Billing Medicare Secondary Payer (MSP) Claims
|
|
|
- Mercy Morris
- 6 years ago
- Views:
Transcription
1 Billing Medicare Secondary Payer (MSP) Claims Per CR8486 effective 1/1/2016 MSP claims for Medicare Part A will be accepted via DDE. Review MM8486 for detailed instructions ( MLN/MLNMattersArticles/Downloads/MM8486.pdf). MSP claims for Home Health can be billed from HAS using a unique Medicare Secondary insurance. Hospice MSP claims can be billed using the standard Medicare insurance. Balances are transferred from the primary payer to MSP after the primary denial or payment is received. The Payments/Transfers Billing Codes tab is used to enter MSP claim specific information. This document lays out the one-time setup of Home Health and Hospice Medicare secondary Option Sets and steps on transferring charges and entering claim Billing Codes. TABLE OF CONTENTS One-Time Setup... 1 Create a Home Health MSP insurance... 1 Create a Home Health MSP RAP Option Set... 2 Create a Home Health MSP Final Option Set... 2 Create a Hospice MSP Option Set... 2 MSP Billing Process... 3 Transfer Balance Due from primary to MSP... 3 Enter MSP Claim Data... 3 Create MSP Electronic Claim(s)... 5 Special Billing Instructions... 6 ONE-TIME SETUP CREATE A HOME HEALTH MSP INSURANCE 716 Newman Springs Road Lincroft, NJ Tel Page 1 of 6
2 Note: Medicare Hospice clients can skip this step. Home Health clinical users should add a new insurance in the clinical system first and then complete the setup in HAS. Go to File > File Maintenance > Entity, Insurance Type to add a new Home Health Medicare insurance. Match the setup to your existing Medicare insurance but leave PPS Billing unchecked. CREATE A HOME HEALTH MSP RAP OPTION SET Go to Billing > Electronic Claims and select the Medicare Electronic Claims Option Set. 1. Click Options then Copy, select a Destination ID # and enter the Description as MSP RAP. 2. Close and reopen Electronic Claims. 3. Select the new MSP RAP option set, click Options and change the following locators: CLM05 Type of Bill: Bill Processing Type: PPS Secondary Include Pat-Ins-Bill Data: set to Bypass this Data Element CREATE A HOME HEALTH MSP FINAL OPTION SET Go to Billing > Electronic Claims and select the Medicare Electronic Claims Option Set. 1. Click Options then Copy, select a Destination ID # and enter the description as MSP Final. 2. Close and reopen Electronic Claims. 3. Select the new MSP Final option set, click Options and change the following locators: CLM05 Type of Bill: ' COB Coordination of Benefit Loops (Secondary Ins): Patient Bill Data Value1 Amount COB Insurance Sequence: Billed Insurance is secondary (COB insurance is primary) COB SBR*09 Claim Indicator: Default Value to (MA, CI) based on prior paid COB CAS*01/02 Claim Adjustment Group/Reason: Patient-Ins Bill Data Adjustment Reason(s) COB NM1*PR Insurance Payor ID: Insurance Submitter Number (Default) Bill Processing Type: PPS Secondary Include Pat-Ins-Bill Data: set to Include All Patient-Insurance Bill Data Items CREATE A HOSPICE MSP OPTION SET Go to Billing > Electronic Claims and select the Medicare Electronic Claims Option Set. 1. Click Options then Copy, select a Destination ID # and enter the Description as MSP Hospice. 2. Close and reopen Electronic Claims. 3. Select the new MSP Hospice option set, click Options and change the following locators: COB Coordination of Benefit Loops (Secondary Ins): Patient Bill Data Value1 Amount COB Insurance Sequence: Billed Insurance is secondary (COB insurance is primary) COB SBR*09 Claim Indicator: Default Value to (MA, CI) based on prior paid COB CAS*01/02 Claim Adjustment Group/Reason: Patient-Ins Bill Data Adjustment Reason(s) COB NM1*PR Insurance Payor ID: Insurance Submitter Number (Default) 716 Newman Springs Road Lincroft, NJ Tel Page 2 of 6
3 Include Pat-Ins-Bill Data: set to Include All Patient-Insurance Bill Data Items MSP BILLING PROCESS TRANSFER BALANCE DUE FROM PRIMARY TO MSP In A/R > Payments/Transfers, transfer the balance to MSP from the primary after the primary payment has been applied or a denial received. On the Detail tab, check Allow Transfer. Leave today s date as the To Bill Date. Set the To Insurance to MSP. (If the MSP insurance isn t shown, add it to the patient s record in HAS or your Clinical system). In the Transfer column enter the balance amount to be billed to MSP. If the visit was paid in full, transfer $0 for that visit. (Tip: if transferring the Net amount for all charges, check the Xfer All Chgs box, then press the Xfer button.) For Home Health, do not transfer an amount for visits that fall outside the episode. For Hospice, transfer a dollar amount for the Per Diem charges and zero dollars for the visits and medications. ENTER MSP CLAIM DATA In A/R > Payments/Transfers, select the MSP claim record and click the Billing Codes tab. Make a selection from the Process Type drop-down. Fill in the necessary fields based on the MSP Process being followed. Fields not needed for the selected Process type are grayed out by default. If billing an atypical scenario and a grayed out field is needed, change the Process Type to Custom Bill Data. Note: CGS Medicare has an online tool to assist with determining which process should be followed at: Newman Springs Road Lincroft, NJ Tel Page 3 of 6
4 Adjustment Reason Code 1: select the Patient Responsibility (PR) Claim Adjustment Reason Code (CARC) from the drop-down based on the primary payer EOB or type in the desired code (required, except for Process D). If more than one Patient Responsibility CARC needed, see Adjustment Reason Code 3 below. Amount 1: enter the Adjustment Reason Code 1 Patient Responsibility (PR) amount (plus one penny) based on the information provided on the primary payer EOB (required if Adjustment Reason Code 1 is used). For PPS, a penny is added to the primary insurance paid amount to accommodate the Medicare Q code line. Adjustment Reason Code 2: Enter a second PR code if needed or if billing with OTAF, select CO*45 from the drop-down or type in the desired code (required if billing OTAF, except for Process D). Amount 2: enter the Contractual Obligation adjustment amount from the primary payer EOB. If unavailable, this can be obtained from the primary insurance Allowance amount under the Stats > Services Provided report when run for the claim period (required if Adjustment Reason Code 2 is used). Adjustment Reason Code 3: Use only if more than one Patient Responsibility CARC received from primary (atypical). Select Reason Code from the drop-down based on the primary payer EOB or type in the desired code (optional). Amount 3: enter the Adjustment Reason Code 3 amount based on the information provided on the primary payer EOB (required if Adjustment Reason Code 3 is used). Occurrence Code 1: select the Occurrence Code from the drop-down based on the MSP Process requirement (required if not grayed out). Date 1: enter the Occurrence date for Occurrence Code 1 (required if Occurrence Code 1 is used). Occurrence Code 2: select the Occurrence Code from the drop-down based on the MSP Process requirement (required if not grayed out). Date 2: enter the Occurrence date for Occurrence Code 2 (required if Occurrence Code 2 is used). Value Code 1: defaults based on Process Type selected (except for Custom), but can be changed. Do not use this field for Value Code 44, use Value Code 2 instead (required if not grayed out). Amount 1: enter the amount paid by the primary payer. If no payment received, enter 0. (required if Value Code 1 is used). Do not use this field for Value Code 44 Amount, use Amount 2 field instead (required if Value Code 1 is used). Value Code 2: defaults based on Process Type selected (except for Custom), but can be changed. When billing with OTAF, this should be used for Value Code 44 (required if not grayed out). Amount 2: enter the OTAF amount. This should equal the Primary insurance paid amount plus any Patient Responsbility amount. (required if Value Code 2 is used). Condition Code 1: enabled only for Process Type Custom Bill Data. Select from the drop-down (optional). 716 Newman Springs Road Lincroft, NJ Tel Page 4 of 6
5 Bill Note: select a Bill Note from the drop-down or type in the desired note (optional but recommended). Press Save when done. The system performs a claim balancing check and alerts the user if data elements are incorrect. Make adjustments as necessary since out of balance claims will be rejected by Medicare. Note that PPS claims should have a penny difference due to the penny Q code line on the Final claim. Example claim balancing issue: Correct claim balancing: CREATE MSP ELECTRONIC CLAIM(S) Go to Billing > Electronic Claims. Select the MSP Option set for RAP, Final or Hospice and follow the normal process for creating claims. When sending an MSP Final claim, make sure the Submitted Type is set to All Records and not Un- Submitted Only. Review the Electronic Claim Submission Report for Value, Occurrence, Condition Codes as well as the Bill Note and COB Payer information. 716 Newman Springs Road Lincroft, NJ Tel Page 5 of 6
6 SPECIAL BILLING INSTRUCTIONS Scenario 1 - Adjustment MSP Claims. Billing an adjustment MSP requires setting up a new option set. In the Adjustment option set, change Locator CLM05 Type of Bill to 327. Change Locator REF*F8 Original Reference Code to Constant value (Entered) and in the text box, enter the DCN for the adjustment claim. NOTE: This step must be done prior to creating each adjustment MSP claim. Scenario 2 - Patient was billed as Medicare primary and they were determined to have alternate primary insurance; payment is expected from the primary insurance. Add the primary insurance for this patient to the patient record. Un-bill the charges from Medicare via the Payments screen and bill them to the primary insurance following normal billing procedures. If a balance needs to be billed to Medicare after the primary pays, follow the MSP process as described under Billing Instructions. NOTE: The MSP insurance will need to be added to the patient record if balance billing. Scenario 3 - Patient was billed as Medicare primary and they were determined to have alternate primary insurance; payment is not expected from the primary insurance. Add the primary insurance for this patient to the patient record. Go to AR>Payments/Transfers and transfer the charges to the primary using a 0 amount for each charge. Submit the claim to the primary insurance and bill Medicare secondary after the denial is received. A new option set will need to be setup for use in this scenario OR you may use your MSP Final option set but change Locator Bill Processing Type to PPS (Contact HAS Support for assistance if needed). NOTE: the Bill Processing Type should be set back to PPS Secondary when done if using this method. Scenario 4 - Patient RAP was billed to Medicare but Final needs to billed as MSP; patient s primary insurance is not going to be billed from HAS. Add the primary insurance for this patient to the patient record. Create a Final electronic claim using the MSP Finals option set but first change Locator Bill Processing Type to PPS (Contact HAS Support for assistance if needed). NOTE: the Bill Processing Type should be set back to PPS Secondary when done. 716 Newman Springs Road Lincroft, NJ Tel Page 6 of 6
Home Health Medicare Secondary Payer Claims
 Home Health Medicare Secondary Payer Claims Attention: Per CR8486 effective January 1, 2016 MSP claims for Medicare Part A will be accepted via DDE. MM8486 (https://www.cms.gov/outreach-and-education/medicare-
Home Health Medicare Secondary Payer Claims Attention: Per CR8486 effective January 1, 2016 MSP claims for Medicare Part A will be accepted via DDE. MM8486 (https://www.cms.gov/outreach-and-education/medicare-
How to bill Patient Co-Pays
 How to bill Patient Co-Pays There are 3 ways to handle patient co-pays in HAS depending on the billing scenario. The co-pay can be transferred to the Self Pay insurance after the primary payer has been
How to bill Patient Co-Pays There are 3 ways to handle patient co-pays in HAS depending on the billing scenario. The co-pay can be transferred to the Self Pay insurance after the primary payer has been
How do I bill patient co-pays?
 How do I bill patient co-pays? To bill patient co-pays, the Patient Pay (Self Pay) insurance must be first entered in the Patient insurance file or the System File must have the default Self Pay insurance
How do I bill patient co-pays? To bill patient co-pays, the Patient Pay (Self Pay) insurance must be first entered in the Patient insurance file or the System File must have the default Self Pay insurance
Billing Pre-Audit Report User Guide (DeVero)
 Billing Pre-Audit Report User Guide (DeVero) The Billing Pre-Audit Report provides a way to identify why a RAP or Final billing audit will not be generated and can also be used to identify issues with
Billing Pre-Audit Report User Guide (DeVero) The Billing Pre-Audit Report provides a way to identify why a RAP or Final billing audit will not be generated and can also be used to identify issues with
Secondary Claims 07/10/2017 1
 Secondary Claims 07/10/2017 1 Example of an MSP Claim (Professional-Processed at Service Line Level) The LOB selected will be the line of business you are submitting to for this claim. Must select Y for
Secondary Claims 07/10/2017 1 Example of an MSP Claim (Professional-Processed at Service Line Level) The LOB selected will be the line of business you are submitting to for this claim. Must select Y for
CREATING SECONDARY CLAIMS IN SERVICE CENTER
 CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
Secondary Claim Reporting Considerations
 Secondary Claim Reporting Considerations Question: How is the 005010X221 Health Care Claim Payment/Advice (835) supposed to be populated by a non-primary payer when one or more other payers have already
Secondary Claim Reporting Considerations Question: How is the 005010X221 Health Care Claim Payment/Advice (835) supposed to be populated by a non-primary payer when one or more other payers have already
Filing Secondary Claims on Provider Express
 Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Secondary Professional Claims on the HCFA-1500
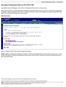 Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
Secondary Professional Claims on the HCFA-500 Log into My Insurance Manager. Then click on Professional Claim Entry on the top menu. If this is the first time you have entered the Professional Claim Entry
Course updated: November 30, 2015 Copyright 2013 Cahaba Government Benefit Administrators, LLC
 This course is designed to provide Medicare Part A providers with an understanding of: The various types of Medicare Secondary Payer (MSP) provisions; How to determine when Medicare is primary or secondary;
This course is designed to provide Medicare Part A providers with an understanding of: The various types of Medicare Secondary Payer (MSP) provisions; How to determine when Medicare is primary or secondary;
Home Health and Hospice and Medicare Secondary Payer
 Home Health and and Medicare Secondary Payer HH+H Virtual Conference 6/8/2016 1826_0616_2 Today s Presenter Jan Wood Provider Outreach and Education Consultant 2 Objectives To educate through the use of
Home Health and and Medicare Secondary Payer HH+H Virtual Conference 6/8/2016 1826_0616_2 Today s Presenter Jan Wood Provider Outreach and Education Consultant 2 Objectives To educate through the use of
JK: Billing Compliant Conditional Claims (Part 1) Doing it Right the First Time!
 JK: Billing Compliant Conditional Claims (Part 1) Doing it Right the First Time! September 2014 1185_0914 Today's Presenter Christine Janiszcak, Provider Outreach & Education Consultant 2 National Government
JK: Billing Compliant Conditional Claims (Part 1) Doing it Right the First Time! September 2014 1185_0914 Today's Presenter Christine Janiszcak, Provider Outreach & Education Consultant 2 National Government
TOP 10 MANAGED CARE & MSP SNF BILLING BATTLES
 WEDNESDAY, APRIL 16, 2014 10-11 A.M. CENTRAL TIME TOP 10 MANAGED CARE & MSP SNF BILLING BATTLES Manufacturing & Distribution Economic Update Julie Bilyeu Director BKD, LLP jbilyeu@bkd.com Lisa McIntire,
WEDNESDAY, APRIL 16, 2014 10-11 A.M. CENTRAL TIME TOP 10 MANAGED CARE & MSP SNF BILLING BATTLES Manufacturing & Distribution Economic Update Julie Bilyeu Director BKD, LLP jbilyeu@bkd.com Lisa McIntire,
Troubleshooting 999 and 277 Rejections. Segments
 Troubleshooting 999 and 277 Rejections Segments NM103 - last name or group name NM104 - first name NM105 - middle initial NM109 - usually specific information tied to that company/providers/subscriber/patient
Troubleshooting 999 and 277 Rejections Segments NM103 - last name or group name NM104 - first name NM105 - middle initial NM109 - usually specific information tied to that company/providers/subscriber/patient
Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request.
 Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request www.providerexpress.com Updated: June 2016 Important Note: Any specific member/provider
Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request www.providerexpress.com Updated: June 2016 Important Note: Any specific member/provider
Medicare claims processing contractors shall use remittance advice remark code RARC M32 to indicate a conditional payment is being made.
 Clarification of Medicare Conditional Payment Policy and Billing Procedures for Liability, No- Fault and Workers Compensation Medicare Secondary Payer (MSP) Claims Change Request (CR) 7355, dated May 2,
Clarification of Medicare Conditional Payment Policy and Billing Procedures for Liability, No- Fault and Workers Compensation Medicare Secondary Payer (MSP) Claims Change Request (CR) 7355, dated May 2,
Kansas Medical Assistance Program. Vertical Perspective. Other Insurance/Medicare Training Packet - Professional
 Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
Kansas Medical Assistance Program Vertical Perspective Other Insurance/Medicare Training Packet - Professional Other Insurance/Medicare Training Packet - Professional The training materials provided in
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
Facility Instruction Manual:
 Facility Instruction Manual: Submitting Secondary Claims with COB Data Elements Overview This supplement to the billing section of the Passport Health Plan (PHP) Provider Manual provides specific coding
Facility Instruction Manual: Submitting Secondary Claims with COB Data Elements Overview This supplement to the billing section of the Passport Health Plan (PHP) Provider Manual provides specific coding
JK: Billing Compliant Conditional Claims (Part 2) The Examples!
 JK: Billing Compliant Conditional Claims (Part 2) The Examples! October 2014 1557_0914 Today's Presenter Christine Janiszcak, Provider Outreach & Education Consultant 2 National Government Services, Inc.
JK: Billing Compliant Conditional Claims (Part 2) The Examples! October 2014 1557_0914 Today's Presenter Christine Janiszcak, Provider Outreach & Education Consultant 2 National Government Services, Inc.
Medicare Secondary Payer (MSP) Chapter 11
 Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
Medicare Secondary Payer (MSP) Chapter 11
 Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
Chapter 11 Contents Introduction 1. Employer Sponsored Group Health Plan Coverage 2. Accident/Injury Insurance 3. Other Government-Sponsored Health Plans 4. Electronic Billing of MSP Claims 5. Medicare
Appendix 3A. MA Companion Guide: CMS Supplemental Instructions for EDR and CRR Data Elements
 Appendix 3A. MA Companion Guide: CMS Supplemental Instructions for EDR and CRR Data s A3A.1 LOOPS AND SEGMENTS APPLIED TO EDR AND CRR SUBMISSIONS... 3 A3A.2 CONTROL SEGMENTS: CMS SUPPLEMENTAL INSTRUCTIONS
Appendix 3A. MA Companion Guide: CMS Supplemental Instructions for EDR and CRR Data s A3A.1 LOOPS AND SEGMENTS APPLIED TO EDR AND CRR SUBMISSIONS... 3 A3A.2 CONTROL SEGMENTS: CMS SUPPLEMENTAL INSTRUCTIONS
Best Practice Recommendation for
 Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Best Practice Recommendation for Exchanging Explanation of Payment Information between Providers and Health Plans (using 5010v transactions) For use with ANSI ASC X12N 5010v Health Care Claim (837) Health
Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 3298 Date: August 06, 2015
 CMS Manual System Pub 100-04 Medicare Claims Processing Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 3298 Date: August 06, 2015 Change Request
CMS Manual System Pub 100-04 Medicare Claims Processing Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 3298 Date: August 06, 2015 Change Request
Claims Resolution Matrix Institutional
 Rev /07 Claims Resolution Matrix Institutional This Claims Resolution Matrix is to be used as a reference tool to troubleshoot institutional claims that have been submitted electronically (i.e., submitted
Rev /07 Claims Resolution Matrix Institutional This Claims Resolution Matrix is to be used as a reference tool to troubleshoot institutional claims that have been submitted electronically (i.e., submitted
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
Medicare Part B Crossover Claim Submission User Guide
 Thank you for using MDH s newest web application to process your Medicare Part B Crossover Claims. Each claim you file is official and will supersede any paper claim you may have filed within the past
Thank you for using MDH s newest web application to process your Medicare Part B Crossover Claims. Each claim you file is official and will supersede any paper claim you may have filed within the past
TheraManager Help Note
 Subject: EDI Claim Troubleshooting Guide TheraManager Help Note This Help Note consists of a list of selected elements within an EDI claim (ANSI 837, version 5010) and the TheraManager screen where the
Subject: EDI Claim Troubleshooting Guide TheraManager Help Note This Help Note consists of a list of selected elements within an EDI claim (ANSI 837, version 5010) and the TheraManager screen where the
Rural Health Clinic Technical Assistance Webinar 6/29/17 RHC Common Claim Errors
 Rural Health Clinic Technical Assistance Webinar 6/29/17 RHC Common Claim Errors by Janet Lytton, Director of Reimbursement Rural Health Development 308-647-6455 janet.lytton@rhdconsult.com 1 Address common
Rural Health Clinic Technical Assistance Webinar 6/29/17 RHC Common Claim Errors by Janet Lytton, Director of Reimbursement Rural Health Development 308-647-6455 janet.lytton@rhdconsult.com 1 Address common
Submitting Secondary Claims with COB Data Elements - Facilities
 Overview Submitting Secondary Claims with COB Data Elements - Facilities This supplement to the billing section of the AmeriHealth Caritas Pennsylvania Claims Filing Instruction Manual provides specific
Overview Submitting Secondary Claims with COB Data Elements - Facilities This supplement to the billing section of the AmeriHealth Caritas Pennsylvania Claims Filing Instruction Manual provides specific
NetSolutions. Common Plan Setups And Reimbursement Tables
 NetSolutions Common Plan Setups And Reimbursement Tables TABLE OF CONTENTS ABOUT PLAN SETUPS... 2 ROOM AND BOARD PLANS... 3 ANCILLARY PLANS... 7 CO-INSURANCE PLANS... 9 REIMBURSEMENT TABLES... 10 MORE
NetSolutions Common Plan Setups And Reimbursement Tables TABLE OF CONTENTS ABOUT PLAN SETUPS... 2 ROOM AND BOARD PLANS... 3 ANCILLARY PLANS... 7 CO-INSURANCE PLANS... 9 REIMBURSEMENT TABLES... 10 MORE
Practice Express 3.0 Update September 25, 2006
 Alpha Inquiry Change Patient (Patient File Maintenance) Added new field: Cell Phone#. It is on the right directly below Work Phone Ext. New feature: Contact Information. You now have the capability of
Alpha Inquiry Change Patient (Patient File Maintenance) Added new field: Cell Phone#. It is on the right directly below Work Phone Ext. New feature: Contact Information. You now have the capability of
Using ERAs with Helper
 Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
Using ERAs with Helper Table of Contents Introduction to ERAs in Helper... 1 Getting Started with ERAs... 1 Set up Multi-User settings for ERAs... 1 Enter the ERA Payer ID in the Insurance Company Library...
Transition Slide. Presenter(s): Topic. Level. Dave Roughen Project Manager Kay Thorpe EDI Analyst. Ron Burke Dental Product Manager
 Topic Level Presenter(s): Dave Roughen Project Manager Kay Thorpe EDI Analyst Transition Slide Ron Burke Dental Product Manager Dave Roughen Project Manager Improving Reimbursements through effective Claims
Topic Level Presenter(s): Dave Roughen Project Manager Kay Thorpe EDI Analyst Transition Slide Ron Burke Dental Product Manager Dave Roughen Project Manager Improving Reimbursements through effective Claims
Rev 7/20/2015. ClaimsConnect Rejection Guide
 ClaimsConnect Rejection Guide Helper Client, The purpose of this document is to assist you in accelerating the resolution of claim rejections. We have identified the most frequent rejection messages, and
ClaimsConnect Rejection Guide Helper Client, The purpose of this document is to assist you in accelerating the resolution of claim rejections. We have identified the most frequent rejection messages, and
PC-ACE Secondary Insurance Setup
 This document is intended as a help guide for entering secondary insurance information in the PC-ACE software. It is not intended to replace the general help (accessible by the F1 key) or specific item
This document is intended as a help guide for entering secondary insurance information in the PC-ACE software. It is not intended to replace the general help (accessible by the F1 key) or specific item
Coordination of Benefits (COB) Claims Submission Guide
 Coordination of Benefits (COB) Claims Submission Guide Coordination of benefits applies to members who have coverage with more than one health care plan and helps to ensure that these members receive benefits
Coordination of Benefits (COB) Claims Submission Guide Coordination of benefits applies to members who have coverage with more than one health care plan and helps to ensure that these members receive benefits
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Emdeon Services Available for Compulink Advantage
 Emdeon Services Available for Compulink Advantage Product and Service Information 02.2014 2645 Townsgate Road, Suite 200 Westlake Village, CA 91361 Support: 800.888.8075 Fax: 805.497.4983 2014 Compulink
Emdeon Services Available for Compulink Advantage Product and Service Information 02.2014 2645 Townsgate Road, Suite 200 Westlake Village, CA 91361 Support: 800.888.8075 Fax: 805.497.4983 2014 Compulink
Version Number: 1.0 Introduction Matrix Wellmark Values. November 01, 2011
 Wellmark Blue Cross and Blue Shield HIPAA Transaction Standard Companion Guide Section 2, 837 Institutional Refers to the X2N Technical Report Type 3 ANSI Version 500A2 Version Number:.0 Introduction Matrix
Wellmark Blue Cross and Blue Shield HIPAA Transaction Standard Companion Guide Section 2, 837 Institutional Refers to the X2N Technical Report Type 3 ANSI Version 500A2 Version Number:.0 Introduction Matrix
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
KY Medicaid. 837P Companion Guide. Cabinet for Health and Family Services Department for Medicaid Services. March 28, 2017 KY MEDICAID COMPANION GUIDE
 KY Medicaid 837P Companion Guide Cabinet for Health and Family Services Department for Medicaid Services March 28, 2017 DMS Approved [2017 005010] 1 Document Change Log Version Changed Date Changed By
KY Medicaid 837P Companion Guide Cabinet for Health and Family Services Department for Medicaid Services March 28, 2017 DMS Approved [2017 005010] 1 Document Change Log Version Changed Date Changed By
 www.mydentalcoverage.com 1 2 3 Complete the Fields as indicated 4 Complete the Fields as indicated click submit 5 6 Security Questions 7 Email sent to Activate Account 8 Close out previous browser and
www.mydentalcoverage.com 1 2 3 Complete the Fields as indicated 4 Complete the Fields as indicated click submit 5 6 Security Questions 7 Email sent to Activate Account 8 Close out previous browser and
Electronic Claims Submission Coordination of Benefits (COB) Dental Examples
 Electronic Claims Submission Coordination of Benefits (COB) Dental Examples Aetna Serrvice Options S SMM forr Health Carre Proffessionals t i ti f lt r i l We prepared this COB Dental Claim Examples document
Electronic Claims Submission Coordination of Benefits (COB) Dental Examples Aetna Serrvice Options S SMM forr Health Carre Proffessionals t i ti f lt r i l We prepared this COB Dental Claim Examples document
Will Boyd and Lindsay Campbell, BAYADA Home Health Care. Copyright
 Will Boyd and Lindsay Campbell, BAYADA Home Health Care Copyright 2017. 1 TODAY S SPEAKERS Will Boyd Director of Home Health Reimbursement Services BAYADA Home Health Lindsay Campbell Manager, Business
Will Boyd and Lindsay Campbell, BAYADA Home Health Care Copyright 2017. 1 TODAY S SPEAKERS Will Boyd Director of Home Health Reimbursement Services BAYADA Home Health Lindsay Campbell Manager, Business
E-Commerce Enrollment
 Electronic Claims Submission HCIQ will electronically submit your primary carrier, professional claims. Please refer to our payer list to view the insurance companies that we currently submit to. Electronic
Electronic Claims Submission HCIQ will electronically submit your primary carrier, professional claims. Please refer to our payer list to view the insurance companies that we currently submit to. Electronic
Entering Payments in Aprima PRM
 Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
Companion Guide for the X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC
 Companion Guide for the 005010X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Name TR3 Values Notes Delimiter: Data
Companion Guide for the 005010X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Name TR3 Values Notes Delimiter: Data
Patient Setup Screen
 The Patient Setup Screen is used to create a new patient chart or modify an existing patient s chart. After opening the Patient Setup screen you will have the ability to choose the correct Patient Tab
The Patient Setup Screen is used to create a new patient chart or modify an existing patient s chart. After opening the Patient Setup screen you will have the ability to choose the correct Patient Tab
VIII STANDARD ENCOUNTER COMPANION GUIDE A. Transaction Introduction
 A. Transaction Introduction Standard Companion Guide (CG) Transaction Information Effective March 27, 2015 IEHP Instructions related to Implementation Guides (IG) based On X12 Version 005010X222A1 Health
A. Transaction Introduction Standard Companion Guide (CG) Transaction Information Effective March 27, 2015 IEHP Instructions related to Implementation Guides (IG) based On X12 Version 005010X222A1 Health
XPressClaim Help. Diagnosis 1,2,3,etc. Enter the number(s) of the corresponding diagnosis code(s) that applies to this service.
 Keying Information Professional Claims CMS 1500 Claim type Please select the type of claim: 1- Original claim 7- Replacement of prior claim Please note: 7- Replacement of prior claim should only be selected
Keying Information Professional Claims CMS 1500 Claim type Please select the type of claim: 1- Original claim 7- Replacement of prior claim Please note: 7- Replacement of prior claim should only be selected
Appendix 3B. Crosswalk from Retired Minimum Data Element List to Appendix 3A MA Companion Guide
 Appendix 3B. Crosswalk from Retired Minimum Data Element List to Appendix 3A MA A3B.1 LOOPS AND SEGMENTS APPLIED TO EDR AND CRR SUBMISSIONS... 3 A3B.2 COLUMN HEADING CROSSWALK FROM APPENDIX 3A MA COMPANION
Appendix 3B. Crosswalk from Retired Minimum Data Element List to Appendix 3A MA A3B.1 LOOPS AND SEGMENTS APPLIED TO EDR AND CRR SUBMISSIONS... 3 A3B.2 COLUMN HEADING CROSSWALK FROM APPENDIX 3A MA COMPANION
SECTION 9 1 CLAIMS PROCEDURES
 SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
KANSAS MEDICAL ASSISTANCE PROGRAM. Fee-for-Service Provider Manual. General TPL Payment
 KANSAS MEDICAL ASSISTANCE PROGRAM Fee-for-Service Provider Manual General TPL Payment Updated 06.2016 PART I GENERAL THIRD-PARTY LIABILITY PAYMENT FEE-FOR-SERVICE KANSAS MEDICAL ASSISTANCE PROGRAM TABLE
KANSAS MEDICAL ASSISTANCE PROGRAM Fee-for-Service Provider Manual General TPL Payment Updated 06.2016 PART I GENERAL THIRD-PARTY LIABILITY PAYMENT FEE-FOR-SERVICE KANSAS MEDICAL ASSISTANCE PROGRAM TABLE
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Encounter Data Work Group Summary Notes for Third Party Submitters: Key Findings and Recommendations
 Summary Notes for : Key Findings and Recommendations Work Group 2 of 3 This report summarizes the findings of the conducted on. Twenty-one organizations participated in this Work Group and included: Alliance
Summary Notes for : Key Findings and Recommendations Work Group 2 of 3 This report summarizes the findings of the conducted on. Twenty-one organizations participated in this Work Group and included: Alliance
837 Professional Health Care Claim - Outbound
 Companion Document 837P 837 Professional Health Care Claim - Outbound Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care transaction for professional
Companion Document 837P 837 Professional Health Care Claim - Outbound Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care transaction for professional
Indiana Health Coverage Programs
 Indiana Health Coverage Programs Standard Companion Guide Transaction Information Instructions related to Transactions based on ASC X12 Implementation Guides, version 005010 Health Care Claim: Institutional
Indiana Health Coverage Programs Standard Companion Guide Transaction Information Instructions related to Transactions based on ASC X12 Implementation Guides, version 005010 Health Care Claim: Institutional
Indiana Health Coverage Programs
 Indiana Health Coverage Programs Standard Companion Guide Transaction Information Instructions related to Transactions based on ASC X12 Implementation Guides, version 005010 Health Care Claim: Institutional
Indiana Health Coverage Programs Standard Companion Guide Transaction Information Instructions related to Transactions based on ASC X12 Implementation Guides, version 005010 Health Care Claim: Institutional
PATIENT ACCOUNTING TRAINING
 PATIENT ACCOUNTING TRAINING Most collection activity will occur in SMS Patient Accounting. However, any changes to patient demographics or insurance will need to be done in Cerner PMOffice. Demographic
PATIENT ACCOUNTING TRAINING Most collection activity will occur in SMS Patient Accounting. However, any changes to patient demographics or insurance will need to be done in Cerner PMOffice. Demographic
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
Healthpac 837 Message Elements - Professional
 Healthpac 837 Message Elements - Version 1.4 March 17, 2003 1 Healthpac 837 Message Elements Table of Contents 1 INTRODUCTION...2 1.1 GENERAL COMMENTS...2 1.2 RELATED DOCUMENTS...3 2 MESSAGE ELEMENTS...4
Healthpac 837 Message Elements - Version 1.4 March 17, 2003 1 Healthpac 837 Message Elements Table of Contents 1 INTRODUCTION...2 1.1 GENERAL COMMENTS...2 1.2 RELATED DOCUMENTS...3 2 MESSAGE ELEMENTS...4
10/2010 Health Care Claim: Professional - 837
 837 Health Care Claim: Professional HIPAA/V4010X098A1/837: 837 Health Care Claim: Professional Version: 1.8 Update 10/20/10 (Latest Changes in RED font) Author: Publication: EDI Department LA Medicaid
837 Health Care Claim: Professional HIPAA/V4010X098A1/837: 837 Health Care Claim: Professional Version: 1.8 Update 10/20/10 (Latest Changes in RED font) Author: Publication: EDI Department LA Medicaid
Health-e Web Entry. July 2007
 Health-e Web Entry July 2007 Introduction Before your installation appointment, complete the following: (Call your assigned installer with any questions.) ENS Payer List Review the ENS payer list and become
Health-e Web Entry July 2007 Introduction Before your installation appointment, complete the following: (Call your assigned installer with any questions.) ENS Payer List Review the ENS payer list and become
Vendor Specifications 837 Institutional Claim ASC X12N Version X223A2. for. State of Idaho MMIS
 Vendor Specifications 837 Institutional Claim ASC X12N Version 005010X223A2 for State of Idaho MMIS Date of Publication: 6/16/2016 Document Number: TL426 Version: 8.0 Revision History Version Date Author
Vendor Specifications 837 Institutional Claim ASC X12N Version 005010X223A2 for State of Idaho MMIS Date of Publication: 6/16/2016 Document Number: TL426 Version: 8.0 Revision History Version Date Author
PC-ACE Claim Management
 This document is a guide to assist PC-ACE users in entering and managing Durable Medical Equipment (DME) claim information. This document includes: Claim Entry... 2 Managing Claims... 15 Preparing to Send
This document is a guide to assist PC-ACE users in entering and managing Durable Medical Equipment (DME) claim information. This document includes: Claim Entry... 2 Managing Claims... 15 Preparing to Send
13. IEHP P PROFESSIONAL CLAIM COMPANION GUIDE A. Included ASC X12 Implementation Guides X222A1 Health Care Claim: Professional
 13. IEHP 5010 837P PROFESSIONAL CLAIM COMPANION GUIDE 1. 005010X222A1 Health Care Claim: Professional Standard Companion Guide (CG) Transaction Information Effective January 1, 2018 IEHP Instructions related
13. IEHP 5010 837P PROFESSIONAL CLAIM COMPANION GUIDE 1. 005010X222A1 Health Care Claim: Professional Standard Companion Guide (CG) Transaction Information Effective January 1, 2018 IEHP Instructions related
ADJ. SYSTEM FLD LEN. Min. Max.
 Loop Loop Repeat Segme nt Element Id Description X12 Page No. ID Min. Max. ADJ. SYSTEM FLD LEN Usage Req. ANSI VALUES COMMENTS 1 ISA Interchange Control Header B.3 1 R ISA08 Interchange Receiver ID AN
Loop Loop Repeat Segme nt Element Id Description X12 Page No. ID Min. Max. ADJ. SYSTEM FLD LEN Usage Req. ANSI VALUES COMMENTS 1 ISA Interchange Control Header B.3 1 R ISA08 Interchange Receiver ID AN
Research and Resolve UB-04 Claim Denials. HP Provider Relations/October 2014
 Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
FINANCE TRAINING CAPITAL PROJECTS Capital Budget Amendment and Create Captial Project
 FINANCE TRAINING CAPITAL PROJECTS Capital Budget Amendment and Create Captial Project CONTENTS: CREATING A CAPITAL PROJECT BUDGET AMENDMENT CREATING A CAPITAL PROJECT Creating a Capital Project Budget
FINANCE TRAINING CAPITAL PROJECTS Capital Budget Amendment and Create Captial Project CONTENTS: CREATING A CAPITAL PROJECT BUDGET AMENDMENT CREATING A CAPITAL PROJECT Creating a Capital Project Budget
Understanding your ChiroTouch-Generated CMS 1500 Health Insurance Claim Form
 Understanding your ChiroTouch-Generated CMS 1500 Health Insurance Claim Form Click on any box on the claim form below for a guide to entering this information into ChiroTouch. ChiroTouch cannot advise
Understanding your ChiroTouch-Generated CMS 1500 Health Insurance Claim Form Click on any box on the claim form below for a guide to entering this information into ChiroTouch. ChiroTouch cannot advise
CoreMMIS bulletin Core benefits Core enhancements Core communications
 CoreMMIS bulletin Core benefits Core enhancements Core communications INDIANA HEALTH COVERAGE PROGRAMS BT201667 OCTOBER 20, 2016 CoreMMIS billing guidance: Part I On December 5, 2016, the Indiana Health
CoreMMIS bulletin Core benefits Core enhancements Core communications INDIANA HEALTH COVERAGE PROGRAMS BT201667 OCTOBER 20, 2016 CoreMMIS billing guidance: Part I On December 5, 2016, the Indiana Health
837 Professional Health Care Claim Outbound. Section 1 837P Professional Health Care Claim: Basic Instructions
 Companion Document 837P 837 Professional Health Care Claim Outbound This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and
Companion Document 837P 837 Professional Health Care Claim Outbound This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and
Companion Guide for the X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC
 Companion Guide for the 005010X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Description TR3 Values Notes Delimiter:
Companion Guide for the 005010X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Description TR3 Values Notes Delimiter:
Claims adjustments Adjustment codes and coordination of benefits (COB)
 Claims adjustments Adjustment codes and coordination of benefits (COB) 23.03.522.1 H (9/17) aetna.com Electronic submission of adjustment group codes and claims adjustment reason codes Aetna is the brand
Claims adjustments Adjustment codes and coordination of benefits (COB) 23.03.522.1 H (9/17) aetna.com Electronic submission of adjustment group codes and claims adjustment reason codes Aetna is the brand
Indiana Health Coverage Programs
 Indiana Health Coverage Programs Standard Companion Guide Transaction Information Instructions related to Transactions based on ASC X12 Implementation Guides, version 005010 Health Care Claim: Dental (837)
Indiana Health Coverage Programs Standard Companion Guide Transaction Information Instructions related to Transactions based on ASC X12 Implementation Guides, version 005010 Health Care Claim: Dental (837)
Best Practice Recommendation for. Processing & Reporting Remittance Information ( v) Version 3.93
 Best Practice Recommendation for Processing & Reporting Remittance Information (835 5010v) Version 3.93 For use with ANSI ASC X12N 835 (005010X222) Health Care Claim Payment/Advice Technical Report Type
Best Practice Recommendation for Processing & Reporting Remittance Information (835 5010v) Version 3.93 For use with ANSI ASC X12N 835 (005010X222) Health Care Claim Payment/Advice Technical Report Type
Pfizer encompass Co-Pay Assistance Program for INFLECTRA :
 Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Medicare claim adjustment reason codes 2016
 Medicare claim adjustment reason codes 2016 Search Claim Adjustment Reason Codes 2017.. 2016. Uniform Use of Claim Adjustment Reason Codes. How to submit a Medicare-Medicaid claim.... Adjustment Remittance
Medicare claim adjustment reason codes 2016 Search Claim Adjustment Reason Codes 2017.. 2016. Uniform Use of Claim Adjustment Reason Codes. How to submit a Medicare-Medicaid claim.... Adjustment Remittance
HEALTHpac 837 Message Elements Institutional
 HEALTHpac 837 Message Elements Version 1.2 March 17, 2003 1 Table of Contents 1 INTRODUCTION...2 1.1 GENERAL COMMENTS...2 1.2 RELATED DOCUMENTS...3 2 MESSAGE ELEMENTS...4 2.1 HEADER...4 2.2 INFO SOURCE...5
HEALTHpac 837 Message Elements Version 1.2 March 17, 2003 1 Table of Contents 1 INTRODUCTION...2 1.1 GENERAL COMMENTS...2 1.2 RELATED DOCUMENTS...3 2 MESSAGE ELEMENTS...4 2.1 HEADER...4 2.2 INFO SOURCE...5
Work with Guarantor Accounts
 Work with Guarantor Accounts Update guarantor information... 2 Demand a statement for a guarantor... 2 Change the guarantor for a hospital account... 2 Change the guarantor for a minor's hospital account...
Work with Guarantor Accounts Update guarantor information... 2 Demand a statement for a guarantor... 2 Change the guarantor for a hospital account... 2 Change the guarantor for a minor's hospital account...
Quick Guide to Secondary Claims
 Quick Guide to Secondary Claims Would you like to: Please click below what you would like help with to be directed to that specific section in this guide. Convert your primary claim to a secondary claims
Quick Guide to Secondary Claims Would you like to: Please click below what you would like help with to be directed to that specific section in this guide. Convert your primary claim to a secondary claims
a. Sign in to TurboTax Online and open your tax return b. On the Home tab, click Save your 2010 return to your computer.
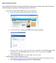 Hawaii Amend Instructions If you used TurboTax Online to prepare and file your original return, follow these steps. If you used TurboTax Desktop, skip down to Desktop Customer Start Here! 1. Save Your
Hawaii Amend Instructions If you used TurboTax Online to prepare and file your original return, follow these steps. If you used TurboTax Desktop, skip down to Desktop Customer Start Here! 1. Save Your
Coordination of Benefits (COB)
 Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more Plans providing benefits or services for medical treatment.
Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more Plans providing benefits or services for medical treatment.
Health Care Claim: Institutional (837)
 Health Care Claim: Institutional (837) Standard Companion Guide Transaction Information November 2, 2015 Version 3.1 Express permission to use ASC X12 copyrighted materials within this document has been
Health Care Claim: Institutional (837) Standard Companion Guide Transaction Information November 2, 2015 Version 3.1 Express permission to use ASC X12 copyrighted materials within this document has been
LEARNING WHAT IT TAKES TO BILL MANAGED CARE INSURANCES
 home health LEARNING WHAT IT TAKES TO BILL MANAGED CARE INSURANCES Lynn Labarta, CEO, Imark Billing 1 home health LYNN LABARTA CEO, Imark Billing Founder of Imark Billing with over 15 years experience
home health LEARNING WHAT IT TAKES TO BILL MANAGED CARE INSURANCES Lynn Labarta, CEO, Imark Billing 1 home health LYNN LABARTA CEO, Imark Billing Founder of Imark Billing with over 15 years experience
MMF Investment Policy Management
 MMF Investment Policy Management Citibank Online Investments Transaction Services MMF Investment Policy Management Table of Contents Table of Contents Money Market Funds Investment Policy Management...2
MMF Investment Policy Management Citibank Online Investments Transaction Services MMF Investment Policy Management Table of Contents Table of Contents Money Market Funds Investment Policy Management...2
D. 0. C H A N G E S & U P D A T E S. Released December 12, 2011 perform your PROscript updates today
 D. 0. C H A N G E S & U P D A T E S Released December 12, 2011 perform your PROscript updates today 1 D.0. Field Changes [Patient Segment] Patient Email Address (350-HN). Place of Service (307-C7). Will
D. 0. C H A N G E S & U P D A T E S Released December 12, 2011 perform your PROscript updates today 1 D.0. Field Changes [Patient Segment] Patient Email Address (350-HN). Place of Service (307-C7). Will
Electronic Claim Adjustments User Guide
 Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
Electronic Adjustments User Guide azblue.com 251405-16 Electronic Adjustments User Guide Contents Introduction... 1 Request for reconsideration or adjustment of adjudicated claims... 1 Appeals and grievance
KY Medicaid. 837I Companion Guide. Cabinet for Health and Family Services Department for Medicaid Services. March 28, 2017 KY MEDICAID COMPANION GUIDE
 KY Medicaid 837I Companion Guide Cabinet for Health and Family Services Department for Medicaid Services March 28, 2017 DMS Approved 2017 005010 1 Document Change Log Version Changed Date Changed By Reason
KY Medicaid 837I Companion Guide Cabinet for Health and Family Services Department for Medicaid Services March 28, 2017 DMS Approved 2017 005010 1 Document Change Log Version Changed Date Changed By Reason
ANSI 837 v5010 to CMS-1500 Crosswalk
 to CMS- Crosswalk The implementation of ANSI ASC X12N electronic transactions to version 5010 presents substantial changes in the content of the data you will submit with your claims. In order to help
to CMS- Crosswalk The implementation of ANSI ASC X12N electronic transactions to version 5010 presents substantial changes in the content of the data you will submit with your claims. In order to help
CLAIM ADJUDICATION CODES AND ACTION
 1 45 Adjusted - Above contract rate Post payment and any adjustment to charges. Do not refile. 2 92 Approved Post payment and any adjustment to charges. Do not refile. 3 198 Authed units exceeded Verify
1 45 Adjusted - Above contract rate Post payment and any adjustment to charges. Do not refile. 2 92 Approved Post payment and any adjustment to charges. Do not refile. 3 198 Authed units exceeded Verify
Topic Keep your Finger on the Pulse: Monitoring the Activity in your NextGen PM System Level Practice Management 300
 Presenter(s): Stacy Stenger PM Corporate Trainer Topic Keep your Finger on the Pulse: Monitoring the Activity in your NextGen PM System Level Practice Management 300 Safe Harbor Provisions/Legal Disclaimer
Presenter(s): Stacy Stenger PM Corporate Trainer Topic Keep your Finger on the Pulse: Monitoring the Activity in your NextGen PM System Level Practice Management 300 Safe Harbor Provisions/Legal Disclaimer
HIPAA 837I (Institutional) Companion Guide
 Companion Guide Prepared for Health Care Providers For use with the Cardinal Innovations claims processing system Version 5.0 January 2011 Table of Contents 1. Introduction...3 2. Approval Procedures...4
Companion Guide Prepared for Health Care Providers For use with the Cardinal Innovations claims processing system Version 5.0 January 2011 Table of Contents 1. Introduction...3 2. Approval Procedures...4
Veterans Choice Program SDMGMA Third Party Payer Day Sioux Falls, SD September 20, 2016
 Veterans Choice Program SDMGMA Third Party Payer Day Sioux Falls, SD September 20, 2016 Veterans Choice Program (VCP) In August 2014, President Obama signed into law the Veterans Access, Choice and Accountability
Veterans Choice Program SDMGMA Third Party Payer Day Sioux Falls, SD September 20, 2016 Veterans Choice Program (VCP) In August 2014, President Obama signed into law the Veterans Access, Choice and Accountability
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
837I Institutional Health Care Claim - for Encounters
 Companion Document 837I - Encounters 837I Institutional Health Care Claim - for Encounters Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care
Companion Document 837I - Encounters 837I Institutional Health Care Claim - for Encounters Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care
Claims Resolution Matrix Professional
 Rev 04/07 Claims Resolution Matrix Professional This Claims Resolution Matrix is to be used as a reference tool to troubleshoot professional claims that have been submitted electronically (i.e., submitted
Rev 04/07 Claims Resolution Matrix Professional This Claims Resolution Matrix is to be used as a reference tool to troubleshoot professional claims that have been submitted electronically (i.e., submitted
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
