kaiser medicaid and the uninsured commission on A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey EXECUTIVE SUMMARY
|
|
|
- Andrea Miller
- 5 years ago
- Views:
Transcription
1 kaiser commission on medicaid and the uninsured A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey EXECUTIVE SUMMARY Prepared by Kathleen Gifford, Vernon K. Smith, and Dyke Snipes Health Management Associates and Julia Paradise Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation September G S T R E E T NW, W A S H I N G T O N, DC P H O N E: (202) , F A X: ( 202) W E B S I T E: W W W. K F F. O R G/ K C M U
2 kaiser commission medicaid uninsured and the The Kaiser Commission on Medicaid and the Uninsured provides information and analysis on health care coverage and access for the low-income population, with a special focus on Medicaid s role and coverage of the uninsured. Begun in 1991 and based in the Kaiser Family Foundation s Washington, DC office, the Commission is the largest operating program of the Foundation. The Commission s work is conducted by Foundation staff under the guidance of a bipartisan group of national leaders and experts in health care and public policy. James R. Tallon Chairman Diane Rowland, Sc.D. Executive Director
3 EXECUTIVE SUMMARY Medicaid, the public insurance program for low-income Americans, is the single largest health care program in the United States. In calendar year 2011, average monthly Medicaid enrollment is projected to exceed 55 million, and a projected 70 million people, or roughly one in five Americans, will be covered by the program for one or more months during the year. Beginning in 2014, the Patient Protection and Affordable Care Act (ACA) will expand Medicaid eligibility to cover nearly all non-elderly Americans with incomes below 133 percent of the federal poverty level ($14,404 for an individual), providing coverage to 16 million additional people mostly, uninsured adults by A growing phenomenon since the early 1980 s has been states use of various models of managed care to deliver and finance care for Medicaid enrollees, with the goals of increasing access to care, improving quality, and, in some cases, reducing costs. Whereas in the traditional fee-for-service system, Medicaid beneficiaries must find providers willing to accept new (or any) Medicaid patients, states with managed care purchase or establish a network of providers for their Medicaid enrollees through contracts with health plans and/or providers who agree to accept Medicaid patients and to meet certain requirements to ensure timely access to care. These contracts give states a mechanism for holding plans or providers accountable for Medicaid enrollees overall experience with the health care system, through performance standards related to access to care, quality of care, data reporting, and other patient care goals. Comprehensive Medicaid Managed Care Penetration by State, October 2010 AK CA NOTE: Includes enrollment in MCOs and PCCMs. Most data as of October SOURCE: KCMU/HMA Survey of Medicaid Managed Care, September At the same time, managed care can fail as a strategy for improving patient care if capitation payment rates are not adequate or they overpay, transitions from fee-for-service are not well-conceived, provider networks are not sufficient to meet the care needs of the enrolled population, or state oversight of managed care programs is lacking. The history of Medicaid managed care provides evidence of the promise of managed care, but also shows that the details of how it is structured and implemented are consequential for Medicaid beneficiaries. The share of Medicaid beneficiaries enrolled in some form of managed care has increased every year except one for over two decades, reaching 71.7 percent as of June 30, 2009 according to CMS. This trend has heightened both policy interest and needs for information about Medicaid managed care, and three dynamics are focusing even more attention on how Medicaid managed care is developing. First, many state policymakers are eyeing managed care as a Medicaid cost containment tool and a means to address concerns about access and quality, particularly as states are facing severe budget pressures from the recession and the slow recovery. Second, many states are expanding managed care to more medically complex and fragile populations, for whom the stakes may be greatest. Third, states are WA OR NV ID AZ UT HI MT WY CO NM U.S. Overall = 65.9% ND SD NE KS TX OK MN IA MO AR LA WI IL MS IN MI TN AL KY OH WV GA 0% - 50% (9 states) SC PA VT VA NC FL NY 51% - 65% (15 states) 66% - 80% (17 states and DC) 80%+ (9 states) ME NH MA CT RI NJ DE MD DC 1
4 expected to rely heavily on managed care to serve the millions of adults who will become newly eligible for Medicaid in In light of the large and growing role of managed care in Medicaid, and the implications for Medicaid beneficiaries, the Kaiser Commission on Medicaid and the Uninsured (KCMU) and Health Management Associates (HMA) conducted a special survey of Medicaid programs to assess the state of Medicaid managed care, identify current issues, and gain perspectives on the directions Medicaid managed care may take in the coming years. This report presents data and findings based on that survey. Key Findings Nearly all states operate comprehensive Medicaid managed care programs. Across all 50 states and DC, only three states (Alaska, New Hampshire and Wyoming) reported that they did not have any Medicaid managed care as of October Of the 48 states with comprehensive managed care programs, 36 reported contracting with risk-based managed care organizations (MCOs) and 31 reported operating a primary care case management (PCCM) program. Nearly two-thirds of all Medicaid beneficiaries are enrolled in comprehensive managed care arrangements. Over 26 million Medicaid beneficiaries are enrolled in MCOs and 8.8 million are enrolled in PCCM programs. Together these beneficiaries in comprehensive managed care represent 65.9 percent of all Medicaid beneficiaries. However, managed care penetration varies considerably from state to state in nine states (including three with no managed care), the rate is 50 percent or less, while in another nine states, at least 80 percent of Medicaid beneficiaries are enrolled in these programs. Half the states with MCOs and/or PCCM programs also contract with non-comprehensive prepaid health plans (PHP) to provide specific categories of services. The types of services most commonly provided by non-comprehensive PHPs, which are risk-based, limited-benefit plans, are inpatient and outpatient behavioral health services and substance abuse treatment. A number of states also contract with non-comprehensive PHPs to provide dental care, non-emergency transportation, or prescription drugs all services that are frequently carved out of MCO contracts. States are increasingly mandating managed care for previously exempt or excluded Medicaid beneficiaries. States have long mandated that most children, pregnant women, and parents and other caretaker adults in Medicaid enroll in managed care. A majority of states reported that, for at least one Medicaid managed care program and/or geographic area, they also mandate enrollment in managed care for children with disabilities receiving Supplemental Security Income (SSI), children with special health care needs, and seniors and people with disabilities who are not dually eligible for Medicare and Medicaid. Risk-based comprehensive managed care Almost two-thirds of Medicaid MCO enrollees are in health plans that primarily or exclusively serve Medicaid. In addition, for-profit plans account for a little over half of all Medicaid MCO enrollment. Roughly 60 percent of Medicaid MCO enrollees are in non-publicly traded plans. Medicaid MCO enrollment is distributed about evenly between local and national plans. Auto-assignment rates appear to vary widely. Auto-assignment rates may provide a useful signal of how well Medicaid beneficiaries understand the managed care system and their choices within it. Across the 26 states that reported auto-assignment rates, half (13 states) reported rates of 20 percent or less; 2
5 four states reported rates higher than 50 percent. More than two-thirds of states with MCOs use thirdparty enrollment brokers to provide plan information to beneficiaries and assist them in choosing an MCO; a small number of vendors dominate the market. Most states allow MCOs to conduct outreach and marketing to Medicaid beneficiaries within federal rules. Most states set MCO capitation rates administratively and risk-adjust their rates. Three-quarters of the states with MCOs reported that they used administrative rate-setting with actuaries to establish MCO rates. Other approaches states reported using are negotiation and competitive bidding, and some states combine multiple methods. Most states adjust their capitation rates for age and eligibility category, and about two-thirds adjust for health status. Risk-sharing arrangements with MCOs, such as stop-loss/reinsurance or risk corridors, are in place in half the states. Over half the states with MCOs include a pay-for-performance (P4P) component in their payment to plans. Capitation withholds and bonus payments were reported most frequently. Examples of other approaches are shared savings, auto-assignment preference, and enhanced capitation. A limited number of states have a minimum medical loss ratio (MLR) requirement for MCOs participating in Medicaid. Eleven states indicated that they have a minimum MLR requirement for plans, 21 states reported that they do not, and three states said they plan to establish one in the future. Minimum MLRs ranged from 80 percent in three states to 93 percent in one state for MCOs serving aged and disabled Medicaid beneficiaries. Three states plan to establish a minimum MLR requirement. All states but one carve out at least one acute-care benefit from their MCO contracts, but several states are carving some benefits back in. More often than not, dental care and outpatient and inpatient behavioral health care are carved out and provided either on a fee-for-service basis or by a noncomprehensive prepaid health plan (PHP) a risk-based, limited-benefit plan. Other common carve-outs are outpatient substance abuse treatment, non-emergency transportation, and pharmacy services. Some states that previously carved out the pharmacy benefit or other Medicaid services are carving them back into their MCO contracts or plan to do so. States use a variety of network adequacy standards. States typically use provider-to-population ratios and distance and travel-time maximums as standards to ensure that MCO networks are adequate. They generally apply different standards for primary and specialty care and frequently apply different standards for rural and urban areas. The standards states use vary widely. In most states, in addition to primary care physicians, providers such as ObGyns, nurse practitioners, federally qualified health centers, and physician groups/clinics are recognized as primary care providers (PCP) for MCO enrollees. Many but not all states report that Medicaid MCO enrollees sometimes face access problems. Over two-thirds of responding states with MCOs reported that Medicaid beneficiaries enrolled in MCOs sometimes experience access problems. Problems with access to dental care, pediatric specialists, psychiatrists and other behavioral health providers, and other specialists (e.g., dermatologists, ear-nosethroat doctors, orthopedists and other surgeons, neurologists, cancer and diabetes specialists) were all cited. At the same time, improved access to care both primary and specialty care was the most frequently cited perceived benefit of managed care relative to fee-for-service. Some states indicated that where an access problem existed, it usually paralleled a similar problem encountered by persons with other types of insurance, for example, due to provider shortages and other market factors. The survey, however, did not directly collect information on access problems in fee-for-service Medicaid. 3
6 Primary care case management (PCCM) programs Nearly as many states have a PCCM program as have contracts with MCOs. Thirty-one states operate PCCM programs, in which PCPs, by contract with the state, agree to provide, manage, and monitor the primary care of Medicaid beneficiaries who select them, or, in some cases, are assigned to them. In addition to serving as a medical home for primary and preventive care, PCPs are contractually responsible for authorizing referrals when specialty care is needed. Most states pay PCPs a small monthly fee for case management in addition to regular fee-for-service payments. A quarter of states include a pay-for-performance element in their payments to PCPs. Many states contract for PCCM administrative services. Over half the states with PCCM programs reported that they have PCCM administrative services contracts and, in a few cases, the administrative fees are at risk. The services provided under these contracts range from case or care management to enrollment broker services to claims administration. Nine states operate Enhanced PCCM (EPCCM) programs. These programs incorporate strengthened quality assurance and care management and coordination. Enhancements include disease management services, coordination/integration of physical and mental health care, case management for highcost/high-risk enrollees, and linkages between primary care and community-based services for targeted groups. Non-comprehensive managed care Half the states contract with non-comprehensive PHPs, separate from their MCO and PCCM programs, to provide some services. The services most commonly provided by these PHPs are inpatient and outpatient behavioral health care and substance abuse treatment, followed by dental care, nonemergency transportation, and prescription drugs all services that are frequently carved out of MCO contracts. Nearly all Medicaid beneficiaries receiving behavioral health care through a PHP were in plans that specialize in Medicaid. Not-for-profit, non-publicly traded, and local plans were strongly dominant. By comparison, Medicaid beneficiaries receiving dental care through a PHP were more likely to be in plans with mixed enrollment, for-profit plans, and plans affiliated with a national company. Measuring, monitoring, and improving quality in Medicaid managed care Sixteen of the 36 states with MCOs require plans to be accredited. All states with MCOs but one, and most states with PCCM programs, require HEDIS and CAHPS data or state-specific measures of performance and patient satisfaction. Required measures focus heavily on Medicaid priority areas such as prenatal and post-partum care, child health preventive care, management of chronic diseases, and access to care. A quarter of the states with MCOs and/or PCCM programs also assess quality in their feefor-service delivery system. Three-fourths of states with MCOs publish reports on MCO quality, and half the states with PCCM programs publish quality reports on their PCCM programs. A smaller number of states also publicly report on PHPs performance, allowing a look at quality across all their managed care arrangements, and a few extend quality reporting to the non-managed fee-for-service component of their program. Fifteen states with MCOs and one PCCM-only state reported that they prepare a quality report card using 4
7 HEDIS, CAHPS, and state-specific measures, which Medicaid beneficiaries can use to compare and choose health plans. Two states publicly reported on quality performance for the first time in FY Quality improvement activities in the states with MCOs reveal a breadth of state priorities. MCOs must conduct performance improvement projects, and all states must contract with External Quality Review Organizations (EQRO) to provide an independent assessment of the quality of care provided by Medicaid MCOs. States reported wide-ranging quality improvement activities, including, for example, projects focused on improving birth outcomes, increasing access to pediatric subspecialists, identifying high-risk individuals for case management, and increasing coordination between behavioral health and medical providers. Four PCCM-only states reported contracting with EQROs. Special initiatives to improve quality and care coordination All but a small number of states have undertaken initiatives to reduce inappropriate use of ERs; many report initiatives to reduce obesity. States often include a focus on ER utilization in their Medicaid contracts with MCOs, and ER use is a factor in some pay-for-performance systems. MCOs may use data on ER use to target high-users for case management or care coordination, and to profile providers and work with medical directors to improve their utilization patterns. Systems that notify PCPs when their Medicaid patients use the ER and 24-hour nurse consultation lines are among the ER diversion strategies in PCCM programs. Initiatives to monitor and reduce obesity were also reported by most states, with Medicaid MCOs often playing a leading role. About half the states reported current or planned initiatives in Medicaid to address racial and ethnic disparities, including participation in broader state efforts. Numerous states reported formal Medicaid performance improvement projects focused on reducing racial and ethnic disparities in certain measures (e.g., adolescents use of well-child visits, breast or cervical cancer screening rates), or on cultural competency. Some states calculate or publish quality measures by race/ethnicity. Several states reported broader public health efforts to reduce disparities, with Medicaid participating in interagency and community task forces and statewide collaboratives. States reported a broad spectrum of other, special managed care quality initiatives. Many states reported managed care quality initiatives in a host of additional areas, such as perinatal care and depression screening; improved care management for individuals with both behavioral health diagnoses and chronic conditions; identification of high-risk enrollees for intensive case management; dental utilization: and improving the data available to providers to benchmark their performance. Many states have initiatives to improve primary care and to better coordinate care for Medicaid beneficiaries with more complex needs. Medical home initiatives are underway or in development in 39 states. The same number of states reported disease management or care management programs, which, in many instances, are integrated into their MCO or PCCM programs. Twenty-two states reported plans to elect the new health home option established by the ACA. Nine states reported that they have an Accountable Care Organization (ACO) initiative underway, planned, or under development. Managed long-term care and managed care initiatives for dual eligibles Over half the states operate PACE sites, and 11 states reported operating additional managed longterm care (MLTC) programs. A total of 29 states operate PACE sites, which are paid on a risk basis to provide and coordinate the full range of medical and long-term services and supports for Medicaid enrollees; however, total PACE enrollment nationally is only about 20,000. Eleven states reported 5
8 operating non-pace MLTC programs as of October 2010, with aggregate enrollment exceeding 400,000. Some of these programs encompass only long-term services and supports, but others include acute medical care as well. Most include only Medicaid services, but programs in three states also include Medicare services. States highlighted numerous operational challenges associated with MLTC programs, such as contracting with Medicare Advantage Special Needs Plans, coordination with physical health MCOs, slow enrollment growth, and plan difficulty contracting with Boarding Homes. Half the states reported enrollment of dual eligibles in non-pace Medicaid managed care arrangements, on either a voluntary or mandatory basis. Overall, 25 states reported that they enroll dual eligibles in some kind of non-pace Medicaid managed care arrangement, on either a voluntary or a mandatory basis. In some states, dual eligibles are enrolled in comprehensive managed care; in others, dual eligibles may be enrolled in non-comprehensive PHPs for specific categories of services, but remain in fee-for-service for all other Medicaid-covered services. In many states, broader efforts focused on dual eligibles are expanding or getting underway. Twentyone states reported on plans to expand or modify current programs or initiate new programs focused on dual eligibles, including 15 states that received grant funding under the ACA initiative, State Demonstrations to Integrate Care for Dual Eligible Individuals, administered by the new Medicare- Medicaid Coordination Office in CMS, to design new approaches to better coordinate care for dual eligibles and integrate Medicare and Medicaid financing. Twenty-one states reported that they contract with Medicare Advantage Special Needs Plans to provide care for dual eligibles. Medicaid managed care and health reform States expect to rely increasingly on managed care in the near term. Continued budget pressures and interest in improving service delivery and payment systems are fueling plans in many states to expand the use of managed care in Medicaid, including mandatory managed care for additional Medicaid populations and in new geographic areas. Key health reform implications for Medicaid managed care are yet to come into focus in many states. A little over half the states with MCOs (20) reported that their plans had or could develop sufficient network capacity to handle increased Medicaid enrollment expected under health reform, while one state said its plans could not. Nine states reported that they did not know whether or not their MCOs could develop the capacity, and six states did not respond to this question. Uncertainty was wider regarding Medicaid MCOs interest in becoming Exchange plans, and especially concerning state intentions to require Medicaid MCOs to participate in the Exchanges or Exchange plans to participate in Medicaid. The widespread uncertainty may be an indication that more immediate issues and pressures still eclipse health reform in many Medicaid programs. Severe budget pressures remain a key challenge for states, and new demands associated with health reform also emerge as issues. The lingering effects of the recession reduced tax revenues, high unemployment, and high demand for Medicaid and other human services all continue to generate intense pressure on states already struggling to meet competing needs with limited resources. States cited additional challenges stemming from health reform, in particular, increased Medicaid enrollment, adequacy of provider networks, Exchange development, and development of systems for claiming the proper federal matching rate. Some states also cited a need for more flexibility to integrate care for dual eligibles. More general pressures, including required implementation of new procedure codes (ICD-10) and strains on state administrative capacity, were raised as well. 6
9 Conclusion For over 30 years, Medicaid programs have relied increasingly on managed care arrangements to deliver and finance care for Medicaid beneficiaries, and both the number and share of beneficiaries in managed care have grown steadily. Medicaid managed care is expected to continue to expand, driven by budget pressures to contain Medicaid spending and by the influx of millions of new Medicaid enrollees when the ACA takes full effect in As individual states look for new ways to improve care and achieve greater value for state dollars, there is much to be learned from the wide and evolving variety of Medicaid managed care program designs and experiences that can be found across the country. This survey documents the diversity in current state Medicaid managed care approaches and activity, and captures state policymakers perspectives on the value of managed care as a strategy to improve access, quality, and accountability and to promote cost-effective care and better health outcomes. As such, it provides a baseline against which to measure and monitor what are likely to be important developments and trends in the coming years. However, an assessment of the impact of Medicaid managed care was beyond the scope of this project, which surveyed state policy officials alone and gathered largely descriptive information. Particularly as states expand managed care to beneficiaries with more complex needs and shape the delivery systems that will serve millions more low-income Americans in the future, rigorous evaluative research, including investigations of beneficiary and provider experiences and perspectives, is crucial to identify the characteristics of managed care programs that are associated with gains for Medicaid beneficiaries and that advance state goals. Robust federal and state oversight is important, as well, to ensure that the design of managed care programs translates into access to high-quality care for the Medicaid enrollees they serve. 7
10
11 The Kaiser Family Foundation, a leader in health policy analysis, health journalism and communication, is dedicated to filling the need for trusted, independent information on the major health issues facing our nation and its people. The Foundation is a non-profit private operating foundation, based in Menlo Park, California.
12 1330 G S T R E E T NW, W A S H I N G T O N, DC P H O N E : (202) , F A X : ( 202) W E B S I T E : W W W. K F F. O R G /KCMU This publication (#8220-ES) is available on the Kaiser Family Foundation s website at
kaiser medicaid and the uninsured commission on A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey
 kaiser commission on medicaid and the uninsured A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey Prepared by Kathleen Gifford, Vernon K. Smith, and Dyke Snipes Health
kaiser commission on medicaid and the uninsured A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey Prepared by Kathleen Gifford, Vernon K. Smith, and Dyke Snipes Health
kaiser medicaid and the uninsured commission on A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey
 kaiser commission on medicaid and the uninsured A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey Prepared by Kathleen Gifford, Vernon K. Smith, and Dyke Snipes Health
kaiser commission on medicaid and the uninsured A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey Prepared by Kathleen Gifford, Vernon K. Smith, and Dyke Snipes Health
The Medicaid Landscape
 The Medicaid Landscape Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation Council of State Governments Washington, DC June 18, 2014 Figure 1 Medicaid
The Medicaid Landscape Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation Council of State Governments Washington, DC June 18, 2014 Figure 1 Medicaid
States and Medicaid Provider Taxes or Fees
 March 2016 Fact Sheet States and Medicaid Provider Taxes or Fees Medicaid is jointly financed by states and the federal government. Provider taxes are an integral source of Medicaid financing governed
March 2016 Fact Sheet States and Medicaid Provider Taxes or Fees Medicaid is jointly financed by states and the federal government. Provider taxes are an integral source of Medicaid financing governed
Medicaid in an Era of Change: Findings from the Annual Kaiser 50 State Medicaid Budget Survey
 Medicaid in an Era of Change: Findings from the Annual Kaiser 50 State Medicaid Budget Survey Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family
Medicaid in an Era of Change: Findings from the Annual Kaiser 50 State Medicaid Budget Survey Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family
Some Speech Titles Are Better Spoken Than Written. Hot Issues in Health Care December 5, 2017 Alan Weil Editor-in-Chief Health Affairs
 Some Speech Titles Are Better Spoken Than Written Hot Issues in Health Care December 5, 2017 Alan Weil Editor-in-Chief Health Affairs Because Whither: (adv) to what situation, position, degree or end Wither:
Some Speech Titles Are Better Spoken Than Written Hot Issues in Health Care December 5, 2017 Alan Weil Editor-in-Chief Health Affairs Because Whither: (adv) to what situation, position, degree or end Wither:
Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
Robin Rudowitz, Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family Foundation
 Medicaid Overview Robin Rudowitz, Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family Foundation Council of State Governments / Medicaid Leadership Policy Academy
Medicaid Overview Robin Rudowitz, Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family Foundation Council of State Governments / Medicaid Leadership Policy Academy
kaiser medicaid and the uninsured commission on The Cost and Coverage Implications of the ACA Medicaid Expansion: National and State-by-State Analysis
 kaiser commission on medicaid and the uninsured The Cost and Coverage Implications of the ACA Expansion: National and State-by-State Analysis Executive Summary John Holahan, Matthew Buettgens, Caitlin
kaiser commission on medicaid and the uninsured The Cost and Coverage Implications of the ACA Expansion: National and State-by-State Analysis Executive Summary John Holahan, Matthew Buettgens, Caitlin
Cost and Coverage Implications of the ACA Medicaid Expansion: National and State by State Analysis
 Cost and Coverage Implications of the ACA Medicaid Expansion: National and State by State Analysis Report Authors: John Holahan, Matthew Buettgens, Caitlin Carroll, and Stan Dorn Urban Institute November
Cost and Coverage Implications of the ACA Medicaid Expansion: National and State by State Analysis Report Authors: John Holahan, Matthew Buettgens, Caitlin Carroll, and Stan Dorn Urban Institute November
SCHIP: Let the Discussions Begin
 Figure 0 SCHIP: Let the Discussions Begin Diane Rowland, Sc.D. Executive Vice President, Henry J. Kaiser Family Foundation and Executive Director, Kaiser Commission on for Alliance for Health Reform February
Figure 0 SCHIP: Let the Discussions Begin Diane Rowland, Sc.D. Executive Vice President, Henry J. Kaiser Family Foundation and Executive Director, Kaiser Commission on for Alliance for Health Reform February
Alternative Paths to Medicaid Expansion
 Alternative Paths to Medicaid Expansion Robin Rudowitz Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation National Health Policy Forum March 28, 2014 Figure 1 The goal of the ACA
Alternative Paths to Medicaid Expansion Robin Rudowitz Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation National Health Policy Forum March 28, 2014 Figure 1 The goal of the ACA
CHARTPACK. Medicaid and its Role in State/Federal Budgets & Health Reform
 CHARTPACK Medicaid and its Role in State/Federal Budgets & Health Reform April 2013 Figure 1 #1: What is Medicaid and What Does it Do? Figure 2 Medicaid has many vital roles in our health care system.
CHARTPACK Medicaid and its Role in State/Federal Budgets & Health Reform April 2013 Figure 1 #1: What is Medicaid and What Does it Do? Figure 2 Medicaid has many vital roles in our health care system.
Latinas Access to Health Insurance
 FACT SHEET Latinas Access to Health Insurance APRIL 2018 Data released by the U.S. Census Bureau show that, despite significant health insurance gains since the Affordable Care Act (ACA) was implemented,
FACT SHEET Latinas Access to Health Insurance APRIL 2018 Data released by the U.S. Census Bureau show that, despite significant health insurance gains since the Affordable Care Act (ACA) was implemented,
Exhibit 1. The Impact of Health Reform: Percent of Women Ages Uninsured by State
 Exhibit 1. The Impact of Health Reform: Percent of Women Ages 19 64 Uninsured by State 2008 09 2019 (estimated) OR CA 23% WA NV 23% AK ID AZ UT MT WY CO NM 28% ND SD NE KS TX 31% OK MN IA MO WI AR 25%
Exhibit 1. The Impact of Health Reform: Percent of Women Ages 19 64 Uninsured by State 2008 09 2019 (estimated) OR CA 23% WA NV 23% AK ID AZ UT MT WY CO NM 28% ND SD NE KS TX 31% OK MN IA MO WI AR 25%
Medicaid s Future. National PACE Association Spring Policy Forum. MaryBeth Musumeci
 Medicaid s Future National PACE Association Spring Policy Forum MaryBeth Musumeci March 20, 2017 Figure 2 The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
Medicaid s Future National PACE Association Spring Policy Forum MaryBeth Musumeci March 20, 2017 Figure 2 The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
The Affordable Care Act (ACA)
 The Affordable Care Act (ACA) An Overview by the Kaiser Family Foundation NBC News Editorial Roundtable June 26, 2013 1. The Basics of the Affordable Care Act (ACA) Expanded Medicaid Coverage Starting
The Affordable Care Act (ACA) An Overview by the Kaiser Family Foundation NBC News Editorial Roundtable June 26, 2013 1. The Basics of the Affordable Care Act (ACA) Expanded Medicaid Coverage Starting
kaiser medicaid and the uninsured commission on
 kaiser commission on medicaid and the uninsured State Demonstrations to Integrate Care and Align Financing for Dual Eligible Beneficiaries: A Review of the 26 Proposals Submitted to CMS October 2012 1330
kaiser commission on medicaid and the uninsured State Demonstrations to Integrate Care and Align Financing for Dual Eligible Beneficiaries: A Review of the 26 Proposals Submitted to CMS October 2012 1330
The Impact of Health Reform s State Exchanges
 The Impact of Health Reform s State Exchanges May 2, 2013 Orlando, Florida Presented by: Layna S. Cook 225-381-7083 lcook@bakerdonelson.com The Affordable Care Act The Patient Protection and Affordable
The Impact of Health Reform s State Exchanges May 2, 2013 Orlando, Florida Presented by: Layna S. Cook 225-381-7083 lcook@bakerdonelson.com The Affordable Care Act The Patient Protection and Affordable
The State of Children s Health
 Figure 0 The State of Children s Health Robin Rudowitz Principal Policy Analyst Kaiser Commission on NCSL Annual Meeting Boston, MA August 8, 2007 Figure 1 SCHIP Builds on Medicaid for Children s Coverage
Figure 0 The State of Children s Health Robin Rudowitz Principal Policy Analyst Kaiser Commission on NCSL Annual Meeting Boston, MA August 8, 2007 Figure 1 SCHIP Builds on Medicaid for Children s Coverage
SCHIP Reauthorization: The Road Ahead
 SCHIP Reauthorization: The Road Ahead The State Children s Health Insurance Program: Past, Present and Future Jocelyn Guyer Georgetown University Health Policy Institute Center for Children and Families
SCHIP Reauthorization: The Road Ahead The State Children s Health Insurance Program: Past, Present and Future Jocelyn Guyer Georgetown University Health Policy Institute Center for Children and Families
Medicaid 1915(c) Home and Community-Based Service Programs: Data Update
 Medicaid 1915(c) Home and Community-Based Service Programs: Data Update OVERVIEW December 2006 Developing home and community-based service (HCBS) alternatives to institutional care has been a priority
Medicaid 1915(c) Home and Community-Based Service Programs: Data Update OVERVIEW December 2006 Developing home and community-based service (HCBS) alternatives to institutional care has been a priority
How is the Affordable Care Act Leading to Changes in Medicaid Today? State Adoption of Five New Options
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured How is the Affordable Care Act Leading to Changes in Medicaid Today? State Adoption of Five New Options May 2012 One primary goal of
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured How is the Affordable Care Act Leading to Changes in Medicaid Today? State Adoption of Five New Options May 2012 One primary goal of
Projected Savings of Medicaid Capitated Care: National and State-by-State. October 2015
 Projected Savings of Medicaid Capitated Care: National and State-by-State October 2015 I. Executive Summary We were asked by the Association for Community Affiliated Plans (ACAP) to estimate the Medicaid
Projected Savings of Medicaid Capitated Care: National and State-by-State October 2015 I. Executive Summary We were asked by the Association for Community Affiliated Plans (ACAP) to estimate the Medicaid
Medicaid Expansion and Section 1115 Waivers
 Medicaid Expansion and Section 1115 Waivers Council of State Governments National Conference December 11, 2015 Figure 1 The goal of the ACA is to make coverage more available, more reliable, and more affordable.
Medicaid Expansion and Section 1115 Waivers Council of State Governments National Conference December 11, 2015 Figure 1 The goal of the ACA is to make coverage more available, more reliable, and more affordable.
Report to Congressional Defense Committees
 Report to Congressional Defense Committees The Department of Defense Comprehensive Autism Care Demonstration December 2016 Quarterly Report to Congress In Response to: Senate Report 114-255, page 205,
Report to Congressional Defense Committees The Department of Defense Comprehensive Autism Care Demonstration December 2016 Quarterly Report to Congress In Response to: Senate Report 114-255, page 205,
Medicaid Managed LTSS Updates from the States and the Feds
 Medicaid Managed LTSS Updates from the States and the Feds Rachel Patterson Christopher & Dana Reeve Foundation July 20, 2015 2015 Summer Leadership Institute Agenda Context: Rising health care costs and
Medicaid Managed LTSS Updates from the States and the Feds Rachel Patterson Christopher & Dana Reeve Foundation July 20, 2015 2015 Summer Leadership Institute Agenda Context: Rising health care costs and
ACA and Medicaid: Current Landscape and Future Outlook
 ACA and Medicaid: Current Landscape and Future Outlook RPCC Health Policy Forum Washington, DC December 5, 2017 Robin Rudowitz Associate Director, Program on Medicaid and the Uninsured Kaiser Family Foundation
ACA and Medicaid: Current Landscape and Future Outlook RPCC Health Policy Forum Washington, DC December 5, 2017 Robin Rudowitz Associate Director, Program on Medicaid and the Uninsured Kaiser Family Foundation
Healthcare Reform. North Carolina Dietetic Association September 12, Duke Medicine
 Healthcare Reform North Carolina Dietetic Association September 12, 2014 Take home messages Healthcare [and health insurance] is transforming at an accelerating pace Key metrics of concern relate to quality,
Healthcare Reform North Carolina Dietetic Association September 12, 2014 Take home messages Healthcare [and health insurance] is transforming at an accelerating pace Key metrics of concern relate to quality,
ACA Medicaid Primary Care Fee Bump: Context and Impact
 ACA Medicaid Primary Care Fee Bump: Context and Impact Stephen Zuckerman Senior Fellow and Co-director, Health Policy Center Presentation at UW Population Health Institute May 5, 2015 ACA Medicaid Fee
ACA Medicaid Primary Care Fee Bump: Context and Impact Stephen Zuckerman Senior Fellow and Co-director, Health Policy Center Presentation at UW Population Health Institute May 5, 2015 ACA Medicaid Fee
Medicaid 101 Damon Terzaghi Senior Director NASUAD
 Medicaid 101 Damon Terzaghi Senior Director NASUAD dterzaghi@nasuad.org www.nasuad.org Contents Overview & History of Medicaid How Medicaid is Administered Overview of Eligibility Overview of Services
Medicaid 101 Damon Terzaghi Senior Director NASUAD dterzaghi@nasuad.org www.nasuad.org Contents Overview & History of Medicaid How Medicaid is Administered Overview of Eligibility Overview of Services
Obamacare in Pictures. Visualizing the Effects of the Patient Protection and Affordable Care Act
 Visualizing the Effects of the Patient Protection and Affordable Care Act Fall 2012 expands dependence on government health care dumps millions into Medicaid and creates new federal subsidies for government-approved
Visualizing the Effects of the Patient Protection and Affordable Care Act Fall 2012 expands dependence on government health care dumps millions into Medicaid and creates new federal subsidies for government-approved
Introducing LiveHealth Online
 Introducing LiveHealth Online Online Health Care when you need it! Meeting Members Wherever They Are 1 Why Consider Tele-Health? Convenience: Employees are able to access care at work, outside of traditional
Introducing LiveHealth Online Online Health Care when you need it! Meeting Members Wherever They Are 1 Why Consider Tele-Health? Convenience: Employees are able to access care at work, outside of traditional
CHAPTER 1. Trends in the Overall Health Care Market
 CHAPTER 1 Trends in the Overall Health Care Market Billions Chart 1.1: Total National Health Expenditures, 1980 2016 $4,000 $3,500 $3,000 $2,500 $2,000 $1,500 $1,000 $500 $0 Inflation Adjusted (2) 80 81
CHAPTER 1 Trends in the Overall Health Care Market Billions Chart 1.1: Total National Health Expenditures, 1980 2016 $4,000 $3,500 $3,000 $2,500 $2,000 $1,500 $1,000 $500 $0 Inflation Adjusted (2) 80 81
Current Trends in the Medicaid RFP Procurement Landscape
 Current Trends in the Medicaid RFP Procurement Landscape This is a Presentation Subtitle PRESENTED BY: Michael Lutz Avalere Health October 31, 2017 About Us Michael Lutz Vice President mlutz@avalere.com
Current Trends in the Medicaid RFP Procurement Landscape This is a Presentation Subtitle PRESENTED BY: Michael Lutz Avalere Health October 31, 2017 About Us Michael Lutz Vice President mlutz@avalere.com
Stand-Alone Prescription Drug Plans Dominated the Rural Market in 2011
 Stand-Alone Prescription Drug Plans Dominated the Rural Market in 2011 Growth Driven by Medicare Advantage Prescription Drug Plan Enrollment Leah Kemper, MPH Abigail Barker, PhD Fred Ullrich, BA Lisa Pollack,
Stand-Alone Prescription Drug Plans Dominated the Rural Market in 2011 Growth Driven by Medicare Advantage Prescription Drug Plan Enrollment Leah Kemper, MPH Abigail Barker, PhD Fred Ullrich, BA Lisa Pollack,
Data Note: What if Per Enrollee Medicaid Spending Growth Had Been Limited to CPI-M from ?
 Data Note: What if Per Enrollee Medicaid Spending Growth Had Been Limited to CPI-M from 2001-2011? Rachel Garfield, Robin Rudowitz, and Katherine Young Congress is currently debating the American Health
Data Note: What if Per Enrollee Medicaid Spending Growth Had Been Limited to CPI-M from 2001-2011? Rachel Garfield, Robin Rudowitz, and Katherine Young Congress is currently debating the American Health
Experts Predict Sharp Decline in Competition across the ACA Exchanges
 Percent of August 19, 2016 Experts Predict Sharp Decline in Competition across the ACA Exchanges Avalere experts predict that one-third of the country will have no exchange plan competition in 2017, leaving
Percent of August 19, 2016 Experts Predict Sharp Decline in Competition across the ACA Exchanges Avalere experts predict that one-third of the country will have no exchange plan competition in 2017, leaving
WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES CLASSIC PLAN WITH LOWER PLAN PREMIUMS
 PR Contact: IR Contact: H. Patel Jeff Potter CKPR WellCare Health Plans, Inc. (312) 616-2471 (813) 290-6313 hpatel@ckpr.biz jeff.potter@wellcare.com WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES
PR Contact: IR Contact: H. Patel Jeff Potter CKPR WellCare Health Plans, Inc. (312) 616-2471 (813) 290-6313 hpatel@ckpr.biz jeff.potter@wellcare.com WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES
PRODUCER ANNUITY SUITABILITY TRAINING REQUIREMENTS BY STATE As of September 11, 2017
 PRODUCER ANNUITY SUITABILITY TRAINING REQUIREMENTS BY STATE As of September 11, 2017 This document provides a summary of the annuity training requirements that agents are required to complete for each
PRODUCER ANNUITY SUITABILITY TRAINING REQUIREMENTS BY STATE As of September 11, 2017 This document provides a summary of the annuity training requirements that agents are required to complete for each
medicaid a n d t h e How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief
 on medicaid a n d t h e uninsured July 2012 How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief Effective January 2014, the ACA establishes a new minimum Medicaid
on medicaid a n d t h e uninsured July 2012 How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief Effective January 2014, the ACA establishes a new minimum Medicaid
Medicaid Home and Community-Based Services Programs:
 REPORT Medicaid Home and Community-Based Services Programs: March 2014 2010 Data Update Prepared by: Terence Ng and Charlene Harrington University of California, San Francisco and MaryBeth Musumeci and
REPORT Medicaid Home and Community-Based Services Programs: March 2014 2010 Data Update Prepared by: Terence Ng and Charlene Harrington University of California, San Francisco and MaryBeth Musumeci and
Health Reform & Immuniza3ons in 2014
 Health Reform & Immuniza3ons in 2014 Associa(on of Immuniza(on Managers Atlanta, Georgia Alexandra Stewart stewarta@gwu.edu Milken Ins(tute, School of Public Health, Department of Health Policy, GWU July
Health Reform & Immuniza3ons in 2014 Associa(on of Immuniza(on Managers Atlanta, Georgia Alexandra Stewart stewarta@gwu.edu Milken Ins(tute, School of Public Health, Department of Health Policy, GWU July
uninsured Hoping for Economic Recovery, Preparing for Health Reform: A Look at Medicaid Spending, Coverage and Policy Trends
 kaiser commission on medicaid and the uninsured Hoping for Economic Recovery, Preparing for Health Reform: A Look at Medicaid Spending, Coverage and Policy Trends Results from a 50-State Medicaid Budget
kaiser commission on medicaid and the uninsured Hoping for Economic Recovery, Preparing for Health Reform: A Look at Medicaid Spending, Coverage and Policy Trends Results from a 50-State Medicaid Budget
ehealth, Inc Fall Cost Report for Individual and Family Policyholders
 ehealth, Inc. 2010 Fall Cost Report for and Family Policyholders Table of Contents Page Methodology.................................................................. 2 ehealth, Inc. 2010 Fall Cost Report
ehealth, Inc. 2010 Fall Cost Report for and Family Policyholders Table of Contents Page Methodology.................................................................. 2 ehealth, Inc. 2010 Fall Cost Report
IOM Workshop The Impact of the Affordable Care Act on U.S. Preparedness Resources and Programs
 IOM Workshop The Impact of the Affordable Care Act on U.S. Preparedness Resources and Programs Session I Opportunities and Challenges within Financing Changes Jack Ebeler Health Policy Alternatives, Inc.
IOM Workshop The Impact of the Affordable Care Act on U.S. Preparedness Resources and Programs Session I Opportunities and Challenges within Financing Changes Jack Ebeler Health Policy Alternatives, Inc.
Health Coverage for the Black Population Today and Under the Affordable Care Act
 fact sheet Health Coverage for the Black Population Today and Under the Affordable Care Act July 2013 As of 2011, 37 million individuals living in the United States identified as Black or African American.
fact sheet Health Coverage for the Black Population Today and Under the Affordable Care Act July 2013 As of 2011, 37 million individuals living in the United States identified as Black or African American.
Rebalancing in Capitated Medicaid Managed Long-Term Services and Supports Programs: Key Issues from a Roundtable Discussion on Measuring Performance
 Rebalancing in Capitated Medicaid Managed Long-Term Services and Supports Programs: Key Issues from a Roundtable Discussion on Measuring Performance MaryBeth Musumeci Medicaid is an important source of
Rebalancing in Capitated Medicaid Managed Long-Term Services and Supports Programs: Key Issues from a Roundtable Discussion on Measuring Performance MaryBeth Musumeci Medicaid is an important source of
Older consumers and student loan debt by state
 August 2017 Older consumers and student loan debt by state New data on the burden of student loan debt on older consumers In January, the Bureau published a snapshot of older consumers and student loan
August 2017 Older consumers and student loan debt by state New data on the burden of student loan debt on older consumers In January, the Bureau published a snapshot of older consumers and student loan
Obamacare in Pictures
 Obamacare in Pictures VISUALIZING THE EFFECTS OF THE PATIENT PROTECTION AND AFFORDABLE CARE ACT Spring 2014 If you like your health care plan, can you really keep it? At least 4.7 million health care plans
Obamacare in Pictures VISUALIZING THE EFFECTS OF THE PATIENT PROTECTION AND AFFORDABLE CARE ACT Spring 2014 If you like your health care plan, can you really keep it? At least 4.7 million health care plans
Medicare Prescription Drug Congress. MMA and Medicaid. Gale Arden Director, Disabled & Elderly Health Programs Group CMSO CMS.
 Medicare Prescription Drug Congress MMA and Medicaid Gale Arden Director, Disabled & Elderly Health Programs Group CMSO CMS October 2005 Part D: Medicare Prescription Drug Coverage Effective: January 1,
Medicare Prescription Drug Congress MMA and Medicaid Gale Arden Director, Disabled & Elderly Health Programs Group CMSO CMS October 2005 Part D: Medicare Prescription Drug Coverage Effective: January 1,
Rural Policy Brief Volume 10, Number 8 (PB ) April 2006 RUPRI Center for Rural Health Policy Analysis
 Rural Policy Brief Volume 10, Number 8 (PB2006-8 ) April 2006 RUPRI Center for Rural Health Policy Analysis Medicare Part D: Early Findings on Enrollment and Choices for Rural Beneficiaries Authors: Timothy
Rural Policy Brief Volume 10, Number 8 (PB2006-8 ) April 2006 RUPRI Center for Rural Health Policy Analysis Medicare Part D: Early Findings on Enrollment and Choices for Rural Beneficiaries Authors: Timothy
Presented by: Matt Turkstra
 Presented by: Matt Turkstra 1 » What s happening in Ohio?» How is health insurance changing? Individual and Group Health Insurance» Important employer terms» Impact small businesses that do not offer insurance?
Presented by: Matt Turkstra 1 » What s happening in Ohio?» How is health insurance changing? Individual and Group Health Insurance» Important employer terms» Impact small businesses that do not offer insurance?
An Update on Commercial Exchanges. Myra Weisfeld, Senior Managing Consultant
 An Update on Commercial Exchanges Myra Weisfeld, Senior Managing Consultant Agenda Introduction & overview ACA Changes to insurance coverage Insurance exchange update Summary & questions 2 3 4 Payment
An Update on Commercial Exchanges Myra Weisfeld, Senior Managing Consultant Agenda Introduction & overview ACA Changes to insurance coverage Insurance exchange update Summary & questions 2 3 4 Payment
Implementing the Medicare Drug Benefit. Robert Donnelly Director, Medicare Drug Benefit Group June 8, 2005
 Implementing the Medicare Drug Benefit Robert Donnelly Director, Medicare Drug Benefit Group June 8, 2005 Medicare Challenges Providing the best care for a Medicare population that has longer life expectancy
Implementing the Medicare Drug Benefit Robert Donnelly Director, Medicare Drug Benefit Group June 8, 2005 Medicare Challenges Providing the best care for a Medicare population that has longer life expectancy
Medicaid Funding and Policies Is There a Medicaid Crisis? A Financial Diagnosis for State and Local Government
 Medicaid Funding and Policies Is There a Medicaid Crisis? A Financial Diagnosis for State and Local Government Matt Powers Health Management Associates March 15, 2007 Main Points Medicaid Remains a Workhorse
Medicaid Funding and Policies Is There a Medicaid Crisis? A Financial Diagnosis for State and Local Government Matt Powers Health Management Associates March 15, 2007 Main Points Medicaid Remains a Workhorse
Health and Health Coverage in the South: A Data Update
 February 2016 Issue Brief Health and Health Coverage in the South: A Data Update Samantha Artiga and Anthony Damico With its recent adoption of the Affordable Care Act (ACA) Medicaid expansion to adults,
February 2016 Issue Brief Health and Health Coverage in the South: A Data Update Samantha Artiga and Anthony Damico With its recent adoption of the Affordable Care Act (ACA) Medicaid expansion to adults,
State Trust Fund Solvency
 Unemployment Insurance State Trust Fund Solvency National Employment Law Project Conference - Washington DC December 7, 2009 Robert Pavosevich pavosevich.robert@dol.gov Unemployment Insurance Program
Unemployment Insurance State Trust Fund Solvency National Employment Law Project Conference - Washington DC December 7, 2009 Robert Pavosevich pavosevich.robert@dol.gov Unemployment Insurance Program
While one in five Californians overall is uninsured, the rate among those who work is even higher: one in four.
 : By the Numbers December 2013 Introduction California had the greatest number of uninsured residents of any state, 7 million, and the seventh largest percentage of uninsured residents under 65 in the
: By the Numbers December 2013 Introduction California had the greatest number of uninsured residents of any state, 7 million, and the seventh largest percentage of uninsured residents under 65 in the
Local Anesthesia Administration by Dental Hygienists State Chart
 Education or AK 1981 General Both Specific Yes WREB 16 hrs didactic; 6 hrs ; 8 hrs lab AZ 1976 General Both Accredited Yes WREB 36 hrs; 9 types of AR 1995 Direct Both Accredited/ Board Approved No 16 hrs
Education or AK 1981 General Both Specific Yes WREB 16 hrs didactic; 6 hrs ; 8 hrs lab AZ 1976 General Both Accredited Yes WREB 36 hrs; 9 types of AR 1995 Direct Both Accredited/ Board Approved No 16 hrs
September Turning 65. Beyond a Rite of Passage. A nonprofit service and advocacy organization National Council on Aging
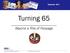 September 2012 Turning 65 Beyond a Rite of Passage 1 Cumulatively 31.4 million adults will turn 65 between 2012 and 2020 4,000,000 3,900,000 Turning 65 by Year 3.8 M 3,800,000 3,700,000 3,600,000 3,500,000
September 2012 Turning 65 Beyond a Rite of Passage 1 Cumulatively 31.4 million adults will turn 65 between 2012 and 2020 4,000,000 3,900,000 Turning 65 by Year 3.8 M 3,800,000 3,700,000 3,600,000 3,500,000
uninsured Moving Ahead Amid Fiscal Challenges: A Look at Medicaid Spending, Coverage and Policy Trends
 kaiser commission on medicaid and the uninsured Moving Ahead Amid Fiscal Challenges: A Look at Medicaid Spending, Coverage and Policy Trends Results from a 50-State Medicaid Budget Survey for State Fiscal
kaiser commission on medicaid and the uninsured Moving Ahead Amid Fiscal Challenges: A Look at Medicaid Spending, Coverage and Policy Trends Results from a 50-State Medicaid Budget Survey for State Fiscal
Getting Better Value for the Healthcare Dollar. National Conference of State Legislators Fall Forum November 30, 2011.
 Getting Better Value for the Healthcare Dollar National Conference of State Legislators Fall Forum November 30, 2011 NCQA History NCQA a non-profit that for 21 years has worked with federal, state, consumer
Getting Better Value for the Healthcare Dollar National Conference of State Legislators Fall Forum November 30, 2011 NCQA History NCQA a non-profit that for 21 years has worked with federal, state, consumer
uninsured Medicaid Today; Preparing for Tomorrow A Look at State Medicaid Program Spending, Enrollment and Policy Trends
 kaiser commission on medicaid and the uninsured Medicaid Today; Preparing for Tomorrow A Look at State Medicaid Program Spending, Enrollment and Policy Trends Results from a 50-State Medicaid Budget Survey
kaiser commission on medicaid and the uninsured Medicaid Today; Preparing for Tomorrow A Look at State Medicaid Program Spending, Enrollment and Policy Trends Results from a 50-State Medicaid Budget Survey
The Acquisition of Regions Insurance Group. April 6, 2018
 The Acquisition of Regions Insurance Group April 6, 2018 Forward-Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform
The Acquisition of Regions Insurance Group April 6, 2018 Forward-Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform
MARKET TRENDS: MEDICARE SUPPLEMENT. Gorman Health Group, LLC
 MARKET TRENDS: MEDICARE SUPPLEMENT Gorman Health Group, LLC Issued: December 1, 2016 TABLE OF CONTENTS EXECUTIVE SUMMARY... 3 OVERALL TRENDS IN MEDICARE SUPPLEMENT ENROLLMENT... 4 NATIONWIDE ENROLLMENT...
MARKET TRENDS: MEDICARE SUPPLEMENT Gorman Health Group, LLC Issued: December 1, 2016 TABLE OF CONTENTS EXECUTIVE SUMMARY... 3 OVERALL TRENDS IN MEDICARE SUPPLEMENT ENROLLMENT... 4 NATIONWIDE ENROLLMENT...
Patient Protection & Affordable Care Act
 Patient Protection & Affordable Care Act Joshua D. Goldberg National Association of Insurance Commissioners Symposium on Health Reform University of Iowa Public Policy Center July 20, 2010 Opportunities
Patient Protection & Affordable Care Act Joshua D. Goldberg National Association of Insurance Commissioners Symposium on Health Reform University of Iowa Public Policy Center July 20, 2010 Opportunities
Comparative Revenues and Revenue Forecasts Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas
 Comparative Revenues and Revenue Forecasts 2010-2014 Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas Comparative Revenues and Revenue Forecasts This data shows tax
Comparative Revenues and Revenue Forecasts 2010-2014 Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas Comparative Revenues and Revenue Forecasts This data shows tax
Florida s Medicaid Funding: A National Overview of Medicaid Waiver Trends
 Florida s Medicaid Funding: A National Overview of Medicaid Waiver Trends Joan Alker Executive Director Georgetown University Center for Children and Families Space Coast Health Foundation Melbourne, Florida
Florida s Medicaid Funding: A National Overview of Medicaid Waiver Trends Joan Alker Executive Director Georgetown University Center for Children and Families Space Coast Health Foundation Melbourne, Florida
Florida s Medicaid Choice: Options and Implications
 Florida s Medicaid Choice: Options and Implications Joan Alker Georgetown University Health Policy Institute Florida Philanthropic Network, Tallahassee, FL February 19, 2013 Florida vs. U.S.! Uninsured
Florida s Medicaid Choice: Options and Implications Joan Alker Georgetown University Health Policy Institute Florida Philanthropic Network, Tallahassee, FL February 19, 2013 Florida vs. U.S.! Uninsured
Lehman Brothers 2007 Global Healthcare Conference March 20, Ronald A. Williams Chairman, CEO and President
 March 20, 2007 Ronald A. Williams Chairman, CEO and President 2 Cautionary Statement CAUTIONARY STATEMENT -- Certain information in this presentation is forward looking information. Forward-looking information
March 20, 2007 Ronald A. Williams Chairman, CEO and President 2 Cautionary Statement CAUTIONARY STATEMENT -- Certain information in this presentation is forward looking information. Forward-looking information
2016 Workers compensation premium index rates
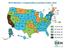 2016 Workers compensation premium index rates NH WA OR NV CA AK ID AZ UT MT WY CO NM MI VT ND MN SD WI NY NE IA PA IL IN OH WV VA KS MO KY NC TN OK AR SC MS AL GA TX LA FL ME MA RI CT NJ DE MD DC = Under
2016 Workers compensation premium index rates NH WA OR NV CA AK ID AZ UT MT WY CO NM MI VT ND MN SD WI NY NE IA PA IL IN OH WV VA KS MO KY NC TN OK AR SC MS AL GA TX LA FL ME MA RI CT NJ DE MD DC = Under
Trends in Spending on Social Assistance Over the Last 25 Years
 Trends in Spending on Social Assistance Over the Last 25 Years Did welfare reform (PRWORA, 1996) influence the trends? Did the federal government successfully shift responsibility for social assistance
Trends in Spending on Social Assistance Over the Last 25 Years Did welfare reform (PRWORA, 1996) influence the trends? Did the federal government successfully shift responsibility for social assistance
2016 GEHA. dental. FEDVIP Plans. let life happen. gehadental.com
 2016 GEHA dental FEDVIP Plans let life happen gehadental.com Smile, you re covered, with great benefits and a large national network. High maximum benefits $25,000 for High Option Growing network of dentists
2016 GEHA dental FEDVIP Plans let life happen gehadental.com Smile, you re covered, with great benefits and a large national network. High maximum benefits $25,000 for High Option Growing network of dentists
James G. Anderson, Ph.D. Purdue University
 Health Care Reform: Its Impact and Future Directions James G. Anderson, Ph.D. Purdue University Andersonj@purdue.edu Health Care System Models Models Other Countries United States Bismark Beveridge National
Health Care Reform: Its Impact and Future Directions James G. Anderson, Ph.D. Purdue University Andersonj@purdue.edu Health Care System Models Models Other Countries United States Bismark Beveridge National
Medicaid s High Cost Enrollees: How Much Do They Drive Program Spending?
 Medicaid s High Cost Enrollees: How Much Do They Drive Program? By Anna Sommers and Mindy Cohen March 2006 Overview Achieving cost savings in the Medicaid program has become increasingly important to federal
Medicaid s High Cost Enrollees: How Much Do They Drive Program? By Anna Sommers and Mindy Cohen March 2006 Overview Achieving cost savings in the Medicaid program has become increasingly important to federal
Yolanda K. Kodrzycki New England Public Policy Center Federal Reserve Bank of Boston
 The Growing Instability of Revenues over the Business Cycle: Putting the New England States in Perspective Yolanda K. Kodrzycki New England Public Policy Center Federal Reserve Bank of Boston Lincoln Institute
The Growing Instability of Revenues over the Business Cycle: Putting the New England States in Perspective Yolanda K. Kodrzycki New England Public Policy Center Federal Reserve Bank of Boston Lincoln Institute
March 10, 2015 HOUSE HEALTH POLICY COMMITTEE PRESENTATION. Rick Murdock Executive Director Michigan Association of Health Plans
 March 10, 2015 HOUSE HEALTH POLICY COMMITTEE PRESENTATION Rick Murdock Executive Director Michigan Association of Health Plans 1 MAHP: Who We Are The Michigan Association of Health Plans is a nonprofit
March 10, 2015 HOUSE HEALTH POLICY COMMITTEE PRESENTATION Rick Murdock Executive Director Michigan Association of Health Plans 1 MAHP: Who We Are The Michigan Association of Health Plans is a nonprofit
Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications
 Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications June 28, 2012 Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy In a 5-4 Decision,
Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications June 28, 2012 Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy In a 5-4 Decision,
Medicare Alert: Temporary Member Access
 Medicare Alert: Temporary Member Access Plan Sponsor: Coventry/Aetna Medicare Part D Effective Date: Jan. 12, 2015 Geographic Area: National If your pharmacy is a Non Participating provider in the Aetna/Coventry
Medicare Alert: Temporary Member Access Plan Sponsor: Coventry/Aetna Medicare Part D Effective Date: Jan. 12, 2015 Geographic Area: National If your pharmacy is a Non Participating provider in the Aetna/Coventry
Medicaid Funding Reform: Impact on Dual Eligible Beneficiaries
 Medicaid Funding Reform: Impact on Dual Eligible Beneficiaries Avalere Health An Inovalon Company April 20, 2017 Overview 1. Executive Summary 2. Understanding Links Between Medicare and Medicaid 3. Medicaid
Medicaid Funding Reform: Impact on Dual Eligible Beneficiaries Avalere Health An Inovalon Company April 20, 2017 Overview 1. Executive Summary 2. Understanding Links Between Medicare and Medicaid 3. Medicaid
WHO GAINED INSURANCE COVERAGE IN 2014, THE FIRST YEAR OF FULL ACA IMPLEMENTATION?
 Journal Code Article ID Dispatch:.0. CE: H E C No. of Pages: ME: HEALTH ECONOMICS Health Econ. () Published online in Wiley Online Library (wileyonlinelibrary.com). DOI:.0/hec. HEALTH ECONOMICS LETTER
Journal Code Article ID Dispatch:.0. CE: H E C No. of Pages: ME: HEALTH ECONOMICS Health Econ. () Published online in Wiley Online Library (wileyonlinelibrary.com). DOI:.0/hec. HEALTH ECONOMICS LETTER
A Blue Cross and Blue Shield Association Presentation
 A Blue Cross and Blue Shield Association Presentation Issues in Healthcare Reform CSG Spring Conference Health Policy Task Force Joan Gardner Executive Director, State Services May 17, 2009 Healthcare
A Blue Cross and Blue Shield Association Presentation Issues in Healthcare Reform CSG Spring Conference Health Policy Task Force Joan Gardner Executive Director, State Services May 17, 2009 Healthcare
The Economic Stimulus and Health Chairs
 The Economic Stimulus and Health Chairs Friday, April 17, 2009, 2:00 pm EDT A partnership between the Kaiser Family Foundation and the NCSL Health Chairs Project Moderators: Donna Folkemer, Group Director,
The Economic Stimulus and Health Chairs Friday, April 17, 2009, 2:00 pm EDT A partnership between the Kaiser Family Foundation and the NCSL Health Chairs Project Moderators: Donna Folkemer, Group Director,
TCJA and the States Responding to SALT Limits
 TCJA and the States Responding to SALT Limits Kim S. Rueben Tuesday, January 29, 2019 1 What does this mean for Individuals under TCJA About two-thirds of taxpayers will receive a tax cut with the largest
TCJA and the States Responding to SALT Limits Kim S. Rueben Tuesday, January 29, 2019 1 What does this mean for Individuals under TCJA About two-thirds of taxpayers will receive a tax cut with the largest
In addition, MCHCP is requesting information about any programs or plans in place for non-medicare retirees.
 Missouri Consolidated Health Care Plan 832 Weathered Rock Court PO Box 104355 Jefferson City, MO 65110 Phone: 800-701-8881 www.mchcp.org Judith Muck, Executive Director February 7, 2018 To: From: Regarding:
Missouri Consolidated Health Care Plan 832 Weathered Rock Court PO Box 104355 Jefferson City, MO 65110 Phone: 800-701-8881 www.mchcp.org Judith Muck, Executive Director February 7, 2018 To: From: Regarding:
Health Benefits for Local Gove rnment. Findings from 2011 ICMA-CIGNA Study /11
 Health Benefits for Local Gove rnment Findings from 2011 ICMA-CIGNA Study 12 848973 09/11 Research Findings Health Benefits for Local Government Table of Contents Introduction...1 Top Operating Concerns...1
Health Benefits for Local Gove rnment Findings from 2011 ICMA-CIGNA Study 12 848973 09/11 Research Findings Health Benefits for Local Government Table of Contents Introduction...1 Top Operating Concerns...1
The Affordable Care Act and Childhood Asthma
 The Affordable Care Act and Childhood Asthma An Opportunity to Help Millions of Children Breathe Easier Webinar sponsored by the Childhood Asthma Leadership Coalition September 13, 2012 The ACA and Childhood
The Affordable Care Act and Childhood Asthma An Opportunity to Help Millions of Children Breathe Easier Webinar sponsored by the Childhood Asthma Leadership Coalition September 13, 2012 The ACA and Childhood
kaiser medicaid and the uninsured commission on O L I C Y R I E F April 2012
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured April 2012 An Update on CMS s Capitated Financial Alignment Demonstration Model for Medicare-Medicaid Enrollees Executive Summary Beginning
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured April 2012 An Update on CMS s Capitated Financial Alignment Demonstration Model for Medicare-Medicaid Enrollees Executive Summary Beginning
The Lincoln National Life Insurance Company Term Portfolio
 The Lincoln National Life Insurance Company Term Portfolio State Availability as of 7/16/2018 PRODUCTS AL AK AZ AR CA CO CT DE DC FL GA GU HI ID IL IN IA KS KY LA ME MP MD MA MI MN MS MO MT NE NV NH NJ
The Lincoln National Life Insurance Company Term Portfolio State Availability as of 7/16/2018 PRODUCTS AL AK AZ AR CA CO CT DE DC FL GA GU HI ID IL IN IA KS KY LA ME MP MD MA MI MN MS MO MT NE NV NH NJ
Percent of Employees Waiving Coverage 27.0% 30.6% 29.1% 23.4% 24.9%
 Number of Health Plans Reported 18,186 3,561 681 2,803 3,088 Offer HRA or HSA 34.0% 42.7% 47.0% 39.7% 35.0% Annual Employer Contribution $1,353 $1,415 $1,037 $1,272 $1,403 Percent of Employees Waiving
Number of Health Plans Reported 18,186 3,561 681 2,803 3,088 Offer HRA or HSA 34.0% 42.7% 47.0% 39.7% 35.0% Annual Employer Contribution $1,353 $1,415 $1,037 $1,272 $1,403 Percent of Employees Waiving
Patient Protection and. Affordable Care Act: The Impact on Employers
 Patient Protection and Affordable Care Act: The Impact on Employers April 2013 Agenda Introductions Individual Mandate Healthcare Exchange Overview Impact on Employers Essential Health Benefits Fees &
Patient Protection and Affordable Care Act: The Impact on Employers April 2013 Agenda Introductions Individual Mandate Healthcare Exchange Overview Impact on Employers Essential Health Benefits Fees &
Figure ES-1. International Comparison of Spending on Health,
 Figure ES-1. International Comparison of Spending on Health, 198 24 Average spending on health per capita ($US PPP) Total expenditures on health as percent of GDP 7 6 5 4 United States Germany Canada France
Figure ES-1. International Comparison of Spending on Health, 198 24 Average spending on health per capita ($US PPP) Total expenditures on health as percent of GDP 7 6 5 4 United States Germany Canada France
Marilyn Tavenner, CMS Administrator Don Moulds, Acting Assistant Secretary for Planning and Evaluation
 TO: The Secretary Through: DS COS ES FROM: Marilyn Tavenner, CMS Administrator Don Moulds, Acting Assistant Secretary for Planning and Evaluation DATE: September 5, 2013 SUBJECT: Projected Monthly Targets
TO: The Secretary Through: DS COS ES FROM: Marilyn Tavenner, CMS Administrator Don Moulds, Acting Assistant Secretary for Planning and Evaluation DATE: September 5, 2013 SUBJECT: Projected Monthly Targets
Presented by: Daniel J. Prescott Regional Senior Vice President
 The Affordable Care Act: Who Wins and Who Loses? Presented by: Daniel J. Prescott Regional Senior Vice President Large Market Winners & Losers in the Affordable Care Act Employers Individuals Insurance
The Affordable Care Act: Who Wins and Who Loses? Presented by: Daniel J. Prescott Regional Senior Vice President Large Market Winners & Losers in the Affordable Care Act Employers Individuals Insurance
Web Briefing for Journalists: Marketplace Open Enrollment in the Trump Era. Presented by the Kaiser Family Foundation October 18, 2017
 Web Briefing for Journalists: Marketplace Open Enrollment in the Trump Era Presented by the Kaiser Family Foundation October 18, 2017 Craig Palosky Director of Communications Larry Levitt Senior Vice President
Web Briefing for Journalists: Marketplace Open Enrollment in the Trump Era Presented by the Kaiser Family Foundation October 18, 2017 Craig Palosky Director of Communications Larry Levitt Senior Vice President
Indexed Universal Life Caps
 Indexed Universal Life Caps Effective March 15, 2013, the caps on FG Life-Elite II will be changing as follows: Cap Illustrative Rate 100% Participation Annual Point-to-Point 14.75% 8.32% 140% Participation
Indexed Universal Life Caps Effective March 15, 2013, the caps on FG Life-Elite II will be changing as follows: Cap Illustrative Rate 100% Participation Annual Point-to-Point 14.75% 8.32% 140% Participation
Medicaid in an Era of Health & Delivery System Reform:
 REPORT Medicaid in an Era of Health & Delivery System Reform: October Results from a 50-State Medicaid Budget Survey for State Fiscal Years and Prepared by: Vernon K Smith, Ph.D., Kathleen Gifford and
REPORT Medicaid in an Era of Health & Delivery System Reform: October Results from a 50-State Medicaid Budget Survey for State Fiscal Years and Prepared by: Vernon K Smith, Ph.D., Kathleen Gifford and
36 Million Without Health Insurance in 2014; Decreases in Uninsurance Between 2013 and 2014 Varied by State
 36 Million Without Health Insurance in 2014; Decreases in Uninsurance Between 2013 and 2014 Varied by State An estimated 36 million people in the United States had no health insurance in 2014, approximately
36 Million Without Health Insurance in 2014; Decreases in Uninsurance Between 2013 and 2014 Varied by State An estimated 36 million people in the United States had no health insurance in 2014, approximately
Medicaid Managed Care Final Rule
 Medicaid Managed Care Final Rule Modernizes and More Closely Aligns Medicaid Managed Care with Medicare Advantage and Exchange Requirements May 19, 2016 Lynn Shapiro Snyder Helaine I. Fingold 2016 Epstein
Medicaid Managed Care Final Rule Modernizes and More Closely Aligns Medicaid Managed Care with Medicare Advantage and Exchange Requirements May 19, 2016 Lynn Shapiro Snyder Helaine I. Fingold 2016 Epstein
