C C VV I. California Workers Compensation Institute 1111 Broadway Suite 2350, Oakland, CA Tel: (510) Fax: (510)
|
|
|
- Priscilla Peters
- 6 years ago
- Views:
Transcription
1 C C VV I California Workers Compensation Institute 1111 Broadway Suite 2350, Oakland, CA Tel: (510) Fax: (510) April 5, 2010 VIA to DWCForums@dir.ca.gov Division of Workers Compensation Post Office Box San Francisco, CA Attn: DWC Forums RE: RBRVS Revision to Physician Section of OMFS Physician fee schedule proposed regulations version version Physician fee schedule draft conversion factor transition version version Adapting the RBRVS Methodology to the California Workers' Compensation Physician Fee Schedule: Supplemental report version This Forum commentary on draft revisions to the Physicians Section of the Official Medical Fee Schedule (OMFS), conversion factor revision and the Lewin Group s Supplemental Report: Adapting the RBRVS Methodology to the California Workers' Compensation Physician Fee Schedule is presented on behalf of the California Workers' Compensation Institute s members. Institute members include insurers writing 87% of California s workers compensation premium, and self-insured employers with $30B of annual payroll (20% of the state s total annual self-insured payroll). Introduction The California Workers Compensation Institute (The Institute) supports the Division s approach to revising the Physician Section of the Official Medical Fee Schedule, including its plan to adopt a budget-neutral RBRVS schedule, retain the physical medicine cascade and to transition to a single conversion factor over a period of four years. The California Workers Compensation Institute congratulates the Division of Workers Compensation on the results of its hard work on this difficult project. The Institute s recommended modifications that are indicated by underline and strikethrough, and comments follow. The Institute recommends allowing at least three months between the adoption and date of service* implementation to allow for the re-programming, testing, training, and other operational preparation necessary for a major fee schedule change.
2 The Lewin Group in its reports did not consider the impact of increasing the allowance for progress reports from $11.69 to $37.98, nor did it consider the impact of extending reimbursement for progress reports from primary treating physicians to all physicians. It treated reports only as a pass-through. If these changes are adopted, the revised schedule will not be cost neutral. Because the current frequency of PTP progress reports is so high, and because the frequency of paid progress reports from non-ptps is also anticipated to be high, the impact will be significant and must be taken into account. The purpose of redesigning the progress report form was to facilitate efficient reporting of the information that physicians must already report. A secondary benefit to physicians was that the form would more effectively support the medical billing. The increase in reimbursement for the form is not necessary and perhaps is unintended. The Institute recommends removing it. Draft OMFS Physician Section Regulations Physician Fee Schedule: Official Medical Fee Schedule for Physician and Non-Physician Professional Provider Services For Services Rendered On or After 10/1/2010* (a) Maximum reasonable fees for physician and non-physician professional medical treatment provided pursuant to Labor Code section 4600, which is rendered on or after October 1, 2010*, shall be no more than the amount determined by the Official Medical Fee Schedule for Physician and Non- Physician Professional Provider Services, consisting of the regulations set forth in Sections through ( Physician Fee Schedule. ) The Physician Fee Schedule shall not govern fees for services covered by a contract setting such fees as permitted by Labor Code section (b) Maximum fees for services of a physician or non-physician professional medical services provider, are governed by the Physician Fee Schedule, regardless of specialty, for services performed within his or her scope of practice or license as defined by California law, except for: (1) E/M codes which are to be used by physicians (as defined by Labor Code ), as well as physician assistants and nurse practitioners who are acting within the scope of their practice and are under the direction of a supervising physician; (2) Physical Medicine and Rehabilitation Evaluation codes (97001 and 97002) which are to be used only by physical therapists; (3) Occupational Therapy Evaluation codes (97003 and 97004) which are to be used only by occupational therapists; and (4) Osteopathic Manipulation Codes ( ) which are to be used only by licensed Doctors of Osteopathy and Medical Doctors.; and (5) Other codes that specify a particular provider-type, which are to be used by the specified type of provider. Page 2
3 The list of exceptions in (b) needs also to include and address other codes that specify in the code descriptions particular provider types Definitions (h) CPT or Current Procedural Terminology" is the book Current Procedural Terminology, Standard Edition, Fourth Edition, dated xxxxxxx, copyright by the American Medical Association. (j) Facility means that the a site of service that receives or is eligible to receive a facility fee payment related to the procedure. (l) Non-Facility means that the a site of service that does not allow for a facility fee payment related to the procedure. Each edition of the CPT book undergoes revisions periodically, therefore it is necessary to include an as of date in (h) and elsewhere in the regulation. The language recommended for (j) and (h) is consistent with the language in other definitions Relative Value Units (RVUs) For services rendered on or after October 1, 2010*, the Administrative Director incorporates by reference the specified portions of the 2010 National Physician Fee Schedule Relative Value File, revised 1/8/2010, entitled PPRRVU10 and RVUPUF10.pdf which can be accessed at: &filterByDID=1&sortByDID=1&sortOrder=ascending&itemID=CMS &intNumPerPage=10 The columns of the PPRRVU10 which are incorporated by reference include: Column A HCPCS (except the alpha-numeric codes) Column B Modifier Column C Description Column D Status Code (except G, I, N, R) Column Q Fully Implemented Non-Facility Total RVUs Column S Fully Implemented Facility Total RVUs Column T PC/TC Indicator Column U Global Days Column V Pre Operative Column W Intra Operative Column X Post Operative Column Y Multiple Procedure Column Z Bilateral Surgery Page 3
4 Column AA Column AB Column AC Column AD Column AH Assistant Surgeon Co-Surgeon Team Surgeon Endoscopic Base Code Diagnostic Imaging Family Indicator The codes of the PPRRVU10 that are incorporated by reference include: xx to xx (add code intervals that are to be included in the Physician Section). The portions of the RVUPUF10.pdf that are incorporated by reference include: (add here the portions that are to be included in the Physician Section). Because the codes listed in PPRRVU10 include codes from other sections of the OMFS, such as the Ambulance Section, the regulation needs to indicate the code intervals included in the Physician Section. RVUPUF10.pdf provides additional necessary and clarifying information, including information on CPT modifiers and status codes Conversion Factors The conversion factor(s) for physician and non-physician professional medical services shall be as follows: (a) Anesthesia services (codes listed in the anesthesia section of the CPT): For services rendered on or after October 1, 2010*: $ (b) For medical treatment services other than anesthesia (codes listed, respectively, in the surgery, radiology, and all other sections of the CPT): Surgery Radiology All Other For services rendered on or after October 1, 2010* For services rendered on or after October 1, 2011* For services rendered on or after October 1, 2012* For services rendered on or after October 1, 2013* Page 4
5 Calculation of the Maximum Reasonable Fee - Services Other than Anesthesia Except for fees determined in et seq., (Anesthesia), the base maximum reasonable fee for physician and non-physician professional medical provider services shall be the non-facility or facility fee calculated as follows: (a) Non-facility site of service fee calculation: For services rendered on or after October 1, 2010*: Fully Implemented Non-Facility Total RVU (Column Q) * CF = Base Maximum Fee The base maximum fee for the procedure code is the maximum reasonable fee, except as otherwise provided by applicable provisions of this fee schedule, including but not limited to the application of ground rules and modifiers that effect reimbursement. (b) Facility site of service fee calculation: For services rendered on or after October 1, 2010*: Fully Implemented Facility Total RVU (Column S) * CF = Base Maximum Fee The base maximum fee for the procedure code is the maximum reasonable fee, except as otherwise provided by applicable provisions of this fee schedule, including but not limited to the application of ground rules and modifiers that effect reimbursement. (c)(1) Total Facility Total RVU shall be used to calculate the fee for services furnished to a patient in the hospital (inpatient or outpatient), comprehensive inpatient rehabilitation facility, inpatient psychiatric facility, skilled nursing facility, community mental health center, or ambulatory surgical center. (2) Total Non-Facility Total RVU shall be used to calculate the fee for services furnished to a patient in the physician s or non-physician provider s office, the patient s home, or in a facility or institution other than those listed above as the site for use of Total Facility Total RVU. The modifications recommended for (c)(1) and (2) to make the term consist with (a) and (b) and in the CMS tables. Page 5
6 Coding; Current Procedural Terminology, Fourth Edition (a) The coding, modifiers, guidelines, appendices and all other provisions of Current Procedural Terminology, Fourth Edition, dated xxxxxxx published by the American Medical Association are applicable to the bills submitted for physician and non-physician professional medical services, except that any regulation in the Physician Fee Schedule that conflicts with a provision in CPT will take precedence over the CPT. For services rendered on or after October 1, 2010*, the Administrative Director incorporates by reference the American Medical Association s "Current Procedural Terminology," 4th Edition, Revised (b) Copies of Current Procedural Terminology, Fourth Edition dated xxxxxxx may be purchased from the American Medical Association: Order Department American Medical Association P.O. Box Atlanta, GA Or over the internet at: Or American Medical Association s toll free order line: (800) California Specific Codes Physicians shall use the California Specific Codes listed below. Maximum reasonable fees for services performed by providers within their scope of practice shall be no more than the fee listed below for the procedure. CA Code Reference to Fee (If Any) Procedure WC001 Not Reimbursable Doctor's First Report of Occupational Illness or Injury (Form 5021) (Section (a)(1)) WC002 $37.98 $11.69 Primary Treating Physician's Progress Report (PR-2 or narrative equivalent submitted by the Primary Treating Physician in accordance with 9785) (Section (b)(1)) WC003 WC004 $37.98 for first page $23.37 each additional page. Maximum of six pages absent prior authorization ($154.83) $37.98 for first page $23.37 each additional Primary Treating Physician s Permanent and Stationary Report (Form PR-3) (Section (b)(2)) Primary Treating Physician s Permanent and Stationary Report (Form PR-4) Page 6
7 page. Maximum of (Section (b)(3)) seven pages absent prior authorization ($178.20) WC005 Not Reimbursable Functional Improvement Report (Form FIR) WC006 WC007 WC008 WC009 $37.98 for first page $23.37 each additional page. Maximum of six pages absent prior authorization ($154.83) $37.98 for first page $23.37 each additional page. Maximum of six pages absent prior authorization ($154.83) $10.00 for up to the first 15 pages. $0.25 for each additional page after the first 15 pages. $10.00 for up to the first 15 pages. $0.25 for each additional page after the first 15 pages. (Section (a)(2)) Other Provider Report Not Legally Mandated (Section (b)(4)) Consultation Reports (Section (b)(5)) Chart Notes (Section (c)) Duplicate Reports (Section (d)) WC010 $ 5.00 per x-ray Duplication of X-Ray WC011 $10.00 per scan Duplication of Scan WC012 $62.50 for each quarter hour or portion thereof spent by the treating physician WC013 No Fee Prescribed / Non Reimbursable absent agreement Medical Testimony (reimburse for all itemized reasonable and necessary time spent related to the testimony, including reasonable preparation and travel time, rounded to the nearest quarter hour. A minimum of one hour shall be reimbursed for a scheduled deposition, even if less than one hour is spent.) Missed Appointments. This code is designated for communication only. It does not imply that compensation is owed. The recommended modification in the WC002 Reference to Fee (if any) box, it is necessary to maintain the revenue neutral revision goal. The Lewin Group in its reports did not consider the impact of increasing the allowance for progress reports from $11.69 to $37.98, nor did it consider the impact of extending reimbursement for progress reports from primary treating physicians to all physicians. It treated reports only as a passthrough. Because the current frequency of PTP progress reports is so high, and Page 7
8 because the frequency of paid progress reports from non-ptps is also anticipated to be high, the impact is expected to be significant and needs to be taken into account. If the changes proposed in this table were adopted, the revised schedule will not be cost neutral. Number Total Paid Adjusted Paid Difference PTP progress report 213,698 $ 2,422,302 $ 8,116,250 $ 5,693,948 All other Physician FS codes 1,147,799 $ 86,797,466 $ 86,797,466 Total 1,361,497 $ 89,219,768 $ 94,913, as % of Total 15.7% 2.7% 8.6% % change increases total Phys FS paid 6.4% Data based on sample of medical bill review data with DOS between Jan June 2009 Adjusted Paid assumes reimbursement change from $11.69 to $37.98 per report Based on a sample of medical bill review data from the ICIS data base, progress reports constitute 15.7% of Physician Fee Schedule codes with dates of service from January through June of 2009, and 2.7% of the total payments. Increasing the payment of those reports from $11.69 to $37.98 would increase the payments for progress reports to 8.6% of the total payments, increasing total payments under the physician fee schedule by 6.4%. If all other physicians are also paid for progress reports, the increase would be significantly more. Since such reports are not currently billed, it is difficult to estimate the extent of that additional increase. For the WC002 Procedure box recommended modification, see the Institute s comments on subsections (a)(4) and (a)(9) of section 9785 regarding the statutory and operational need to limit the required progress reporting the PR-2 or equivalent, to the primary treating physician California-Specific Modifiers (a) The following modifiers are to be appended to the applicable CPT Code or California Specific code in addition to any applicable CPT modifier. -01 Primary treating physician report/service: This modifier shall be used to identify a required report issued or E&M service performed by the primary treating physician. This modifier shall be appended to each of the following codes, as appropriate: evaluation and management codes, report codes and prolonged service codes. Page 8
9 -02 Secondary treating physician report/service: This modifier shall be used to identify a required report issued or E&M service performed by the secondary treating physician. This modifier shall be appended to each of the following codes, as appropriate: evaluation and management codes, report codes and prolonged service codes. -03 Non-physician provider report/service: This modifier shall be used to identify a required report issued by, or E&M service performed by, a non-physician professional provider. -04 Consultant Report/service: This modifier shall be used to identify a report issued by, or E&M service performed by, a Consultant. This modifier shall be appended to each of the following codes, as appropriate: evaluation and management codes, report codes and prolonged service codes. -05 Consultation Service During Medical-Legal Evaluation: This modifier shall be used to identify services or procedures performed by a consultant in the context of a medical-legal evaluation where those services are paid under the Physician Fee Schedule. -83 Surgical Assistant Services Provided by a Licensed Non-Physician Professional Provider This modifier shall be used to identify services performed by licensed non-physician professional providers acting within their scope of practice, and used in lieu of an assistant physician. Reimbursed at 10% of allowable surgical fee. -93 Interpreter Required at the Time of Examination: Where this modifier is applicable, the value of the evaluation and management service is modified by multiplying the normal value by 1.1. Prolonged service codes may not be used in combination with this modifier unless it is documented that the reason for the code is additional time required as a result of factors beyond the need for an interpreter. Although similar types of modifiers are included in the current fee schedule, except for those that affect reimbursement, they remain largely unused and ignored. Unless there is some consequence attached to their use, consider deleting unused codes as the situation is unlikely to change Evaluation and Management Coding New Patient For purposes of workers compensation billing, the CPT definitions of new patient and established patient are altered as follows: Page 9
10 (a) A new patient is one who is new to the physician or an established patient with a new industrial injury or illness. Only one new patient visit is reimbursable to a single physician or medical group per specialty for evaluation of the same patient relating to the same incident, injury or illness. (b) An established patient is a patient who has been seen previously for the same industrial injury or illness by the physician or medical group. Medical group is needed in (b) for consistency with (a) Correct Coding Initiative For services rendered on or after October 1, 2010*, the Administrative Director incorporates by reference the National Correct Coding Initiative Edits - Physicians and the National Correct Coding Initiative Coding Policy Manual for Medicare Services, version 15.3, effective October 1, By Report - Reimbursement for Unlisted Procedures / Procedures Lacking RBRVUs (a) An unlisted procedure shall be billed using the appropriate unlisted procedure code from the CPT. The procedure shall be billed by report (report not separately reimbursable), justifying that the service was reasonable and necessary to cure or relieve from the effects of the industrial injury or illness. (c) In some instances, the value of a By Report procedure may be determined using based on the value assigned to a comparable procedure. The comparable procedure should reflect the same amount of time, complexity, expertise, etc. as required for the procedure performed or the differences considered when assigning a value. The modification to (a) will avoid disputes over whether the report is separately reimbursable. The reimbursement amount for a By Report procedure can be determined by increasing or decreasing the fee for another procedure according to the differences in factors such as time, complexity, expertise, etc. Page 10
11 Reimbursement for Reports, Duplicate Reports, Chart Notes (a) Treatment Reports Not Separately Reimbursable. The following treatment reports are not separately reimbursable as the appropriate fee is included within the underlying Evaluation and Management service, Physical Therapy Evaluation service or Occupational Therapy Evaluation service for an office visit: (1) Doctor's First Report of Occupational Illness or Injury (Form 5021) issued in accordance with section 9785(e). Use Code WC001; (2) Functional Improvement Report (DWC Form FIR) issued in accordance with section 9785(g)(2). Use Code WC005. (3) Non-PTP s Progress Report (4) Documents submitted for the purpose of supporting medical bills or requests for authorization. (b) Treatment Reports That Are Separately Reimbursable. The following treatment reports are separately reimbursable. Where an office visit is included, the report charge is payable in addition to the underlying Evaluation and Management service for an office visit. (1) Treating Physician s Progress Report (Form PR-2), by primary treating physician or secondary treating physician, issued in accordance with section 9785(f), using DWC form PR-2, its narrative equivalent, or letter format where allowed by section Use Code WC002. Maximum reimbursement is $ (4) Provider Reports That Are Not Legally Mandated. When a claims administrator or its authorized agent requests that a provider complete a form that is not legally mandated or submit information in excess of that required pursuant to section 9785 except for documents submitted for the purpose of supporting medical bills or requests for authorization, the provider shall be separately reimbursed using code WC006. Maximum reimbursement is $37.98 for first page, plus $23.37, for each additional page. Maximum of six pages absent prior authorization. Maximum total reimbursement is $ (5) Consultation Reports that are separately reimbursable. The following reports are separately reimbursable. Where an examination of the patient is performed, the report charge is payable in addition to the underlying Evaluation and Management visit code. Use Code WC007. Where there is no examination of the patient, see "Prolonged Service Codes", below. (A) A report by a consulting physician, where consultation was requested on one or more medical issues by the treating physician, including a second medical opinion on the necessity or appropriateness of previously recommended medical treatment or a surgical procedure. Page 11
12 (B) A report by a consulting physician, where consultation was requested on one or more medical issues by a party, the Administrative Director, or the Workers' Compensation Appeals Board. Reports included under this section are those reports that are admissible and reimbursable in accordance with Labor Code section 4064(d). (C) A report by the treating physician, where medical information other than that required to be reported under the treatment report section above was requested by a party, the Administrative Director, or the Workers' Compensation Appeals Board., however this does not include documents submitted for the purpose of supporting medical bills or requests for authorization. (D) A report by a consulting physician where the claim does not meet the criteria of a "contested claim" as set forth in 8 CCR 9793(b). (I think this is covered in (A) and (B). (E) A consultation code may not be billed when care or any part of care has been clearly transferred by the primary treating physician to another physician. Clarification is needed that progress reports by non-ptps (see previous comments) and documents submitted for the purpose of supporting medical billings are also not separately reimbursable. (D) appears to be necessary because it is covered by (A) and (B). Thank you for considering these comments. Please contact me for clarification or other assistance. Sincerely, Brenda Ramirez CWCI Claims and Medical Director BR/pm cc: Carrie Nevans, DWC Acting Administrative Director Susan Honor-Vangerov, J.D., DWC Medical Unit Manager CWCI Claims Committee CWCI Medical Care Committee CWCI Return to Work Committee CWCI Legal Committee CWCI Regular Members CWCI Associate Members Page 12
WORKERS COMPENSATION REFORMS OFFICIAL MEDICAL FEE SCHEDULE PHYSICIAN SERVICES SUMMARY CHANGES TO THE OFFICIAL MEDICAL FEE SCHEDULE PHYSICIAN SERVICES
 SUMMARY CHANGES TO THE SB 863, enacted in 2012, required the Division of Workers Compensation to transition the Official Medical Fee Schedule for physician services to a Medicare RBRVS system over four
SUMMARY CHANGES TO THE SB 863, enacted in 2012, required the Division of Workers Compensation to transition the Official Medical Fee Schedule for physician services to a Medicare RBRVS system over four
PREDESIGNATION OF PERSONAL PHYSICIANS AND REPORTING DUTIES OF THE PRIMARY TREATING PHYSICIAN REGULATIONS
 PREDESIGNATION OF PERSONAL PHYSICIANS AND REPORTING DUTIES OF THE PRIMARY TREATING PHYSICIAN REGULATIONS Title 8, California Code of Regulations Chapter 4.5. Division of Workers Compensation Subchapter
PREDESIGNATION OF PERSONAL PHYSICIANS AND REPORTING DUTIES OF THE PRIMARY TREATING PHYSICIAN REGULATIONS Title 8, California Code of Regulations Chapter 4.5. Division of Workers Compensation Subchapter
C C VV I. California Workers Compensation Institute 1111 Broadway Suite 2350, Oakland, CA Tel: (510) Fax: (510)
 C C VV I California Workers Compensation Institute 1111 Broadway Suite 2350, Oakland, CA 94607 Tel: (510) 251-9470 Fax: (510) 251-9485 August 19, 2013 VIA E-MAIL to dwcrules@dir.ca.gov Maureen Gray, Regulations
C C VV I California Workers Compensation Institute 1111 Broadway Suite 2350, Oakland, CA 94607 Tel: (510) 251-9470 Fax: (510) 251-9485 August 19, 2013 VIA E-MAIL to dwcrules@dir.ca.gov Maureen Gray, Regulations
(a) For the purposes of this section, the following definitions apply:
 9785. Reporting Duties of the Primary Treating Physician. (a) For the purposes of this section, the following definitions apply: (1) The primary treating physician is the physician who is primarily responsible
9785. Reporting Duties of the Primary Treating Physician. (a) For the purposes of this section, the following definitions apply: (1) The primary treating physician is the physician who is primarily responsible
Modifier 51 - Multiple Procedure Fee Reductions
 Manual: Policy Title: Reimbursement Policy Modifier 51 - Multiple Procedure Fee Reductions Section: Modifiers Subsection: None Date of Origin: Last Updated: 1/1/2000 Policy Number: 4/10/2018 Last Reviewed:
Manual: Policy Title: Reimbursement Policy Modifier 51 - Multiple Procedure Fee Reductions Section: Modifiers Subsection: None Date of Origin: Last Updated: 1/1/2000 Policy Number: 4/10/2018 Last Reviewed:
(1) Ambulatory surgical center (ASC) means any center, service, office facility, or other entity that:
 .1 Definitions. Subtitle 09 WORKERS' COMPENSATION COMMISSION 14.09.08 Guide of Medical and Surgical Fees Authority: Labor and Employment Article, 9-309, 9-663 and 9-731, Annotated Code of Maryland Effective
.1 Definitions. Subtitle 09 WORKERS' COMPENSATION COMMISSION 14.09.08 Guide of Medical and Surgical Fees Authority: Labor and Employment Article, 9-309, 9-663 and 9-731, Annotated Code of Maryland Effective
Newly Payable Workers Compensation Codes for Non-Face-to-Face Service. CPT / l 1
 CPT 99358 & 99359 Newly Payable Workers Compensation Codes for Non-Face-to-Face Service DaisyBill 2017 CPT 99358 / 99359 l 1 Ask Questions!? DaisyBill 2017 CPT 99358 / 99359 l 2 Really, We Love Questions?
CPT 99358 & 99359 Newly Payable Workers Compensation Codes for Non-Face-to-Face Service DaisyBill 2017 CPT 99358 / 99359 l 1 Ask Questions!? DaisyBill 2017 CPT 99358 / 99359 l 2 Really, We Love Questions?
Adjunct Professional Services Policy
 Policy Number 2017R7114C Adjunct Professional Services Policy Annual Approval Date 11/9/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Policy Number 2017R7114C Adjunct Professional Services Policy Annual Approval Date 11/9/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Payment Policy Medicine
 Payment Policy Medicine 01/01/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck ND 58506-5585 701-328-3800 800-777-5033 www.workforcesafety.com Copyright Notice The five character codes included in the
Payment Policy Medicine 01/01/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck ND 58506-5585 701-328-3800 800-777-5033 www.workforcesafety.com Copyright Notice The five character codes included in the
New procedure in workers compensation for pre-designation of your personal physician.
 Date: To All Employees: RE: New procedure in workers compensation for pre-designation of your personal physician. As of April 19, 2004, the California Legislature enacted Senate Bill 899. This bill has
Date: To All Employees: RE: New procedure in workers compensation for pre-designation of your personal physician. As of April 19, 2004, the California Legislature enacted Senate Bill 899. This bill has
Payment Policy: Code Editing Overview Reference Number: CC.PP.011 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 06/28/2018
 Payment Policy: Code Editing Overview Reference Number: CC.PP.011 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 06/28/2018 Coding Implications Revision Log See Important Reminder at the
Payment Policy: Code Editing Overview Reference Number: CC.PP.011 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 06/28/2018 Coding Implications Revision Log See Important Reminder at the
Professional/Technical Component Policy, Professional
 Professional/Technical Component Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R0012F Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT
Professional/Technical Component Policy, Professional REIMBURSEMENT POLICY Policy Number 2018R0012F Annual Approval Date 7/11/2018 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT
Adjunct Professional Services Policy
 Policy Number 2017R7114K Adjunct Professional Services Policy Annual Approval Date 11/9/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Policy Number 2017R7114K Adjunct Professional Services Policy Annual Approval Date 11/9/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission
Multiple Procedure Payment Reduction (MPPR) for Medical and Surgical Services Policy, Professional
 REIMBURSEMENT POLICY CMS-1500 Multiple Payment Reduction (MPPR) for Medical and Surgical Services Policy, Professional Policy Number 2019R0034B Annual Approval Date 7/11/2018 Approved By Reimbursement
REIMBURSEMENT POLICY CMS-1500 Multiple Payment Reduction (MPPR) for Medical and Surgical Services Policy, Professional Policy Number 2019R0034B Annual Approval Date 7/11/2018 Approved By Reimbursement
-1- BEFORE THE DEPARTMENT OF LABOR AND INDUSTRY STATE OF MONTANA ) ) ) ) ) ) ) ) )
 -1- BEFORE THE DEPARTMENT OF LABOR AND INDUSTRY STATE OF MONTANA In the matter of the adoption of NEW RULES I through IV, and the amendment of ARM 24.29.1401A, 24.29.1402, 24.29.1406, 24.29.1432, 24.29.1510,
-1- BEFORE THE DEPARTMENT OF LABOR AND INDUSTRY STATE OF MONTANA In the matter of the adoption of NEW RULES I through IV, and the amendment of ARM 24.29.1401A, 24.29.1402, 24.29.1406, 24.29.1432, 24.29.1510,
Multiple Procedure Policy
 Policy Policy Number 2018R0034C Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate claims. This
Policy Policy Number 2018R0034C Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS You are responsible for submission of accurate claims. This
Claims and Billing Manual
 2019 Claims and Billing Manual ProviDRs Care 1/2019 1 Contents Introduction... 3 How to Use This Manual... 3 About WPPA, Inc. dba ProviDRs Care... 3 How to Contact ProviDRs Care... 3 ProviDRs Care Network
2019 Claims and Billing Manual ProviDRs Care 1/2019 1 Contents Introduction... 3 How to Use This Manual... 3 About WPPA, Inc. dba ProviDRs Care... 3 How to Contact ProviDRs Care... 3 ProviDRs Care Network
Modifier 22 - Increased Procedural Services
 Manual: Policy Title: Reimbursement Policy Modifier 22 - Increased Procedural Services Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM007 Last Updated: 7/10/2017 Last Reviewed:
Manual: Policy Title: Reimbursement Policy Modifier 22 - Increased Procedural Services Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM007 Last Updated: 7/10/2017 Last Reviewed:
Modifier 22 - Increased Procedural Services
 Manual: Policy Title: Reimbursement Policy Modifier 22 - Increased Procedural Services Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM007 Last Updated: 3/17/2018 Last Reviewed:
Manual: Policy Title: Reimbursement Policy Modifier 22 - Increased Procedural Services Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM007 Last Updated: 3/17/2018 Last Reviewed:
Payment Policy Medicine
 Payment Policy Medicine 01/01/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck ND 58506-5585 701-328-3800 800-777-5033 www.workforcesafety.com Copyright Notice The five character codes included in the
Payment Policy Medicine 01/01/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck ND 58506-5585 701-328-3800 800-777-5033 www.workforcesafety.com Copyright Notice The five character codes included in the
Multiple Procedure Payment Reduction (MPPR) for Surgical Procedures
 Policy Number MPS04242013RP Approved By UnitedHealthcare Medicare Committee Current Approval Date 03/26/2014 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare
Policy Number MPS04242013RP Approved By UnitedHealthcare Medicare Committee Current Approval Date 03/26/2014 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to UnitedHealthcare
Professional/Technical Component Policy
 Professional/Technical Component Policy Policy Number 2018R0012A Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are
Professional/Technical Component Policy Policy Number 2018R0012A Annual Approval Date 7/12/2017 Approved By Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY You are
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION
 RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-06 GENERAL RULES OF THE WORKERS COMPENSATION PROGRAM TABLE OF CONTENTS 0800-02-06-.01 Definitions
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-06 GENERAL RULES OF THE WORKERS COMPENSATION PROGRAM TABLE OF CONTENTS 0800-02-06-.01 Definitions
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER MEDICAL COST CONTAINMENT PROGRAM
 RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-17 MEDICAL COST CONTAINMENT PROGRAM TABLE OF CONTENTS 0800-02-17-.01 Purpose and Scope
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-17 MEDICAL COST CONTAINMENT PROGRAM TABLE OF CONTENTS 0800-02-17-.01 Purpose and Scope
Professional/Technical Component Policy Annual Approval Date
 Policy Number 2018R0012B Professional/Technical Component Policy Annual Approval Date 7/13/2017 Approved By REIMBURSEMENT POLICY CMS-1500 Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS
Policy Number 2018R0012B Professional/Technical Component Policy Annual Approval Date 7/13/2017 Approved By REIMBURSEMENT POLICY CMS-1500 Reimbursement Policy Oversight Committee IMPORTANT NOTE ABOUT THIS
Florida Medicaid Fee Schedule Overview. Bureau of Medicaid Policy Agency for Health Care Administration March 20, :00 3:00 pm
 Florida Medicaid Fee Schedule Overview Bureau of Medicaid Policy Agency for Health Care Administration March 20, 2018 2:00 3:00 pm Disclaimer The information provided in this presentation is only intended
Florida Medicaid Fee Schedule Overview Bureau of Medicaid Policy Agency for Health Care Administration March 20, 2018 2:00 3:00 pm Disclaimer The information provided in this presentation is only intended
Florida Workers Compensation
 Florida Workers Compensation Reimbursement Manual for Ambulatory Surgical Centers Rule 69L-7.100, F.A.C. 2015 Edition THIS PAGE LEFT INTENTIONALLY BLANK 2015 Edition Page 2 of 42 Effective Date TBD TABLE
Florida Workers Compensation Reimbursement Manual for Ambulatory Surgical Centers Rule 69L-7.100, F.A.C. 2015 Edition THIS PAGE LEFT INTENTIONALLY BLANK 2015 Edition Page 2 of 42 Effective Date TBD TABLE
Yes, written or oral approval is required, based upon medical policies.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhc.com/calpers or by calling 1-877-359-3714. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhc.com/calpers or by calling 1-877-359-3714. Important
INTRODUCTION_final doc Revision Date: 1/1/2018 INTRODUCTION FOR NATIONAL CORRECT CODING INITIATIVE POLICY MANUAL FOR MEDICARE SERVICES
 INTRODUCTION_final10312017.doc Revision Date: 1/1/2018 INTRODUCTION FOR NATIONAL CORRECT CODING INITIATIVE POLICY MANUAL FOR MEDICARE SERVICES Current Procedural Terminology (CPT) codes, descriptions and
INTRODUCTION_final10312017.doc Revision Date: 1/1/2018 INTRODUCTION FOR NATIONAL CORRECT CODING INITIATIVE POLICY MANUAL FOR MEDICARE SERVICES Current Procedural Terminology (CPT) codes, descriptions and
Reimbursement Policy Subject: Modifier 26 and TC: Professional and Technical Component Coding 07/01/17 08/01/16 Policy
 Reimbursement Policy Subject: Modifier 26 and TC: Professional and Technical Component Effective Date: Committee Approval Obtained: Section: Coding 07/01/17 08/01/16 *****The most current version of the
Reimbursement Policy Subject: Modifier 26 and TC: Professional and Technical Component Effective Date: Committee Approval Obtained: Section: Coding 07/01/17 08/01/16 *****The most current version of the
Modifier 50 - Bilateral Procedure
 Manual: Policy Title: Reimbursement Policy Modifier 50 - Bilateral Procedure Section: Modifier Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM057 Last Updated: 4/6/2018 Last Reviewed: 4/11/2018
Manual: Policy Title: Reimbursement Policy Modifier 50 - Bilateral Procedure Section: Modifier Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM057 Last Updated: 4/6/2018 Last Reviewed: 4/11/2018
Ch. 127 MEDICAL COST CONTAINMENT CHAPTER 127. WORKERS COMPENSATION MEDICAL COST CONTAINMENT
 Ch. 127 MEDICAL COST CONTAINMENT 34 127.1 CHAPTER 127. WORKERS COMPENSATION MEDICAL COST CONTAINMENT Subch. Sec. A. PRELIMINARY PROVISIONS... 127.1 B. MEDICAL FEES AND FEE REVIEW... 127.101 C. MEDICAL
Ch. 127 MEDICAL COST CONTAINMENT 34 127.1 CHAPTER 127. WORKERS COMPENSATION MEDICAL COST CONTAINMENT Subch. Sec. A. PRELIMINARY PROVISIONS... 127.1 B. MEDICAL FEES AND FEE REVIEW... 127.101 C. MEDICAL
MULTIPLE PROCEDURES POLICY
 Oxford MULTIPLE PROCEDURES POLICY UnitedHealthcare Oxford Reimbursement Policy Policy Number: SURGERY 022.34 T0 Effective Date: January 22, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 APPLICABLE
Oxford MULTIPLE PROCEDURES POLICY UnitedHealthcare Oxford Reimbursement Policy Policy Number: SURGERY 022.34 T0 Effective Date: January 22, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 APPLICABLE
Modifier 52 - Reduced Services
 Manual: Policy Title: Reimbursement Policy Modifier 52 - Reduced Services Section: Modifiers Subsection: None Date of Origin: 9/13/2007 Policy Number: RPM003 Last Updated: 3/6/2017 Last Reviewed: 3/9/2017
Manual: Policy Title: Reimbursement Policy Modifier 52 - Reduced Services Section: Modifiers Subsection: None Date of Origin: 9/13/2007 Policy Number: RPM003 Last Updated: 3/6/2017 Last Reviewed: 3/9/2017
29:10 NORTH CAROLINA REGISTER NOVEMBER 17,
 Note from the Codifier: The notices published in this Section of the NC Register include the text of proposed rules. The agency must accept comments on the proposed rule(s) for at least 60 days from the
Note from the Codifier: The notices published in this Section of the NC Register include the text of proposed rules. The agency must accept comments on the proposed rule(s) for at least 60 days from the
Section: Administrative Subsection: None Date of Origin: 1/22/2004 Policy Number: RPM002 Last Updated: 1/6/2017 Last Reviewed: 1/18/2017
 Manual: Policy Title: Reimbursement Policy Clinical Editing Section: Administrative Subsection: None Date of Origin: 1/22/2004 Policy Number: RPM002 Last Updated: 1/6/2017 Last Reviewed: 1/18/2017 IMPORTANT
Manual: Policy Title: Reimbursement Policy Clinical Editing Section: Administrative Subsection: None Date of Origin: 1/22/2004 Policy Number: RPM002 Last Updated: 1/6/2017 Last Reviewed: 1/18/2017 IMPORTANT
New Psychiatric Services Procedure Codes for 2013 HCPCS Now Available
 New Psychiatric Services Procedure Codes for 2013 HCPCS Now Available Information posted December 21, 2012 The 2013 Healthcare Common Procedure Coding System (HCPCS) additions, changes, and deletions for
New Psychiatric Services Procedure Codes for 2013 HCPCS Now Available Information posted December 21, 2012 The 2013 Healthcare Common Procedure Coding System (HCPCS) additions, changes, and deletions for
Reimbursement Policy Subject: Modifier 26 and TC: Professional and Technical Component Coding 07/01/17 08/01/16 https://mediproviders.anthem.
 Anthem Blue Cross Blue Shield Medicaid Reimbursement Policy Subject: Effective Date: 07/01/17 Committee Approval Obtained: 08/01/16 Section: Coding ***** The most current version of our reimbursement policies
Anthem Blue Cross Blue Shield Medicaid Reimbursement Policy Subject: Effective Date: 07/01/17 Committee Approval Obtained: 08/01/16 Section: Coding ***** The most current version of our reimbursement policies
Amended Date: October 1, Table of Contents
 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 1.1.1 Telemedicine... 1 1.1.2 Telepsychiatry... 1 1.1.3 Service Sites... 1 1.1.4 Providers... 1 2.0 Eligibility
Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 1.1.1 Telemedicine... 1 1.1.2 Telepsychiatry... 1 1.1.3 Service Sites... 1 1.1.4 Providers... 1 2.0 Eligibility
Payment Policy: Clinical Validation of Modifer 25 Reference Number: CC.PP.013 Product Types: ALL
 Payment Policy: Clinical Validation of Modifer 25 Reference Number: CC.PP.013 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 02/24/2018 Coding Implications Revision Log See Important Reminder
Payment Policy: Clinical Validation of Modifer 25 Reference Number: CC.PP.013 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 02/24/2018 Coding Implications Revision Log See Important Reminder
Payment Policy:Modifier to Procedure Code Validation: Payment Modifiers Reference Number: CC.PP.028
 Payment Policy:: Payment Modifiers Reference Number: CC.PP.028 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 02/23/2018 See Important Reminder at the end of this policy for important
Payment Policy:: Payment Modifiers Reference Number: CC.PP.028 Product Types: ALL Effective Date: 01/01/2013 Last Review Date: 02/23/2018 See Important Reminder at the end of this policy for important
ANALYSIS OF THE PROPOSED CHANGES TO THE FLORIDA WORKERS COMPENSATION HEALTH CARE PROVIDER REIMBURSMENT MANUAL EFFECTIVE UPON ADOPTION
 NCCI estimates that the proposed changes to the Florida Workers Compensation Health Care Provider Reimbursement Manual (FWCRM) would result in an overall Florida workers compensation system cost impact
NCCI estimates that the proposed changes to the Florida Workers Compensation Health Care Provider Reimbursement Manual (FWCRM) would result in an overall Florida workers compensation system cost impact
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER RULES FOR MEDICAL PAYMENTS
 RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-17 RULES FOR MEDICAL PAYMENTS TABLE OF CONTENTS 0800-02-17-.01 Purpose and Scope 0800-02-17-.02
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-17 RULES FOR MEDICAL PAYMENTS TABLE OF CONTENTS 0800-02-17-.01 Purpose and Scope 0800-02-17-.02
RESEARCH UPDATE. Analysis of California Workers Compensation Reforms
 December 2007 RESEARCH UPDATE Analysis of California Workers Compensation Reforms Part 1: Medical Utilization & Reimbursement Outcomes Accident Years 2002-2006 Claims Experience by Alex Swedlow, MHSA and
December 2007 RESEARCH UPDATE Analysis of California Workers Compensation Reforms Part 1: Medical Utilization & Reimbursement Outcomes Accident Years 2002-2006 Claims Experience by Alex Swedlow, MHSA and
Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy
 Policy Number Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy 2017R0125B Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight
Policy Number Multiple Procedure Payment Reduction (MPPR) for Diagnostic Cardiovascular and Ophthalmology Procedures Policy 2017R0125B Annual Approval Date 3/8/2017 Approved By Reimbursement Policy Oversight
Adult Preventive Medicine Clinical Coverage Policy No.: 1A-2 Annual Health Assessment Amended Date: October 1, 2015.
 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
$1,500 Individual/$3,000 Family for participating providers. $3,000 Individual/$6,000. Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
Sexually Transmitted Disease Treatment Clinical Coverage Policy No: 1D-2 Provided in Health Departments Amended Date: October 1, 2015
 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
CHAP13-CPTcodes0001T-0999T_final doc Revision Date: 1/1/2017
 CHAP13-CPTcodes0001T-0999T_final103116.doc Revision Date: 1/1/2017 CHAPTER XIII Category III Codes CPT Codes 0001T 0999T FOR NATIONAL CORRECT CODING INITIATIVE POLICY MANUAL FOR MEDICARE SERVICES Current
CHAP13-CPTcodes0001T-0999T_final103116.doc Revision Date: 1/1/2017 CHAPTER XIII Category III Codes CPT Codes 0001T 0999T FOR NATIONAL CORRECT CODING INITIATIVE POLICY MANUAL FOR MEDICARE SERVICES Current
INDIVIDUAL PRACTICE ASSOCIATION MEDICAL GROUP OF SANTA CLARA COUNTY (SCCIPA)
 INDIVIDUAL PRACTICE ASSOCIATION MEDICAL GROUP OF SANTA CLARA COUNTY (SCCIPA) AB 1455 Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455,
INDIVIDUAL PRACTICE ASSOCIATION MEDICAL GROUP OF SANTA CLARA COUNTY (SCCIPA) AB 1455 Downstream Provider Notice CLAIMS SETTLEMENT PRACTICES & DISPUTE RESOLUTION MECHANISM As required by Assembly Bill 1455,
Billing for Rehabilitation Services
 Billing for Rehabilitation Services Julia R. Olson, CPC Austin-Webster Group, Ltd julolson@gmail.com (651) 430-1850 Disclaimer The information contained in this booklet is designed to provide accurate
Billing for Rehabilitation Services Julia R. Olson, CPC Austin-Webster Group, Ltd julolson@gmail.com (651) 430-1850 Disclaimer The information contained in this booklet is designed to provide accurate
National Correct Coding Initiative
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE National Correct Coding Initiative L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 0 P U B L I S H E D : D E C E M B E R 1
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE National Correct Coding Initiative L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 0 P U B L I S H E D : D E C E M B E R 1
UniCare ClaimsXten TM Rules (Version 4.4) Effective February 15, 2013
 UniCare ClaimsXten TM Rules (Version 4.4) Effective February 15, 2013 Rules Edit logic Example Supported After Hours 99050 not Reimbursable with Preventive Diagnosis Qualitative Drug Screening This will
UniCare ClaimsXten TM Rules (Version 4.4) Effective February 15, 2013 Rules Edit logic Example Supported After Hours 99050 not Reimbursable with Preventive Diagnosis Qualitative Drug Screening This will
Important Questions Answers Why this Matters:
 Student Employee Health Plan: NYS Health Insurance Program Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual or Family
Student Employee Health Plan: NYS Health Insurance Program Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual or Family
Florida Medicaid Fee Schedule Overview
 Florida Medicaid Fee Schedule Overview Bureau of Medicaid Policy Agency for Health Care Administration Fall 2017 Disclaimer The information provided in this presentation is only intended to be general
Florida Medicaid Fee Schedule Overview Bureau of Medicaid Policy Agency for Health Care Administration Fall 2017 Disclaimer The information provided in this presentation is only intended to be general
General Ophthalmological Services Clinical Coverage Policy No: 1T-1 Amended Date: October 1, Table of Contents
 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
P.L. 2005, CHAPTER 172, approved August 5, 2005 Assembly, No (First Reprint)
 P.L. 00, CHAPTER, approved August, 00 Assembly, No. (First Reprint) - C.:S-. - Note to - 0 0 0 AN ACT concerning managed behavioral health care services and amending and supplementing P.L., c.. BE IT ENACTED
P.L. 00, CHAPTER, approved August, 00 Assembly, No. (First Reprint) - C.:S-. - Note to - 0 0 0 AN ACT concerning managed behavioral health care services and amending and supplementing P.L., c.. BE IT ENACTED
Payment Policy: Unbundled Professional Services Reference Number: CC.PP.043 Product Types: ALL
 Payment Policy: Reference Number: CC.PP.043 Product Types: ALL Effective Date: 01/01/2014 Last Review Date: 03/01/2018 Coding Implications Revision Log See Important Reminder at the end of this policy
Payment Policy: Reference Number: CC.PP.043 Product Types: ALL Effective Date: 01/01/2014 Last Review Date: 03/01/2018 Coding Implications Revision Log See Important Reminder at the end of this policy
Important Questions Answers Why this Matters:
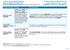 Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
What is the overall deductible? are separate and do not. towards each other. Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
UnitedHealthcare Medicare Advantage Reimbursement Policy CMS 1500 Multiple Procedure Payment Reduction (MPPR) for Therapy Services Policy
 Multiple Procedure Payment Reduction (MPPR) for Therapy Services Policy Policy Number Annual Approval Date 3/14/2018 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This
Multiple Procedure Payment Reduction (MPPR) for Therapy Services Policy Policy Number Annual Approval Date 3/14/2018 Approved By Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This
Chapter 3 Section 1. Reimbursement Of Individual Health Care Professionals And Other Non-Institutional Health Care Providers
 Operational Requirements Chapter 3 Section 1 Reimbursement Of Individual Health Care Professionals And Other Issue Date: Authority: 1.0 GENERAL 1.1 TRICARE reimbursement of a non-network individual health
Operational Requirements Chapter 3 Section 1 Reimbursement Of Individual Health Care Professionals And Other Issue Date: Authority: 1.0 GENERAL 1.1 TRICARE reimbursement of a non-network individual health
HealthKeepers, Inc. Anthem HealthKeepers University of Virginia Physicians Group Anthem HealthKeepers- $750/$1,500 deductible
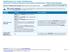 HealthKeepers, Inc. Anthem HealthKeepers University of Virginia Physicians Group Anthem HealthKeepers- $750/$1,500 deductible Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
HealthKeepers, Inc. Anthem HealthKeepers University of Virginia Physicians Group Anthem HealthKeepers- $750/$1,500 deductible Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
MULTIPLE PROCEDURE PAYMENT REDUCTION (MPPR) FOR DIAGNOSTIC CARDIOVASCULAR AND OPHTHALMOLOGY PROCEDURES POLICY
 UnitedHealthcare Oxford Reimbursement Policy MULTIPLE PROCEDURE PAYMENT REDUCTION (MPPR) FOR DIAGNOSTIC CARDIOVASCULAR AND OPHTHALMOLOGY PROCEDURES POLICY Policy Number: ADMINISTRATIVE 258.2 T0 Effective
UnitedHealthcare Oxford Reimbursement Policy MULTIPLE PROCEDURE PAYMENT REDUCTION (MPPR) FOR DIAGNOSTIC CARDIOVASCULAR AND OPHTHALMOLOGY PROCEDURES POLICY Policy Number: ADMINISTRATIVE 258.2 T0 Effective
Issue Comment Response Commenter
 Regulation 9789.12.1 (Scope and applicability of the physician fee schedule Issue Comment Response Commenter Inform which version of the physician fee schedule should be used by date of service Commenter
Regulation 9789.12.1 (Scope and applicability of the physician fee schedule Issue Comment Response Commenter Inform which version of the physician fee schedule should be used by date of service Commenter
Important Questions Answers Why this Matters:
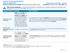 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4902. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4902. Important Questions
Oregon Medical Fee and Payment Rules Oregon Administrative Rules Chapter 436, Division 009
 Oregon Medical Fee and Payment Rules Oregon Administrative Rules Chapter 436, Division 009 Rule Proposed TABLE OF CONTENTS Page 436-009-0015 Limitations on Medical Billings... 1 436-009-0050 CPT Sections...
Oregon Medical Fee and Payment Rules Oregon Administrative Rules Chapter 436, Division 009 Rule Proposed TABLE OF CONTENTS Page 436-009-0015 Limitations on Medical Billings... 1 436-009-0050 CPT Sections...
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 Anthem Blue Cross CSEBA Classic HMO-6-C Coverage Period: 07/01/2016-06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HMO This
Anthem Blue Cross CSEBA Classic HMO-6-C Coverage Period: 07/01/2016-06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HMO This
Corporate Reimbursement Policy
 Corporate Reimbursement Policy File Name: Origination: Last Review: Next Review: modifier_guidelines 1/2000 11/2017 11/2018 Description Policy A modifier enables a provider to report that a service or
Corporate Reimbursement Policy File Name: Origination: Last Review: Next Review: modifier_guidelines 1/2000 11/2017 11/2018 Description Policy A modifier enables a provider to report that a service or
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
1199SEIU National Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs
 1199SEIU National Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Wage Classes I & II and Early Retirees with
1199SEIU National Benefit Fund Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Wage Classes I & II and Early Retirees with
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-309-2955. Important Questions
Summary of Benefits and Coverage for Assurant Health individual major medical Bronze plans
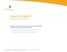 Assurant Health Time Insurance Company Summary of Benefits and Coverage for Assurant Health individual major medical Bronze plans View Summary of Benefits and Coverage for an individual plan View Summary
Assurant Health Time Insurance Company Summary of Benefits and Coverage for Assurant Health individual major medical Bronze plans View Summary of Benefits and Coverage for an individual plan View Summary
Anthem BlueCross BlueShield Christian Care Communities Blue Access PPO Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Summary of Benefits and Coverage for Assurant Health individual major medical Bronze plans
 Assurant Health Time Insurance Company Summary of Benefits and Coverage for Assurant Health individual major medical Bronze plans View Summary of Benefits and Coverage for an individual plan View Summary
Assurant Health Time Insurance Company Summary of Benefits and Coverage for Assurant Health individual major medical Bronze plans View Summary of Benefits and Coverage for an individual plan View Summary
CA UHC Bronze Plus EVN/3J8 Summary of Benefits and Coverage: What This Plan Covers & What it Costs
 CA UHC Bronze Plus EVN/3J8 Summary of Benefits and Coverage: What This Plan Covers & What it Costs Coverage Period: 12/01/2016 11/30/2017 Coverage for: All Coverage Tiers Plan Type: HMO Important Questions
CA UHC Bronze Plus EVN/3J8 Summary of Benefits and Coverage: What This Plan Covers & What it Costs Coverage Period: 12/01/2016 11/30/2017 Coverage for: All Coverage Tiers Plan Type: HMO Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Regence BlueCross BlueShield of Oregon: Preferred Coverage Period: 07/01/ /31/2016
 Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
Important Questions Answers Why this Matters:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
California Workers Compensation Aggregate Medical Payment Trends 2016 Update
 August 24, 2017 California Workers Compensation Aggregate Medical Payment Trends 2016 Update 1 California Workers Compensation Aggregate Medical Payment Trends 2016 Update I. Executive Summary This report
August 24, 2017 California Workers Compensation Aggregate Medical Payment Trends 2016 Update 1 California Workers Compensation Aggregate Medical Payment Trends 2016 Update I. Executive Summary This report
You must pay all of the costs for these services up to the specific deductible amount before the plan begins to pay for these services.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
IWDCNE Health and Welfare Plan: Active Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 IWDCNE Health and Welfare Plan: Active Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: Beginning on or after 1/1/2016 Coverage for: All Coverage Types This
IWDCNE Health and Welfare Plan: Active Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: Beginning on or after 1/1/2016 Coverage for: All Coverage Types This
University of Virginia Physicians Group: Anthem HealthKeepers- $750/$1,500 Deductible Coverage Period: 07/01/ /30/2017
 University of Virginia Physicians Group: Anthem HealthKeepers- $750/$1,500 Deductible Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016-06/30/2017 Coverage
University of Virginia Physicians Group: Anthem HealthKeepers- $750/$1,500 Deductible Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016-06/30/2017 Coverage
Address: 220 French Landing Drive, 1-B, Nashville, TN Phone:
 Department of State Division of Publications 312 Rosa L. Parks, 8th Floor SnodgrassfTN Tower Nashville, TN 37243 ' Phone: 615.741.2650 Email: publications.information@tn.gov For Department of State Use
Department of State Division of Publications 312 Rosa L. Parks, 8th Floor SnodgrassfTN Tower Nashville, TN 37243 ' Phone: 615.741.2650 Email: publications.information@tn.gov For Department of State Use
Your Plan: BCBSHP Essential DirectAccess gjia Your Network: Blue Open Access POS 10NR S-OAP2 4K/20 6.3K p1
 Your Plan: BCBSHP Essential DirectAccess gjia Your Network: Blue Open Access POS 10NR S-OAP2 4K/20 6.3K p1 This summary of benefits is a brief outline of coverage, designed to help you with the selection
Your Plan: BCBSHP Essential DirectAccess gjia Your Network: Blue Open Access POS 10NR S-OAP2 4K/20 6.3K p1 This summary of benefits is a brief outline of coverage, designed to help you with the selection
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
How are allowable charge determinations to be made in the determination of reimbursement for 1992 and forward?
 ALLOWABLE CHARGES CHAPTER 5 SECTION 3 ALLOWABLE CHARGES - CHAMPUS MAXIMUM ALLOWABLE CHARGES (CMAC) ISSUE DATE: March 3, 1992 AUTHORITY: 32 CFR 199.14 I. APPLICABILITY This policy is mandatory for reimbursement
ALLOWABLE CHARGES CHAPTER 5 SECTION 3 ALLOWABLE CHARGES - CHAMPUS MAXIMUM ALLOWABLE CHARGES (CMAC) ISSUE DATE: March 3, 1992 AUTHORITY: 32 CFR 199.14 I. APPLICABILITY This policy is mandatory for reimbursement
: Federal Employees Standard Option Coverage Period: 01/01/ /31/2017 Summary of Benefits and Coverage
 This is only a summary. Please read the FEHB Plan brochure (RI 73-815) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 73-815) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Coverage for: All Coverage Tiers Plan Type: POS. 1 of 9
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.paramounthealthcare.com or by calling 1-800-462-3589.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.paramounthealthcare.com or by calling 1-800-462-3589.
Important Questions Answers Why this Matters: For PPO Providers: $1,500 Member/$3,000 Family For Non-PPO Providers:
 Anthem Blue Cross Life and Health Insurance Company ACWA / JPIA: Account Based Health Plan (EV85) Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
Anthem Blue Cross Life and Health Insurance Company ACWA / JPIA: Account Based Health Plan (EV85) Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it
Anthem BlueCross BlueShield Eastern Kentucky University Economy Coverage Period: {01/01/ /31/2013} Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. For prescription
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. For prescription
$1,500 Individual/$3,000 Family for In-Network providers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-877-244-3593. HRA FUNDING
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-877-244-3593. HRA FUNDING
Full PPO Savings Two-Tier Embedded Deductible 2250/2700/4500 Effective January 1, 2019
 Benefit Modification for Members with Full PPO Savings Two-Tier Embedded Deductible 2250/2700/4500 Effective January 1, 2019 This chart is a summary of specific benefit changes to your plan. For a list
Benefit Modification for Members with Full PPO Savings Two-Tier Embedded Deductible 2250/2700/4500 Effective January 1, 2019 This chart is a summary of specific benefit changes to your plan. For a list
1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs
 1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Rochester Area Employers
1199SEIU National Benefit Fund for Rochester Area Members Summary of Benefits and Coverage: What This Plan Covers and What It Costs Coverage Period: Beginning 04/01/2014 Coverage for: Rochester Area Employers
HMSA: Catastrophic Plan
 HMSA: Catastrophic Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual Plan Type: PPO This is only a summary. If
HMSA: Catastrophic Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual Plan Type: PPO This is only a summary. If
CRCS Exam Study Manual Update for 2017
 CRCS Exam Study Manual Update for 2017 This document reflects updates made to the instructional content from the Certified Revenue Cycle Specialist (CRCS-I, CRCS-P) Exam Study Manual - 2016 to the 2017
CRCS Exam Study Manual Update for 2017 This document reflects updates made to the instructional content from the Certified Revenue Cycle Specialist (CRCS-I, CRCS-P) Exam Study Manual - 2016 to the 2017
Upper Arlington City School District: Lumenos Health Savings Accounts Coverage Period: 01/01/ /31/2016
 Upper Arlington City School District: Lumenos Health Savings Accounts Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
Upper Arlington City School District: Lumenos Health Savings Accounts Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
Reopening and Redetermination Submissions
 A CMS Medicare Administrative Contractor http://www.ngsmedicare.com Reopening and Redetermination Submissions Understanding your next steps are very important for quick reimbursement and providers are
A CMS Medicare Administrative Contractor http://www.ngsmedicare.com Reopening and Redetermination Submissions Understanding your next steps are very important for quick reimbursement and providers are
Some of the services this plan doesn t cover are listed on pages 5. See your policy Yes. doesn t cover?
 Molina Healthcare of Florida, Inc.: Molina Silver 100 Plan Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family
Molina Healthcare of Florida, Inc.: Molina Silver 100 Plan Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family
