Anthem Serving Hoosier Healthwise State Sponsored Business
|
|
|
- Myles Miles
- 6 years ago
- Views:
Transcription
1 Anthem Serving Hoosier Healthwise State Sponsored Business 2007 IHCP Provider Seminar
2 Overview UB 04 Community Resource Center Who to Contact Member Benefits Resources Provider File Information Prior Authorization Claims UB 04 Remittance Advice Claims Reconsideration Claims Overpayment Recovery Grievances and Appeals 2007 IHCP Provider Seminar 2
3 We Are Local We are not just another health plan.. We are your neighbor! 2007 IHCP Provider Seminar 3
4 In The Community, Reaching Out To Help Community Resource Centers (CRC) Staffed to connect members and providers to needed resources: Director/Manager Network Education Representative Health Promotion Consultant Outreach Specialist RN Quality Management Specialist Administrative Assistant 2007 IHCP Provider Seminar 4
5 Community Resource Centers (CRC) Staff Southeast Indiana Southwest Indiana Columbus Evansville Brenda Wheat, Director Connie Menale, Network Education Rep Michelle Eilerman, Outreach Specialist Lisa Lant, Manager Cory Hadley-Hurt, Network Education Rep Kayci Merriwether, Outreach Specialist Tammy Queen, RN Quality Management Specialist Ginny France, Health Promotion Consultant Central Indiana Northern Indiana Indianapolis Merrillville Julia Brillhart, Statewide Director Renee Hudson-Johnson, Network Education Rep Ada Hart, Outreach Specialist Jeane Maitland, RN Quality Management Specialist April Thayer, Health Promotion Consultant Tye Demby, Manager Angela Edmond, Network Education Rep Chantelle Johnson, Outreach Specialist Acquanetta McKinney, RN Quality Management Specialist Juanita Fitzgerald, Health Promotion Consultant 2007 IHCP Provider Seminar 5
6 CRCs Our Hands And Heart In The Community Building strong provider and member relations. Working with Members, Government, Providers and Communities to help improve the health and lives of low income families and individuals. Government CRCs enable Anthem to truly help improve lives Members CRC -A A Holistic Approach to Health care Providers Community 2007 IHCP Provider Seminar 6
7 Working In The Community To Improve Lives Refer Members to Agencies for Assistance (child care, transportation, utility assistance, etc.) Provide Grants to Non-profit Agencies Annual mini grants for programs designed to improve health. Community and Agency Events/Programs (agency and school-based) Sponsorship Participation We d like to set up a booth at your event. Community Outreach Vehicle (home visits, events, etc.) Serving on Boards of Local Non-profit Agencies Collaborating With Community Partners to Promote Health Have an idea? Please let us know IHCP Provider Seminar 7
8 Who to Contact Network Education Representative - available to work with providers as it relates to: Provider Contracting Provider Education Provider Servicing Customer Care Center first point of contact to help you with: Claim status Claim inquiries Member eligibility Routine claims submission questions Benefit questions Customer Care Center Phone Number: IHCP Provider Seminar 8
9 Coverage For Members Benefits include: Medical Pharmacy Vision Behavioral Health Chiropractic Dental Long-term Care 2007 IHCP Provider Seminar 9
10 Member Benefit Packages Package A The standard plan which provides full coverage for children, low-income families and some pregnant women. Package B The pregnancy coverage only plan which provides pregnancy-related and urgent care services for some pregnant women. Package C The Children s Health Insurance Plan (CHIP) which provides primary and acute care services for some children under 19 years old. Note: Refer to the Provider Operations Manual (POM), Benefits Matrix, Chapter 4 for covered/non-covered services IHCP Provider Seminar 10
11 Going Beyond Health Coverage We offer our members these additional benefits: Free, unlimited transportation to medical, dental, vision appointments, health ed, and re-determination appointments. Phone # is MedCall 24-hour nurse hotline. Home visits. Help understanding and navigating the healthcare system. Connecting them to other community services. Local programs for healthy living. A gift to new mothers who complete their postpartum visit. Health education IHCP Provider Seminar 11
12 Interpreter Service Interpreters are available by calling the Customer Care Center during normal business hours: Need 72 business hours advance notice 24 business hours to cancel the request Additional information located online at The type of interpreters available are: Interpreters available for 140 languages Telephone Interpreters Services for Members with Hearing Loss Face-to-Face Interpreters Sign Language Interpreters Assistance for the Visually Impaired 2007 IHCP Provider Seminar 12
13 Member Eligibility Helpful Hints You should verify the member s eligibility prior to services. You are able to check member eligibility through the Web Interchange at: Members are issued 2 cards: 1. One card from the State listing the Medicaid #. 2. One card from Anthem Hoosier Healthwise listing the ID # beginning with a prefix of YRH. In Form Locator 60 of the UB 04, ALWAYS include the YRH prefix in front of the member s Medicaid # IHCP Provider Seminar 13
14 Outreach Specialist Services of our Outreach Specialists: Member orientations. Member benefit education. (Note: A member may request Health Education Materials by calling ) Community events. Health fairs. Assisting members with community resources, such as food, clothing, heating, etc IHCP Provider Seminar 14
15 Outreach Specialist continued Helping expectant mothers with pre-selection of a Primary Care Provider for their new baby. Conduct member home visits at the request from a provider or our case management department. When to use the Outreach Request Form: The member is noncompliant. The member needs assistance making their doctor appointments. The member needs health education classes. The member needs new member benefits orientation. The member needs assistance from community resources IHCP Provider Seminar 15
16 Health Promotion Prenatal Program a comprehensive program designed to: Identify members who are pregnant. Encourage early and ongoing prenatal care. Increase members access to prenatal information and services. Encourage self-care throughout the stages of pregnancy. Gift incentive for timely prenatal care. Members are identified through: Physician notification. Outreach Calls Visits Member calls to Customer Care Center Claims Data 2007 IHCP Provider Seminar 16
17 Resources Anthem Website Claims Status Member Handbook Provider Bulletins Provider Operations Manual (POM) Prior Authorization Toolkit Forms and Tools Library Anthem Medical Policies Clinical Practice Guidelines Pharmacy Guidelines Indiana Health Coverage Programs - Provider Services Pharmacy Services Managed Care Publications 2007 IHCP Provider Seminar 17
18 Provider File Information It s important to have current provider file information in our system for claims processing and claim payments. Report any changes to us in writing using your letterhead, such as: Provider Name Tax ID Practice Location Billing Location Phone Number Specialty type Mail provider file updates to: Anthem Blue Cross and Blue Shield Attn: Network Services PO Box 6144 Indianapolis, IN IHCP Provider Seminar 18
19 Prior Authorization Prior Authorization Toolkit listed on our website: Website includes the Services Requiring Prior Authorization. Request for Preservice Review. Non-par providers, all services require prior authorization. Participating providers: some services require Prior Authorization such as: Home Oxygen Apnea monitors CPAP/ BIPAP Hearing aids Motorized and manual wheelchairs / scooters See materials insert for a more inclusive list 2007 IHCP Provider Seminar 19
20 Prior Authorization Helpful Hints Physician is responsible for obtaining the preservice review for both professional and institutional services. Hospital or ancillary provider should always contact us to verify pre-service review status. Authorization not required if referring a member to an innetwork specialist. Authorization is required when referring to an out-of-network specialist IHCP Provider Seminar 20
21 Prior Authorization Include the following on the Request for Preservice Review: Member name and Medicaid ID # including the YRH prefix. Diagnosis with ICD-9 code. Procedure with CPT/HCPCS code. Date of injury/date of hospital admission. Third party liability information (if applicable). Facility name (if applicable). Primary medical provider name. Specialist or name of attending physician. Clinical information supporting request IHCP Provider Seminar 21
22 Prior Authorization Phone: Fax: Timeframe: usually a 3-day turnaround time. If request has missing information, it may take longer. If you have an urgent request, please call and indicate this to the Intake Specialist. Urgent requests will be completed within 24 hours. Note: an urgent request means that a delay in the authorization would be detrimental to the member s health IHCP Provider Seminar 22
23 Pharmacy Formulary is available through the Anthem website: Epocrates is a drug reference software application that allows you to check: Formulary status Prior authorization requirements Formulary alternatives General substitutes Quantity limits 2007 IHCP Provider Seminar 23
24 Pharmacy, continued Epocrates also features drug reference information including: Indication Dosing Contraindications Drug interactions Adverse reactions Cost information Epocrates website: IHCP Provider Seminar 24
25 Claims UB 04 Newborns Encourage the pregnant patient to select a PMP for her child prior to its birth. Pre-selection Form will soon be available on our website. A copy is in your packet. All newborns must be billed under their own Medicaid ID number. DO NOT bill under the mother s Medicaid ID number It could be 30 days before our system will receive the newborn s Medicaid ID number in our system IHCP Provider Seminar 25
26 Claims UB 04 Newborns continued: We have instituted a process to allow for billing when you have the Newborn s Medicaid ID number before we receive it in our membership file IHCP Provider Seminar 26
27 Claims UB 04 Newborns continued: Step 1: Fill out the Newborn Notification Enrollment Report. See for the form. materials to of fax materials to Step 2: File your claims electronically after the 3 rd business day from the date you submitted the Newborn Notification Enrollment Report. Daily cutoff is 3:00 pm. Eastern (Indianapolis time) 2007 IHCP Provider Seminar 27
28 Claims UB 04 Outpatient Surgery and Ambulatory Surgery Centers (ASC) Reimbursement is all-inclusive flat fee Lump all charges and services with surgical procedure 2007 IHCP Provider Seminar 28
29 Claims UB 04 Outpatient Surgery and ASC, continued Multiple Surgeries Maximum of two reimbursed, regardless of number of incisions. Same incision only reimburse the one with the highest ASC rate. Separate incision only reimburse the one with highest ASC rate. Primary surgery reimbursed at 100%. One separate incision / secondary surgery reimbursed at 50%. Bilateral procedures are reimbursed at 150%. List appropriate revenue code and CPT code as two separate detail line items IHCP Provider Seminar 29
30 Claims UB 04 Ambulance Transportation Emergency Transportation: All emergency transportation should be billed to Anthem Hoosier Healthwise using the CMS Emergency Transportation is any transportation requiring Advanced or Basic Life Support. A0425 Ground Mileage, per statute mile. Modifiers include: U1, U2, U3, U4, and U IHCP Provider Seminar 30
31 Claims UB 04 Ambulance Transportation, continued Non emergent transportation: Should be arranged through LCP Transportation at hours notice for non emergent appointments 24 hours or less notice may be given in a case of sickness with a physician appointment scheduled that day. Non emergent transportation is unlimited IHCP Provider Seminar 31
32 Claims UB 04 Laboratories / Professional Components Hospital outpatient bill on UB92/CMS1450/UB 04 Physicians and Independent Labs bill on CMS IHCP Provider Seminar 32
33 Claims UB 04 Coordination of Benefits (COB) When submitting COB claims, specify the other coverage and payment information in the appropriate Form Locator 50A-55C of the UB 04 form. We must receive COB claims within 180 days from the date on the other carrier s or program s RA, or letter denial of coverage. COB claims must be submitted on paper. Do not file electronically. Include the member s Medicaid number, including the YRH prefix along with the member s Medicaid #. Attach the third party Remittance Advice or letter explaining the denial with the CMS claim form IHCP Provider Seminar 33
34 Claims UB 04 Helpful Hints for Electronic claim filing: EDI Help Desk: Use the UB 04 format. COB Medicaid claims cannot be filed electronically. The member s ID must include the YRH prefix. Use the Anthem 12-digit PIN and/or NPI. Note: The Medicaid # may also be submitted along with the qualifier # 1D. Include the Tax ID number IHCP Provider Seminar 34
35 Claims UB 04 Helpful Hints for Electronic claim filing continued: Include the Provider Medicaid ID Number. The Anthem Payor ID number is: (professional claims) (institutional claims) Review your electronic submission reports from Anthem. Call the Anthem EDI Help Desk if you/your vendor has problems with electronic claims filing IHCP Provider Seminar 35
36 Claims UB 04 Helpful Hints for filing Paper claims: Use the UB 04 claim form. The member s Medicaid ID number must include the YRH prefix. Use your Medicaid ID # in Form Locator 57A of the UB 04 form. (Do not use your Anthem 12-digit PIN). Medicaid COB claims must be filed on the paper UB 04 form. Mail your paper claims to: Anthem Blue Cross and Blue Shield PO Box Louisville, KY IHCP Provider Seminar 36
37 Remittance Advice (RA) Checks and Remittance Advices are issued daily. Example of RA below. Remark Code 45 - also in the Plan Not Allowed column of the Remittance Advice for another code. Explanations for codes are at the end of the Remittance Advice in the Remittance Advice Summary. Service Description Billed Procedure Procedure Units Plan Allowed Plan Not Allowed Other Carrier Member Co-pay Interest Withhold Claim Remark Date of Service Amount code Modifiers Paid /Deductibles Amount Amount Payment Codes 06/26/2007 Surgery /27 00, IHCP Provider Seminar 37
38 Remittance Advice (RA) A specific Reason Code can be found in the Plan Not Allowed column. A general remark code appears in the Remark Codes column. DRG payments will show an additional line item at the end of the claim with the DRG pricing. Whole claim pricing claims will not show a DRG or procedure code and will show payment on an additional line item at the end of the claim. Explanations of codes used will be at the end on a Summary Page IHCP Provider Seminar 38
39 Electronic Funds Transfer & Electronic RA Electronic Funds Transfer (EFT) option for claims payment transactions. Claim payments to be deposited directly into a selected bank account. Contracted providers may choose to receive Electronic Remittance Advice (ERA). Enroll by completing the ERA/EFT Enrollment Form found in the Forms Toolkit on our website: Submit the form to the address or fax number indicated on the ERA/EFT Enrollment Form IHCP Provider Seminar 39
40 Claims Reconsideration Providers may request a reconsideration of a claim payment or denial. Provider would complete the Dispute Resolution Request Form. Refer to The Dispute Resolution Request Form must be submitted within 60 days from the date you receive the Remittance IHCP Provider Seminar 40
41 Claims Reconsideration Mail Reconsideration Requests to: Anthem Blue Cross Blue Shield PO Box 6144 Indianapolis, IN Claims will be resolved 45 business days from the receipt of the dispute IHCP Provider Seminar 41
42 Claims Overpayment Recovery Anthem seeks recovery of all excess claim payments from the payee to whom the benefit check is made payable. When an overpayment is discovered, an overpayment recovery process is initiated by sending written notification of the overpayment to the provider. Mail a copy of the overpayment notification and /or the EOB from Anthem or other carriers and a check to: Anthem Blue Cross and Blue Shield Attn: Cost Containment PO Box 9207 Oxnard, CA IHCP Provider Seminar 42
43 Grievances and Appeals Providers can file a written grievance related to dissatisfaction or concern about: Another Anthem provider Anthem A member Providers may file a written appeal on behalf of a member for : Denial Deferral Modification of a prior authorization request 2007 IHCP Provider Seminar 43
44 Grievances and Appeals Complete and submit the form to: Anthem Blue Cross and Blue Shield Attn: Appeals and Complaints Department PO Box 6144 Indianapolis, IN Complete and submit via fax to: IHCP Provider Seminar 44
45 Grievances and Appeals Timelines for filing: Grievance: 60 calendar days from the date the provider became aware of the issue Appeals: 30 calendar days from the date of the notice of action letter advising of the adverse determination Anthem s Response/Resolution: Grievances within 20 business days from the receipt Appeals within 30 business days 2007 IHCP Provider Seminar 45
46 We re partnering with health care providers to improve the health of our communities and the lives of the people we serve Thank you! 2007 IHCP Provider Seminar
CMS-1500 professional providers 2017 annual workshop
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS-1500 professional providers 2017 annual workshop Reminders and updates The (Anthem) Provider Manual was updated in July 2017. The provider manual is
CMS 1450 (UB-04) institutional providers
 Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Serving Hoosier Healthwise, Healthy Indiana Plan CMS 1450 (UB-04) institutional providers 2017 Annual Workshop Reminders and updates The provider manual was updated in July 2017. The provider manual is
Avenues of Resolution for Indiana Health Coverage Programs
 Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Avenues of Resolution for Indiana Health Coverage Programs HP Provider Relations/October 2013 Agenda Resolving Claims-related Questions Provider Enrollment Prior Authorization Fee Schedule Indiana Health
Anthem Blue Cross and Blue Shield. Serving Hoosier Healthwise and Healthy Indiana Plan
 Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise and Healthy Indiana Plan 3rd Quarter Updates NDC Denials The following elements are required for claims with NDC information J code NDC N4
Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates
 Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
Serving Hoosier Healthwise, Healthy Indiana Plan Anthem Blue Cross and Blue Shield (Anthem) Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect 2017 summer updates Agenda Billing
MDwise Annual IHCP Seminar. Exclusively serving Indiana families since 1994.
 MDwise 101 2016 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda MDwise history IHCP Overview MDwise Delivery System Model IHCP Program Overview Hoosier Healthwise Healthy Indiana
MDwise 101 2016 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda MDwise history IHCP Overview MDwise Delivery System Model IHCP Program Overview Hoosier Healthwise Healthy Indiana
IHCP Annual Workshop October 2016
 IHCP Annual Workshop October 2016 MDwise UB-04 Billing and Claim Processing Exclusively serving Indiana families since 1994. APP0216 (9/15) Agenda Who is MDwise? Provider Enrollment: Are you a MDwise contracted
IHCP Annual Workshop October 2016 MDwise UB-04 Billing and Claim Processing Exclusively serving Indiana families since 1994. APP0216 (9/15) Agenda Who is MDwise? Provider Enrollment: Are you a MDwise contracted
Healthy Indiana Plan (HIP) Provider Orientation
 Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
IHCP Annual Workshop October 2017
 IHCP Annual Workshop October 2017 MDwise 101 HHW-HIPP0519( 10/17) Exclusively serving Indiana families since 1994. Agenda MDwise History IHCP Overview MDwise Delivery System Model IHCP Program Overview
IHCP Annual Workshop October 2017 MDwise 101 HHW-HIPP0519( 10/17) Exclusively serving Indiana families since 1994. Agenda MDwise History IHCP Overview MDwise Delivery System Model IHCP Program Overview
Insert photo here. Common Denials. Presented by EDS Provider Field Consultants
 Insert photo here Common Denials Presented by EDS Provider Field Consultants October 2007 Common Denials Agenda Session Objectives Edits and Audits Defined Edit Grouping Denial Overview Questions 2 October
Insert photo here Common Denials Presented by EDS Provider Field Consultants October 2007 Common Denials Agenda Session Objectives Edits and Audits Defined Edit Grouping Denial Overview Questions 2 October
Managed Health Services
 Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
Managed Health Services National Provider Identifier MHS needs to obtain NPI numbers prior to January 2008. Please submit directly to MHS for entry into our claims payment system. Submit NPI via MHS Web
Fidelis Care uses TriZetto's Claims Editing Software to automatically review and edit health care claims submitted by physicians and facilities.
 BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
BILLING AND CLAIMS Instructions for Submitting Claims The physician s office should prepare and electronically submit a CMS 1500 claim form. Hospitals should prepare and electronically submit a UB04 claim
MDwise Healthy Indiana Plan (HIP)
 MDwise Healthy Indiana Plan (HIP) Annual IHCP Seminar October 2012 Exclusively serving Indiana families since 1994. HIPP0080 (10/11) Topics Comparison between Hoosier Healthwise and Healthy Indiana Plan
MDwise Healthy Indiana Plan (HIP) Annual IHCP Seminar October 2012 Exclusively serving Indiana families since 1994. HIPP0080 (10/11) Topics Comparison between Hoosier Healthwise and Healthy Indiana Plan
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise.
 Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
P R O V I D E R B U L L E T I N B T J U N E 1,
 P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
P R O V I D E R B U L L E T I N B T 2 0 0 5 1 1 J U N E 1, 2 0 0 5 To: All Providers Subject: Overview The purpose of this bulletin is to provide information about system modifications that are effective
Chapter 7 General Billing Rules
 7 General Billing Rules Reviewed/Revised: 10/10/2017, 07/13/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 General Information This chapter contains general information related to Health Choice Arizona
7 General Billing Rules Reviewed/Revised: 10/10/2017, 07/13/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 General Information This chapter contains general information related to Health Choice Arizona
Pharmacy Coverage and Claim Submission Guidelines
 P R O V I D E R B U L L E T I N B T 2 0 0 0 0 1 8 J U N E 1, 2 0 0 0 To: Subject: All Indiana Health Coverage Programs Providers Overview The purpose of this bulletin is to provide coverage and reimbursement
P R O V I D E R B U L L E T I N B T 2 0 0 0 0 1 8 J U N E 1, 2 0 0 0 To: Subject: All Indiana Health Coverage Programs Providers Overview The purpose of this bulletin is to provide coverage and reimbursement
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise.
 Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Prior Authorization All non-emergent services rendered by non-contracted providers require prior authorization, unless specified otherwise. Abortions, Hysterectomies and Sterilizations Ambulance Emergency
Administrative Guide
 Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide 2012 KanCare Program DRAFT PENDING ADDITIONAL UPDATES AND STATE OF KANSAS APPROVAL DRAFT PENDING ADDITIONAL UPDATES
Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide 2012 KanCare Program DRAFT PENDING ADDITIONAL UPDATES AND STATE OF KANSAS APPROVAL DRAFT PENDING ADDITIONAL UPDATES
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents
 Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Passport Advantage Provider Manual Section 13.0 Provider Billing Manual Table of Contents 13.1 Claim Submissions 13.2 Provider/Claims Specific Guidelines 13.3 Understanding the Remittance Advice 13.4 Denial
Important Questions Answers Why this Matters:
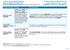 Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
IHCP Annual Workshop October 2016
 IHCP Annual Workshop October 2016 MDwise CMS-1500 Billing and Claim Processing Exclusively serving Indiana families since 1994. Agenda Who is MDwise? Provider Enrollment: Are you a contracted MDwise Provider?
IHCP Annual Workshop October 2016 MDwise CMS-1500 Billing and Claim Processing Exclusively serving Indiana families since 1994. Agenda Who is MDwise? Provider Enrollment: Are you a contracted MDwise Provider?
LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH
 LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to:
LTC/MMA Monthly Claims Training Claims & Prior Authorization ACS & AFCH Submitting Claims Providers may submit claims to Molina in the following ways: On paper, using a current version CMS-1500 form, to:
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Montgomery County Public Schools- PPO Coverage Period: 10/01/ /30/2017
 Montgomery County Public Schools- PPO Coverage Period: 10/01/2016 09/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
Montgomery County Public Schools- PPO Coverage Period: 10/01/2016 09/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
Indiana Health Coverage Program Seminar Presented by MDwise UB-04 October 22-24, 2007
 Indiana Health Coverage Program Seminar Presented by MDwise UB-04 October 22-24, 2007 Topics for today Who is MDwise MDwise Delivery Systems UB-04 Claims submission and Inquiries Referrals and Prior Authorization
Indiana Health Coverage Program Seminar Presented by MDwise UB-04 October 22-24, 2007 Topics for today Who is MDwise MDwise Delivery Systems UB-04 Claims submission and Inquiries Referrals and Prior Authorization
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal
 Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
Network Providers. deductible?
 Hoosier Heartland School Trust: Plan 1 Blue Access (PPO) Coverage Period: 1/01/2017-08/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan
Hoosier Heartland School Trust: Plan 1 Blue Access (PPO) Coverage Period: 1/01/2017-08/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT
 CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
CHAPTER 7: CLAIMS, BILLING, AND REIMBURSEMENT UNIT 1: HEALTH OPTIONS CLAIMS SUBMISSION AND REIMBURSEMENT IN THIS UNIT TOPIC SEE PAGE General Information 2 Reporting Practitioner Identification Number 2
Important Questions Answers Why this Matters: In-network: $0/Individual; $0/Family Out-of-network: $750/Individual; $1,500/Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-421-1880. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-421-1880. Important Questions
UnitedHealthcare Community Plan of Missouri
 UnitedHealthcare Community Plan of Missouri Agenda UnitedHealthcare Community Plan of Missouri Member Eligibility and Benefits Notification and Prior Authorization Claims Management Care Provider Resources
UnitedHealthcare Community Plan of Missouri Agenda UnitedHealthcare Community Plan of Missouri Member Eligibility and Benefits Notification and Prior Authorization Claims Management Care Provider Resources
Anthem BlueCross BlueShield Christian Care Communities Blue Access PPO Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Welcome Third Quarter EDS Workshop Presented by MDwise, Inc., CompCare and MDwise Delivery Systems Provider Relation Reps.
 Welcome Third Quarter EDS Workshop Presented by MDwise, Inc., CompCare and MDwise Delivery Systems Provider Relation Reps. The Best Care. Because We Care. -1- 1. Claims Submission 2. Members Eligibility
Welcome Third Quarter EDS Workshop Presented by MDwise, Inc., CompCare and MDwise Delivery Systems Provider Relation Reps. The Best Care. Because We Care. -1- 1. Claims Submission 2. Members Eligibility
ISMA Coalition Meeting September 13, 2013
 ISMA Coalition Meeting September 13, 2013 Questions and Answers 1. For OMPP and each MCE: When will all the Medicaid payers be able to accept electronic claims (837 files) for secondary claims with Primary
ISMA Coalition Meeting September 13, 2013 Questions and Answers 1. For OMPP and each MCE: When will all the Medicaid payers be able to accept electronic claims (837 files) for secondary claims with Primary
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Anthem BlueCross BlueShield Eastern Kentucky University Economy Coverage Period: {01/01/ /31/2013} Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. For prescription
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. For prescription
MHS CMS 1500 Tips and Billing Guidelines
 MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
MHS CMS 1500 Tips and Billing Guidelines AGENDA Creating Claim on MHS Web Portal Claim Process Claim Rejection Claim Denial Claim Adjustment Dispute Resolution Taxonomy Eligibility Reviewing Claims DME
Important Questions Answers Why this Matters:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Frequently Asked Questions
 Corrected Claims Submissions 1. What is a corrected claim? If a claim was submitted to and accepted by Healthfirst but was later found to have incorrect information, certain data elements on the claim
Corrected Claims Submissions 1. What is a corrected claim? If a claim was submitted to and accepted by Healthfirst but was later found to have incorrect information, certain data elements on the claim
Important Questions Answers Why this Matters:
 This is only a summary. Medical benefits are covered through Anthem Blue Cross and Blue Shield. If you want more detail about your coverage and costs for health benefits, you can get the complete terms
This is only a summary. Medical benefits are covered through Anthem Blue Cross and Blue Shield. If you want more detail about your coverage and costs for health benefits, you can get the complete terms
PROVIDER MANUAL. Revised January Page 1
 PROVIDER MANUAL Revised January 2018 Page 1 Table of Contents Introduction 3 General Information 4 Who Do I Call? 5 ID Card Logos 6 Credentialing/Recredentialing 7 Provider Changes 8 Referral and Authorization
PROVIDER MANUAL Revised January 2018 Page 1 Table of Contents Introduction 3 General Information 4 Who Do I Call? 5 ID Card Logos 6 Credentialing/Recredentialing 7 Provider Changes 8 Referral and Authorization
HIPAA 5010 Webinar Questions and Answer Session
 HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
HIPAA 5010 Webinar Questions and Answer Session Q: After Jan 2012, do the providers who bill on paper have to worry about 5010? Q: What if a provider submits all claims via paper? Do the new 5010 guidelines
Important Questions Answers Why this Matters: In-network: $0/Individual; $0/Family Out-of-network: $500/Individual; $1,000/Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling 1-800-445-7490.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling 1-800-445-7490.
Important Questions Answers Why this Matters: $300 Single/$600 Family for Network Providers. $500 Single/$1,000 Family for Non- What is the overall
 Bellefontaine City Schools: Blue Access (PPO) Coverage Period: 04/01/2015-03/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO
Bellefontaine City Schools: Blue Access (PPO) Coverage Period: 04/01/2015-03/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO
Provider Contacts List
 Common telephone numbers, email addresses and websites for providers and Oregon Health Plan (OHP) members Fax numbers and telephone numbers for prior authorization requests Mailing addresses for claims,
Common telephone numbers, email addresses and websites for providers and Oregon Health Plan (OHP) members Fax numbers and telephone numbers for prior authorization requests Mailing addresses for claims,
Dell Children s Health Plan transition to Amerigroup. Misty Arayata & Emily Rhine Provider Engagement October 2016
 Dell Children s Health Plan transition to Amerigroup Misty Arayata & Emily Rhine Provider Engagement October 2016 TSPEC-0123-16 October 2016 Introduction Effective December 1, 2016 Seton Health Plan will
Dell Children s Health Plan transition to Amerigroup Misty Arayata & Emily Rhine Provider Engagement October 2016 TSPEC-0123-16 October 2016 Introduction Effective December 1, 2016 Seton Health Plan will
Sunflower Health Plan. Regional Provider Workshop
 Sunflower Health Plan Regional Provider Workshop Agenda & Objectives e Third Party Liability (TPL) & Coordination of Benefits (COB) Claims Submission Requirements Overview Sunflower TPL & COB Claims Processing
Sunflower Health Plan Regional Provider Workshop Agenda & Objectives e Third Party Liability (TPL) & Coordination of Benefits (COB) Claims Submission Requirements Overview Sunflower TPL & COB Claims Processing
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
Welcome. The Best Care. Because We Care. -1-
 Welcome Second Quarter 2007 EDS Workshop Presented by Corporate MDwise Sherri Miles Provider Relations Manager Jacquie Marsalis-Provider Relations Manger/CompCare The Best Care. Because We Care. -1- About
Welcome Second Quarter 2007 EDS Workshop Presented by Corporate MDwise Sherri Miles Provider Relations Manager Jacquie Marsalis-Provider Relations Manger/CompCare The Best Care. Because We Care. -1- About
Important Questions Answers Why this Matters:
 Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
MDwise, Inc. MDwise Updates 2017 IHCP First-Quarter Workshop. Exclusively serving Indiana families since 1994.
 MDwise, Inc. MDwise Updates 2017 IHCP First-Quarter Workshop Exclusively serving Indiana families since 1994. Agenda MDwise History Meet your Provider Relations Team IHCP Managed Care Overview MDwise Delivery
MDwise, Inc. MDwise Updates 2017 IHCP First-Quarter Workshop Exclusively serving Indiana families since 1994. Agenda MDwise History Meet your Provider Relations Team IHCP Managed Care Overview MDwise Delivery
Important Questions Answers Why this Matters:
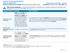 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
$200 per member / $600 per family in-network. See the chart starting on page 2 for your costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-866-627-0705. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-866-627-0705. Important Questions
Important Questions Answers Why this Matters:
 Anthem BlueCross BlueShield Blue Access PPO Option 14 / Rx Option AE Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
Anthem BlueCross BlueShield Blue Access PPO Option 14 / Rx Option AE Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
$1,500 Individual/$3,000 Family for participating providers. $3,000 Individual/$6,000. Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
Life of a Claim. HP Provider Relations/August 2014
 Life of a Claim HP Provider Relations/August 2014 Agenda General requirements for reimbursement by the Indiana Health Coverage Programs (IHCP) System edits System audits Pricing methodologies Suspended
Life of a Claim HP Provider Relations/August 2014 Agenda General requirements for reimbursement by the Indiana Health Coverage Programs (IHCP) System edits System audits Pricing methodologies Suspended
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 Anthem HealthKeepers Premier POS: Henrico County General Government and Public Schools Coverage Period: 1/1/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
Anthem HealthKeepers Premier POS: Henrico County General Government and Public Schools Coverage Period: 1/1/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
Important Questions Answers Why this Matters:
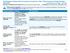 Southeastern Indiana School Insurance Consortium: Plan F Blue Access for Health Savings Accounts Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
Southeastern Indiana School Insurance Consortium: Plan F Blue Access for Health Savings Accounts Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4902. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4902. Important Questions
Section Eleven. Referrals and Prior Authorization REFERRAL PROCESS. Physician Referrals within Plan Network
 REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
REFERRAL PROCESS Physician Referrals within Plan Network Physicians may refer members to any Specialty Care Physician (Specialist) or ancillary provider within the Fidelis Care network. Except as noted
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 CEBCO: Champaign County Plan 1a Blue Access (PPO) Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
CEBCO: Champaign County Plan 1a Blue Access (PPO) Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
Important Questions Answers Why this Matters: For PPO Providers: $1,500 Member/$3,000 Family For Non-PPO Providers:
 Anthem Blue Cross Life and Health Insurance Company ACWA / JPIA: Account Based Health Plan (EV85) Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
Anthem Blue Cross Life and Health Insurance Company ACWA / JPIA: Account Based Health Plan (EV85) Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
HealthTrust: LUMENOS $2500 Coverage Period: 07/01/ /30/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4896. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4896. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-421-1880. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-421-1880. Important Questions
Innovation Health At-A-Glance
 Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
Innovation Health At-A-Glance A quick reference guide for health care professionals 71.02.801.1 (8/13) innovation-health.com A guide for doing business with Innovation Health Getting started with Innovation
General SRC #16, Attachment 4: Claims Appeal Operations Desktop Procedure
 General SRC #16, Attachment 4: Claims Appeal Operations Desktop Procedure Desktop Procedure: Claim Appeal Operations Related P&Ps: Provider Complaint System NE.MCD.7.03.(B)-(P).FL.MCC.FL CMC Last Updated:
General SRC #16, Attachment 4: Claims Appeal Operations Desktop Procedure Desktop Procedure: Claim Appeal Operations Related P&Ps: Provider Complaint System NE.MCD.7.03.(B)-(P).FL.MCC.FL CMC Last Updated:
Anthem BlueCross BlueShield Blue Access PPO Option 10 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 Anthem BlueCross BlueShield Blue Access PPO Option 10 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2015-0 /30/2016 Coverage For: Individual/Family
Anthem BlueCross BlueShield Blue Access PPO Option 10 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2015-0 /30/2016 Coverage For: Individual/Family
What is the overall deductible? are separate and do not. towards each other. Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
Does not apply to Network Preventive deductible?
 Wittenberg University: Blue Access (PPO) Option 2 Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
Wittenberg University: Blue Access (PPO) Option 2 Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
Western Kentucky University Anthem BlueCross BlueShield Basic PPO Plan Coverage Period: 01/01/ /31/2018 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling 1-888-650-4047.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling 1-888-650-4047.
GENERAL BENEFIT INFORMATION
 Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Authorization Policy The following policy applies to Tufts Health Plan contracted providers rendering outpatient and inpatient services. This policy applies to Commercial 1 products (including Tufts Health
Important Questions Answers Why this Matters:
 Anthem BlueCross Lumenos HSA 1500 (80/50) Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 12/01/2013-11/30/2014 Coverage For: Individual/Family Plan Type:
Anthem BlueCross Lumenos HSA 1500 (80/50) Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 12/01/2013-11/30/2014 Coverage For: Individual/Family Plan Type:
Excellus BlueCross BlueShield Provider Relations Fall Seminar
 Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
Excellus BlueCross BlueShield Provider Relations Fall Seminar Agenda Product Updates Safety Net Clear Coverage Authorization Tool Website Updates EDI Updates Clinical Editing BlueCard Medicare Updates
Important Questions Answers Why this Matters:
 Anthem BlueCross Solution PPO 1500/15/20 / $15/$30/$50/30% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 11/01/2014-10/31/2015 Coverage For: Individual/Family
Anthem BlueCross Solution PPO 1500/15/20 / $15/$30/$50/30% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 11/01/2014-10/31/2015 Coverage For: Individual/Family
Important Questions Answers Why this Matters:
 Anthem BlueCross BlueShield Blue Access PPO Option D54 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 04/01/2013-03/31/2014 Coverage For: Individual/Family
Anthem BlueCross BlueShield Blue Access PPO Option D54 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 04/01/2013-03/31/2014 Coverage For: Individual/Family
Important Questions Answers Why this Matters:
 Anthem BlueCross Classic PPO 250/20/20 / $10/$30/$50/30% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family Plan
Anthem BlueCross Classic PPO 250/20/20 / $10/$30/$50/30% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family Plan
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-333-5735. Important Questions
Training Documentation
 Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Training Documentation Substance Abuse Rehab Facilities 2017 Health care benefit programs issued or administered by Capital BlueCross and/or its subsidiaries, Capital Advantage Insurance Company, Capital
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
Research and Resolve UB-04 Claim Denials. HP Provider Relations/October 2014
 Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Research and Resolve UB-04 Claim Denials HP Provider Relations/October 2014 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Coverage Period: 08/01/ /31/2016
 Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 08/01/2015-07/31/2016
Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 08/01/2015-07/31/2016
Important Questions. Why this Matters: For PPO Providers: $0 Member/$0 Family For Non-PPO Providers: $0 Member/$0 Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-759-5758. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-800-759-5758. Important
You don t have to meet deductibles for specific services, but see the chart starting on page 3 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
Archived SECTION 15-BILLING INSTRUCTIONS. Section 15 - Billing Instructions
 SECTION 15-BILLING INSTRUCTIONS 15.1 ELECTRONIC DATA INTERCHANGE... 2 15.2 INTERNET ELECTRONIC CLAIM SUBMISSION... 2 15.3 CMS-1500 CLAIM FORM... 3 15.4 PROVIDER COMMUNICATION UNIT... 3 15.5 RESUBMISSION
SECTION 15-BILLING INSTRUCTIONS 15.1 ELECTRONIC DATA INTERCHANGE... 2 15.2 INTERNET ELECTRONIC CLAIM SUBMISSION... 2 15.3 CMS-1500 CLAIM FORM... 3 15.4 PROVIDER COMMUNICATION UNIT... 3 15.5 RESUBMISSION
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield BluePreferred for Individuals
 Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield BluePreferred for Individuals PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK CARE COVERED? 1
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield BluePreferred for Individuals PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK CARE COVERED? 1
0518.PR.P.PP.2 7/18. The Ins and Outs of CMS 1500 Billing
 0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
0518.PR.P.PP.2 7/18 The Ins and Outs of CMS 1500 Billing AGENDA Claim Process Creating Claim on MHS Web Portal Reviewing Claims Claim Denial Claim Adjustment Dispute Resolution Taxonomy Allwell Information
HealthKeepers, Inc. Anthem HealthKeepers University of Virginia Physicians Group Anthem HealthKeepers- $750/$1,500 deductible
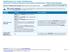 HealthKeepers, Inc. Anthem HealthKeepers University of Virginia Physicians Group Anthem HealthKeepers- $750/$1,500 deductible Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
HealthKeepers, Inc. Anthem HealthKeepers University of Virginia Physicians Group Anthem HealthKeepers- $750/$1,500 deductible Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
Upper Arlington City School District: Lumenos Health Savings Accounts Coverage Period: 01/01/ /31/2016
 Upper Arlington City School District: Lumenos Health Savings Accounts Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
Upper Arlington City School District: Lumenos Health Savings Accounts Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
SutterSelect Administrative Manual. June 2017
 SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
SutterSelect Administrative Manual June 2017 Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.arcsvs.com or by calling 1-877-309-2955. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.arcsvs.com or by calling 1-877-309-2955. Important Questions
Important Questions Answers Why this Matters: For in-network providers Deductible is not applicable innetwork
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-922-6621. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-922-6621. Important Questions
$0 Single/$0 Family for In- Network Providers. See the chart starting on page 2 for your costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-634-3383. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-634-3383. Important Questions
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield Name of Carrier Tonik for Individuals $3,000 Name of Plan
 Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield Name of Carrier Tonik for Individuals $3,000 Name of Plan PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. CARE
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield Name of Carrier Tonik for Individuals $3,000 Name of Plan PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. CARE
Employee Benefit Plan: Missoula County Public Schools Coverage Period: 01/01/ /31/2014 Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Anthem Blue Cross Blue Shield: Anthem Silver DirectAccess - cbka Coverage Period: 01/01/ /31/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-231-5046. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-231-5046. Important Questions
You must pay all of the costs for these services up to the specific deductible amount before the plan begins to pay for these services.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
$5,000 person. Does not apply to preventive care. Coverage for: Individual + Family Plan Type: PPO
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/ca/aso or by calling 1-877-442-4686.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/ca/aso or by calling 1-877-442-4686.
