You should always bill your usual charge to BCBSLA regardless of the allowable charge, for the following reasons:
|
|
|
- Albert Baldwin
- 6 years ago
- Views:
Transcription
1 Reimbursement Allowable Charges BCBSLA reimburses participating providers based on allowable charges. The allowable charge is the lesser of the submitted charge or the amount established by BCBSLA as the maximum amount allowed for provider services covered under the terms of the Subscriber Contract/Certificate. You should always bill your usual charge to BCBSLA regardless of the allowable charge, for the following reasons: It enables us to determine allowable charges for procedures and maintain allowances that are fair and equitable. Billing one standard charge to all insurance companies helps reduce the chance of billing errors. If more than one insurance company has liability for a claim, your standard charge eliminates confusion and helps to ensure proper payment. Allowable charges are provided to participating providers to help avoid refund situations. They are for informational purposes and not intended to establish fees. BCBSLA regularly audits our allowable charge schedule to ensure that the allowable charge amounts are accurate. From time to time we must adjust an allowable charge because it may have been incorrectly loaded into our system or the CPT code description has changed. Allowable charges are added periodically due to new CPT code or updates in code descriptions. If you need the allowable charge for a select code or group of codes, please call Network Administration at , option 3 or September 2002 IV - 1
2 SAMPLE WEEKLY PROVIDER PAYMENT REGISTER S PATIENT S NAME 3 10 DAYS ADMIT DT/ CLAIM TOTAL MD CONTRACT CPT4 PATIENT ABOVE ALLOWABLE AMOUNT STAT SCH PERFORMING C CONTRACT NO PAT ACCT DISCH DT NUMBER CHARGES CD BENEFITS REV LIABILITY AMOUNT PAID CD COB DRG PROVIDER PREVIOUS CREDIT BALANCE Doe John R /21/ S /21/00 ** CPT % ** CPT S ** CPT S ** CPT S ** CPT REJECT RD Doe Suzie Q /06/ , ,665.00CR 4,572.42CR 1, CR 1,665.00CR /17/00 1,65 CPY Doe Suzie Q /06/ , ,663.00AJ 3,526.00AJ 2, AJ 3,663.00AJ /17/00 1,65 CPY Smith Jane X /09/ , , , , S /09/ DED COI ** CPT % ** CPT % ** CPT % ** CPT % ** CPT S Smith John Q /20/ , ,072.17CR 4,697.27CR 5,072.17CR /31/00 1,05 CPY Smith John Q /20/ , ,331.00AJ 7,438.44AJ 2,331.00AJ /31/00 1,05 CPY TOTAL SCB: SCC: 21 BALANCE: $ (AMOUNT PAID) 23 CHECK NO: BLUE CROSS/BLUE SHIELD OF LOUISIANA PAID PROV: SAMPLE MEMBER PROVIDER 22 POST OFFICE BOX DATE: 10/23/ MAIN STREET BATON ROUGE, LA CHECK NO: ANYTOWN, LA / *Note: All charges are examples. September 2002 IV - 2
3 Provider Payment Register Following is a description of each item on the BCBSLA Weekly Provider Payment Register. A copy of the payment register appears on the preceding page. 1. Patient s Name - The last name and first five letters of the first name of the patient. 2. Contract No - The subscriber s Blue Cross and Blue Shield identification number. 3. Pat Acct. - The patient identification number assigned by the provider s office. This information will appear only if provided on the claim. 4. Admit Dt/Disch Dt - The beginning and ending date(s) of service for a claim. 5. Days - The number of visits that the line item charge represents. 6. Claim Number - The number assigned to the claim by BCBSLA for document identification purposes. NOTE: When making inquiries about a specific payment, always refer to this number. 7. Total Charges - The charge for each service and the total claim charges submitted to Blue Cross and Blue Shield. 8. Contract Benefits - The benefit amount payable by Blue Cross and Blue Shield according to the subscriber s contract. 9. CPT -4 Code - The code used to describe the services performed by the provider. 10. Patient Liability - The total amount owed by a patient for each claim including deductible, coinsurance, copayment, non-covered charges, etc. 11. Above Allowable Amount - The amount above the allowable charge. NOTE: This amount cannot be collected from the member. 12. Amount Paid - The amount paid by BCBSLA. 13. Stat CD A one- or two-position alpha code that describes the above allowable (if applicable) followed by a three-position alpha reject code that indicates why a claim was not paid (if applicable). 14. COB - An asterisk in this column denotes that Blue Cross and Blue Shield is the secondary carrier. 15. SCH DRG - Not applicable to providers. 16. Performing Provider - The name and ten-position provider number of the provider who performed the service. September 2002 IV - 3
4 17 Previous Credit Balance - This amount indicates the total of previous overpayments made to the provider. 18 Totals - The total of days, charges, contract benefits, patient liability, above allowable amount, and amount paid for all patients listed. 19. Total SCB - Not applicable to providers. 20. SCC - Not applicable to providers. 21. Balance - The amount adjusted by BCBSLA to recover any overpayments made to the provider. 22. Provider Name - Provider/Clinic name and address to which payment is made. 23. Paid Prov. - Provider s/clinic s BCBSLA provider number under which payment is made. 24 Date - Date the Provider Payment Register is generated by BCBSLA. 25. Check No. - The number assigned to the check mailed with the payment register. September 2002 IV - 4
5 Sample BCBSLA Explanation of Benefits 1 Grp # --- Name --- Address --- City, State, Zip--- EXPLANATION OF BENEFITS 2 THIS IS NOT A BILL Duplicate Copy Date Patient Contract# Group Patient Name Major Medical Network Accumulation Amount Satisfied YTD Deductible Coinsurance 6 Family 7 Provider or Type Services Date of Service 8 9 Amount Charged Not Covered Amount/Reason Deductible 12 Coinsurance Lifetime Benefits Paid for Other Carrier Benefits 13 Basic Benefits 14 Major Medical Benefits 15 Amount Credited 16 Total BENEFITS CREDITED TO PROVIDER COINSURANCE: THE PERCENTAGE OF THE COVERED CHARGES FOR WHICH YOU ARE RESPONSIBLE UNDER THIS CONTRACT. *REASON 19 EXPLANATION OR REASON NOTE: IF YOU HAVE FILED A CLAIM WITH BENEFITS ASSIGNED TO YOU, YOU WILL RECEIVE A SEPARATE EXPLANATION OF BENEFITS. September 2002 IV - 5
6 Explanation of Benefits (EOB) The Explanation of Benefits (EOB) is a notice sent to the subscriber after a claim has been processed by BCBSLA that explains the action taken on that claim. Following is a description of each item on the BCBSLA EOB. A copy of the EOB appears on the preceding page. 1. Subscriber s group number, name and address. 2. Date - The date the EOB was generated by BCBSLA. 3. Patient - Patient s first name. 4. Contract # - Subscriber s identification number. 5. Group - The number assigned to the subscriber s employer, association or organization. 6. The total year-to-date amount that the subscriber has paid toward his/her deductible and the total benefits paid by BCBSLA for this subscriber. 7. Provider or Type Service - The name of the provider who provided services. 8. Dates of Service - Date(s) the service(s) was/were rendered including from and to date(s). 9. Amount Charged - Total charge for each service rendered. 10. Not Covered Amount Reason - The amount of ineligible charges or services. A brief explanation of the reason a charge is not covered will appear in the Explanation of Reason #19. NOTE: The patient is not responsible for payment of any amount above the allowable charge. 11. Deductible - The amount, if any, applied to the subscriber s deductible. The patient is responsible for payment of this amount. 12. Coinsurance - The amount the subscriber is responsible to pay after the deductible has been met. 13. Other Carrier Benefits - The amount paid by another insurance carrier (Coordination of Benefits). 14. Basic Benefits - The total amount of benefits paid under the subscriber s basic health benefits contract. September 2002 IV - 6
7 15. Major Medical Benefits - The total amount of benefits paid under the major medical portion of the subscriber s contract. 16. Amount Credited - The total amount of benefits paid on behalf of a member. 17. Total - The totals of amount charged, not covered amount, deductible, coinsurance, other carrier payment, basic payment, major medical payment and total payment. 18. Benefits to Provider - The total amount of benefits paid. 19. Explanation of Reason - An explanation about a payment or ineligible service or charge. September 2002 IV - 7
8 Sample FEP EOB September 2002 IV - 8
9 Federal Employee Program (FEP) EOB The Federal Employee Program (FEP) is a health care benefits plan designed for personnel employed by the Federal Government. The FEP EOB is a notice sent to the FEP subscriber after a claim has been processed by BCBSLA that explains the action taken on that claim. Following is a description of each item on the FEP EOB. A copy of the FEP EOB appears on the preceding page. 1. Claim Number- The number assigned to the claim by Blue Cross and Blue Shield for document identification purposes. 2. Date the Claim was Received, Processed and Paid by BCBSLA 3. Patient s Name and Patient Account Number (Optional) 4. A Summary of Standard Option and/or Basic Option Benefits on This Claim See Page V Whether or Not the Benefit Check Has Been Enclosed Informs the subscriber if the payment has been sent directly to the provider or has been enclosed with their EOB. 6. Provider Name and Dates of Service Information for the Subscriber 7. Type of Service An abbreviated description of the types of services rendered by the provider. 8. Submitted Charges - The charges submitted by the provider for each service. 9. Negotiated Savings The amount above the allowable charge. 10. Non-covered Charges - A charge (for a non-covered service) for which there is no provision for either partial or total benefit/payment under the Subscriber Contract/Certificate. 11. Allowable Charges - The lesser of the submitted charge or the amount established by the PLAN, based on an analysis of provider charges, as the maximum amount allowed for physician services covered under the terms of the Subscriber Contract/Certificate. 12. Deductible - The specific amount of covered services, usually expressed in dollars, that must be incurred by a subscriber before BCBSLA is obligated to the subscriber to assume financial responsibility for all or part of the remaining covered services under a Subscriber Contract/Certificate. 13. Coinsurance/Co-pay The portion of covered services, usually expressed as a percentage (Coinsurance) or dollar amount (Co-Pay), for which the subscriber is financially responsible under a Subscriber Contract/Certificate. 14. Other Coverage The amount paid by another insurance carrier. 15. Explanation of Codes and Other Remarks A detailed explanation of any CPT codes used in the FEP EOB as well as other information pertinent to the subscriber. September 2002 IV - 9
10 Sample NASCO Provider Check Voucher September 2002 IV - 10
11 NASCO Provider Check Voucher Following is a description of each item on the NASCO (National Accounts Service Company) Provider Check Voucher. NASCO is a national accounts membership and claims processing system used by BCBSLA. A copy of the check voucher appears on the preceding page. 1. Sub. ID - The subscriber s identification number also referred to as contract number. 2. Patient s Name - Patient s last name and first three letters of his/her first name. 3. Patient Account - The account number assigned to the patient by the provider s office. This information will appear only if provided on the claim. 4. Prescription No. - Pharmacy claims only. 5. Claim No. - The number assigned to the claim by Blue Cross and Blue Shield for document purposes. 6. Service Dates From/To - The beginning and ending date(s) of service for a claim. 7. Procedure Code - The CPT procedure code(s) for the service(s) billed. 8. CVD/NCVD - The amount of charges that are covered or non-covered by a subscriber s policy. 9. Total Charges - The charge for each service submitted to Blue Cross and Blue Shield. 10. Allowed Amount - The lesser of the provider s charge or allowable charge on which benefits were based. 11. NCVD CHG - The amount not covered by a subscriber s health benefits contract. This amount is collectible from the subscriber. 12. Subscriber s Liability - The amount owed by a patient for each claim. 13. Co-Pay/Ded. - The total of copayment and/or deductible. This is the amount owed by a patient for each claim. 14. Approved To Pay Amount - The benefit amount payable by Blue Cross and Blue Shield according to the subscriber s contract. 15. Amount Paid - The amount paid by Blue Cross and Blue Shield. 16. A message that provides pertinent information about the claim. September 2002 IV - 11
12 17. Traditional Paid Claim Subtotals - The subtotals of charges, allowed amount, non-covered charges, subscriber liability, copayment/deductible, approved to pay amount and amount paid for all claims listed on the Provider Check Voucher. 18. Total - The total charges, allowed amount, non-covered charges, subscriber liability, copayment/deductible, approved to pay amount and amount paid for all claims listed on the Provider Check Voucher. 19. Provider Number - The number assigned to a provider/clinic for NASCO claims processing purposes. 20. Tax ID - The tax identification number under which claims payments are reported to the Internal Revenue Service for the physician/clinic to whom payment was made. 21. Payment Date - The date the Provider Check Voucher was generated. 22. For Related Inquiries Please Call or Write - The name, address and telephone number to which NASCO claims and inquiries should be directed. 23. Provider s/clinic s name and address September 2002 IV - 12
13 Sample NASCO EOB THIS IS NOT A BILL Explanation of Benefits Payments 1 STATEMENT DATE MON DAY YEAR CHECK REF NO: Contract#: 18 Group#: THIS STATEMENT REPORTS ON A CLAIM(S) WE RECENTLY PROCESSED FOR YOU AND/OR YOUR DEPENDENTS. IF YOU HAVE ANY QUESTIONS PLEASE CALL OR WRITE: BLUE CROSS BLUE SHIELD OF LOUISIANA NASCO DEDICATED UNIT P.O. BOX BATON ROUGE, LA Patient: Provider: Claim: DATES OF SERVICES 11/27/ DESCRIPTION OF SERVICES AMOUNT CHARGED 4,35 ALLOWED AMOUNT 2, OTHER INSURANCE $ 9 YOUR RESPONSIBILITY DEDUCTIBLE COPAY COINSURANCE OTHER AMOUNTS NOT COVERED , AMOUNT PAID 2, RSN CODE 16 R 11/27/ , , R 11/27/ Explanations: R- Service Is Not A Covered Benefit. (E232) 20 PLEASE KEEP YOUR RECORDS. THIS IS A DUPLICATE. BLUE CROSS BLUE SHEILD OF LOUISIANA NASCO DEDICATED UNIT P.O. BOX BATON ROUGE, LA /670 T Subscriber Name Subscriber Address Anytown, LA September 2002 IV - 13
14 NASCO EOB NASCO is a national accounts membership and claims processing system used by BCBSLA. The NASCO EOB is a notice sent to the subscriber after a claim has been processed by BCBSLA that explains the action taken on that claim. 1. Statement Due - Date the EOB was generated. 2. Patient Name - The last and first name of the patient. 3. Provider s Name - The name of the provider who performed the service. 4. Claim Number - The number assigned to the claim by Blue Cross and Blue Shield for document identification purposes. 5. Dates of Service - The beginning and ending date(s) of service for a claim. 6. Description of Services - A written description of the types of services rendered. 7. Amount Charged - The amount charged for each service. 8. Allowed Amount - The benefit amount payable by Blue Cross and Blue Shield. 9. Other Insurance - The amount paid by another insurance carrier. 10. Your Responsibility - The total amount owed by a patient. The deductible, coinsurance and other subscriber liability amounts not covered are itemized. 11. YTD Deductible Amount - The year-to-date amount that has been applied to a subscriber s deductible. 12. YTD Co-pay - The year-to-date aggregate co-pay paid by the subscriber. 13 YTD Coinsurance - The year-to-date aggregate coinsurance paid by the subscriber. 14. Other Amounts Not Covered The difference between the amount charged (Item 7) and the allowed amount (Item 8). This is the amount the participating provider has agreed not to collect from the member. 15. Amount Paid - The amount paid by Blue Cross and Blue Shield. 16. RSN Code - A code that provides pertinent information about a claim. A detailed explanation of the RSN code appears in Item Check Reference Number The number of the check submitted for charges. 18. Contract Number - The subscriber s identification number. 19. Group Number - The number assigned to the subscriber s employer, association or organization. 20. Explanation of Column 16 - A detailed explanation of the code contained in Column Subscriber Name/Address September 2002 IV - 14
WELCOME. Allegiance Benefit Plan Management, Inc S. Garfield St. P.O. Box 3018 Missoula, MT
 WELCOME TO YOUR EMPLOYEE BENEFITS Allegiance Benefit Plan Management, Inc. 2806 S. Garfield St. P.O. Box 3018 Missoula, MT 59806 www.askallegiance.com /preventive TABLE OF CONTENTS Identification Cards
WELCOME TO YOUR EMPLOYEE BENEFITS Allegiance Benefit Plan Management, Inc. 2806 S. Garfield St. P.O. Box 3018 Missoula, MT 59806 www.askallegiance.com /preventive TABLE OF CONTENTS Identification Cards
Coordination of Benefits (COB)
 Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more Plans providing benefits or services for medical treatment.
Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more Plans providing benefits or services for medical treatment.
3. The Health Plan accepts the standard current billing forms: the CMS 1500 (02/12) form and the UB- 04 hospital billing forms.
 BILLING PROCEDURES SECTION 11 Billing Procedures 1. All claims should be submitted to: The Health Plan 1110 Main St Wheeling WV 26003 Claim forms must be completed in their entirety. The efficiency with
BILLING PROCEDURES SECTION 11 Billing Procedures 1. All claims should be submitted to: The Health Plan 1110 Main St Wheeling WV 26003 Claim forms must be completed in their entirety. The efficiency with
Coordination of Benefits (COB)
 Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more plans providing benefits or services for medical treatment.
Coordination of Benefits (COB) COB is intended to avoid claims payment delays and duplication of benefits when a person is covered by two or more plans providing benefits or services for medical treatment.
Arkansas Blue Cross and Blue Shield
 Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Arkansas Blue Cross and Blue Shield November 2005 Inside the November 2005 Issue: Name of Article Page Air and/or Ground Ambulance Claims Filing Procedures 6 Attachments to Claims 8 Bill Types for Facility
Be certain your secondary ClaimLinx ID card matches the below sample. If it does not you will need to read a different member packet.
 Welcome to! We are so happy to have you as a member. Our company specializes in helping businesses change the way they purchase health insurance so they can provide comprehensive benefits at an affordable
Welcome to! We are so happy to have you as a member. Our company specializes in helping businesses change the way they purchase health insurance so they can provide comprehensive benefits at an affordable
Availity Claim Research Tool
 December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
December 2016 Availity Claim Research Tool The Claim Research Tool is the recommended method for providers to acquire status on claims processed by Blue Cross and Blue Shield of Illinois ().* Organizations
Be certain your secondary ClaimLinx ID card matches the below sample. If it does not you will need to read a different member packet.
 ClaimLinx Phone (800) 858-1772 or (513) 677-6262 Fax (800) 858-1913 or (513) 677-6263 help@claimlinx.com Welcome to ClaimLinx! We are so happy to have you as a member. Our company specializes in helping
ClaimLinx Phone (800) 858-1772 or (513) 677-6262 Fax (800) 858-1913 or (513) 677-6263 help@claimlinx.com Welcome to ClaimLinx! We are so happy to have you as a member. Our company specializes in helping
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
CHAPTER 3: MEMBER INFORMATION
 CHAPTER 3: MEMBER INFORMATION UNIT 4: COORDINATION OF BENEFITS IN THIS UNIT TOPIC SEE PAGE 3.4 COORDINATION OF BENEFITS (COB) 2 3.4 COB: TWO AND THREE PAYER CLAIMS Updated! 4 3.4 FREQUENTLY ASKED QUESTIONS
CHAPTER 3: MEMBER INFORMATION UNIT 4: COORDINATION OF BENEFITS IN THIS UNIT TOPIC SEE PAGE 3.4 COORDINATION OF BENEFITS (COB) 2 3.4 COB: TWO AND THREE PAYER CLAIMS Updated! 4 3.4 FREQUENTLY ASKED QUESTIONS
OTHER PARTY LIABILITY PHONE BLUE CROSS AND BLUE SHIELD OF KANSAS TOLL FREE PO BOX 239 FAX TOPEKA, KS
 OTHER PARTY LIABILITY PHONE 785-291-4013 BLUE CROSS AND BLUE SHIELD OF KANSAS TOLL FREE 800-430-1274 PO BOX 239 FAX 785-291-8981 TOPEKA, KS 66601-9913 OTHER PARTY LIABILITY (OPL) is the area within Blue
OTHER PARTY LIABILITY PHONE 785-291-4013 BLUE CROSS AND BLUE SHIELD OF KANSAS TOLL FREE 800-430-1274 PO BOX 239 FAX 785-291-8981 TOPEKA, KS 66601-9913 OTHER PARTY LIABILITY (OPL) is the area within Blue
CHAPTER 9: CLAIM AND BILLING INFORMATION
 CHAPTER 9: CLAIM AND BILLING INFORMATION UNIT 2: THE REMITTANCE ADVICE IN THIS UNIT TOPIC SEE PAGE 9.2 THE REMITTANCE ADVICE 2 9.2 DETAIL REPORT: DATA ELEMENT DESCRIPTIONS 6 9.2 DETAIL REPORT: CLAIM ADJUSTMENT
CHAPTER 9: CLAIM AND BILLING INFORMATION UNIT 2: THE REMITTANCE ADVICE IN THIS UNIT TOPIC SEE PAGE 9.2 THE REMITTANCE ADVICE 2 9.2 DETAIL REPORT: DATA ELEMENT DESCRIPTIONS 6 9.2 DETAIL REPORT: CLAIM ADJUSTMENT
Companion Guide for the X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC
 Companion Guide for the 005010X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Name TR3 Values Notes Delimiter: Data
Companion Guide for the 005010X223A2 Health Care Claim: Institutional (837I) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Name TR3 Values Notes Delimiter: Data
Provider Manual. The BlueCard Program
 The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
The BlueCard Program Provider Manual 23XX4272 R12/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
PROVIDER VOUCHER OTHER INSURANCE
 00435 9875667 000522 0000961 00001/00002 k00425 1351 WILLIAM HOWARD TAFTROAD FOR RELATED INQUIRES PLEASE CALL OR WRITE: ANTHEM BLUE CROSS AND BLUE SHIELD P.O. BOX 105557 ATLANTA, GA 30348 XXX-XXX-XXXX
00435 9875667 000522 0000961 00001/00002 k00425 1351 WILLIAM HOWARD TAFTROAD FOR RELATED INQUIRES PLEASE CALL OR WRITE: ANTHEM BLUE CROSS AND BLUE SHIELD P.O. BOX 105557 ATLANTA, GA 30348 XXX-XXX-XXXX
This Issue: Subsidies and Grace Periods October 2013
 hcrnews provider New Rules, New Challenges, New Opportunities Provider HCR (health care reform) News is a monthly special edition publication for network providers from the Network Administration Division
hcrnews provider New Rules, New Challenges, New Opportunities Provider HCR (health care reform) News is a monthly special edition publication for network providers from the Network Administration Division
NEWS. Welcome to the New ilinkblue! ilinkblue Features. March
 NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
NEWS A special edition newsletter for Blue Cross and Blue Shield of Louisiana network providers. March 2017 Welcome to the New ilinkblue! Blue Cross and Blue Shield of Louisiana s ilinkblue has received
THE REMITTANCE ADVICE
 THE REMITTANCE ADVICE The purpose of this section is to familiarize the provider with the design and content of the Remittance Advice (RA). This document plays an important communication role between the
THE REMITTANCE ADVICE The purpose of this section is to familiarize the provider with the design and content of the Remittance Advice (RA). This document plays an important communication role between the
web-denis resources Getting to web-denis resources Log in to web-denis. You ll need your password. Click BCN Provider Publications and Resources.
 web-denis resources Getting to web-denis resources Log in to web-denis. You ll need your password. Click BCN Provider Publications and Resources. 1 web-denis resources web-denis Behavioral Health page
web-denis resources Getting to web-denis resources Log in to web-denis. You ll need your password. Click BCN Provider Publications and Resources. 1 web-denis resources web-denis Behavioral Health page
Crossover claims should be submitted to Molina Medicaid Solutions, P.O. Box 91020, Baton Rouge, LA
 Dear Provider, Thank you for your participation in the Louisiana Medicaid Program. Payment may be made to your provider type for recipients who also have Medicare coverage. For these recipients, Louisiana
Dear Provider, Thank you for your participation in the Louisiana Medicaid Program. Payment may be made to your provider type for recipients who also have Medicare coverage. For these recipients, Louisiana
Believe in BLUE. Office Manual. Participating Provider
 Participating Provider Office Manual Believe in BLUE 23XX6767 R10/05 Blue Cross and Blue Shield of Louisiana incorporated as Louisiana Health Service & Indemnity Company Table of Contents Table of Contents...
Participating Provider Office Manual Believe in BLUE 23XX6767 R10/05 Blue Cross and Blue Shield of Louisiana incorporated as Louisiana Health Service & Indemnity Company Table of Contents Table of Contents...
Paying for care. KaiSer permanente deductible HMo plan. Learn more about how your deductible plan works at kp.org.
 KaiSer permanente deductible HMo plan Paying for care we re here to help you better understand the financial aspects of your deductible plan. understanding your costs can help you feel more comfortable
KaiSer permanente deductible HMo plan Paying for care we re here to help you better understand the financial aspects of your deductible plan. understanding your costs can help you feel more comfortable
WELCOME. Allegiance Benefit Plan Management, Inc S. Garfield St. P.O. Box 3018 Missoula, MT
 HEALTH BENEFITS WELCOME TO YOUR Allegiance Benefit Plan Management, Inc. 2806 S. Garfield St. P.O. Box 3018 Missoula, MT 59806 www.askallegiance.com/ccg TABLE OF CONTENTS Identification Cards 4 Network
HEALTH BENEFITS WELCOME TO YOUR Allegiance Benefit Plan Management, Inc. 2806 S. Garfield St. P.O. Box 3018 Missoula, MT 59806 www.askallegiance.com/ccg TABLE OF CONTENTS Identification Cards 4 Network
CMS 1500 Claim Filing Instructions. 1 Not Required Type of health insurance coverage applicable to claim. Patient s type of coverage.
 Field Locator Requirements CMS 1500 Claim Filing Instructions Field Description 1 Not Required Type of health insurance coverage to claim Patient s type of coverage. 1a Required Insured s ID Number Identification
Field Locator Requirements CMS 1500 Claim Filing Instructions Field Description 1 Not Required Type of health insurance coverage to claim Patient s type of coverage. 1a Required Insured s ID Number Identification
EXPLANATION OF REMITTANCE ADVICE DETAIL REPORT HEADINGS
 EXPLANATION OF REMITTANCE ADVICE DETAIL REPORT HEADINGS First Line PAT CONTROL NUMBER Patient Control Number PATIENT LNAME Patient Last Name FIRST Patient First name A Accommodation Code 1 SER FROM Service
EXPLANATION OF REMITTANCE ADVICE DETAIL REPORT HEADINGS First Line PAT CONTROL NUMBER Patient Control Number PATIENT LNAME Patient Last Name FIRST Patient First name A Accommodation Code 1 SER FROM Service
Blue Cross OGB-dedicated Customer Service:
 Blue Cross OGB-dedicated Customer Service: 1.800.392.4089 Frequently Asked uestions Blue Cross and Blue Shield of Louisiana administers benefits for the Office of Group Benefits (OGB) for their PPO, HMO
Blue Cross OGB-dedicated Customer Service: 1.800.392.4089 Frequently Asked uestions Blue Cross and Blue Shield of Louisiana administers benefits for the Office of Group Benefits (OGB) for their PPO, HMO
Dental Office Implementation Guide
 Dental Office Implementation Guide 9/29/2017 Identification Card FEP BlueDental Announcement The Blue Cross Blue Shield Association (BCBSA) has partnered with the GRID Dental Corporation (GDC) to administer
Dental Office Implementation Guide 9/29/2017 Identification Card FEP BlueDental Announcement The Blue Cross Blue Shield Association (BCBSA) has partnered with the GRID Dental Corporation (GDC) to administer
WELCOME. Allegiance Benefit Plan Management, Inc S. Garfield St. P.O. Box 3018 Missoula, MT
 HEALTH BENEFITS WELCOME TO YOUR Allegiance Benefit Plan Management, Inc. 2806 S. Garfield St. P.O. Box 3018 Missoula, MT 59806 www.askallegiance.com/dsbcc TABLE OF CONTENTS Identification Cards 3 Network
HEALTH BENEFITS WELCOME TO YOUR Allegiance Benefit Plan Management, Inc. 2806 S. Garfield St. P.O. Box 3018 Missoula, MT 59806 www.askallegiance.com/dsbcc TABLE OF CONTENTS Identification Cards 3 Network
REINSTATEMENT And IMPLEMENTATION Of LAHIPP THIRD PARTY LIABILITY (TPL) CLAIMS PAYMENT
 REINSTATEMENT And IMPLEMENTATION Of LAHIPP THIRD PARTY LIABILITY (TPL) CLAIMS PAYMENT April 7, 2017 LOUISIANA MEDICAID PROGRAM DEPARTMENT OF HEALTH BUREAU OF HEALTH SERVICES FINANCING TABLE OF CONTENTS
REINSTATEMENT And IMPLEMENTATION Of LAHIPP THIRD PARTY LIABILITY (TPL) CLAIMS PAYMENT April 7, 2017 LOUISIANA MEDICAID PROGRAM DEPARTMENT OF HEALTH BUREAU OF HEALTH SERVICES FINANCING TABLE OF CONTENTS
CREATING SECONDARY CLAIMS IN SERVICE CENTER
 CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
CREATING SECONDARY CLAIMS IN SERVICE CENTER Page 1 To find payers who accept secondary claims, go to the Resource Center> Payer List, and look for the indicator Y in the SEC column. This indicates that
Anthem Commercial Remittance Advice Explanation
 Anthem Commercial Remittance Advice Explanation Cover Page Information Provider Name and Address Remittance Date Check Number or Automatic Clearing House (ACH) Deposit trace number o If ACH, ABA and Account
Anthem Commercial Remittance Advice Explanation Cover Page Information Provider Name and Address Remittance Date Check Number or Automatic Clearing House (ACH) Deposit trace number o If ACH, ABA and Account
ancillary claims filing requirements: specialty pharmacy
 ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
ancillary claims filing requirements: specialty pharmacy Presented by: Valesca Weerasinghe, Network Manager Ancillary & Specialty Networks Blue Shield of California September 26, 2012 agenda objectives
Availity ' Eligibility and Benefits SM'
 Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
Updated 12/2012 Availity ' Eligibility and Benefits SM' An eligibility and benefits inquiry should be completed for every patient at every visit to confirm membership, verify coverage and determine other
ASI FUNDING PLANS. What is an ASi Funding Plan?
 ASI FUNDING PLANS What is an ASi Funding Plan? The ASi Funding Plan is a benefit plan that can provide you and your employees with significant savings without diminishing your benefits. With this plan,
ASI FUNDING PLANS What is an ASi Funding Plan? The ASi Funding Plan is a benefit plan that can provide you and your employees with significant savings without diminishing your benefits. With this plan,
FREQUENTLY ASKED QUESTIONS (DESIGNED FOR GOOSE CREEK CONSOLIDATED INDEPENDENT SCHOOL DISTRICT)
 FREQUENTLY ASKED QUESTIONS (DESIGNED FOR GOOSE CREEK CONSOLIDATED INDEPENDENT SCHOOL DISTRICT) What is NexStep? NexStep is underwritten by Fidelity Security Life Insurance Company (Kansas City, Missouri)
FREQUENTLY ASKED QUESTIONS (DESIGNED FOR GOOSE CREEK CONSOLIDATED INDEPENDENT SCHOOL DISTRICT) What is NexStep? NexStep is underwritten by Fidelity Security Life Insurance Company (Kansas City, Missouri)
SutterSelect Administrative Manual. June 2017
 SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
Helpful Tips for Preventing Claim Delays. An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11
 Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
Helpful Tips for Preventing Claim Delays An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 Overview + The Do s of Claim Filing + Blue e + Clear Claim Connection (C3) +
NEUROLOGICAL INSTITUTE OF MICHIGAN PATIENT INFORMATION FORM
 NEUROLOGICAL INSTITUTE OF MICHIGAN PATIENT INFORMATION FORM PATIENT NAME: HOME ADDRESS: BIRTH : SSN#: CELL: HOME TELEPHONE: EMPLOYER: WORK: EMERGENCY CONTACT: REFERRING DOCTOR: PRIMARY CARE MD: PHONE:
NEUROLOGICAL INSTITUTE OF MICHIGAN PATIENT INFORMATION FORM PATIENT NAME: HOME ADDRESS: BIRTH : SSN#: CELL: HOME TELEPHONE: EMPLOYER: WORK: EMERGENCY CONTACT: REFERRING DOCTOR: PRIMARY CARE MD: PHONE:
IOANA A. BINA, M.D. Gastroenterology Tel: (707) Fax: (707)
 IOANA A. BINA, M.D. Gastroenterology Tel: (707) 963-3311 Fax: (707)963-3322 (circle) Today's Date: Best Contact Phone# Cell Home Work PATIENT INFORMATION Name: Soc Sec #: Last Name First Name Initial Address:
IOANA A. BINA, M.D. Gastroenterology Tel: (707) 963-3311 Fax: (707)963-3322 (circle) Today's Date: Best Contact Phone# Cell Home Work PATIENT INFORMATION Name: Soc Sec #: Last Name First Name Initial Address:
PROVIDERTIDBITS. Identification Card Guide. Preferred Care PPO Alpha Prefix: Varies. HMO Louisiana, Inc. Alpha Prefix: Varies TB
 Identification Card Guide Identification (ID) cards are useful tools for both members and providers. They are designed to assist you in identifying the member s type of coverage. Always ask for a copy
Identification Card Guide Identification (ID) cards are useful tools for both members and providers. They are designed to assist you in identifying the member s type of coverage. Always ask for a copy
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM
 HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
HUMBOLDT INDEPENDENT PRACTICE ASSOCIATION CLAIMS SETTLEMENT PRACTICES AND DISPUTE RESOLUTIONS MECHANISM As required by Assembly Bill 1455, the California Department of Managed Health Care has set forth
Transparency Claim Payment Policies & Other Information URL
 Transparency Claim Payment Policies & Other Information URL s a. Out of network liability and balance billing Balance billing occurs when an out-of-network provider bills an enrollee for charges other
Transparency Claim Payment Policies & Other Information URL s a. Out of network liability and balance billing Balance billing occurs when an out-of-network provider bills an enrollee for charges other
Seg Loop Name TR3 Values Notes Delimiter: Data Element. (:) Colon Separator
 Companion Guide for the 005010X223A1 Health Care Claim: Institutional (837I) Lines of Business: Private Business, 65C Plus, QUEST, Blue Card, FEP, Away From Home Care Delimiter: Data Element (*) Asterisk
Companion Guide for the 005010X223A1 Health Care Claim: Institutional (837I) Lines of Business: Private Business, 65C Plus, QUEST, Blue Card, FEP, Away From Home Care Delimiter: Data Element (*) Asterisk
Welcome to the BlueChoice Network
 Welcome to the BlueChoice Network BlueChoice Network Objective The BlueChoice network is composed of hospitals, physicians, health care professionals, and ancillary providers that have contracted with
Welcome to the BlueChoice Network BlueChoice Network Objective The BlueChoice network is composed of hospitals, physicians, health care professionals, and ancillary providers that have contracted with
837 Professional Health Care Claim Outbound. Section 1 837P Professional Health Care Claim: Basic Instructions
 Companion Document 837P 837 Professional Health Care Claim Outbound This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and
Companion Document 837P 837 Professional Health Care Claim Outbound This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and
Credit payment & adjustments off of Member s Account
 PAGE: 1 10/29/2014 PROVIDER REIMBURSEMENT VOUCHER PROVIDER S NAME PROVIDER NO: _ TAX ID: _ CLAIMS PAID *** SECURE CARE *** CHECK NUMBER: 989898 PER PROVIDER LETTER CLAIM IS PAID IN DUPLICATE. 03/24/2014
PAGE: 1 10/29/2014 PROVIDER REIMBURSEMENT VOUCHER PROVIDER S NAME PROVIDER NO: _ TAX ID: _ CLAIMS PAID *** SECURE CARE *** CHECK NUMBER: 989898 PER PROVIDER LETTER CLAIM IS PAID IN DUPLICATE. 03/24/2014
Availity TM Eligibility and Benefits Inquiry
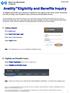 October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
October 2016 Availity TM Eligibility and Benefits Inquiry An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient
Dental Network Office Manual
 July 2008 Provider Network News 3 Dental Network Office Manual Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana
July 2008 Provider Network News 3 Dental Network Office Manual Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana
Filing Secondary Claims on Provider Express
 Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
Filing Secondary Claims on Provider Express October 2013 Agenda Introductions Overview of accessing the long form Overview of filing secondary (COB) claims on Provider Express Overview of other long form
PLEASE PRINT AND COMPLETE ALL ENTRIES
 Patient Name: (Last, First, MI) E mail Address: PLEASE PRINT AND COMPLETE ALL ENTRIES Your Date of Birth: / / Male Female Marital Status: S M Minor D W Your Social Security No: Address: Street Home Phone:
Patient Name: (Last, First, MI) E mail Address: PLEASE PRINT AND COMPLETE ALL ENTRIES Your Date of Birth: / / Male Female Marital Status: S M Minor D W Your Social Security No: Address: Street Home Phone:
Pfizer encompass Co-Pay Assistance Program for INFLECTRA :
 Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Pfizer encompass Co-Pay Assistance Program for INFLECTRA : Guide to Claim Submission and Payment INFLECTRA is a trademark of Hospira UK, a Pfizer company. Pfizer encompass is a trademark of Pfizer. Table
Health Information Technology and Management
 Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
Working with Anthem Subject Specific Webinar Series
 Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
Working with Anthem Subject Specific Webinar Series BlueCard Program Introduction Access to Audio Portion of Conference: Dial-In Number: 877-497-8913 Conference Code: 1322819809# Please Mute Your Phone
COORDINATION OF BENEFITS. 33 rd Annual Open Season Seminar
 COORDINATION OF BENEFITS 33 rd Annual Open Season Seminar Definition of COB COB (Coordination of Benefits): The process by which a health insurance company determines if it should be the primary or secondary
COORDINATION OF BENEFITS 33 rd Annual Open Season Seminar Definition of COB COB (Coordination of Benefits): The process by which a health insurance company determines if it should be the primary or secondary
HCFA Mapping to BCBSNC Local Proprietary Format (LPF) and the HIPAA 837-Professional Implementation Guide
 HCFA Mapping to BCBSNC Local Proprietary at (LPF) n/a Header and Trailer - Header & Footers information will be in the ISA/IEA, GS/GE & THE ST/SE HDR 1-3 TRL1-3 1 Leave blank n/a n/a 1a Insured s ID Enter
HCFA Mapping to BCBSNC Local Proprietary at (LPF) n/a Header and Trailer - Header & Footers information will be in the ISA/IEA, GS/GE & THE ST/SE HDR 1-3 TRL1-3 1 Leave blank n/a n/a 1a Insured s ID Enter
Other Coverage Questionnaire
 PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
PO Box 94059 Seattle, WA 98111 Other Coverage Questionnaire In order to pay your claims in a timely manner, we need information about other health plan coverage you may have even if you have none. Please
Southern Healthcare Agency Field Employees Summary of Benefits Blue Cross Blue Shield of MS
 Southern Healthcare Agency Field Employees Summary of Benefits Blue Cross Blue Shield of MS Dual Option #1 Plan: Network Blue Deductible: $5000 Coinsurance: 70% Network/50% Non-Network Out of Pocket: $6450
Southern Healthcare Agency Field Employees Summary of Benefits Blue Cross Blue Shield of MS Dual Option #1 Plan: Network Blue Deductible: $5000 Coinsurance: 70% Network/50% Non-Network Out of Pocket: $6450
The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
 Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
Ancillary Claims Filing Requirements Frequently Asked Questions The following questions were received in response to our provider webinars presented by Blue Shield of California s network management teams.
Over the past several months, HMSA announced its plans to convert to a new
 HMSA s For Participating Providers August 2007 INSIDE Referral exceptions 2 Administrative review 2 Behavioral health services 3 Health center operations 3 Tax reporting: HMO and federal plans 4 Fee schedule
HMSA s For Participating Providers August 2007 INSIDE Referral exceptions 2 Administrative review 2 Behavioral health services 3 Health center operations 3 Tax reporting: HMO and federal plans 4 Fee schedule
CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM
 CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM The California Department of Managed Health Care has set forth regulations establishing certain claim settlement practices and a process for resolving
CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM The California Department of Managed Health Care has set forth regulations establishing certain claim settlement practices and a process for resolving
The PT Patient s Guide to Understanding Insurance
 The PT Patient s Guide to Understanding Insurance Insurance 101 for PT Patients So, your insurance covers physical therapy which means you won t have to pay anything out-of-pocket for your therapy visits,
The PT Patient s Guide to Understanding Insurance Insurance 101 for PT Patients So, your insurance covers physical therapy which means you won t have to pay anything out-of-pocket for your therapy visits,
Physical Therapy. Contact your Primary Access Administrator (PAA) if Eligibility and Benefits is not listed in the navigation menu.
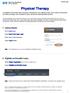 October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
October 2016 Physical Therapy An eligibility and benefits inquiry should be completed for every patient at each visit to confirm membership and verify coverage, such as patient s copay, coinsurance and
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2011-2012 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year 2011-2012 Summary of
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN 2011-2012 Call APS Healthcare Toll-Free: 1-877-239-1458 Website: www.apshelplink.com Company Code: SOM2002 Year 2011-2012 Summary of
837 Institutional Health Care Claim. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
PAGE OF CREATION DATE TOTALS
 1 2 3a PAT. CNTL # b MED. REC. # 5 FED TAX NO 6 STATEMENT COVERS PERIOD FROM THROUGH 7. 4 TYPE OF BILL 8 PATIENT NAME a 9 PATIENT ADDRESS a b b c d e 10 BIRTHDATE 11 SEX ADMISSION 12 DATE 13 HR 14 TYPE
1 2 3a PAT. CNTL # b MED. REC. # 5 FED TAX NO 6 STATEMENT COVERS PERIOD FROM THROUGH 7. 4 TYPE OF BILL 8 PATIENT NAME a 9 PATIENT ADDRESS a b b c d e 10 BIRTHDATE 11 SEX ADMISSION 12 DATE 13 HR 14 TYPE
The Physical Therapy Patient s Guide to Understanding Insurance
 The Physical Therapy Patient s Guide to Understanding Insurance Insurance 101 for PT Patients So, your insurance covers physical therapy which means you won t have to pay anything out-of-pocket for your
The Physical Therapy Patient s Guide to Understanding Insurance Insurance 101 for PT Patients So, your insurance covers physical therapy which means you won t have to pay anything out-of-pocket for your
837 Institutional Health Care Claim Outbound. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
I. Claim submission instructions
 Humboldt Del Norte Independent Practice Association And Humboldt Del Norte Foundation for Medical Care Claims Settlement Practices and Dispute Resolutions Mechanism As required by Assembly Bill 1455, the
Humboldt Del Norte Independent Practice Association And Humboldt Del Norte Foundation for Medical Care Claims Settlement Practices and Dispute Resolutions Mechanism As required by Assembly Bill 1455, the
To learn more about the requirements for your debit card claims, go directly to Section 3, page 4.
 FSA Debit Card Guide IMPORTANT: Please Read There are many misconceptions about debit cards and FSAs. Before you read any further, it s important to understand that using the FSA debit card does NOT eliminate
FSA Debit Card Guide IMPORTANT: Please Read There are many misconceptions about debit cards and FSAs. Before you read any further, it s important to understand that using the FSA debit card does NOT eliminate
hcrnews provider REFORM is coming to our MEMBER ID CARDS get involved? New Rules, New Challenges, New Opportunities What can I do to
 hcrnews provider New Rules, New Challenges, New Opportunities Provider HCR (health care reform) News is a monthly special edition publication for network providers from the Network Administration Division
hcrnews provider New Rules, New Challenges, New Opportunities Provider HCR (health care reform) News is a monthly special edition publication for network providers from the Network Administration Division
2012 ALL PAYERS WORKSHOP BLUE CROSS AND BLUE SHIELD OF KANSAS AGENDA
 2012 ALL PAYERS WORKSHOP BLUE CROSS AND BLUE SHIELD OF KANSAS AGENDA Connecting with Providers Other Party Liability (OPL) Quality Based Reimbursement Program (QBRP) Electronic Data Interchange (EDI) 1
2012 ALL PAYERS WORKSHOP BLUE CROSS AND BLUE SHIELD OF KANSAS AGENDA Connecting with Providers Other Party Liability (OPL) Quality Based Reimbursement Program (QBRP) Electronic Data Interchange (EDI) 1
P R O V I D E R B U L L E T I N B T N O V E M B E R 1 5,
 P R O V I D E R B U L L E T I N B T 2 0 0 5 2 7 N O V E M B E R 1 5, 2 0 0 5 To: All Providers Subject: Overview Beginning on January 1, 2006, the Family and Social Services Administration (FSSA) will
P R O V I D E R B U L L E T I N B T 2 0 0 5 2 7 N O V E M B E R 1 5, 2 0 0 5 To: All Providers Subject: Overview Beginning on January 1, 2006, the Family and Social Services Administration (FSSA) will
UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION
 CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
CHAPTER 5: CLAIMS SUBMISSION UNIT 2: CLAIMS SUBMISSION AND BILLING INFORMATION IN THIS UNIT TOPIC SEE PAGE General Guidelines for Submitting Claims 2 Timely Filing 7 West Virginia Prompt Pay Act 9 New
Frequently Asked Questions About Your Consumer Accounts MasterCard Card
 Frequently Asked Questions About Your Consumer Accounts MasterCard Card 1. What is the Consumer Accounts MasterCard Card? The Consumer Accounts MasterCard Card is a special purpose financial debit card
Frequently Asked Questions About Your Consumer Accounts MasterCard Card 1. What is the Consumer Accounts MasterCard Card? The Consumer Accounts MasterCard Card is a special purpose financial debit card
All Providers. Provider Network Operations. Date: June 22, 2001
 To: From: All Providers Provider Network Operations Date: June 22, 2001 Please te: This newsletter contains information pertaining to Arkansas Blue Cross Blue Shield, a mutual insurance company, it s wholly
To: From: All Providers Provider Network Operations Date: June 22, 2001 Please te: This newsletter contains information pertaining to Arkansas Blue Cross Blue Shield, a mutual insurance company, it s wholly
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT
 CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
HEALTHpac 835 Message Elements
 Version 1.2 April 21, 2003 1 Table of Contents 1 INTRODUCTION...3 1.1 GENERAL COMMENTS...3 1.2 RELATED DOCUMENTS...4 2 835 MESSAGE ELEMENTS...5 2.1 HEADER - INITIAL...5 2.2 PAYER IDENTIFICATION...6 2.3
Version 1.2 April 21, 2003 1 Table of Contents 1 INTRODUCTION...3 1.1 GENERAL COMMENTS...3 1.2 RELATED DOCUMENTS...4 2 835 MESSAGE ELEMENTS...5 2.1 HEADER - INITIAL...5 2.2 PAYER IDENTIFICATION...6 2.3
Remittance Advice and Financial Updates
 Insert photo here Remittance Advice and Financial Updates Presented by EDS Provider Field Consultants August 2007 Agenda Session Objectives Remittance Advice (RA) General Information The 835 Electronic
Insert photo here Remittance Advice and Financial Updates Presented by EDS Provider Field Consultants August 2007 Agenda Session Objectives Remittance Advice (RA) General Information The 835 Electronic
837 Institutional Health Care Claim. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
837 Institutional Health Care Claim. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Inter-Plan Operations (BlueCard )
 Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
Inter-Plan Operations (BlueCard ) Sharing our success An independent licensee of the Blue Cross and Blue Shield Association Agenda History of BlueCard Claim reminders Program performance Claim tips On
APPLICATION FOR GROUP COVERAGE
 Blue Cross and Blue Shield of Louisiana HMO Louisiana Southern National Life APPLICATION FOR GROUP COVERAGE SECTION A - COVERAGE SELECTION Blue Cross and Blue Shield of Louisiana GroupCare PPO (Plan) BlueSaver
Blue Cross and Blue Shield of Louisiana HMO Louisiana Southern National Life APPLICATION FOR GROUP COVERAGE SECTION A - COVERAGE SELECTION Blue Cross and Blue Shield of Louisiana GroupCare PPO (Plan) BlueSaver
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
INSTRUCTIONS FOR BILLING MEDICARE CROSSOVER SERVICES CMS-1500 (02/15) INSTRUCTIONS
 INSTRUCTIONS FOR BILLING MEDICARE CROSSOVER SERVICES CMS-1500 (02/15) INSTRUCTIONS OVERVIEW OF MEDICARE CROSSOVER BILLING Professional services are billed on the CMS-1500 (02/12) claim form. A sample copy
INSTRUCTIONS FOR BILLING MEDICARE CROSSOVER SERVICES CMS-1500 (02/15) INSTRUCTIONS OVERVIEW OF MEDICARE CROSSOVER BILLING Professional services are billed on the CMS-1500 (02/12) claim form. A sample copy
Aetna Group Medicare Advantage Frequently Asked Questions
 Aetna Group Medicare Advantage Frequently Asked Questions Providers & the Aetna Network 1. How do I find out if my providers are in the Aetna Medicare Advantage Network or if they accept the Aetna plan?
Aetna Group Medicare Advantage Frequently Asked Questions Providers & the Aetna Network 1. How do I find out if my providers are in the Aetna Medicare Advantage Network or if they accept the Aetna plan?
Instructions for Completing Standard Authorization Form To Complete Form go to Page 4 of 5
 BlueCross BlueShield of Oklahoma Instructions for Completing Standard Authorization Form To Complete Form go to Page 4 of 5 Under the HIPAA Privacy Rule, an individual may authorize the release of his
BlueCross BlueShield of Oklahoma Instructions for Completing Standard Authorization Form To Complete Form go to Page 4 of 5 Under the HIPAA Privacy Rule, an individual may authorize the release of his
Servicing Out-of-Area Blue Members
 Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
Servicing Out-of-Area Blue Members BlueCross BlueShield of Tennessee BlueCard 101 Servicing Out-of-Area Members Overview BlueCard Program Blue Products Member ID Cards Verifying Eligibility Utilization
CALVERT COUNTY PUBLIC SCHOOLS. ITB: #CCPS-INSUR-MED-2017 DATE OF ISSUE: October 31, 2017 BIDDING INSTRUCTIONS FOR
 CALVERT COUNTY PUBLIC SCHOOLS DATE OF ISSUE: BIDDING INSTRUCTIONS FOR MEDICAL BENEFITS FOR EMPLOYEES OF CALVERT COUNTY PUBLIC SCHOOLS Contents: Section 1 - Instructions to Bidders page 2-3 Section 2 -
CALVERT COUNTY PUBLIC SCHOOLS DATE OF ISSUE: BIDDING INSTRUCTIONS FOR MEDICAL BENEFITS FOR EMPLOYEES OF CALVERT COUNTY PUBLIC SCHOOLS Contents: Section 1 - Instructions to Bidders page 2-3 Section 2 -
Table of Contents. Table of Figures
 Table of Contents 1. Section Modifications... 1 2.... 2 2.1. Introduction... 2 2.1.1. General Policy... 2 2.1.2. Claim Status... 2 2.1.3. Internal Control Number (ICN)... 3 2.2. Banner Page for Paper RA...
Table of Contents 1. Section Modifications... 1 2.... 2 2.1. Introduction... 2 2.1.1. General Policy... 2 2.1.2. Claim Status... 2 2.1.3. Internal Control Number (ICN)... 3 2.2. Banner Page for Paper RA...
Charge Entry Physician Billing. Module 5
 Charge Entry Physician Billing Module 5 Table of Contents Accessing the Batch Control Screen... 3 Create a New Batch... 4 Querying for an Existing Batch... 7 Posting Transactions... 7 Step by Step on how
Charge Entry Physician Billing Module 5 Table of Contents Accessing the Batch Control Screen... 3 Create a New Batch... 4 Querying for an Existing Batch... 7 Posting Transactions... 7 Step by Step on how
Dental Network Office Manual
 July 2008 Provider Network News 3 Dental Network Office Manual /ilinkblue July 2008 Provider Network News 3 23XX4296 R08/10 Blue Cross and Blue Shield of Louisiana incorporated as Louisiana Health Services
July 2008 Provider Network News 3 Dental Network Office Manual /ilinkblue July 2008 Provider Network News 3 23XX4296 R08/10 Blue Cross and Blue Shield of Louisiana incorporated as Louisiana Health Services
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents
 Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Coordination of Benefits (COB) Professional
 Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
Coordination of Benefits (COB) Professional Submitting COB claims electronically saves providers time and eliminates the need for paper claims with copies of the other payer s explanation of benefits (EOB)
Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request.
 Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request www.providerexpress.com Updated: June 2016 Important Note: Any specific member/provider
Provider Express Claim Submission Overview: Long Form (including COB Claims) Corrected Claims Claim Adjustment Request www.providerexpress.com Updated: June 2016 Important Note: Any specific member/provider
Your Flexible Benefit Plan -- Premium Conversion and the Flexible Spending Accounts
 Your Flexible Benefit Plan -- Premium Conversion and the Flexible Spending Accounts Updated: April 2015 YOUR FLEXIBLE BENEFIT PLAN PREMIUM CONVERSION AND THE FLEXIBLE SPENDING ACCOUNTS Introduction The
Your Flexible Benefit Plan -- Premium Conversion and the Flexible Spending Accounts Updated: April 2015 YOUR FLEXIBLE BENEFIT PLAN PREMIUM CONVERSION AND THE FLEXIBLE SPENDING ACCOUNTS Introduction The
Companion Guide for the X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC
 Companion Guide for the 005010X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Description TR3 Values Notes Delimiter:
Companion Guide for the 005010X222A1 Health Care Claim: Professional (837P) Lines of Business: Private Business Senior Plans QUEST Blue Card FEP AFHC Segment Loop Description TR3 Values Notes Delimiter:
837 Institutional Health Care Claim. Section 1 837I Institutional Health Care Claim: Basic Instructions
 Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Companion Document 837I This companion document is for informational purposes only to describe certain aspects and expectations regarding the transaction and is not a complete guide. The details contained
Arthritis & Joint Center of Florida 2328 Medico Lane, Melbourne, Florida fax Financial Policy
 Arthritis & Joint Center of Florida 2328 Medico Lane, Melbourne, Florida 32940 321.956.1501 fax 321.956.1502 Financial Policy We are committed to providing the best care at the most reasonable cost. We
Arthritis & Joint Center of Florida 2328 Medico Lane, Melbourne, Florida 32940 321.956.1501 fax 321.956.1502 Financial Policy We are committed to providing the best care at the most reasonable cost. We
10/2010 Health Care Claim: Professional - 837
 837 Health Care Claim: Professional HIPAA/V4010X098A1/837: 837 Health Care Claim: Professional Version: 1.8 Update 10/20/10 (Latest Changes in RED font) Author: Publication: EDI Department LA Medicaid
837 Health Care Claim: Professional HIPAA/V4010X098A1/837: 837 Health Care Claim: Professional Version: 1.8 Update 10/20/10 (Latest Changes in RED font) Author: Publication: EDI Department LA Medicaid
Archived SECTION 17 - CLAIMS DISPOSITION. Section 17 - Claims Disposition
 SECTION 17 - CLAIMS DISPOSITION 17.1 ACCESS TO REMITTANCE ADVICES...2 17.2 INTERNET AUTHORIZATION...3 17.3 ON-LINE HELP...3 17.4 REMITTANCE ADVICE...3 17.5 CLAIM STATUS MESSAGE CODES...7 17.5.A FREQUENTLY
SECTION 17 - CLAIMS DISPOSITION 17.1 ACCESS TO REMITTANCE ADVICES...2 17.2 INTERNET AUTHORIZATION...3 17.3 ON-LINE HELP...3 17.4 REMITTANCE ADVICE...3 17.5 CLAIM STATUS MESSAGE CODES...7 17.5.A FREQUENTLY
