Benefits Preview Weber State University. Look inside for important information about how to use your PEHP benefits.
|
|
|
- Preston Lang
- 5 years ago
- Views:
Transcription
1 Weber State University Benefits Preview Look inside for important information about how to use your PEHP benefits.
2 Weber State University » Contact Information Welcome to PEHP We want to make accessing and understanding your healthcare benefits simple. This Benefits Summary contains important information on how best to use PEHP s comprehensive benefits. Please contact the following PEHP departments or affiliates if you have questions. On the Web»myPEHP mypehp is your online source for personal health and plan benefit information. You can review your claims history, see a comprehensive list of your coverages, look up contracted providers, and more. Create a mypehp account to enroll in PEHP benefits electronically. Customer Service or Weekdays from 8 a.m. to 5 p.m. Have your PEHP ID or Social Security number on hand for faster service. Foreign language assistance available Pre-notification/pre-authorization»Inpatient hospital pre-notification or Mental Health/Substance Abuse pre-authorization»pehp Customer Service or Prescription drug benefits»pehp Customer Service or »Express Scripts Specialty pharmacy»accredo PEHP flex$/limited FLEX$»PEHP FLEX$ Department or health savings accounts (HSA)»Health Equity Prenatal program» PEHP WeeCare or wellness and disease management» PEHP Healthy Utah or PEHP Waist Aweigh or » PEHP Integrated Care or /weecare Value-Added Benefits program» PEHPplus.../plus»Blomquist Hale Online enrollment help line or Claims mailing address PEHP 560 East 200 South Salt Lake City, Utah PAGE 2
3 Weber State University » Benefit Changes & Reminders Benefit Changes & Reminders All Medical Plans» Healthcare Reform requires a Summary of Benefits and Coverage (SBC) to be distributed to all benefiteligible employees before open enrollment. This will be distributed through a WSU Special Campus Bulletin during the first week of April.» Effective Jan. 1, 2013, new preventive services for women have been added to the Affordable Care Act list. Please see the Master Policy for a complete list of preventive services.» Accupuncture services are no longer a covered benefit.» Medco, PEHP s pharmacy benefit manager, is now known as Express Scripts and can be found online at Members who made changes to their PEHP plans will receive a new ID card in the mail from Express Scripts. It will serve as your medical, pharmacy, and out-of-state network ID card. If you did not make changes, continue to use your current card(s).» Members can shop for value, compare prices, and save money using PEHP s new Cost & Quality Tools, accessible through their mypehp account.» Medicare Supplement plans PEHP offers three Medicare Supplement Medical plans and Medicare Part D approved Prescription Drug plans. PEHP also offers a value-added Discount Dental plan to individuals who enroll in one of the PEHP Medicare Medical Supplement options. Please contact PEHP Customer Service for more details and enrollment information. The STAR Plan» The STAR Plan will continue to be an option using the Advantage and Summit Care networks. The STAR Plan has two components: A High Deductible Health Plan HDHP) and a Health Savings Account (HSA). There is no employee cost share for this plan. Those enrolled in the STAR PLAN will receive semimonthly contributions to their HSA in the amount of $31.25 single / $62.50 double and family each pay day. FLEX$ Changes» Due to Federal Healthcare Reform, the medical Flexible Spending Account maximum has been reduced to $2,500. The dependent day care maximum will remain at $5,000.» Beginning April 1, 2013, PEHP FLEX$ card holders may be required to enter a Personal Identification Number (PIN) when making point-of-sale purchases. To view your PIN, you will need your PEHP member ID (last 6 digits) and FLEX$ card number. Log in to your mypehp account and, once on the FLEX$ page, click on Card Status. Follow the online steps to view your PIN, as well as PINs for other cardholders on your account. Questions? Please contact PEHP FLEX$ at PAGE 3
4 Weber State University » PEHP Medical Networks PEHP Medical Networks PEHP Advantage Care The PEHP Advantage Care network of contracted providers consists of predominantly Intermountain Healthcare (IHC) providers and facilities. It includes 34 participating hospitals and more than 7,500 participating providers. PARTICIPATING HOSPITALS Beaver County Beaver Valley Hospital Milford Valley Memorial Hospital Box Elder County Bear River Valley Hospital Cache County Logan Regional Hospital Carbon County Castleview Hospital Davis County Davis Hospital Duchesne County Uintah Basin Medical Center Garfield County Garfield Memorial Hospital Grand County Moab Regional Hospital Iron County Valley View Medical Center Juab County Central Valley Medical Center Kane County Kane County Hospital Millard County Delta Community Medical Center Fillmore Community Hospital Salt Lake County Alta View Hospital Intermountain Medical Center PEHP Preferred Care Salt Lake County (cont.) The Orthopedic Specialty Hospital (TOSH) LDS Hospital Primary Children s Medical Center Riverton Hospital San Juan County Blue Mountain Hospital San Juan Hospital Sanpete County Gunnison Valley Hospital Sanpete Valley Hospital Sevier County Sevier Valley Medical Center Summit County Park City Medical Center Tooele County Mountain West Medical Center Uintah County Ashley Valley Medical Center Utah County American Fork Hospital Orem Community Hospital Utah Valley Regional Medical Center Wasatch County Heber Valley Medical Center Washington County Dixie Regional Medical Center Weber County McKay-Dee Hospital The PEHP Preferred Care network of contracted providers consists of providers and facilities in both the Advantage Care and Summit Care networks. It includes 46 participating hospitals and more than 12,000 participating providers. PEHP Summit Care The PEHP Summit Care network of contracted Providers consists of predominantly IASIS, MountainStar, and University of Utah hospitals & clinics providers and facilities. It includes 38 participating hospitals and more than 7,500 participating providers. PARTICIPATING HOSPITALS Beaver County Beaver Valley Hospital Milford Valley Memorial Hospital Box Elder County Bear River Valley Hospital Brigham City Community Hospital Cache County Logan Regional Hospital Carbon County Castleview Hospital Davis County Lakeview Hospital Davis Hospital Duchesne County Uintah Basin Medical Center Garfield County Garfield Memorial Hospital Grand County Moab Regional Hospital Iron County Valley View Medical Center Juab County Central Valley Medical Center Kane County Kane County Hospital Millard County Delta Community Medical Center Fillmore Community Hospital Salt Lake County Huntsman Cancer Hospital Jordan Valley Hospital Salt Lake County (cont.) Pioneer Valley Hospital Primary Children s Medical Center Riverton Children s Unit St. Marks Hospital Salt Lake Regional Medical Center University of Utah Hospital University Orthopaedic Center San Juan County Blue Mountain Hospital San Juan Hospital Sanpete County Gunnison Valley Hospital Sanpete Valley Hospital Sevier County Sevier Valley Medical Center Summit County Park City Medical Center Tooele County Mountain West Medical Center Uintah County Ashley Valley Medical Center Utah County Mountain View Hospital Timpanogos Regional Hospital Wasatch County Heber Valley Medical Center Washington County Dixie Regional Medical Center Weber County Ogden Regional Medical Center Find Participating Providers Go to to look up participating providers for each plan. PAGE 4
5 Weber State University » Understanding Your Benefit Grid Understanding Your Benefits Grid DeDuctibles, Plan MaxiMuMs, and limits Medical Plan year Deductible $250 per individual, $500 per family. Does not apply to Out-of-Pocket Maximum 1 Only applies for inpatient, outpatient hospital ch Pharmacy Deductible Does not apply to Out-of-Pocket Maximum Plan year Out-of-Pocket Maximum Maximum Lifetime Benefit Pre-existing Condition Waiting Period inpatient facility services al and Surgical Requires Pre-notification lity Non-custodial $100 per individual, $200 per family. $2,000 per individual, $4,000 per family None 9-month Waiting Period waived with evid 90% of MAF after Deductible 90% of MAF after Co Copayment A specific amount you pay directly to a provider when you receive covered services. This can be either a fixed dollar amount or a percentage of the PEHP Maximum Allowable Fee. Contracted Contracted benefits apply when you receive covered services from contracted providers. You are responsible to pay the applicable copayment. Non-Contracted If your plan allows the use of non-contracted providers, noncontracted benefits apply when you receive covered services. You are responsible to pay the applicable copayment, plus the difference between the billed amount and PEHP s Maximum Allowable Fee (see Page 12). Maximum Allowable Fee (MAF) A schedule of maximum allowable fees established by PEHP and accepted by contracted providers, along with any required member copayment as payment in full (see Page 12) medical Deductible The set dollar amount that you must pay for yourself and/or your family members before PEHP begins to pay for covered medical benefits. Pharmacy deductible The set dollar amount separate from the medical plan year deductible that you must pay for pharmacy for yourself and/or your family members before PEHP begins to pay for covered pharmacy benefits. Plan Year Out-of-Pocket Maximum The maximum dollar amount that you and/ or your family pays each year for covered medical services in the form of copayments and coinsurance (includes deductibles on The STAR Plan). Maximum LIFETIME BENEFIT The total amount the plan pays for each covered family member in his or her lifetime. Pre-Existing Condition Waiting Period A condition that is present six months before your plan enrollment date for which medical treatment, consultation, or diagnostic testing was received. This section tells you if you have a waiting period before coverage for a preexisting condition begins. PAGE 5
6 Weber State University » Medical Benefits Grid» Advantage, Summit & Preferred Care Traditional (Non-HSA) Summit care Advantage care Preferred care * Services received by a non-contracted provider will be paid at a percentage of PEHP s Maximum Allowable Fee (MAF). You will be responsible for your assigned coinsurance and deductible (if applicable). You will also be responsible for any amounts billed by a noncontracted provider in excess of PEHP s Maximum Allowable Fee. There is no Out-of-Pocket Maximum for services received from a non-contracted provider. Contracted Provider Non-Contracted Provider Deductibles, Plan Maximums, and Limits Plan Year Deductible In and Out of Network Deductibles are combined $250 per individual, $500 per family Same as using a contracted provider *See Above for Additional Information **See Below for Additional Information Pharmacy Deductible $100 per individual, $200 per family Not applicable Plan year Out-of-Pocket Maximum Pharmacy Out-of-Pocket Maximum Does not apply to non-preferred drugs Specialty Drug Out-of-Pocket Maximum, office/outpatient Separate yearly out-of-pocket maximum $2,500 per individual $5,000 per double $7,500 per family $2,000 per individual Not applicable No Out-of-Pocket Maximum *See Above for Additional Information **See Below for Additional Information $3,600 per individual No Out-of-Pocket Maximum Maximum Lifetime Benefit None None Pre-existing Condition Waiting Period Does not apply to any individuals up to age 19 9-month Waiting Period waived or reduced with evidence of prior Creditable Coverage 9-month Waiting Period waived or reduced with evidence of prior Creditable Coverage **Applicable deductibles and coinsurance for services provided by a non-contracted provider will apply to your in-network plan year deductible and Out-of- Pocket Maximum. However, once your in-network deductible and Out-of-Pocket Maximum are met, coinsurance amounts for noncontracted providers will still apply. Inpatient facility services Medical and Surgical Requires pre-notification Skilled Nursing Facility Non-custodial Up to 60 days per plan year. Requires pre-authorization through Medical Case Management Hospice Up to 6 months in a 3-year period. Requires pre-authorization through Medical Case Management Rehabilitation Requires pre-authorization through Medical Case Management Mental Health and Substance Abuse Requires pre-authorization MAF = Maximum Allowable Fee Non-contracted providers may charge more than the MAF unless they have an agreement with you not to. Any amount above the MAF will be billed to you and will not count toward your deductible or out-of-pocket maximum. PAGE 6
7 Weber State University » Medical Benefits Grid» Advantage, Summit & Preferred Care Contracted Provider Non-Contracted Provider OUTPATIENT facility services Outpatient Facility and Ambulatory Surgery Ambulance (ground or air) 80% of MAF after deductible 80% of MAF after deductible Medical emergencies only, as determined by PEHP Emergency Room 80% of MAF, minimum $150 copayment per visit 80% of MAF, minimum $150 copayment per visit Medical emergencies only, as determined by PEHP. If admitted, inpatient facitlity benefit will be applied Urgent Care Facility 100% of MAF after $45 copayment per visit 60% of MAF after deductible University of Utah Medical Group Urgent Care Facility Preferred Care only Diagnostic Tests, X-rays, Minor For each test allowing $350 or less Diagnostic Tests, X-rays, Major For each test allowing more than $ % of MAF after $50 copayment per visit Not applicable Chemotherapy, Radiation, and Dialysis Dialysis with non-contracted providers requires pre-authorization Physical and Occupational Therapy Requires pre-authorization after 8 visits per plan year 100% of MAF after applicable office copayment per visit 60% of MAF after deductible professional services Inpatient Physician Visits 100% of MAF after applicable office copayment 60% of MAF after deductible per visit Surgery and Anesthesia Primary Care Office Visits and Office Surgeries 100% of MAF after $25 copayment per visit 60% of MAF after deductible Specialist Office Visits and Office Surgeries 100% of MAF after $35 copayment per visit 60% of MAF after deductible University of Utah Medical Group 100% of MAF after $50 copayment per visit Not applicable Preferred Care only Emergency Room Specialist 100% of MAF after $35 copayment per visit 100% of MAF after $35 copayment per visit Diagnostic Tests, X-rays, Minor For each test allowing $350 or less Diagnostic Tests, X-rays, Major For each test allowing more than $350 Mental Health and Substance Abuse No pre-authorization required for outpatient services. Inpatient services require pre-authorization Outpatient: 100% of MAF after $35 copayment per visit Inpatient: 80% of MAF after deductible Outpatient: 60% of MAF after deductible Inpatient: 60% of MAF after deductible MAF = Maximum Allowable Fee Non-contracted providers may charge more than the MAF unless they have an agreement with you not to. Any amount above the MAF will be billed to you and will not count toward your deductible or out-of-pocket maximum. PAGE 7
8 Weber State University » Medical Benefits Grid» Advantage, Summit & Preferred Care Contracted Provider Non-Contracted Provider prescription drugs Retail Pharmacy Up to 30-day supply Mail-Order 90-day supply Specialty Medications, retail pharmacy Up to 30-day supply Specialty Medications, office/outpatient Up to 30-day supply Specialty Medications, through specialty vendor Accredo Up to 30-day supply MISCELLANEOUS services Adoption See limitations Preferred generic: $10 copayment after deductible Preferred brand name: 75% of discounted cost after deductible. $25 minimum, no maximum copayment Non-preferred: 50% of discounted cost after deductible. $50 minimum, no maximum copayment Preferred generic: $20 copayment after deductible Preferred brand name: 75% of discounted cost after deductible. $50 minimum, no maximum copayment Non-preferred: 50% of discounted cost after deductible. $100 minimum, no maximum copayment Tier A: 80% of MAF after deductible. No maximum copayment Tier B: 70% of MAF after deductible. No maximum copayment Tier A: 80% of MAF after deductible. No maximum copayment Tier B: 70% of MAF after deductible. No maximum copayment Tier A: 80% of MAF after deductible. $150 maximum copayment Tier B: 70% of MAF after deductible. $225 maximum copayment 100% after deductible, up to $4,000 per adoption Plan pays up to the discounted cost, minus the applicable copayment. Member pays any balance Plan pays up to the discounted cost, minus the applicable copayment. Member pays any balance Plan pays up to the discounted cost, minus the preferred copayment. Member pays any balance 60% of MAF after deductible Not covered 100% after deductible, up to $4,000 per adoption Affordable Care Act Preventive Services 100% of MAF 60% of MAF after deductible See Master Policy for complete list Allergy Serum Chiropractic Care Up to 10 visits per plan year 100% of MAF after applicable office copayment 60% of MAF after deductible per visit Durable Medical Equipment, DME Except for oxygen and sleep disorder equipment, DME over $750, rentals that exceed 60 days, or as indicated in Appendix A of the Master Policy require pre-authorization. Maximum limits apply on many items. See the Master Policy for benefit limits Medical Supplies Home Health/Skilled Nursing Up to 60 visits per plan year. Requires pre-authorization and Medical Case Management Infertility Services Select services only. See the Master Policy 50% of MAF after deductible 30% of MAF after deductible Injections Requires pre-authorization if over $750 Temporomandibular Joint Dysfunction 50% of MAF after deductible 30% of MAF after deductible Up to $1,000 lifetime maximum **Some services on your plan are payable at a reduced benefit of 50% of Maximum Allowable Fee or 30% of Maximum Allowable Fee. These services do not apply to any Outof-Pocket Maximum. Deductible may apply. Refer to the Master Policy for specific criteria for the benefits listed above, as well as information on limitations and exclusions. MAF = Maximum Allowable Fee Non-contracted providers may charge more than the MAF unless they have an agreement with you not to. Any amount above the MAF will be billed to you and will not count toward your deductible or out-of-pocket maximum. PAGE 8
9 Weber State University » Medical Benefits Grid» Advantage & Summit STAR The PEHP STAR Plan (HSA-Qualified) Summit care* Advantage care* Refer to the applicable Master Policy for specific criteria for the benefits listed below, as well as information on limitations and Exclusions. * Services received by a non-contracted provider will be paid at a percentage of PEHP s Maximum Allowable Fee (MAF). You will be responsible for your assigned coinsurance and deductible (if applicable). You will also be responsible for any amounts billed by a non-contracted provider in excess of PEHP s Maximum Allowable Fee. There is no Out-of-Pocket Maximum for services received from a noncontracted provider. Deductibles, Plan Maximums, and Limits Plan Year Deductible $1,500 single plan $3,000 double or family plan Plan Year Out-of-Pocket Maximum Includes amounts applied to deductible and prescription drugs $2,500 single plan $5,000 double plan $7,500 family plan Maximum Lifetime Benefit None None Pre-existing Condition Waiting Period Does not apply to any individuals up to age 19 INPATIENT FACILITY SERVICES 9-month Waiting Period waived or reduced with evidence of prior Creditable Coverage Same as using a contracted provider *See Above for Additional Information No Out of Network Out-of-Pocket Maximum *See Above for Additional Information 9-month Waiting Period waived or reduced with evidence of prior Creditable Coverage Medical and Surgical Requires pre-authorization Skilled Nursing Facility Non-custodial Up to 60 days per plan year. Requires pre-authorization through Medical Case Management Hospice Up to 6 months in a 3-year period. Requires pre-authorization through Medical Case Management Rehabilitation Requires pre-authorization through Medical Case Management Mental Health and Substance Abuse Requires pre-authorization Contracted Provider Non-Contracted Provider 80% of MAF after deductible 80% of MAF after deductible MAF = Maximum Allowable Fee Non-contracted providers may charge more than the MAF unless they have an agreement with you not to. Any amount above the MAF will be billed to you and will not count toward your deductible or out-of-pocket maximum. PAGE 9
10 Weber State University » Medical Benefits Grid» Advantage & Summit STAR OUTPATIENT facility services Outpatient Facility and Ambulatory Surgery Ambulance (ground or air) 80% of MAF after deductible 80% of MAF after deductible Medical emergencies only, as determined by PEHP Emergency Room 80% of MAF after deductible 80% of MAF after deductible Medical emergencies only, as determined by PEHP Urgent Care Facility Diagnostic Tests, X-rays, Minor For each test allowing $350 or less Diagnostic Tests, X-rays, Major For each test allowing more than $350 Chemotherapy, Radiation, and Dialysis Dialysis with non-contracted providers requires pre-authorization Physical and Occupational Therapy Requires pre-authorization after 8 visits Contracted Provider Non-Contracted Provider professional services Inpatient Physician Visits Surgery and Anesthesia Primary Care Office Visits and Office Surgeries Specialist Office Visits and Office Surgeries Emergency Room Specialist 80% of MAF after deductible 80% of MAF after deductible Diagnostic Tests, X-rays, Minor For each test allowing $350 or less Diagnostic Tests, X-rays, Major For each test allowing more than $350 Immunizations 100% of MAF 60% of MAF after deductible Mental Health and Substance Abuse Up to 30 visits per plan year for outpatient services. No pre-authorization required for outpatient services. Inpatient services require pre-authorization Outpatient: 50% of MAF after deductible Inpatient: 80% of MAF after deductible Outpatient: 30% of MAF after deductible Inpatient: 60% of MAF after deductible MAF = Maximum Allowable Fee Non-contracted providers may charge more than the MAF unless they have an agreement with you not to. Any amount above the MAF will be billed to you and will not count toward your deductible or out-of-pocket maximum. PAGE 10
11 Weber State University » Medical Benefits Grid» Advantage & Summit STAR prescription drugs Retail Pharmacy Up to 30-day supply Mail-Order 90-day supply Specialty Medications, retail pharmacy Up to 30-day supply Contracted Provider Preferred generic: $10 copayment after deductible Preferred brand name: 75% of discounted cost after deductible. $25 minimum, no maximum copayment Non-preferred: 50% of discounted cost after deductible. $50 minimum, no maximum copayment Preferred generic: $20 copayment after deductible Preferred brand name: 75% of discounted cost after deductible. $50 minimum, no maximum copayment Non-preferred: 50% of discounted cost after deductible. $100 minimum, no maximum copayment Tier A: 80% of MAF after deductible. No maximum copayment. Tier B: 70% of MAF after deductible. No maximum copayment. Non-Contracted Provider Plan pays up to the discounted cost after deductible, minus the applicable copayment. Member pays any balance Plan pays up to the discounted cost after deductible, minus the applicable copayment. Member pays any balance Plan pays up to the discounted cost after deductible, minus the applicable copayment. Member pays any balance Specialty Medications, office/outpatient Up to 30-day supply Specialty Medications, through specialty vendor Accredo Up to 30-day supply MISCELLANEOUS services Adoption See limitations Tier A: 80% of MAF after deductible. No maximum copayment. Tier B: 70% of MAF after deductible. No maximum copayment. Tier A: 80% of MAF after deductible. $150 maximum copayment. Tier B: 70% of MAF after deductible. $225 maximum copayment. 100% after deductible, up to $4,000 per adoption 60% of MAF after deductible Not covered 100% after deductible, up to $4,000 per adoption Affordable Care Act Preventive Services 100% of MAF 60% of MAF after deductible See Master Policy for complete list Allergy Serum Chiropractic Care Up to 10 visits per plan year Durable Medical Equipment, DME Except for oxygen and sleep disorder equipment, DME over $750, rentals that exceed 60 days, or as indicated in Appendix A of the Master Policy require pre-authorization. Maximum limits apply on many items. See the Master Policy for benefit limits Medical Supplies Home Health/Skilled Nursing Up to 60 visits per plan year. Requires pre-authorization and Medical Case Management Infertility Services Select services only. See the Master Policy for details 50% of MAF after deductible 30% of MAF after deductible Injections Requires pre-authorization if over $750 Temporomandibular Joint Dysfunction Up to $1,000 lifetime maximum 50% of MAF after deductible 30% of MAF after deductible MAF = Maximum Allowable Fee Non-contracted providers may charge more than the MAF unless they have an agreement with you not to. Any amount above the MAF will be billed to you and will not count toward your deductible or out-of-pocket maximum. PAGE 11
12 Weber State University » Weber State Benefits Preview» Supplemental Pharmacy Supplemental Pharmacy Weber State University has established a supplemental plan with PEHP to cover members whose individual out-of-pocket pharmacy costs exceed $2,000 during the plan year. While the State pharmacy out-of-pocket maximum is $3,000, Weber State s supplemental coverage will cap your qualified out-of-pocket pharmacy expenses at $2,000 per individual per plan year. Out-of-pocket costs that apply to this supplemental coverage include preferred generic drugs, preferred brand name drugs, and preferred specialty medications obtained through the pharmacy benefit. Out-of-pocket costs that are not eligible for supplemental coverage include non-preferred drugs, the cost difference between generic drug and brand name drugs when a substitute is available, and specialty medications obtained through the medical benefit. Meeting your deductible» It is PEHP s discounted cost of an eligible medication that is applied toward the deductible.» Once the deductible is met, you are responsible to pay the applicable copayment or coinsurance. Meeting your pharmacy out-of-pocket Maximum» Your Pharmacy deductible does apply to the pharmacy out-of-pocket maximum.» If your pharmacy deductible is applied to the purchase of a non-preferred medication, it does not apply to the out-of-pocket maximum because non-preferred medications do not apply to the pharmacy out-ofpocket maximum.» Once your pharmacy deductible is met, your pharmacy copayments or coinsurances are applied to your pharmacy out-of-pocket maximum.
13 Weber State University » Benefits Preview» Understanding Your EOBs 9 8 Understanding Your EOB (Explanation of Benefits) We send an EOB each time we process a claim for you or someone on your plan. Go paperless and view EOBs at your mypehp account at. AMOUNT CHARGED The medical provider s (e.g., doctor, hosptial, or clinic) bill for your service. AMOUNT INELIGIBLE The part of the bill that includes services not covered by your plan. This is between you and the provider. AMOUNT ELIGIBLE This is PEHP s maximum allowable fee (MAF). This is the most we allow contracted providers to charge for this service. However, non-contracted providers may charge more than the MAF. Avoid paying more by using only contracted providers (find them at ). DEDUCTIBLE The set amount you pay for eligible charges in a plan year before cost sharing takes place COINSURANCE The percentage of the cost you must pay under your plan. You may already have paid this amount when you received services. If so, the provider s bill may be lower than what s shown on the EOB. COPAY The fixed dollar amount you must pay under your plan. You may already have paid this amount when you received services. If so, the provider s bill may be lower than what s shown on the EOB. AMOUNT PAID The part of the bill PEHP paid. CLAIM NUMBER Keep this number as reference if you call PEHP about your claim. YOUR TOTAL RESPONSIBILITY The amount of the bill the provider expects you to pay. This is between you and the provider. See your applicable benefits summary and master policy for complete terms of your plan. 3/26/12
14 Weber State University » Benefits Preview» mypehp How to Set Up Your mypehp Account during open enrollment, You can access online enrollment. You can also access your claims history, explanation of benefits (EOB) and coverage levels online at my PEHP. You can enroll, access claims history, download explanation of benefits (EOB), check coverage levels, and much more by logging on to mypehp. Step 4: Enter your Social Security number, date of birth, and PEHP subscriber ID number to verify your identity. The 16-digit subscriber ID number can be found on your Medco/PEHP insurance card. If you do not have the number, call PEHP or fill out the online request to receive your ID number in the mail. Then, you will be asked to select a user name and password for future access. Here s how to set up your personal account: Step 1: Go to Step 2: Locate the mypehp Login on the right side of the page. The first time you log in, you must create an account. Once you have successfully set up your profile, enter your user ID and password into the boxes to access your information. Once you have successfully logged in, you are ready to enroll during open enrollment. You will also see a summary of all the plans you have enrolled in, a detailed list of all claims submitted to PEHP, and PDF files of your EOBs. You may also update your mailing address. However, if you wish to make any other changes outside of annual enrollment to your existing plans, you must submit a signed Change Form to PEHP. StepS FOR ONLINE ENROLLMENT: See next page. Step 3: To set up an account, click on Create my PEHP account. You must agree to the conditions detailed in the document on the next page to proceed. Once you have read and agreed to the terms, click I Agree to continue creating your personal profile. Graphical website depictions may vary from actual website.
15 Weber State University » Benefits Preview» Online Enrollment How to Enroll Online During open enrollment, if you re not adding or deleting dependents or changing benefit plans, you don t need to re-enroll. You must reenroll in FLEX$ every year. During open enrollment, online enrollment is available to active employees who have PEHP medical coverage. Early retirees, COBRA, and LTD enrollees must complete a paper enrollment form to make any plan changes. During open enrollment, online enrollment for FLEX$ is available only if you have been previously enrolled in medical and FLEX$. Otherwise, you must complete a paper enrollment form. New employees must complete enrollment forms for all plans. STEP 1: Log in to your mypehp account. See instructions on the previous page about how to create yours. STEP 5: Select among plans. STEP 2: If you re a returning user, you ll be directed to the mypehp main page. During open enrollment, you will have access to online enrollment through a link on the menu at left. STEP 3: You ll go straight to the online enrollment main page. It shows the PEHP benefits available to you. STEP 6: Add dependents by clicking New Dependent. STEP 7: If you, your spouse, or any dependents are covered by another health plan, supply the information. STEP 4: Click Enroll beneath the desired benefit to begin. For assistance with online enrollment, call or Graphical website depictions may vary from actual website. STEP 8: When you are finished adding dependents and other coverage information, you will have the opportunity to carefully review your information. Click the box after you have read the terms and conditions and signify you agree to them by typing your name. Once you click Confirm you will not be able to make additional changes to your medical plan. STEP 9: You will receive an enrollment confirmation. Click Print for a print-formatted PDF. This confirmation is for your personal records. When you return, the main page will show the benefits in which you have enrolled. NOTE: You can change your FLEX$ amount at anytime through May 15.
16
Snow College » Introduction. Snow College Snow College Benefits Summary
 Snow College 2016-17» Introduction Snow College 2016-17 SNOW COLLEGE Benefits Summary Effective July 2016 2016 Public Employees Health Program Snow College Benefits Summary This Benefits Summary should
Snow College 2016-17» Introduction Snow College 2016-17 SNOW COLLEGE Benefits Summary Effective July 2016 2016 Public Employees Health Program Snow College Benefits Summary This Benefits Summary should
Jordan School District
 Jordan School District 2014-2015 PEHP JORDAN SCHOOL DISTRICT Advantage, SUMMIT, AND Preferred Care MEDICAL PLANS Effective September 2014 Advantage, Summit and Preferred Care Medical Benefits 2014 Public
Jordan School District 2014-2015 PEHP JORDAN SCHOOL DISTRICT Advantage, SUMMIT, AND Preferred Care MEDICAL PLANS Effective September 2014 Advantage, Summit and Preferred Care Medical Benefits 2014 Public
Enrollment Guide Weber State University. Look inside for an overview of your benefits and what s new for the plan year.
 2017-2018 Enrollment Guide Weber State University Look inside for an overview of your benefits and what s new for the 2017-18 plan year. PROUDLY SERVING UTAH PUBLIC EMPLOYEES Contact Introduction Information
2017-2018 Enrollment Guide Weber State University Look inside for an overview of your benefits and what s new for the 2017-18 plan year. PROUDLY SERVING UTAH PUBLIC EMPLOYEES Contact Introduction Information
Summary of Benefits. Wasatch Essential, Wasatch Enhanced, Southwest and Central Utah, Cache Valley.
 Summary of Benefits Wasatch Essential, Wasatch Enhanced, Southwest and Central Utah, Cache Valley. 1 Our Plan. Your Advantage. >> $0 or low monthly premium >> $0 medical deductible >> $0 copay for all
Summary of Benefits Wasatch Essential, Wasatch Enhanced, Southwest and Central Utah, Cache Valley. 1 Our Plan. Your Advantage. >> $0 or low monthly premium >> $0 medical deductible >> $0 copay for all
Super Blue Plus QHDHP HDHP Non Emb 100%
 Super Blue Plus QHDHP 1 2017 HDHP Non Emb 100% Effective Date April 1, 2018 to November 31, 2018, then restart December 1, 2018. Benefit Period (used for Deductible and Coinsurances limits and certain
Super Blue Plus QHDHP 1 2017 HDHP Non Emb 100% Effective Date April 1, 2018 to November 31, 2018, then restart December 1, 2018. Benefit Period (used for Deductible and Coinsurances limits and certain
SelectHealth. It all starts with one good choice UTAH INDIVIDUAL PLANS
 2017 UTAH INDIVIDUAL PLANS Improving health is a journey and the hardest step is always the first. We re committed to helping our community stay healthy by providing access to high-quality healthcare at
2017 UTAH INDIVIDUAL PLANS Improving health is a journey and the hardest step is always the first. We re committed to helping our community stay healthy by providing access to high-quality healthcare at
MEDICAL DENTAL VOLUNTARY BENEFITS OVERVIEW. New Hire Enrollment: FY Human Resources I Benefits
 MEDICAL I DENTAL I VOLUNTARY BENEFITS OVERVIEW New Hire Enrollment: FY 2016-2017 Human Resources I Benefits TABLE OF CONTENTS Eligibility and Enrollment 2-3 How to Enroll in PEHP 4 Insurance Premiums 5-6
MEDICAL I DENTAL I VOLUNTARY BENEFITS OVERVIEW New Hire Enrollment: FY 2016-2017 Human Resources I Benefits TABLE OF CONTENTS Eligibility and Enrollment 2-3 How to Enroll in PEHP 4 Insurance Premiums 5-6
Coverage for: Individual and Family plans Plan Type: PPO
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/18-6/30/19 Group Name: Salt Lake City STAR Summit Coverage for: Individual and Family plans
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/18-6/30/19 Group Name: Salt Lake City STAR Summit Coverage for: Individual and Family plans
An Overview of Your Health and Dental Benefits
 An Overview of Your Health and Dental Benefits Educators Health Alliance Direct Bill Plan 2 \ EDUCATORS HEALTH ALLIANCE HEALTH AND DENTAL PLAN OPTIONS Exclusively for Educators Health Alliance Direct Bill
An Overview of Your Health and Dental Benefits Educators Health Alliance Direct Bill Plan 2 \ EDUCATORS HEALTH ALLIANCE HEALTH AND DENTAL PLAN OPTIONS Exclusively for Educators Health Alliance Direct Bill
Medical Plan Summary: PPO Core Plan
 Medical Plan Summary: PPO Core Plan Healthcare is one of the most important and necessary parts of your benefit package. The following is a summary of our benefit plan. For a more detailed explanation
Medical Plan Summary: PPO Core Plan Healthcare is one of the most important and necessary parts of your benefit package. The following is a summary of our benefit plan. For a more detailed explanation
Maximums Note: Out-of-Pocket maximum is the amount of covered expenses that you and/or your covered dependents will pay.
 PRIORITY HEALTH priorityhealth.com PRIORITYHMO SUMMARY OF BENEFITS 100% HOSPITAL PLAN State of Michigan Active Plan October 14, 2012 - October 13, 2013 The following information is provided as a summary
PRIORITY HEALTH priorityhealth.com PRIORITYHMO SUMMARY OF BENEFITS 100% HOSPITAL PLAN State of Michigan Active Plan October 14, 2012 - October 13, 2013 The following information is provided as a summary
PEIA PPB Plan A Benefits At a Glance
 PEIA PPB Plan A Benefits At a Glance Benefit Description PEIA PPB Plan A In-Network PEIA PPB Plan A Out-of-Network Annual deductible Varies by salary and employer type. See premium charts. Twice the in-network
PEIA PPB Plan A Benefits At a Glance Benefit Description PEIA PPB Plan A In-Network PEIA PPB Plan A Out-of-Network Annual deductible Varies by salary and employer type. See premium charts. Twice the in-network
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
Super Blue Plus QHDHP 1 HDHP Non Emb 100%
 Super Blue Plus QHDHP 1 HDHP Non Emb 100% Effective Date December 1, 2018 Benefit Period 2 (used for Deductible and Coinsurances limits and certain Contract Year benefit frequencies.) Note: All Services
Super Blue Plus QHDHP 1 HDHP Non Emb 100% Effective Date December 1, 2018 Benefit Period 2 (used for Deductible and Coinsurances limits and certain Contract Year benefit frequencies.) Note: All Services
ARUP Laboratories, Inc. EPO Medical 750 Plan Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/aruplabs/ or by calling 1-888-271-5870.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/aruplabs/ or by calling 1-888-271-5870.
The Harvard Pilgrim Primary Choice HMO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services
 Massachusetts The Harvard Pilgrim Primary Choice HMO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 07/01/2018 06/30/2019 Coverage for: Individual
Massachusetts The Harvard Pilgrim Primary Choice HMO Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 07/01/2018 06/30/2019 Coverage for: Individual
Anthem BlueCross BlueShield Christian Care Communities Blue Access PPO Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-650-4047. Important Questions
Are there services covered before you meet your deductible?
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18-12/31/18 Salt Lake County HDHP Summit Coverage for: Individual and Family plans Plan
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 1/1/18-12/31/18 Salt Lake County HDHP Summit Coverage for: Individual and Family plans Plan
Adventist Health System Schedule of Benefits for Adventist Health System Effective January 1, 2018
 Adventist Health System Schedule of Benefits for Adventist Health System Effective January 1, 2018 High Health Plan with Health Savings Account (Health Savings Plan) TIER 1 TIER 2 TIER 3 CALENDAR YEAR
Adventist Health System Schedule of Benefits for Adventist Health System Effective January 1, 2018 High Health Plan with Health Savings Account (Health Savings Plan) TIER 1 TIER 2 TIER 3 CALENDAR YEAR
schedule of benefits INDIVIDUAL PPO PLAN What s covered under your SummaCare plan This plan is underwritten by the Summa Insurance Company
 schedule of benefits What s covered under your SummaCare plan INDIVIDUAL PPO PLAN 10-70 This plan is underwritten by the Summa Insurance Company PPO10-70 REV0707 www.summacare.com The following is a Schedule
schedule of benefits What s covered under your SummaCare plan INDIVIDUAL PPO PLAN 10-70 This plan is underwritten by the Summa Insurance Company PPO10-70 REV0707 www.summacare.com The following is a Schedule
Summary Of Benefits. UTAH Davis, Salt Lake, Utah and Weber. Healthy Advantage Plus (HMO)
 Summary Of Benefits UTAH Davis, Salt Lake, Utah and Weber Healthy Advantage Plus (HMO) (877) 644-0344, TTY/TDD 711 7 days a week, 8 a.m. 8 p.m. local time HealthyAdvantagePlus.org 2018 H5628_18_1099_0007_HPSB
Summary Of Benefits UTAH Davis, Salt Lake, Utah and Weber Healthy Advantage Plus (HMO) (877) 644-0344, TTY/TDD 711 7 days a week, 8 a.m. 8 p.m. local time HealthyAdvantagePlus.org 2018 H5628_18_1099_0007_HPSB
Coverage for: Individual and Family plans Plan Type: PPO
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/18-6/30/19 Dixie State STAR Summit & Advantage Coverage for: Individual and Family plans
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/18-6/30/19 Dixie State STAR Summit & Advantage Coverage for: Individual and Family plans
Important Questions Answers Why This Matters: If took HealthQuotient:
 HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
(30- to 34-day supply) 100% after $40 copay; significant or new therapeutic class drugs: 50%
 C O U N T Y S I N T R A N E T S I T E : H T T P : / / I N T R A N E T. C O. R I V E R S I D E. C A. U S 25 Exclusive Care Select Medicare Coordination Plan Tier 1: Exclusive Care Network Tier 2: Any Provider
C O U N T Y S I N T R A N E T S I T E : H T T P : / / I N T R A N E T. C O. R I V E R S I D E. C A. U S 25 Exclusive Care Select Medicare Coordination Plan Tier 1: Exclusive Care Network Tier 2: Any Provider
Aetna Choice POS II Medical Plan PLAN FEATURES NETWORK OUT-OF-NETWORK. Individual Deductible* $1,000 $2,000. Family Deductible* $2,000 $4,000
 Schedule of Benefits Employer: Adobe Systems Incorporated ASC: 660819 Effective Date: January 1, 2012 Schedule: 2B Booklet Base: 1 For: Aetna Choice POS II 80/60 Plan This is an ERISA plan, and you have
Schedule of Benefits Employer: Adobe Systems Incorporated ASC: 660819 Effective Date: January 1, 2012 Schedule: 2B Booklet Base: 1 For: Aetna Choice POS II 80/60 Plan This is an ERISA plan, and you have
AvMed In-Network Tier A Providers: $1,500 individual / $3,000 family AvMed In-Network Tier B Providers: What is the overall deductible?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
Retirees with Medicare (RETIREMENT DATE ON or AFTER March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2019
 Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
PLAN DESIGN AND BENEFITS - IN MANAGED CHOICE POS OPEN ACCESS 90/60/60 $1,000 PREFERRED CARE
 PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
PLAN FEATURES NON- Deductible (per calendar year) $1,000 Individual $2,000 Individual $2,000 Family $4,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
Retirees with Medicare (RETIREMENT DATE BEFORE March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2019
 Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana
Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana
You must pay all of the costs for these services up to the specific deductible amount before this plan begins to pay for these services.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-477-8768. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.empireblue.com/eocdps/fi or by calling 1-855-220-3341.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.empireblue.com/eocdps/fi or by calling 1-855-220-3341.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Retirees with Medicare (RETIREMENT DATE BEFORE March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2017
 Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers (retirement date BEFORE 3/1/2015) Magnolia Local Plus Blue
Network Eligible OGB Members Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers (retirement date BEFORE 3/1/2015) Magnolia Local Plus Blue
What is the overall deductible? Are there other deductibles for specific services? Is there an out-ofpocket
 Association of Washington Cities HealthFirst 250 Medical Plan Coverage Period: 01/01/2016 12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
Association of Washington Cities HealthFirst 250 Medical Plan Coverage Period: 01/01/2016 12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
CHRISTUS Health Plan Generations (HMO) Summary of Benefits. Finally, access to the doctor and hospital you know and trust. christushealthplan.
 CHRISTUS Health Plan Generations Summary of Benefits Finally, access to the doctor and hospital you know and trust. christushealthplan.org Summary of Benefits CHRISTUS Health Plan Generations H1189 This
CHRISTUS Health Plan Generations Summary of Benefits Finally, access to the doctor and hospital you know and trust. christushealthplan.org Summary of Benefits CHRISTUS Health Plan Generations H1189 This
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-603-7982. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-855-603-7982. Important Questions
Regence HDHP-1 with Alternative Care Coverage Period: 01/01/ /31/2017
 Regence HDHP-1 with Alternative Care Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2017-12/31/2017 Coverage for: Individual & Eligible Family Plan Type:
Regence HDHP-1 with Alternative Care Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2017-12/31/2017 Coverage for: Individual & Eligible Family Plan Type:
Regence BlueShield: Choice HSA 1500 Coverage Period: 01/01/ /31/2016
 Regence BlueShield: Choice HSA 1500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual & Eligible Family Plan Type:
Regence BlueShield: Choice HSA 1500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual & Eligible Family Plan Type:
$1,500 Individual/$3,000 Family for participating providers. $3,000 Individual/$6,000. Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
Sigma-Aldrich Corporation Healthcare Plans MEDIUM Option Coverage Period: 01/01/ /31/2016 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mysialbenefits.com or by calling 1-877-335-7515, option
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mysialbenefits.com or by calling 1-877-335-7515, option
Summary of Benefits. Wasatch Essential, Wasatch Enhanced.
 Summary of Benefits Wasatch Essential, Wasatch Enhanced. 1 Our Plan. Your Advantage. The advantage is not only in our superior service, but in our outstanding benefits. In addition to our always $0 medical
Summary of Benefits Wasatch Essential, Wasatch Enhanced. 1 Our Plan. Your Advantage. The advantage is not only in our superior service, but in our outstanding benefits. In addition to our always $0 medical
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 Anthem HealthKeepers Premier POS: Henrico County General Government and Public Schools Coverage Period: 1/1/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
Anthem HealthKeepers Premier POS: Henrico County General Government and Public Schools Coverage Period: 1/1/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage
GEORGIA. CIGNA health savings plans. Health and Pharmacy Benefits c GA 07/ CIGNA
 GEORGIA Individual & Family Plans CIGNA health savings plans Health and Pharmacy Benefits PLAN comparison 822163c GA 07/10 2010 CIGNA CIGNA HealthCare plans, offered through Connecticut General Life Insurance
GEORGIA Individual & Family Plans CIGNA health savings plans Health and Pharmacy Benefits PLAN comparison 822163c GA 07/10 2010 CIGNA CIGNA HealthCare plans, offered through Connecticut General Life Insurance
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 333-5735.
Summary of Benefits. January 1, 2016 to December 31, 2016
 Summary of Benefits Summary of Benefits January 1, 2016 to December 31, 2016 This booklet gives you a summary of what we cover and what you pay. It doesn t list every service that we cover or list every
Summary of Benefits Summary of Benefits January 1, 2016 to December 31, 2016 This booklet gives you a summary of what we cover and what you pay. It doesn t list every service that we cover or list every
MEDICAL SCHEDULE OF BENEFITS COPAY GOLD
 LIFETIME MAXIMUM BENEFIT Unlimited CALENDAR YEAR MAXIMUM BENEFIT CALENDAR YEAR DEDUCTIBLE Single Family CALENDAR YEAR OUT-OF-POCKET MAXIMUM (includes medical Deductible, medical Coinsurance, medical Copays
LIFETIME MAXIMUM BENEFIT Unlimited CALENDAR YEAR MAXIMUM BENEFIT CALENDAR YEAR DEDUCTIBLE Single Family CALENDAR YEAR OUT-OF-POCKET MAXIMUM (includes medical Deductible, medical Coinsurance, medical Copays
University of Cincinnati Medical Plan Summary and Comparison Non AAUP - Effective January 1- December 31, 2018
 Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
Annual Deductible Annual Health Savings Account Funding (UC) $1500 individual $3,000 family Varies by Annual Base Pay as of 1/1/18 $3,000 per person $6,000 family Varies by Annual Base Pay as of 1/1/18
Retirees with Medicare (RETIREMENT DATE ON or AFTER March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2017
 Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Pelican HRA1000 Magnolia Local Plus Network Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Regence BlueCross BlueShield of Oregon: Preferred Coverage Period: 07/01/ /31/2016
 Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
Schedule of Benefits Phoenix Health Plans, Inc.
 Your Policy gives You important information about Your health care benefits. It includes information such as Pre-Authorization requirements. This Schedule of Benefits is issued to You with Your Policy.
Your Policy gives You important information about Your health care benefits. It includes information such as Pre-Authorization requirements. This Schedule of Benefits is issued to You with Your Policy.
Medical Plan. Comparison
 Medical Plan Comparison 2018 ATTENTION: This Medical Plan Comparison is considered a summary of material modifications (SMM) to one or more of the WHOI benefit plans. It contains a summary of important
Medical Plan Comparison 2018 ATTENTION: This Medical Plan Comparison is considered a summary of material modifications (SMM) to one or more of the WHOI benefit plans. It contains a summary of important
Important Questions Answers Why this Matters: Network: $500 Individual / $1,000 Family Non-Network: $1,000 Individual / $2,000 Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-262-4772.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-262-4772.
Non-Medicare Retirees (RETIREMENT DATE BEFORE March 1, 2015) Benefits Comparison Benefits effective January 1, December 31, 2019
 Network Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Network Pelican HRA1000 Blue Cross and Blue Shield of Louisiana Preferred Care Providers & Blue Cross National Providers Magnolia Local Plus Blue Cross and Blue Shield of Louisiana Preferred Care Providers
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summacare.com or by calling 1-800-996-8701. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summacare.com or by calling 1-800-996-8701. Important
Anthem Blue Cross Your Plan: Premier HMO 10/100% - MUST Trust Your Network: California Care HMO
 Anthem Blue Cross Your Plan: Premier HMO 10/100% - MUST Trust Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Premier HMO 10/100% - MUST Trust Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Regence BlueShield: Engage 70 Coverage Period: 11/01/ /31/2017
 Regence BlueShield: Engage 70 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 11/01/2016 10/31/2017 Coverage for: Individual and Eligible Family Plan Type: PPO
Regence BlueShield: Engage 70 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 11/01/2016 10/31/2017 Coverage for: Individual and Eligible Family Plan Type: PPO
Schedule of Benefits Allegian Health Plans
 NOTE: This consumer choice health benefit plan does not include all state mandated health insurance benefits. The following benefit is provided at a reduced level from what is mandated: Mandated Benefit
NOTE: This consumer choice health benefit plan does not include all state mandated health insurance benefits. The following benefit is provided at a reduced level from what is mandated: Mandated Benefit
Coverage for: Single Enrollee Plan Type: TRAD/PPO. Important Questions Answers Why This Matters: $2,500/single Network $5,000/single Non-Network
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 STRS OHIO : Basic Plan with Medicare Part B Only Coverage for: Single
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018-12/31/2018 STRS OHIO : Basic Plan with Medicare Part B Only Coverage for: Single
What is the overall deductible?
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/2018 6/30/2019 WEA Trust Essential Health Plan: Kenosha School District Coverage for: Individual/Family
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 7/1/2018 6/30/2019 WEA Trust Essential Health Plan: Kenosha School District Coverage for: Individual/Family
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-800-342-9816. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-800-342-9816. Important
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.etf.wi.gov or by calling 1-877-533-5020. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.etf.wi.gov or by calling 1-877-533-5020. Important Questions
EMPLOYEE BENEFITS GUIDE SEPTEMBER 1, 2017 AUGUST 31, 2018
 EMPLOYEE BENEFITS GUIDE SEPTEMBER 1, 2017 AUGUST 31, 2018 If you have questions regarding Call Click General Benefits Information Sue Medina (435) 833-1900 Ext. 1103 smedina@tooeleschools.org Medical
EMPLOYEE BENEFITS GUIDE SEPTEMBER 1, 2017 AUGUST 31, 2018 If you have questions regarding Call Click General Benefits Information Sue Medina (435) 833-1900 Ext. 1103 smedina@tooeleschools.org Medical
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling (855) 333-5735.
01/01/ /31/2019 UMR: PALO PINTO GENERAL HOSPITAL:
 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 UMR: PALO PINTO GENERAL HOSPITAL: 7670-00-160036 001 Coverage for: Individual
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2019 12/31/2019 UMR: PALO PINTO GENERAL HOSPITAL: 7670-00-160036 001 Coverage for: Individual
Regence BlueShield: Innova 2500 Coverage Period: 11/01/ /31/2017
 Regence BlueShield: Innova 2500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 11/01/2016 10/31/2017 Coverage for: Individual and Eligible Family Plan Type: PPO
Regence BlueShield: Innova 2500 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 11/01/2016 10/31/2017 Coverage for: Individual and Eligible Family Plan Type: PPO
What is the overall deductible? Are there other deductibles for specific services? Is there an out-ofpocket
 Regence BlueShield: Regence Direct Silver with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers &
Regence BlueShield: Regence Direct Silver with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers &
MEDICAL SCHEDULE OF BENEFITS COPAY GOLD
 LIFETIME MAXIMUM BENEFIT CALENDAR YEAR MAXIMUM BENEFIT CALENDAR YEAR DEDUCTIBLE Single Family CALENDAR YEAR OUT-OF-POCKET MAXIMUM (includes medical Deductible, medical Coinsurance, medical Copays and Precertification
LIFETIME MAXIMUM BENEFIT CALENDAR YEAR MAXIMUM BENEFIT CALENDAR YEAR DEDUCTIBLE Single Family CALENDAR YEAR OUT-OF-POCKET MAXIMUM (includes medical Deductible, medical Coinsurance, medical Copays and Precertification
MEDICAL SCHEDULE OF BENEFITS HDHP $4,000 PLAN
 MEDICAL SCHEDULE OF BENEFITS HDHP $4,000 PLAN HDHP 4000 LIFETIME MAXIMUM BENEFIT CALENDAR YEAR MAXIMUM BENEFIT Unlimited Unlimited CALENDAR YEAR DEDUCTIBLE (combined with Prescription Drug Card Deductible)
MEDICAL SCHEDULE OF BENEFITS HDHP $4,000 PLAN HDHP 4000 LIFETIME MAXIMUM BENEFIT CALENDAR YEAR MAXIMUM BENEFIT Unlimited Unlimited CALENDAR YEAR DEDUCTIBLE (combined with Prescription Drug Card Deductible)
MIT Affiliate Health Plans
 MIT Affiliate Health Plans 2017 2018 Overview In this book: Insurance plans and rates How to enroll Your medical benefits Commonly used terms Useful contact information 1 Insurance plans and rates MIT
MIT Affiliate Health Plans 2017 2018 Overview In this book: Insurance plans and rates How to enroll Your medical benefits Commonly used terms Useful contact information 1 Insurance plans and rates MIT
Schedule of Benefits (GR-9N-S DE)
 Schedule of Benefits (GR-9N-S-01-001-01 DE) Plan Sponsor: The Church of Jesus Christ of Latter-Day Saints-Senior Missionaries Group Policy Number: 840232 Issue Date: June 3, 2013 Effective Date: August
Schedule of Benefits (GR-9N-S-01-001-01 DE) Plan Sponsor: The Church of Jesus Christ of Latter-Day Saints-Senior Missionaries Group Policy Number: 840232 Issue Date: June 3, 2013 Effective Date: August
01/01/ /31/2018 FLORIDA SCHOOLS HEALTH INSURANCE PROG:
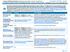 Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018 12/31/2018 FLORIDA SCHOOLS HEALTH INSURANCE PROG: 7670-00-410536 010 020 Coverage
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 01/01/2018 12/31/2018 FLORIDA SCHOOLS HEALTH INSURANCE PROG: 7670-00-410536 010 020 Coverage
What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-376-6651. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-376-6651. Important Questions
Even though you pay these expenses, they don t count toward the outof-pocket limit.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summit-inc.net or www.yctrust.net or by calling Summit
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.summit-inc.net or www.yctrust.net or by calling Summit
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling 1-800-542-9402.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/fi or by calling 1-800-542-9402.
For: 80/20 Plan for Retired Employees Over Age 65 and Dependents
 Schedule of Benefits Employer: Cornell University ASC: 397366 Issue Date: September 1, 2010 Effective Date: September 1, 2010 Schedule: 11A Booklet Base: 11 For: 80/20 Plan for Retired Employees Over Age
Schedule of Benefits Employer: Cornell University ASC: 397366 Issue Date: September 1, 2010 Effective Date: September 1, 2010 Schedule: 11A Booklet Base: 11 For: 80/20 Plan for Retired Employees Over Age
BH Media Group, Inc. Coverage Period: 01/01/ /31/2016
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: HDHP What is the overall deductible? This is only a summary. If you want more detail about
Lee s Summit School District
 Plan Type Plan Description (Visit our website at www.bluekc.com to receive a complete listing of network hospitals and physicians) Lee s Summit School District Effective Date: 1/1/16 Health Benefit Plan
Plan Type Plan Description (Visit our website at www.bluekc.com to receive a complete listing of network hospitals and physicians) Lee s Summit School District Effective Date: 1/1/16 Health Benefit Plan
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Schedule of Benefits. Plan Information. Member Cost Sharing
 Schedule of Benefits Panther Gold Plan - Enhanced Access HMO Applies to Bradford, Johnstown and Greensburg campuses only HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600
Schedule of Benefits Panther Gold Plan - Enhanced Access HMO Applies to Bradford, Johnstown and Greensburg campuses only HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600
Important Questions Answers Why this Matters: For in-network providers: $11,000 Individual $22,000 Family of 2 or more
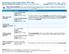 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/burton-lumber/or by calling 1-888-271-5870.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.uhealthplan.utah.edu/burton-lumber/or by calling 1-888-271-5870.
AvMed Network: $1,500 individual / $3,000 family Doesn t apply to preventive care. What is the overall deductible?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-376-6651. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.avmed.org or by calling 1-800-376-6651. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-855-333-5734. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.empireblue.com or by calling 1-855-333-5734. Important
SERVICES WITH A 1 MAY REQUIRE PRIOR AUTHORIZATION
 Monthly Plan Premium YOU PAY $0 You must continue to pay your Medicare Part C Deductible YOU PAY nothing This plan does not have a medical Maximum Out of Pocket $6,000 annually The most you pay for Copayments,
Monthly Plan Premium YOU PAY $0 You must continue to pay your Medicare Part C Deductible YOU PAY nothing This plan does not have a medical Maximum Out of Pocket $6,000 annually The most you pay for Copayments,
Other Participating UPMC Facilities Level 2 Benefit Period
 Schedule of Benefits Advantage Panther Gold Plan - Enhanced Access HMO Applies to Oakland and Titusville campuses HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600 Primary
Schedule of Benefits Advantage Panther Gold Plan - Enhanced Access HMO Applies to Oakland and Titusville campuses HMO Deductible: $0 / $0 Coinsurance: 0% Total Annual Out-of-Pocket: $1,800 / $3,600 Primary
Important Questions Answers Why this Matters:
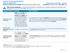 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-843-6447. Important Questions
Special Care SM. Helping lower-income individuals and families afford health care benefits. A Guaranteed Issue Health Insurance Plan for Individuals
 Special Care SM A Guaranteed Issue Health Insurance Plan for Individuals Helping lower-income individuals and families afford health care benefits Basic hospitalization issued by Capital BlueCross; medical
Special Care SM A Guaranteed Issue Health Insurance Plan for Individuals Helping lower-income individuals and families afford health care benefits Basic hospitalization issued by Capital BlueCross; medical
This chart summaries the coverage under the Standard Health Savings Account (HSA) Option using the Open Access Plus (OAP) network.
 STANDARD HSA OPTION 2017 OPTIONS AT A GLANCE (DEDUCTIBLE 3000/6000) USING THE OPEN ACCESS PLUS (OAP) NETWORK This chart summaries the coverage under the Standard Health Savings Account (HSA) Option using
STANDARD HSA OPTION 2017 OPTIONS AT A GLANCE (DEDUCTIBLE 3000/6000) USING THE OPEN ACCESS PLUS (OAP) NETWORK This chart summaries the coverage under the Standard Health Savings Account (HSA) Option using
$300 Individual; $ 800 Family. Applies to out-of-network services only. What is the overall deductible?
 What is the overall deductible? This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.indecscorp.com or by
What is the overall deductible? This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.indecscorp.com or by
South Central Ohio Insurance Consortium
 South Central Ohio Insurance Consortium Health Plan Amendment No.: 31 Summary Plan Description: South Central Ohio Insurance Consortium Health Plan for Employees of Logan-Hocking Local Schools Certified/Classified
South Central Ohio Insurance Consortium Health Plan Amendment No.: 31 Summary Plan Description: South Central Ohio Insurance Consortium Health Plan for Employees of Logan-Hocking Local Schools Certified/Classified
$1,000/Individual, $2,000/Family per benefit period. What is the overall deductible?
 The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about
Summary of Benefits. Albemarle Select KeyCare PPO
 Summary of Benefits Albemarle Select KeyCare PPO Effective October 1, 2018-December 31, 2019 Anthem KeyCare 25 PPO - Albemarle Select plan 10/01/18-12/31/19 In-Network Services Preventive Care Services
Summary of Benefits Albemarle Select KeyCare PPO Effective October 1, 2018-December 31, 2019 Anthem KeyCare 25 PPO - Albemarle Select plan 10/01/18-12/31/19 In-Network Services Preventive Care Services
HealthTrust: Access Blue 20-RX10/20/45 Coverage Period: 07/01/ /30/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-870-3122. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-870-3122. Important Questions
What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/cuhealthplan or by calling 1-800-735-6072.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/cuhealthplan or by calling 1-800-735-6072.
CoventryOne Fusion 100%/50% POS Plans
 CoventryOne Fusion 100%/50% POS Plans $3,000 $5,000 In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member) $6,000,000 $6,000,000 Deductible (per benefit year) - Maximum 3 per family
CoventryOne Fusion 100%/50% POS Plans $3,000 $5,000 In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member) $6,000,000 $6,000,000 Deductible (per benefit year) - Maximum 3 per family
Marsh and McLennan: Anthem Blue Cross and Blue Shield $400 Deductible Plan Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://eoc.anthem.com/eocdps/aso or by calling (855) 570-1150.
Employee Benefit Plan: Missoula County Public Schools Coverage Period: 01/01/ /31/2014 Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by calling 1-585-343-0055 ext. 6415. Important Questions Answers
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document by calling 1-585-343-0055 ext. 6415. Important Questions Answers
