Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request.
|
|
|
- Kory Russell
- 6 years ago
- Views:
Transcription
1 Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request Updated: June 2016
2 Important Note: Any specific member/provider data has been redacted for this training tool. 2
3 Topics Covered: Long Form: Steps 1 and 2 Overview page 4 Long Form: Step 2 > Filing COB (aka Secondary) Claims page 7 Long Form: Other attributes page 15 Long Form: Steps 3 and 4 Overview page 19 Long Form: The most common error messages for COB claims page 22 Submitting Corrected or Void Claims page 24 When to use the Corrected Claim option vs the Claim Adjustment Request feature page 27 3
4 LONG FORM: STEPS 1 AND 2 OVERVIEW 4
5 Claim Entry > Long Form Overview and Step 1 The Long Form is presented when a user identifies in Step 1 that any of the following elements are needed: More than 5 dates of service COB Details Claim notes Paperwork attachments If the claim includes any of those elements, the User would click Yes (default is No ). User would also fill out the other fields as required to get to any of the claim forms, then clicks the Proceed to Step 2 button. 5
6 Long Form Overview and Step 2 The Long Form brings up a claim similar to the Short Form, with the addition of several sections: 1. Is there another health benefit plan? If yes is checked, then several more fields will display 2. Notes Claim Level 3. Paperwork Attachment Claim Level Lines of Service
7 LONG FORM: STEP 2 > FILING COB (aka Secondary) CLAIMS 7
8 Long Form Step 2 > COB Details If Yes is chosen as the answer to Is there another health benefit plan? it will result in additional fields being displayed: Other Insured, Coordination of Benefits, Medicare Outpatient adjudication, and COB Claim Adjustments. Please note: By filling in these sections, the primary EOB/statement does NOT need to be submitted separately. 8
9 Long Form Step 2 > COB Details > Other Insured For all COB claims, the Other Insured section must be filled out. The orange highlighted sections are required fields. Payer ID is typically a 5-digit # used for electronic claim submission, but can be any other identifying number specific to that insurance. Insurance Type has a dropdown of many options including: Preferred Provider Org BCBS Medicare 9
10 Long Form Step 2 > COB Details > Coord of Benefits The Coordination of Benefits section details payment info from the primary insured and would be found on the primary EOB/PRA: Claim adjudication date (date claim was paid) COB payer paid amount (amount paid by primary if nothing paid, then this should be left blank or listed as 0.00) Remaining patient liability (auto-populates from amount(s) entered in COB Claim Adjustments section) 10
11 Long Form Step 2 > COB Details > MOA If the Insurance Type is Medicare, this section needs to be completed. Primary claims that have been processed through Medicare need to have additional information provided, all of which can be retrieved from the Medicare EOB: Payable percent (if one is indicated) Payable amount Non-payable amount Remark code(s) Please note: Required fields vary depending on information submitted in other areas. If a required field is not completed, Provider Express messaging will inform you prior to submitting the claim. 11
12 Long Form Step 2 > COB Details > COB Claim Adjs Finally, COB Claim Adjustments would be added to the mix, whether at a Claim Level (completed in the upper section of the form) or at a Line Level (completed for each line of service entered at the bottom of the form). This section would be used to identify the unpaid portions of the claim, including patient responsibility, all info coming from the primary EOB. Group code would be chosen: CO-Contractual Obligation CR-Correction and Reversals OA-Other Adjustments PI-Payer Initiated Reductions (e.g. non-allowed) PR-Patient Responsibility (e.g. copay, coinsurance, deductible) Reason code (reason amount was not paid code should be on EOB, but Provider Express offers a lookup option) Adjustment amount (the amount not covered by the Primary Payer) Clicking Add will allow multiple adjustments to be entered, if necessary. IMPORTANT: Do not duplicate Reason codes if filing at a Claim Level. Add up all amounts and note the quantity if that code involves more than one DOS. 12
13 Long Form Step 2 > Filing Adjustments at Claim Level When filing adjustments, you have the option to file them at a Claim Level or at a Line Level. Filing adjustments at a Claim Level is most effective when there is only one DOS on the claim, or if all adjustment reasons and amounts are the same. If filing at a Claim Level for multiple DOS and multiple codes, you need to file one line per code, otherwise the claim will reject, which will delay processing. CORRECT INCORRECT 13
14 Long Form Step 2 > Filing Adjustments at a Line Level The Line Level option offers the most accurate portrayal of how the primary payer processed the claim, and allows you to enter multiple codes and/or amounts, based on a specific date of service. Just click on the COB box to the right of each date of service that requires an adjustment. 14
15 LONG FORM: OTHER ATTRIBUTES 15
16 Long Form Step 2 > Notes Claim Level Additional information, descriptive types of detail that need to be added to a claim can now be done using the Notes Claim Level field. User would choose one of the four Reference Codes: Additional Information Certification Narrative Goals, Rehab Potential, or Discharge Plans Diagnosis Description Then add text in the Reference Text field with the necessary information. 16
17 Long Form Step 2 > Paperwork Attachment Sometimes paperwork needs to be included for a claim to be processed correctly. Choose the Report Type Code from the dropdown list Examples: Progress Notes, Drug/ Lab Reports, Admit Summary Choose the Report Transmission Code from the dropdown list Examples: By mail, , By Fax User would enter the Report control number found on the actual report (this is so claims can reference the report and match it up to the correct claim) Please note: a paperwork attachment cannot be attached to the claim itself via Provider Express this section is only used to note to Claims that paperwork is available and/or forthcoming via the transmission method noted. 17
18 Long Form Step 2 > Entering info at a line level The previous pages showed how to enter Paperwork, Notes and COB info at a full claim level. The same info can be entered for one or more specific dates of service instead, indicating a line level entry. To the right of each line of service are three options: PWK = paperwork NTE = notes COB = coordination of benefits (adjustment info only) When any of these options are checked, fields will drop down below that will need to be completed. It is not necessary to enter any of these sections at both the full claim AND line levels. Please note: for COB, the upper portions of the form, including the Other Insured and the Coordination of Benefits sections, will still need to be completed. The COB section at this line level only indicates the COB Claim Adjustments info. 18
19 LONG FORM: STEPS 3 AND 4 OVERVIEW 19
20 Long Form Step 3 As with any claim submitted online, once the necessary fields are filled out, user would click the preview button in the lower right portion of the claim form. Any errors found will be noted and must be corrected before the claim can be submitted. If there are no errors found, user can then click the Submit this Claim button to submit the claim. 20
21 Long Form Step 4 Once the claim is submitted, user will receive a Confirmation Number, which can be used to reference the status of the claim online via My Provider Express > My Submitted Claims. 21
22 LONG FORM: THE MOST COMMON ERROR MESSAGE FOR COB (SECONDARY) CLAIMS 22
23 The Most Common Error Messages for COB Claims Total charges must equal the sum of COB payer paid amount and all Claim adjustment amounts. This means that the total charge for the date(s) of service entered should ONLY equal what the COB payer paid amount and Remaining patient liability amounts total. In other words, do not enter any amounts that were disallowed/written off by the primary payer, unless you entered an adjustment for them. 23
24 SUBMITTING CORRECTED (OR VOID) CLAIMS 24
25 Submitting Corrected (or Void) Claims Regardless of the claim form (short or long), you do have the ability to submit a corrected or void claim request as well, when a previouslysubmitted claim had incorrect information on it. In the Service info section, the Claim frequency code is what is used to determine the type of claim you are filing. Provider Express defaults to Original but you can change it to Corrected or Void. 25
26 Submitting Corrected (or Void) Claims As the help icon next to this section indicates: Claim frequency - To submit a Corrected or Void claim, you will need to enter the Claim Number found on the claim record in Claim Inquiry. The claim number will also be reported on the paper remittance advice or electronic 835 file. You can not submit a Corrected or Void claim until a claim number has been assigned. Payer control number = Claim number 26
27 WHEN TO USE THE CORRECTED CLAIM OPTION VIA CLAIM ENTRY vs. THE CLAIM ADJUSTMENT REQUEST FEATURE VIA CLAIM INQUIRY 27
28 Submitting Corrected Claim vs Claim Adjustment Q: When should I submit a corrected claim via Claim Entry vs an adjustment via Claim Inquiry? A: Use the following guidelines to help in your decision: If the issue with the claim was because of a problem in how it was originally filed by the provider/group that now needs to be corrected, submit a corrected claim via Claim Entry (see pg 25) e.g. filing an incorrect procedure code; forgetting a modifier If the issue with the claim was because of an alleged problem in how Optum processed it, submit an adjustment request via Claim Inquiry e.g. processing against member s deductible when it was already met; noting an auth was required when there is an auth on file (please reference the Guided Tour video titled Claim Inquiry and Claim Adjustment Request for additional information) 28
29 Please contact Provider Express Live Chat (via Tech Support on the Contact Us page) if you need further assistance. Thank You!
Filing Secondary Claims on Provider Express
 Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Medicare Part B Crossover Claim Submission User Guide
 Thank you for using MDH s newest web application to process your Medicare Part B Crossover Claims. Each claim you file is official and will supersede any paper claim you may have filed within the past
Thank you for using MDH s newest web application to process your Medicare Part B Crossover Claims. Each claim you file is official and will supersede any paper claim you may have filed within the past
Companion Guide for the X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC
 Companion Guide for the 005010X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Name TR3 Values Notes Delimiter: Data
Companion Guide for the 005010X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Name TR3 Values Notes Delimiter: Data
Claims adjustments Adjustment codes and coordination of benefits (COB)
 Claims adjustments Adjustment codes and coordination of benefits (COB) 23.03.522.1 H (9/17) aetna.com Electronic submission of adjustment group codes and claims adjustment reason codes Aetna is the brand
Claims adjustments Adjustment codes and coordination of benefits (COB) 23.03.522.1 H (9/17) aetna.com Electronic submission of adjustment group codes and claims adjustment reason codes Aetna is the brand
Secondary Claim Reporting Considerations
 Secondary Claim Reporting Considerations Question: How is the 005010X221 Health Care Claim Payment/Advice (835) supposed to be populated by a non-primary payer when one or more other payers have already
Secondary Claim Reporting Considerations Question: How is the 005010X221 Health Care Claim Payment/Advice (835) supposed to be populated by a non-primary payer when one or more other payers have already
Kansas Medical Assistance Program. Vertical Perspective. Other Insurance/Medicare Training Packet - Professional
 Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
Entering Payments in Aprima PRM
 Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
UB-04 Billing Instructions
 UB-04 Billing Instructions Updated October 2016 The UB-04 is a claim form that is utilized for Hospital Services and select residential services. Please note that these instructions are specifically written
UB-04 Billing Instructions Updated October 2016 The UB-04 is a claim form that is utilized for Hospital Services and select residential services. Please note that these instructions are specifically written
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
Provider Healthcare Portal Demonstration:
 Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
CREATING SECONDARY CLAIMS IN SERVICE CENTER
 CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
Network Health Claims Editing Portal
 Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
XPressClaim Help. Diagnosis 1,2,3,etc. Enter the number(s) of the corresponding diagnosis code(s) that applies to this service.
 Keying Information Professional Claims CMS 1500 Claim type Please select the type of claim: 1- Original claim 7- Replacement of prior claim Please note: 7- Replacement of prior claim should only be selected
Keying Information Professional Claims CMS 1500 Claim type Please select the type of claim: 1- Original claim 7- Replacement of prior claim Please note: 7- Replacement of prior claim should only be selected
3. The Health Plan accepts the standard current billing forms: the CMS 1500 (02/12) form and the UB- 04 hospital billing forms.
 BILLING PROCEDURES SECTION 11 Billing Procedures 1. All claims should be submitted to: The Health Plan 1110 Main St Wheeling WV 26003 Claim forms must be completed in their entirety. The efficiency with
BILLING PROCEDURES SECTION 11 Billing Procedures 1. All claims should be submitted to: The Health Plan 1110 Main St Wheeling WV 26003 Claim forms must be completed in their entirety. The efficiency with
Rev 7/20/2015. ClaimsConnect Rejection Guide
 ClaimsConnect Rejection Guide Helper Client, The purpose of this document is to assist you in accelerating the resolution of claim rejections. We have identified the most frequent rejection messages, and
ClaimsConnect Rejection Guide Helper Client, The purpose of this document is to assist you in accelerating the resolution of claim rejections. We have identified the most frequent rejection messages, and
Facility Instruction Manual:
 Facility Instruction Manual: Submitting Secondary Claims with COB Data Elements Overview This supplement to the billing section of the Passport Health Plan (PHP) Provider Manual provides specific coding
Facility Instruction Manual: Submitting Secondary Claims with COB Data Elements Overview This supplement to the billing section of the Passport Health Plan (PHP) Provider Manual provides specific coding
Claims Claim Submission QUICK REFERENCE
 Claims Claim Submission QUICK REFERENCE This will review the process of how to submit a claim online and check the status of a previously submitted claim. Get Started 1. From, click Link and sign in NOTE:
Claims Claim Submission QUICK REFERENCE This will review the process of how to submit a claim online and check the status of a previously submitted claim. Get Started 1. From, click Link and sign in NOTE:
PC-ACE Claim Management
 This document is a guide to assist PC-ACE users in entering and managing Durable Medical Equipment (DME) claim information. This document includes: Claim Entry... 2 Managing Claims... 15 Preparing to Send
This document is a guide to assist PC-ACE users in entering and managing Durable Medical Equipment (DME) claim information. This document includes: Claim Entry... 2 Managing Claims... 15 Preparing to Send
Amazing Charts PM Billing & Clearinghouse Portal
 Amazing Charts PM Billing & Clearinghouse Portal Agenda Charge Review Charge Entry Applying Patient Payments Claims Management Claim Batches Claim Reports Resubmitting Claims Reviewing claim batches in
Amazing Charts PM Billing & Clearinghouse Portal Agenda Charge Review Charge Entry Applying Patient Payments Claims Management Claim Batches Claim Reports Resubmitting Claims Reviewing claim batches in
Troubleshooting 999 and 277 Rejections. Segments
 Troubleshooting 999 and 277 Rejections Segments NM103 - last name or group name NM104 - first name NM105 - middle initial NM109 - usually specific information tied to that company/providers/subscriber/patient
Troubleshooting 999 and 277 Rejections Segments NM103 - last name or group name NM104 - first name NM105 - middle initial NM109 - usually specific information tied to that company/providers/subscriber/patient
CHAPTER 9: CLAIM AND BILLING INFORMATION
 CHAPTER 9: CLAIM AND BILLING INFORMATION UNIT 2: THE REMITTANCE ADVICE IN THIS UNIT TOPIC SEE PAGE 9.2 THE REMITTANCE ADVICE 2 9.2 DETAIL REPORT: DATA ELEMENT DESCRIPTIONS 6 9.2 DETAIL REPORT: CLAIM ADJUSTMENT
CHAPTER 9: CLAIM AND BILLING INFORMATION UNIT 2: THE REMITTANCE ADVICE IN THIS UNIT TOPIC SEE PAGE 9.2 THE REMITTANCE ADVICE 2 9.2 DETAIL REPORT: DATA ELEMENT DESCRIPTIONS 6 9.2 DETAIL REPORT: CLAIM ADJUSTMENT
Secondary Claims 07/10/2017 1
 Secondary Claims 07/10/2017 1 Example of an MSP Claim (Professional-Processed at Service Line Level) The LOB selected will be the line of business you are submitting to for this claim. Must select Y for
Secondary Claims 07/10/2017 1 Example of an MSP Claim (Professional-Processed at Service Line Level) The LOB selected will be the line of business you are submitting to for this claim. Must select Y for
Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide
 Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide Version 5.0 February 26, 2007 Revision History Document Version Date Name Comments 1.0 12/27/2006 Patti George Created. 2.0
Commonwealth of Kentucky KyHealth Choices KyHealth Net Dental Companion Guide Version 5.0 February 26, 2007 Revision History Document Version Date Name Comments 1.0 12/27/2006 Patti George Created. 2.0
Prescriber Web Prior Authorization
 Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
eauthorization Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with
 Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
Providers e-authorization Application on eclaimlink SEPTEMBER 2016 in partnership with www.eclaimlink.ae 1 Table of Contents Getting Started 3 Registration 4 Logging In 5 Prior Request Form 6 Eligibility
UB04 Billing Instructions
 UB04 Billing Instructions T h e U B 0 4 i s a f o r m t h a t i s u s e d t o b i l l i n s t i t u t i o n a l c l a i m s f o r h o s p i t a l and select residential services. T h i s m a n u a l g
UB04 Billing Instructions T h e U B 0 4 i s a f o r m t h a t i s u s e d t o b i l l i n s t i t u t i o n a l c l a i m s f o r h o s p i t a l and select residential services. T h i s m a n u a l g
EXPLANATION OF REMITTANCE ADVICE DETAIL REPORT HEADINGS
 EXPLANATION OF REMITTANCE ADVICE DETAIL REPORT HEADINGS First Line PAT CONTROL NUMBER Patient Control Number PATIENT LNAME Patient Last Name FIRST Patient First name A Accommodation Code 1 SER FROM Service
EXPLANATION OF REMITTANCE ADVICE DETAIL REPORT HEADINGS First Line PAT CONTROL NUMBER Patient Control Number PATIENT LNAME Patient Last Name FIRST Patient First name A Accommodation Code 1 SER FROM Service
837I Institutional Health Care Claim - for Encounters
 Companion Document 837I - Encounters 837I Institutional Health Care Claim - for Encounters Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care
Companion Document 837I - Encounters 837I Institutional Health Care Claim - for Encounters Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care
Version 1/Revision 18 Page 1 of 36. epaces Professional Claim REFERENCE GUIDE
 Version 1/Revision 18 Page 1 of 36 Table of Contents GENERAL CLAIM INFORMATION TAB... 3 PROFESSIONAL CLAIM INFORMATION TAB... 5 PROVIDER INFORMATION TAB... 10 DIAGNOSIS TAB... 12 OTHER PAYERS TAB... 13
Version 1/Revision 18 Page 1 of 36 Table of Contents GENERAL CLAIM INFORMATION TAB... 3 PROFESSIONAL CLAIM INFORMATION TAB... 5 PROVIDER INFORMATION TAB... 10 DIAGNOSIS TAB... 12 OTHER PAYERS TAB... 13
HNS CMS Claim Checklist
 HNS CMS 1500 - Claim Checklist Prior to submitting paper claims, please carefully check your completed claim form against this checklist. Please contact your HNS Service Representative if you have any
HNS CMS 1500 - Claim Checklist Prior to submitting paper claims, please carefully check your completed claim form against this checklist. Please contact your HNS Service Representative if you have any
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Claims Management and Insurance Follow-Up Reports
 Claims Management and Insurance Follow-Up Reports Insurance Collection Reporting A. Insurance Control Summary 1. Description: 2. Purpose: a) Report used to view all claims generated for a given run. b)
Claims Management and Insurance Follow-Up Reports Insurance Collection Reporting A. Insurance Control Summary 1. Description: 2. Purpose: a) Report used to view all claims generated for a given run. b)
Connecticut Medical Assistance Program Workshop Web Claim Submission
 Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Connecticut Medical Assistance Program Workshop Web Claim Submission Presented by The Department of Social Services & HP for Billing Providers Training Topics Web Claim Submission Benefits Access to Claim
Companion Guide for the X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC
 Companion Guide for the 005010X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Description TR3 Values Notes Delimiter:
Companion Guide for the 005010X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Description TR3 Values Notes Delimiter:
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
eclinicalworks Training Eligibility Tool
 eclinicalworks Training Eligibility Tool The ADI eclinicalworks database utilizes the Navicure clearinghouse for all eligibility and benefits queries. Eligibility is scheduled to run each night for the
eclinicalworks Training Eligibility Tool The ADI eclinicalworks database utilizes the Navicure clearinghouse for all eligibility and benefits queries. Eligibility is scheduled to run each night for the
Billing Medicare Secondary Payer (MSP) Claims
 Billing Medicare Secondary Payer (MSP) Claims Per CR8486 effective 1/1/2016 MSP claims for Medicare Part A will be accepted via DDE. Review MM8486 for detailed instructions (https://www.cms.gov/outreach-and-education/medicare-learning-network-
Billing Medicare Secondary Payer (MSP) Claims Per CR8486 effective 1/1/2016 MSP claims for Medicare Part A will be accepted via DDE. Review MM8486 for detailed instructions (https://www.cms.gov/outreach-and-education/medicare-learning-network-
Home Health Medicare Secondary Payer Claims
 Home Health Medicare Secondary Payer Claims Attention: Per CR8486 effective January 1, 2016 MSP claims for Medicare Part A will be accepted via DDE. MM8486 (https://www.cms.gov/outreach-and-education/medicare-
Home Health Medicare Secondary Payer Claims Attention: Per CR8486 effective January 1, 2016 MSP claims for Medicare Part A will be accepted via DDE. MM8486 (https://www.cms.gov/outreach-and-education/medicare-
Practice Express 3.0 Update September 25, 2006
 Alpha Inquiry Change Patient (Patient File Maintenance) Added new field: Cell Phone#. It is on the right directly below Work Phone Ext. New feature: Contact Information. You now have the capability of
Alpha Inquiry Change Patient (Patient File Maintenance) Added new field: Cell Phone#. It is on the right directly below Work Phone Ext. New feature: Contact Information. You now have the capability of
837 Institutional Health Care Claim. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Seg Loop Name TR3 Values Notes Delimiter: Data Element. (:) Colon Separator
 Companion Guide for the 005010X223A1 Health Care Claim: Institutional (837I) Lines of Business: Private Business, 65C Plus, QUEST, Blue Card, FEP, Away From Home Care Delimiter: Data Element (*) Asterisk
Companion Guide for the 005010X223A1 Health Care Claim: Institutional (837I) Lines of Business: Private Business, 65C Plus, QUEST, Blue Card, FEP, Away From Home Care Delimiter: Data Element (*) Asterisk
WEDI SNIP Claredi EDI Edit Description Claim Type 837P 837I. 1 H10006 Value is too long X X
 EDI Claim Edits UnitedHealthcare applies Health Insurance Portability and Accountability Act (HIPAA) edits for professional (837p) and institutional (837i) claims submitted electronically. Enhancements
EDI Claim Edits UnitedHealthcare applies Health Insurance Portability and Accountability Act (HIPAA) edits for professional (837p) and institutional (837i) claims submitted electronically. Enhancements
Secondary Professional Claims on the HCFA-1500
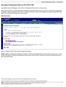 Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
New MN ITS Direct Data Entry (DDE) Screens Professional (837P)
 New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
New MN ITS Direct Data Entry (DDE) Screens Professional (837P) This handout is intended to accompany the MN ITS DDE Professional 837P Training Webinar session. It is not intended to replace the MN-ITS
PATIENT ACCOUNTING TRAINING
 PATIENT ACCOUNTING TRAINING Most collection activity will occur in SMS Patient Accounting. However, any changes to patient demographics or insurance will need to be done in Cerner PMOffice. Demographic
PATIENT ACCOUNTING TRAINING Most collection activity will occur in SMS Patient Accounting. However, any changes to patient demographics or insurance will need to be done in Cerner PMOffice. Demographic
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM
 HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
Why is change necessary? One of the biggest changes in the healthcare industry is technology which allows fast and accurate service to customers.
 1 Why is change necessary? One of the biggest changes in the healthcare industry is technology which allows fast and accurate service to customers. It is because of these technological advances we are
1 Why is change necessary? One of the biggest changes in the healthcare industry is technology which allows fast and accurate service to customers. It is because of these technological advances we are
Health Information Technology and Management
 Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
Availity ' Eligibility and Benefits SM'
 Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
Booklet on Advisory Issued for Taxpayers. Table of Contents
 Table of Contents 1. Advisory about Invoice Upload in GSTR 2... 2 2. Advisory about accepting missed invoices in GSTR 1A and paying the liability in the same month.... 3 3. Advisory on discrepancy between
Table of Contents 1. Advisory about Invoice Upload in GSTR 2... 2 2. Advisory about accepting missed invoices in GSTR 1A and paying the liability in the same month.... 3 3. Advisory on discrepancy between
Quick Guide to Secondary Claims
 Quick Guide to Secondary Claims Would you like to: Please click below what you would like help with to be directed to that specific section in this guide. Convert your primary claim to a secondary claims
Quick Guide to Secondary Claims Would you like to: Please click below what you would like help with to be directed to that specific section in this guide. Convert your primary claim to a secondary claims
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
NCPDP Version 5 Request Payer Sheet
 NCPDP Version 5 Request Payer Sheet NCPDP Rev.04.16.02 General Information Payer Name: 4-D Pharmacy Benefits Plan Name/Group Name: 4-D Pharmacy Benefits Processor: Argus Payer Sheet Revision Effective
NCPDP Version 5 Request Payer Sheet NCPDP Rev.04.16.02 General Information Payer Name: 4-D Pharmacy Benefits Plan Name/Group Name: 4-D Pharmacy Benefits Processor: Argus Payer Sheet Revision Effective
P R O V I D E R B U L L E T I N B T J U N E 1,
 P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
837 Institutional Health Care Claim Outbound. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Third Party Administrator (TPA) Guide to CONNECT
 Third Party Administrator (TPA) Guide to CONNECT TABLE OF CONTENTS Table of Contents... 2 1. Introduction... 3 1.1 Guide Instructions... 3 1.2 CONNECT System Overview... 3 2. Navigate CONNECT as a TPA...
Third Party Administrator (TPA) Guide to CONNECT TABLE OF CONTENTS Table of Contents... 2 1. Introduction... 3 1.1 Guide Instructions... 3 1.2 CONNECT System Overview... 3 2. Navigate CONNECT as a TPA...
Submitting Secondary Claims with COB Data Elements - Facilities
 Overview Submitting Secondary Claims with COB Data Elements - Facilities This supplement to the billing section of the AmeriHealth Caritas Pennsylvania Claims Filing Instruction Manual provides specific
Overview Submitting Secondary Claims with COB Data Elements - Facilities This supplement to the billing section of the AmeriHealth Caritas Pennsylvania Claims Filing Instruction Manual provides specific
Research and Resolve UB-04 Claim Denials. HP Provider Relations/October 2014
 Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Archived SECTION 17 - CLAIMS DISPOSITION. Section 17 - Claims Disposition
 SECTION 17 - CLAIMS DISPOSITION 17.1 ACCESS TO REMITTANCE ADVICES...2 17.2 INTERNET AUTHORIZATION...3 17.3 ON-LINE HELP...3 17.4 REMITTANCE ADVICE...3 17.5 CLAIM STATUS MESSAGE CODES...7 17.5.A FREQUENTLY
SECTION 17 - CLAIMS DISPOSITION 17.1 ACCESS TO REMITTANCE ADVICES...2 17.2 INTERNET AUTHORIZATION...3 17.3 ON-LINE HELP...3 17.4 REMITTANCE ADVICE...3 17.5 CLAIM STATUS MESSAGE CODES...7 17.5.A FREQUENTLY
ADJ. SYSTEM FLD LEN. Min. Max.
 Loop Loop Repeat Segme nt Element Id Description X12 Page No. ID Min. Max. ADJ. SYSTEM FLD LEN Usage Req. ANSI VALUES COMMENTS 1 ISA Interchange Control Header B.3 1 R ISA08 Interchange Receiver ID AN
Loop Loop Repeat Segme nt Element Id Description X12 Page No. ID Min. Max. ADJ. SYSTEM FLD LEN Usage Req. ANSI VALUES COMMENTS 1 ISA Interchange Control Header B.3 1 R ISA08 Interchange Receiver ID AN
CPT is a registered trademark of the American Medical Association.
 Welcome to s Webinar and Audio Conference Training. We hope that the information contained herein will give you valuable tips that you can use to improve your skills and performance on the job. Each year,
Welcome to s Webinar and Audio Conference Training. We hope that the information contained herein will give you valuable tips that you can use to improve your skills and performance on the job. Each year,
Medical Eligibility & Benefits Lookup Tips
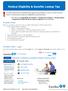 Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Medical Eligibility & Benefits Lookup Tips Excellus BlueCross BlueShield requires providers to use its self-service tools to determine patient eligibility and benefits. Provider Portal Note: Please see
Best Practice Recommendation for
 Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Best Practice Recommendation for. Processing & Reporting Remittance Information ( v) Version 3.93
 Best Practice Recommendation for Processing & Reporting Remittance Information (835 5010v) Version 3.93 For use with ANSI ASC X12N 835 (005010X222) Health Care Claim Payment/Advice Technical Report Type
Best Practice Recommendation for Processing & Reporting Remittance Information (835 5010v) Version 3.93 For use with ANSI ASC X12N 835 (005010X222) Health Care Claim Payment/Advice Technical Report Type
CLAIM ADJUDICATION CODES AND ACTION
 1 45 Adjusted - Above contract rate Post payment and any adjustment to charges. Do not refile. 2 92 Approved Post payment and any adjustment to charges. Do not refile. 3 198 Authed units exceeded Verify
1 45 Adjusted - Above contract rate Post payment and any adjustment to charges. Do not refile. 2 92 Approved Post payment and any adjustment to charges. Do not refile. 3 198 Authed units exceeded Verify
Coordination of Benefits (COB) Claims Submission Guide
 Coordination of Benefits (COB) Claims Submission Guide Coordination of benefits applies to members who have coverage with more than one health care plan and helps to ensure that these members receive benefits
Coordination of Benefits (COB) Claims Submission Guide Coordination of benefits applies to members who have coverage with more than one health care plan and helps to ensure that these members receive benefits
UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION
 CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
Axium: Entering Insurance
 Axium: Entering Insurance To enter insurance in Axium follow the directions below: Is the Patient the Policy Holder? If so, we need to indicate this! (Front Desk Primary Responsibility) 1. Select the Patient.
Axium: Entering Insurance To enter insurance in Axium follow the directions below: Is the Patient the Policy Holder? If so, we need to indicate this! (Front Desk Primary Responsibility) 1. Select the Patient.
Guide to Credit Card Processing
 CBS ACCOUNTS RECEIVABLE Guide to Credit Card Processing version 2007.x.x TL 25476 (07/27/12) Copyright Information Text copyright 1998-2012 by Thomson Reuters. All rights reserved. Video display images
CBS ACCOUNTS RECEIVABLE Guide to Credit Card Processing version 2007.x.x TL 25476 (07/27/12) Copyright Information Text copyright 1998-2012 by Thomson Reuters. All rights reserved. Video display images
Transition Slide. Presenter(s): Topic. Level. Dave Roughen Project Manager Kay Thorpe EDI Analyst. Ron Burke Dental Product Manager
 Topic Level Presenter(s): Dave Roughen Project Manager Kay Thorpe EDI Analyst Transition Slide Ron Burke Dental Product Manager Dave Roughen Project Manager Improving Reimbursements through effective Claims
Topic Level Presenter(s): Dave Roughen Project Manager Kay Thorpe EDI Analyst Transition Slide Ron Burke Dental Product Manager Dave Roughen Project Manager Improving Reimbursements through effective Claims
Appendix 3A. MA Companion Guide: CMS Supplemental Instructions for EDR and CRR Data Elements
 Appendix 3A. MA Companion Guide: CMS Supplemental Instructions for EDR and CRR Data s A3A.1 LOOPS AND SEGMENTS APPLIED TO EDR AND CRR SUBMISSIONS... 3 A3A.2 CONTROL SEGMENTS: CMS SUPPLEMENTAL INSTRUCTIONS
Appendix 3A. MA Companion Guide: CMS Supplemental Instructions for EDR and CRR Data s A3A.1 LOOPS AND SEGMENTS APPLIED TO EDR AND CRR SUBMISSIONS... 3 A3A.2 CONTROL SEGMENTS: CMS SUPPLEMENTAL INSTRUCTIONS
Eligibility Troubleshooting 101
 Eligibility Troubleshooting 101 Reference Guide Contents Introduction... 3 Invalid/Missing Search Criteria... 3 Invalid/Missing Subscriber/Insured Name... 3 Resubmit... 5 Patient vs. Subscriber... 7 Invalid
Eligibility Troubleshooting 101 Reference Guide Contents Introduction... 3 Invalid/Missing Search Criteria... 3 Invalid/Missing Subscriber/Insured Name... 3 Resubmit... 5 Patient vs. Subscriber... 7 Invalid
web-denis resources Getting to web-denis resources Log in to web-denis. You ll need your password. Click BCN Provider Publications and Resources.
 web-denis resources Getting to web-denis resources Log in to web-denis. You ll need your password. Click BCN Provider Publications and Resources. 1 web-denis resources web-denis Behavioral Health page
web-denis resources Getting to web-denis resources Log in to web-denis. You ll need your password. Click BCN Provider Publications and Resources. 1 web-denis resources web-denis Behavioral Health page
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2012-2013 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 1 of 8 Year 2012-2013 Summary
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2012-2013 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 1 of 8 Year 2012-2013 Summary
The claims will appear on the list in order of Date Created. The search criteria at the top of the list will assist you in locating past claims.
 P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
P r a c t i c e M a t e M a n u a l 63 CLAIMS/BILLING TAB Your claim submissions are managed in the Claims/Billing Tab. Claims can be printed, deleted, submitted or unsubmitted here, and rejected or failed
Coordination of Benefits (COB) Professional
 Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
New MN ITS Direct Data Entry (DDE) Screens Institutional (837I)
 New MN ITS Direct Data Entry (DDE) Screens Institutional (837I) This handout is intended to accompany the MN ITS DDE Institutional (837I) Training Webinar session. It is not intended to replace the MN-ITS
New MN ITS Direct Data Entry (DDE) Screens Institutional (837I) This handout is intended to accompany the MN ITS DDE Institutional (837I) Training Webinar session. It is not intended to replace the MN-ITS
Archived SECTION 15-BILLING INSTRUCTIONS. Section 15 - Billing Instructions
 SECTION 15-BILLING INSTRUCTIONS 15.1 ELECTRONIC DATA INTERCHANGE... 2 15.2 INTERNET ELECTRONIC CLAIM SUBMISSION... 2 15.3 CMS-1500 CLAIM FORM... 3 15.4 PROVIDER COMMUNICATION UNIT... 3 15.5 RESUBMISSION
SECTION 15-BILLING INSTRUCTIONS 15.1 ELECTRONIC DATA INTERCHANGE... 2 15.2 INTERNET ELECTRONIC CLAIM SUBMISSION... 2 15.3 CMS-1500 CLAIM FORM... 3 15.4 PROVIDER COMMUNICATION UNIT... 3 15.5 RESUBMISSION
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2011-2012 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year 2011-2012 Summary of
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2011-2012 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year 2011-2012 Summary of
Full Intake Form Financial Information
 1. Financial Information A. Number in Household a. Enter the Number of People 18 and Over b. Enter the Number of People Under 18 2. Household Income B C D E A F G A applicant name (will already be filled
1. Financial Information A. Number in Household a. Enter the Number of People 18 and Over b. Enter the Number of People Under 18 2. Household Income B C D E A F G A applicant name (will already be filled
Claim Preparation and Filing Overview for U.S.
 Claim Preparation and Filing Overview for U.S. During the course of a patient visit, invoices will be created by various staff within the office. It is recommended that when an insurance invoice is created
Claim Preparation and Filing Overview for U.S. During the course of a patient visit, invoices will be created by various staff within the office. It is recommended that when an insurance invoice is created
837I Institutional Health Care Claim
 Section 2B 837I Institutional Health Care Claim Companion Document Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care transaction for Institutional
Section 2B 837I Institutional Health Care Claim Companion Document Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care transaction for Institutional
LTC/MMA Monthly Claims Training Prior Authorization Submission
 LTC/MMA Monthly Claims Training Prior Authorization Submission Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to: Molina
LTC/MMA Monthly Claims Training Prior Authorization Submission Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to: Molina
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
837 Institutional Health Care Claim. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES MENTAL HEALTH AND SUBSTANCE ABUSE PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES MENTAL HEALTH AND SUBSTANCE ABUSE PLAN 2010-2011 Call APS Healthcare, Inc. Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES MENTAL HEALTH AND SUBSTANCE ABUSE PLAN 2010-2011 Call APS Healthcare, Inc. Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Claim Form Billing Instructions UB-04 Claim Form
 Claim Form Billing Instructions UB-04 Claim Form Presbyterian Health Plan / Presbyterian Insurance Company, Inc 02/19/08 Page 1 of 5 Presbyterian Health Plan / Presbyterian Insurance Company, Inc 02/19/08
Claim Form Billing Instructions UB-04 Claim Form Presbyterian Health Plan / Presbyterian Insurance Company, Inc 02/19/08 Page 1 of 5 Presbyterian Health Plan / Presbyterian Insurance Company, Inc 02/19/08
Charge Entry Physician Billing. Module 5
 Charge Entry Physician Billing Module 5 Table of Contents Accessing the Batch Control Screen... 3 Create a New Batch... 4 Querying for an Existing Batch... 7 Posting Transactions... 7 Step by Step on how
Charge Entry Physician Billing Module 5 Table of Contents Accessing the Batch Control Screen... 3 Create a New Batch... 4 Querying for an Existing Batch... 7 Posting Transactions... 7 Step by Step on how
Using ERAs with Helper
 Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
UB-04 Billing Instructions for Hemodialysis Claims
 UB-04 Billing Instructions for Hemodialysis Claims 1 Provider Name, Address, Telephone # 2 Pay to Name/Address/ID Required. Enter the name and address of the facility Situational. Enter the name, address,
UB-04 Billing Instructions for Hemodialysis Claims 1 Provider Name, Address, Telephone # 2 Pay to Name/Address/ID Required. Enter the name and address of the facility Situational. Enter the name, address,
Medical Billing Assistant - Program Options
 Medical Billing Assistant - Program Options Program Options allows you to control the behavior of MBA in situations where making a permanent change in the program wasn t possible. You may find this option
Medical Billing Assistant - Program Options Program Options allows you to control the behavior of MBA in situations where making a permanent change in the program wasn t possible. You may find this option
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents
 Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Electronic Prior Authorization - Provider Guide. July 2017
 Electronic Prior Authorization - Provider Guide July 2017 Table of Contents Getting Started 3 Registration 4 Logging In 5 System Configurations (Post Office Settings) 6 Prior Request Form 7 General 7 Patient
Electronic Prior Authorization - Provider Guide July 2017 Table of Contents Getting Started 3 Registration 4 Logging In 5 System Configurations (Post Office Settings) 6 Prior Request Form 7 General 7 Patient
Chapter 5: Billing on the CMS 1500 Claim Form
 Chapter 5: Billing on the CMS 1500 Claim Form Introduction The CMS 1500 claim form is used to bill for non facility services, including professional services, freestanding surgery centers, transportation,
Chapter 5: Billing on the CMS 1500 Claim Form Introduction The CMS 1500 claim form is used to bill for non facility services, including professional services, freestanding surgery centers, transportation,
837 Professional Health Care Claim Outbound. Section 1 837P Professional Health Care Claim: Basic Instructions
 Companion Document 837P 837 Professional Health Care Claim Outbound This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and
Companion Document 837P 837 Professional Health Care Claim Outbound This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and
Medicare claims processing contractors shall use remittance advice remark code RARC M32 to indicate a conditional payment is being made.
 Clarification of Medicare Conditional Payment Policy and Billing Procedures for Liability, No- Fault and Workers Compensation Medicare Secondary Payer (MSP) Claims Change Request (CR) 7355, dated May 2,
Clarification of Medicare Conditional Payment Policy and Billing Procedures for Liability, No- Fault and Workers Compensation Medicare Secondary Payer (MSP) Claims Change Request (CR) 7355, dated May 2,
EHR Go Guide: Claims and Ledgers
 EHR Go Guide: Claims and Ledgers Introduction Understanding how to submit patient claims and work with patient ledgers is a vital skill. This guide will provide an overview of how to enter and edit new
EHR Go Guide: Claims and Ledgers Introduction Understanding how to submit patient claims and work with patient ledgers is a vital skill. This guide will provide an overview of how to enter and edit new
