aligning managed care contracts, compensation plans, and incentive models
|
|
|
- Ami Thornton
- 5 years ago
- Views:
Transcription
1 REPRINT NOVEMBER 2011 Michael E. Nugent healthcare financial management association aligning managed care contracts, compensation plans, and incentive models Providers should take the lead to align their organization s internal and external payment models with the basic tenets of payment reform. AT A GLANCE > Today s pure production-based compensation and incentive models are lagging behind new, third-party, value based payment models, such as shared savings, bundled payments, and pay for performance. > Financial executives are struggling with the emerging disconnects between new, external payment models and traditional methods providers use to distribute funds internally. > To begin to align internal payment models with emerging third-party payment models, providers should inventory the misaligned incentives within their own organizations, engage their physicians and payers in a dialogue on what needs to be paid and how, and learn from past mistakes. > No perfect payment distribution model exists. Rather, providers should choose a best-fit model based on their market position, culture, and readiness for change. > Ultimately, finance executives should take the lead in aligning their organization s internal and external payment models. Providers of all sizes are exploring a variety of new third-party payment models with public and private payers. These models have significant implications not just for providers revenue streams, but also for how they structure physician compensation and incentives. Mindful of this proliferation of new payment models, providers will need to be much more assertive and selective about how and what they want to be paid by CMS and commercial payers. The days of automatic 6 to 8 percent commercial rate increases are numbered. Likewise, providers will need to be more deliberate about how they move beyond traditional compensation and incentive formulas that reward only physician production and tenure. For example, providers will need to explore new models that specify minimum performance standards, penalize noncompliance with standards, and reward results related to service, access, satisfaction, and efficiency improvements. They also should ask a number of internal and external payment design questions: > What are the organization s ultimate performance-improvement metrics and goals, by service, provider, group, and population? > Where do current incentives get in the way of these goals? > What is the base salary target for physicians (e.g., 80 percent of the market median)? > What is the maximum upside bonus versus downside risk potential (e.g., 0 to 25 percent of market median salary)? > How should internal and external payment models align so that income isn t simply redistributed to politically powerful stakeholders, but instead results in improved patient quality, service, and affordability? > What direct investments will be made in infrastructure, data, and care management to improve practice efficiency (e.g., $100,000/physician)? 1 NOVEMBER 2011 healthcare financial management
2 > What are the bonus distribution percentages (e.g., 67 percent to primary care, 33 percent to specialists)? This new mindset is a far cry from the current purely production-based compensation and incentive practices summarized in the table below. Finance, managed care, clinical improvement, and physician executives will play pivotal roles in aligning their third-party contract terms with internal compensation, bonus, and loss distribution models. Unfortunately, there is no instruction manual or tool to automatically align external and internal payment models. So to assist finance, managed care, clinical improvement, and physician executives in their journey, we tackle three of the more common questions we observe as providers transition from a volume-based payment system to a value-based payment system: > What problems are arising with compensation and incentive models as third-party managed care contracts become more performance-based? > What types of internal and external payment alignment models are working and where? > What are some early lessons learned from organizations on the cutting edge of new payment models? External and Internal Payment Models: Emerging Problems At least three tangible problems are emerging with internal compensation and incentive models as third-party contracts become more performance-based: insufficient funding sources, inadequate incentive levels, and a focus that considers compensation before patient concerns. Insufficient funding sources. Many of the nation s largest health systems and hospitals are compensating physicians at above-market rates. These large systems have been able to pay above-market rates because they have negotiated above-market commercial payment rates with private payers. Providers will need to be more deliberate about how they move beyond traditional compensation and incentive formulas that reward only physician production and tenure. But as payers and regulators begin to reduce unit payment on high-margin imaging, procedural, and lab services and scrutinize hospital directorship and management fees to physicians, the funding sources for physician compensation and incentives are expected to stagnate, if not decrease. Consequently, hospitals and physicians should acknowledge the potential for fewer dollars and the need to evolve their approach to compensation and incentives. Inadequate incentive levels. How much incentive is enough to change hospital and physician behavior? Historically, researchers have reported that physicians experienced less conflict of interest when less than 10 percent of their incomes was at risk of not materializing. When more than 20 percent of physician incomes was at risk, the conflict of interest was greater. In between 10 and 20 percent, experience was mixed (Pearson, S.D., Sabin, J.E., and Emmanuel, E.J., Ethical Guidelines for Physician Compensation TRAJECTORY OF PROVIDER PAYMENT MODELS Percentage of Practices Using These Metrics 2000 Survey 2010 Survey Gross Charges 24.9% 21.0% Adjusted Charges 15.5% 13.4% Net Collections 56.7% 38.9% Patient Encounters 11.13% 7.1% Patient Panel Size 3.41% 3.5% Relative Value Units 17.25% 60.6% Source: Medical Group Management Association. hfma.org NOVEMBER
3 Based on Capitation, New England Journal of Medicine, Sept. 3, 1998). Recent research shows that a small percentage (generally 0 to 5 percent) of physician incomes is at risk for quality and service performance under most providers current internal compensation and incentive arrangements. However, the same research indicates most large health systems envision that 10 to 20 percent of physician incentives will be at risk in the future. So in addition to acknowledging the compensation funding gap, providers need to rethink how much incentive will be necessary to influence behavior change in their organization. For one recent multispecialty group, a $20,000 to $30,000 annual bonus potential for each primary care physician, coupled with a payer-direct investment in physician practice variation reports and a case manager, was critical to achieving that organization s goals. Focus that considers compensation before patient concerns. Patients interests can become secondary issues during controversial, politically charged managed care, compensation, and incentive alignment negotiations. Consequently, pure production-based compensation and incentive models (e.g., ones paid on relative value units the physician produces) still thrive today, that reward any volume, regardless of whether care is necessary or avoidable and regardless of the impact on patient out-of-pocket cost sharing. Providers can make matters worse by negotiating the greatest payment increases on services they expect to generate the most volume growth, Emerging Performance-Based Payment Models Both the Centers for Medicare & Medicaid Services (CMS), with the issuance of the Medicare Bundled Payments for Care Improvement Initiative, and commercial payers are exploring performance-based payment models that involve, to a great extent, bundled payments. Commercial Payers Among the emerging payment models used with commercial payers, such as Blue Cross and Blue Shield plans, are: > Advanced pay-for-performance models that tie providers pay raises and bonuses to achieving efficiency goals > Bundled facility and professional payment models for acute inpatient care > Bundled payment models for care of chronic conditions across the inpatient and outpatient spectrum Advanced pay-for-performance models. In these models, payers tie providers future pay raises and/or bonuses to performance metrics. These metrics have been evolving beyond traditional process metrics (e.g., vaccination rates) to efficiency-oriented metrics (e.g., generic prescribing rate, readmission rate, and expected versus actual expenditures), which all but guarantee some reduction in utilization and/or unit cost for the payer. If providers fail to achieve the negotiated performance improvements, they will leave money on the table. It s not uncommon for providers to leave up to 50 percent of the bonus potential on the table, depending on the metrics they negotiate with payers. Facility and professional bundled payment for acute inpatient services, including hearts, hips, knees, and backs. Providers are expending significant effort to design inpatient payment bundles in response to requests from CMS and commercial payers. These bundles combine hospital and physician reimbursement into one payment to cover services within some time span before and/or after the admission. Hospitals use these bundles to attract physician referrals by sharing cost savings (e.g., supply standardization savings) and utilization savings (e.g., reductions in unnecessary days or steerage of patients to lower cost sites of care) with physicians who use the hospital the most. But hospitals are struggling with whether and how to align their physician compensation and incentive programs with these new bundled payment options. 3 NOVEMBER 2011 healthcare financial management
4 regardless of whether such growth is clinically necessary. Furthermore, most incentive and bonus dollars are typically distributed to hospitals and physicians, not to patients. Only a few organizations surveyed transparently invest a portion of their bonuses in programs that improve future access, efficiency, and service. Consequently, underlying performance improvements may not be sustained, costs escalate after small decreases, and patients foot a larger percentage of their ever increasing bills. So mindful of emerging third-party payment models and their inherent disconnects, providers need to devise a strategy to align their internal compensation, incentive, and investment models with emerging, value-based contracting terms. Unfortunately, many providers are opting for a standard approach to resolve a short-term emergency without a thoughtful analysis of market competitors, immediate priorities, and long-term goals. Considerable caution and time are necessary as providers attempt to align their internal compensation, incentive, and investment models with emerging third-party payment models. Payment Alignment Models: 3 Examples There are several internal/external payment alignment models worth considering, but the three described here represent the more common models. Hospitals and health systems should choose the model that works best for them given their competitors, market position (e.g., size, specialization), and readiness for change. Bundled payment for chronic conditions. Payers and providers are also exploring bundled payment for chronic conditions, such as diabetes and asthma. These payer-provider payment arrangements typically cover cross-continuum, care management services for specific, high-cost chronically ill populations. Examples include a $40 to $50 per patient per month (PMPM) case management fee for primary care services and nurse care management services, plus additional fee-for-service payments for comprehensive, periodic check-ups. Providers are looking for ways to integrate these payments into their compensation and incentive plans. Medicare Bundled Payments for Care Improvement Initiative The four payment models announced by CMS in August only accelerate providers interest in bundling, because these payment arrangements permit hospitals that CMS selects to share savings with employed and/or affiliated physicians. Model 1. Hospitals commit to a 2 to 3 percent inpatient facility, across-the-board discount in all diagnosis-related groups (DRGs) for the opportunity to share unit cost and utilization savings with their physicians, who continue to be paid on a traditional fee-for-service schedule. Model 2. Hospitals agree to a 2 to 3 percent inpatient facility discount tied to specific DRGs (e.g., cardiac) and follow-up care within a 30-, 60-, or 90-day window postdischarge. Model 3. Providers agree to a small discount for postacute care only, associated with specific DRGs, to help drive delivery innovations postdischarge where savings potential is significant. Model 4. Hospitals and physicians jointly agree to a prospective, 3 percent or greater discount rate off current rates for select DRGs. The contracting hospital receives a check from CMS and distributes the fees among participating physicians in accordance with performance-based criteria. hfma.org NOVEMBER
5 Payment alignment model 1. The let s own it all payment alignment model is a rare breed. Few providers own their own multispecialty physician practice and health plan, but the ones that do control their cash flow, referral channels, and underlying risks. Provider-led integrated delivery systems with a relentless focus on reducing avoidable unit costs and utilization within specific patient populations use simple and elegant compensation and incentive models. Their incentives are rooted in ongoing analytics that track avoidable costs (e.g., excessive, riskadjusted drug or procedural spend) by specific primary care physicians, specialists, and patients. Their compensation and incentive models are managed centrally and tied closely to the organization s go-to-market strategy (e.g., reward top-performing physicians who improve access and grow underserved segments). Their models link directly to their long-term operating and capital budget as well, so that compensation, incentive, and risk pools are properly funded. Finally, the close-knit culture of these organizations permits them to penalize and/or eliminate underperforming providers who are not achieving minimum performance standards. Payment alignment model 2. In this model, a single, large provider partners with a large payer to implement third-party payment terms, including pay for performance, bundles, and partial capitation arrangements. About half of the arrangements are designed to grow patients/membership at competitors expense (e.g., expand into a new geography or patient population with a branded health plan and physician group). Where a payer and provider can jointly enter a new market with a higher quality, lower cost product that doesn t simply shift more costs to patients, the payer, providers, employers, and patients can win. All parties can win because new volume growth can fund deep compensation and incentive pools that can (for a time) make up for lackluster improvements in underlying overuse and misuse of resources. Over time, though, the new volume potential will decrease. If payers and providers fail to reinvest savings from low-hanging fruit (e.g., reductions in excessive emergency department [ED] use or high brand-name prescription use) early in their arrangement, cost savings and compensation and bonus pools evaporate quickly. So ignoring the need to invest some of the bonus up front becomes a major problem for these types of arrangements. Payment alignment model 3. In this model, several independent providers partner with each other to design a high-performing network, payment model, and payment distribution model in conjunction with a large payer. The independent providers tend to operate in highly fragmented markets, where a series of smaller hospitals, physician groups, and independent practice associations can come together only through a full merger or acquisition. These models have the most complexity by design, because they rely on a series of management contracts that cover medical management, analytic services, facility rental, and other activities. Despite their inherent complexity, they are also vehicles payers desire to begin to integrate and align historically fragmented parties to improve performance that independent parties cannot achieve on their own. One common evolution path is for providers (rather than payers) to initiate the creation of these high-performing networks. Then the networks contract with one or two payers and provide medical management services to specific payer subpopulations in return for a PMPM fee, fee schedule bonus (e.g., 10 percent), and/or direct investment (e.g., in health information exchange technology, which allows disparate providers to track referral and utilization patterns). Over time, these high-performing networks become strategic assets for payers that cultivate them. In return, providers benefit from a payer-funded, shared savings pool and/or volume steerage away from competitors that do not participate in the highperformance network. In these models in particular, the payment alignment model requires a stable, physician-led governing body across disparate providers to practice by fundamental performance and payment principles (e.g., evolve into 5 NOVEMBER 2011 healthcare financial management
6 KEY SIMILARITIES AND DIFFERENCES AMONG PAYMENT ALIGNMENT MODELS Model 1: IDS with Provider-Sponsored Health Plan Model 2: Large System/Large Payer Model Model 3: Multiprovider Network Model Description Health system owns its own primary care physician and multispecialty medical groups and branded HMO/PPO health plan; contracts with or owns hospitals. Health system partners with dominant commercial insurer (or CMS) to share savings via bundled reimbursement bonus model. Multiple health systems come together to contract with one or more commercial insurers. Market Characteristics The health system consolidated a highly fragmented payer market historically; market is characterized by relatively poor or undeveloped payer/provider relationships. The region s largest provider partners with the largest commercial payer to profitably grow a particular geography, type of service. Payers, providers, IPAs sign an affiliation agreement to coordinate care management activities, analytics, and IT spending; to begin to defragment care in an otherwise highly fragmented market. Third-Party Payer Involvement Commercial payers have a very limited market share, because provider-owned health plans keep costs out better than commercial plans could. Dominant commercial payer uses largest system to set the bar to drive costs out across the market; provider gets a large bonus pool to distribute if actual performance exceeds expected performance. One or more commercial payers use the network to sell to particular customers. Internal Payment Model Terms Simple pay-for-performance and/or shared savings arrangements that support Triple Aim; extra effort bonuses for contribution to specific strategic initiative; integrated with systemwide strategy, budget, and performance improvement plan. Physicians share in a large bonus pool in first few years; downside risk and penalties are adopted if savings do not materialize. This is the most complex model. It consists of a series of management service contracts and performance-based bonus dollars. risk, build in early wins, raise the bar). The actual payment distribution formulas vary, but tend to reward primary care rather heavily at first. Over time, the payment distribution and investment approach focuses on rewarding reductions in excessive specialty and hospital utilization through the use of the highest performing providers. The exhibit above summarizes key similarities and differences among the three payment alignment models profiled here. Payment Alignment Models: Early Lessons Learned The three payment alignment models underscore a few key takeaways for health systems as they design internal and external payment models that achieve the Institute for Healthcare Improvement s Triple Aim goals of improving population health, enhancing the patient experience, and reducing costs in an increasingly competitive environment. hfma.org NOVEMBER
7 Strategic foundation. The health systems should ensure that the payment alignment model supports its broader competitive strategy. The best payment models are not the ones with the most sophisticated math formulas. Nor are the best payment models the ones that drive the highest compensation levels to providers. The best payment models align internal incentives with what the market values, and in so doing drive both top-line and bottom-line improvements, as well as overall population health. Top-line improvements come from several sources, including preferential unit payment increases, shared savings, bonuses, and selective steerage/volume gains, particularly from historically underserved areas. Bottom-line improvements come from reductions in avoidable input unit costs (e.g., paying too much for particular supplies) and avoidable resource consumption/waste (e.g., excessive imaging and lab services associated with ED services). Health systems should not be enticed by large one-time-only bonus pools or cash infusions that reward the organization for nothing in particular. Data-driven design. Health systems should demand detailed claims data from payers and partner with them to perform analytics. They should benchmark unit payment, utilization, and input costs by patient population, not just by hospital or physician practice. Credibility and trust with participating physicians should be built by using fair market valuation techniques to benchmark and establish internal and external payments. Furthermore, payers should be wary of designing payment models that lavishly reward individual physicians with bonuses in the high five to low six figures for simply reducing bed days and/or admissions, but not improving underlying health conditions. organizations and are well positioned to provide input into a three- to five-year change management plan, which incorporates: > Updates to the health system s strategic capital plan to reflect market payment and compensation rates, as well as future performanceimprovement initiatives required to maintain current margins > A road map that outlines which incentives and investments need to change to drive performance > A list of early wins, including patientcentered medical homes, high-performance managed care networks, individualized patient care plans, and cost-effective risk adjustment techniques Finance Should Lead All the talk about payment reform, payment reductions, bundling, and shared savings strikes a profoundly personal note when these changes translate into compensation and incentive changes. Providers will need to be much more deliberate in how they align their external managed care contracting approaches and internal compensation and incentive approaches. This article provides a few key insights into what is working and what is not working today. Ultimately, no perfect model exists. Rather, finance executives will need to take a lead role in aligning their organization s external and internal payment models. About the author Michael E. Nugent, CHFP, is a managing director, provider and payer strategy practice, Navigant Consulting, Inc., Chicago, and a member of HFMA s First Illinois Chapter (mnugent@ navigantconsulting.com). Get the right team behind a deliberate change management plan. The most successful payment alignment models are being designed by integrated teams consisting of finance, clinical improvement, and physician practice staff. These staff members understand the underlying financial, clinical, and operational barriers at their Reprinted from the November 2011 issue of hfm magazine. Copyright 2011 by Healthcare Financial Management Association, Two Westbrook Corporate Center, Suite 700, Westchester, IL For more information, call HFMA or visit
budget planning under payment reform
 REPRINT JULY 2011 Michael E. Nugent healthcare financial management association www.hfma.org budget planning under payment reform AT A GLANCE > Healthcare reform makes budgeting topline reimbursement,
REPRINT JULY 2011 Michael E. Nugent healthcare financial management association www.hfma.org budget planning under payment reform AT A GLANCE > Healthcare reform makes budgeting topline reimbursement,
partnering with payers? key lessons to keep in mind
 REPRINT January 2014 Bill Eggbeer Kevin Sears Kenneth Homer healthcare financial management association hfma.org partnering with payers? key lessons to keep in mind As providers enter into risk-sharing
REPRINT January 2014 Bill Eggbeer Kevin Sears Kenneth Homer healthcare financial management association hfma.org partnering with payers? key lessons to keep in mind As providers enter into risk-sharing
THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION
 THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION HFMA First Illinois Chapter August 12, 2014 Stu Schaff Manager, DGA Partners Agenda > Background & Context > Measures
THE $10,000 QUESTION: TACKLING THE COMPLEXITIES OF VALUE-BASED PHYSICIAN COMPENSATION HFMA First Illinois Chapter August 12, 2014 Stu Schaff Manager, DGA Partners Agenda > Background & Context > Measures
evaluating the fair market value of pay for performance
 REPRINT April 2014 Jen Johnson Alexandra Higgins healthcare financial management association hfma.org evaluating the fair market value of pay for performance A critical test for determining whether a pay-for-performance
REPRINT April 2014 Jen Johnson Alexandra Higgins healthcare financial management association hfma.org evaluating the fair market value of pay for performance A critical test for determining whether a pay-for-performance
FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS
 CENTER FOR INDUSTRY TRANSFORMATION MAY 2015 FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS Authors Amy Bibby Partner, DHG Healthcare amy.bibby@dhgllp.com Matthew Fadel Manager, DHG Healthcare matt.fadel@dhgllp.com
CENTER FOR INDUSTRY TRANSFORMATION MAY 2015 FUNDS FLOW METHODOLOGY FOR RISK-BASED CONTRACTS Authors Amy Bibby Partner, DHG Healthcare amy.bibby@dhgllp.com Matthew Fadel Manager, DHG Healthcare matt.fadel@dhgllp.com
Cutting Edge Issues Related to. April 16, Payments to Physicians Under P4P Compensation Models
 Cutting Edge Issues Related to Payments to Physicians Under P4P Compensation Models April 16, 2014 2515 McKinney Avenue, Suite 1500 Dallas, Texas 75201 Telephone: 214.369.4888 Fax: 214.369.0541 3100 West
Cutting Edge Issues Related to Payments to Physicians Under P4P Compensation Models April 16, 2014 2515 McKinney Avenue, Suite 1500 Dallas, Texas 75201 Telephone: 214.369.4888 Fax: 214.369.0541 3100 West
capital planning for clinical integration
 Daniel M. Grauman Gerald Neff Molly Martha Johnson REPRINT APRIL 2011 healthcare financial management association www.hfma.org capital planning for clinical integration Hospitals should view physician
Daniel M. Grauman Gerald Neff Molly Martha Johnson REPRINT APRIL 2011 healthcare financial management association www.hfma.org capital planning for clinical integration Hospitals should view physician
The Health Insurance Market in Virginia. Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017
 The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
5 critical issues for BPCI-A
 REPRINT June 2018 John M. Harris Molly Johnson Amanda Brown healthcare financial management association hfma.org 5 critical issues for BPCI-A Many hospitals and health systems may benefit from participation
REPRINT June 2018 John M. Harris Molly Johnson Amanda Brown healthcare financial management association hfma.org 5 critical issues for BPCI-A Many hospitals and health systems may benefit from participation
Delivering Value-Based Care:
 Discussion Summary Delivering Value-Based Care: Episodes of Care Analytics for Health Care Providers, Payers and ACOs July 2015 Interview Featuring: J. Peter Chingos, Senior Industry Consultant, Health
Discussion Summary Delivering Value-Based Care: Episodes of Care Analytics for Health Care Providers, Payers and ACOs July 2015 Interview Featuring: J. Peter Chingos, Senior Industry Consultant, Health
Are You Optimizing Your Provider-Sponsored Medicare Advantage Plan?
 Are You Optimizing Your Provider-Sponsored Medicare Advantage Plan? April 2016 WRITTEN BY: TYRONNE JOLLY, RICH TREMBOWICZ The Medicare market is swelling as the nation s aging population continues to grow.
Are You Optimizing Your Provider-Sponsored Medicare Advantage Plan? April 2016 WRITTEN BY: TYRONNE JOLLY, RICH TREMBOWICZ The Medicare market is swelling as the nation s aging population continues to grow.
back to basics 5 ways to pick low-hanging fruit
 REPRINT AUGUST 2012 Steven Berger healthcare financial management association hfma.org back to basics 5 ways to pick low-hanging fruit Hospital finance leaders should perform a few analyses to reduce their
REPRINT AUGUST 2012 Steven Berger healthcare financial management association hfma.org back to basics 5 ways to pick low-hanging fruit Hospital finance leaders should perform a few analyses to reduce their
Value Based Contracting
 Value Based Contracting CONCEPTS FOR THE MEDICAL PRACTICE dhgllp.com/healthcare 225 Peachtree Street NE, Suite 600 Atlanta, GA 30303 Bill Hannah PRINCIPAL Bill.Hannah@dhgllp.com 404.575.8921 Doral Davis-Jacobsen
Value Based Contracting CONCEPTS FOR THE MEDICAL PRACTICE dhgllp.com/healthcare 225 Peachtree Street NE, Suite 600 Atlanta, GA 30303 Bill Hannah PRINCIPAL Bill.Hannah@dhgllp.com 404.575.8921 Doral Davis-Jacobsen
Considerations for a Hospital-Based ACO. Insurance Premium Construction: Tim Smith, ASA, MAAA, MS
 Insurance Premium Construction: Considerations for a Hospital-Based ACO Tim Smith, ASA, MAAA, MS I once saw a billboard advertising a new insurance product co-branded by the local hospital system and a
Insurance Premium Construction: Considerations for a Hospital-Based ACO Tim Smith, ASA, MAAA, MS I once saw a billboard advertising a new insurance product co-branded by the local hospital system and a
Approved Models to Align Incentives between Hospitals and their Physicians
 Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
Fee for Service: Paying for Volume, Not Value
 Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
IT TAKES THREE TO TANGO
 IT TAKES THREE TO TANGO Structural Collaboration Between Carriers, Providers and Consumers A HEALTHSCAPE ADVISORS EXECUTIVE BRIEFING This HealthScape Advisors Executive Brief discusses a more comprehensive
IT TAKES THREE TO TANGO Structural Collaboration Between Carriers, Providers and Consumers A HEALTHSCAPE ADVISORS EXECUTIVE BRIEFING This HealthScape Advisors Executive Brief discusses a more comprehensive
acknowledging the importance of BAI accounts
 REPRINT SEPTEMBER 2011 FEATURE STORY Steve Levin healthcare financial management association www.hfma.org acknowledging the importance of BAI accounts Hospitals should not underestimate the importance
REPRINT SEPTEMBER 2011 FEATURE STORY Steve Levin healthcare financial management association www.hfma.org acknowledging the importance of BAI accounts Hospitals should not underestimate the importance
Rewarding High Quality: Practical Models for Value- Based Physician Payment
 Rewarding High Quality: Practical Models for Value- Based Physician Payment Introduction In its 2013 report, Moving Beyond Fee-for-Service, the Alliance of Community Health Plans (ACHP) addressed the increasing
Rewarding High Quality: Practical Models for Value- Based Physician Payment Introduction In its 2013 report, Moving Beyond Fee-for-Service, the Alliance of Community Health Plans (ACHP) addressed the increasing
The Case For Value ACA to MACRA to MIPS
 The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
The Case For Value ACA to MACRA to MIPS 2016-2019 Robert E Nesse M.D. Professor of Family Medicine Mayo Medical School Senior Director of Health Care Policy and Payment Reform nesse.robert@mayo.edu What
Using Analytics To Transform Your ACO
 Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
Insight to Value-Based Care and A Joint Venture Case Study. Whitney Courser SVP, Sales and Marketing
 Insight to Value-Based Care and A Joint Venture Case Study Whitney Courser SVP, Sales and Marketing WCourser@nuehealth.com Meet NueHealth 22-year-old, privately held, nationally trusted healthcare partner
Insight to Value-Based Care and A Joint Venture Case Study Whitney Courser SVP, Sales and Marketing WCourser@nuehealth.com Meet NueHealth 22-year-old, privately held, nationally trusted healthcare partner
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations
 10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. Speaker Disclosures Steve Selbst is employed by a business firm that provides services related
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. Speaker Disclosures Steve Selbst is employed by a business firm that provides services related
10 Best Practices For Payer Contracting:
 10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. 2016 NHIA Annual Conference & Exposition 1 Speaker Disclosures Steve Selbst is employed by
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. 2016 NHIA Annual Conference & Exposition 1 Speaker Disclosures Steve Selbst is employed by
Figure 1: Original APM Framework
 Contents Overview... 2 This Year s APM Measurement Effort... 3 Scope... 3 Data Source... 4 The LAN Survey... 4 The Blue Cross Blue Shield Association Survey... 8 The America s Health Insurance Plans Survey...
Contents Overview... 2 This Year s APM Measurement Effort... 3 Scope... 3 Data Source... 4 The LAN Survey... 4 The Blue Cross Blue Shield Association Survey... 8 The America s Health Insurance Plans Survey...
Medicare Advantage 2.0 next generation growth strategies
 REPRINT August 2017 Cary Badger Brad Helfand healthcare financial management association hfma.org Medicare Advantage 2.0 next generation growth strategies Healthcare organizations are looking to data-driven
REPRINT August 2017 Cary Badger Brad Helfand healthcare financial management association hfma.org Medicare Advantage 2.0 next generation growth strategies Healthcare organizations are looking to data-driven
Providers involved in the Centers for Medicare & Medicaid Services ACE demonstration project share
 Pursuing Bundled Payments Lessons from the ACE Demonstration Providers involved in the Centers for Medicare & Medicaid Services ACE demonstration project share lessons learned from their experiences in
Pursuing Bundled Payments Lessons from the ACE Demonstration Providers involved in the Centers for Medicare & Medicaid Services ACE demonstration project share lessons learned from their experiences in
Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models
 Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models Kristina Rollings Product Director, Emerging Solutions March 24, 2014 Agenda 1. State of the
Configuration of Network and Financial Management Systems to Support Multiple Value Based Reimbursement Models Kristina Rollings Product Director, Emerging Solutions March 24, 2014 Agenda 1. State of the
What s Next for MSSP ACOs? The Case for Moving to Medicare Risk
 What s Next for MSSP ACOs? The Case for Moving to Medicare Risk Picking Your Path on a Journey Towards Value-Based Care Participants in one of Medicare s boldest attempts to overhaul how doctors and physicians
What s Next for MSSP ACOs? The Case for Moving to Medicare Risk Picking Your Path on a Journey Towards Value-Based Care Participants in one of Medicare s boldest attempts to overhaul how doctors and physicians
using the Medicare cost report to improve financial performance
 REPRINT OCTOBER 2010 Kathleen J. LaBrake Holly S. Pokrandt healthcare financial management association www.hfma.org using the Medicare cost report to improve financial performance The Medicare cost report
REPRINT OCTOBER 2010 Kathleen J. LaBrake Holly S. Pokrandt healthcare financial management association www.hfma.org using the Medicare cost report to improve financial performance The Medicare cost report
FROM SILOS TO SERVICES FOR VALUE-BASED CARE
 White Paper FROM SILOS TO SERVICES FOR VALUE-BASED CARE A bundled payment program built by hand 25 years ago is still delivering lessons for HIT today By Amy Larsson RN, BSN, MBA, Vice President, Clinical
White Paper FROM SILOS TO SERVICES FOR VALUE-BASED CARE A bundled payment program built by hand 25 years ago is still delivering lessons for HIT today By Amy Larsson RN, BSN, MBA, Vice President, Clinical
National APM Data Collection Frequently Asked Questions for 2018
 National APM Data Collection Frequently Asked Questions for 2018 Last updated on 1/25/18 Please note this document may be updated and improved periodically based on feedback from health plans and other
National APM Data Collection Frequently Asked Questions for 2018 Last updated on 1/25/18 Please note this document may be updated and improved periodically based on feedback from health plans and other
developing a CIN for strategic value
 REPRINT July 2014 Daniel Grauman John Harris Idette Elizondo Sean Looby healthcare financial management association hfma.org developing a CIN for strategic value Having a clinically integrated network
REPRINT July 2014 Daniel Grauman John Harris Idette Elizondo Sean Looby healthcare financial management association hfma.org developing a CIN for strategic value Having a clinically integrated network
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business?
 Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
DELIVERING HIGHER-VALUE MATERNITY CARE
 DELIVERING HIGHER-VALUE MATERNITY CARE Designing Alternative Payment Models for Better Care, Lower Spending, and Financially Viable Maternity Care Providers Harold D. Miller President and CEO Center for
DELIVERING HIGHER-VALUE MATERNITY CARE Designing Alternative Payment Models for Better Care, Lower Spending, and Financially Viable Maternity Care Providers Harold D. Miller President and CEO Center for
Population-Based Healthcare: Structural Models and Options
 Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers
 Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers Montana Chamber of Commerce Healthcare Forum November 29-30, 2016 Shane Wolverton SVP CORPORATE DEVELOPMENT, QUANTROS
Healthcare Value Purchasing: Perspectives from Employers, Facilities and Consumers Montana Chamber of Commerce Healthcare Forum November 29-30, 2016 Shane Wolverton SVP CORPORATE DEVELOPMENT, QUANTROS
The Emergence of Value-Based Care: Present and Future Tense
 The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
The U.S. Healthcare System: How Pharmacy Benefit Managers Impact Prescription Drug Use. Presented by Daniel Tomaszewski Pharmd, PhD
 The U.S. Healthcare System: How Pharmacy Benefit Managers Impact Prescription Drug Use Presented by Daniel Tomaszewski Pharmd, PhD 1 Medical Vs. Pharmacy Coverage Medical Insurance Managed by an Insurance
The U.S. Healthcare System: How Pharmacy Benefit Managers Impact Prescription Drug Use Presented by Daniel Tomaszewski Pharmd, PhD 1 Medical Vs. Pharmacy Coverage Medical Insurance Managed by an Insurance
INFORMATION ABOUT YOUR OXFORD COVERAGE
 OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
All About APMs: What Will It Take for Physicians to Earn the APM Bonus Under MACRA?
 All About APMs: What Will It Take for Physicians to Earn the APM Bonus Under MACRA? By Robert F. Atlas, David B. Tatge, and Lesley R. Yeung June 2016 On May 9, 2016, the Centers for Medicare & Medicaid
All About APMs: What Will It Take for Physicians to Earn the APM Bonus Under MACRA? By Robert F. Atlas, David B. Tatge, and Lesley R. Yeung June 2016 On May 9, 2016, the Centers for Medicare & Medicaid
CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives
 CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives Presented by: Peter R. Epp, CPA S e p t e m b e r 2 9, 2 0 1 6 HMA I n t r o d u c t i o n One of the overarching objectives
CURRENT DEVELOPMENTS IN VALUE BASED PAYMENT (VBP): Part 1 Recent Initiatives Presented by: Peter R. Epp, CPA S e p t e m b e r 2 9, 2 0 1 6 HMA I n t r o d u c t i o n One of the overarching objectives
UnityPoint Accountable Care Aligning Provider Incentives in Risk- Bearing, Value-Based Contracts. March 10, 2018
 UnityPoint Accountable Care Aligning Provider Incentives in Risk- Bearing, Value-Based Contracts March 10, 2018 1 Aligning Provider Incentives in Risk- Bearing, Value-Based Contracts UnityPoint Accountable
UnityPoint Accountable Care Aligning Provider Incentives in Risk- Bearing, Value-Based Contracts March 10, 2018 1 Aligning Provider Incentives in Risk- Bearing, Value-Based Contracts UnityPoint Accountable
The Four Knows and Tips of Contracting with Managed Care Organizations October 7, 2012
 The Four Knows and Tips of Contracting with Managed Care Organizations October 7, 2012 The Four Knows of Contracting 1. Know the Rules 2. Know What the MCOs Need/Want? 3. Provider Know Thyself 4. Know
The Four Knows and Tips of Contracting with Managed Care Organizations October 7, 2012 The Four Knows of Contracting 1. Know the Rules 2. Know What the MCOs Need/Want? 3. Provider Know Thyself 4. Know
HEALTH POLICY & EDUCATION SERIES
 HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
Healthcare reimbursement is facing some of the biggest changes and challenges of the past 50 years.
 Healthcare reimbursement is facing some of the biggest changes and challenges of the past 50 years. While in many ways this evolution is a good thing, it does require organizations to fundamentally rethink
Healthcare reimbursement is facing some of the biggest changes and challenges of the past 50 years. While in many ways this evolution is a good thing, it does require organizations to fundamentally rethink
than value. infrastructure for value-based payment, it is apparent that greater assumption of
 EXECUTIVE BRIEFING Value-Based Contracting: How to Think Like a Payer It is widely recognized that the rate of healthcare spending in the U.S. is unsustainable. In recent years, experts of all types, from
EXECUTIVE BRIEFING Value-Based Contracting: How to Think Like a Payer It is widely recognized that the rate of healthcare spending in the U.S. is unsustainable. In recent years, experts of all types, from
Valuation of Alternative Payment Models
 Valuation of Alternative Payment Models No portion of this white paper may be used or duplicated by any person or entity for any purpose without the express written permission of PYA. I. Introduction:
Valuation of Alternative Payment Models No portion of this white paper may be used or duplicated by any person or entity for any purpose without the express written permission of PYA. I. Introduction:
Narrow, Tailored, Tiered and High Performance Networks: An Emerging Trend
 Narrow, Tailored, Tiered and High Performance Networks: An Emerging Trend Bill Eggbeer, Managing Director, and Dudley Morris, Senior Advisor, BDC Advisors, LLC Executive Summary A recent BDC survey of
Narrow, Tailored, Tiered and High Performance Networks: An Emerging Trend Bill Eggbeer, Managing Director, and Dudley Morris, Senior Advisor, BDC Advisors, LLC Executive Summary A recent BDC survey of
From Silos to Services for Value-Based Care
 White Paper From Silos to Services for Value-Based Care Author Amy Larsson, RN, BSN, MBA Vice President, Clinical Claims Management, Change Healthcare A bundled payment program built by hand 25 years ago
White Paper From Silos to Services for Value-Based Care Author Amy Larsson, RN, BSN, MBA Vice President, Clinical Claims Management, Change Healthcare A bundled payment program built by hand 25 years ago
Comprehensive Primary Care Payment Calculator User s Guide
 1 Comprehensive Primary Care Payment Calculator User s Guide Prepared by Health Data Decisions August 2017 Disclaimer: Information provided in connection with this calculator by FMAHealth and its contributors
1 Comprehensive Primary Care Payment Calculator User s Guide Prepared by Health Data Decisions August 2017 Disclaimer: Information provided in connection with this calculator by FMAHealth and its contributors
Facility editing: Enhance payment integrity while building strong provider relationships
 Facility editing: Enhance payment integrity while building strong provider relationships Optum www.optuminsight.com Page 1 Five steps toward effective facility editing It is a real challenge to edit facility
Facility editing: Enhance payment integrity while building strong provider relationships Optum www.optuminsight.com Page 1 Five steps toward effective facility editing It is a real challenge to edit facility
Value Based Purchasing. RHP 9 Learning Collaborative February 22, 2017
 Value Based Purchasing RHP 9 Learning Collaborative February 22, 2017 Purpose Dialogue with RHP stakeholders on the following topics: What Value Based Purchasing (VBP) is and why HHSC is promoting it VBP
Value Based Purchasing RHP 9 Learning Collaborative February 22, 2017 Purpose Dialogue with RHP stakeholders on the following topics: What Value Based Purchasing (VBP) is and why HHSC is promoting it VBP
Problems with Current Health Plans
 Problems with Current Health Plans Poor Integration, Coordination and Collaboration - Current plans offer limited coordination between the health plan, Providers, and the Members, as well as limited mobile
Problems with Current Health Plans Poor Integration, Coordination and Collaboration - Current plans offer limited coordination between the health plan, Providers, and the Members, as well as limited mobile
How Health Reform Saves Consumers and Taxpayers Money
 How Health Reform Saves Consumers and Taxpayers Money The Affordable Care Act Lowers Costs and Improves Quality June Health reform s three major goals insurance reform, affordable coverage, and slower
How Health Reform Saves Consumers and Taxpayers Money The Affordable Care Act Lowers Costs and Improves Quality June Health reform s three major goals insurance reform, affordable coverage, and slower
assessing the impact pricing commodity outpatient procedures
 REPRINT October 2015 William O. Cleverley healthcare financial management association hfma.org pricing commodity outpatient procedures assessing the impact Hospital executives are facing unrelenting pressure
REPRINT October 2015 William O. Cleverley healthcare financial management association hfma.org pricing commodity outpatient procedures assessing the impact Hospital executives are facing unrelenting pressure
Implications of Health Care Reform for Physician Compensation
 Sullivan, Cotter and Associates, Inc. 612.294.3645 tomdobosenski@sullivancotter.com 2013 Sullivan, Cotter and Associates, Inc. The material may not be reproduced or copied without written consent of SullivanCotter.
Sullivan, Cotter and Associates, Inc. 612.294.3645 tomdobosenski@sullivancotter.com 2013 Sullivan, Cotter and Associates, Inc. The material may not be reproduced or copied without written consent of SullivanCotter.
A Path to Accountable Care Organizations: How Do We Get From There to Here? Financial Considerations for Accountable
 A Path to Accountable Care Organizations: How Do We Get From There to Here? Financial Considerations for Accountable Care Entity Engagement Presented by Milliman, Inc. San Francisco, CA susan.pantely@milliman.com
A Path to Accountable Care Organizations: How Do We Get From There to Here? Financial Considerations for Accountable Care Entity Engagement Presented by Milliman, Inc. San Francisco, CA susan.pantely@milliman.com
Future Healthcare Payment Models An Overview
 Future Healthcare Payment Models An Overview Carter Dredge THERE IS A CRITICAL NEED TO TRANSFORM HEALTHCARE DELIVERY & PAYMENT 2 Significant Variation in Population Utilization Spine Surgeries per 1,000
Future Healthcare Payment Models An Overview Carter Dredge THERE IS A CRITICAL NEED TO TRANSFORM HEALTHCARE DELIVERY & PAYMENT 2 Significant Variation in Population Utilization Spine Surgeries per 1,000
Advanced Analytics. The key to unlocking the Triple Aim and Value-Based Purchasing. Ines Vigil MD, MPH, MBA
 Advanced Analytics The key to unlocking the Triple Aim and Value-Based Purchasing Ines Vigil MD, MPH, MBA Advanced Analytics: The key to unlocking the Triple Aim and Value-Based Purchasing Current State
Advanced Analytics The key to unlocking the Triple Aim and Value-Based Purchasing Ines Vigil MD, MPH, MBA Advanced Analytics: The key to unlocking the Triple Aim and Value-Based Purchasing Current State
Stuart H. Altman. The Changing Health Care System: Economic Forces Pushing States To Become More Involved
 The Changing Health Care System: Economic Forces Pushing States To Become More Involved Stuart H. Altman Sol Chaikin Professor of Health Policy The Heller School for Social Policy and Management Brandeis
The Changing Health Care System: Economic Forces Pushing States To Become More Involved Stuart H. Altman Sol Chaikin Professor of Health Policy The Heller School for Social Policy and Management Brandeis
C - Suite Transformation Management Training: Finance and Operations Overview. May 17, 2017
 C - Suite Transformation Management Training: Finance and Operations Overview Presented by: Peter R. Epp, CPA May 17, 2017 Overview Summary of Value Based Payment (VBP) Initiatives Underlying VBP Payment
C - Suite Transformation Management Training: Finance and Operations Overview Presented by: Peter R. Epp, CPA May 17, 2017 Overview Summary of Value Based Payment (VBP) Initiatives Underlying VBP Payment
Healthcare Reform and Its Impact on the Care Delivery System
 Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Working Draft: Health Care Entities Revenue Recognition Implementation Issue. Financial Reporting Center Revenue Recognition
 October 2, 2017 Financial Reporting Center Revenue Recognition Working Draft: Health Care Entities Revenue Recognition Implementation Issue Issue #8-9 Risk Sharing Arrangements Expected Overall Level of
October 2, 2017 Financial Reporting Center Revenue Recognition Working Draft: Health Care Entities Revenue Recognition Implementation Issue Issue #8-9 Risk Sharing Arrangements Expected Overall Level of
REPORT OF THE COUNCIL ON MEDICAL SERVICE. (J. Leonard Lichtenfeld, MD, Chair)
 REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -A-0 Subject: Presented by: Referred to: Appropriate Hospital Charges David O. Barbe, MD, Chair Reference Committee G (J. Leonard Lichtenfeld, MD, Chair)
REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -A-0 Subject: Presented by: Referred to: Appropriate Hospital Charges David O. Barbe, MD, Chair Reference Committee G (J. Leonard Lichtenfeld, MD, Chair)
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making. Introduction. William Bednar, FSA, FCA, MAAA
 Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study
 Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study Presented by Bill O Brien, FSA, MAAA Consulting Actuary Milliman Houston, TX (832) 878-4078 Preconference I Agenda
Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study Presented by Bill O Brien, FSA, MAAA Consulting Actuary Milliman Houston, TX (832) 878-4078 Preconference I Agenda
9/23/2016. Our Services. Transitioning from Fee-for-Service to Value-based Reimbursement. Key Trends and Strategies for Rural Health Providers
 Transitioning from Fee-for-Service to Value-based Reimbursement Key Trends and Strategies for Rural Health Providers Paul MacLellan, CEO >> Health care consulting company >> Wholly owned subsidiary of
Transitioning from Fee-for-Service to Value-based Reimbursement Key Trends and Strategies for Rural Health Providers Paul MacLellan, CEO >> Health care consulting company >> Wholly owned subsidiary of
Healthcare Financial Management Association Certification Program. Module I: The Business of Health Care Learner s Guide
 Healthcare Financial Management Association Certification Program Module I: The Business of Health Care Learner s Guide For examination period beginning June 2015 1 Course 1 - The Big Picture Learning
Healthcare Financial Management Association Certification Program Module I: The Business of Health Care Learner s Guide For examination period beginning June 2015 1 Course 1 - The Big Picture Learning
Payment Reform in Support of Population Health Management
 Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
Payment Reform in Support of Population Health Management Aligning Forces for Quality Employers - Providers Summit October 25, 2011 Charles Chodroff, MD, MBA, FACP Senior Vice President, Chief Clinical
Embracing the Future of Care Delivery: What have we learned?
 Embracing the Future of Care Delivery: What have we learned? Robert Nesse, M.D. Senior Advisor for Healthcare Policy and Payment Reform CEO, Mayo Clinic Health System 2010-2015 2014 MFMER slide-1 Fundamental
Embracing the Future of Care Delivery: What have we learned? Robert Nesse, M.D. Senior Advisor for Healthcare Policy and Payment Reform CEO, Mayo Clinic Health System 2010-2015 2014 MFMER slide-1 Fundamental
Value-Based Payments (VBP)
 Value-Based Payments (VBP) Overview September 27, 2016 September 27, 2016 2 NYS What is Value Based Payment? NYS Timeline VBP Outcomes and Levels P4P vs. VBP VBP Overview Agenda MCTAC VBP Arrangements
Value-Based Payments (VBP) Overview September 27, 2016 September 27, 2016 2 NYS What is Value Based Payment? NYS Timeline VBP Outcomes and Levels P4P vs. VBP VBP Overview Agenda MCTAC VBP Arrangements
educate. elevate. HEALTHCARE FINANCIAL TRAINING GEARED TO YOUR NEEDS course catalog
 educate. elevate. HEALTHCARE FINANCIAL TRAINING GEARED TO YOUR NEEDS course catalog 2017 welcome This catalog is your essential, easy-to-use reference for e2 Learning from HFMA. It identifies specific
educate. elevate. HEALTHCARE FINANCIAL TRAINING GEARED TO YOUR NEEDS course catalog 2017 welcome This catalog is your essential, easy-to-use reference for e2 Learning from HFMA. It identifies specific
Presented by: Steven Flores. Prepared for: The Predictive Modeling Summit
 Presented by: Steven Flores Prepared for: The Predictive Modeling Summit November 13, 2014 Disease Management Introduction A multidisciplinary, systematic approach to health care delivery that: Includes
Presented by: Steven Flores Prepared for: The Predictive Modeling Summit November 13, 2014 Disease Management Introduction A multidisciplinary, systematic approach to health care delivery that: Includes
Assessing ACO Performance
 Assessing ACO Performance David V. Axene, FSA, FCA, CERA, MAAA As more health plans utilize Accountable Care Organizations (i.e., ACOs) as part of their network operations, ACO performance assessment is
Assessing ACO Performance David V. Axene, FSA, FCA, CERA, MAAA As more health plans utilize Accountable Care Organizations (i.e., ACOs) as part of their network operations, ACO performance assessment is
Evidence-Based Program Reimbursement Strategies. Timothy P. McNeill, RN, MPH
 Evidence-Based Program Reimbursement Strategies Timothy P. McNeill, RN, MPH 1 Medicare & Value Based Purchasing 2 Medicare Advantage Changes 3 DSMT Requirements 4 CDSME Tip Sheet Opportunities for EB Programs
Evidence-Based Program Reimbursement Strategies Timothy P. McNeill, RN, MPH 1 Medicare & Value Based Purchasing 2 Medicare Advantage Changes 3 DSMT Requirements 4 CDSME Tip Sheet Opportunities for EB Programs
This is a sample of the instructor materials for The Core Elements of Value in Healthcare, by Paveljit S. Bindra.
 This is a sample of the instructor materials for The Core Elements of Value in Healthcare, by Paveljit S. Bindra. The complete instructor materials include the following: Test bank PowerPoint slides for
This is a sample of the instructor materials for The Core Elements of Value in Healthcare, by Paveljit S. Bindra. The complete instructor materials include the following: Test bank PowerPoint slides for
Aligning health plans and providers: Working together to control costs
 Aligning health plans and providers: Working together to control costs US health care costs continue to rise more rapidly than is sustainable. Health care spending was $3.2 trillion in 2015, a 5.3% increase
Aligning health plans and providers: Working together to control costs US health care costs continue to rise more rapidly than is sustainable. Health care spending was $3.2 trillion in 2015, a 5.3% increase
When the Dust Settles-What s Next?
 When the Dust Settles-What s Next? AMA IPPS Conference Robert Nesse M.D. Senior Director of Payment Reform Mayo Clinic nesse.robert@mayo.edu What is Driving the Change in Healthcare? Common Belief: The
When the Dust Settles-What s Next? AMA IPPS Conference Robert Nesse M.D. Senior Director of Payment Reform Mayo Clinic nesse.robert@mayo.edu What is Driving the Change in Healthcare? Common Belief: The
Transforming Not-for-Profit Healthcare in the Era of Reform Ratings Driven Increasingly By Management Effectiveness in Executing New Strategies
 MAY 2010 U.S. PUBLIC FINANCE SPECIAL COMMENT Transforming Not-for-Profit Healthcare in the Era of Reform Ratings Driven Increasingly By Management Effectiveness in Executing New Strategies Table of Contents:
MAY 2010 U.S. PUBLIC FINANCE SPECIAL COMMENT Transforming Not-for-Profit Healthcare in the Era of Reform Ratings Driven Increasingly By Management Effectiveness in Executing New Strategies Table of Contents:
March 1, Chairman Lamar Alexander United States Senate Committee on Health, Education, Labor, and Pensions Washington, DC 20510
 March 1, 2019 Chairman Lamar Alexander United States Senate Committee on Health, Education, Labor, and Pensions Washington, DC 20510 Dear Chairman Alexander: On behalf of AMGA and our members, I appreciate
March 1, 2019 Chairman Lamar Alexander United States Senate Committee on Health, Education, Labor, and Pensions Washington, DC 20510 Dear Chairman Alexander: On behalf of AMGA and our members, I appreciate
How Bundled Payments Create Value in New Product Designs Cognizant
 How Bundled Payments Create Value in New Product Designs 1 About Cognizant 2 This Will Not Take Long. 3 What is a Health Insurance Product? 4 Understanding Product Design Commercial Insurance One specific
How Bundled Payments Create Value in New Product Designs 1 About Cognizant 2 This Will Not Take Long. 3 What is a Health Insurance Product? 4 Understanding Product Design Commercial Insurance One specific
10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD. AccountableCareInstitute.com
 10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD FQHCs Bridge the Gap in Care Bridge Built and Maintained by FFS Dollars 2 CMMI View of FFS Medicine 3 Accountability High
10/17/2014 Risk-Based Payment Methodologies A National Perspective Art Jones, MD FQHCs Bridge the Gap in Care Bridge Built and Maintained by FFS Dollars 2 CMMI View of FFS Medicine 3 Accountability High
Medicare payment policy and its impact on program spending
 Medicare payment policy and its impact on program spending James E. Mathews, Ph.D. Deputy Director, Medicare Payment Advisory Commission February 8, 2013 Outline of today s presentation Brief background
Medicare payment policy and its impact on program spending James E. Mathews, Ph.D. Deputy Director, Medicare Payment Advisory Commission February 8, 2013 Outline of today s presentation Brief background
11/16/2015. Valence Health Solutions To Support. Vision. 20 years of Serving ~100 Hospital & Health System Clients Nationally.
 Valence Health Solutions To Support Prepared for First Illinois HFMA Optimize risk contracts Analyze and improve in-network utilization Improve quality November 2015 2015 Valence Health. All rights reserved.
Valence Health Solutions To Support Prepared for First Illinois HFMA Optimize risk contracts Analyze and improve in-network utilization Improve quality November 2015 2015 Valence Health. All rights reserved.
Building a healthier world
 Building a healthier world Improving health care with accountable care John Stockton April 6, 2017 51.25.913.1 (12/16) The current system isn t working It isn t working for our country It isn t working
Building a healthier world Improving health care with accountable care John Stockton April 6, 2017 51.25.913.1 (12/16) The current system isn t working It isn t working for our country It isn t working
Common Managed Care Terms & Definitions
 Contact Us: Email: info@emedbiz.com Phone: 561-430-2090 Fax: 561-430-2091 Website: www.emedbiz.com Common Managed Care Terms & Definitions Balance billing: The practice of billing a patient for the amount
Contact Us: Email: info@emedbiz.com Phone: 561-430-2090 Fax: 561-430-2091 Website: www.emedbiz.com Common Managed Care Terms & Definitions Balance billing: The practice of billing a patient for the amount
2.05 Predictive Modeling P4P and Physician Engagement. Pay for Performance Summit February 7, 2006
 2.05 Predictive Modeling P4P and Physician Engagement Pay for Performance Summit February 7, 2006 1 Agenda Three Key Healthcare Trends About Predictive Modeling About Reporting Business and Clinical Outcomes
2.05 Predictive Modeling P4P and Physician Engagement Pay for Performance Summit February 7, 2006 1 Agenda Three Key Healthcare Trends About Predictive Modeling About Reporting Business and Clinical Outcomes
Evaluating the Fair Market Value of Pay for Performance
 April 2014 healthcare financial management FEATURE STORY Jen Johnson Alexandra Higgins Evaluating the Fair Market Value of Pay for Performance 1 AT A GLANCE When assessing a pay-for-performance arrangement,
April 2014 healthcare financial management FEATURE STORY Jen Johnson Alexandra Higgins Evaluating the Fair Market Value of Pay for Performance 1 AT A GLANCE When assessing a pay-for-performance arrangement,
Alternative Payment Models and Clearinghouses Education and Impacts. White Paper by the Emerging Trends and Strategic Innovation Committee
 Alternative Payment Models and Clearinghouses Education and Impacts White Paper by the Emerging Trends and Strategic Innovation Committee May 5, 2017 Introduction Alternative Payment Models, or APMs, are
Alternative Payment Models and Clearinghouses Education and Impacts White Paper by the Emerging Trends and Strategic Innovation Committee May 5, 2017 Introduction Alternative Payment Models, or APMs, are
Risk adjustment is an important opportunity to ensure the sustainability of the exchanges and coverage for patients with chronic conditions.
 RISK ADJUSTMENT Risk adjustment is an important opportunity to ensure the sustainability of the exchanges and coverage for patients with chronic conditions. If risk adjustment is not implemented correctly,
RISK ADJUSTMENT Risk adjustment is an important opportunity to ensure the sustainability of the exchanges and coverage for patients with chronic conditions. If risk adjustment is not implemented correctly,
SEC actions compel new focus on disclosure
 REPRINT November 2013 Heidi H. Jeffery David Y. Bannard healthcare financial management association hfma.org SEC actions compel new focus on disclosure Healthcare organizations should take a lesson from
REPRINT November 2013 Heidi H. Jeffery David Y. Bannard healthcare financial management association hfma.org SEC actions compel new focus on disclosure Healthcare organizations should take a lesson from
Health Action Council. Community Health Data: Improving Employer Investment in Overall Employee Health
 Health Action Council Health Data: Improving Employer Investment in Overall Employee Health Health Data: Improving Employer Investment in Overall Employee Health. UnitedHealthcare White Paper Employers
Health Action Council Health Data: Improving Employer Investment in Overall Employee Health Health Data: Improving Employer Investment in Overall Employee Health. UnitedHealthcare White Paper Employers
March 1, Dear Mr. Kouzoukas:
 March 1, 2019 Mr. Demetrios L. Kouzoukas Principal Deputy Administrator and Director Center for Medicare Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: Advance
March 1, 2019 Mr. Demetrios L. Kouzoukas Principal Deputy Administrator and Director Center for Medicare Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: Advance
Value over volume The drivers of health care M&A in 2017
 Value over volume The drivers of health care M&A in 2017 How to win in a thriving deal market Value over volume The drivers of health care M&A in 2017 Gregory Park Partner, US Health Transaction Advisory
Value over volume The drivers of health care M&A in 2017 How to win in a thriving deal market Value over volume The drivers of health care M&A in 2017 Gregory Park Partner, US Health Transaction Advisory
RE: Additional Input regarding Accountable Care Organizations (ACOs) and the Medicare Shared Saving Program
 221 MAIN STREET, SUITE 1500 SAN FRANCISCO, CA 94105 PBGH.ORG OFFICE 415.281.8660 FACSIMILE 415.520.0927 February 14, 2011 Donald M. Berwick, M.D. Administrator Centers for Medicare and Medicaid Services
221 MAIN STREET, SUITE 1500 SAN FRANCISCO, CA 94105 PBGH.ORG OFFICE 415.281.8660 FACSIMILE 415.520.0927 February 14, 2011 Donald M. Berwick, M.D. Administrator Centers for Medicare and Medicaid Services
Initiative Options for Simulation Scenarios
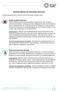 Initiative Options for Simulation Scenarios The following options are in version 2h of the ReThink Health simulation model. Enable healthier behaviors Promote healthy behavior and help people to stop behaviors
Initiative Options for Simulation Scenarios The following options are in version 2h of the ReThink Health simulation model. Enable healthier behaviors Promote healthy behavior and help people to stop behaviors
Improving Innovation in Health Services Through Better Payment Reforms
 Improving Innovation in Health Services Through Better Payment Reforms FDA & Health James C. Capretta The views expressed are those of the author in his personal capacity and not in his official/professional
Improving Innovation in Health Services Through Better Payment Reforms FDA & Health James C. Capretta The views expressed are those of the author in his personal capacity and not in his official/professional
Catalyzing Payment Innovation. Suzanne Delbanco, Ph.D. Executive Director September 20, 2012
 Catalyzing Payment Innovation Suzanne Delbanco, Ph.D. Executive Director September 20, 2012 Payment Reform: Why Should We Care? The health care payment systems of the status quo continue to drain the value
Catalyzing Payment Innovation Suzanne Delbanco, Ph.D. Executive Director September 20, 2012 Payment Reform: Why Should We Care? The health care payment systems of the status quo continue to drain the value
Stakeholder Innovation Group (SIG):
 Stakeholder Innovation Group (SIG): Intake Form for New Payment Model Idea that Requires State/Federal Approval (to be added to the Innovations Website) Purpose: The purpose of this form is to collect
Stakeholder Innovation Group (SIG): Intake Form for New Payment Model Idea that Requires State/Federal Approval (to be added to the Innovations Website) Purpose: The purpose of this form is to collect
