Building an Effective Reimbursement System. Population Based Reimbursement: Introduction. The Challenge. David Axene, FSA, FCA, CERA, MAAA
|
|
|
- Cleopatra Hardy
- 5 years ago
- Views:
Transcription
1 Population Based Reimbursement: Building an Effective Reimbursement System David Axene, FSA, FCA, CERA, MAAA Introduction As more and more health systems consider population based reimbursement, pursue the development of ACOs, and consider value based reimbursement methods, they are faced with the age-old question of how do we distribute the funds to providers?. As the old scripture proverb states History merely repeats itself. It has all been done before. Nothing under the sun is truly new. This is truly the case with provider reimbursement and the task of distributing funds among the various stakeholders. The Challenge As financial risk is transferred from the payer/ administrator to individual health care providers, the provider payment process becomes increasingly complicated and requires innovation to assure appropriate financial outcomes. Under the traditional fee-for-service system, providers are paid or reimbursed only when they provide a service. However, as provider payments are based on alternate reimbursement methods different payment and allocation approaches must be deployed. The question becomes what method should be used? What method works the best? What method will achieve the best results?
2 A Generic Approach I usually recommend a rather simple approach based upon a generic framework that can achieve the desired results for almost any configuration of health care providers. This is based upon very simple and straightforward principles familiar to most observers. What are the basic categories of care? They consist of: Primary care services Specialty care services Ancillaries Institutional services Prescription drugs Organizing the reimbursement system around these five categories provides a consistent framework that is highly adaptable to various provider structures. For example, if the reimbursement is focused on a group of primary care providers, the primary care segment can be used to craft the desirable approach. When it is focused on a multispecialty medical group, both physician categories can be combined to develop the desired approach for entire physician segment. If it is a broader Clinically Integrated Network (i.e., CIN) or ACO, perhaps the entire group of categories are combined in some fashion. As categories are grouped into broader categories, basic principles of reimbursement for the individual categories can be preserved. As the individual categories are grouped to determine overall reimbursement levels, basic principles of reimbursement within each of the five categories can be preserved within the broader structure to achieve the optimal reimbursement approach. Primary Care Services Once primary care services are clearly defined, preferably in terms of CPT codes, the reimbursement methodology can be selected. Personal preference leans towards primary care capitation, although capitation is clearly not required. As long as the assigned member panel is large enough for statistical reliability, capitation works well. With the advent of reliable risk adjustors in the marketplace, risk adjustment solves most of the earlier concerns by primary care providers. I usually recommend both demographic and risk adjustment. I prefer both withholds and gain sharing of referral services. I recommend a variable withhold model that decreases the withhold (i.e., required risk margin) for those providers consistently earning incentive payments and increases the withhold for those generating losses or consistently using their withholds for higher than expected payment levels. Specialty Care Services Since few specialists have direct assignment to individual patients, they don t explicitly control referral patterns or demand for their services. As a result, they oftentimes experience volatility from one time period to another and it is usually inappropriate to utilize specialty capitation. As a result, traditional fee-for-service reimbursement is most common. For those specialists willing to accept a withhold, some gain sharing is possible and reasonable. Most institutional care and the use of ancillary services are driven by the specialists so it is reasonable to include some type of incentive based upon the appropriateness of institutional and ancillary utilization or performance. Usually inappropriate to use specialty capitation. The selection of the individual specialist is usually the direct choice of the primary care provider (i.e., the PCP s referral pattern), so it is always reasonable to include the primary care doctor in the performance analysis. Ancillary Services The use of ancillary services is directly tied to referrals by specialists and some primary care providers. Ancillary providers do what they are told to do, should be held accountable for doing it right the first time, and have little to do with the overall performance. They are not able to do much to impact performance, perhaps with the exception of refusing to perform a medically inappropriate referral. They function as vendors in the health care system, very important vendors, yet not controlling much of the cost of the health care system. Most ancillary services are performed on a fee-for-service basis although some (e.g., lab services) have agreed to various forms of capitation. Institutional Services Institutional services are often viewed as the most critical category of services since these are the ones where care management efforts potentially achieve the greatest savings. Our consulting assignments show that two-thirds of what can be saved is often associated with inpatient care. In care management parlance, the greatest opportunity for changes in cost are in shortening and eliminating potentially avoidable inpatient stays. Different approaches have been used to reimburse institutional services with the most current 2
3 and most popular approach being DRG case rates for inpatient and APC related for outpatient services. Important to incorporate acuity/ severity in payment mechanism to match payments with required resources. Experience suggests that DRG case rates may provide long term savings but do not provide immediate or short term savings from length of stay reduction. Traditional per diem methodologies provide the greatest savings but market trends have clearly gravitated to DRG case rates. The integrated delivery system models (i.e., ACO and CIN) also utilize forms of capitation although usually incorporate some cost reconciliation at the end of the reporting period. I recommend an approach that incorporates acuity severity if using a DRG case rate approach (i.e., APR-DRGs or MS-DRGs). Recognizing acuity and severity in the reimbursement methodology better matches the consumption of resources with the reimbursement reducing the concerns of the institutions. This same organization graphically presented the risk transfer showing population risk on the vertical axis and clinical risk on the horizontal axis. Most of the incentive mechanisms compare budgeted institutional services with those provided including the savings or cost reductions in the incentive program with providers. Prescription Drugs Prescription drug costs are an increasingly importance cost category especially as drug costs now increase at a much higher rate than other services. Specialty drugs have become a more important category with the introduction of very expensive drugs (i.e., Hep-C drugs, HIV drugs, etc.). Pharmacy management programs are increasing in effectiveness through the use of sophisticated formulary management practices and benefit design enhancements. Some incentive plans transfer much of the risk to providers and in turn their incentive programs, while other approaches delegate much of the management of that to contracted PBMs. Capitation programs are popular in some markets. Basic Incentive Design Considerations As the strategist begins to design the system it is helpful to categorize and quantify the impact of various risk transfer efforts. The chart below is one organization s attempt to quantify risk for various reimbursement methods (i.e., red is high risk, blue is low risk). As this last chart shows, global capitation transfers the greatest risk to the provider entity (i.e., high population risk and high clinical risk). The key considerations of an effective reimbursement and incentive system are: Population: Clear understanding of who the population is so that prior experience can be reviewed and compared to proposed reimbursement levels Demographic Adjustment: Prior to the development of appropriate risk adjustment methodologies, one of the most effective adjustments available in the marketplace were 3
4 demographic or age/gender adjustments. Utilization and costs tend to increase as the person ages. Female costs tends to be higher than male costs. As the population mix changes costs can vary significantly. For pediatric populations the gender difference is much smaller than for other populations. Risk adjustment: Providers must be protected from shifts in the population mix, especially shifts in underlying morbidity/health status. As morbidity/health status changes, anticipated health costs and burden of illness change which must be reflected in the health care budgets. There are several key considerations to develop an effective reimbursement and incentive system. Reimbursement levels: The historical data is based upon some negotiated reimbursement level. If there is no assumed change in reimbursement levels, then no adjustment is necessary. If there is a change, especially a reduction, then it needs to be reconciled to be sure the budgets are reasonable Care Management Effectiveness: The historical data is based upon the prior care management. To the extent that the care management process changes or is improved, the impact to the budgets needs to be understood. From the provider s perspective, one of the reasons it is willing to assume the additional risk is the opportunity to benefit from any improvements in care management they are able to implement. Trend and Inflationary Adjustments: To the extent that some inflationary trend has occurred and or an inflation adjustment is necessary, the budget needs to reflect that adjustment. Without appropriate adjustments the budgets can quickly become unreasonable. Division of Financial Responsibility (DOFR): The DOFR is used to identify what is included in the budget and who is responsible for it. This is a document that clearly defines what the capitation payment covers. This is critical to understand. This often includes a description of any carve-out or stop-loss protection that the health plan is offering the risk bearing organization. Potential Incentive Payments: The budget assessment requires a good understanding of what potential incentive payments might exist and how they would work. This is most important when only a portion of the health care dollar is capitated. If global capitation then this is not as critical. Risk Pools A frequently recommended incentive model is built around the concept of risk pools. The simplest such approach has been called the HARP Fund (i.e., Hospital and Risk Pool). The scope and size of the HARP fund varies depending upon what services are included. The simplest approach is: Primary Care Services HARP Fund In this situation, primary care services might be capitated with primary care doctors sharing a portion of the savings from all other services. In this case the HARP Fund would include specialty services, ancillary services, hospital inpatient and outpatient services and pharmacy. In a situation where Medical Group capitation was considered, it could be modified to: Professional services (i.e., Medical Group capitation) HARP Fund In the case of global capitation, it could be modified to: All services (i.e., global capitation) Empty HARP fund This highly flexible approach enables the planners to develop what is best for their own organization and structure. It is highly flexible. Quality Adjustment Any incentive payments from the above approaches should always be adjusted by quality performance. One frequently used approach adjusted using three specific performance components which are weighted as follows: Quality Measures: 25% Customer Satisfaction Measures: 25% Cost Measures: 50% Separate measures would be developed for each type of provider with actual payments based upon provider specific scoring in each of these areas. Some recommended measures for the first year are included in the table below by type of provider. Actual metrics, measures and goals would be set collaboratively and updated on an annual basis. 4
5 The overall intent is to pay 100% of the allocated risk incentive amount for excellent performance across the above metrics. We assume that no payment would be made if there is unacceptable performance, even if funds were available. A 50% payment would be appropriate for moderate or average performance. The goal is to maximize the performance so all providers are getting 100% of what they have earned. The previous table shows suggested performance measures. These should be collaboratively determined and agreed to in advance. It is critical that measures are administratively easy to obtain and reliable. The performance on each measure would correspond to a specific set of points ranging from 0% to 25% for Quality, 0% to 25% for Customer Satisfaction, and 0% to 50% for Cost Measures. The total of the three scores would determine an overall score determining the percentage of the incentive payments that would be paid to the provider. For example, a quality score of 20%, a customer satisfaction score of 15%, and a 40% cost score would total to 75%. A provider with this score would be paid 75% of their earned incentive payment. Any unpaid amount could be added to pool for future payments to providers. Key Success Factors The following table presents key success factors in achieving longterm success with provider reimbursement and incentives: 5
6 Adaptations of Model The above model is designed to be a convenient management tool to use when operating as a risk bearing organization. It can be adapted in a variety of ways to meet the unique requirements of any health plan or payer. For example, in an environment where an organization would take global capitation for a broad set of members, we would recommend that the organization internally manage the distribution of revenues using this approach even though receiving a global payment rate for all services. If in another situation the organization agreed to a professional capitation from a health plan or payer, we would recommend managing the professional capitation in total the way the primary care, specialty and super-specialty area was described above. This provides a useful approach to manage almost any type of reimbursement arrangement. It also provides a framework that the organization can use to negotiate an arrangement with a particular health plan and provides guidance as to how to share risk with a health plan. Health plans can also use this approach to maximize the consistency of its proposals to providers. The same underlying methodology can serve as the framework for arrangements made on a primary capitation only basis, a professional capitation basis and also a global capitation basis. We encourage organizations to consider this as a framework to use in its negotiations with health plans and payers. Summary Provider reimbursement and incentive systems can be complex, challenging to develop, and somewhat temperamental as different objectives or goals are introduced into the process. The above template provides a generic format that can be used to simplify the process. 1 Ecclesiastes 1:9 NLT. 2 Somewhat arbitrary allocation of importance. Goal was to have no less than half based upon quality and customer satisfaction. About the Author: David Axene, FSA, FCA, CERA, MAAA, is the President and Founding Partner of Axene Health Partners, LLC and is based in AHP s Murrieta, CA office. Dave can be reached at (951) or david.axene@axenehp.com. Axene Health Partners, LLC
Assessing ACO Performance
 Assessing ACO Performance David V. Axene, FSA, FCA, CERA, MAAA As more health plans utilize Accountable Care Organizations (i.e., ACOs) as part of their network operations, ACO performance assessment is
Assessing ACO Performance David V. Axene, FSA, FCA, CERA, MAAA As more health plans utilize Accountable Care Organizations (i.e., ACOs) as part of their network operations, ACO performance assessment is
Accountability: Hospital and Health System Pricing. Introduction. David V. Axene, FSA, CERA, FCA, MAAA
 Accountability: Hospital and Health System Pricing David V. Axene, FSA, CERA, FCA, MAAA Introduction In a traditional economic business model, the tension and interaction between supply and demand in a
Accountability: Hospital and Health System Pricing David V. Axene, FSA, CERA, FCA, MAAA Introduction In a traditional economic business model, the tension and interaction between supply and demand in a
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making. Introduction. William Bednar, FSA, FCA, MAAA
 Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
Building Actuarial Cost Models from Health Care Claims Data for Strategic Decision-Making William Bednar, FSA, FCA, MAAA Introduction Health care spending across the country generates billions of claim
Could an All-Payer System Improve the Affordability of US Health Care? Overview. David V. Axene, FSA, FCA, CERA, MAAA
 Could an All-Payer System Improve the Affordability of US Health Care? David V. Axene, FSA, FCA, CERA, MAAA Overview Do you ever get annoyed knowing that someone on your flight paid less than you did for
Could an All-Payer System Improve the Affordability of US Health Care? David V. Axene, FSA, FCA, CERA, MAAA Overview Do you ever get annoyed knowing that someone on your flight paid less than you did for
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations
 10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. Speaker Disclosures Steve Selbst is employed by a business firm that provides services related
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. Speaker Disclosures Steve Selbst is employed by a business firm that provides services related
10 Best Practices For Payer Contracting:
 10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. 2016 NHIA Annual Conference & Exposition 1 Speaker Disclosures Steve Selbst is employed by
10 Best Practices For Payer Contracting: A Roadmap for Successful Negotiations Steve Selbst Healthcents, Inc. 2016 NHIA Annual Conference & Exposition 1 Speaker Disclosures Steve Selbst is employed by
Calculating Accurate Metrics for the Actuarial Cost Model. Introduction. William Bednar, FSA, FCA, MAAA
 Calculating Accurate Metrics for the Actuarial Cost Model William Bednar, FSA, FCA, MAAA Introduction Calculating metrics for an actuarial model sounds simple enough (just sum up the data!), but if proper
Calculating Accurate Metrics for the Actuarial Cost Model William Bednar, FSA, FCA, MAAA Introduction Calculating metrics for an actuarial model sounds simple enough (just sum up the data!), but if proper
Roadmap to Successful Risk Contracting for Providers. Joe Slater, FSA, MAAA Partner and Consulting Actuary Axene Health Partners April 27, 2017
 Roadmap to Successful Risk Contracting for Providers Joe Slater, FSA, MAAA Partner and Consulting Actuary Axene Health Partners Overview Risk contracting basics for provider organizations The characteristics
Roadmap to Successful Risk Contracting for Providers Joe Slater, FSA, MAAA Partner and Consulting Actuary Axene Health Partners Overview Risk contracting basics for provider organizations The characteristics
Session 38PD, Use of Big Data to Optimize Plan Design. Moderator/Presenter: David V. Axene, FSA, CERA, FCA, MAAA
 Session 38PD, Use of Big Data to Optimize Plan Design Moderator/Presenter: David V. Axene, FSA, CERA, FCA, MAAA Presenters: Jordan Armstrong David V. Axene, FSA, CERA, FCA, MAAA Timothy W. Smith, ASA,
Session 38PD, Use of Big Data to Optimize Plan Design Moderator/Presenter: David V. Axene, FSA, CERA, FCA, MAAA Presenters: Jordan Armstrong David V. Axene, FSA, CERA, FCA, MAAA Timothy W. Smith, ASA,
AFFORDABILITY REVIEW. Mysteries of the Medical Loss Ratio
 AFFORDABILITY REVIEW Mysteries of the Medical Loss Ratio NANCY DJORDJEVIC DIRECTOR, HEALTHCARE ANALYTICS APRIL 2016 WHO IS GORMAN HEALTH GROUP? Gorman Health Group is the leading solutions and consulting
AFFORDABILITY REVIEW Mysteries of the Medical Loss Ratio NANCY DJORDJEVIC DIRECTOR, HEALTHCARE ANALYTICS APRIL 2016 WHO IS GORMAN HEALTH GROUP? Gorman Health Group is the leading solutions and consulting
Insightsfeature. Managing Specialty Drug Spend Under the Medical Benefit. Innovations and Automation for More Effective Management.
 Insightsfeature Managing Specialty Drug Spend Under the Medical Benefit Innovations and Automation for More Effective Management March 30, 2017 The Less-Visible Part of Specialty Spend By most estimates,
Insightsfeature Managing Specialty Drug Spend Under the Medical Benefit Innovations and Automation for More Effective Management March 30, 2017 The Less-Visible Part of Specialty Spend By most estimates,
10 Best Payer Contracting Practices for Presented By: Mr. Steve Selbst, CEO Healthcents Inc. November 7, 2018
 10 Best Payer Contracting Practices for 2019 Presented By: Mr. Steve Selbst, CEO Healthcents Inc. November 7, 2018 Healthcents Services Payer contracts analysis and negotiations Healthcare Consulting Services
10 Best Payer Contracting Practices for 2019 Presented By: Mr. Steve Selbst, CEO Healthcents Inc. November 7, 2018 Healthcents Services Payer contracts analysis and negotiations Healthcare Consulting Services
Considerations for a Hospital-Based ACO. Insurance Premium Construction: Tim Smith, ASA, MAAA, MS
 Insurance Premium Construction: Considerations for a Hospital-Based ACO Tim Smith, ASA, MAAA, MS I once saw a billboard advertising a new insurance product co-branded by the local hospital system and a
Insurance Premium Construction: Considerations for a Hospital-Based ACO Tim Smith, ASA, MAAA, MS I once saw a billboard advertising a new insurance product co-branded by the local hospital system and a
Session 115IF, Provider Risk-Sharing Arrangements in Medicaid. Presenters: Puneet Budhiraja, ASA, MAAA Michael Minor Sudha Shenoy, FSA, MAAA, CERA
 Session 115IF, Provider Risk-Sharing Arrangements in Medicaid Presenters: Puneet Budhiraja, ASA, MAAA Michael Minor Sudha Shenoy, FSA, MAAA, CERA SOA Antitrust Disclaimer SOA Presentation Disclaimer 2018
Session 115IF, Provider Risk-Sharing Arrangements in Medicaid Presenters: Puneet Budhiraja, ASA, MAAA Michael Minor Sudha Shenoy, FSA, MAAA, CERA SOA Antitrust Disclaimer SOA Presentation Disclaimer 2018
Factors in Physician Practice Valuation. May 2017
 Factors in Physician Practice Valuation May 2017 Factors in Physician Practice Valuation Physician practice owners considering a sale may not have experience assessing the value of their practices in terms
Factors in Physician Practice Valuation May 2017 Factors in Physician Practice Valuation Physician practice owners considering a sale may not have experience assessing the value of their practices in terms
Glossary of Terms. Adjudication: The way a health plan decides how much it will pay for certain expenses.
 Page 1 Glossary of Terms Adjudication: The way a health plan decides how much it will pay for certain expenses. Affordable Care Act (ACA): The comprehensive health care reform law enacted in March 2010.
Page 1 Glossary of Terms Adjudication: The way a health plan decides how much it will pay for certain expenses. Affordable Care Act (ACA): The comprehensive health care reform law enacted in March 2010.
Milliman RBRVS for Hospitals
 Will Fox, FSA, MAAA Ed Jhu, FSA, MAAA Charlie Mills, FSA, MAAA WHAT IS RBRVS FOR HOSPITALS? The Fee Schedule provides a simple solution for comparing hospital contractual allowed amounts, billed charge
Will Fox, FSA, MAAA Ed Jhu, FSA, MAAA Charlie Mills, FSA, MAAA WHAT IS RBRVS FOR HOSPITALS? The Fee Schedule provides a simple solution for comparing hospital contractual allowed amounts, billed charge
The Health Insurance Market in Virginia. Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017
 The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
Total Cost of Care in Oregon s Commercial Market. March 2, 2017
 Total Cost of Care in Oregon s Commercial Market March 2, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary Mission
Total Cost of Care in Oregon s Commercial Market March 2, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary Mission
Chapter 17 CAPITATION, RATE SETTING, AND RISK SHARING
 Chapter 17 CAPITATION, RATE SETTING, AND RISK SHARING NOTE: This chapter duplicates some of the material contained in Chapter 3 of this edition of Fundamentals of Healthcare Finance. However, it includes
Chapter 17 CAPITATION, RATE SETTING, AND RISK SHARING NOTE: This chapter duplicates some of the material contained in Chapter 3 of this edition of Fundamentals of Healthcare Finance. However, it includes
New payment models: Withholds
 I. Introduction Payment withholds are a long-standing type of risk arrangement. Under a withhold arrangement, the health plan retains or withholds a portion of the payments that are contractually due you
I. Introduction Payment withholds are a long-standing type of risk arrangement. Under a withhold arrangement, the health plan retains or withholds a portion of the payments that are contractually due you
Population-Based Healthcare: Structural Models and Options
 Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Population-Based Healthcare: Structural Models and Options George Choriatis, Esq. Rivkin Radler LLP Presented at: Annual Fall Meeting New York State Bar Association Health Law Section Albany, New York
Fee for Service: Paying for Volume, Not Value
 Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
Payment Reform 1 Fee for Service: Paying for Volume, Not Value Most healthcare services are reimbursed with a fee-for-service model. Pay regardless of quality, outcomes Pay for every test and procedure
APPENDIX. Methodology COST AND UTILIZATION 2018 REPORT MN Community Measurement. All Rights Reserved.
 APPENDIX Methodology COST AND UTILIZATION 2018 REPORT mncm.org mnhealthscores.org METHODOLOGY Calculation of Total Cost of Care, Relative Resources and Price Index The total cost of care metric is allowed
APPENDIX Methodology COST AND UTILIZATION 2018 REPORT mncm.org mnhealthscores.org METHODOLOGY Calculation of Total Cost of Care, Relative Resources and Price Index The total cost of care metric is allowed
Problems with Current Health Plans
 Problems with Current Health Plans Poor Integration, Coordination and Collaboration - Current plans offer limited coordination between the health plan, Providers, and the Members, as well as limited mobile
Problems with Current Health Plans Poor Integration, Coordination and Collaboration - Current plans offer limited coordination between the health plan, Providers, and the Members, as well as limited mobile
BlueOptions. Making the Important Choices Easier. floridablue.com. Enrollment Guide For Group Employees
 BlueOptions Enrollment Guide For Group Employees Making the Important Choices Easier. floridablue.com Health plan benefits Enrolling in your benefits When your employer offers Florida Blue benefits, we
BlueOptions Enrollment Guide For Group Employees Making the Important Choices Easier. floridablue.com Health plan benefits Enrolling in your benefits When your employer offers Florida Blue benefits, we
DHCFP. Provider Payment: Trends and Methods in the Massachusetts Health Care System
 DHCFP Provider Payment: Trends and Methods in the Massachusetts Health Care System Prepared by Allison Barrett and Timothy Lake, Mathematica Policy Research, Inc. February 2010 Deval L. Patrick, Governor
DHCFP Provider Payment: Trends and Methods in the Massachusetts Health Care System Prepared by Allison Barrett and Timothy Lake, Mathematica Policy Research, Inc. February 2010 Deval L. Patrick, Governor
Comprehensive Primary Care Payment Calculator User s Guide
 1 Comprehensive Primary Care Payment Calculator User s Guide Prepared by Health Data Decisions August 2017 Disclaimer: Information provided in connection with this calculator by FMAHealth and its contributors
1 Comprehensive Primary Care Payment Calculator User s Guide Prepared by Health Data Decisions August 2017 Disclaimer: Information provided in connection with this calculator by FMAHealth and its contributors
Health Plans Dashboard
 Health Plans Dashboard Q2 2015 Dashboard Summary Report A review of Inpatient, Outpatient and RX trends January 14, 2016 Prepared by HSS and Aon Hewitt Introduction This report completes the first phase
Health Plans Dashboard Q2 2015 Dashboard Summary Report A review of Inpatient, Outpatient and RX trends January 14, 2016 Prepared by HSS and Aon Hewitt Introduction This report completes the first phase
Total Cost of Care in Oregon s Commercial Market. February 24, 2017
 Total Cost of Care in Oregon s Commercial Market February 24, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary
Total Cost of Care in Oregon s Commercial Market February 24, 2017 Background: Q Corp About us Independent, nonprofit organization Neutral, multistakeholder collaboration Celebrated our 16 th anniversary
Health Care Coverage You Need. A Company You Know.
 Health Care Coverage You Need. A Company You Know. 2018 Call 800-477-2000, visit bcbsil.com or contact an independent, authorized agent to get a quote today. When It s Time to Get Health Care Coverage,
Health Care Coverage You Need. A Company You Know. 2018 Call 800-477-2000, visit bcbsil.com or contact an independent, authorized agent to get a quote today. When It s Time to Get Health Care Coverage,
Healthcare Financial Management Association Certification Program. Module I: The Business of Health Care Learner s Guide
 Healthcare Financial Management Association Certification Program Module I: The Business of Health Care Learner s Guide For examination period beginning June 2015 1 Course 1 - The Big Picture Learning
Healthcare Financial Management Association Certification Program Module I: The Business of Health Care Learner s Guide For examination period beginning June 2015 1 Course 1 - The Big Picture Learning
Health Care Coverage You Need. A Company You Know.
 Health Care Coverage You Need. A Company You Know. 2018 Call 855-593-1515, visit www.bcbsmt.com or contact an independent, authorized agent to get a quote today. When It s Time to Get Health Care Coverage,
Health Care Coverage You Need. A Company You Know. 2018 Call 855-593-1515, visit www.bcbsmt.com or contact an independent, authorized agent to get a quote today. When It s Time to Get Health Care Coverage,
 Page 1 of 8 January 25, 2011 It's (somewhat) about the money (Part 2) By Alan S Gassman, JD, LLM,Frederic R. Simmons Jr., CPME, CPA New healthcare delivery systems: Arm yourself with negotiating power
Page 1 of 8 January 25, 2011 It's (somewhat) about the money (Part 2) By Alan S Gassman, JD, LLM,Frederic R. Simmons Jr., CPME, CPA New healthcare delivery systems: Arm yourself with negotiating power
2017 EMPLOYER SERIES. 6 Things Employers Need to Know About Rising Health Care Costs. Cost Management Key Findings
 2017 EMPLOYER SERIES 6 Things Employers Need to Know About Rising Health Care Costs Cost Management 2017 Key Findings It s one of the biggest challenges employers face today: keeping health care costs
2017 EMPLOYER SERIES 6 Things Employers Need to Know About Rising Health Care Costs Cost Management 2017 Key Findings It s one of the biggest challenges employers face today: keeping health care costs
Value-Based Payment Study
 Value-Based Payment Study Page 2 of 133 Value Based Payment Survey TABLE OF CONTENTS EXECUTIVE SUMMARY... 4 METHODOLOGY... 5 DETAILED FINDINGS... 7 Staff at Primary Location... 7 /Health Plans Received
Value-Based Payment Study Page 2 of 133 Value Based Payment Survey TABLE OF CONTENTS EXECUTIVE SUMMARY... 4 METHODOLOGY... 5 DETAILED FINDINGS... 7 Staff at Primary Location... 7 /Health Plans Received
Glossary. Adults: Individuals ages 19 through 64. Allowed amounts: See prices paid. Allowed costs: See prices paid.
 Glossary Acute inpatient: A subservice category of the inpatient facility clams that have excluded skilled nursing facilities (SNF), hospice, and ungroupable claims. This subcategory was previously known
Glossary Acute inpatient: A subservice category of the inpatient facility clams that have excluded skilled nursing facilities (SNF), hospice, and ungroupable claims. This subcategory was previously known
INFORMATION ABOUT YOUR OXFORD COVERAGE
 OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
Health Care Coverage You Need. A Company You Know.
 Health Care Coverage You Need. A Company You Know. 2018 Call 800-531-4456, visit bcbstx.com or contact an independent, authorized agent to get a quote today. When It s Time to Get Health Care Coverage,
Health Care Coverage You Need. A Company You Know. 2018 Call 800-531-4456, visit bcbstx.com or contact an independent, authorized agent to get a quote today. When It s Time to Get Health Care Coverage,
Article from. Predictive Analytics and Futurism. June 2017 Issue 15
 Article from Predictive Analytics and Futurism June 2017 Issue 15 Using Predictive Modeling to Risk- Adjust Primary Care Panel Sizes By Anders Larson Most health actuaries are familiar with the concept
Article from Predictive Analytics and Futurism June 2017 Issue 15 Using Predictive Modeling to Risk- Adjust Primary Care Panel Sizes By Anders Larson Most health actuaries are familiar with the concept
How ACO s Can Impact Contracting A Real World Example. Mike Medel Pharm D, MBA Banner Health
 How ACO s Can Impact Contracting A Real World Example Mike Medel Pharm D, MBA Banner Health Agenda Banner Pharmacy Services Introduction Accountable Care Organization Summary Basic Constructs of ACO Partnership
How ACO s Can Impact Contracting A Real World Example Mike Medel Pharm D, MBA Banner Health Agenda Banner Pharmacy Services Introduction Accountable Care Organization Summary Basic Constructs of ACO Partnership
Hospital Payment Reform Summit
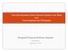 How Risk-Adjusted Global Payment Systems Can Work and How Hospitals Can Participate Experience with the Patient Choice System Hospital Payment Reform Summit Ann Robinow September 16, 2009 Patient Choice
How Risk-Adjusted Global Payment Systems Can Work and How Hospitals Can Participate Experience with the Patient Choice System Hospital Payment Reform Summit Ann Robinow September 16, 2009 Patient Choice
Milliman RBRVS for Hospitals
 Milliman RBRVS for Hospitals Will Fox, FSA, MAAA Ed Jhu, FSA, MAAA Charlie Mills, FSA, MAAA Kevin Frodsham, ASA, MAAA What is RBRVS for Hospitals? The Milliman RBRVS for Hospitals Fee Schedule provides
Milliman RBRVS for Hospitals Will Fox, FSA, MAAA Ed Jhu, FSA, MAAA Charlie Mills, FSA, MAAA Kevin Frodsham, ASA, MAAA What is RBRVS for Hospitals? The Milliman RBRVS for Hospitals Fee Schedule provides
CARECOUNSEL TIPS SELECTING A HEALTH PLAN. Step 1: Gather Basic Information. Step 2: Assess Your Needs
 SELECTING A HEALTH PLAN Choosing between health plans is no longer a simple matter. As a healthcare consumer, it s important that you educate yourself about the various health plans available to you. You
SELECTING A HEALTH PLAN Choosing between health plans is no longer a simple matter. As a healthcare consumer, it s important that you educate yourself about the various health plans available to you. You
National APM Data Collection Frequently Asked Questions for 2018
 National APM Data Collection Frequently Asked Questions for 2018 Last updated on 1/25/18 Please note this document may be updated and improved periodically based on feedback from health plans and other
National APM Data Collection Frequently Asked Questions for 2018 Last updated on 1/25/18 Please note this document may be updated and improved periodically based on feedback from health plans and other
Approved Models to Align Incentives between Hospitals and their Physicians
 Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
Following is a list of common health insurance terms and definitions*.
 Health Terms Glossary Following is a list of common health insurance terms and definitions*. Ambulatory Care Health services delivered on an outpatient basis. A patient's treatment at a doctor's office
Health Terms Glossary Following is a list of common health insurance terms and definitions*. Ambulatory Care Health services delivered on an outpatient basis. A patient's treatment at a doctor's office
Reinsurance Section News
 Article from: Reinsurance Section News May 2006 Issue 57 MANAGED CARE UPDATE by Mark Troutman [Portions of this article were reprinted with permission from Contingencies magazine] Introduction This article
Article from: Reinsurance Section News May 2006 Issue 57 MANAGED CARE UPDATE by Mark Troutman [Portions of this article were reprinted with permission from Contingencies magazine] Introduction This article
Presented by: Steven Flores. Prepared for: The Predictive Modeling Summit
 Presented by: Steven Flores Prepared for: The Predictive Modeling Summit November 13, 2014 Disease Management Introduction A multidisciplinary, systematic approach to health care delivery that: Includes
Presented by: Steven Flores Prepared for: The Predictive Modeling Summit November 13, 2014 Disease Management Introduction A multidisciplinary, systematic approach to health care delivery that: Includes
Milliman Healthcare Services
 Milliman Healthcare Services Milliman Introduction About Milliman Milliman is the leader in providing actuarial consulting services to the health industry. We also develop and maintain sophisticated healthcare
Milliman Healthcare Services Milliman Introduction About Milliman Milliman is the leader in providing actuarial consulting services to the health industry. We also develop and maintain sophisticated healthcare
PROVIDER SERVICES Section IV Provider Services
 Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Section IV Provider Services Provider Services 98 NaviNet www.navinet.net Using NaviNet reduces the time spent on paperwork and allows you to focus on more important tasks patient care. NaviNet is a one-stop
Get the Right Coverage
 Get the Right Coverage Call 855-381-1212, visit bcbstx.com or contact an independent Blue Cross and Blue Shield of Texas agent to get a quote today. 2016 Life is Full of Important Choices Some choices
Get the Right Coverage Call 855-381-1212, visit bcbstx.com or contact an independent Blue Cross and Blue Shield of Texas agent to get a quote today. 2016 Life is Full of Important Choices Some choices
Overview of Reimbursement Strategies for Novel Medical Technologies
 Overview of Reimbursement Strategies for Novel Medical Technologies Nov 9, 2016 Goals and Objectives Develop understanding of U.S. medical technology reimbursement landscape and provide information about
Overview of Reimbursement Strategies for Novel Medical Technologies Nov 9, 2016 Goals and Objectives Develop understanding of U.S. medical technology reimbursement landscape and provide information about
The Physician-Owned Management Services Organization
 The Physician-Owned Management Services Organization By Joe Laden www.onemso.com/consulting A Management Services Organization (MSO) is a legal entity created to provide management and administrative services
The Physician-Owned Management Services Organization By Joe Laden www.onemso.com/consulting A Management Services Organization (MSO) is a legal entity created to provide management and administrative services
RE: Additional Input regarding Accountable Care Organizations (ACOs) and the Medicare Shared Saving Program
 221 MAIN STREET, SUITE 1500 SAN FRANCISCO, CA 94105 PBGH.ORG OFFICE 415.281.8660 FACSIMILE 415.520.0927 February 14, 2011 Donald M. Berwick, M.D. Administrator Centers for Medicare and Medicaid Services
221 MAIN STREET, SUITE 1500 SAN FRANCISCO, CA 94105 PBGH.ORG OFFICE 415.281.8660 FACSIMILE 415.520.0927 February 14, 2011 Donald M. Berwick, M.D. Administrator Centers for Medicare and Medicaid Services
Clinical Integration:
 Clinical Integration: The First Step in Moving Toward Value-Based Reimbursement ELLIS MAC KNIGHT, MD, MBA Senior Vice President/CMO November 2018 CONTACT For further information about Coker Group and how
Clinical Integration: The First Step in Moving Toward Value-Based Reimbursement ELLIS MAC KNIGHT, MD, MBA Senior Vice President/CMO November 2018 CONTACT For further information about Coker Group and how
Information About Your Oxford Coverage
 Information About Your Oxford Coverage Overview of provider reimbursement methodologies Generally, we pay participating providers ("network providers") on a fee-for-service basis. Feefor-service based
Information About Your Oxford Coverage Overview of provider reimbursement methodologies Generally, we pay participating providers ("network providers") on a fee-for-service basis. Feefor-service based
Inside: Critical information about your company s prescription drug benefit.
 Inside: Critical information about your company s prescription drug benefit. Questions Company Benefits Managers Must Ask Their PBM It pays to make an informed decision harmacy Benefit Managers, often
Inside: Critical information about your company s prescription drug benefit. Questions Company Benefits Managers Must Ask Their PBM It pays to make an informed decision harmacy Benefit Managers, often
APPLICATION BY BLUECROSS BLUESHIELD OF WESTERN NEW YORK TO THE NEW YORK STATE DEPARTMENT OF FINANCIAL SERVICES FOR A PREMIUM ADJUSTMENT
 1. Introduction. APPLICATION BY BLUECROSS BLUESHIELD OF WESTERN NEW YORK TO THE NEW YORK STATE DEPARTMENT OF FINANCIAL SERVICES FOR A PREMIUM ADJUSTMENT NAIC #: 55204 SERFF Tracking #: HLTH 129082986 TO
1. Introduction. APPLICATION BY BLUECROSS BLUESHIELD OF WESTERN NEW YORK TO THE NEW YORK STATE DEPARTMENT OF FINANCIAL SERVICES FOR A PREMIUM ADJUSTMENT NAIC #: 55204 SERFF Tracking #: HLTH 129082986 TO
What is Group Medicare Advantage PPO?
 What is Group Medicare Advantage PPO? Current Group Medicare Advantage HMO Group Medicare Advantage PPO Value to Medicare eligible retirees Geographic availability Defined Service Area Only 22 counties
What is Group Medicare Advantage PPO? Current Group Medicare Advantage HMO Group Medicare Advantage PPO Value to Medicare eligible retirees Geographic availability Defined Service Area Only 22 counties
Land of Lincoln Health : LAND OF LINCOLN PREFERRED PPO GOLD Coverage Period: 01/01/ /31/2015
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.landoflincolnhealth.org or by calling 1-844-674-3834.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.landoflincolnhealth.org or by calling 1-844-674-3834.
Valuation of Alternative Payment Models
 Valuation of Alternative Payment Models No portion of this white paper may be used or duplicated by any person or entity for any purpose without the express written permission of PYA. I. Introduction:
Valuation of Alternative Payment Models No portion of this white paper may be used or duplicated by any person or entity for any purpose without the express written permission of PYA. I. Introduction:
Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Coverage Period: 08/01/ /31/2016
 Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 08/01/2015-07/31/2016
Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 08/01/2015-07/31/2016
for Individuals and Families LIVE LIFE ASSURED
 for Individuals and Families LIVE LIFE ASSURED Options as unique as you Coverage that s all yours Health Tradition for Individuals is designed for people who may not have access to a group or employer
for Individuals and Families LIVE LIFE ASSURED Options as unique as you Coverage that s all yours Health Tradition for Individuals is designed for people who may not have access to a group or employer
Figure 1: Original APM Framework
 Contents Overview... 2 This Year s APM Measurement Effort... 3 Scope... 3 Data Source... 4 The LAN Survey... 4 The Blue Cross Blue Shield Association Survey... 8 The America s Health Insurance Plans Survey...
Contents Overview... 2 This Year s APM Measurement Effort... 3 Scope... 3 Data Source... 4 The LAN Survey... 4 The Blue Cross Blue Shield Association Survey... 8 The America s Health Insurance Plans Survey...
Super Blue Plus QHDHP 1 HDHP Non Emb 100%
 Super Blue Plus QHDHP 1 HDHP Non Emb 100% Effective Date December 1, 2018 Benefit Period 2 (used for Deductible and Coinsurances limits and certain Contract Year benefit frequencies.) Note: All Services
Super Blue Plus QHDHP 1 HDHP Non Emb 100% Effective Date December 1, 2018 Benefit Period 2 (used for Deductible and Coinsurances limits and certain Contract Year benefit frequencies.) Note: All Services
The Challenge of Implementing Interoperable Electronic Medical Records
 Annals of Health Law Volume 19 Issue 1 Special Edition 2010 Article 37 2010 The Challenge of Implementing Interoperable Electronic Medical Records James C. Dechene Follow this and additional works at:
Annals of Health Law Volume 19 Issue 1 Special Edition 2010 Article 37 2010 The Challenge of Implementing Interoperable Electronic Medical Records James C. Dechene Follow this and additional works at:
Provider Payment. Jones & Bartlett Learning, LLC NOT FOR SALE OR DISTRIBUTION
 & CHAPTER 5 Provider Payment CHAPTER STUDY REVIEW Bartlett Learning, 1. It s Not LLC Reimbursement. It s Payment. Reimbursement: - It s what you get when you submit your travel expenses to your employer
& CHAPTER 5 Provider Payment CHAPTER STUDY REVIEW Bartlett Learning, 1. It s Not LLC Reimbursement. It s Payment. Reimbursement: - It s what you get when you submit your travel expenses to your employer
Session 84 PD, Predictive Analytics for Actuaries: A look At Case Studies in Healthcare Analytics. Moderator: Carol J.
 Session 84 PD, Predictive Analytics for Actuaries: A look At Case Studies in Healthcare Analytics Moderator: Carol J. McCall, FSA, MAAA Presenters: Lillian Louise Dittrick, FSA, MAAA Wu-Chyuan (Gary) Gau,
Session 84 PD, Predictive Analytics for Actuaries: A look At Case Studies in Healthcare Analytics Moderator: Carol J. McCall, FSA, MAAA Presenters: Lillian Louise Dittrick, FSA, MAAA Wu-Chyuan (Gary) Gau,
FMV Considerations for Bundled Payment Arrangements
 FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
Kaiser Family Foundation, Assessing Americans Familiarity with Health Insurance Terms and Concepts Appendix Tables
 Kaiser Family Foundation, Assessing Americans Familiarity with Health Insurance Terms and Concepts Appendix Tables Total Insurance Status Age Gender Education Level Insured (age 18-64) Uninsured (age 18-64)
Kaiser Family Foundation, Assessing Americans Familiarity with Health Insurance Terms and Concepts Appendix Tables Total Insurance Status Age Gender Education Level Insured (age 18-64) Uninsured (age 18-64)
Facility editing: Enhance payment integrity while building strong provider relationships
 Facility editing: Enhance payment integrity while building strong provider relationships Optum www.optuminsight.com Page 1 Five steps toward effective facility editing It is a real challenge to edit facility
Facility editing: Enhance payment integrity while building strong provider relationships Optum www.optuminsight.com Page 1 Five steps toward effective facility editing It is a real challenge to edit facility
CS VEBA 2016 UnitedHealthcare Medicare Advantage PPO Plan
 CS VEBA 2016 UnitedHealthcare Medicare Advantage PPO Plan Replaced Senior Supplement Plan in 2016 UnitedHealthcare Group Medicare Advantage (PPO) plan. Also known as a Medicare Part C, this plan offers
CS VEBA 2016 UnitedHealthcare Medicare Advantage PPO Plan Replaced Senior Supplement Plan in 2016 UnitedHealthcare Group Medicare Advantage (PPO) plan. Also known as a Medicare Part C, this plan offers
Re: Comments on proposed rule for the Medicare Shared Savings Program: Accountable Care Organizations
 June 6, 2011 Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1345-P PO Box 8013 Baltimore, MD 21244-8013 Re: Comments on proposed rule for the Medicare Shared
June 6, 2011 Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1345-P PO Box 8013 Baltimore, MD 21244-8013 Re: Comments on proposed rule for the Medicare Shared
If you enroll through the GPA hosted PSBP website, Health Net will automatically assign you to a PCP.
 MEDICAL INSURANCE What is an HMO Plan? One of the main components of an HMO that distinguishes the model from other types of plans is the Primary Care Physician who acts as your gatekeeper for all of your
MEDICAL INSURANCE What is an HMO Plan? One of the main components of an HMO that distinguishes the model from other types of plans is the Primary Care Physician who acts as your gatekeeper for all of your
for Employer Groups LIVE LIFE ASSURED
 for Employer Groups LIVE LIFE ASSURED 1 Live life assured Together, creating better health and better health care consumers Successfully providing excellent health benefits costeffectively requires a partner
for Employer Groups LIVE LIFE ASSURED 1 Live life assured Together, creating better health and better health care consumers Successfully providing excellent health benefits costeffectively requires a partner
Important Questions Answers Why this Matters: For In-Network Providers $0 Individual/ $0 Family For Out-of-Network Providers
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
ERM , Getzen Economics and Financing (Sec. 5.4, 5.5)
 ERM 512-13, Getzen (Sec. 5.4, 5.5) 1/17 Key Points Types of Managed Care Plans Ways to Reduce Costs Features of Managed Care Utilization Review 2/17 Managed Care Plans Why Managed Care? Primary reason
ERM 512-13, Getzen (Sec. 5.4, 5.5) 1/17 Key Points Types of Managed Care Plans Ways to Reduce Costs Features of Managed Care Utilization Review 2/17 Managed Care Plans Why Managed Care? Primary reason
CONSULTING FOR INSURANCE BROKERS AND SELF-FUNDED GROUPS
 CONSULTING FOR INSURANCE BROKERS AND SELF-FUNDED GROUPS Axene Health Partners (AHP) has extensive experience across the entire healthcare system, and our expertise can help entities of every size better
CONSULTING FOR INSURANCE BROKERS AND SELF-FUNDED GROUPS Axene Health Partners (AHP) has extensive experience across the entire healthcare system, and our expertise can help entities of every size better
HEALTH INSURANCE 101. Finding the Right Plan
 HEALTH INSURANCE 101 Finding the Right Plan HEALTH CARE 101: FINDING THE RIGHT PLAN Introduction... 2 Common Health Insurance Terms and Definitions... 3 Health Care Reform: What You Need to Know... 7 Important
HEALTH INSURANCE 101 Finding the Right Plan HEALTH CARE 101: FINDING THE RIGHT PLAN Introduction... 2 Common Health Insurance Terms and Definitions... 3 Health Care Reform: What You Need to Know... 7 Important
Prior to getting your Medicaid or health coverage through the marketplace, would you have been able to access and/or afford this care?
 Exhibit 1 Three of Five Adults with Marketplace or Medicaid Coverage Who Had Used Their Plan Said They Would Not Have Been Able to Access or Afford This Care Before Prior to getting your Medicaid or health
Exhibit 1 Three of Five Adults with Marketplace or Medicaid Coverage Who Had Used Their Plan Said They Would Not Have Been Able to Access or Afford This Care Before Prior to getting your Medicaid or health
Let us help you choose the health insurance plan that fits you best
 Let us help you choose the health insurance plan that fits you best Call 800-531-4456, visit bcbstx.com or contact an independent Blue Cross and Blue Shield of Texas agent to get a quote today. Life is
Let us help you choose the health insurance plan that fits you best Call 800-531-4456, visit bcbstx.com or contact an independent Blue Cross and Blue Shield of Texas agent to get a quote today. Life is
Highmark Delaware: Shared Cost Blue EPO 1000 Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbsde.com or by calling 1-888-601-2242. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbsde.com or by calling 1-888-601-2242. Important
Employer Health Insurance
 Employer Health Insurance PRODUCT GUIDE 2016 PLANS FOR EMPLOYERS WITH 1-50 EMPLOYEES 1 AND 51-99 EMPLOYEES 2 1 These plans are offered to employers considered small for purposes of the Affordable Care
Employer Health Insurance PRODUCT GUIDE 2016 PLANS FOR EMPLOYERS WITH 1-50 EMPLOYEES 1 AND 51-99 EMPLOYEES 2 1 These plans are offered to employers considered small for purposes of the Affordable Care
Annual Notice of Changes for 2017
 WellCare Value (HMO-POS) offered by WellCare Health Insurance Company of Kentucky, Inc. Annual Notice of Changes for 2017 You are currently enrolled as a member of WellCare Value (HMO-POS). Next year,
WellCare Value (HMO-POS) offered by WellCare Health Insurance Company of Kentucky, Inc. Annual Notice of Changes for 2017 You are currently enrolled as a member of WellCare Value (HMO-POS). Next year,
All About APMs: What Will It Take for Physicians to Earn the APM Bonus Under MACRA?
 All About APMs: What Will It Take for Physicians to Earn the APM Bonus Under MACRA? By Robert F. Atlas, David B. Tatge, and Lesley R. Yeung June 2016 On May 9, 2016, the Centers for Medicare & Medicaid
All About APMs: What Will It Take for Physicians to Earn the APM Bonus Under MACRA? By Robert F. Atlas, David B. Tatge, and Lesley R. Yeung June 2016 On May 9, 2016, the Centers for Medicare & Medicaid
Antitrust Rules for Provider Collaboration: How to Form and Operate a Network of Competing Providers
 Antitrust Rules for Provider Collaboration: How to Form and Operate a Network of Competing Providers By Mitchell D. Raup, Shareholder, Polsinelli PC, Washington DC I. Introduction: A. Many forms of provider
Antitrust Rules for Provider Collaboration: How to Form and Operate a Network of Competing Providers By Mitchell D. Raup, Shareholder, Polsinelli PC, Washington DC I. Introduction: A. Many forms of provider
Assurant Clarity SM. Questions about your plan? Benefits Guide. Time Insurance Company John Alden Life Insurance Company. Finally, Original Thinking
 Assurant Clarity SM Benefits Guide Finally, Original Thinking Questions about your plan? Call your Front Desk team at 888.345.6007 Time Insurance Company John Alden Life Insurance Company Assurant Health
Assurant Clarity SM Benefits Guide Finally, Original Thinking Questions about your plan? Call your Front Desk team at 888.345.6007 Time Insurance Company John Alden Life Insurance Company Assurant Health
for Employer Groups 2018
 for Employer Groups 2018 LIVE LIFE ASSURED 1 Excellent coverage with Mayo Clinic care. That s the Health Tradition difference. A powerful partnership creates a valuable benefit for your workforce We understand
for Employer Groups 2018 LIVE LIFE ASSURED 1 Excellent coverage with Mayo Clinic care. That s the Health Tradition difference. A powerful partnership creates a valuable benefit for your workforce We understand
Growth and Success of Accountable Care Organizations (ACOs) in the US from Dennis Horrigan June 2016
 Growth and Success of Accountable Care Organizations (ACOs) in the US from 2010-2016 Dennis Horrigan June 2016 Introducing Dennis Horrigan Dennis R. Horrigan President and Chief Executive Officer Catholic
Growth and Success of Accountable Care Organizations (ACOs) in the US from 2010-2016 Dennis Horrigan June 2016 Introducing Dennis Horrigan Dennis R. Horrigan President and Chief Executive Officer Catholic
December 2009 Report No
 December 2009 Report No. 09-40 University Students Pay $68 Million for Health Services; Mandating Health Insurance Would Produce Benefits But Raise Uninsured Students Cost of Attendance 5% to 7% at a glance
December 2009 Report No. 09-40 University Students Pay $68 Million for Health Services; Mandating Health Insurance Would Produce Benefits But Raise Uninsured Students Cost of Attendance 5% to 7% at a glance
Benefits Education Session. New Team Member Experience
 Benefits Education Session New Team Member Experience Today s Objectives Review Key New Hire Enrollment Information Review Benefits Overview and Considerations Share Resources and Answer Questions New
Benefits Education Session New Team Member Experience Today s Objectives Review Key New Hire Enrollment Information Review Benefits Overview and Considerations Share Resources and Answer Questions New
Advancing Healthcare Crowe Healthcare Summit 2017 RCA Optimization: Keys to Interpreting Net Revenue
 Advancing Healthcare Crowe Healthcare Summit 2017 RCA Optimization: Keys to Interpreting Net Revenue September 19, 2017 Bryan Rector, CNRA, CPA Megan Beasley, RHIA, CPMA, CPC Smart decisions. Lasting value.
Advancing Healthcare Crowe Healthcare Summit 2017 RCA Optimization: Keys to Interpreting Net Revenue September 19, 2017 Bryan Rector, CNRA, CPA Megan Beasley, RHIA, CPMA, CPC Smart decisions. Lasting value.
You must pay all of the costs for these services up to the specific deductible amount before this plan begins to pay for these services.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
HMO Louisiana, Inc.: Blue POS copay 80/60 $500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-495-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-495-2583. Important Questions
Effectiveness of WC Fee Schedules A Closer Look
 NCCI RESEARCH BRIEF February 2009 By Barry Lipton, Dan Corro, Natasha Moore and John Robertson Effectiveness of WC Fee Schedules A Closer Look Executive Summary This brief summarizes findings from a study
NCCI RESEARCH BRIEF February 2009 By Barry Lipton, Dan Corro, Natasha Moore and John Robertson Effectiveness of WC Fee Schedules A Closer Look Executive Summary This brief summarizes findings from a study
Pay For Performance Summit Ann Robinow March 10, 2009
 Pay For Performance Summit Ann Robinow March 10, 2009 1 Force providers to manage cost and improve quality Give consumers incentives and tools to migrate to better performing providers Do this without
Pay For Performance Summit Ann Robinow March 10, 2009 1 Force providers to manage cost and improve quality Give consumers incentives and tools to migrate to better performing providers Do this without
Cummins Central Power, LLC Coverage Period: 05/01/ /30/2015
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Health Information Technology and Management
 Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
Health Information Technology and Management CHAPTER 9 Healthcare Coding and Reimbursement Pretest (True/False) CPT-4 codes are used to bill for disease and illness. Medicare Part B provides medical insurance
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business?
 Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
