AHLA. V. Complex Contracting in the 21st Century between Payers and Providers
|
|
|
- Madlyn Martin
- 5 years ago
- Views:
Transcription
1 AHLA V. Complex Contracting in the 21st Century between Payers and Providers Lisa A. Hathaway Vice President and Chief Medicare Counsel Aetna Bethesda, MD Alan E. Schabes Benesch Friedlander Coplan & Aronoff LLP Cleveland, OH Annual Meeting June 26-28, 2017
2 American Health Lawyers Association 2017 Annual Meeting Lisa Hathaway, Esq. Alan E. Schabes, Esq. Agenda General Overview Types of Alternative Payment Models Fraud and Abuse Issues Bundling Waivers under Anti Kickback Statute and Stark Medicare Loss Ratio Issues Contracting Issues and Requirements 2 1
3 Generally The Centers for Medicare and Medicaid Innovation ( CMMI ) was established by 3021 of the Affordable Care Act ( ACA ). As set forth in 3021 of the Affordable Care Act, the purpose of the [CMMI] is to test innovative payment and service delivery models to reduce program expenditures... while preserving or enhancing the quality of care furnished to individuals under such titles. CMMI has identified many opportunities for its Alternative Payment Models, including: (a) promoting broad based reform in primary care via patient centered medical homes and other innovating care models; (b) supporting healthcare IT infrastructure; (c) varied payments for imaging based on best practices; and (d) giving States authority to test and evaluate payment reform. 3 Generally Models include: 1) Accountable Care Organizations ( ACO ); 2) Bundled Payments for Care (generally, BPCI ); 3) Comprehensive Care for Joint Replacement ( CJR ); 4) Other Models: Acute Myocardial Infarction ( AMI ); Coronary Artery Bypass Graft ( CABG ); and Surgical Hip and Femur Fracture Treatment ( SHFFT ). 4 2
4 (1) ACOs Generally The ACO and similar models are designed to incentivize health care providers to become accountable for a patient population by investing in infrastructure and processes that promote coordinated, quality, and efficient care. Hospitals, payors, and clinicians that participate in an ACO are financially accountable for the quality and cost of care for Medicare beneficiaries who are enrolled in traditional fee for service programs. To the extent participants are successful, they will share in the Medicare savings they promote. On the other hand, ACOs will be held financially responsible in the event costs exceed benchmark levels. There are several different ACO models. 5 ACO: Models Pioneer Model designed for organizations and providers that had experience in coordinated care across settings; this model concluded on December 31, 2016; A majority of the 8 participants sharing in savings as of the 2015 Performance Year End report. Under the Pioneer model, provider groups were able to move from a shared savings payment model to a population based payment model outside of the Medicare Shared Savings Program. Designed to work in coordination with private payors. 6 3
5 ACO: Models Next Generation Model Also designed for providers experienced in coordinating care for populations of patients. This model allowed participants to assume higher levels of financial risk than as compared to the Pioneer and Medicare Shared Savings Program models there are currently 44 participants 7 ACO: Models Investment Model In contrast to the Pioneer model, the Investment Model is designed for ACOs that are participating in the Medicare Shared Savings Program. Participants receive a combination of an upfront fixed payment; and upfront variable payment based on the number of assigned beneficiaries, and a monthly variable payment based on the ACOs size. There are currently almost 500,000 Medicare beneficiaries covered by this model as of January
6 (2) BPCI: Generally The Bundled Payments for Care Improvement ( BPCI ) initiative consists of four broadly defined models linking payments for beneficiaries receiving multiple different services during an episode of care. Under these initiatives, Medicare makes a single payment which is subsequently divided amongst the various caregivers. 9 BPCI: Models Model 1 Model 1 defined the episode of care as the inpatient stay in the acute care hospital; Medicare paid the hospital, retrospectively, a discounted amount based on the Inpatient Prospective Payment System and physicians under the Medicare Fee Schedule; Concluded December 31, 2016; 10 5
7 BPCI: Models Model 2 Medicare makes a retrospective bundled payment where actual expenses are reconciled against a target price for an episode of care. During the episode inpatient stay in the acute care hospital, post acute care, and related services ending either 30, 60, or 90 days after discharge providers receive FFS payments. Model 2 participants may select up to 48 clinical episodes. After reconciliation as against the target price, a payment or recoupment amount is made as compared to the established target price. Medicare payments for hospitalization and 90 days post discharge declined $864 more for orthopedic surgery episodes at BPCI participating hospitals than at non participating hospitals because of reduced use of institutional post acute care following hospitalization. Model 2 is ongoing and currently has 335 acute care hospitals and 204 physician group practice participants. 11 BPCI: Models Model 3 Medicare continues to make FFS payments to providers and subsequently reconciles charges against a set target. Here, the episode of care is triggered by the inpatient stay and begins at initiation of the post acute care services with a SNF, IRF, LTC, or HHA. As under Model 2, participants in Model 3 can select from 48 clinical conditions to test in this model. Naturally, SNFs and then HHAs were the most frequent participants in Model 3. Here, SNF payments and SNF days after a triggering episode of care declined relative to comparison groups in support of the Model s goal. 12 6
8 BPCI: Models Model 4 Medicare makes a single payment to a hospital that encompasses all services furnished by the hospital, physicians, and other caregivers for the defined episode of care. Again, participants may select up to 48 clinical conditions to test in this model. Physicians and other clinicians submit no pay claims to Medicare for tracking and evaluation purposes, but are otherwise paid out of the single lump sum payment made to the hospital. Under this model, it is important to note, that all readmissions for 30 days after discharge are included in the payment amount. There are currently 5 participating hospitals in this model. 13 (3) Comprehensive Joint Replacement (CJR) The Comprehensive Care for Joint Replacement ( CJR ) model s goal: to support better and more efficient care for patients undergoing hip and knee replacement. Under CJR, the episode of care begins with the admission of a patient to a participating hospital who is ultimately discharged under DRG 469 or 470, major joint replacement or reattachment of lower extremity, with or without major complications or comorbidities, respectively. Similar to BPCI Models 2 and 3, participants are paid under traditional Medicare FFS. Medicare sets a target price based on historical spending, adjusted based on risk stratification. At the end of each participant year, the total payments to each participant hospital will be compared to the target price. Depending on quality and spending performance, the hospital will either receive an additional payment ( gainshare ), or be required to repay Medicare ( alignment ) for a portion of the episode spending. 14 7
9 CJR (cont.) Federal rules set forth the terms under which a CJR participant hospital may distribute either a gainsharing payment or receive an alignment payment from the other actors involved in delivering care (each a CJR Collaborator ). Hospitals may not make or receive payments except in accordance with a sharing arrangement with CJR Collaborators as formalized and documented in a signed collaborator agreement. CMS may review any sharing arrangement for compliance. Hospitals are required to include update their own compliance programs to include oversight over their CJR collaborators at the board or governing body level. 15 CJR (cont.) The specific terms of the collaborator agreement are highly regulated: The arrangement must comply with all applicable fraud and abuse laws. Additionally, a CJR Collaborator s participation must be voluntary and without penalty; No party may condition the opportunity to make or receive gainsharing payments or alignment payments conditional on the volume or value of referrals between the hospital and CJR Collaborator; No hospital can make a gainsharing payment to a CJR Collaborator that is subject to any action for non compliance with fraud and abuse laws, underscoring the importance of effective compliance programs. In addition to fraud and abuse considerations, arrangements must not incentivize a reduction in providing medically necessary services; Payments to a CJR Collaborator must be at least in part based on achieving certain quality benchmarks. 16 8
10 CJR (cont.) In addition to setting forth the goals of the sharing arrangement, CMS sets forth the specific components that are required to be in each agreement with CJR Collaborators. The agreement must contain a description of the relationship, including the parties, date, purpose, financial terms, safeguards, etc.; The agreement must require the CJR Collaborator to act in compliance with CJR regulations; The agreement must require the collaborator to have a valid TIN or NPI during the term; The CJR Collaborator must have a compliance program; The must be a specific methodology for determining the cost savings to Medicare; The agreement must state the quality criteria used to determine the gainsharing payment. The hospital must have the right to recoup payments in the event an overpayment is assessed. 17 CJR Contracting Requirements The Collaborator Agreement must comply with the following: Describe the sharing arrangement between the hospital and the CJR collaborator, specifically: The parties; date; purpose and scope; financial or economic terms, including frequency of payment, method of accounting, and amounts; safeguards to ensure alignment payments made solely for purposes related to sharing responsibility for funds needed to repay Medicare; plans for redesign; care coordination; success measures; management and staff information. 18 9
11 CJR Contracting Requirements Cont d. The Agreement must contain a requirement that the Collaborator and its employees/contractors must comply with CJR Rules: Medicare enrollment requirements; Compliance program; Internal cost saving verification mechanisms; Criteria for gainsharing; Ability to recoup overpayments. 19 (4) Other Models On December 20, 2016, CMS published a final rule regarding several Episode Payment Models: AMI; CABG; SHFFT; and changes to CJR (collectively EPM Models ). Unlike the previously discussed ACO and BPCI Models, participation in the EPM Models is mandatory, putting hospitals at financial risk. Delays: Mandatory bundled payments under the EPM Models were set to begin July 1, However, by Interim Rule, published March 21, 2017, CMS delayed the start for until October 1, 2017, and sought comments with respect to further delaying the implementation of the AMI as discussed in this Section (and certain changes to the CJR program) until January 1, 2018, in order to align payment periods with the calendar year. The delay does not impact existing BPCI and CJR models only changes to the CJR model. By Final Rule, published May 20, 2017, CMS confirmed its intent to delay implementing changes to the CJR, and implementing the mandatory AMI, CABG, and SHFFT models until January 1,
12 Other Models Acute Myocardial Infarction On January 1, 2018, acute care hospitals in 98 selected geographic areas will participate in retrospective bundled payments for items and services that are related to Acute Myocardial Infarction Model ( AMI ) treatment and recovery beginning with hospitalization and continuing for 90 days after discharge. This model holds the hospital financially accountable for the quality and cost of an episode of care. An AMI episode begins on the admission of an eligible Medicare fee forservice beneficiary that results in a discharge paid under DRGs and Other Models Coronary Artery Bypass Graft Model CMS will begin making mandatory bundled payments under the Coronary Artery Bypass Graft Model ( CABG ). Under this model CMS will begin making bundled payments to acute care hospitals in 98 selected geographic areas for CABG treatment as defined by DRGs , to also include recovery and care for 90 days following discharge
13 Other Models Surgical Hip and Femur Fracture Treatment CMS will begin making mandatory bundled payments to acute care hospitals for Surgical Hip and Femur Fracture Treatment ( SHFFT ) as defined by DRGs Unlike AMI and CABG, this program is limited to 67 discreet geographic areas. 23 Fraud and Abuse Implications Federal Anti Kickback Statute ( AKS ) Physician Self Referral Law ( Stark Law ) Beneficiary Inducement of Civil Monetary Penalties ( CMP ) Gainsharing Civil Monetary Penalty Law 24 12
14 Gainsharing Civil Monetary Penalty Law Purpose: To address the risk of a physician holding back on necessary care or discharging patients early in the interest of reducing costs and services in gainsharing arrangements. Prohibits A hospital or critical access hospital knowingly makes a payment, directly or indirectly, to a physician as an inducement to reduce or limit services with respect to individuals who: (1) are entitled to benefits under part A or part B Medicare or to medical assistance under a State plan; and (2) are under the direct care of the physician, the hospital or critical access hospital shall be subject to a CMP of not more than $2,000 for each such individual with respect to whom the payment is made. 25 Gainsharing Civil Monetary Penalty Law (cont.) Any physician who accepts receipt of a payment described above is also subject to the CMP for each individual with respect to whom the payment is made. Physicians who certify that patients meet the requirements of 42 USC 1395(f)(a)(2)(C) or 1395n(a)(2)(A) knowing that the requirements are not met is subject to a CMP of the greater of $5,000 or three times the amount of payments for services made pursuant to such certification
15 AKS and Stark Law Bundling Waivers The Secretary may waive certain fraud and abuse requirements as necessary to carry out the provisions of the Medicare Shared Savings Program. On October 29, 2015, the OIG and CMS jointly published a Final Rule with regard to final waivers in connection with the Shared Saving Program. This Final Rule sets forth 5 waivers that provide flexibility for ACOs to pursue a wide array of activities, including those in the Shared Savings Program. 27 AKS and Stark Law Bundling Waivers (cont.) ACO Pre Participation Waiver. The OIG waives the Stark Law and AKS for ACO related start up arrangements in anticipation of participating in the Shared Savings Program. ACO Participation Waiver. Under this waiver the OIG waives the Stark Law and AKS application during the term of the ACO s participating agreement under the Shared Savings Program and for a certain duration after the participating agreement ends. Shared Savings Distributions Waiver. Again, the Stark and AKS are waived with respect to distributions and uses of payments earned through the Shared Savings Program. ACO Waiver. The OIG will not enforce the AKS for ACO arrangements that implicate the Stark Law. Patient Incentive Waiver. OIG will waive beneficiary inducement provisions of the CMP and the AKS for medically related incentives offered by ACOs, ACO participants, or ACO providers and suppliers under the Shared Savings Program for encouraging preventative care and compliance with treatment regimens
16 BPCI Model 1 Waiver On September 13, 2012, the OIG and CMS jointly issued waivers for specified arrangements involving BPCI Model 1 Participants. Protects hospitals and physicians from Stark Law and AKS exposure from sharing gains, or Incentive Payments, made under Model 1. The waiver does not protect distribution of funds from any other source or funds generated by means other than the approved gainsharing methodology outlined in the Gainsharing Arrangement, or financial arrangements other than Incentive Payments. The waiver does not protect payments made to reduce or limit medically necessary services. 29 BPCI Model 1 (cont.) Protects Incentive Payments received by an enrolled practitioner, including those made directly or indirectly to the enrolled practitioner by a BPCI Awardee, and incentive payments received by a BPCI entity and passed through to an enrolled practitioner. Incentive Payments received and retained by a BPCI entity for the BPCI entity s administrative services directly related to administration of the gainsharing arrangement are protected. The waiver applies to incentive payments derived from internal hospital cost savings generated by the BPCI Awardee s approved gainsharing arrangement during the performance years
17 BPCI Models, 2, 3, and 4 On July 26, 2013, the OIG and CMS jointly issued waivers for specific programs involving BPCI Models 2, 3, and 4. Models 2 and 3 include payments for both inpatient stays in an acute care hospital and post acute care and related services, the waivers protect a post acute provider s arrangement with a Model Awardee Hospital. Waivers under these models protect those covered from Stark Law, AKS, and CMP exposure. Waivers include the Savings Pool Contribution Waiver for internal cost savings contributed by Episode Integrated Providers ( EIPs ) to the BPCI Savings Pool. Such cost savings contributed to the Savings Pool must be realized by the EIP and result from care redesign undertaken by the EIP with providing services and items to beneficiaries within specific episodes of care. The contribution must consist only of internal cost savings. The EIP (contributor) must not knowingly make the contribution to induce the reduction of medically necessary items or services to patients. 31 BPCI Models, 2, 3, and 4 (cont.) Under the Incentive Payments Waiver, certain distributions from the BPCI Savings Pool made pursuant to the BPCI Agreement are afforded protection. Incentive Payment means: (a) a payment made directly or indirectly from the BPCI Savings Pool to an Awardee or EIP Pursuant to a Gainsharing Arrangement set forth in a Participant Agreement, (b) a payment of a portion of a BPCI Savings from an EIP to a Gainsharer, pursuant to a written gainsharing agreement, or (c) a payment made directly or indirect from the BPCI Savings Pool to a BPCI entity for administrative services pursuant to a gainsharing arrangement. BPCI entities in receipt of Incentive Payments must pass the entire amount through to an EIP or other BPCI entity, less amounts appropriately retained for administrative services. Again, the party making the Incentive Payment must not knowingly induce the recipient to reduce or limit Medically Necessary Services
18 BPCI Models, 2, 3, and 4 (cont.) As set forth in the Patient Engagement Incentive Waiver, participants are afforded protection with respect to items or services provided by a Model Awardee, EIP, or Gainsharer to a Model Beneficiary for free or below market value. The below market items or services must have a reasonable connection to the medical care provided. Specifically, the items and services must be in kind and be preventative care items that advance one of the following clinical goals: (1) adherence to a drug regime; (2) adherence to a follow up care plan; or (3) management of a chronic disease or condition. 33 BPCI Models, 2, 3, and 4 (cont.) In Model 4, AKS enforcement is waived under the Professional Services Fee waiver. Compensation paid by an Episode initiator/hospital to a physician or nonphysician that has not opted out that may otherwise implicate the AKS for Part B covered services furnished to a Model 4 Beneficiary during an Episode of Care is protected. Requirements include the compensation arrangement be fully compliant with a Stark Law exception set forth at 42 CFR (c), (d), or (l): employment; personal services; or fair market value, respectively. Additionally, payments must not knowingly be made to limit medically necessary items or services
19 Waivers for CJR On November 16, 2015, the OIG and CMS jointly issued waivers for specified arrangements involving CJR Model participants. The OIG will waive enforcement of the AKS and Stark Law in connection with gainsharing payments (surplus) and alignment payments (deficit) arrangements. Such payments must satisfy the requirements set forth in 42 CFR and 42 CFR Medical Loss Ratio Commercial plans (small, individual, large group) must achieve ratio of 80 or 85% MA Plans 85% Directs percentage of payments for members services and quality care activities Decrease amounts spent on administration profits Affects plan arrangements with vendors and providers Commercial remit payment to employers or policy holders MA Remit payment to CMS Penalties for MA ban on new enrollment (3 years not meeting) or lose CMS contract (5 years not meeting) Other risks false claims, CMPs, reputation Data retention 11 years, 10 years after year filed 36 18
20 Basic Calculation Numerator Incurred claims plus any expenses to improve health care quality (and other limited adjustments (additional items for Medicare Advantage such as amount reduction in Part B premium) Denominator Earned premiums less federal and state taxes and licensing or regulatory fees Incurred claim what the plan pays to providers for covered services i.e. what is in the EOC or in the benefits agreement (insurance policy) Exclusions from incurred claims non claims costs such as network development, claims processing, administration fees, medical record copying costs, etc. (see later for more) Medical Claim Paid + Quality Improvement Expense + Fraud & Abuse (+ Supplemental Benefits for MA) (ex. 85) Customer Premium Taxes & Assessments Paid Licenses & Fees Paid (ex. 100) = 85% * this is for MA MLR 37 Definition of Quality Improvement Expense 45 CFR or 42 CFR (a) and (a) Activity must meet the ALL FOUR of the following requirements: i) improve health quality; ii) increase likelihood of desired outcome in ways that can be objectively measured and provide verifiable results; iii) be directed at individual enrollees or segments of enrollees or provide health improvements to population as long as no costs are incurred by enrollees; and iv) be grounded in evidence based medicine, widely accepted clinical practice, criteria used by professionals such as medical associations, accreditation bodies gov t agencies or other nationally recognized bodies
21 In addition, the QIE activities must be Primarily designed to: (Meet one or more of 4 Items in Bold) Activity must be primarily designed to produce likelihood of desired outcome. Examples: effective case mgmt., care coordination, chronic disease mgmt., care compliance initiatives such as PCMH, ID ethnic racial or cultural disparities for best clinical practice, non electronic quality reporting and documentation, accreditation fees directly related to quality of care activities Implement and promote wellness Ex. assessments, life style coaching to specific and measureable improvements, coaching program for chronic disease, actual awards, incentives, bonuses, HIT to support such activities Prevent hospital readmits through comprehensive discharge programarrangement and manage transitions Ex. Patient centered education and counseling, personalized post discharge reinforcement, HIT to support such QI activities Improve patient safety, reduce medical errors, lower infection and mortality rates Ex. best clinical practice to reduce harm, activities using evidenced based medicine ( EBM ), prospective UR to id adverse drug interactions 39 Exclusions from QIE Primarily designed to control or contain costs Activities paid for with grant money Retrospective and concurrent UR review Certain prospective UM Benefits administrative type activities Fraud prevention (can claim recoveries) Credentialing Marketing expenses Cost of provider contracting, executing contracting Prospective UR that does not meet the definition of QIE Claims adjudication Handling enrollee and provider appeals Record copying costs 40 20
22 More Complex Analysis FFS payments Capitation to a provider is generally all medical costs. Is payment going to a licensed hc provider or to a vendor? Vendors likely a portion of capitation payment is for administration (If a provider is generally all incurred claim, but if to non clinical entity, may not be.) Payments for medical cost reduction Is likely administrative Bonus payment based on cost saving measures (most likely not QIE) Ex. Payment to hospital to reduce length of stay or to reduce total claims costs vs. bonus payment to decrease admissions to less than 1200 a month. Bonus or shared savings payments impt to understand whom Dr. Group?, Hospital system?, ACO?, 3 rd party entity? Payment for achieving quality metrics or care coordination Bundled payments are they for covered services and to whom are the payments being made? 41 Clinical Risk Bearing Entity Must meet 4 Part Test 1) Entity contracts with an issuer to deliver, provide, or arrange for delivery & provision of clinical services to issuer s enrollees (and entity is not issuer) 2) Entity contractually bears financial & utilization risk for delivery, provision, or arrangement but entity is not issuer with respect to those services 3) Entity delivers, provides or arranges for the delivery and provision of clinical services through a system of integrated care delivery that provides for the coordinating of care, and sharing of clinical information, and which includes programs such as provider performance reviews, tracking clinical outcomes, communicating evidence based guidelines to entity s clinical providers, and others; and 42 21
23 Clinical Risk Bearing Entity 4) Functions other than clinical services that are included in the payment (capitation or fee for service) must be reasonably be related or incident to the clinical services, and must be performed on behalf of the entity or the entity s providers. Must meet ALL 4 Prongs Ex. Vendor meets No. 1 insurer s enrollees and No. 2 at risk for financial & utilization (not just financial), but not No. 3 & 4. Ex. Apply to third parties such as IPAs, PHOs, ACOs PBM will not meet this, generally. 43 Network Adequacy ACA Plan standards sufficient no. & type of providers, includes essential providers, includes mental health & substance abuse State standards on network adequacy vary and some are detailed NCQA availability practitioners, accessibility of services NAIC model network adequacy standards 44 22
24 CMS Network Adequacy Standards Must meet when an entity applies to be a MA or Part D plan or upon expansion 90% of MA enrollees residing in a county must have access to certain provider types Depends on county designation of large metro, metro, micro, rural, and certain extreme counties CMS has details in their HPMS system regarding the providers and facilities Does not include HH, DME or transplant providers It is a time and distance standard Ex. oncology, neurology, cardiology, psychiatry, rheumatology, urology, PCPs Limited and rare exceptions for not meeting the standards retirement, moving, provider or facility will not contract with any MAOs, exclusive contract with one MAO or prove a unique pattern of care Applicability to contracting Plans will reach out to contract Can effect ability to expand to a new county if a provider or facility refuses to contract Relationships Effects on members 45 Provider Directory Requirements ACA Plans on the Exchange ACA requirements for QHPs Machine readable No longer accepting patients List provider name, license, credentials, specialty, contact info, accommodations for limited English Update every 30 days for Exchange NAIC, States, & Medicaid NAIC in 2015 AMA has tried to propose standards State of CA SB 137 FL, GA, IL, MD, WA Pending laws NJ, NY, CT, RI Medicaid Plans have directory requirements 46 23
25 CMS Plan Directory Requirements Under CMS scrutiny and evaluation since 2016 AHIP study validated the difficulty of maintaining the directory and getting the information Need for accurate information for members CMS has issued several sets of memo guidance No misleading info, indicate if providers are only available to certain enrollees. Ex. Native American Indians, only available for home visits or practice concierge medicine Clearly note non physicians Required to maintain online and provide hard copy directory upon request Elements are listed in Chapter 4 MA Manual Quarterly outreach to providers to verify accuracy is required (was monthly) Plan contract requirements notice of any change within 30 days, or even penalties for not providing Educate providers on need for updated and accurate info. Reaching out by , phone call, fax, letter to verify accuracy 47 Contracting Considerations Credentialing Not excluded, suspended, disbarred & monthly checks of OIG & SAMs data bases Payment terms clear, prompt pay, interest Definitions still impt! Clear obligations of both parties for services What is a covered service? Medical necessity and coverage will vary by product What products does the contract cover?? Non Discrimination health status, mental, type of coverage, race, color Provide scope of services within provider s licensure and as they treat other non Plan patients 1557 requirements ex. translators, interpreters 48 24
26 Mandated Medicare and Medicaid Provisions Expectation CMS requires certain language when a MA Plan contracts with a first tier, downstream and related party Template flowdown provisions Use of other terms that are Plan legal requirements in addition Medicaid requirements ex. hold harmless, encounter data, detail the services, credentialing and provider ID info, cultural competency, confidentiality and maintenance of records, report Impt. Example Language Comply with all applicable CMS requirements Hold harmless language Keep records for 10+ years Right privacy and confidentiality Right HHS, CMS, Comptroller Gen & Plan to inspect, auditor, requires records, electronic info and computers Clearly set forth delegated duties (separate attachment or contract) 49 Terminations Important for network adequacy MA Plan & providers must give at least 60 days notice for non cause terminations Key relationships 180 to 1 year notice Plans will want a with cause loss of licensure or accreditation, significant fines, penalties, or member issues, or regulatory issues, and non compliance with laws, lack of insurance, insolvency/bankruptcy Providers will want a with cause for late payment that is not cured, Plan regulatory issues Right to cure or not? Short time frame, plan discretion to extend Transition obligations need to be part of termination 50 25
Final Rule Summary. Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, December 31, 2021
 Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
Final Rule Summary Medicare Advancing Care Coordination through Episode Payment Models Program Years: October 1, 2017- December 31, 2021 April 2017 1 TABLE OF CONTENTS Overview and Resources... 3 Model
FMV Considerations for Bundled Payment Arrangements
 FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
FMV Considerations for Bundled Payment Arrangements Matthew J. Milliron, MBA HealthCare Appraisers, Inc. Becker s CEO + CFO Roundtable November 8, 2016 Today s Roadmap Healthcare Transactions Refresh Bundled
Medicare Program; Advancing Care Coordination Through Episode Payment. Models (EPMs); Cardiac Rehabilitation Incentive Payment Model; and Changes to
 This document is scheduled to be published in the Federal Register on 05/19/2017 and available online at https://federalregister.gov/d/2017-10340, and on FDsys.gov CMS-5519-F3 DEPARTMENT OF HEALTH AND
This document is scheduled to be published in the Federal Register on 05/19/2017 and available online at https://federalregister.gov/d/2017-10340, and on FDsys.gov CMS-5519-F3 DEPARTMENT OF HEALTH AND
INFORMATION ABOUT YOUR OXFORD COVERAGE
 OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
OXFORD HEALTH PLANS (CT), INC. INFORMATION ABOUT YOUR OXFORD COVERAGE PART I. REIMBURSEMENT Overview of Provider Reimbursement Methodologies Generally, Oxford pays Network Providers on a fee-for-service
Housekeeping. Questions
 Housekeeping To join us on audio, dial the phone number in the teleconference box and follow the prompts. Please dial in with your Attendee ID number. The Attendee ID number will connect your name in WebEx
Housekeeping To join us on audio, dial the phone number in the teleconference box and follow the prompts. Please dial in with your Attendee ID number. The Attendee ID number will connect your name in WebEx
Impact of ACOs on Care Coordination
 Impact of ACOs on Care Coordination Presented by: Michelle L. Templin Vice President Legislative Affairs and Business Development MHA ACO Network March 2, 2017 Agenda Agenda Key Regulatory Drivers Accountable
Impact of ACOs on Care Coordination Presented by: Michelle L. Templin Vice President Legislative Affairs and Business Development MHA ACO Network March 2, 2017 Agenda Agenda Key Regulatory Drivers Accountable
A Practical Discussion of Value and Quality Based Payments What Do I Do Now?
 Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities
 BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities A Presentation for the ACC April 3, 2018 Christopher J. Donovan Partner Foley & Lardner LLP C. Frederick (Fred) Geilfuss
BPCI Advanced Understanding the Latest Episode Based Program and the Opportunities A Presentation for the ACC April 3, 2018 Christopher J. Donovan Partner Foley & Lardner LLP C. Frederick (Fred) Geilfuss
No change from proposed rule. healthcare providers and suppliers of services (e.g.,
 American College of Physicians Medicare Shared Savings/Accountable Care Organization (ACO) Final Rule Summary Analysis Category Final Rule Summary Change from Proposed Rule and Comments ACO refers to a
American College of Physicians Medicare Shared Savings/Accountable Care Organization (ACO) Final Rule Summary Analysis Category Final Rule Summary Change from Proposed Rule and Comments ACO refers to a
Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017
 To Dial-in: 877.668.4490 or 408.792.6300 Event Number: 669 367 723 Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017 CMS Final Rule and Materials Advancing Care Coordination through
To Dial-in: 877.668.4490 or 408.792.6300 Event Number: 669 367 723 Cardiac Bundle (AMI, CABG, and SHFFT), CR and ACO Track 1+ January 11, 2017 CMS Final Rule and Materials Advancing Care Coordination through
Disclaimer. The materials and views expressed in this presentation are the views of the presenters and not necessarily the views of Northwell Health
 Helpful Tips for Value Based Payment (VBP) Compliance Programs Greg Radinsky Vice President & Chief Corporate Compliance Officer Aaron Lund Director of Corporate Compliance & Privacy Officer Disclaimer
Helpful Tips for Value Based Payment (VBP) Compliance Programs Greg Radinsky Vice President & Chief Corporate Compliance Officer Aaron Lund Director of Corporate Compliance & Privacy Officer Disclaimer
Issue brief: Medicaid managed care final rule
 Issue brief: Medicaid managed care final rule Overview In the past decade, the Medicaid managed care landscape has changed considerably in terms of the number of beneficiaries enrolled in managed care
Issue brief: Medicaid managed care final rule Overview In the past decade, the Medicaid managed care landscape has changed considerably in terms of the number of beneficiaries enrolled in managed care
Top 10 Issues in APM Contract Negotiations
 Legal Issues in New Contracting and Risk Sharing Models - What To Know Before You Sign Alexis Finkelberg Bortniker Foley & Lardner LLP 617-226-3177 Abortniker@foley.com June 2, 2017 Top 10 Issues in APM
Legal Issues in New Contracting and Risk Sharing Models - What To Know Before You Sign Alexis Finkelberg Bortniker Foley & Lardner LLP 617-226-3177 Abortniker@foley.com June 2, 2017 Top 10 Issues in APM
Medical Loss Ratio. Institute for Health Plan Counsel May 8, Presenters:
 Medical Loss Ratio Institute for Health Plan Counsel May 8, 2013 Presenters: Melissa J. Hulke, CPA, ABV, CFF Navigant, Phoenix, AZ melissa.hulke@navigant.com Scott O. Jones, FSA, MAAA Milliman, Seattle,
Medical Loss Ratio Institute for Health Plan Counsel May 8, 2013 Presenters: Melissa J. Hulke, CPA, ABV, CFF Navigant, Phoenix, AZ melissa.hulke@navigant.com Scott O. Jones, FSA, MAAA Milliman, Seattle,
Awardee: Meridian Hospitals Corporation d/b/a Jersey Shore University Medical Center
 Bundled Payments for Care Improvement Model 4 Bundled Payments for Care Improvement Model 4 Awardee Agreement Awardee: Meridian Hospitals Corporation d/b/a Jersey Shore University Medical Center 4007-000
Bundled Payments for Care Improvement Model 4 Bundled Payments for Care Improvement Model 4 Awardee Agreement Awardee: Meridian Hospitals Corporation d/b/a Jersey Shore University Medical Center 4007-000
HEALTH POLICY & EDUCATION SERIES
 HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
HEALTH POLICY & PAYMENT EDUCATION SERIES Medicare s Bundled Payment Initiatives The information in this document is based off of policy information available as of August 2016. Updated information may
Opportunities for Orthopedic Specialists in BPCI Advanced
 Opportunities for Orthopedic Specialists in BPCI Advanced January 13 th, 2018 Introduction CMS announced the voluntary Bundled Payment for Care Improvement (BPCI) Advanced program on Tuesday, Jan 9 th
Opportunities for Orthopedic Specialists in BPCI Advanced January 13 th, 2018 Introduction CMS announced the voluntary Bundled Payment for Care Improvement (BPCI) Advanced program on Tuesday, Jan 9 th
Overview of Pay For Performance
 STARK AND ITS APPLICATION TO: PAY FOR PERFORMANCE Charles B. Oppenheim FOLEY & LARDNER LLP 2029 Century Park East, Suite 3500 Los Angeles, CA 90067-3021 coppenheim@foley.com 310.975.7790 HCCA 2007 Pacific
STARK AND ITS APPLICATION TO: PAY FOR PERFORMANCE Charles B. Oppenheim FOLEY & LARDNER LLP 2029 Century Park East, Suite 3500 Los Angeles, CA 90067-3021 coppenheim@foley.com 310.975.7790 HCCA 2007 Pacific
SUMMARY TABLE OF CONTENTS
 FINAL RULE: MEDICARE PROGRAM; ADVANCING CARE COORDINATION THROUGH EPISODE PAYMENT MODELS (EPMs); CARDIAC REHABILITATION INCENTIVE PAYMENT MODEL; AND CHANGES TO THE COMPREHENSIVE CARE FOR JOINT REPLACEMENT
FINAL RULE: MEDICARE PROGRAM; ADVANCING CARE COORDINATION THROUGH EPISODE PAYMENT MODELS (EPMs); CARDIAC REHABILITATION INCENTIVE PAYMENT MODEL; AND CHANGES TO THE COMPREHENSIVE CARE FOR JOINT REPLACEMENT
Healthcare Reform and Its Impact on the Care Delivery System
 Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Healthcare Reform and Its Impact on the Care Delivery System Agenda 1) The Era of Healthcare Reform 2) Healthcare Reform and Post-Acute Care 3) Succeeding in the Reform Era: Managing the Continuum of Health
Comprehensive Care for Joint Replacement Payment Model Final Rule Fact Sheet
 Comprehensive Care for Joint Replacement Payment Model Final Rule Fact Sheet 1 Description: This document provides an overview of the final rule to implement a new Comprehensive Care for Joint Replacement
Comprehensive Care for Joint Replacement Payment Model Final Rule Fact Sheet 1 Description: This document provides an overview of the final rule to implement a new Comprehensive Care for Joint Replacement
Medicare Program; Cancellation of Advancing Care Coordination through Episode. Payment and Cardiac Rehabilitation Incentive Payment Models; Changes to
 This document is scheduled to be published in the Federal Register on 12/01/2017 and available online at https://federalregister.gov/d/2017-25979, and on FDsys.gov DEPARTMENT OF HEALTH AND HUMAN SERVICES
This document is scheduled to be published in the Federal Register on 12/01/2017 and available online at https://federalregister.gov/d/2017-25979, and on FDsys.gov DEPARTMENT OF HEALTH AND HUMAN SERVICES
Required CMS Contract Clauses Revised 8/28/14 CMS MCM Guidance Chapter 21
 Required CMS Contract Clauses Revised 8/28/14 CMS MCM Guidance Chapter 21 The following provisions are required to be incorporated into all contracts with first tier, downstream, or related entities as
Required CMS Contract Clauses Revised 8/28/14 CMS MCM Guidance Chapter 21 The following provisions are required to be incorporated into all contracts with first tier, downstream, or related entities as
Proposed ACO Rule: A Giant Step Toward Reform or a Leap of Faith for Providers? April 27, 2011
 Proposed ACO Rule: A Giant Step Toward Reform or a Leap of Faith for Providers? April 27, 2011 Barbara Eyman Ropes & Gray Barbara.Eyman@ropesgray.com 202.508.4760 Ropes & Gray LLP Stephen Warnke Ropes
Proposed ACO Rule: A Giant Step Toward Reform or a Leap of Faith for Providers? April 27, 2011 Barbara Eyman Ropes & Gray Barbara.Eyman@ropesgray.com 202.508.4760 Ropes & Gray LLP Stephen Warnke Ropes
This Webcast Will Begin Shortly
 This Webcast Will Begin Shortly If you have any technical problems with the Webcast or the streaming audio, please contact us via email at: webcast@acc.com Thank You! 1 Accountable Care Organizations Under
This Webcast Will Begin Shortly If you have any technical problems with the Webcast or the streaming audio, please contact us via email at: webcast@acc.com Thank You! 1 Accountable Care Organizations Under
HHS Issues Final ACO Regulations
 Client Alert October 25, 2011 HHS Issues Final ACO Regulations On Oct. 20, 2011, the Department of Health and Human Services (HHS) and the Centers for Medicare and Medicaid Services (CMS) released the
Client Alert October 25, 2011 HHS Issues Final ACO Regulations On Oct. 20, 2011, the Department of Health and Human Services (HHS) and the Centers for Medicare and Medicaid Services (CMS) released the
Shared Savings Program ACOs and Payors: Opportunities and Challenges in a New Era of Accountable Care
 APRIL 2012 EXECUTIVE SUMMARY PAYORS, PLANS, AND MANAGED CARE PRACTICE GROUP Shared Savings Program ACOs and Payors: Opportunities and Challenges in a New Era of Accountable Care Amy J. Davis, Esquire Lumeris
APRIL 2012 EXECUTIVE SUMMARY PAYORS, PLANS, AND MANAGED CARE PRACTICE GROUP Shared Savings Program ACOs and Payors: Opportunities and Challenges in a New Era of Accountable Care Amy J. Davis, Esquire Lumeris
Advancing Risk Capability in 2015: Medicare Shared Savings Program and ACO Investment Model. March 23, 2015 // 12:00 P.M. 1:00 P.M.
 Advancing Risk Capability in 2015: Medicare Shared Savings Program and ACO Investment Model March 23, 2015 // 12:00 P.M. 1:00 P.M. EST CENTER FOR INDUSTRY TRANSFORMATION The DHG Healthcare Center for Industry
Advancing Risk Capability in 2015: Medicare Shared Savings Program and ACO Investment Model March 23, 2015 // 12:00 P.M. 1:00 P.M. EST CENTER FOR INDUSTRY TRANSFORMATION The DHG Healthcare Center for Industry
Executive Summary: Hospital episode initiators: Change in mandatory MSAs:
 On November 16, 2015, the Centers for Medicare and Medicare Services (CMS) released the final rule for the Comprehensive Care for Joint Replacement (CJR) model, which creates a mandatory lower extremity
On November 16, 2015, the Centers for Medicare and Medicare Services (CMS) released the final rule for the Comprehensive Care for Joint Replacement (CJR) model, which creates a mandatory lower extremity
Medicare Parts C & D General Compliance Training
 Medicare Parts C & D General Compliance Training Developed by the Centers for Medicare & Medicaid Services Issued: February, 2013 Part 2: Medicare Parts C & D Compliance Training Developed by the Centers
Medicare Parts C & D General Compliance Training Developed by the Centers for Medicare & Medicaid Services Issued: February, 2013 Part 2: Medicare Parts C & D Compliance Training Developed by the Centers
Hospital Incentive Payments to Physicians for Quality and Cost Savings
 Hospital Incentive Payments to Physicians for Quality and Cost Savings Implications under the Fraud and Abuse Laws March 1, 2011 Dennis S. Diaz Davis Wright Tremaine LLP dennisdiaz@dwt.com 213-633-6876
Hospital Incentive Payments to Physicians for Quality and Cost Savings Implications under the Fraud and Abuse Laws March 1, 2011 Dennis S. Diaz Davis Wright Tremaine LLP dennisdiaz@dwt.com 213-633-6876
Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]
![Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701] Coverage Expansion [Sections 310, 323, 324, 341, 342, 343, 344, and 1701]](/thumbs/87/96500790.jpg) Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
Summary of the U.S. House of Representatives Health Reform Bill October 2009 The following summarizes the major hospital and health system provisions included in the U.S. House of Representatives health
Subpart D MCO, PIHP and PAHP Standards Availability of services.
 Center for Medicare & Medicaid Services (CMS) Medicaid and CHIP Managed Care Final Rule (CMS 2390-F) Fact Sheet: Subpart D and E of 438 Quality of Care Each state must ensure that all services covered
Center for Medicare & Medicaid Services (CMS) Medicaid and CHIP Managed Care Final Rule (CMS 2390-F) Fact Sheet: Subpart D and E of 438 Quality of Care Each state must ensure that all services covered
Healthcare Finance Trends and Perspectives
 Healthcare Finance Trends and Perspectives AONE Annual Conference, Fort Worth, TX April 2 nd, 2016 Chuck Alsdurf, MAcc, CPA Director, Healthcare Finance Policy, Operational Initiatives Healthcare Financial
Healthcare Finance Trends and Perspectives AONE Annual Conference, Fort Worth, TX April 2 nd, 2016 Chuck Alsdurf, MAcc, CPA Director, Healthcare Finance Policy, Operational Initiatives Healthcare Financial
MEDICARE NEXT GENERATION ACO PREFERRED PROVIDER AGREEMENT
 MEDICARE NEXT GENERATION ACO PREFERRED PROVIDER AGREEMENT THIS AGREEMENT ( Agreement ) is entered into as of the day of, 2016 (the Effective Date ) by and between Trinity Health ACO, Inc., a Delaware nonprofit
MEDICARE NEXT GENERATION ACO PREFERRED PROVIDER AGREEMENT THIS AGREEMENT ( Agreement ) is entered into as of the day of, 2016 (the Effective Date ) by and between Trinity Health ACO, Inc., a Delaware nonprofit
Bundled Payments for Care Improvement Advanced
 Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Patient Care Models Group Bundled Payments for Care Improvement Advanced Request for Applications (RFA) Last Modified:
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Patient Care Models Group Bundled Payments for Care Improvement Advanced Request for Applications (RFA) Last Modified:
Medical Monitoring Program: PPACA and CMS Final Recommended Guidelines vs. Rules: New License Monthly Screening Requirements
 PPACA and CMS Final Recommended Guidelines vs. Rules: New License Monthly Screening Requirements The Patient Protection and Affordable Care Act of 2010, as amended by the Health Care and Education Reconciliation
PPACA and CMS Final Recommended Guidelines vs. Rules: New License Monthly Screening Requirements The Patient Protection and Affordable Care Act of 2010, as amended by the Health Care and Education Reconciliation
The Transition to Value-Based Health Care: Recommendations for Medical Device Manufacturers
 The Transition to Value-Based Health Care: Recommendations for Medical Device Manufacturers April 27, 2017 LLP Agenda Introduction Shift to Value-Based Care New Models of Medical Device Company Operation
The Transition to Value-Based Health Care: Recommendations for Medical Device Manufacturers April 27, 2017 LLP Agenda Introduction Shift to Value-Based Care New Models of Medical Device Company Operation
Network Adequacy Standards Constance L. Akridge July 21, 2016
 Network Adequacy Standards Constance L. Akridge July 21, 2016 Agenda Network Adequacy Developments Overview NAIC Network Adequacy Model Act 2 Network Adequacy Developments Overview --Growing concern over
Network Adequacy Standards Constance L. Akridge July 21, 2016 Agenda Network Adequacy Developments Overview NAIC Network Adequacy Model Act 2 Network Adequacy Developments Overview --Growing concern over
MANAGED CARE READINESS TOOLKIT
 MANAGED CARE READINESS TOOLKIT Please note: The following managed care definitions reflect a general understanding of the terms. It will be important to read managed care contracts very carefully as they
MANAGED CARE READINESS TOOLKIT Please note: The following managed care definitions reflect a general understanding of the terms. It will be important to read managed care contracts very carefully as they
CMS Cardiac (AMI & CABG), SHFFT and Cardiac Rehab. Demo - Overview. September 13, 2016
 CMS Cardiac (AMI & CABG), SHFFT and Cardiac Rehab. Demo - Overview September 13, 2016 Cardiac (AMI & CABG), SHFFT (Surgical Hip/Femur Fracture Treatment) & Cardiac Rehabilitation Demo Why expand Comprehensive
CMS Cardiac (AMI & CABG), SHFFT and Cardiac Rehab. Demo - Overview September 13, 2016 Cardiac (AMI & CABG), SHFFT (Surgical Hip/Femur Fracture Treatment) & Cardiac Rehabilitation Demo Why expand Comprehensive
ACO: Shared Savings Model
 ACO: Shared Savings Model Checklist of Key Questions Risk Upside only? Downside risk? How much? How will downside losses be paid for? Shared Savings How much of the savings will be shared (or retained
ACO: Shared Savings Model Checklist of Key Questions Risk Upside only? Downside risk? How much? How will downside losses be paid for? Shared Savings How much of the savings will be shared (or retained
July 23, Dear Mr. Slavitt:
 Andy Slavitt Acting Administrator Centers for Medicare & Medicaid Services Hubert H. Humphrey Building 200 Independence Avenue, S.W., Room 445-G Washington, DC 20201 RE: Proposed Rule: RIN 0938-AS25 Medicaid
Andy Slavitt Acting Administrator Centers for Medicare & Medicaid Services Hubert H. Humphrey Building 200 Independence Avenue, S.W., Room 445-G Washington, DC 20201 RE: Proposed Rule: RIN 0938-AS25 Medicaid
Approved Models to Align Incentives between Hospitals and their Physicians
 Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
Approved Models to Align Incentives between Hospitals and their Physicians Agenda I. Alignment Model Overview II. Co-Management III. Clinically Integrated Networks CIN Definition & Overview Network Development
GAINSHARING & PAY FOR PERFORMANCE -- P4P UPDATE ON RECENT DEVELOPMENTS AND INITIATIVES
 GAINSHARING & PAY FOR PERFORMANCE -- P4P UPDATE ON RECENT DEVELOPMENTS AND INITIATIVES presented by Robert D. Girard, Esq. Davis Wright Tremaine LLP A. Gain-Sharing B. Provider P4P programs C. Government
GAINSHARING & PAY FOR PERFORMANCE -- P4P UPDATE ON RECENT DEVELOPMENTS AND INITIATIVES presented by Robert D. Girard, Esq. Davis Wright Tremaine LLP A. Gain-Sharing B. Provider P4P programs C. Government
IDN Goals (cont d) Integrated Delivery Networks and What They Mean for Compliance. Integrated Delivery Network (IDN) Goals
 Integrated Delivery Networks and What They Mean for Compliance Chris Rossman, Esq. Foley & Lardner LLP Detroit, Michigan Attorney Advertising Prior results do not guarantee a similar outcome Models used
Integrated Delivery Networks and What They Mean for Compliance Chris Rossman, Esq. Foley & Lardner LLP Detroit, Michigan Attorney Advertising Prior results do not guarantee a similar outcome Models used
MAINE MEDICAL ASSOCIATION PAYMENT REFORM READINESS: A LEGAL TOOLKIT FOR PHYSICIANS
 MAINE MEDICAL ASSOCIATION PAYMENT REFORM READINESS: A LEGAL TOOLKIT FOR PHYSICIANS This publication has been prepared by the Maine Medical Association and the law firm of Kozak & Gayer, P.A., solely as
MAINE MEDICAL ASSOCIATION PAYMENT REFORM READINESS: A LEGAL TOOLKIT FOR PHYSICIANS This publication has been prepared by the Maine Medical Association and the law firm of Kozak & Gayer, P.A., solely as
Lifetime Limits Effective September 23, 2010, payors are prohibited from placing lifetime dollar limits on medical claims.
 A P R I L 2 0 1 0 Health Care Reform The Patient Protection and Affordable Care Act of 2010, as amended by the Health Care and Education Reconciliation Act of 2010 (collectively, the "Act") consists of
A P R I L 2 0 1 0 Health Care Reform The Patient Protection and Affordable Care Act of 2010, as amended by the Health Care and Education Reconciliation Act of 2010 (collectively, the "Act") consists of
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244
 Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244 Next Generation ACO Model Participation Agreement Last
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244 Next Generation ACO Model Participation Agreement Last
Subject HHS Commentary From Preamble Regulatory Provision Agent Specific Provisions Definition of Agent/Broker
 National Association of Health Underwriters Overview of Provisions in the Proposed Federal Rule on the Establishment of Exchanges and Qualified Health Plans (Released on July 11, 2011) of Specific Interest
National Association of Health Underwriters Overview of Provisions in the Proposed Federal Rule on the Establishment of Exchanges and Qualified Health Plans (Released on July 11, 2011) of Specific Interest
Evaluating the Fair Market Value of Pay for Performance
 April 2014 healthcare financial management FEATURE STORY Jen Johnson Alexandra Higgins Evaluating the Fair Market Value of Pay for Performance 1 AT A GLANCE When assessing a pay-for-performance arrangement,
April 2014 healthcare financial management FEATURE STORY Jen Johnson Alexandra Higgins Evaluating the Fair Market Value of Pay for Performance 1 AT A GLANCE When assessing a pay-for-performance arrangement,
Government Issues Eagerly Awaited Proposed ACO Regulations
 Client Advisory Health Care April 12, 2011 Government Issues Eagerly Awaited Proposed ACO Regulations At long last, the oft-delayed Proposed Rule for Accountable Care Organizations (the Proposed Rule)
Client Advisory Health Care April 12, 2011 Government Issues Eagerly Awaited Proposed ACO Regulations At long last, the oft-delayed Proposed Rule for Accountable Care Organizations (the Proposed Rule)
Compliance Program. Health First Health Plans Medicare Parts C & D Training
 Compliance Program Health First Health Plans Medicare Parts C & D Training Compliance Training Objectives Meeting regulatory requirements Defining an effective compliance program Communicating the obligation
Compliance Program Health First Health Plans Medicare Parts C & D Training Compliance Training Objectives Meeting regulatory requirements Defining an effective compliance program Communicating the obligation
evaluating the fair market value of pay for performance
 REPRINT April 2014 Jen Johnson Alexandra Higgins healthcare financial management association hfma.org evaluating the fair market value of pay for performance A critical test for determining whether a pay-for-performance
REPRINT April 2014 Jen Johnson Alexandra Higgins healthcare financial management association hfma.org evaluating the fair market value of pay for performance A critical test for determining whether a pay-for-performance
The Emergence of Value-Based Care: Present and Future Tense
 The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
The Emergence of Value-Based Care: Present and Future Tense Erik Johnson, Vice President for Value-Based Care May 2016 What Is Value-Based Care? While the concept of value-based care has existed for years,
21% Total Medicare Beneficiaries (2017): 58 million
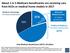 About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
About 1 in 5 Medicare beneficiaries are receiving care from ACOs or medical home models in 2017 Medicare Advantage: 19 million beneficiaries 33% 21% ACOs and Medical Homes 12 million beneficiaries Traditional
PARTICIPATING PROVIDER AGREEMENT
 PARTICIPATING PROVIDER AGREEMENT THIS PARTICIPATING PROVIDER AGREEMENT ( Agreement ) is made and entered into as of ( Effective Date ) by and between WellCare Health Insurance of Illinois, Inc. d/b/a WellCare
PARTICIPATING PROVIDER AGREEMENT THIS PARTICIPATING PROVIDER AGREEMENT ( Agreement ) is made and entered into as of ( Effective Date ) by and between WellCare Health Insurance of Illinois, Inc. d/b/a WellCare
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244
 Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244 Next Generation ACO Model Participation Agreement (First
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244 Next Generation ACO Model Participation Agreement (First
ACO Legal Issues Update
 ACO Legal Issues Update Third National Accountable Care Organization Congress October 30 November 1, 2012, Beverly Hilton Hotel, Los Angeles, CA Robert Homchick roberthomchick@dwt.com Robert L. Schuchard
ACO Legal Issues Update Third National Accountable Care Organization Congress October 30 November 1, 2012, Beverly Hilton Hotel, Los Angeles, CA Robert Homchick roberthomchick@dwt.com Robert L. Schuchard
RE: Patient Protection and Affordable Care Act; Establishment of Exchanges and Qualified Health Plans: Proposed Rule CMS-9989-P
 October 25, 2011 Dr. Donald Berwick Centers for Medicare & Medicaid Services Department of Health and Human Services P.O. Box 8010 Baltimore, MD 21244-8010 RE: Patient Protection and Affordable Care Act;
October 25, 2011 Dr. Donald Berwick Centers for Medicare & Medicaid Services Department of Health and Human Services P.O. Box 8010 Baltimore, MD 21244-8010 RE: Patient Protection and Affordable Care Act;
Stark Self-Disclosure. Thomas S. Crane 1/ Mintz Levin Cohn Ferris Glovsky and Popeo, PC
 Stark Self-Disclosure Thomas S. Crane 1/ Mintz Levin Cohn Ferris Glovsky and Popeo, PC A. Background 1. Stark Law The Physician Self-Referral Statute (or the Stark Law ) prohibits a physician from referring
Stark Self-Disclosure Thomas S. Crane 1/ Mintz Levin Cohn Ferris Glovsky and Popeo, PC A. Background 1. Stark Law The Physician Self-Referral Statute (or the Stark Law ) prohibits a physician from referring
Bundled Payments for Care Improvement: ADLS # 5 Contractual and Governance Issues Among Providers in Bundled Payments
 Bundled Payments for Care Improvement: ADLS # 5 Contractual and Governance Issues Among Providers in Bundled Payments Copyright 2012 American Institutes for Research All rights reserved. Weslie Kary, Moderator
Bundled Payments for Care Improvement: ADLS # 5 Contractual and Governance Issues Among Providers in Bundled Payments Copyright 2012 American Institutes for Research All rights reserved. Weslie Kary, Moderator
ACO Essentials Series
 ACO Essentials Series How to Use Health Endeavors Technology January, 2017 1/11/2017 1 Agenda Day 1&2 Interactive Analytic Tools Define ACO Goals- Success Plan Organizational Structure Executive TIN and
ACO Essentials Series How to Use Health Endeavors Technology January, 2017 1/11/2017 1 Agenda Day 1&2 Interactive Analytic Tools Define ACO Goals- Success Plan Organizational Structure Executive TIN and
Managed Care Contracting The Plan Perspective
 Managed Care Contracting The Plan Perspective Harold Iselin, Greenberg Traurig Whitney M. Phelps, Greenberg Traurig Andrew Cleek, PsyD, McSilver Institute Dan Ferris, MPA, McSilver Institute MCTAC.info@nyu.edu
Managed Care Contracting The Plan Perspective Harold Iselin, Greenberg Traurig Whitney M. Phelps, Greenberg Traurig Andrew Cleek, PsyD, McSilver Institute Dan Ferris, MPA, McSilver Institute MCTAC.info@nyu.edu
AMENDMENT 5 TO THE ADMINISTRATIVE SERVICES AGREEMENT WITH SAN JOAQUIN VALLEY INSURANCE AUTHORITY
 AMENDMENT 5 TO THE ADMINISTRATIVE SERVICES AGREEMENT WITH SAN JOAQUIN VALLEY INSURANCE AUTHORITY This is an Amendment to the Administrative Services Agreement as of January 1, 2015. This Amendment shall
AMENDMENT 5 TO THE ADMINISTRATIVE SERVICES AGREEMENT WITH SAN JOAQUIN VALLEY INSURANCE AUTHORITY This is an Amendment to the Administrative Services Agreement as of January 1, 2015. This Amendment shall
ALSTON&BIRD LLP. Summary of Agency Proposals Related to Accountable Care Organizations and the Medicare Shared Savings Program. I.
 ALSTON&BIRD LLP Summary of Agency Proposals Related to Accountable Care Organizations and the Medicare Shared Savings Program I. Executive Summary On March 31, 2011, the Centers for Medicare & Medicaid
ALSTON&BIRD LLP Summary of Agency Proposals Related to Accountable Care Organizations and the Medicare Shared Savings Program I. Executive Summary On March 31, 2011, the Centers for Medicare & Medicaid
Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries
 P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
P O L I C Y B R I E F kaiser commission on medicaid and the uninsured Explaining the State Integrated Care and Financial Alignment Demonstrations for Dual Eligible Beneficiaries October 2012 Over the last
CMS 1701 P UnityPoint Health. October 16, 2018
 CMS 1701 P UnityPoint Health 1776 West Lakes Parkway, Suite 400 West Des Moines, IA 50266 unitypoint.org October 16, 2018 Seema Verma, Administrator Centers for Medicare & Medicaid Services Department
CMS 1701 P UnityPoint Health 1776 West Lakes Parkway, Suite 400 West Des Moines, IA 50266 unitypoint.org October 16, 2018 Seema Verma, Administrator Centers for Medicare & Medicaid Services Department
FUNDAMENTALS OF MANAGED CARE AND RECENT TRENDS
 FUNDAMENTALS OF MANAGED CARE AND RECENT TRENDS Presented by the American Bar Association Health Law Section, Young Lawyers Division and Center for Professional Development American Bar Association Center
FUNDAMENTALS OF MANAGED CARE AND RECENT TRENDS Presented by the American Bar Association Health Law Section, Young Lawyers Division and Center for Professional Development American Bar Association Center
Stark and the Anti Kickback Statute. Regulating Referral Relationship. February 27-28, HCCA Board Audit Committee Compliance Conference.
 Stark and the Anti Kickback Statute Ryan Meade, JD, CHRC, CHC F Director, Regulatory Compliance Studies Beazley Institute for Health Law and Policy Loyola University Chicago School of Law rmeade@luc.edu
Stark and the Anti Kickback Statute Ryan Meade, JD, CHRC, CHC F Director, Regulatory Compliance Studies Beazley Institute for Health Law and Policy Loyola University Chicago School of Law rmeade@luc.edu
CHAPTER 20 - MANAGED CARE HEALTH BENEFIT PLANS SECTION MANAGED CARE DEFINITIONS
 CHAPTER 20 - MANAGED CARE HEALTH BENEFIT PLANS SECTION.0100 - MANAGED CARE DEFINITIONS 11 NCAC 20.0101 SCOPE AND DEFINITIONS (a) Scope. (1) Sections.0200,.0300, and.0400 of this Chapter apply to HMOs,
CHAPTER 20 - MANAGED CARE HEALTH BENEFIT PLANS SECTION.0100 - MANAGED CARE DEFINITIONS 11 NCAC 20.0101 SCOPE AND DEFINITIONS (a) Scope. (1) Sections.0200,.0300, and.0400 of this Chapter apply to HMOs,
Medicare Shared Savings Program: Accountable Care Organizations final rule
 Medicare Shared Savings Program: Accountable Care Organizations final rule Summary Table of Contents: Background.......1-2 Executive Summary......2-3 Medicare ACO Eligibility........3 Medicare ACO Structure
Medicare Shared Savings Program: Accountable Care Organizations final rule Summary Table of Contents: Background.......1-2 Executive Summary......2-3 Medicare ACO Eligibility........3 Medicare ACO Structure
AAOS MACRA Proposed Rule Summary (Short)
 AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
AAOS MACRA Proposed Rule Summary (Short) Merit-Based Incentive Payment System (MIPS), Advanced Alternative Payment Model (APM) Incentive, and Criteria for Physician-Focused Payment Models Ref: CMS-5517-P
Bundled Payment: Practicalities, Contractual and Governance Issues
 Bundled Payment: Practicalities, Contractual and Governance Issues Alice G. Gosfield Medicare Medicaid Institute American Health Lawyers Association March 22, 2013 c.2013, Alice G. Gosfield Overview Definitions,
Bundled Payment: Practicalities, Contractual and Governance Issues Alice G. Gosfield Medicare Medicaid Institute American Health Lawyers Association March 22, 2013 c.2013, Alice G. Gosfield Overview Definitions,
Compliance and Fraud, Waste, and Abuse Awareness Training. First Tier, Downstream, and Related Entities
 Compliance and Fraud, Waste, and Abuse Awareness Training First Tier, Downstream, and Related Entities 1 Course Outline Overview Purpose of training Effective Compliance program Definition of Fraud, Waste,
Compliance and Fraud, Waste, and Abuse Awareness Training First Tier, Downstream, and Related Entities 1 Course Outline Overview Purpose of training Effective Compliance program Definition of Fraud, Waste,
Ohio Hospital Association 2014 Annual Meeting. Compensating Employed Physicians In An Evolving Health Care Environment
 Ohio Hospital Association 2014 Annual Meeting June 10, 2014 Compensating Employed Physicians In An Evolving Health Care Environment Kimberly Mobley, Sullivan, Cotter and Associates, Inc., kimmobley@sullivancotter.com
Ohio Hospital Association 2014 Annual Meeting June 10, 2014 Compensating Employed Physicians In An Evolving Health Care Environment Kimberly Mobley, Sullivan, Cotter and Associates, Inc., kimmobley@sullivancotter.com
Summary of Medicare Provisions in the President s Budget for Fiscal Year 2016
 February 2015 Issue Brief Summary of Medicare Provisions in the President s Budget for Fiscal Year 2016 Gretchen Jacobson, Cristina Boccuti, Juliette Cubanski, Christina Swoope, and Tricia Neuman On February
February 2015 Issue Brief Summary of Medicare Provisions in the President s Budget for Fiscal Year 2016 Gretchen Jacobson, Cristina Boccuti, Juliette Cubanski, Christina Swoope, and Tricia Neuman On February
FIRST AMENDMENT TO THE FIRST AMENDED AND RESTATED RISK ACCEPTING ENTITY PARTICIPATION AGREEMENT
 FIRST AMENDMENT TO THE FIRST AMENDED AND RESTATED RISK ACCEPTING ENTITY PARTICIPATION AGREEMENT This First Amendment (this Amendment ) to the First Amended and Restated Risk Accepting Entity Participation
FIRST AMENDMENT TO THE FIRST AMENDED AND RESTATED RISK ACCEPTING ENTITY PARTICIPATION AGREEMENT This First Amendment (this Amendment ) to the First Amended and Restated Risk Accepting Entity Participation
CY 2014 Physician Quality Reporting System (PQRS)
 CY 2014 Physician Quality Reporting System (PQRS) 101 Table of Contents Step 1: Understand PQRS and how it impacts you A. When was PQRS first established and implemented? B. What is PQRS? C. How does CMS
CY 2014 Physician Quality Reporting System (PQRS) 101 Table of Contents Step 1: Understand PQRS and how it impacts you A. When was PQRS first established and implemented? B. What is PQRS? C. How does CMS
Goals of the Presentation. ACO Compliance Planning: Navigating 1/22/2016. Disclaimer
 ACO Compliance Planning: Navigating the Briar Patch HCCA Managed Care Compliance Conference February 1, 2016 Erin Roberts, Partner, Smith Moore Leatherwood LLP Barry Herrin, Partner, Smith Moore Leatherwood
ACO Compliance Planning: Navigating the Briar Patch HCCA Managed Care Compliance Conference February 1, 2016 Erin Roberts, Partner, Smith Moore Leatherwood LLP Barry Herrin, Partner, Smith Moore Leatherwood
kaiser medicaid and the uninsured commission on
 kaiser commission on medicaid and the uninsured State Demonstrations to Integrate Care and Align Financing for Dual Eligible Beneficiaries: A Review of the 26 Proposals Submitted to CMS October 2012 1330
kaiser commission on medicaid and the uninsured State Demonstrations to Integrate Care and Align Financing for Dual Eligible Beneficiaries: A Review of the 26 Proposals Submitted to CMS October 2012 1330
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244
 Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244 Next Generation ACO Model Participation Agreement (First
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Seamless Care Models Group 7205 Windsor Blvd Baltimore, MD 21244 Next Generation ACO Model Participation Agreement (First
ANCILLARY services: How to Stay Out of Trouble. The neurosurgical minefield Informed consent
 ANCILLARY services: How to Stay Out of Trouble Richard N.W. Wohns, M.D. JD, MBA NeoSpine, Puget Sound Region, Washington The neurosurgical minefield 2013 Informed consent HIPAA ARRA and HITECH Anti-Kickback
ANCILLARY services: How to Stay Out of Trouble Richard N.W. Wohns, M.D. JD, MBA NeoSpine, Puget Sound Region, Washington The neurosurgical minefield 2013 Informed consent HIPAA ARRA and HITECH Anti-Kickback
2016 Medicaid Managed Care Final Rule 1 Summary
 2016 Medicaid Managed Care Final Rule 1 Summary The final Medicaid Managed Care rule retains nearly all of the requirements of the proposed rule and does not make substantial changes to it. In particular,
2016 Medicaid Managed Care Final Rule 1 Summary The final Medicaid Managed Care rule retains nearly all of the requirements of the proposed rule and does not make substantial changes to it. In particular,
Medicare Program; Medicare Shared Savings Program: Accountable Care Organizations Proposed Rule
 701 Pennsylvania Ave., NW, Suite 800 Washington, DC 20004-2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org February 6, 2015 Marilyn Tavenner, Administrator Centers for Medicare & Medicaid Services
701 Pennsylvania Ave., NW, Suite 800 Washington, DC 20004-2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org February 6, 2015 Marilyn Tavenner, Administrator Centers for Medicare & Medicaid Services
Transparency, Reporting & Data Mining
 Transparency, Reporting & Data Mining Kimberly Brandt, CHC, JD Alston & Bird, LLP Shawn DeGroot, CHC-F, CCEP, CHRC Vice President of Corporate Responsibility Regional Health Size and Scope of Data 2 1
Transparency, Reporting & Data Mining Kimberly Brandt, CHC, JD Alston & Bird, LLP Shawn DeGroot, CHC-F, CCEP, CHRC Vice President of Corporate Responsibility Regional Health Size and Scope of Data 2 1
Bundled Payment: Practicalities, Contractual and Governance Issues
 Bundled Payment: Practicalities, Contractual and Governance Issues Alice G. Gosfield Physicians and Physician Organizations Law Institute Hospitals and Health Systems Law Institute February 12, 2013 c.2013,
Bundled Payment: Practicalities, Contractual and Governance Issues Alice G. Gosfield Physicians and Physician Organizations Law Institute Hospitals and Health Systems Law Institute February 12, 2013 c.2013,
FAQS ABOUT AFFORDABLE CARE ACT IMPLEMENTATION (PART XV) April 29, 2013
 FAQS ABOUT AFFORDABLE CARE ACT IMPLEMENTATION (PART XV) April 29, 2013 Set out below are additional Frequently Asked Questions (FAQs) regarding implementation of various provisions of the Affordable Care
FAQS ABOUT AFFORDABLE CARE ACT IMPLEMENTATION (PART XV) April 29, 2013 Set out below are additional Frequently Asked Questions (FAQs) regarding implementation of various provisions of the Affordable Care
Request for Applications
 Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Next Generation ACO Model Request for Applications Table of Contents I. Background and Introduction... 1 II. Statutory
Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Next Generation ACO Model Request for Applications Table of Contents I. Background and Introduction... 1 II. Statutory
The ACO Effort: A Status Report
 1 The ACO Effort: A Status Report J. Mark Waxman mwaxman@foley.com 617-342-4055 2 Whats the fuss about? A need for accountability for cost and quality A belief that the system can improve if: Provider
1 The ACO Effort: A Status Report J. Mark Waxman mwaxman@foley.com 617-342-4055 2 Whats the fuss about? A need for accountability for cost and quality A belief that the system can improve if: Provider
CMS Final Rule: Medicaid Managed Care The Medicaid Mega-Reg
 CMS Final Rule: Medicaid Managed Care The Medicaid Mega-Reg FaegreBD Consulting For Delta Dental Plans Association and National Association of Dental Plans October 2016 1 st Major Medicaid Managed Care
CMS Final Rule: Medicaid Managed Care The Medicaid Mega-Reg FaegreBD Consulting For Delta Dental Plans Association and National Association of Dental Plans October 2016 1 st Major Medicaid Managed Care
Re: Patient Protection and Affordable Care Act; Establishment of Exchanges and Qualified Health Plans. File Code CMS 9989 P
 October 24, 2011 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-9989-P P.O. Box 8010 Baltimore, MD 21244-8010 Re: Patient Protection and Affordable Care
October 24, 2011 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-9989-P P.O. Box 8010 Baltimore, MD 21244-8010 Re: Patient Protection and Affordable Care
Overview of October 24, 2013 Final Rule on Program Integrity: Exchange, Premium Stabilization Programs, and Market Standards
 Overview of October 24, 2013 Final Rule on Program Integrity: Exchange, Premium Stabilization Programs, and Market Standards November 1, 2013 Overview of October 24, 2013 Final Rule on Program Integrity:
Overview of October 24, 2013 Final Rule on Program Integrity: Exchange, Premium Stabilization Programs, and Market Standards November 1, 2013 Overview of October 24, 2013 Final Rule on Program Integrity:
Working Draft: Health Care Entities Revenue Recognition Implementation Issue. Financial Reporting Center Revenue Recognition
 October 2, 2017 Financial Reporting Center Revenue Recognition Working Draft: Health Care Entities Revenue Recognition Implementation Issue Issue #8-9 Risk Sharing Arrangements Expected Overall Level of
October 2, 2017 Financial Reporting Center Revenue Recognition Working Draft: Health Care Entities Revenue Recognition Implementation Issue Issue #8-9 Risk Sharing Arrangements Expected Overall Level of
Scope: Hometown Health Compliance Policies & Procedures apply to the following individuals and entities:
 Category: Author: HOMETOWN HEALTH POLICY Compliance Manager of Compliance Current Version Effective Date: Page 1 of 5 05/01/18 Next Review 05/01/19 Date: Revision History: 02/28/13 04/17/15 08/19/16 04/28/17
Category: Author: HOMETOWN HEALTH POLICY Compliance Manager of Compliance Current Version Effective Date: Page 1 of 5 05/01/18 Next Review 05/01/19 Date: Revision History: 02/28/13 04/17/15 08/19/16 04/28/17
The Road to Value. Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017
 The Road to Value Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017 1,500 Physicians UnityPoint Clinic 17 hospitals + 15 rural network hospitals 35,000
The Road to Value Aric R. Sharp, MHA, CMPE, FACHE Vice President Accountable Care UnityPoint Health February 3, 2017 1,500 Physicians UnityPoint Clinic 17 hospitals + 15 rural network hospitals 35,000
Bundled Payments for Care Improvement Advanced Program Compliance. To Receive CPE Credit. Individuals. Groups
 Bundled Payments for Care Improvement Advanced Program Compliance BKD National Health Care Group November 19, 2018 To Receive CPE Credit Individuals Participate in entire webinar Answer polls when they
Bundled Payments for Care Improvement Advanced Program Compliance BKD National Health Care Group November 19, 2018 To Receive CPE Credit Individuals Participate in entire webinar Answer polls when they
Proposed Rule on Medicaid Managed Care: A Summary of Major Provisions
 Proposed Rule on Medicaid Managed Care: A Summary of Major Provisions Julia Paradise and MaryBeth Musumeci On June 1, 2015, the Centers for Medicare & Medicaid Services (CMS) published a Notice of Proposed
Proposed Rule on Medicaid Managed Care: A Summary of Major Provisions Julia Paradise and MaryBeth Musumeci On June 1, 2015, the Centers for Medicare & Medicaid Services (CMS) published a Notice of Proposed
Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure
 Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of
Merit-Based Incentive Payment System (MIPS): ST-Elevation Myocardial Infarction (STEMI) with Percutaneous Coronary Intervention (PCI) Measure Measure Information Form 2019 Performance Period 1 Table of
PARTICIPATING ALLIED HEALTH PROFESSIONAL AGREEMENT TIOPA, INC.
 PARTICIPATING ALLIED HEALTH PROFESSIONAL AGREEMENT TIOPA, INC. August 24, 1998 Rev. January 26, 2000 August 2008 August 2009 March 2013 (LAST PAGE AGREEMENT WILL NEED TO BE SIGNED, DATED AND RETURNED)
PARTICIPATING ALLIED HEALTH PROFESSIONAL AGREEMENT TIOPA, INC. August 24, 1998 Rev. January 26, 2000 August 2008 August 2009 March 2013 (LAST PAGE AGREEMENT WILL NEED TO BE SIGNED, DATED AND RETURNED)
