As announced in the Winter 2013 edition of
|
|
|
- Alexander Black
- 5 years ago
- Views:
Transcription
1 The Newsletter of the Screen Actors Guild Producers Pension and Health Plans Volume XXII, Number 2 Summer 2014 INSIDE TAKE 2 Anesthesia During Colonoscopy... 3 Therapy Bene t Limits and Allowances... 4 Changes to Non-Network Medical Bene ts... 5 Pension Bene t Payments Transition... 6 Combined Earnings Eligibility Reminder... 7 Self-Pay vs. Marketplace... 7 Prescription Drug Step Therapy Requirements Added Effective July 1, 2014 As announced in the Winter 2013 edition of Take 2, the Trustees have added a step therapy program for the prescription drug benefit in their effort to help reduce cost increases for participants and dependents. The step therapy program will be effective July 1, 2014 and will apply to medications first prescribed after July 1, 2014 and received at retail pharmacies or through Express Scripts (formerly Medco) home delivery service. The Plan is implementing step therapy, as have a number of other health plans, in order to counter the ever-increasing cost of prescription drug spending. What is step therapy? Step therapy requires that people who have certain conditions, such as high blood pressure, nasal allergies or acid reflux, try effective and more affordable prescription drugs first before stepping up to more expensive drugs. Step 1 drugs Front-line drugs are generic and sometimes lower-cost brand name drugs that are proven to be safe, effective and affordable. In most cases you should try these drugs first because they usually provide the same health benefit as a more expensive drug, at a lower cost to you and the Plan. Step 2 and Step 3 drugs Second-line drugs are brand name alternative drugs that generally are necessary for only a small number of patients for whom front-line drugs have failed. Third-line drugs are the most expensive option and have not shown greater clinical efficacy than lower-cost drugs. Who decides what drugs are covered in step therapy? Step therapy is developed under the guidance and direction of independent licensed doctors, pharmacists and other medical experts. Together with Express Scripts, they review the most current research on thousands of drugs tested and approved by the FDA for safety and effectiveness. Then they recommend appropriate prescription drugs for the program. Not all medications are subject to the step therapy requirement and the prescription drugs that are may change from time to time. Your pharmacist can tell you if your prescription requires step therapy or you can find out by logging in to your account at and clicking Price a Medication. Continued on page 2
2 Prescription Drug Step Therapy Requirements Added Continued from page 1 Why couldn t I fill my prescription at the pharmacy? The first time you submit a prescription that is not for a front-line drug, your pharmacist should tell you that with step therapy you need to first try a front-line drug if you would rather not pay full price for the medication. To receive a front-line drug: Ask your pharmacist to call your doctor and request a new prescription; or Contact your doctor to get a new prescription. Only your doctor can change your current prescription to a front-line drug covered by the step therapy program. What can I do when I need a prescription filled immediately? If you have just been prescribed a medication subject to step therapy, you may be informed at your pharmacy that your prescription is not covered. If this should happen and you need the medication immediately, you can talk with your pharmacist about filling a small supply right away. You will have to pay full price for this quantity of the drug. Then, you or your pharmacist can contact your doctor for a new prescription for a front-line drug. What can I do if I have already tried the front-line drugs on the list? With step therapy, more expensive brand-name drugs are usually covered as second-line alternative drugs if: 1. You have already tried the generic drugs covered in the step therapy program and they were unsuccessful. 2. You cannot take a specific generic drug (for example, because of a documented allergy). 3. Your doctor decides, for medical reasons, that you need a brand-name drug. If one of these situations applies to you, your doctor can request an override from Express Scripts, allowing you to take a second-line prescription drug. Once the override is approved, you will pay the appropriate copay for the drug. What happens if my doctor s request for an override is denied? You can follow the appeals process as outlined in Express Scripts denial letter or in the Health Summary Plan Description available at If you choose not to appeal or your appeal is denied, you can talk to your doctor again about prescribing one of the safe, effective front-line drugs covered by the step therapy program. Or you can choose to pay the full price for the drug. How does step therapy work at the home delivery pharmacy? When Express Scripts home delivery pharmacy receives a prescription that requires step therapy, a representative contacts your doctor to request a new prescription for a front-line drug. If after several attempts Express Scripts is unable to reach your doctor, you will be notified by phone that there is a delay with your order. You may want to let your doctor know that the home delivery pharmacy will be requesting this information. Your doctor will write you a new prescription for a front-line drug covered by the step therapy program. Or, if your doctor decides your current drug is medically necessary, he or she can ask for an override. The appeals process is also available if your doctor s request is denied. What if I am already taking a second-line drug on July 1, 2014? This medication will not be subject to the step therapy requirement for as long as your doctor continues to prescribe it, provided you remain continuously eligible for prescription drug coverage under the Health Plan. Who should I call if I have additional step therapy questions? Express Scripts (800)
3 Anesthesia During Colonoscopy and Upper GI Endoscopy Understanding Your Coverage The Health Plan encourages participants to take advantage of the wellness benefits offered by the Plan. One of these important benefits is a routine colonoscopy offered to participants beginning at age 50. The Plan also covers diagnostic colonoscopies and upper gastrointestinal endoscopies regardless of age, although these procedures are not considered under the wellness benefit. Best medical practices indicate that these procedures, whether diagnostic or preventive, should be performed under moderate sedation provided by a gastroenterologist or a member of his or her team. This level of sedation is highly effective and is included in the doctor s surgical package fee at no additional expense to the patient when performed in this manner. If a separate anesthesiologist is used, the Plan will not cover his or her charges. However, patients with certain health conditions or physical abnormalities may need a deeper level of sedation using different medications than those used in moderate sedation. Deep sedation may affect your ability to breathe on your own and your cardiovascular function. Due to the need for more intensive monitoring, deep sedation usually requires that an anesthesiologist be present to administer the specific medications that induce the deep sedation. The Plan s coverage of an anesthesiologist is based on whether you have a health condition or abnormality which necessitates the use of these different medications. The Plan does provide coverage for a separate anesthesiologist for patients over the age of 70 or under the age of 18. The Plan will not provide coverage for an anesthesiologist simply because they are used to achieve deeper sedation in patients for whom they are not considered medically necessary. Talk with your doctor regarding your particular needs ahead of the procedure if you have concerns about your comfort during a colonoscopy or upper gastrointestinal endoscopy. Some providers offer deep sedation for an additional fee that the patient must pay. If you have any questions about coverage of an anesthesiologist under these circumstances, please call the Plan Office. 3
4 Therapy Benefit Limits and Allowances The Health Plan s therapy benefits include coverage for different types of therapies such as physical therapy, occupational therapy, chiropractic care and acupuncture. The Plan has a maximum allowance it will consider that depends on the type of therapy and whether you are using a network or non-network provider. In addition, the Plan has a maximum number of visits for certain types of therapy. The chart below outlines these allowances and maximums. Therapy Network Allowance Non-Network Allowance Maximum Visits Per Quarter Acupuncture Contract Allowance $55 per visit 8 visits* Biofeedback Contract Allowance $55 per visit 9 visits Chiropractic $45 per visit $45 per visit 12 visits* Physical,Occupational and Osteopathic Contract Allowance $65 per visit None Speech and Vision Contract Allowance $55 per visit None * The Plan will not consider more than 12 visits per calendar quarter for chiropractic treatment or eight visits per calendar quarter for acupuncture. Chiropractic visits count toward the acupuncture maximum and vice versa. While the number of visits for physical, occupational, osteopathic, speech and vision therapies do not have a visit limit, they will count toward the chiropractic and acupuncture limits. As an example of how these visit limits apply, suppose you have six physical therapy visits during a calendar quarter followed by four chiropractic visits. This is allowable because you are still within your 12 visit limit (6 + 4 = 10 visits). If you then wanted to go to an acupuncturist, no acupuncture visits would be payable for the rest of the quarter. You are over the eight visit acupuncture maximum because your earlier physical therapy and chiropractic care visits count toward that limit. If you are receiving multiple types of therapy from different providers, you should be aware that the Plan applies visits toward the limits as it processes claims rather than according to the date of service. Providers submit their claims in accordance with their own billing schedules and claims are frequently not received in the order of their date of service. The therapy benefits are subject to additional requirements and limitations regarding provider type and covered services. For a more complete description of the benefits, please refer to your Health Plan Summary Plan Description. Mental health therapy visits are not counted towards any of the above therapies. Like physical, occupational, osteopathic, speech and vision therapies, there is no maximum number of visits per quarter, however all therapy visits are subject to medical necessity. 4
5 Reminder of Changes to Non-Network Medical Benefits Effective July 1, 2014 The Trustees periodically review the provisions of the Health Plan in order to make sure they are in line with industry practice and make sense for the Plan. In an effort to encourage network utilization, effective July 1, 2014, the Plan will add copays to non-network medical benefits for Plan I and Plan II. The non-network copays will be the same as the copays under network medical benefits. Please refer to the chart below: Medical Copays Network or Non-Network Plan I Plan II Office Visit $15 per visit $25 per visit Surgeon Doctor s Office $15 per surgery $25 per surgery Inpatient $100 per surgery $100 per surgery Outpatient Hospital, Surgical Center, Surgical Suite $100 per surgery $100 per surgery Maternity Prenatal Visits No copay No copay Delivery $100 per delivery $100 per delivery Although the non-network copays will be the same as the network amounts, you still have lower outof-pocket expenses from a network provider. The network deductible is significantly lower than the non-network deductible. So is the coinsurance, which is the percentage of covered charges that you pay after the deductible and copay are satisfied 10% as compared to 30%. Plus, as announced in the Fall 2013 Take 2, the Plan added a new overall out-of-pocket maximum of $6,350 per person and $12,700 per family for network hospital and medical services effective January 1, Non-network services do not have an overall out-of-pocket maximum. Instead you continue to be charged a copay for each visit and surgery even if your coinsurance maximum has been satisfied. 5
6 You can withdraw money, put some in savings or pay bills - all the things you do with your money now. The only difference is your check is not printed or mailed. At this time, direct deposit is only mandatory for those planning to retire on or after July 1, However, as of January 1, 2015 the Plan will require that all retirees receive their benefit electronically. If you are currently receiving retirement benefits and you did not sign up for electronic payments, we encourage you to do so now. Sign up for direct deposit by contacting the Pension Department at (818) extension If your Senior Performers premium is currently deducted from your pension benefit, it will continue to be deducted. Pension Benefit Payments to Transition to Electronic Funds Transfer Effective July 1, 2014 the Screen Actors Guild- Producers Pension Plan will require that all new retirees receive pension benefit payments electronically. You may choose to have your payments directly deposited to a bank or credit union account. Or, like Social Security, if you do not have a checking or savings account, the Plan will set up a debit card account for you. The benefits of using electronic payments are numerous for the Plan as well as for Plan participants. Electronic payments eliminate the cost and waste associated with the use of paper, ink, printers and postage; The possibility of lost or stolen checks will be eliminated; Your benefits will be available in your account on time, even if you are out of town, sick or unable to get to the bank; and Your money is safe. 6
7 Combined Earnings Eligibility Reminder For Coverage Beginning July 1, 2014 or After Participants who do not qualify for health coverage under either the AFTRA Health Plan or the SAG-Producers Health Plan may combine their earnings reportable to each Plan in order to meet the dollar earnings requirement for Plan II eligibility (currently $15,100) for coverage beginning July 1, To find out if you qualify, go to click on the Apply for Combined Earnings Eligibility button and follow the instructions on the web. Self-Pay (COBRA) vs. Marketplace Coverage... Which One is Right for You? In today's changing marketplace, every participant needs to understand their health insurance options. At the time earned eligibility terminates, you have 60 days to enroll in the Self-Pay (COBRA) Program. This Program offers you the option of continuing the same coverage you had under the Plan (except life insurance and AD&D benefits). Unfortunately, this option may not be affordable for more than a few months. The Affordable Care Act (ACA) has created an alternative for many members to consider! Some people might even be eligible for assistance in paying their monthly premiums. The Actors Fund s Covered California Helpline (855) is there to help you understand your options, determine if an ACA plan is right for you, and figure out how to move forward. But act quickly. You only have that same 60-day period from when your earned eligibility terminates to make your decision and sign up for an ACA plan. Keep in mind, while The Actors Fund Helpline is focused on providing information on Covered California, they can direct you to resources all across the country. 7
8 SCREEN ACTORS GUILD PRODUCERS PENSION AND HEALTH PLANS PO Box 7830 Burbank, CA Moving??? When you move, you must notify the Pension and Health Plan Office so that you will continue to receive information about your eligibility and benefits. This is especially im - portant now that premium payment coupons are mailed every quarter to your address on file. You can change your address with the Plan Office four different ways: Online at Call the Plan Office File a Change of Address Card Write or FAX a letter to the Plan Office SAG-AFTRA is a separate entity from the Pension and Health Plans and requires a separate notice for change of address. Sign up for web access to all your information at sagph.org PENSION AND HEALTH PLANS DIRECTORY Burbank Plan Office: (818) or (800) Fax: (818) address: psd@sagph.org website: IF YOU NEED:... ASK FOR: Benefit and Eligibility Information... Participant Services Pension Plan Information... Pension Department, Ext Information on Medical Claims... Participant Services Information on Mental Health/Substance Abuse Coverage ValueOptions... (866) Information on Dental Claims Delta Dental Member Services... (800) Directories... (800) Information on Prescription Drugs Express Scripts... (800) Prescription Pre-Authorizations... (800) NEW YORK Plan Office... (212) Madison Ave. #1819, New York, NY
The Trustees are pleased to announce that
 The Newsletter of the Screen Actors Guild Producers Pension and Health Plans Volume XXI, Number 3 Winter 2013 INSIDE TAKE 2 Hospital/Medical Conversion Option Eliminated...2 Prescription Drug Step Therapy
The Newsletter of the Screen Actors Guild Producers Pension and Health Plans Volume XXI, Number 3 Winter 2013 INSIDE TAKE 2 Hospital/Medical Conversion Option Eliminated...2 Prescription Drug Step Therapy
The Board of Trustees is
 The Newsletter of the Screen Actors Guild Producers Pension and Health Plans Volume XVI, Number 2 Summer 2008 INSIDE TAKE 2 Industry Health Network Major Medical Deductible Eliminated... 2 epay Direct...
The Newsletter of the Screen Actors Guild Producers Pension and Health Plans Volume XVI, Number 2 Summer 2008 INSIDE TAKE 2 Industry Health Network Major Medical Deductible Eliminated... 2 epay Direct...
Coverage for: Single Enrollee Plan Type: TRAD/PPO. Important Questions Answers Why This Matters: $2,500/single Network $5,000/single Non-Network
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 STRS OHIO : Basic Plan with Medicare Part B Only Coverage for: Single
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 STRS OHIO : Basic Plan with Medicare Part B Only Coverage for: Single
GUIDE TO MEDICAL AND DENTAL PLANS
 GUIDE TO MEDICAL AND DENTAL PLANS B e n e f i t s e f f e c t i v e J u l y 1, 2 0 1 4 t h r o u g h J u n e 3 0, 2 0 1 5 Choosing your benefits is an important decision. This guide provides you with the
GUIDE TO MEDICAL AND DENTAL PLANS B e n e f i t s e f f e c t i v e J u l y 1, 2 0 1 4 t h r o u g h J u n e 3 0, 2 0 1 5 Choosing your benefits is an important decision. This guide provides you with the
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
Important Questions. Why this Matters: For PPO Providers: $0 Member/$0 Family For Non-PPO Providers: $0 Member/$0 Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-759-5758. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-759-5758. Important
$1,500 Individual/$3,000 Family for participating providers. $3,000 Individual/$6,000. Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
The Harvard Pilgrim Primary Choice HMO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services
 Massachusetts The Harvard Pilgrim Primary Choice HMO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 07/01/2018 06/30/2019 Coverage for: Individual
Massachusetts The Harvard Pilgrim Primary Choice HMO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 07/01/2018 06/30/2019 Coverage for: Individual
Anthem BlueCross BlueShield Eastern Kentucky University Economy Coverage Period: {01/01/ /31/2013} Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. For prescription
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. For prescription
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by calling 1-585-343-0055 ext. 6415. Important Questions Answers
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by calling 1-585-343-0055 ext. 6415. Important Questions Answers
University of Cincinnati Medical Plan Summary and Comparison Non AAUP - Effective January 1- December 31, 2018
 Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
Coverage Period: Beginning on or after 01/01/2019 Coverage for: Individual or Family Plan Type: EPO
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
Aetna Open Access Health Network Only HMO 2 (Not available in CA, CT or NY)
 Aetna Open Access Health Network Only HMO 2 (Not available in CA, CT or NY) Health Network Only HMO 2 MEDICAL PLAN ENROLLMENT CODE ANH2 Estimated Metal Level Gold Carrier Network Aetna Health Network Only
Aetna Open Access Health Network Only HMO 2 (Not available in CA, CT or NY) Health Network Only HMO 2 MEDICAL PLAN ENROLLMENT CODE ANH2 Estimated Metal Level Gold Carrier Network Aetna Health Network Only
SCHEDULE OF BENEFITS
 SCHEDULE OF BENEFITS To receive the highest level of benefits at the lowest Out-of-Pocket Maximum expense, Covered Services must be provided by PPO Network Providers. When you use other Providers who are
SCHEDULE OF BENEFITS To receive the highest level of benefits at the lowest Out-of-Pocket Maximum expense, Covered Services must be provided by PPO Network Providers. When you use other Providers who are
SPD Prescription Drugs Plan
 Prescription Drugs Plan 08/01/2017 3-1 Your Prescription Drug Benefits The prescription drug benefit available to you is based on the medical plan in which you are enrolled. Regardless of the benefit design
Prescription Drugs Plan 08/01/2017 3-1 Your Prescription Drug Benefits The prescription drug benefit available to you is based on the medical plan in which you are enrolled. Regardless of the benefit design
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
NATIONAL HEALTH & WELFARE FUND PLAN C
 H E A LT H A N N U I T Y I O N P E N S I O N V A C AT NATIONAL HEALTH & WELFARE FUND PLAN C BENEFITS AT A GLANCE Introduction The IATSE National Health & Welfare Fund was set up to provide health care
H E A LT H A N N U I T Y I O N P E N S I O N V A C AT NATIONAL HEALTH & WELFARE FUND PLAN C BENEFITS AT A GLANCE Introduction The IATSE National Health & Welfare Fund was set up to provide health care
Summary of Benefits. Albemarle Select KeyCare PPO
 Summary of Benefits Albemarle Select KeyCare PPO Effective October 1, 2018-December 31, 2019 Anthem KeyCare 25 PPO - Albemarle Select plan 10/01/18-12/31/19 In-Network Services Preventive Care Services
Summary of Benefits Albemarle Select KeyCare PPO Effective October 1, 2018-December 31, 2019 Anthem KeyCare 25 PPO - Albemarle Select plan 10/01/18-12/31/19 In-Network Services Preventive Care Services
Tier 1: $0/$0 Tier 2: $500/$1,500 Tier 3:$1,000/$3,000 Does not apply to preventive care. What is the overall deductible?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by contacting benefits@northside.com or by calling 1-404-851-8393.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by contacting benefits@northside.com or by calling 1-404-851-8393.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-603-7982. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-603-7982. Important Questions
Quote Effective: 04/01/ /30/2019 Version Updated: 01/07/2019
 Quote Effective: 04/01/2019-06/30/2019 Version Updated: 01/07/2019 Print Package: HIOS ID (Enrollment Code) 78124NY1000265-00 (SON5) Plan Name: Rating Region: Rate Rochester For the Benefits described
Quote Effective: 04/01/2019-06/30/2019 Version Updated: 01/07/2019 Print Package: HIOS ID (Enrollment Code) 78124NY1000265-00 (SON5) Plan Name: Rating Region: Rate Rochester For the Benefits described
State of Florida Health Investor HMO Plan Coverage Period: 1/1/ /31/2014
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Family Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Family Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you
Anthem BlueCross BlueShield Christian Care Communities Blue Access PPO Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Annual Notice of Changes for 2019
 VIVA MEDICARE Me (HMO) offered by VIVA HEALTH, Inc. Annual Notice of Changes for 2019 You are currently enrolled as a member of VIVA MEDICARE Me. Next year, there will be some changes to the plan s costs
VIVA MEDICARE Me (HMO) offered by VIVA HEALTH, Inc. Annual Notice of Changes for 2019 You are currently enrolled as a member of VIVA MEDICARE Me. Next year, there will be some changes to the plan s costs
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-421-1880. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-421-1880. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.arcsvs.com or by calling 1-877-309-2955. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.arcsvs.com or by calling 1-877-309-2955. Important Questions
Upper Arlington City School District: Lumenos Health Savings Accounts Coverage Period: 01/01/ /31/2016
 Upper Arlington City School District: Lumenos Health Savings Accounts Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
Upper Arlington City School District: Lumenos Health Savings Accounts Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
PHARMACY BENEFIT MEMBER BOOKLET
 PHARMACY BENEFIT MEMBER BOOKLET Printed on: VALUE, QUALITY AND CONFIDENCE Costco Health Solutions Customer Care HOURS: 24 Hours a Day 7 Days a Week (877) 908-6024 (toll-free) TTY 711 MAILING ADDRESS: Costco
PHARMACY BENEFIT MEMBER BOOKLET Printed on: VALUE, QUALITY AND CONFIDENCE Costco Health Solutions Customer Care HOURS: 24 Hours a Day 7 Days a Week (877) 908-6024 (toll-free) TTY 711 MAILING ADDRESS: Costco
WEA Select Medical Plans
 WEA Select Medical Plans Summary of benefits and rates 11.1.2015 10.31.2016 Note: This summary of benefits and rates is intended to assist you in decision making. Details of covered benefits, limitations,
WEA Select Medical Plans Summary of benefits and rates 11.1.2015 10.31.2016 Note: This summary of benefits and rates is intended to assist you in decision making. Details of covered benefits, limitations,
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling 1-800-542-9402.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling 1-800-542-9402.
Live it 2019 Aetna Federal Plans
 Live it 2019 Aetna Federal Plans The health plan that gets you 19.02.319.1-FED E (9/18) aetnafeds.com From the comfort of your home. Getting in touch is easier than ever. Whether it s a health plan question
Live it 2019 Aetna Federal Plans The health plan that gets you 19.02.319.1-FED E (9/18) aetnafeds.com From the comfort of your home. Getting in touch is easier than ever. Whether it s a health plan question
Annual Notice of Changes for 2017
 Providence Medicare Align Group Plan + RX (HMO) offered by Providence Health Plans Annual Notice of Changes for 2017 You are currently enrolled as a member of Providence Medicare Align Group Plan + RX
Providence Medicare Align Group Plan + RX (HMO) offered by Providence Health Plans Annual Notice of Changes for 2017 You are currently enrolled as a member of Providence Medicare Align Group Plan + RX
Retiree Medical and Life Insurance
 Retiree Medical and Life Insurance Eligibility Full-time employees are eligible for retiree medical and life insurance based on their date of employment: o Before July 1, 2004. You are eligible for retiree
Retiree Medical and Life Insurance Eligibility Full-time employees are eligible for retiree medical and life insurance based on their date of employment: o Before July 1, 2004. You are eligible for retiree
Aetna Open Access Managed Choice POS 3
 Aetna Open Access Managed Choice POS 3 Managed Choice POS 3 MEDICAL PLAN ENROLLMENT CODE AMPS3 Estimated Metal Level Gold Carrier Network Managed Choice POS In-Network Out-of-Network Calendar Year Deductible
Aetna Open Access Managed Choice POS 3 Managed Choice POS 3 MEDICAL PLAN ENROLLMENT CODE AMPS3 Estimated Metal Level Gold Carrier Network Managed Choice POS In-Network Out-of-Network Calendar Year Deductible
Medical Plan Summary: PPO Core Plan
 Medical Plan Summary: PPO Core Plan Healthcare is one of the most important and necessary parts of your benefit package. The following is a summary of our benefit plan. For a more detailed explanation
Medical Plan Summary: PPO Core Plan Healthcare is one of the most important and necessary parts of your benefit package. The following is a summary of our benefit plan. For a more detailed explanation
Annual Notice of Changes for 2017
 Providence Medicare Flex Group Plan + RX (HMO-POS) offered by Providence Health Plans Annual Notice of Changes for 2017 You are currently enrolled as a member of Providence Medicare Flex Group Plan + RX
Providence Medicare Flex Group Plan + RX (HMO-POS) offered by Providence Health Plans Annual Notice of Changes for 2017 You are currently enrolled as a member of Providence Medicare Flex Group Plan + RX
ARUP Laboratories, Inc. EPO Medical 750 Plan Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/aruplabs/ or by calling 1-888-271-5870.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/aruplabs/ or by calling 1-888-271-5870.
2015 Retiree Benefits Open Enrollment Highlights NOVEMBER 5-19, 2014
 2015 Retiree Benefits Open Enrollment Highlights NOVEMBER 5-19, 2014 Table of Contents About Open Enrollment 2015... 3 Summary of Changes for 2015... 3 New Prescription Drug Provider Beginning January
2015 Retiree Benefits Open Enrollment Highlights NOVEMBER 5-19, 2014 Table of Contents About Open Enrollment 2015... 3 Summary of Changes for 2015... 3 New Prescription Drug Provider Beginning January
This chart summaries the coverage under the Standard Health Savings Account (HSA) Option using the Open Access Plus (OAP) network.
 STANDARD HSA OPTION 2017 OPTIONS AT A GLANCE (DEDUCTIBLE 3000/6000) USING THE OPEN ACCESS PLUS (OAP) NETWORK This chart summaries the coverage under the Standard Health Savings Account (HSA) Option using
STANDARD HSA OPTION 2017 OPTIONS AT A GLANCE (DEDUCTIBLE 3000/6000) USING THE OPEN ACCESS PLUS (OAP) NETWORK This chart summaries the coverage under the Standard Health Savings Account (HSA) Option using
Aetna Open Access Managed Choice POS HDHP 2
 Aetna Open Access Managed Choice POS HDHP 2 Managed Choice POS HDHP 2 MEDICAL PLAN ENROLLMENT CODE AMHD2 Estimated Metal Level Silver Carrier Network Managed Choice POS In-Network Out-of-Network Calendar-Year
Aetna Open Access Managed Choice POS HDHP 2 Managed Choice POS HDHP 2 MEDICAL PLAN ENROLLMENT CODE AMHD2 Estimated Metal Level Silver Carrier Network Managed Choice POS In-Network Out-of-Network Calendar-Year
Group Health Options, Inc.
 FEDERAL EMPLOYEES RATES & BENEFITS Group Health Options, Inc. 2016 Federal Plans Compare your plan options Choose the plan that fits you and your family Why choose Group Health Options, Inc. The Network
FEDERAL EMPLOYEES RATES & BENEFITS Group Health Options, Inc. 2016 Federal Plans Compare your plan options Choose the plan that fits you and your family Why choose Group Health Options, Inc. The Network
Summary Plan Description Accenture Prescription Drug Plan
 Summary Plan Description Accenture Prescription Drug Plan Effective January 1, 2018 Group Number: ACCRXS1 TABLE OF CONTENTS SECTION 1 - WELCOME... 1 SECTION 2 PLAN HIGHLIGHTS... 3 SECTION 3 - ADDITIONAL
Summary Plan Description Accenture Prescription Drug Plan Effective January 1, 2018 Group Number: ACCRXS1 TABLE OF CONTENTS SECTION 1 - WELCOME... 1 SECTION 2 PLAN HIGHLIGHTS... 3 SECTION 3 - ADDITIONAL
NEW CASTLE COUNTY COMPARISON OF PRE-65 RETIREES/PENSIONERS BENEFITS PLAN YEAR 2019
 Deductible Per Calendar Year (Individual/Family) $200 Individual $400 Family (DME, Prosthetics and Hearing Aids only) $200 per Individual $400 per Family $200 per Individual $400 per Family $200 per Individual
Deductible Per Calendar Year (Individual/Family) $200 Individual $400 Family (DME, Prosthetics and Hearing Aids only) $200 per Individual $400 per Family $200 per Individual $400 per Family $200 per Individual
Annual Notice of Changes for 2019
 offered by Bright Health You are currently enrolled as a member of. Next year, there will be some changes to the plan s costs and benefits. This booklet tells about the changes. You have from October 15
offered by Bright Health You are currently enrolled as a member of. Next year, there will be some changes to the plan s costs and benefits. This booklet tells about the changes. You have from October 15
Important Questions Answers Why this Matters:
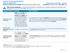 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
Important Questions Answers Why this Matters:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Annual Notice of Changes for 2019
 HealthPartners Journey Stride (PPO) offered by HealthPartners, Inc. (HPI) Annual Notice of Changes for 2019 You are currently enrolled as a member of HealthPartners Journey Stride. Next year, there will
HealthPartners Journey Stride (PPO) offered by HealthPartners, Inc. (HPI) Annual Notice of Changes for 2019 You are currently enrolled as a member of HealthPartners Journey Stride. Next year, there will
University of New Hampshire Student Health Plan: Self-Funded Coverage Period: 8/24/13 8/22/14
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
Annual Notice of Changes for 2018
 SCAN Balance (HMO SNP) offered by SCAN Health Plan Annual Notice of Changes for 2018 You are currently enrolled as a member of SCAN Balance. Next year, there will be some changes to the plan s costs and
SCAN Balance (HMO SNP) offered by SCAN Health Plan Annual Notice of Changes for 2018 You are currently enrolled as a member of SCAN Balance. Next year, there will be some changes to the plan s costs and
$500 Individual/$1,000 Family See the chart starting on page 2 for your costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cvtrust.org or by calling 1-800-288-9870. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cvtrust.org or by calling 1-800-288-9870. Important Questions
California Natural Products: EPO Option Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.deltahealthsystems.com or by calling 1-209-858-2525 Ext
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.deltahealthsystems.com or by calling 1-209-858-2525 Ext
2017 OPTIONS AT A GLANCE (DEDUCTIBLE 2250/4500) USING THE OAP NETWORK
 CHOICE OPTION OAP 2017 OPTIONS AT A GLANCE (DEDUCTIBLE 2250/4500) USING THE OAP NETWORK This chart summarizes the coverage under the Choice Option using the Open Access Plus (OAP) network. At enrollment
CHOICE OPTION OAP 2017 OPTIONS AT A GLANCE (DEDUCTIBLE 2250/4500) USING THE OAP NETWORK This chart summarizes the coverage under the Choice Option using the Open Access Plus (OAP) network. At enrollment
WEA Select Medical Plans
 WEA Select Medical Plans Summary of benefits and rates 11.1.2016 10.31.2017 Note: This summary of benefits and rates is intended to assist you in decision making. Details of covered benefits, limitations,
WEA Select Medical Plans Summary of benefits and rates 11.1.2016 10.31.2017 Note: This summary of benefits and rates is intended to assist you in decision making. Details of covered benefits, limitations,
Important Questions Answers Why this Matters: For PPO Providers: $1,500 Member/$3,000 Family For Non-PPO Providers:
 Anthem Blue Cross Life and Health Insurance Company ACWA / JPIA: Account Based Health Plan (EV85) Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
Anthem Blue Cross Life and Health Insurance Company ACWA / JPIA: Account Based Health Plan (EV85) Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
Important Questions Answers Why this Matters:
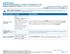 HealthKeepers Anthem HealthKeepers 25 POS / $10/$30/$50 or 20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/01/2014-09/30/2015 Coverage For: Individual/Family
HealthKeepers Anthem HealthKeepers 25 POS / $10/$30/$50 or 20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/01/2014-09/30/2015 Coverage For: Individual/Family
Summary of Benefits. Albemarle Choice HDHP-HSA. (Plan uses KeyCare PPO. providers)
 Summary of Benefits Albemarle Choice HDHP-HSA (Plan uses KeyCare PPO providers) Effective October 1, 2018-December 31, 2019 Lumenos HSA-HDHP 478 Albemarle Choice plan 10/1/18-12/31/19 In-Network Services
Summary of Benefits Albemarle Choice HDHP-HSA (Plan uses KeyCare PPO providers) Effective October 1, 2018-December 31, 2019 Lumenos HSA-HDHP 478 Albemarle Choice plan 10/1/18-12/31/19 In-Network Services
UConn Co-op Plan I: Grandfathered Coverage Period: 1/1/14 12/31/14
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpbenefits.com or by calling 1-800-633-7867. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpbenefits.com or by calling 1-800-633-7867. Important
Medex 3 Plan 2013 Summary of Benefits with 3-Tier Prescription Drug Coverage: $5/$10/$25
 Medex 3 Plan 2013 Summary of Benefits with 3-Tier Prescription Drug Coverage: $5/$10/$25 This Medex plan provides benefits for the: Medicare Part A Deductible and Co-insurances Medicare Part B Deductible
Medex 3 Plan 2013 Summary of Benefits with 3-Tier Prescription Drug Coverage: $5/$10/$25 This Medex plan provides benefits for the: Medicare Part A Deductible and Co-insurances Medicare Part B Deductible
Annual Notice of Changes for 2018
 Health Net Seniority Plus Sapphire Premier (HMO) offered by Health Net Community Solutions, Inc. Annual Notice of Changes for 2018 You are currently enrolled as a member of Health Net Seniority Plus Sapphire
Health Net Seniority Plus Sapphire Premier (HMO) offered by Health Net Community Solutions, Inc. Annual Notice of Changes for 2018 You are currently enrolled as a member of Health Net Seniority Plus Sapphire
Essentials Choice Rx 14 (HMO-POS) offered by PacificSource Medicare
 Essentials Choice Rx 14 (HMO-POS) offered by PacificSource Medicare Annual Notice of Changes for 2018 You are currently enrolled as a member of Essentials Choice Rx 14 (HMO-POS). Next year, there will
Essentials Choice Rx 14 (HMO-POS) offered by PacificSource Medicare Annual Notice of Changes for 2018 You are currently enrolled as a member of Essentials Choice Rx 14 (HMO-POS). Next year, there will
2019 Pre-Medicare Retiree Healthcare Open Enrollment
 2019 Pre-Medicare Retiree Healthcare Open Enrollment CHANGES ONLY ENROLLMENT Submit Enrollment Changes Before November 21 You MUST complete and submit the enclosed enrollment form by November 21 if you
2019 Pre-Medicare Retiree Healthcare Open Enrollment CHANGES ONLY ENROLLMENT Submit Enrollment Changes Before November 21 You MUST complete and submit the enclosed enrollment form by November 21 if you
Coverage Period: Beginning on or after 01/01/2019 Coverage for: Individual or Family Plan Type: EPO
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
Manage your Prescriptions Online Through the Express Scripts Pharmacy
 Manage your Prescriptions Online Through the Express Scripts Pharmacy www.express-scripts.com Customer service specialists are also available 24 hours a day/7 days a week at 1-800-711-0917. Get a 90-day
Manage your Prescriptions Online Through the Express Scripts Pharmacy www.express-scripts.com Customer service specialists are also available 24 hours a day/7 days a week at 1-800-711-0917. Get a 90-day
Annual deductibles and maximums In-network Out-of-network Lifetime maximum
 SUMMARY OF BENEFITS City of Richmond & Richmond Public Schools (Plan B) Connecticut General Life Insurance Co. Annual deductibles and maximums Lifetime maximum Unlimited per individual Pre-Existing Condition
SUMMARY OF BENEFITS City of Richmond & Richmond Public Schools (Plan B) Connecticut General Life Insurance Co. Annual deductibles and maximums Lifetime maximum Unlimited per individual Pre-Existing Condition
You have from October 15 until December 7 to make changes to your Medicare coverage for next year.
 Explorer Rx 7 (PPO) offered by PacificSource Medicare Annual Notice of Changes for 2018 You are currently enrolled as a member of Explorer Rx 7 (PPO). Next year, there will be some changes to the plan
Explorer Rx 7 (PPO) offered by PacificSource Medicare Annual Notice of Changes for 2018 You are currently enrolled as a member of Explorer Rx 7 (PPO). Next year, there will be some changes to the plan
Coverage for: Individual/Family Plan Type: PPO
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
This chart summarizes the coverage under the Health Savings Account 3000/5500 (HSA) Option using the Open Access Plus (OAP) network.
 HSA 3000/5500 2018 Options at a Glance (Deductible 3000/5500) Using the Open Access Plus (OAP) Network This chart summarizes the coverage under the Health Savings Account 3000/5500 (HSA) Option using the
HSA 3000/5500 2018 Options at a Glance (Deductible 3000/5500) Using the Open Access Plus (OAP) Network This chart summarizes the coverage under the Health Savings Account 3000/5500 (HSA) Option using the
Aetna Standard Open Choice PPO 1 (Only available in IN, IL and in other states outside of managed choice
 Aetna Standard Open Choice PPO 1 (Only available in IN, IL and in other states outside of managed choice operational areas) Open Choice PPO 1 MEDICAL PLAN ENROLLMENT CODE ACPPO Estimated Metal Level Platinum
Aetna Standard Open Choice PPO 1 (Only available in IN, IL and in other states outside of managed choice operational areas) Open Choice PPO 1 MEDICAL PLAN ENROLLMENT CODE ACPPO Estimated Metal Level Platinum
Montgomery County Public Schools- PPO Coverage Period: 10/01/ /30/2017
 Montgomery County Public Schools- PPO Coverage Period: 10/01/2016 09/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
Montgomery County Public Schools- PPO Coverage Period: 10/01/2016 09/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cvtrust.org or by calling 1-800-288-9870. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cvtrust.org or by calling 1-800-288-9870. Important Questions
CoventryOne Fusion 100%/50% POS Plans
 CoventryOne Fusion 100%/50% POS Plans $3,000 $5,000 In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member) $6,000,000 $6,000,000 Deductible (per benefit year) - Maximum 3 per family
CoventryOne Fusion 100%/50% POS Plans $3,000 $5,000 In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member) $6,000,000 $6,000,000 Deductible (per benefit year) - Maximum 3 per family
Annual Notice of Changes for 2018
 Health Net Seniority Plus Ruby (HMO) offered by Health Net of California, Inc. Annual Notice of Changes for 2018 You are currently enrolled as a member of Health Net Seniority Plus Ruby. Next year, there
Health Net Seniority Plus Ruby (HMO) offered by Health Net of California, Inc. Annual Notice of Changes for 2018 You are currently enrolled as a member of Health Net Seniority Plus Ruby. Next year, there
Paramount Care, Inc.: LUCAS COUNTY EMPLOYEES Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary*: A quick reference guide to coverage and costs under the Plan. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
This is only a summary*: A quick reference guide to coverage and costs under the Plan. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
Coverage for: Individual/Family Plan Type: PPO
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
Annual Notice of Changes for 2015
 Forever Blue Medicare PPO 751 offered by BlueCross BlueShield of Western New York Annual Notice of Changes for 2015 You are currently enrolled as a member of Forever Blue Medicare PPO 751. Next year, there
Forever Blue Medicare PPO 751 offered by BlueCross BlueShield of Western New York Annual Notice of Changes for 2015 You are currently enrolled as a member of Forever Blue Medicare PPO 751. Next year, there
Anthem Blue Cross University of Southern California Modified Classic Choice HMO 30/40 Coverage Period: 01/01/ /31/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-888-8288. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-888-8288. Important
COSE MEWA : HRA W RX
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at MedMutual.com/SBC or by calling 800.540.2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at MedMutual.com/SBC or by calling 800.540.2583. Important Questions
Important Questions Answers Why this Matters: In-network: $0/Individual; $0/Family Out-of-network: $500/Individual; $1,000/Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling 1-800-445-7490.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling 1-800-445-7490.
Coverage for: Individual/Family Plan Type: PPO
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
UNIVERSITY OF MISSOURI. Benefits Summary for Full-Time Faculty & Staff
 UNIVERSITY OF MISSOURI Benefits Summary for Full-Time Faculty & Staff Effective January 1, 2010 This benefits summary is designed to give you an overview of the major points of UM s various benefits programs.
UNIVERSITY OF MISSOURI Benefits Summary for Full-Time Faculty & Staff Effective January 1, 2010 This benefits summary is designed to give you an overview of the major points of UM s various benefits programs.
Annual Notice of Changes for 2019
 offered by Bright Health You are currently enrolled as a member of Bright Advantage (HMO). Next year, there will be some changes to the plan s costs and benefits. This booklet tells about the changes.
offered by Bright Health You are currently enrolled as a member of Bright Advantage (HMO). Next year, there will be some changes to the plan s costs and benefits. This booklet tells about the changes.
Annual Notice of Changes
 Annual Notice of Changes January 1 December 31, 2018 Generations State of Oklahoma Group Retirees (HMO) GlobalHealth is an HMO plan with a Medicare contract. Enrollment in GlobalHealth depends on contract
Annual Notice of Changes January 1 December 31, 2018 Generations State of Oklahoma Group Retirees (HMO) GlobalHealth is an HMO plan with a Medicare contract. Enrollment in GlobalHealth depends on contract
Harvard Pilgrim s Stride (HMO) Medicare Advantage Plan
 HP19ANOCNHBASIC 2019 Harvard Pilgrim s Stride (HMO) Medicare Advantage Plan Annual Notice of Changes Basic Rx New Hampshire Y0098_19020_M Stride SM Basic Rx (HMO) offered by Harvard Pilgrim Health Care
HP19ANOCNHBASIC 2019 Harvard Pilgrim s Stride (HMO) Medicare Advantage Plan Annual Notice of Changes Basic Rx New Hampshire Y0098_19020_M Stride SM Basic Rx (HMO) offered by Harvard Pilgrim Health Care
Sigma-Aldrich Corporation Healthcare Plans MEDIUM Option Coverage Period: 01/01/ /31/2016 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mysialbenefits.com or by calling 1-877-335-7515, option
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mysialbenefits.com or by calling 1-877-335-7515, option
Important Questions Answers Why This Matters: If took HealthQuotient:
 HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
Marsh and McLennan: Anthem Blue Cross and Blue Shield $900 Deductible Plan Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
$1,500 Individual/$3,000 Family for In-Network providers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-877-244-3593. HRA FUNDING
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-877-244-3593. HRA FUNDING
FloridaBlue BlueCare HMO 3
 FloridaBlue BlueCare HMO 3 HMO 3 MEDICAL PLAN ENROLLMENT CODE FCH3 Estimated Metal Level Gold Carrier Network BlueCare Plan 67 Calendar-Year Deductible (Deductible applies where specifically stated) Person
FloridaBlue BlueCare HMO 3 HMO 3 MEDICAL PLAN ENROLLMENT CODE FCH3 Estimated Metal Level Gold Carrier Network BlueCare Plan 67 Calendar-Year Deductible (Deductible applies where specifically stated) Person
Marsh and McLennan: Anthem Blue Cross and Blue Shield $400 Deductible Plan Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
You must pay all of the costs for these services up to the specific deductible amount before the plan begins to pay for these services.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
HealthTrust: Access Blue 20-RX10/20/45 Coverage Period: 07/01/ /30/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-870-3122. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-870-3122. Important Questions
Coverage Period: 07/01/ /31/2018 Coverage for: Individual, Family Plan Type: EPO
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services New England Health Care Employees Welfare Fund: Wage Class I Coverage Period: 07/01/2018 12/31/2018 Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services New England Health Care Employees Welfare Fund: Wage Class I Coverage Period: 07/01/2018 12/31/2018 Coverage
Retirees with Medicare (RETIREMENT DATE ON or AFTER March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2019
 Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Retirees with Medicare (RETIREMENT DATE BEFORE March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2019
 Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana
Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com/montefiore or by calling 1-866-236-6748
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com/montefiore or by calling 1-866-236-6748
This health plan meets Minimum Creditable Coverage standards and will satisfy the individual mandate that you have health insurance.
 This is a Massachusetts Individual and Small Group Gold Plan. This health plan meets Minimum Creditable Coverage standards and will satisfy the individual mandate that you have health insurance. Massachusetts
This is a Massachusetts Individual and Small Group Gold Plan. This health plan meets Minimum Creditable Coverage standards and will satisfy the individual mandate that you have health insurance. Massachusetts
Important Questions Answers Why this Matters:
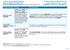 Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
Annual Notice of Changes for 2019
 Annual Notice of Changes for 2019 Anthem MediBlue Plus (HMO) Offered by Anthem Blue Cross Next year, there will be some changes to the plan's costs and benefits. This booklet tells about the changes. 1-888-230-7338,
Annual Notice of Changes for 2019 Anthem MediBlue Plus (HMO) Offered by Anthem Blue Cross Next year, there will be some changes to the plan's costs and benefits. This booklet tells about the changes. 1-888-230-7338,
