Claim Investigation Submission Guide
|
|
|
- Damon May
- 5 years ago
- Views:
Transcription
1 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and with Highmark Blue Shield independent Page 1 of licensees 11 of the Blue Cross and Blue Shield Association.
2 The Claim Investigation Submission transaction lets you submit questions or comments about a claim for Independence Blue Cross (Independence) members through the NaviNet web portal. You can then track and review the health plan s response to your questions using the Claim Investigation Inquiry transaction. Important notes The Claim Investigation link is available for claims in a finalized status. Claim Investigation submissions for pre-migrated claims are no longer supported. Claim edits and claim corrections are not permitted through Claim Investigation. Claim Investigation is by claim and not by line item. If you need to draw attention to a specific claim line, enter that line number in the Investigation Comments box. Please be specific when describing the reason for the claim review. Note: If a claim is denied for lack of referral or authorization and one was required, you must submit a valid referral or authorization number in order for the claim to be reconsidered. See the Best practices for common claim review requests section at the end of this guide. A response for a Claim Investigation is generally expected within 30 days after submission. Please note: If you have a large volume of claim review requests for the same issue, please contact your Network Coordinator to discuss before submitting multiple claim review requests through NaviNet. Accessing Claims: Claim Search To begin, first perform a Claim Status Inquiry to locate the claim. Select Claim Inquiry and Maintenance from the Independence Workflows menu, and then select Claim Status Inquiry. This will take you to the Claim Status Search screen. Page 2 of 11
3 On the Claim Status Search screen, enter your search criteria to find a claim. Page 3 of 11
4 1. Select the Billing Entity field to display the list of provider groups or use the type-ahead feature and type the billing entity group name, NPI, provider ID, or address. Select the provider from the drop-down list returned. Note: If the number of provider groups associated with your NaviNet office is too large, you will see the message Too many results found, please narrow the search criteria. You may need to use the type-ahead feature to locate the desired provider group. 2. Search by Member ID or Patient Name and Date of Birth: For a Member ID search, enter Member ID as it appears on the member s identification card. For a Patient Name search, enter Last Name, First Name, and Date of Birth (mm/dd/yyyy). When searching by Patient Name and Date of Birth, if more than one record matches your search criteria, the Patient Search Results screen will display. You will then need to select the appropriate record to view the list of associated claims. 3. For Service Start/End, enter a claim start date (mm/dd/yyyy) or click the calendar icon to select a date. Note: The updated transaction will eventually allow you to search for a member s claim up to three years in the past from the current date. However, initially you will only be able to access claims processed on our new platform. You cannot search for pre-migrated claims processed on our legacy platform. 4. Claim ID is an optional field and is used to filter your search. Note: Searches cannot be performed by entering a Claim ID alone. 5. After entering all claim search criteria, select Search. Page 4 of 11
5 For finalized claims, you can access the Claim Investigation link from either the Claim Status Search Results screen or the Claim Status Details screen. Claim Investigation link from the Claim Status Search Results screen To access the Claim Details screen from the Search Results screen, select the Claim ID link for the desired patient. For finalized claims, you can select Claim Investigation to start an investigation for a specific claim. Claim Investigation link from the Claims Status Details screen On the Claim Status Details screen, you can view the detailed claim information for your patient. For a finalized claim, select Claim Investigation to start a claim investigation. Page 5 of 11
6 Once you select Claim Investigation, the Investigation Entry pop-up appears. You will need to complete this form by following the below instructions. Select the reason for your request by selecting a description from the Investigation Type drop-down list. Enter your comments for the investigation reviewers. Please be specific when describing the reason for the investigation. In the remaining fields, enter the contact information specific to this investigation. Populate the remaining fields regarding the contact. Once complete, select the Submit button one time only. The submission of your completed investigation may take a few moments. Please note: Do not press the Enter key on your keyboard when completing a Claim Investigation request as this may submit the request prematurely. Page 6 of 11
7 The system will display a confirmation screen when the submission is complete. To inquire about the submitted investigation in the future, use the Claim Investigation Inquiry transaction. Claim Investigation Inquiry Select Claim Inquiry and Maintenance from the Independence Workflows menu, and then select Claim Investigation Inquiry. On the Claims Investigation Inquiry Search screen, enter your search criteria to track your investigation. See image on page Select the Billing Provider field to display the provider list and select the appropriate Billing Provider. 2. The displayed Request Date From and Request Date To dates default to the most current 30-day period. These dates can be modified. 3. Narrow your search by Adjustment ID (optional field). 4. Narrow your search by Investigation Status Submitted or Closed (optional field). 5. After making all selections, select Search. Page 7 of 11
8 On the Claims Investigation Search Results screen, select the Request Date link for the correlated member to access the Claim Investigation response screen. Note: A Closed status indicates that the health plan has responded to the investigation. An investigation status of Submitted indicates the request remains under review. The Claim Investigation response screen will open. Page 8 of 11
9 If the Claim Investigation has been closed, the Investigation Reply will appear below the Investigation Comments. If the claim has been adjusted, the details may appear in the Adjusted Service Line Detail section. Best practices for common claim review requests Follow the guidelines below to help expedite processing of your claim review requests. Submission preparation Prior to submitting a claim review request for facility pricing, take the following steps: Using the Claim Investigation Inquiry transaction, confirm that there is not an existing investigation for the same claim that may have been previously submitted by your office. Verify the line of business (LOB) for the member s benefit plan, the member s coverage effective date compared to the date of service (DOS), and the member s eligibility for the service(s) performed. Review your Independence Agreement effective date and expected reimbursement. Page 9 of 11
10 Review the admission date and discharge information. Note: Remittance is established by the date of admission, regardless of a change in the provider s Agreement or member s benefit plan during an inpatient stay. Refer to field 12 on the UB-04 claim form for the date of admission and fields 16 and 17 for the discharge status. Verify the status of the authorization, if applicable (i.e., pending vs. approved, level of care, dates of service, and service(s) performed). In addition, please review the following: Modifiers. The application of modifier pricing is administered per Ambulatory Payment Classifications (APC)-based outpatient contracts only. Independence does not acknowledge modifiers if you are a facility that is contracted according to the outpatient fee schedule (i.e., not through APC [non-apc]). Quarterly fee schedule updates.* As outlined in your Independence Agreement, due to changes in clinical practice and/or modifications to standard coding systems, we may add, delete, and/or re-categorize the fee schedule for outpatient procedures. Independence provides a 30-day advanced written notice to facilities of such changes. It is imperative that these changes are reviewed to ensure accurate billing and claims reimbursement. *Quarterly fee schedule updates are not applicable to skilled nursing facilities. Pharmacy fee schedule. Confirm if your facility is currently contracted per the Outpatient Cost-Based Pharmacy Fee Schedule. For APC facilities. In the event the Centers for Medicare & Medicaid Services (CMS) makes updates to APC Grouper/Pricer and/or Fee Schedules, Independence will update the APC Grouper/Pricer within 60 days of CMS publishing such updates. The parties agree, however, that retrospective changes made by CMS shall not apply. Claim Investigation Submission When submitting a claim review request for facility pricing variances, the following information must be included in order for Independence to research your request: Inpatient claims The inquiry must include certain information, depending on your reimbursement methodology: Diagnosis related group (DRG). If you are questioning the manner in which a DRG inpatient claim is paid, the inquiry must include the following: expected DRG; its base rate; its weight; adjustment factor; whether you expect the inlier, outlier, or transfer rate. Page 10 of 11
11 Per diem. If you are questioning the manner in which a per diem inpatient claim is paid, the inquiry must include the following: revenue code(s); number of days; expected per diem rate. Outpatient fee schedule claims If you are questioning the manner in which outpatient fee schedule claims are paid, the inquiry must include the following: procedure code(s); corresponding base rate (Note: Our fee schedules are updated quarterly; therefore, please ensure you are pulling the base rate from the fee schedule that corresponds with the claim DOS); adjustment factor. APC claims If you are questioning the manner in which APC claims are paid, the inquiry must include the following: date of the APC version; adjustment factor. Note: Independence currently receives hundreds of APC pricing inquiries per month that do not meet the criteria for adjustment because the pricing differential is due to CMS retrospective updates. If you have questions about using the Claim Investigation Submission transaction, call the ebusiness Hotline at NaviNet is a registered trademark of NaviNet, Inc., an independent company. Page 11 of 11
Claim Investigation Submission Guide
 Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Claim Status Inquiry Guide. January AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey. Page 1 of 7
 Claim Status Inquiry Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 7 The NaviNet Claim Status Inquiry lets you view real-time, detailed claims information
Claim Status Inquiry Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 7 The NaviNet Claim Status Inquiry lets you view real-time, detailed claims information
Claims Dashboard Guide
 Claims Dashboard Guide July 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and with Highmark
Claims Dashboard Guide July 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and with Highmark
Eligibility and Benefits Inquiry Guide
 Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Provider Self-Service Requirements
 Provider Self-Service Requirements March 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Self-service requirements Over the last several years, AmeriHealth has instituted a number
Provider Self-Service Requirements March 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Self-service requirements Over the last several years, AmeriHealth has instituted a number
Claims INFO Adjustment Submission Guide
 Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
Precertification requirements for FEP members for BRCA testing and outpatient services
 2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
2 3 4 5 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers
Network Health Claims Editing Portal
 Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Network Health Claims Editing Portal CPT codes, descriptions and other CPT material only are copyright 2010 American Medical Association (AMA). All Rights Reserved. No fee schedules, basic units, relative
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Secure Provider Web Portal Overview 0917.MA.P.PP
 Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Secure Provider Web Portal Overview 0917.MA.P.PP Agenda Secure Web Portal Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims Review Claims Secure Messaging Administration
Referral and Prior Authorization Tool Guide
 Referral and Prior Authorization Tool Guide An Independent 1 Licensee of the Blue Cross Blue Shield Association 044509 (2-1-2018) Referral & Prior Authorization Please check the prior authorization code
Referral and Prior Authorization Tool Guide An Independent 1 Licensee of the Blue Cross Blue Shield Association 044509 (2-1-2018) Referral & Prior Authorization Please check the prior authorization code
Medicare Reimbursement Information
 Introduction to CodeMap Online A Comprehensive Medicare Resource CodeMap Online includes Medicare fee schedules, coverage policies, CCI and MUE edits, and valuable utilization data that can answer all
Introduction to CodeMap Online A Comprehensive Medicare Resource CodeMap Online includes Medicare fee schedules, coverage policies, CCI and MUE edits, and valuable utilization data that can answer all
Chapter 4 Health Care Management Unit 2: Introduction to Authorizations
 Chapter 4 Health Care Management Unit 2: Introduction to s In This Unit Topic See Page Unit 2: Introduction To s Introduction To s 2 Remember: Highmark has eliminated referral requirements; however, authorization
Chapter 4 Health Care Management Unit 2: Introduction to s In This Unit Topic See Page Unit 2: Introduction To s Introduction To s 2 Remember: Highmark has eliminated referral requirements; however, authorization
INSIDE THIS ISSUE NATIONAL PROVIDER IDENTIFIER (NPI) PREVENTIVE HEALTH
 www.ibx.com Working Together For Quality Health Care INSIDE THIS ISSUE Update your provider information with IBC Have you made any changes to your key practice information, such as your mailing address
www.ibx.com Working Together For Quality Health Care INSIDE THIS ISSUE Update your provider information with IBC Have you made any changes to your key practice information, such as your mailing address
Montgomery County Medical Society
 Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions
 WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
WV Bureau for Medical Services, KEPRO, & Molina Medicaid Solutions 1 The West Virginia Medicaid and West Virginia Children s Health Insurance Program web portal for Members and Providers provides significant
UB-04 Billing Instructions
 UB-04 Billing Instructions Updated October 2016 The UB-04 is a claim form that is utilized for Hospital Services and select residential services. Please note that these instructions are specifically written
UB-04 Billing Instructions Updated October 2016 The UB-04 is a claim form that is utilized for Hospital Services and select residential services. Please note that these instructions are specifically written
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Unit 14 Radiology Management
 Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Healthy Indiana Plan POWER Account Debit Card
 Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
Healthy Indiana Plan POWER Account Debit Card AINPEC-0499-15 Agenda Healthy Indiana Plan (HIP) POWER Account debit card First step eligibility verification Eligibility and Benefits Anthem Provider Portal
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
SECTION 9 1 CLAIMS PROCEDURES
 SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
SECTION 9 1 CLAIMS PROCEDURES Timely Filing 1 Claims Submission 1 Electronic Claims 1 Paper Claims 1 Claims for Referred Services 2 Claims for Authorized Services 2 Claims Resubmission Policy 2 Refunds
* PREPARING FOR THE TRANSITION TO HIPAA VERSION 5010: MISCELLANEOUS CHANGES IN FACILITY BILLING AS A RESULT THE TRANSITION TO VERSION 5010 *
 * PREPARING FOR THE TRANSITION TO HIPAA VERSION 5010: MISCELLANEOUS CHANGES IN FACILITY BILLING AS A RESULT OF THE TRANSITION TO VERSION 5010 * Read this bulletin on-line via NaviNet NOVEMBER 3, 2010 MS-PROV-2010-001
* PREPARING FOR THE TRANSITION TO HIPAA VERSION 5010: MISCELLANEOUS CHANGES IN FACILITY BILLING AS A RESULT OF THE TRANSITION TO VERSION 5010 * Read this bulletin on-line via NaviNet NOVEMBER 3, 2010 MS-PROV-2010-001
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 11/09/2016 *all red text is new for 11/09/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Hospital Monthly Important Message Updated as of 11/09/2016 *all red text is new for 11/09/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
HealthChoice Illinois
 HealthChoice Illinois November 2017 Presented by: Matt Wolf and Lori Lomahan Meeting Agenda Introductions Credentialing Update Billing Instructions Claims Adjudication Reimbursement Methodology MCO Website
HealthChoice Illinois November 2017 Presented by: Matt Wolf and Lori Lomahan Meeting Agenda Introductions Credentialing Update Billing Instructions Claims Adjudication Reimbursement Methodology MCO Website
edispense Vaccine Manager Coverage Inquiry
 edispense Coverage Inquiry 1 Getting Started To perform a Coverage Inquiry, open your browser, go to www.edispense5.com Click on Menu,, Coverage Inquiry 2 Enter Patient Information/Check Eligibility Select
edispense Coverage Inquiry 1 Getting Started To perform a Coverage Inquiry, open your browser, go to www.edispense5.com Click on Menu,, Coverage Inquiry 2 Enter Patient Information/Check Eligibility Select
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT
 CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
Prior Authorization and Medical Necessity Determination Processes
 Prior Authorization and Medical Necessity Determination Processes Prior authorizations (PAs) are required for inpatient admissions, various procedures, prescription medications and physical and occupational
Prior Authorization and Medical Necessity Determination Processes Prior authorizations (PAs) are required for inpatient admissions, various procedures, prescription medications and physical and occupational
Quick guide to Blue member ID cards
 Quick guide to Blue member ID cards A guide for providers who treat out-of-area Blue Cross Blue Shield members Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity
Quick guide to Blue member ID cards A guide for providers who treat out-of-area Blue Cross Blue Shield members Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity
Vermont Collaborative Care, LLC. Release date: May 15, 2013 Updates to original March 2013 Overview highlighted in yellow
 Vermont Collaborative Care, LLC Release date: May 15, 2013 Updates to original March 2013 view highlighted in yellow Vermont Collaborative Care, LLC (VCC) will begin operations on July 1, 2013. VCC was
Vermont Collaborative Care, LLC Release date: May 15, 2013 Updates to original March 2013 view highlighted in yellow Vermont Collaborative Care, LLC (VCC) will begin operations on July 1, 2013. VCC was
Clear Coverage Online Authorizations Community Health Network of CT, Inc.
 Clear Coverage Online Authorizations Community Health Network of CT, Inc. Overview Clear coverage is an online authorization tool which: Lowers authorization turn around time Improves workflow by decreasing
Clear Coverage Online Authorizations Community Health Network of CT, Inc. Overview Clear coverage is an online authorization tool which: Lowers authorization turn around time Improves workflow by decreasing
The benefits of using ExpressPAth for your practice include: Easy access. With 24/7 access, you can submit requests and get answers at any time.
 Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Getting Started The 1199SEIU Benefit Funds (the Benefit Funds) are partnering with Care Continuum, an Express Scripts, Inc. company, to help manage prior authorization requests from providers for certain
Intensive Case Management Primary Care Provider Training
 Intensive Case Management Primary Care Provider Training NaviNet Enhancements Kelley Royer-Marek Manager, Risk Adjustment Programs kroyer-marek@amerihealthcaritas.com December, 2017 What is the purpose
Intensive Case Management Primary Care Provider Training NaviNet Enhancements Kelley Royer-Marek Manager, Risk Adjustment Programs kroyer-marek@amerihealthcaritas.com December, 2017 What is the purpose
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Housekeeping. Link Participant ID with Audio. Mute your line UNMUTED. Raise your hand with questions
 Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Housekeeping Link Participant ID with Audio If your Participant ID has not been entered, dial #ParticipantID#. EXAMPLE: Participant ID is 16, then enter #16#. Mute your line UNMUTED MUTED OTHER MUTE OPTIONS
Specialty Drug Medical Benefit Management
 Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Provider Orientation. style. Click to edit Master subtitle style. December, 2017
 Click EMHS to Employee edit Master Health title Plan Provider Orientation Click to edit Master subtitle December, 2017 Pam Hageny Director of Health Plan Operations & Provider Network Beacon Health EMHS
Click EMHS to Employee edit Master Health title Plan Provider Orientation Click to edit Master subtitle December, 2017 Pam Hageny Director of Health Plan Operations & Provider Network Beacon Health EMHS
Health Information Technology and Management
 Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18
 MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18 Agenda Save Time by Utilizing the MHS Secure Web Portal: Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims
MHS Secure Provider Web Portal Overview 0718.MA.P.PP 8/18 Agenda Save Time by Utilizing the MHS Secure Web Portal: Administration Quality Reports Eligibility Member Record Patient List Authorizations Claims
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Kentucky Medicaid. Spring 2009 Billing Workshop UB04
 Kentucky Medicaid Spring 2009 Billing Workshop UB04 Agenda Representative List Reference List UB Claim Form Detailed Billing Instructions NDC (Hospitals and Renal Dialysis) Forms Timely Filing FAQ S Did
Kentucky Medicaid Spring 2009 Billing Workshop UB04 Agenda Representative List Reference List UB Claim Form Detailed Billing Instructions NDC (Hospitals and Renal Dialysis) Forms Timely Filing FAQ S Did
Availity TM Eligibility and Benefits Inquiry
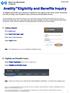 October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
Reimbursement Policy Subject: Modifier 26 and TC: Professional and Technical Component Coding 07/01/17 08/01/16 https://mediproviders.anthem.
 Anthem Blue Cross Blue Shield Medicaid Reimbursement Policy Subject: Effective Date: 07/01/17 Committee Approval Obtained: 08/01/16 Section: Coding ***** The most current version of our reimbursement policies
Anthem Blue Cross Blue Shield Medicaid Reimbursement Policy Subject: Effective Date: 07/01/17 Committee Approval Obtained: 08/01/16 Section: Coding ***** The most current version of our reimbursement policies
UB-04 Completion Guide Hospital Services
 1 3a 2 3b 4 5 6 1 2 3a Provider Name, Address, and Telephone Number Pay-to Name, Address, and Secondary ID Fields Patient Control Number Enter the provider s name and mailing address and telephone number.
1 3a 2 3b 4 5 6 1 2 3a Provider Name, Address, and Telephone Number Pay-to Name, Address, and Secondary ID Fields Patient Control Number Enter the provider s name and mailing address and telephone number.
P R O V I D E R B U L L E T I N B T J U N E 1,
 P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
Getting Started. Enter Patient Information/Check Eligibility. To perform a Coverage Inquiry, open your browser, go to
 Medicare part D Coverage Inquiry Manual Getting Started To perform a Coverage Inquiry, open your browser, go to www.mytransactrx.com Click on Menu, Part D Coverage Inquiry Enter Patient Information/Check
Medicare part D Coverage Inquiry Manual Getting Started To perform a Coverage Inquiry, open your browser, go to www.mytransactrx.com Click on Menu, Part D Coverage Inquiry Enter Patient Information/Check
Community Health Network of CT, Inc.
 PRPRE0024-0712 Clear Coverage Online Authorizations Outpatient Surgery Community Health Network of CT, Inc. A New Way to Request Authorizations As of July 31, 2012, there are now three options for requesting
PRPRE0024-0712 Clear Coverage Online Authorizations Outpatient Surgery Community Health Network of CT, Inc. A New Way to Request Authorizations As of July 31, 2012, there are now three options for requesting
Prescriber Web Prior Authorization
 Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Prescriber Web Prior Authorization Table of Contents Table of Contents Access the Prescriber Web Prior Authorization Form... 1 Patient Information... 2 Prescriber Information... 2 Diagnosis and Medical
Coordination of Benefits (COB)
 Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
Maine Chapter of the Healthcare Financial Management Association. MaineCare Provider Relations
 Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
Maine Chapter of the Healthcare Financial Management Association MaineCare Provider Relations Agenda New Drug Testing Laboratory Codes Improve your Search for Prior Authorization (PA) Completing Pathways
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Chapter 7 General Billing Rules
 7 General Billing Rules Reviewed/Revised: 10/10/2017, 07/13/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 General Information This chapter contains general information related to Health Choice Arizona
7 General Billing Rules Reviewed/Revised: 10/10/2017, 07/13/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 General Information This chapter contains general information related to Health Choice Arizona
INSTITUTIONAL. [Type text] [Type text] [Type text]
![INSTITUTIONAL. [Type text] [Type text] [Type text] INSTITUTIONAL. [Type text] [Type text] [Type text]](/thumbs/79/79654010.jpg) New York State Medicaid General Billing Guidelines [Type text] [Type text] [Type text] E M E D N Y IN F O R M A TI O N emedny is the name of the electronic New York State Medicaid system. The emedny system
New York State Medicaid General Billing Guidelines [Type text] [Type text] [Type text] E M E D N Y IN F O R M A TI O N emedny is the name of the electronic New York State Medicaid system. The emedny system
UB04 Billing Instructions
 UB04 Billing Instructions T h e U B 0 4 i s a f o r m t h a t i s u s e d t o b i l l i n s t i t u t i o n a l c l a i m s f o r h o s p i t a l and select residential services. T h i s m a n u a l g
UB04 Billing Instructions T h e U B 0 4 i s a f o r m t h a t i s u s e d t o b i l l i n s t i t u t i o n a l c l a i m s f o r h o s p i t a l and select residential services. T h i s m a n u a l g
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
RESIDENTIAL HEALTH CARE. [Type text] [Type text] [Type text] Version
![RESIDENTIAL HEALTH CARE. [Type text] [Type text] [Type text] Version RESIDENTIAL HEALTH CARE. [Type text] [Type text] [Type text] Version](/thumbs/77/75761243.jpg) New York State UB04 Billing Guidelines [Type text] [Type text] [Type text] Version 2013-01 2/11/2013 E M E D N Y I N F O R M A T I O N emedny is the name of the electronic New York State Medicaid system.
New York State UB04 Billing Guidelines [Type text] [Type text] [Type text] Version 2013-01 2/11/2013 E M E D N Y I N F O R M A T I O N emedny is the name of the electronic New York State Medicaid system.
Kareo Feature Guide Real-Time Patient Eligibility November 2009
 Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Kareo Feature Guide Real-Time Patient Eligibility November 2009 1. Overview You can perform real-time patient eligibility checks for hundreds of the nation's largest government and commercial insurance
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Chapter 6 Section 2. Hospital Reimbursement - TRICARE Diagnosis Related Group (DRG)-Based Payment System (General Description Of System)
 Diagnosis Related Groups (DRGs) Chapter 6 Section 2 Hospital Reimbursement - TRICARE Diagnosis Related Group (DRG)-Based Payment System (General Issue Date: October 8, 1987 Authority: 32 CFR 199.14(a)(1)
Diagnosis Related Groups (DRGs) Chapter 6 Section 2 Hospital Reimbursement - TRICARE Diagnosis Related Group (DRG)-Based Payment System (General Issue Date: October 8, 1987 Authority: 32 CFR 199.14(a)(1)
CHAPTER 9: CLAIM AND BILLING INFORMATION
 CHAPTER 9: CLAIM AND BILLING INFORMATION UNIT 2: THE REMITTANCE ADVICE IN THIS UNIT TOPIC SEE PAGE 9.2 THE REMITTANCE ADVICE 2 9.2 DETAIL REPORT: DATA ELEMENT DESCRIPTIONS 6 9.2 DETAIL REPORT: CLAIM ADJUSTMENT
CHAPTER 9: CLAIM AND BILLING INFORMATION UNIT 2: THE REMITTANCE ADVICE IN THIS UNIT TOPIC SEE PAGE 9.2 THE REMITTANCE ADVICE 2 9.2 DETAIL REPORT: DATA ELEMENT DESCRIPTIONS 6 9.2 DETAIL REPORT: CLAIM ADJUSTMENT
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
New York State UB-04 Billing Guidelines
 New York State UB-04 Billing Guidelines [Type text] [Type text] [Type text] Version 2018-1 2/13/2018 EMEDNY INFORMATION emedny is the name of the New York State Medicaid system. The emedny system allows
New York State UB-04 Billing Guidelines [Type text] [Type text] [Type text] Version 2018-1 2/13/2018 EMEDNY INFORMATION emedny is the name of the New York State Medicaid system. The emedny system allows
DAY TREATMENT SERVICES. [Type text] [Type text] [Type text] Version
![DAY TREATMENT SERVICES. [Type text] [Type text] [Type text] Version DAY TREATMENT SERVICES. [Type text] [Type text] [Type text] Version](/thumbs/81/83451254.jpg) New York State UB04 Billing Guidelines [Type text] [Type text] [Type text] Version 2011-01 6/1/2011 EMEDNY INFORMATION emedny is the name of the electronic New York State Medicaid system. The emedny system
New York State UB04 Billing Guidelines [Type text] [Type text] [Type text] Version 2011-01 6/1/2011 EMEDNY INFORMATION emedny is the name of the electronic New York State Medicaid system. The emedny system
Chapter 6 Section 2. Hospital Reimbursement - TRICARE DRG-Based Payment System (General Description Of System)
 Diagnostic Related Groups (DRGs) Chapter 6 Section 2 Hospital Reimbursement - TRICARE DRG-Based Payment System (General Description Of System) Issue Date: October 8, 1987 Authority: 32 CFR 199.14(a)(1)
Diagnostic Related Groups (DRGs) Chapter 6 Section 2 Hospital Reimbursement - TRICARE DRG-Based Payment System (General Description Of System) Issue Date: October 8, 1987 Authority: 32 CFR 199.14(a)(1)
Portal User Guide. Submitting Inpatient Notifications and Prior Authorization Requests. Tufts Health Together and Tufts Health Direct
 MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
MedHOK Provider Portal User Guide Submitting Inpatient Notifications and Prior Authorization Requests Tufts Health Together and Tufts Health Direct 06/2017 DMS XXXXXXX 1 MedHOK Provider Portal User Guide
2018 Independence Blue Cross Medicare Group Options
 2018 Independence Blue Cross Medicare Group Options Medical Coverage Keystone 65 Select HMO Value Standard Enhanced CovID H672, 10010705, QN, Y H673, 10010706, QN, Y H675, 10013103, QN, Y Plan premium
2018 Independence Blue Cross Medicare Group Options Medical Coverage Keystone 65 Select HMO Value Standard Enhanced CovID H672, 10010705, QN, Y H673, 10010706, QN, Y H675, 10013103, QN, Y Plan premium
INPATIENT HOSPITAL. [Type text] [Type text] [Type text] Version
![INPATIENT HOSPITAL. [Type text] [Type text] [Type text] Version INPATIENT HOSPITAL. [Type text] [Type text] [Type text] Version](/thumbs/77/75751668.jpg) New York State UB-04 Billing Guidelines [Type text] [Type text] [Type text] Version 2011-02 10/28/2011 EMEDNY INFORMATION emedny is the name of the New York State Medicaid system. The emedny system allows
New York State UB-04 Billing Guidelines [Type text] [Type text] [Type text] Version 2011-02 10/28/2011 EMEDNY INFORMATION emedny is the name of the New York State Medicaid system. The emedny system allows
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Archived SECTION 15 - BILLING INSTRUCTIONS. Section 15 - Billing Instructions
 SECTION 15 - BILLING INSTRUCTIONS 15.1 ELECTRONIC DATA INTERCHANGE...2 15.2 INTERNET ELECTRONIC CLAIM SUBMISSION...2 15.3 UB-04 CLAIM FORM...3 15.4 PROVIDER RELATIONS COMMUNICATION UNIT...3 15.5 RESUBMISSION
SECTION 15 - BILLING INSTRUCTIONS 15.1 ELECTRONIC DATA INTERCHANGE...2 15.2 INTERNET ELECTRONIC CLAIM SUBMISSION...2 15.3 UB-04 CLAIM FORM...3 15.4 PROVIDER RELATIONS COMMUNICATION UNIT...3 15.5 RESUBMISSION
CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES
 CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES UNIT 5: OUTPATIENT RADIOLOGY AND LABORATORY IN THIS UNIT TOPIC SEE PAGE Radiology Management Program Overview 2 Privileging for Radiology Services 3
CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES UNIT 5: OUTPATIENT RADIOLOGY AND LABORATORY IN THIS UNIT TOPIC SEE PAGE Radiology Management Program Overview 2 Privileging for Radiology Services 3
Administrative Guide
 Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide 2012 KanCare Program DRAFT PENDING ADDITIONAL UPDATES AND STATE OF KANSAS APPROVAL DRAFT PENDING ADDITIONAL UPDATES
Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide 2012 KanCare Program DRAFT PENDING ADDITIONAL UPDATES AND STATE OF KANSAS APPROVAL DRAFT PENDING ADDITIONAL UPDATES
Entering Payments in Aprima PRM
 Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
Entering Payments in Aprima PRM Introduction The Insurance Payment and Responsible Party Payment windows are very similar in their look and functionality, but there are some differences. The differences
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Chapter 6 Section 2. Hospital Reimbursement - TRICARE DRG-Based Payment System (General Description Of System)
 Diagnostic Related Groups (DRGs) Chapter 6 Section 2 Hospital Reimbursement - TRICARE DRG-Based Payment System (General Description Of System) Issue Date: October 8, 1987 Authority: 32 CFR 199.14(a)(1)
Diagnostic Related Groups (DRGs) Chapter 6 Section 2 Hospital Reimbursement - TRICARE DRG-Based Payment System (General Description Of System) Issue Date: October 8, 1987 Authority: 32 CFR 199.14(a)(1)
Provider Healthcare Portal Demonstration:
 Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Provider Healthcare Portal Demonstration: Claim Denials Professional Claims (CMS-1500) HPE October 2016 Agenda Getting started Searching claims Copying and correcting claims Most common denials; how to
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
(MO HealthNet) Text Telephone Medical Claims Reimbursement Rate Dispute Medical Necessity Appeal. Attn: Claim Disputes
 KEY CONTACTS The following chart includes several important telephone and fax numbers available to your office. When calling, please have the following information available: NPI (National Provider Identifier)
KEY CONTACTS The following chart includes several important telephone and fax numbers available to your office. When calling, please have the following information available: NPI (National Provider Identifier)
Choice 100+ Frequently Asked Questions Brokers and Producers
 Choice 100+ Frequently Asked Questions Brokers and Producers 1 Choice 100+ Frequently Asked Questions Q: Who do members call for assistance for medical, pharmacy, dental, or vision? A: For questions about
Choice 100+ Frequently Asked Questions Brokers and Producers 1 Choice 100+ Frequently Asked Questions Q: Who do members call for assistance for medical, pharmacy, dental, or vision? A: For questions about
C H A P T E R 9 : Billing on the UB Claim Form
 C H A P T E R 9 : Billing on the UB Claim Form Reviewed/Revised: 10/1/2018 9.0 INTRODUCTION The UB claim form is used to bill for all hospital inpatient, outpatient, emergency room services, dialysis clinic,
C H A P T E R 9 : Billing on the UB Claim Form Reviewed/Revised: 10/1/2018 9.0 INTRODUCTION The UB claim form is used to bill for all hospital inpatient, outpatient, emergency room services, dialysis clinic,
HOW TO SUBMIT OWCP-04 BILLS TO ACS
 HOW TO SUBMIT OWCP-04 BILLS TO ACS OFFICE OF WORKERS COMPENSATION PROGRAMS DIVISION OF ENERGY EMPLOYEES OCCUPATIONAL ILLNESS COMPENSATION The following services should be billed on the OWCP-04 Form: General
HOW TO SUBMIT OWCP-04 BILLS TO ACS OFFICE OF WORKERS COMPENSATION PROGRAMS DIVISION OF ENERGY EMPLOYEES OCCUPATIONAL ILLNESS COMPENSATION The following services should be billed on the OWCP-04 Form: General
GENERAL BENEFIT INFORMATION
 Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Availity ' Eligibility and Benefits SM'
 Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop
 CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
CT Transition of SAGA Clients to Medicaid Low Income Adults (Medicaid LIA) Workshop Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Overview Recoupment of SAGA
Medicare Advantage Outreach and Education Bulletin
 Medicare Advantage Outreach and Education Bulletin Anthem Blue Cross Medicare Advantage Reimbursement Policy Changes: Second Communication Update Anthem Medicare Advantage published Medicare Advantage
Medicare Advantage Outreach and Education Bulletin Anthem Blue Cross Medicare Advantage Reimbursement Policy Changes: Second Communication Update Anthem Medicare Advantage published Medicare Advantage
Patient Billing and Financial Services
 Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
Second quarter provider updates. July 2016
 Second quarter provider updates July 2016 Agenda Introductions Healthy Indiana Plan (HIP) debit card Claim disputes Behavioral health Updated Network Relations representatives map 2 HIP debit card - Background
Second quarter provider updates July 2016 Agenda Introductions Healthy Indiana Plan (HIP) debit card Claim disputes Behavioral health Updated Network Relations representatives map 2 HIP debit card - Background
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 A (3/15) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Chapter 7. Billing and Claims Processing
 Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Using the Availity Web Portal
 Using the Availity Web Portal The Availity multi payer Web Portal presented by Anthem and Availity 2016 Annual Workshop What we will cover Healthy Indiana Plan (HIP) overview POWER Account Visa debit card
Using the Availity Web Portal The Availity multi payer Web Portal presented by Anthem and Availity 2016 Annual Workshop What we will cover Healthy Indiana Plan (HIP) overview POWER Account Visa debit card
Physical Therapy. Contact your Primary Access Administrator (PAA) if Eligibility and Benefits is not listed in the navigation menu.
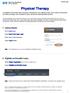 October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
Connecticut Medical Assistance Program Long Term Care Refresher Workshop. Presented by: The Department of Social Services & HP for Billing Providers
 Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
Connecticut Medical Assistance Program Long Term Care Refresher Workshop Presented by: The Department of Social Services & HP for Billing Providers Training Topics www.ctdssmap.com Web Portal Demographic
Welcome to Blue Cross Commercial Risk Adjustment Webinar
 Welcome to Blue Cross Commercial Risk Adjustment Webinar For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background
Welcome to Blue Cross Commercial Risk Adjustment Webinar For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background
Chapter 9 Billing on the UB Claim Form
 9 Billing on the UB Claim Form Reviewed/Revised: 10/10/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 Introduction The UB claim form is used to bill for all hospital inpatient, outpatient, emergency
9 Billing on the UB Claim Form Reviewed/Revised: 10/10/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 Introduction The UB claim form is used to bill for all hospital inpatient, outpatient, emergency
Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage
 Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage Effective January 1, 2008 through December 31, 2008 1-800-645-3965 TTY/TDD: 1-888-857-4816 Seven days a week 8 a.m. 8
Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage Effective January 1, 2008 through December 31, 2008 1-800-645-3965 TTY/TDD: 1-888-857-4816 Seven days a week 8 a.m. 8
