Assessing the Financial Condition of Provider-Sponsored Health Plans
|
|
|
- Oswin Curtis
- 5 years ago
- Views:
Transcription
1 Original Research Assessing the Financial Condition of Provider-Sponsored Health Plans Michael J. McCue, DBA INTRODUCTION The onset of managed care across both commercial and government payers in the early 1990s led to a surge in the number of hospitals and health systems sponsoring health plans, referred to as provider-sponsored health plans (PSHPs). By 1995, the number of hospitals with some form of sponsorship arrangement (eg, full ownership, system affiliation, network alliance, joint venture) with a health plan totaled 737 (McCue 2000). However, by 1998, growing financial losses from the health plans, eroding capital base of hospitals to fund the plans, and lower Medicare reimbursement from the Balanced Budget Act of 1997 resulted in closures or sale of 80 health plans by hospitals (Rauber 1999). In 2011, 640 hospitals had an affiliated arrangement with a health plan (Myers 2013). Three underlying forces are expected to create another upward trend in the membership growth of existing provider plans as well as the development of new ones. First, the passage of the Affordable Care Act (ACA) in 2010 contained provisions intended to expand commercial and Medicaid health insurance coverage to underand uninsured populations. The second force is the advent of value-based payment systems, which reimburse through fixed fees to co ordinate patient care for a set of services as long as quality standards are met. Third, the movement by employers to give their employees defined dollar amounts to buy coverage and select a health plan will create a competitive consumerfocused insurance market. Under this type of market, local health care systems may be appealing to consumers because of their brand name, lower ABSTRACT Purpose: The aim of this study was to assess the performance of health plans sponsored by provider organizations, with respect to plans generating strong positive cash flow relative to plans generating weaker cash flow. A secondary aim was to assess their capital adequacy. Design: The study identified 24 provider-sponsored health plans (PSHPs) with an average positive cash flow margin from 2011 through 2013 at or above the top 75th percentile, defined as strong cash flow PSHPs. This group was compared with 72 PSHPs below the 75th percentile, defined as weak cash flow PSHPs. Methodology: Atlantic Information Services Directory of Health Plans was used to identify the PSHPs. Financial ratios were computed from 2013 National Association of Insurance Commissioners Financial Filings. The study conducted a t test mean comparison between strong and weak cash flow PSHPs across an array of financial performance and capital adequacy measures. Results: In 2013, the strong cash flow PSHPs averaged a cash-flow margin ratio of 6.6%. averaged a cash-flow margin of 0.4%. The net worth capital position of both groups was more than 4.5 times authorized capital. Conclusion: The operational analysis shows that strong cash-flow margin PSHPs are managing their medical costs to achieve this position. Although their medical loss ratio increased by almost 300 basis points from 2011 to 2013, it was still statistically significantly lower than the weaker cash flow PSHP group (P<.001). In terms of capital adequacy, both strong and weak cash-flow margin PSHP groups possessed sufficient capital to ensure the viability of these plans. premiums, and access to a network of providers. As a result of these forces, more health care systems are expected to acquire or form a health plan or, in the case of existing PSHPs, expand into the commercial or Medicaid markets. A recent analysis of PSHPs from 2011 through 2013 indicates that 10 health care systems have either started a new plan or have acquired an existing one (Myers 2013). Given this changing environment for existing and startup PSHPs, health care providers and policy makers would want to gain insight into how well these health plans are performing financially. The aim of this study is to assess the financial performance of health plans owned, affiliated with, or sponsored by providers. Providers include hospitals, health systems, and physician groups. Given the expansion of commercial products on both public and private exchanges and the competition from national publicly traded health insurers, such as Aetna, Cigna, United- Healthcare Group, and Anthem and Blue Cross Blue Shield plans, the study focuses on the financial performance and capital adequacy of provider-sponsored organizations (PSOs) JUNE 2015 / MANAGED CARE 39
2 offering a commercial product. This study identifies PSHPs that are participating in commercial insurance markets and are generating high positive cash flow from operations relative to those with weaker cash flows. Secondarily, this study seeks to assess the capital adequacy of PSOs with high cash flows. Capital adequacy is critical in financing the expansion of commercial health insurance markets as well as expanding into government markets. A study of this nature will also identify the financial and operational drivers of PSHPs that are financially strong. In turn, financially weaker PSHPs can utilize these findings to turn around their performance. More importantly, providers either starting or launching a new PSHP can evaluate these performance indicators to gain an understanding of the underlying factors for financial success. METHODS To identify the population of health plans sponsored or affiliated with providers (both hospitals and physician groups), the study references the AIS (Atlantic Information Services) Directory of Health Plans for 2014, which samples 2013 plan data. This database listed 71 PSOs that offered a commercial product. The AIS Directory also included 5 PSHPs in California that do not report their financial filings to the National Association of Insurance Commissioners (NAIC). Funding source: None Disclosures: None Corresponding author: Michael J. McCue, DBA R. Timothy Stack Professor Department of Health Administration PO Box Virginia Commonwealth University Richmond, VA Telephone: (804) Fax: (804) mccue@vcu.edu Key points In health plans with strong cash flows, lower medical loss ratios appear to be the underlying reason for healthy cash flow, although medical loss ratios have increased (from 83.5% in 2011 to 86.4% in 2013). The profit margin ratio of provider-sponsored health plans with strong cash flows declined from 2.5% in 2011 to 0.4% in Rising medical loss ratios may be the reason for the decline. In 2013, the average risk-based capital (RBC) ratio for the strong cash flow group was significantly higher (5.75 vs 4.68) than it was for the weak cash flow group in The RBC ratio for both groups was well above the insurance regulator threshold of 1.5. It appears that provider-sponsored health plans have the capital necessary to finance expansion into commercial markets and government programs. California s Department of Managed Health Care does not required managed care plans to submit financial filings to NAIC. Excluding the 5 PSHPs from California resulted in a total of 66 PSHPs. Within the NAIC data, state regulations for PPO and HMO products may require a health system to have separate legal entities and financial filings for health systems offering a HMO and PPO product. As a result, this study identified from the NAIC filings 104 PSHPs in 2013 and 19 health care providers sponsoring more than 1 plan. Because state and federal regulators view health plans with >1000 members as credible plans, the study excluded 6 PSO plans with less than 1000 members in In addition, the study excluded 2 plans with missing financial data from 2012 and 2011, resulting in a final sample of 96 plans. Risk-based capital (RBC) ratio is the primary ratio analyzed by state insurance examiners to assess solvency and is defined as the health plan s total adjusted capital divided by its authorized control capital or minimum capital level. Total adjusted capital reflects a health plan s state-authorized control capital plus its surplus or net worth capital. However, state examiners, as well as credit rating companies such as A.M. Best (2014), also assess performance ratios of health insurers. Cash flow margin ratio is a key ratio because changes in cash flow can increase or decrease the health insurer s capital position (DHCFP 2010). Cash flow margin ratio is defined as cash flow from operations as a percentage Glossary Administrative cost ratio Percentage of premium dollars spent on administrative expenses. Cash-flow margin ratio Cash flow from operations as a percentage of total revenues. Medical loss ratio Percentage of premium dollars spent on medical expenses. Profit margin ratio Profit (total revenues minus medical and administrative costs) as a percentage of total revenues. Risk-based capital ratio Total capital (as determined by a formula) divided by the capital adjusted for risk (also determined by a formula). Provider-sponsored health plans with an average cash flow margin in the top 25th percentile. Provider-sponsored health plans with an average cash flow margin in the bottom 25th percentile. 40 MANAGED CARE / JUNE 2015
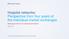
3 can be paid off by selling its assets, and it is viewed as a liquidity measure because the majority of health insurers assets is invested in securities. The capital/surplus PMPM (capital PMPM) assesses how much capital is accounted for by its membership base. These financial ratios were comof total revenues. A.M. Best considers an array of other performance ratios and capital-adequacy ratios in assigning a rating to a health insurer. These ratios include the medical loss ratio, which measures percentage of premium dollars spent on medical expenses, and the administrative cost ratio, which measures the percentage of premium dollars spent on administrative expenses. Finally, for the profit margin ratio, profits are defined as total revenues minus medical costs and administrative costs and were measured as percentage of total revenues (A.M. Best 2014). In addition, the credit rating agency measures capital adequacy measures. As previously mentioned, RBC is one measure. This study included 2 other adequacy ratios, total liabilities to total assets and capital and surplus per member per month (PMPM). The total liabilities to total asset ratio measures what percentage of its liabilities Strong vs weak Average risk-based capital (RBC) ratios of strong cash flow health plans vs weak cash flow plans puted from 2013 NAIC financial filings, which list key financial accounts from 2011 through 2013 from a statement called the Five-Year Historical Data. For the performance ratios, the form includes only total revenue and not premium revenue; therefore, this value may be slightly overvalued be RBC 2011 RBC 2012 RBC 2013 Table 1 Mean and standard deviation for financial performance ratios of strong cash flow margin PSHPs vs weak cash flow margin PSHPs, (n=24) (n=72) Mean SD Mean SD P value 2013 plans Medical loss ratio 86.4% 4.85% 90.3% 5.85% <.001 Administrative costs ratio 13.1% 6.38% 12.2% 4.75%.52 Profit margin ratio 0.4% 6.46% 2.5% 6.48%.04 Cash flow margin ratio 6.6% 6.4% 0.4% 5.20 % < plans Medical loss ratio 83.5% 7.28% 90.8% 7.58% <.001 Administrative costs ratio 14.1% 6.72% 11.7% 3.90%.03 Profit margin ratio 2.3% 7.80% 2.6% 7.30%.01 Cash flow margin ratio 5.9% 6.90% 1.6% 6.20% < plans Medical loss ratio 83.5% 5.28% 89.1% 5.79% <.001 Administrative costs ratio 13.9% 6.98% 11.5% 4.18%.04 Profit margin ratio 2.5% 7.63% 0.6% 5.79%.03 Cash flow margin ratio 6.5% 5.40% 0.1% 3.90% <.001 SD=standard deviation. JUNE 2015 / MANAGED CARE 41
4 cause it includes other minor accounts such as premium reserves and other nonhealth revenues. To assess PSHPs generating high cash flow, the study first measured their cash flow margin ratio from 2011 through 2013, which was defined as cash flow from operations divided by total revenue, and computed its average value for each health plan. Because the aim of the study was to identify PSHPs that were performing well financially, the study classified PSHPs with an average cash flow margin in the top 25th percentile, which was 3.9%, and defined them as strong cash flow PSHPs. The study identified 24 high cash flow margin PSHPs. The comparison group was identified as PSHPs with an average cash flow margin in the bottom 25th percentile and included 72 PSHPs that were defined as weak cash flow margin PSHPs. The high cash flow margin group each year had PSHPs with outlier values for cash flow margin, which increased variation of this measure. The study adjusted these outlier values to the RESULTS Table 1 (page 41) shows the findings from 2011 through 2013 for the performance measures. For the PSHPs generating strong cash flow, the cash flow margin ratio was 6.5% in 2011 but declined slightly to 5.9% in In 2013, however, the ratio increased to 6.6%. For PSHPs generating weak cash flow (PSHPs below the 75th percentile), cash flow was 0.09% in 2011 but declined to a cash flow operating loss of 1.6% in In 2013, these plans reduced their cash flow operating loss and generated a cash flow margin of 0.4%. For all 3 years, as expected, the 75th percentile PSHPs generated a significantly higher cash flow margin (P<.01). In the strong cash flow margin group, lower medical loss ratios aptop 99th percentile and bottom first percentile values. The statistical analysis was conducted using t test mean comparison between strong cash flow PSHPs and weak cash flow PSHPs for an array of financial performance and capital adequacy measures. The average membership over the 3-year period for the group with cash flow margin above the 75th percentile was 150,710, which was higher than the average membership of 113,400 for the comparison PSHP group. Thus, high cash flow margin PSHPs were larger in size than weak cash flow margin PSHPs. To identify the health insurance markets in which PSHPs offered products, as well as the membership in these markets, the study collected 2013 health insurers data. In 2013, the percentage of total membership in Medicare, Medicaid, and commercial markets for the strong cash flow PSHPs was 10% for Medicare, 27% for Medicaid, and 63% for commercial. The comparison group market percentages were 11% for Medicare, 14% for Medicaid, and 75% for commercial. Thus, the strong cash flow PSHPs insured a higher percentage of Medicaid members and a lesser percentage of commercial members than the comparison group. Table 2 Mean and standard deviation for capital adequacy ratios of strong cash flow margin PSHPs vs weak cash flow margin PSHPs, (n=24) (n=72) Mean SD Mean SD P Value 2013 plans Risk-based capital ratio Liabilities to total assets 46.2% 19.73% 49.20% 13.28%.411 Total capital PMPM $ $ $73.60 $ plans Risk-based capital ratio <.001 Liabilities to total assets 42.2% 16.08% 49.40% 14.97%.04 Total capital PMPM $ $ $68.70 $ plans Risk-based capital ratio <.001 Liabilities to total assets 38.4% 18.08% 50.50% 14.74%.01 Total capital PMPM $ $ $61.10 $41.60 <.001 PMPM=per member per month, SD=standard deviation. 42 MANAGED CARE / JUNE 2015
5 3 years, the decline in the RBC ratio may stem from an increase in regulated authorized capital (numerator of the RBC ratio) or outflow of capital to the sponsored provider organization (denominator of the RBC ratio). For the liquidity measure of total liabilities to total assets, the strong cash flow group experienced a rise in liabilities relative to total assets. In 2011, liabilities accounted for 38% of total assets, while in 2013 the percentage of total liabilities covered by total assets increased to 46%. For the weak cash flow group, the percentage of total liabilities covered by total assets was around 50% for all 3 years. The final ratio of total capital PMPM reflects a significantly higher amount of capital covering the insured base for the strong cash flow group relative to the weak cash flow group (P<.001 [2011], P=.02 [2012], P=.03 [2013]). From 2011 to 2013, the strong cash flow PSHP group s total capital PMPM increased by almost $44 PMPM, to $153 PMPM, while the weak cash flow PSHP group s total capital PMPM grew by only $12 PMPM, to $73.60 PMPM. There were several limitations to this study. First, the study sample excluded 5 PSHPs from California because they were not required to submit their financial data to NAIC. Second, the sample includes only PSHPs that offer a commercial product. Therefore, the sample excludes PSHPs that insure members covered by Medicare, Medicaid, or both. The Medicaid PSHPs typically are affiliated with safety net providers or major academic medical centers. Finally, the mean comparison/ univariate analysis design does not control for external factors, such as competition from national health insurers, size of commercial insurance market, and type of insurance plan (HMO vs PPO). Given the descriptive mean difference analysis of the study, it is diffipear to be the underlying reason for higher cash flow. In 2011 and 2012, this group s average medical loss ratio was 83.5%. The average medical loss ratio in weak cash flow groups was 89.1% in 2011 and 90.8% in In 2013, however, for the strong cash flow group, the medical loss ratio increased by almost 3 percentage points, from 83.5% in 2012 to 86.4% in Despite this rise, the 2013 medical loss ratio value was still significantly lower than that for the weak cash flow group (90.3%, P<.01). The administrative cost ratio for the strong cash flow PSHP group was significantly higher than the comparison groups for 2011 and 2012 (P=.03). In addition, this group s administrative ratio declined from 14.1% in 2012 to 13.1% in The weak cash flow PSHP group administrative cost ratio rose from 11.5% in 2011 to 12.2% in 2013 and was no longer significantly different from the higher cash flow group (P=.04). In terms of profit margin ratios, the strong cash flow group experienced a decline in the profit margin ratio from 2011 to The ratio was 2.5% in 2011 and declined to 0.4% in 2013, which may stem from rising medical loss ratio. For the weak cash flow group, the profit margin declined from 0.6% in 2011 to 2.5% and 2.6%, respectively, in 2012 and For all 3 years, the strong cash flow group had significantly higher profit margin than the comparison group (P=.03 [2011], P=.01 [2012], P=.04 [2013]). Table 2 presents the findings for the capital adequacy ratios for 2011 through The RBC ratio declined for the strong cash flow group from 7.44 in 2011 to 5.75 in The RBC ratio for the weak cash flow group was significantly lower and increased slightly from 4.26 in 2011 to 4.68 in 2013 (P<.001, P=.02). Although the strong cash flow group generated higher cash flow over the cult to tease out other effects related to market and demand factors. An extension of the study would involve a multivariate analysis, which could attempt to control for market effects on the mean values. DIscussion There are several underlying reasons health care providers are either expanding their existing insurance products or starting a new health insurance entity. The first reason relates to the onset of ACA regulation in offering affordable commercial health insurance plans on public exchanges. These plans are made affordable by offering tax subsidies for low-income enrollees who are uninsured and under insured on the public health insurance exchange (Claxton 2015). The second reason stems from insurers movements toward narrower provider networks and value-based purchasing payment arrangements with providers (Herman 2015). Given this change in the business model of health care, health policy makers, employers, and health care provider systems will have an interest in knowing how health care systems with existing health plans are performing financially. This study identified a sample of 96 PSHPs in 2013 and computed key financial ratios to measure their financial performance and capital adequacy from 2011 through The study identified 24 PSHPs that generated an average cash flow margin ratio of 3.9%, which was above the 75th percentile of this ratio. The analysis shows that strong cash flow margin PSHPs are managing their medical costs to achieve this position. Although their medical loss ratio increased by almost 300 basis points from 2011 to 2013, it was still lower than the weak cash flow PSHP group. In terms of capital position, both groups had high RBC ratios. State in- JUNE 2015 / MANAGED CARE 43
6 surance regulators assess this ratio to gauge the overall risk of bankruptcy for the health plan. The ratio accounts for a range of risk factors, including risk of default of reinsurers and other creditors, risk of investments, fixed income and equity, and its underwriting risk of its reserves and premiums. Health plans with RBC ratios valued below 1.5 will be required by state insurers to take correction action. Conclusion This study found the overall capital adequacy of both groups to be financially sound. Although the average RBC ratio for the strong cash flow PSHP group was significantly higher (5.75 vs 4.68) than the weak cash flow PSHP group (P=.02), the ratio value for both groups was well above the regulator threshold. The other capital adequacy of total liabilities to total assets was only slightly lower for the strong cash flow PSHP group relative to its comparison group. This finding implies that either group can pay off its liabilities with less than half its assets. Given this assessment, it appears PSHPs have sufficient capital to finance expansion into the commercial markets as well as government programs. Initially, PSHPs entering these new markets may experience capital shortfalls in cash flow from underpricing products and higher medical costs. However, some of the larger regional health care systems are financially strong with sufficient cash and investments on hand to lend to their health plan (McCue 2010) in case they face financial difficulties. References A.M. Best Co. Understanding BCAR for U.S. and Canadian life/health insurers. A.M. Best Methodology: Criteria-Life/Health. April 2, www3.ambest.com/ ambv/ratingmethodology/openpdf. aspx?rc= Accessed May 7, DHCFP (Division of Health Care Finance and Policy). Study of the reserves and capital of health insurers in Massachusetts. May archives.lib.state.ma.us/bitstream/ handle/2452/201830/ocn pdf?sequence=2&isallowed=y. Accessed May 7, Claxton G, Cox C, Rae M. The cost of care with marketplace coverage. Henry J. Kaiser Family Foundation. February 11, issue-brief/the-cost-of-care-withmarketplace-coverage. Accessed May 7, Herman B, Evans M. Transformers push to modify pay must overcome legacy system. Mod Healthc Feb 2;45(5):8,10. McCue MJ. What determines hospital sponsorship of an HMO? Inquiry. 2000;37(3): McCue MJ. A descriptive analysis of the 2008 credit crisis on multistate healthcare systems: what impact did it have on their financial performance? Hosp Top. 2010;88(2): Myers C, Fleming K, Newell B. Providersponsored health plans: past, present and future. Navigant Pulse. Aug. 21, Accessed May 7, NAIC (National Association of Insurance Commissioners) Quarterly, Financial Analysis Handbook, Health Edition. Kansas City, MO: NAIC. Rauber C. Market deflates for providerowned HMOs. Survey shows many plans are losing ground to growing national and regional players. Mod Healthc. 1999;29(24):34 38,40 44, MANAGED CARE / JUNE 2015
Lessons Learned, What s Next
 Provider Sponsored Risk: Lessons Learned, What s Next AHA Leadership Summit July 28, 2017 San Diego Paul H. Keckley, Ph.D. The Keckley Report Provider-Sponsored Risk: The Big Picture Realities: Insurers
Provider Sponsored Risk: Lessons Learned, What s Next AHA Leadership Summit July 28, 2017 San Diego Paul H. Keckley, Ph.D. The Keckley Report Provider-Sponsored Risk: The Big Picture Realities: Insurers
Issue Brief. Insurers Medical Loss Ratios and Quality Improvement Spending in Mark A. Hall and Michael J. McCue OVERVIEW
 March 2013 Issue Brief Insurers Medical Loss Ratios and Quality Improvement Spending in 2011 Mark A. Hall and Michael J. McCue The mission of The Commonwealth Fund is to promote a high performance health
March 2013 Issue Brief Insurers Medical Loss Ratios and Quality Improvement Spending in 2011 Mark A. Hall and Michael J. McCue The mission of The Commonwealth Fund is to promote a high performance health
Realizing Health Reform s Potential
 The COMMONWEALTH FUND Realizing Health Reform s Potential AUGUST 2015 Comparing Individual Health Coverage On and Off the Affordable Care Act s Insurance Exchanges Michael J. McCue and Mark A. Hall The
The COMMONWEALTH FUND Realizing Health Reform s Potential AUGUST 2015 Comparing Individual Health Coverage On and Off the Affordable Care Act s Insurance Exchanges Michael J. McCue and Mark A. Hall The
CENTER FOR HEALTH INFORMATION AND ANALYSIS PERFORMANCE OF THE MASSACHUSETTS HEALTH CARE SYSTEM PRIVATE COMMERCIAL CONTRACT ENROLLMENT COVERAGE COSTS
 CENTER FOR HEALTH INFORMATION AND ANALYSIS PERFORMANCE OF THE MASSACHUSETTS HEALTH CARE SYSTEM PRIVATE COMMERCIAL CONTRACT ENROLLMENT COVERAGE COSTS COST-SHARING PAYER USE OF FUNDS TECHNICAL APPENDIX 2018
CENTER FOR HEALTH INFORMATION AND ANALYSIS PERFORMANCE OF THE MASSACHUSETTS HEALTH CARE SYSTEM PRIVATE COMMERCIAL CONTRACT ENROLLMENT COVERAGE COSTS COST-SHARING PAYER USE OF FUNDS TECHNICAL APPENDIX 2018
New York s Medicare Advantage Market,
 S P E C I A L S U P P L E M E N T T O T H E B I G P I C T U R E V New York s Medicare Advantage Market, 2010 2012 Peter Newell, Health Insurance Project Director, United Hospital Fund Allan Baumgarten,
S P E C I A L S U P P L E M E N T T O T H E B I G P I C T U R E V New York s Medicare Advantage Market, 2010 2012 Peter Newell, Health Insurance Project Director, United Hospital Fund Allan Baumgarten,
The medical loss ratio is a key financial. Impact Of Medical Loss Regulation On The Financial Performance Of Health Insurers. Medical Loss Regulation
 Medical Loss Regulation doi: 10.1377/hlthaff.2012.1316 HEALTH AFFAIRS 32, NO. 9 (2013): 1546 1551 2013 Project HOPE The People-to-People Health Foundation, Inc. By Michael McCue, Mark Hall, and Xinliang
Medical Loss Regulation doi: 10.1377/hlthaff.2012.1316 HEALTH AFFAIRS 32, NO. 9 (2013): 1546 1551 2013 Project HOPE The People-to-People Health Foundation, Inc. By Michael McCue, Mark Hall, and Xinliang
EXECUTIVE SUMMARY ENROLLMENT GROWS YET MARGINS DROP FOR OHIO S HEALTH INSURING CORPORATIONS. 970,000 Ohioans remained uninsured in 2014.
 OHA exists to collaborate with member hospitals and health systems to ensure a healthy Ohio. February 2016 EXECUTIVE SUMMARY ENROLLMENT GROWS YET MARGINS DROP FOR OHIO S HEALTH INSURING CORPORATIONS In
OHA exists to collaborate with member hospitals and health systems to ensure a healthy Ohio. February 2016 EXECUTIVE SUMMARY ENROLLMENT GROWS YET MARGINS DROP FOR OHIO S HEALTH INSURING CORPORATIONS In
Plan Management Navigator
 Plan Management Navigator Analytics for Health Plan Administration July 2016 Healthcare Analysts Douglas B. Sherlock, CFA sherlock@sherlockco.com Christopher E. de Garay cgaray@sherlockco.com Erin Ottolini
Plan Management Navigator Analytics for Health Plan Administration July 2016 Healthcare Analysts Douglas B. Sherlock, CFA sherlock@sherlockco.com Christopher E. de Garay cgaray@sherlockco.com Erin Ottolini
Medicaid managed care financial results for 2017
 Medicaid managed care financial results for 2017 May 2018 Jeremy D. Palmer, FSA, MAAA Christopher T. Pettit, FSA, MAAA Ian M. McCulla, FSA, MAAA Table of Contents INTRODUCTION...1 TEN YEARS OF ANALYSIS...3
Medicaid managed care financial results for 2017 May 2018 Jeremy D. Palmer, FSA, MAAA Christopher T. Pettit, FSA, MAAA Ian M. McCulla, FSA, MAAA Table of Contents INTRODUCTION...1 TEN YEARS OF ANALYSIS...3
Key Trends within the Individual and Small Group Health Insurance Segments
 Key Trends within the Individual and Small Group Health Insurance Segments 5/26/2016 by Mark Farrah Associates With two full years of health insurance activity under the Affordable Care Act (ACA), some
Key Trends within the Individual and Small Group Health Insurance Segments 5/26/2016 by Mark Farrah Associates With two full years of health insurance activity under the Affordable Care Act (ACA), some
Session 99AB Provider-Sponsored Health Plans Are Increasing in Number: What Leaders Need to Know
 Prepared for the Foundation of the American College of Healthcare Executives Session 99AB Provider-Sponsored Health Plans Are Increasing in Number: What Leaders Need to Know Presented by: Bruce Henderson
Prepared for the Foundation of the American College of Healthcare Executives Session 99AB Provider-Sponsored Health Plans Are Increasing in Number: What Leaders Need to Know Presented by: Bruce Henderson
How Bundled Payments Create Value in New Product Designs Cognizant
 How Bundled Payments Create Value in New Product Designs 1 About Cognizant 2 This Will Not Take Long. 3 What is a Health Insurance Product? 4 Understanding Product Design Commercial Insurance One specific
How Bundled Payments Create Value in New Product Designs 1 About Cognizant 2 This Will Not Take Long. 3 What is a Health Insurance Product? 4 Understanding Product Design Commercial Insurance One specific
2016 individual market losses are in the high single digits a slight improvement from 2015
 June 2017 2016 individual market losses are in the high single digits a slight improvement from 2015 Jim Oatman, Erica Coe A new McKinsey analysis suggests that overall carrier losses in the individual
June 2017 2016 individual market losses are in the high single digits a slight improvement from 2015 Jim Oatman, Erica Coe A new McKinsey analysis suggests that overall carrier losses in the individual
Anthem Blue Cross. CCHCA Physician Handbook (7 th Edition)
 Part II Section B Introduction 1 Verifying Member Eligibility and Benefits 1 Sample Member ID Card 2 Eligibility Certification Form 3 CCHCA Physician Handbook (7 th Edition) INTRODUCTION, created in 1986
Part II Section B Introduction 1 Verifying Member Eligibility and Benefits 1 Sample Member ID Card 2 Eligibility Certification Form 3 CCHCA Physician Handbook (7 th Edition) INTRODUCTION, created in 1986
Hospital networks: Perspective from four years of the individual market exchanges
 Hospital networks: Perspective from four years of the individual market exchanges McKinsey Center for U.S. Health System Reform May 017 Any use of this material without specific permission of is strictly
Hospital networks: Perspective from four years of the individual market exchanges McKinsey Center for U.S. Health System Reform May 017 Any use of this material without specific permission of is strictly
Oxford Health Plans (NY), Inc.
 Oxford Health Plans (NY), Inc. Statutory Basis Financial Statements as of and for the Years Ended December 31, 2014 and 2013, Supplemental Schedules as of and for the Year Ended December 31, 2014, Independent
Oxford Health Plans (NY), Inc. Statutory Basis Financial Statements as of and for the Years Ended December 31, 2014 and 2013, Supplemental Schedules as of and for the Year Ended December 31, 2014, Independent
The Health Insurance Market in Virginia. Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017
 The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
HEALTH SERVICE SYSTEM OTHER EMPLOYEE BENEFIT TRUST FUND CITY AND COUNTY OF SAN FRANCISCO. Financial Statements. June 30, 2016 and 2015
 Financial Statements (With Independent Auditors Report Thereon) TABLE OF CONTENTS Page Independent Auditors Report 1 Management s Discussion and Analysis 3 Basic Financial Statements: Statements of Net
Financial Statements (With Independent Auditors Report Thereon) TABLE OF CONTENTS Page Independent Auditors Report 1 Management s Discussion and Analysis 3 Basic Financial Statements: Statements of Net
HEALTH CARE REFORM Focus on Group Coverage Blue Cross and Blue Shield of Minnesota. All rights reserved.
 HEALTH CARE REFORM Focus on Group Coverage 2011 Blue Cross and Blue Shield of Minnesota. All rights reserved. Current Insurance Coverage Environment Minnesota United States Uninsured 9% Ot her Public 1%
HEALTH CARE REFORM Focus on Group Coverage 2011 Blue Cross and Blue Shield of Minnesota. All rights reserved. Current Insurance Coverage Environment Minnesota United States Uninsured 9% Ot her Public 1%
Oxford Health Plans (NJ), Inc.
 Oxford Health Plans (NJ), Inc. Statutory Basis Financial Statements as of and for the Years Ended December 31, 2014 and 2013, Supplemental Schedules as of and for the Year Ended December 31, 2014, Independent
Oxford Health Plans (NJ), Inc. Statutory Basis Financial Statements as of and for the Years Ended December 31, 2014 and 2013, Supplemental Schedules as of and for the Year Ended December 31, 2014, Independent
Individual Insurance Market Performance in Mid- 2018
 October 2018 Issue Brief Individual Insurance Market Performance in Mid- 2018 Rachel Fehr, Cynthia Cox and Larry Levitt Despite concerns about the stability of the individual insurance market under the
October 2018 Issue Brief Individual Insurance Market Performance in Mid- 2018 Rachel Fehr, Cynthia Cox and Larry Levitt Despite concerns about the stability of the individual insurance market under the
A MERICAN ACADEMY of ACTUARIES
 A MERICAN ACADEMY of ACTUARIES Actuarial Solvency Issues of Health Plans in the United States February 1994 Monograph Number Four M O N O G R A P H S E R I E S O N H E A L T H C A R E R E F O R M A MERICAN
A MERICAN ACADEMY of ACTUARIES Actuarial Solvency Issues of Health Plans in the United States February 1994 Monograph Number Four M O N O G R A P H S E R I E S O N H E A L T H C A R E R E F O R M A MERICAN
Plan Management Navigator
 Plan Management Navigator Analytics for Health Plan Administration September 2016 Healthcare Analysts Douglas B. Sherlock, CFA sherlock@sherlockco.com Christopher E. de Garay cgaray@sherlockco.com Erin
Plan Management Navigator Analytics for Health Plan Administration September 2016 Healthcare Analysts Douglas B. Sherlock, CFA sherlock@sherlockco.com Christopher E. de Garay cgaray@sherlockco.com Erin
Health Enrollment Trends and Market Outlook
 Health Enrollment Trends and Market Outlook 6/30/2015 by Mark Farrah Associates Following the Supreme Court ruling to uphold the ACA's federal subsidies, the healthcare industry is now bracing for a potential
Health Enrollment Trends and Market Outlook 6/30/2015 by Mark Farrah Associates Following the Supreme Court ruling to uphold the ACA's federal subsidies, the healthcare industry is now bracing for a potential
Public and Private Payer Responses to Pharmaceutical Pricing in the United States
 Public and Private Payer Responses to Pharmaceutical Pricing in the United States James C. Robinson Leonard D. Schaeffer Professor of Health Economics Director, Berkeley Center for Health Technology University
Public and Private Payer Responses to Pharmaceutical Pricing in the United States James C. Robinson Leonard D. Schaeffer Professor of Health Economics Director, Berkeley Center for Health Technology University
Session 34 PD, Healthcare Exchanges: Case Studies in the ACA. Moderator: William James Swacker II, FSA, MAAA
 Session 34 PD, Healthcare Exchanges: Case Studies in the ACA Moderator: William James Swacker II, FSA, MAAA Presenters: David G. Hayes, FSA, MAAA Michael N. Muldoon, ASA, FCA, MAAA William James Swacker
Session 34 PD, Healthcare Exchanges: Case Studies in the ACA Moderator: William James Swacker II, FSA, MAAA Presenters: David G. Hayes, FSA, MAAA Michael N. Muldoon, ASA, FCA, MAAA William James Swacker
Massachusetts Risk Adjustment Program: Executive Summary
 Massachusetts Risk Adjustment Program: Executive Summary Introduction Wakely Consulting Group, Inc. has been retained by issuers in the Massachusetts market to review the methodology of the Massachusetts
Massachusetts Risk Adjustment Program: Executive Summary Introduction Wakely Consulting Group, Inc. has been retained by issuers in the Massachusetts market to review the methodology of the Massachusetts
2015 Small Group Health Insurance Market
 2015 Small Group Health Insurance Market 6/30/2016 by Mark Farrah Associates In 2015, small group health insurers provided coverage for 13.537 million people through policies written within 1.088 million
2015 Small Group Health Insurance Market 6/30/2016 by Mark Farrah Associates In 2015, small group health insurers provided coverage for 13.537 million people through policies written within 1.088 million
Health Insurance Cost Report. The Colorado General Assembly. for. Calendar year in accordance with (4)(c) & (d), C.R.S.
 Health Insurance Cost Report to The Colorado General Assembly for Calendar year 2015 in accordance with 10-16-111(4)(c) & (d), C.R.S. Published January 3, 2016 Marguerite Salazar Commissioner January 3,
Health Insurance Cost Report to The Colorado General Assembly for Calendar year 2015 in accordance with 10-16-111(4)(c) & (d), C.R.S. Published January 3, 2016 Marguerite Salazar Commissioner January 3,
Medicare Advantage: Program Overview and Recent Experience. James Cosgrove, Ph.D. Director, Health Care U.S. Government Accountability Office
 Medicare Advantage: Program Overview and Recent Experience James Cosgrove, Ph.D. Director, Health Care U.S. Government Accountability Office January 15, 2009 01/15/2009 1 In 2008, About 22 Percent of Medicare
Medicare Advantage: Program Overview and Recent Experience James Cosgrove, Ph.D. Director, Health Care U.S. Government Accountability Office January 15, 2009 01/15/2009 1 In 2008, About 22 Percent of Medicare
Healthcare Reform Will Accelerate the Move to Self-Insured Products
 A Decision Resources, Inc. Company e x e c u t i v e b r i e f i n g Healthcare Reform Will Accelerate the Move to Self-Insured Products By Jane DuBose Employers eager to stem rising healthcare benefit
A Decision Resources, Inc. Company e x e c u t i v e b r i e f i n g Healthcare Reform Will Accelerate the Move to Self-Insured Products By Jane DuBose Employers eager to stem rising healthcare benefit
The Value of Health Plan Networks January 28 th, 2016
 The Texas Association of Health Plans The Value of Health Plan Networks January 28 th, 2016 JAMIE DUDENSING, CEO The Texas Association of Health Plans The Texas Association of Health Plans (TAHP) is the
The Texas Association of Health Plans The Value of Health Plan Networks January 28 th, 2016 JAMIE DUDENSING, CEO The Texas Association of Health Plans The Texas Association of Health Plans (TAHP) is the
Aetna 2001 Annual Report, Financial Report
 Aetna 2001 Annual Report, Financial Report AETNA ANNUAL REPORT, FINANCIAL REPORT 2001 Management s Discussion and Analysis Overview 2 Health Care 5 Group Insurance 12 Large Case Pensions 14 Corporate Interest
Aetna 2001 Annual Report, Financial Report AETNA ANNUAL REPORT, FINANCIAL REPORT 2001 Management s Discussion and Analysis Overview 2 Health Care 5 Group Insurance 12 Large Case Pensions 14 Corporate Interest
shared responsibility
 A report from the Blue Cross Blue Shield of Massachusetts Foundation. March 2009 shared responsibility Government, Business, and Individuals: Who pays what for health reform? Prepared by: Robert Seifert,
A report from the Blue Cross Blue Shield of Massachusetts Foundation. March 2009 shared responsibility Government, Business, and Individuals: Who pays what for health reform? Prepared by: Robert Seifert,
PRICE TRANSPARENCY Frequently Asked Questions
 PRICE TRANSPARENCY Frequently Asked Questions Introduction Price transparency is one of the most confusing topics in today s healthcare world. Healthcare consumers are becoming more engaged and asking
PRICE TRANSPARENCY Frequently Asked Questions Introduction Price transparency is one of the most confusing topics in today s healthcare world. Healthcare consumers are becoming more engaged and asking
Introduction. About Me
 Introduction About Me Worked for a brokerage firm founded in 1845 COBRA had just been written into law IRC Sec. 89 was passed 3 years later Medical plans had rates of $100 per month. Day Job: Founder &
Introduction About Me Worked for a brokerage firm founded in 1845 COBRA had just been written into law IRC Sec. 89 was passed 3 years later Medical plans had rates of $100 per month. Day Job: Founder &
HEALTH PLAN ADMINISTRATIVE COST TRENDS
 BLUE CROSS BLUE SHIELD ASSOCIATION HEALTH PLAN ADMINISTRATIVE COST TRENDS Prepared by: Kent J. Sacia Robert H. Dobson February 20, 2003 Table of Contents Executive Summary... 1 A. Introduction... 3 Purpose...
BLUE CROSS BLUE SHIELD ASSOCIATION HEALTH PLAN ADMINISTRATIVE COST TRENDS Prepared by: Kent J. Sacia Robert H. Dobson February 20, 2003 Table of Contents Executive Summary... 1 A. Introduction... 3 Purpose...
CHAPTER 2 The Financial Environment
 Copyright 2008 by the Foundation of the American College of Healthcare Executives 6/7/07 Version 2-1 CHAPTER 2 The Financial Environment Forms of business organization and ownership Taxes and financial
Copyright 2008 by the Foundation of the American College of Healthcare Executives 6/7/07 Version 2-1 CHAPTER 2 The Financial Environment Forms of business organization and ownership Taxes and financial
The Big Picture VI: New York s Private and Public Insurance Markets, 2014
 O C T O B E R 2 0 1 6 The Big Picture VI: New York s Private and Public Insurance Markets, 2014 The Big Picture VI: New York s Private and Public Insurance Markets, 2014 Prepared by Peter Newell Allan
O C T O B E R 2 0 1 6 The Big Picture VI: New York s Private and Public Insurance Markets, 2014 The Big Picture VI: New York s Private and Public Insurance Markets, 2014 Prepared by Peter Newell Allan
ACTUARIAL ASPECTS OF MASSACHUSETTS REFORM. Ian Duncan FSA FIA FCIA MAAA. New England Actuaries Club November 2012
 ACTUARIAL ASPECTS OF MASSACHUSETTS REFORM Ian Duncan FSA FIA FCIA MAAA New England Actuaries Club November 2012 Agenda 1. History and accomplishments of Massachusetts Reform 2. Actuarial Implications of
ACTUARIAL ASPECTS OF MASSACHUSETTS REFORM Ian Duncan FSA FIA FCIA MAAA New England Actuaries Club November 2012 Agenda 1. History and accomplishments of Massachusetts Reform 2. Actuarial Implications of
Issue Brief. What s in the Stars? Quality Ratings of Medicare Advantage Plans, 2010
 Issue Brief What s in the Stars? Quality Ratings of Medicare Advantage Plans, 00 December 009 What s in the Stars? Quality Ratings of Medicare Advantage Plans, 00 The Centers for Medicare and Medicaid
Issue Brief What s in the Stars? Quality Ratings of Medicare Advantage Plans, 00 December 009 What s in the Stars? Quality Ratings of Medicare Advantage Plans, 00 The Centers for Medicare and Medicaid
CHAPTER 1. Trends in the Overall Health Care Market
 CHAPTER 1 Trends in the Overall Health Care Market Billions Chart 1.1: Total National Health Expenditures, 1980 2016 $4,000 $3,500 $3,000 $2,500 $2,000 $1,500 $1,000 $500 $0 Inflation Adjusted (2) 80 81
CHAPTER 1 Trends in the Overall Health Care Market Billions Chart 1.1: Total National Health Expenditures, 1980 2016 $4,000 $3,500 $3,000 $2,500 $2,000 $1,500 $1,000 $500 $0 Inflation Adjusted (2) 80 81
Key Indicators: Quarterly Enrollment Update
 Commonwealth of Massachusetts Deval L. Patrick Governor Timothy P. Murray Lieutenant Governor JudyAnn Bigby, M.D. Secretary Executive Office of Health and Human Services Key Indicators: Quarterly Enrollment
Commonwealth of Massachusetts Deval L. Patrick Governor Timothy P. Murray Lieutenant Governor JudyAnn Bigby, M.D. Secretary Executive Office of Health and Human Services Key Indicators: Quarterly Enrollment
REPORT OF THE COUNCIL ON MEDICAL SERVICE. Effects of the Massachusetts Reform Effort and the Individual Mandate
 REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -A-0 Subject: Presented by: Effects of the Massachusetts Reform Effort and the Individual Mandate David O. Barbe, MD, Chair 0 0 0 At the 00 Interim Meeting,
REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -A-0 Subject: Presented by: Effects of the Massachusetts Reform Effort and the Individual Mandate David O. Barbe, MD, Chair 0 0 0 At the 00 Interim Meeting,
Stuart H. Altman PhD
 The U.S. Healthcare Financing System: Where Is It Today and Where Is It Going Stuart H. Altman PhD Sol Chaikin Professor of National Health Policy The Heller School for Social Policy and Management Brandeis
The U.S. Healthcare Financing System: Where Is It Today and Where Is It Going Stuart H. Altman PhD Sol Chaikin Professor of National Health Policy The Heller School for Social Policy and Management Brandeis
Marc Claussen, Chiesi USA, Director, Market Access. Donna White, Chiesi USA, Sr. Director, Contracting and Compliance
 Marc Claussen, Chiesi USA, Director, Market Access Donna White, Chiesi USA, Sr. Director, Contracting and Compliance The views/observations expressed in this presentation are the personal views/observations
Marc Claussen, Chiesi USA, Director, Market Access Donna White, Chiesi USA, Sr. Director, Contracting and Compliance The views/observations expressed in this presentation are the personal views/observations
The Emergence of Value-Based Care: Present and Future Tense
 The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
Savings Generated by New York s Medicaid Pharmacy Reform
 Savings Generated by New York s Medicaid Pharmacy Reform Sponsored by: Pharmaceutical Care Management Association Prepared by: Special Needs Consulting Services, Inc. October 2012 Table of Contents I.
Savings Generated by New York s Medicaid Pharmacy Reform Sponsored by: Pharmaceutical Care Management Association Prepared by: Special Needs Consulting Services, Inc. October 2012 Table of Contents I.
RATE FILING DISCLOSURE
 Attachment Three Jt. Executive (EX) Committee/Plenary 12/16/10 Rate Filing Disclosure Form Background and Project Summary December 2010 Background State insurance regulators were asked to assist the Department
Attachment Three Jt. Executive (EX) Committee/Plenary 12/16/10 Rate Filing Disclosure Form Background and Project Summary December 2010 Background State insurance regulators were asked to assist the Department
The Effect of the ACA on Self-Funded Plans & Free Market Providers PRESENTED BY: Maria Robles Meyers, Esq. Health Law Advisors, PLLC August 21, 2015
 The Effect of the ACA on Self-Funded Plans & Free Market Providers PRESENTED BY: Maria Robles Meyers, Esq. Health Law Advisors, PLLC August 21, 2015 Glossary of Terms You have been provided a glossary
The Effect of the ACA on Self-Funded Plans & Free Market Providers PRESENTED BY: Maria Robles Meyers, Esq. Health Law Advisors, PLLC August 21, 2015 Glossary of Terms You have been provided a glossary
Medicare for All: Leaving No One Behind
 Medicare for All: Leaving No One Behind May, 206 Presidential candidate Bernie Sanders has designed a replacement for the Affordable Care Act (ACA), called Medicare for All: Leaving No One Behind. The
Medicare for All: Leaving No One Behind May, 206 Presidential candidate Bernie Sanders has designed a replacement for the Affordable Care Act (ACA), called Medicare for All: Leaving No One Behind. The
An Analysis of 2017 Medicare Business Competition
 An Analysis of 2017 Medicare Business Competition 10/14/2016 by Mark Farrah Associates The Annual Election Period (AEP), or open enrollment, for Medicare Advantage and prescription drug plans (PDPs) will
An Analysis of 2017 Medicare Business Competition 10/14/2016 by Mark Farrah Associates The Annual Election Period (AEP), or open enrollment, for Medicare Advantage and prescription drug plans (PDPs) will
Health Reform: Where Are We Now?
 Health Reform: Where Are We Now? Andrew Croshaw President, Leavitt Partners Consulting Geologic tectonic forces create our current landscape 2 November 13, 1963 South of Iceland 3 A new landscape emerges
Health Reform: Where Are We Now? Andrew Croshaw President, Leavitt Partners Consulting Geologic tectonic forces create our current landscape 2 November 13, 1963 South of Iceland 3 A new landscape emerges
Healthcare Reform CEEP Presentation
 Healthcare Reform CEEP Presentation Laurie Kazilionis Sr. Vice President Garth Howe Director Integrated Benefits Account Management & Sales February, 2014 / Atlanta Do Americans Understand the Affordable
Healthcare Reform CEEP Presentation Laurie Kazilionis Sr. Vice President Garth Howe Director Integrated Benefits Account Management & Sales February, 2014 / Atlanta Do Americans Understand the Affordable
UNIVERSAL HEALTHCARE COUNCIL 2013 OVERVIEW OF THE AFFORDABLE CARE ACT
 UNIVERSAL HEALTHCARE COUNCIL 2013 OVERVIEW OF THE AFFORDABLE CARE ACT Introduction The Patient Protection and Affordable Care Act (ACA) was signed into federal law on March 23, 2010. While many reforms
UNIVERSAL HEALTHCARE COUNCIL 2013 OVERVIEW OF THE AFFORDABLE CARE ACT Introduction The Patient Protection and Affordable Care Act (ACA) was signed into federal law on March 23, 2010. While many reforms
Coordination of Benefits (COB)
 Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
Page 1 of 5 Advanced Search Contact Us Employer Home Health & Wellness Plans & Benefits Answers@Anthem Communications Request a Quote Benefits Manager Services Click the Login button to View Group Information,
Health Care Reform Template Language for Employers
 Health Care Reform Template Language for Employers The health care reform law requires health insurance issuers and sponsors to provide certain notices to employees, either as a separate notice or as part
Health Care Reform Template Language for Employers The health care reform law requires health insurance issuers and sponsors to provide certain notices to employees, either as a separate notice or as part
Why HANYS opposes the American Health Care Act
 Why HANYS opposes the American Health Care Act. 3/14/2017 Slide 1 It is complex Slide 2 The Affordable Care Act Coverage Expansion and Comprehensive Benefits 3/14/2017 Slide 3 Insurance in America 3/14/2017
Why HANYS opposes the American Health Care Act. 3/14/2017 Slide 1 It is complex Slide 2 The Affordable Care Act Coverage Expansion and Comprehensive Benefits 3/14/2017 Slide 3 Insurance in America 3/14/2017
Comments of Aetna Inc. before the Joint Public Hearing of the Florida Office of Insurance Regulation And the Florida health Insurance Advisory Board
 Comments of Aetna Inc. before the Joint Public Hearing of the Florida Office of Insurance Regulation And the Florida health Insurance Advisory Board May 4, 2010 Mark LaBorde President, Jacksonville/Tampa
Comments of Aetna Inc. before the Joint Public Hearing of the Florida Office of Insurance Regulation And the Florida health Insurance Advisory Board May 4, 2010 Mark LaBorde President, Jacksonville/Tampa
Narrow, Tailored, Tiered and High Performance Networks: An Emerging Trend
 Narrow, Tailored, Tiered and High Performance Networks: An Emerging Trend Bill Eggbeer, Managing Director, and Dudley Morris, Senior Advisor, BDC Advisors, LLC Executive Summary A recent BDC survey of
Narrow, Tailored, Tiered and High Performance Networks: An Emerging Trend Bill Eggbeer, Managing Director, and Dudley Morris, Senior Advisor, BDC Advisors, LLC Executive Summary A recent BDC survey of
Health Benefits Briefing
 Health Benefits Briefing Teacher Retirement System of Texas December 7, 2016 Copyright 2015 GRS All rights reserved. TRS-Care Health Care Program For Retired Public School Employees and Their Dependents
Health Benefits Briefing Teacher Retirement System of Texas December 7, 2016 Copyright 2015 GRS All rights reserved. TRS-Care Health Care Program For Retired Public School Employees and Their Dependents
Reinsurance and Cost-Sharing Reductions Estimates
 Reinsurance and Cost-Sharing Reductions Estimates May 9, 208 In response to the 208 premium increases in the Affordable Care Act s individual market, members of Congress have written various pieces of
Reinsurance and Cost-Sharing Reductions Estimates May 9, 208 In response to the 208 premium increases in the Affordable Care Act s individual market, members of Congress have written various pieces of
Innovation with proven results: Enhanced Personal Health Care
 Innovation with proven results: Enhanced Personal Health Care Enhanced Personal Health Care is Anthem's marquee value-based payment initiative and part of a national collection of programs called Blue
Innovation with proven results: Enhanced Personal Health Care Enhanced Personal Health Care is Anthem's marquee value-based payment initiative and part of a national collection of programs called Blue
Investigating the Affordable Care Act: Five Areas for Congressional Oversight of the Healthcare Reform Law
 Investigating the Affordable Care Act: Five Areas for Congressional Oversight of the Healthcare Reform Law Douglas Holtz-Eakin & Michael Ramlet l November 2010 Introduction In the midst of the legislative
Investigating the Affordable Care Act: Five Areas for Congressional Oversight of the Healthcare Reform Law Douglas Holtz-Eakin & Michael Ramlet l November 2010 Introduction In the midst of the legislative
Federal and State Methodologies for Medical Loss Ratio Calculations
 Seton Hall Law Center for Health & Pharmaceutical Law & Policy i Federal and State Methodologies for Medical Loss Ratio Calculations Tara Adams Ragone, J.D. 2013 Health Insurance Rate Review Forum April
Seton Hall Law Center for Health & Pharmaceutical Law & Policy i Federal and State Methodologies for Medical Loss Ratio Calculations Tara Adams Ragone, J.D. 2013 Health Insurance Rate Review Forum April
Employer Health Benefits
 63% $721 2008 The Kaiser Family Foundation -and- Health Research & Educational Trust Employer Health Benefits 2 0 0 8 S u m m a r y o f F i n d i n g s Emp l o y e r-sponsored i n s u r a n c e is t h
63% $721 2008 The Kaiser Family Foundation -and- Health Research & Educational Trust Employer Health Benefits 2 0 0 8 S u m m a r y o f F i n d i n g s Emp l o y e r-sponsored i n s u r a n c e is t h
Covered California: Continuing to Serve Millions in Uncertain Times
 Covered California: Continuing to Serve Millions in Uncertain Times 22 nd Annual ITUP Conference: Advancing Health in California Peter V. Lee February 6, 2018 California: Much to Celebrate After Five Years
Covered California: Continuing to Serve Millions in Uncertain Times 22 nd Annual ITUP Conference: Advancing Health in California Peter V. Lee February 6, 2018 California: Much to Celebrate After Five Years
Ohio s Health Insurance Market
 Ohio s Health Insurance Market Miranda Motter President and CEO OAHP Lunch and Learn Series March 5, 2018 Gretchen Blazer Thompson Director of Govt. Affairs OAHP Overview Who We Are: The Ohio Association
Ohio s Health Insurance Market Miranda Motter President and CEO OAHP Lunch and Learn Series March 5, 2018 Gretchen Blazer Thompson Director of Govt. Affairs OAHP Overview Who We Are: The Ohio Association
MILLIMAN RESEARCH REPORT Medicaid risk-based managed care: Analysis of financial results for June 2017
 Medicaid risk-based managed care: Analysis of financial results for 2016 June 2017 Jeremy D. Palmer, FSA, MAAA Christopher T. Pettit, FSA, MAAA Table of Contents INTRODUCTION... 1 SUMMARY OF RESULTS...
Medicaid risk-based managed care: Analysis of financial results for 2016 June 2017 Jeremy D. Palmer, FSA, MAAA Christopher T. Pettit, FSA, MAAA Table of Contents INTRODUCTION... 1 SUMMARY OF RESULTS...
Employer Health Benefits
 57% $5,884 2013 Employer Health Benefits 2 0 1 3 S u m m a r y o f F i n d i n g s Employer-sponsored insurance covers about 149 million nonelderly people. 1 To provide current information about employer-sponsored
57% $5,884 2013 Employer Health Benefits 2 0 1 3 S u m m a r y o f F i n d i n g s Employer-sponsored insurance covers about 149 million nonelderly people. 1 To provide current information about employer-sponsored
RE: CMS-9989-P, Proposed Rule: Patient Protection and Affordable Care Act; Establishment of Exchanges and Qualified Health Plans
 RUPRI Rural Health Panel Keith J. Mueller, PhD (Panel Chair) Andrew F. Coburn, PhD Jennifer P. Lundblad, PhD A. Clinton MacKinney, MD, MS Timothy D. McBride, PhD Sidney Watson, JD October 31, 2011 Donald
RUPRI Rural Health Panel Keith J. Mueller, PhD (Panel Chair) Andrew F. Coburn, PhD Jennifer P. Lundblad, PhD A. Clinton MacKinney, MD, MS Timothy D. McBride, PhD Sidney Watson, JD October 31, 2011 Donald
A Blue Cross and Blue Shield Association Presentation
 A Blue Cross and Blue Shield Association Presentation Issues in Healthcare Reform CSG Spring Conference Health Policy Task Force Joan Gardner Executive Director, State Services May 17, 2009 Healthcare
A Blue Cross and Blue Shield Association Presentation Issues in Healthcare Reform CSG Spring Conference Health Policy Task Force Joan Gardner Executive Director, State Services May 17, 2009 Healthcare
Medicare Advantage Freestanding Patient Centered Care (FPCC) Program
 2015 Anthem Blue Cross and Blue Shield Provider Expo Medicare Advantage Freestanding Patient Centered Care (FPCC) Program Kathy Morris, Provider Network Manager II Anthem Medicare Advantage This presentation
2015 Anthem Blue Cross and Blue Shield Provider Expo Medicare Advantage Freestanding Patient Centered Care (FPCC) Program Kathy Morris, Provider Network Manager II Anthem Medicare Advantage This presentation
$6,438 $4,819 $1, Employer Contribution. Source: Kaiser/HRET Survey of Employer-Sponsored Health Benefits,
 69% $899 2010 The Kaiser Foundation -and- Health Research Employer & Health Educational Benefits An n u a l Trust S u r v e y Employer Health Benefits 2 0 1 0 S u m m a r y o f F i n d i n g s Employer-sponsored
69% $899 2010 The Kaiser Foundation -and- Health Research Employer & Health Educational Benefits An n u a l Trust S u r v e y Employer Health Benefits 2 0 1 0 S u m m a r y o f F i n d i n g s Employer-sponsored
California Employer Health Benefits Survey
 2005 Introduction Employer-based coverage is the primary source of health insurance in California and the nation. The percentage of employers offering health benefits, the way those benefits are designed,
2005 Introduction Employer-based coverage is the primary source of health insurance in California and the nation. The percentage of employers offering health benefits, the way those benefits are designed,
Capital Health Plan, Inc. Financial Statements and Supplemental Schedules Statutory Basis of Accounting December 31, 2017 and 2016
 Financial Statements and Supplemental Schedules Statutory Basis of Accounting Index Page(s) Report of Independent Auditors... 1 2 Statutory Financial Statements Statements of Admitted Assets, Liabilities
Financial Statements and Supplemental Schedules Statutory Basis of Accounting Index Page(s) Report of Independent Auditors... 1 2 Statutory Financial Statements Statements of Admitted Assets, Liabilities
Point of View: Medicare Profitability in a Reform Market
 Point of View: Profitability in a Reform Market Bill Eggbeer, Managing Director, & Krista Bowers, Director, BDC Advisors, LLC Introduction Overall, accounts for approximately 20% of the total domestic
Point of View: Profitability in a Reform Market Bill Eggbeer, Managing Director, & Krista Bowers, Director, BDC Advisors, LLC Introduction Overall, accounts for approximately 20% of the total domestic
THE FAST AND THE FURIOUS REVENUE CYCLE (A.K.A.) THE REVENUE CYCLE OF THE FUTURE
 THE FAST AND THE FURIOUS REVENUE CYCLE - 3.0 (A.K.A.) THE REVENUE CYCLE OF THE FUTURE INDUSTRY ANALYSIS 82% of people say price is the most important factor when making a healthcare purchasing decision*
THE FAST AND THE FURIOUS REVENUE CYCLE - 3.0 (A.K.A.) THE REVENUE CYCLE OF THE FUTURE INDUSTRY ANALYSIS 82% of people say price is the most important factor when making a healthcare purchasing decision*
RE: 2017 Open Enrollment & Client Service Change Announcement
 RE: 2017 Open Enrollment & Client Service Change Announcement Dear Individual, Family & Medicare Clients, We have appreciated your business. We hold ourselves to a higher level of performance when it comes
RE: 2017 Open Enrollment & Client Service Change Announcement Dear Individual, Family & Medicare Clients, We have appreciated your business. We hold ourselves to a higher level of performance when it comes
Optum. Actuarial Toolbox Proven, sophisticated and market-leading actuarial models for health plans and benefits consultants
 Optum Actuarial Toolbox Proven, sophisticated and market-leading actuarial models for health plans and benefits consultants In recent years, the health care landscape has shifted tremendously, prompting
Optum Actuarial Toolbox Proven, sophisticated and market-leading actuarial models for health plans and benefits consultants In recent years, the health care landscape has shifted tremendously, prompting
Exchanges year 2: New findings and ongoing trends
 Intelligence Brief Exchanges year 2: New findings and ongoing trends The open enrollment period (OEP) for year 2 of the individual exchanges is officially under way, having begun on November 15 th. To
Intelligence Brief Exchanges year 2: New findings and ongoing trends The open enrollment period (OEP) for year 2 of the individual exchanges is officially under way, having begun on November 15 th. To
Report on Merging the Individual and Small Group Markets
 www.pwc.com Report on Merging the Individual and Small Group Markets Draft October 12, 2018 Prepared by PwC for Covered California (10/12/18) Covered California 1601 Exposition Blvd. Sacramento, CA 95815
www.pwc.com Report on Merging the Individual and Small Group Markets Draft October 12, 2018 Prepared by PwC for Covered California (10/12/18) Covered California 1601 Exposition Blvd. Sacramento, CA 95815
Quantifying Tax Credits for People Now Buying Insurance on Their Own
 issue brief Quantifying Tax Credits for People Now Buying Insurance on Their Own August 2013 A number of states have recently released information on what premiums will be in the individual insurance market
issue brief Quantifying Tax Credits for People Now Buying Insurance on Their Own August 2013 A number of states have recently released information on what premiums will be in the individual insurance market
A more efficient you.
 A more efficient you. Introducing EmployerAccess Anthem s easy-to-use online benefits management system Anthem Blue Cross and Blue Shield is the trade name of: In Colorado: Rocky Mountain Hospital and
A more efficient you. Introducing EmployerAccess Anthem s easy-to-use online benefits management system Anthem Blue Cross and Blue Shield is the trade name of: In Colorado: Rocky Mountain Hospital and
Financial Analysis of Anthem/WellPoint
 Financial Analysis of Anthem/WellPoint By David Belk MD Overview Health insurance finances are very complicated to say the least. Companies that provide most types of insurance have a rather simple business
Financial Analysis of Anthem/WellPoint By David Belk MD Overview Health insurance finances are very complicated to say the least. Companies that provide most types of insurance have a rather simple business
I. II. III. IV. V. VI. OBJECTIVES OF THE SERIES
 I II III IV V VI I. II. Nearly a decade after the passage of the Affordable Care Act, health care continues to be a top issue among voters in the U.S., with the two major parties offering distinctly different
I II III IV V VI I. II. Nearly a decade after the passage of the Affordable Care Act, health care continues to be a top issue among voters in the U.S., with the two major parties offering distinctly different
State of New Jersey Department of Banking and Insurance PO Box 325 Life & Health Actuarial, 11th Floor Trenton, NJ Tel (609) Fax
 State of New Jersey Department of Banking and Insurance PO Box 325 Life & Health Actuarial, 11th Floor Trenton, NJ 08625-0325 Tel (609) 292-7272 Fax (609) 633-0527 1 R. Neil Vance, Managing Actuary NJ
State of New Jersey Department of Banking and Insurance PO Box 325 Life & Health Actuarial, 11th Floor Trenton, NJ 08625-0325 Tel (609) 292-7272 Fax (609) 633-0527 1 R. Neil Vance, Managing Actuary NJ
Individual Health Insurance Options Boom or Bust
 Individual Health Insurance Options Boom or Bust 6/26/2012 by Debra A. Donahue Health insurance purchased by individual consumers will be impacted the most by the impending U.S. Supreme Court (SCOTUS)
Individual Health Insurance Options Boom or Bust 6/26/2012 by Debra A. Donahue Health insurance purchased by individual consumers will be impacted the most by the impending U.S. Supreme Court (SCOTUS)
The Role of the Actuary in Employee Benefits
 The Role of the Actuary in Employee Benefits Topics to Cover Healthcare Review Underwriting Review Funding Mechanisms in Employee Benefits Fully Insured Self Insured Actuarial Practice Overview Role of
The Role of the Actuary in Employee Benefits Topics to Cover Healthcare Review Underwriting Review Funding Mechanisms in Employee Benefits Fully Insured Self Insured Actuarial Practice Overview Role of
In This Issue (click to jump):
 May 7, 2014 In This Issue (click to jump): Analysis of Trends in Health Spending 2013 2014 Spotlight on Medicare Advantage Enrollment Oncology Drug Trend Report S&P Predicts Shift from Job-Based Coverage
May 7, 2014 In This Issue (click to jump): Analysis of Trends in Health Spending 2013 2014 Spotlight on Medicare Advantage Enrollment Oncology Drug Trend Report S&P Predicts Shift from Job-Based Coverage
Minnesota Health Care Spending Trends,
 Minnesota Health Care Spending Trends, 1993-2000 April 2003 h ealth e conomics p rogram Health Policy and Systems Compliance Division Minnesota Department of Health Minnesota Health Care Spending Trends,
Minnesota Health Care Spending Trends, 1993-2000 April 2003 h ealth e conomics p rogram Health Policy and Systems Compliance Division Minnesota Department of Health Minnesota Health Care Spending Trends,
Attachment 1 Puerto Rico Rate Filing Instruction Manual
 Attachment 1 Puerto Rico Rate Filing Instruction Manual March 2014 1 Overview This instruction manual supports implementation of the requirement of Ruling Letter No. CN- 2017-218-AS of March 1, 2017. For
Attachment 1 Puerto Rico Rate Filing Instruction Manual March 2014 1 Overview This instruction manual supports implementation of the requirement of Ruling Letter No. CN- 2017-218-AS of March 1, 2017. For
REPORT 4 OF THE COUNCIL ON MEDICAL SERVICE (I-14) Network Adequacy (Resolutions 113-A-14, 125-A-14 and 130-A-14) (Reference Committee J)
 REPORT OF THE COUNCIL ON MEDICAL SERVICE (I-) Network Adequacy (Resolutions -A-, -A- and 0-A-) (Reference Committee J) EXECUTIVE SUMMARY At the Annual Meeting, the House of Delegates referred three resolutions
REPORT OF THE COUNCIL ON MEDICAL SERVICE (I-) Network Adequacy (Resolutions -A-, -A- and 0-A-) (Reference Committee J) EXECUTIVE SUMMARY At the Annual Meeting, the House of Delegates referred three resolutions
Health Care Reform Eric H. Schultz, President and CEO
 Health Care Reform Eric H. Schultz, President and CEO Sentinel Benefits & Financial Group September 21, 2011 Affordable Care Act The Basics Insures the uninsured Individual and employer mandates Reforms
Health Care Reform Eric H. Schultz, President and CEO Sentinel Benefits & Financial Group September 21, 2011 Affordable Care Act The Basics Insures the uninsured Individual and employer mandates Reforms
2016 Segal Health Plan Cost Trend Survey
 Practical Research for Multiemployer Plans Summer 2015 Health benefit plan cost trend rates for 2016 will increase for most medical plan options and increase substantially for prescription drug coverage
Practical Research for Multiemployer Plans Summer 2015 Health benefit plan cost trend rates for 2016 will increase for most medical plan options and increase substantially for prescription drug coverage
The Competitive Landscape for 2016 Medicare Business
 The Competitive Landscape for 2016 Medicare Business 10/19/2015 by Mark Farrah Associates Medicare Advantage (MA) plans have established a strong foothold in the industry, providing medical coverage for
The Competitive Landscape for 2016 Medicare Business 10/19/2015 by Mark Farrah Associates Medicare Advantage (MA) plans have established a strong foothold in the industry, providing medical coverage for
PRIVATE PAYOR OUTLOOK KELLI BACK, ATTORNEY AND APMA CONSULTANT
 PRIVATE PAYOR OUTLOOK KELLI BACK, ATTORNEY AND APMA CONSULTANT Insurance Coverage by Source (2015) Employer Group 49% Non-group (individual and association) 7% Medicaid 20% (includes dual eligibles) Medicare
PRIVATE PAYOR OUTLOOK KELLI BACK, ATTORNEY AND APMA CONSULTANT Insurance Coverage by Source (2015) Employer Group 49% Non-group (individual and association) 7% Medicaid 20% (includes dual eligibles) Medicare
2016 Mid-Year. Health Insurance Industry Analysis Report CONTENTS
 2016 Mid-Year Health Insurance Industry Analysis Report CONTENTS Underwri ng Results Premium Revenues Liquidity Capital and Surplus Merger Update 2 2 3 4 4 5 Contributors NAIC Financial Regulatory Services
2016 Mid-Year Health Insurance Industry Analysis Report CONTENTS Underwri ng Results Premium Revenues Liquidity Capital and Surplus Merger Update 2 2 3 4 4 5 Contributors NAIC Financial Regulatory Services
A Publication by the Massachusetts Association of Health Plans. Health Insurance 101 How Are Premiums Developed for Individuals and Small Groups?
 OnPoint: Issue Brief A Publication by the Massachusetts Association of Health Plans Volume VIII, April 2017 Written by Eric Linzer Health Insurance 101 How Are Premiums Developed for Individuals and Small
OnPoint: Issue Brief A Publication by the Massachusetts Association of Health Plans Volume VIII, April 2017 Written by Eric Linzer Health Insurance 101 How Are Premiums Developed for Individuals and Small
ARKANSAS BLUE CROSS and BLUE SHIELD
 Reason for Requesting Rate Increase Arkansas Blue Cross and Blue Shield is filing a modified rate request for 2018 in response to the Arkansas Insurance Department (AID) Bulletin number 14-2017 dated August
Reason for Requesting Rate Increase Arkansas Blue Cross and Blue Shield is filing a modified rate request for 2018 in response to the Arkansas Insurance Department (AID) Bulletin number 14-2017 dated August
