Medicaid Managed Care Final Rule
|
|
|
- Archibald Mathews
- 5 years ago
- Views:
Transcription
1 Medicaid Managed Care Final Rule Modernizes and More Closely Aligns Medicaid Managed Care with Medicare Advantage and Exchange Requirements May 19, 2016 Lynn Shapiro Snyder Helaine I. Fingold 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
2 Presented by Helaine Fingold Senior Counsel Phone: Lynn Shapiro Snyder Senior Member of the Firm Phone: Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
3 Agenda I. Background on Medicaid Managed Care II. Major Provisions of the Proposed Rule a. Introduction b. Network Adequacy c. Medical Loss Ratio d. Actuarially Sound Capitation Rates e. Quality of Care Standards f. Appeals and Grievances g. State Monitoring Standards h. Information Standards i. Managed Long-Term Services and Supports j. Beneficiary Enrollment Protections III. Key Takeaways 3
4 I. Background on Medicaid Managed Care 2015 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
5 I. Background on Medicaid Managed Care OVERVIEW Medicaid is largest U.S. payer (by headcount) Covers 72 million Americans $492 billion Core financing source for safety-net hospitals and health centers that serve lowincome communities, plus long-term care facilities 39 states contract with comprehensive Managed Care Organizations (MCOs) for Medicaid More than 70 percent (46 million) of all Medicaid beneficiaries get at least some care through these entities CMS last issued comprehensive Medicaid managed care regulations in 2002 Rule also governs managed care under Children s Health Insurance Program (CHIP) SOURCES: The Henry J. Kaiser Family Foundation, Medicaid Moving Forward (Mar. 9, 2015), available at See also The Henry J. Kaiser Family Foundation, State Health Facts, Total Monthly Medicaid and CHIP Enrollment (Feb. 2016), available at The Henry J. Kaiser Family Foundation, Key Findings on Medicaid Managed Care: Highlights from the Medicaid Managed Care Market Tracker, (Dec. 2, 2014) 5
6 I. Background on Medicaid Managed Care MEDICAID ENROLLMENT TRENDS Affordable Care Act enacted Health Insurance Exchanges and insurance subsidies available Total Enrollment Medicaid Managed Care Traditional Medicaid Medicaid Expansion In Millions No data No data No data None None 1 0* Source: Centers for Medicare & Medicaid 2013 Statistical Supplement, Table 13.4; AIS Medicare and Medicaid Market Data, 2015; Kaiser Family Foundation, Total Monthly Medicaid and CHIP Enrollment for May 2014 and May 2015; CMS, Medicaid Managed Care Penetration Rates as of December 31, 2010; CMS National Summary Of Medicaid Managed Care Programs And Enrollment as of July 1, 2010; CMS, Total Medicaid Enrollees - VIII Group Break Out Report, March 2015, Reported on the CMS-64. Coverage Gains Under Recent Section 1115 Waivers: A Data Update, S. Artiga and C. Mann, Kaiser Family Foundation, August *Enrollment was above zero but under 500,000, thus was rounded down. 6
7 I. Background on Medicaid Managed Care DEVELOPMENT TIMELINE Section 1115 added to Social Security Act to allow for waiver of program requirements for pilot or experimental projects Health Maintenance Organization Act OBRA added 1915(b) freedom of choice waivers and replaced 50/50 with 75/25 rule Oregon statewide Medicaid managed care waiver approved, allowed for service prioritization CMS releases changes to the Medicaid managed care rules CMS releases first comprehensive changes to the Medicaid managed care rules in 14 years Medicaid Program enacted HMO Amendments adds 50/50 rule for Medicaid risk plans Arizona granted the first statewide Medicaid managed care waiver under Section 1115 Balanced Budget Act allows for mandatory managed care without waiver and eliminates 75/25 rule ACA extends Medicaid drug rebate program to managed care, allows for expansion up to 138% of Poverty 7
8 I. Background on Medicaid Managed Care MOST STATES USE MEDICAID MANAGED CARE PLANS CA OR WA NV ID UT AZ MT WY CO NM ND SD NE KS OK MN IA MO AR WI IL MS MI IN TN AL OH KY WV GA PA SC VT NY VA NC ME NH CT RI NJ DE MD DC MA AK TX LA FL HI MCO only MCO and Primary Care Case Management PCCM only (may include ACO) No Comprehensive MMC Source: Adapted from data from the Kaiser Family Foundation, Medicaid Reforms to Expand Coverage, Control Costs and Improve Care: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2015 and 2016, October 15,
9 II.a. Major Provisions of the Final Rule Introduction 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
10 II.a. Major Provisions of the Final Rule Introduction AIM OF FINAL RULE Modernize managed care in Medicaid and CHIP to Reflect changes in managed care delivery systems Facilitate and support delivery system reform initiatives to improve outcomes and manage costs Strengthen the quality of care provided to Medicaid beneficiaries and Promote more effective use of data in overseeing managed care programs Revise MMC and CHIP rules to better align with Medicare Advantage ( MA ) and qualified health plans ( QHPs ) sold through ACA marketplaces Improve experience for persons who move between coverage options due to changes in circumstances Reduce administrative burden on regulators and issuers operating in multiple markets Encourages issuers in MA and ACA marketplaces to enter the Medicaid market this rule modernizes the Medicaid managed care regulatory 10
11 II.a. Major Provisions of the Final Rule Introduction WHAT KINDS OF ENTITIES ARE AFFECTED? Applies to all Medicaid Managed Care ( MMC ) entities, including Managed Care Organizations ( MCOs ) Prepaid Inpatient Health Plans ( PIHPs ) Prepaid Ambulatory Health Plans ( PAHPs ) Managed Long-Term Services and Supports ( MLTSS ) programs New types of entity -- PCCM [Primary Care Case Management] Entities Reflects entities conducting enhanced PCCM services, paid more robust capitation CMS would hold PCCM Entities to the same standards as other MMC entities Does not apply to ACOs or Primary Care Medical Homes 11
12 II.b. Major Provisions of the Final Rule Network Adequacy 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
13 II.b. Major Provisions of the Final Rule NETWORK ADEQUACY States must set time and distance standards for providers of: Pharmacy Primary care (adult and pediatric) OB/GYN Mental health/substance use disorder (adult and pediatric) Pediatric dental Exceptions allowed if monitored by the state Other factors states must consider Specialists (adult and pediatric) (can be further defined by states) Hospital Other providers if applying such standards promotes the objectives of the Medicaid program Expected Medicaid enrollment and utilization of services Characteristics and health needs of the covered population Number and types of health care professionals required to provide covered services Number of network providers that are not accepting new Medicaid patients Geographic location and accessibility of both providers and enrollees Ability of providers to ensure accessibility and required equipment for the disabled Reasonable accommodations Providers ability to communicate in a culturally competent manner Availability of technological solutions States may apply additional factors which need not be the same or applied uniformly across a state or across provider types 13
14 II.b. Major Provisions of the Final Rule NETWORK ADEQUACY States are also advised to look to The state s network adequacy standards for commercial insurance MA plan network adequacy standards Historical patterns of Medicaid utilization Timeliness would be assessed as routine, urgent, or emergency care Publish network adequacy standards for transparency MMC entity required to document network adequacy for state review at least yearly and when a significant change to operations would affect capacity and services External Quality Review Organization must validate plans network adequacy for the previous 12 months MLTSS must have distinct network adequacy standards Based on the same factors as for medical services May vary, based on whether the enrollee or provider must travel to provide services Should consider strategies to ensure the health and welfare of enrollees using LTSS and to support community integration of individuals receiving LTSS 14
15 II.c. Major Provisions of the Final Rule Medical Loss Ratio 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
16 II.c. Major Provisions of the Final Rule MEDICAL LOSS RATIO States must develop capitation rates so that managed care plans can be expected to reasonably achieve at least an 85 percent MLR States may choose higher minimum Standards for calculating the MLR are consistent with those for MA and the private market with some variation due to unique characteristics of the Medicaid and CHIP Calculates the MLR over a 12-month period States may collect remittances if MMC entity has MLR <85 percent (with FMAP percentage returned to the federal government) CMS acknowledges its lack of enforcement authority over Medicaid MLR However, CMS will use its authority over approval of capitation rates to ensure that rates are adequate to enable plans to show an expected MLR of 85 percent or higher 16
17 II.c. Major Provisions of the Final Rule MEDICAL LOSS RATIO Medicaid MLR Incurred claims + Quality Improvement Expenditures Premium Revenue - Federal & State Taxes, Licensing & Regulatory Fees Incurred claims consist of all claims costs for covered state plan services, including, for example Incentive and bonus payments paid and expected to be paid to providers Anticipated coordination of benefits recoveries Amounts which must be deducted from incurred claims include, for example Prescription drug rebates Overpayment recoveries Amounts paid, including to a provider, for professional or administrative services that do not represent compensation or reimbursement for State plan services 17
18 II.c. Major Provisions of the Final Rule MEDICAL LOSS RATIO Medicaid MLR Incurred claims + Quality Improvement Expenditures Premium Revenue - Federal & State Taxes, Licensing & Regulatory Fees Quality improvement activities include those related to service coordination, case management and activities supporting state goals for community integration Detail not stated in regulation leaving it to individual states to determine which activities qualify as quality improvement Pass-through payments as directed by the state that are not tied to utilization or quality are not included in either the numerator or the denominator, for example Graduate medical education payments or supplemental payments for uncompensated care 18
19 II.d. Major Provisions of the Final Rule Setting Actuarially Sound Capitation Rates 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
20 II.d. Major Provisions of the Final Rule SETTING ACTUARIALLY SOUND CAPITATION RATES Aims to ensure that MCO, PIHP, and PAHP Medicaid rates are developed in a transparent and consistent manner across MMC programs Incorporates principles of actuarial soundness: Rates should be sufficient and appropriate for the anticipated service utilization of the populations and services covered and compensate plans for reasonable non-benefit costs Capitation rates should promote program goals, such as quality of care, improved health, community integration of enrollees, and cost containment Actuarial rate certification should give sufficient detail, documentation, and transparency of rate-setting components Transparent and uniformly applied rate review and approval process based on actuarial practices should ensure that both the state and CMS act effectively as fiscal stewards and in the interests of beneficiary access to care Sets forth the types of data to be used for rate setting and the level of documentation/ detail so CMS can more effectively review and approve rates 20
21 II.d. Major Provisions of the Final Rule SETTING ACTUARIALLY SOUND CAPITATION RATES States need to certify each individual rate per rate cell as actuarially sound Rate cell is a set of mutually exclusive categories of enrollees defined by one or more characteristics for the purpose of determining the capitation rate, o May include age, gender, eligibility category, and region or geographic area May no longer use capitation rate ranges States are given flexibility to increase or decrease the certified capitation rate by one and a half percent without the need to submit a revised rate certification for CMS review and approval State may use risk sharing arrangements, incentive arrangements, and withholds arrangements to reward MCOs, PIHPs, and PAHPs for meeting performance targets specified in the contract Contracts would need to include a description of any risk sharing mechanisms and those mechanisms must be computed on an actuarially sound basis 21
22 II.e. Major Provisions of the Final Rule Quality of Care Provisions 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
23 II.e. Major Provisions of the Final Rule QUALITY OF CARE STANDARDS Quality provisions of Final Rule seek to enhance transparency, align quality measurements with other systems of care where possible, and strive to improve consumer and stakeholder engagement Proposed changes center on Quality Performance review and approval process Development of a quality rating system Expansion of the comprehensive quality strategy to encompass FFS and MMC Data and information disclosure to increase accountability Standards for performance measures and topics for performance improvement projects Revisions to the external quality review system 23
24 II.e. Major Provisions of the Final Rule QUALITY OF CARE STANDARDS Quality Performance Review and Approval Process ( QPRAP ) States must Require through contract that each MCO, PIHP, PAHP, and certain PCCM entities establish and implement an ongoing comprehensive quality assessment program for the services it provides to enrollees Review at least annually the impact and effectiveness of the QPRAP of each entity QPRAPs must include Performance Improvement Projects ( PIPs ) Collection and submission of performance measurement data Mechanisms to detect both underutilization and overutilization of services Mechanisms to assess the quality and appropriateness of care furnished to enrollees with special health care needs, including those in MLTSS Information from annual reviews must be publicly available on the state s website 24
25 II.e. Major Provisions of the Final Rule QUALITY OF CARE STANDARDS Quality Rating System ( QRS ) State may use CMS-defined QRS or develop its own subject to CMS approval Based on (but not identical to) summary indicators used in Exchange QRS Clinical quality management Member experience Plan efficiency, affordability and management Refined by robust public process, including notice and comment, over 3-5 years Methodology reassessed every 2-3 years to accommodate changes Did NOT finalize proposal to allow states to rely on the MA 5-star ratings for dual eligible plans States must post ratings online to help beneficiaries to make informed decisions 25
26 II.e. Major Provisions of the Final Rule QUALITY OF CARE STANDARDS External Quality Review The Secretary will develop protocols for External Quality Review ( EQR ) State must contract with EQR Organization ( EQRO ) EQR activities include Validation of network adequacy for prior 12 months, different from assessing availability of services (required) Validation of compliance with MCO, PIHP and PAHP standards for previous 3-year period (required) PIP validation Validation of encounter data (optional) Administration of consumer or provider surveys on quality of care (optional) State may rely on results of Medicare review or private accreditation survey instead of requiring EQR performance of required EQR activities 26
27 II.f. Major Provisions of the Final Rule Appeals and Grievances 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
28 II.f. Major Provisions of the Final Rule APPEALS & GRIEVANCES Aligns Medicaid/CHIP appeals and grievance processes with those for MA and QHPs Current differences hinder creation of a streamlined process across the public and private managed care sectors, creating unnecessary administrative complexity for those participating across product lines Appeals and grievances requirements are extended to PAHPs MMC plans must offer one level of internal appeal after which beneficiaries may request a state fair hearing, similar to rules for individual QHP products and MA Plan failure to meet timeframes deems enrollee as meeting exhaustion requirements Providers would be allowed to appeal on behalf of beneficiaries with written consent from enrollees (changed from proposed rule which said without consent) Timing for resolution of appeals would be reduced For standard appeal determinations to 30 days from 45 For expedited appeal determinations to 72 hours from 3 working days 28
29 II.f. Major Provisions of the Final Rule APPEALS & GRIEVANCES Procedural protections for appeals are strengthened Clarifies information that must be considered in an appeal and that which must be made available to beneficiaries Requires implementation of reversal of adverse benefit determination within 72 hours Timeframe for enrollees to request a state fair hearing extended from a maximum of 90 days to 120 calendar days Continuation of benefits while appeal is pending MMC plans would no longer be able to stop any services pending determination of appeals States may allow recoupment from enrollee if adverse determination upheld so long as the same standard is applied to both FFS and managed Medicaid 29
30 II.g. Major Provisions of the Final Rule State Monitoring Standards 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
31 II.g. Major Provisions of the Final Rule STATE MONITORING STANDARDS States must Implement a monitoring/oversight system to address, at a minimum: Administration and management Appeal and grievance systems Claims management Enrollee materials and customer services Finance, including MLR reporting Information systems, including encounter data reporting Marketing Medical management, including utilization management Program integrity Provider network management Quality improvement Delivery of LTSS Submit annual program assessment to CMS and post the assessment publicly Use data collected from its monitoring activities to improve the performance of its managed care program Conduct readiness assessments of each MCO, PIHP, PAHP and PCCM entity as follows: o Prior to start of a new managed care program, when a new contractor enters an existing program or when the state adds new benefits, populations, or geographic areas to the scope of its contracted managed care plans Readiness review would, at baseline, assess: plan operations and administration, service delivery, financial management and systems management 31
32 II.h. Major Provisions of the Final Rule Information Requirements 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
33 II.h. Major Provisions of the Final Rule INFORMATION REQUIREMENTS Changes made to strengthen MMC beneficiary information dissemination rules, more closely align with MA and commercial, better reflect technology advances, recognize cultural/linguistic diversity of Medicaid beneficiaries Apply consistently across MMC plans, including MCOs, PIHPs, PAHPs, PCCM and PCCM entities, with respect to enrollee materials States and MMC entities must make materials available in prevalent languages To include taglines on availability of written materials in those languages and oral interpretation in understanding the materials MMC entities must also make available vital documents in each prevalent non- English language in the MMC s service area, to include Provider directories Member handbooks Formulary Other notices critical to obtaining services MMC entities also must post provider directories on their websites in a CMSspecified machine-readable file and format 33
34 II.i. Major Provisions of the Final Rule Managed Long-Term Services & Supports 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
35 II.i. Major Provisions of the Final Rule MANAGED LONG-TERM SERVICES AND SUPPORTS In 2004, eight states (AZ, FL, MA, MI, MN, NY, TX, and WI) had implemented MLTSS programs. By January 2014, 12 additional states had implemented MLTSS programs (CA, DE, IL, KS, NC, NM, OH, PA, RI, TN, VA, WA) New requirements on MLTSS when provided through MCOs, PIHPs and PAHPs Enrollment and benefits complaint mechanism Education Assistance with grievances, appeals, and fair hearings, and Review of program data to identify and resolve systemic issues Regulation provides new requirements on MLTSS in support of the 10 key principles for MLTSS set out in 2013 guidance Adequate program planning Stakeholder engagement Enhanced home and community-based services Payment alignment Beneficiary support and protections Person-centered process Comprehensive, integrated service package Qualified providers Participant protections Quality 35
36 II.j. Major Provisions of the Final Rule Beneficiary Enrollment Provisions 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
37 II.j. Major Provisions of the Final Rule Other BENEFICIARY ENROLLMENT PROVISIONS States may passively enroll beneficiaries effective upon eligibility determination, subject to the enrollees right to opt-out or elect a different managed care plan CMS declined to finalize 14-day choice period to affirmatively choose a plan or opt for FFS For passive or default enrollment States must seek to preserve provider-beneficiary relationships and relationships with providers that have traditionally served Medicaid If not possible, states must equitably distribute beneficiaries among available plans and may not arbitrarily exclude any plans Additional assignment criteria are permitted, to reflect o Beneficiary location and preferences o Previous plan assignment o Access needs for disabled beneficiaries o Quality and procurement considerations 37
38 III. Key Takeaways 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
39 III. Key Takeaways CMS goal: harmonization across MMC, MA, QHPs i. Administrative simplification ii. Continuity for beneficiaries as they move between markets Provider impact: Generally positive i. Floor on MMC medical spend thanks to minimum MLR, actuarial soundness ii. More emphasis/value on health care quality iii.consistency across Medicaid, Medicare, commercial managed care Impact on health plans: Neutral to positive i. Actuarial soundness promotes adequate capitation rates ii. State-to-state consistency lessens burden on multi-state issuers Impact on states: Variable i. Potentially heavy transition burden on states w/ most developed MMC 39
40 Questions? Helaine Fingold Senior Counsel, Epstein Becker & Green Phone: Lynn Shapiro Snyder Senior Member of the Firm, Epstein Becker & Green Phone:
41 IV. Appendix 2016 Epstein Becker & Green, P.C. All Rights Reserved. ebglaw.com
42 IV. Appendix FEDERAL AUTHORITIES FOR MEDICAID MANAGED CARE DELIVERY Section 1915(a) of the Social Security Act (the SSA) Allows states to implement a voluntary managed care program State plan amendment (SPA) under section 1932 of the SSA Allows states to implement mandatory managed care program Does not allow for inclusion of dual eligibles, American Indians/Alaska Natives, or children with special health care needs Section 1915(b) of the SSA (waiver authority) Allows states to pursue a waiver to implement mandatory managed care, including for those excepted under a SPA Section 1115(a) of the SSA (waiver authority) Allows states to pursue waiver to implement mandatory managed care for all beneficiaries as part of a demonstration project State may request approval to provide services not typically covered by Medicaid 42
43 IV. Appendix PROVISIONS ELIGIBLE FOR WAIVER UNDER SSA 1915(b) & 1115 Statewideness (section 1902(a)(1) of the SSA) Waiver allows states to implement managed care in specific areas of the State (generally counties/parishes) rather than the entire state Comparability of Services (section 1902(a)(10) of the SSA) Waiver allows states to provide different benefits to beneficiaries enrolled in a managed care delivery system as compared to those in fee-for-service Medicaid Freedom of Choice (section 1902(a)(23)(A) of the SSA) Waiver allows states to require beneficiaries to receive their Medicaid services only from a managed care plan or primary care provider Allows for payment of costs not otherwise eligible under section 1903 of the SSA (Section 1115 only) 43
44 IV. Appendix PERCENTAGE OF MEDICAID POPULATION IN MCOS AK CA OR WA NV ID AZ UT MT WY NM HI CO ND SD NE N/A Source: Adapted from data from the Kaiser Family Foundation, Medicaid Reforms to Expand Coverage, Control Costs and Improve Care: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2015 and 2016, October 15, KS TX OK MN IA MO AR LA WI IL MS MI IN TN AL KY OH WV GA SC PA VT VA NC FL NY ME CT NJ DE MD DC NH RI MA 78% - 100% 63% - 77% 51% - 53% 9% - 21% 44
45 IV. Appendix PERCENTAGE OF MEDICAID POPULATION IN PCCMS WA OR NV CA ID AZ UT MT WY CO NM ND SD NE KS OK MN WI IA IL MO AR MS MI OH IN KY TN AL VT NY PA WV VA NC SC GA ME NH MA CT RI NJ DE MD DC AK TX LA FL 65% - 86% 58% - 64% 27% - 41% HI 1% - 21% Source: Adapted from data from the Kaiser Family Foundation, Medicaid Reforms to Expand Coverage, Control Costs and Improve Care: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2015 and 2016, October 15, N/A 45
46 IV. Appendix PERCENTAGE OF MEDICAID POPULATION IN FFS (NO COMPREHENSIVE MMC) WA OR NV CA ID AZ UT MT WY CO NM ND SD NE KS OK MN WI IA IL MO AR MS MI OH IN KY TN AL VT NY PA WV VA NC SC GA ME NH MA CT RI NJ DE MD DC AK TX LA FL 100% 50% - 51% 25% - 42% HI 0% - 23% Source: Adapted from data from the Kaiser Family Foundation, Medicaid Reforms to Expand Coverage, Control Costs and Improve Care: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2015 and 2016, October 15, N/A 46
Medicaid in an Era of Change: Findings from the Annual Kaiser 50 State Medicaid Budget Survey
 Medicaid in an Era of Change: Findings from the Annual Kaiser 50 State Medicaid Budget Survey Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family
Medicaid in an Era of Change: Findings from the Annual Kaiser 50 State Medicaid Budget Survey Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family
Alternative Paths to Medicaid Expansion
 Alternative Paths to Medicaid Expansion Robin Rudowitz Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation National Health Policy Forum March 28, 2014 Figure 1 The goal of the ACA
Alternative Paths to Medicaid Expansion Robin Rudowitz Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation National Health Policy Forum March 28, 2014 Figure 1 The goal of the ACA
Cost and Coverage Implications of the ACA Medicaid Expansion: National and State by State Analysis
 Cost and Coverage Implications of the ACA Medicaid Expansion: National and State by State Analysis Report Authors: John Holahan, Matthew Buettgens, Caitlin Carroll, and Stan Dorn Urban Institute November
Cost and Coverage Implications of the ACA Medicaid Expansion: National and State by State Analysis Report Authors: John Holahan, Matthew Buettgens, Caitlin Carroll, and Stan Dorn Urban Institute November
Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
The Impact of Health Reform s State Exchanges
 The Impact of Health Reform s State Exchanges May 2, 2013 Orlando, Florida Presented by: Layna S. Cook 225-381-7083 lcook@bakerdonelson.com The Affordable Care Act The Patient Protection and Affordable
The Impact of Health Reform s State Exchanges May 2, 2013 Orlando, Florida Presented by: Layna S. Cook 225-381-7083 lcook@bakerdonelson.com The Affordable Care Act The Patient Protection and Affordable
Medicaid Managed LTSS Updates from the States and the Feds
 Medicaid Managed LTSS Updates from the States and the Feds Rachel Patterson Christopher & Dana Reeve Foundation July 20, 2015 2015 Summer Leadership Institute Agenda Context: Rising health care costs and
Medicaid Managed LTSS Updates from the States and the Feds Rachel Patterson Christopher & Dana Reeve Foundation July 20, 2015 2015 Summer Leadership Institute Agenda Context: Rising health care costs and
Medicaid Expansion and Section 1115 Waivers
 Medicaid Expansion and Section 1115 Waivers Council of State Governments National Conference December 11, 2015 Figure 1 The goal of the ACA is to make coverage more available, more reliable, and more affordable.
Medicaid Expansion and Section 1115 Waivers Council of State Governments National Conference December 11, 2015 Figure 1 The goal of the ACA is to make coverage more available, more reliable, and more affordable.
The Medicaid Landscape
 The Medicaid Landscape Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation Council of State Governments Washington, DC June 18, 2014 Figure 1 Medicaid
The Medicaid Landscape Robin Rudowitz Associate Director, Kaiser Commission on Medicaid and the Uninsured Kaiser Family Foundation Council of State Governments Washington, DC June 18, 2014 Figure 1 Medicaid
Proposed Rule on Medicaid Managed Care: A Summary of Major Provisions
 Proposed Rule on Medicaid Managed Care: A Summary of Major Provisions Julia Paradise and MaryBeth Musumeci On June 1, 2015, the Centers for Medicare & Medicaid Services (CMS) published a Notice of Proposed
Proposed Rule on Medicaid Managed Care: A Summary of Major Provisions Julia Paradise and MaryBeth Musumeci On June 1, 2015, the Centers for Medicare & Medicaid Services (CMS) published a Notice of Proposed
Robin Rudowitz, Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family Foundation
 Medicaid Overview Robin Rudowitz, Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family Foundation Council of State Governments / Medicaid Leadership Policy Academy
Medicaid Overview Robin Rudowitz, Associate Director, Kaiser Commission on Medicaid and the Uninsured The Henry J. Kaiser Family Foundation Council of State Governments / Medicaid Leadership Policy Academy
ACA and Medicaid: Current Landscape and Future Outlook
 ACA and Medicaid: Current Landscape and Future Outlook RPCC Health Policy Forum Washington, DC December 5, 2017 Robin Rudowitz Associate Director, Program on Medicaid and the Uninsured Kaiser Family Foundation
ACA and Medicaid: Current Landscape and Future Outlook RPCC Health Policy Forum Washington, DC December 5, 2017 Robin Rudowitz Associate Director, Program on Medicaid and the Uninsured Kaiser Family Foundation
kaiser medicaid and the uninsured commission on
 kaiser commission on medicaid and the uninsured State Demonstrations to Integrate Care and Align Financing for Dual Eligible Beneficiaries: A Review of the 26 Proposals Submitted to CMS October 2012 1330
kaiser commission on medicaid and the uninsured State Demonstrations to Integrate Care and Align Financing for Dual Eligible Beneficiaries: A Review of the 26 Proposals Submitted to CMS October 2012 1330
Medicaid s Future. National PACE Association Spring Policy Forum. MaryBeth Musumeci
 Medicaid s Future National PACE Association Spring Policy Forum MaryBeth Musumeci March 20, 2017 Figure 2 The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
Medicaid s Future National PACE Association Spring Policy Forum MaryBeth Musumeci March 20, 2017 Figure 2 The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
States and Medicaid Provider Taxes or Fees
 March 2016 Fact Sheet States and Medicaid Provider Taxes or Fees Medicaid is jointly financed by states and the federal government. Provider taxes are an integral source of Medicaid financing governed
March 2016 Fact Sheet States and Medicaid Provider Taxes or Fees Medicaid is jointly financed by states and the federal government. Provider taxes are an integral source of Medicaid financing governed
PRODUCER ANNUITY SUITABILITY TRAINING REQUIREMENTS BY STATE As of September 11, 2017
 PRODUCER ANNUITY SUITABILITY TRAINING REQUIREMENTS BY STATE As of September 11, 2017 This document provides a summary of the annuity training requirements that agents are required to complete for each
PRODUCER ANNUITY SUITABILITY TRAINING REQUIREMENTS BY STATE As of September 11, 2017 This document provides a summary of the annuity training requirements that agents are required to complete for each
The Affordable Care Act (ACA)
 The Affordable Care Act (ACA) An Overview by the Kaiser Family Foundation NBC News Editorial Roundtable June 26, 2013 1. The Basics of the Affordable Care Act (ACA) Expanded Medicaid Coverage Starting
The Affordable Care Act (ACA) An Overview by the Kaiser Family Foundation NBC News Editorial Roundtable June 26, 2013 1. The Basics of the Affordable Care Act (ACA) Expanded Medicaid Coverage Starting
CHAPTER 1. Trends in the Overall Health Care Market
 CHAPTER 1 Trends in the Overall Health Care Market Billions Chart 1.1: Total National Health Expenditures, 1980 2016 $4,000 $3,500 $3,000 $2,500 $2,000 $1,500 $1,000 $500 $0 Inflation Adjusted (2) 80 81
CHAPTER 1 Trends in the Overall Health Care Market Billions Chart 1.1: Total National Health Expenditures, 1980 2016 $4,000 $3,500 $3,000 $2,500 $2,000 $1,500 $1,000 $500 $0 Inflation Adjusted (2) 80 81
kaiser medicaid and the uninsured commission on O L I C Y R I E F April 2012
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured April 2012 An Update on CMS s Capitated Financial Alignment Demonstration Model for Medicare-Medicaid Enrollees Executive Summary Beginning
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured April 2012 An Update on CMS s Capitated Financial Alignment Demonstration Model for Medicare-Medicaid Enrollees Executive Summary Beginning
Medicaid and CHIP Managed Care Final Rule (CMS-2390-F) Overview of the Final Rule. Center for Medicaid and CHIP Services
 Medicaid and CHIP Managed Care Final Rule (CMS-2390-F) Overview of the Final Rule Center for Medicaid and CHIP Services Background This final rule is the first update to Medicaid and CHIP managed care
Medicaid and CHIP Managed Care Final Rule (CMS-2390-F) Overview of the Final Rule Center for Medicaid and CHIP Services Background This final rule is the first update to Medicaid and CHIP managed care
Center for Medicare & Medicaid Services (CMS) Medicaid and CHIP Managed Care Final Rule (CMS 2390-F) Fact Sheet: Subpart B State Responsibilities
 Center for Medicare & Medicaid Services (CMS) Medicaid and CHIP Managed Care Final Rule (CMS 2390-F) Fact Sheet: Subpart B State Responsibilities Definition of Terms The final rule provides for a definition
Center for Medicare & Medicaid Services (CMS) Medicaid and CHIP Managed Care Final Rule (CMS 2390-F) Fact Sheet: Subpart B State Responsibilities Definition of Terms The final rule provides for a definition
1332 State Innovaton Waivers and the Exceutive Order on Insurance
 1332 State Innovaton Waivers and the Exceutive Order on Insurance December 10, 2017 San Diego NCSL Capitol Forum http://www.ncsl.org/default.aspx?tabid=30219 1 Presenters today: Kevin Lucia, JD Georgetown
1332 State Innovaton Waivers and the Exceutive Order on Insurance December 10, 2017 San Diego NCSL Capitol Forum http://www.ncsl.org/default.aspx?tabid=30219 1 Presenters today: Kevin Lucia, JD Georgetown
Older consumers and student loan debt by state
 August 2017 Older consumers and student loan debt by state New data on the burden of student loan debt on older consumers In January, the Bureau published a snapshot of older consumers and student loan
August 2017 Older consumers and student loan debt by state New data on the burden of student loan debt on older consumers In January, the Bureau published a snapshot of older consumers and student loan
Current Trends in the Medicaid RFP Procurement Landscape
 Current Trends in the Medicaid RFP Procurement Landscape This is a Presentation Subtitle PRESENTED BY: Michael Lutz Avalere Health October 31, 2017 About Us Michael Lutz Vice President mlutz@avalere.com
Current Trends in the Medicaid RFP Procurement Landscape This is a Presentation Subtitle PRESENTED BY: Michael Lutz Avalere Health October 31, 2017 About Us Michael Lutz Vice President mlutz@avalere.com
Presented by: Matt Turkstra
 Presented by: Matt Turkstra 1 » What s happening in Ohio?» How is health insurance changing? Individual and Group Health Insurance» Important employer terms» Impact small businesses that do not offer insurance?
Presented by: Matt Turkstra 1 » What s happening in Ohio?» How is health insurance changing? Individual and Group Health Insurance» Important employer terms» Impact small businesses that do not offer insurance?
Healthcare Reform. North Carolina Dietetic Association September 12, Duke Medicine
 Healthcare Reform North Carolina Dietetic Association September 12, 2014 Take home messages Healthcare [and health insurance] is transforming at an accelerating pace Key metrics of concern relate to quality,
Healthcare Reform North Carolina Dietetic Association September 12, 2014 Take home messages Healthcare [and health insurance] is transforming at an accelerating pace Key metrics of concern relate to quality,
Obamacare in Pictures. Visualizing the Effects of the Patient Protection and Affordable Care Act
 Visualizing the Effects of the Patient Protection and Affordable Care Act Fall 2012 expands dependence on government health care dumps millions into Medicaid and creates new federal subsidies for government-approved
Visualizing the Effects of the Patient Protection and Affordable Care Act Fall 2012 expands dependence on government health care dumps millions into Medicaid and creates new federal subsidies for government-approved
SCHIP: Let the Discussions Begin
 Figure 0 SCHIP: Let the Discussions Begin Diane Rowland, Sc.D. Executive Vice President, Henry J. Kaiser Family Foundation and Executive Director, Kaiser Commission on for Alliance for Health Reform February
Figure 0 SCHIP: Let the Discussions Begin Diane Rowland, Sc.D. Executive Vice President, Henry J. Kaiser Family Foundation and Executive Director, Kaiser Commission on for Alliance for Health Reform February
CMS Final Rule: Medicaid Managed Care The Medicaid Mega-Reg
 CMS Final Rule: Medicaid Managed Care The Medicaid Mega-Reg FaegreBD Consulting For Delta Dental Plans Association and National Association of Dental Plans October 2016 1 st Major Medicaid Managed Care
CMS Final Rule: Medicaid Managed Care The Medicaid Mega-Reg FaegreBD Consulting For Delta Dental Plans Association and National Association of Dental Plans October 2016 1 st Major Medicaid Managed Care
Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications
 Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications June 28, 2012 Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy In a 5-4 Decision,
Supreme Court Ruling on the Affordable Care Act (ACA): Overview & Implications June 28, 2012 Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy In a 5-4 Decision,
Issue brief: Medicaid managed care final rule
 Issue brief: Medicaid managed care final rule Overview In the past decade, the Medicaid managed care landscape has changed considerably in terms of the number of beneficiaries enrolled in managed care
Issue brief: Medicaid managed care final rule Overview In the past decade, the Medicaid managed care landscape has changed considerably in terms of the number of beneficiaries enrolled in managed care
Some Speech Titles Are Better Spoken Than Written. Hot Issues in Health Care December 5, 2017 Alan Weil Editor-in-Chief Health Affairs
 Some Speech Titles Are Better Spoken Than Written Hot Issues in Health Care December 5, 2017 Alan Weil Editor-in-Chief Health Affairs Because Whither: (adv) to what situation, position, degree or end Wither:
Some Speech Titles Are Better Spoken Than Written Hot Issues in Health Care December 5, 2017 Alan Weil Editor-in-Chief Health Affairs Because Whither: (adv) to what situation, position, degree or end Wither:
The State of Children s Health
 Figure 0 The State of Children s Health Robin Rudowitz Principal Policy Analyst Kaiser Commission on NCSL Annual Meeting Boston, MA August 8, 2007 Figure 1 SCHIP Builds on Medicaid for Children s Coverage
Figure 0 The State of Children s Health Robin Rudowitz Principal Policy Analyst Kaiser Commission on NCSL Annual Meeting Boston, MA August 8, 2007 Figure 1 SCHIP Builds on Medicaid for Children s Coverage
Medicaid 101 Damon Terzaghi Senior Director NASUAD
 Medicaid 101 Damon Terzaghi Senior Director NASUAD dterzaghi@nasuad.org www.nasuad.org Contents Overview & History of Medicaid How Medicaid is Administered Overview of Eligibility Overview of Services
Medicaid 101 Damon Terzaghi Senior Director NASUAD dterzaghi@nasuad.org www.nasuad.org Contents Overview & History of Medicaid How Medicaid is Administered Overview of Eligibility Overview of Services
An Update on Commercial Exchanges. Myra Weisfeld, Senior Managing Consultant
 An Update on Commercial Exchanges Myra Weisfeld, Senior Managing Consultant Agenda Introduction & overview ACA Changes to insurance coverage Insurance exchange update Summary & questions 2 3 4 Payment
An Update on Commercial Exchanges Myra Weisfeld, Senior Managing Consultant Agenda Introduction & overview ACA Changes to insurance coverage Insurance exchange update Summary & questions 2 3 4 Payment
The Lincoln National Life Insurance Company Term Portfolio
 The Lincoln National Life Insurance Company Term Portfolio State Availability as of 7/16/2018 PRODUCTS AL AK AZ AR CA CO CT DE DC FL GA GU HI ID IL IN IA KS KY LA ME MP MD MA MI MN MS MO MT NE NV NH NJ
The Lincoln National Life Insurance Company Term Portfolio State Availability as of 7/16/2018 PRODUCTS AL AK AZ AR CA CO CT DE DC FL GA GU HI ID IL IN IA KS KY LA ME MP MD MA MI MN MS MO MT NE NV NH NJ
CHARTPACK. Medicaid and its Role in State/Federal Budgets & Health Reform
 CHARTPACK Medicaid and its Role in State/Federal Budgets & Health Reform April 2013 Figure 1 #1: What is Medicaid and What Does it Do? Figure 2 Medicaid has many vital roles in our health care system.
CHARTPACK Medicaid and its Role in State/Federal Budgets & Health Reform April 2013 Figure 1 #1: What is Medicaid and What Does it Do? Figure 2 Medicaid has many vital roles in our health care system.
WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES CLASSIC PLAN WITH LOWER PLAN PREMIUMS
 PR Contact: IR Contact: H. Patel Jeff Potter CKPR WellCare Health Plans, Inc. (312) 616-2471 (813) 290-6313 hpatel@ckpr.biz jeff.potter@wellcare.com WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES
PR Contact: IR Contact: H. Patel Jeff Potter CKPR WellCare Health Plans, Inc. (312) 616-2471 (813) 290-6313 hpatel@ckpr.biz jeff.potter@wellcare.com WELLCARE WINS BID IN EVERY REGION FOR 2007 AND INTRODUCES
Medicare Alert: Temporary Member Access
 Medicare Alert: Temporary Member Access Plan Sponsor: Coventry/Aetna Medicare Part D Effective Date: Jan. 12, 2015 Geographic Area: National If your pharmacy is a Non Participating provider in the Aetna/Coventry
Medicare Alert: Temporary Member Access Plan Sponsor: Coventry/Aetna Medicare Part D Effective Date: Jan. 12, 2015 Geographic Area: National If your pharmacy is a Non Participating provider in the Aetna/Coventry
Report to Congressional Defense Committees
 Report to Congressional Defense Committees The Department of Defense Comprehensive Autism Care Demonstration December 2016 Quarterly Report to Congress In Response to: Senate Report 114-255, page 205,
Report to Congressional Defense Committees The Department of Defense Comprehensive Autism Care Demonstration December 2016 Quarterly Report to Congress In Response to: Senate Report 114-255, page 205,
Medicare Prescription Drug Congress. MMA and Medicaid. Gale Arden Director, Disabled & Elderly Health Programs Group CMSO CMS.
 Medicare Prescription Drug Congress MMA and Medicaid Gale Arden Director, Disabled & Elderly Health Programs Group CMSO CMS October 2005 Part D: Medicare Prescription Drug Coverage Effective: January 1,
Medicare Prescription Drug Congress MMA and Medicaid Gale Arden Director, Disabled & Elderly Health Programs Group CMSO CMS October 2005 Part D: Medicare Prescription Drug Coverage Effective: January 1,
Obamacare in Pictures
 Obamacare in Pictures VISUALIZING THE EFFECTS OF THE PATIENT PROTECTION AND AFFORDABLE CARE ACT Spring 2014 If you like your health care plan, can you really keep it? At least 4.7 million health care plans
Obamacare in Pictures VISUALIZING THE EFFECTS OF THE PATIENT PROTECTION AND AFFORDABLE CARE ACT Spring 2014 If you like your health care plan, can you really keep it? At least 4.7 million health care plans
Introducing LiveHealth Online
 Introducing LiveHealth Online Online Health Care when you need it! Meeting Members Wherever They Are 1 Why Consider Tele-Health? Convenience: Employees are able to access care at work, outside of traditional
Introducing LiveHealth Online Online Health Care when you need it! Meeting Members Wherever They Are 1 Why Consider Tele-Health? Convenience: Employees are able to access care at work, outside of traditional
Patient Protection & Affordable Care Act
 Patient Protection & Affordable Care Act Joshua D. Goldberg National Association of Insurance Commissioners Symposium on Health Reform University of Iowa Public Policy Center July 20, 2010 Opportunities
Patient Protection & Affordable Care Act Joshua D. Goldberg National Association of Insurance Commissioners Symposium on Health Reform University of Iowa Public Policy Center July 20, 2010 Opportunities
2016 Workers compensation premium index rates
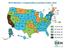 2016 Workers compensation premium index rates NH WA OR NV CA AK ID AZ UT MT WY CO NM MI VT ND MN SD WI NY NE IA PA IL IN OH WV VA KS MO KY NC TN OK AR SC MS AL GA TX LA FL ME MA RI CT NJ DE MD DC = Under
2016 Workers compensation premium index rates NH WA OR NV CA AK ID AZ UT MT WY CO NM MI VT ND MN SD WI NY NE IA PA IL IN OH WV VA KS MO KY NC TN OK AR SC MS AL GA TX LA FL ME MA RI CT NJ DE MD DC = Under
ehealth, Inc Fall Cost Report for Individual and Family Policyholders
 ehealth, Inc. 2010 Fall Cost Report for and Family Policyholders Table of Contents Page Methodology.................................................................. 2 ehealth, Inc. 2010 Fall Cost Report
ehealth, Inc. 2010 Fall Cost Report for and Family Policyholders Table of Contents Page Methodology.................................................................. 2 ehealth, Inc. 2010 Fall Cost Report
Local Anesthesia Administration by Dental Hygienists State Chart
 Education or AK 1981 General Both Specific Yes WREB 16 hrs didactic; 6 hrs ; 8 hrs lab AZ 1976 General Both Accredited Yes WREB 36 hrs; 9 types of AR 1995 Direct Both Accredited/ Board Approved No 16 hrs
Education or AK 1981 General Both Specific Yes WREB 16 hrs didactic; 6 hrs ; 8 hrs lab AZ 1976 General Both Accredited Yes WREB 36 hrs; 9 types of AR 1995 Direct Both Accredited/ Board Approved No 16 hrs
The Acquisition of Regions Insurance Group. April 6, 2018
 The Acquisition of Regions Insurance Group April 6, 2018 Forward-Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform
The Acquisition of Regions Insurance Group April 6, 2018 Forward-Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform
ACA Medicaid Primary Care Fee Bump: Context and Impact
 ACA Medicaid Primary Care Fee Bump: Context and Impact Stephen Zuckerman Senior Fellow and Co-director, Health Policy Center Presentation at UW Population Health Institute May 5, 2015 ACA Medicaid Fee
ACA Medicaid Primary Care Fee Bump: Context and Impact Stephen Zuckerman Senior Fellow and Co-director, Health Policy Center Presentation at UW Population Health Institute May 5, 2015 ACA Medicaid Fee
Florida s Medicaid Funding: A National Overview of Medicaid Waiver Trends
 Florida s Medicaid Funding: A National Overview of Medicaid Waiver Trends Joan Alker Executive Director Georgetown University Center for Children and Families Space Coast Health Foundation Melbourne, Florida
Florida s Medicaid Funding: A National Overview of Medicaid Waiver Trends Joan Alker Executive Director Georgetown University Center for Children and Families Space Coast Health Foundation Melbourne, Florida
Healthcare Reform Update
 Healthcare Reform Update Kim Holland Executive Director, State Affairs Health Insurance Exchange Summit West November 4, 013 150 Years of State Based Regulation States have been the primary regulator of
Healthcare Reform Update Kim Holland Executive Director, State Affairs Health Insurance Exchange Summit West November 4, 013 150 Years of State Based Regulation States have been the primary regulator of
IOM Workshop The Impact of the Affordable Care Act on U.S. Preparedness Resources and Programs
 IOM Workshop The Impact of the Affordable Care Act on U.S. Preparedness Resources and Programs Session I Opportunities and Challenges within Financing Changes Jack Ebeler Health Policy Alternatives, Inc.
IOM Workshop The Impact of the Affordable Care Act on U.S. Preparedness Resources and Programs Session I Opportunities and Challenges within Financing Changes Jack Ebeler Health Policy Alternatives, Inc.
Projected Savings of Medicaid Capitated Care: National and State-by-State. October 2015
 Projected Savings of Medicaid Capitated Care: National and State-by-State October 2015 I. Executive Summary We were asked by the Association for Community Affiliated Plans (ACAP) to estimate the Medicaid
Projected Savings of Medicaid Capitated Care: National and State-by-State October 2015 I. Executive Summary We were asked by the Association for Community Affiliated Plans (ACAP) to estimate the Medicaid
Marilyn Tavenner, CMS Administrator Don Moulds, Acting Assistant Secretary for Planning and Evaluation
 TO: The Secretary Through: DS COS ES FROM: Marilyn Tavenner, CMS Administrator Don Moulds, Acting Assistant Secretary for Planning and Evaluation DATE: September 5, 2013 SUBJECT: Projected Monthly Targets
TO: The Secretary Through: DS COS ES FROM: Marilyn Tavenner, CMS Administrator Don Moulds, Acting Assistant Secretary for Planning and Evaluation DATE: September 5, 2013 SUBJECT: Projected Monthly Targets
Health Insurance Exchanges and the Changing Marketplace. Leanne Gassaway, MHA Regional Vice President West Region, State Advocacy July 31, 2013
 Health Insurance Exchanges and the Changing Marketplace Leanne Gassaway, MHA Regional Vice President West Region, State Advocacy July 31, 2013 End Goal An Efficient, Effective, Competitive and Robust Health
Health Insurance Exchanges and the Changing Marketplace Leanne Gassaway, MHA Regional Vice President West Region, State Advocacy July 31, 2013 End Goal An Efficient, Effective, Competitive and Robust Health
CMS s 2018 Proposed Medicaid Managed Care Rule: A Summary of Major Provisions
 January 2019 Issue Brief CMS s 2018 Proposed Medicaid Managed Care Rule: A Summary of Major Provisions Elizabeth Hinton and MaryBeth Musumeci Executive Summary Managed care is the predominant Medicaid
January 2019 Issue Brief CMS s 2018 Proposed Medicaid Managed Care Rule: A Summary of Major Provisions Elizabeth Hinton and MaryBeth Musumeci Executive Summary Managed care is the predominant Medicaid
Florida 1/1/2016 Workers Compensation Rate Filing
 Florida 1/1/2016 Workers Compensation Rate Filing Kirt Dooley, FCAS, MAAA October 21, 2015 1 $ Billions 4.0 3.5 3.0 2.5 2.0 1.5 1.0 0.5 0.0 Florida s Workers Compensation Premium Volume 2.368 0.765 0.034
Florida 1/1/2016 Workers Compensation Rate Filing Kirt Dooley, FCAS, MAAA October 21, 2015 1 $ Billions 4.0 3.5 3.0 2.5 2.0 1.5 1.0 0.5 0.0 Florida s Workers Compensation Premium Volume 2.368 0.765 0.034
medicaid a n d t h e How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief
 on medicaid a n d t h e uninsured July 2012 How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief Effective January 2014, the ACA establishes a new minimum Medicaid
on medicaid a n d t h e uninsured July 2012 How will the Medicaid Expansion for Adults Impact Eligibility and Coverage? Key Findings in Brief Effective January 2014, the ACA establishes a new minimum Medicaid
Exhibit 1. The Impact of Health Reform: Percent of Women Ages Uninsured by State
 Exhibit 1. The Impact of Health Reform: Percent of Women Ages 19 64 Uninsured by State 2008 09 2019 (estimated) OR CA 23% WA NV 23% AK ID AZ UT MT WY CO NM 28% ND SD NE KS TX 31% OK MN IA MO WI AR 25%
Exhibit 1. The Impact of Health Reform: Percent of Women Ages 19 64 Uninsured by State 2008 09 2019 (estimated) OR CA 23% WA NV 23% AK ID AZ UT MT WY CO NM 28% ND SD NE KS TX 31% OK MN IA MO WI AR 25%
National Network Trends
 National Network Trends Katherine Hempstead, PhD Senior Advisor Robert Wood Johnson Foundation Tiered and Narrow Networks, the New Frontier in Health Insurance: Implications for New Jersey s Regulatory
National Network Trends Katherine Hempstead, PhD Senior Advisor Robert Wood Johnson Foundation Tiered and Narrow Networks, the New Frontier in Health Insurance: Implications for New Jersey s Regulatory
How to Assist Beneficiaries Impacted by Aetna/Coventry 2015 Part D Plans
 **SPECIAL ALERT** How to Assist Beneficiaries Impacted by Aetna/Coventry 2015 Part D Plans Due to inaccurate information posted about in-network pharmacies and cost-sharing for certain Aetna/Coventry Part
**SPECIAL ALERT** How to Assist Beneficiaries Impacted by Aetna/Coventry 2015 Part D Plans Due to inaccurate information posted about in-network pharmacies and cost-sharing for certain Aetna/Coventry Part
kaiser medicaid and the uninsured commission on The Cost and Coverage Implications of the ACA Medicaid Expansion: National and State-by-State Analysis
 kaiser commission on medicaid and the uninsured The Cost and Coverage Implications of the ACA Expansion: National and State-by-State Analysis Executive Summary John Holahan, Matthew Buettgens, Caitlin
kaiser commission on medicaid and the uninsured The Cost and Coverage Implications of the ACA Expansion: National and State-by-State Analysis Executive Summary John Holahan, Matthew Buettgens, Caitlin
TCJA and the States Responding to SALT Limits
 TCJA and the States Responding to SALT Limits Kim S. Rueben Tuesday, January 29, 2019 1 What does this mean for Individuals under TCJA About two-thirds of taxpayers will receive a tax cut with the largest
TCJA and the States Responding to SALT Limits Kim S. Rueben Tuesday, January 29, 2019 1 What does this mean for Individuals under TCJA About two-thirds of taxpayers will receive a tax cut with the largest
In addition, MCHCP is requesting information about any programs or plans in place for non-medicare retirees.
 Missouri Consolidated Health Care Plan 832 Weathered Rock Court PO Box 104355 Jefferson City, MO 65110 Phone: 800-701-8881 www.mchcp.org Judith Muck, Executive Director February 7, 2018 To: From: Regarding:
Missouri Consolidated Health Care Plan 832 Weathered Rock Court PO Box 104355 Jefferson City, MO 65110 Phone: 800-701-8881 www.mchcp.org Judith Muck, Executive Director February 7, 2018 To: From: Regarding:
How is the Affordable Care Act Leading to Changes in Medicaid Today? State Adoption of Five New Options
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured How is the Affordable Care Act Leading to Changes in Medicaid Today? State Adoption of Five New Options May 2012 One primary goal of
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured How is the Affordable Care Act Leading to Changes in Medicaid Today? State Adoption of Five New Options May 2012 One primary goal of
James G. Anderson, Ph.D. Purdue University
 Health Care Reform: Its Impact and Future Directions James G. Anderson, Ph.D. Purdue University Andersonj@purdue.edu Health Care System Models Models Other Countries United States Bismark Beveridge National
Health Care Reform: Its Impact and Future Directions James G. Anderson, Ph.D. Purdue University Andersonj@purdue.edu Health Care System Models Models Other Countries United States Bismark Beveridge National
The State Tax Implications of Federal Tax Reform Legislation
 The State Tax Implications of Federal Tax Reform Legislation Executive Committee Task Force on State and Local Taxation Phoenix, Arizona January 14, 2017 Joe Crosby, Multistate Associates Karl Frieden,
The State Tax Implications of Federal Tax Reform Legislation Executive Committee Task Force on State and Local Taxation Phoenix, Arizona January 14, 2017 Joe Crosby, Multistate Associates Karl Frieden,
Q INVESTOR PRESENTATION. May 4, 2018
 Q 208 INVESTOR PRESENTATION May 4, 208 DISCLAIMERS FORWARD-LOOKING STATEMENTS. The financial results in this presentation reflect preliminary unaudited results, which are not final until Form 0-Q for the
Q 208 INVESTOR PRESENTATION May 4, 208 DISCLAIMERS FORWARD-LOOKING STATEMENTS. The financial results in this presentation reflect preliminary unaudited results, which are not final until Form 0-Q for the
Percent of Employees Waiving Coverage 27.0% 30.6% 29.1% 23.4% 24.9%
 Number of Health Plans Reported 18,186 3,561 681 2,803 3,088 Offer HRA or HSA 34.0% 42.7% 47.0% 39.7% 35.0% Annual Employer Contribution $1,353 $1,415 $1,037 $1,272 $1,403 Percent of Employees Waiving
Number of Health Plans Reported 18,186 3,561 681 2,803 3,088 Offer HRA or HSA 34.0% 42.7% 47.0% 39.7% 35.0% Annual Employer Contribution $1,353 $1,415 $1,037 $1,272 $1,403 Percent of Employees Waiving
A Blue Cross and Blue Shield Association Presentation
 A Blue Cross and Blue Shield Association Presentation Issues in Healthcare Reform CSG Spring Conference Health Policy Task Force Joan Gardner Executive Director, State Services May 17, 2009 Healthcare
A Blue Cross and Blue Shield Association Presentation Issues in Healthcare Reform CSG Spring Conference Health Policy Task Force Joan Gardner Executive Director, State Services May 17, 2009 Healthcare
Subpart D MCO, PIHP and PAHP Standards Availability of services.
 Center for Medicare & Medicaid Services (CMS) Medicaid and CHIP Managed Care Final Rule (CMS 2390-F) Fact Sheet: Subpart D and E of 438 Quality of Care Each state must ensure that all services covered
Center for Medicare & Medicaid Services (CMS) Medicaid and CHIP Managed Care Final Rule (CMS 2390-F) Fact Sheet: Subpart D and E of 438 Quality of Care Each state must ensure that all services covered
Florida s Medicaid Choice: Options and Implications
 Florida s Medicaid Choice: Options and Implications Joan Alker Georgetown University Health Policy Institute Florida Philanthropic Network, Tallahassee, FL February 19, 2013 Florida vs. U.S.! Uninsured
Florida s Medicaid Choice: Options and Implications Joan Alker Georgetown University Health Policy Institute Florida Philanthropic Network, Tallahassee, FL February 19, 2013 Florida vs. U.S.! Uninsured
Comparative Revenues and Revenue Forecasts Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas
 Comparative Revenues and Revenue Forecasts 2010-2014 Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas Comparative Revenues and Revenue Forecasts This data shows tax
Comparative Revenues and Revenue Forecasts 2010-2014 Prepared By: Bureau of Legislative Research Fiscal Services Division State of Arkansas Comparative Revenues and Revenue Forecasts This data shows tax
2016 GEHA. dental. FEDVIP Plans. let life happen. gehadental.com
 2016 GEHA dental FEDVIP Plans let life happen gehadental.com Smile, you re covered, with great benefits and a large national network. High maximum benefits $25,000 for High Option Growing network of dentists
2016 GEHA dental FEDVIP Plans let life happen gehadental.com Smile, you re covered, with great benefits and a large national network. High maximum benefits $25,000 for High Option Growing network of dentists
Property Tax Relief in New England
 Property Tax Relief in New England January 23, 2015 Adam H. Langley Senior Research Analyst Lincoln Institute of Land Policy www.lincolninst.edu Property Tax as a % of Personal Income OK AL IN UT SD MS
Property Tax Relief in New England January 23, 2015 Adam H. Langley Senior Research Analyst Lincoln Institute of Land Policy www.lincolninst.edu Property Tax as a % of Personal Income OK AL IN UT SD MS
Medicaid & CHIP Managed Care: Looking at the Rule through a Children s Lens June 17, Tricia Brooks Sarah Somers Kelly Whitener
 Medicaid & CHIP Managed Care: Looking at the Rule through a Children s Lens June 17, 2016 Tricia Brooks Sarah Somers Kelly Whitener INTRODUCTION Tricia Brooks 2 Children in Managed Care o CMS finalized
Medicaid & CHIP Managed Care: Looking at the Rule through a Children s Lens June 17, 2016 Tricia Brooks Sarah Somers Kelly Whitener INTRODUCTION Tricia Brooks 2 Children in Managed Care o CMS finalized
Unemployment Insurance Benefit Adequacy: How many? How much? How Long?
 Unemployment Insurance Benefit Adequacy: How many? How much? How Long? Joel Sacks, Deputy Commissioner Washington State Employment Security Department March 1, 2012 1 Outline How many get unemployment
Unemployment Insurance Benefit Adequacy: How many? How much? How Long? Joel Sacks, Deputy Commissioner Washington State Employment Security Department March 1, 2012 1 Outline How many get unemployment
NCSL Spring Forum NCSL Task Force on Federal Health Reform Implementation May 4, 2013
 NCSL Spring Forum NCSL Task Force on Federal Health Reform Implementation May 4, 2013 Laura Tobler, National Conference of State Legislatures, laura.tobler@ncsl.org, Optional Medicaid Expansion The ACA
NCSL Spring Forum NCSL Task Force on Federal Health Reform Implementation May 4, 2013 Laura Tobler, National Conference of State Legislatures, laura.tobler@ncsl.org, Optional Medicaid Expansion The ACA
Frequently Asked Questions on Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS) 2015 Medicare Payment Final Rules (CMS-1614-F)
 Frequently Asked Questions on Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS) 2015 Medicare Payment Final Rules (CMS-1614-F) Adjusting DMEPOS Payment Amounts Using Competitive
Frequently Asked Questions on Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS) 2015 Medicare Payment Final Rules (CMS-1614-F) Adjusting DMEPOS Payment Amounts Using Competitive
Medicaid 1915(c) Home and Community-Based Service Programs: Data Update
 Medicaid 1915(c) Home and Community-Based Service Programs: Data Update OVERVIEW December 2006 Developing home and community-based service (HCBS) alternatives to institutional care has been a priority
Medicaid 1915(c) Home and Community-Based Service Programs: Data Update OVERVIEW December 2006 Developing home and community-based service (HCBS) alternatives to institutional care has been a priority
Medicare Part D Prescription Drug Benefit For Agent Use Only
 MEMORANDUM Date: October 20, 2006 To: First UA Part D Licensed Agents From: First UA Sales Department Medicare Part D Prescription Drug Benefit For Agent Use Only Introduction The Medicare Modernization
MEMORANDUM Date: October 20, 2006 To: First UA Part D Licensed Agents From: First UA Sales Department Medicare Part D Prescription Drug Benefit For Agent Use Only Introduction The Medicare Modernization
Stand-Alone Prescription Drug Plans Dominated the Rural Market in 2011
 Stand-Alone Prescription Drug Plans Dominated the Rural Market in 2011 Growth Driven by Medicare Advantage Prescription Drug Plan Enrollment Leah Kemper, MPH Abigail Barker, PhD Fred Ullrich, BA Lisa Pollack,
Stand-Alone Prescription Drug Plans Dominated the Rural Market in 2011 Growth Driven by Medicare Advantage Prescription Drug Plan Enrollment Leah Kemper, MPH Abigail Barker, PhD Fred Ullrich, BA Lisa Pollack,
Health Reform & Immuniza3ons in 2014
 Health Reform & Immuniza3ons in 2014 Associa(on of Immuniza(on Managers Atlanta, Georgia Alexandra Stewart stewarta@gwu.edu Milken Ins(tute, School of Public Health, Department of Health Policy, GWU July
Health Reform & Immuniza3ons in 2014 Associa(on of Immuniza(on Managers Atlanta, Georgia Alexandra Stewart stewarta@gwu.edu Milken Ins(tute, School of Public Health, Department of Health Policy, GWU July
ANALYSIS OF THE IMPACTS OF THE ACA S TAX ON HEALTH INSURANCE IN 2018 AND BEYOND - REVISED
 ANALYSIS OF THE IMPACTS OF THE ACA S TAX ON HEALTH INSURANCE IN 2018 AND BEYOND - REVISED CHRIS CARLSON, FSA, MAAA GLENN GIESE, FSA, MAAA STEVEN ARMSTRONG, ASA, MAAA OCTOBER 10, 2017 ACA's Tax on Health
ANALYSIS OF THE IMPACTS OF THE ACA S TAX ON HEALTH INSURANCE IN 2018 AND BEYOND - REVISED CHRIS CARLSON, FSA, MAAA GLENN GIESE, FSA, MAAA STEVEN ARMSTRONG, ASA, MAAA OCTOBER 10, 2017 ACA's Tax on Health
The Challenging but Promising Environment for LTC Insurance. Susan Coronel, America s Health Insurance Plans
 The Challenging but Promising Environment for LTC Insurance Susan Coronel, America s Health Insurance Plans Agenda NAIC LTCI Structure & Responsibilities Interstate Compact State Level What We Need to
The Challenging but Promising Environment for LTC Insurance Susan Coronel, America s Health Insurance Plans Agenda NAIC LTCI Structure & Responsibilities Interstate Compact State Level What We Need to
Medicare Modernization Act and Medicare Part D: Status of Implementation
 Medicare Modernization Act and Medicare Part D: Status of Implementation November 1, 2005 John Richardson Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy What
Medicare Modernization Act and Medicare Part D: Status of Implementation November 1, 2005 John Richardson Avalere Health LLC Avalere Health LLC The intersection of business strategy and public policy What
Patient Protection and. Affordable Care Act: The Impact on Employers
 Patient Protection and Affordable Care Act: The Impact on Employers April 2013 Agenda Introductions Individual Mandate Healthcare Exchange Overview Impact on Employers Essential Health Benefits Fees &
Patient Protection and Affordable Care Act: The Impact on Employers April 2013 Agenda Introductions Individual Mandate Healthcare Exchange Overview Impact on Employers Essential Health Benefits Fees &
Implementing the Medicare Drug Benefit. Robert Donnelly Director, Medicare Drug Benefit Group June 8, 2005
 Implementing the Medicare Drug Benefit Robert Donnelly Director, Medicare Drug Benefit Group June 8, 2005 Medicare Challenges Providing the best care for a Medicare population that has longer life expectancy
Implementing the Medicare Drug Benefit Robert Donnelly Director, Medicare Drug Benefit Group June 8, 2005 Medicare Challenges Providing the best care for a Medicare population that has longer life expectancy
INTERIM SUMMARY REPORT ON RISK ADJUSTMENT FOR THE 2016 BENEFIT YEAR
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Center for Consumer Information and Insurance Oversight 200 Independence Avenue SW Washington, DC 20201 INTERIM SUMMARY REPORT
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Center for Consumer Information and Insurance Oversight 200 Independence Avenue SW Washington, DC 20201 INTERIM SUMMARY REPORT
Value Choice. Summary of Benefits. January 1 December 31, 2014 S5660 & S5983. Y0046_B00SNS4B Accepted
 Value Choice Summary of Benefits January 1 December 31, 2014 S5660 & S5983 Y0046_B00SNS4B Accepted B00SNS4P Introduction to Summary of Benefits Thank you for your interest in Express Scripts Medicare (PDP).
Value Choice Summary of Benefits January 1 December 31, 2014 S5660 & S5983 Y0046_B00SNS4B Accepted B00SNS4P Introduction to Summary of Benefits Thank you for your interest in Express Scripts Medicare (PDP).
State Treatment of Social Security Treatment of Pension Income Other Income Tax Breaks Property Tax Breaks
 State-By-State Tax Breaks for Seniors, 2016 State Treatment of Social Security Treatment of Pension Income Other Income Tax Breaks Property Tax Breaks AL Payments from defined benefit private plans are
State-By-State Tax Breaks for Seniors, 2016 State Treatment of Social Security Treatment of Pension Income Other Income Tax Breaks Property Tax Breaks AL Payments from defined benefit private plans are
The Economic Stimulus and Health Chairs
 The Economic Stimulus and Health Chairs Friday, April 17, 2009, 2:00 pm EDT A partnership between the Kaiser Family Foundation and the NCSL Health Chairs Project Moderators: Donna Folkemer, Group Director,
The Economic Stimulus and Health Chairs Friday, April 17, 2009, 2:00 pm EDT A partnership between the Kaiser Family Foundation and the NCSL Health Chairs Project Moderators: Donna Folkemer, Group Director,
Getting Better Value for the Healthcare Dollar. National Conference of State Legislators Fall Forum November 30, 2011.
 Getting Better Value for the Healthcare Dollar National Conference of State Legislators Fall Forum November 30, 2011 NCQA History NCQA a non-profit that for 21 years has worked with federal, state, consumer
Getting Better Value for the Healthcare Dollar National Conference of State Legislators Fall Forum November 30, 2011 NCQA History NCQA a non-profit that for 21 years has worked with federal, state, consumer
Rural Policy Brief Volume 10, Number 8 (PB ) April 2006 RUPRI Center for Rural Health Policy Analysis
 Rural Policy Brief Volume 10, Number 8 (PB2006-8 ) April 2006 RUPRI Center for Rural Health Policy Analysis Medicare Part D: Early Findings on Enrollment and Choices for Rural Beneficiaries Authors: Timothy
Rural Policy Brief Volume 10, Number 8 (PB2006-8 ) April 2006 RUPRI Center for Rural Health Policy Analysis Medicare Part D: Early Findings on Enrollment and Choices for Rural Beneficiaries Authors: Timothy
ANALYSIS OF THE IMPACTS OF THE ACA S TAX ON HEALTH INSURANCE IN YEAR 2020 AND LATER
 ANALYSIS OF THE IMPACTS OF THE ACA S TAX ON HEALTH INSURANCE IN YEAR 2020 AND LATER CHRIS CARLSON, FSA, MAAA GLENN GIESE, FSA, MAAA THOMAS SAUDER, ASA, MAAA AUGUST 28, 2018 ACA's Tax on Health Insurers
ANALYSIS OF THE IMPACTS OF THE ACA S TAX ON HEALTH INSURANCE IN YEAR 2020 AND LATER CHRIS CARLSON, FSA, MAAA GLENN GIESE, FSA, MAAA THOMAS SAUDER, ASA, MAAA AUGUST 28, 2018 ACA's Tax on Health Insurers
MARKET TRENDS: MEDICARE SUPPLEMENT. Gorman Health Group, LLC
 MARKET TRENDS: MEDICARE SUPPLEMENT Gorman Health Group, LLC Issued: December 1, 2016 TABLE OF CONTENTS EXECUTIVE SUMMARY... 3 OVERALL TRENDS IN MEDICARE SUPPLEMENT ENROLLMENT... 4 NATIONWIDE ENROLLMENT...
MARKET TRENDS: MEDICARE SUPPLEMENT Gorman Health Group, LLC Issued: December 1, 2016 TABLE OF CONTENTS EXECUTIVE SUMMARY... 3 OVERALL TRENDS IN MEDICARE SUPPLEMENT ENROLLMENT... 4 NATIONWIDE ENROLLMENT...
Taxing Investment Income in the States New Hampshire Fiscal Policy Institute 2 nd Annual Budget and Policy Conference Concord, NH January 23, 2015
 Taxing Investment Income in the States New Hampshire Fiscal Policy Institute 2 nd Annual Budget and Policy Conference Concord, NH January 23, 2015 Norton Francis State and Local Finance Initiative Urban-Brookings
Taxing Investment Income in the States New Hampshire Fiscal Policy Institute 2 nd Annual Budget and Policy Conference Concord, NH January 23, 2015 Norton Francis State and Local Finance Initiative Urban-Brookings
Charles Gullickson (Penn Treaty/ANIC Task Force Chair), Richard Klipstein (NOLHGA)
 MEMO DATE: TO: Charles Gullickson (Penn Treaty/ANIC Task Force Chair), Richard Klipstein (NOLHGA) FROM: Vincent L. Bodnar, ASA, MAAA RE: Penn Treaty Network American Insurance Company and American Network
MEMO DATE: TO: Charles Gullickson (Penn Treaty/ANIC Task Force Chair), Richard Klipstein (NOLHGA) FROM: Vincent L. Bodnar, ASA, MAAA RE: Penn Treaty Network American Insurance Company and American Network
State Trust Fund Solvency
 Unemployment Insurance State Trust Fund Solvency National Employment Law Project Conference - Washington DC December 7, 2009 Robert Pavosevich pavosevich.robert@dol.gov Unemployment Insurance Program
Unemployment Insurance State Trust Fund Solvency National Employment Law Project Conference - Washington DC December 7, 2009 Robert Pavosevich pavosevich.robert@dol.gov Unemployment Insurance Program
Medicaid Funding and Policies Is There a Medicaid Crisis? A Financial Diagnosis for State and Local Government
 Medicaid Funding and Policies Is There a Medicaid Crisis? A Financial Diagnosis for State and Local Government Matt Powers Health Management Associates March 15, 2007 Main Points Medicaid Remains a Workhorse
Medicaid Funding and Policies Is There a Medicaid Crisis? A Financial Diagnosis for State and Local Government Matt Powers Health Management Associates March 15, 2007 Main Points Medicaid Remains a Workhorse
Please print using blue or black ink. Please keep a copy for your records and send completed form to the following address.
 20 Disbursement for Beneficiary/QDRO Account IBEW Local Union No. 716 Retirement Plan Instructions About You Please print using blue or black ink. Please keep a copy for your records and send completed
20 Disbursement for Beneficiary/QDRO Account IBEW Local Union No. 716 Retirement Plan Instructions About You Please print using blue or black ink. Please keep a copy for your records and send completed
