Hancock, et al. ORGANIZATION bill analysis 5/8/2009 (CSHB 2256 by Hancock) Mediation of out-of-network health benefit claim disputes
|
|
|
- Sara Walton
- 6 years ago
- Views:
Transcription
1 HOUSE HB 2256 RESEARCH Hancock, et al. ORGANIZATION bill analysis 5/8/2009 (CSHB 2256 by Hancock) SUBJECT: COMMITTEE: VOTE: Mediation of out-of-network health benefit claim disputes Insurance committee substitute recommended 8 ayes Smithee, Martinez Fischer, Eiland, Hancock, Hunter, Isett, Taylor, Thompson 0 nays 1 absent Deshotel WITNESSES: For Jerry Stamps, North Richland Hills Baptist Against Patrick Giam, Greater Houston Anesthesiology, P.A.; Michael Hicks, Pinnacle Partners in Medicine, P.A.; William Hinchey, Texas Medical Association; Jeff Jekot, Texas Society of Anesthesiologists; Greg Karnaze, Texas Radiological Society, Austin Radiological Association; Sam Roberts, Texas College of Emergency Physicians; William Schlotter, Capitol Anesthesiology Association, Texas Medical Group Management; Ezequiel Silva, Texas Radiological Society, South Texas Radiology Group; Michael Stanley, Pediatrix Medical Group Texas; Susan Strate, Texas Society of Pathologists; Dan Stultz, Texas Hospital Association; Jared Wolfe, Texas Association of Health Plans; (Registered, but did not testify: Susan Baer, Clinical Pathology Associates, P.A.; Ronald Booker, Greater Houston Anesthesiology, P.A.; Cheryl Conner, Emergency Service Partners; Robert Connor; David Marwitz, Texas Dermatalogical Society; Joe Monk, Texas Society of Anesthesiologists; Jaime Ronderos, Pinnacle Partners in Medicine; Mark Silberman, Clinical Pathology Associates) On (Registered, but did not testify: Jay Thompson, Texas Association of Life and Health Insurers) BACKGROUND: A preferred provider benefit plan may reimburse health care providers in the plan s preferred provider network at a different rate than the plan reimburses out-of-network health care providers. Health benefits for state of Texas employees may be provided through a health maintenance organization (HMO) or through an arrangement in which patients pay different rates for in-network and out-of-network providers.
2 page 2 DIGEST: CSHB 2256 would allow enrollees of preferred provider benefit plans or of a Texas employee health benefit plan that was not an HMO to request mediation of an out-of-network claim settlement if: the amount for which the enrollee was responsible for payment to a facility-based physician after copayments, deductibles, and coinsurance was greater than $500; and the facility-based physician provided the service in a preferred provider hospital or a hospital that contracted with the health plan administrator. Facility-based physicians would include anesthesiologists, pathologists, radiologists, emergency physicians, or neonatologists that provided services to patients in a facility under which they had been granted clinical privileges. A facility-based physician would not be required to mediate an enrollee s billed charge if the patient had signed a disclosure from the physician that explained the amounts for which the enrollee could be responsible. Participation in mediation. Both the insurer and facility-based physician would be required to participate in the mediation if this signed disclosure had not been obtained. The insurer or physician could be issued an administrative penalty for bad faith mediation, which would be constituted by behaviors such as failing to participate in the mediation or provide certain information to the mediator. The enrollee or enrollee s representative would not have to participate in the teleconference or mediation for mediation to proceed. Dispute resolution procedures. The bill would define the process by which the enrollee would request mediation from the Texas Department of Insurance (TDI) and how the insurer and physician would be notified of the request. The facility-based physician could not pursue collection of the bill once request for mediation was received. The parties to the mediation would be required to participate in an informal settlement teleconference to attempt to settle the dispute before mediation. If the teleconference was not successful, mediation would proceed by consent of the enrollee.
3 page 3 The mediation would be conducted by a mediator agreed upon by all parties or appointed by the chief administrative law judge by random assignment. A mediation could not exceed four hours unless agreed upon by all parties. Each party would have the opportunity to state the party s position. The mediation would consider whether: the amount charged by the facility-based physician was excessive; the amount paid by the insurer for the service was the usual and customary rate or was unreasonably low; or the amount for which the enrollee would be responsible would be excessive. If the mediation was not successful, the chief administrative law judge would refer the matter for trial by a special judge. The parties would pay a proportionate share of the special judge s fee. The special judge s verdict would proceed according to the established procedures of Civil Practice and Remedies Code, ch The mediator would prepare a confidential mediation agreement and order that stated the total amount for which the enrollee would be responsible to pay the facility-based physician and any agreements made between the insurer and physician. Additional remedies. The remedies provided by this bill would be in addition to any other defense, remedy, or procedure provided by law. The enrollee could file a complaint with the Texas Medical Board for improper billing or with TDI for unfair claim settlement practices. These entities would adopt rules regulating investigation and review of complaints related to settlement of an out-of-network health benefit claim. TDI and the Texas Medical Board would maintain information on each of these complaints, on any related mediation, and on the claim upon which the complaint was based. Insurer requirements. The insurance commissioner would adopt rules for network adequacy standards adapted to local markets in which a preferred provider benefit plan operated. An insurer would submit to TDI the methods by which the insurer computed out-of-network reimbursements under preferred provider benefit plans and the effect these methods had on the insureds out-of-pocket costs.
4 page 4 Provider disclosures. A facility-based physician who provided services out-of-network to an insured would have to notify the patient of the mandatory mediation process. A health care facility would provide to patients a contact list of all facility-based physicians with privileges at the facility and would inform patients that these physicians could bill them for amounts not paid by their insurer. The bill would take immediate effect if finally passed by a two-thirds record vote of the membership of each house. Otherwise, it would take effect September 1, The bill only would apply to health benefit claims filed on or after this effective date. SUPPORTERS SAY: CSHB 2256 would provide health insurance consumers recourse to dispute balance billing practices by establishing a mediation process in which patients, insurers, and health care providers could agree upon fair payment of certain out-of-network medical charges. Insurers often set a maximum allowable cost for out-of-network medical services. They calculate the amount of coinsurance that the patient would owe for the out-of-network procedure based on the maximum allowable cost. When the amount charged by an out-of-network provider exceeds the maximum allowable cost, the patient is balance billed for this difference in addition to paying coinsurance. This can leave patients with unexpectedly high medical bills and no recourse. Insurers will claim providers have charged too much while providers will claim insurers underpaid for their services. CSHB 2256 would allow health consumers to initiate a mediation process when their out-of-network charges exceeded $500. There are many instances in which consumers have tried to avoid out-of-network services but have been balance-billed despite their efforts. For example, a patient could see an in-network surgeon for a procedure but the facility could schedule an out-of-network anesthesiologist to attend the surgery. Further, patients diligently could check that all services they were to receive would be performed by an in-network specialist, but unbeknownst to patients, their lab results could be sent for review by an out-of-network practitioner. Patients also may be harmed by balanced billing due to the practices of the insurer or provider. Some providers intentionally avoid contracting with any health plans yet accept positions with busy health care facilities so that they are assured referrals through which they can bill high service charges
5 page 5 because every patient they see will be out-of-network. In addition, many insurers set the maximum allowable cost they use to calculate payment for out-of-network services much lower than the amount they have negotiated to pay in-network service providers. This can make insurer reimbursement rates artificially low for out-of-network providers, which shifts more costs to the health consumer. The mediation option established by CSHB 2256 would provide the most fair and effective resolution for balance billing issues for all parties. It would require the participation of the insurer and provider so the charges billed by the provider as well as the amount reimbursed by the insurer could be reviewed and subject to negotiation. The $500 threshold that a patient s out-of-network charges must exceed to initiate mediation would ensure the parties were not drawn into mediation for charges that did not impose an unreasonable burden on a consumer. There would be several points during the conflict resolution process at which an agreement could be reached. The parties would have an incentive to negotiate because the sooner in the process that an agreement was reached, the less costs would be incurred by the mediation participants. The bill would establish other consumer protections standards. DSHS would be required to establish provider network adequacy standards for state employee health plans and preferred provider organizations. This would decrease the likelihood that a consumer was forced to see an out-ofnetwork provider and could incur higher medical bills. The standards would be adapted to the unique local health care market so insurers would not be required to meet unreasonable standards for participating providers if they were in a smaller market. Further consumer protections would include the requirement that preferred provider benefit plans would have to provide TDI information regarding the methods used to compute out-of-network reimbursements such as maximum allowable amounts. Patients also would receive lists of out-ofnetwork doctors when they were admitted to a hospital. Consumers still could go through their insurer s grievance process and could file complaints against insurers with TDI and against health care providers with the Texas Medical Board. Being able to pursue a complaint with the Texas Medical Board in addition to engaging in the mediation process would be critical, because certain medical practitioners deserve further reprimand for charging exorbitant fees.
6 page 6 Other alternatives to address billing issues would not be as effective or appropriate as the mediation process in CSHB Facilities and physicians already are required to provide estimates of charges for certain non-emergency procedures upon request by a patient. Any more extensive transparency requirements, such as requirements for providers to post their service charges, could lead more providers to increase their charges to amounts they recognize other providers have been able to obtain for the same services. Imposing further regulations on health insurers regarding how much they must reimburse out-of-network providers would put insurers at a competitive disadvantage in negotiating contracts with potential network providers. OPPONENTS SAY: CSHB 2256 should not require providers and insurers to engage in a mediation process initiated by a consumer regarding balanced billing concerns. The consumer would have nothing at stake in requesting expensive mediation regarding any eligible out-of-network charges they were billed because the insurer and provider would split the cost of the mediation process and the consumer would have no penalty for failing to attend the mediation. This mediation process would cost time and money to insurers and providers when it is possible that neither of these parties acted inappropriately with respect to the patient s claim. A better approach to consumer balance billing issues would be to target policies to curb inappropriate practices engaged in by either the insurer or provider. Often doctors will charge the insured significantly lower amounts than they charge to out-of-network patients. Lower charges to those with health insurance are justified by the discounts insurers can obtain from the quantity of business insurers provide to doctors. If a health consumer truly has been overbilled or excessively charged by a provider, other approaches would be preferable to mediation. If health pricing were made more transparent by requirements that health providers make public the prices they charge for services, consumers could research more effectively the amounts they would be charged by out-of-network providers. In addition, patients currently may file a complaint with the Texas Medical Board against any doctor that the patient felt was price gouging. The board can and has sanctioned physicians for excessive charges. Revisions could be made to insurer practice as well. Insurers should be required to calculate the enrollee s coinsurance owed for an out-ofnetwork service based on the amount charged by the provider and not based on the maximum allowable cost established by the insurer. This
7 page 7 would reduce the consumer s share of costs. Consumers are led to believe they pay more for their premiums in a preferred provider organization to get out-of-network coverage and that these higher premiums would reduce their long-term, out-of-pocket costs. Requirements also should be instituted for the timeframe in which insurers must update changes to their list of in-network providers. Preferred provider organizations never should charge out-of-network rates for emergency services. Insurance enrollees in need of emergency services have no choice but to seek treatment at the closest emergency facility. Avoiding the conflict resolution approach proposed by this bill also would avoid the negative impact to general revenue funds of $11.5 million during the biennium with costs increasing in subsequent years. The Employees Retirement System has worked hard to reduce administrative costs, and this bill would increase these costs due to mediation participation and settlements. NOTES: The fiscal note indicates a cost to general revenue funds from the CSHB 2256 of $11.5 million during fiscal These costs would be incurred by the Employees Retirement System as a result of increased administrative costs due to the mediation process and increased claim payments as a result of mediation.
DRAFT NCOIL OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT
 DRAFT NCOIL OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT Section 1. Title This Act shall be known as the Out-of-Network Balance Billing Transparency Act. Section 2. Purpose The purpose of this
DRAFT NCOIL OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT Section 1. Title This Act shall be known as the Out-of-Network Balance Billing Transparency Act. Section 2. Purpose The purpose of this
National Council of Insurance Legislators (NCOIL) OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT
 National Council of Insurance Legislators (NCOIL) OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT Adopted by the Health, Long Term Care, and Health Retirement Issues Committee on November 18, 2017
National Council of Insurance Legislators (NCOIL) OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT Adopted by the Health, Long Term Care, and Health Retirement Issues Committee on November 18, 2017
The Value of Health Plan Networks
 The Texas Association of Health Plans Representing health insurers, health maintenance organizations, and other related health care entities operating in Texas. The Value of Health Plan Networks What are
The Texas Association of Health Plans Representing health insurers, health maintenance organizations, and other related health care entities operating in Texas. The Value of Health Plan Networks What are
Balance Billing: A Survey Report of Recent Efforts to Protect Consumers
 Balance Billing: A Survey Report of Recent Efforts to Protect Consumers TABLE OF CONTENTS Introduction... 2 National Models... 3 National Association of Insurance Commissioners Model Act...3 National Conference
Balance Billing: A Survey Report of Recent Efforts to Protect Consumers TABLE OF CONTENTS Introduction... 2 National Models... 3 National Association of Insurance Commissioners Model Act...3 National Conference
The Value of Health Plan Networks January 28 th, 2016
 The Texas Association of Health Plans The Value of Health Plan Networks January 28 th, 2016 JAMIE DUDENSING, CEO The Texas Association of Health Plans The Texas Association of Health Plans (TAHP) is the
The Texas Association of Health Plans The Value of Health Plan Networks January 28 th, 2016 JAMIE DUDENSING, CEO The Texas Association of Health Plans The Texas Association of Health Plans (TAHP) is the
Provider Networks and the ACA: Webinar Series Webinar 2: Surprise Billing. Manatt Health May 19, 2016
 2 Provider Networks and the ACA: Webinar Series Webinar 2: Surprise Billing Manatt Health May 19, 2016 3 Introduction 4 Provider Networks and the ACA: Webinar Series This webinar series will cover pressing
2 Provider Networks and the ACA: Webinar Series Webinar 2: Surprise Billing Manatt Health May 19, 2016 3 Introduction 4 Provider Networks and the ACA: Webinar Series This webinar series will cover pressing
SENATE, No. 485 STATE OF NEW JERSEY
 SENATE BUDGET AND APPROPRIATIONS COMMITTEE STATEMENT TO [First Reprint] SENATE, No. 485 STATE OF NEW JERSEY DATED: APRIL 5, 2018 The Senate Budget and Appropriations Committee reports favorably Senate
SENATE BUDGET AND APPROPRIATIONS COMMITTEE STATEMENT TO [First Reprint] SENATE, No. 485 STATE OF NEW JERSEY DATED: APRIL 5, 2018 The Senate Budget and Appropriations Committee reports favorably Senate
CHAPTER 32. AN ACT concerning health insurance and health care providers and supplementing various parts of the statutory law.
 CHAPTER 32 AN ACT concerning health insurance and health care providers and supplementing various parts of the statutory law. BE IT ENACTED by the Senate and General Assembly of the State of New Jersey:
CHAPTER 32 AN ACT concerning health insurance and health care providers and supplementing various parts of the statutory law. BE IT ENACTED by the Senate and General Assembly of the State of New Jersey:
Out-of-Network Law (OON) Guidance (Part H of Chapter 60 of the Laws of 2014)
 Health Plan Disclosure Requirements Out-of-Network Law (OON) Guidance (Part H of Chapter 60 of the Laws of 2014) 1. Provider Directory: Insurance Law 3217-a(a)(17) and 4324(a)(17) and Public Health Law
Health Plan Disclosure Requirements Out-of-Network Law (OON) Guidance (Part H of Chapter 60 of the Laws of 2014) 1. Provider Directory: Insurance Law 3217-a(a)(17) and 4324(a)(17) and Public Health Law
ASSEMBLY, No STATE OF NEW JERSEY. 218th LEGISLATURE INTRODUCED FEBRUARY 12, 2018
 ASSEMBLY, No. STATE OF NEW JERSEY th LEGISLATURE INTRODUCED FEBRUARY, 0 Sponsored by: Assemblyman ROBERT AUTH District (Bergen and Passaic) SYNOPSIS Health Care Consumer s Out-of-Network Protection, Transparency,
ASSEMBLY, No. STATE OF NEW JERSEY th LEGISLATURE INTRODUCED FEBRUARY, 0 Sponsored by: Assemblyman ROBERT AUTH District (Bergen and Passaic) SYNOPSIS Health Care Consumer s Out-of-Network Protection, Transparency,
Statement for Hearing on. Examining Surprise Billing: Protecting Patients from Financial Pain
 Statement for Hearing on Examining Surprise Billing: Protecting Patients from Financial Pain Submitted to the House Education and Labor Committee Subcommittee on Health, Employment, Labor, and Pensions
Statement for Hearing on Examining Surprise Billing: Protecting Patients from Financial Pain Submitted to the House Education and Labor Committee Subcommittee on Health, Employment, Labor, and Pensions
SENATE, No STATE OF NEW JERSEY. 217th LEGISLATURE INTRODUCED FEBRUARY 8, 2016
 SENATE, No. STATE OF NEW JERSEY th LEGISLATURE INTRODUCED FEBRUARY, 0 Sponsored by: Senator JOSEPH F. VITALE District (Middlesex) Senator LORETTA WEINBERG District (Bergen) Senator NILSA CRUZ-PEREZ District
SENATE, No. STATE OF NEW JERSEY th LEGISLATURE INTRODUCED FEBRUARY, 0 Sponsored by: Senator JOSEPH F. VITALE District (Middlesex) Senator LORETTA WEINBERG District (Bergen) Senator NILSA CRUZ-PEREZ District
House Insurance Committee Interim Charge #5:
 The Texas Association of Health Plans House Insurance Committee Interim Charge #5: Evaluate recent efforts by the Legislature and the Texas Department of Insurance to minimize instances of surprise medical
The Texas Association of Health Plans House Insurance Committee Interim Charge #5: Evaluate recent efforts by the Legislature and the Texas Department of Insurance to minimize instances of surprise medical
Hot Topics in Practice of Medicine and Dentistry
 Hot Topics in Practice of Medicine and Dentistry Dallas Bar Association-Health Law Section, September 21, 2016 Bradford E. Adatto & Jay D. Reyero 8150 N. Central Expressway, Suite 930 Dallas, Texas 75206
Hot Topics in Practice of Medicine and Dentistry Dallas Bar Association-Health Law Section, September 21, 2016 Bradford E. Adatto & Jay D. Reyero 8150 N. Central Expressway, Suite 930 Dallas, Texas 75206
List of Insurance Terms and Definitions for Uniform Translation
 Term actuarial value Affordable Care Act allowed charge Definition The percentage of total average costs for covered benefits that a plan will cover. For example, if a plan has an actuarial value of 70%,
Term actuarial value Affordable Care Act allowed charge Definition The percentage of total average costs for covered benefits that a plan will cover. For example, if a plan has an actuarial value of 70%,
The Empire Plan is a comprehensive health insurance program, consisting of four main parts:
 Minimum of 10 years of service required to qualify for Retiree Health & Welfare Benefits Note that all benefits described herein are benefits that are currently in effect. These benefits are all subject
Minimum of 10 years of service required to qualify for Retiree Health & Welfare Benefits Note that all benefits described herein are benefits that are currently in effect. These benefits are all subject
AHIP COMMENTS AND REDLINED RECOMMENDED CHANGES TO DRAFT NCOIL OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT
 AHIP COMMENTS AND REDLINED RECOMMENDED CHANGES TO DRAFT NCOIL OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT Formatted: Centered Section 1. Title This Act shall be known as the Out-of-Network Balance
AHIP COMMENTS AND REDLINED RECOMMENDED CHANGES TO DRAFT NCOIL OUT-OF-NETWORK BALANCE BILLING TRANSPARENCY MODEL ACT Formatted: Centered Section 1. Title This Act shall be known as the Out-of-Network Balance
ASSEMBLY, No STATE OF NEW JERSEY. 218th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 2018 SESSION
 ASSEMBLY, No. 0 STATE OF NEW JERSEY th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 0 SESSION Assemblyman CRAIG J. COUGHLIN District (Middlesex) District (Middlesex) Assemblyman GARY S. SCHAER District
ASSEMBLY, No. 0 STATE OF NEW JERSEY th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 0 SESSION Assemblyman CRAIG J. COUGHLIN District (Middlesex) District (Middlesex) Assemblyman GARY S. SCHAER District
Isett, et al. ORGANIZATION bill analysis 4/21/2005 (CSHB 1006 by Ritter) Lower rollback tax rates and super-rollback tax rates
 HOUSE HB 1006 RESEARCH Isett, et al. ORGANIZATION bill analysis 4/21/2005 (CSHB 1006 by Ritter) SUBJECT: COMMITTEE: VOTE: Lower rollback tax rates and super-rollback tax rates Ways and Means committee
HOUSE HB 1006 RESEARCH Isett, et al. ORGANIZATION bill analysis 4/21/2005 (CSHB 1006 by Ritter) SUBJECT: COMMITTEE: VOTE: Lower rollback tax rates and super-rollback tax rates Ways and Means committee
SUMMARY OF OUT OF NETWORK LEGISLATION June 2018
 SUMMARY OF OUT OF NETWORK LEGISLATION June 2018 MSNJ has worked for years to protect patients and find compromise on insurance network laws and policies in the state. We achieved a great victory 8 years
SUMMARY OF OUT OF NETWORK LEGISLATION June 2018 MSNJ has worked for years to protect patients and find compromise on insurance network laws and policies in the state. We achieved a great victory 8 years
ILYSE SCHUMAN SENIOR VICE PRESIDENT, HEALTH POLICY AMERICAN BENEFITS COUNCIL BEFORE THE
 TESTIMONY OF ILYSE SCHUMAN SENIOR VICE PRESIDENT, HEALTH POLICY AMERICAN BENEFITS COUNCIL BEFORE THE UNITED STATES HOUSE OF REPRESENTATIVES COMMITTEE ON EDUCATION AND LABOR, SUBCOMMITTEE ON HEALTH, EMPLOYMENT,
TESTIMONY OF ILYSE SCHUMAN SENIOR VICE PRESIDENT, HEALTH POLICY AMERICAN BENEFITS COUNCIL BEFORE THE UNITED STATES HOUSE OF REPRESENTATIVES COMMITTEE ON EDUCATION AND LABOR, SUBCOMMITTEE ON HEALTH, EMPLOYMENT,
UnitedHealthcare Insurance Company Written Plan Description
 UnitedHealthcare Insurance Company Written Plan Description [CHOICE][EXCLUSIVE PROVIDER PLAN] This coverage is provided by UnitedHealthcare Insurance Company (UnitedHealthcare). This coverage provides
UnitedHealthcare Insurance Company Written Plan Description [CHOICE][EXCLUSIVE PROVIDER PLAN] This coverage is provided by UnitedHealthcare Insurance Company (UnitedHealthcare). This coverage provides
6/1/2015 prg BPU# G:\CMUCOM\I206\SCM14-15\I206_0004.DOC CL 235 SR 210 TR xxx. SENATE COMMITTEE SUBSTITUTE FOR SENATE, No. 20 STATE OF NEW JERSEY
 6/1/2015 prg BPU# G:\CMUCOM\I206\SCM14-15\I206_0004.DOC CL 235 SR 210 TR xxx SENATE COMMITTEE SUBSTITUTE FOR SENATE, No. 20 STATE OF NEW JERSEY Sponsored by Senator VITALE AN ACT concerning health insurance,
6/1/2015 prg BPU# G:\CMUCOM\I206\SCM14-15\I206_0004.DOC CL 235 SR 210 TR xxx SENATE COMMITTEE SUBSTITUTE FOR SENATE, No. 20 STATE OF NEW JERSEY Sponsored by Senator VITALE AN ACT concerning health insurance,
Glossary of Health Coverage and Medical Terms x
 Glossary of Health Coverage and Medical Terms x x x This glossary defines many commonly used terms, but isn t a full list. These glossary terms and definitions are intended to be educational and may be
Glossary of Health Coverage and Medical Terms x x x This glossary defines many commonly used terms, but isn t a full list. These glossary terms and definitions are intended to be educational and may be
CAUSE NO. TEXAS ASSOCIATION OF IN THE DISTRICT COURT FOR THE HEALTH PLANS, Plaintiff, 419TH vs. JUDICIAL DISTRICT. Defendant. TRAVIS COUNTY, TEXAS
 D-1-GN-18-003846 CAUSE NO. 7/26/2018 11:28 AM Velva L. Price District Clerk Travis County D-1-GN-18-003846 Ruben Tamez TEXAS ASSOCIATION OF IN THE DISTRICT COURT FOR THE HEALTH PLANS, Plaintiff, 419TH
D-1-GN-18-003846 CAUSE NO. 7/26/2018 11:28 AM Velva L. Price District Clerk Travis County D-1-GN-18-003846 Ruben Tamez TEXAS ASSOCIATION OF IN THE DISTRICT COURT FOR THE HEALTH PLANS, Plaintiff, 419TH
NON-PARTICIPATING PROVIDERS. Deductible of $1000 enrollee; $1000 enrolled spouse/domestic partner; $1000 all dependent children.
 Hospital Program (Empire Blue Cross Blue Shield) For Pre-Admission/MRI: Network Benefits In Hospital: Paid-in-full benefits for inpatient hospital, hospice or skilled nursing facility care at a network
Hospital Program (Empire Blue Cross Blue Shield) For Pre-Admission/MRI: Network Benefits In Hospital: Paid-in-full benefits for inpatient hospital, hospice or skilled nursing facility care at a network
Interim Report. to the 85 th Texas Legislature. House Committee on Insurance
 Interim Report to the 85 th Texas Legislature House Committee on Insurance January 2017 HOUSE COMMITTEE ON INSURANCE TEXAS HOUSE OF REPRESENTATIVES INTERIM REPORT 2016 A REPORT TO THE HOUSE OF REPRESENTATIVES
Interim Report to the 85 th Texas Legislature House Committee on Insurance January 2017 HOUSE COMMITTEE ON INSURANCE TEXAS HOUSE OF REPRESENTATIVES INTERIM REPORT 2016 A REPORT TO THE HOUSE OF REPRESENTATIVES
I WANT TO FIND A FACILITY
 You have access to the Cigna LifeSOURCE Transplant Network, a network of participating organ and tissue transplant centers. The transplant network includes over 800 transplant programs at more than 165
You have access to the Cigna LifeSOURCE Transplant Network, a network of participating organ and tissue transplant centers. The transplant network includes over 800 transplant programs at more than 165
Legal Implications of Concierge Medical Practice for Health Plan Providers and Enrollees
 Legal Implications of Concierge Medical Practice for Health Plan Providers and Enrollees James F. Doherty, Jr. Pecore & Doherty, LLC Columbia, Maryland Samantha E. Freed Law Student University of Maryland
Legal Implications of Concierge Medical Practice for Health Plan Providers and Enrollees James F. Doherty, Jr. Pecore & Doherty, LLC Columbia, Maryland Samantha E. Freed Law Student University of Maryland
Network Adequacy Standards Constance L. Akridge July 21, 2016
 Network Adequacy Standards Constance L. Akridge July 21, 2016 Agenda Network Adequacy Developments Overview NAIC Network Adequacy Model Act 2 Network Adequacy Developments Overview --Growing concern over
Network Adequacy Standards Constance L. Akridge July 21, 2016 Agenda Network Adequacy Developments Overview NAIC Network Adequacy Model Act 2 Network Adequacy Developments Overview --Growing concern over
State of Illinois Health Plan Members HealthLink Open Access III Coverage Period: 07/01/ /30/2016 Summary of Benefits and Coverage:
 State of Illinois Health Plan Members HealthLink Open Access III Coverage Period: 07/01/2015 06/30/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
State of Illinois Health Plan Members HealthLink Open Access III Coverage Period: 07/01/2015 06/30/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
The Empire Plan is a comprehensive health insurance program, consisting of four main parts:
 Note that all benefits described herein are benefits that are currently in effect. These benefits are all subject to change, including termination thereof, at any time in the sole discretion of the MTA.
Note that all benefits described herein are benefits that are currently in effect. These benefits are all subject to change, including termination thereof, at any time in the sole discretion of the MTA.
Florida 2016 Legislative Update House Bill 221 & House Bill 1175
 Florida 2016 Legislative Update House Bill 221 & House Bill 1175 Tracy Lutz, Esquire, Managing Partner Specialized Healthcare Partners September 16, 2016 House Bill ( HB ) 221- Extends balance billing
Florida 2016 Legislative Update House Bill 221 & House Bill 1175 Tracy Lutz, Esquire, Managing Partner Specialized Healthcare Partners September 16, 2016 House Bill ( HB ) 221- Extends balance billing
Coventry Health Care of Georgia, Inc. Point-of-Service (POS) Amendment to HMO Certificate of Coverage
 Point-of-Service (POS) Amendment to HMO Certificate of Coverage This Point-of-Service ( POS ) Amendment is an amending attachment to the HMO Certificate of Coverage ( HMO Certificate ). The purpose of
Point-of-Service (POS) Amendment to HMO Certificate of Coverage This Point-of-Service ( POS ) Amendment is an amending attachment to the HMO Certificate of Coverage ( HMO Certificate ). The purpose of
***2017 FORMS ARE PENDING TDI APPROVAL***
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
Out-of-Network Billing
 Out-of-Network Billing Balance Billing A bill to a consumer from a provider for the difference between an insurer s payment to the provider and the provider s charges Occurs when consumers receive covered
Out-of-Network Billing Balance Billing A bill to a consumer from a provider for the difference between an insurer s payment to the provider and the provider s charges Occurs when consumers receive covered
Is there an out of pocket limit on my expenses? Even though you pay these expenses, they don t count toward the out-ofpocket
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-877-988-1918.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-877-988-1918.
Coverage Period: Western Health Advantage: Plan A - Sierra 50 Silver. Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
Scott & White Health Plan: ERS Coverage Period: 9/1/2015 8/31/2016 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.ers.swhp.org or by calling (800) 321-7947, TTY (800)
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.ers.swhp.org or by calling (800) 321-7947, TTY (800)
PRIMARY CARE PHYSICIAN AGREEMENT
 PRIMARY CARE PHYSICIAN AGREEMENT THIS AGREEMENT is made and entered into by and among HealthKeepers, Inc., Peninsula Health Care, Inc., and Priority Health Care, Inc., corporations organized and operated
PRIMARY CARE PHYSICIAN AGREEMENT THIS AGREEMENT is made and entered into by and among HealthKeepers, Inc., Peninsula Health Care, Inc., and Priority Health Care, Inc., corporations organized and operated
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
Wisconsin Society of Pathologists
 563 Carter Court Suite B Kimberly, WI 54136 920-560-5634 Wisconsin Society of Pathologists December 15, 2017 Via email: elizabeth.hizmi@wisconsin.gov Hon. Theodore K. Nickel Wisconsin Office of the Commissioner
563 Carter Court Suite B Kimberly, WI 54136 920-560-5634 Wisconsin Society of Pathologists December 15, 2017 Via email: elizabeth.hizmi@wisconsin.gov Hon. Theodore K. Nickel Wisconsin Office of the Commissioner
South Texas Foot Specialist
 South Texas Foot Specialist Mark Sands, DPM Jeffrey Baxter, DPM Bernabe Canlas, DPM Brett Smith, DPM 119 E. Edgewood Friendswood, TX 77546 FINANCIAL POLICY Tel: (281) 996-9546 Fax: (281) 996-7645 Thank
South Texas Foot Specialist Mark Sands, DPM Jeffrey Baxter, DPM Bernabe Canlas, DPM Brett Smith, DPM 119 E. Edgewood Friendswood, TX 77546 FINANCIAL POLICY Tel: (281) 996-9546 Fax: (281) 996-7645 Thank
Glossary of Health Coverage and Medical Terms
 Glossary of Health Coverage and Medical Terms This glossary defines many commonly used terms, but isn t a full list. These glossary terms and definitions are intended to be educational and may be different
Glossary of Health Coverage and Medical Terms This glossary defines many commonly used terms, but isn t a full list. These glossary terms and definitions are intended to be educational and may be different
Western Health Advantage: WHA Bronze 60 HMO 6000/70 w/child Dental. Coverage Period: 1/1/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
[First Reprint] ASSEMBLY, No STATE OF NEW JERSEY. 218th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 2018 SESSION
![[First Reprint] ASSEMBLY, No STATE OF NEW JERSEY. 218th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 2018 SESSION [First Reprint] ASSEMBLY, No STATE OF NEW JERSEY. 218th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 2018 SESSION](/thumbs/81/83156264.jpg) [First Reprint] ASSEMBLY, No. 0 STATE OF NEW JERSEY th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 0 SESSION Assemblyman CRAIG J. COUGHLIN District (Middlesex) Assemblyman GARY S. SCHAER District (Bergen
[First Reprint] ASSEMBLY, No. 0 STATE OF NEW JERSEY th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 0 SESSION Assemblyman CRAIG J. COUGHLIN District (Middlesex) Assemblyman GARY S. SCHAER District (Bergen
Some of the services this plan doesn t cover are listed on page 5. See your policy Yes plan doesn t cover?
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Network This is only a summary. If you want more detail about your coverage and costs, you can
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Network This is only a summary. If you want more detail about your coverage and costs, you can
Annual deductibles and maximums In-network Out-of-network Lifetime maximum
 SUMMARY OF BENEFITS City of Richmond & Richmond Public Schools (Plan B) Connecticut General Life Insurance Co. Annual deductibles and maximums Lifetime maximum Unlimited per individual Pre-Existing Condition
SUMMARY OF BENEFITS City of Richmond & Richmond Public Schools (Plan B) Connecticut General Life Insurance Co. Annual deductibles and maximums Lifetime maximum Unlimited per individual Pre-Existing Condition
Blue Cross Blue Shield of Louisiana: BlueConnect POS Plan 2 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-599-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-599-2583. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
Important Questions Answers Why this Matters:
 Student Employee Health Plan: NYS Health Insurance Program Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual or Family
Student Employee Health Plan: NYS Health Insurance Program Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual or Family
[Second Reprint] ASSEMBLY, No STATE OF NEW JERSEY. 217th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 2016 SESSION
![[Second Reprint] ASSEMBLY, No STATE OF NEW JERSEY. 217th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 2016 SESSION [Second Reprint] ASSEMBLY, No STATE OF NEW JERSEY. 217th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 2016 SESSION](/thumbs/89/97653414.jpg) [Second Reprint] ASSEMBLY, No. STATE OF NEW JERSEY th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 0 SESSION Sponsored by: Assemblyman CRAIG J. COUGHLIN District (Middlesex) Assemblyman GARY S. SCHAER
[Second Reprint] ASSEMBLY, No. STATE OF NEW JERSEY th LEGISLATURE PRE-FILED FOR INTRODUCTION IN THE 0 SESSION Sponsored by: Assemblyman CRAIG J. COUGHLIN District (Middlesex) Assemblyman GARY S. SCHAER
$0 See the chart starting on page 2 for your costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.chchealth.org/affordablehealth/planbrochure/silver.aspx
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.chchealth.org/affordablehealth/planbrochure/silver.aspx
You don t have to meet deductibles for specific services, but see the chart starting on page 3 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
Choosing Between Traditional Medicare and Medicare Advantage
 Choosing Between Traditional Medicare and Medicare Advantage If you are eligible for Medicare you can chose between getting Medicare benefits through traditional Medicare (also known as original Medicare
Choosing Between Traditional Medicare and Medicare Advantage If you are eligible for Medicare you can chose between getting Medicare benefits through traditional Medicare (also known as original Medicare
Colorado Chiropractic Association 2017 Legislative Update As of May 11, 2017
 Colorado Chiropractic Association 2017 Legislative Update As of May 11, 2017 Bill: HB17-1057 Interstate Physical Therapy Licensure Compact The bill enacts the Interstate Physical Therapy Licensure Compact
Colorado Chiropractic Association 2017 Legislative Update As of May 11, 2017 Bill: HB17-1057 Interstate Physical Therapy Licensure Compact The bill enacts the Interstate Physical Therapy Licensure Compact
1/01/ /31/2019 IBEW LOCAL 351 WELFARE FUND
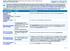 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/01/2019-12/31/2019 IBEW LOCAL 351 WELFARE FUND Coverage for: Family Plan Type: PPO The Summary
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/01/2019-12/31/2019 IBEW LOCAL 351 WELFARE FUND Coverage for: Family Plan Type: PPO The Summary
Blue Cross Blue Shield of Louisiana: Blue Max 2500 Maternity Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-599-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-599-2583. Important Questions
CalPERS: Sharp Performance Plus HMO Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.sharphealthplan.com/calpers or by calling 1-855-995-5004.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.sharphealthplan.com/calpers or by calling 1-855-995-5004.
NETWORK: $4,000 single / $10,000 family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
Is there an out of pocket limit on my expenses? Even though you pay these expenses, they don t count toward the out-ofpocket
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-877-988-1918.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-877-988-1918.
Coverage Period: 1/1/ /31/2016. Western Health Advantage: WHA Silver 70 HSA HMO 2000/20% w/child Dental. Coverage For: Self Only Plan Type: HMO
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
 BlueCross BlueShield Healthcare Plan of Georgia Premier Plus POS Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2013-01/01/2014 Coverage For: Individual/Family
BlueCross BlueShield Healthcare Plan of Georgia Premier Plus POS Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2013-01/01/2014 Coverage For: Individual/Family
Summary of Benefits and Coverage
 Summary of Benefits and Coverage Anthem Blue Cross is the trade name of Blue Cross of California. Independent licensee of the Blue Cross Association. ANTHEM is a registered trademark of Anthem Insurance
Summary of Benefits and Coverage Anthem Blue Cross is the trade name of Blue Cross of California. Independent licensee of the Blue Cross Association. ANTHEM is a registered trademark of Anthem Insurance
Important Questions Answers Why this Matters:
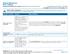 Anthem BlueCross PPO 1500/$35 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/15/2013-10/14/2014 Coverage For: Individual/Family Plan Type: PPO This is only
Anthem BlueCross PPO 1500/$35 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/15/2013-10/14/2014 Coverage For: Individual/Family Plan Type: PPO This is only
State of Florida Health Investor HMO Plan Coverage Period: 1/1/ /31/2014
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Family Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Family Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you
You can see the specialist you choose without permission from this plan.
 Prominence HealthFirst of Texas: Silver 10 Coverage Period: 1/1/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HMO This
Prominence HealthFirst of Texas: Silver 10 Coverage Period: 1/1/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HMO This
Thompson, et al. ORGANIZATION bill analysis 5/6/2011 (CSHB 3610 by Cook) Allowing periodic rate adjustments by electric utilities
 HOUSE HB 3610 RESEARCH Thompson, et al. ORGANIZATION bill analysis 5/6/2011 (CSHB 3610 by Cook) SUBJECT: COMMITTEE: VOTE: Allowing periodic rate adjustments by electric utilities State Affairs committee
HOUSE HB 3610 RESEARCH Thompson, et al. ORGANIZATION bill analysis 5/6/2011 (CSHB 3610 by Cook) SUBJECT: COMMITTEE: VOTE: Allowing periodic rate adjustments by electric utilities State Affairs committee
Important Questions Answers Why this Matters:
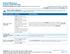 Anthem BlueCross Solution 5000 PPO Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/15/2013-10/14/2014 Coverage For: Individual/Family Plan Type: PPO This
Anthem BlueCross Solution 5000 PPO Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 10/15/2013-10/14/2014 Coverage For: Individual/Family Plan Type: PPO This
House Bill 2339 Ordered by the House April 7 Including House Amendments dated April 7
 th OREGON LEGISLATIVE ASSEMBLY-- Regular Session A-Engrossed House Bill Ordered by the House April Including House Amendments dated April Introduced and printed pursuant to House Rule.00. Presession filed
th OREGON LEGISLATIVE ASSEMBLY-- Regular Session A-Engrossed House Bill Ordered by the House April Including House Amendments dated April Introduced and printed pursuant to House Rule.00. Presession filed
BlueCross 0.50, a Multi-State Plan STD
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.capbluecross.com/sbcsia or by calling 1-800-730-7219.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.capbluecross.com/sbcsia or by calling 1-800-730-7219.
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Prev. Plus Plan This is only a summary. If you want more detail about your coverage and costs,
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Prev. Plus Plan This is only a summary. If you want more detail about your coverage and costs,
Going to hospital. What you need to know
 Going to hospital What you need to know Going to hospital Going into hospital for treatment? Find out everything you need to know in this step-by-step guide. We ll take you through what you re covered
Going to hospital What you need to know Going to hospital Going into hospital for treatment? Find out everything you need to know in this step-by-step guide. We ll take you through what you re covered
Important Questions Answers Why this Matters: What is the overall deductible? $0 Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/bor or by calling 1-800-424-8950. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/bor or by calling 1-800-424-8950. Important
Important Questions Answers Why this Matters: What is the overall deductible? $0 Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/usg or by calling 1-800-424-8950. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/usg or by calling 1-800-424-8950. Important
GENERAL ASSEMBLY OF NORTH CAROLINA SESSION 2017 S 1 SENATE BILL 629. Short Title: Health Care Services Billing Transparency.
 GENERAL ASSEMBLY OF NORTH CAROLINA SESSION S 1 SENATE BILL Short Title: Health Care Services Billing Transparency. (Public) Sponsors: Referred to: Senators Hise, Meredith (Primary Sponsors); and Krawiec.
GENERAL ASSEMBLY OF NORTH CAROLINA SESSION S 1 SENATE BILL Short Title: Health Care Services Billing Transparency. (Public) Sponsors: Referred to: Senators Hise, Meredith (Primary Sponsors); and Krawiec.
Western Health Advantage: WHA Platinum 90 HMO 0/20 w/child Dental. Coverage Period: 1/1/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or by calling 1-888-563-2250. Important
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
Some of the services this plan doesn t cover are listed on page 6. See your policy or plan Yes. plan doesn t cover?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nslijcareconnect.com or by calling 1-855-706-7545. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nslijcareconnect.com or by calling 1-855-706-7545. Important
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.centralpateamsters.com or by calling 1-800-422-8330 (PA)
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.centralpateamsters.com or by calling 1-800-422-8330 (PA)
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplan.memorialhermann.org or by calling 1-888-594-0671.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
Out-of-Network Payment: The most confusing public health topic you ll ever love
 Out-of-Network Payment: The most confusing public health topic you ll ever love Sherif Zaafran, M.D. Chair, Ad Hoc Committee on Out-of-Network Payment MSA SPRING CONFERENCE 2017 May 20 th, 2017 asahq.org
Out-of-Network Payment: The most confusing public health topic you ll ever love Sherif Zaafran, M.D. Chair, Ad Hoc Committee on Out-of-Network Payment MSA SPRING CONFERENCE 2017 May 20 th, 2017 asahq.org
Important Questions Answers Why this Matters: In-Network: $300 Individual / $600 Family;
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-314-5366.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-314-5366.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family
 This is only a summary If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at wwwmvphealthcarecom or by calling 1-888-687-6277 Important
This is only a summary If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at wwwmvphealthcarecom or by calling 1-888-687-6277 Important
INFORMATION ABOUT YOUR OXFORD COVERAGE
 OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Coverage Period: 08/01/ /31/2016
 Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 08/01/2015-07/31/2016
Anthem Blue Cross University of the Pacific Student Health Plan PPO with Student Health Center (100/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 08/01/2015-07/31/2016
$ 200 family deductible per benefit year for Major Medical benefits. Only applies to out-ofnetwork. $ No
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.njcf.org or by calling 1-800-624-3096. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.njcf.org or by calling 1-800-624-3096. Important Questions
Retirees with Medicare (RETIREMENT DATE ON or AFTER March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2019
 Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
SOAH DOCKET NO C TDI CASE NO Argus Health Systems, Inc. Administrative Hearings. First Amended Notice of Hearing
 SOAH DOCKET NO. 454-15-4787.C TDI CASE NO. 6438 Texas Department of Insurance, Petitioner Before the State Office V. of Argus Health Systems, Inc. Respondent Administrative Hearings First Amended The Texas
SOAH DOCKET NO. 454-15-4787.C TDI CASE NO. 6438 Texas Department of Insurance, Petitioner Before the State Office V. of Argus Health Systems, Inc. Respondent Administrative Hearings First Amended The Texas
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
Retirees with Medicare (RETIREMENT DATE BEFORE March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2019
 Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana
Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana
California s Surprise Medical Bill Statute: Part 2: Comparison to New York s Emergency Medical Services and Surprise Bills Law
 California s Surprise Medical Bill Statute: Part 2: Comparison to New York s Emergency Medical By Jackie Selby and Kevin J. Malone December 2016 I. Executive Summary On September 23, 2016, the California
California s Surprise Medical Bill Statute: Part 2: Comparison to New York s Emergency Medical By Jackie Selby and Kevin J. Malone December 2016 I. Executive Summary On September 23, 2016, the California
Saint Mary s Health Plans: HMOMyPlan 10S_RX 15/55/100 Coverage Period: 01/01/14-12/31/14
 Important Questions Answers Why this Matters: This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.saintmaryshealthplans.com
Important Questions Answers Why this Matters: This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.saintmaryshealthplans.com
HMO Louisiana, Inc.: Blue POS copay 80/60 $500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-495-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsla.com or by calling 1-800-495-2583. Important Questions
Aetna Group Medicare Advantage Frequently Asked Questions
 Aetna Group Medicare Advantage Frequently Asked Questions Providers & the Aetna Network 1. How do I find out if my providers are in the Aetna Medicare Advantage Network or if they accept the Aetna plan?
Aetna Group Medicare Advantage Frequently Asked Questions Providers & the Aetna Network 1. How do I find out if my providers are in the Aetna Medicare Advantage Network or if they accept the Aetna plan?
IWDCNE Health and Welfare Plan: Active Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 IWDCNE Health and Welfare Plan: Active Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: Beginning on or after 1/1/2016 Coverage for: All Coverage Types This
IWDCNE Health and Welfare Plan: Active Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: Beginning on or after 1/1/2016 Coverage for: All Coverage Types This
