HEALTH POLICY AND PLANNING; 13(4): 371^383 ß Oxford University Press 1998
|
|
|
- Robyn Willis
- 5 years ago
- Views:
Transcription
1 HEALTH POLICY AND PLANNING; 13(4): 371^383 ß Oxford University Press 1998 Household health expenditures in Nepal: implications for health care financing reform DAVID R HOTCHKISS, 1 JEFFREY J ROUS, 2 KESHAV KARMACHARYA 3 AND PREM SANGRAULA 3 1 School of Public Health and Tropical Medicine, Tulane University, New Orleans, USA, 2 Dept of Economics, University of North Texas, USA, and 3 Central Bureau of Statistics, His Majesty's Government of Nepal His Majesty's Government of Nepal has embarked on an ambitious social welfare programme of increasing the accessibility of primary education and health care services in rural communities. The implications on the financing of health care services are substantial, as the number of health posts has increased twelve-fold from 1992 to 1996, from 200 to To strengthen health care financing, government policy-makers are considering a number of financing strategies that are likely to have a substantial impact on household health care expenditures. However, more needs to be known about the role of households in the current structure of the health economy before the government designs and implements policies that affect household welfare. This paper uses the Nepal Living Standards Survey, a rich, nationally-representative sample of households from 1996, to investigate the level and distribution of household out-of-pocket health expenditures. Utilization and expenditures for different types of providers are presented by urban/rural status and by socioeconomic status. In addition, the sources of health sector funds are analyzed by contrasting household out-of-pocket expenditures with expenditures by the government and donors. The results indicate that households spend about 5.5 % of total household expenditures on health care and that households account for 74 % of the total level of funds used to finance the health economy. In addition, rural households are found to spend more on health care than urban households, after controlling for income status. Distributing health care expenditures by type of care utilized indicates that the wealthy, as well as the poor, rely heavily on services provided by the public sector. The results of this analysis are used to discuss the feasibility of implementing alternative health care financing policies. Introduction In many developing countries, governments are facing increasing pressure to improve the efficiency and financial viability of health service delivery systems, particularly in light of renewed commitments to improve living conditions for the poor (World Bank 1993). The case of Nepal provides an excellent example. Nepal is one of the poorest countries in the world, with a per capita GDP of US$200 and a life expectancy at birth of 54 years in 1994 (World Bank 1996). With the passage of the Eighth Economic Plan, the policy of His Majesty's Government (HMG/Nepal) has been to invest resources derived from tax revenues and donor assistance to increase the availability of primary education and health care in rural communities. The implications on the financing of health care delivery are substantial, as the government has begun to ensure that residents of each rural community have access to health care services from a health post. This has translated into a period of extensive construction of health care facilities in Nepal. Between 1992 and 1996, the number of subhealth posts increased twelve-fold, from 200 to 2597 (HMG/Nepal 1996). These commitments to improve health outcomes among the rural poor come at a time in which improved yet unstable economic performance and
2 372 David R Hotchkiss et al. high rates of population growth threaten the government's ability to finance and further expand the delivery of health services. Among the macroeconomic factors that are cause for concern are a relatively low tax base, substantial budget deficits, a foreign exchange rate that has depreciated in recent years, and a lower level of grant assistance from international donors, which has become an increasingly unpredictable source of funds (HMG/Nepal 1996). With the assistance of international donors, government officials are considering a number of reforms that are intended to increase the financial viability and efficiency of the public health care system. The strategies include an increased role of user fees, community health insurance programmes, and incentives to increase the role of the private sector. However, before the government of Nepal designs and implements policies that affect the cost of health care for private households, more needs to be known about the current structure and financing of the health economy. How much are households currently spending on health care? What types of services are being utilized? Do the health care utilization and expenditure patterns of poor households differ from those of better-off households? What percentage of household out-of-pocket funds are spent on private providers, either traditional or modern? Knowing the answers to these questions is critical for policymakers who design social welfare policies. If, for example, households lack the ability and the willingness to spend more on health care, the government will probably need to provide only very basic health care at an extremely low price. However, if individuals are found to have the ability and willingness to pay for good quality health care, then the government's options are expanded. They can offer a wider variety of health services and still recover a substantial portion of the costs. Unfortunately, only a few studies have investigated the level and distribution of household health expenditures in developing countries. Most household-level studies of illness-related out-of-pocket expenditures are based on responses from rural areas (Parker 1986; Berman et al. 1987; Sauerborn et al. 1995; Sauerborn et al. 1996). However, the spending patterns of rural areas are likely to be quite different to those found in urban areas. In addition, most nationally-representative financial studies of health care expenditures focus only on the public sector, despite the fact that policy decisions based only on public expenditure data can have severe long-term consequences. Because as much as 40^80 % of total health expenditures may be excluded from such an analysis in many developing countries, the government's ability to affect health practices and expenditure patterns will be severely hampered if it makes policy decisions on this basis (Newbrander et al. 1994). In recent years, an increasing number of studies have applied national health accounts (NHA) analysis, which estimates the sources and uses of funds in the health sector (see Berman 1997 for a review of NHA studies). The few studies that have conducted this more complete assessment of health care expenditures suggest that, even in countries where health care services are either free or nominally priced, the role of households is far larger than previously thought (Berman 1997). For example, the percentage of total health funds that come from households is 74 % in Burkina Faso (Sauerborn et al. 1995) and 55 % in Egypt (Berman 1997). The purpose of this paper is to investigate the role of households in Nepal's health economy. In the first section, we discuss the data we have available to analyze household health care expenditures. Second, we evaluate the role households play in Nepal's health economy by comparing expenditures from all sources of funding: households, the government, donors, and private companies. Third, we investigate the level and distribution of household health care expenditure by geography, income status, and source of care. In addition, we investigate the prevalence and severity of illness and the type of practitioner as determinants of health care usage. We conclude the paper with a discussion of the implications of our results on future efforts to design and implement health care reform in Nepal. Data and methodology The data used in this analysis come from the Nepal Living Standards Survey (NLSS), which was administered by Nepal's Central Bureau of Statistics (CBS) with assistance from the World Bank. This nationally-representative survey collected information from 3338 households ( individuals) in 275 communities from June 1995 to May The sample was divided into four strata based on the geographic and ecological regions of the country: (i) the mountains, (ii) the urban hills, (iii) the rural hills, and (iv) the Terai. 1 A two-stage stratified sampling procedure was used to select the sample. In the first stage, communities were randomly selected with
3 a probability of being included directly proportional to their population. In the second stage, a fixed number of households was randomly selected from each chosen community. Household health expenditures in Nepal 373 The household survey included questions pertaining to a wide array of economic, demographic, and health-related behaviours of each member of the household, not just the head of the household. The topics covered by the NLSS include demographic characteristics, access to facilities, housing, migration, food expenses and agricultural production, nonfood expenditures, education, health, anthropometry, marriage and maternal history, wage employment, income, and nutrition. The health section of the survey included questions on whether each household member was perceived to have suffered from a chronic disease or from an illness or injury in the past month, whether the individuals used health care services, the type of place and practitioner consulted, and the consultation and travel costs for the last two consultations. Information was also collected on immunizations and child births. These data come from the most comprehensive and complete household-level survey ever administered in Nepal. The health component of the survey captures information on the wide range of health care choices available in Nepal, from traditional healers in the mountain areas to modern hospitals in the capital city, Kathmandu. Role of households in health care financing As a first step in our evaluation of the role of households in the financing of health care services in Nepal, we carried out a careful accounting of expenditures incurred by households, the government, donors, and private companies. This analysis is described in Hotchkiss et al. (1997). 2 Figure 1 provides the absolute level of health care funds and a percentage distribution by the sources of funds for Fiscal Year 1994/95. The total expenditure of Rs billion spent on health care was equivalent to 5.45 % of GDP or Rs per capita (US$11.45 per capita). This estimate of the proportion of GDP devoted to the health sector is substantially higher than estimates from previous studies. For example, Shrestha and Shrestha (1995) estimate that in FY 1993/94, 4.5 % of GDP was devoted to health expenditures. Figure 1. The role of households in Nepal's health economy (total = Rs billion) Source: 1996 Nepal Living Standards Survey; 1994 and 1995 United Nations Development Project Survey of External Assistance; 1996 HMG/Nepal Ministry of Finance, Department of Health Services; 1996 Asian Development Bank Survey of Private Companies. Moreover, our estimate of the proportion of GDP devoted to the health sector is substantially higher than estimates from other countries in the South Asian region, such as Bangladesh or Pakistan. Only India, at 6 % of GDP, spends relatively more than Nepal (World Bank 1993). However, it should be pointed out that we have not assessed the reliability of the estimates of expenditures in Bangladesh, India, and Pakistan. Previous studies tended to underestimate national health care expenditure because they lacked information on private health expenditure. Our estimate is not only based on information coming from the government and donors, but also from a survey of private companies and the NLSS. As a result, we estimate that private expenditures on health account for 3.9 % of GDP, while the World Bank, for example, provides an estimate of 2.3 %. Of the Rs billion that we estimate is spent on health care, the overwhelming majority was provided by private households, while donors, the government, and private companies accounted for much smaller levels. Household out-of-pocket payments are the
4 374 David R Hotchkiss et al. source for over 75 % of all health sector funds. International donors, the government, and private companies made up 13.1, 10.1, and 1.5 %, respectively. That a country as poor as Nepal is heavily reliant on households for financing health care is consistent with previous research findings. For example, Schieber and Maeda (1997) report national-level findings which indicate that the income elasticity for the public and private components of health care expenditures is 1.21 and 1.02, respectively. This suggests that public health spending is more responsive to income differences than private health spending and is consistent with the fact that low income countries have a larger private share of total health expenditures (Schieber and Maeda 1997). The importance of households in the funding of health care not only suggests that households are willing to expend considerable resources on health care, but also underscores the importance of understanding the determinants of household health care expenditure. Health as a share of the household budget Despite Nepal's status as one of the poorest countries in the world, households at all income levels spend a significant amount on health care. On average, Nepalese spend Rs. 505 per year on health-related goods and services. This translates to over 5 % of total per-capita household expenditures. Table 1 presents total per capita out-of-pocket health expenditures by urban/rural status and by income status. The measure of health expenditure used in this table includes the travel and consultation costs of non-chronic illnesses and injuries, chronic illnesses, and birth deliveries. 3 Excluded are the costs of immunizations and family planning services, which were not measured in the NLSS instrument. The percentage of total household expenditures used for health care services increases with the level of household income. 4 For example, the percentage of expenditures used for health is 3.2 % for the poorest quartile, 4.6 % for the second quartile, 6.7 % for the third quartile, and 7.8 % for the wealthiest quartile. As expected, urban households spend more on health care than rural households. Urban households spend Rs per capita on health care, which is 120 % higher than the rural average of Rs However, Table 1 also shows that, unexpectedly, rural households spend more than urban households if income per capita is introduced as a control variable. For example, for each quartile group except for the second group, rural households spend more than urban households, both as a percentage of total expenditures and as absolute levels. The difference is particularly large among households in the poorest quartile, where rural per capita spending is Rs. 106, three times higher than the per capita average of urban households, Rs. 35. In addition, for all four income groups, the share of household expenditures devoted to health care is higher for rural households than for urban households. In the next section, we will explain some of this variation. Overall, we find that prevalence and severity of illness, age, income, and provider choice account for much of the noted health expenditure variation between urban and rural households.
5 Household health expenditures in Nepal 375 Determinants of health expenditure Frequency of illness That rural households spend more on health care than urban households (controlling for income per capita) can largely be explained by investigating the incidence of illness in rural and urban areas. Overall, 9.4 % of the individuals surveyed report suffering from a non-chronic illness or injury in the month prior to the survey. Table 2 presents the percentage of persons who report to be ill or injured by income per capita group and by urban/rural area. Individuals living in rural households report themselves to be sicker, on average, than individuals in urban households (9.5 % vs 7.9 %). 5 The most frequent symptoms reported in both rural and urban areas are diarrhoea and fever. 6 In addition, the severity of illness among rural individuals who reported an illness in the past month is substantially greater than among comparable urban individuals. Specifically, the average number of activity days missed due to illness in the previous month is 4.38 for rural individuals, compared to 3.88 for urban individuals (Table 3). The magnitude of this urban/rural differential is most dramatic among the first three income quartiles. For example, the number of days missed among sick individuals in the second income quartile is 5.38 in rural areas, which is significantly higher than the 0.86 average number of days missed among comparable individuals in urban areas. This may indicate one of several urban/rural differences. For example, rural households may be less likely to report an illness if it is not severe. Alternatively, diseases causing illness in rural areas may be more disabling. Another related explanation is that rural individuals, once sick, may delay the utilization of treatment from modern practitioners, perhaps because traditional practitioners are their preferred choice. If traditional treatment does not cure an individual of an illness, then treatment from modern practitioners may be sought, by which time the severity of the illness might be greater and treatment costs higher. Sorting out this difference is not possible with the NLSS. Age is generally considered to be an important determinant of illness. As expected, the relationship between age and reported illnesses and injuries is U-shaped. Children. under five years of age and adults 45 years of age and older have higher prevalence rates
6 376 David R Hotchkiss et al. than other individuals. The U-shape of the relationship is particularly pronounced in urban areas, as the prevalence rate for young children is higher and the prevalence rate for individuals 5 to 29 years of age is lower than the rates of comparable individuals in rural areas. Although it might be expected that households with higher incomes would suffer lower rates of illness, this is not usually found to be the case. Table 2 indicates a positive correlation between reported illnesses and income per capita. This positive relationship is a result of both an older age structure and a higher prevalence of reported illness among wealthier households. The older age distribution is reflected in the fact that the mean age of individuals living in wealthy households is 26.6 years of age, compared to 21.1 years of individuals living in the poorest quartile of households. The higher prevalence of illnesses is evidenced by the higher proportion of wealthy children under five years of age who are reported to be ill. For example, 21.6 % of children in the top income quartile are reported to be ill compared to 8 % of children in the lowest expenditure quartile. This high prevalence rate among children of wealthy households is largely attributable to a higher frequency of diarrhoea and fever cases. A possible explanation of this negative relationship between income class and prevalence of illness, which seems counterintuitive, may be associated with how individuals from different social classes perceive the symptoms of illness. According to Table 2, 5.5 % of the sample report suffering from a chronic illness. The rate is higher among rural individuals than among urban individuals (5.6 % vs. 4.7 %), which is surprising given that the rural population is substantially younger. However, age-specific rates of chronic illness are generally higher for each age group in rural areas except for children under five years of age. Not reported in Table 2 is the finding that individuals in the mountain areas more frequently report chronic illnesses than individuals in the hill or Terai regions. The percentage of persons who report suffering from chronic problems is 7.8 % among mountain individuals, compared to 8.8 % for hill and 4.3 % for Terai individuals. This relationship also holds when age is introduced as a control variable. Health care utilization The supply environment Persons in need of health care in Nepal have the choice of using either modern or traditional health care providers. The modern sector consists of government services, private services, and services provided by quasi-public agencies such as nongovernmental organizations (NGOs), while the traditional sector consists of government and private providers. The bulk of public modern services are provided by facilities administered by the Ministry of Health (MOH), which constitutes over 90 % of public health expenditures. However, public health care is also offered in hospitals administered by the Ministry of Defense, the Ministry of Home, and the Ministry of Education and Culture. While all urban communities have access to services from a public health care clinic, only about twothirds of rural communities (65.4 %) are within 60 minutes travel time of a public clinic, despite the fact that HMG/Nepal has made substantial progress in improving access to health care in the past five years. Moreover, only 10.2 % of rural communities are within one hour of a public hospital. The private health care sector consists of pharmacies that offer health care services and prescribe and sell drugs, private hospitals (referred to as nursing homes in Nepal), private clinics, x-ray laboratories, and services offered by private factories as a benefit to their employees. In the past decade, the government has encouraged the private sector to play a greater role in health care delivery by providing a more tolerant regulatory environment and by granting import duty waivers for the purchase of equipment and drugs necessary for health care provision. The effect of these policies appears to be substantial. For example, in the past 12 years, the number of private hospitals located in urban areas has mushroomed from one facility offering ten beds in 1984 to 61 facilities offering 1126 beds in In rural areas, there is a limited availability of private practitioners who provide modern health care. In fact, only 17.6 % of rural communities were reported to be less than one hour from a private nurse or doctor. Pharmacies are considerably more prevalent: 38.0 % of communities were reported to be within one hour of a pharmacy. A number of public providers other than the government also provide health care services in Nepal.
7 Household health expenditures in Nepal 377 These providers include multilateral organizations such as the World Health Organization, bilateral organizations such as the German Agency for Technical Cooperation, international NGOs such as Save the Children, domestic non-governmental organizations, and missions such as United Mission to Nepal. Choice of practitioner At the most basic level, total health expenditure is made up of two components, the quantity of health services consumed and the price of those services. The quantity of services that members of a household consume is determined by their likelihood of visiting a practitioner when they get sick. Table 2 presents the percentage of persons who reported an illness or injury in the past month by whether they sought treatment from a medical practitioner, either modern or traditional. As expected, urban individuals are more likely to seek health care treatment than rural individuals. On average, 77.4 % of urban individuals and 66 % of rural individuals receive treatment from a health care practitioner when they get sick. Individuals from wealthier households are considerably more likely to utilize health care services than individuals from poorer households. As Table 2 indicates, 75 % of sick individuals in the richest quartile of households use health care services, compared with 53 % of individuals living in the poorest quartile. Given that public facilities charge only nominal fees for their services whereas private facilities rely on user fees to cover most of their costs, choice of practitioner would be expected to have a large impact on household health expenditure. In addition, we expected that, as in many developing countries, wealthier households would choose private practitioners and poorer households would choose public practitioners. We found that most households rely heavily on services provided by the public sector for the treatment of illnesses and injuries. Table 4 presents a percentage distribution of persons seeking treatment for illness in the past month by the type of health care setting that is first utilized. The results indicate that, of those seeking an initial consultation, 55 % rely on government hospitals and clinics, 37 % rely on private facilities, and 7 % use a traditional healer. 7 As one would expect, most poor individuals who utilize health care services relied on public care. A somewhat surprising finding, however, is the degree to which better-off households rely on public health care services. As Table 4 indicates, 49 % of individuals in the wealthiest income quartile and 58 % of individuals in the next-to-wealthiest quartile who seek treatment choose a public clinic or hospital for their first consultation, compared to 56 % of individuals living in the poorest quartile. Public providers are an important source of health care in both urban and rural areas. Table 4 indicates
8 378 David R Hotchkiss et al. that 56 % of individuals using health care in rural areas utilize public services, compared to 41 % in urban areas. The type of public facility most frequently used by rural individuals is the health post, while the hospital is the government facility of choice for urban individuals, which is most likely due to the fact that hospitals are considerably more accessible in urban areas such as Kathmandu. Regarding the use of private services, urban individuals are considerably more likely to utilize private hospitals and other types of private care than their rural counterparts (56 % for urban individuals vs. 35 % for rural individuals). In addition, rural individuals are four times as likely to utilize a traditional healer as their first choice (7.4 % for rural individuals and 1.8 % for urban individuals). Traditional health care is found to be a more important source of care for individuals in the mountain areas (25 %) than for individuals in the hill and Terai areas (9.7 % and 3.8 %, respectively). Cost of health care Even though user fees are almost non-existent at public facilities in Nepal, individuals who seek health care from public providers incur substantial monetary costs. Table 5, which presents average outof-pocket consultation and travel expenditures for each type of health care setting, shows that the average cost of a public consultation is comparable to, if not higher than, a private consultation. For example, the average cost of a consultation at a health post or clinic is Rs. 272, which is 25 % higher than the average household cost of a consultation at a pharmacy, which is usually provided by a health care practitioner. Moreover, the average cost of a public hospital consultation is Rs. 544, considerably higher than the average cost of Rs. 437 incurred at private hospitals or other private settings. As Table 5 indicates, the finding that the costs of public and private care are comparable holds after controlling for severity of illness. For example, if only ill or injured individuals who report not missing any days from their normal activities are included in the analysis, the average cost of a consultation in a public health post is Rs. 201, which is slightly cheaper than the average cost of a consultation at a private pharmacy, Rs That public care is associated with substantial out-of-pocket costs suggests that many public
9 Household health expenditures in Nepal 379 consultations involve purchasing drugs and services in the private market. For example, a doctor may initially treat an individual in a government clinic but then continue the treatment episode in his private chambers, or an individual may consult a practitioner in a public clinic but purchase medicines from a private pharmacy, perhaps as a response to drug stock-outs. The structure of the NLSS precludes distinguishing the extent of these two possibilities for individuals whose sole treatment consists of one visit to a doctor in a public clinic. Unfortunately, we do not have the ability to determine the percentage of expenditures that flows to private providers for drugs and services because the survey did not include specific questions that itemized consultation costs. Each individual reported only where the first and second consultation took place and how much was spent. Because of these limitations in the survey instrument, the average costs reported in Table 5 should be interpreted as out-of-pocket costs ``associated'' with utilizing the specific types of providers for an initial consultation rather than as the cost of the initial visittothatprovider. 8 We also investigated whether consultation costs of public and private providers varied by urban/rural area and by income group. As expected, average expenditures per visit to a health clinic are 51 % higher among urban individuals than among rural individuals. Urban individuals also spend more on both public and private hospital consultations than rural individuals (23 % and 13 %, respectively).when visiting a health post or clinic, wealthier individuals spend more on consultation costs than poorer individuals. For example, the costs of a government consultation at a health post is Rs. 798 for individuals in the wealthiest quartile and Rs. 138 for individuals in the poorest quartile. As Parker (1986) suggests, this finding may reflect the practice in government facilities of prescribing more expensive medicines for the wealthy patient to purchase in the market. Poorer patients, on the other hand, may be given free government drugs or may not purchase medicines if given a prescription. Distribution of illness-related expenditures by type of practitioner Combining the previous sections on the choice to obtain medical care and the cost of visiting alternative practitioners, we can now examine how much households spend on public and private health care alternatives. Table 6 provides estimates of annual per capita out-of-pocket expenditures on the treatment of non-chronic illnesses and injuries. On average, households spend Rs. 361 per capita on health care. Over 61 % of expenditures is associated with care provided in public facilities, while 34 % is associated with private care offered in clinics, hospitals, or pharmacies, or through practitioners who make house visits. In the previous section, we discussed that we are unable to separate out-of-pocket pharmaceutical costs from the overall expenditure on health care because
10 380 David R Hotchkiss et al. of limits in the NLSS instrument. However, a household-level survey carried out in 1993 (Center for Economic and Technical Studies, 1993) indicates that 77 % of household expenditures on modern health care is used to purchase medicines. In addition, the percentage of health care expenditures that is spent on pharmaceuticals is substantially higher in urban areas than in rural areas. In urban areas, 86 % of modern treatment expenditures is spent on medicines, compared to 74 % in rural areas. In view of these results, it is likely that the vast maority of household out-of-pocket expenditures are used for drug purchases in the private market. As expected, urban households spend more on health care than rural households. Urban households spend an average of Rs. 595 per capita on the treatment of illnesses and injuries, which is 74 % higher than the rural average of Rs The percentage of per capita expenditures used for public care is almost identical in urban and rural areas (60 % vs. 61 %, respectively). However, urban households spend relatively more on privatelyprovided health care than rural households (39 % vs. 33 %, respectively). Much of the expenditure for private care in urban areas is used for care offered in hospitals. Care provided by NGOs and Missions account for 2 % of household illness-related expenditures. Urban individuals reportedly spend relatively less on traditional health care than rural individuals (1 % vs. 5 %, respectively). As is the case when total health care expenditures are considered, average per capita health expenditures are found to be higher for rural households than for urban households if income per capita is introduced as a control. As Table 6 indicates, rural households spend more per capita than urban households for three of the four quartiles considered (the second quartile is the exception). For example rural households in the wealthiest expenditure quartile spend Rs per capita for health care, compared to the Rs. 838 per capita that is spent by urban households. Table 6 also shows that for each income quartile, the percentage of illness-related expenditures spent on care associated with public providers is substantial. In fact, wealthy households rely more extensively on public facilities than poor households. In urban areas, for example, 59 % of illness-related expenditures of wealthy individuals is associated with government care, compared to 54 % for the poor. In rural areas,64% of expenditures spent by wealthy individuals is associated with government care, compared to 44 % for the poor. Conclusions Using a rich, nationally-representative household survey, this paper presents a descriptive analysis of health care utilization and expenditure behaviour in Nepal. The results of our analysis indicate a diverse use of modern and traditional health care. More than half of rural individuals who are ill choose public facilities which may offer either traditional or modern treatments, while private care is the preferred choice in urban areas. Surprisingly, wealthy households are no less reliant on publicly-provided services than poor households. On average, health care accounts for about 5.5 % of total household expenditure. The share of total expenditure devoted to health care increases with the level of household income. In terms of the role of households in the total health economy, out-ofpocket contributions account for almost three-quarters of the total funds used to finance Nepal's health care sector. This finding that households are the largest source of health sector funds is consistent with findings from other developing countries (Berman 1997; Schieber and Maeda 1997). The analysis of the distribution of household expenditures on health care yields a number of surprising findings. First, despite the lower availability of health care services, rural households spend relatively and absolutely more on illness-related expenditures than urban households, after controlling for income per capita. The heavier economic burden of illnesses on rural households is found to be exacerbated during the rainy months of the year. The reasons for this urban/rural differential are complex. It is possible that the quality of publicly provided health care that is available in rural areas is low, resulting in a higher reliance of households on the private sector, both traditional and modern. Although rural households are less likely to seek care when they become ill, the prevalence of illness is higher and the severity of illness is greater in rural areas than in urban areas. The severity of illness may be greater because illnesses suffered in rural areas may be more disabling or perhaps because rural households delay the use of modern practitioners. One explanation for delaying modern treatment is that health care services are not readily accessible in rural areas.
11 Household health expenditures in Nepal 381 A second unexpected finding is that households spend substantial amounts on health care when their initial consultation is with a public practitioner, despite the fact that public care is free or nominally priced. More than 60 % of out-of-pocket expenditures for the treatment of illness is incurred by households that choose public treatment. This finding provides an indication that individuals use private services as a complement to the initial public consultation. For example, patients who visit a public facility may continue to see the doctor privately or purchase pharmaceuticals in the private sector because of stock-outs in public facilities. How can the government use the results of this analysis to formulate policies that will potentially improve health outcomes among the population? A country's health care reform options largely depend on the ability of government health ministries to recover their costs. If households are able and willing to pay more for health care services in the form of user fees and/or insurance premiums, alternative financing strategies such as community health funds accompanied by user fees and quality improvements may be potentially successful in improving the degree of cost recovery and service quality and efficiency. Moreover, financing reform may be an effective tool to reduce the urban/rural differential in health care need and expenditures if the moneys collected by charging higher fees and premiums to individuals can be used to improve the financing of preventative health care programmes in rural areas. The effect of user fees on health care utilization and health outcomes has been a subject of considerable debate in the past decade. Much of this debate has centred on the ability and willingness of households to pay larger out-of-pocket payments for health care. On one hand, the results of numerous studies in developing countries indicate that health care utilization rates among both poor and non-poor individuals would not be greatly affected by small increases in user fees (Akin et al. 1995; Shaw and Griffin 1995). Moreover, many studies also suggest that health care utilization would actually increase if increased user fees are accompanied by improvements in the quality of services (see Alderman and Lavy 1996 for an excellent review of the literature on this topic). On the other hand, other researchers have found that the price elasticity among the poor is substantial, which suggests that user fee schemes would have a regressive distributional impact (Gertler and van der Gaag 1990). Would cost recovery strategies based on user fees and health insurance be successful in Nepal? Our findings clearly show that the financial resources available for funding the health sector are greater than previous estimates indicate. Despite the fact that Nepal is a very poor country, households are already spending considerable amounts on health care. We have shown above that households of all income groups frequent both public and private providers despite the fact that private providers charge user fees that recover a substantial portion of their costs and that there are substantial costs to households associated with visiting a ``free'' public provider. That better-off households are heavy users of the public system indicates that carefully designed financing strategies may be effective in achieving a higher level of cost recovery. In fact, a number of health financing reform experiments previously carried out in Nepal by United Mission to Nepal, The Britain Nepal Medical Trust, the World Health Organization, et al. and HMG/Nepal have demonstrated that households are willing to pay for higher quality care (Cross et al. 1996). While these findings are encouraging, more research is clearly needed on how households in the South Asian context will respond to health care reform initiatives. Important policy relevant questions include: how will user fees in the public sector affect modern health care utilization and health outcomes, particularly among the poor?; how much are healthy individuals willing to pay for insurance premiums?; and, does the institutional and managerial capacity necessary to administer procedures such as collection and billing exist in Nepal? Because the consensus for health sector reform based on user fees and community health insurance probably does not exist in Nepal, reform strategies should be attempted first through pilot studies to determine whether they result in their intended effects. If these pilot projects are successful, they would hopefully result in a consensus among the government, international donors, health care providers, and the public-at-large to begin to implement an appropriate reform programme on a larger scale. End notes 1 The Terai refers to the flat river plain of the Ganges in the southern region of Nepal. 2 This analysis of the sources of health spending is based on the NLSS, government statistics from the HMG/Nepal's Ministry of Finance and the Ministry of Health, the United Nations Survey of
12 382 David R Hotchkiss et al. External Assistance, and recent surveys of private factories and companies funded by the Asian Development Bank. The estimate of household out-of-pocket expenditures accounts was deflated to FY 1994/95. 3 To estimate expenditures on birth deliveries, we administered a survey of the normal costs of deliveries away from home in both private and public facilities, as well as the normal fees charged by traditional birth attendants in rural areas. This inforination, along with the survey response data on whether the woman delivered away from home or at home; and whether the practitioner was modern or traditional, was used to estimate expenditures for birth deliveries. 4 Throughout this study, we use total household expenditure per capita as a proxy for household income per capita. This is a reasonable assumption given that household expenditure may more closely approximate household permanent income than an income measure. In addition, total expenditure is generally measured more accurately than income in developing countries. To create total income quartiles, we ranked all households by their level of total per capita household expenditure and then divided the households into four groups. 5 The prevalence rates of illnesses and injuries are not significantly different between individuals living in the mountain, hill or Terai ecological zones. 6 Not reported in Table 2 are our findings on the association between seasonality and the prevalence of illness. As expected, individuals report illness more frequently during the rainy season (12.0 %) than in the dry season (7.3 %). At the same time, utilization rates do not change substantially, resulting in significantly higher health care expenditures in the rainy season. These findings of higher reported prevalence of illnesses and increased health care expenditures during the rainy season conflicts with previous research in Africa on this topic. For example, Sauerborn et al. (1996) found that perceptions of illness and health care use were actually lower in Burkina Faso during the rainy season, despite the fact that health needs are higher. 7 Ayurvedic health care services in Nepal are provided by government facilities as well as by private practitioners. In the NLSS, consultations provided by ayurvedic practitioners were not coded as traditional health care. Because the survey did not distinguish ayurvedic and modern practitioners, we had no alternative but to include ayurvedic treatments as modern care. 8 The survey did not include questions on whether individuals are covered by health insurance policies. While health insurance is certainly not commonplace in Nepal, there are an increasing number of companies in Kathmandu that supply health insurance policies. References Akin JS, Guilkey DK and Denton EH Quality of services and demand for health care in Nigeria: a multinomial probit estimation. Social Science and Medicine 40: 1527^37. Alderman H and Lavy V Household responses to public health services: cost and quality tradeoffs. World Bank Research Observer 11: 3^22. Berman P Treatment use and expenditure on curative care in rural Indonesia. Health Policy and Planning 2(4): 289^300. Berman P National health accounts in developing countries: appropriate methods and recent applications. Health Economics 6(1): 11^30. Barnum H and Kutzin J Public Hospitals in Developing Countries: Resource Use, Cost Financing. Baltimore: The Johns Hopkins Press. Center for Education and Technical Studies Private Sector Health Expenditures in Nepal. Kathmandu: Center for Education and Technical Studies. Cross PN, Dias V and Bates J Rational Pharmaceutical Management Project: Nepal Cost Sharing in Pharmaceutical Distribution. Boston: Management Sciences for Health. Gertler P and van der Gaag J The willingness to pay for medical care: evidence from two developing countries. Baltimore: The Johns Hopkins Press. Griffin CC Health Care in Asia: A Comparative Study of Cost and Financing. Washington DC: The World Bank. His Majesty's Government of Nepal; Ministry of Finance Economic Survey: Fiscal Year 1995^1996. Kathmandu, Nepal. Hotchkiss D, Shrestha S, Shrestha BR and Lohani SR National Accounts Analysis and Social Sector Reform in Nepal. Manila: Asian Development Bank. Huber PJ The behavior of maximum likelihood estimates under non-standard conditions. In: Proceedings of the Fifth Berkeley Symposium in Mathematical Statistics and Probability. Berkeley, CA: University of California Press; 1, 221^33. Mathema P Review of Current Health Expenditure Resource Allocation and Trends. Proceedings of The First Workshop on Long Term Health Plan Development. Kathmandu: HMG/Nepal National Planning Commission. Newbrander W, Carrin G and Le Touze D Developing countries' health expenditure information: what exists and what is needed? Health Policy and Planning 9(4): 396^408. Parker RL Health care expenditures in a rural Indian community. Social Science and Medicine 22(1): 23^27. Ramsey JB Tests for specification errors in classical linear least squares regression analysis. Journal of the Royal Statistical Society, Series B 31: 350^71. Rannan-Eliya R and Berman P National Health Accounts of Developing Countries: Improving the Foundations. Data for Decision Making, Harvard School of Public Health; Publication No. 2. Sauerborn R, Ibrango I, Nougtara A et al The economic costs of illness for rural households in rural Burkina Faso. Tropical Medicine Parasitology 46: 54^60. Sauerborn R, Nougtara A, Hien M and Diesfeld HJ Seasonal variations of household cost of illness in Burkina Faso. Social Science and Medicine 43(3): 281^90. Schieber GJ and Maeda A A curmudgeon's to financing health care in developing countries. In: Schieber GJ (ed). Innovations in Health Care Financing: Proceedings of a World Bank Conference, March 10^11, Washington DC: The World Bank. Shaw P and Griffin CC Financing Health Care in Sub- Saharan Africa through User Fees and Insurance. Washington DC: The World Bank. Shrestha S and Shrestha BR Analysis of Health Economics in Nepal. Kathmandu: HMG/Nepal Ministry of Health, Policy, Planning, Foreign Aid and Monitoring Division. World Bank World Development Report 1993: Investing in Health. New York: Oxford University Press. World Bank World Development Report 1996: From Plan to Market. New York: Oxford University Press. Acknowledgments This project was supported by the Asian Development Bank (ADB). The views presented are those of the authors and should not be construed as reflecting those who funded this work. We
13 Household health expenditures in Nepal 383 would like to thank Anthony Drexler, Vincent D'Witt and Giovanna Prennushi for comments on earlier drafts of this paper. Biographies Dr David R Hotchkiss is Assistant Professor of Health Economics at Tulane University's School of Public Health and Tropical Medicine. He received his PhD in Economics from the University of North Carolina in Prior to joining the faculty at Tulane, he was Research Associate at the International Food Policy Research Institute and Pre-Doctorate Trainee at the University of North Carolina's Carolina Population Center. Dr Jeffrey J Rous is Assistant Professor of Economics at the University of North Texas. He received his PhD in Economics from the University of North Carolina in He has carried out research on health care financing and health care utilization issues in the Philippines and Morocco. Mr Keshav Karmacharya is the Central Bureau of Statistics' (CBS) Project Co-ordinator for the Nepal Living Standards Survey, which was jointly administered by CBS and the World Bank. Mr Prem Sangraula is the Central Bureau of Statistics' (CBS) Data Manager for the Nepal Living Standards Survey. He is currently a student of Economic Management at Columbia University. Correspondence: Dr David Hotchkiss, Tulane University, School of Public Health and Tropical Medicine, Department of International Health and Development, 1440 Canal Street, Suite 2200, New Orleans, Louisiana 70012, USA.
Household Health Expenditures in Morocco: Implications for Health Care Reform
 Household Health Expenditures in Morocco: Implications for Health Care Reform David R. Hotchkiss, Amparo Gordillo School of Public Health and Tropical Medicine Department of International Health and Development
Household Health Expenditures in Morocco: Implications for Health Care Reform David R. Hotchkiss, Amparo Gordillo School of Public Health and Tropical Medicine Department of International Health and Development
Rural Characteristics
 2. The effects of reforms aimed at the health care delivery system. Many delivery system reforms are intended either to encourage or restrain the managed care market and the way the delivery system is
2. The effects of reforms aimed at the health care delivery system. Many delivery system reforms are intended either to encourage or restrain the managed care market and the way the delivery system is
9FG jg\e[`e^ fe _\Xck_ ?fn cxi^\ `j k_\ dxib\k6
 Rural East Africa illustrates both the challenges BOP households face in obtaining health care and the potential health market they represent. Access to public health care is often very limited. Even finding
Rural East Africa illustrates both the challenges BOP households face in obtaining health care and the potential health market they represent. Access to public health care is often very limited. Even finding
Universal Health Coverage Assessment: Nepal. Universal Health Coverage Assessment. Nepal. Shiva Raj Adhikari. Global Network for Health Equity (GNHE)
 Universal Health Coverage Assessment Nepal Shiva Raj Adhikari Global Network for Health Equity (GNHE) December 2015 1 Universal Health Coverage Assessment: Nepal Prepared by Shiva Raj Adhikari 1 For the
Universal Health Coverage Assessment Nepal Shiva Raj Adhikari Global Network for Health Equity (GNHE) December 2015 1 Universal Health Coverage Assessment: Nepal Prepared by Shiva Raj Adhikari 1 For the
Universal Health Coverage Assessment. Republic of the Fiji Islands. Wayne Irava. Global Network for Health Equity (GNHE)
 Universal Health Coverage Assessment Republic of the Fiji Islands Wayne Irava Global Network for Health Equity (GNHE) July 2015 1 Universal Health Coverage Assessment: Republic of the Fiji Islands Prepared
Universal Health Coverage Assessment Republic of the Fiji Islands Wayne Irava Global Network for Health Equity (GNHE) July 2015 1 Universal Health Coverage Assessment: Republic of the Fiji Islands Prepared
The Trend and Pattern of Health Expenditure in India and Its Impact on the Health Sector
 EUROPEAN ACADEMIC RESEARCH Vol. III, Issue 9/ December 2015 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) The Trend and Pattern of Health Expenditure in India and Its
EUROPEAN ACADEMIC RESEARCH Vol. III, Issue 9/ December 2015 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) The Trend and Pattern of Health Expenditure in India and Its
ETHIOPIA S FIFTH NATIONAL HEALTH ACCOUNTS, 2010/2011
 Federal Democratic Republic of Ethiopia Ministry of Health ETHIOPIAN HEALTH ACCOUNTS HOUSEHOLD HEALTH SERVICE UTILIZATION AND EXPENDITURE SURVEY BRIEF ETHIOPIA S 2015/16 FIFTH NATIONAL HEALTH ACCOUNTS,
Federal Democratic Republic of Ethiopia Ministry of Health ETHIOPIAN HEALTH ACCOUNTS HOUSEHOLD HEALTH SERVICE UTILIZATION AND EXPENDITURE SURVEY BRIEF ETHIOPIA S 2015/16 FIFTH NATIONAL HEALTH ACCOUNTS,
Health care systems today account for about 9 percent of
 Health Care Financing And Delivery In Developing Countries Developing countries, which contain 84 percent of the world s population, claim only 11 percent of the world s health spending. by George Schieber
Health Care Financing And Delivery In Developing Countries Developing countries, which contain 84 percent of the world s population, claim only 11 percent of the world s health spending. by George Schieber
Nepal National Health Accounts
 Nepal National Health Accounts 2006/2007-2008/2009 Government of Nepal Ministry of Health and Population Policy, Planning and International Cooperation Division Health Economics and Financing Unit Nepal
Nepal National Health Accounts 2006/2007-2008/2009 Government of Nepal Ministry of Health and Population Policy, Planning and International Cooperation Division Health Economics and Financing Unit Nepal
Medicaid: A Lower-Cost Approach to Serving a High-Cost Population
 P O L I C Y kaiser commission on medicaid and the uninsured March 2004 B R I E F : A Lower-Cost Approach to Serving a High-Cost Population is our nation s principal provider of health insurance coverage
P O L I C Y kaiser commission on medicaid and the uninsured March 2004 B R I E F : A Lower-Cost Approach to Serving a High-Cost Population is our nation s principal provider of health insurance coverage
World Health Organization 2009
 World Health Organization 2009 This document is not a formal publication of the World Health Organization (WHO), and all rights are reserved by the Organization. The document may, however, be freely reviewed,
World Health Organization 2009 This document is not a formal publication of the World Health Organization (WHO), and all rights are reserved by the Organization. The document may, however, be freely reviewed,
Households Study on Out-of-Pocket Health Expenditures in Pakistan
 Forman Journal of Economic Studies Vol. 12, 2016 (January December) pp. 75-88 Households Study on Out-of-Pocket Health Expenditures in Pakistan Mahmood Khalid and Abdul Sattar 1 Abstract Public Health
Forman Journal of Economic Studies Vol. 12, 2016 (January December) pp. 75-88 Households Study on Out-of-Pocket Health Expenditures in Pakistan Mahmood Khalid and Abdul Sattar 1 Abstract Public Health
Rural Policy Brief Volume 10, Number 7 (PB ) November 2005 RUPRI Center for Rural Health Policy Analysis
 Rural Policy Brief Volume 10, Number 7 (PB2005-7 ) November 2005 RUPRI Center for Rural Health Policy Analysis Why Are Health Care Expenditures Increasing and Is There A Rural Differential? Timothy D.
Rural Policy Brief Volume 10, Number 7 (PB2005-7 ) November 2005 RUPRI Center for Rural Health Policy Analysis Why Are Health Care Expenditures Increasing and Is There A Rural Differential? Timothy D.
Booklet A1: Cost and Expenditure Analysis
 Booklet A1: Cost and Expenditure Analysis This booklet explains how cost analysis can be used to improve the planning and management of SRH programmes, and describes six simple analyses. Before discussion
Booklet A1: Cost and Expenditure Analysis This booklet explains how cost analysis can be used to improve the planning and management of SRH programmes, and describes six simple analyses. Before discussion
DOG BITES MAN: AMERICANS ARE SHORTSIGHTED ABOUT THEIR FINANCES
 February 2015, Number 15-3 RETIREMENT RESEARCH DOG BITES MAN: AMERICANS ARE SHORTSIGHTED ABOUT THEIR FINANCES By Steven A. Sass, Anek Belbase, Thomas Cooperrider, and Jorge D. Ramos-Mercado* Introduction
February 2015, Number 15-3 RETIREMENT RESEARCH DOG BITES MAN: AMERICANS ARE SHORTSIGHTED ABOUT THEIR FINANCES By Steven A. Sass, Anek Belbase, Thomas Cooperrider, and Jorge D. Ramos-Mercado* Introduction
How to do (or not to do)...a benefit incidence analysis
 Published by Oxford University Press in association with The London School of Hygiene and Tropical Medicine ß The Author 2010; all rights reserved. Advance Access publication 4 August 2010 Health Policy
Published by Oxford University Press in association with The London School of Hygiene and Tropical Medicine ß The Author 2010; all rights reserved. Advance Access publication 4 August 2010 Health Policy
Hong He Min-Min Lyu Nari Park May 2, 2012 South Korea Health Care System South Korea formed a Universal Healthcare system in 1977 which is controlled
 Hong He Min-Min Lyu Nari Park May 2, 2012 South Korea Health Care System South Korea formed a Universal Healthcare system in 1977 which is controlled by the government and managed under the NHIC (National
Hong He Min-Min Lyu Nari Park May 2, 2012 South Korea Health Care System South Korea formed a Universal Healthcare system in 1977 which is controlled by the government and managed under the NHIC (National
Number Obstacles in the process. of establishing sustainable. National Health Insurance Scheme: insights from Ghana
 WHO/HSS/HSF/PB/10.01 Number 1 2010 Obstacles in the process of establishing sustainable National Health Insurance Scheme: insights from Ghana Department of Health Systems Financing Health Financing Policy
WHO/HSS/HSF/PB/10.01 Number 1 2010 Obstacles in the process of establishing sustainable National Health Insurance Scheme: insights from Ghana Department of Health Systems Financing Health Financing Policy
Colombia REACHING THE POOR WITH HEALTH SERVICES. Using Proxy-Means Testing to Expand Health Insurance for the Poor. Public Disclosure Authorized
 Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized REACHING THE POOR WITH HEALTH SERVICES Colombia s poor now stand a chance of holding
Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized REACHING THE POOR WITH HEALTH SERVICES Colombia s poor now stand a chance of holding
Charu C. Garg Sr. Health Economist The World Bank Health, Nutrition and Population Human Development Network Hotel Palomar, Washington DC, October
 Charu C. Garg Sr. Health Economist The World Bank Health, Nutrition and Population Human Development Network Hotel Palomar, Washington DC, October 20, 2010 NHA: A framework to Convert Raw Data into Actionable
Charu C. Garg Sr. Health Economist The World Bank Health, Nutrition and Population Human Development Network Hotel Palomar, Washington DC, October 20, 2010 NHA: A framework to Convert Raw Data into Actionable
ECONOMICS INTERACTIONS WITH OTHER DISCIPLINES Vol. I - Sources of Health Care Funding Throughout the Globe - Stephen P. Neun
 SOURCES OF HEALTH CARE FUNDING THROUGHOUT THE GLOBE Professor of Economics, Utica College of Syracuse University, New York, USA Keywords: Financing Health Care, Risk Sharing, Third Party Payers Contents
SOURCES OF HEALTH CARE FUNDING THROUGHOUT THE GLOBE Professor of Economics, Utica College of Syracuse University, New York, USA Keywords: Financing Health Care, Risk Sharing, Third Party Payers Contents
The Center for Hospital Finance and Management
 The Center for Hospital Finance and Management 624 North Broadway/Third Floor Baltimore MD 21205 410-955-3241/FAX 410-955-2301 Mr. Chairman, and members of the Aging Committee, thank you for inviting me
The Center for Hospital Finance and Management 624 North Broadway/Third Floor Baltimore MD 21205 410-955-3241/FAX 410-955-2301 Mr. Chairman, and members of the Aging Committee, thank you for inviting me
The Development of Community-Based Health Insurance in Rwanda: Experiences and Lessons
 TECH N IC A L B R I E F MARCH 2016 Photo by Todd Shapera The Development of Community-Based Health Insurance in Rwanda: Experiences and Lessons W ith support from The Rockefeller Foundation s Transforming
TECH N IC A L B R I E F MARCH 2016 Photo by Todd Shapera The Development of Community-Based Health Insurance in Rwanda: Experiences and Lessons W ith support from The Rockefeller Foundation s Transforming
National Health and Nutrition Sector Budget Brief:
 Budget Brief Ethiopia UNICEF Ethiopia/2017/ Ayene National Health and Nutrition Sector Budget Brief: 2006-2016 Key Messages National on-budget health expenditure has increased 10 fold in nominal terms
Budget Brief Ethiopia UNICEF Ethiopia/2017/ Ayene National Health and Nutrition Sector Budget Brief: 2006-2016 Key Messages National on-budget health expenditure has increased 10 fold in nominal terms
COUNTRY CASE STUDY UNIVERSAL HEALTH INSURANCE IN COSTA RICA. Prepared by: Di McIntyre Health Economics Unit, University of Cape Town
 COUNTRY CASE STUDY UNIVERSAL HEALTH INSURANCE IN COSTA RICA Prepared by: Di McIntyre Health Economics Unit, University of Cape Town Preparation of this material was funded through a grant from the Rockefeller
COUNTRY CASE STUDY UNIVERSAL HEALTH INSURANCE IN COSTA RICA Prepared by: Di McIntyre Health Economics Unit, University of Cape Town Preparation of this material was funded through a grant from the Rockefeller
Research Report No. 69 UPDATING POVERTY AND INEQUALITY ESTIMATES: 2005 PANORA SOCIAL POLICY AND DEVELOPMENT CENTRE
 Research Report No. 69 UPDATING POVERTY AND INEQUALITY ESTIMATES: 2005 PANORA SOCIAL POLICY AND DEVELOPMENT CENTRE Research Report No. 69 UPDATING POVERTY AND INEQUALITY ESTIMATES: 2005 PANORAMA Haroon
Research Report No. 69 UPDATING POVERTY AND INEQUALITY ESTIMATES: 2005 PANORA SOCIAL POLICY AND DEVELOPMENT CENTRE Research Report No. 69 UPDATING POVERTY AND INEQUALITY ESTIMATES: 2005 PANORAMA Haroon
Booklet C.2: Estimating future financial resource needs
 Booklet C.2: Estimating future financial resource needs This booklet describes how managers can use cost information to estimate future financial resource needs. Often health sector budgets are based on
Booklet C.2: Estimating future financial resource needs This booklet describes how managers can use cost information to estimate future financial resource needs. Often health sector budgets are based on
Distribution of Public Spending across Health Facilities: A study of Karnataka, Rajasthan, Madhya Pradesh and Assam
 Distribution of Public Spending across Health Facilities: A study of Karnataka, Rajasthan, Madhya Pradesh and Assam Mita Choudhury 1 H.K. Amar Nath Bharatee Bhusana Dash National Institute of Public Finance
Distribution of Public Spending across Health Facilities: A study of Karnataka, Rajasthan, Madhya Pradesh and Assam Mita Choudhury 1 H.K. Amar Nath Bharatee Bhusana Dash National Institute of Public Finance
Increasing equity in health service access and financing: Health strategy, policy achievements and new challenges
 Increasing equity in health service access and financing: Health strategy, policy achievements and new challenges Policy Note Cambodia Health Systems in Transition A WPR/2016/DHS/009 World Health Organization
Increasing equity in health service access and financing: Health strategy, policy achievements and new challenges Policy Note Cambodia Health Systems in Transition A WPR/2016/DHS/009 World Health Organization
Presentation to SAMA Conference 2015
 Presentation to SAMA Conference 2015 NHI MODEL, RELATIONSHIP TO FINANCE AND ITS EFFECTS ON PUBLIC AND PRIVATE MEDICAL PRACTITIONERS Date: 19 SEPTEMBER 2015 Venue: Sandton Convention Centre Dr Aquina Thulare
Presentation to SAMA Conference 2015 NHI MODEL, RELATIONSHIP TO FINANCE AND ITS EFFECTS ON PUBLIC AND PRIVATE MEDICAL PRACTITIONERS Date: 19 SEPTEMBER 2015 Venue: Sandton Convention Centre Dr Aquina Thulare
Agent Network Accelerator Survey: Uganda Country Report 2013
 Agent Network Accelerator Survey: Uganda Country Report 2013 January, 2014 Contributing Authors: Kimathi Githachuri, Mike McCaffrey, Leena Anthony Annabel Lee, Anne Marie van Swinderen, Graham A. N. Wright
Agent Network Accelerator Survey: Uganda Country Report 2013 January, 2014 Contributing Authors: Kimathi Githachuri, Mike McCaffrey, Leena Anthony Annabel Lee, Anne Marie van Swinderen, Graham A. N. Wright
Out-of-Pocket Health Spending by Medicare Beneficiaries Age 65 and Older: 1997 Projections
 #9705 December 1997 Out-of-Pocket Health Spending by Medicare Beneficiaries Age 65 and Older: 1997 Projections AARP Public Policy Institute The Lewin Group David J. Gross Mary Jo Gibson Lisa Alecxih Craig
#9705 December 1997 Out-of-Pocket Health Spending by Medicare Beneficiaries Age 65 and Older: 1997 Projections AARP Public Policy Institute The Lewin Group David J. Gross Mary Jo Gibson Lisa Alecxih Craig
Medicaid Benefits for Children and Adults: Issues Raised by the National Governors Association s Preliminary Recommendations
 Medicaid Benefits for Children and Adults: Issues Raised by the National Governors Association s Preliminary Recommendations July 12, 2005 Cindy Mann Overview The Medicaid benefit package determines which
Medicaid Benefits for Children and Adults: Issues Raised by the National Governors Association s Preliminary Recommendations July 12, 2005 Cindy Mann Overview The Medicaid benefit package determines which
Implementing the New Cooperative Medical System in China. June 15, 2005
 Implementing the New Cooperative Medical System in China Philip H. Brown and Alan de Brauw June 15, 2005 DRAFT: PLEASE DO NOT CITE Department of Economics, Colby College and William Davidson Institute,
Implementing the New Cooperative Medical System in China Philip H. Brown and Alan de Brauw June 15, 2005 DRAFT: PLEASE DO NOT CITE Department of Economics, Colby College and William Davidson Institute,
PROJECT INFORMATION DOCUMENT (PID) APPRAISAL STAGE
 Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized PROJECT INFORMATION DOCUMENT (PID) APPRAISAL STAGE Project Name Kosovo Health Project
Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized PROJECT INFORMATION DOCUMENT (PID) APPRAISAL STAGE Project Name Kosovo Health Project
CONTRACTING FOR THE DELIVERY OF PRIMARY HEALTH CARE IN CAMBODIA: DESIGN AND INITIAL EXPERIENCE OF A LARGE PILOT- TEST
 Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized CONTRACTING FOR THE DELIVERY OF PRIMARY HEALTH CARE IN CAMBODIA: DESIGN AND INITIAL EXPERIENCE
Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized CONTRACTING FOR THE DELIVERY OF PRIMARY HEALTH CARE IN CAMBODIA: DESIGN AND INITIAL EXPERIENCE
Cost Sharing: Towards Sustainable Health Care in Sub-Saharan Africa
 Findings reports on ongoing operational, economic and sector work carried out by the World Bank and its member governments in the Africa Region. It is published periodically by the Africa Technical Department
Findings reports on ongoing operational, economic and sector work carried out by the World Bank and its member governments in the Africa Region. It is published periodically by the Africa Technical Department
STATUS REPORT ON MACROECONOMICS AND HEALTH NEPAL
 STATUS REPORT ON MACROECONOMICS AND HEALTH NEPAL 1. Introduction: Nepal has made a significant progress in health sector in terms of its geographical coverage by establishing at least one health care facility
STATUS REPORT ON MACROECONOMICS AND HEALTH NEPAL 1. Introduction: Nepal has made a significant progress in health sector in terms of its geographical coverage by establishing at least one health care facility
A Profile of Payday Loans Consumers Based on the 2014 Canadian Financial Capability Survey. Wayne Simpson. Khan Islam*
 A Profile of Payday Loans Consumers Based on the 2014 Canadian Financial Capability Survey Wayne Simpson Khan Islam* * Professor and PhD Candidate, Department of Economics, University of Manitoba, Winnipeg
A Profile of Payday Loans Consumers Based on the 2014 Canadian Financial Capability Survey Wayne Simpson Khan Islam* * Professor and PhD Candidate, Department of Economics, University of Manitoba, Winnipeg
Ashadul Islam Director General, Health Economics Unit Ministry of Health and Family Welfare
 Ashadul Islam Director General, Health Economics Unit Ministry of Health and Family Welfare 1 Indicator 2000-01 2012-14 Population (WDI) 132,383,265 156,594,962 Maternal mortality ratio (per 100,000 live
Ashadul Islam Director General, Health Economics Unit Ministry of Health and Family Welfare 1 Indicator 2000-01 2012-14 Population (WDI) 132,383,265 156,594,962 Maternal mortality ratio (per 100,000 live
PUBLIC HEALTH CARE CONSUMPTION: TRAGEDY OF THE COMMONS OR
 PUBLIC HEALTH CARE CONSUMPTION: TRAGEDY OF THE COMMONS OR A COMMON GOOD? Department of Demography University of California, Berkeley March 1, 2007 TABLE OF CONTENTS I. Introduction... 1 II. Background...
PUBLIC HEALTH CARE CONSUMPTION: TRAGEDY OF THE COMMONS OR A COMMON GOOD? Department of Demography University of California, Berkeley March 1, 2007 TABLE OF CONTENTS I. Introduction... 1 II. Background...
Universal Healthcare. Universal Healthcare. Universal Healthcare. Universal Healthcare
 Universal Healthcare Universal Healthcare In 2004, health care spending in the United States reached $1.9 trillion, and is projected to reach $2.9 trillion in 2009 The annual premium that a health insurer
Universal Healthcare Universal Healthcare In 2004, health care spending in the United States reached $1.9 trillion, and is projected to reach $2.9 trillion in 2009 The annual premium that a health insurer
of-pocket Expenses, Financial Protection, and Catastrophic Health Expenditures The Case of INDIA
 2nd International Conference Health Financing in Developing Countries Health Insurance, Out-of of-pocket Expenses, Financial Protection, and Catastrophic Health Expenditures The Case of INDIA Vijay Kalavakonda
2nd International Conference Health Financing in Developing Countries Health Insurance, Out-of of-pocket Expenses, Financial Protection, and Catastrophic Health Expenditures The Case of INDIA Vijay Kalavakonda
NEPAL'S DEMOGRAPHIC ISSUES. Trilochan Pokharel Nepal Administrative Staff College
 NEPAL'S DEMOGRAPHIC ISSUES Trilochan Pokharel pokharel.trilochan@gmail.com Nepal Administrative Staff College Presentation Outline 2 1. Key highlights of Nepal based on different sources 2. Future demographic
NEPAL'S DEMOGRAPHIC ISSUES Trilochan Pokharel pokharel.trilochan@gmail.com Nepal Administrative Staff College Presentation Outline 2 1. Key highlights of Nepal based on different sources 2. Future demographic
Issue Brief. Findings from the Commonwealth Fund Survey of Older Adults
 TASK FORCE ON THE FUTURE OF HEALTH INSURANCE Issue Brief JUNE 2005 Paying More for Less: Older Adults in the Individual Insurance Market Findings from the Commonwealth Fund Survey of Older Adults Sara
TASK FORCE ON THE FUTURE OF HEALTH INSURANCE Issue Brief JUNE 2005 Paying More for Less: Older Adults in the Individual Insurance Market Findings from the Commonwealth Fund Survey of Older Adults Sara
Overview of the ACA and 2014 Premiums
 Overview of the ACA and 2014 Premiums July 10, 2013 An independent licensee of the Blue Cross and Blue Shield Association. U7430b, 2/11 Introduction Topics for today s discussion: + Overview of the Louisiana
Overview of the ACA and 2014 Premiums July 10, 2013 An independent licensee of the Blue Cross and Blue Shield Association. U7430b, 2/11 Introduction Topics for today s discussion: + Overview of the Louisiana
The Role of the Private Sector in Expanding Health Access to the Base of the Pyramid
 The Role of the Private Sector in Expanding Health Access to the Base of the Pyramid ABOUT IFC IFC, a member of the World Bank Group, is the largest global development institution focused exclusively on
The Role of the Private Sector in Expanding Health Access to the Base of the Pyramid ABOUT IFC IFC, a member of the World Bank Group, is the largest global development institution focused exclusively on
Co-payments, Choices and Coverage: Meeting the Challenge of Health Financing for Consumers
 Co-payments, Choices and Coverage: Meeting the Challenge of Health Financing for Consumers Dr Sharon Willcox, Health Policy Solutions Catholic Health Australia National Conference 27 August 2013 OUTLINE
Co-payments, Choices and Coverage: Meeting the Challenge of Health Financing for Consumers Dr Sharon Willcox, Health Policy Solutions Catholic Health Australia National Conference 27 August 2013 OUTLINE
I. Introduction. Source: CIA World Factbook. Population in the World
 How electricity consumption affects social and economic development by comparing low, medium and high human development countries By Chi Seng Leung, associate researcher and Peter Meisen, President, GENI
How electricity consumption affects social and economic development by comparing low, medium and high human development countries By Chi Seng Leung, associate researcher and Peter Meisen, President, GENI
LESOTHO HEALTH BUDGET BRIEF 1 NOVEMBER 2017
 @UNICEF/Lesotho/CLThomas2016 LESOTHO HEALTH BUDGET BRIEF 1 NOVEMBER 2017 This budget brief is one of four that explores the extent to which the national budget addresses the needs of the health of Lesotho
@UNICEF/Lesotho/CLThomas2016 LESOTHO HEALTH BUDGET BRIEF 1 NOVEMBER 2017 This budget brief is one of four that explores the extent to which the national budget addresses the needs of the health of Lesotho
Evaluation of the Primary Health Care Strategy: Changes in Fees and Consultation Rates between 2001 and 2007
 Evaluation of the Primary Health Care Strategy: Changes in Fees and Consultation Rates between 2001 and 2007 Antony Raymont Jacqueline Cumming Barry Gribben SEPTEMBER 2013 1 Published in September 2013
Evaluation of the Primary Health Care Strategy: Changes in Fees and Consultation Rates between 2001 and 2007 Antony Raymont Jacqueline Cumming Barry Gribben SEPTEMBER 2013 1 Published in September 2013
The Distribution of Federal Taxes, Jeffrey Rohaly
 www.taxpolicycenter.org The Distribution of Federal Taxes, 2008 11 Jeffrey Rohaly Overall, the federal tax system is highly progressive. On average, households with higher incomes pay taxes that are a
www.taxpolicycenter.org The Distribution of Federal Taxes, 2008 11 Jeffrey Rohaly Overall, the federal tax system is highly progressive. On average, households with higher incomes pay taxes that are a
Results from a social protection technical assistance program. July 2011
 Results from a social protection technical assistance program July 2011 Political and Development Context Simultaneous transitions Conflict to peace Unitary system to a federal polity Monarchical, hierarchical
Results from a social protection technical assistance program July 2011 Political and Development Context Simultaneous transitions Conflict to peace Unitary system to a federal polity Monarchical, hierarchical
Checkup on Health Insurance Choices
 Page 1 of 17 Checkup on Health Insurance Choices Today, there are more types of health insurance, and more choices, than ever before. The information presented here will help you choose a plan that is
Page 1 of 17 Checkup on Health Insurance Choices Today, there are more types of health insurance, and more choices, than ever before. The information presented here will help you choose a plan that is
September 2013
 September 2013 Copyright 2013 Health Care Cost Institute Inc. Unless explicitly noted, the content of this report is licensed under a Creative Commons Attribution Non-Commercial No Derivatives 3.0 License
September 2013 Copyright 2013 Health Care Cost Institute Inc. Unless explicitly noted, the content of this report is licensed under a Creative Commons Attribution Non-Commercial No Derivatives 3.0 License
Executive Summary. Findings from Current Research
 Current State of Research on Social Inclusion in Asia and the Pacific: Focus on Ageing, Gender and Social Innovation (Background Paper for Senior Officials Meeting and the Forum of Ministers of Social
Current State of Research on Social Inclusion in Asia and the Pacific: Focus on Ageing, Gender and Social Innovation (Background Paper for Senior Officials Meeting and the Forum of Ministers of Social
Resource Allocation, Purchasing and Payment Mechanisms in Health Financing
 Resource Allocation, Purchasing and Payment Mechanisms in Health Financing by William C. Hsiao K.T. Li Professor of Economics Harvard School of Public Health SA Regional High Level Forum on Health Financing
Resource Allocation, Purchasing and Payment Mechanisms in Health Financing by William C. Hsiao K.T. Li Professor of Economics Harvard School of Public Health SA Regional High Level Forum on Health Financing
PROJECT INFORMATION DOCUMENT (PID) CONCEPT STAGE
 Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Project Name PROJECT INFORMATION DOCUMENT (PID) CONCEPT STAGE Health Sector Support Project
Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Project Name PROJECT INFORMATION DOCUMENT (PID) CONCEPT STAGE Health Sector Support Project
H.R American Health Care Act of 2017
 CONGRESSIONAL BUDGET OFFICE COST ESTIMATE May 24, 2017 H.R. 1628 American Health Care Act of 2017 As passed by the House of Representatives on May 4, 2017 SUMMARY The Congressional Budget Office and the
CONGRESSIONAL BUDGET OFFICE COST ESTIMATE May 24, 2017 H.R. 1628 American Health Care Act of 2017 As passed by the House of Representatives on May 4, 2017 SUMMARY The Congressional Budget Office and the
The Impact of Community-Based Health Insurance on Access to Care and Equity in Rwanda
 TECH N IC A L B R I E F MARCH 16 Photo by Todd Shapera The Impact of Community-Based Health Insurance on Access to Care and Equity in Rwanda W ith support from The Rockefeller Foundation s Transforming
TECH N IC A L B R I E F MARCH 16 Photo by Todd Shapera The Impact of Community-Based Health Insurance on Access to Care and Equity in Rwanda W ith support from The Rockefeller Foundation s Transforming
Proposed Changes to Medicare in the Path to Prosperity Overview and Key Questions
 Proposed Changes to Medicare in the Path to Prosperity Overview and Key Questions APRIL 2011 On April 5, 2011, Representative Paul Ryan (R-WI), chairman of the House Budget Committee, released a budget
Proposed Changes to Medicare in the Path to Prosperity Overview and Key Questions APRIL 2011 On April 5, 2011, Representative Paul Ryan (R-WI), chairman of the House Budget Committee, released a budget
Health Insurance for Poor People in the Province Of Santa Fe, Argentina: The Power of the Clear Model for All
 ARGENTINA Health Insurance for Poor People in the Province Of Santa Fe, Argentina: The Power of the Clear Model for All FAMEDIC and Ministry of Health of Santa Fe. SUMMARY In Argentina, the system is characterized
ARGENTINA Health Insurance for Poor People in the Province Of Santa Fe, Argentina: The Power of the Clear Model for All FAMEDIC and Ministry of Health of Santa Fe. SUMMARY In Argentina, the system is characterized
Mitigating the Impact of the Global Economic Crisis on Household Health Spending
 50834 Mitigating the Impact of the Global Economic Crisis on Household Health Spending Elizabeth Docteur Key Messages The economic crisis is impacting the ability of households in ECA countries to pay
50834 Mitigating the Impact of the Global Economic Crisis on Household Health Spending Elizabeth Docteur Key Messages The economic crisis is impacting the ability of households in ECA countries to pay
Fiscal Implications of Chronic Diseases. Peter S. Heller SAIS, Johns Hopkins University November 23, 2009
 Fiscal Implications of Chronic Diseases Peter S. Heller SAIS, Johns Hopkins University November 23, 2009 Defining Chronic Diseases of Concern Cancers Diabetes Cardiovascular diseases Mental Dementia (Alzheimers
Fiscal Implications of Chronic Diseases Peter S. Heller SAIS, Johns Hopkins University November 23, 2009 Defining Chronic Diseases of Concern Cancers Diabetes Cardiovascular diseases Mental Dementia (Alzheimers
How would an expansion of IDA reduce poverty and further other development goals?
 Measuring IDA s Effectiveness Key Results How would an expansion of IDA reduce poverty and further other development goals? We first tackle the big picture impact on growth and poverty reduction and then
Measuring IDA s Effectiveness Key Results How would an expansion of IDA reduce poverty and further other development goals? We first tackle the big picture impact on growth and poverty reduction and then
A Publication by the Massachusetts Association of Health Plans. Health Insurance 101 How Are Premiums Developed for Individuals and Small Groups?
 OnPoint: Issue Brief A Publication by the Massachusetts Association of Health Plans Volume VIII, April 2017 Written by Eric Linzer Health Insurance 101 How Are Premiums Developed for Individuals and Small
OnPoint: Issue Brief A Publication by the Massachusetts Association of Health Plans Volume VIII, April 2017 Written by Eric Linzer Health Insurance 101 How Are Premiums Developed for Individuals and Small
Issue Brief. Does Medicaid Make a Difference? The COMMONWEALTH FUND. Findings from the Commonwealth Fund Biennial Health Insurance Survey, 2014
 Issue Brief JUNE 2015 The COMMONWEALTH FUND Does Medicaid Make a Difference? Findings from the Commonwealth Fund Biennial Health Insurance Survey, 2014 The mission of The Commonwealth Fund is to promote
Issue Brief JUNE 2015 The COMMONWEALTH FUND Does Medicaid Make a Difference? Findings from the Commonwealth Fund Biennial Health Insurance Survey, 2014 The mission of The Commonwealth Fund is to promote
December 2009 Report No
 December 2009 Report No. 09-40 University Students Pay $68 Million for Health Services; Mandating Health Insurance Would Produce Benefits But Raise Uninsured Students Cost of Attendance 5% to 7% at a glance
December 2009 Report No. 09-40 University Students Pay $68 Million for Health Services; Mandating Health Insurance Would Produce Benefits But Raise Uninsured Students Cost of Attendance 5% to 7% at a glance
Healthcare and Health Insurance Choices: How Consumers Decide
 Healthcare and Health Insurance Choices: How Consumers Decide CONSUMER SURVEY FALL 2016 Despite the growing importance of healthcare consumerism, relatively little is known about consumer attitudes and
Healthcare and Health Insurance Choices: How Consumers Decide CONSUMER SURVEY FALL 2016 Despite the growing importance of healthcare consumerism, relatively little is known about consumer attitudes and
Vermont Health Care Cost and Utilization Report
 2007 2011 Vermont Health Care Cost and Utilization Report Revised December 2014 Copyright 2014 Health Care Cost Institute Inc. Unless explicitly noted, the content of this report is licensed under a Creative
2007 2011 Vermont Health Care Cost and Utilization Report Revised December 2014 Copyright 2014 Health Care Cost Institute Inc. Unless explicitly noted, the content of this report is licensed under a Creative
ASSESSMENT OF FINANCIAL PROTECTION IN THE VIET NAM HEALTH SYSTEM: ANALYSES OF VIETNAM LIVING STANDARD SURVEY DATA
 WORLD HEALTH ORGANIZATION IN VIETNAM HA NOI MEDICAL UNIVERSITY Research report ASSESSMENT OF FINANCIAL PROTECTION IN THE VIET NAM HEALTH SYSTEM: ANALYSES OF VIETNAM LIVING STANDARD SURVEY DATA 2002-2010
WORLD HEALTH ORGANIZATION IN VIETNAM HA NOI MEDICAL UNIVERSITY Research report ASSESSMENT OF FINANCIAL PROTECTION IN THE VIET NAM HEALTH SYSTEM: ANALYSES OF VIETNAM LIVING STANDARD SURVEY DATA 2002-2010
Sector-wide Health System and Social Development Support Project Region
 PROJECT INFORMATION DOCUMENT (PID) CONCEPT STAGE Report No.: AB1473 Country Mali Prpoject ID P093689 Project Name Sector-wide Health System and Social Development Support Project Region AFRICA Sector Health
PROJECT INFORMATION DOCUMENT (PID) CONCEPT STAGE Report No.: AB1473 Country Mali Prpoject ID P093689 Project Name Sector-wide Health System and Social Development Support Project Region AFRICA Sector Health
Predictive Analytics in the People s Republic of China
 Predictive Analytics in the People s Republic of China Rong Yi, PhD Senior Consultant Rong.Yi@milliman.com Tel: 781.213.6200 4 th National Predictive Modeling Summit Arlington, VA September 15-16, 2010
Predictive Analytics in the People s Republic of China Rong Yi, PhD Senior Consultant Rong.Yi@milliman.com Tel: 781.213.6200 4 th National Predictive Modeling Summit Arlington, VA September 15-16, 2010
Aging in India: Its Socioeconomic. Implications
 Aging in India: Its Socioeconomic and Health Implications By the year 2000, India is likely to rank second to China in the absolute numbers of its elderly population By H.B. Chanana and P.P. Talwar* The
Aging in India: Its Socioeconomic and Health Implications By the year 2000, India is likely to rank second to China in the absolute numbers of its elderly population By H.B. Chanana and P.P. Talwar* The
How Much Are Medicare Beneficiaries Paying Out-of-Pocket for Prescription Drugs?
 #9914 September 1999 How Much Are Medicare Beneficiaries Paying Out-of-Pocket for Prescription Drugs? by Mary Jo Gibson Normandy Brangan David Gross Craig Caplan AARP Public Policy Institute The Public
#9914 September 1999 How Much Are Medicare Beneficiaries Paying Out-of-Pocket for Prescription Drugs? by Mary Jo Gibson Normandy Brangan David Gross Craig Caplan AARP Public Policy Institute The Public
m e d i c a i d Five Facts About the Uninsured
 kaiser commission o n K E Y F A C T S m e d i c a i d a n d t h e uninsured Five Facts About the Uninsured September 2011 September 2010 The number of non elderly uninsured reached 49.1 million in 2010.
kaiser commission o n K E Y F A C T S m e d i c a i d a n d t h e uninsured Five Facts About the Uninsured September 2011 September 2010 The number of non elderly uninsured reached 49.1 million in 2010.
Social Health Protection In Lao PDR
 Social Health Protection In Lao PDR Presented by Lao Team in the International Forum on the development of Social Health Protection in the Southeast Asian Region Hanoi, 27-28/10/2014 Presentation Outline
Social Health Protection In Lao PDR Presented by Lao Team in the International Forum on the development of Social Health Protection in the Southeast Asian Region Hanoi, 27-28/10/2014 Presentation Outline
Texas Small Employer Health Insurance Survey Results: 2001 and Texas Department of Insurance
 Texas Small Employer Health Insurance Survey Results: 2001 and 2004 Texas Department of Insurance November 2005 Table of Contents Section I: Survey Overview.1 Section II: Employers Not Currently Offering
Texas Small Employer Health Insurance Survey Results: 2001 and 2004 Texas Department of Insurance November 2005 Table of Contents Section I: Survey Overview.1 Section II: Employers Not Currently Offering
Re: Medicare Prescription Drug Benefit Manual Draft Chapter 5
 September 18, 2006 BY ELECTRONIC DELIVERY Cynthia Tudor, Ph.D. Director, Medicare Drug Benefit Group Centers for Medicare and Medicaid Services Department of Health and Human Services Mail Stop C4-13-01
September 18, 2006 BY ELECTRONIC DELIVERY Cynthia Tudor, Ph.D. Director, Medicare Drug Benefit Group Centers for Medicare and Medicaid Services Department of Health and Human Services Mail Stop C4-13-01
POLICY BRIEF. Figure 1: Total, general government, and private expenditures on health as percentages of GDP
 POLICY BRIEF Financial Burden of Health Payments in Mongolia The World Health Report 2010 drew attention to the fact that each year 150 million people globally are facing catastrophic health expenditures,
POLICY BRIEF Financial Burden of Health Payments in Mongolia The World Health Report 2010 drew attention to the fact that each year 150 million people globally are facing catastrophic health expenditures,
WHY ARE OLDER WORKERS AT GREATER RISK OF DISPLACEMENT?
 May 2009, Number 9-10 WHY ARE OLDER WORKERS AT GREATER RISK OF DISPLACEMENT? By Alicia H. Munnell, Steven A. Sass, and Natalia A. Zhivan* Introduction The conventional wisdom says that older workers are
May 2009, Number 9-10 WHY ARE OLDER WORKERS AT GREATER RISK OF DISPLACEMENT? By Alicia H. Munnell, Steven A. Sass, and Natalia A. Zhivan* Introduction The conventional wisdom says that older workers are
Determinants of Expenditure on Health in Pakistan
 The Pakistan Development Review 34 : 4 Part III (Winter 1995) pp. 959 970 Determinants of Expenditure on Health in Pakistan REHANA SIDDIQUI, USMAN AFRIDI, and RASHIDA HAQ An important component of human
The Pakistan Development Review 34 : 4 Part III (Winter 1995) pp. 959 970 Determinants of Expenditure on Health in Pakistan REHANA SIDDIQUI, USMAN AFRIDI, and RASHIDA HAQ An important component of human
Data and Methods in FMLA Research Evidence
 Data and Methods in FMLA Research Evidence The Family and Medical Leave Act (FMLA) was passed in 1993 to provide job-protected unpaid leave to eligible workers who needed time off from work to care for
Data and Methods in FMLA Research Evidence The Family and Medical Leave Act (FMLA) was passed in 1993 to provide job-protected unpaid leave to eligible workers who needed time off from work to care for
Aging in Asia and Oceania AARP Multinational Survey of Opinion Leaders 2006
 Aging in Asia and Oceania AARP Multinational Survey of Opinion Leaders 2006 Highlights and Implications March 2007 Prepared by Princeton Survey Research Associates International for Aging in Asia and
Aging in Asia and Oceania AARP Multinational Survey of Opinion Leaders 2006 Highlights and Implications March 2007 Prepared by Princeton Survey Research Associates International for Aging in Asia and
NEPAL. Public Disclosure Authorized. Public Disclosure Authorized. Public Disclosure Authorized. Public Disclosure Authorized
 Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Health Equity and Financial Protection DATASHEET NEPAL The Health Equity and Financial
Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Public Disclosure Authorized Health Equity and Financial Protection DATASHEET NEPAL The Health Equity and Financial
This report summarizes the major arguments put forward by Richard Lane & Kara Hanson, Faculty of Public Health, London School of Hygiene and Tropical
 This report summarizes the major arguments put forward by Richard Lane & Kara Hanson, Faculty of Public Health, London School of Hygiene and Tropical Medicine. In this podcast produced by the Lancet, they
This report summarizes the major arguments put forward by Richard Lane & Kara Hanson, Faculty of Public Health, London School of Hygiene and Tropical Medicine. In this podcast produced by the Lancet, they
THE COMMONWEALTH FUND SURVEY OF HEALTH CARE IN NEW YORK CITY
 THE COMMONWEALTH FUND SURVEY OF HEALTH CARE IN NEW YORK CITY David Sandman, Cathy Schoen, Catherine Des Roches, and Meron Makonnen MARCH 1998 THE COMMONWEALTH FUND The Commonwealth Fund is a philanthropic
THE COMMONWEALTH FUND SURVEY OF HEALTH CARE IN NEW YORK CITY David Sandman, Cathy Schoen, Catherine Des Roches, and Meron Makonnen MARCH 1998 THE COMMONWEALTH FUND The Commonwealth Fund is a philanthropic
Living Standards. Why can t I have what he s got?
 Living Standards Why can t I have what he s got? OR Is it possible for everyone to have the same standard of living (in a country and around the world)? Standard of Living standard of living refers to
Living Standards Why can t I have what he s got? OR Is it possible for everyone to have the same standard of living (in a country and around the world)? Standard of Living standard of living refers to
Medicare Advantage (MA) Proposed Benchmark Update and Other Adjustments for CY2020: In Brief
 Medicare Advantage (MA) Proposed Benchmark Update and Other Adjustments for CY2020: In Brief February 7, 2019 Congressional Research Service https://crsreports.congress.gov R45494 Contents Introduction...
Medicare Advantage (MA) Proposed Benchmark Update and Other Adjustments for CY2020: In Brief February 7, 2019 Congressional Research Service https://crsreports.congress.gov R45494 Contents Introduction...
Critical Demographics: Rapid Aging and the Shape of the Future in China, South Korea, and Japan
 Critical Demographics: Rapid Aging and the Shape of the Future in China, South Korea, and Japan Briefing for Fast Forward Scenario Planning Workshop February 27, 29 DIFFERENT SHAPES, DIFFERENT REALITIES
Critical Demographics: Rapid Aging and the Shape of the Future in China, South Korea, and Japan Briefing for Fast Forward Scenario Planning Workshop February 27, 29 DIFFERENT SHAPES, DIFFERENT REALITIES
Although a larger percentage of the world s population
 Social health protection coverage 3 Although a larger percentage of the world s population has access to health-care services than to various cash benefits, nearly one-third has no access to any health
Social health protection coverage 3 Although a larger percentage of the world s population has access to health-care services than to various cash benefits, nearly one-third has no access to any health
Sri Lanka s Health Sector
 Sri Lanka s Health Sector Issues, Challenges and Future Dr Ravi P. Rannan-Eliya Director Institute for Health Policy www.ihp.lk Ceylon Chamber of Commerce Colombo 26 September 2005 Outline A performance
Sri Lanka s Health Sector Issues, Challenges and Future Dr Ravi P. Rannan-Eliya Director Institute for Health Policy www.ihp.lk Ceylon Chamber of Commerce Colombo 26 September 2005 Outline A performance
Health Care Financing: Looking Towards Kurdistan s Future
 Health Care Financing: Looking Towards Kurdistan s Future Presentation for International Congress on Reform and Development of Health Care in Kurdistan Region C. Ross Anthony, Ph.D. 2-4 February 2011 Erbil
Health Care Financing: Looking Towards Kurdistan s Future Presentation for International Congress on Reform and Development of Health Care in Kurdistan Region C. Ross Anthony, Ph.D. 2-4 February 2011 Erbil
Correlates of Out-of-Pocket Spending in Nepal: Implications for Policy. Indrani Gupta and Samik Chowdhury
 Correlates of Out-of-Pocket Spending in Nepal: Implications for Policy Indrani Gupta and Samik Chowdhury 1. Introduction Health equity has been conceptualized and defined in several ways, as its principles
Correlates of Out-of-Pocket Spending in Nepal: Implications for Policy Indrani Gupta and Samik Chowdhury 1. Introduction Health equity has been conceptualized and defined in several ways, as its principles
Health Insurance Glossary of Terms
 1 Health Insurance Glossary of Terms On March 23, 2010, President Obama signed the Patient Protection and Affordable Care Act (PPACA) into law. When making decisions about health coverage, consumers should
1 Health Insurance Glossary of Terms On March 23, 2010, President Obama signed the Patient Protection and Affordable Care Act (PPACA) into law. When making decisions about health coverage, consumers should
Benefit Incidence, Financing Incidence and Need of Healthcare Services in South Africa
 Benefit Incidence, Financing Incidence and Need of Healthcare Services in South Africa Dr Paula Armstrong, Mariné Erasmus & Elize Rich In the context of the envisaged implementation of National Health
Benefit Incidence, Financing Incidence and Need of Healthcare Services in South Africa Dr Paula Armstrong, Mariné Erasmus & Elize Rich In the context of the envisaged implementation of National Health
HEALTH CARE MODELS: INTERNATIONAL COMPARISONS
 HEALTH CARE MODELS: INTERNATIONAL COMPARISONS Dr. Jaime Llambías-Wolff, Ph.D. York University Based and adapted from presentation by : Dr. Sibu Saha, MD, MBA Professor of Surgery University of Kentucky
HEALTH CARE MODELS: INTERNATIONAL COMPARISONS Dr. Jaime Llambías-Wolff, Ph.D. York University Based and adapted from presentation by : Dr. Sibu Saha, MD, MBA Professor of Surgery University of Kentucky
Populations: an Introduction to Demography. Population Trends In Canada
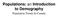 Populations: an Introduction to Demography Population Trends In Canada Demography Demography is the study of populations over time and over place. The three major components of demography are: (1) mortality,
Populations: an Introduction to Demography Population Trends In Canada Demography Demography is the study of populations over time and over place. The three major components of demography are: (1) mortality,
Review of Federal Funding to Florida in Fiscal Year 2009
 Review of Federal Funding to Florida in Fiscal Year 2009 March 2011 The Florida Legislature s Office of Economic and Demographic Research Executive Summary Office of Economic and Demographic Research
Review of Federal Funding to Florida in Fiscal Year 2009 March 2011 The Florida Legislature s Office of Economic and Demographic Research Executive Summary Office of Economic and Demographic Research
Ensuring financial risk protection
 Long-term effects of the abolition of user fees in Uganda Juliet Nabyonga, i Maximillan Mapunda, ii Laurent Musango iii and Frederick Mugisha iv Corresponding author: Juliet Nabyonga, e-mail: nabyongaj@ug.afro.who.int
Long-term effects of the abolition of user fees in Uganda Juliet Nabyonga, i Maximillan Mapunda, ii Laurent Musango iii and Frederick Mugisha iv Corresponding author: Juliet Nabyonga, e-mail: nabyongaj@ug.afro.who.int
