INSTITUTE OF MEDICINE COMMITTEE ON THE DETERMINATION OF ESSENTIAL HEALTH BENEFITS
|
|
|
- James Jenkins
- 5 years ago
- Views:
Transcription
1 COMMENTS 1310 G Street, N.W. Washington, D.C Fax Before the INSTITUTE OF MEDICINE COMMITTEE ON THE DETERMINATION OF ESSENTIAL HEALTH BENEFITS On How Insurers Make Determinations of Benefit Design, Necessity and Coverage Submitted by: Virginia Calega, MD, MBA Vice President of Medical Management and Policy Highmark Blue Cross and Blue Shield January 13, 2011
2 Introduction My name is Virginia Calega and I am the Vice President of Medical Management and Policy at Highmark Blue Cross and Blue Shield of Pennsylvania. I would like to thank you for the opportunity to be part of this panel today to discuss how insurers develop benefits and determine medical necessity for covered benefits. I am here today representing the Blue Cross and Blue Shield Association (BCBSA). BCBSA is a national federation of 39 independent, community-based Blue Cross and Blue Shield companies that collectively provide health care coverage for more than 98 million individuals one in three Americans. Highmark is a nonprofit, independent licensee of BCBSA with 4.7 million members in Western and Central Pennsylvania and West Virginia. We offer HMO, PPO, HDHP, Medicare Advantage and individual products to our members. At Highmark, I have the responsibility for managing our medical policies for our commercial products. I also oversee medical management activities for our commercial, CHIP and Medicare Advantage lines of business, behavioral health, and pharmacy. This role allows me to positively impact a larger population of patients than when I was in private practice as an internist and geriatrician. The work of this committee is critical to the implementation of the Patient Protection and Affordable Care Act ( ACA ). Any definition of an essential health benefit must balance the need to provide reasonable, appropriate, high quality coverage with the need to assure affordability and access to care for consumers. The definition of essential heath benefits will primarily impact individual consumers, small businesses and the self employed, who will be the main customers for the state-based Exchanges beginning in 2014; therefore, it is important that the initial scope of the essential health benefits package reflect the typical employer plan of small businesses. Research indicates that buyers in the individual and small group markets are especially sensitive to price as individuals in such plans bear much of the premium cost. A definition that is overly inclusive and does not require a sound evidence base for essential health benefits could negatively impact affordability for consumers. 2
3 In my remarks today, I will describe the industry practice for developing benefit designs and products. I will also explain Highmark s practice for determining medical necessity and benefit coverage (which is driven by evidence-based research, national standards and collaboration with the provider community). Based on our experience, Highmark and BCBSA recommend that: o Any definition of essential health benefits must preserve an insurers ability to utilize medical management tools, including medical necessity tools. These tools are critical to ensuring individuals receive safe, effective, and appropriate services, while maximizing affordability for consumers; and o The process through which essential health benefits are identified and updated be based upon evidence-based research and market-based input. Industry Practice for Benefit Designs and Product Development At Highmark, benefit design is a critical element of the product development process that involves the participation of several areas of the company and relies on information from various external data sources. Benefit designs both influence and are influenced by premiums in the process of creating products that offer meaningful coverage at an affordable price. Where the cost of an added benefit requires an increase in premium that may impact an individual s access to coverage, issuers must have the flexibility to adjust the benefit structure to ensure that individuals have access to necessary care at an affordable cost. For example, adjustments in cost-sharing (such as copayments or co-insurance) may be required as a result of adding a benefit in order to offer the coverage at an affordable cost. The benefit design and overall product development process includes input from various internal business areas and the analysis of internal and external data. o Customer. We collect market research from several sources to ensure that our coverage and premiums match market demand throughout different market segments. For example, information gathered from consumer focus groups as well as customer satisfaction surveys provide direct input from members and potential customers on market demand for different benefit designs and specific 3
4 benefits. Insurance brokers and sales representatives also provide critical information on market demand. o Internal Performance Reviews. Senior leadership conducts ongoing review and analysis of product portfolio performance, which includes analysis of sales data and medical trends by geographic area, product type and benefit type. This data is a direct indicator of existing consumer preferences and is essential to predicting future trends to ensure that products meet the needs of customers. o Changes in Medical Treatment. Medical Management staff, comprised of board certified physicians, registered nurses and other health professionals, continually review medical literature and collaborate with providers on an ongoing basis to identify any new treatments or changes in medical protocols that may necessitate a change in benefits. o Product Portfolio Analysis. The entire product portfolio is continually reviewed to ensure that consumers are provided with a broad choice of products at different premium levels. As I ve outlined, product development is an iterative process that requires continual collection and analysis of a variety of data to ensure that meaningful coverage at a variety of price points can be offered across different markets. Industry Practice for Determinations of Necessity and Benefit Coverage The primary goal of using medical necessity to determine coverage of benefits for a patient is to ensure that members receive the most appropriate care at the right time and in the right setting. Published research from the Dartmouth Atlas and other sources reveal that where evidence-based protocols are not utilized to support the decision making process, variations in the delivery of care across the country result. Procedures that are potentially more intensive or harmful are may be performed rather than alternatives procedures which provide the same or similar beneficial results with less risk. To ensure that consumers receive the most appropriate, safe and effective care, Highmark and other insurers utilize evidence-based medical necessity protocols. 4
5 In general, health care services, tests, procedures or medical supplies are deemed to be medically necessary, and therefore covered, if a provider, exercising prudent clinical judgment, would provide such services to a patient and such services are: o in accordance with generally accepted standards of medical practice; o clinically appropriate, in terms of type, frequency, extent, site and duration, and considered effective for the patient's illness, injury or disease; and o not primarily for the convenience of the patient or the provider and not more costly than an alternative service or sequence of services at least as likely to produce equivalent therapeutic or diagnostic results as to the diagnosis or treatment of that patient's illness, injury or disease. For these purposes, "generally accepted standards of medical practice" means standards that are based on credible scientific evidence published in peer-reviewed medical literature generally recognized by the relevant medical community, Specialty Society recommendations, and the views of providers practicing in relevant clinical areas and any other relevant factors. Advanced imaging services are a good example to highlight the benefits to consumers of medical necessity determinations. Many studies have documented the increased utilization of imaging services, with U.S. national expenditures on all medical imaging now exceeding $100 billion annually. There are a variety of factors that have contributed to this growth over the past 10 years, including increasingly sophisticated equipment, new clinical applications, consumer demand and variations in the prescribing and delivery of advanced imaging by providers. Highmark s analysis of its data related to the use of advanced imaging services identified 25-35% annual increases in utilization of such services, with many members receiving repeat and potentially unnecessary tests. Concerns regarding the quality of the images being produced led Highmark to implement a privileging program in 2005 prior to implementing our prior authorization program in Providers were required to meet specific quality requirements and safety standards in addition to being accredited and licensed to perform services that they were delivering. National accreditation requirements, as established by professional organizations such as the American College of Radiology (ACR) and the American College of Cardiology (ACC), 5
6 were utilized. The goal was to reduce the number of duplicate tests due to poor imaging quality and equipment and to implement safety programs to ensure that the lowest necessary radiation doses for members were followed. Our experience has shown that 42% of the advanced imaging studies requested are combination requests meaning that more than one body region is being imaged in a single session. Many of these combination requests are not medically necessary and result in a clinical disapproval saving members from unnecessary radiation exposure. In addition, an alternate course of treatment such as an ultrasound or MRI may be more appropriate to obtain the answer being sought without the potential risk of increased radiation to the member. In these cases, we work to educate our members and providers that alternative and equally beneficial treatment options are available. Medical necessity is further defined for all of our benefits by over 400 medical policies. Highmark medical policies are also based on substantial professional input, including: o A panel of approximately 280 actively practicing health care professionals; o Current medical literature, including the published and peer-reviewed results of clinical studies; o FDA or other regulatory approval where applicable; o State and national professional organizations (such as the American College of Cardiology or the Pennsylvania Medical Society); and o Evidence-based healthcare technology assessments from organizations such as BCBSA s Technology Evaluation Center (TEC) and the Agency for Healthcare Research and Quality (AHRQ). Collectively, this information allows Highmark to develop medical policies for determinations of medical necessity and coverage. InterQual clinical decision support products from McKesson are used in conjunction with these medical policies. McKesson is an independent company that develops national clinical decision support products which are used by many private insurers, CMS and military health systems. Such evidence-based criteria sets are critical to identifying safe, effective, and appropriate services in order to guide patients and providers through a continuum of 6
7 care. The goal is to protect our members and assist providers in decision making to further the goal of providing the appropriate treatment at the right time and in the right setting at each stage of an illness or condition. The definition of essential health benefits must preserve insurers ability to use medical necessity and other medical management tools. BCBSA and Highmark respectfully recommend that the IOM and the Secretary of the Department of Health and Human Services (HHS) do not limit the use of medical necessity or other commonly used medical management tools as part of the administration of essential health benefits. Employers, insurers and the Federal Employees Health Benefits Program (FEHBP) all use these tools to help keep coverage affordable while also ensuring the consumers receive the right care at the right place and at the right time. It also should be noted that the Medicare program follows an evidence-based approach for coverage determinations and also has policies to guide administration of hundreds of categories of Medicare covered services. Congress did not call for a definition of medical necessity in the ACA. Congress explicitly preserved the right of group health plans and health insurance issuers to employ commonly used management techniques like medical necessity. (See, ACA 1563(d)). Moreover, inclusion of such a definition is unnecessary given that extensive medical and legal negotiations on this subject have resulted in a standard definition of medical necessity agreed upon by national physician organizations and major health insurers. Today, this definition of medical necessity is incorporated into all comprehensive health insurance contracts that are reviewed and approved by state insurance commissioners. Similarly, the U.S. Office of Personnel Management (OPM) reviews and approves the medical necessity provisions used by FEHBP. Thus, medical necessity is currently generally subject to a standard definition and is subject to oversight from state regulators and employers. For these reasons, BCBSA and Highmark believe that there is no need or legal authority for IOM or HHS to develop a standard definition for medical necessity. 7
8 In addition to the comments already made describing medical necessity, examples of other medical management tools that should continue to be permissible in the administration of essential health benefits include: o Coverage of benefits through only licensed providers and facilities to ensure that consumers receive benefits from professionals that perform services within the scope of their license or certification. o Use of provider networks and cost sharing to direct consumers to those providers that deliver the best value and highest quality medical services to Highmark members. o Precertification and prior approval for inpatient hospital admissions except in cases of a medical emergency and certain outpatient surgical services such as bariatric surgery. This allows for an evaluation of appropriateness and medical necessity. o General exclusions for services not medically necessary or appropriate under accepted standards of medical practice such as benefits for cosmetic purposes or custodial care. Such management tools are essential to further the goal of affordability and should not be considered as part of the definition of essential health benefits. It is also important to recognize that members and providers have appeals rights, which frequently include an independent assessment. This appeals process provides an important check and balance to the medical necessity review process which effectively protects the consumer by furthering the goal of providing appropriate care at the right time and in the right setting. The process for determining and updating essential health benefits should be grounded in evidence-based research and market-based input. We respectfully recommend the following key principles to drive the criteria and process to define and update the definition of essential health benefits: 8
9 o To provide access to consumers to appropriate care at the right time and in the right setting, the processes, principles, or criteria used to define essential health benefits must be rigorously evidence based, free from political influence, and involve considerations of cost-effectiveness, quality and appropriateness. o The definition of essential health benefits should focus on the set of categories of services specifically established in the ACA. A definition that is too specific regarding covered services creates the risk of undermining affordability and the flexibility necessary to accommodate advancements in medical science. o The process of identifying essential health benefits also requires a determination of what is not an essential health benefit. The independent analyses of what is an essential benefit should consider medical efficacy and social and financial impacts. The creation of a consistent decision-making process that includes independent analysis and explicit guidelines to apply when making these determinations will best service all interested parties. o The process should consider the findings of comparative effectiveness research, including the work of the Patient-Centered Outcomes Research Institute (PCORI) established under the ACA. o The process should involve a periodic survey of the marketplace, which furthers the intent of the ACA requirement that the Department of Labor survey employer plans, to ensure that the scope of essential health benefits is equal to the scope of benefits provided under a typical employer plan. We recommend that this survey initially focus on the scope of benefits offered by smaller companies to more accurately represent the needs of the Exchange-based market. o Essential health benefits should be evaluated on a de novo basis that includes a review of authoritative scientific evidence rather than the frequency or design of state benefit mandates. State benefit mandates may be the result of political pressure from special interest groups, and the adoption process for such mandates may lack the rigorous level of evaluation of efficacy or evidence-based support from medical experts that should be required in determining essential health benefits 9
10 o The process should establish minimum thresholds which allow for innovation in benefit designs. Meaningful differentiations will provide consumer choice across Bronze, Silver, Gold plans on Exchanges. Examples of market-based innovation that should be encouraged include: value-based plan designs with differential cost sharing; and use of provider network models allowing insurers to incent the use of high quality and efficient providers (e.g., centers of excellence). Conclusion The decisions this IOM Committee and HHS ultimately make regarding the definition of the essential health benefits package will play a critical role in determining whether the ACA is successful in encouraging the creation of affordable health insurance products that are responsive to consumer demands in local markets nationwide. As leaders in the health care community for over 80 years, BCBSA and member Blue Plans such as Highmark look forward to assisting the IOM in developing specific recommendations for defining the essential health benefits package. Thank you for the opportunity to present our views. 10
4/29/2014. April 30, 2014
 April 30, 2014 Rachel Peura, RN Educated in PA; worked in a variety of settings in PA including: Acute care In and outpatient medical rehab Office settings Clinical trials House supervisor positions Employed
April 30, 2014 Rachel Peura, RN Educated in PA; worked in a variety of settings in PA including: Acute care In and outpatient medical rehab Office settings Clinical trials House supervisor positions Employed
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION
 RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-06 GENERAL RULES OF THE WORKERS COMPENSATION PROGRAM TABLE OF CONTENTS 0800-02-06-.01 Definitions
RULES OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT DIVISION OF WORKERS COMPENSATION CHAPTER 0800-02-06 GENERAL RULES OF THE WORKERS COMPENSATION PROGRAM TABLE OF CONTENTS 0800-02-06-.01 Definitions
Anthem Provider Appeal Policy and Procedure
 Anthem Provider Appeal Policy and Procedure I. INTRODUCTION Anthem Health Plans of Virginia, Inc., d/b/a Anthem Blue Cross and Blue Shield, HealthKeepers, Inc., Peninsula Health Care, Inc., and Priority
Anthem Provider Appeal Policy and Procedure I. INTRODUCTION Anthem Health Plans of Virginia, Inc., d/b/a Anthem Blue Cross and Blue Shield, HealthKeepers, Inc., Peninsula Health Care, Inc., and Priority
INFORMATION ABOUT YOUR OXFORD COVERAGE
 OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 Highmark Blue Cross Blue Shield: BlueCare HMO Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 Highmark Blue Cross Blue Shield: BlueCare HMO Coverage for: Individual/Family
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 Highmark Blue Cross Blue Shield: BlueCare Custom PPO Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 Highmark Blue Cross Blue Shield: BlueCare Custom PPO Coverage for: Individual/Family
ESSENTIAL HEALTH BENEFITS BULLETIN Center for Consumer Information and Insurance Oversight December 16, 2011
 ESSENTIAL HEALTH BENEFITS BULLETIN Center for Consumer Information and Insurance Oversight December 16, 2011 Contents ESSENTIAL HEALTH BENEFITS BULLETIN... 1 Purpose... 1 Defining Essential Health Benefits...
ESSENTIAL HEALTH BENEFITS BULLETIN Center for Consumer Information and Insurance Oversight December 16, 2011 Contents ESSENTIAL HEALTH BENEFITS BULLETIN... 1 Purpose... 1 Defining Essential Health Benefits...
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/ /31/2019
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark West Virginia: my Blue Access WV EPO Silver 4450 HSA Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark West Virginia: my Blue Access WV EPO Silver 4450 HSA Coverage
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-800-342-9816. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-800-342-9816. Important
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/ /31/2019
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark West Virginia: my Blue Access WV EPO Bronze 4000 Coverage for:
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark West Virginia: my Blue Access WV EPO Bronze 4000 Coverage for:
Common Managed Care Terms & Definitions
 Contact Us: Email: info@emedbiz.com Phone: 561-430-2090 Fax: 561-430-2091 Website: www.emedbiz.com Common Managed Care Terms & Definitions Balance billing: The practice of billing a patient for the amount
Contact Us: Email: info@emedbiz.com Phone: 561-430-2090 Fax: 561-430-2091 Website: www.emedbiz.com Common Managed Care Terms & Definitions Balance billing: The practice of billing a patient for the amount
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 Highmark Blue Shield: PPO Blue Coverage for: Individual/Family Plan Type:
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 Highmark Blue Shield: PPO Blue Coverage for: Individual/Family Plan Type:
$0 individual/$0 family network. $250 individual/$500 family out-ofnetwork.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Shield: PPO Coverage for: Individual/Family Plan Type: PPO
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Shield: PPO Coverage for: Individual/Family Plan Type: PPO
$1,500 individual/$3,000 family network. $3,000 individual/$6,000 family out-ofnetwork.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Journey Health Systems: PPO Coverage for: Individual/Family Plan Type:
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Journey Health Systems: PPO Coverage for: Individual/Family Plan Type:
Employee Benefit Plan: Missoula County Public Schools Coverage Period: 01/01/ /31/2014 Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
$350 individual/$700 family network. $700 individual/$1,400 family out-ofnetwork.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 04/01/2018-03/31/2019 Gannon University: PPO Coverage for: Individual/Family Plan Type: PPO
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 04/01/2018-03/31/2019 Gannon University: PPO Coverage for: Individual/Family Plan Type: PPO
Provider Training Program. Date
 Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Mountain State Blue Cross Blue Shield Provider Training Program Presenter Date Provider Training Program Agenda Welcome and Opening Remarks About NIA The Provider Partnership The Program Components The
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/ /31/2019
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark West Virginia: my Blue Access WV EPO Silver 3500-2 Free PCP Visits
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark West Virginia: my Blue Access WV EPO Silver 3500-2 Free PCP Visits
January 31, Dear Mr. Larsen:
 January 31, 2012 Steve Larsen Director, Center for Consumer Information and Insurance Oversight Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services 7500 Security Boulevard
January 31, 2012 Steve Larsen Director, Center for Consumer Information and Insurance Oversight Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services 7500 Security Boulevard
Patient Credit and Collections Policy. Penn State Health Revenue Cycle
 Patient Credit and Collections Policy Penn State Health Revenue Cycle Effective Date: RC-002 5/11/2017 PURPOSE To provide clear and consistent guidelines for conducting billing, collections, and recovery
Patient Credit and Collections Policy Penn State Health Revenue Cycle Effective Date: RC-002 5/11/2017 PURPOSE To provide clear and consistent guidelines for conducting billing, collections, and recovery
Blue Care Elect $250 Deductible MIIA Coverage Period: on or after 07/01/2015
 Blue Care Elect $250 Deductible MIIA Coverage Period: on or after 07/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This
Blue Care Elect $250 Deductible MIIA Coverage Period: on or after 07/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/ /31/2018
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Pennsylvania Turnpike Commission: Highmark PPO Blue Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Pennsylvania Turnpike Commission: Highmark PPO Blue Coverage for: Individual/Family
Healthcare Reform 2010 Major Insurance Market Reform
 Healthcare Reform 2010 Major Insurance Market Reform An Independent Licensee of the Blue Cross and Blue Shield Association 2010 Major Insurance Market Reform Table of Contents Pre-Ex Exclusion Periods...
Healthcare Reform 2010 Major Insurance Market Reform An Independent Licensee of the Blue Cross and Blue Shield Association 2010 Major Insurance Market Reform Table of Contents Pre-Ex Exclusion Periods...
$200 individual/$400 family combined network and out-of-network.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 New Castle County Government : Blue Choice PPO Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019-12/31/2019 New Castle County Government : Blue Choice PPO Coverage for: Individual/Family
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Cross Blue Shield: Major Events Blue PPO 7350 a Community
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Cross Blue Shield: Major Events Blue PPO 7350 a Community
Coding and Reimbursement
 Coding and Reimbursement IORT Reimbursement Kathy Francisco The Pinnacle Health Group, Inc., Pennsylvania The statements of the healthcare professional giving this presentation reflect only their personal
Coding and Reimbursement IORT Reimbursement Kathy Francisco The Pinnacle Health Group, Inc., Pennsylvania The statements of the healthcare professional giving this presentation reflect only their personal
Issue Brief: Interaction between California State Benefit Mandates and the Affordable Care Act s Essential Health Benefits
 Issue Brief: Interaction between California State Benefit Mandates and the Affordable Care Act s Essential Health Benefits March 2012 CHBRP Issue Brief: Interaction between California State Benefit Mandates
Issue Brief: Interaction between California State Benefit Mandates and the Affordable Care Act s Essential Health Benefits March 2012 CHBRP Issue Brief: Interaction between California State Benefit Mandates
Some of the services this plan doesn t cover are listed on page 5. See your policy Yes plan doesn t cover?
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Network This is only a summary. If you want more detail about your coverage and costs, you can
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Network This is only a summary. If you want more detail about your coverage and costs, you can
Health Plan Benefits and Coverage Matrix
 Health Plan Benefits and Coverage Matrix THIS MATRI IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF COVERAGE AND PLAN CONTRACT SHOULD BE CONSULTED FOR
Health Plan Benefits and Coverage Matrix THIS MATRI IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF COVERAGE AND PLAN CONTRACT SHOULD BE CONSULTED FOR
Health Plan Benefits and Coverage Matrix
 Health Plan Benefits and Coverage Matrix THIS MATRI IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF COVERAGE AND PLAN CONTRACT SHOULD BE CONSULTED FOR
Health Plan Benefits and Coverage Matrix THIS MATRI IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF COVERAGE AND PLAN CONTRACT SHOULD BE CONSULTED FOR
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/ /31/2018
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2018 12/31/2018 Highmark Delaware: Shared Cost Blue EPO 6950 Coverage for: Individual/Family Plan Type: EPO
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2018 12/31/2018 Highmark Delaware: Shared Cost Blue EPO 6950 Coverage for: Individual/Family Plan Type: EPO
CANCER LEADERSHIP COUNCIL
 CANCER LEADERSHIP COUNCIL A PATIENT-CENTERED FORUM OF NATIONAL ADVOCACY ORGANIZATIONS ADDRESSING PUBLIC POLICY ISSUES IN CANCER December 26, 2012 Via Electronic Filing http://www.regulations.gov The Honorable
CANCER LEADERSHIP COUNCIL A PATIENT-CENTERED FORUM OF NATIONAL ADVOCACY ORGANIZATIONS ADDRESSING PUBLIC POLICY ISSUES IN CANCER December 26, 2012 Via Electronic Filing http://www.regulations.gov The Honorable
RE: Additional Input regarding Accountable Care Organizations (ACOs) and the Medicare Shared Saving Program
 221 MAIN STREET, SUITE 1500 SAN FRANCISCO, CA 94105 PBGH.ORG OFFICE 415.281.8660 FACSIMILE 415.520.0927 February 14, 2011 Donald M. Berwick, M.D. Administrator Centers for Medicare and Medicaid Services
221 MAIN STREET, SUITE 1500 SAN FRANCISCO, CA 94105 PBGH.ORG OFFICE 415.281.8660 FACSIMILE 415.520.0927 February 14, 2011 Donald M. Berwick, M.D. Administrator Centers for Medicare and Medicaid Services
Contents. Page. Chapter
 Contents Chapter I. Summary and Policy Options........................................ 3 2. Physician Payment Under the Medicare Program: Problems and Changing Context...................................................
Contents Chapter I. Summary and Policy Options........................................ 3 2. Physician Payment Under the Medicare Program: Problems and Changing Context...................................................
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Prev. Plus Plan This is only a summary. If you want more detail about your coverage and costs,
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Prev. Plus Plan This is only a summary. If you want more detail about your coverage and costs,
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myscrippshealthplan.com or by calling 1-877-552-7247.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myscrippshealthplan.com or by calling 1-877-552-7247.
MANAGED CARE READINESS TOOLKIT
 MANAGED CARE READINESS TOOLKIT Please note: The following managed care definitions reflect a general understanding of the terms. It will be important to read managed care contracts very carefully as they
MANAGED CARE READINESS TOOLKIT Please note: The following managed care definitions reflect a general understanding of the terms. It will be important to read managed care contracts very carefully as they
Highmark Blue Cross Blue Shield: PPO Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
$50 individual/$150 family. No. No. Yes, Prescription drugs $50 individual/$150there are no other specific deductibles.
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2017-06/30/2018 LCIC Penn College of Technology: Traditional Coverage for: Individual/Family Plan Type: Indemnity
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2017-06/30/2018 LCIC Penn College of Technology: Traditional Coverage for: Individual/Family Plan Type: Indemnity
Blue Care Elect $250 Deductible Coverage Period: on or after 07/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 Blue Care Elect $250 Deductible Coverage Period: on or after 07/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is
Blue Care Elect $250 Deductible Coverage Period: on or after 07/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is
ECONOMIC PRINCIPLES IMPACTING MANAGED CARE PHARMACY. Adrian Washington PharmD., MBA Vice President of Client Management United Healthcare OptumRx
 ECONOMIC PRINCIPLES IMPACTING MANAGED CARE PHARMACY Adrian Washington PharmD., MBA Vice President of Client Management United Healthcare OptumRx As vice president, Adrian is responsible for strategic planning
ECONOMIC PRINCIPLES IMPACTING MANAGED CARE PHARMACY Adrian Washington PharmD., MBA Vice President of Client Management United Healthcare OptumRx As vice president, Adrian is responsible for strategic planning
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers
 NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
NIA Magellan i Frequently Asked Questions (FAQs) For Blue Cross of Northeastern Pennsylvania Providers Question GENERAL Why is Blue Cross of Northeastern Pennsylvania implementing an outpatient imaging
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Health Insurance Company: my Direct Blue Major Events EPO 7350
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Health Insurance Company: my Direct Blue Major Events EPO 7350
You don t have to meet deductibles for specific services, but see the chart starting on page 3 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
The Health Insurance Market in Virginia. Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017
 The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
The Health Insurance Market in Virginia Maureen Dempsey, MD, MSc, ACC, FAAP Anthem Blue Cross and Blue Shield June 8, 2017 Anthem Inc. at a Glance Broad geographic footprint and customer base ` BCBS plans
Benefits. Guide to. Small Business Health Plan Hawaii Choice - A
 Guide to Benefits Small Business Health Plan Hawaii Choice - A (Includes Drug and Children's Vision) Health Maintenance Organization (HMO) January 2016 An Independent Licensee of the Blue Cross and Blue
Guide to Benefits Small Business Health Plan Hawaii Choice - A (Includes Drug and Children's Vision) Health Maintenance Organization (HMO) January 2016 An Independent Licensee of the Blue Cross and Blue
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Vanderbilt University. Aetna Choice POS II Health Fund Plan
 BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Carey International, Inc. High Deductible Choice POS II
 BENEFIT PLAN Prepared Exclusively for Carey International, Inc. What Your Plan Covers and How Benefits are Paid High Deductible Choice POS II Table of Contents Schedule of Benefits... Issued with Your
BENEFIT PLAN Prepared Exclusively for Carey International, Inc. What Your Plan Covers and How Benefits are Paid High Deductible Choice POS II Table of Contents Schedule of Benefits... Issued with Your
Medical Policy Guidelines and Procedures
 Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
Medical Policy Guidelines and Procedures An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee
Cummins Central Power, LLC Coverage Period: 05/01/ /30/2015
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Medicare Part C Medical Coverage Policy
 Medicare Part C Medical Coverage Policy Investigational (Experimental) Services Origination: November 2009 Review Date: July 12, 2017 Next Review: July 2019 DESCRIPTION OF PROCEDURE OR SERVICE Title XVIII
Medicare Part C Medical Coverage Policy Investigational (Experimental) Services Origination: November 2009 Review Date: July 12, 2017 Next Review: July 2019 DESCRIPTION OF PROCEDURE OR SERVICE Title XVIII
Important Questions Answers Why this Matters:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Cummins Central Power, LLC Coverage Period: 05/01/ /30/2016
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
CareFirst BlueChoice, Inc. 840 First Street, NE Washington, DC
 CareFirst BlueChoice, Inc. 840 First Street, NE Washington, DC 20065 202-479-8000 An independent licensee of the Blue Cross and Blue Shield Association ELECTRONIC CONTRACT ACCURACY DISCLAIMER CareFirst
CareFirst BlueChoice, Inc. 840 First Street, NE Washington, DC 20065 202-479-8000 An independent licensee of the Blue Cross and Blue Shield Association ELECTRONIC CONTRACT ACCURACY DISCLAIMER CareFirst
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Cross Blue Shield: my Direct Blue Conemaugh EPO 6950B Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Blue Cross Blue Shield: my Direct Blue Conemaugh EPO 6950B Coverage
BH Media Group, Inc. Coverage Period: 01/01/ /31/2016
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Student Health Insurance Plan Insurance Company Coverage Period: 08/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.studentplanscenter.com or by calling 1-800-756-3702.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.studentplanscenter.com or by calling 1-800-756-3702.
Marsh and McLennan: Anthem Blue Cross and Blue Shield $2,850 Deductible Plan Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Health Insurance Company: my Direct Blue Lehigh Valley EPO 6950B
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 Highmark Health Insurance Company: my Direct Blue Lehigh Valley EPO 6950B
HEALTH CARRIER GRIEVANCE PROCEDURE MODEL ACT
 Table of Contents Model Regulation Service April 2012 HEALTH CARRIER GRIEVANCE PROCEDURE MODEL ACT Section 1. Section 2. Section 3. Section 4. Section 5. Section 6. Section 7. Section 8. Section 9. Section
Table of Contents Model Regulation Service April 2012 HEALTH CARRIER GRIEVANCE PROCEDURE MODEL ACT Section 1. Section 2. Section 3. Section 4. Section 5. Section 6. Section 7. Section 8. Section 9. Section
Important Questions Answers Why This Matters: If took HealthQuotient:
 HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
Comments of Aetna Inc. before the Joint Public Hearing of the Florida Office of Insurance Regulation And the Florida health Insurance Advisory Board
 Comments of Aetna Inc. before the Joint Public Hearing of the Florida Office of Insurance Regulation And the Florida health Insurance Advisory Board May 4, 2010 Mark LaBorde President, Jacksonville/Tampa
Comments of Aetna Inc. before the Joint Public Hearing of the Florida Office of Insurance Regulation And the Florida health Insurance Advisory Board May 4, 2010 Mark LaBorde President, Jacksonville/Tampa
You don t have to meet deductibles for specific services.
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark Delaware: Health Savings Embedded Blue EPO Silver 4450 HSA Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 Highmark Delaware: Health Savings Embedded Blue EPO Silver 4450 HSA Coverage
Wellesley College Health Insurance Program Information
 Wellesley College Health Insurance Program Information Beginning August 15, 2014 Health Services All Wellesley College students, including Davis Scholars and Exchange students are encouraged to seek services
Wellesley College Health Insurance Program Information Beginning August 15, 2014 Health Services All Wellesley College students, including Davis Scholars and Exchange students are encouraged to seek services
MedTech/BioTech Reimbursement: Getting Paid in the USA. MDCC Greater MSP September, 2016
 MedTech/BioTech Reimbursement: Getting Paid in the USA MDCC Greater MSP September, 2016 1 World Wide Market Access through Life Sciences International, Inc. Mpls/St. Paul Chicago Mexico Brussels London
MedTech/BioTech Reimbursement: Getting Paid in the USA MDCC Greater MSP September, 2016 1 World Wide Market Access through Life Sciences International, Inc. Mpls/St. Paul Chicago Mexico Brussels London
Coverage Period: 01/01/ /31/2018
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Blue Cross and Blue Shield of North Carolina: Blue Select Gold 2500 Coverage Period: 01/01/2018-12/31/2018 Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Blue Cross and Blue Shield of North Carolina: Blue Select Gold 2500 Coverage Period: 01/01/2018-12/31/2018 Coverage
Important Questions Answers Why this Matters:
 Student Employee Health Plan: NYS Health Insurance Program Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual or Family
Student Employee Health Plan: NYS Health Insurance Program Coverage Period: 01/01/2014 12/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual or Family
PRICE TRANSPARENCY Frequently Asked Questions
 PRICE TRANSPARENCY Frequently Asked Questions Introduction Price transparency is one of the most confusing topics in today s healthcare world. Healthcare consumers are becoming more engaged and asking
PRICE TRANSPARENCY Frequently Asked Questions Introduction Price transparency is one of the most confusing topics in today s healthcare world. Healthcare consumers are becoming more engaged and asking
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.crystalrunhp.com or by calling 1-844-638-6506. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.crystalrunhp.com or by calling 1-844-638-6506. Important
: BlueEssentials Silver 3
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs : BlueEssentials Silver 3 Coverage Period: 1/1/2014 12/31/14 Coverage for: Single Plan Type: EPO This is only a summary. If you want
Summary of Benefits and Coverage: What this Plan Covers & What it Costs : BlueEssentials Silver 3 Coverage Period: 1/1/2014 12/31/14 Coverage for: Single Plan Type: EPO This is only a summary. If you want
Glossary. Last Reviewed 11/10/14
 Glossary ACCC ACA ACS AHFS AHRQ AMA APC Association of Community Cancer Centers Affordable Care Act American Cancer Society American Hospital Formulary Service Agency for Healthcare Research and Quality
Glossary ACCC ACA ACS AHFS AHRQ AMA APC Association of Community Cancer Centers Affordable Care Act American Cancer Society American Hospital Formulary Service Agency for Healthcare Research and Quality
Important Questions Answers Why this Matters: What is the overall deductible? $0 Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/usg or by calling 1-800-424-8950. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/usg or by calling 1-800-424-8950. Important
Important Questions Answers Why this Matters: What is the overall deductible? $0 Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/bor or by calling 1-800-424-8950. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsga.com/bor or by calling 1-800-424-8950. Important
WPAHS: Community Blue EPO Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at Highmarkbcbs.com or by calling 1-800-472-1506. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at Highmarkbcbs.com or by calling 1-800-472-1506. Important
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.askallegiance.com/mckinney or by calling 1-855-999-1054.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.askallegiance.com/mckinney or by calling 1-855-999-1054.
SUMMARY OF BENEFITS. Montgomery College Open Access Plus Coinsurance Plan. Connecticut General Life Insurance Co. Notice of Grandfathered Plan Status
 SUMMARY OF BENEFITS Connecticut General Life Insurance Co. Notice of Grandfathered Plan Status This plan is being treated as a grandfathered health plan under the Patient Protection and Affordable Care
SUMMARY OF BENEFITS Connecticut General Life Insurance Co. Notice of Grandfathered Plan Status This plan is being treated as a grandfathered health plan under the Patient Protection and Affordable Care
CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES
 CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES UNIT 5: OUTPATIENT RADIOLOGY AND LABORATORY IN THIS UNIT TOPIC SEE PAGE Radiology Management Program Overview 2 Privileging for Radiology Services 3
CHAPTER 4: PROVIDER RESPONSIBILITIES AND GUIDELINES UNIT 5: OUTPATIENT RADIOLOGY AND LABORATORY IN THIS UNIT TOPIC SEE PAGE Radiology Management Program Overview 2 Privileging for Radiology Services 3
The Affordable Care Act and the Essential Health Benefits Package
 October 24, 2011 The Affordable Care Act and the Essential Health Benefits Package A. Background Under the Affordable Care Act (the ACA or the Act ), and starting in 2014, certain low to moderate income
October 24, 2011 The Affordable Care Act and the Essential Health Benefits Package A. Background Under the Affordable Care Act (the ACA or the Act ), and starting in 2014, certain low to moderate income
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: Beginning On or After 1/1/2018 Gold 80 HMO Trio Coverage for: Individual + Family Plan Type:
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: Beginning On or After 1/1/2018 Gold 80 HMO Trio Coverage for: Individual + Family Plan Type:
Medicare Program; Medicare Shared Savings Program: Accountable Care Organizations Proposed Rule
 701 Pennsylvania Ave., NW, Suite 800 Washington, DC 20004-2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org February 6, 2015 Marilyn Tavenner, Administrator Centers for Medicare & Medicaid Services
701 Pennsylvania Ave., NW, Suite 800 Washington, DC 20004-2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org February 6, 2015 Marilyn Tavenner, Administrator Centers for Medicare & Medicaid Services
Anthem Blue Cross: Anthem Silver DirectAccess, a Multi-State Plan Coverage Period: 01/01/ /31/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
REPORT OF THE COUNCIL ON MEDICAL SERVICE
 REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -A- Subject: Presented by: Referred to: Essential Health Care Benefits (Resolution 0-A-0) William E. Kobler, MD, Chair Reference Committee A (Joseph
REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -A- Subject: Presented by: Referred to: Essential Health Care Benefits (Resolution 0-A-0) William E. Kobler, MD, Chair Reference Committee A (Joseph
Coverage Period: 01/01/ /31/2019 Gold Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services
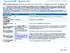 BlueCare 1565 Coverage Period: 01/01/2019-12/31/2019 Gold Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage for: Individual and/or Family Plan Type: HMO
BlueCare 1565 Coverage Period: 01/01/2019-12/31/2019 Gold Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage for: Individual and/or Family Plan Type: HMO
An inpatient confinement facility includes:
 [184] [MEDICAL EXPENSE INSURANCE [185] UTILIZATION MANAGEMENT PROGRAM In order to monitor the use of inpatient health care services, services within specialized facilities, and other kinds of medical treatment,
[184] [MEDICAL EXPENSE INSURANCE [185] UTILIZATION MANAGEMENT PROGRAM In order to monitor the use of inpatient health care services, services within specialized facilities, and other kinds of medical treatment,
New Mental Health/Substance Abuse Parity Rules Will Apply in 2015
 Nov. 19, 2013 New Mental Health/Substance Abuse Parity Rules Will Apply in 2015 It s a simple goal: Make health plan benefits for one group of conditions at least as generous as the plan s benefits for
Nov. 19, 2013 New Mental Health/Substance Abuse Parity Rules Will Apply in 2015 It s a simple goal: Make health plan benefits for one group of conditions at least as generous as the plan s benefits for
Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2018-06/30/2019 Allegheny County Schools Health Insurance Consortium: Community Blue Flex Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2018-06/30/2019 Allegheny County Schools Health Insurance Consortium: Community Blue Flex Coverage for: Individual/Family
STATE OF FL Employees PPO Coverage Period: 01/01/ /31/2017
 STATE OF FL Employees PPO Coverage Period: 01/01/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and/or Family Plan Type: PPO This is only
STATE OF FL Employees PPO Coverage Period: 01/01/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and/or Family Plan Type: PPO This is only
EnhancedBlue SM Gold 1000 PPO
 EnhancedBlue SM Gold 1000 PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Single & Family Plan Type: PPO This is only a
EnhancedBlue SM Gold 1000 PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Single & Family Plan Type: PPO This is only a
CalPERS: Sharp Performance Plus HMO Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.sharphealthplan.com/calpers or by calling 1-855-995-5004.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.sharphealthplan.com/calpers or by calling 1-855-995-5004.
You don t have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 Massachusetts The Harvard Pilgrim HMO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2017 12/31/2017 Coverage for: Individual + Family Plan Type: HMO This
Massachusetts The Harvard Pilgrim HMO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2017 12/31/2017 Coverage for: Individual + Family Plan Type: HMO This
BALTIMORE COUNTY PUBLIC SCHOOLS. Vision Care Option ASO CFMI/GHMSI FS VISION (1/18)
 BALTIMORE COUNTY PUBLIC SCHOOLS Vision Care Option CareFirst of Maryland, Inc. doing business as CareFirst BlueCross BlueShield 10455 Mill Run Circle Owings Mills, MD 21117-5559 A private not-for-profit
BALTIMORE COUNTY PUBLIC SCHOOLS Vision Care Option CareFirst of Maryland, Inc. doing business as CareFirst BlueCross BlueShield 10455 Mill Run Circle Owings Mills, MD 21117-5559 A private not-for-profit
CHAPTER 32. AN ACT concerning health insurance and health care providers and supplementing various parts of the statutory law.
 CHAPTER 32 AN ACT concerning health insurance and health care providers and supplementing various parts of the statutory law. BE IT ENACTED by the Senate and General Assembly of the State of New Jersey:
CHAPTER 32 AN ACT concerning health insurance and health care providers and supplementing various parts of the statutory law. BE IT ENACTED by the Senate and General Assembly of the State of New Jersey:
Description of Policy Options. Expanding Health Care Coverage: Proposals to Provide Affordable Coverage to All Americans
 Description of Policy Options Expanding Health Care Coverage: Proposals to Provide Affordable Coverage to All Americans Senate Finance Committee May 14, 2009 TABLE OF CONTENTS SECTION I: Insurance Market
Description of Policy Options Expanding Health Care Coverage: Proposals to Provide Affordable Coverage to All Americans Senate Finance Committee May 14, 2009 TABLE OF CONTENTS SECTION I: Insurance Market
Coverage Period: 07/01/ /31/2018 Coverage for: Individual, Family Plan Type: EPO
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services New England Health Care Employees Welfare Fund: Wage Class I Coverage Period: 07/01/2018 12/31/2018 Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services New England Health Care Employees Welfare Fund: Wage Class I Coverage Period: 07/01/2018 12/31/2018 Coverage
CASA, INC. : Health Network Only SM - HDHP (ACO Plan)
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-888-982-3862.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthreformplansbc.com or by calling 1-888-982-3862.
Mental Health Parity and Addiction Equity Act FAQs
 Mental Health Parity and Addiction Equity Act FAQs This document contains the Frequently Asked Questions and responses (FAQs) concerning implementation of the Paul Wellstone and Pete Domenici Mental Health
Mental Health Parity and Addiction Equity Act FAQs This document contains the Frequently Asked Questions and responses (FAQs) concerning implementation of the Paul Wellstone and Pete Domenici Mental Health
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Preferred Blue PPO $500 Deductible Coverage Period: on or after 01/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 Preferred Blue PPO $500 Deductible Coverage Period: on or after 01/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This
Preferred Blue PPO $500 Deductible Coverage Period: on or after 01/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This
Important Questions Answers Why this Matters: What is the overall deductible?
 HMO Blue New England Premier Value with HCCS Coverage Period: on or after 01/01/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type:
HMO Blue New England Premier Value with HCCS Coverage Period: on or after 01/01/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type:
