How you are being measured by health plans, PBMs and accreditation organizations. December 2013
|
|
|
- Hilary Cunningham
- 6 years ago
- Views:
Transcription
1 How you are being measured by health plans, PBMs and accreditation organizations December
2 The U.S. health care system is rapidly moving to valuebased purchasing or value-driven healthcare Value is the balance of quality and costs, thus we can optimize value by improving quality while reducing costs One of the biggest challenges in driving better quality is that we can t always agree on how to define and measure quality PQA takes the lead on development of medicationrelated quality measures for evaluation of health plans, PBMs and pharmacies, and EQuIPP allows pharmacies to track their performance on quality metrics 2
3 Established in April 2006, as a public-private partnership Now a consensus-based, non-profit, alliance with >110 member organizations, including: Health Plans & PBMs Pharmacies & professional associations Federal agencies (CMS, FDA) Pharmaceutical mfrs Consumer advocates Technology & consulting groups Universities 3 Mission: Improve the quality of medication management and use across health care settings with the goal of improving patients health through a collaborative process to develop and implement performance measures and recognize examples of exceptional pharmacy quality.
4 Medicare Part D Plan Ratings Star measures: medication adherence (diabetes, BP, cholesterol) medication safety (HRM, Diabetes/RASA) Display measures (2 safety measures and 1 MTM measure) URAC and CPPA Accreditation PBM, mail/specialty pharmacy, community Rx Health Plan Accreditation NCQA (HEDIS measure set) NBCH (evalue8 measure set) State Insurance Exchanges / Marketplaces 4
5 Community Pharmacy Accreditation is now available Voluntary participation; no payers require it yet Cost > $3000 per store On-site survey of each store may be required Pharmacies must engage in quality measurement (including consumer surveys), but are not required to report actual performance scores yet. PQA measures are encouraged but not required. Pharmacies must engage in quality improvement 5
6 PBM accreditation program has been active for several years, and mail/specialty programs are also in place now Starting in 2014, PBMs are required to submit data for quality measures Quality measures include several from PQA, including medication adherence (PDC rates for several drug classes) Community pharmacy accreditation standards have been developed, but the program has not yet been rolled out Accreditation reviews/surveys may allow chains to receive chainwide accreditation based on sample of stores (not clear yet) 6
7 Health plan accreditation has been in place since 1990s HEDIS is the performance measure set HEDIS contains numerous performance measures related to medications, including asthma, arthritis and antidepressant classes Many HEDIS outcomes measures may be heavily influenced by medication use (e.g., A1c, LDL, BP control) HEDIS measures are also used for Medicare Part C (MA) plans Pharmacies have not optimized their ability to drive improvements in these measures for health plans. The HEDIS measures for Medicare Advantage (MA) plans affect the quality bonus payments for these plans and create need for better medication use. 7
8 The National Business Coalition on Health (NBCH) collects performance data on health plans via the evalue8 program evalue8 is focused on the commercial book of business for health plans since NBCH represents employer coalitions evalue8 contains several PQA quality measures, including medication adherence, asthma, & drug-drug interactions evalue8 is not as widely used as NCQA s HEDIS reports for evaluating health plans 8
9 Annual ratings of Medicare plans that are made available on Medicare Plan Finder and CMS website Ratings are displayed as 1 to 5 stars Stars are calculated for each measure, as well as each domain, summary, and overall (applies to MA-PDs) level Ratings of all Medicare plans can be found at: Coverage/PrescriptionDrugCovGenIn/PerformanceData.html 9
10 Medicare drug plans receive a summary rating on quality as well as four domain, and individual measure, scores (15 individual measures) Five measures are from PQA: 2 measures of medication safety High risk medications in the elderly Appropriate treatment of blood pressure in persons with diabetes 3 measures of medication adherence Oral diabetes medications Cholesterol medication (statins) Blood pressure (renin-angiotensin system antagonists) Due to the higher weighting of clinically-relevant measures, the PQA measures account for 45% of Part D summary ratings in
11 Display measures are not a part of the Star Ratings, but are used to provide benchmarks and feedback to plans CMS also monitors display measures to assess plan performance; poor performance can lead to compliance actions by CMS Display measures (from PQA): Drug-Drug Interactions Excessive doses of oral diabetes medications Comprehensive Medication Review (CMR) Completion Rate (moving to stars!) HIV antiretroviral medication adherence (only in safety reports) New Display measure (NOT from PQA) Use of atypical antipsychotics 11
12 Released on Monday, Oct 21 (delayed due to gov t shutdown) Top Performers for Part D: Kaiser Permanente Some Humana plans (IL was 5-star, other states lower) Most top-performance plans tended to be on west coast or in upper Midwest (many hypotheses as to why this is the case) 12 Worst Performers for Part D: 39 Medicare contracts received a low performer icon which means that they have consistently been below 3 stars Most low-performance contracts were in southern states and Puerto Rico; many contracts in AL, GA, TN, LA, TX and PR had 1-2 stars on medication adherence/safety measures
13 A study published in JAMA on January 16, 2013, concluded that Medicare's 5-star rating program for Medicare Advantage is associated with beneficiaries' enrollment decisions. Among first-time enrollees, a 1-star higher rating was associated with a 9.5 (95% CI, ) percentage-point increase in likelihood to enroll. Among enrollees switching plans, a 1-star higher rating was associated with a 4.4 (95% CI, ) percentage-point increase in likelihood to enroll. Star ratings were less strongly associated with enrollment for black, rural, low-income, and the youngest beneficiaries. 13
14 The star ratings now affect payment to Medicare Advantage plans wherein higher-rated plans get higher payment Quality Bonus Payments (QBPs) are being awarded on a sliding scale according to star ratings QBPs were created by PPACA but have been phased in via a demonstration project 2015 payments will be based on 2014 ratings which are based on 2012 and 2013 data QBP opportunity for large MA-PDs (Humana, United Healthcare, Aetna/Coventry, CIGNA/HealthSpring) may exceed $100 million 14
15 Formularies, clinical strategies, network contracts, marketing/promotions, aligning with star measures Significant investments in drive to 5 Contract strategies for pharmacy networks Pay for Performance (P4P) pharmacies may be eligible for bonus payment based on star performance Preferred pharmacy network based partly on star performance of chain or stores 15
16 A few health plans have already implemented P4P for pharmacies, including Health Partners and Inland Empire Health Plan Example: Inland Empire Health Plan (IEHP) Launched in October 2013 Pharmacies are evaluated on Star measures plus asthma and GDR EQuIPP allows pharmacies to track their performance Pharmacies will receive bonus payments every six months depending on their performance on each measure: 3-star attainment = small bonus 5-star attainment = large bonus Bonus is based on number of patients at each store in addition to score on each measure IEHP may also do public recognition of top performers 16
17 As Health Plans and PBMs create financial consequences for pharmacies related to the star ratings, there is a need for a neutral intermediary to ensure accuracy, consistency and transparency. EQuIPP, from PQS, is increasingly being tapped to serve as the neutral intermediary. In this role, EQuIPP Ensures that the star measure scores for pharmacies are calculated accurately (i.e., according to PQA/CMS specifications), Ensures that star measure scores are calculated consistently across plans/pbms so that pharmacies can avoid dueling report cards, Provides transparency in the calculation of the star measure score calculations so that pharmacies understand how their scores were calculated. 17
18 EQuIPP is a multi-plan, multi-pharmacy, collaborative to: Support collaboration of health plans, PBMs and pharmacies for Quality Improvement related to medication use Allow consistent, standardized assessment of community pharmacy performance on Part D stars and other quality measures Enable faster, more-refined, benchmarking of Part D stars performance in key market areas EQuIPP provides a neutral assessment of quality for trusted performance assessment and benchmarking by all parties. EQuIPP lays the foundation for performance-based contracts and payment systems for pharmacy networks 18
19 EQuIPP measures are from PQA: - 3 measures of medication safety - High risk medications in the elderly - Appropriate treatment of blood pressure in persons with diabetes - Drug-drug interactions - 3 measures of medication adherence - Oral diabetes medications - Cholesterol medication (statins) - Blood pressure (renin-angiotensin system antagonists) Additional quality measures can be added to align with CMS, NCQA, URAC or other initiatives 19
20 Health plans & PBMs: Access to performance dashboards that display their performance and relevant benchmarks on Star Ratings metrics across lines of business and across geographic regions Visibility into the performance of their pharmacy network Pharmacies: Access to performance dashboards that report their scores and relevant benchmarks across the same key quality measures EQuIPP supports multi-tier views of a pharmacy organization s performance from the individual store, through districts/regions, to the corporate rollup 20
21 Home Page 21 21
22 22
23 23
24 24 Pharmacy names listed in this space PQA
25 Pharmacy View 25 PQA
26 26 Health Plan names here PQA
27 27
28 Pharmacies are being evaluated NOW on quality measures related to Part D stars A few health plans have already implemented P4P for pharmacies Several more health plans and PBMs have indicated their intent to implement P4P for the pharmacy network Some PBMs have formulated strategies for moving towards preferred networks that only include top-performers on stars (price will still matter, but quality will also matter) EQuIPP serves as a neutral intermediary for calculation of pharmacy quality scores and makes the information available to pharmacies Know your quality scores! 28
29 29
The Impact of Adherence Quality Measures on the US Healthcare Marketplace
 The Impact of Adherence Quality Measures on the US Healthcare Marketplace Samuel Stolpe, PharmD Associate Director, Quality Initiatives Pharmacy Quality Alliance Pharmacy Quality Alliance (PQA) Established
The Impact of Adherence Quality Measures on the US Healthcare Marketplace Samuel Stolpe, PharmD Associate Director, Quality Initiatives Pharmacy Quality Alliance Pharmacy Quality Alliance (PQA) Established
Pay for Performance & the Changing Landscape for Pharmacy: A Panel Discussion
 Pay for Performance & the Changing Landscape for Pharmacy: A Panel Discussion Panelists: Mark Conklin, Pharmacy Quality Solutions Alex Cruz, Healthfirst Crystal Lennartz, Health Mart Jesse McCullough,
Pay for Performance & the Changing Landscape for Pharmacy: A Panel Discussion Panelists: Mark Conklin, Pharmacy Quality Solutions Alex Cruz, Healthfirst Crystal Lennartz, Health Mart Jesse McCullough,
How Medication Adherence and Outcomes Are Changing the Business Model
 How Medication Adherence and Outcomes Are Changing the Business Model Laura Cranston Executive Director Todd Sega Manager, Payer Relations Lari Harding VP, Strategy & Growth Healthcare Network 3 Session
How Medication Adherence and Outcomes Are Changing the Business Model Laura Cranston Executive Director Todd Sega Manager, Payer Relations Lari Harding VP, Strategy & Growth Healthcare Network 3 Session
STAR RATINGS PBM PARTNERSHIP, MAXIMUM RESULTS. Michelle Juhanson, CHC, CHPC Director of Compliance and Quality PerformRx
 STAR RATINGS PBM PARTNERSHIP, MAXIMUM RESULTS Michelle Juhanson, CHC, CHPC Director of Compliance and Quality PerformRx Agenda History & Timeline Quality Bonus Payment CMS Changes The PBM Role Best Practices
STAR RATINGS PBM PARTNERSHIP, MAXIMUM RESULTS Michelle Juhanson, CHC, CHPC Director of Compliance and Quality PerformRx Agenda History & Timeline Quality Bonus Payment CMS Changes The PBM Role Best Practices
DIR fees are knocking down pharmacy profits
 16 America s PHARMACIST November 2016 DIR fees are knocking down pharmacy profits by Bruce A. Semingson, Pharmacist In 2016, retail pharmacy will pay between $360 million and $2.16 billion in direct and
16 America s PHARMACIST November 2016 DIR fees are knocking down pharmacy profits by Bruce A. Semingson, Pharmacist In 2016, retail pharmacy will pay between $360 million and $2.16 billion in direct and
Understanding Pay For Performance and DIR Impact to Pharmacy Reimbursement
 Understanding Pay For and DIR Impact to Pharmacy Reimbursement A Public Service Announcement brought to you by Melanie Maxwell, MHP Vice President RxSelect Pharmacy Services Please Don t Shoot the Messenger
Understanding Pay For and DIR Impact to Pharmacy Reimbursement A Public Service Announcement brought to you by Melanie Maxwell, MHP Vice President RxSelect Pharmacy Services Please Don t Shoot the Messenger
2017 Number of Contracts. Weighted by Enrollment
 Fact Sheet - 2019 Part C and D Star Ratings Note: The information included in this Fact Sheet is based on the 2019 Star Ratings published on Medicare Plan Finder (MPF) on October 10, 2018. For details
Fact Sheet - 2019 Part C and D Star Ratings Note: The information included in this Fact Sheet is based on the 2019 Star Ratings published on Medicare Plan Finder (MPF) on October 10, 2018. For details
CMS Medicare Advantage 2018 Advance Notice Summary
 CMS Medicare Advantage 2018 Advance Notice Summary KEY HIGHLIGHTS February 2017 Risk Adjustment Part C Coding Intensity Adjustment: 5.91% Part C Normalization Factor: 1.017 Adjusted Effective Growth Rate
CMS Medicare Advantage 2018 Advance Notice Summary KEY HIGHLIGHTS February 2017 Risk Adjustment Part C Coding Intensity Adjustment: 5.91% Part C Normalization Factor: 1.017 Adjusted Effective Growth Rate
Disease Management and the Medicare Drug Benefit: Opportunities and Threats for the Pharmaceutical Industry
 Disease Management and the Medicare Drug Benefit: Opportunities and Threats for the Pharmaceutical Industry Jeffrey A. Bourret, M.S., R.Ph., FASHP Senior Director, Managed Markets Healthcare Systems Marketing
Disease Management and the Medicare Drug Benefit: Opportunities and Threats for the Pharmaceutical Industry Jeffrey A. Bourret, M.S., R.Ph., FASHP Senior Director, Managed Markets Healthcare Systems Marketing
Fact Sheet Part C and D Star Ratings
 Fact Sheet - 2018 Part C and D Star Ratings Note: The information included in this Fact Sheet is based on the 2018 Star Ratings published on Medicare Plan Finder (MPF) on October 11, 2017. For details
Fact Sheet - 2018 Part C and D Star Ratings Note: The information included in this Fact Sheet is based on the 2018 Star Ratings published on Medicare Plan Finder (MPF) on October 11, 2017. For details
Medicare 2017 Part C & D Star Rating Technical Notes
 Medicare 2017 Part C & D Star Rating Technical Notes Updated 09/26/2016 Document Change Log Previous Version Description of Change Revision Date - Final 2017 Part C & D Star Ratings Technical Notes, fall
Medicare 2017 Part C & D Star Rating Technical Notes Updated 09/26/2016 Document Change Log Previous Version Description of Change Revision Date - Final 2017 Part C & D Star Ratings Technical Notes, fall
Strategies to Increase CMR Completion Rates in Medicare MTM Programs
 Strategies to Increase CMR Completion Rates in Medicare MTM Programs Erwin Jeong, Pharm.D., FCSHP Clinical Operations Manager, Medicare MTM Program Kaiser Permanente, Southern California October 29, 2016
Strategies to Increase CMR Completion Rates in Medicare MTM Programs Erwin Jeong, Pharm.D., FCSHP Clinical Operations Manager, Medicare MTM Program Kaiser Permanente, Southern California October 29, 2016
The Medicare Advantage program: Status report
 C H A P T E R12 The Medicare Advantage program: Status report C H A P T E R 12 The Medicare Advantage program: Status report Chapter summary In this chapter Each year the Commission provides a status
C H A P T E R12 The Medicare Advantage program: Status report C H A P T E R 12 The Medicare Advantage program: Status report Chapter summary In this chapter Each year the Commission provides a status
Seeing Stars in Puerto Rico
 Seeing Stars in Puerto Rico Stephen Wood Senior Vice President, Development Universal American March 6, 2014 1 What s in the Stars? 2014 Stars scores have improved na
Seeing Stars in Puerto Rico Stephen Wood Senior Vice President, Development Universal American March 6, 2014 1 What s in the Stars? 2014 Stars scores have improved na
March 1, Dear Mr. Kouzoukas:
 March 1, 2019 Mr. Demetrios L. Kouzoukas Principal Deputy Administrator and Director Center for Medicare Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: Advance
March 1, 2019 Mr. Demetrios L. Kouzoukas Principal Deputy Administrator and Director Center for Medicare Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: Advance
Estimate of Medicare Part D Costs After Accounting for Manufacturer Rebates
 October 2016 Estimate of Medicare Part D Costs After Accounting for Manufacturer Rebates A Study of Original Branded Products in the U.S. $ Introduction The cost of medicines in the U.S. has been the subject
October 2016 Estimate of Medicare Part D Costs After Accounting for Manufacturer Rebates A Study of Original Branded Products in the U.S. $ Introduction The cost of medicines in the U.S. has been the subject
WorldatWork You and Your PBM: Improving Discounts, Fees and Rebates, and Beyond. Kristin Begley, Pharm.D. Principal
 WorldatWork You and Your PBM: Improving Discounts, Fees and Rebates, and Beyond Kristin Begley, Pharm.D. Principal Presentation Overview The future of drug trend Prescription drug management levers: Contracting
WorldatWork You and Your PBM: Improving Discounts, Fees and Rebates, and Beyond Kristin Begley, Pharm.D. Principal Presentation Overview The future of drug trend Prescription drug management levers: Contracting
Pharmacy Trend Management
 Pharmacy Trend Management Strategies for Maximizing the Value of Your Pharmacy Spend Presenter's Name Presentation Date May 1, 2008 Today s speakers Bridget Eber, Pharm.D. Principal and National Pharmacy
Pharmacy Trend Management Strategies for Maximizing the Value of Your Pharmacy Spend Presenter's Name Presentation Date May 1, 2008 Today s speakers Bridget Eber, Pharm.D. Principal and National Pharmacy
Standing strong for payers and patients
 Standing strong for payers and patients Eric Slusser, EVP, Chief Financial Officer Everett Neville, SVP Supply Chain and Specialty B A N K O F A M E R I C A M E R R I L L L Y N C H H E A LTH C A RE CONFERENCE
Standing strong for payers and patients Eric Slusser, EVP, Chief Financial Officer Everett Neville, SVP Supply Chain and Specialty B A N K O F A M E R I C A M E R R I L L L Y N C H H E A LTH C A RE CONFERENCE
VALUE-BASED PAYMENTS, STAR RATINGS AND THE LESSONS OF MEDICARE ADVANTAGE. A Presentation to the 11 th Annual Value-Based Payment and P4P Summit
 VALUE-BASED PAYMENTS, STAR RATINGS AND THE LESSONS OF MEDICARE ADVANTAGE A Presentation to the 11 th Annual Value-Based Payment and P4P Summit JOHN GORMAN EXECUTIVE CHAIRMAN FEBRUARY 19, 2016 CUT TO THE
VALUE-BASED PAYMENTS, STAR RATINGS AND THE LESSONS OF MEDICARE ADVANTAGE A Presentation to the 11 th Annual Value-Based Payment and P4P Summit JOHN GORMAN EXECUTIVE CHAIRMAN FEBRUARY 19, 2016 CUT TO THE
SPECIALTY PHARMACY MANDATORY MEASURES
 SPECIALTY PHARMACY MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # DESCRIPTION NUMERATOR DENOMINATOR DTM
SPECIALTY PHARMACY MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # DESCRIPTION NUMERATOR DENOMINATOR DTM
2012 Checklist for Community Pharmacy. Medicare Part D-Related Information
 NATIONAL COMMUNITY PHARMACISTS ASSOCIATION 2012 Checklist for Community Pharmacy Medicare Part D-Related Information Medicare Part D Valid Prescriber Identifiers For 2012, CMS will continue to permit the
NATIONAL COMMUNITY PHARMACISTS ASSOCIATION 2012 Checklist for Community Pharmacy Medicare Part D-Related Information Medicare Part D Valid Prescriber Identifiers For 2012, CMS will continue to permit the
Brian Bertha VP, Corporate Strategy and Business Development McKesson U.S. Pharmaceutical
 Brian Bertha VP, Corporate Strategy and Business Development McKesson U.S. Pharmaceutical 2 Safe Harbor Clause Some of the information in this presentation may constitute forwardlooking statements that
Brian Bertha VP, Corporate Strategy and Business Development McKesson U.S. Pharmaceutical 2 Safe Harbor Clause Some of the information in this presentation may constitute forwardlooking statements that
Medicare Advantage: Early Views and Trend Spotting: What We Know From Analyzing Public Data Files
 Medicare Advantage: Early Views and Trend Spotting: What We Know From Analyzing Public Data Files By Marsha Gold, Sc.D. Senior Fellow Mathematica Policy Research Presentation to the Alliance for Health
Medicare Advantage: Early Views and Trend Spotting: What We Know From Analyzing Public Data Files By Marsha Gold, Sc.D. Senior Fellow Mathematica Policy Research Presentation to the Alliance for Health
Draft Released: February 1, Final Released: April 2, Effective Date: January 1, 2019
 AMCP Summary: Announcement of Calendar Year (CY) 2019 Medicare Advantage Capitation Rates and Medicare Advantage and Part D Payment Policies and Final Call Letter Draft Released: February 1, 2018 Final
AMCP Summary: Announcement of Calendar Year (CY) 2019 Medicare Advantage Capitation Rates and Medicare Advantage and Part D Payment Policies and Final Call Letter Draft Released: February 1, 2018 Final
DIR FEES: WHAT YOU NEED TO KNOW JULY 13, :00 10:00 AM
 DIR FEES: WHAT YOU NEED TO KNOW JULY 13, 2017 9:00 10:00 AM ACPE UAN: 0107-9999-17-078-L04-P 0.1 CEU/1.0 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists: Upon completion of this CPE
DIR FEES: WHAT YOU NEED TO KNOW JULY 13, 2017 9:00 10:00 AM ACPE UAN: 0107-9999-17-078-L04-P 0.1 CEU/1.0 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists: Upon completion of this CPE
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business?
 Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Gulf Coast and LA HFMA Payer Summit Value-based contracts same healthcare business? Richard R. Vath, MD FMOLHS SVP/Chief Clinical Transformation Officer President Health Leaders Network and Medicare ACO
Part One: FEDERAL POLICY AND MEDICARE S IMPACT ON THE ECONOMY
 Introducing the first in a three-part series of white papers designed to explore 1) Why the nation s health system is facing a financial crisis, 2) How providers that accept Medicare Advantage plans and
Introducing the first in a three-part series of white papers designed to explore 1) Why the nation s health system is facing a financial crisis, 2) How providers that accept Medicare Advantage plans and
How Does CCNC s Model Align with Value Based Payments? Lead Community Pharmacy Coordinator CCNC V.P. Moose Pharmacy Joe Moose, PharmD
 Improving care through shared knowledge How Does CCNC s Model Align with Value Based Payments? Lead Community Pharmacy Coordinator CCNC V.P. Moose Pharmacy Joe Moose, PharmD $100 Total Healthcare Spend
Improving care through shared knowledge How Does CCNC s Model Align with Value Based Payments? Lead Community Pharmacy Coordinator CCNC V.P. Moose Pharmacy Joe Moose, PharmD $100 Total Healthcare Spend
STARs Program and SETMA s Solution By James L. Holly, MD Your Life Your Health The Examiner April 26, 2012
 STARs Program and SETMA s Solution By James L. Holly, MD Your Life Your Health The Examiner April 26, 2012 Increasingly, health plans and particularly Federal programs are requiring evidence of quality
STARs Program and SETMA s Solution By James L. Holly, MD Your Life Your Health The Examiner April 26, 2012 Increasingly, health plans and particularly Federal programs are requiring evidence of quality
Think like a 5 Star Plan. Act like a 5 Star Plan. Be a 5 Star Plan.
 The Road to 5 Stars Think like a 5 Star Plan. Act like a 5 Star Plan. Be a 5 Star Plan. A whitepaper 5550 W. Idlewild Avenue, Suite 150. Tampa, FL 33634. (813) 304-2800. Innovation@MedHOK.com The quest
The Road to 5 Stars Think like a 5 Star Plan. Act like a 5 Star Plan. Be a 5 Star Plan. A whitepaper 5550 W. Idlewild Avenue, Suite 150. Tampa, FL 33634. (813) 304-2800. Innovation@MedHOK.com The quest
Healthcare Purchasing in an Era of Accountable Care: How Will Provider Groups Define and Deliver Value?? What will it take?
 Healthcare Purchasing in an Era of Accountable Care: How Will Provider Groups Define and Deliver Value?? What will it take? P sharon.levine@kp.org The Permanente Medical Group June 2013 Copyright 2013
Healthcare Purchasing in an Era of Accountable Care: How Will Provider Groups Define and Deliver Value?? What will it take? P sharon.levine@kp.org The Permanente Medical Group June 2013 Copyright 2013
Medicare Advantage star ratings: Expectations for new organizations
 Medicare Advantage star ratings: Expectations for new organizations February 2018 Kelly S. Backes, FSA, MAAA Julia M. Friedman, FSA, MAAA Dustin J. Grzeskowiak, FSA, MAAA Elizabeth L. Phillips Patricia
Medicare Advantage star ratings: Expectations for new organizations February 2018 Kelly S. Backes, FSA, MAAA Julia M. Friedman, FSA, MAAA Dustin J. Grzeskowiak, FSA, MAAA Elizabeth L. Phillips Patricia
Cigna. Confirmed complaints: 5. Quality Overview. How Often Do Members Complain About This Company? Accreditation Exchange Product
 Quality Overview Accreditation Exchange Product Accrediting Organization: NCQA Health Plan Accreditation (Exchange) Accreditation Status: Pending (214) Accreditation Commercial Product Accreditation Organization:
Quality Overview Accreditation Exchange Product Accrediting Organization: NCQA Health Plan Accreditation (Exchange) Accreditation Status: Pending (214) Accreditation Commercial Product Accreditation Organization:
January 16, Ms. Seema Verma Administrator Centers for Medicare & Medicaid Services 7500 Security Blvd. Baltimore, Maryland 21244
 January 16, 2018 Ms. Seema Verma Administrator Centers for Medicare & Medicaid Services 7500 Security Blvd. Baltimore, Maryland 21244 Re: MAPRx Draft Comment Letter on Medicare Program; Contract Year 2019
January 16, 2018 Ms. Seema Verma Administrator Centers for Medicare & Medicaid Services 7500 Security Blvd. Baltimore, Maryland 21244 Re: MAPRx Draft Comment Letter on Medicare Program; Contract Year 2019
The Management of Specialty Drugs: Opportunities and Challenges
 The Management of Specialty Drugs: Opportunities and Challenges Scott Woods Senior Director, Policy PCMA Innovations X April 5, 2016 Specialty Drugs to be Half of Spend by 2018 Forecast PMPM Net Drug
The Management of Specialty Drugs: Opportunities and Challenges Scott Woods Senior Director, Policy PCMA Innovations X April 5, 2016 Specialty Drugs to be Half of Spend by 2018 Forecast PMPM Net Drug
Note: Accredited is the highest rating an exchange product can have for 2015.
 Quality Overview Permanente Accreditation Exchange Product Accrediting Organization: NCQA HMO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange product can
Quality Overview Permanente Accreditation Exchange Product Accrediting Organization: NCQA HMO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange product can
Understanding PBM Quality. The 2 nd National Alliance PBM Report. John Miller
 Understanding PBM Quality The 2 nd National Alliance PBM Report John Miller john.miller@mabgh.org 1 2 2 MARKET SHARE All Other 3% MedImpact 5% Prime Therapeutics 6% CVS/Caremark 25% Humana 7% Envision
Understanding PBM Quality The 2 nd National Alliance PBM Report John Miller john.miller@mabgh.org 1 2 2 MARKET SHARE All Other 3% MedImpact 5% Prime Therapeutics 6% CVS/Caremark 25% Humana 7% Envision
Compensation and Reimbursement
 492 Pharmacy Management: Compensation and Reimbursement Positions Compensation and Reimbursement Revenue Cycle Compliance and Management (1710) To encourage pharmacists to serve as leaders in the development
492 Pharmacy Management: Compensation and Reimbursement Positions Compensation and Reimbursement Revenue Cycle Compliance and Management (1710) To encourage pharmacists to serve as leaders in the development
KEEPING PRESCRIPTION DRUGS AFFORDABLE: The Value of Pharmacy Benefit Managers (PBMs)
 The Texas Association of Health Plans Representing health insurers, health maintenance organizations, and other related health care entities operating in Texas. KEEPING PRESCRIPTION DRUGS AFFORDABLE: The
The Texas Association of Health Plans Representing health insurers, health maintenance organizations, and other related health care entities operating in Texas. KEEPING PRESCRIPTION DRUGS AFFORDABLE: The
32 nd Annual J.P. Morgan Healthcare Conference
 Bruce Broussard President and Chief Executive Officer 32 nd Annual J.P. Morgan Healthcare Conference San Francisco, CA January 13, 2014 Cautionary Statement This presentation includes forward-looking statements
Bruce Broussard President and Chief Executive Officer 32 nd Annual J.P. Morgan Healthcare Conference San Francisco, CA January 13, 2014 Cautionary Statement This presentation includes forward-looking statements
Value Based Pay for Performance Results for Measurement Year September 2014
 Value Based Pay for Performance Results for Measurement Year 2013 September 2014 Program Overview 2016 Integrated Healthcare Association. All rights reserved. 2 Value Based Pay for Performance 2016 Integrated
Value Based Pay for Performance Results for Measurement Year 2013 September 2014 Program Overview 2016 Integrated Healthcare Association. All rights reserved. 2 Value Based Pay for Performance 2016 Integrated
Via Electronic Submission (www.regulations.gov) January 16, 2018
 Via Electronic Submission (www.regulations.gov) January 16, 2018 Ms. Seema Verma Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services ATTN: CMS-4182-P 7500
Via Electronic Submission (www.regulations.gov) January 16, 2018 Ms. Seema Verma Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services ATTN: CMS-4182-P 7500
Session 8L, Future of Medicare Advantage: Trends of an Expanding Market. Moderator/Presenter: Gregory V. Sgrosso, FSA, MAAA
 Session 8L, Future of Medicare Advantage: Trends of an Expanding Market Moderator/Presenter: Gregory V. Sgrosso, FSA, MAAA Presenters: Haitham Aly David Hayes, FSA, MAAA Gregory V. Sgrosso, FSA, MAAA SOA
Session 8L, Future of Medicare Advantage: Trends of an Expanding Market Moderator/Presenter: Gregory V. Sgrosso, FSA, MAAA Presenters: Haitham Aly David Hayes, FSA, MAAA Gregory V. Sgrosso, FSA, MAAA SOA
Implement a definition of negotiated price to include all pharmacy price concessions.
 NCPA Analysis of Medicare Part D Pharmacy DIR Fee Reform Policy Proposal and Other Policies Impacting Community Pharmacies in the CMS Proposed Rule, Modernizing Part D and Medicare Advantage to Lower Drug
NCPA Analysis of Medicare Part D Pharmacy DIR Fee Reform Policy Proposal and Other Policies Impacting Community Pharmacies in the CMS Proposed Rule, Modernizing Part D and Medicare Advantage to Lower Drug
A Practical Discussion of Value and Quality Based Payments What Do I Do Now?
 Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
Emerging Challenges in Primary Care: 2016 A Practical Discussion of Value and Quality Based Payments What Do I Do Now? Modified from AHLA Physicians and Hospitals Law Institute 2016 Faculty Ellie Bane
Released: February 19, Comments Due: March 4, 2016
 SUMMARY AMCP Summary: Advance Notice of Methodological Changes for Calendar Year (CY) 2017 for Medicare Advantage (MA) Capitation Rates, Part C and Part D Payment Policies and 2017 Call Letter Released:
SUMMARY AMCP Summary: Advance Notice of Methodological Changes for Calendar Year (CY) 2017 for Medicare Advantage (MA) Capitation Rates, Part C and Part D Payment Policies and 2017 Call Letter Released:
Meeting the Health Care Challenges of Tomorrow. Jon Roberts Executive Vice President & President, CVS Caremark
 Meeting the Health Care Challenges of Tomorrow Jon Roberts Executive Vice President & President, CVS Caremark Agenda PBMs: Needed Now More Than Ever Performance Highlights How We Address Payors #1 Priority:
Meeting the Health Care Challenges of Tomorrow Jon Roberts Executive Vice President & President, CVS Caremark Agenda PBMs: Needed Now More Than Ever Performance Highlights How We Address Payors #1 Priority:
I. PURPOSE. A. The primary objectives of Molina Healthcare s Transition Policy and Procedure are:
 I. PURPOSE The purpose of the Policy and Procedure is to ensure necessary continuity of treatment and to provide adequate time and transition process to introduce the enrollee and their prescribing physician
I. PURPOSE The purpose of the Policy and Procedure is to ensure necessary continuity of treatment and to provide adequate time and transition process to introduce the enrollee and their prescribing physician
PREFERRED PHARMACY NETWORKS AND THEIR IMPACT ON PART D PREMIUMS
 PREFERRED PHARMACY NETWORKS AND THEIR IMPACT ON PART D PREMIUMS March 13, 2018 RANDALL FITZPATRICK FSA, MAAA GLENN GIESE FSA, MAAA ZACH HANSON ASA, MAAA CONTENTS Executive Summary... 2 Introduction...
PREFERRED PHARMACY NETWORKS AND THEIR IMPACT ON PART D PREMIUMS March 13, 2018 RANDALL FITZPATRICK FSA, MAAA GLENN GIESE FSA, MAAA ZACH HANSON ASA, MAAA CONTENTS Executive Summary... 2 Introduction...
March 2, Dear Acting Administrator Tavenner:
 Marilyn Tavenner, Acting Administrator Center for Medicare and Medicaid Services (CMS) 7500 Security Boulevard C1-13-07 Baltimore, Maryland 21244 Re: Advance Notice of Methodological Changes for Calendar
Marilyn Tavenner, Acting Administrator Center for Medicare and Medicaid Services (CMS) 7500 Security Boulevard C1-13-07 Baltimore, Maryland 21244 Re: Advance Notice of Methodological Changes for Calendar
DIR: Trends, Issues, and Impending Impacts
 DIR: Trends, Issues, and Impending Impacts Lari Harding Vice President, Product Marketing Chris Smith, R.Ph Director, Pharmacy Business Intelligence 1 Disclosures Lari Harding is the Vice President, Product
DIR: Trends, Issues, and Impending Impacts Lari Harding Vice President, Product Marketing Chris Smith, R.Ph Director, Pharmacy Business Intelligence 1 Disclosures Lari Harding is the Vice President, Product
Medicare Health & Drug Plan Quality and Performance Ratings 2012 Part C & Part D Technical Notes. First Plan Preview DRAFT
 Medicare Health & Drug Plan Quality and Performance Ratings 2012 Part C & Part D Technical Notes First Plan Preview Updated 08/04/2011 Table of Contents INTRODUCTION... 1 DIFFERENCES BETWEEN THE 2011 PLAN
Medicare Health & Drug Plan Quality and Performance Ratings 2012 Part C & Part D Technical Notes First Plan Preview Updated 08/04/2011 Table of Contents INTRODUCTION... 1 DIFFERENCES BETWEEN THE 2011 PLAN
September 6, Re: CMS-1600-P; CY 2014 Physician Fee Schedule Proposed rule comments
 September 6, 2013 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention CMS-1600-P Mail Stop C4-26-05 7500 Security Boulevard Baltimore, MD 21244-1850 Re: CMS-1600-P;
September 6, 2013 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention CMS-1600-P Mail Stop C4-26-05 7500 Security Boulevard Baltimore, MD 21244-1850 Re: CMS-1600-P;
Co-Pay Incentives: Medicare Advantage (Part D) Can Replicate Successes of Commercial Payers
 Co-Pay Incentives: Medicare Advantage (Part D) Can Replicate Successes of Commercial Payers Co-pay incentives proven to drive behavior change, reduce costs, and accelerate positive outcomes Center for
Co-Pay Incentives: Medicare Advantage (Part D) Can Replicate Successes of Commercial Payers Co-pay incentives proven to drive behavior change, reduce costs, and accelerate positive outcomes Center for
March 3, VIA Electronic Filing:
 March 3, 2017 VIA Electronic Filing: AdvanceNotice2018@cms.hhs.gov Cynthia G. Tudor, PhD Acting Administrator Centers for Medicare & Medicaid Services 7500 Security Blvd. Baltimore, Maryland 21244 Dear
March 3, 2017 VIA Electronic Filing: AdvanceNotice2018@cms.hhs.gov Cynthia G. Tudor, PhD Acting Administrator Centers for Medicare & Medicaid Services 7500 Security Blvd. Baltimore, Maryland 21244 Dear
Medicare Advantage Star Rating of California Physician Organizations Measurement Year December 2015
 Medicare Advantage Star Rating of California Physician Organizations Measurement Year 2014 December 2015 Why Measure Medicare Advantage (MA)? IHA measures Medicare Advantage (MA) star ratings (1-5 stars)
Medicare Advantage Star Rating of California Physician Organizations Measurement Year 2014 December 2015 Why Measure Medicare Advantage (MA)? IHA measures Medicare Advantage (MA) star ratings (1-5 stars)
Healthcare Reform. North Carolina Dietetic Association September 12, Duke Medicine
 Healthcare Reform North Carolina Dietetic Association September 12, 2014 Take home messages Healthcare [and health insurance] is transforming at an accelerating pace Key metrics of concern relate to quality,
Healthcare Reform North Carolina Dietetic Association September 12, 2014 Take home messages Healthcare [and health insurance] is transforming at an accelerating pace Key metrics of concern relate to quality,
SPECIALTY PHARMACY ACCREDITATION V3.0 MANDATORY MEASURES
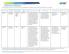 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual basis. # DESCRIPTION NUMERATOR DENOMINATOR DATA SOURCE DM2012-13 Drug-Drug
MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual basis. # DESCRIPTION NUMERATOR DENOMINATOR DATA SOURCE DM2012-13 Drug-Drug
August 4, The Honorable Charles Rangel, Chairman Committee on Ways and Means United States House of Representatives Washington, D.C.
 August 4, 2009 The Honorable Charles Rangel, Chairman Committee on Ways and Means United States House of Representatives Washington, D.C. 20515 The Honorable Henry A. Waxman, Chairman Committee on Energy
August 4, 2009 The Honorable Charles Rangel, Chairman Committee on Ways and Means United States House of Representatives Washington, D.C. 20515 The Honorable Henry A. Waxman, Chairman Committee on Energy
Linking Performance and Compliance: How Part D Quality Measures Relate to Plan Performance
 Linking Performance and Compliance: How Part D Quality Measures Relate to Plan Performance Medicare Rx Part D Compliance Conf. Monday, December 8, 2008 9:45 a.m. 10:45 a.m. Cynthia Tudor, PhD Director
Linking Performance and Compliance: How Part D Quality Measures Relate to Plan Performance Medicare Rx Part D Compliance Conf. Monday, December 8, 2008 9:45 a.m. 10:45 a.m. Cynthia Tudor, PhD Director
Better Medicare Alliance Webinar: Medicare Advantage and Part D 2019 Advance Notice and Draft Call Letter. February 8, 2018
 Better Medicare Alliance Webinar: Medicare Advantage and Part D 2019 Advance Notice and Draft Call Letter February 8, 2018 RATE NOTICE CRASH Opening COURSE Remarks PAGE http://bettermedicarealliance.org/campaigns
Better Medicare Alliance Webinar: Medicare Advantage and Part D 2019 Advance Notice and Draft Call Letter February 8, 2018 RATE NOTICE CRASH Opening COURSE Remarks PAGE http://bettermedicarealliance.org/campaigns
Gateway to Practitioner Excellence (GPE)
 Gateway to Practitioner Excellence (GPE) 2018 Medicaid Recognizing and Rewarding Excellent Practices Improving the Health of Gateway Members Practice Eligibility (see PCMH slide #15 for separate eligibility
Gateway to Practitioner Excellence (GPE) 2018 Medicaid Recognizing and Rewarding Excellent Practices Improving the Health of Gateway Members Practice Eligibility (see PCMH slide #15 for separate eligibility
Released: February 1, Comments Due: March 3, 2017
 AMCP Summary: Advance Notice of Methodological Changes for Calendar Year (CY) 2018 for Medicare Advantage (MA) Capitation Rates, Part C and Part D Payment Policies and 2018 Call Letter Released: February
AMCP Summary: Advance Notice of Methodological Changes for Calendar Year (CY) 2018 for Medicare Advantage (MA) Capitation Rates, Part C and Part D Payment Policies and 2018 Call Letter Released: February
2020 Medicare Advantage
 www.wakely.com 2020 Medicare Advantage Summary of Advance Rate Notice Part 2 February 7, 2019 page i Table of Contents Executive Summary... 1 Attachment I: Preliminary Estimates of the National Per Capita
www.wakely.com 2020 Medicare Advantage Summary of Advance Rate Notice Part 2 February 7, 2019 page i Table of Contents Executive Summary... 1 Attachment I: Preliminary Estimates of the National Per Capita
Standing strong for payers and patients
 Standing strong for payers and patients Dr. Steve Miller, SVP, Chief Medical Officer Ben Bier, VP Investor Relations W I L L I A M B L A I R 3 7 TH ANNUAL G ROWTH STOCK C ONFERENCE 6.14.17 1 Safe harbor
Standing strong for payers and patients Dr. Steve Miller, SVP, Chief Medical Officer Ben Bier, VP Investor Relations W I L L I A M B L A I R 3 7 TH ANNUAL G ROWTH STOCK C ONFERENCE 6.14.17 1 Safe harbor
Medicare Part D in 2018: The Latest on Enrollment, Premiums, and Cost Sharing
 May 2018 Data Brief Medicare Part D in 2018: The Latest on Enrollment, Premiums, and Cost Sharing Juliette Cubanski, Anthony Damico, and Tricia Neuman Summary This analysis presents findings on Medicare
May 2018 Data Brief Medicare Part D in 2018: The Latest on Enrollment, Premiums, and Cost Sharing Juliette Cubanski, Anthony Damico, and Tricia Neuman Summary This analysis presents findings on Medicare
Are You Optimizing Your Provider-Sponsored Medicare Advantage Plan?
 Are You Optimizing Your Provider-Sponsored Medicare Advantage Plan? April 2016 WRITTEN BY: TYRONNE JOLLY, RICH TREMBOWICZ The Medicare market is swelling as the nation s aging population continues to grow.
Are You Optimizing Your Provider-Sponsored Medicare Advantage Plan? April 2016 WRITTEN BY: TYRONNE JOLLY, RICH TREMBOWICZ The Medicare market is swelling as the nation s aging population continues to grow.
CureMD & Physician Quality Reporting Programs. Presented by Sara Irshad Consultant,
 CureMD & Physician Quality Reporting Programs Presented by Sara Irshad Consultant, www.curemd.com OPENING WORDS Quality is not an accident. It is always the result of an intelligent effort. AGENDA Overview
CureMD & Physician Quality Reporting Programs Presented by Sara Irshad Consultant, www.curemd.com OPENING WORDS Quality is not an accident. It is always the result of an intelligent effort. AGENDA Overview
Avalere Health 2015 Industry Outlook
 2015 Industry Outlook 2 Introduction Industry Outlook 2015 Changes in healthcare financing, delivery, and organization are transforming the sector. Health plans and providers are revising their business
2015 Industry Outlook 2 Introduction Industry Outlook 2015 Changes in healthcare financing, delivery, and organization are transforming the sector. Health plans and providers are revising their business
2018 Medicare Advantage and Part D Rate Announcement and Call Letter, and Request
 2018 Medicare Advantage and Part D Rate Announcement and Call Letter, and Request for Information Date 2017-04-03 Title 2018 Medicare Advantage and Part D Rate Announcement and Call Letter, and Request
2018 Medicare Advantage and Part D Rate Announcement and Call Letter, and Request for Information Date 2017-04-03 Title 2018 Medicare Advantage and Part D Rate Announcement and Call Letter, and Request
Assessing the Medicare Advantage Star Ratings
 July 2018 Healthcare Systems and Services Practice Assessing the Medicare Advantage Star Ratings Dan Jamieson, Monisha Machado-Pereira, Stephanie Carlton, and Cara Repasky 1 Assessing the Medicare Advantage
July 2018 Healthcare Systems and Services Practice Assessing the Medicare Advantage Star Ratings Dan Jamieson, Monisha Machado-Pereira, Stephanie Carlton, and Cara Repasky 1 Assessing the Medicare Advantage
9/23/2016. Our Services. Transitioning from Fee-for-Service to Value-based Reimbursement. Key Trends and Strategies for Rural Health Providers
 Transitioning from Fee-for-Service to Value-based Reimbursement Key Trends and Strategies for Rural Health Providers Paul MacLellan, CEO >> Health care consulting company >> Wholly owned subsidiary of
Transitioning from Fee-for-Service to Value-based Reimbursement Key Trends and Strategies for Rural Health Providers Paul MacLellan, CEO >> Health care consulting company >> Wholly owned subsidiary of
2008 Medicare Part D: Pharmacist's Survival Guide. Ronnie DePue, R.Ph., CGP
 2008 Medicare Part D: Pharmacist's Survival Guide Ronnie DePue, R.Ph., CGP Objectives At the completion of this program, the participant will be able to: 1. Give an overview of the Medicare Prescription
2008 Medicare Part D: Pharmacist's Survival Guide Ronnie DePue, R.Ph., CGP Objectives At the completion of this program, the participant will be able to: 1. Give an overview of the Medicare Prescription
Evidence Based Benefit Design: A Key Pillar of Value Based Purchasing
 Evidence Based Benefit Design: A Key Pillar of Value Based Purchasing Andrew Webber, President and CEO National Business Coalition on Health Center for Value Based Insurance Design University of Michigan,
Evidence Based Benefit Design: A Key Pillar of Value Based Purchasing Andrew Webber, President and CEO National Business Coalition on Health Center for Value Based Insurance Design University of Michigan,
Deep Dive Medicare Advantage Advance Notices Part I and II
 Deep Dive Medicare Advantage Advance Notices Part I and II Noah Champagne, FSA, MAAA Noah Champagne is a consulting actuary in Milliman s New York office. Noah has a breadth of Medicare experience working
Deep Dive Medicare Advantage Advance Notices Part I and II Noah Champagne, FSA, MAAA Noah Champagne is a consulting actuary in Milliman s New York office. Noah has a breadth of Medicare experience working
Health Plans Dashboard
 Health Plans Dashboard Q2 2015 Dashboard Summary Report A review of Inpatient, Outpatient and RX trends January 14, 2016 Prepared by HSS and Aon Hewitt Introduction This report completes the first phase
Health Plans Dashboard Q2 2015 Dashboard Summary Report A review of Inpatient, Outpatient and RX trends January 14, 2016 Prepared by HSS and Aon Hewitt Introduction This report completes the first phase
MEDICARE-MEDICAID CAPITATED FINANCIAL ALIGNMENT MODEL QUALITY WITHHOLD TECHNICAL NOTES (DY 2 5)
 MEDICARE-MEDICAID CAPITATED FINANCIAL ALIGNMENT MODEL QUALITY WITHHOLD TECHNICAL NOTES (DY 2 5) Effective as of January 1, 2015; Issued April 29, 2016; Updated XXXXX Introduction The Medicare-Medicaid
MEDICARE-MEDICAID CAPITATED FINANCIAL ALIGNMENT MODEL QUALITY WITHHOLD TECHNICAL NOTES (DY 2 5) Effective as of January 1, 2015; Issued April 29, 2016; Updated XXXXX Introduction The Medicare-Medicaid
Medicare payment policy and its impact on program spending
 Medicare payment policy and its impact on program spending James E. Mathews, Ph.D. Deputy Director, Medicare Payment Advisory Commission February 8, 2013 Outline of today s presentation Brief background
Medicare payment policy and its impact on program spending James E. Mathews, Ph.D. Deputy Director, Medicare Payment Advisory Commission February 8, 2013 Outline of today s presentation Brief background
SAVINGS GENERATED BY PHARMACY BENEFIT MANAGERS IN THE MEDICARE PART D PROGRAM
 February 6, 2014 GLENN GIESE KELLY BACKES SAVINGS GENERATED BY PHARMACY BENEFIT MANAGERS IN THE MEDICARE PART D PROGRAM June 26, 2017 GLENN GIESE RANDALL FITZPATRICK KEVIN MEYER CONTENTS Findings... 1
February 6, 2014 GLENN GIESE KELLY BACKES SAVINGS GENERATED BY PHARMACY BENEFIT MANAGERS IN THE MEDICARE PART D PROGRAM June 26, 2017 GLENN GIESE RANDALL FITZPATRICK KEVIN MEYER CONTENTS Findings... 1
2017 URAC SPECIALTY PHARMACY PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT
 2017 URAC SPECIALTY PHARMACY PERFORMANCE MEASUREMENT: December 2017 Table of Contents Executive Summary... 1 Specialty Pharmacy Organization Characteristics... 2 Data Validation Overview... 7 Results:
2017 URAC SPECIALTY PHARMACY PERFORMANCE MEASUREMENT: December 2017 Table of Contents Executive Summary... 1 Specialty Pharmacy Organization Characteristics... 2 Data Validation Overview... 7 Results:
Rocky Mountain Health Plans PPO
 Quality Overview Rocky Health Plans PPO Accreditation Exchange Product Accrediting Organization: NCQA PPO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange
Quality Overview Rocky Health Plans PPO Accreditation Exchange Product Accrediting Organization: NCQA PPO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating an exchange
SecurityBlue HMO. Link to Specific Guidance Regarding Exceptions and Appeals
 SecurityBlue HMO Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality
SecurityBlue HMO Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality
Coordinating Patient Assistance Programs with Medicare Part D: A Manufacturer s Perspective June 5, 2006
 Coordinating Patient Assistance Programs with Medicare Part D: A Manufacturer s Perspective June 5, 2006 Karissa A. Laur Director, Prescription Assistance Programs Background Over the past 28 years, AstraZeneca
Coordinating Patient Assistance Programs with Medicare Part D: A Manufacturer s Perspective June 5, 2006 Karissa A. Laur Director, Prescription Assistance Programs Background Over the past 28 years, AstraZeneca
PURPOSE OF THE POLICY STATEMENT OF THE POLICY PROCEDURES
 PURPOSE OF THE POLICY The purpose of this policy is to describe Health Alliance s process for transitions and ensure that continued drug coverage is provided to new and current Part D members. The transition
PURPOSE OF THE POLICY The purpose of this policy is to describe Health Alliance s process for transitions and ensure that continued drug coverage is provided to new and current Part D members. The transition
Final Policy, Payment, and Quality Provisions in the Medicare Physician Fee Schedule for Calendar Year 2018
 Final Policy, Payment, and Quality Provisions in the Medicare Physician Fee Schedule for Calendar Year 2018 Date 2017-11-02 Title Contact Final Policy, Payment, and Quality Provisions in the Medicare Physician
Final Policy, Payment, and Quality Provisions in the Medicare Physician Fee Schedule for Calendar Year 2018 Date 2017-11-02 Title Contact Final Policy, Payment, and Quality Provisions in the Medicare Physician
Centers for Medicare & Medicaid Services: Innovation Center New Direction Request For Information: Medicare Advantage (MA) Innovation Models
 Centers for Medicare & Medicaid Services: Innovation Center New Direction Request For Information: Medicare Advantage (MA) Innovation Models 1. Do you have any comments on the guiding principles or focus
Centers for Medicare & Medicaid Services: Innovation Center New Direction Request For Information: Medicare Advantage (MA) Innovation Models 1. Do you have any comments on the guiding principles or focus
CMS 1701 P UnityPoint Health. October 16, 2018
 CMS 1701 P UnityPoint Health 1776 West Lakes Parkway, Suite 400 West Des Moines, IA 50266 unitypoint.org October 16, 2018 Seema Verma, Administrator Centers for Medicare & Medicaid Services Department
CMS 1701 P UnityPoint Health 1776 West Lakes Parkway, Suite 400 West Des Moines, IA 50266 unitypoint.org October 16, 2018 Seema Verma, Administrator Centers for Medicare & Medicaid Services Department
Innovative Strategies for Managing the Rising Cost of Specialty Drugs
 Innovative Strategies for Managing the Rising Cost of Specialty Drugs Mid-sized Retirement and Healthcare Plan Management Conference Chicago, IL June 5, 2013 Managing the Rising Cost of Specialty Drugs
Innovative Strategies for Managing the Rising Cost of Specialty Drugs Mid-sized Retirement and Healthcare Plan Management Conference Chicago, IL June 5, 2013 Managing the Rising Cost of Specialty Drugs
VIA ELECTRONIC SUBMISSION. July 27, 2015
 VIA ELECTRONIC SUBMISSION Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-2390-P P. O. Box 8016 Baltimore, MD 21244-8016 Subject: Medicaid and Children s
VIA ELECTRONIC SUBMISSION Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-2390-P P. O. Box 8016 Baltimore, MD 21244-8016 Subject: Medicaid and Children s
BlueRx PDP. Link to Specific Guidance Regarding Exceptions and Appeals
 BlueRx PDP Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality Assurance
BlueRx PDP Conditions and Limitations Potential for Contract Termination Disenrollment Rights and Instructions Exceptions, Prior Authorization, Appeals and Grievances Out-of-Network Coverage Quality Assurance
Presentation to the IOM Committee on Core Metrics Tom Williams, Dr PH, President & CEO, IHA January 7, 2014, Irvine, California
 Presentation to the IOM Committee on Core Metrics Tom Williams, Dr PH, President & CEO, IHA January 7, 2014, Irvine, California Organization: California multi-sector healthcare leadership group Mission:
Presentation to the IOM Committee on Core Metrics Tom Williams, Dr PH, President & CEO, IHA January 7, 2014, Irvine, California Organization: California multi-sector healthcare leadership group Mission:
The Medicare Drug Benefit: Implications for Chronic Disease Care
 The Medicare Drug Benefit: Implications for Chronic Disease Care Introduction Most of California s 4.3 million Medicare beneficiaries will experience major changes in coverage for prescription medications
The Medicare Drug Benefit: Implications for Chronic Disease Care Introduction Most of California s 4.3 million Medicare beneficiaries will experience major changes in coverage for prescription medications
Formulary Access for Patients with Mental Health Conditions
 Formulary Access for Patients with Mental Health Conditions Background on Avalere s PlanScape and Methodology for Formulary Analysis PlanScape Methodology This analysis reviews formulary coverage in the
Formulary Access for Patients with Mental Health Conditions Background on Avalere s PlanScape and Methodology for Formulary Analysis PlanScape Methodology This analysis reviews formulary coverage in the
Supporting Appropriate Payer Coverage Decisions
 Supporting Appropriate Payer Coverage Decisions Providing Services for Janssen Pharmaceutical Companies of Johnson & Johnson Table of Contents Introduction 3 This document is presented for informational
Supporting Appropriate Payer Coverage Decisions Providing Services for Janssen Pharmaceutical Companies of Johnson & Johnson Table of Contents Introduction 3 This document is presented for informational
Summary of CY2019 Proposed Medicare Advantage and Part D Policy & Technical Changes
 Summary of CY2019 Proposed Medicare Advantage and Part D Policy & Technical Changes Overview Prepared by Wakely Consulting Group The Centers for Medicare and Medicaid Services ( CMS ) recently released
Summary of CY2019 Proposed Medicare Advantage and Part D Policy & Technical Changes Overview Prepared by Wakely Consulting Group The Centers for Medicare and Medicaid Services ( CMS ) recently released
Specialty Pharmacy: A Key to Organizational Success in Population Health Management
 Specialty Pharmacy: A Key to Organizational Success in Population Health Management Scott Knoer, MS, PharmD, FASHP Chief Pharmacy Officer, Cleveland Clinic Steve Rough, MS, RPh, FASHP Director of Pharmacy,
Specialty Pharmacy: A Key to Organizational Success in Population Health Management Scott Knoer, MS, PharmD, FASHP Chief Pharmacy Officer, Cleveland Clinic Steve Rough, MS, RPh, FASHP Director of Pharmacy,
June 18, RE: Comments on General Guidance on Federally Facilitated Exchanges. Dear Mr. Larsen:
 June 18, 2012 Steve Larsen Deputy Administrator and Director Center for Consumer Information and Insurance Oversight Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services
June 18, 2012 Steve Larsen Deputy Administrator and Director Center for Consumer Information and Insurance Oversight Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services
Elevate by Denver Health Medical Plan
 Quality Overview Elevate by Denver Health Medical Plan Accreditation Exchange Product Accrediting Organization: NCQA HMO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating
Quality Overview Elevate by Denver Health Medical Plan Accreditation Exchange Product Accrediting Organization: NCQA HMO (Exchange) Accreditation Status: Accredited Note: Accredited is the highest rating
How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments?
 How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments? 1:10 PM 2:10 PM Steering Toward Success: Achieving Value in Whole Person Care September 25 and
How are the State, Managed Medicaid Organizations and Providers Preparing for Medicaid Value-Based Payments? 1:10 PM 2:10 PM Steering Toward Success: Achieving Value in Whole Person Care September 25 and
