CHILDREN'S SPECIAL HEALTH CARE SERVICES
|
|
|
- Anthony Beasley
- 5 years ago
- Views:
Transcription
1 CHILDREN'S SPECIAL HEALTH CARE SERVICES Indiana State Department of Health 2 North Meridian Street Section 7-B Indianapolis, IN (800) (In-State only) (317) Fax (317) August 2003
2 Table of Contents MISSION STATEMENT... 1 GENERAL INFORMATION... 1 SERVICES... 2 SERVICE LIMITS... 2 EXCLUSIONS... 3 PROVIDERS... 3 PRIOR AUTHORIZATION (PA)... 4 PAYER OF LAST RESORT... 5 MEDICAID... 6 APPEALS... 6 DEDUCTIBLES, CO-PAYMENTS & MEDICAID SPEND-DOWN... 7 PAYMENT...7 RE-EVALUATIONS... 7 CASE CLOSURE... 8
3 MISSION STATEMENT The Children s Special Health Care Services (CSHCS) program provides financial assistance for needed medical treatment to children with serious and chronic medical conditions to reduce complications and promote maximum quality of life. GENERAL INFORMATION Welcome to the CSHCS Program! This manual defines services and responsibilities for participants (newborn to 21 years of age or individuals with Cystic Fibrosis for lifetime), their families (parents, legal guardians, foster care providers), and medical providers (physicians, dentists, therapists, pharmacies, hospitals, clinics, suppliers). The CSHCS Program financially assists families for the medical care of chronically ill children with special needs. Participants approved for the program must meet financial and medical guidelines. The program pays for all appropriate authorized care relating to an eligible diagnosis. CSHCS pays only after all other sources of payment are exhausted. CSHCS is not a Medicaid program. CSHCS is a separate program (formerly known as the Indiana Crippled Children s Program) administered by the Indiana State Department of Health (ISDH). CSHCS pays medical providers at the maximum allowable Medicaid rate and uses Medicaid coding and claim forms. The CSHCS office provides Care Coordination, Eligibility, Prior Authorization (PA), Claims Processing, Provider Relations, and Travel Reimbursement support services for providers and participants or their families at (800) (In-State only) or (317) Participants and providers must report changes such as address, telephone numbers, or corporate or individual names to CSHCS to ensure coverage and timely claims payment. 1
4 SERVICES The CSHCS program links all participants to a primary, specialty, and dental provider: Each participant must have a Primary Care Provider (PCP). The PCP is a doctor or clinic providing routine care such as a physical examination, immunizations, or sick child visit in an office setting. Each participant may have a Specialty Care Provider (SCP). The SCP provider is a doctor or clinic providing specialty care for the participant s eligible medical diagnosis. The PCP and SCP may be the same provider. Each participant may have a Dental Care Provider (DCP). The DCP is a dentist or clinic providing routine dental care to keep the participant s teeth and gums healthy. The CSHCS Program provides specialty dental care to treat a participant s eligible medical diagnosis such as cleft lip and palate. CSHCS pays for lab work, x-rays, and prescription medicines. These services need not relate to the participant s eligible diagnosis or require prior authorization, but the participant s PCP, SCP, DCP, or specialty dental provider must prescribe these services. CSHCS may pay for some over-the-counter (OTC) vitamins, formula, and supplies with PA that treat an eligible diagnosis. CSHCS pays for some travel to and from providers under State Travel and CSHCS rules. SERVICE LIMITS These are some examples of service limits. The PA Unit assists with unusual circumstances: Most equipment is limited to one item. "Back-up" equipment is not covered. 2
5 Some replacement equipment is limited to once within five years. Specialty care must relate to the participant s eligible medical diagnosis. EXCLUSIONS CSHCS does not cover all services such as these: Over-the-counter (OTC) drugs such as Tylenol and cough syrup, even with a prescription. OTC supplies such as diapers, non-sterile gloves, alcohol, tape, bleach, Band- Aids. Mental health services, counseling, testing, therapy, except with PA, substance abuse treatment. Prenatal care or other pregnancy-related care. Emergency room visits not related to the participant's eligible diagnosis such as an emergency room visit for a broken arm and a CSHCS qualifying diagnosis of asthma. Hospitalization not related to the eligible diagnosis. Organ transplants. Eyeglasses, if not related to the eligible diagnosis. Earplugs. Egg crate mattress covers. Communication boards or devices. PROVIDERS Participants must be sure their providers are CSHCS providers before making appointments. CSHCS cannot assist participants with bills from providers not enrolled in CSHCS, and participants are responsible for those bills. CSHCS will assist both families and providers with enrolling in the program. Providers must have a signed provider 3
6 agreement with CSHCS for legal purposes and under the terms of the Health Insurance Portability and Accountability Act of 1996 (HIPAA). PRIOR AUTHORIZATION (PA) A CSHCS PA confirms medical necessity and its relationship to a CSHCS eligible diagnosis. A CSHCS PA does not guarantee payment by CSHCS. All CSHCS services must have CSHCS PA. Accepting or providing services before securing PA causes claim denial except in an emergency. These are examples of services requiring PA: Initial authorization for primary, specialty, routine and specialty dental care. Further authorization is not necessary for in-office services. In-patient services (hospitalizations). Equipment and supplies. Surgery. Specialty dental services. Therapy. Home health care. Referral to other physicians or providers. Emergency Room Services. Providers must secure CSHCS PA for participants or their families enrolled in CSHCS. CSHCS cannot pay for services denied by private insurance because the provider did not obtain PA or prior certification (PC). CSHCS cannot pay for services denied by Hoosier Healtwise, or Medicaid because the provider did not obtain PA. Providers may not bill participants or their families if the provider did not secure PA or PC. CSHCS may consider a PA for unusual circumstances of service out-side of insurance, HMO, PPO, Hoosier Healthwise or Medicaid provider groups or procedure. Strong and 4
7 compelling documentation of proper appeal, medical necessity, continuity of service, economy, and financial consequence to providers, families, and the program must support exceptions. Participants must notify the CSHCS program of emergency care or emergency hospitalizations within five working days of the visit. CSHCS PA requires a mailed or faxed discharge summary or medical notes from the emergency room visit. The provider is responsible for obtaining and sending these documents to CSHCS. CSHCS authorizes only services related to an eligible medical condition. PAYER OF LAST RESORT The CSHCS program is the payer of last resort. CSHCS considers claims after insurance, HMO, PPO, or Medicaid payments. The provider must accept insurance payments made at or above the Medicaid rate as payment in full for an eligible CSHCS service. Providers may not bill participants or their families for an unpaid balance after CSHCS adjudication. Families and providers must use all available private insurance (HMO, PPO, BC/BS, Travelers, etc.) or public resources (Hoosier Healthwise or Medicaid) before billing CSHCS. Participants or their families must report all changes or loss of private or public coverage to CSHCS and providers as soon as possible. A participant s failure to report changes to CSHCS and providers can make the participant responsible for the cost of service. Participants or their families must follow the procedures of their insurance company, HMO, PPO, Hoosier Healthwise or Medicaid such as securing PA or PC, visiting only network providers, or outside referrals. Insurance company service representatives and HMO, PPO, Hoosier Healthwise and Medicaid caseworkers can assist providers and participants or their families in following procedure. CSHCS encourages participants or their families to contact and verify CSHCS PA for services with CSHCS and their providers. Providers are responsible for securing CSHCS, Hoosier Healthwise and Medicaid PA as the entity receiving payment 5
8 for services. CSHCS does not pay participants or their families directly except for travel reimbursement. MEDICAID Medicaid pays before CSHCS. Participants must apply for Medicaid when applying for CSHCS and enroll in Medicaid if eligible to qualify for CSHCS. Participants or their families must report Medicaid enrollment to medical providers and CSHCS including identification number, effective date, and any changes to providers and CSHCS. Participants or their families enrolled in Hoosier Healthwise or Medicaid must see Medicaid providers and follow Hoosier Healthwise or Medicaid guidelines. Providers may contact the CSHCS PA Unit for consideration of coverage if Medicaid denies a PA request. CSHCS will consider paying claims denied by Medicaid on a case-by-case basis. APPEALS CSHCS may ask a participant to appeal a denial by an insurance company, HMO, PPO, or Medicaid of services the participant, provider, or CSHCS consider necessary and allowed. Providers must cooperate with a participant s request for necessary information. CSHCS will not consider authorizing and paying for services until the appeal process is complete and documentation received by CSHCS. 6
9 DEDUCTIBLES, CO-PAYMENTS & MEDICAID SPEND-DOWN CSHCS may cover the insurance deductibles, co-payments, and Medicaid "spenddown." CSHCS will pay co-payments up to $25. CSHCS pays charges applied to the participant s insurance deductible at Medicaid rates. CSHCS deducts amounts paid by the insurance company from the Medicaid rate. This may result in no CSHCS payment if insurance pays more than the Medicaid rate. If this occurs, the provider may not bill the participant for the unpaid balance or deductible. PAYMENT CSHCS pays at Indiana Medicaid rates. Providers must submit claims within one year of service. If primary insurance pays more than the Medicaid rate, the provider must accept this as payment in full. Under the terms of the provider agreement, the provider may not bill the participant for the difference between the billed amount and the Medicaid rate. ISDH mails checks to providers with an Explanation of Payment (EOP). The EOP details information such as payments exceeding the Medicaid rate or reasons for denial. RE-EVALUATIONS CSHCS re-evaluates participants once a year by mail to maintain active status. During re-evaluation, participants must update income status, insurance information, household members, and other changes. Participants should provide changes as they occur to speed the annual process. 7
10 CASE CLOSURE Case closures occur for various reasons: Failure to complete and return the annual re-evaluation form within the allotted time. Failure to provide updated income information. The participant reaches the age of 21 years. Failure to use health insurance. 8
Glossary of Terms. Adjudication: The way a health plan decides how much it will pay for certain expenses.
 Page 1 Glossary of Terms Adjudication: The way a health plan decides how much it will pay for certain expenses. Affordable Care Act (ACA): The comprehensive health care reform law enacted in March 2010.
Page 1 Glossary of Terms Adjudication: The way a health plan decides how much it will pay for certain expenses. Affordable Care Act (ACA): The comprehensive health care reform law enacted in March 2010.
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Lee County Board of County Commissioners. Aetna Choice POS II
 BENEFIT PLAN Prepared Exclusively for Lee County Board of County Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Table of Contents Schedule of Benefits... Issued with
BENEFIT PLAN Prepared Exclusively for Lee County Board of County Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Table of Contents Schedule of Benefits... Issued with
Additional Information Provided by Aetna Life Insurance Company
 Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
Healthy Indiana Plan (HIP) Provider Orientation
 Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
Serving Hoosier Healthwise, Healthy Indiana Plan Healthy Indiana Plan (HIP) Provider Orientation Agenda Program overview Benefit coverage Eligibility HIP offerings Medically frail and various member categories
RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER COVERKIDS TABLE OF CONTENTS
 RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER 1200-13-21 COVERKIDS TABLE OF CONTENTS 1200-13-21-.01 Scope and Authority 1200-13-21-.02 Definitions 1200-13-21-.03
RULES OF TENNESSEE DEPARTMENT OF FINANCE AND ADMINISTRATION DIVISION OF TENNCARE CHAPTER 1200-13-21 COVERKIDS TABLE OF CONTENTS 1200-13-21-.01 Scope and Authority 1200-13-21-.02 Definitions 1200-13-21-.03
CARECOUNSEL TIPS SELECTING A HEALTH PLAN. Step 1: Gather Basic Information. Step 2: Assess Your Needs
 SELECTING A HEALTH PLAN Choosing between health plans is no longer a simple matter. As a healthcare consumer, it s important that you educate yourself about the various health plans available to you. You
SELECTING A HEALTH PLAN Choosing between health plans is no longer a simple matter. As a healthcare consumer, it s important that you educate yourself about the various health plans available to you. You
Important Questions Answers Why this Matters: Is there an overall annual limit on what the plan pays?
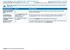 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy from the Open Enrollment Self Service site. Important Questions Answers Why this
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy from the Open Enrollment Self Service site. Important Questions Answers Why this
CA HMO Deductible $1,500 70%
 Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
This is an ERISA plan, and you have certain rights under this plan. Please contact your Employer for additional information.
 Schedule of Benefits Employer: Adobe Systems Incorporated MSA: 660819 Issue Date: January 1, 2018 Effective Date: January 1, 2018 Schedule: 2B Booklet Base: 2 For: Aetna Choice POS II HDHP - HealthSave
Schedule of Benefits Employer: Adobe Systems Incorporated MSA: 660819 Issue Date: January 1, 2018 Effective Date: January 1, 2018 Schedule: 2B Booklet Base: 2 For: Aetna Choice POS II HDHP - HealthSave
Optimum Health Designs
 Designed for Individuals, Families & Employers (PCP or Specialist) Preventive Care Tests Diagnostic, Xray & Laboratory Emergency Room Surgery (Inpatient & Outpatient) Anesthesia Supplemental Accident for
Designed for Individuals, Families & Employers (PCP or Specialist) Preventive Care Tests Diagnostic, Xray & Laboratory Emergency Room Surgery (Inpatient & Outpatient) Anesthesia Supplemental Accident for
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Gwinnett County Board Of Commissioners
 BENEFIT PLAN Prepared Exclusively for Gwinnett County Board Of Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POSII and HSA Table of Contents Schedule of Benefits (SOB) Issued
BENEFIT PLAN Prepared Exclusively for Gwinnett County Board Of Commissioners What Your Plan Covers and How Benefits are Paid Aetna Choice POSII and HSA Table of Contents Schedule of Benefits (SOB) Issued
For: Choice POS II High Deductible Health Plan - Faculty, Managerial & Professional Employees
 Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 28, 2017 Effective Date: January 1, 2017 Schedule: 6A Booklet Base: 6 For: Choice POS II High Deductible Health Plan - Faculty,
Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 28, 2017 Effective Date: January 1, 2017 Schedule: 6A Booklet Base: 6 For: Choice POS II High Deductible Health Plan - Faculty,
BRONZE PPO PLAN BENEFIT SUMMARY
 BRONZE PPO PLAN BENEFIT SUMMARY All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special
BRONZE PPO PLAN BENEFIT SUMMARY All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special
Not applicable Optional. CHE PREFERRED CARE (Home Host) Covered 100%
 PLAN FEATURES Catholic Health East PROVIDED BY LIFE INSURANCE COMPANY Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
PLAN FEATURES Catholic Health East PROVIDED BY LIFE INSURANCE COMPANY Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
OVERVIEW OF YOUR BENEFITS
 OVERVIEW OF YOUR BENEFITS 9 IMPORTANT PHONE NUMBERS Rochester Benefit Fund Office (585) 244-0830 For questions about eligibility, Coordination of Benefits, your 1199SEIU Health Benefits ID card, prescription
OVERVIEW OF YOUR BENEFITS 9 IMPORTANT PHONE NUMBERS Rochester Benefit Fund Office (585) 244-0830 For questions about eligibility, Coordination of Benefits, your 1199SEIU Health Benefits ID card, prescription
Additional Information Provided by Aetna Life Insurance Company
 Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
Choice 750 Gold 49831WA
 Choice 750 Gold Choice 750 Gold 49831WA1860004 INTRODUCTION Welcome Thank you for choosing Premera Blue Cross (Premera) for your healthcare coverage. This benefit booklet tells you about your plan benefits
Choice 750 Gold Choice 750 Gold 49831WA1860004 INTRODUCTION Welcome Thank you for choosing Premera Blue Cross (Premera) for your healthcare coverage. This benefit booklet tells you about your plan benefits
Not applicable. Immunizations 1 exam per 12 months for members age 18 to age 65; 1 exam per 12 months for adults age 65 and older.
 PLAN FEATURES NON- Deductible (per calendar year) $300 Employee $600 Employee $900 Family $1,800 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
PLAN FEATURES NON- Deductible (per calendar year) $300 Employee $600 Employee $900 Family $1,800 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
GUIDE TO MEDICAL AND DENTAL PLANS
 GUIDE TO MEDICAL AND DENTAL PLANS B e n e f i t s e f f e c t i v e J u l y 1, 2 0 1 4 t h r o u g h J u n e 3 0, 2 0 1 5 Choosing your benefits is an important decision. This guide provides you with the
GUIDE TO MEDICAL AND DENTAL PLANS B e n e f i t s e f f e c t i v e J u l y 1, 2 0 1 4 t h r o u g h J u n e 3 0, 2 0 1 5 Choosing your benefits is an important decision. This guide provides you with the
Aetna Choice POS II Medical Plan PLAN FEATURES NETWORK OUT-OF-NETWORK. Individual Deductible* $3,500 $5,000. Family Deductible* $7,000 $10,000
 Schedule of Benefits Employer: County of El Paso MSA: 866233 Effective Date: January 1, 2017 Schedule: 1C Booklet Base: 1 For: Aetna Choice POS II Consumer Driven Health Plan (CDHP) Aetna Choice POS II
Schedule of Benefits Employer: County of El Paso MSA: 866233 Effective Date: January 1, 2017 Schedule: 1C Booklet Base: 1 For: Aetna Choice POS II Consumer Driven Health Plan (CDHP) Aetna Choice POS II
This is an ERISA plan, and you have certain rights under this plan. Please contact your Employer for additional information.
 Schedule of Benefits Employer: Adobe Systems Incorporated MSA: 660819 Issue Date: January 1, 2018 Effective Date: January 1, 2018 Schedule: 1A Booklet Base: 1 For: Aetna Choice POS II with Health Fund
Schedule of Benefits Employer: Adobe Systems Incorporated MSA: 660819 Issue Date: January 1, 2018 Effective Date: January 1, 2018 Schedule: 1A Booklet Base: 1 For: Aetna Choice POS II with Health Fund
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield Name of Carrier Tonik for Individuals $3,000 Name of Plan
 Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield Name of Carrier Tonik for Individuals $3,000 Name of Plan PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. CARE
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield Name of Carrier Tonik for Individuals $3,000 Name of Plan PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. CARE
California Small Group MC Aetna Life Insurance Company NETWORK CARE
 PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Vanderbilt University. Aetna Choice POS II Health Fund Plan
 BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
This is an ERISA plan, and you have certain rights under this plan. Please contact your Employer for additional information.
 Schedule of Benefits Employer: VMware, Inc. MSA: 307138 Issue Date: April 25, 2017 Effective Date: January 1, 2017 Schedule: 4A Booklet Base: 4 For: Choice POS II - High Deductible Health Plan This is
Schedule of Benefits Employer: VMware, Inc. MSA: 307138 Issue Date: April 25, 2017 Effective Date: January 1, 2017 Schedule: 4A Booklet Base: 4 For: Choice POS II - High Deductible Health Plan This is
SILVER PPO PLAN BENEFIT SUMMARY
 SILVER PPO PLAN BENEFIT SUMMARY All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special
SILVER PPO PLAN BENEFIT SUMMARY All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special
PLAN E-1 PPO BENEFIT SUMMARY LANDSCAPERS
 LANDSCAPERS All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special limits noted in
LANDSCAPERS All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special limits noted in
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Carey International, Inc. High Deductible Choice POS II
 BENEFIT PLAN Prepared Exclusively for Carey International, Inc. What Your Plan Covers and How Benefits are Paid High Deductible Choice POS II Table of Contents Schedule of Benefits... Issued with Your
BENEFIT PLAN Prepared Exclusively for Carey International, Inc. What Your Plan Covers and How Benefits are Paid High Deductible Choice POS II Table of Contents Schedule of Benefits... Issued with Your
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Vanderbilt University Medical Center
 BENEFIT PLAN Prepared Exclusively for Vanderbilt University Medical Center What Your Plan Covers and How Benefits are Paid Aetna Choice POS II (Plus) Plan Table of Contents Schedule of Benefits... Issued
BENEFIT PLAN Prepared Exclusively for Vanderbilt University Medical Center What Your Plan Covers and How Benefits are Paid Aetna Choice POS II (Plus) Plan Table of Contents Schedule of Benefits... Issued
Yes. Some of the services this plan doesn t cover are listed on page 4
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.centuryhealthcare/com/user/login or by calling 1-877-685-2432.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.centuryhealthcare/com/user/login or by calling 1-877-685-2432.
AETNA MEMBER GUIDEBOOK
 State of New Jersey AETNA MEMBER GUIDEBOOK Aetna Value HD Plan Aetna Freedom Plan Aetna Medicare Advantage PPO ESA Plan FOR EMPLOYEES AND RETIREES ENROLLED IN THE STATE HEALTH BENEFITS PROGRAM OR SCHOOL
State of New Jersey AETNA MEMBER GUIDEBOOK Aetna Value HD Plan Aetna Freedom Plan Aetna Medicare Advantage PPO ESA Plan FOR EMPLOYEES AND RETIREES ENROLLED IN THE STATE HEALTH BENEFITS PROGRAM OR SCHOOL
PLAN DESIGN AND BENEFITS - NYC Community Plan SM 6-11 PARTICIPATING PROVIDER REFERRED*
 Aetna Health Inc. for Referred Benefits Plan Effective Date: 10/1/2011 PLAN FEATURES Deductible (per calendar ) $5,000 Individual $15,000 Family Unless otherwise indicated, the Deductible must be met prior
Aetna Health Inc. for Referred Benefits Plan Effective Date: 10/1/2011 PLAN FEATURES Deductible (per calendar ) $5,000 Individual $15,000 Family Unless otherwise indicated, the Deductible must be met prior
UnitedHealthcare Choice Plus. United HealthCare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus United HealthCare Insurance Company Certificate of Coverage For the Definity Health Savings Account (HSA) Plan 7PC of East Central College Enrolling Group Number: 711369 Effective
UnitedHealthcare Choice Plus United HealthCare Insurance Company Certificate of Coverage For the Definity Health Savings Account (HSA) Plan 7PC of East Central College Enrolling Group Number: 711369 Effective
Additional Information Provided by Aetna Life Insurance Company
 Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
SDMGMA Third Party Payer Day. Anja Aplan, Payment Control Officer
 SDMGMA Third Party Payer Day Anja Aplan, Payment Control Officer Agenda Medicaid Overview Third Party Liability Common TPL Errors NPI and Taxonomy Billing Transportation Billing Diagnosis codes Aid Category
SDMGMA Third Party Payer Day Anja Aplan, Payment Control Officer Agenda Medicaid Overview Third Party Liability Common TPL Errors NPI and Taxonomy Billing Transportation Billing Diagnosis codes Aid Category
Preferred Savings Plan
 An independent member of the Blue Shield Association Preferred Savings Plan Benefit Booklet Long Beach Unified School District Group Number: 977924 Effective Date: January 1, 2014 Claims Administered by
An independent member of the Blue Shield Association Preferred Savings Plan Benefit Booklet Long Beach Unified School District Group Number: 977924 Effective Date: January 1, 2014 Claims Administered by
SUMMARY OF BENEFITS Fisk University Open Access Plus -BUY-UP PLAN Effective 10/1/2015 Customer Service:
 SUMMARY OF BENEFITS Fisk University Open Access Plus -BUY-UP PLAN Effective www.mycigna.com Customer Service: 866-494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
SUMMARY OF BENEFITS Fisk University Open Access Plus -BUY-UP PLAN Effective www.mycigna.com Customer Service: 866-494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
The PPO Savings Plan. Faculty, Staff & Technical Service. Schedule of Benefits
 The PPO Savings Plan Faculty, Staff & Technical Service Schedule of Benefits Prepared exclusively for: Employer: The Pennsylvania State University Contract number: 285717 Control number: 285739 Technical
The PPO Savings Plan Faculty, Staff & Technical Service Schedule of Benefits Prepared exclusively for: Employer: The Pennsylvania State University Contract number: 285717 Control number: 285739 Technical
Schedule of Benefits
 Aetna Whole Health SM Accountable Care Network Choice POS II - $1,500 Plan Schedule of Benefits If this is an ERISA plan, you have certain rights under this plan. Please contact your employer for additional
Aetna Whole Health SM Accountable Care Network Choice POS II - $1,500 Plan Schedule of Benefits If this is an ERISA plan, you have certain rights under this plan. Please contact your employer for additional
RETIREE BENEFIT SUMMARY
 All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services, or Medicare-allowable fee limits for Medicare-eligible
All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services, or Medicare-allowable fee limits for Medicare-eligible
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
Employee Benefit Plan: Missoula County Public Schools Coverage Period: 01/01/ /31/2014 Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Gwinnett County Board Of Commissioners. Aetna Choice POSII
 BENEFIT PLAN Prepared Exclusively for Gwinnett County Board Of Commissioners Aetna Choice POSII What Your Plan Covers and How Benefits are Paid 1 Welcome Thank you for choosing Aetna. This is your booklet.
BENEFIT PLAN Prepared Exclusively for Gwinnett County Board Of Commissioners Aetna Choice POSII What Your Plan Covers and How Benefits are Paid 1 Welcome Thank you for choosing Aetna. This is your booklet.
Schedule of Benefits. Plumbers Union Local 12 HMO. A Prime Solutions HMO Plan
 Schedule of Benefits Plumbers Union Local 12 HMO A Prime Solutions HMO Plan health plan meets Minimum Creditable Coverage standards and will satisfy the individual mandate that you have health insurance.
Schedule of Benefits Plumbers Union Local 12 HMO A Prime Solutions HMO Plan health plan meets Minimum Creditable Coverage standards and will satisfy the individual mandate that you have health insurance.
Health Care Law & You
 Health Care Law & You How to get the most out of your health care dollars Table of Contents Introduction 1 Part I: The ABCs of Health Insurance 2 How Health Insurance Works Paying for Care Types of Health
Health Care Law & You How to get the most out of your health care dollars Table of Contents Introduction 1 Part I: The ABCs of Health Insurance 2 How Health Insurance Works Paying for Care Types of Health
OFFICE OF INSURANCE REGULATION Life & Health Product Review INDIVIDUAL HEALTH CONTRACT CHECKLIST
 Statute/Rule Description Yes No N/A Page # 69O-154.001 Important Notice must appear in a prominent manner. 69O-154.003 Notice of Insured's Right to Return Policy: The insured has 10 days from receipt of
Statute/Rule Description Yes No N/A Page # 69O-154.001 Important Notice must appear in a prominent manner. 69O-154.003 Notice of Insured's Right to Return Policy: The insured has 10 days from receipt of
OPERATORS HEALTH CENTER (OHC) PLAN BENEFIT SUMMARY
 OPERATORS HEALTH CENTER (OHC) PLAN BENEFIT SUMMARY All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for VBP Plan provider
OPERATORS HEALTH CENTER (OHC) PLAN BENEFIT SUMMARY All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for VBP Plan provider
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield RightPlan PPO 40 (With Generic Prescription Drug Coverage)
 Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield RightPlan PPO 40 (With Generic Prescription Drug Coverage) PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield RightPlan PPO 40 (With Generic Prescription Drug Coverage) PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK
PLAN A-5 PPO BENEFIT SUMMARY MUNICIPALITY (MONTHLY)
 MUNICIPALITY (MONTHLY) All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special limits
MUNICIPALITY (MONTHLY) All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special limits
Aetna Select Medical Plan PLAN FEATURES NETWORK OUT-OF-NETWORK. Plan Maximum Out of Pocket Limit excludes precertification penalties.
 Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 25, 2016 Effective Date: January 1, 2016 Schedule: 12D Booklet Base: 12 For: Aetna Select - Security Staff (Outside CT) Electing
Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: July 25, 2016 Effective Date: January 1, 2016 Schedule: 12D Booklet Base: 12 For: Aetna Select - Security Staff (Outside CT) Electing
Blue Cross Blue Shield of Arizona BluePreferred Plan Comparison
 Blue Cross Blue Shield of Arizona BluePreferred Plan Comparison Benefits BluePreferred Plan 100 BluePreferred Copay 100 BluePreferred Copay 250 BluePreferred Copay 500 Blue Preferred Copay 1000 Blue Preferred
Blue Cross Blue Shield of Arizona BluePreferred Plan Comparison Benefits BluePreferred Plan 100 BluePreferred Copay 100 BluePreferred Copay 250 BluePreferred Copay 500 Blue Preferred Copay 1000 Blue Preferred
PARTICIPATING PROVIDERS / REFERRED Deductible (per calendar year)
 Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Your HMO Plan Primary Care Physician - You choose a Primary Care Physician. The Aetna HMO Deductible provider network gives you access to a wide selection of Primary Care Physicians ( PCP's) and Specialists
Basic Fixed indemnity health insurance for individuals and families
 Basic Fixed indemnity health insurance for individuals and families Basic is a group association fixed indemnity health insurance plan underwritten by Madison National Life Insurance Company, Inc., a Wisconsin
Basic Fixed indemnity health insurance for individuals and families Basic is a group association fixed indemnity health insurance plan underwritten by Madison National Life Insurance Company, Inc., a Wisconsin
15% 30% $7,350 Individual Unlimited Individual (per calendar year) Out-Of-Pocket Maximum
 PLAN FEATURES Deductible (per calendar year) $1,750 Individual $20,000 Individual $3,500 Family $40,000 Family All covered expenses accumulate toward both the preferred and non-preferred Deductible. Unless
PLAN FEATURES Deductible (per calendar year) $1,750 Individual $20,000 Individual $3,500 Family $40,000 Family All covered expenses accumulate toward both the preferred and non-preferred Deductible. Unless
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18 12/31/18
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18 12/31/18 Wood County Employee Health Benefits Plan: Health & RX only Coverage for: Single/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18 12/31/18 Wood County Employee Health Benefits Plan: Health & RX only Coverage for: Single/Family
PLAN DESIGN AND BENEFITS - IN MANAGED CHOICE POS OPEN ACCESS 90/60/60 $1,000 PREFERRED CARE
 PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
For: Choice POS II - Clerical & Technical and Service & Maintenance Employees Choice POS II (Base Rx) Plan
 Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: June 23, 2016 Effective Date: January 1, 2016 Schedule: 2A Booklet Base: 2 For: Choice POS II - Clerical & Technical and Service &
Schedule of Benefits Employer: Yale University ASA: 877076 Issue Date: June 23, 2016 Effective Date: January 1, 2016 Schedule: 2A Booklet Base: 2 For: Choice POS II - Clerical & Technical and Service &
Important Questions Answers Why this Matters:
 Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
Florida - EPO Aetna Select - ASC PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY PLAN FEATURES
 PLAN FEATURES Deductible (per calendar year) $100 Individual $200 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Pharmacy expenses do not apply towards the
PLAN FEATURES Deductible (per calendar year) $100 Individual $200 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Pharmacy expenses do not apply towards the
DY574_261023_br. Indiana Association for Home & Hospice Care Reimbursement Meeting February 24, 2010
 Indiana Association for Home & Hospice Care Reimbursement Meeting February 24, 2010 Medical Necessity Reviews Providers have raised concerns regarding the need for signed MD orders to approve a request
Indiana Association for Home & Hospice Care Reimbursement Meeting February 24, 2010 Medical Necessity Reviews Providers have raised concerns regarding the need for signed MD orders to approve a request
PLAN COMPARISON (Blue Cross Blue Shield of Massachusetts) For Members Who Are Eligible For Medicare
 Quarterly Premium Rate * Per Person $2,215.08 $1,789.50 $618.99 $890.70 Rates effective: 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 Eligibility Service
Quarterly Premium Rate * Per Person $2,215.08 $1,789.50 $618.99 $890.70 Rates effective: 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 1/1/16 through 12/31/16 Eligibility Service
PLAN COMPARISON (Blue Cross Blue Shield of Massachusetts) For Members Who Are Eligible For Medicare
 Quarterly Premium Rate * Per Person $2,358.60 $1,905.33 $658.74 $1,165.11 Rates effective: 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 Eligibility Service
Quarterly Premium Rate * Per Person $2,358.60 $1,905.33 $658.74 $1,165.11 Rates effective: 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 1/1/17 through 12/31/17 Eligibility Service
Terms Defined. Participating/Non-Participating Provider. Benefits Coverage Charts. Prescription Drug Purchases. Pre-Authorization
 Medical Coverage Terms Defined Participating/Non-Participating Provider Benefits Coverage Charts Prescription Drug Purchases Section Two MEDICAL COVERAGE Pre-Authorization Coordination of Benefits Questions
Medical Coverage Terms Defined Participating/Non-Participating Provider Benefits Coverage Charts Prescription Drug Purchases Section Two MEDICAL COVERAGE Pre-Authorization Coordination of Benefits Questions
Covered 100% 20% 1 exam per 12 months for members age 18 and older.
 PLAN FEATURES NON- Deductible (per calendar year) $1,200 Individual $2,000 Individual $3,600 Family $6,000 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred
PLAN FEATURES NON- Deductible (per calendar year) $1,200 Individual $2,000 Individual $3,600 Family $6,000 Family All covered expenses, excluding prescription drugs, accumulate toward both the preferred
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Conroe Independent School District
 BENEFIT PLAN Prepared Exclusively for Conroe Independent School District What Your Plan Covers and How Benefits are Paid Aetna Select - Aetna Whole Health - Memorial Hermann Accountable Care Network Table
BENEFIT PLAN Prepared Exclusively for Conroe Independent School District What Your Plan Covers and How Benefits are Paid Aetna Select - Aetna Whole Health - Memorial Hermann Accountable Care Network Table
Lourdes Health System Proposed Effective Date: Aetna Helathfund Aetna Choice POS ll - ASC Salary Band: Less than $21,000 to $41,999
 PROVIDED BY LIFE INSURANCE COMPANY FUND FEATURES HealthFund Amount $750 Employee $1,500 Employee + Spouse $1,500 Employee + Child(ren) $1,500 Family Amount contributed to the Fund by the employer Fund
PROVIDED BY LIFE INSURANCE COMPANY FUND FEATURES HealthFund Amount $750 Employee $1,500 Employee + Spouse $1,500 Employee + Child(ren) $1,500 Family Amount contributed to the Fund by the employer Fund
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING NO-REFERRAL 4.4 ($2,000 DED) $2,000 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
Pharmacy Coverage and Claim Submission Guidelines
 P R O V I D E R B U L L E T I N B T 2 0 0 0 0 1 8 J U N E 1, 2 0 0 0 To: Subject: All Indiana Health Coverage Programs Providers Overview The purpose of this bulletin is to provide coverage and reimbursement
P R O V I D E R B U L L E T I N B T 2 0 0 0 0 1 8 J U N E 1, 2 0 0 0 To: Subject: All Indiana Health Coverage Programs Providers Overview The purpose of this bulletin is to provide coverage and reimbursement
Network Providers. deductible?
 Hoosier Heartland School Trust: Plan 1 Blue Access (PPO) Coverage Period: 1/01/2017-08/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan
Hoosier Heartland School Trust: Plan 1 Blue Access (PPO) Coverage Period: 1/01/2017-08/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan
$0 Family coverage not provided. Family coverage not provided
 Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield RightPlan PPO 40 (With Prescription Drug Coverage) PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK
Colorado Health Plan Description Form Anthem Blue Cross and Blue Shield RightPlan PPO 40 (With Prescription Drug Coverage) PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK
PLAN DESIGN AND BENEFITS - New York Open Access MC 3-11 HSA Compatible
 PLAN FEATURES Deductible (per plan year) $3,000 Individual $6,000 Individual $6,000 Family $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered
PLAN FEATURES Deductible (per plan year) $3,000 Individual $6,000 Individual $6,000 Family $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal
 Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
Introduction to UnitedHealthcare Community Plan of California/Medi-Cal Welcome/Agenda: Mission/Vision UnitedHealthcare Community Plan of California/Medi-Cal Member Eligibility and Benefits Notification
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PA of Educators Benefit Services, Inc. Enrolling Group Number: 717578
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PA of Educators Benefit Services, Inc. Enrolling Group Number: 717578
Blue Choice New England - Enhanced Northeastern University Coverage Period: on or after 01/01/2015
 Blue Choice New England - Enhanced Northeastern University Coverage Period: on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family
Blue Choice New England - Enhanced Northeastern University Coverage Period: on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
MIT Affiliate Health Plans
 MIT Affiliate Health Plans 2017 2018 Overview In this book: Insurance plans and rates How to enroll Your medical benefits Commonly used terms Useful contact information 1 Insurance plans and rates MIT
MIT Affiliate Health Plans 2017 2018 Overview In this book: Insurance plans and rates How to enroll Your medical benefits Commonly used terms Useful contact information 1 Insurance plans and rates MIT
Highest level of coverage with free-choice of hospitals and physicians worldwide, with the richest maternity and organ transplant benefits.
 Highest level of coverage with free-choice of hospitals and physicians worldwide, with the richest maternity and organ transplant benefits. Global Superior Plus is tailored exclusively for individuals
Highest level of coverage with free-choice of hospitals and physicians worldwide, with the richest maternity and organ transplant benefits. Global Superior Plus is tailored exclusively for individuals
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING 3.4 ($1,500 DED) PARTICIPATING PROVIDERS. $1,500 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
*2017 Plan Cost Comparison
 *2017 Plan Cost Comparison The following health insurance plans are available to Medicare-eligible plan participants enrolled in both Medicare Part A and Part B, unless you have Medicare due to ESRD and
*2017 Plan Cost Comparison The following health insurance plans are available to Medicare-eligible plan participants enrolled in both Medicare Part A and Part B, unless you have Medicare due to ESRD and
FREQUENTLY ASKED QUESTIONS (DESIGNED FOR GOOSE CREEK CONSOLIDATED INDEPENDENT SCHOOL DISTRICT)
 FREQUENTLY ASKED QUESTIONS (DESIGNED FOR GOOSE CREEK CONSOLIDATED INDEPENDENT SCHOOL DISTRICT) What is NexStep? NexStep is underwritten by Fidelity Security Life Insurance Company (Kansas City, Missouri)
FREQUENTLY ASKED QUESTIONS (DESIGNED FOR GOOSE CREEK CONSOLIDATED INDEPENDENT SCHOOL DISTRICT) What is NexStep? NexStep is underwritten by Fidelity Security Life Insurance Company (Kansas City, Missouri)
CHE PREFERRED CARE (Home Host)
 PLAN FEATURES Catholic Health East PROVIDED BY LIFE INSURANCE COMPANY Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
PLAN FEATURES Catholic Health East PROVIDED BY LIFE INSURANCE COMPANY Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family
BENEFITS CHI. Summary of Benefits Coverage. Basic Blue Cross Blue Shield of Illinois. Effective January 1, 2015
 CHI BENEFITS Summary of Benefits Coverage Basic Blue Cross Blue Shield of Illinois Effective January 1, 2015 The following is an overview of your Catholic Health Initiatives Basic medical plan option for
CHI BENEFITS Summary of Benefits Coverage Basic Blue Cross Blue Shield of Illinois Effective January 1, 2015 The following is an overview of your Catholic Health Initiatives Basic medical plan option for
PREFERRED CARE. Covered 100%; deductible waived Not Covered
 PLAN FEATURES NON- Deductible (per calendar year) $1,300 Individual $1,300 Individual $2,600 Family $2,600 Family All covered expenses including prescription drugs accumulate toward both the preferred
PLAN FEATURES NON- Deductible (per calendar year) $1,300 Individual $1,300 Individual $2,600 Family $2,600 Family All covered expenses including prescription drugs accumulate toward both the preferred
Chapter 7 General Billing Rules
 7 General Billing Rules Reviewed/Revised: 10/10/2017, 07/13/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 General Information This chapter contains general information related to Health Choice Arizona
7 General Billing Rules Reviewed/Revised: 10/10/2017, 07/13/2017, 02/01/2017, 02/15/2016, 09/16/2015, 09/18/2014 General Information This chapter contains general information related to Health Choice Arizona
MSI Fairview and North Memorial Vantage ASO % Coverage Period: Beginning on or after 1/1/2017 Summary of Benefits and Coverage:
 This is only a summary: If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.medica.com or by calling 1-855-569-7526. Important Questions
This is only a summary: If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.medica.com or by calling 1-855-569-7526. Important Questions
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. RADCO Health Savings Account Open Access Plus
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. RADCO Health Savings Account Open Access Plus General Services In-Network Out-of-Network Physician office visit Primary Care Physician (PCP) Physician
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. RADCO Health Savings Account Open Access Plus General Services In-Network Out-of-Network Physician office visit Primary Care Physician (PCP) Physician
BlueSecure Plus HMO Plan Benefit Summary
 BlueSecure Plus HMO Plan Benefit Summary This plan is available for issuance effective October 1, 2008 Network Providers Except for emergencies, all covered services must be rendered by a network provider.
BlueSecure Plus HMO Plan Benefit Summary This plan is available for issuance effective October 1, 2008 Network Providers Except for emergencies, all covered services must be rendered by a network provider.
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Important Questions Answers Why this Matters. $2,000 per individual/$4,000 per family
 Health New England: Health Connector - HNE Essential 2000 Coverage Period: 1/1/2013-12/31/2013 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family
Health New England: Health Connector - HNE Essential 2000 Coverage Period: 1/1/2013-12/31/2013 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Sarasota County Government
 BENEFIT PLAN Prepared Exclusively for Sarasota County Government What Your Plan Covers and How Benefits are Paid Aetna Choice POS II with Aetna HeathFund Non -Union Table of Contents Schedule of Benefits...
BENEFIT PLAN Prepared Exclusively for Sarasota County Government What Your Plan Covers and How Benefits are Paid Aetna Choice POS II with Aetna HeathFund Non -Union Table of Contents Schedule of Benefits...
BUSINESS BLUE COMPLETE (formerly Preferred Blue) My employees want a plan with excellent benefits. I need a plan that is customized for my business.
 BUSINESS BLUE COMPLETE (formerly Preferred Blue) My employees want a plan with excellent benefits. I need a plan that is customized for my business. This is our plan. Business Blue SM Complete (formerly
BUSINESS BLUE COMPLETE (formerly Preferred Blue) My employees want a plan with excellent benefits. I need a plan that is customized for my business. This is our plan. Business Blue SM Complete (formerly
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co.
 SUMMARY OF BENEFITS Ohio Associated Enterprises Health Savings Account Open Access Plus www.mycigna.com Member Services: (866) 494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
SUMMARY OF BENEFITS Ohio Associated Enterprises Health Savings Account Open Access Plus www.mycigna.com Member Services: (866) 494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
Blue Care Elect $250 Deductible Coverage Period: on or after 07/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 Blue Care Elect $250 Deductible Coverage Period: on or after 07/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is
Blue Care Elect $250 Deductible Coverage Period: on or after 07/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is
PLAN DESIGN AND BENEFITS - PA POS HSA COMPATIBLE NO-REFERRAL 2.4 ($2,500 Ded) PARTICIPATING PROVIDERS
 PLAN FEATURES Deductible (per plan year) $2,500 Individual NON- $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All
PLAN FEATURES Deductible (per plan year) $2,500 Individual NON- $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All
PLAN A-4 PPO BENEFIT SUMMARY STAFF EMPLOYEES OWNERS/RELATIVES
 STAFF EMPLOYEES OWNERS/RELATIVES All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special
STAFF EMPLOYEES OWNERS/RELATIVES All benefits are subject to eligibility, maximum Plan benefit, reasonable and customary determination (or negotiated fee amounts for PPO provider services), and any special
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Blue Care Elect Preferred Northeastern University
 Blue Care Elect Preferred Northeastern University Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: on or after 01/01/2014 Coverage for: Individual and Family Plan
Blue Care Elect Preferred Northeastern University Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: on or after 01/01/2014 Coverage for: Individual and Family Plan
$8,300 $24,900 Maximum Lifetime Benefit
 PPO Schedule of Health Plus 2 C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive
PPO Schedule of Health Plus 2 C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive
$4,800 $9,600 Maximum Lifetime Benefit
 PPO Schedule of PPO Medical C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive months
PPO Schedule of PPO Medical C & A Industries, Inc. Plan Effective Date: January 1, 2019 In-Network Out-of-Network** Benefit Year means a calendar year, which is the period of twelve (12) consecutive months
Appendix A Colorado Health Plan Description Form. PacifiCare Life Assurance Company. Individual Plan 70-50/3000
 Appendix A Colorado Health Plan Description Form PacifiCare Life Assurance Company Individual Plan 70-50/3000 PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan. 2. OUT-OF-NETWORK CARE COVERED?
Appendix A Colorado Health Plan Description Form PacifiCare Life Assurance Company Individual Plan 70-50/3000 PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan. 2. OUT-OF-NETWORK CARE COVERED?
