Aetna Open Access Managed Choice POS 3
|
|
|
- Rosamond Parker
- 6 years ago
- Views:
Transcription
1 Aetna Open Access Managed Choice POS 3 Managed Choice POS 3 MEDICAL PLAN ENROLLMENT CODE AMPS3 Estimated Metal Level Gold Carrier Network Managed Choice POS In-Network Out-of-Network Calendar Year Deductible Person $1,500 $5,000 Family $4,500 $15,000 Calendar-Year Out-of-Pocket Expense Maximum (Includes deductible, coinsurance and medical/rx copays unless otherwise stated) Person $6,350 $15,000 Family $12,700 $45,000 Preventive Care (Out-of-Network expenses vary by state. Refer to COC.) (Deductible waived for In-Network expenses) Well-woman, Well-baby, Well-man 100% covered Refer to your COC or contact Aetna for further details Physician Office Visit $35/visit Specialist: $50/visit Surgery Outpatient 70% covered AD Hospital Inpatient (Room and Board, Surgery, Anesthesia and Drugs/Supplies) 70% covered AD Emergency Room (Copay waived if admitted) 70% covered AD Urgent Care $75/visit Prenatal Care and Inpatient Prenatal: 100% covered Inpatient: 70% covered AD X-Ray and Lab Outpatient 70% covered AD MRIs (Complex Imaging) Outpatient 70% covered AD Chiropractic** $50/visit Vision Testing Subject to routine physical exam cost sharing Hearing Testing Subject to routine physical exam cost sharing Physical, Occupational and Speech Therapy** (Up to 60 visits/year combined) 70% covered AD Mental Health Inpatient 70% covered AD Mental Health Outpatient $50/visit Substance Abuse Inpatient 70% covered AD Substance Abuse Outpatient $50/visit Ambulance 70% covered AD Home Health Care** 100% AD Durable Medical Equipment Prescription Drugs Prescription drug plan year deductible: $200 individual/$600 family must be met before any drug benefits are paid Retail In-Network (30-day supply if not specified) $20/$40/$70 $20/$40/$70 plus 50% Mail-Order In-Network (90-day supply if not specified; out-of-network not covered) $40/$80/$140 Not covered Specialty Pharmacy (Includes many specialty drugs. Call your carrier for more information.) 25%/$250 max/prescription Not covered This material is general description only. To request a copy of your Certificate of Coverage, please contact TriNet SOI at AD: after deductible. State-mandated differences may apply, please see your SBC for more information. ** Limitations may apply. *Enrollment in this plan includes a $10,000 group life insurance benefit/ad&d coverage for the worksite employee. Benefits are subject to an age-based reduction starting at age 65. Basic life and AD&D policies are not included with COBRA medical plan continuation coverage. 1
2 Prescription Coverage All of the Aetna medical plans in this book include prescription coverage. Most major pharmaceutical chains participate in the Aetna National Network. Additional cost savings may be available if you order your prescriptions through Aetna Rx Home Delivery. What can I expect to pay? The amount you will pay depends on the tier associated with the medication that your doctor prescribes. A tier is a level of coverage. You will either pay a flat fee or a percentage of the total cost of the prescription. The Aetna plans TriNet offers classify medications in one of four tiers: Tier 1: Preferred generic medications You typically pay the lowest cost for medications in this level. Some plans may provide certain Tier 1 medications at an even lower cost to you - these are considered Value Medications/Tier 1a and include generics and some over-the-counter brands. Value Medications/Tier 1a are available at the lowest cost share indicated in your plan materials. Tier 2: Preferred brand name medications You generally pay a slightly higher cost for medications in this level. Tier 3: Non-preferred generics and brand name medications not on the formulary list* You typically pay the highest cost for medications in this level. Tier 4: All specialty medications You generally pay a higher cost for specialty medications in this level. Specialty medications may be injected, infused or taken orally. *A formulary is a list of prescription medications that are covered by a benefit plan. You may access current formulary information for the Aetna plans on aetna.com: 1 Select Individuals & Families > Find a Medication 2 Scroll down to complete a public search and select Yes to indicate that the pharmacy coverage is through an employer 3 Choose 2017 for the plan year, and Value Plans under the plan drop down, then click Continue 4 Refer to the 2017 Four Tier Open Plans You may also call the number on the back of your member ID card or refer to the numbers provided in the Carrier Contact Information. In addition, the following limitations apply to certain prescriptions: Mandatory generic medications Precertification Quantity limits Step therapy Generic medications will be substituted for all prescriptions whenever they are available unless the doctor specifies dispense as written on the prescription (DAW Override). If you prefer the brand-name medication and your doctor does not specify dispense as written on your prescription, you will pay the difference in cost between the generic and brandname medication in addition to the applicable co-payment. Precertification means that you or your doctor need to get approval from Aetna before certain medications will be covered. These limits help your doctor and pharmacist make sure that the medication is used correctly and safely. Aetna uses medical guidelines and FDA-approved recommendations to set the limits. Your doctor can ask for an exception if it is medically necessary to prescribe a higher medication quantity. Some medications require step therapy. This means that you must try one or more other medications before a step therapy medication is covered. The medications required before step therapy medications can be approved, are equally effective, have FDA approval, may cost less and treat the same condition. If you don t try the other medication first, you may need to pay full cost for the step therapy medication. 2 Please refer to the Certificate of Coverage for more information. As soon as administratively possible, Carrier Certificates of Coverage will be posted on trinetsoi.com.
3 Aetna Point of Service (POS) Plan With POS plans, you may choose to obtain care from in-network or out-of-network providers, facilities, or medical equipment suppliers. With POS plans, you can visit an out-of-network physician without a referral, but you will usually pay more for this care due to higher co-insurance and amounts not recognized by the carrier. Managed Choice POS (Open Access) (MCPOS): A PCP is not required in-network but the carrier recommends that you select one for this plan. Referrals for specialists are not necessary but may help you manage your costs. Affordable Care Act All TriNet medical plans meet the Minimum Essential Coverage (MEC) requirements for the Affordable Care Act (ACA) individual mandate. This means that you will not have to pay the individual mandate penalty during any period you and your eligible dependents are enrolled in TriNet medical coverage. Important Information In accordance with the ACA, a Summary of Benefits and Coverage (SBC) has been prepared for your review. SBCs are intended to provide clear, consistent and comparable information about health plans and benefits coverage. The SBCs can be accessed by logging into trinetsoi.com. Visit the Resources tab, click Forms from the menu options, and then select SOI Health Plan SBC Docs folder. You may also request a copy by contacting the TriNet Solution Center at , Monday Friday, 4:30 a.m. 9 p.m. PT. A uniform glossary of health coverage and medical terms is provided by the Department of Labor (DOL) to help you understand the terms used in the SBCs. The uniform glossary is available online at dol.gov/ebsa/pdf/sbcuniformglossary.pdf. The TriNet Benefits Guidebook and Summary Plan Description (SPD) include important information such as the HIPAA Privacy Notice, Medicare Part D Creditable Coverage, the Notice of Mandated Benefits, information about the Children s Health Insurance Program (CHIP) and more. To access the Benefits Guidebook and SPD, visit trinetsoi.com or call the TriNet Solution Center at , Monday Friday, 4:30 a.m. 9 p.m. PT to request a copy. 3 3
4 Carrier Contact Information Carrier Contact Information: For pre-enrollment questions, contact Aetna at with Group Number For post-enrollment questions, contact the number on the back of your ID card. For general questions, contact Aetna at Participating doctors, hospitals, pharmacies, and other providers are listed in Aetna s online directory, DocFind. You can access DocFind by clicking on Find a Doctor at aetna.com. For More Information About TriNet SOI Medical Benefits: Contact the TriNet SOI Solution Center at Please refer to your insurance carrier s Certificate of Coverage and ID Cards for more information. As soon as administratively possible, Carrier Certificates of Coverage will be posted on trinetsoi.com. You will receive an ID card from the carrier approximately two weeks after your initial enrollment has been processed by TriNet. If you need additional card(s) please contact the carrier. Frequently Asked Questions (FAQs) How do I enroll for benefits? You have two options for enrolling for benefits online or by submitting a paper form. If you enroll online, you will only see the plans available to you and the TriNet Online Benefits Enrollment tool will walk you through an easy stepby-step process to make your elections. To enroll online, log in to trinetsoi.com, click Benefits, then Benefits Enrollment. To enroll by paper form, contact the TriNet Solution Center at , Monday Friday, 4:30 a.m. 9 p.m. PT to request a copy of the Benefits Election form. When will deductions for coverage begin? Deductions will begin on the first paycheck of the month in which your coverage begins or, if you are newly eligible for TriNet benefits, the first paycheck after the date your benefit elections are processed. If a benefits election form is submitted after your initial effective date (and prior to the enrollment deadline), your coverage will be set-up retroactively and any missed payments will be deducted from your next paycheck in a lump sum. 4
5 When can I elect to make changes to my coverage? The rules under Section 125 of the Internal Revenue Code require that the benefit elections you make when you are initially eligible or during Open Enrollment be irrevocable and remain in effect until the end of the benefits plan year. Aside from your contributions to an HSA, no changes may be made to any benefit elections during the benefits plan year, regardless whether such benefits are paid on a pre-tax or taxable basis, unless you experience a life status change event. Changes to your benefit elections may be made if the life status change event is reported in a timely manner to TriNet and the benefit changes you request are consistent with the event and are allowed under the TriNet plan and carrier contracts. For more information, refer to the TriNet Benefits Guidebook, or contact the TriNet Solution Center at , Monday-Friday, 4:30 a.m. 9 p.m. PT. How do I know if my dependents are eligible for benefits? Eligible dependents include: Your spouse. Your spouse is your legally married husband or wife, as defined by applicable state law. Your (same-sex or opposite-sex) domestic partner who meets the criteria set forth in the TriNet Declaration of Domestic Partnership form. Your, your spouse s, or your domestic partner s natural child, stepchild, adopted child, child placed for adoption, or child for whom you or your spouse, or domestic partner have been appointed legal guardianship, who is less than age 26 (medical coverage may extend past the age of 26 as mandated by applicable state law); a disabled child (insurance carrier approval required); the child of a dependent (this may include grandchildren and great grandchildren if the dependents coverage is mandated by state law and the coverage is permitted by the applicable insurance carrier), or a child named in a Qualified Medical Child Support Order (QMCSO). If you elect coverage for a dependent with a different last name than yours, TriNet may request additional documentation to verify eligibility. What if I am in an active course of treatment with an out-of-network doctor when I enroll in an Aetna plan? Members who are in an active course of treatment with an out-of-network provider may apply for Aetna s transition of coverage program. To apply, the prospective member and his/her physician must complete a Transition Coverage Request form and submit it to Aetna. The Aetna Transition Coverage Request form can be found on the Aetna website at aetna.com. When will my active TriNet Health Plan coverage end? Active coverage in the TriNet Health Plan will terminate on the date that your active employment or eligibility for the health plan ends (for example, the date you move from full-time to part-time employment). Do I have other options to see a doctor instead of going to the Emergency Room or urgent care for a non-emergency or while I m traveling? Aetna plans offer access to a physician virtually through Teladoc at a much lower copay. Doctors are available 24/7/365 to resolve many non-emergency medical issues through phone or video consults. Contact Teladoc online at or call to request a consult. Is Aetna required to pre-certify any services? Precertification is required for certain services. Please refer to your insurance carrier s Certificate of Coverage for more information. When can I contact the TriNet Solution Center? Contact the TriNet Solution Center for assistance at , Monday Friday, 4:30 a.m. 9 p.m. PT. (Hay representantes de habla hispana disponibles por teléfono.) COBRA Continuation Coverage Rights If you or your covered dependents are no longer eligible for health care coverage through the TriNet Benefits Plan, under certain circumstances you and they may be eligible to continue coverage under the Federal Consolidated Omnibus Budget Reconciliation Act (COBRA) of When you are initially covered under the Plan, TriNet will send a notice that explains COBRA coverage, when it may become available to you and your covered dependents, and what you need to do to protect your right to elect COBRA coverage. For more information about your COBRA rights and obligations under the Plan and under federal law, you should review the TriNet Benefits Guidebook and Summary Plan Description, or contact the TriNet Solution Center at , Monday Friday, 4:30 a.m. 9 p.m. PT. 5
Aetna Open Access Managed Choice POS HDHP 2
 Aetna Open Access Managed Choice POS HDHP 2 Managed Choice POS HDHP 2 MEDICAL PLAN ENROLLMENT CODE AMHD2 Estimated Metal Level Silver Carrier Network Managed Choice POS In-Network Out-of-Network Calendar-Year
Aetna Open Access Managed Choice POS HDHP 2 Managed Choice POS HDHP 2 MEDICAL PLAN ENROLLMENT CODE AMHD2 Estimated Metal Level Silver Carrier Network Managed Choice POS In-Network Out-of-Network Calendar-Year
Aetna Standard Open Choice PPO 1 (Only available in IN, IL and in other states outside of managed choice
 Aetna Standard Open Choice PPO 1 (Only available in IN, IL and in other states outside of managed choice operational areas) Open Choice PPO 1 MEDICAL PLAN ENROLLMENT CODE ACPPO Estimated Metal Level Platinum
Aetna Standard Open Choice PPO 1 (Only available in IN, IL and in other states outside of managed choice operational areas) Open Choice PPO 1 MEDICAL PLAN ENROLLMENT CODE ACPPO Estimated Metal Level Platinum
Aetna Open Access Health Network Only HMO 2 (Not available in CA, CT or NY)
 Aetna Open Access Health Network Only HMO 2 (Not available in CA, CT or NY) Health Network Only HMO 2 MEDICAL PLAN ENROLLMENT CODE ANH2 Estimated Metal Level Gold Carrier Network Aetna Health Network Only
Aetna Open Access Health Network Only HMO 2 (Not available in CA, CT or NY) Health Network Only HMO 2 MEDICAL PLAN ENROLLMENT CODE ANH2 Estimated Metal Level Gold Carrier Network Aetna Health Network Only
FloridaBlue BlueCare HMO 3
 FloridaBlue BlueCare HMO 3 HMO 3 MEDICAL PLAN ENROLLMENT CODE FCH3 Estimated Metal Level Gold Carrier Network BlueCare Plan 67 Calendar-Year Deductible (Deductible applies where specifically stated) Person
FloridaBlue BlueCare HMO 3 HMO 3 MEDICAL PLAN ENROLLMENT CODE FCH3 Estimated Metal Level Gold Carrier Network BlueCare Plan 67 Calendar-Year Deductible (Deductible applies where specifically stated) Person
FloridaBlue BlueOptions PPO 3
 FloridaBlue BlueOptions PPO 3 PPO 3 MEDICAL PLAN ENROLLMENT CODE FBO3 Estimated Metal Level Silver Carrier Network BlueOptions 05901 In-Network Out-of-Network Calendar-Year Deductible (Deductible applies
FloridaBlue BlueOptions PPO 3 PPO 3 MEDICAL PLAN ENROLLMENT CODE FBO3 Estimated Metal Level Silver Carrier Network BlueOptions 05901 In-Network Out-of-Network Calendar-Year Deductible (Deductible applies
FloridaBlue BlueOptions HDHP Bronze
 FloridaBlue BlueOptions HDHP Bronze HDHP Bronze MEDICAL PLAN ENROLLMENT CODE FHDB Estimated Metal Level Bronze Carrier Network BlueOptions Plans 05172 & 05173 In-Network Out-of-Network Calendar-Year Deductible
FloridaBlue BlueOptions HDHP Bronze HDHP Bronze MEDICAL PLAN ENROLLMENT CODE FHDB Estimated Metal Level Bronze Carrier Network BlueOptions Plans 05172 & 05173 In-Network Out-of-Network Calendar-Year Deductible
Fort Worth Firefighters Healthcare Trust 2019 Benefits Guide
 Fort Worth Firefighters Healthcare Trust 2019 Benefits Guide What s Inside The Local 440 Benefits Trust provides participants and their eligible dependents a vital program of benefits designed to keep
Fort Worth Firefighters Healthcare Trust 2019 Benefits Guide What s Inside The Local 440 Benefits Trust provides participants and their eligible dependents a vital program of benefits designed to keep
Medical Plan Summary: PPO Core Plan
 Medical Plan Summary: PPO Core Plan Healthcare is one of the most important and necessary parts of your benefit package. The following is a summary of our benefit plan. For a more detailed explanation
Medical Plan Summary: PPO Core Plan Healthcare is one of the most important and necessary parts of your benefit package. The following is a summary of our benefit plan. For a more detailed explanation
$4,800.00/ individual. $9,600.00/family
 Medical Plans Please note, this brochure provides an overview of certain health care plan provisions under the Adobe Systems Incorporated Group Welfare Plan. It is not intended to be a complete description
Medical Plans Please note, this brochure provides an overview of certain health care plan provisions under the Adobe Systems Incorporated Group Welfare Plan. It is not intended to be a complete description
PLAN DESIGN AND BENEFITS - PA POS HSA COMPATIBLE NO-REFERRAL 2.4 ($2,500 Ded) PARTICIPATING PROVIDERS
 PLAN FEATURES Deductible (per plan year) $2,500 Individual NON- $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All
PLAN FEATURES Deductible (per plan year) $2,500 Individual NON- $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All
Coverage for: Individual Plan Type: POS. Important Questions Answers Why this Matters: In network: $0 Out-of -network: $300 Individual; $600 Family
 Doctors Community Hospital BlueChoice Opt-Out Plus OA Coverage Period: 01/01/2016 12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type:
Doctors Community Hospital BlueChoice Opt-Out Plus OA Coverage Period: 01/01/2016 12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type:
For: Choice POS II - Clerical & Technical and Service & Maintenance Employees Choice POS II (Base Rx) Plan
 Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: June 23, 2016 Effective Date: January 1, 2016 Schedule: 2A Booklet Base: 2 For: Choice POS II - Clerical & Technical and Service &
Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: June 23, 2016 Effective Date: January 1, 2016 Schedule: 2A Booklet Base: 2 For: Choice POS II - Clerical & Technical and Service &
2016 Plan HSA $6,000. $6,000 individual/$12,000 family. $6,000 individual/$12,000 family
 Benefit Changes This is an overview of some of the benefit changes for. For complete details about plans, refer to the carrier documents provided to the member upon enrollment. Refer to CBIA's Benefit
Benefit Changes This is an overview of some of the benefit changes for. For complete details about plans, refer to the carrier documents provided to the member upon enrollment. Refer to CBIA's Benefit
Version: 15/02/2017 [ TPID: ] Page 1
![Version: 15/02/2017 [ TPID: ] Page 1 Version: 15/02/2017 [ TPID: ] Page 1](/thumbs/88/117441870.jpg) PLAN FEATURES NETWORK CARE OUT-OF-NETWORK CARE Primary Care Physician Selection Not required Not required Deductible (per calendar year) $1,500 Individual $3,000 Family $3,000 Individual $9,000 Family
PLAN FEATURES NETWORK CARE OUT-OF-NETWORK CARE Primary Care Physician Selection Not required Not required Deductible (per calendar year) $1,500 Individual $3,000 Family $3,000 Individual $9,000 Family
ACTION REQUIRED: 2018 Benefits Open Enrollment
 September 5, 2017 ACTION REQUIRED: 2018 Benefits Open Enrollment In June, MITRE announced that we are consolidating health insurance plans under a single, national administrator: Aetna. This packet includes
September 5, 2017 ACTION REQUIRED: 2018 Benefits Open Enrollment In June, MITRE announced that we are consolidating health insurance plans under a single, national administrator: Aetna. This packet includes
2014 Side-by-side comparison between the Aetna CDHP and the Aetna PPO for Medical Coverage
 2014 Side-by-side comparison between the and the for Medical Coverage Medical Coverage Carrier Aetna Aetna Aetna Aetna Deductible Individual $1,750 $3,250 $750 $2,250 Family $3,500 $6,500 $1,500 $4,500
2014 Side-by-side comparison between the and the for Medical Coverage Medical Coverage Carrier Aetna Aetna Aetna Aetna Deductible Individual $1,750 $3,250 $750 $2,250 Family $3,500 $6,500 $1,500 $4,500
Aetna Select Medical Plan PLAN FEATURES NETWORK OUT-OF-NETWORK. Plan Maximum Out of Pocket Limit excludes precertification penalties.
 Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 25, 2016 Effective Date: January 1, 2016 Schedule: 12D Booklet Base: 12 For: Aetna Select - Security Staff (Outside CT) Electing
Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 25, 2016 Effective Date: January 1, 2016 Schedule: 12D Booklet Base: 12 For: Aetna Select - Security Staff (Outside CT) Electing
PLAN DESIGN AND BENEFITS - IN MANAGED CHOICE POS OPEN ACCESS 90/60/60 $1,000 PREFERRED CARE
 PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
2017 Open Enrollment is October 31 November 18, 2016
 Non-Union Support Staff and Local 2110 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of Non-Union Support Staff or Local 2110, you can take advantage
Non-Union Support Staff and Local 2110 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of Non-Union Support Staff or Local 2110, you can take advantage
Plan changes are in red In-Network 2015 Out-of-Network
 General Information Lifetime Maximum Benefit Unlimited Unlimited Annual Maximum Benefit Unlimited Unlimited Coinsurance Percentage 80.00% 50.00% Precertification Requirements Precertification Penalty Covered
General Information Lifetime Maximum Benefit Unlimited Unlimited Annual Maximum Benefit Unlimited Unlimited Coinsurance Percentage 80.00% 50.00% Precertification Requirements Precertification Penalty Covered
PPO HSA HDHP $2,500 90/50
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $2,500 Individual $5,000 Family $5,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $2,500 Individual $5,000 Family $5,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member
NETWORK CARE Managed Choice POS (Open Access)
 PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Managed Choice POS (Open Access) Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
PLAN FEATURES Network Primary Care Physician Selection Deductible (per calendar year) Managed Choice POS (Open Access) Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
California Small Group MC Aetna Life Insurance Company NETWORK CARE
 PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
University of Cincinnati Medical Plan Summary and Comparison Non AAUP - Effective January 1- December 31, 2018
 Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
TABLE OF CONTENTS. OVERVIEW Using This Summary... 3
 RETIREE SUMMARY OF BENEFITS 2015 2 TABLE OF CONTENTS OVERVIEW Using This Summary... 3 ELIGIBILITY Retiree Eligibility... 4 Dependent Eligibility... 4 Surviving Spouse/Domestic Partner Continuation Coverage...
RETIREE SUMMARY OF BENEFITS 2015 2 TABLE OF CONTENTS OVERVIEW Using This Summary... 3 ELIGIBILITY Retiree Eligibility... 4 Dependent Eligibility... 4 Surviving Spouse/Domestic Partner Continuation Coverage...
Florida Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012
 Florida 2-100 Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN FEATURES PREFERRED PROVIDERS NON-PREFERRED PROVIDERS Deductible (per calendar year) PLAN DESIGN
Florida 2-100 Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN FEATURES PREFERRED PROVIDERS NON-PREFERRED PROVIDERS Deductible (per calendar year) PLAN DESIGN
Health Plan Shopping Guide
 Health Plan Shopping Guide Use this guide to help you choose a health insurance plan through the Massachusetts Health Connector. Step 1: Know which plans you qualify for First, you ll need to know which
Health Plan Shopping Guide Use this guide to help you choose a health insurance plan through the Massachusetts Health Connector. Step 1: Know which plans you qualify for First, you ll need to know which
All covered expenses accumulate separately toward the Network and Out-of-Network Coinsurance Maximum.
 PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Not Applicable Deductible (per calendar year) $250 per member (2-member maximum) Unless otherwise indicated, the
PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Not Applicable Deductible (per calendar year) $250 per member (2-member maximum) Unless otherwise indicated, the
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING NO-REFERRAL 4.4 ($2,000 DED) $2,000 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING 3.4 ($1,500 DED) PARTICIPATING PROVIDERS. $1,500 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
Member Cost Sharing Participating Provider Non-Participating Provider Annual Deductible Individual $250 $750 Family $750 $2,250
 Schedule of Benefits UPMC Business Advantage PPO - Premium Network Deductible: $250 / $750 Coinsurance: 0% Total Annual Out-of-Pocket: $6,350 / $12,700 Primary Care Provider: $20 Copayment per visit Specialist:
Schedule of Benefits UPMC Business Advantage PPO - Premium Network Deductible: $250 / $750 Coinsurance: 0% Total Annual Out-of-Pocket: $6,350 / $12,700 Primary Care Provider: $20 Copayment per visit Specialist:
All covered expenses accumulate separately toward the Network and Out-of-Network Coinsurance Maximum.
 PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Deductible (per calendar year) Not Applicable $500 per member Not Applicable $500 per member (2-member maximum) (2-member
PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Deductible (per calendar year) Not Applicable $500 per member Not Applicable $500 per member (2-member maximum) (2-member
NETWORK CARE. $4,500 (2-member maximum)
 PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Not Applicable Deductible (per calendar year) $4,500 (2-member maximum) Unless otherwise indicated, the Deductible
PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Not Applicable Deductible (per calendar year) $4,500 (2-member maximum) Unless otherwise indicated, the Deductible
NETWORK CARE. $250 per member (2-member maximum)
 PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Not Applicable Deductible (per calendar year) $250 per member (2-member maximum) Unless otherwise indicated, the
PLAN FEATURES Network Managed Choice POS (Open Access) Primary Care Physician Selection Not Applicable Deductible (per calendar year) $250 per member (2-member maximum) Unless otherwise indicated, the
Florida Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012
 Florida 2-100 Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOption Plan 12-2000-70 PLAN FEATURES PARTICIPATING PROVIDERS
Florida 2-100 Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOption Plan 12-2000-70 PLAN FEATURES PARTICIPATING PROVIDERS
PLAN DESIGN AND BENEFITS MC Open Access Plan 1913
 PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year) $1,500 Individual $4,500 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior
PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year) $1,500 Individual $4,500 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior
Emergency Department: $175 Copayment per visit Coinsurance: 0%
 Schedule of Benefits UPMC Small Business Advantage Primary Care Provider: $25 Copayment per visit Gold PPO $1,000 $25/$50 - Premium Network Specialist: $50 Copayment per visit Deductible: $1,000 / $2,000
Schedule of Benefits UPMC Small Business Advantage Primary Care Provider: $25 Copayment per visit Gold PPO $1,000 $25/$50 - Premium Network Specialist: $50 Copayment per visit Deductible: $1,000 / $2,000
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
COMPASS ROSE HEALTH PLAN PROTECTING OUR MEMBERS SINCE 1948
 PLAN YEAR 2018 COMPASS ROSE HEALTH PLAN PROTECTING OUR MEMBERS SINCE 1948 POWERED BY compassrosebenefits.com 1 WELCOME WE ARE HERE TO HELP YOU SOLVE THE COMPLEXITIES OF INSURANCE PLAN HIGHLIGHTS COMPASS
PLAN YEAR 2018 COMPASS ROSE HEALTH PLAN PROTECTING OUR MEMBERS SINCE 1948 POWERED BY compassrosebenefits.com 1 WELCOME WE ARE HERE TO HELP YOU SOLVE THE COMPLEXITIES OF INSURANCE PLAN HIGHLIGHTS COMPASS
Yes, written or oral approval is required, based upon medical policies.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhc.com/calpers or by calling 1-877-359-3714. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhc.com/calpers or by calling 1-877-359-3714. Important
Annual Notice of Changes for 2018
 HMO Basic No Rx (Medicare Advantage HMO) offered by Tufts Health Plan Medicare Preferred Annual Notice of Changes for 2018 You are currently enrolled as a member of Tufts Medicare Preferred HMO Basic No
HMO Basic No Rx (Medicare Advantage HMO) offered by Tufts Health Plan Medicare Preferred Annual Notice of Changes for 2018 You are currently enrolled as a member of Tufts Medicare Preferred HMO Basic No
Medical Plans. Aetna Medical Plans. Medical Plan Options
 Medical Plans Please note: This brochure provides an overview of certain health care plan provisions under the Adobe Systems Incorporated Group Welfare Plan. It is not intended to be a complete description
Medical Plans Please note: This brochure provides an overview of certain health care plan provisions under the Adobe Systems Incorporated Group Welfare Plan. It is not intended to be a complete description
2018 Retiree Medical Premiums and Coverage Summary MAP Plus - Option 1 Low Deductible
 MAP Plus - Option 1 Low Deductible You and your SP of Record/DP of Record both are Pre-Medicare Eligible Retiree + + $462.00 $923.00 $923.00 $1,385.00 You are Medicare Eligible and your SP of Record/ DP
MAP Plus - Option 1 Low Deductible You and your SP of Record/DP of Record both are Pre-Medicare Eligible Retiree + + $462.00 $923.00 $923.00 $1,385.00 You are Medicare Eligible and your SP of Record/ DP
Essentials Choice Rx 14 (HMO-POS) offered by PacificSource Medicare
 Essentials Choice Rx 14 (HMO-POS) offered by PacificSource Medicare Annual Notice of Changes for 2018 You are currently enrolled as a member of Essentials Choice Rx 14 (HMO-POS). Next year, there will
Essentials Choice Rx 14 (HMO-POS) offered by PacificSource Medicare Annual Notice of Changes for 2018 You are currently enrolled as a member of Essentials Choice Rx 14 (HMO-POS). Next year, there will
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Gwinnett County Board Of Commissioners
 BENEFIT PLAN Prepared Exclusively for Gwinnett County Board Of Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POSII and HSA Table of Contents Schedule of Benefits (SOB) Issued
BENEFIT PLAN Prepared Exclusively for Gwinnett County Board Of Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POSII and HSA Table of Contents Schedule of Benefits (SOB) Issued
ElevateHealth Gold 1000 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services
 New Hampshire ElevateHealth Gold 1000 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018 12/31/2018 Coverage for: Individual + Family
New Hampshire ElevateHealth Gold 1000 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018 12/31/2018 Coverage for: Individual + Family
Florida Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012. PLAN DESIGN AND BENEFITS MC OA Plan A-50
 Florida 2-100 Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS MC OA Plan 12-3000A-50 PLAN FEATURES PREFERRED PROVIDERS NON-PREFERRED PROVIDERS
Florida 2-100 Open Access Managed Choice Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS MC OA Plan 12-3000A-50 PLAN FEATURES PREFERRED PROVIDERS NON-PREFERRED PROVIDERS
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
Important Questions Answers Why this Matters:
 Glatfelter: Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single+2Party+Family Plan Type: PPO This is only a summary. If you
Glatfelter: Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single+2Party+Family Plan Type: PPO This is only a summary. If you
Frequently Asked Questions
 Frequently Asked Questions Q. What is an Open Delivery System? A. An Open Delivery System provides access to a host of affiliated providers with admitting privileges at various HAP-contracted hospitals
Frequently Asked Questions Q. What is an Open Delivery System? A. An Open Delivery System provides access to a host of affiliated providers with admitting privileges at various HAP-contracted hospitals
NATIONAL HEALTH & WELFARE FUND PLAN C
 H E A LT H A N N U I T Y I O N P E N S I O N V A C AT NATIONAL HEALTH & WELFARE FUND PLAN C BENEFITS AT A GLANCE Introduction The IATSE National Health & Welfare Fund was set up to provide health care
H E A LT H A N N U I T Y I O N P E N S I O N V A C AT NATIONAL HEALTH & WELFARE FUND PLAN C BENEFITS AT A GLANCE Introduction The IATSE National Health & Welfare Fund was set up to provide health care
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/ /31/2018
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Pennsylvania Turnpike Commission: Highmark PPO Blue Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Pennsylvania Turnpike Commission: Highmark PPO Blue Coverage for: Individual/Family
NETWORK CARE. $4,500 Individual. (2-member maximum)
 PLAN FEATURES Network Open Choice PPO Primary Care Physician Selection Deductible (per calendar year) Not Applicable $750 per member Not Applicable $750 per member (2-member maximum) (2-member maximum)
PLAN FEATURES Network Open Choice PPO Primary Care Physician Selection Deductible (per calendar year) Not Applicable $750 per member Not Applicable $750 per member (2-member maximum) (2-member maximum)
Aetna Savings Plus Plan Guide
 Aetna Savings Plus Plan Guide For businesses with 2-50 eligible employees in the Chicagoland area Aetna Avenue Your Destination for Small Business Solutions Health Insurance plans are offered and/or underwritten
Aetna Savings Plus Plan Guide For businesses with 2-50 eligible employees in the Chicagoland area Aetna Avenue Your Destination for Small Business Solutions Health Insurance plans are offered and/or underwritten
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: Beginning on or after 1/1/2019
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: Beginning on or after 1/1/2019 Kalamazoo College, G-1013: Orange Plan Coverage for: Covered
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: Beginning on or after 1/1/2019 Kalamazoo College, G-1013: Orange Plan Coverage for: Covered
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 Anthem HealthKeepers Premier POS: Henrico County General Government and Public Schools Coverage Period: 1/1/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
Anthem HealthKeepers Premier POS: Henrico County General Government and Public Schools Coverage Period: 1/1/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
Aetna 1-50 HMO DC 01/01/2018
 HMO DC 01/01/2018 Plan Name DC Gold HMO 70% DC Gold HMO 500 90% DC Gold HMO 1600 100% HSA T DC Silver HMO 3000 100% HSA E DC Silver HMO 4500 80% DC Bronze HMO 5000 80% HSA E In Network In Network In Network
HMO DC 01/01/2018 Plan Name DC Gold HMO 70% DC Gold HMO 500 90% DC Gold HMO 1600 100% HSA T DC Silver HMO 3000 100% HSA E DC Silver HMO 4500 80% DC Bronze HMO 5000 80% HSA E In Network In Network In Network
Schedule of Benefits. Plan Information. Member Cost Sharing
 Schedule of Benefits Panther Gold Plan - Enhanced Access HMO Applies to Bradford, Johnstown and Greensburg campuses only HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600
Schedule of Benefits Panther Gold Plan - Enhanced Access HMO Applies to Bradford, Johnstown and Greensburg campuses only HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600
Schedule of Benefits (GR-29N OK)
 Schedule of Benefits (GR-29N 01-01 01 OK) Employer: Group Policy Number: HS-Real Estate, Inc. dba Hal Smith Restaurant Group GP-493042 Issue Date: April 28, 2017 Effective Date: March 1, 2017 Schedule:
Schedule of Benefits (GR-29N 01-01 01 OK) Employer: Group Policy Number: HS-Real Estate, Inc. dba Hal Smith Restaurant Group GP-493042 Issue Date: April 28, 2017 Effective Date: March 1, 2017 Schedule:
University of Cincinnati Medical Plan Summary and Comparison Effective January 1- December 31, 2018-AAUP only
 Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/2018 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/2018
Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/2018 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/2018
Other Participating UPMC Facilities Level 2 Benefit Period
 Schedule of Benefits Advantage Panther Gold Plan - Enhanced Access HMO Applies to Oakland and Titusville campuses HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600 Primary
Schedule of Benefits Advantage Panther Gold Plan - Enhanced Access HMO Applies to Oakland and Titusville campuses HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600 Primary
Adventist Health System Schedule of Benefits for Adventist Health System Effective January 1, 2018
 Adventist Health System Schedule of Benefits for Adventist Health System Effective January 1, 2018 High Health Plan with Health Savings Account (Health Savings Plan) TIER 1 TIER 2 TIER 3 CALENDAR YEAR
Adventist Health System Schedule of Benefits for Adventist Health System Effective January 1, 2018 High Health Plan with Health Savings Account (Health Savings Plan) TIER 1 TIER 2 TIER 3 CALENDAR YEAR
2019 Summary of Benefits Medicare Advantage Plans with Part D Prescription Drug Coverage
 2019 Summary of Benefits Medicare Advantage Plans with Part D Prescription Drug Coverage Plus H1035-002 H1035-006 H1035-014 January 1, 2019 December 31, 2019 The plan's service area includes: Flagler and
2019 Summary of Benefits Medicare Advantage Plans with Part D Prescription Drug Coverage Plus H1035-002 H1035-006 H1035-014 January 1, 2019 December 31, 2019 The plan's service area includes: Flagler and
What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/cuhealthplan or by calling 1-800-735-6072.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/cuhealthplan or by calling 1-800-735-6072.
2018 Summary of Benefits. BlueCross Secure SM (HMO)
 2018 Summary of Benefits BlueCross Secure SM (HMO) Jan. 1, 2018 Dec. 31, 2018 855-204-2744 TTY 711 Seven Days a Week, 8 a.m. to 8 p.m. (Oct. 1, 2017, to Feb. 14, 2018) Monday-Friday, 8 a.m. to 8 p.m. (All
2018 Summary of Benefits BlueCross Secure SM (HMO) Jan. 1, 2018 Dec. 31, 2018 855-204-2744 TTY 711 Seven Days a Week, 8 a.m. to 8 p.m. (Oct. 1, 2017, to Feb. 14, 2018) Monday-Friday, 8 a.m. to 8 p.m. (All
Maine's Choice HSA HMO 5000 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services
 Maine Maine's Choice HSA HMO 5000 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018 12/31/2018 Coverage for: Individual + Family Plan
Maine Maine's Choice HSA HMO 5000 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018 12/31/2018 Coverage for: Individual + Family Plan
$0 individual/$0 family network. $250 individual/$500 family out-ofnetwork.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Shield: PPO Coverage for: Individual/Family Plan Type: PPO
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Shield: PPO Coverage for: Individual/Family Plan Type: PPO
Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 09/01/2018 08/31/2019 Aetna: Select Open Access Coverage for: Individual, Parent/Child, Employee/Spouse,
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 09/01/2018 08/31/2019 Aetna: Select Open Access Coverage for: Individual, Parent/Child, Employee/Spouse,
2019 FAQs Medical plan. Frequently Asked Questions from employees
 2019 FAQs Medical plan Frequently Asked Questions from employees September 2018 Medical plan benefits Here are some commonly asked questions about the Medical Plan Benefits that our employees have raised.
2019 FAQs Medical plan Frequently Asked Questions from employees September 2018 Medical plan benefits Here are some commonly asked questions about the Medical Plan Benefits that our employees have raised.
Aetna HealthNetworkOnlyOpenAccess Aetna Whole Health-Baptist Health and St. Vincent's Healthcare 1/1/2018
 Plan Name FL Bapt/STV HNOnly Copay 25/50 (0118) FL Bapt/STV HNOnly 2000 100% (0118) FL Bapt/STV HNOnly 3000 100% (0118) FL Bapt/STV HNOnly 4000 100% (0118) FL Bapt/STV HNOnly 5000 100% (0118) Deductible
Plan Name FL Bapt/STV HNOnly Copay 25/50 (0118) FL Bapt/STV HNOnly 2000 100% (0118) FL Bapt/STV HNOnly 3000 100% (0118) FL Bapt/STV HNOnly 4000 100% (0118) FL Bapt/STV HNOnly 5000 100% (0118) Deductible
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
Important Questions Answers Why this Matters:
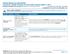 Anthem BlueCross BlueShield Lumenos Health Savings Account (with copays) Option 1 Rx 9 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/01/2014-09/30/2015 Coverage
Anthem BlueCross BlueShield Lumenos Health Savings Account (with copays) Option 1 Rx 9 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/01/2014-09/30/2015 Coverage
CA HMO Deductible $1,500 70%
 Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
A Quick Look at Your Health Plan
 A Quick Look at Your Health Plan Memorial Community Hospital Group #14693 When you enroll with Meritain Health, you re taking the next step towards a healthier, more balanced you. It s important for you
A Quick Look at Your Health Plan Memorial Community Hospital Group #14693 When you enroll with Meritain Health, you re taking the next step towards a healthier, more balanced you. It s important for you
East Hartford BOE (Administrators) 2014 High Deductible Health Plan Information Meeting L O C K T O N C O M P A N I E S
 East Hartford BOE (Administrators) 2014 High Deductible Health Plan Information Meeting L O C K T O N C O M P A N I E S 2014 Health & Welfare Benefits July 1, 2014 there will be no change to our current
East Hartford BOE (Administrators) 2014 High Deductible Health Plan Information Meeting L O C K T O N C O M P A N I E S 2014 Health & Welfare Benefits July 1, 2014 there will be no change to our current
Deductible Per Calendar Year In-network Out-of-network
 PSGBS.ID.SG.MED.HMO.0119 F3927435 Medical Benefit Summary BrightIdea Gold 1000 Provider Network: BrightPath Deductible Per Calendar Year In-network Out-of-network Individual/Family $1,000/$2,000 $10,000/$20,000
PSGBS.ID.SG.MED.HMO.0119 F3927435 Medical Benefit Summary BrightIdea Gold 1000 Provider Network: BrightPath Deductible Per Calendar Year In-network Out-of-network Individual/Family $1,000/$2,000 $10,000/$20,000
2017 Open Enrollment is October 31 November 18, 2016
 TWU 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of TWU, you can take advantage of a comprehensive benefits package. Now is the time to review your
TWU 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of TWU, you can take advantage of a comprehensive benefits package. Now is the time to review your
Anthem BlueCross BlueShield Christian Care Communities Blue Access PPO Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Annual Notice of Changes for 2017
 Providence Medicare Align Group Plan + RX (HMO) offered by Providence Health Plans Annual Notice of Changes for 2017 You are currently enrolled as a member of Providence Medicare Align Group Plan + RX
Providence Medicare Align Group Plan + RX (HMO) offered by Providence Health Plans Annual Notice of Changes for 2017 You are currently enrolled as a member of Providence Medicare Align Group Plan + RX
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.soundhealthwellness.com or by calling 1-800-225-7620.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.soundhealthwellness.com or by calling 1-800-225-7620.
Choice Plus 750 Plan
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Service Choice Plus 750 Plan Coverage Period: 01/01/2018 12/31/2018 Coverage for: Family Plan Type: PS1 The Summary of
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Service Choice Plus 750 Plan Coverage Period: 01/01/2018 12/31/2018 Coverage for: Family Plan Type: PS1 The Summary of
$200 individual/$400 family combined network and out-of-network.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 New Castle County Government : Blue Choice PPO Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 New Castle County Government : Blue Choice PPO Coverage for: Individual/Family
MEDICAL SCHEDULE OF BENEFITS COPAY GOLD
 NON- LIFETIME MAXIMUM BENEFIT Unlimited CALENDAR YEAR MAXIMUM BENEFIT CALENDAR YEAR DEDUCTIBLE Single Family CALENDAR YEAR OUT-OF-POCKET MAXIMUM (includes Deductible, Coinsurance, Copays and Precertification
NON- LIFETIME MAXIMUM BENEFIT Unlimited CALENDAR YEAR MAXIMUM BENEFIT CALENDAR YEAR DEDUCTIBLE Single Family CALENDAR YEAR OUT-OF-POCKET MAXIMUM (includes Deductible, Coinsurance, Copays and Precertification
AvMed In-Network Tier A Providers: $1,500 individual / $3,000 family AvMed In-Network Tier B Providers: What is the overall deductible?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
Schedule of Benefits. Plan Information Participating Provider Non-Participating Provider. Deductible: $250 / $750 Rx: $10/$25/$40/$40 Coinsurance: 0%
 Schedule of Benefits UPMC Business Advantage PPO - Premium Network Primary Care Provider: $20 Copayment per visit Specialist: $20 Copayment per visit Deductible: $250 / $750 Rx: $10/$25/$40/$40 Coinsurance:
Schedule of Benefits UPMC Business Advantage PPO - Premium Network Primary Care Provider: $20 Copayment per visit Specialist: $20 Copayment per visit Deductible: $250 / $750 Rx: $10/$25/$40/$40 Coinsurance:
2015 Benefits Overview
 2015 Benefits Overview ASPIRE HEALTH ADVANTAGE VALUE (HMO) BENEFIT Monthly Plan Premium Out-of-Pocket Limit (In-Network Medicare-covered benefits) Annual Part C Deductible (all services except for Prescription
2015 Benefits Overview ASPIRE HEALTH ADVANTAGE VALUE (HMO) BENEFIT Monthly Plan Premium Out-of-Pocket Limit (In-Network Medicare-covered benefits) Annual Part C Deductible (all services except for Prescription
Paramount Care, Inc.: LUCAS COUNTY EMPLOYEES Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary*: A quick reference guide to coverage and costs under the Plan. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
This is only a summary*: A quick reference guide to coverage and costs under the Plan. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
Coverage Period: 01/01/ /31/2018
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Blue Cross and Blue Shield of North Carolina: Blue Select Gold 2500 Coverage Period: 01/01/2018-12/31/2018 Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Blue Cross and Blue Shield of North Carolina: Blue Select Gold 2500 Coverage Period: 01/01/2018-12/31/2018 Coverage
Blue Cross Blue Shield PPO1 Medical Plan CVS Caremark 10/20/30 Prescription Plan
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
2019 Summary of Benefits
 2019 Summary of MVP Health Plan, Inc. (HMO-POS) (HMO-POS) (HMO-POS) H3305: Plan 030, Plan 015 and Plan 007 This is a summary of drug and health services covered by MVP Health Plan January 1, 2019 - December
2019 Summary of MVP Health Plan, Inc. (HMO-POS) (HMO-POS) (HMO-POS) H3305: Plan 030, Plan 015 and Plan 007 This is a summary of drug and health services covered by MVP Health Plan January 1, 2019 - December
Coverage for: Individual + Family Plan Type: PPO
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 09/01/2018-12/31/2018 Venezia Transport Service: High Plan Coverage for: Individual + Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 09/01/2018-12/31/2018 Venezia Transport Service: High Plan Coverage for: Individual + Family
Aetna 1-50 PPOMedical WA 01/01/2019
 Plan Name WA Gold PPO 500 80/50 WA Gold PPO 1000 80/50 WA Silver PPO 2000 70/50 Deductible (Individual/Family) $500/$1,000 $5,000/$10,000 $1,000/$2,000 $5,000/$10,000 $2,000/$4,000 $8,000/$16,000 Out-of-pocket
Plan Name WA Gold PPO 500 80/50 WA Gold PPO 1000 80/50 WA Silver PPO 2000 70/50 Deductible (Individual/Family) $500/$1,000 $5,000/$10,000 $1,000/$2,000 $5,000/$10,000 $2,000/$4,000 $8,000/$16,000 Out-of-pocket
The Harvard Pilgrim PPO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services
 Massachusetts The Harvard Pilgrim PPO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 12/01/2017 11/30/2018 Coverage for: Individual + Family
Massachusetts The Harvard Pilgrim PPO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 12/01/2017 11/30/2018 Coverage for: Individual + Family
Important Questions Answers Why this Matters:
 Glatfelter: Ohio Union Hourly Employees* Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single + Family Plan Type: PPO This
Glatfelter: Ohio Union Hourly Employees* Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single + Family Plan Type: PPO This
NV Silver Health Network HMO 2000 $30/60. In Network In Network In Network $0/$0 $2,000/$4,000 $5,000/$10,000
 HMO NV Gold Health Network HMO $30/60 NV Silver Health Network HMO 2000 $30/60 NV Silver Health Network HMO 5000 $25/60 In Network In Network In Network Deductible (Individual/Family) Out-of-pocket limit
HMO NV Gold Health Network HMO $30/60 NV Silver Health Network HMO 2000 $30/60 NV Silver Health Network HMO 5000 $25/60 In Network In Network In Network Deductible (Individual/Family) Out-of-pocket limit
2014 BENEFITS HIGHLIGHTS. It s all about choices. And you.
 2014 BENEFITS HIGHLIGHTS It s all about choices. And you. 2 What s new for 2014 Katy ISD s 2014 annual enrollment is almost here. This means it s a good time to begin learning about your options as you
2014 BENEFITS HIGHLIGHTS It s all about choices. And you. 2 What s new for 2014 Katy ISD s 2014 annual enrollment is almost here. This means it s a good time to begin learning about your options as you
Coverage for: Individual + Family Plan Type: NPOS ACC&CPY OV&DED/COIN IP/OP
 SBC0157W091420170939TXHL0004 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: Beginning on or after 10/01/2017 HUMANA HEALTH PLAN OF TX, INC/HUMANA
SBC0157W091420170939TXHL0004 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: Beginning on or after 10/01/2017 HUMANA HEALTH PLAN OF TX, INC/HUMANA
Schedule of Benefits. Plan Information. Primary Care Provider: $10 Copayment per visit
 Schedule of Benefits PPO IA - Premium Network Deductible: $500 / $1,000 Coinsurance: 0% Total Annual Out-of-Pocket: $6,450 / $12,900 Primary Care : $10 Copayment per visit Specialist: $30 Copayment per
Schedule of Benefits PPO IA - Premium Network Deductible: $500 / $1,000 Coinsurance: 0% Total Annual Out-of-Pocket: $6,450 / $12,900 Primary Care : $10 Copayment per visit Specialist: $30 Copayment per
