Prescription Drug Plan Update
|
|
|
- Kory Dawson
- 5 years ago
- Views:
Transcription
1 Prescription Drug Plan Update Kenyon College May 24,
2 Plan Design Changes effective July 1, 2018 Basic Plan Current Basic Plan 7/1/2018 Premium Plan Current Premium Plan 7/1/2018 Annual Deductible $75 / $225 None $50 / $150 None Retail 30 day supply Tier 1 20% after ded. $10 min, $200 max. 10%, $10 min, $150 max. 20% after ded. $150 max. 10%, $10 min, $150 max. Tier 2 20% after ded. $10 min, $200 max. 20%, $25 min, $150 max. 20% after ded. $150 max. 20%, $25 min, $150 max. Tier 3 20% after ded. $10 min, $200 max. 30%, $50 min, $250 max. 20% after ded. $150 max. 30%, $50 min, $250 max. Mail Order 90 day supply (Tier 1/2/3) No coverage $20 / $50 / $100 $15 / $30 / $45 $20 / $50 / $100 Note: Copays charged will be the lesser of: the actual cost of the drug; Or the minimum copay amount listed in the chart above. 2
3 RxOC Clinical Trend Package-Effective 07/01/2018 Category Drug Quantity Management (DQM) Description Aligns the dispensed quantity of prescription medication with FDAapproved dosage guidelines Prior Authorization (PA) Monitors to ensure the appropriate medication at the appropriate time in therapy Preferred Specialty Management (PSM) Step Therapy (ST) Reduces waste by promoting the use of cost effective front line drugs in therapy classes where clinically available Reduces waste by promoting the use of generics and cost effective front line drugs in therapy classes where clinically available Fraud, Waste and Abuse (FWA) Retrospective Drug Utilization (RDUR) Investigative service program that helps plan sponsors identify potential problem prescribers and members with unusual or excessive utilization patterns Evaluates a prescription against a patient s prescription history and evidence-based guidelines to alert the prescribing physician to important, drug-specific, patient-specific health and safety issues 3
4 Voluntary Smart90 CVS-Effective 08/01/2018 Maintenance medication network Member chooses where to fill maintenance medications Express Scripts Pharmacy SM CVS Pharmacy TM Value Adherence Savings Our independent model combined with size and scale drives greater value, no matter where a member chooses to fill Members filling prescriptions for 90-day supplies are 19% more adherent to their therapy regimen Greater savings for both plan sponsors and members 4
5 * Price may vary slightly at retail vs. home delivery for coinsurance plans. 5
6 Prior Authorization: The Right Patient Prior Authorization ensures the clinically appropriate use of medications. Prior Authorization ensures that medications are used safely. Prior Authorization asks the question: Is this the right medication for this patient? 6
7 How Prior Authorization Works Drives savings and patient safety through monitoring: Targeted, high-cost medications Medications with the highest potential for inappropriate use If an active prior authorization exists, claim pays Physician Visit Rx written RPh System checks existing prior authorization Prior authorization required; call physician QUICKER PROCESS IF SUBMITTED ELECTRONICALLY If no active prior authorization exists, claim rejects Physician contacts PA department If clinical criteria is met, then an override is issued, and the claim will pay If criteria is not met, then claim will reject 7
8 Prior Authorization sample template member letter 8
9 Step Therapy: The Right Drug Step Therapy encourages members and physicians to try clinically effective, front-line medications (usually generics) before trying second-line (usually brand name) medications Step Therapy asks the question What other medications has this patient taken for this condition? All members currently on a drug with a Step Therapy will be Grandfathered. 9
10 How Step Therapy Works Step therapy reduces waste by promoting the use of generics If history is present, claim pays Physician Visit Rx written RPh System checks for history of step 1 or step 2 drug(s) If no history, claim rejects Prior authorization required; call physician; must try step 1 drug first After 4 days, if claim for front line or back-up drug(s) is not in system, ESI contacts member and physician explaining process 10
11 Step Therapy sample template member letter 11
12 Drug Quantity Management: The Right Amount Drug Quantity Management aligns the quantity dispensed with FDAapproved dosage guidelines and other supportive evidence Drug Quantity Management asks Is this the correct quantity (tablets/capsules) of this medication? 12
13 How Drug Quantity Management Works Aligns the dispensed quantity of prescription medication with FDA-approved dosage guidelines Ensures that the most cost-effective product strength is dispensed Helps reduce waste in the pharmacy benefit If quantity is less than or equal to program limit, the claim pays Physician Visit Rx written RPh System checks for appropriate quantity Messaging to pharmacy with maximum quantity allowed RPh can submit for allowed amount or ask physician to request an exception If quantity exceeds the program limit the claim rejects 13
14 Drug Quantity Management sample template member letter 14
15 15
Individual Business Prescription Drug Utilization Management Changes Frequently Asked Questions
 Individual Business Prescription Drug Utilization Management Changes Frequently Asked Questions Overview: Up to six prescription drug utilization/benefit management (UM) programs will be added to the individual
Individual Business Prescription Drug Utilization Management Changes Frequently Asked Questions Overview: Up to six prescription drug utilization/benefit management (UM) programs will be added to the individual
CDHP Special Administration
 CDHP Special Administration Your prescription coverage under the Consumer Driven Health Plan (CDHP) is subject to special administration from the PPO plans and this page will explain those differences:
CDHP Special Administration Your prescription coverage under the Consumer Driven Health Plan (CDHP) is subject to special administration from the PPO plans and this page will explain those differences:
Plan Comparison Checklist
 Plan Comparison Checklist Date: The chart below should serve as a comprehensive guide for users when comparing health insurance plans during open enrollment. This chart is also used by Compass case managers
Plan Comparison Checklist Date: The chart below should serve as a comprehensive guide for users when comparing health insurance plans during open enrollment. This chart is also used by Compass case managers
Medicare Part D Transition Policy CY 2018 HCSC Medicare Part D
 Contract: H0107, H0927, H1666, H3251, H3822, H3979, H8133, H8634, H8554, S5715 Policy Name: Medicare Formulary Transition Purpose: This procedure describes the standard process Health Care Service Corporation
Contract: H0107, H0927, H1666, H3251, H3822, H3979, H8133, H8634, H8554, S5715 Policy Name: Medicare Formulary Transition Purpose: This procedure describes the standard process Health Care Service Corporation
Understanding Your Prescription Program. CCIU Employee Meeting September 7, 2016
 Understanding Your Prescription Program CCIU Employee Meeting September 7, 2016 Welcome to FutureScripts! Founded in 2006 Philadelphia presence Strong ties to community and local businesses 68,000 pharmacies
Understanding Your Prescription Program CCIU Employee Meeting September 7, 2016 Welcome to FutureScripts! Founded in 2006 Philadelphia presence Strong ties to community and local businesses 68,000 pharmacies
Pharmacy Benefit Management in Oncology
 Pharmacy Benefit Management in Oncology October 28 th, 2015 Business Health Care Group Protecting the Future of Oncology Care: A Community Conversation Brent Eberle RPh MBA Chief Pharmacy Officer, Navitus
Pharmacy Benefit Management in Oncology October 28 th, 2015 Business Health Care Group Protecting the Future of Oncology Care: A Community Conversation Brent Eberle RPh MBA Chief Pharmacy Officer, Navitus
2019 Transition Policy
 2019 Number: 5.8 Prescription Drug Replaces: 5.8 v.2018 Cross 5.1.2 Transition Fill Monitoring Procedure References: Purpose: To provide guidance on the transition process for new or current Plan members
2019 Number: 5.8 Prescription Drug Replaces: 5.8 v.2018 Cross 5.1.2 Transition Fill Monitoring Procedure References: Purpose: To provide guidance on the transition process for new or current Plan members
2015 PacificSource Medicare Part D Transition Process for contracts H3864 & H4754:
 2015 PacificSource Medicare Part D Transition Process for contracts H3864 & H4754: Essentials Rx 6 (HMO), Essentials Rx 14 (HMO), Essentials Rx 15 (HMO), Essentials Rx 16 (HMO), Essentials Rx 19 (HMO),
2015 PacificSource Medicare Part D Transition Process for contracts H3864 & H4754: Essentials Rx 6 (HMO), Essentials Rx 14 (HMO), Essentials Rx 15 (HMO), Essentials Rx 16 (HMO), Essentials Rx 19 (HMO),
SecurityBlue HMO. Link to Specific Guidance Regarding Exceptions and Appeals
 SecurityBlue HMO Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality
SecurityBlue HMO Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality
2018 Medicare Part D Transition Policy
 Regulation/ Requirements Purpose Scope Policy 2018 Medicare Part D Transition Policy 42 CFR 423.120(b)(3) 42 CFR 423.154(a)(1)(i) 42 CFR 423.578(b) Medicare Prescription Drug Benefit Manual, Chapter 6,
Regulation/ Requirements Purpose Scope Policy 2018 Medicare Part D Transition Policy 42 CFR 423.120(b)(3) 42 CFR 423.154(a)(1)(i) 42 CFR 423.578(b) Medicare Prescription Drug Benefit Manual, Chapter 6,
Amerigroup Medicare Member PBM Conversion Talking Points
 Amerigroup Medicare Member PBM Conversion Talking Points Overview On January 1, 2015, pharmacy benefits for L-Amerigroup Amerivantage (AMV) members will be covered through Express Scripts, Inc. (ESI).
Amerigroup Medicare Member PBM Conversion Talking Points Overview On January 1, 2015, pharmacy benefits for L-Amerigroup Amerivantage (AMV) members will be covered through Express Scripts, Inc. (ESI).
The State of New Mexico Group Benefits Plan Plan Year: January December 2018 Prescription Drug Program
 The State of New Mexico Group Benefits Plan Plan Year: January December 2018 Prescription Drug Program 1 Who Is Express Scripts? Express Scripts administers your prescription drug benefit and you automatically
The State of New Mexico Group Benefits Plan Plan Year: January December 2018 Prescription Drug Program 1 Who Is Express Scripts? Express Scripts administers your prescription drug benefit and you automatically
BlueRx PDP. Link to Specific Guidance Regarding Exceptions and Appeals
 BlueRx PDP Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality Assurance
BlueRx PDP Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality Assurance
Lindsey Imada, PharmD Candidate 2016 Midwestern University, Chicago College of Pharmacy
 Lindsey Imada, PharmD Candidate 2016 Midwestern University, Chicago College of Pharmacy Under the Preceptorship of Dr. Craig Stern Pro Pharma Pharmaceutical Consultants, Inc. September 11, 2015 S OBJECTIVES
Lindsey Imada, PharmD Candidate 2016 Midwestern University, Chicago College of Pharmacy Under the Preceptorship of Dr. Craig Stern Pro Pharma Pharmaceutical Consultants, Inc. September 11, 2015 S OBJECTIVES
2012 Medicare Part D Transition Process for contracts H3864 & H4754:
 2012 Medicare Part D Transition Process for contracts H3864 & H4754: Essentials Rx 6, Essentials Rx 14, Essentials Rx 15, Essentials Rx 16, Premier Rx 7, Explorer Rx 1, Explorer Rx 2, and Explorer Rx 4
2012 Medicare Part D Transition Process for contracts H3864 & H4754: Essentials Rx 6, Essentials Rx 14, Essentials Rx 15, Essentials Rx 16, Premier Rx 7, Explorer Rx 1, Explorer Rx 2, and Explorer Rx 4
Innovative Strategies for Managing the Rising Cost of Specialty Drugs
 Innovative Strategies for Managing the Rising Cost of Specialty Drugs Mid-sized Retirement and Healthcare Plan Management Conference Chicago, IL June 5, 2013 Managing the Rising Cost of Specialty Drugs
Innovative Strategies for Managing the Rising Cost of Specialty Drugs Mid-sized Retirement and Healthcare Plan Management Conference Chicago, IL June 5, 2013 Managing the Rising Cost of Specialty Drugs
Medicare Advantage Part D Pharmacy Policy
 Page 1 of 27 DISCLAIMER NOTICE: The purpose of this policy is to provide guidance for benefit and coverage determinations only. Benefit and coverage determinations are subject to the contractual limitations
Page 1 of 27 DISCLAIMER NOTICE: The purpose of this policy is to provide guidance for benefit and coverage determinations only. Benefit and coverage determinations are subject to the contractual limitations
Best Practice Recommendation for
 Best Practice Recommendation for Exchanging & Processing about Pharmacy Benefit Management Version 020915a Issue Date Version Explanation 10-20-2014 First Release 02-09-15 Clarify language under Health
Best Practice Recommendation for Exchanging & Processing about Pharmacy Benefit Management Version 020915a Issue Date Version Explanation 10-20-2014 First Release 02-09-15 Clarify language under Health
2008 Medicare Part D: Pharmacist's Survival Guide. Ronnie DePue, R.Ph., CGP
 2008 Medicare Part D: Pharmacist's Survival Guide Ronnie DePue, R.Ph., CGP Objectives At the completion of this program, the participant will be able to: 1. Give an overview of the Medicare Prescription
2008 Medicare Part D: Pharmacist's Survival Guide Ronnie DePue, R.Ph., CGP Objectives At the completion of this program, the participant will be able to: 1. Give an overview of the Medicare Prescription
Classification: Clinical Department Policy Number: Subject: Medicare Part D General Transition
 Classification: Clinical Department Policy Number: 3404.00 Subject: Medicare Part D General Transition Effective Date: 01/01/2019 Process Date Revised: 07/20/2018 Date Reviewed: 05/29/2018 POLICY STATEMENT:
Classification: Clinical Department Policy Number: 3404.00 Subject: Medicare Part D General Transition Effective Date: 01/01/2019 Process Date Revised: 07/20/2018 Date Reviewed: 05/29/2018 POLICY STATEMENT:
Medicare Transition POLICY AND PROCEDURES
 Medicare Transition POLICY AND PROCEDURES POLICY The Plan will maintain an appropriate transition process, consistent with 42 CFR 423.120(b)(3), Chapter 6 of the Medicare Prescription Drug Benefit Manual
Medicare Transition POLICY AND PROCEDURES POLICY The Plan will maintain an appropriate transition process, consistent with 42 CFR 423.120(b)(3), Chapter 6 of the Medicare Prescription Drug Benefit Manual
Arkansas State University System Prescription Drug Program
 Arkansas State University System Prescription Drug Program The Arkansas State University (ASU) prescription drug program involves a partnership with the University of Arkansas for Medical Sciences (UAMS)
Arkansas State University System Prescription Drug Program The Arkansas State University (ASU) prescription drug program involves a partnership with the University of Arkansas for Medical Sciences (UAMS)
White Paper: Formulary Development at Express Scripts
 White Paper: Formulary Development at Express Scripts Express Scripts works with health-benefit plan sponsors and individual members of health plans to provide affordable access to clinically sound, high-quality
White Paper: Formulary Development at Express Scripts Express Scripts works with health-benefit plan sponsors and individual members of health plans to provide affordable access to clinically sound, high-quality
Chapter 17: Pharmacy and Drug Formulary
 Chapter 17: Pharmacy and Drug Formulary Introduction Health Choice Insurance Co. (Health Choice) is pleased to provide the Health Choice Formulary, which is available on line at www.healthchoiceessential.com/members/rxdrugs.
Chapter 17: Pharmacy and Drug Formulary Introduction Health Choice Insurance Co. (Health Choice) is pleased to provide the Health Choice Formulary, which is available on line at www.healthchoiceessential.com/members/rxdrugs.
Prescription Medication Rider
 Prescription Medication Rider Rx Member Cost-Sharing: $16/$40/$80/$90 According to this prescription medication program, you may receive coverage for prescription medications in the amounts specified in
Prescription Medication Rider Rx Member Cost-Sharing: $16/$40/$80/$90 According to this prescription medication program, you may receive coverage for prescription medications in the amounts specified in
Farm Bureau Select Rx 2017 Summary of Benefits January 1, December 31, 2017
 P.O. Box 266380 Weston, FL 33326 Farm Bureau Select Rx 2017 Summary of Benefits January 1, 2017 - December 31, 2017 Thank you for your interest in Farm Bureau Select Rx, Our plan is offered by Members
P.O. Box 266380 Weston, FL 33326 Farm Bureau Select Rx 2017 Summary of Benefits January 1, 2017 - December 31, 2017 Thank you for your interest in Farm Bureau Select Rx, Our plan is offered by Members
Prescription Medication Schedule of Benefits
 Prescription Medication Schedule of Benefits Rx Member Cost-Sharing: $15/$35/$70/$70 When you go to a pharmacy that participates in the UPMC Health Plan pharmacy network, you will be able to receive coverage
Prescription Medication Schedule of Benefits Rx Member Cost-Sharing: $15/$35/$70/$70 When you go to a pharmacy that participates in the UPMC Health Plan pharmacy network, you will be able to receive coverage
UC SHIP Premium Formulary. Effective September 1, 2016
 UC SHIP Premium Formulary Effective September 1, 2016 Formulary A formulary identifies the drugs available for certain conditions and organizes them into cost levels, also known as tiers. An important
UC SHIP Premium Formulary Effective September 1, 2016 Formulary A formulary identifies the drugs available for certain conditions and organizes them into cost levels, also known as tiers. An important
2019 Transition Policy and Procedure
 2019 Transition Policy and Procedure POLICY Steward Health Choice Generations (SHCG) provides a Part D drug transition process in order to prevent enrollee medication coverage gaps. SHCG s transition process
2019 Transition Policy and Procedure POLICY Steward Health Choice Generations (SHCG) provides a Part D drug transition process in order to prevent enrollee medication coverage gaps. SHCG s transition process
Medicare Part D Transition Policy
 Medicare Part D Transition Policy Transition Policy for New and Current Enrollees of our Medicare Part D Prescription Drug Plan PURPOSE: Simply Healthcare Plans, Inc. must maintain an appropriate transition
Medicare Part D Transition Policy Transition Policy for New and Current Enrollees of our Medicare Part D Prescription Drug Plan PURPOSE: Simply Healthcare Plans, Inc. must maintain an appropriate transition
Prescription Drug Schedule of Benefits
 Prescription Drug Schedule of Benefits Rx Member Cost-Sharing: $5/$15/$35/$35 When you go to a pharmacy that participates in the UPMC Health Plan pharmacy network, you will be able to receive coverage
Prescription Drug Schedule of Benefits Rx Member Cost-Sharing: $5/$15/$35/$35 When you go to a pharmacy that participates in the UPMC Health Plan pharmacy network, you will be able to receive coverage
SelectHealth Prescriptions
 SelectHealth Prescriptions pharmacy benefit management program SM SelectHealth Prescriptions is a full-service Pharmacy Benefit Manager (PBM) that offers transparent pricing, clinically based programs,
SelectHealth Prescriptions pharmacy benefit management program SM SelectHealth Prescriptions is a full-service Pharmacy Benefit Manager (PBM) that offers transparent pricing, clinically based programs,
Pharmacy Benefit Managers Overview
 Pharmacy Benefit Managers Overview A Presentation to the House Health Innovation Subcommittee Mary Alice Nye, Ph.D. Health and Human Services Staff Director, OPPAGA December 6, 2017 Pharmacy Benefit Managers
Pharmacy Benefit Managers Overview A Presentation to the House Health Innovation Subcommittee Mary Alice Nye, Ph.D. Health and Human Services Staff Director, OPPAGA December 6, 2017 Pharmacy Benefit Managers
Prescription Medication Rider
 Prescription Medication Rider Rx Member Cost-Sharing: $16/$40/$80/$90 HealthyU HIA/HRA According to this prescription medication program, you may receive coverage for prescription medications in the amounts
Prescription Medication Rider Rx Member Cost-Sharing: $16/$40/$80/$90 HealthyU HIA/HRA According to this prescription medication program, you may receive coverage for prescription medications in the amounts
SPD Prescription Drugs Plan
 Prescription Drugs Plan 08/01/2017 3-1 Your Prescription Drug Benefits The prescription drug benefit available to you is based on the medical plan in which you are enrolled. Regardless of the benefit design
Prescription Drugs Plan 08/01/2017 3-1 Your Prescription Drug Benefits The prescription drug benefit available to you is based on the medical plan in which you are enrolled. Regardless of the benefit design
Prescription Drug Rider
 Prescription Drug Rider Rx Member Cost-Sharing: $10/$25/$40/$40 According to this prescription drug program, you may receive coverage for prescription drugs in the amounts specified in your rider when
Prescription Drug Rider Rx Member Cost-Sharing: $10/$25/$40/$40 According to this prescription drug program, you may receive coverage for prescription drugs in the amounts specified in your rider when
PURPOSE OF THE POLICY STATEMENT OF THE POLICY PROCEDURES
 PURPOSE OF THE POLICY The purpose of this policy is to describe Health Alliance s process for transitions and ensure that continued drug coverage is provided to new and current Part D members. The transition
PURPOSE OF THE POLICY The purpose of this policy is to describe Health Alliance s process for transitions and ensure that continued drug coverage is provided to new and current Part D members. The transition
Farm Bureau Essential Rx 2018 Summary of Benefits January 1, December 31, 2018
 Farm Bureau Health Plans P.O. Box 266380 Weston, FL 33326 Farm Bureau Essential Rx 2018 Summary of Benefits January 1, 2018 - December 31, 2018 Thank you for your interest in Farm Bureau Essential Rx.
Farm Bureau Health Plans P.O. Box 266380 Weston, FL 33326 Farm Bureau Essential Rx 2018 Summary of Benefits January 1, 2018 - December 31, 2018 Thank you for your interest in Farm Bureau Essential Rx.
Important Information about our prescription drug program
 under your prescription drug benefit. Our records indicate a drug prescribed for you is affected by a prior authorization change. Changes to prior authorization requirements As of , the drug(s)
under your prescription drug benefit. Our records indicate a drug prescribed for you is affected by a prior authorization change. Changes to prior authorization requirements As of , the drug(s)
Martin s Point Generations Advantage Policy and Procedure Form
 Martin s Point Generations Advantage Policy and Procedure Form Policy #: PartD.923 Effective Date: 4/16/10 Policy Title: Part D Transition Policy Section of Manual: Medicare Prescription Drug Benefit Manual
Martin s Point Generations Advantage Policy and Procedure Form Policy #: PartD.923 Effective Date: 4/16/10 Policy Title: Part D Transition Policy Section of Manual: Medicare Prescription Drug Benefit Manual
I. PURPOSE. A. The primary objectives of Molina Healthcare s Transition Policy and Procedure are:
 I. PURPOSE The purpose of the Policy and Procedure is to ensure necessary continuity of treatment and to provide adequate time and transition process to introduce the enrollee and their prescribing physician
I. PURPOSE The purpose of the Policy and Procedure is to ensure necessary continuity of treatment and to provide adequate time and transition process to introduce the enrollee and their prescribing physician
Harvard Pilgrim Health Care Pharmacy Services Policy & Criteria. Medicare Advantage Transition of Care
 SCOPE: Harvard Pilgrim Health Care Medicare Advantage enrollees, their providers, and all HPHC Pharmacy, Customer Service and Appeals & Grievances Staff. OBJECTIVE: To efficiently provide new enrollees
SCOPE: Harvard Pilgrim Health Care Medicare Advantage enrollees, their providers, and all HPHC Pharmacy, Customer Service and Appeals & Grievances Staff. OBJECTIVE: To efficiently provide new enrollees
POLICY STATEMENT: PROCEDURE:
 PAGE 1 OF 12 POLICY STATEMENT: NPS shall provide an automated process to assist beneficiaries who are transitioning from drug regimens or therapies that are not covered on the Part D Plan S are on the
PAGE 1 OF 12 POLICY STATEMENT: NPS shall provide an automated process to assist beneficiaries who are transitioning from drug regimens or therapies that are not covered on the Part D Plan S are on the
21 - Pharmacy Services
 21 - Pharmacy Services The role of Health Plan of Nevada s (HPN) Pharmacy Services is to evaluate and determine the appropriateness of quality drug therapy while maintaining and improving therapeutic outcomes.
21 - Pharmacy Services The role of Health Plan of Nevada s (HPN) Pharmacy Services is to evaluate and determine the appropriateness of quality drug therapy while maintaining and improving therapeutic outcomes.
MEDICARE PART D POLICY FORMULARY: TRANSITION PROCESS Policy Number: 6-C
 MEDICARE PART D POLICY FORMULARY: TRANSITION PROCESS Policy Number: 6-C Coverage Statement This Policy is applicable to: Medco PDP, Beneficiaries, Enhanced PDPs, Client PDPs and Client MA-PDs, to the extent
MEDICARE PART D POLICY FORMULARY: TRANSITION PROCESS Policy Number: 6-C Coverage Statement This Policy is applicable to: Medco PDP, Beneficiaries, Enhanced PDPs, Client PDPs and Client MA-PDs, to the extent
summary of benefits Blue Shield of California Medicare Rx Plan (PDP)
 summary of benefits Blue Shield of California Medicare Rx Plan (PDP) An employer-sponsored Medicare Prescription Drug Plan for City and County of San Francisco retirees, spouses and eligible dependents
summary of benefits Blue Shield of California Medicare Rx Plan (PDP) An employer-sponsored Medicare Prescription Drug Plan for City and County of San Francisco retirees, spouses and eligible dependents
Coverage Determinations, Appeals and Grievances
 Coverage Determinations, Appeals and Grievances Filing a grievance (making a complaint) about your prescription coverage Asking for a coverage determination (coverage decision) 60-day formulary change
Coverage Determinations, Appeals and Grievances Filing a grievance (making a complaint) about your prescription coverage Asking for a coverage determination (coverage decision) 60-day formulary change
Harvard Pilgrim Health Care Pharmacy Services Policy & Criteria. Medicare Advantage Transition of Care
 SCOPE: Medicare Advantage enrollees, their providers, and all HPHC Pharmacy, Customer Service and Appeals & Grievances Staff. OBJECTIVE: To avoid interruption in therapy, timely access to a temporary supply
SCOPE: Medicare Advantage enrollees, their providers, and all HPHC Pharmacy, Customer Service and Appeals & Grievances Staff. OBJECTIVE: To avoid interruption in therapy, timely access to a temporary supply
Kroll Ontrack, LLC Prescription Drug Plan. Plan Document and Summary Plan Description
 Kroll Ontrack, LLC Prescription Drug Plan Plan Document and Summary Plan Description Effective December 9, 2016 Kroll Ontrack, LLC reserves the right to amend the Kroll Ontrack, LLC Health & Welfare Plan
Kroll Ontrack, LLC Prescription Drug Plan Plan Document and Summary Plan Description Effective December 9, 2016 Kroll Ontrack, LLC reserves the right to amend the Kroll Ontrack, LLC Health & Welfare Plan
PRESCRIPTION DRUG SPENDING IN THE U.S. HEALTH CARE SYSTEM: AN ACTUARIAL PERSPECTIVE
 PRESCRIPTION DRUG SPENDING IN THE U.S. HEALTH CARE SYSTEM: AN ACTUARIAL PERSPECTIVE Moderator Audrey Halvorson, Vice Chairperson, Health Practice Council Presenters Karen Bender, Member, Prescription Drug
PRESCRIPTION DRUG SPENDING IN THE U.S. HEALTH CARE SYSTEM: AN ACTUARIAL PERSPECTIVE Moderator Audrey Halvorson, Vice Chairperson, Health Practice Council Presenters Karen Bender, Member, Prescription Drug
The Real Deal About Real-Time Benefits. Proven Savings with Up-to-the-Minute, Member-Specific Information Across Multiple Points of Care
 The Real Deal About Real-Time Benefits Proven Savings with Up-to-the-Minute, Member-Specific Information Across Multiple Points of Care Cost is a key issue for plan members and a common barrier to medication
The Real Deal About Real-Time Benefits Proven Savings with Up-to-the-Minute, Member-Specific Information Across Multiple Points of Care Cost is a key issue for plan members and a common barrier to medication
Putting the Pieces Together, a Review of the Benefits Investigation Process. Thomas Cohn, Asembia
 Putting the Pieces Together, a Review of the Benefits Investigation Process Thomas Cohn, Asembia Introductions Thomas Cohn Chief Strategy Officer Asembia Tony Scheuth CEO and Managing Partner Point-of-Care
Putting the Pieces Together, a Review of the Benefits Investigation Process Thomas Cohn, Asembia Introductions Thomas Cohn Chief Strategy Officer Asembia Tony Scheuth CEO and Managing Partner Point-of-Care
AETNA LIFE INSURANCE COMPANY
 1 AETNA LIFE INSURANCE COMPANY Former Employer/Union/Trust Name: Kansas State Employee Health Plan Group Agreement Effective Date: January 1, 2018 Group Number: AE466595, AE466596, AE466597, AE466598 This
1 AETNA LIFE INSURANCE COMPANY Former Employer/Union/Trust Name: Kansas State Employee Health Plan Group Agreement Effective Date: January 1, 2018 Group Number: AE466595, AE466596, AE466597, AE466598 This
Manage your Prescriptions Online Through the Express Scripts Pharmacy
 Manage your Prescriptions Online Through the Express Scripts Pharmacy www.express-scripts.com Customer service specialists are also available 24 hours a day/7 days a week at 1-800-711-0917. Get a 90-day
Manage your Prescriptions Online Through the Express Scripts Pharmacy www.express-scripts.com Customer service specialists are also available 24 hours a day/7 days a week at 1-800-711-0917. Get a 90-day
2018 Retiree Medical Premiums and Coverage Summary MAP Plus - Option 1 Low Deductible
 MAP Plus - Option 1 Low Deductible You and your SP of Record/DP of Record both are Pre-Medicare Eligible Retiree + + $462.00 $923.00 $923.00 $1,385.00 You are Medicare Eligible and your SP of Record/ DP
MAP Plus - Option 1 Low Deductible You and your SP of Record/DP of Record both are Pre-Medicare Eligible Retiree + + $462.00 $923.00 $923.00 $1,385.00 You are Medicare Eligible and your SP of Record/ DP
Blue Essentials, Blue Advantage HMO SM and Blue Premier SM Provider Manual - Pharmacy
 Blue Essentials, Blue Advantage HMO SM and Blue Premier SM Provider Manual - In this Section there are references unique to Blue Essentials, Blue Advantage HMO and Blue Premier. These network specific
Blue Essentials, Blue Advantage HMO SM and Blue Premier SM Provider Manual - In this Section there are references unique to Blue Essentials, Blue Advantage HMO and Blue Premier. These network specific
Contract Summary. OptumRx Administrative Services, LLC
 Contract Summary OptumRx Administrative Services, LLC Subcontractors This contract includes the following subcontractors or pass through to other providers. Name Service(s) Amount Interpreting Services
Contract Summary OptumRx Administrative Services, LLC Subcontractors This contract includes the following subcontractors or pass through to other providers. Name Service(s) Amount Interpreting Services
Summary of Benefits. Regence Medicare Script TM. Enhanced (PDP) Basic (PDP) Medicare Prescription Drug Plan for Utah
 2013 Summary of Benefits Medicare Prescription Drug Plan for Utah Regence Medicare Script TM Enhanced (PDP) Regence Medicare Script TM Basic (PDP) Regence BlueCross BlueShield of Utah is an Independent
2013 Summary of Benefits Medicare Prescription Drug Plan for Utah Regence Medicare Script TM Enhanced (PDP) Regence Medicare Script TM Basic (PDP) Regence BlueCross BlueShield of Utah is an Independent
Survey Analysis of January 2014 CMS Medicare Part D Proposed Rule
 Survey Analysis of January 2014 CMS Medicare Part D Proposed Rule Prepared for: Pharmaceutical Care Management Association Prepared by: Stephen J. Kaczmarek, FSA, MAAA Principal and Consulting Actuary
Survey Analysis of January 2014 CMS Medicare Part D Proposed Rule Prepared for: Pharmaceutical Care Management Association Prepared by: Stephen J. Kaczmarek, FSA, MAAA Principal and Consulting Actuary
TRANSITION POLICY. Members Health Insurance Company
 Members Health Insurance Company TRANSITION POLICY POLICY The Company will maintain an appropriate transition process, consistent with 42 CFR 423.120(b)(3), Chapter 6 of the Medicare Prescription Drug
Members Health Insurance Company TRANSITION POLICY POLICY The Company will maintain an appropriate transition process, consistent with 42 CFR 423.120(b)(3), Chapter 6 of the Medicare Prescription Drug
BMR Prescription Drug Plan
 United Workers Health Fund BMR Prescription Drug Plan Welcome Kit Dear United Workers Health Fund Member: Welcome to Broadreach Medical Resources, Inc. (BMR), the program administrator for the United Workers
United Workers Health Fund BMR Prescription Drug Plan Welcome Kit Dear United Workers Health Fund Member: Welcome to Broadreach Medical Resources, Inc. (BMR), the program administrator for the United Workers
PLAN F MEDICARE (PART A) HOSPITAL SERVICES PER BENEFIT PERIOD
 PLAN F MEDICARE (PART A) HOSPITAL SERVICES PER BENEFIT PERIOD - 2018 * A benefit period begins on the first day you receive service as an inpatient in a hospital and ends after you have been out of the
PLAN F MEDICARE (PART A) HOSPITAL SERVICES PER BENEFIT PERIOD - 2018 * A benefit period begins on the first day you receive service as an inpatient in a hospital and ends after you have been out of the
Share a Clear View. El Paso Children's Hospital. Printed on:
 Share a Clear View El Paso Children's Hospital Printed on: Share a Clear View NAVITUS CUSTOMER CARE HOURS: 24 Hours a Day 7 Days a Week 855-673-6504 (toll-free) TTY (toll-free) 711 MAILING ADDRESS: Navitus
Share a Clear View El Paso Children's Hospital Printed on: Share a Clear View NAVITUS CUSTOMER CARE HOURS: 24 Hours a Day 7 Days a Week 855-673-6504 (toll-free) TTY (toll-free) 711 MAILING ADDRESS: Navitus
PLAN F or HIGH DEDUCTIBLE PLAN F MEDICARE (PART A) HOSPITAL SERVICES PER BENEFIT PERIOD
 SERVICES DS-GRMSP10(46) Page 1 MEDICARE PAYS AFTER YOU PAY $2240 PLAN PAYS HOSPITALIZATION * Semiprivate room and board, general nursing and miscellaneous services and supplies First 60 days All but $1340
SERVICES DS-GRMSP10(46) Page 1 MEDICARE PAYS AFTER YOU PAY $2240 PLAN PAYS HOSPITALIZATION * Semiprivate room and board, general nursing and miscellaneous services and supplies First 60 days All but $1340
Pharmacy Benefits Guide
 Commercial Individual & Family Plans and Small Business Group Essential Pharmacy Benefits Guide Making the most of your pharmacy benefits Lisa Pasillas-Le, Health Net We re part of your health team. Understanding
Commercial Individual & Family Plans and Small Business Group Essential Pharmacy Benefits Guide Making the most of your pharmacy benefits Lisa Pasillas-Le, Health Net We re part of your health team. Understanding
Medical Benefits Trust
 UAW RETIREE Medical Benefits Trust Dear UAW Trust Member, HEALTH CARE BENEFIT HIGHLIGHTS 2018 At the UAW Retiree Medical Benefits Trust (the Trust ), we recognize how important health care benefits are
UAW RETIREE Medical Benefits Trust Dear UAW Trust Member, HEALTH CARE BENEFIT HIGHLIGHTS 2018 At the UAW Retiree Medical Benefits Trust (the Trust ), we recognize how important health care benefits are
Rose Tree Media School District
 Rose Tree Media School District Health Reimbursement Arrangement (HRA), Prescription Drug Plan & Flexible Spending Account (FSA) Benefits Presented by Gallagher Benefit Services Public Entity Team 2017
Rose Tree Media School District Health Reimbursement Arrangement (HRA), Prescription Drug Plan & Flexible Spending Account (FSA) Benefits Presented by Gallagher Benefit Services Public Entity Team 2017
PHARMACY BENEFIT MEMBER BOOKLET
 PHARMACY BENEFIT MEMBER BOOKLET Printed on: VALUE, QUALITY AND CONFIDENCE Costco Health Solutions Customer Care HOURS: 24 Hours a Day 7 Days a Week (877) 908-6024 (toll-free) TTY 711 MAILING ADDRESS: Costco
PHARMACY BENEFIT MEMBER BOOKLET Printed on: VALUE, QUALITY AND CONFIDENCE Costco Health Solutions Customer Care HOURS: 24 Hours a Day 7 Days a Week (877) 908-6024 (toll-free) TTY 711 MAILING ADDRESS: Costco
PHARMACY COVERAGE GUIDELINES ORIGINAL EFFECTIVE DATE: 1/18/18 SECTION: DRUGS LAST REVIEW DATE: 8/13/18 LAST CRITERIA REVISION DATE: ARCHIVE DATE:
 STEP THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage Guideline must
STEP THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage Guideline must
Jill Rosenthal, MD, MA, MPH, FACOEM SVP, Chief Medical Officer Zenith Insurance Company
 Jill Rosenthal, MD, MA, MPH, FACOEM SVP, Chief Medical Officer Zenith Insurance Company The prescription drug (Rx) share of total workers compensation (WC) medical costs for Accident Year 2014 = 17% Rx
Jill Rosenthal, MD, MA, MPH, FACOEM SVP, Chief Medical Officer Zenith Insurance Company The prescription drug (Rx) share of total workers compensation (WC) medical costs for Accident Year 2014 = 17% Rx
Prescription Drug Coverage
 The Company s medical plans automatically include coverage for prescription drugs which is administered by Envision Pharmaceutical Services, Inc. (Envision Rx) for prescriptions filled at retail pharmacies
The Company s medical plans automatically include coverage for prescription drugs which is administered by Envision Pharmaceutical Services, Inc. (Envision Rx) for prescriptions filled at retail pharmacies
State Health Plan 101
 State Health Plan 101 2017 Pharmacy Benefit Changes November 2016 Agenda New Pharmacy Benefit Manager Pharmacy Benefits Overview and Changes Q&A session 2 New Pharmacy Benefit Manager As of Jan. 1, 2017,
State Health Plan 101 2017 Pharmacy Benefit Changes November 2016 Agenda New Pharmacy Benefit Manager Pharmacy Benefits Overview and Changes Q&A session 2 New Pharmacy Benefit Manager As of Jan. 1, 2017,
Navitus Prior Authorization and Exception to Coverage. October 2016
 Navitus Prior Authorization and Exception to Coverage October 2016 PRIOR AUTHORIZATIONS DEFINITION AND PURPOSE Prior Authorizations (PA) are predetermined criteria a member must meet for a request to be
Navitus Prior Authorization and Exception to Coverage October 2016 PRIOR AUTHORIZATIONS DEFINITION AND PURPOSE Prior Authorizations (PA) are predetermined criteria a member must meet for a request to be
Summary of Benefits for Blue MedicareRx Standard SM (PDP), Blue MedicareRx Plus SM (PDP) and Blue MedicareRx Premier SM (PDP)
 Summary of Benefits for Standard SM (PDP), Plus SM (PDP) and Premier SM (PDP) Available in Colorado A -approved Part D sponsor. Anthem Insurance Companies, Inc. (AICI) has contracted with the Centers for
Summary of Benefits for Standard SM (PDP), Plus SM (PDP) and Premier SM (PDP) Available in Colorado A -approved Part D sponsor. Anthem Insurance Companies, Inc. (AICI) has contracted with the Centers for
Get the most from your
 Get the most from your FOREIGN SERVICE BENEFIT PLAN (FSBP) Welcome to Express Scripts What s Inside Your benefit at a glance...2 FSBP s preferred medicines...2 Coverage limits...3 Home delivery overseas...5
Get the most from your FOREIGN SERVICE BENEFIT PLAN (FSBP) Welcome to Express Scripts What s Inside Your benefit at a glance...2 FSBP s preferred medicines...2 Coverage limits...3 Home delivery overseas...5
Clinical Policy: Request for Medically Necessary Drug Not on the PDL Reference Number: CP.PMN.16 Effective Date: Last Review Date: 11.
 Clinical Policy: Reference Number: CP.PMN.16 Effective Date: 09.01.06 Last Review Date: 11.18 Line of Business: Medicaid See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: Reference Number: CP.PMN.16 Effective Date: 09.01.06 Last Review Date: 11.18 Line of Business: Medicaid See Important Reminder at the end of this policy for important regulatory and legal
YOUR TRUST PLAN BENEFITS
 YOUR TRUST PLAN BENEFITS Benefit Overview Express Scripts Medicare (PDP) for the Insurance Trust for Delta Retirees (ITDR) YOUR 2017 PRESCRIPTION DRUG PLAN BENEFIT Here is a summary of what you will pay
YOUR TRUST PLAN BENEFITS Benefit Overview Express Scripts Medicare (PDP) for the Insurance Trust for Delta Retirees (ITDR) YOUR 2017 PRESCRIPTION DRUG PLAN BENEFIT Here is a summary of what you will pay
Contract Summary. OptumRx Administrative Services, LLC
 Attachment C Contract Summary OptumRx Administrative Services, LLC Subcontractors This contract includes the following subcontractors or pass through to other providers. Name Service(s) Amount Interpreting
Attachment C Contract Summary OptumRx Administrative Services, LLC Subcontractors This contract includes the following subcontractors or pass through to other providers. Name Service(s) Amount Interpreting
For Large Groups Health Benefit Plan 03359
 Summary of Benefits for Covered Services Office Services Physician Office Services Family Physician Specialist Office Visit e-office Visit e-office Visit Advanced Imaging Services (AIS) (MRI, MRA, PET,
Summary of Benefits for Covered Services Office Services Physician Office Services Family Physician Specialist Office Visit e-office Visit e-office Visit Advanced Imaging Services (AIS) (MRI, MRA, PET,
YOUR TRUST PLAN BENEFITS
 YOUR TRUST PLAN BENEFITS Benefit Overview Express Scripts Medicare (PDP) for the Insurance Trust for Delta Retirees (ITDR) YOUR 2018 PRESCRIPTION DRUG PLAN BENEFIT Here is a summary of what you will pay
YOUR TRUST PLAN BENEFITS Benefit Overview Express Scripts Medicare (PDP) for the Insurance Trust for Delta Retirees (ITDR) YOUR 2018 PRESCRIPTION DRUG PLAN BENEFIT Here is a summary of what you will pay
For Large Groups Lower Premium Health Benefit Plan 03900
 Summary of Benefits for Services In-Network Out-of-Network Financial Features (DED 1 ) (PBP 2 ) $2,000 $4,500 (DED is the amount the member is responsible for before Florida Blue pays) Coinsurance (Coinsurance
Summary of Benefits for Services In-Network Out-of-Network Financial Features (DED 1 ) (PBP 2 ) $2,000 $4,500 (DED is the amount the member is responsible for before Florida Blue pays) Coinsurance (Coinsurance
Pharmaceutical Management Community Plans 2018
 Pharmaceutical Management Community Plans 2018 Customer Service: (888) 327-0671 TTY: 711 Pharmacy Administration: (810) 244-1660 Introduction Pharmaceutical management promotes the use of the most clinically
Pharmaceutical Management Community Plans 2018 Customer Service: (888) 327-0671 TTY: 711 Pharmacy Administration: (810) 244-1660 Introduction Pharmaceutical management promotes the use of the most clinically
CWAG Prescription Drug Pricing Webinar
 CWAG Prescription Drug Pricing Webinar January 9, 2018 Kipp Snider, J.D. Vice President, State Policy Pharmaceutical Research & Manufacturers of America (PhRMA) Medicines Are Expected to Account for a
CWAG Prescription Drug Pricing Webinar January 9, 2018 Kipp Snider, J.D. Vice President, State Policy Pharmaceutical Research & Manufacturers of America (PhRMA) Medicines Are Expected to Account for a
Get the most from your prescription benefit
 Get the most from your prescription benefit TE Connectivity HealthFund HRA Plan Welcome to Express Scripts What s Inside Your benefit at a glance...2 Your plan s preferred medicines...2 Prior authorization...2
Get the most from your prescription benefit TE Connectivity HealthFund HRA Plan Welcome to Express Scripts What s Inside Your benefit at a glance...2 Your plan s preferred medicines...2 Prior authorization...2
YOUR GUIDE TO PRESCRIPTION DRUG BENEFITS
 YOUR GUIDE TO PRESCRIPTION DRUG BENEFITS PHARMACY BENEFITS CAN BE CONFUSING, AND YOU PROBABLY HAVE LOTS OF QUESTIONS ABOUT USING YOUR DRUG PLAN. We re here to help. Because taking the right medicines when
YOUR GUIDE TO PRESCRIPTION DRUG BENEFITS PHARMACY BENEFITS CAN BE CONFUSING, AND YOU PROBABLY HAVE LOTS OF QUESTIONS ABOUT USING YOUR DRUG PLAN. We re here to help. Because taking the right medicines when
SPECIALTY PHARMACY ACCREDITATION V3.0 MANDATORY MEASURES
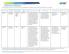 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual basis. # DESCRIPTION NUMERATOR DENOMINATOR DATA SOURCE DM2012-13 Drug-Drug
MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual basis. # DESCRIPTION NUMERATOR DENOMINATOR DATA SOURCE DM2012-13 Drug-Drug
CIS Responses to Vendor Questions PBM RFP September 23, 2015 Addendum #1
 CIS Responses to Vendor Questions PBM RFP September 23, 2015 Addendum #1 A. BACKGROUND On September 4, 2015, CIS issued a Request for Proposals (RFP) for pharmacy benefit management services. CIS is issuing
CIS Responses to Vendor Questions PBM RFP September 23, 2015 Addendum #1 A. BACKGROUND On September 4, 2015, CIS issued a Request for Proposals (RFP) for pharmacy benefit management services. CIS is issuing
Y0076_ALL Trans Pol
 Policy Title: Medicare Part D Transition Policy Policy Number: PCM-2018 TB Policy Owner: Antonio Petitta, Vice President Pharmacy Care Management Department(s): Pharmacy Care Management Effective Date:
Policy Title: Medicare Part D Transition Policy Policy Number: PCM-2018 TB Policy Owner: Antonio Petitta, Vice President Pharmacy Care Management Department(s): Pharmacy Care Management Effective Date:
Contents General Information General Information
 Contents General Information... 1 Preferred Drug List... 2 Pharmacies... 3 Prescriptions... 4 Generic and Preferred Drugs... 5 Express Scripts Website and Mobile App... 5 Specialty Medicines... 5 Prior
Contents General Information... 1 Preferred Drug List... 2 Pharmacies... 3 Prescriptions... 4 Generic and Preferred Drugs... 5 Express Scripts Website and Mobile App... 5 Specialty Medicines... 5 Prior
KEEPING PRESCRIPTION DRUGS AFFORDABLE: The Value of Pharmacy Benefit Managers (PBMs)
 The Texas Association of Health Plans Representing health insurers, health maintenance organizations, and other related health care entities operating in Texas. KEEPING PRESCRIPTION DRUGS AFFORDABLE: The
The Texas Association of Health Plans Representing health insurers, health maintenance organizations, and other related health care entities operating in Texas. KEEPING PRESCRIPTION DRUGS AFFORDABLE: The
Excellus BlueCross BlueShield Participating Provider Manual. 5.0 Pharmacy Management
 Excellus BlueCross BlueShield Participating Provider Manual 5.0 Pharmacy Management 5.1 Pharmacy Benefits The Health Plan is committed to effectively managing prescription drug benefit costs and providing
Excellus BlueCross BlueShield Participating Provider Manual 5.0 Pharmacy Management 5.1 Pharmacy Benefits The Health Plan is committed to effectively managing prescription drug benefit costs and providing
(PDP) 2014 Summary of benefits for our Medicare prescription drug plans (Enhanced and Standard)
 (PDP) 2014 Summary of benefits for our prescription drug plans (Enhanced and Standard) Contract S5540, Plans 004 and 002 January 1, 2014 December 31, 2014 U5073c, 8/13 Y0079_6249 CMS Accepted 09112013
(PDP) 2014 Summary of benefits for our prescription drug plans (Enhanced and Standard) Contract S5540, Plans 004 and 002 January 1, 2014 December 31, 2014 U5073c, 8/13 Y0079_6249 CMS Accepted 09112013
As announced in the Winter 2013 edition of
 The Newsletter of the Screen Actors Guild Producers Pension and Health Plans Volume XXII, Number 2 Summer 2014 INSIDE TAKE 2 Anesthesia During Colonoscopy... 3 Therapy Bene t Limits and Allowances... 4
The Newsletter of the Screen Actors Guild Producers Pension and Health Plans Volume XXII, Number 2 Summer 2014 INSIDE TAKE 2 Anesthesia During Colonoscopy... 3 Therapy Bene t Limits and Allowances... 4
Chapter 10 Prescriptions Benefits and Drug Formulary
 10 Prescription Benefits and Drug Formulary Health Choice Generations is a Medicare Advantage Special Needs Plan (SNP) with Medicare Part D Prescription Drug Coverage. Medicare Part D drugs covered by
10 Prescription Benefits and Drug Formulary Health Choice Generations is a Medicare Advantage Special Needs Plan (SNP) with Medicare Part D Prescription Drug Coverage. Medicare Part D drugs covered by
PHARMACY GENERAL INFORMATION
 Pharmacy Program Cenpatico Integrated Care (Cenpatico IC) is committed to providing appropriate high quality and cost-effective medication therapy to all Cenpatico IC members. Cenpatico IC works with providers
Pharmacy Program Cenpatico Integrated Care (Cenpatico IC) is committed to providing appropriate high quality and cost-effective medication therapy to all Cenpatico IC members. Cenpatico IC works with providers
Summary of Benefits. Aetna Medicare Rx Costco Plus Plan (PDP) S5810. California. January 1, 2010 to December 31, 2010
 January 1, 2010 to December 31, 2010 Summary of Benefits Aetna Medicare Rx S5810 California S5810_D_PE_SB_90712 (08/2009) Visit us www.aetnamedicare.com 1 Summary of Benefits: Aetna Medicare Rx Section
January 1, 2010 to December 31, 2010 Summary of Benefits Aetna Medicare Rx S5810 California S5810_D_PE_SB_90712 (08/2009) Visit us www.aetnamedicare.com 1 Summary of Benefits: Aetna Medicare Rx Section
PLAN F MEDICARE (PART A) HOSPITAL SERVICES PER BENEFIT PERIOD 2019
 PLAN F MEDICARE (PART A) HOSPITAL SERVICES PER BENEFIT PERIOD 2019 * A benefit period begins on the first day you receive service as an inpatient in a hospital and ends after you have been out of the hospital
PLAN F MEDICARE (PART A) HOSPITAL SERVICES PER BENEFIT PERIOD 2019 * A benefit period begins on the first day you receive service as an inpatient in a hospital and ends after you have been out of the hospital
Subject: Pharmacy Services & Formulary Management (Page 1 of 5)
 Subject: Pharmacy Services & Formulary Management (Page 1 of 5) Objective: I. To ensure the clinically appropriate prescription and use of pharmaceuticals by Tuality Health Alliance (THA) providers and
Subject: Pharmacy Services & Formulary Management (Page 1 of 5) Objective: I. To ensure the clinically appropriate prescription and use of pharmaceuticals by Tuality Health Alliance (THA) providers and
Q Formulary Performance:
 Insights Executive Briefing Issue 10, 2016 Q1 2016 Performance: Key Data to Consider as You Look Ahead to 2017 Increasingly our clients see proactive, dynamic formulary management as a necessary response
Insights Executive Briefing Issue 10, 2016 Q1 2016 Performance: Key Data to Consider as You Look Ahead to 2017 Increasingly our clients see proactive, dynamic formulary management as a necessary response
Understanding Pharmacy Benefit Management Services
 Understanding Pharmacy Benefit Management Services Peter Cullen VP, Business Development and Strategic Initiatives March 12, 2014 Innovation Session Overview and Learning Objectives Session Overview: Provide
Understanding Pharmacy Benefit Management Services Peter Cullen VP, Business Development and Strategic Initiatives March 12, 2014 Innovation Session Overview and Learning Objectives Session Overview: Provide
