variation in pricing (e.g. inflation, changes in DRG weight, etc) Apply Patient Case Mix Adjustment to account for varying levels of patient severity Apply Peer Adjusted Trend (PAT) Factor to account for differences in peer hospitals
13 Overview of Episode-Specific Price Setting Start with 4 years of historical baseline data: Standardize payments to remove variations caused by geography (e.g. Area Wage) and Payment Policy (e.g. IME) Index Price Trending to standardize year to year variation in pricing (e.g. inflation, changes in DRG weight, etc) Apply Patient Case Mix Adjustment to account for varying levels of patient severity Apply Peer Adjusted Trend (PAT) Factor to account for differences in peer hospitals
14 Overview of Episode-Specific Price Setting Start with 4 years of historical baseline data: Standardize payments to remove variations caused by geography (e.g. Area Wage) and Payment Policy (e.g. IME) Index Price Trending to standardize year to year variation in pricing (e.g. inflation, changes in DRG weight, etc) Apply Patient Case Mix Adjustment to risk-adjust for varying levels of patient severity (episode specific regression) Apply Peer Adjusted Trend (PAT) Factor to account for differences in peer hospitals
15 CMS to apply Episode Specific, Two-Stage Risk Adjustment Stage 1: Benchmark participant against other providers with patient populations of similar levels of expenditure risk Patient Case-mix Adjustment HCCs Demographics (age, dual eligibility, etc) Recent resource use Long term Institutional MS-DRGs APCs Episode Specific Factors (fractures)
16 CMS uses Hierarchical Condition Categories (HCCs) to risk adjust payments based on patient complexity Methodology uses a patient s documented diagnostic coding history to predict financial utilization and risk Accurate coding and complete documentation is needed to capture the full complexity of a patient population 2017 CMS-HCC Risk Adjustment Model (V. 22) 9,500 ICD-10-CM codes map to one or more of the 79 HCC codes included Version 22 HCC Examples: Cancer, Heart Disease, Kidney Disease, Liver Disease, Pneumonia, Major Depressive, Bipolar, Paranoid Disorders, Drug/Alcohol dependence
17 Example: Impact of Patient Case-mix Adjustments Avg Episode Payment per HCC Count for MS-DRG 470, MJRLE Avg Episode Payment per HCC Count for MS-DRG 291, CHF w/mcc
18 CMS to apply Episode Specific, Two-Stage Risk Adjustment Stage 1: Benchmark participant against other providers with patient populations of similar levels of expenditure risk Patient Case-mix Adjustment HCCs Demographics (age, dual eligibility, etc) Recent resource use Long term Institutional MS-DRGs APCs Episode Specific Factors (fractures)
19 Example: Impact of Patient Case-mix Adjustments Avg Episode Payment by Age category and dual eligibility status for MS-DRG 470, MJRLE Avg Episode Payment by Age category and dual eligibility status for MS-DRG 291, CHF w/mcc 28,192 31,261 Age Dual Eligibility Age No Yes Dual Eligibility
20 CMS to apply Episode Specific, Two-Stage Risk Adjustment Stage 1: Benchmark participant against other providers with patient populations of similar levels of expenditure risk Patient Case-mix Adjustment HCCs Demographics (age, dual eligibility, etc) Recent resource use Long term Institutional MS-DRGs APCs Episode Specific Factors (fractures)
21 Overview of Episode-Specific Price Setting Start with 4 years of historical baseline data: Standardize payments to remove variations caused by geography (e.g. Area Wage) and Payment Policy (e.g. IME) Index Price Trending to standardize year to year variation in pricing (e.g. inflation, changes in DRG weight, etc) Apply Patient Case Mix Adjustment to risk-adjust for varying levels of patient severity (episode specific regression) Apply Peer Adjusted Trend (PAT) Factor to account for differences in peer hospitals (episode specific regression)
22 CMS to apply Episode Specific, Two-Stage Risk Adjustment Stage 2: Benchmark participant against other providers with similar hospital-level characteristics (peer groups) Patient Case-mix Adjustment HCCs Demographics (age, dual eligibility, etc) Recent resource use Long term Institutional MS-DRGs APCs Episode Specific Factors (fractures) Peer Groups Adjustment Census Division- 9 regions Academic Medical Centers Urban-Rural Safety-Net Hospitals- >60% duals Bed-size
23 9 US Census Regions CMS employed Census Regions in CJR and Cardiac EPMs pricing methodology
24 Example: Impact of Regional Adjustments for AMI States vs 9 Regions
25 Example: Impact of Regional Adjustments for CHF States vs 9 Regions State: $22,317 - $28,506 Regional: $23,230 - $27,380
26 Example: Impact of Regional Adjustments for OP PCI States vs 9 Regions State: $14,516 - $17,420 Regional: $14,983 - $16,584
27 CMS to apply Episode Specific, Two-Stage Risk Adjustment Stage 2: Benchmark participant against other providers with similar hospital-level characteristics (peer groups) Patient Case-mix Adjustment HCCs Demographics (age, dual eligibility, etc) Recent resource use Long term Institutional MS-DRGs APCs Episode Specific Factors (fractures) Peer Groups Adjustment Census Division- 9 regions Academic Medical Centers Urban-Rural Safety-Net Hospitals- >60% duals Bed-size
28 Example: Impact of Peer-Group Characteristics Comparing Like Providers Episode: Major Joint Replacement of Lower Extremity. MS-DRG: 470
29 Setting Hospital and PGP Prices 03 29
30 Hospital Benchmark Price Based on hospital historical performance with adjustments for trends in spending of peer group hospitals and patient case mix: Hospital Benchmark Price = Standardized Baseline Spending x Patient Case Mix Adjustment x Peer Adjusted Trend Factor
31 Calculation of Hospital Benchmark Price (HBP) Adjust for hospital historical payment Adjust for patient severity Adjust for hospital peer group trend Dollar Amount (Average episode spending across hospitals) $40,350 Efficiency Measure Standardized Baseline Spending Patient Case Mix Adjustment Peer Adjusted Trend Factor Hospital Benchmark Price x 1.06 $42,962 x 0.81 x 1.36 $47,327 x 0.99 $40,125 x 0.80 x 1.15 $36,915
32 Hospital-Specific PGP Benchmark Price PGP benchmark price builds upon Hospital Benchmark Price PGP will have unique benchmark price for each hospital that initiates an episode Hospital-specific PGP Benchmark Price = Hospital Benchmark Price x PGP Offset x PGP Relative Case Mix PGP Offset Measures PGP s historical efficiency relative to the efficiency of the acute hospital during baseline PGP Relative Case Mix Measures PGP s case-mix relative to the case-mix of the ACH during the baseline
33 Adjust for PGP historical payment Adjust for PGP patient severity Calculation of PGP Benchmark Hospital Benchmark Price PGP Offset PGP s historical efficiency relative to hospital PGP Relative Case Mix PGP-ACH Benchmark Price Price $47,327 x 1.00 x 1.06 $50,167 PGP 1-ACH1 x 0.96 x 0.93 $42,254 PGP 2-ACH1 x 1.06 x 0.88 $34,434 PGP 1-ACH2 $36,915 x 1.00 x 1.15 $42,452 PGP 2-ACH2
34 Preliminary and Final Target Price Preliminary Target Price = Benchmark Price - Program Discount(3%) x Real $ conversion Final Target Price = Preliminary Target Price adjusted with Case Mix and Real $ Conversion in Model Year Participants will receive Preliminary Target Price during the application process (May 2018) Final Target Price will be determined after performance period is complete to account for case-mix changes during implementation
35 Calculation of Preliminary Target Price Adjust for 3% program discount Convert standardized $ to real $ Preliminary Benchmark Price (hospital or PGP) Program Discount (3%) Preliminary Target Price (in standardized $) Real to Standardized Payment Ratio (Reverse payment standardization) Preliminary Target Price (in real $) $47,327 x 0.97 $45,907 x 1.01 $46,366
36 Additional Risk Protection Individual Case Level: Capping episode payment at 1 st and the 99 th percentiles to reduce the impact of outlier spend and protect providers from loss due to catastrophic events Aggregate Episode Initiator Level: 20% stop-loss
37 Implications of Pricing Methodology 04 37
38 Impact of Model Year and Baseline Period on Opportunity ~ 2 Year Lag ? ? Model Year ? ?
39 Evaluating Your Opportunity during Five-Year BPCI Advanced Performance Period Low-cost hospital with continuous cost reduction Low-cost hospital with no cost reduction Scenario 1: Initially highperforming lowcost provider (assumes 10% lower cost than peer group) $14,000 $13,000 $12,000 $11,000 $10,000 $9,000 Peer Group Performance Actual Performance Target Price $14,000 $13,000 $12,000 $11,000 $10,000 $9,000 Peer Group Performance Actual Performance Target Price $8, $8, Model Year Model Year If an initial low cost provider (assume 10% lower cost) continues to reduce costs but at a lower rate of reduction (3%) than peer groups (5%), the provider will maintain 3-5% savings during the program If the provider reduces cost at the same rate as its peer group, the provider could increase savings from 7% to 18% If initial low cost provider doesn t reduce their cost while peer groups are reducing the cost (5%) they will likely lose their initial 2% pricing advantage and could end up losing 2% at later model years
40 Evaluating Opportunity during Five-Year BPCI Advanced Performance Period High-cost hospital with continuous cost reduction High-cost hospital with no cost reduction Scenario 2: Initially lowperforming high-cost provider (assumes 10% higher cost than peers) $15,000 $14,000 $13,000 $12,000 $11,000 $10,000 $9,000 $8,000 Peer Group Performance Actual Performance Target Price Model Year $15,000 $14,000 $13,000 $12,000 $11,000 $10,000 $9,000 $8, Model Year Peer Group Performance Actual Performance Target Price The high cost provider (assumes 10% higher cost than peer group) will require a 7% cost-reduction to break even in the first year If the high cost provider continues to reduce the cost at the same rate as peer group (5% cost reduction), the provider will begin to save in 2020 and increase their savings from 2% to 10% If high-cost provider does not reduce their cost while the peer groups are reducing their cost (5%), the provider will lose throughout the model year and their losses will increase over time from 8% to 12%.
41 Criteria Archway will be evaluating to help providers make informed decisions on program and episode participation Risk Parameter Sample Size Payment Variation Episode Post-Acute Spend Price Risk Quality Measures Savings Opportunity Break Even Catastrophic/cases outliers High cost patients Definition The number of episodes in the measurement period Variation among episode payment Percent of episode PAC spend Difference between target price and historic spend Impact of quality measure on discount or savings Amount of potential savings from Benchmark The amount of savings opportunity to break-even on price Evaluate stop-loss threshold for outliers Percent of high cost patients that don t reach stop loss
42 Criteria Archway will be evaluating to help providers make informed decisions on program and episode participation Risk Parameter Trending Baseline Trending Pre-Implementation Price Advantage Stability PGP-AC Heterogeneity within Episode Impact of model pricing parameters Prior Value Based Experience Market Advantage Program Policy and Pricing Changes Definition Episode Risk in by quarter Episode Risk in 2017 Q1-Q3 Evaluation of savings relative to savings of peers over time Exposure ratio of patients at multiple hospitals Evaluate within episode the impact of case-mix on pricing variations Evaluate within episode the impact of model fit to savings BPCI Participant, ACO etc. Local market characteristics-competitive Evaluate potential program changes based on prior BPCI and OCM
43 Keys to Success 1 2 Providers will need to understand their historical performance to fully evaluate their opportunity in the program. What impacted their price What are the major cost drivers of price relative to their peers Implementation strategies will need to be provider specific. High-cost providers will benefit from reducing costs through improving quality and efficiency Low-cost providers will need to evaluate their pricing advantage, as well as their ability to further improve against feasible benchmarks. 3 Providers will need to continuously evaluate their opportunity during the 5-year performance period ( ). Success will be driven not just by your initial pricing, but also pricing changes over the course of the program and your opportunity to increase savings relative to their peers. 4 With hospital-specific prices for PGPs, new alignments will be forged between PGPs and hospitals Partnering with the right providers will be critical
44 Community Learning 05 44
45 Archway Academy Online, self-paced learning program to get you prepared for BPCI Advanced Join the Discussion Forum and see what your peers are asking
46 Participate in Archway s BPCI Advanced Workshop Tuesday, June 26, 2018 Join other applicants for a one-day event featuring BPCI Advanced insights and updates from experienced program experts Shared learning and best practices from BPCI participants Networking with other applicants and peers Detailed data and pricing model review One-on-one meetings to review your data Strategies for how to drive success in the first few program quarters Demonstration of the latest features in Archway Carelink and Analytics Workshop Details: Time: 10 am to 9 pm, including cocktails and dinner following the program Location: Archway Main Office, 311 Arsenal Street, Watertown, MA (10 minutes from downtown Boston) Cost: Event registration is complimentary and includes all meals and activities Additional: Participants are responsible for transportation and lodging RSVP today to reserve your spot. Contact events@archwayha.com. Space is limited.
47 Keely Macmillan GM BPCI Advanced Archway Health Q&A Ginger Biesbrock Vice President MedAxiom Consulting Joel Sauer Vice President MedAxiom Consulting 47
Opportunities for Orthopedic Specialists in BPCI Advanced
 Opportunities for Orthopedic Specialists in BPCI Advanced January 13 th, 2018 Introduction CMS announced the voluntary Bundled Payment for Care Improvement (BPCI) Advanced program on Tuesday, Jan 9 th
Opportunities for Orthopedic Specialists in BPCI Advanced January 13 th, 2018 Introduction CMS announced the voluntary Bundled Payment for Care Improvement (BPCI) Advanced program on Tuesday, Jan 9 th
Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017
 To Dial-in: 877.668.4490 or 408.792.6300 Event Number: 669 367 723 Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017 CMS Final Rule and Materials Advancing Care Coordination through
To Dial-in: 877.668.4490 or 408.792.6300 Event Number: 669 367 723 Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017 CMS Final Rule and Materials Advancing Care Coordination through
Housekeeping. Questions
 Housekeeping To join us on audio, dial the phone number in the teleconference box and follow the prompts. Please dial in with your Attendee ID number. The Attendee ID number will connect your name in WebEx
Housekeeping To join us on audio, dial the phone number in the teleconference box and follow the prompts. Please dial in with your Attendee ID number. The Attendee ID number will connect your name in WebEx
Get Straight on MACRA in 2018
 Quality Reporting Roundtable Get Straight on MACRA in 2018 FAQs, Advisory Board Guidance, and Resources Ye Hoffman, MS, CPHIMS Consultant March 27, 2018 research technology consulting 2 Manage Your Audio
Quality Reporting Roundtable Get Straight on MACRA in 2018 FAQs, Advisory Board Guidance, and Resources Ye Hoffman, MS, CPHIMS Consultant March 27, 2018 research technology consulting 2 Manage Your Audio
Troubleshooting Audio
 Welcome! Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Welcome! Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
HEALTH POLICY & EDUCATION SERIES
 HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
Appendix B. LDO Financial Methodology (LDO CEC Model)
 Appendix B LDO Financial Methodology (LDO CEC Model) TABLE OF CONTENTS Table of Contents... i Table of Exhibits... iii Glossary... iv List of Acronyms... viii 1. Introduction... 1 1.1 Identifying and Aligning
Appendix B LDO Financial Methodology (LDO CEC Model) TABLE OF CONTENTS Table of Contents... i Table of Exhibits... iii Glossary... iv List of Acronyms... viii 1. Introduction... 1 1.1 Identifying and Aligning
Total Cost of Care (TCOC) Workgroup. January 30, 2019
 Total Cost of Care (TCOC) Workgroup January 30, 2019 Agenda Introductions Updates on initiatives with CMS Y1 MPA (PY18) Implementation Timing Y2 MPA (PY19) MPA Operations Reporting and Attribution Stability
Total Cost of Care (TCOC) Workgroup January 30, 2019 Agenda Introductions Updates on initiatives with CMS Y1 MPA (PY18) Implementation Timing Y2 MPA (PY19) MPA Operations Reporting and Attribution Stability
OPPS Webinar Information
 OPPS Webinar Information 1.You will not hear any audio until the webinar begins. 2. To join the audio, select call me and enter your phone number or select I will call in. If you select I will call in,
OPPS Webinar Information 1.You will not hear any audio until the webinar begins. 2. To join the audio, select call me and enter your phone number or select I will call in. If you select I will call in,
Executive Summary: Hospital episode initiators: Change in mandatory MSAs:
 On November 16, 2015, the Centers for Medicare and Medicare Services (CMS) released the final rule for the Comprehensive Care for Joint Replacement (CJR) model, which creates a mandatory lower extremity
On November 16, 2015, the Centers for Medicare and Medicare Services (CMS) released the final rule for the Comprehensive Care for Joint Replacement (CJR) model, which creates a mandatory lower extremity
Understanding the 2020 Medicare Advantage Advance Notice Part I
 Understanding the 2020 Medicare Advantage Advance Notice Part I Jennifer Carioto, FSA, MAAA Jennifer Carioto is a consulting actuary with the New York office of Milliman. She specializes in Medicare Advantage
Understanding the 2020 Medicare Advantage Advance Notice Part I Jennifer Carioto, FSA, MAAA Jennifer Carioto is a consulting actuary with the New York office of Milliman. She specializes in Medicare Advantage
FMV Considerations for Bundled Payment Arrangements
 FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
Medicare Spending Per Beneficiary (MSPB) Measure
 Medicare Spending Per Beneficiary (MSPB) Measure Audio for this event is available via INTERNET STREAMING. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming
Medicare Spending Per Beneficiary (MSPB) Measure Audio for this event is available via INTERNET STREAMING. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming
Impact of ACOs on Care Coordination
 Impact of ACOs on Care Coordination Presented by: Michelle L. Templin Vice President Legislative Affairs and Business Development MHA ACO Network March 2, 2017 Agenda Agenda Key Regulatory Drivers Accountable
Impact of ACOs on Care Coordination Presented by: Michelle L. Templin Vice President Legislative Affairs and Business Development MHA ACO Network March 2, 2017 Agenda Agenda Key Regulatory Drivers Accountable
Healthcare Reform and Its Impact on the Care Delivery System
 Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Commercial Risk Adjustment: The most important thing about the ACA that nobody understands
 Commercial Risk Adjustment: The most important thing about the ACA that nobody understands Thursday, October 13, 2016 Noon 1:30 Pacific / 1:00 2:30 Mountain / 2:00 3:30 Central / 3:00-4:30 PM Eastern J.
Commercial Risk Adjustment: The most important thing about the ACA that nobody understands Thursday, October 13, 2016 Noon 1:30 Pacific / 1:00 2:30 Mountain / 2:00 3:30 Central / 3:00-4:30 PM Eastern J.
Final Rule Summary. Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, December 31, 2021
 Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
Transitioning Into a Successful Risk-Based ACO
 Transitioning Into a Successful Risk-Based ACO Part 2: How to prepare for risk June 19, 2018 1pm EST PRESENTERS John Schmitt, Ph.D., FASHCRM Managing Director Reliance Consulting Group Chuck Newton Sr.
Transitioning Into a Successful Risk-Based ACO Part 2: How to prepare for risk June 19, 2018 1pm EST PRESENTERS John Schmitt, Ph.D., FASHCRM Managing Director Reliance Consulting Group Chuck Newton Sr.
Hospital Report Spring 2017
 Hospital Report Spring 2017 360179 BETHESDA NORTH CINCINNATI, OH Beds: 320 Teaching Hospital: Yes Urban or Rural: URBAN Reference: IPPS, Medicare Cost Report - HCRIS Hospital Cost Report Information System
Hospital Report Spring 2017 360179 BETHESDA NORTH CINCINNATI, OH Beds: 320 Teaching Hospital: Yes Urban or Rural: URBAN Reference: IPPS, Medicare Cost Report - HCRIS Hospital Cost Report Information System
Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure
 Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of
Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of
MN DEPARTMENT OF HEALTH PROVIDER PEER GROUPING (PPG) ADVISORY GROUP DEFINING PARAMETERS ANN ROBINOW
 MN DEPARTMENT OF HEALTH PROVIDER PEER GROUPING (PPG) ADVISORY GROUP DEFINING PARAMETERS ANN ROBINOW MEETING 2: JUNE 26, 2009 Introduction Comments and changes to meeting summary? Review of questions or
MN DEPARTMENT OF HEALTH PROVIDER PEER GROUPING (PPG) ADVISORY GROUP DEFINING PARAMETERS ANN ROBINOW MEETING 2: JUNE 26, 2009 Introduction Comments and changes to meeting summary? Review of questions or
The Road to Value. Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017
 The Road to Value Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017 1,500 Physicians UnityPoint Clinic 17 hospitals + 15 rural network hospitals 35,000
The Road to Value Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017 1,500 Physicians UnityPoint Clinic 17 hospitals + 15 rural network hospitals 35,000
5 critical issues for BPCI-A
 REPRINT June 2018 John M. Harris Molly Johnson Amanda Brown healthcare financial management association hfma.org 5 critical issues for BPCI-A Many hospitals and health systems may benefit from participation
REPRINT June 2018 John M. Harris Molly Johnson Amanda Brown healthcare financial management association hfma.org 5 critical issues for BPCI-A Many hospitals and health systems may benefit from participation
The Case For Value ACA to MACRA to MIPS
 The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
Healthcare Finance Trends and Perspectives
 Healthcare Finance Trends and Perspectives AONE Annual Conference, Fort Worth, TX April 2 nd, 2016 Chuck Alsdurf, MAcc, CPA Director, Healthcare Finance Policy, Operational Initiatives Healthcare Financial
Healthcare Finance Trends and Perspectives AONE Annual Conference, Fort Worth, TX April 2 nd, 2016 Chuck Alsdurf, MAcc, CPA Director, Healthcare Finance Policy, Operational Initiatives Healthcare Financial
MEDICARE ADVANTAGE MA Plans. to $28 per month 46% HOW HEALTH SYSTEMS CAN THRIVE WITH. Developing Your Medicare Advantage Strategy PRODUCT
 HOW HEALTH SYSTEMS CAN THRIVE WITH MEDICARE ADVANTAGE The 2019 Medicare Advantage (MA) plan year began on January 1st and once again more Americans enrolled in MA plans than the year before. Fueled by
HOW HEALTH SYSTEMS CAN THRIVE WITH MEDICARE ADVANTAGE The 2019 Medicare Advantage (MA) plan year began on January 1st and once again more Americans enrolled in MA plans than the year before. Fueled by
WYOMING MEDICAID IMPLEMENTATION OF APR DRGS
 CLICK TO EDIT MASTER TITLE STYLE WYOMING MEDICAID IMPLEMENTATION OF APR DRGS ALL PROVIDER MEETING WYOMING DEPARTMENT OF HEALTH JANUARY 25, 2018 1 / 2018 NAVIGANT CONSULTING, INC. ALL RIGHTS RESERVED CLICK
CLICK TO EDIT MASTER TITLE STYLE WYOMING MEDICAID IMPLEMENTATION OF APR DRGS ALL PROVIDER MEETING WYOMING DEPARTMENT OF HEALTH JANUARY 25, 2018 1 / 2018 NAVIGANT CONSULTING, INC. ALL RIGHTS RESERVED CLICK
Bundled Payments for Care Improvement Advanced
 Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Patient Care Models Group Bundled Payments for Care Improvement Advanced Request for Applications (RFA) Last Modified:
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Patient Care Models Group Bundled Payments for Care Improvement Advanced Request for Applications (RFA) Last Modified:
CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives
 CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives Presented by: Peter R. Epp, CPA S e p t e m b e r 2 9, 2 0 1 6 HMA I n t r o d u c t i o n One of the overarching objectives
CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives Presented by: Peter R. Epp, CPA S e p t e m b e r 2 9, 2 0 1 6 HMA I n t r o d u c t i o n One of the overarching objectives
Gainsharing Arrangements and Bundled Payments: OIG Advisory Opinion and Other Developments
 Presenting a live 90 minute webinar with interactive Q&A Gainsharing Arrangements and Bundled Payments: OIG Advisory Opinion and Other Developments Complying With Legal and Regulatory Requirements, Overcoming
Presenting a live 90 minute webinar with interactive Q&A Gainsharing Arrangements and Bundled Payments: OIG Advisory Opinion and Other Developments Complying With Legal and Regulatory Requirements, Overcoming
RISE RAPS / EDS Collaboration: Comments for the Advance Notice February 21, 2017 Webinar Presentation at 10:30 a.m. P.T/ 1:30 p.m. E.
 RISE RAPS / EDS Collaboration: Comments for the Advance Notice February 21, 2017 Webinar Presentation at 10:30 a.m. P.T/ 1:30 p.m. E.T We are the How To people Meet the Panel Christie Teigland, PhD, Avalere
RISE RAPS / EDS Collaboration: Comments for the Advance Notice February 21, 2017 Webinar Presentation at 10:30 a.m. P.T/ 1:30 p.m. E.T We are the How To people Meet the Panel Christie Teigland, PhD, Avalere
Revenue Portfolio Design and Care Transformation: or How I Learned to Love Bundles. TAHFA/HFMA Road show Lubbock, Texas
 Revenue Portfolio Design and Care Transformation: or How I Learned to Love Bundles TAHFA/HFMA Road show Lubbock, Texas February 17, 2017 Its Friday so This will be low stress 2 Goals of Our Session In
Revenue Portfolio Design and Care Transformation: or How I Learned to Love Bundles TAHFA/HFMA Road show Lubbock, Texas February 17, 2017 Its Friday so This will be low stress 2 Goals of Our Session In
21% Total Medicare Beneficiaries (2017): 58 million
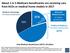 About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
Comprehensive Care for Joint Replacement Payment Model Final Rule Fact Sheet
 Comprehensive Care for Joint Replacement Payment Model Final Rule Fact Sheet 1 Description: This document provides an overview of the final rule to implement a new Comprehensive Care for Joint Replacement
Comprehensive Care for Joint Replacement Payment Model Final Rule Fact Sheet 1 Description: This document provides an overview of the final rule to implement a new Comprehensive Care for Joint Replacement
Total Cost of Care in Oregon s Commercial Market. March 2, 2017
 Total Cost of Care in Oregon s Commercial Market March 2, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary Mission
Total Cost of Care in Oregon s Commercial Market March 2, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary Mission
Delivering Value-Based Care:
 Discussion Summary Delivering Value-Based Care: Episodes of Care Analytics for Health Care Providers, Payers and ACOs July 2015 Interview Featuring: J. Peter Chingos, Senior Industry Consultant, Health
Discussion Summary Delivering Value-Based Care: Episodes of Care Analytics for Health Care Providers, Payers and ACOs July 2015 Interview Featuring: J. Peter Chingos, Senior Industry Consultant, Health
Demystifying Hospital Readmissions Penalties
 Financial Leadership Council Research Note August 1, 2016 Demystifying Hospital Readmissions Penalties Commonly Asked Questions from Hospital CFOs Highlights Readmissions penalties will likely get larger
Financial Leadership Council Research Note August 1, 2016 Demystifying Hospital Readmissions Penalties Commonly Asked Questions from Hospital CFOs Highlights Readmissions penalties will likely get larger
MACRA: APPLICATIONS & IMPLICATIONS September 13, /13/2016. Mark Blessing, CPA, FHFMA Partner
 MACRA: APPLICATIONS & IMPLICATIONS September 13, 2016 Mark Blessing, CPA, FHFMA Partner mblessing@bkd.com Zach Remmich Managing Consultant zremmich@bkd.com 1 TO RECEIVE CPE CREDIT Participate in entire
MACRA: APPLICATIONS & IMPLICATIONS September 13, 2016 Mark Blessing, CPA, FHFMA Partner mblessing@bkd.com Zach Remmich Managing Consultant zremmich@bkd.com 1 TO RECEIVE CPE CREDIT Participate in entire
Medicare Accountable Care Organizations What & Why?
 Medicare Accountable Care Organizations What & Why? Third National Accountable Care Organization Congress David Saÿen, MBA Regional Administrator Centers for Medicare & Medicaid Services San Francisco
Medicare Accountable Care Organizations What & Why? Third National Accountable Care Organization Congress David Saÿen, MBA Regional Administrator Centers for Medicare & Medicaid Services San Francisco
Using Analytics To Transform Your ACO
 Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
PREPARING FOR THE NEXT GENERATION OF MANAGED CARE CONTRACTING
 PREPARING FOR THE NEXT GENERATION OF MANAGED CARE CONTRACTING Nanci Robertson, RN BSN President - Robertson Consulting, Inc. Doral Jacobsen, MBA FACMPE CEO - Prosper Beyond, Inc. DORAL JACOBSEN AND NANCI
PREPARING FOR THE NEXT GENERATION OF MANAGED CARE CONTRACTING Nanci Robertson, RN BSN President - Robertson Consulting, Inc. Doral Jacobsen, MBA FACMPE CEO - Prosper Beyond, Inc. DORAL JACOBSEN AND NANCI
Clinic Comparison Reporting. June 30, 2016
 Clinic Comparison Reporting June 30, 2016 Agenda Introduction and Background Meredith Roberts Tomasi, Q Corp Program Director Measures, Methodology and Reports Doug Rupp, Q Corp Senior Analyst Application
Clinic Comparison Reporting June 30, 2016 Agenda Introduction and Background Meredith Roberts Tomasi, Q Corp Program Director Measures, Methodology and Reports Doug Rupp, Q Corp Senior Analyst Application
Critical Issues in Performance Evaluation for Medicaid ACOs
 Critical Issues in Performance Evaluation for Medicaid ACOs Derek DeLia, Ph.D. Associate Research Professor Center for State Health Policy Seventh National Medicaid Congress Arlington, VA Wednesday May
Critical Issues in Performance Evaluation for Medicaid ACOs Derek DeLia, Ph.D. Associate Research Professor Center for State Health Policy Seventh National Medicaid Congress Arlington, VA Wednesday May
Point of View: Medicare Profitability in a Reform Market
 Point of View: Profitability in a Reform Market Bill Eggbeer, Managing Director, & Krista Bowers, Director, BDC Advisors, LLC Introduction Overall, accounts for approximately 20% of the total domestic
Point of View: Profitability in a Reform Market Bill Eggbeer, Managing Director, & Krista Bowers, Director, BDC Advisors, LLC Introduction Overall, accounts for approximately 20% of the total domestic
Advanced Analytics. The key to unlocking the Triple Aim and Value-Based Purchasing. Ines Vigil MD, MPH, MBA
 Advanced Analytics The key to unlocking the Triple Aim and Value-Based Purchasing Ines Vigil MD, MPH, MBA Advanced Analytics: The key to unlocking the Triple Aim and Value-Based Purchasing Current State
Advanced Analytics The key to unlocking the Triple Aim and Value-Based Purchasing Ines Vigil MD, MPH, MBA Advanced Analytics: The key to unlocking the Triple Aim and Value-Based Purchasing Current State
A.J. Yates, Jr., MD Chief of Orthopaedic Surgery UPMC Shadyside Associate Professor Vice Chairman for Quality Management UPMC Department of
 Creation of Value The CJR: Bundled Care in Arthroplasty A.J. Yates, Jr., MD Chief of Orthopaedic Surgery UPMC Shadyside Associate Professor Vice Chairman for Quality Management UPMC Department of Orthopaedic
Creation of Value The CJR: Bundled Care in Arthroplasty A.J. Yates, Jr., MD Chief of Orthopaedic Surgery UPMC Shadyside Associate Professor Vice Chairman for Quality Management UPMC Department of Orthopaedic
Performance Measurement Work Group Meeting 01/17/2018
 Performance Measurement Work Group Meeting 01/17/2018 Agenda RY 2020 MHAC DRAFT FINAL Policy Modeling Additional Stakeholder feedback? RY 2020 RRIP Improvement Target National Forecasting (data delays);
Performance Measurement Work Group Meeting 01/17/2018 Agenda RY 2020 MHAC DRAFT FINAL Policy Modeling Additional Stakeholder feedback? RY 2020 RRIP Improvement Target National Forecasting (data delays);
CMS Cardiac (AMI & CABG), SHFFT and Cardiac Rehab. Demo - Overview. September 13, 2016
 CMS Cardiac (AMI & CABG), SHFFT and Cardiac Rehab. Demo - Overview September 13, 2016 Cardiac (AMI & CABG), SHFFT (Surgical Hip/Femur Fracture Treatment) & Cardiac Rehabilitation Demo Why expand Comprehensive
CMS Cardiac (AMI & CABG), SHFFT and Cardiac Rehab. Demo - Overview September 13, 2016 Cardiac (AMI & CABG), SHFFT (Surgical Hip/Femur Fracture Treatment) & Cardiac Rehabilitation Demo Why expand Comprehensive
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making. Introduction. William Bednar, FSA, FCA, MAAA
 Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD. AccountableCareInstitute.com
 10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD FQHCs Bridge the Gap in Care Bridge Built and Maintained by FFS Dollars 2 CMMI View of FFS Medicine 3 Accountability High
10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD FQHCs Bridge the Gap in Care Bridge Built and Maintained by FFS Dollars 2 CMMI View of FFS Medicine 3 Accountability High
Bundled Payments for Care Improvement: ADLS # 5 Contractual and Governance Issues Among Providers in Bundled Payments
 Bundled Payments for Care Improvement: ADLS # 5 Contractual and Governance Issues Among Providers in Bundled Payments Copyright 2012 American Institutes for Research All rights reserved. Weslie Kary, Moderator
Bundled Payments for Care Improvement: ADLS # 5 Contractual and Governance Issues Among Providers in Bundled Payments Copyright 2012 American Institutes for Research All rights reserved. Weslie Kary, Moderator
For the RRU Index Ratio, an EXC is displayed if the denominator is <200 for the condition or if the calculated indexed ratio is <0.33 or >3.00.
 General Questions What changes were made for HEDIS 2016? RRU specification changes: - We removed the Use of Appropriate Medications for People With Asthma (ASM) measure from the Relative Resource Use for
General Questions What changes were made for HEDIS 2016? RRU specification changes: - We removed the Use of Appropriate Medications for People With Asthma (ASM) measure from the Relative Resource Use for
BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities
 BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities A Presentation for the ACC April 3, 2018 Christopher J. Donovan Partner Foley & Lardner LLP C. Frederick (Fred) Geilfuss
BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities A Presentation for the ACC April 3, 2018 Christopher J. Donovan Partner Foley & Lardner LLP C. Frederick (Fred) Geilfuss
2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet
 2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
PRINCIPAL ACCOUNTABLE PROVIDER MANUAL
 Health Care Payment Improvement Building a healthier future for all Arkansans Arkansas Payment Improvement Initiative Episodes of Care PRINCIPAL ACCOUNTABLE PROVIDER MANUAL Program Overview MPI 6037 1/17
Health Care Payment Improvement Building a healthier future for all Arkansans Arkansas Payment Improvement Initiative Episodes of Care PRINCIPAL ACCOUNTABLE PROVIDER MANUAL Program Overview MPI 6037 1/17
Merit-Based Incentive Payment System (MIPS): Elective Outpatient Percutaneous Coronary Intervention (PCI) Measure
 Merit-Based Incentive Payment System (MIPS): Elective Outpatient Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
Merit-Based Incentive Payment System (MIPS): Elective Outpatient Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
Health Data for Action Leveraging Health Data for Actionable Insights. Applicant Informational Webinar May 2, 2017
 1 Health Data for Action Leveraging Health Data for Actionable Insights Applicant Informational Webinar May 2, 2017 Speakers 2 Megan Collado, M.P.H. Director AcademyHealth Amanda Frost, M.A., Ph.D. Senior
1 Health Data for Action Leveraging Health Data for Actionable Insights Applicant Informational Webinar May 2, 2017 Speakers 2 Megan Collado, M.P.H. Director AcademyHealth Amanda Frost, M.A., Ph.D. Senior
Affordable Care Act Part 1: Impact on Counties as Employers
 Affordable Care Act Part 1: Impact on Counties as Employers November 22, 2013 1 Webinar Recording and Evaluation Survey This webinar is being recorded and will be made available online to view later Recording
Affordable Care Act Part 1: Impact on Counties as Employers November 22, 2013 1 Webinar Recording and Evaluation Survey This webinar is being recorded and will be made available online to view later Recording
2018 Merit-Based Incentive Payment System (MIPS) Scoring Overview
 The Physicians Advocacy Institute s Medicare Quality Payment Program (QPP) Physician Education Initiative 2018 Merit-Based Incentive Payment System (MIPS) Scoring Overview 1 P a g e MEDICARE QPP PHYSICIAN
The Physicians Advocacy Institute s Medicare Quality Payment Program (QPP) Physician Education Initiative 2018 Merit-Based Incentive Payment System (MIPS) Scoring Overview 1 P a g e MEDICARE QPP PHYSICIAN
The Transition to Value-Based Health Care: Recommendations for Medical Device Manufacturers
 The Transition to Value-Based Health Care: Recommendations for Medical Device Manufacturers April 27, 2017 LLP Agenda Introduction Shift to Value-Based Care New Models of Medical Device Company Operation
The Transition to Value-Based Health Care: Recommendations for Medical Device Manufacturers April 27, 2017 LLP Agenda Introduction Shift to Value-Based Care New Models of Medical Device Company Operation
Insights on Rural Health Insurance Market Challenges from the NACRHHS. Housekeeping. Q & A to follow Submit questions using Q&A area
 ruralhealthinfo.org Insights on Rural Health Insurance Market Challenges from the NACRHHS Housekeeping Q & A to follow Submit questions using Q&A area Slides are available at https://www.ruralhealthinfo.org/webinars/nacrhhsinsurance-market-challenges
ruralhealthinfo.org Insights on Rural Health Insurance Market Challenges from the NACRHHS Housekeeping Q & A to follow Submit questions using Q&A area Slides are available at https://www.ruralhealthinfo.org/webinars/nacrhhsinsurance-market-challenges
Evidence-Based Program Reimbursement Strategies. Timothy P. McNeill, RN, MPH
 Evidence-Based Program Reimbursement Strategies Timothy P. McNeill, RN, MPH 1 Medicare & Value Based Purchasing 2 Medicare Advantage Changes 3 DSMT Requirements 4 CDSME Tip Sheet Opportunities for EB Programs
Evidence-Based Program Reimbursement Strategies Timothy P. McNeill, RN, MPH 1 Medicare & Value Based Purchasing 2 Medicare Advantage Changes 3 DSMT Requirements 4 CDSME Tip Sheet Opportunities for EB Programs
Predictive Analytics in the People s Republic of China
 Predictive Analytics in the People s Republic of China Rong Yi, PhD Senior Consultant Rong.Yi@milliman.com Tel: 781.213.6200 4 th National Predictive Modeling Summit Arlington, VA September 15-16, 2010
Predictive Analytics in the People s Republic of China Rong Yi, PhD Senior Consultant Rong.Yi@milliman.com Tel: 781.213.6200 4 th National Predictive Modeling Summit Arlington, VA September 15-16, 2010
Merit-Based Incentive Payment System (MIPS): Knee Arthroplasty Measure. Measure Information Form 2019 Performance Period
 Merit-Based Incentive Payment System (MIPS): Knee Arthroplasty Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction... 3 1.1 Measure Name... 3 1.2 Measure Description...
Merit-Based Incentive Payment System (MIPS): Knee Arthroplasty Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction... 3 1.1 Measure Name... 3 1.2 Measure Description...
Volume to Value The Great Transformation of American Medicine
 Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
MACRAnomics. Patient-Level Economics and Strategic Implications for Providers. Presented to: NW Ohio HFMA October 20, 2016
 MACRAnomics Patient-Level Economics and Strategic Implications for Providers Presented to: NW Ohio HFMA October 20, 2016 Property of HealthScape Advisors Strictly Confidential 2 MACRAnomics: Objectives
MACRAnomics Patient-Level Economics and Strategic Implications for Providers Presented to: NW Ohio HFMA October 20, 2016 Property of HealthScape Advisors Strictly Confidential 2 MACRAnomics: Objectives
Total Cost of Care in Oregon s Commercial Market. February 24, 2017
 Total Cost of Care in Oregon s Commercial Market February 24, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary
Total Cost of Care in Oregon s Commercial Market February 24, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary
Eight Indispensable Financial Considerations of Shifting from Volume to Value Reimbursement
 Eight Indispensable Financial Considerations of Shifting from Volume to Value Reimbursement September 25-26, 2017 Max Reiboldt, CPA President CEO Learning Objectives This session will provide you with
Eight Indispensable Financial Considerations of Shifting from Volume to Value Reimbursement September 25-26, 2017 Max Reiboldt, CPA President CEO Learning Objectives This session will provide you with
Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers
 Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers Montana Chamber of Commerce Healthcare Forum November 29-30, 2016 Shane Wolverton SVP CORPORATE DEVELOPMENT, QUANTROS
Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers Montana Chamber of Commerce Healthcare Forum November 29-30, 2016 Shane Wolverton SVP CORPORATE DEVELOPMENT, QUANTROS
RRU Frequently Asked Questions
 RRU Frequently Asked Questions General Questions What changes were made for HEDIS 2015? RRU specification changes: We removed the Cholesterol Management for Patients With Cardiovascular Conditions (CMC)
RRU Frequently Asked Questions General Questions What changes were made for HEDIS 2015? RRU specification changes: We removed the Cholesterol Management for Patients With Cardiovascular Conditions (CMC)
QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NOVEMBER 15, 2018
 QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NOVEMBER 15, 2018 Disclaimers This presentation was prepared as a tool to assist providers and is not intended to grant rights or impose obligations.
QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NOVEMBER 15, 2018 Disclaimers This presentation was prepared as a tool to assist providers and is not intended to grant rights or impose obligations.
Welcome to our webinar!
 Welcome to our webinar! Here are some directions for you When you first join a session, the Control Panel appears on the right side of your screen. Use the Control Panel to manage your session. To free
Welcome to our webinar! Here are some directions for you When you first join a session, the Control Panel appears on the right side of your screen. Use the Control Panel to manage your session. To free
SUMMARY TABLE OF CONTENTS
 FINAL RULE: MEDICARE PROGRAM; ADVANCING CARE COORDINATION THROUGH EPISODE PAYMENT MODELS (EPMs); CARDIAC REHABILITATION INCENTIVE PAYMENT MODEL; AND CHANGES TO THE COMPREHENSIVE CARE FOR JOINT REPLACEMENT
FINAL RULE: MEDICARE PROGRAM; ADVANCING CARE COORDINATION THROUGH EPISODE PAYMENT MODELS (EPMs); CARDIAC REHABILITATION INCENTIVE PAYMENT MODEL; AND CHANGES TO THE COMPREHENSIVE CARE FOR JOINT REPLACEMENT
Proposed ACO Rule: How Will It Affect Academic Medical Centers?
 Proposed ACO Rule: How Will It Affect Academic Medical Centers? This roundtable discussion is brought to you by the Teaching Hospitals and Academic Medical Centers Practice Group Wednesday, May 25, 2011
Proposed ACO Rule: How Will It Affect Academic Medical Centers? This roundtable discussion is brought to you by the Teaching Hospitals and Academic Medical Centers Practice Group Wednesday, May 25, 2011
Payment Reform in Support of Population Health Management
 Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
2016 ICR Changes and Filing Procedures. Form CMS Transmittals #7 and #8. Demonstration of Software Enhancements
 2016 ICR Changes and Filing Procedures Form CMS-2552-10 Transmittals #7 and #8 Demonstration of Software Enhancements NYSICR Road Shows April 11-15, 2016 Joe Sellars, Director, KPMG LLP, Jacksonville,
2016 ICR Changes and Filing Procedures Form CMS-2552-10 Transmittals #7 and #8 Demonstration of Software Enhancements NYSICR Road Shows April 11-15, 2016 Joe Sellars, Director, KPMG LLP, Jacksonville,
JOINT TASK FORCE ON HEALTH CARE COST REVIEW (Senate Bill 419)
 May 11 th, 2018 JOINT TASK FORCE ON HEALTH CARE COST REVIEW (Senate Bill 419) 1 AGENDA 8:30-8:35 AM Welcome and Opening Remarks 8:35-9:30 AM Multi-stakeholder Approaches to Address Total Cost of Care 9:35-9:50
May 11 th, 2018 JOINT TASK FORCE ON HEALTH CARE COST REVIEW (Senate Bill 419) 1 AGENDA 8:30-8:35 AM Welcome and Opening Remarks 8:35-9:30 AM Multi-stakeholder Approaches to Address Total Cost of Care 9:35-9:50
Pricing Transparency: Focus on the Chargemaster
 Pricing Transparency: Focus on the Chargemaster Presented by Sandy Sage RN, HomeTown Health, LLC August 10, 2017 A PORTION OF THESE MATERIALS WERE PRODUCED PURSUANT TO THE Iowa Small Hospital Improvement
Pricing Transparency: Focus on the Chargemaster Presented by Sandy Sage RN, HomeTown Health, LLC August 10, 2017 A PORTION OF THESE MATERIALS WERE PRODUCED PURSUANT TO THE Iowa Small Hospital Improvement
Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]
![Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701] Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]](/thumbs/87/96500790.jpg) Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
Measure Information Form Collected For: CMS Efficiency Measures (Claims Based) Performance Measure Name: Medicare Spending Per Beneficiary (MSPB)
 Last Updated: New Measure: Version 4.4 Measure Information Form Collected For: CMS Efficiency Measures (Claims Based) Measure Set: CMS Payment Measures Set Measure ID#: MSPB-1 Performance Measure Name:
Last Updated: New Measure: Version 4.4 Measure Information Form Collected For: CMS Efficiency Measures (Claims Based) Measure Set: CMS Payment Measures Set Measure ID#: MSPB-1 Performance Measure Name:
PRINCIPAL ACCOUNTABLE PROVIDER MANUAL
 Health Care Payment Improvement Building a healthier future for all Arkansans Arkansas Payment Improvement Initiative Episodes of Care PRINCIPAL ACCOUNTABLE PROVIDER MANUAL Program Overview MPI 6037 1/17
Health Care Payment Improvement Building a healthier future for all Arkansans Arkansas Payment Improvement Initiative Episodes of Care PRINCIPAL ACCOUNTABLE PROVIDER MANUAL Program Overview MPI 6037 1/17
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business?
 Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet
 2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
Alternative Payment Models in the Quality Payment Program as of November 2018
 Alternative Payment s in the Payment Program as of November 2018 The table below displays the Alternative Payment s (s) that CMS currently operates or has announced, as of November 2018. In the table,
Alternative Payment s in the Payment Program as of November 2018 The table below displays the Alternative Payment s (s) that CMS currently operates or has announced, as of November 2018. In the table,
Clinical Episode Contracting for Commercial Payers January 2019
 Clinical Episode Contracting for Commercial Payers January 2019 1 About This Resource Background Bundled payments for care delivery have received significant attention within the Medicare payment program
Clinical Episode Contracting for Commercial Payers January 2019 1 About This Resource Background Bundled payments for care delivery have received significant attention within the Medicare payment program
Risk Adjustment Best Practices
 Sponsored By: Risk Adjustment Best Practices Tuesday March 14, 2017 (12:00 1:00 pm Pacific / 1:00 2:00 pm Mountain / 2:00 3:00 p.m. Central / 3:00 4:00 pm Eastern) Colleen Farrell, Managing Director Dr.
Sponsored By: Risk Adjustment Best Practices Tuesday March 14, 2017 (12:00 1:00 pm Pacific / 1:00 2:00 pm Mountain / 2:00 3:00 p.m. Central / 3:00 4:00 pm Eastern) Colleen Farrell, Managing Director Dr.
Calculating Savings in the New Jersey Medicaid Accountable Care Organization Demonstration Program
 Calculating Savings in the New Jersey Medicaid Accountable Care Organization Demonstration Program Affiliated Accountable Care Organizations Webinar September 10, 2013 Center for State Health Policy Joel
Calculating Savings in the New Jersey Medicaid Accountable Care Organization Demonstration Program Affiliated Accountable Care Organizations Webinar September 10, 2013 Center for State Health Policy Joel
Merit-Based Incentive Payment System (MIPS): Routine Cataract Removal with Intraocular Lens (IOL) Implantation Measure
 Merit-Based Incentive Payment System (MIPS): Routine Cataract Removal with Intraocular Lens (IOL) Implantation Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
Merit-Based Incentive Payment System (MIPS): Routine Cataract Removal with Intraocular Lens (IOL) Implantation Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
Sent via electronic transmission to:
 March 3, 2017 Patrick Conway, MD Acting Administrator Centers for Medicare and Medicaid Services US Department of Health and Human Services 200 Independence Avenue, SW Washington, DC 20201 Sent via electronic
March 3, 2017 Patrick Conway, MD Acting Administrator Centers for Medicare and Medicaid Services US Department of Health and Human Services 200 Independence Avenue, SW Washington, DC 20201 Sent via electronic
The Fundamentals of Medicare. Jim Hahn, CRS National Health Policy Forum February 11, 2011
 The Fundamentals of Medicare Jim Hahn, CRS National Health Policy Forum February 11, 2011 Medicare is health insurance for people age 65 or older, under age 65 with certain disabilities, and any age with
The Fundamentals of Medicare Jim Hahn, CRS National Health Policy Forum February 11, 2011 Medicare is health insurance for people age 65 or older, under age 65 with certain disabilities, and any age with
DEADLINE WHERE TO SEND APPLICATIONS. Mail eight (8) copies of each completed application to the following address:
 Centers for Medicare & Medicaid Services Center for Medicare Management 7500 Security Boulevard Baltimore, Maryland 21244-1850 Application for New Medical Services and Technologies Seeking to Qualify for
Centers for Medicare & Medicaid Services Center for Medicare Management 7500 Security Boulevard Baltimore, Maryland 21244-1850 Application for New Medical Services and Technologies Seeking to Qualify for
MACRA: New Medicare Reimbursement Models Sharp HealthCare
 MACRA: New Medicare Reimbursement Models Sharp HealthCare August 15, 2016 Nathan M. Bays, Esq. General Counsel, The Health Management Academy Executive Director, Advisors Caitlin Greenbaum, MPH Director,
MACRA: New Medicare Reimbursement Models Sharp HealthCare August 15, 2016 Nathan M. Bays, Esq. General Counsel, The Health Management Academy Executive Director, Advisors Caitlin Greenbaum, MPH Director,
Medicare payment policy and its impact on program spending
 Medicare payment policy and its impact on program spending James E. Mathews, Ph.D. Deputy Director, Medicare Payment Advisory Commission February 8, 2013 Outline of today s presentation Brief background
Medicare payment policy and its impact on program spending James E. Mathews, Ph.D. Deputy Director, Medicare Payment Advisory Commission February 8, 2013 Outline of today s presentation Brief background
FORM CMS This page is reserved for future use Rev. 8
 11-16 FORM CMS-2552-10 4064.1 4064. WORKSHEET L - CALCULATION OF CAPITAL PAYMENT Worksheet L, Parts I through III, calculate program settlement for PPS inpatient hospital capitalrelated costs in accordance
11-16 FORM CMS-2552-10 4064.1 4064. WORKSHEET L - CALCULATION OF CAPITAL PAYMENT Worksheet L, Parts I through III, calculate program settlement for PPS inpatient hospital capitalrelated costs in accordance
Strategic Purchasing of Medical Devices
 Strategic Purchasing of Medical Devices James C. Robinson Leonard D. Schaeffer Professor of Health Economics Director, Berkeley Center for Health Technology University of California, Berkeley Overview
Strategic Purchasing of Medical Devices James C. Robinson Leonard D. Schaeffer Professor of Health Economics Director, Berkeley Center for Health Technology University of California, Berkeley Overview
REDUCING THE RISK OF RISK-BASED CONTRACTS
 REDUCING THE RISK OF RISK-BASED CONTRACTS Payers are promoting risk-based contracting as a solution for escalating health care costs. The question health care organizations must ask is, How much risk can
REDUCING THE RISK OF RISK-BASED CONTRACTS Payers are promoting risk-based contracting as a solution for escalating health care costs. The question health care organizations must ask is, How much risk can
HERE WE GO AGAIN: THE LATEST ON ICD-10 AND MEDICARE AUDITS
 HERE WE GO AGAIN: THE LATEST ON ICD-10 AND MEDICARE AUDITS TODAY S OBJECTIVES International Classification of Diseases (ICD )-10: Delay to 2015? Medicare Cost Report : Desk Review and Audit Findings 2
HERE WE GO AGAIN: THE LATEST ON ICD-10 AND MEDICARE AUDITS TODAY S OBJECTIVES International Classification of Diseases (ICD )-10: Delay to 2015? Medicare Cost Report : Desk Review and Audit Findings 2
March 1, Dear Mr. Kouzoukas:
 March 1, 2019 Mr. Demetrios L. Kouzoukas Principal Deputy Administrator and Director Center for Medicare Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: Advance
March 1, 2019 Mr. Demetrios L. Kouzoukas Principal Deputy Administrator and Director Center for Medicare Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: Advance
Provider Payment. Jones & Bartlett Learning, LLC NOT FOR SALE OR DISTRIBUTION
 & CHAPTER 5 Provider Payment CHAPTER STUDY REVIEW Bartlett Learning, 1. It s Not LLC Reimbursement. It s Payment. Reimbursement: - It s what you get when you submit your travel expenses to your employer
& CHAPTER 5 Provider Payment CHAPTER STUDY REVIEW Bartlett Learning, 1. It s Not LLC Reimbursement. It s Payment. Reimbursement: - It s what you get when you submit your travel expenses to your employer
Medicare Quality Payment Program Overview (MACRA)
 Medicare Quality Payment Program Overview (MACRA) December 2016 Rev. 12/1/16 Some general observations MACRA is complex More than a replacement for the SGR Many of the new requirements are revisions to
Medicare Quality Payment Program Overview (MACRA) December 2016 Rev. 12/1/16 Some general observations MACRA is complex More than a replacement for the SGR Many of the new requirements are revisions to
