Precertification requirements for FEP members for BRCA testing and outpatient services
|
|
|
- Jayson Price
- 6 years ago
- Views:
Transcription
1 INSIDE THIS EDITION Reminder: Delinquent payment indicator on NaviNet for APTC members Learn about a field that informs providers when APTC members are delinquent in paying their premiums Providers financially responsible for preapproval/precertification of inpatient facility services for Understand provider responsibility for preapproval of inpatient facility services for Expediting medical record requests from the Host Plan Read about the importance of completing medical record requests from a Host Plan in a timely way Use the Medical Policy/ Precertification Router for Find coverage requirements for through NaviNet Ask to complete the COB Questionnaire with other registration forms Have complete the COB Questionnaire before receiving services WINTER 2015 Precertification requirements for FEP members for BRCA testing and outpatient services Effective January 1, 2015, BRCA (breast cancer gene) testing requires precertification for members who have coverage under the Federal Employee Program (FEP). As previously communicated, the services listed below also now require precertification: outpatient intensity-modulated radiation therapy (IMRT), except related to the treatment of head, neck, anal canal, anal, breast, or prostate cancer (Note: Brain cancer is not considered a form of head or neck cancer; therefore, precertification is required for IMRT treatment of brain cancer); outpatient surgery for morbid obesity (refer to the Service Benefit Plan summary at benefit-plans-brochures-and-forms/#tab-brochures for specific pre-surgical criteria that must be met); outpatient surgical correction of congenital anomalies; outpatient surgery needed to correct accidental injuries to the jaw, cheeks, lips, tongue, and roof or floor of mouth. Services must meet the requirements listed in the applicable FEP medical policies, which are available on the FEP website at Scroll to the bottom of the page and select Medical Policies. To obtain precertification for services for BRCA testing or outpatient services for FEP members, call Highmark Blue Shield, an independent company, at As a reminder, precertification requests for inpatient and hospice services for FEP members will continue to be performed by Independence. Failure to obtain precertification will result in a retrospective review to determine compliance with FEP medical policies. Should services be denied for lack of medical necessity, reimbursement will not be made and the member may not be billed. v
2 Reminder: Delinquent payment indicator on NaviNet for APTC members The Advanced Premium Tax Credit (APTC) is part of the Patient Protection and Affordable Care Act, also known as Health Care Reform. The APTC helps qualifying individuals and families obtain health insurance by reducing monthly premiums. Health Care Reform mandates a three-month (i.e., 90-day) grace period for individual APTC members who are delinquent in paying their portion of the premiums. Under the mandate, insurers are required to pay medical claims received during the first 30 days of the grace period, but they may pend medical claims for services rendered to those members and their eligible dependents during the second and third months of the grace period. If payment is not received by the end of the grace period, the pended claims will be denied and the member s policy will be terminated. Delinquent payment indicator A field called APTC displays within the Eligibility and Benefits Details screen on the NaviNet web portal to show providers when a patient is in the grace period and to provide a status of the member s claims. When an APTC member is delinquent on his or her monthly insurance premiums, the APTC member indicator and current status will display on the Eligibility and Benefits Details screen. The current status includes (1) the number of months that the member is delinquent, (2) whether the insurance company will pay, suspend, or deny the member s medical claims. Note: The APTC field will only display when an APTC member is in a delinquency status. If an APTC member s claim is suspended due to a delinquent payment, the corresponding code and reason will also appear within the claim line in the Claims Status Inquiry transaction. Select Additional Details for an explanation of why the claim is not yet finalized. For more information To help you navigate information for APTC members who have a delinquent payment, a user guide is available in the NaviNet Transaction Changes section of our Business Transformation site at If you have any questions about NaviNet transactions, please call the ebusiness Hotline at v 2
3 Providers financially responsible for preapproval/precertification of inpatient facility services for Participating providers are financially responsible for obtaining preapproval/ precertification for inpatient facility services for, and are held harmless for these services. While most providers currently obtain preapproval/precertification for inpatient facility services, this new requirement moved financial responsibility for lack of preapproval/precertification from the member to the provider. Failure to obtain preapproval/precertification for inpatient facility services for will result in a denied claim. To avoid claim denials, it is important to preapprove/precertify the inpatient stay and check that additional days are authorized before an out-of-area member is discharged. Providers must notify the member s Home Plan of the following: within 48 hours, notify of any changes to the original pre-service review; within 72 hours, notify of emergency/urgent pre-service review. Inpatient stay extensions for DRG/case rate facilities In diagnosis related group (DRG)/case rate situations, when the length of an inpatient stay extends beyond the preapproved/precertified length of stay, any additional days should be approved by the last day of the originally approved days. For example, if five days are approved by the Home Plan and the patient has not been discharged by the fifth day, the provider should contact the Home Plan and ask to have the authorization updated. Please ensure that you seek approval of additional days to avoid payment issues. Denied days within an approved inpatient stay for non-drg/ case rate facilities In non-drg/case rate situations, if there are denied days within an approved inpatient stay, the provider will be financially liable for the denied days and the member will be held harmless. Get preapproval/precertification electronically Independence offers Electronic Provider Access (EPA) through the NaviNet web portal to access the provider portal of an out-of-area member s Home Plan and conduct electronic pre-service reviews. Please note that providers may still need to call the member s Home Plan to request preapproval/ precertification if the Home Plan does not offer electronic pre-service review. The Pre-Service Review for Out-of-Area Members transaction is available under the Blue Exchange Out of Area option in the menu of plan transactions. A user guide for this transaction is available in the NaviNet Transaction Changes section of our Business Transformation site at pnc/businesstransformation. If you have any questions regarding NaviNet transaction changes, call the ebusiness Hotline at Note: Providers can also get preapproval/precertification for out-of-area members by calling the BlueCard Eligibility line at BLUE and asking to be transferred to the utilization review area. v Expediting medical record requests from the Host Plan When a Host Plan receives a request for medical records from a Home Plan, it is very important that the records be sent in a timely manner to ensure that the provider is reimbursed and the services rendered by the out-of-area member are covered appropriately. To expedite the handling for Host Plan medical record requests, please adhere to the following tips and guidelines: Include a copy of the request letter with the medical records. Submit medical records by fax or for the quickest processing. Only send the medical records that have been requested. Note: Independence cannot forward unsolicited medical records to another plan. Host Plan medical records can be sent in the following ways: Fax. Securely fax medical records to medical records to Mail. If you do not have access to fax or , send medical records on a CD or in hardcopy to: Host Medical Records Department 1901 Market Street SG1 Philadelphia, PA Note: This information does not apply to medical record requests directly from a Home Plan or to appeals. v Reminder: Appeals sent should clearly indicate the patient s name, member ID number (including alpha prefix), and claim number, when applicable. 3
4 Use the Medical Policy/Precertification Router for Understanding a benefit plan s precertification requirements is crucial for both members and providers. Because providers typically obtain precertification on behalf of members, it is important that they have easy access to information about these requirements. In the BlueCard environment, medical policy and precertification requirements are dictated by the Home Plan. Local providers may be unaware when the Home Plan s medical policy or precertification requirements are different from the local Plan s requirements. Use the Medical Policy/Precertification Router Using the Medical Policy/Precertification Router on the NaviNet web portal, you will be routed to the Home Plan s website that contains medical policies and general precertification requirements. This transition happens seamlessly based on the alpha prefix of the out-of-area member s Plan, and it gives providers easy access to medical policy and precertification requirements. To view medical policy and precertification requirements for out-of-area Blue members, select Medical Policy/PreCert Inquiry from the BlueExchange Out of Area option in the menu of plan transactions. Then to conduct a search, select Medical Policy or Pre-Certification from the drop-down menu under Type of Inquiry. Simply enter the alpha prefix noted on the member s ID card and select Submit. The information that will be displayed is provided by the member s Home Plan. If you have any questions regarding the information, please contact the member s Home Plan. v 4
5 Dependent(s) listed on the other insurance Policyholder s Employer INSIDE IPP WINTER 2015 Additional resources For BlueCard facility claims, call ASK-BLUE ( ). For questions about BlueCard eligibility, call the BlueCard Eligibility line at BLUE ( ). Inside IPP is a publication of Independence Blue Cross and its affiliates (Independence). Suggestions are welcome. Contact information Provider Communications Independence Blue Cross 1901 Market Street, 27th floor Philadelphia, PA provider_communications@ibx.com NaviNet is a registered trademark of NaviNet, Inc., an independent company. CPT copyright 2013 American Medical Association. All rights reserved. CPT is a registered trademark of the American Medical Association. Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East and QCC Insurance Company, and with Highmark Blue Shield independent licensees of the Blue Cross and Blue Shield Association. Ask to complete the COB Questionnaire with other registration forms Coordination of benefits (COB) refers to how the Blue System ensures that members receive full benefits and prevents double payment for services when he or she has coverage from two or more sources. When providing services to out-of-area* Blue members, it is important that they complete the COB Questionnaire for the following reasons: streamlined claims processing; expedited payment to providers; reduction in the number of denials related to COB; ability for employer groups to finalize out-of-area claims for their employees. Instructions for completing the questionnaire Out-of-area Blue members should complete the COB Questionnaire with other registration forms. The questionnaire is available on our website at /claims_and_billing/bluecard. html or through the NaviNet web portal by selecting BlueCard COB Questionnaire from the BlueExchange Out of Area option in the menu of plan transactions. Office staff should complete the first two fields of the questionnaire: provider name and NPI. Then, the out-of-area member should complete the remaining sections of the questionnaire before services are rendered. Please immediately process the completed questionnaire by faxing it to or by mailing it to the address printed on the first page of the questionnaire. If you have any questions about this important process, contact your Network Coordinator. Note: The COB Questionnaire should not be used for local Independence members or Federal Employee Program members. v *Out-of-area members are members of other Blue Cross and Blue Shield plans who travel or live in the Independence five-county service area, which includes Philadelphia, Bucks, Montgomery, Chester, and Delaware counties. Coordination of Benefits Questionnaire: Out of Area Members Provider: After the policy holder has completed and signed, please forward this form to your local Blue Cross and/or Blue Shield Plan immediately. Do not hold to submit with the claim. Please fax or mail this form to the following: PO Box Harrisburg, PA Fax: Member: Your Blue Cross and/or Blue Shield contract may contain a Coordination of Benefits (COB) provision. Your Plan depends upon your help in order to process your claims correctly and appreciates your prompt and accurate reply. If any of the information below changes, please contact your Blue Cross and/or Blue Shield Plan immediately. Provider Name NPI (Give Tax ID if No NPI Number) Policyholder Last Name Policyholder First Name Group Number Member ID Number with Three Letter Prefix (Must Include Plan Alpha Prefix) Section A Other Insurance If this does not apply, check No and skip to Section B Are you or any other member of this Blue Cross Blue Shield policy covered by another medical or dental insurance policy, any other Blue Cross Blue Shield policy or Medicare? No If No, please complete Section D, sign, date and return this questionnaire to us, indicating No other insurance. Yes If Yes, please complete all the fields below that pertain to the member(s) that has the other coverage. Mark those that apply: Other Health Insurance Other Dental Insurance What type of policy is this? Group Individual Policy Student Policy Medicare Supplemental Other Insurance Carrier s Name Address Address State Zip Phone Number Other Insurance Policyholder s Name Policyholder s Date of Birth ID Number Effective Date of Other Insurance If Cancelled, Cancellation Date Is the policy holder: Actively working for the group Inactive Retired, retirement date: On COBRA, which began: Address City State Zip Phone Number 5
Eligibility and Benefits Inquiry Guide
 Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Eligibility and Benefits Inquiry Guide February 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Claim Investigation Submission Guide
 Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Claim Investigation Submission Guide August 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company,
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Claims Dashboard Guide
 Claims Dashboard Guide July 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and with Highmark
Claims Dashboard Guide July 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and with Highmark
Claims INFO Adjustment Submission Guide
 Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
Claims INFO Adjustment Submission Guide Revised March 2013 Overview Claims adjustments can be performed only on claims in a Paid or Denied status and are allowable during a period of up to 18 months following
Quick guide to Blue member ID cards
 Quick guide to Blue member ID cards A guide for providers who treat out-of-area Blue Cross Blue Shield members Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity
Quick guide to Blue member ID cards A guide for providers who treat out-of-area Blue Cross Blue Shield members Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity
Questions and Answers
 Questions and Answers Radiation Oncology Utilization Management Program Why did Florida Blue implement a radiation oncology utilization management program? The purpose of the program is to ensure radiation
Questions and Answers Radiation Oncology Utilization Management Program Why did Florida Blue implement a radiation oncology utilization management program? The purpose of the program is to ensure radiation
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
INSIDE THIS ISSUE NATIONAL PROVIDER IDENTIFIER (NPI) PREVENTIVE HEALTH
 www.ibx.com Working Together For Quality Health Care INSIDE THIS ISSUE Update your provider information with IBC Have you made any changes to your key practice information, such as your mailing address
www.ibx.com Working Together For Quality Health Care INSIDE THIS ISSUE Update your provider information with IBC Have you made any changes to your key practice information, such as your mailing address
Inter-Plan Operations (BlueCard )
 Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Chapter 7. Billing and Claims Processing
 Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Chapter 7. Billing and Claims Processing 7.1 Electronic Claims Submission 3 7.1.1 How it Works... 3 7.1.2 Advantages... 3 7.1.3 How to Initiate... 4 7.1.4 Transactions Available... 5 7.1.5 NAIC Codes...
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Servicing Out-of-Area Blue Members BlueShield of Northeastern New York BlueCard 101 May 31, 2011 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Claim Investigation Submission Guide
 Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Claim Investigation Submission Guide January 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Page 1 of 9 The Claim Investigation Submission transaction lets you submit questions
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Servicing Out-of-Area Blue Members BlueCross BlueShield of Western New York BlueCard 101 May 31, 2011 A presentation of the Blue Cross and Blue Shield Association. All rights reserved. Servicing Out-of-Area
Health. AmeriHealth New Jersey to Transition to Electronic Referral Submission
 P A R T N E R S Health in W O R K I N G T O G E T H E R F O R Q U A L I T Y H E A L T H C A R E INSIDE THIS ISSUE: MARCH 2005 ANNOUNCEMENTS Enhanced Provider Search Launching this Spring Restorative/Therapy
P A R T N E R S Health in W O R K I N G T O G E T H E R F O R Q U A L I T Y H E A L T H C A R E INSIDE THIS ISSUE: MARCH 2005 ANNOUNCEMENTS Enhanced Provider Search Launching this Spring Restorative/Therapy
Specialty Drug Medical Benefit Management
 Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Specialty Drug Medical Benefit Management Agenda Introduction Specialty Medical Benefit Management (SMBM) Strategy Prior Authorization Process Other Important Information Provider Tools Provider Relations
Arkansas Blue Cross and Blue Shield
 Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access audio conference: 877-497-8913 Conference code: 132-281-9809# Please Mute Your
Availity TM Eligibility and Benefits Inquiry
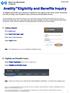 October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
AWAY FROM HOME CARE GUEST MEMBERSHIP APPLICATION
 AWAY FROM HOME CARE GUEST MEMBERSHIP APPLICATION Please print clearly. Application must be completed and signed by the subscriber. All five pages must be completed and returned. Today s date: Guest membership
AWAY FROM HOME CARE GUEST MEMBERSHIP APPLICATION Please print clearly. Application must be completed and signed by the subscriber. All five pages must be completed and returned. Today s date: Guest membership
Physical Therapy. Contact your Primary Access Administrator (PAA) if Eligibility and Benefits is not listed in the navigation menu.
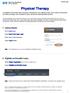 October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
Vermont Collaborative Care, LLC. Release date: May 15, 2013 Updates to original March 2013 Overview highlighted in yellow
 Vermont Collaborative Care, LLC Release date: May 15, 2013 Updates to original March 2013 view highlighted in yellow Vermont Collaborative Care, LLC (VCC) will begin operations on July 1, 2013. VCC was
Vermont Collaborative Care, LLC Release date: May 15, 2013 Updates to original March 2013 view highlighted in yellow Vermont Collaborative Care, LLC (VCC) will begin operations on July 1, 2013. VCC was
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Unit 14 Radiology Management
 Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
Montgomery County Medical Society
 Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Montgomery County Medical Society CareFirst BlueCross BlueShield Presentation November 12, 2015 CareFirst BlueCross BlueShield is the shared business name of CareFirst of Maryland, Inc. and Group Hospitalization
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
The BlueCard Program Provider Manual. March 2018
 M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
M The BlueCard Program Provider Manual March 2018 Page: 2 of 31 Table of Contents Table of Contents... 2 1. Introduction: The BlueCard Program Makes Filing Claims Easy... 3 2. What is the BlueCard Program?...
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES
 CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES UNIT 5: OUTPATIENT RADIOLOGY AND LABORATORY IN THIS UNIT TOPIC SEE PAGE Radiology Management Program Overview 2 Privileging for Radiology Services 3
CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES UNIT 5: OUTPATIENT RADIOLOGY AND LABORATORY IN THIS UNIT TOPIC SEE PAGE Radiology Management Program Overview 2 Privileging for Radiology Services 3
CHAPTER 3: MEMBER INFORMATION
 CHAPTER 3: MEMBER INFORMATION UNIT 4: COORDINATION OF BENEFITS IN THIS UNIT TOPIC SEE PAGE 3.4 COORDINATION OF BENEFITS (COB) 2 3.4 COB: TWO AND THREE PAYER CLAIMS Updated! 4 3.4 FREQUENTLY ASKED QUESTIONS
CHAPTER 3: MEMBER INFORMATION UNIT 4: COORDINATION OF BENEFITS IN THIS UNIT TOPIC SEE PAGE 3.4 COORDINATION OF BENEFITS (COB) 2 3.4 COB: TWO AND THREE PAYER CLAIMS Updated! 4 3.4 FREQUENTLY ASKED QUESTIONS
2012 ALL PAYERS WORKSHOP BLUE CROSS AND BLUE SHIELD OF KANSAS AGENDA
 2012 ALL PAYERS WORKSHOP BLUE CROSS AND BLUE SHIELD OF KANSAS AGENDA Connecting with Providers Other Party Liability (OPL) Quality Based Reimbursement Program (QBRP) Electronic Data Interchange (EDI) 1
2012 ALL PAYERS WORKSHOP BLUE CROSS AND BLUE SHIELD OF KANSAS AGENDA Connecting with Providers Other Party Liability (OPL) Quality Based Reimbursement Program (QBRP) Electronic Data Interchange (EDI) 1
Choice 100+ Frequently Asked Questions Brokers and Producers
 Choice 100+ Frequently Asked Questions Brokers and Producers 1 Choice 100+ Frequently Asked Questions Q: Who do members call for assistance for medical, pharmacy, dental, or vision? A: For questions about
Choice 100+ Frequently Asked Questions Brokers and Producers 1 Choice 100+ Frequently Asked Questions Q: Who do members call for assistance for medical, pharmacy, dental, or vision? A: For questions about
BlueCard Tutorial Requesting Authorizations
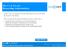 BlueCard Tutorial Requesting Authorizations Learn how to request an authorization for out-of-state Blue plan members. After completing the Requesting Authorizations tutorial, you will be able to: Locate
BlueCard Tutorial Requesting Authorizations Learn how to request an authorization for out-of-state Blue plan members. After completing the Requesting Authorizations tutorial, you will be able to: Locate
2015 Summary of Benefits
 2015 Summary of Benefits Effective January 1, 2015, through December 31, 2015 H3909 Y0041_H3909_PC_15_18889 Accepted 09/01/2014 Section I: Introduction to Summary of Benefits You have choices about how
2015 Summary of Benefits Effective January 1, 2015, through December 31, 2015 H3909 Y0041_H3909_PC_15_18889 Accepted 09/01/2014 Section I: Introduction to Summary of Benefits You have choices about how
CHAPTER 5: PROGRAM INFORMATION
 CHAPTER 5: PROGRAM INFORMATION UNIT 3: THE BLUECARD PROGRAM IN THIS UNIT TOPIC SEE PAGE 5.3 INTRODUCTION 2 5.3 WHAT IS THE BLUECARD PROGRAM? 3 5.3 HOW THE BLUECARD PROGRAM WORKS: AN EXAMPLE 5 5.3 HOW TO
CHAPTER 5: PROGRAM INFORMATION UNIT 3: THE BLUECARD PROGRAM IN THIS UNIT TOPIC SEE PAGE 5.3 INTRODUCTION 2 5.3 WHAT IS THE BLUECARD PROGRAM? 3 5.3 HOW THE BLUECARD PROGRAM WORKS: AN EXAMPLE 5 5.3 HOW TO
UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION
 CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
DELAWARE CHILDREN S CARE PLAN
 DELAWARE CHILDREN S CARE PLAN About DCCP Available through Highmark Blue Cross Blue Shield Delaware (Highmark Delaware), the Delaware Children s Care Plan (DCCP) provides comprehensive health benefits
DELAWARE CHILDREN S CARE PLAN About DCCP Available through Highmark Blue Cross Blue Shield Delaware (Highmark Delaware), the Delaware Children s Care Plan (DCCP) provides comprehensive health benefits
Prior Authorization and Medical Necessity Determination Processes
 Prior Authorization and Medical Necessity Determination Processes Prior authorizations (PAs) are required for inpatient admissions, various procedures, prescription medications and physical and occupational
Prior Authorization and Medical Necessity Determination Processes Prior authorizations (PAs) are required for inpatient admissions, various procedures, prescription medications and physical and occupational
For Participating Rehabilitation Therapists May 2006
 For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
For Participating Rehabilitation Therapists May 2006 Updating coding resources A recent event illustrates the need to keep coding references updated. The 2006 ICD-9-CM code book published by a particular
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PA of Educators Benefit Services, Inc. Enrolling Group Number: 717578
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PA of Educators Benefit Services, Inc. Enrolling Group Number: 717578
Blue Cross OGB-dedicated Customer Service:
 Blue Cross OGB-dedicated Customer Service: 1.800.392.4089 Frequently Asked uestions Blue Cross and Blue Shield of Louisiana administers benefits for the Office of Group Benefits (OGB) for their PPO, HMO
Blue Cross OGB-dedicated Customer Service: 1.800.392.4089 Frequently Asked uestions Blue Cross and Blue Shield of Louisiana administers benefits for the Office of Group Benefits (OGB) for their PPO, HMO
* PREPARING FOR THE TRANSITION TO HIPAA VERSION 5010: MISCELLANEOUS CHANGES IN FACILITY BILLING AS A RESULT THE TRANSITION TO VERSION 5010 *
 * PREPARING FOR THE TRANSITION TO HIPAA VERSION 5010: MISCELLANEOUS CHANGES IN FACILITY BILLING AS A RESULT OF THE TRANSITION TO VERSION 5010 * Read this bulletin on-line via NaviNet NOVEMBER 3, 2010 MS-PROV-2010-001
* PREPARING FOR THE TRANSITION TO HIPAA VERSION 5010: MISCELLANEOUS CHANGES IN FACILITY BILLING AS A RESULT OF THE TRANSITION TO VERSION 5010 * Read this bulletin on-line via NaviNet NOVEMBER 3, 2010 MS-PROV-2010-001
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT
 CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona
 Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Blue Medicare HMO Blue Medicare PPO
 Blue Medicare HMO Blue Medicare PPO Medicare Fast Track Appeals Medicare Fast Track Appeals An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and BlueShield
Blue Medicare HMO Blue Medicare PPO Medicare Fast Track Appeals Medicare Fast Track Appeals An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and BlueShield
WINASAP: A step-by-step walkthrough. Updated: 2/21/18
 WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
WINASAP: A step-by-step walkthrough Updated: 2/21/18 Welcome to WINASAP! WINASAP allows a submitter the ability to submit claims to Wyoming Medicaid via an electronic method, either through direct connection
BCBSNC Welcome! Health Insurance Institute North Carolina Healthcare Financial Management Association
 BCBSNC Welcome! Health Insurance Institute 2010 North Carolina Healthcare Financial Management Association Workshop Overview HealthCare Reform ICD-10 Inter-Plan Programs Blue Medicare HMO/PPO Federal Employee
BCBSNC Welcome! Health Insurance Institute 2010 North Carolina Healthcare Financial Management Association Workshop Overview HealthCare Reform ICD-10 Inter-Plan Programs Blue Medicare HMO/PPO Federal Employee
Ambulance and Emergency Medical Transport Services
 Ambulance and Emergency Medical Transport Services Understanding the basics of BCBSNC processes An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Agenda + Enrollment +
Ambulance and Emergency Medical Transport Services Understanding the basics of BCBSNC processes An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Agenda + Enrollment +
When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective?
 GENERAL When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective? The bill has been signed into law by the Governor and will be effective July 1, 2008. However, DCH
GENERAL When will the Medicaid Care Management Organizations Act (AKA: House Bill 1234) be effective? The bill has been signed into law by the Governor and will be effective July 1, 2008. However, DCH
2015 BlueCross BlueShield of South Carolina PROVIDER OFFICE ADMINISTRATIVE MANUAL
 2015 BlueCross BlueShield of South Carolina PROVIDER OFFICE ADMINISTRATIVE MANUAL Introduction BlueCross BlueShield of South Carolina is committed to providing quality service, education and problem resolution
2015 BlueCross BlueShield of South Carolina PROVIDER OFFICE ADMINISTRATIVE MANUAL Introduction BlueCross BlueShield of South Carolina is committed to providing quality service, education and problem resolution
Availity ' Eligibility and Benefits SM'
 Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
This Issue: Subsidies and Grace Periods October 2013
 hcrnews provider New Rules, New Challenges, New Opportunities Provider HCR (health care reform) News is a monthly special edition publication for network providers from the Network Administration Division
hcrnews provider New Rules, New Challenges, New Opportunities Provider HCR (health care reform) News is a monthly special edition publication for network providers from the Network Administration Division
Health Insurance Marketplaces (Exchanges)
 Health Insurance Marketplaces (Exchanges) Essential Health Benefits Starting in 2014, non-grandfathered health plans in the individual and small group markets, within the Health Insurance Marketplace (exchanges),
Health Insurance Marketplaces (Exchanges) Essential Health Benefits Starting in 2014, non-grandfathered health plans in the individual and small group markets, within the Health Insurance Marketplace (exchanges),
1. Women s Health and Cancer Rights Act of 1998 (WHCRA)
 Medical Coverage Policy Mastectomy Treatment, Breast Reconstruction and Mastectomy Hospital Stays Mandates EFFECTIVE DATE: 01 01 2019 POLICY LAST UPDATED: 10 16 2018 OVERVIEW This policy documents coverage
Medical Coverage Policy Mastectomy Treatment, Breast Reconstruction and Mastectomy Hospital Stays Mandates EFFECTIVE DATE: 01 01 2019 POLICY LAST UPDATED: 10 16 2018 OVERVIEW This policy documents coverage
HOST CLAIM VOLUMES 2009
 1 CLAIMS Claims HOST CLAIM VOLUMES 2009 2 Mountain State Host/Par Claims 3 Medical Policy and Pre-Certification/Pre-Auth Router 4 Medical Policy and Pre-certification/ Pre-Authorization Router Effective
1 CLAIMS Claims HOST CLAIM VOLUMES 2009 2 Mountain State Host/Par Claims 3 Medical Policy and Pre-Certification/Pre-Auth Router 4 Medical Policy and Pre-certification/ Pre-Authorization Router Effective
updatesm July 2016 Updated InterQual guidelines for 2016 page 8 Claim notifications and common ICD coding errors on paper and electronic claims page 5
 updatesm July 2016 Claim notifications and common ICD coding errors on paper and electronic claims page 5 Updated InterQual guidelines for 2016 page 8 Utilization management program for genetic/ genomic
updatesm July 2016 Claim notifications and common ICD coding errors on paper and electronic claims page 5 Updated InterQual guidelines for 2016 page 8 Utilization management program for genetic/ genomic
Provider Manual. The BlueCard Program
 The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
HSA-qualified High-deductible Health Plans. A new way to manage your health care costs. Colorado
 HSA-qualified High-deductible Health Plans A new way to manage your health care costs An independent licensee of the Blue Cross and Blue Shield Association. Anthem Blue Cross and Blue Shield is the trade
HSA-qualified High-deductible Health Plans A new way to manage your health care costs An independent licensee of the Blue Cross and Blue Shield Association. Anthem Blue Cross and Blue Shield is the trade
ProviderNews PLEASE SHARE WITH YOUR APPROPRIATE CLINIC PERSONNEL December 2015
 PLEASE SHARE WITH YOUR APPROPRIATE CLINIC PERSONNEL December 2015 Important: To ensure that your questions are answered by the appropriate person, we have created new email addresses. Please use one of
PLEASE SHARE WITH YOUR APPROPRIATE CLINIC PERSONNEL December 2015 Important: To ensure that your questions are answered by the appropriate person, we have created new email addresses. Please use one of
Yavapai Unified Employee Benefit Trust
 Yavapai Unified Employee Benefit Trust Group No.: 13853 Plan Document and Summary Plan Description Amended and Restated Effective: July 1, 2016 18444 N. 25th Avenue #410 Phoenix, AZ 85023 (866) 300-8449
Yavapai Unified Employee Benefit Trust Group No.: 13853 Plan Document and Summary Plan Description Amended and Restated Effective: July 1, 2016 18444 N. 25th Avenue #410 Phoenix, AZ 85023 (866) 300-8449
GENERAL Why is BlueCross and BlueChoice implementing an MSK Program focused on interventional pain management procedures?
 Musculoskeletal Care Management (MSK) Program Interventional Pain Management (IPM) Frequently Asked Questions (FAQ s) For BlueCross BlueShield of South Carolina 1 and BlueChoice HealthPlan of South Carolina
Musculoskeletal Care Management (MSK) Program Interventional Pain Management (IPM) Frequently Asked Questions (FAQ s) For BlueCross BlueShield of South Carolina 1 and BlueChoice HealthPlan of South Carolina
Understanding Your Health Care Benefits
 Understanding Your Health Care Benefits A Handbook For Employees of Air Products and Chemicals, Inc. Preferred Provider Organization Program 2013 TABLE OF CONTENTS I. Introduction... 1 II. Member Services...
Understanding Your Health Care Benefits A Handbook For Employees of Air Products and Chemicals, Inc. Preferred Provider Organization Program 2013 TABLE OF CONTENTS I. Introduction... 1 II. Member Services...
RECONTRACTING 10/31/2016. Aetna Medicare Advantage. Aetna Behavioral Health
 DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Other Coverage Questionnaire
 PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
Anthem Blue Cross and Blue Shield Medicare Advantage Reimbursement Policy Changes and Code Editing Enhancements
 Medicare Advantage Outreach and Education Bulletin Anthem Blue Cross and Blue Shield Medicare Advantage Reimbursement Policy Changes and Code Editing Enhancements Summary of changes: Code Editing Enhancements
Medicare Advantage Outreach and Education Bulletin Anthem Blue Cross and Blue Shield Medicare Advantage Reimbursement Policy Changes and Code Editing Enhancements Summary of changes: Code Editing Enhancements
Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage
 Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage Effective January 1, 2008 through December 31, 2008 1-800-645-3965 TTY/TDD: 1-888-857-4816 Seven days a week 8 a.m. 8
Keystone 65 Choice Point-of-Service Rider An Addendum to Your Evidence of Coverage Effective January 1, 2008 through December 31, 2008 1-800-645-3965 TTY/TDD: 1-888-857-4816 Seven days a week 8 a.m. 8
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For Aetna New York Providers Performing Physical Medicine Services Question Answer General Who is National Imaging Associates,
Small Group Underwriting Guidelines
 F Small Group Underwriting Guidelines (Groups of 2-50 Full-time equivalents) Broker Edition Independence Blue Cross Underwriting Department This document is for informational purposes only and is not intended
F Small Group Underwriting Guidelines (Groups of 2-50 Full-time equivalents) Broker Edition Independence Blue Cross Underwriting Department This document is for informational purposes only and is not intended
This is our plan. My employees want a plan with excellent benefits. I need a plan that is customized for my business. Complete.
 My employees want a plan with excellent benefits. I need a plan that is customized for my business. BUSINESS BLUE COMPLETE This is our plan. Business Blue SM Complete PLAN FEATURES By customizing your
My employees want a plan with excellent benefits. I need a plan that is customized for my business. BUSINESS BLUE COMPLETE This is our plan. Business Blue SM Complete PLAN FEATURES By customizing your
2018 Independence Blue Cross Medicare Group Options
 2018 Independence Blue Cross Medicare Group Options Medical Coverage Keystone 65 Select HMO Value Standard Enhanced CovID H672, 10010705, QN, Y H673, 10010706, QN, Y H675, 10013103, QN, Y Plan premium
2018 Independence Blue Cross Medicare Group Options Medical Coverage Keystone 65 Select HMO Value Standard Enhanced CovID H672, 10010705, QN, Y H673, 10010706, QN, Y H675, 10013103, QN, Y Plan premium
Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.
 Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.* Revised effective Nov. 15, 2016 *Human Affairs International
Magellan Claims Settlement Practices and Dispute Resolution Notice to Providers Contracted with California Subsidiaries of Magellan Health, Inc.* Revised effective Nov. 15, 2016 *Human Affairs International
Using the Availity Web Portal
 Using the Availity Web Portal The Availity multi payer Web Portal presented by Anthem and Availity 2016 Annual Workshop What we will cover Healthy Indiana Plan (HIP) overview POWER Account Visa debit card
Using the Availity Web Portal The Availity multi payer Web Portal presented by Anthem and Availity 2016 Annual Workshop What we will cover Healthy Indiana Plan (HIP) overview POWER Account Visa debit card
P R O V I D E R B U L L E T I N B T J U N E 1,
 P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
All Providers. Provider Network Operations. Date: June 22, 2001
 To: From: All Providers Provider Network Operations Date: June 22, 2001 Please te: This newsletter contains information pertaining to Arkansas Blue Cross Blue Shield, a mutual insurance company, it s wholly
To: From: All Providers Provider Network Operations Date: June 22, 2001 Please te: This newsletter contains information pertaining to Arkansas Blue Cross Blue Shield, a mutual insurance company, it s wholly
Patient Billing and Financial Services
 Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
Patient Billing and Financial Services UNDERSTANDING YOUR OBLIGATIONS BAYHEALTH.ORG We realize this can be a stressful time for you and your family. We particularly understand how frustrating it can be
Training Documentation
 Training Documentation Durable Medical Equipment 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital Advantage
Training Documentation Durable Medical Equipment 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital Advantage
Chapter 4 Health Care Management Unit 2: Introduction to Authorizations
 Chapter 4 Health Care Management Unit 2: Introduction to s In This Unit Topic See Page Unit 2: Introduction To s Introduction To s 2 Remember: Highmark has eliminated referral requirements; however, authorization
Chapter 4 Health Care Management Unit 2: Introduction to s In This Unit Topic See Page Unit 2: Introduction To s Introduction To s 2 Remember: Highmark has eliminated referral requirements; however, authorization
Healthcare Benefits for NJM s Medicare-eligible Retirees, Spouses and Surviving Spouses
 Healthcare Benefits for NJM s Medicare-eligible Retirees, Spouses and Surviving Spouses About this guide This guide explains the steps you must take to ensure that you make sound, timely choices regarding
Healthcare Benefits for NJM s Medicare-eligible Retirees, Spouses and Surviving Spouses About this guide This guide explains the steps you must take to ensure that you make sound, timely choices regarding
Sunflower Health Plan. Regional Provider Workshop
 Sunflower Health Plan Regional Provider Workshop Agenda & Objectives e Third Party Liability (TPL) & Coordination of Benefits (COB) Claims Submission Requirements Overview Sunflower TPL & COB Claims Processing
Sunflower Health Plan Regional Provider Workshop Agenda & Objectives e Third Party Liability (TPL) & Coordination of Benefits (COB) Claims Submission Requirements Overview Sunflower TPL & COB Claims Processing
Prior Authorization/Organization Determination
 Prior Authorization/Organization Determination A Quick Guide on the Importance and Process of Requesting a Prior Authorization/Organization Determination Prior Authorizations Benefits of Using Prior Authorizations
Prior Authorization/Organization Determination A Quick Guide on the Importance and Process of Requesting a Prior Authorization/Organization Determination Prior Authorizations Benefits of Using Prior Authorizations
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Vanderbilt University Medical Center
 BENEFIT PLAN Prepared Exclusively for Vanderbilt University Medical Center What Your Plan Covers and How Benefits are Paid Aetna Choice POS II (Plus) Plan Table of Contents Schedule of Benefits... Issued
BENEFIT PLAN Prepared Exclusively for Vanderbilt University Medical Center What Your Plan Covers and How Benefits are Paid Aetna Choice POS II (Plus) Plan Table of Contents Schedule of Benefits... Issued
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Vanderbilt University. Aetna Choice POS II Health Fund Plan
 BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
Provider Self-Service Requirements
 Provider Self-Service Requirements March 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Self-service requirements Over the last several years, AmeriHealth has instituted a number
Provider Self-Service Requirements March 2017 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Jersey Self-service requirements Over the last several years, AmeriHealth has instituted a number
Radiation Therapy Services Contact AIM for Delivery, Amerigroup for Planning
 Radiation Therapy Services Contact AIM for, Amerigroup for Planning Prior authorization of outpatient radiation therapy services for Amerigroup* Community Care Medicare Advantage and Medicare Medicaid
Radiation Therapy Services Contact AIM for, Amerigroup for Planning Prior authorization of outpatient radiation therapy services for Amerigroup* Community Care Medicare Advantage and Medicare Medicaid
School Accident Program Parent/Guardian Guide Program 3
 School Accident Program Parent/Guardian Guide Program 3 A nonprofit independent licensee of the BlueCross BlueShield Association Dear Parent or Guardian: This packet contains important documents regarding
School Accident Program Parent/Guardian Guide Program 3 A nonprofit independent licensee of the BlueCross BlueShield Association Dear Parent or Guardian: This packet contains important documents regarding
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. NV Silver PPO /50. Aetna Life Insurance Company Certificate
 BENEFIT PLAN Silver PPO 2000 75/50 What Your Plan Covers and How Benefits are Paid Aetna Life Insurance Company Certificate This Certificate is part of the Group Insurance Policy between Aetna Life Insurance
BENEFIT PLAN Silver PPO 2000 75/50 What Your Plan Covers and How Benefits are Paid Aetna Life Insurance Company Certificate This Certificate is part of the Group Insurance Policy between Aetna Life Insurance
Oregon Portability Plans
 Oregon Portability Plans Effective May 1, 2013 Regence BlueCross BlueShield of Oregon is an Independent Licensee of the Blue Cross and Blue Shield Association 06556rep05211-or/05-13 Read the contract carefully
Oregon Portability Plans Effective May 1, 2013 Regence BlueCross BlueShield of Oregon is an Independent Licensee of the Blue Cross and Blue Shield Association 06556rep05211-or/05-13 Read the contract carefully
3. The Health Plan accepts the standard current billing forms: the CMS 1500 (02/12) form and the UB- 04 hospital billing forms.
 BILLING PROCEDURES SECTION 11 Billing Procedures 1. All claims should be submitted to: The Health Plan 1110 Main St Wheeling WV 26003 Claim forms must be completed in their entirety. The efficiency with
BILLING PROCEDURES SECTION 11 Billing Procedures 1. All claims should be submitted to: The Health Plan 1110 Main St Wheeling WV 26003 Claim forms must be completed in their entirety. The efficiency with
HIPAA 5010 Webinar Questions and Answer Session
 HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Lee County Board of County Commissioners. Aetna Choice POS II
 BENEFIT PLAN Prepared Exclusively for Lee County Board of County Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Table of Contents Schedule of Benefits... Issued with
BENEFIT PLAN Prepared Exclusively for Lee County Board of County Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Table of Contents Schedule of Benefits... Issued with
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers
 NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
