Third Party Payer & TPA Day. October 18 th, 2018
|
|
|
- Calvin Wright
- 5 years ago
- Views:
Transcription
1 Third Party Payer & TPA Day October 18 th, 2018
2 Mike Dooley Director of Provider Contracting and Engagement Ph: Michael Nour Provider Relations Specialist Ph:
3 Universal Provider Agreement Avera Insurance Division Provider Agreement mailed to over 1,300 professional provider practices (by TIN) across the region in April. Professional provider services only. Participation for both Avera Health Plans and DAKOTACARE in one Universal agreement. Universal fee schedule, except John Morrell Food Group (Smithfield Foods), AHP and State Employee Plan, DAS. 97% returned, executed copies being sent back. Disruption notices as needed to member s, employer groups and distribution channels in November.
4 Credentialing Topics Credentialing carries forward under new agreement. Western Providers, Inc. & credentialing. Credentialing & re-credentialing applies for both insurance plans, reduces admin burden. Credentialing policies / alignment both plans Keep data for primary credentialing contact current with Avera Centralized Verification Services. Provider not credentialed denials. ERA (835) message codes: CARC 251, RARC N570
5 Alignment of Health Services AHP and DKC fully-insured and Avera Health Employee Health Plan alignment of medical policy, preauthorization and experimental / investigational. DAS client decisions pending, expected by 1/1/19 (expected to also align). Comprehensive review similarities / differences. Medical policies have been aligned. Preauthorization lists aligned 1/1/19. Experimental / Investigational lists aligned 1/1/19. State Employee Plan under DAS continues to use HMP. Website re-design early 2019 to create consistent look / feel. Simplifying administrative functions.
6 Alignment of Reimbursement Policy Reimbursement Policy Committee comprised of crossfunctional representation of both AHP / DKC staff. Co-chaired by Mike and Scott. Policies posted online in a uniform format. Web re-design work planned with release early AHP policy on pre-payment review of modifier 59 claims to be retired 1/1/19. Will significantly reduce denials for medical records requests and delays in settlement of claims. Fraud Waste and Abuse efforts will be enhanced, shifting efforts to post-payment review. Core claims system platform investment. RFP process wrapping up now. Target 2021 launch.
7 Imaging Preauthorization Changes Preauthorization of MRI, MRA, CT, PET and Nuclear Studies through evicore, will sunset for AHP fullyinsured and Avera Health Employee Health Benefit Plan members 1/1/19. Pre-service notification-only process will replace evicore preauth for these lines of business. More details on notification process forthcoming. Watch for announcements. John Morrell Food Groups (Smithfield Foods) will retain evicore preauth requirements.
8 Inpatient Notification Change implemented effective 1/1/17 IP stays < 5 days notification only Preauthorization required at beginning of 6 th day Note this does not apply to City of Sioux Falls & Minnehaha County employees
9 2018 Provider Satisfaction Survey Please encourage your providers to participate in our upcoming Provider Satisfaction Survey Look for information in our ProviderView newsletter!
10 Submitted Questions Q: Supplies splints braces how to bill. Wellmark allows POS 12 to be paid what are other payers policies on how to bill for these supplies from POS 11? A: A review of our data for commonly dispensed supplies, splints and braces from a physician office setting shows we receive and pay for them routinely with POS codes 11, 12 and 20. We do not restrict this to POS 12. Q: SL Modifier for VFC (State Supplied) vaccines what payers allow / require this modifier? A: State supplied vaccines must be billed with the SL modifier. A charged amount of zero can be accepted but some offices will bill a dollar, likely because the zero charge isn t allowed with their software. The line and associated charge (if any) will deny as a provider liability. We do allow and pay separately for the vaccine administration. Do not append the SL modifier to the administration fee as that will cause that line to deny.
11 Submitted Questions Q: Why is it that quite a few payers won t pay on the same day services? Ex: (initial psych diagnostic evaluation) and either (subsequent inpatient E/M visit) or (individual therapy session)? A: on the same day as denies the as a National Correct Coding Initiative (NCCI) edit, and is considered a mutually exclusive code pairing on the same day as is also an NCCI edit which results in the denial of the Often referred to as incidental services not separately allowed on the same day or comprehensive / component edits. Demo of the Clear Claim Connection Tool
12 Submitted Questions Q: G0444 Annual depression screening, 15 minutes. Why are so many payers not willing to pay on this code when the patient has been diagnosed with depression? A: G0444 is an annual screening service for depression and billing for this service for a patient that has already been diagnosed with depression would be duplicative and not medically necessary. For patients whom have not already been diagnosed with depression, billing G0444 with nearly any other E/M or mental health services code would be denied as an NCCI edit. When documentation supports that the depression screening is medically necessary and separate from your E/M service, a modifier 25 on the E/M code would be necessary for separate reimbursement. Example follows.
13 Submitted Questions Scenario for G0444 with an E/M and use of Modifier 25 You see a patient who complains of dizziness. You treat the patient for the dizziness and provide a depression screening because of warning signs that arise during your visit. In this case, it may be appropriate to bill for a depression screening plus an E/M service because the patient presented for a reason separate from the depression screening. Be mindful of National Correct Coding Initiative (NCCI) rules, which give G0444 a modifier indicator of 1 with common E/M codes (and others), meaning you can bill both services on the same date of service as long as you show medical necessity and append modifier 25 to the E/M code. That modifier shows that the service is separate from the depression screening. As with any use of modifier 25, your notes must clearly show medical necessity for the additional service your provide. Time must be clearly documented for G0444 in the record.
14 Thank you! Brief Web Portal Walk Through Other Questions?
evicore healthcare Utilization management programs Frequently asked questions
 evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
evicore healthcare Utilization management programs Frequently asked questions Who is evicore? evicore is a specialty medical benefits management company that provides utilization management services for
Unit 14 Radiology Management
 Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Unit 14 Radiology Management In this unit This unit covers the topics listed below: Topic See Page Introduction 14-2 Prior Authorization Overview 14-4 Retrospective Review, Appeal Process 14-7 Highmark
Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona
 Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Doc #: UHC1782m_20120305 Frequently Asked Questions Radiology Prior Authorization Program for the UnitedHealthcare Community Plan, Arizona 1. What is the UnitedHealthcare Radiology Prior Authorization
Frequently Asked Questions Radiology Management Program
 Frequently Asked Questions Radiology Management Program Neighborhood Health Plan of Rhode Island (Neighborhood) has implemented a prior authorization program with MedSolutions. This will include clinical
Frequently Asked Questions Radiology Management Program Neighborhood Health Plan of Rhode Island (Neighborhood) has implemented a prior authorization program with MedSolutions. This will include clinical
Commercial Insurance
 covers medical expenses of individuals and groups Types of benefits and policies vary Group vs. Individual coverage Regulated by individual states 2 1 Fee-for-Service Types of Coverage High-Risk pools
covers medical expenses of individuals and groups Types of benefits and policies vary Group vs. Individual coverage Regulated by individual states 2 1 Fee-for-Service Types of Coverage High-Risk pools
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 11/09/2016 *all red text is new for 11/09/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Hospital Monthly Important Message Updated as of 11/09/2016 *all red text is new for 11/09/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Authorizations & Notifications
 6 Medical Authorizations & Notifications OVERVIEW Health Choice Generations is confident that our Primary Care Physicians are capable of providing the majority of medically necessary services to the patients
6 Medical Authorizations & Notifications OVERVIEW Health Choice Generations is confident that our Primary Care Physicians are capable of providing the majority of medically necessary services to the patients
CAQH CORE Training Session
 CAQH CORE Training Session 2016 Marketbased Adjustments Survey Thursday, December 8, 2016 2:00 3:00 PM ET Logistics Presentation Slides & How to Participate in Today s Session Download a copy of today
CAQH CORE Training Session 2016 Marketbased Adjustments Survey Thursday, December 8, 2016 2:00 3:00 PM ET Logistics Presentation Slides & How to Participate in Today s Session Download a copy of today
PCG and Birth to Three Billing Guidance
 This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
This information summarizes PCG s and Programs role in accepting data, billing and moving claims towards full adjudication. 1 Workable Claims: Commercial Claims: For Dates of Service from July 1, 2017
PROVIDER MANUAL. In the Colorado Access Provider Manual, you will find information about:
 In the Colorado Access Provider Manual, you will find information about: Section 1. Colorado Access General Information Section 2. Colorado Access Policies Section 3. Quality Management Section 4. Provider
In the Colorado Access Provider Manual, you will find information about: Section 1. Colorado Access General Information Section 2. Colorado Access Policies Section 3. Quality Management Section 4. Provider
Prior Authorizations with InterQual Integration
 Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
Prior Authorizations with InterQual Integration Webinar Training 2018 Class Description This class will provide general information regarding the prior authorization process when InterQual integration
CoventryCares of Kentucky Provider Training Program
 CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
CoventryCares of Kentucky Provider Training Program Provider Training Program Agenda About NIA Provider Partnership Program Components Provider Assessment Program How the Program Works: The Authorization
NIA Frequently Asked Questions (FAQ s) For Sunshine State Health Plan Providers
 Question GENERAL Why is Sunshine State Health Plan implementing an outpatient imaging program? NIA Frequently Asked Questions (FAQ s) For Providers Answer To improve quality and manage the utilization
Question GENERAL Why is Sunshine State Health Plan implementing an outpatient imaging program? NIA Frequently Asked Questions (FAQ s) For Providers Answer To improve quality and manage the utilization
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-603-7982. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-603-7982. Important Questions
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 CEBCO: Champaign County Plan 1a Blue Access (PPO) Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
CEBCO: Champaign County Plan 1a Blue Access (PPO) Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 09/14/2016 *all red text is new for 09/14/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Hospital Monthly Important Message Updated as of 09/14/2016 *all red text is new for 09/14/2016 Hospital Modernization - Ambulatory Payment Classification (APC) Hospitals can refer to the Hospital Modernization
Reopening and Redetermination Submissions
 A CMS Medicare Administrative Contractor http://www.ngsmedicare.com Reopening and Redetermination Submissions Understanding your next steps are very important for quick reimbursement and providers are
A CMS Medicare Administrative Contractor http://www.ngsmedicare.com Reopening and Redetermination Submissions Understanding your next steps are very important for quick reimbursement and providers are
: POS HD 3000 Silver Coverage Period: 2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Family Plan Type: POS
 Standard Silver Point-of-Service This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.connecticare.com or
Standard Silver Point-of-Service This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.connecticare.com or
interchange Provider Important Message
 Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
Hospital Monthly Important Message Updated as of 09/13/2017 *all red text is new for 09/13/2017 The following documents were recently updated: CMAP Addendum B The date of the special cycle will be announced
PROVIDER MANUAL. In the Colorado Access Provider Manual, you will find information about:
 In the Colorado Access Provider Manual, you will find information about: Section 1. Colorado Access General Information Section 2. Colorado Access Policies Section 3. Quality Management Section 4. Provider
In the Colorado Access Provider Manual, you will find information about: Section 1. Colorado Access General Information Section 2. Colorado Access Policies Section 3. Quality Management Section 4. Provider
What is the overall deductible? Are there other deductibles for specific services?
 Standard Gold Point-of-Service (POS) : POS HD 1000 Gold Coverage Period: 2014 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy
Standard Gold Point-of-Service (POS) : POS HD 1000 Gold Coverage Period: 2014 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy
$1,000 individual innetwork/$2,000. $1,000 individual out-ofnetwork/$2,000. family innetwork
 Group Health Options, Inc.: Options Basic Plan Coverage Period: 7/1/2012 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Group Conversion Plan Type: POS This
Group Health Options, Inc.: Options Basic Plan Coverage Period: 7/1/2012 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Group Conversion Plan Type: POS This
: POS UPD $6,350 30PCP Coverage Period: 2014
 Standard Basic Point-of-Service (POS) : POS UPD $6,350 30PCP Coverage Period: 2014 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy
Standard Basic Point-of-Service (POS) : POS UPD $6,350 30PCP Coverage Period: 2014 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy
Yes, written or oral approval is required, based upon medical policies.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhc.com/calpers or by calling 1-877-359-3714. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhc.com/calpers or by calling 1-877-359-3714. Important
KanCare All MCO Training FQHC s & RHC s Spring 2018
 KanCare All MCO Training FQHC s & RHC s Spring 2018 Welcome Introductions Welcome, Introductions & Agenda Agenda Encounter Rates Place of Service (POS) Secondary Claims Credentialing Issues How to avoid
KanCare All MCO Training FQHC s & RHC s Spring 2018 Welcome Introductions Welcome, Introductions & Agenda Agenda Encounter Rates Place of Service (POS) Secondary Claims Credentialing Issues How to avoid
Provider Manual. ChoiceBenefits. BayCare Health System Medical Plan
 2019 Provider Manual ChoiceBenefits BayCare Health System Medical Plan 1 Table of Contents BayCare... 2 BayCare Exclusive Network... 2 Rules unique to Cigna BayCare Members... 2 Provider Relations Representative...
2019 Provider Manual ChoiceBenefits BayCare Health System Medical Plan 1 Table of Contents BayCare... 2 BayCare Exclusive Network... 2 Rules unique to Cigna BayCare Members... 2 Provider Relations Representative...
1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs
 1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Rochester Area Employers
1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Rochester Area Employers
Zoom Health Plan, Inc. (ZOOM+): ZOOM+ Bronze Plan Coverage Period: January 1, 2016 December 31, 2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.zoomcare.com or by calling 1-844-ZOOM-777. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.zoomcare.com or by calling 1-844-ZOOM-777. Important
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
Group Health Options, Inc.: Snohomish County (group# ) Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 Group Health Options, Inc.: Snohomish County (group#6432900) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 4/1/2014 to 4/1/2015 Coverage for: Group Plan Type:
Group Health Options, Inc.: Snohomish County (group#6432900) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 4/1/2014 to 4/1/2015 Coverage for: Group Plan Type:
GENERAL BENEFIT INFORMATION
 Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Shield Spectrum PPO Plan 750 Value
 Shield Spectrum PPO Plan 750 Value Benefit Summary (For groups 2 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Life & Health Insurance Company Effective July 1, 2012
Shield Spectrum PPO Plan 750 Value Benefit Summary (For groups 2 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Life & Health Insurance Company Effective July 1, 2012
Important Questions. Why this Matters: For PPO Providers: $0 Member/$0 Family For Non-PPO Providers: $0 Member/$0 Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-759-5758. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-759-5758. Important
New Hampshire Healthy Families Quick Reference Guide for Rendering Providers
 New Hampshire Healthy Families Quick Reference Guide for Rendering Providers December 1, 2013 New Hampshire Healthy Families has selected NIA Magellan 1 to implement a radiology benefit management program
New Hampshire Healthy Families Quick Reference Guide for Rendering Providers December 1, 2013 New Hampshire Healthy Families has selected NIA Magellan 1 to implement a radiology benefit management program
Payment Policy: Code Editing Overview Reference Number: CC.PP.011 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 06/28/2018
 Payment Policy: Code Editing Overview Reference Number: CC.PP.011 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 06/28/2018 Coding Implications Revision Log See Important Reminder at the
Payment Policy: Code Editing Overview Reference Number: CC.PP.011 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 06/28/2018 Coding Implications Revision Log See Important Reminder at the
Important Questions Answers Why this Matters:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: PPO This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: PPO This is only a summary. If you want more detail about your coverage and costs, you
CareCore National Musculoskeletal Management Program Physical Medicine and Therapy Frequently Asked Questions
 EVIDENCE-BASED HEALTHCARE SOLUTIONS CareCore National Physical Medicine and Therapy Prepared for December 2, 2014 Table of Contents Introduction to CareCore National... 3 Who is CareCore National?... 3
EVIDENCE-BASED HEALTHCARE SOLUTIONS CareCore National Physical Medicine and Therapy Prepared for December 2, 2014 Table of Contents Introduction to CareCore National... 3 Who is CareCore National?... 3
Add Title. Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information
 Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
Add Title Michigan Osteopathic Association Meeting 11/3/2017 Professional Provider Billing Tips & Policy Information Topics Timely Filing Limitation Billing Policy Exceptions to Timely Filing Limits Emergency
New Bedford PEC Q&A. For Active Employees or Non-Medicare Eligible Retirees
 New Bedford PEC Q&A For Active Employees or Non-Medicare Eligible Retirees Q: What are the new deductibles for the HMO, POS and PPO plans? A: $250 Individual, $500 for two people and $750 for family Q:
New Bedford PEC Q&A For Active Employees or Non-Medicare Eligible Retirees Q: What are the new deductibles for the HMO, POS and PPO plans? A: $250 Individual, $500 for two people and $750 for family Q:
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.arcsvs.com or by calling 1-877-309-2955. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.arcsvs.com or by calling 1-877-309-2955. Important Questions
City of Springfield Point of Service (POS) Plan HealthLink (Open Access III Network)
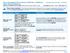 City of Springfield Point of Service (POS) Plan HealthLink (Open Access III Network) Coverage Period: 03/01/2017 02/28/2018 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
City of Springfield Point of Service (POS) Plan HealthLink (Open Access III Network) Coverage Period: 03/01/2017 02/28/2018 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER COVERKIDS TABLE OF CONTENTS
 RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER 1200-13-21 COVERKIDS TABLE OF CONTENTS 1200-13-21-.01 Scope and Authority 1200-13-21-.02 Definitions 1200-13-21-.03
RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER 1200-13-21 COVERKIDS TABLE OF CONTENTS 1200-13-21-.01 Scope and Authority 1200-13-21-.02 Definitions 1200-13-21-.03
Medicare Part A Quarterly Updates. Palmetto GBA JM A/B MAC Provider Outreach & Education September 13, 2017
 Medicare Part A Quarterly Updates Palmetto GBA JM A/B MAC Provider Outreach & Education September 13, 2017 1 Disclaimer This information is current as of August 25, 2017. Any changes or new information
Medicare Part A Quarterly Updates Palmetto GBA JM A/B MAC Provider Outreach & Education September 13, 2017 1 Disclaimer This information is current as of August 25, 2017. Any changes or new information
Anthem BlueCross BlueShield Christian Care Communities Blue Access PPO Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Section Eleven. Referrals and Prior Authorization REFERRAL PROCESS. Physician Referrals within Plan Network
 REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
Prior Authorization/Organization Determination
 Prior Authorization/Organization Determination A Quick Guide on the Importance and Process of Requesting a Prior Authorization/Organization Determination Prior Authorizations Benefits of Using Prior Authorizations
Prior Authorization/Organization Determination A Quick Guide on the Importance and Process of Requesting a Prior Authorization/Organization Determination Prior Authorizations Benefits of Using Prior Authorizations
CareCore National Frequently Asked Questions (FAQ)
 CareCore National Frequently Asked Questions (FAQ) 1. What is changing? Based on the implementation date of your provider notification letter, a limited range of Musculoskeletal Pain, Sleep and Cardiology
CareCore National Frequently Asked Questions (FAQ) 1. What is changing? Based on the implementation date of your provider notification letter, a limited range of Musculoskeletal Pain, Sleep and Cardiology
For non-preferred providers: $14,300 Person/$28,600 Family. Doesn t apply to preventive care services or glasses for children.
 WPS Preferred Plan: Bronze 7150 Coverage Period: 1/1/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: PPO This is only a summary.
WPS Preferred Plan: Bronze 7150 Coverage Period: 1/1/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: PPO This is only a summary.
Webinar Schedule Join us for our next webinar! Are you a newly contracted Provider? Existing Provider who has new staff? Would your office like to lea
 Fall 2018 Provider Newsletter What s New? Provider Services Phone Number 888-243-3312 We are excited to share a change with you! Our dedicated Provider Services telephone number launched on November 1
Fall 2018 Provider Newsletter What s New? Provider Services Phone Number 888-243-3312 We are excited to share a change with you! Our dedicated Provider Services telephone number launched on November 1
Important Questions Answers Why this Matters:
 Blue Shield of CA Life & Health Vital Shield Plus 2900 Generic Rx - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
Blue Shield of CA Life & Health Vital Shield Plus 2900 Generic Rx - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
Louisiana Medicaid. ClaimCheck & Clear Claim Connection Orientation. April 27-29, 2010
 Louisiana Medicaid ClaimCheck & Clear Claim Connection Orientation April 27-29, 2010 1 ClaimCheck & Clear Claim Connection Project Overview Louisiana Medicaid is pleased to announce the implementation
Louisiana Medicaid ClaimCheck & Clear Claim Connection Orientation April 27-29, 2010 1 ClaimCheck & Clear Claim Connection Project Overview Louisiana Medicaid is pleased to announce the implementation
Introduction to the Texas Credentialing Verification Organization
 Introduction to the Texas Credentialing Verification Organization March 1, 2018 Amanda Hudgens Texas Association of Health Plans CVO Vision Simplify the credentialing process by reducing administrative
Introduction to the Texas Credentialing Verification Organization March 1, 2018 Amanda Hudgens Texas Association of Health Plans CVO Vision Simplify the credentialing process by reducing administrative
NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers
 NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers Question GENERAL Why is Home State Health Plan implementing an outpatient imaging program? Answer To improve quality and manage
NIA Frequently Asked Questions (FAQ s) For Home State Health Plan Providers Question GENERAL Why is Home State Health Plan implementing an outpatient imaging program? Answer To improve quality and manage
Important Questions Answers Why this Matters:
 Shield Spectrum PPO Plan 2000 - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: PPO
Shield Spectrum PPO Plan 2000 - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: PPO
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
Paramount Advantage. Facility Orientation
 Paramount Advantage Facility Orientation Overview Paramount Advantage Toledo-based Ohio Managed Care Plan (MCP) Established 1993 Provides health care coverage to Covered Families and Children (CFC) Aged,
Paramount Advantage Facility Orientation Overview Paramount Advantage Toledo-based Ohio Managed Care Plan (MCP) Established 1993 Provides health care coverage to Covered Families and Children (CFC) Aged,
Important Questions Answers Why this Matters:
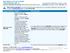 Blue Shield of CA Life & Health Vital Shield Plus 400 - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Blue Shield of CA Life & Health Vital Shield Plus 400 - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Sharing Program Summary of Benefits
 Sharing Program Summary of Benefits Individual and Family Plan Network Only Gold Sharing Program This Sharing Program Summary of Benefits shows the amount eligible for sharing for eligible Medical Needs
Sharing Program Summary of Benefits Individual and Family Plan Network Only Gold Sharing Program This Sharing Program Summary of Benefits shows the amount eligible for sharing for eligible Medical Needs
CHI Health Coverage Period: 01/01/ /31/2017 Employee Assistance Program
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Plan Type: (EAP) This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Plan Type: (EAP) This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in
HealthTrust: LUMENOS $2500 Coverage Period: 07/01/ /30/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4896. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4896. Important Questions
P.L. 2005, CHAPTER 172, approved August 5, 2005 Assembly, No (First Reprint)
 P.L. 00, CHAPTER, approved August, 00 Assembly, No. (First Reprint) - C.:S-. - Note to - 0 0 0 AN ACT concerning managed behavioral health care services and amending and supplementing P.L., c.. BE IT ENACTED
P.L. 00, CHAPTER, approved August, 00 Assembly, No. (First Reprint) - C.:S-. - Note to - 0 0 0 AN ACT concerning managed behavioral health care services and amending and supplementing P.L., c.. BE IT ENACTED
1 Buckeye Community Health Plan. Quick Reference Guide for Rendering Providers November 1, 2014
 Buckeye Community Health Plan Quick Reference Guide for Rendering Providers November 1, 2014 Buckeye Community Health Plan has selected NIA Magellan to implement a radiology benefit management program
Buckeye Community Health Plan Quick Reference Guide for Rendering Providers November 1, 2014 Buckeye Community Health Plan has selected NIA Magellan to implement a radiology benefit management program
Sunshine Health Quick Reference Guide for Rendering Providers
 Sunshine Health Quick Reference Guide for Rendering Providers Effective June 1, 2011 Revised May 2, 2014 Sunshine Health selected NIA Magellan 1 to implement a radiology benefit management program for
Sunshine Health Quick Reference Guide for Rendering Providers Effective June 1, 2011 Revised May 2, 2014 Sunshine Health selected NIA Magellan 1 to implement a radiology benefit management program for
Important Questions Answers Why this Matters:
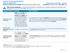 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Ambetter from Sunshine Health Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did Ambetter from implement an outpatient imaging program? Answer To improve quality and manage the utilization of nonemergent
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why did Ambetter from implement an outpatient imaging program? Answer To improve quality and manage the utilization of nonemergent
Introduction to the Texas Credentialing Verification Organization
 Introduction to the Texas Credentialing Verification Organization March 1, 2018 Amanda Hudgens Texas Association of Health Plans CVO Vision Simplify the credentialing process by reducing administrative
Introduction to the Texas Credentialing Verification Organization March 1, 2018 Amanda Hudgens Texas Association of Health Plans CVO Vision Simplify the credentialing process by reducing administrative
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Gateway Health Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging program? Why did Gateway Health select NIA Magellan to manage its
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Providers Question GENERAL Why is Gateway Health implementing an outpatient imaging program? Why did Gateway Health select NIA Magellan to manage its
2019 Summary of Benefits Medicare Advantage Plans with Part D Prescription Drug Coverage
 2019 Summary of Benefits Medicare Advantage Plans with Part D Prescription Drug Coverage Plus H1035-002 H1035-006 H1035-014 January 1, 2019 December 31, 2019 The plan's service area includes: Flagler and
2019 Summary of Benefits Medicare Advantage Plans with Part D Prescription Drug Coverage Plus H1035-002 H1035-006 H1035-014 January 1, 2019 December 31, 2019 The plan's service area includes: Flagler and
BlueCross 0.50, a Multi-State Plan STD
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.capbluecross.com/sbcsia or by calling 1-800-730-7219.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.capbluecross.com/sbcsia or by calling 1-800-730-7219.
Important Questions Answers Why this Matters:
 Blue Shield of CA Balance Plan 2500 - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
Blue Shield of CA Balance Plan 2500 - G Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Working with Anthem Subject Specific Webinar Series Provider Claim Submission and Adjustment Request Tips and Tools Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code:
Over the past several months, HMSA announced its plans to convert to a new
 HMSA s For Participating Providers August 2007 INSIDE Referral exceptions 2 Administrative review 2 Behavioral health services 3 Health center operations 3 Tax reporting: HMO and federal plans 4 Fee schedule
HMSA s For Participating Providers August 2007 INSIDE Referral exceptions 2 Administrative review 2 Behavioral health services 3 Health center operations 3 Tax reporting: HMO and federal plans 4 Fee schedule
Important Questions Answers Why this Matters: For Native American providers: $0 per individual / $0 per family. For participating and nonparticipating
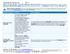 Silver 70 PPO AI-AN Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Silver 70 PPO AI-AN Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
AmeriHealth Caritas District of Columbia. Provider Complaints, Appeals, and Disputes
 AmeriHealth Caritas District of Columbia Provider Complaints, Appeals, and Disputes Updated: May 2015 Complaints Provider Complaint System AmeriHealth Caritas DC providers may file an informal dispute
AmeriHealth Caritas District of Columbia Provider Complaints, Appeals, and Disputes Updated: May 2015 Complaints Provider Complaint System AmeriHealth Caritas DC providers may file an informal dispute
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
Managed Health Services
 Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers
 gat NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers Question GENERAL Why is West Virginia Family Health implementing an outpatient imaging program? Why did West
gat NIA Magellan 1 Frequently Asked Questions (FAQ s) For West Virginia Family Health Providers Question GENERAL Why is West Virginia Family Health implementing an outpatient imaging program? Why did West
National Imaging Associates Inc. (NIA) Frequently Asked Questions (FAQs) for AmeriHealth Caritas Delaware Providers
 National Imaging Associates Inc. (NIA) Frequently Asked Questions (FAQs) for AmeriHealth Caritas Delaware Providers Question GENERAL Why is AmeriHealth Caritas Delaware implementing an outpatient imaging
National Imaging Associates Inc. (NIA) Frequently Asked Questions (FAQs) for AmeriHealth Caritas Delaware Providers Question GENERAL Why is AmeriHealth Caritas Delaware implementing an outpatient imaging
Important Questions Answers Why this Matters:
 HealthKeepers Anthem HealthKeepers 25 POS / $10/$30/$50 or 20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/01/2014-09/30/2015 Coverage For: Individual/Family
HealthKeepers Anthem HealthKeepers 25 POS / $10/$30/$50 or 20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/01/2014-09/30/2015 Coverage For: Individual/Family
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Coventry Health Care of Virginia, Inc. Providers
 NIA Magellan 1 Frequently Asked Questions (FAQ s) For Coventry Health Care of Providers Question GENERAL Why did Coventry Health Care of implementing an outpatient imaging program? Answer To improve quality
NIA Magellan 1 Frequently Asked Questions (FAQ s) For Coventry Health Care of Providers Question GENERAL Why did Coventry Health Care of implementing an outpatient imaging program? Answer To improve quality
Comparison of Benefits
 2018 Comparison of Benefits for Large Groups HMO POS Access POS myhfhp.org (10/10/17) 17HLG-COMPBEN3 Health First Large Group HMO Plans Health First HF13 HMO 6036 Health First HF15 HMO 6040 Out of Pocket
2018 Comparison of Benefits for Large Groups HMO POS Access POS myhfhp.org (10/10/17) 17HLG-COMPBEN3 Health First Large Group HMO Plans Health First HF13 HMO 6036 Health First HF15 HMO 6040 Out of Pocket
For non-participating providers: $11,000 Person/$22,000 Family. Doesn t apply to preventive care. Are there other deductibles for specific services?
 Arise Health Plan: POS HDHP Bronze 5500 Coverage Period: 1/1/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: POS This is only
Arise Health Plan: POS HDHP Bronze 5500 Coverage Period: 1/1/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: POS This is only
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For AmeriHealth Caritas District of Columbia (DC) Providers
 National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For AmeriHealth Caritas District of Columbia (DC) Providers Question GENERAL Why is AmeriHealth Caritas DC implementing an outpatient
National Imaging Associates, Inc. (NIA) Frequently Asked Questions (FAQ s) For AmeriHealth Caritas District of Columbia (DC) Providers Question GENERAL Why is AmeriHealth Caritas DC implementing an outpatient
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers
 Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers Question GENERAL Why is CareSource implementing an outpatient imaging program? Answer To improve quality and manage the
Magellan Healthcare 1 Frequently Asked Questions (FAQ s) For CareSource Providers Question GENERAL Why is CareSource implementing an outpatient imaging program? Answer To improve quality and manage the
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
I. PLAN DESCRIPTIONS. A. POS Point of Service
 I. PLAN DESCRIPTIONS A. POS Point of Service The Partnership Plan offers a single point of service plan to provide healthcare services both within and outside a defined network of Providers. No referrals
I. PLAN DESCRIPTIONS A. POS Point of Service The Partnership Plan offers a single point of service plan to provide healthcare services both within and outside a defined network of Providers. No referrals
Group Health Cooperative: Wa Fire Commissioners Association Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 Group Health Cooperative: Wa Fire Commissioners Association Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 1/1/2015 to 1/1/2016 Coverage for: Group Plan Type:
Group Health Cooperative: Wa Fire Commissioners Association Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 1/1/2015 to 1/1/2016 Coverage for: Group Plan Type:
Important Questions Answers Why this Matters: Network: $500 Individual / $1,000 Family Non-Network: $1,000 Individual / $2,000 Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-262-4772.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-262-4772.
EverydayHealth 5000/100 Alliance Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 EverydayHealth 5000/100 Alliance Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: On and after 10/18/16 Coverage for: Individual Plan Type: PPO This is only a summary.
EverydayHealth 5000/100 Alliance Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: On and after 10/18/16 Coverage for: Individual Plan Type: PPO This is only a summary.
RECONTRACTING 10/31/2016. Aetna Medicare Advantage. Aetna Behavioral Health
 DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
DOING BUSINESS WITH AETNA & COFINIT Y 1 2 RECONTRACTING -Separate agreements. -Separate networks. - Aetna is a Payer, Cofinity is a Network Access Agreement. Aetna Medicare Advantage Employer Based Plan.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.careconnect.com or by calling 1-855-706-7545. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.careconnect.com or by calling 1-855-706-7545. Important
HNE Medicare Value (HMO)
 2016 Medicare Advantage Summary of Benefits January 1, 2016 - December 31, 2016 H8578_2016_453 Accepted HNE MEDICARE ADVANTAGE ENROLLMENT KIT 2016 SECTION I - INTRODUCTION TO SUMMARY OF BENEFITS You have
2016 Medicare Advantage Summary of Benefits January 1, 2016 - December 31, 2016 H8578_2016_453 Accepted HNE MEDICARE ADVANTAGE ENROLLMENT KIT 2016 SECTION I - INTRODUCTION TO SUMMARY OF BENEFITS You have
9/17/2018. Non-covered services. Description: Billing for services not covered under the Medicare program
 Top billing and coding errors: Duplicate claims submitted The claim was previously processed (no payment made, allowed amount applied to deductible on the initial claim). The provider re-files the claim
Top billing and coding errors: Duplicate claims submitted The claim was previously processed (no payment made, allowed amount applied to deductible on the initial claim). The provider re-files the claim
: FlexPOS-CNT D-07 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Family Plan Type: POS
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.connecticare.com or by calling 1-800-251-7722. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.connecticare.com or by calling 1-800-251-7722. Important
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
University of New Hampshire Student Health Plan: Self-Funded Coverage Period: 8/24/13 8/22/14
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
2019 Open Enrollment Chatham County Pre-65 Retirees
 2019 Open Enrollment Chatham County Pre-65 Retirees Welcome to your 2019 Open Enrollment. The pages of this guide will explain your health options. Important points to remember: If you are adding a spouse
2019 Open Enrollment Chatham County Pre-65 Retirees Welcome to your 2019 Open Enrollment. The pages of this guide will explain your health options. Important points to remember: If you are adding a spouse
HUMANA HEALTH PLAN OF OHIO:
 HUMANA HEALTH PLAN OF OHIO: Humana Connect Silver 4600/6300 Plan Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
HUMANA HEALTH PLAN OF OHIO: Humana Connect Silver 4600/6300 Plan Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
NIA Frequently Asked Questions (FAQ s) For Dean Health Plan Providers
 Question GENERAL Why does Dean Health Plan utilize an outpatient imaging program? Why did select National Imaging Associates, Inc. (NIA) to manage its outpatient advanced imaging NIA Frequently Asked Questions
Question GENERAL Why does Dean Health Plan utilize an outpatient imaging program? Why did select National Imaging Associates, Inc. (NIA) to manage its outpatient advanced imaging NIA Frequently Asked Questions
