Illinois & Wisconsin Chapter: Proposed Fee schedule Getting ready for 2019
|
|
|
- Ernest Hampton
- 5 years ago
- Views:
Transcription
1 Illinois & Wisconsin Chapter: Proposed Fee schedule Getting ready for 2019 Cathleen Biga President/CEO Cardiovascular Management of Illinois
2 "The nine most terrifying words in the English language are: I'm from the government and I'm here to help." Timeline Ronald Reagan
3 PFS Highlights Rules released 7/12/18 ACC commented 9/10/18 Final rule will be out --- Trick or Treat Conversion Factor increases to $36.06 ($35.99)
4 Key elements Changes to E&M Changes to 25 Modifier Increased uses for telehealth/ communication strategies AUC mandate
5 E & M changes: aka Patients over Paperwork Reduced Administrative burden thank you Consults: bundling Levels 2-5 into 1 Level paid at $135 Established patients: Level 1 and Level all others paid at $93 Eliminates the prohibition on practitioners in the same group billing E&M on the same day 4 methods for documentation: Time, 95 guidelines, 97 guidelines, and Medical decision making
6 E/M Proposal Financial Impact
7 Prolonged Services There are 3 Prolonged Services: Office or outpatient Face to Face - 1 hour beyond normal services + q 30 min Same day E&M Physician or APP Prolonged Service: Inpatient Face to Face 1 hour beyond normal + 30 min. Same Day E&M Physician or APP
8 Prolonged Service w/o Direct Patient Contact Effective 1/1/ Prolonged evaluation and management service before and/or after direct patient care; first hour ** actually billed for the first 30 to 74 minutes each additional 30 minutes(list separately in addition to code for prolonged service) Prolonged service less than 30 minutes not separately reported This service can be reported for a different date than the primary service Cannot be reported during same service period as Chronic Care Management or Transitional Care Management Services
9 Prolonged service w/o face to face
10 Examples of non F2F Prolonged Services Billing Application of codes: 1. Provider spends 45 minutes reviewing extensive medical records the day after the patient visit. Total time spent = 45 minutes, report Provider spends 35 minutes speaking to another physician on the phone about transfer of patient care and 45 minutes doing an extensive review of the patient s records. Total time spent = 1 hr and 20 minutes, report and Provider spends 15 minutes in the morning discussing patient s care with another physician and 40 minutes in the afternoon reviewing the patient s records from another facility. Total time spent = 55 minutes, report
11 Doctor Note 1. Open a new encounter in the EMR 2. Select Patient Communication as the Visit Type 3. Click on the Doctor Note tab 4. Open the Doctor Note and document prolonged services with time, dates and activities 5. Check the Dr Signed box and click Accept 6. Click on Create Document 7. Click on the Fee Ticket and submit charge for Prolonged Services
12 New Code For Prolonged Service Add on To E/M Proposing A new code to add-on to any office visit lasting more than 30 minutes beyond the office visit (i.e., hour long visits in total). GPRO1 Prolonged evaluation and management or psychotherapy services(s) (List separately in addition to code for office or other outpatient Evaluation and Management or psychotherapy service) Will have a payment rate of $67 (1.85 wrvu s) Example: A cardiologist currently reporting a and spending more than 60 minutes with a patient would be paid $211. Under the proposed new method, the cardiologist would report: , depending on their documentation selection, - $135 GCG0X specialty add on - $14 GPRO1 prolonged service $67 Total combined payment of $215.
13 What is normal time New Patient Visit Typical Time (minutes) Establish ed Patient Visit Typical Time (minutes)
14 Issues Questions How many of our visits last 60 minutes 95 or 97 guidelines Should help with cloning audits Medical Decision Making Medical necessity of a Level 2 is required Will this facilitate team based care? How will it impact risk scores? MIPS Mortality
15 25 Modifier..aka E/M MPPR Used in conjunction with another service on same day Imperative to know your MAC rules: do they require it with an EKG on same day? Echo? Device Check? Immunization? Reduction of 50% of the least expensive procedure or visit provided by same TIN w identifiable E&M
16 Practice Expense Proposal Impacts ultrasound and vascular Reframes cost of our ultrasound rooms Reduces the general ultrasound room price by 65% (from $369,945 to $130,253) Results in a 9% reduction in payment - OFFICE
17 PE proposed changes Office imaging
18 Tele-Health Still need to meet the main geographical rules Remote monitoring (RPM) of physiological parameters RPM is outside tele-health requirements New codes for interpersonal internet consultation 6 codes Imperative to understand your patient flow
19 AUC mandate Voluntary 7/18 through 12/19 Effective 1/1/20 for a year of education must be reported on both tech and pro bill if split billing Providers must Will include consult IDTF s, will AUC implement via a G qualified codes, clinical and will allow non-physicians to consult AUC decision support mechanism both ordering and rendering what if you are interpreting only? Will include IDTF s Will implement G codes, and will allow nonphysicians to consult AUC
20 This and that Section 603 off-campus PBD: 40% payment factor remains Shared Decision making for specific ICD implants Placement and removal of loop recorders (1.53 and 1.50 wrvus) SET for PAD
21 HOPPS: PROPOSALS FOR 2019
22 Proposed OPPS Site neutrality becoming a common theme: $46 for off-campus G0463 $115 for on campus G0463 Exceptions to 603 clinical families of services 19 clinical families Comments requested for using prior auth for offcampus HOPD s Addition of 12 cardiac cath codes to approved ASC s Cardiac MRI: & watch APC classification: 15% reduction
23 Proposed Additions to ASC
24 OBL vs ASC for PAD
25 QPP: MIPS PROPOSALS FOR 2019
26 Yesterday s results..and Today s
27 2019 Overview Start with 2018: Scores recalculated Costs released for education 435,000 clinicians took the penalty in 2018 based on 2016 data (<3 points) PROPOSED: 2019: Quality 45% and 12 months Cost: 15% - 12 months; 10 episodes IA: 15% and 90 days MU/ACI/Promoting Interoperability: 25% and 90 days
28 2017 Data Cost Detail
29 MSPB: 2017 MSPB Cost
30 2017: TC TPCC Cost Detail
31 Currently 10 Episodes 3-4 for cardiology
32 Episodes for 2019 data Elective Outpatient PCI Cost Measure: Summary Results Understanding Your Cost Measure Score No Data Click here to provide feedback on the report With a total of 121 episodes for this cost measure: Your overall risk-adjusted cost measure The national average risk-adjusted cost measure score is: $11,137 $10,902 score is: And your cost measure score is 2% higher than the national average No Data No Data No Data STEMI with PCI Cost Measure: Summary Results Understanding Your Cost Measure Score No Data Click here to provide feedback on the report Breakdown of Part B Physician/Supplier Episode Cost by Your TIN vs. Other TINs The table and pie charts below show the breakdown of the average share of cost per episode where the source of Part B Physician/Supplier costs is the attributed clinician's TIN versus other TINs. This is presented for your TIN and for all TINs nationally (including your TIN). Below, the pie chart on the left presents the values for this breakdown for the average share of cost per episode for your TIN. The pie chart on the right presents the same values for all TINs nationally. With a total of 10 episodes for this cost measure: Your overall risk-adjusted cost measure The national average risk-adjusted cost measure score is: $17,245 $19,320 score is: No Data No Data Average Share of Cost Per Episode for Your TIN Average Share of Cost Per Episode for All TINs Nationally And your cost measure score is 11% lower than the national average No Data No Data Source of Part B Physician/Supplier Cost During Episode Average Share of Cost Per Episode Your TIN All TINs Nationally 5% No Data 6% Breakdown of Part B Physician/Supplier Episode Cost by Your TIN vs. Other TINs The table and pie charts below show the breakdown of the average share of cost per episode where the source of Part B Physician/Supplier costs is the attributed clinician's TIN versus other TINs. This is presented for your TIN and for all TINs nationally (including your TIN). Below, the pie chart on the left presents the values for this breakdown for the average share of cost per episode for your TIN. The pie chart on the right presents the same values for all TINs nationally. From Providers in the Attributed Clinician's TIN 95% 94% From Providers in a Different TIN 5% 6% Breakdown of Utilization and Cost by Selected Clinical Theme No Data 95% From Providers in the Attributed Clinician's TIN From Providers in a Different TIN 94% From Providers in the Attributed Clinician's TIN From Providers in a Different TIN Source of Part B Physician/Supplier Cost During Episode From Providers in the Attributed Clinician's TIN No Data Average Share of Cost Per Episode Your TIN All TINs Nationally 59% 51% Average Share of Cost Per Episode for Your TIN 41% No Data 59% No Data Average Share of Cost Per Episode for All TINs Nationally 49% 51% From Providers in a Different TIN 41% 49% From Providers in the Attributed Clinician's TIN From Providers in a Different TIN From Providers in the Attributed Clinician's TIN From Providers in a Different TIN
33 Key proposed changes for 2019 Will need 30 points for threshold Exceptional performance will be > 80 points ($500M available) Payment adjustment to 7% MUST have 2015-certified EHR (only 66% are in compliance) Claims data is on the hook in the future may be only available to small groups Watch your quality benchmarked No benchmark only 3 points
34 Getting ready for 2020 New Field Tested Reports just released In addition to the 8 added 10 (CABG and COPD) Educational in purpose Covers calendar year 2017 Attribution has changed MSPB and Total cost and new episodes Total cost/attributed beneficiary Detail available but format is different Gives you your %tile ranking
35 Getting ready for 2020 Attribution changes TPCC: much higher attribution rates 2 step attribution process is proposed to sunset MSPB: provides 30% of E&M or perform the episodic procedure Adds any clinician within the TIN who does any E&M
36 Medicare Spend/Beneficiary
37 Total per capita cost
38 Measure or Sub-Group Name Episodes Inpatient COPD Exacerbation Cost Measure: Results Click here to provide feedback on the report Understanding Your Cost Measure Score No Data With a total of 40 episodes for this cost measure: Your overall risk-adjusted cost measure score is: $13,597 image of multiple people to indicate your TIN The national average risk-adjusted cost measure score is: $13,477 This cell includes an image No Data And your cost measure score is 1% higher than the national average Table 1. Breakdown of Cost Measure Score by Episode Sub-Group Breakdown of Cost Measure Score by Episode Sub-Group Cost Measure Score Episode Count for Your TIN Name Short Form Name Your TIN National Average Percent Difference Between Your TIN's Average Risk-Adjusted Episode Cost and National Average Risk- Adjusted Episode Cost No Data Percent Difference Between Your TIN's Average Risk-Adjusted Episode Cost and National Average Risk-Adjusted Episode Cost Less Cost to Medicare National Average More Cost to Medicare Inpatient Chronic Obstructive Pulmonary Disease (COPD) Exacerbation ip_copd 40 $13,597 $13,477 1% 1% ip_copd COPD Exacerbation with Mechanical Ventilation > 24 hours mv_great_24 1 $25,484 $33,347-24% -24% mv_great_24 COPD Exacerbation with no Mechanical Ventilation or Mechanical Ventilation < 24 hours mv_less_24 39 $12,787 $12,599 1% The chart above presents the performance of your TIN relative to the national average for each of the episode sub-groups comprising this episode-based cost measure. An episode sub-group is a division of a cost measure s episode group that defines more homogenous patient cohorts to ensure clinical comparability (i.e., the cost measure fairly compares like patients). Specifically, for the cost measure and each episode sub-group, it displays the percent difference between your TIN's average risk-adjusted episode cost to Medicare and the national average risk-adjusted cost to Medicare. Negative values indicate that your TIN represents a lower cost to Medicare than the national average, and positive values indicate that your TIN represents a higher cost to Medicare than the national average. -120% -90% -60% -30% 0% 30% 60% 90% 120% + 1% Value mv_less_24 chart, there are two arrows that indicate how the values for this metric represent either less cost to Medicare (i.e., negative values) or more +
39 Table 3. Breakdown of Episode Cost by Your TIN vs. Other TINs Source of Cost During Episode Your TIN Average Share of Cost Per Episode National Average TINs in Your Risk Bracket Average Share of Cost Per Episode for Your TIN 32% 5% No Data Average Share of Cost Per Episode for the National Average 20% 6% Services Provided By Clinicians Under Your TIN 5% 6% 6% Services Associated with Clinicians Under Your TIN 62% 74% 74% 62% Services Provided By Clinicians Under Your TIN 74% Services Provided By Clinicians Under Your TIN All Other Services 32% 20% 20% Services Associated with Clinicians Under Your TIN Services Associated with Clinicians Under Your TIN All Other Services All Other Services inicians Under Your TIN, (2) Services Associated with Clinicians Under Your TIans Under Your TIN, (2) Services Associated with Clinicians Under You No Data Table 4. Breakdown of Utilization and Cost by Selected Clinical Theme Clinical Theme Your Average Cost Per Episode Percent Difference in Average Cost of Clinical Theme Services for Your TIN Versus TINs in Your Risk Bracket Share of Episodes with Any Cost From Given Clinical Theme Your TIN National Average TINs in Your Risk Bracket (1) Physical Therapy / DME $218-4% 62.5% 60.5% 61.1% (2) Bronchoscopy $0-100% 0.0% 0.4% 0.4% (3) Post-Acute Care $3,171 22% 35.0% 38.2% 38.5% (4) COPD Exacerbation $673-35% 67.5% 62.4% 63.7% (5) Pulmonary Complications, Other $357-38% 50.0% 58.1% 57.5% (6) Renal Failure and Metabolic Abnormalities $0-100% 0.0% 1.5% 1.4% (7) Cardiac Complications $21-76% 22.5% 15.8% 15.6% (8) Diabetic Complications $0-100% 0.0% 0.8% 0.8% (9) Sepsis $0-100% 0.0% 1.0% 0.9% (10) Thromboembolism (DVT/PE) $7-54% 2.5% 1.1% 1.2%
40 Current state 427 ACO s in received $799M of savings 16 of the MSSP Tracks 2 & 3 paid penalties of $57M Total savings across all the MSSP s = $313.7M
41 ACO update Proposed rules out comments complete No new APM s forthcoming Significant changes proposed 2 Tracks: Basic & Enhanced 5 yr. plans Basic: glide path from one-sided to 2-sided risk Plans A-E and E qualifies as a QAPM Lower shared savings 25% vs current 50% Enhanced: QAPM and mirrors MSSP Track 3
42 Do ACO s work?? Savings equaled $36/beneficiary 9 million patients enrolled We are in the 5 th year what have we learned? Those in down-side risk saved less There were 39 ACO s and they saved $27/beneficiary Will these new rules help?
43 Questions?
2018 Merit-Based Incentive Payment System (MIPS) Scoring Overview
 The Physicians Advocacy Institute s Medicare Quality Payment Program (QPP) Physician Education Initiative 2018 Merit-Based Incentive Payment System (MIPS) Scoring Overview 1 P a g e MEDICARE QPP PHYSICIAN
The Physicians Advocacy Institute s Medicare Quality Payment Program (QPP) Physician Education Initiative 2018 Merit-Based Incentive Payment System (MIPS) Scoring Overview 1 P a g e MEDICARE QPP PHYSICIAN
Quality Payment Program Year 2
 Quality Payment Program Year 2 MIPS Highlights Raising the performance threshold to 15 points in Year 2 (from 3 points in the transition year). Allowing the use of 2014 Edition and/or 2015 Certified Electronic
Quality Payment Program Year 2 MIPS Highlights Raising the performance threshold to 15 points in Year 2 (from 3 points in the transition year). Allowing the use of 2014 Edition and/or 2015 Certified Electronic
PRIMER: MACRA and the Merit-based Incentive Payment System (MIPS) Tara O Neill Hayes January 31, 2016
 PRIMER: MACRA and the Merit-based Incentive Payment System (MIPS) Tara O Neill Hayes January 31, 2016 Background On April 16, 2015, the Medicare Access and CHIP Reauthorization Act (MACRA) was signed into
PRIMER: MACRA and the Merit-based Incentive Payment System (MIPS) Tara O Neill Hayes January 31, 2016 Background On April 16, 2015, the Medicare Access and CHIP Reauthorization Act (MACRA) was signed into
2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet
 2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
2019 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure
 Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of
Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of
The Future Of Medicare Physician Reimbursement
 Portfolio Media. Inc. 111 West 19 th Street, 5th Floor New York, NY 10011 www.law360.com Phone: +1 646 783 7100 Fax: +1 646 783 7161 customerservice@law360.com The Future Of Medicare Physician Reimbursement
Portfolio Media. Inc. 111 West 19 th Street, 5th Floor New York, NY 10011 www.law360.com Phone: +1 646 783 7100 Fax: +1 646 783 7161 customerservice@law360.com The Future Of Medicare Physician Reimbursement
Proposed 2018 Medicare Physician Payment and Quality Reporting Changes. Executive s Insights
 Proposed 2018 Medicare Physician Payment and Quality Reporting Changes MGMA MEMBER-EXCLUSIVE ANALYSIS The Centers for Medicare & Medicaid Services (CMS) recently proposed changes to both Medicare physician
Proposed 2018 Medicare Physician Payment and Quality Reporting Changes MGMA MEMBER-EXCLUSIVE ANALYSIS The Centers for Medicare & Medicaid Services (CMS) recently proposed changes to both Medicare physician
Volume to Value The Great Transformation of American Medicine
 Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
Volume to Value The Great Transformation of American Medicine 2010-2020 Richard I. Fogel, MD FHRS Chief Clinical Officer St. Vincent Health October 2015 Fee for Service You get paid for what you do The
AAOS MACRA Proposed Rule Summary (Short)
 AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
Final Policy, Payment, and Quality Provisions in the Medicare Physician Fee Schedule for Calendar Year 2018
 Final Policy, Payment, and Quality Provisions in the Medicare Physician Fee Schedule for Calendar Year 2018 Date 2017-11-02 Title Contact Final Policy, Payment, and Quality Provisions in the Medicare Physician
Final Policy, Payment, and Quality Provisions in the Medicare Physician Fee Schedule for Calendar Year 2018 Date 2017-11-02 Title Contact Final Policy, Payment, and Quality Provisions in the Medicare Physician
CY 2018 Quality Payment Program Final Rule Summary
 CY 2018 Quality Payment Program Final Rule Summary On November 2, 2017, the Centers for Medicare and Medicaid Services (CMS) released its final rule outlining the requirements for year two of the Quality
CY 2018 Quality Payment Program Final Rule Summary On November 2, 2017, the Centers for Medicare and Medicaid Services (CMS) released its final rule outlining the requirements for year two of the Quality
2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet
 2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
2018 Merit-based Incentive Payment System (MIPS) Cost Performance Category Fact Sheet What is the Quality Payment Program? The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable
CY 2014 Physician Quality Reporting System (PQRS)
 CY 2014 Physician Quality Reporting System (PQRS) 101 Table of Contents Step 1: Understand PQRS and how it impacts you A. When was PQRS first established and implemented? B. What is PQRS? C. How does CMS
CY 2014 Physician Quality Reporting System (PQRS) 101 Table of Contents Step 1: Understand PQRS and how it impacts you A. When was PQRS first established and implemented? B. What is PQRS? C. How does CMS
MACRA: THE FINAL RULE. Last updated 12/13/16
 MACRA: THE FINAL RULE Last updated 12/13/16 1 Background April 2015 MACRA (Medicare Access & CHIP Reauthorization Act) is signed into law to repeal the sustainable growth rate (SGR) which drastically cut
MACRA: THE FINAL RULE Last updated 12/13/16 1 Background April 2015 MACRA (Medicare Access & CHIP Reauthorization Act) is signed into law to repeal the sustainable growth rate (SGR) which drastically cut
9/7/17. MACRA: The Knowns and the Unknowns. Disclosures. Goals and Objectives
 MACRA: The Knowns and the Unknowns Sharon K. Merrick, M.S., CCS-P Director of Payment and Practice Management American Society of Anesthesiologists Wisconsin Society of Anesthesiologists September 10,
MACRA: The Knowns and the Unknowns Sharon K. Merrick, M.S., CCS-P Director of Payment and Practice Management American Society of Anesthesiologists Wisconsin Society of Anesthesiologists September 10,
Medicare Releases Final Rule for the Second Year of the Quality Payment Program
 Medicare Releases Final Rule for the Second Year of the Quality Payment Program On Nov. 2, 2017, CMS issued the Calendar Year 2018 Quality Payment Program (QPP) final rule for the second transition year
Medicare Releases Final Rule for the Second Year of the Quality Payment Program On Nov. 2, 2017, CMS issued the Calendar Year 2018 Quality Payment Program (QPP) final rule for the second transition year
Merit-Based Incentive Payment System (MIPS): Knee Arthroplasty Measure. Measure Information Form 2019 Performance Period
 Merit-Based Incentive Payment System (MIPS): Knee Arthroplasty Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction... 3 1.1 Measure Name... 3 1.2 Measure Description...
Merit-Based Incentive Payment System (MIPS): Knee Arthroplasty Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction... 3 1.1 Measure Name... 3 1.2 Measure Description...
MID-YEAR QUALITY AND RESOURCE USE REPORT
 MID-YEAR QUALITY AND RESOURCE USE REPORT SOUTHEAST TEXAS MEDICAL ASSOCIATES LLP Last Four Digits of Your Medicare Taxpayer Identification Number (TIN): 7095 PERFORMANCE PERIOD: 07/01/2014-06/30/2015 ABOUT
MID-YEAR QUALITY AND RESOURCE USE REPORT SOUTHEAST TEXAS MEDICAL ASSOCIATES LLP Last Four Digits of Your Medicare Taxpayer Identification Number (TIN): 7095 PERFORMANCE PERIOD: 07/01/2014-06/30/2015 ABOUT
Fact Sheet: 2019 Merit-based Incentive Payment System (MIPS) Payment Adjustments based on 2017 MIPS Final Scores
 Fact Sheet: 2019 Merit-based Incentive Payment System (MIPS) Payment Adjustments based on 2017 MIPS Final Scores The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) repealed the Medicare sustainable
Fact Sheet: 2019 Merit-based Incentive Payment System (MIPS) Payment Adjustments based on 2017 MIPS Final Scores The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) repealed the Medicare sustainable
The Physician Value-Based Payment Modifier under the 2014 Medicare Physician Fee Schedule. December 3, 2013
 The Physician Value-Based Payment Modifier under the 2014 Medicare Physician Fee Schedule December 3, 2013 Medicare Learning Network This MLN Connects National Provider Call (MLN Connects Call) is part
The Physician Value-Based Payment Modifier under the 2014 Medicare Physician Fee Schedule December 3, 2013 Medicare Learning Network This MLN Connects National Provider Call (MLN Connects Call) is part
CMS PROPOSES KEY PROVISIONS OF MACRA PHYSICIAN PAYMENT SYSTEM FOR 2019
 Thursday, April 28, 2016 CMS PROPOSES KEY PROVISIONS OF MACRA PHYSICIAN PAYMENT SYSTEM FOR 2019 The Centers for Medicare & Medicaid Services (CMS) late yesterday issued a proposed rule implementing key
Thursday, April 28, 2016 CMS PROPOSES KEY PROVISIONS OF MACRA PHYSICIAN PAYMENT SYSTEM FOR 2019 The Centers for Medicare & Medicaid Services (CMS) late yesterday issued a proposed rule implementing key
QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NOVEMBER 15, 2018
 QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NOVEMBER 15, 2018 Disclaimers This presentation was prepared as a tool to assist providers and is not intended to grant rights or impose obligations.
QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NOVEMBER 15, 2018 Disclaimers This presentation was prepared as a tool to assist providers and is not intended to grant rights or impose obligations.
Medicare Physician Fee Schedule (PFS) Proposed Rule 2019
 Medicare Physician Fee Schedule (PFS) Proposed Rule 2019 (As on July 23, 2018; Note: This document may be updated) Executive Summary Physician Fee Schedule The 2019 Medicare Physician Payment Schedule
Medicare Physician Fee Schedule (PFS) Proposed Rule 2019 (As on July 23, 2018; Note: This document may be updated) Executive Summary Physician Fee Schedule The 2019 Medicare Physician Payment Schedule
2017 Proposed Rule MIPS Composite Performance Score Resource Use Performance Category
 Starting at Noon EDT 8/22/2016 2017 Proposed Rule MIPS Composite Performance Score Resource Use Performance Category Dr. Dan Mingle Register for Webinars or Access Recordings http://mingleanalytics.com/webinars
Starting at Noon EDT 8/22/2016 2017 Proposed Rule MIPS Composite Performance Score Resource Use Performance Category Dr. Dan Mingle Register for Webinars or Access Recordings http://mingleanalytics.com/webinars
Quality Payment Program Year 3
 Quality Payment Program Year 3 Final Rule Overview The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable Growth Rate (SGR) formula for clinician payment, and established
Quality Payment Program Year 3 Final Rule Overview The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ended the Sustainable Growth Rate (SGR) formula for clinician payment, and established
Pamela Ballou-Nelson, RN, MSPH, CMPE, PhD, Principal, MGMA Consulting April 10, , Telligen, Inc.
 MIPS 2018 Cost Reporting and Your QRUR Pamela Ballou-Nelson, RN, MSPH, CMPE, PhD, Principal, MGMA Consulting April 10, 2018 2016, Telligen, Inc. Quality Payment Program Cost Reporting Quality Payment Program
MIPS 2018 Cost Reporting and Your QRUR Pamela Ballou-Nelson, RN, MSPH, CMPE, PhD, Principal, MGMA Consulting April 10, 2018 2016, Telligen, Inc. Quality Payment Program Cost Reporting Quality Payment Program
Merit-Based Incentive Payment System (MIPS): Elective Outpatient Percutaneous Coronary Intervention (PCI) Measure
 Merit-Based Incentive Payment System (MIPS): Elective Outpatient Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
Merit-Based Incentive Payment System (MIPS): Elective Outpatient Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
AMERICAN COLLEGE OF GASTROENTEROLOGY MAKING $ENSE OF MACRA
 AMERICAN COLLEGE OF GASTROENTEROLOGY 6400 Goldsboro Road, Suite 200, Bethesda, Maryland 20817-5842; P: 301-263-9000; F: 301-263-9025 MAKING $ENSE OF MACRA CMS.SGR MACRA MIPS APMs QCDRs ACOs Why does Washington
AMERICAN COLLEGE OF GASTROENTEROLOGY 6400 Goldsboro Road, Suite 200, Bethesda, Maryland 20817-5842; P: 301-263-9000; F: 301-263-9025 MAKING $ENSE OF MACRA CMS.SGR MACRA MIPS APMs QCDRs ACOs Why does Washington
Major Provisions in the CY 2017 Medicare Physician Fee Schedule Proposed Rule Payment Policy
 On July 15, 2016, the calendar year (CY) 2017 Medicare Physician Fee Schedule (PFS) Proposed Rule was published in the Federal Register. AGA, ACG and ASGE have developed this summary of key provisions
On July 15, 2016, the calendar year (CY) 2017 Medicare Physician Fee Schedule (PFS) Proposed Rule was published in the Federal Register. AGA, ACG and ASGE have developed this summary of key provisions
HOW TO UNDERSTAND YOUR QUALITY AND RESOURCE USE REPORT (QRUR)
 HOW TO UNDERSTAND YOUR QUALITY AND RESOURCE USE REPORT (QRUR) Kaitlin Nolte Kansas Foundation for Medical Care, Inc. QI Project Manager Kaitlin.nolte@area-A.hcqis.org greatplainsqin.org 785-273-2552 ext.
HOW TO UNDERSTAND YOUR QUALITY AND RESOURCE USE REPORT (QRUR) Kaitlin Nolte Kansas Foundation for Medical Care, Inc. QI Project Manager Kaitlin.nolte@area-A.hcqis.org greatplainsqin.org 785-273-2552 ext.
What You Need to Know About CMS Quality and Resource Use Report
 What You Need to Know About CMS Quality and Resource Use Report Heidy Robertson-Cooper, MPA Maryland Family Medicine Summit June 24, 2016 Learning Objectives Describe the purpose of CMS Quality Resource
What You Need to Know About CMS Quality and Resource Use Report Heidy Robertson-Cooper, MPA Maryland Family Medicine Summit June 24, 2016 Learning Objectives Describe the purpose of CMS Quality Resource
2015 ANNUAL QUALITY AND RESOURCE USE REPORT
 Download Your Report to: --> PDF 508 Compliance CSV 2015 ANNUAL QUALITY AND RESOURCE USE REPORT AND THE 2017 VALUE-BASED PAYMENT MODIFIER SOUTHEAST TEXAS MEDICAL ASSOCIATES LLP LAST FOUR DIGITS OF YOUR
Download Your Report to: --> PDF 508 Compliance CSV 2015 ANNUAL QUALITY AND RESOURCE USE REPORT AND THE 2017 VALUE-BASED PAYMENT MODIFIER SOUTHEAST TEXAS MEDICAL ASSOCIATES LLP LAST FOUR DIGITS OF YOUR
CMS Proposals for Quality Reporting Programs Under the 2015 Medicare Physician Fee Schedule Proposed Rule
 CMS Proposals for Quality Reporting Programs Under the 2015 Medicare Physician Fee Schedule Proposed Rule PQRS, EHR Incentive Program, Physician Compare, and VBM Kate Goodrich, M.D., M.H.S. Director, Quality
CMS Proposals for Quality Reporting Programs Under the 2015 Medicare Physician Fee Schedule Proposed Rule PQRS, EHR Incentive Program, Physician Compare, and VBM Kate Goodrich, M.D., M.H.S. Director, Quality
SUMMARY TABLE OF CONTENTS
 FINAL RULE: MEDICARE PROGRAM; ADVANCING CARE COORDINATION THROUGH EPISODE PAYMENT MODELS (EPMs); CARDIAC REHABILITATION INCENTIVE PAYMENT MODEL; AND CHANGES TO THE COMPREHENSIVE CARE FOR JOINT REPLACEMENT
FINAL RULE: MEDICARE PROGRAM; ADVANCING CARE COORDINATION THROUGH EPISODE PAYMENT MODELS (EPMs); CARDIAC REHABILITATION INCENTIVE PAYMENT MODEL; AND CHANGES TO THE COMPREHENSIVE CARE FOR JOINT REPLACEMENT
Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017
 To Dial-in: 877.668.4490 or 408.792.6300 Event Number: 669 367 723 Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017 CMS Final Rule and Materials Advancing Care Coordination through
To Dial-in: 877.668.4490 or 408.792.6300 Event Number: 669 367 723 Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017 CMS Final Rule and Materials Advancing Care Coordination through
CMS makes major proposal impacting outpatient Evaluation & Management (E&M) services
 CMS makes major proposal impacting outpatient Evaluation & Management (E&M) services Proposal Requires physicians to only document up to a Level 2 visit Transitions to a single payment rate for all Level
CMS makes major proposal impacting outpatient Evaluation & Management (E&M) services Proposal Requires physicians to only document up to a Level 2 visit Transitions to a single payment rate for all Level
2018 Quality Measure Benchmarks Overview
 2018 Quality Benchmarks Overview What Are Quality Benchmarks? When a clinician or group submits measures for the Merit-based Incentive Payment System (MIPS) quality performance category, each measure is
2018 Quality Benchmarks Overview What Are Quality Benchmarks? When a clinician or group submits measures for the Merit-based Incentive Payment System (MIPS) quality performance category, each measure is
Merit-Based Incentive Payment System (MIPS): Routine Cataract Removal with Intraocular Lens (IOL) Implantation Measure
 Merit-Based Incentive Payment System (MIPS): Routine Cataract Removal with Intraocular Lens (IOL) Implantation Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
Merit-Based Incentive Payment System (MIPS): Routine Cataract Removal with Intraocular Lens (IOL) Implantation Measure Measure Information Form 2019 Performance Period 1 Table of Contents 1.0 Introduction...
MACRA Final Rule Summary
 MACRA Final Rule Summary On October 14, 2016, the Centers for Medicare and Medicaid Services (CMS) released its final rule implementing the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA),
MACRA Final Rule Summary On October 14, 2016, the Centers for Medicare and Medicaid Services (CMS) released its final rule implementing the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA),
Copyright Scottsdale Institute All Rights Reserved.
 Copyright Scottsdale Institute 2017. All Rights Reserved. No part of this document may be reproduced or shared with anyone outside of your organization without prior written consent from the author(s).
Copyright Scottsdale Institute 2017. All Rights Reserved. No part of this document may be reproduced or shared with anyone outside of your organization without prior written consent from the author(s).
MACRA: Alternative Payment Models Proposed Rule CY 2016
 powered by Vizient & AAMC MACRA: Alternative Payment Models Proposed Rule CY 2016 June 2, 2016 Page 1 Housekeeping When you called in, did you enter your attendee ID number? Dial-in number: 1-866-469-3239
powered by Vizient & AAMC MACRA: Alternative Payment Models Proposed Rule CY 2016 June 2, 2016 Page 1 Housekeeping When you called in, did you enter your attendee ID number? Dial-in number: 1-866-469-3239
A PRIMER FOR PRIMARY CARE
 MACRA / MIPS Transition to value-based payment in Medicare A PRIMER FOR PRIMARY CARE Robert Resnik MD MBA Source: CMS What does MACRA Accomplish? Repeals the Sustainable Growth Rate (SGR) Formula Changes
MACRA / MIPS Transition to value-based payment in Medicare A PRIMER FOR PRIMARY CARE Robert Resnik MD MBA Source: CMS What does MACRA Accomplish? Repeals the Sustainable Growth Rate (SGR) Formula Changes
MACRA: New Medicare Reimbursement Models Sharp HealthCare
 MACRA: New Medicare Reimbursement Models Sharp HealthCare August 15, 2016 Nathan M. Bays, Esq. General Counsel, The Health Management Academy Executive Director, Advisors Caitlin Greenbaum, MPH Director,
MACRA: New Medicare Reimbursement Models Sharp HealthCare August 15, 2016 Nathan M. Bays, Esq. General Counsel, The Health Management Academy Executive Director, Advisors Caitlin Greenbaum, MPH Director,
Medicare s Shared Savings Program: Accountable Care Organizations Proposed Rule
 Medicare s Shared Savings Program: Accountable Care Organizations Proposed Rule On March 31, 2011, the Centers for Medicare and Medicaid Services (CMS) issued its proposed rule on Medicare s Shared Savings
Medicare s Shared Savings Program: Accountable Care Organizations Proposed Rule On March 31, 2011, the Centers for Medicare and Medicaid Services (CMS) issued its proposed rule on Medicare s Shared Savings
Final Rule Summary. Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, December 31, 2021
 Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
ACOs/Shared Savings Demonstration Project: What Does It All Mean?
 ACOs/Shared Savings Demonstration Project: What Does It All Mean? None Conflicts of Interest Sean P. Roddy, MD Albany, NY Accountable Care Organizations Term introduced in 2006 by Fisher et al. the hospital
ACOs/Shared Savings Demonstration Project: What Does It All Mean? None Conflicts of Interest Sean P. Roddy, MD Albany, NY Accountable Care Organizations Term introduced in 2006 by Fisher et al. the hospital
ACO Essentials Series
 ACO Essentials Series How to Use Health Endeavors Technology January, 2017 1/11/2017 1 Agenda Day 1&2 Interactive Analytic Tools Define ACO Goals- Success Plan Organizational Structure Executive TIN and
ACO Essentials Series How to Use Health Endeavors Technology January, 2017 1/11/2017 1 Agenda Day 1&2 Interactive Analytic Tools Define ACO Goals- Success Plan Organizational Structure Executive TIN and
Opportunities for Orthopedic Specialists in BPCI Advanced
 Opportunities for Orthopedic Specialists in BPCI Advanced January 13 th, 2018 Introduction CMS announced the voluntary Bundled Payment for Care Improvement (BPCI) Advanced program on Tuesday, Jan 9 th
Opportunities for Orthopedic Specialists in BPCI Advanced January 13 th, 2018 Introduction CMS announced the voluntary Bundled Payment for Care Improvement (BPCI) Advanced program on Tuesday, Jan 9 th
A Practical Discussion of Value and Quality Based Payments What Do I Do Now?
 Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
2012 Medicare Physician Fee Schedule Final Rule Summary
 2012 Medicare Physician Fee Schedule Final Rule Summary On November, 1, 2011, the Centers for Medicare and Medicaid Services (CMS) posted the final Medicare Physician Fee Schedule (MPFS) for 2012. It is
2012 Medicare Physician Fee Schedule Final Rule Summary On November, 1, 2011, the Centers for Medicare and Medicaid Services (CMS) posted the final Medicare Physician Fee Schedule (MPFS) for 2012. It is
AMERICAN COLLEGE OF GASTROENTEROLOGY MAKING $ENSE OF MACRA
 AMERICAN COLLEGE OF GASTROENTEROLOGY 6400 Goldsboro Road, Suite 200, Bethesda, Maryland 20817-5842; P: 301-263-9000; F: 301-263-9025 MAKING $ENSE OF MACRA CMS.SGR MACRA MIPS APMs QCDRs ACOs Why does Washington
AMERICAN COLLEGE OF GASTROENTEROLOGY 6400 Goldsboro Road, Suite 200, Bethesda, Maryland 20817-5842; P: 301-263-9000; F: 301-263-9025 MAKING $ENSE OF MACRA CMS.SGR MACRA MIPS APMs QCDRs ACOs Why does Washington
Thank you, and enjoy the webinar.
 Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws. This should not be used as legal advice. Itentive recognizes that
Disclaimer This webinar may be recorded. This webinar presents a sampling of best practices and overviews, generalities, and some laws. This should not be used as legal advice. Itentive recognizes that
Topics to be covered. Do I have to participate in MACRA/MIPS/QPP? Choices for participation. Timelines. What is changing with QPP
 Topics to be covered Do I have to participate in MACRA/MIPS/QPP? Choices for participation Timelines What is changing with QPP I have no relevant financial relationships to disclose. Participant engagement
Topics to be covered Do I have to participate in MACRA/MIPS/QPP? Choices for participation Timelines What is changing with QPP I have no relevant financial relationships to disclose. Participant engagement
Next Generation Accountable Care Organization (ACO) Model Overview
 The Physicians Advocacy Institute s Medicare Quality Payment Program (QPP) Physician Education Initiative Next Generation Accountable Care Organization (ACO) Model Overview Ad 1 P a g e MEDICARE QPP PHYSICIAN
The Physicians Advocacy Institute s Medicare Quality Payment Program (QPP) Physician Education Initiative Next Generation Accountable Care Organization (ACO) Model Overview Ad 1 P a g e MEDICARE QPP PHYSICIAN
September 6, Re: CMS-1600-P; CY 2014 Physician Fee Schedule Proposed rule comments
 September 6, 2013 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention CMS-1600-P Mail Stop C4-26-05 7500 Security Boulevard Baltimore, MD 21244-1850 Re: CMS-1600-P;
September 6, 2013 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention CMS-1600-P Mail Stop C4-26-05 7500 Security Boulevard Baltimore, MD 21244-1850 Re: CMS-1600-P;
CMS 1701 P UnityPoint Health. October 16, 2018
 CMS 1701 P UnityPoint Health 1776 West Lakes Parkway, Suite 400 West Des Moines, IA 50266 unitypoint.org October 16, 2018 Seema Verma, Administrator Centers for Medicare & Medicaid Services Department
CMS 1701 P UnityPoint Health 1776 West Lakes Parkway, Suite 400 West Des Moines, IA 50266 unitypoint.org October 16, 2018 Seema Verma, Administrator Centers for Medicare & Medicaid Services Department
Impact of Work RVU Changes. Impact of PE RVU Changes. Total $93,149 0% 0% 0% 0% $1,745 0% 1% 0% 1%
 On November 2, 2017, the Centers for Medicare & Medicaid Services (CMS) issued the Medicare Physician Fee Schedule (MPFS) final rule. The final rule updates the payment policies, payment rates, and quality
On November 2, 2017, the Centers for Medicare & Medicaid Services (CMS) issued the Medicare Physician Fee Schedule (MPFS) final rule. The final rule updates the payment policies, payment rates, and quality
2018 Final Rule from CMS for the Quality Payment Program
 2018 Final Rule from CMS for the Quality Payment Program Starting at Noon EST Wed 12/6/2017 Dr. Dan Mingle Register for Webinars or Access Recordings http://mingleanalytics.com/webinars 2017 Mingle Analytics
2018 Final Rule from CMS for the Quality Payment Program Starting at Noon EST Wed 12/6/2017 Dr. Dan Mingle Register for Webinars or Access Recordings http://mingleanalytics.com/webinars 2017 Mingle Analytics
4/8/17. The Changing Nature of Physician Payment and Health Care Reform in The AMA A Unifying Voice for Physicians
 The Changing Nature of Physician Payment and Health Care Reform in 2017 U of Mo Family Medicine Update April 7, 2017 David Barbe, MD MHA President-elect American Medical Association VP Regional Operations
The Changing Nature of Physician Payment and Health Care Reform in 2017 U of Mo Family Medicine Update April 7, 2017 David Barbe, MD MHA President-elect American Medical Association VP Regional Operations
CPC+ PAYMENT METHODOLOGIES: BENEFICIARY ATTRIBUTION, CARE MANAGEMENT FEE, PERFORMANCE-BASED INCENTIVE PAYMENT, AND PAYMENT UNDER THE MEDICARE
 CPC+ PAYMENT METHODOLOGIES: BENEFICIARY ATTRIBUTION, CARE MANAGEMENT FEE, PERFORMANCE-BASED INCENTIVE PAYMENT, AND PAYMENT UNDER THE MEDICARE PHYSICIAN FEE SCHEDULE Version 2 February 17, 2017 Table of
CPC+ PAYMENT METHODOLOGIES: BENEFICIARY ATTRIBUTION, CARE MANAGEMENT FEE, PERFORMANCE-BASED INCENTIVE PAYMENT, AND PAYMENT UNDER THE MEDICARE PHYSICIAN FEE SCHEDULE Version 2 February 17, 2017 Table of
Health Care Policy Landscape: Market Trends & Frontline Perspectives
 Health Care Policy Landscape: Market Trends & Frontline Perspectives December 1, 2016 www.leavittpartners.com Post-Election, New Administration Insights Top 10 Health Policy Actions to Watch 1 2 3 4 Substantial
Health Care Policy Landscape: Market Trends & Frontline Perspectives December 1, 2016 www.leavittpartners.com Post-Election, New Administration Insights Top 10 Health Policy Actions to Watch 1 2 3 4 Substantial
AMGA MIPS Collaborative. June 21, 2017
 AMGA MIPS Collaborative June 21, 2017 Calculating the MIPS score The MIPS composite performance score will include four weighted categories: MIPS Composite Performance Score Quality Cost Improvement activities
AMGA MIPS Collaborative June 21, 2017 Calculating the MIPS score The MIPS composite performance score will include four weighted categories: MIPS Composite Performance Score Quality Cost Improvement activities
New Medicare Merit-Based Incentive Payment System: Navigating Changes Under MACRA
 Presenting a live 90-minute webinar with interactive Q&A New Medicare Merit-Based Incentive Payment System: Navigating Changes Under MACRA Overcoming Challenges in Transforming Payment and Care Delivery
Presenting a live 90-minute webinar with interactive Q&A New Medicare Merit-Based Incentive Payment System: Navigating Changes Under MACRA Overcoming Challenges in Transforming Payment and Care Delivery
Predictive Qualifying Alternative Payment Model (APM) Participants (QPs) Methodology Fact Sheet What is the Predictive QP Status Analysis?
 Predictive Qualifying Alternative Payment Model (APM) Participants (QPs) Methodology Fact Sheet What is the Predictive QP Status Analysis? One of the Quality Payment Program s goals is to be clear about
Predictive Qualifying Alternative Payment Model (APM) Participants (QPs) Methodology Fact Sheet What is the Predictive QP Status Analysis? One of the Quality Payment Program s goals is to be clear about
HEALTH POLICY & EDUCATION SERIES
 HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
Revenue Portfolio Design and Care Transformation: or How I Learned to Love Bundles. TAHFA/HFMA Road show Lubbock, Texas
 Revenue Portfolio Design and Care Transformation: or How I Learned to Love Bundles TAHFA/HFMA Road show Lubbock, Texas February 17, 2017 Its Friday so This will be low stress 2 Goals of Our Session In
Revenue Portfolio Design and Care Transformation: or How I Learned to Love Bundles TAHFA/HFMA Road show Lubbock, Texas February 17, 2017 Its Friday so This will be low stress 2 Goals of Our Session In
Evidence-Based Program Reimbursement Strategies. Timothy P. McNeill, RN, MPH
 Evidence-Based Program Reimbursement Strategies Timothy P. McNeill, RN, MPH 1 Medicare & Value Based Purchasing 2 Medicare Advantage Changes 3 DSMT Requirements 4 CDSME Tip Sheet Opportunities for EB Programs
Evidence-Based Program Reimbursement Strategies Timothy P. McNeill, RN, MPH 1 Medicare & Value Based Purchasing 2 Medicare Advantage Changes 3 DSMT Requirements 4 CDSME Tip Sheet Opportunities for EB Programs
MACRA: How the 2018 Quality Payment Program Final Rule Impacts Providers
 Medical Group Strategy Council MACRA: How the 2018 Quality Payment Program Final Rule Impacts Providers Rob Lazerow Managing Director Tony Panjamapirom Senior Consultant Hamza Hasan Practice Manager Julie
Medical Group Strategy Council MACRA: How the 2018 Quality Payment Program Final Rule Impacts Providers Rob Lazerow Managing Director Tony Panjamapirom Senior Consultant Hamza Hasan Practice Manager Julie
Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study
 Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study Presented by Bill O Brien, FSA, MAAA Consulting Actuary Milliman Houston, TX (832) 878-4078 Preconference I Agenda
Risk Adjusted Episodes as Benchmarks for ACOs: A Society of Actuaries Sponsored Study Presented by Bill O Brien, FSA, MAAA Consulting Actuary Milliman Houston, TX (832) 878-4078 Preconference I Agenda
Key Financial and Operational Impacts from the Proposed Rule to Implement MACRA:
 Key Financial and Operational Impacts from the Proposed Rule to Implement MACRA: The proposed rule implementing Access and CHIP Reauthorization Act of 2015 (MACRA) was made available on May 9, 2016. A
Key Financial and Operational Impacts from the Proposed Rule to Implement MACRA: The proposed rule implementing Access and CHIP Reauthorization Act of 2015 (MACRA) was made available on May 9, 2016. A
HFMA s Regulatory Sound Bites. An Overview of the Final 2019 Inpatient Prospective Payment System Rule & Quick look at the Proposed 2019 OPPS
 HFMA s Regulatory Sound Bites An Overview of the Final 2019 Inpatient Prospective Payment System Rule & Quick look at the Proposed 2019 OPPS Presentation Objectives Review the 2019 Final Medicare Inpatient
HFMA s Regulatory Sound Bites An Overview of the Final 2019 Inpatient Prospective Payment System Rule & Quick look at the Proposed 2019 OPPS Presentation Objectives Review the 2019 Final Medicare Inpatient
2018 Washington Update
 2018 Washington Update Drew Voytal, MPA Associate Director MGMA Government Affairs 2018 MGMA. All rights reserved. - 1 - - 2 - Agenda Current political and legislative environment Evolving federal payment
2018 Washington Update Drew Voytal, MPA Associate Director MGMA Government Affairs 2018 MGMA. All rights reserved. - 1 - - 2 - Agenda Current political and legislative environment Evolving federal payment
Medicare Quality Payment Program Overview (MACRA)
 Medicare Quality Payment Program Overview (MACRA) December 2016 Rev. 12/1/16 Some general observations MACRA is complex More than a replacement for the SGR Many of the new requirements are revisions to
Medicare Quality Payment Program Overview (MACRA) December 2016 Rev. 12/1/16 Some general observations MACRA is complex More than a replacement for the SGR Many of the new requirements are revisions to
2013 Medicare Physician Fee Schedule Proposed Rule Summary
 2013 Medicare Physician Fee Schedule Proposed Rule Summary On July 6, 2012, CMS issued the 2013 Medicare physician fee schedule (PFS) proposed rule, which was published in the Federal Register on July
2013 Medicare Physician Fee Schedule Proposed Rule Summary On July 6, 2012, CMS issued the 2013 Medicare physician fee schedule (PFS) proposed rule, which was published in the Federal Register on July
2018 Quality Payment Program Final Rule. Summary
 Summary On Thursday, November 3, 2017, CMS issued the 2018 Quality Payment Program (QPP) final rule. Comments on the final rule are due January 1, 2018. The QPP encompasses the Merit-based Incentive Payment
Summary On Thursday, November 3, 2017, CMS issued the 2018 Quality Payment Program (QPP) final rule. Comments on the final rule are due January 1, 2018. The QPP encompasses the Merit-based Incentive Payment
Improving your ASC s performance in 2018
 Improving your ASC s performance in 2018 The ASC guide to major trends that will impact your practice Marilyn Denegre Rumbin, JD MBA Director, Payer & Reimbursement Strategy February 2018 1 Welcome Marilyn
Improving your ASC s performance in 2018 The ASC guide to major trends that will impact your practice Marilyn Denegre Rumbin, JD MBA Director, Payer & Reimbursement Strategy February 2018 1 Welcome Marilyn
Scripps Health ACO Update
 June 2016 Scripps Health ACO Update Marc Reynolds Senior Vice President, Payer Relations Scripps Health Anil N. Keswani, MD Corporate Vice President, Population Health Management Scripps Health 10 Key
June 2016 Scripps Health ACO Update Marc Reynolds Senior Vice President, Payer Relations Scripps Health Anil N. Keswani, MD Corporate Vice President, Population Health Management Scripps Health 10 Key
MACRA: Redefining How CMS Pays Doctors. White Paper ELLIS MAC KNIGHT, MD DAN KIEHL, JD CONTACT. Senior Vice President/CMO. Associate Consultant
 MACRA: Redefining How CMS Pays Doctors White Paper ELLIS MAC KNIGHT, MD Senior Vice President/CMO DAN KIEHL, JD Associate Consultant June 2016 CONTACT For further information about Coker Group and how
MACRA: Redefining How CMS Pays Doctors White Paper ELLIS MAC KNIGHT, MD Senior Vice President/CMO DAN KIEHL, JD Associate Consultant June 2016 CONTACT For further information about Coker Group and how
Evolving Payment Methods EVOLVING PAYMENT METHODS. Melinda Hancock National HFMA Chair Elect January 23, 2015
 Evolving Payment Methods EVOLVING PAYMENT METHODS Melinda Hancock National HFMA Chair Elect January 23, 2015 Medicare IP Reductions OCT OCT OCT OCT OCT OCT OCT OCT OCT 2012 2013 2014 2015 2016 2017 2018
Evolving Payment Methods EVOLVING PAYMENT METHODS Melinda Hancock National HFMA Chair Elect January 23, 2015 Medicare IP Reductions OCT OCT OCT OCT OCT OCT OCT OCT OCT 2012 2013 2014 2015 2016 2017 2018
Introduction to the Centers for Medicare & Medicaid Services (CMS) Payment Process
 Introduction to the Centers for Medicare & Medicaid Services (CMS) Payment Process Thomas Barker, Foley Hoag LLP tbarker@foleyhoag.com (202) 261-7310 October 1, 2009 Overview Medicare Basics Paths to Medicare
Introduction to the Centers for Medicare & Medicaid Services (CMS) Payment Process Thomas Barker, Foley Hoag LLP tbarker@foleyhoag.com (202) 261-7310 October 1, 2009 Overview Medicare Basics Paths to Medicare
Growth and Success of Accountable Care Organizations (ACOs) in the US from Dennis Horrigan June 2016
 Growth and Success of Accountable Care Organizations (ACOs) in the US from 2010-2016 Dennis Horrigan June 2016 Introducing Dennis Horrigan Dennis R. Horrigan President and Chief Executive Officer Catholic
Growth and Success of Accountable Care Organizations (ACOs) in the US from 2010-2016 Dennis Horrigan June 2016 Introducing Dennis Horrigan Dennis R. Horrigan President and Chief Executive Officer Catholic
Housekeeping. Questions
 Housekeeping To join us on audio, dial the phone number in the teleconference box and follow the prompts. Please dial in with your Attendee ID number. The Attendee ID number will connect your name in WebEx
Housekeeping To join us on audio, dial the phone number in the teleconference box and follow the prompts. Please dial in with your Attendee ID number. The Attendee ID number will connect your name in WebEx
September 6, Submitted on September 6, 2016 via Dear Acting Administrator Slavitt:
 September 6, 2016 Andrew Slavitt Acting Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services Hubert H. Humphrey Building 200 Independence Avenue, S.W. Washington,
September 6, 2016 Andrew Slavitt Acting Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services Hubert H. Humphrey Building 200 Independence Avenue, S.W. Washington,
Future Healthcare Payment Models An Overview
 Future Healthcare Payment Models An Overview Carter Dredge THERE IS A CRITICAL NEED TO TRANSFORM HEALTHCARE DELIVERY & PAYMENT 2 Significant Variation in Population Utilization Spine Surgeries per 1,000
Future Healthcare Payment Models An Overview Carter Dredge THERE IS A CRITICAL NEED TO TRANSFORM HEALTHCARE DELIVERY & PAYMENT 2 Significant Variation in Population Utilization Spine Surgeries per 1,000
QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW
 QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NEAL LOGUE, HEALTH INSURANCE SPECIALIST, DIVISION OF FINANCIAL MANAGEMENT & FEE FOR SERVICE OPERATIONS DECEMBER 12, 2018 Disclaimers This presentation
QUALITY PAYMENT PROGRAM YEAR 3 (2019) FINAL RULE OVERVIEW NEAL LOGUE, HEALTH INSURANCE SPECIALIST, DIVISION OF FINANCIAL MANAGEMENT & FEE FOR SERVICE OPERATIONS DECEMBER 12, 2018 Disclaimers This presentation
Get Straight on MACRA in 2018
 Quality Reporting Roundtable Get Straight on MACRA in 2018 FAQs, Advisory Board Guidance, and Resources Ye Hoffman, MS, CPHIMS Consultant March 27, 2018 research technology consulting 2 Manage Your Audio
Quality Reporting Roundtable Get Straight on MACRA in 2018 FAQs, Advisory Board Guidance, and Resources Ye Hoffman, MS, CPHIMS Consultant March 27, 2018 research technology consulting 2 Manage Your Audio
CMS released the 2018 Physician Fee Schedule Final Rule last week. The following is a summary of the AHRA-related policies.
 CMS released the 2018 Physician Fee Schedule Final Rule last week. The following is a summary of the AHRA-related policies. 1. Appropriate Use Criteria Delayed Until 2020 CMS had already proposed to delay
CMS released the 2018 Physician Fee Schedule Final Rule last week. The following is a summary of the AHRA-related policies. 1. Appropriate Use Criteria Delayed Until 2020 CMS had already proposed to delay
2019 Hospital Outpatient and Ambulatory Surgery Payment Systems (OPPS) Proposed Rule Summary (Last revised on July 28, 2018)
 2019 Hospital Outpatient and Ambulatory Surgery Payment Systems (OPPS) Proposed Rule Summary (Last revised on July 28, 2018) The Centers for Medicare and Medicaid Services (CMS) released the 2019 Hospital
2019 Hospital Outpatient and Ambulatory Surgery Payment Systems (OPPS) Proposed Rule Summary (Last revised on July 28, 2018) The Centers for Medicare and Medicaid Services (CMS) released the 2019 Hospital
Stakeholder Innovation Group (SIG):
 Stakeholder Innovation Group (SIG): Intake Form for New Payment Model Idea that Requires State/Federal Approval (to be added to the Innovations Website) Purpose: The purpose of this form is to collect
Stakeholder Innovation Group (SIG): Intake Form for New Payment Model Idea that Requires State/Federal Approval (to be added to the Innovations Website) Purpose: The purpose of this form is to collect
21% Total Medicare Beneficiaries (2017): 58 million
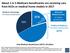 About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
Population Health and Wellness: 2 Stories from Cleveland Clinic. Elizabeth Sump Senior Director, Health Policy Cleveland Clinic
 Population Health and Wellness: 2 Stories from Cleveland Clinic Elizabeth Sump Senior Director, Health Policy Cleveland Clinic 1 2 population health stories Cleveland Clinic Employee Health Plan Cleveland
Population Health and Wellness: 2 Stories from Cleveland Clinic Elizabeth Sump Senior Director, Health Policy Cleveland Clinic 1 2 population health stories Cleveland Clinic Employee Health Plan Cleveland
Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]
![Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701] Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]](/thumbs/87/96500790.jpg) Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
WORKERS COMPENSATION REFORMS OFFICIAL MEDICAL FEE SCHEDULE PHYSICIAN SERVICES SUMMARY CHANGES TO THE OFFICIAL MEDICAL FEE SCHEDULE PHYSICIAN SERVICES
 SUMMARY CHANGES TO THE SB 863, enacted in 2012, required the Division of Workers Compensation to transition the Official Medical Fee Schedule for physician services to a Medicare RBRVS system over four
SUMMARY CHANGES TO THE SB 863, enacted in 2012, required the Division of Workers Compensation to transition the Official Medical Fee Schedule for physician services to a Medicare RBRVS system over four
You Down with QPP? Daniel Collins Director of Finance Orlando Health Physician Enterprise
 You Down with QPP? Daniel Collins Director of Finance Orlando Health Physician Enterprise Why Was the QPP created? Source: https://www.youtube.com/watch?v=7df7chghas4 What is QPP? Quality Payment Program
You Down with QPP? Daniel Collins Director of Finance Orlando Health Physician Enterprise Why Was the QPP created? Source: https://www.youtube.com/watch?v=7df7chghas4 What is QPP? Quality Payment Program
Session 1: Mandated Report: Medicare Payment for Ambulance Services
 Medicare Payment Advisory Committee Meeting, Nov. 1 2 Session 1: Mandated Report: Medicare Payment for Ambulance Services Session 2: Reducing the Hospitalization Rate for Medicare Beneficiaries Receiving
Medicare Payment Advisory Committee Meeting, Nov. 1 2 Session 1: Mandated Report: Medicare Payment for Ambulance Services Session 2: Reducing the Hospitalization Rate for Medicare Beneficiaries Receiving
Using Analytics To Transform Your ACO
 Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
Using Analytics To Transform Your ACO How to Develop Effective Cost Reduction Strategies Presented July 2016 Agenda and Presenter External Forces and Market Response Critical Success Factors Analytics
No change from proposed rule. healthcare providers and suppliers of services (e.g.,
 American College of Physicians Medicare Shared Savings/Accountable Care Organization (ACO) Final Rule Summary Analysis Category Final Rule Summary Change from Proposed Rule and Comments ACO refers to a
American College of Physicians Medicare Shared Savings/Accountable Care Organization (ACO) Final Rule Summary Analysis Category Final Rule Summary Change from Proposed Rule and Comments ACO refers to a
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business?
 Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
HEALTH ECONOMICS AND REIMBURSEMENT
 HEALTH ECONOMICS AND REIMBURSEMENT VASCULAR CY 2016 MEDICARE PHYSICIAN FEE SCHEDULE (PFS) UPDATE Abbott Vascular is pleased to provide you with this summary of the Medicare Physician Fee Schedule (PFS)
HEALTH ECONOMICS AND REIMBURSEMENT VASCULAR CY 2016 MEDICARE PHYSICIAN FEE SCHEDULE (PFS) UPDATE Abbott Vascular is pleased to provide you with this summary of the Medicare Physician Fee Schedule (PFS)
Payment for Covered Services
 A WellCare Company Payment for Covered Services Today s Options PFFS reimburses deemed (non-contracted) providers at 100% of the current Medicare-approved amount for all Medicare-covered services, less
A WellCare Company Payment for Covered Services Today s Options PFFS reimburses deemed (non-contracted) providers at 100% of the current Medicare-approved amount for all Medicare-covered services, less
