$0 per covered individual up to $0 per family. What is the overall deductible?
|
|
|
- Bertram Martin
- 6 years ago
- Views:
Transcription
1 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 This is only a summary. Please read the FEHB Plan brochure (RI ) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth in the FEHB Plan brochure. Benefits may vary if you have other coverage, such as Medicare. You can get the FEHB Plan brochure at kp.org/feds or by calling Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? What is not included in the out of pocket limit? Is there an overall annual limit on what the plan pays? Does this plan use a network of providers? Do I need a referral to see a specialist? Are there services this plan doesn t cover? $0 per covered individual up to $0 per family No $3,500 per covered individual up to $7,000 per family Premiums, balance-billed charges and health care this plan doesn t cover. No Yes, see kp.org/feds or call for a list of plan providers. Yes Yes See the chart starting on page 2 for your costs for services this plan covers. You don t have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers. The out-of-pocket limit, or catastrophic maximum, is the most you could pay during the year for your share of the cost of covered services. This limit helps you plan for health care expenses. The per covered individual amount is the most that any one member would have to pay, regardless of whether the individual is enrolled in Self Plus One or Self and Family. Even though you pay these expenses, they don t count toward the out-of-pocket limit. The chart starting on page 2 describes any limits on what the plan will pay for specific covered services, such as office visits. If you use an in-network doctor or other health care provider, this plan will pay some or all of the costs of covered services. Be aware, your in-network doctor or hospital may use an out-of-network provider for some services. We use the term Plan for providers in our network. See the chart starting on page 2 for how this plan pays different kinds of providers. This plan will pay some or all of the costs to see a specialist for covered services but only if you have the plan's permission before you see the specialist. Some of the services this plan doesn t cover are listed on page 5. See this plan s FEHB brochure for additional information about excluded services. 1 of 8 You can view the Glossary at kp.org/feds or call to request a copy
2 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 Copayments are fixed dollar amounts (for example, $15) you pay for covered health care, usually when you receive the service. Coinsurance is your share of the costs of a covered service, calculated as a percent of the allowed amount for the service. For example, if the plan s allowed amount for an overnight hospital stay is $1,000, your coinsurance payment of 20% would be $200. This may change if you haven t met your deductible. The amount the plan pays for covered services is based on the allowed amount. If an out-of-network provider charges more than the allowed amount, you may have to pay the difference. For example, if an out-of-network hospital charges $1,500 for an overnight stay and the allowed amount is $1,000, you may have to pay the $500 difference. (This is called balance billing.) This plan may encourage you to use participating providers by charging you lower deductibles, copayments and coinsurance amounts. Common Medical Event If you visit a health care provider s office or clinic If you have a test Services You May Need Primary care visit to treat an injury or illness Your Cost If You Use a Plan Provider $15 per visit (No charge for children through age 17) Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Specialist visit $30 per visit Other practitioner office visit Preventive care/screening/immunization Diagnostic test (x-ray, blood work) Imaging (CT/PET scans, MRIs) $30 per visit for self referred chiropractor No charge No charge in office setting; $150 per visit in an outpatient setting $30 per visit in an office setting; $150 per visit in outpatient hospital Limitations & Exceptions Up to 20 chiropractic visits per calendar year 2 of 8 You can view the Glossary at kp.org/feds or call to request a copy
3 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 Common Medical Event If you need drugs to treat your illness or condition More information about prescription drug coverage is available at kp.org/formulary If you have outpatient surgery If you need immediate medical attention Services You May Need Generic drugs Preferred Brand drugs Non-Preferred Brand drugs Your Cost If You Use a Plan Provider $10 copayment (retail) KP pharmacy; $20 copayment (retail) Network pharmacy; $20 copayment (mail order) $40 copayment (retail) KP pharmacy; $50 copayment (retail) Network pharmacy; $80 copayment (mail order) $40 copayment (retail) KP pharmacy; $50 copayment (retail) Network pharmacy; $80 copayment (mail order) Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Specialty drugs 20% up to $100 Facility fee (e.g., ambulatory surgery center) $150 per visit Physician/surgeon fees No charge Emergency room services $150 per visit $150 per visit Emergency medical transportation $100 per trip $100 per trip Urgent care $30 per visit $30 per visit Limitations & Exceptions Up to 30-day supply (retail); day supply (mail order) Up to 30-day supply (retail); day supply (mail order) Up to 30-day supply (retail); day supply (mail order) Requires approved formulary exception. Up to 30-day supply (retail); day supply (mail order) Non-Plan providers covered when outside a Kaiser Permanente service area 3 of 8 You can view the Glossary at kp.org/feds or call to request a copy
4 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 Common Medical Event If you have a hospital stay If you have mental health, behavioral health, or substance abuse needs If you are pregnant If you need help recovering or have other special health needs Services You May Need Facility fee (e.g., hospital room) Your Cost If You Use a Plan Provider $250 per day up to $750 per admission Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Physician/surgeon fee No charge Limitations & Exceptions Mental/Behavioral health $15 per visit outpatient services $7 per group visit Mental/Behavioral health $250 per day up to $750 per inpatient services admission Substance use disorder $15 per visit outpatient services $7 per group visit Substance use disorder inpatient $250 per day up to $750 per services admission Prenatal and postnatal care No charge After the confirmation of pregnancy Delivery and all inpatient services $250 per day up to $750 Home health care No charge Rehabilitation services Habilitation services $30 per visit (outpatient); $250 per day up to $750 per admission (inpatient) $30 per visit (outpatient); $250 per day up to $750 per admission (inpatient) Outpatient services: Up to 20 visits per condition per calendar year Outpatient services: Up to 20 visits per condition per calendar year Skilled nursing care No charge Limited to 100 days per calendar year Durable medical equipment 20% coinsurance Hospice service No charge Eye exam $30 per visit 4 of 8 You can view the Glossary at kp.org/feds or call to request a copy
5 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 Common Medical Event If your child needs dental or eye care Services You May Need Your Cost If You Use a Plan Provider Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Limitations & Exceptions Glasses Eye glasses are not covered Dental check-up 30% coinsurance Excluded Services & Other Covered Services: Services Your Plan Does NOT Cover (This isn t a complete list. Check this plan s FEHB brochure for other excluded services.) Acupuncture Cosmetic surgery Eye glasses Long-term care Private-duty nursing Weight loss programs Other Covered Services (This isn t a complete list. Check this plan's FEHB brochure for other covered services and your costs for these services.) Bariatric surgery Chiropractic care Dental care (Adult) Hearing aids (Child) Infertility treatment Non-emergency care when traveling outside the U.S. Routine eye care (Adult) Routine foot care Your Rights to Continue Coverage: If you lose coverage under the plan, then, depending on the circumstances, you may be eligible for a 31-day free extension of coverage, to convert to an individual policy, and to receive temporary continuation of coverage (TCC). Your TCC rights will be limited in duration and will require you to pay a premium, which may be significantly higher than the premium you pay while covered under the plan. An individual policy may also provide different benefits than you had while covered under the plan. Other limitations on your rights to continue coverage may also apply. For more information on your rights to continue coverage, see the FEHB Plan brochure, contact your HR office/retirement system, contact your plan at or visit Your Appeal Rights: If you are dissatisfied with a denial of coverage for claims under your plan, you may be able to appeal. For information about your appeal rights please see Section 3, How you get care, and Section 8 The disputed claims process, in your plan's FEHB brochure. If you need assistance, you can contact: Member Services at , Monday through Friday, 7:00 AM to 7:00 PM. If you are enrolled through a plan that is subject to the Employee Retirement Income Security Act (ERISA), you may file a civil action under section 502(a) of the federal ERISA statute. To understand these rights, you should check with your 5 of 8 You can view the Glossary at kp.org/feds or call to request a copy
6 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 benefits office or contact the Employee Benefits Security Administration (part of the U.S. Department of Labor) at EBSA (3272) or Additionally, a consumer assistance program can help you file your appeal. You may contact the State Department of Insurance at: Georgia Office of Insurance and Safety Fire Commissioner Consumer Services Division 2 Martin Luther King, Jr. Drive West Tower, Suite 716 Atlanta, Georgia Does this Coverage Provide Minimum Essential Coverage? The Affordable Care Act requires most people to have health care coverage that qualifies as minimum essential coverage. Coverage under this plan qualifies as minimum essential coverage. Does this Coverage Meet the Minimum Value Standard? The Affordable Care Act establishes a minimum value standard of benefits of a health plan. The minimum value standard is 60% (actuarial value). The health coverage of this plan does meet the minimum value standard for the benefits the plan provides. Language Access Services: Spanish (Español): Para obtener asistencia en Español, llame al Tagalog (Tagalog): Kung kailangan ninyo ang tulong sa Tagalog tumawag sa Chinese ( 中文 ): 如果需要中文的帮助, 请拨打这个号码 Navajo (Dine): Dinek'ehgo shika at'ohwol ninisingo, kwiijigo holne' To see examples of how this plan might cover costs for a sample medical situation, see the next page. 6 of 8 You can view the Glossary at kp.org/feds or call to request a copy
7 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 About these Coverage Examples: These examples show how this plan might cover medical care in given situations. Use these examples to see, in general, how much financial protection a sample patient might get if they are covered under different plans. This is not a cost estimator. Don t use these examples to estimate your actual costs under this plan. The actual care you receive will be different from these examples, and the cost of that care will also be different. See the next page for important information about these examples. Having a baby (normal delivery) Amount owed to providers: $7,540 Plan pays $7,040 Patient pays $500 Sample care costs: Hospital charges (mother) $2,700 Routine obstetric care $2,100 Hospital charges (baby) $900 Anesthesia $900 Laboratory tests $500 Prescriptions $200 Radiology $200 Vaccines, other preventive $40 Total $7,540 Patient pays: Deductibles $0 Copays $300 Coinsurance $0 Limits or exclusions $200 Total $500 Managing type 2 diabetes (routine maintenance of a well-controlled condition) Amount owed to providers: $5,400 Plan pays $4,520 Patient pays $880 Sample care costs: Prescriptions $2,900 Medical Equipment and Supplies $1,300 Office Visits and Procedures $700 Education $300 Laboratory tests $100 Vaccines, other preventive $100 Total $5,400 Patient pays: Deductibles $0 Copays $800 Coinsurance $0 Limits or exclusions $80 Total $880 7 of 8 You can view the Glossary at kp.org/feds or call to request a copy
8 Kaiser Foundation Health Plan of Georgia, Inc.: High Option Coverage Period: 1/01/ /31/2016 Questions and answers about the Coverage Examples: What are some of the assumptions behind the Coverage Examples? Costs don t include premiums. Sample care costs are based on national averages supplied by the U.S. Department of Health and Human Services, and aren t specific to a particular geographic area or health plan. The patient s condition was not an excluded or preexisting condition. All services and treatments started and ended in the same coverage period. There are no other medical expenses for any member covered under this plan. Out-of-pocket expenses are based only on treating the condition in the example. The patient received all care from innetwork providers. If the patient had received care from out-of-network providers, costs would have been higher. What does a Coverage Example show? For each treatment situation, the Coverage Example helps you see how deductibles, copayments, and coinsurance can add up. It also helps you see what expenses might be left up to you to pay because the service or treatment isn t covered or payment is limited. Does the Coverage Example predict my own care needs? No. Treatments shown are just examples. The care you would receive for this condition could be different based on your doctor s advice, your age, how serious your condition is, and many other factors. Does the Coverage Example predict my future expenses? No. Coverage Examples are not cost estimators. You can t use the examples to estimate costs for an actual condition. They are for comparative purposes only. Your own costs will be different depending on the care you receive, the prices your providers charge, and the reimbursement your health plan allows. Can I use Coverage Examples to compare plans? Yes. When you look at the Summary of Benefits and Coverage for other plans, you ll find the same Coverage Examples. When you compare plans, check the Patient Pays box in each example. The smaller that number, the more coverage the plan provides. Are there other costs I should consider when comparing plans? Yes. An important cost is the premium you pay. Generally, the lower your premium, the more you ll pay in out-ofpocket costs, such as copayments, deductibles, and coinsurance. You should also consider contributions to accounts such as health savings accounts (HSAs), flexible spending arrangements (FSAs) or health reimbursement accounts (HRAs) that help you pay out-of-pocket expenses. 8 of 8 You can view the Glossary at kp.org/feds or call to request a copy
9 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 This is only a summary. Please read the FEHB Plan brochure (RI ) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth in the FEHB Plan brochure. Benefits may vary if you have other coverage, such as Medicare. You can get the FEHB Plan brochure at kp.org/feds or by calling Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? What is not included in the out of pocket limit? Is there an overall annual limit on what the plan pays? Does this plan use a network of providers? Do I need a referral to see a specialist? Are there services this plan doesn t cover? $250 per covered individual up to $500 per family No $3,500 per covered individual up to $7,000 per family Premiums, balancebilled charges and health care this plan doesn t cover. No Yes, see kp.org/feds or call for a list of plan providers. Yes Yes You must pay all the costs up to the deductible amount before this plan begins to pay for certain covered services you use. Copayments and coinsurance amounts do not count toward your deductible, which generally starts over January 1st. When a covered service or supply is subject to a deductible, only the Plan allowance for the service or supply counts toward the deductible. See the chart starting on page 2 for how much you pay for covered services after you meet the deductible and for which services are subject to the deductible. You don t have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers. The out-of-pocket limit, or catastrophic maximum, is the most you could pay during the year for your share of the cost of covered services. This limit helps you plan for health care expenses. The per covered individual amount is the most that any one member would have to pay, regardless of whether the individual is enrolled in Self Plus One or Self and Family. Even though you pay these expenses, they don t count toward the out-of-pocket limit. The chart starting on page 2 describes any limits on what the plan will pay for specific covered services, such as office visits. If you use an in-network doctor or other health care provider, this plan will pay some or all of the costs of covered services. Be aware, your in-network doctor or hospital may use an out-ofnetwork provider for some services. We use the term Plan for providers in our network. See the chart starting on page 2 for how this plan pays different kinds of providers. This plan will pay some or all of the costs to see a specialist for covered services but only if you have the plan's permission before you see the specialist. Some of the services this plan doesn t cover are listed on page 5. See this plan s FEHB brochure for additional information about excluded services. 1 of 9 You can view the Glossary at kp.org/feds or call to request a copy
10 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 Copayments are fixed dollar amounts (for example, $15) you pay for covered health care, usually when you receive the service. Coinsurance is your share of the costs of a covered service, calculated as a percent of the allowed amount for the service. For example, if the plan s allowed amount for an overnight hospital stay is $1,000, your coinsurance payment of 20% would be $200. This may change if you haven t met your deductible. The amount the plan pays for covered services is based on the allowed amount. If an out-of-network provider charges more than the allowed amount, you may have to pay the difference. For example, if an out-of-network hospital charges $1,500 for an overnight stay and the allowed amount is $1,000, you may have to pay the $500 difference. (This is called balance billing.) This plan may encourage you to use participating providers by charging you lower deductibles, copayments and coinsurance amounts. Common Medical Event If you visit a health care provider s office or clinic If you have a test Services You May Need Your Cost If You Use a Plan Provider Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Primary care visit to treat an $20 per visit (No charge for children injury or illness through age 17) Specialist visit $35 per visit Other practitioner office visit $35 per visit for self-referred chiropractor Preventive care/screening/ immunization Diagnostic test (x-ray, blood work) Imaging (CT/PET scans, MRIs) No charge No charge in an office setting; 20% after deductible in an outpatient setting Limitations & Exceptions Up to 20 chiropractic visits per calendar year 20% coinsurance after deductible 2 of 9 You can view the Glossary at kp.org/feds or call to request a copy
11 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 Common Medical Event If you need drugs to treat your illness or condition More information about prescription drug coverage is available at kp.org/formulary Services You May Need Generic drugs Preferred Brand drugs Non-Preferred Brand drugs Your Cost If You Use a Plan Provider $15 copayment (retail) KP pharmacy; $25 copayment (retail) Network pharmacy; $30 copayment (mail order) $40 copayment (retail) KP pharmacy; $50 copayment (retail) Network pharmacy; $80 copayment (mail order) $50 copayment (retail) KP pharmacy; $60 copayment (retail) Network pharmacy; $100 copayment (mail order) Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Specialty drugs 30% up to $150 Limitations & Exceptions Up to 30-day supply (retail); day supply (mail order) Up to 30-day supply (retail); day supply (mail order) Up to 30-day supply (retail); day supply (mail order). Requires approved formulary exception. Up to 30-day supply (retail); day supply (mail order) If you have outpatient surgery If you need immediate medical attention If you have a hospital stay Facility fee (e.g., ambulatory surgery center) 20% coinsurance after deductible Physician/surgeon fees 20% coinsurance after deductible Emergency room services $175 per visit $175 per visit Emergency medical transportation $125 per trip $125 per trip Urgent care $40 per visit $40 per visit Facility fee (e.g., hospital room) $250 per day up to $1,000 per admission Physician/surgeon fee 20% coinsurance after deductible Non-Plan providers covered when outside a Kaiser Permanente service area 3 of 9 You can view the Glossary at kp.org/feds or call to request a copy
12 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 Common Medical Event If you have mental health, behavioral health, or substance abuse needs If you are pregnant Services You May Need Mental/Behavioral health outpatient services Mental/Behavioral health inpatient services Substance use disorder outpatient services Substance use disorder inpatient services Your Cost If You Use a Plan Provider $20 per visit $10 per group visit $250 per day up to $1,000 per admission, and 20% coinsurance after deductible for physician charges $20 per visit $10 per group visit $250 per day up to $1,000 per admission, and 20% coinsurance after deductible for physician charges Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Prenatal and postnatal care No charge Delivery and all inpatient services $250 per day up to $1,000 per admission, and 20% coinsurance after deductible for physician charges Limitations & Exceptions After the confirmation of pregnancy 4 of 9 You can view the Glossary at kp.org/feds or call to request a copy
13 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 Common Medical Event If you need help recovering or have other special health needs If your child needs dental or eye care Services You May Need Your Cost If You Use a Plan Provider Home health care No charge Rehabilitation services Habilitation services $35 per visit (outpatient); $250 per day up to $1,000 per admission, and 20% coinsurance after deductible for physician charges (inpatient) $35 per visit (outpatient); $250 per day up to $1,000 per admission, and 20% coinsurance after deductible for physician charges (inpatient) Your Cost If You Use a Non- Plan Provider (plus you may be balance billed) Skilled nursing care No charge Durable medical equipment 20% coinsurance after deductible Hospice service No charge Eye exam $35 per visit Limitations & Exceptions Outpatient services: Up to 20 visits per condition per calendar year. Outpatient services: Up to 20 visits per condition per calendar year. Limited to 100 days per calendar year Glasses Eye glasses are not covered Dental check-up 30% coinsurance Excluded Services & Other Covered Services: Services Your Plan Does NOT Cover (This isn t a complete list. Check this plan s FEHB brochure for other excluded services.) Acupuncture Cosmetic surgery Eye glasses Long-term care Private-duty nursing Weight loss programs 5 of 9 You can view the Glossary at kp.org/feds or call to request a copy
14 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 Other Covered Services (This isn t a complete list. Check this plan's FEHB brochure for other covered services and your costs for these services.) Bariatric surgery Dental care (Adult) Hearing aids (Child) Infertility treatment Non-emergency care when traveling outside the U.S. Routine foot care Routine eye care (Adult) Your Rights to Continue Coverage: If you lose coverage under the plan, then, depending on the circumstances, you may be eligible for a 31-day free extension of coverage, to convert to an individual policy, and to receive temporary continuation of coverage (TCC). Your TCC rights will be limited in duration and will require you to pay a premium, which may be significantly higher than the premium you pay while covered under the plan. An individual policy may also provide different benefits than you had while covered under the plan. Other limitations on your rights to continue coverage may also apply. For more information on your rights to continue coverage, see the FEHB Plan brochure, contact your HR office/retirement system, contact your plan at or visit Your Appeal Rights: If you are dissatisfied with a denial of coverage for claims under your plan, you may be able to appeal. For information about your appeal rights please see Section 3, How you get care, and Section 8 The disputed claims process, in your plan's FEHB brochure. If you need assistance, you can contact: Member Services at , Monday through Friday, 7:00 AM to 7:00 PM. If you are enrolled through a plan that is subject to the Employee Retirement Income Security Act (ERISA), you may file a civil action under section 502(a) of the federal ERISA statute. To understand these rights, you should check with your benefits office or contact the Employee Benefits Security Administration (part of the U.S. Department of Labor) at EBSA (3272) or Additionally, a consumer assistance program can help you file your appeal. You may contact the State Department of Insurance at: Georgia Office of Insurance and Safety Fire Commissioner Consumer Services Division 2 Martin Luther King, Jr. Drive West Tower, Suite 716 Atlanta, Georgia of 9 You can view the Glossary at kp.org/feds or call to request a copy
15 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 Does this Coverage Provide Minimum Essential Coverage? The Affordable Care Act requires most people to have health care coverage that qualifies as minimum essential coverage. Coverage under this plan qualifies as minimum essential coverage. Does this Coverage Meet the Minimum Value Standard? The Affordable Care Act establishes a minimum value standard of benefits of a health plan. The minimum value standard is 60% (actuarial value). The health coverage of this plan does meet the minimum value standard for the benefits the plan provides. Language Access Services: Spanish (Español): Para obtener asistencia en Español, llame al Tagalog (Tagalog): Kung kailangan ninyo ang tulong sa Tagalog tumawag sa Chinese ( 中文 ): 如果需要中文的帮助, 请拨打这个号码 Navajo (Dine): Dinek'ehgo shika at'ohwol ninisingo, kwiijigo holne' To see examples of how this plan might cover costs for a sample medical situation, see the next page. 7 of 9 You can view the Glossary at kp.org/feds or call to request a copy
16 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 About these Coverage Examples: These examples show how this plan might cover medical care in given situations. Use these examples to see, in general, how much financial protection a sample patient might get if they are covered under different plans. This is not a cost estimator. Don t use these examples to estimate your actual costs under this plan. The actual care you receive will be different from these examples, and the cost of that care will also be different. See the next page for important information about these examples. Having a baby (normal delivery) Amount owed to providers: $7,540 Plan pays $6,540 Patient pays $1,000 Sample care costs: Hospital charges (mother) $2,700 Routine obstetric care $2,100 Hospital charges (baby) $900 Anesthesia $900 Laboratory tests $500 Prescriptions $200 Radiology $200 Vaccines, other preventive $40 Total $7,540 Patient pays: Deductibles $300 Copays $300 Coinsurance $200 Limits or exclusions $200 Total $1,000 Managing type 2 diabetes (routine maintenance of a well-controlled condition) Amount owed to providers: $5,400 Plan pays $ 4,220 Patient pays $ 1,180 Sample care costs: Prescriptions $2,900 Medical Equipment and Supplies $1,300 Office Visits and Procedures $700 Education $300 Laboratory tests $100 Vaccines, other preventive $100 Total $5,400 Patient pays: Deductibles $0 Copays $1,100 Coinsurance $0 Limits or exclusions $80 Total $1,180 8 of 9 You can view the Glossary at kp.org/feds or call to request a copy
17 Kaiser Foundation Health Plan of Georgia, Inc.: Standard Option Coverage Period: 1/01/ /31/2016 Questions and answers about the Coverage Examples: What are some of the assumptions behind the Coverage Examples? Costs don t include premiums. Sample care costs are based on national averages supplied by the U.S. Department of Health and Human Services, and aren t specific to a particular geographic area or health plan. The patient s condition was not an excluded or preexisting condition. All services and treatments started and ended in the same coverage period. There are no other medical expenses for any member covered under this plan. Out-of-pocket expenses are based only on treating the condition in the example. The patient received all care from innetwork providers. If the patient had received care from out-of-network providers, costs would have been higher. What does a Coverage Example show? For each treatment situation, the Coverage Example helps you see how deductibles, copayments, and coinsurance can add up. It also helps you see what expenses might be left up to you to pay because the service or treatment isn t covered or payment is limited. Does the Coverage Example predict my own care needs? No. Treatments shown are just examples. The care you would receive for this condition could be different based on your doctor s advice, your age, how serious your condition is, and many other factors. Does the Coverage Example predict my future expenses? No. Coverage Examples are not cost estimators. You can t use the examples to estimate costs for an actual condition. They are for comparative purposes only. Your own costs will be different depending on the care you receive, the prices your providers charge, and the reimbursement your health plan allows. Can I use Coverage Examples to compare plans? Yes. When you look at the Summary of Benefits and Coverage for other plans, you ll find the same Coverage Examples. When you compare plans, check the Patient Pays box in each example. The smaller that number, the more coverage the plan provides. Are there other costs I should consider when comparing plans? Yes. An important cost is the premium you pay. Generally, the lower your premium, the more you ll pay in out-ofpocket costs, such as copayments, deductibles, and coinsurance. You should also consider contributions to accounts such as health savings accounts (HSAs), flexible spending arrangements (FSAs) or health reimbursement accounts (HRAs) that help you pay out-of-pocket expenses. 9 of 9 You can view the Glossary at kp.org/feds or call to request a copy
18 Glossary of Health Coverage and Medical Terms This glossary has many commonly used terms, but isn t a full list. These glossary terms and definitions are intended to be educational and may be different from the terms and definitions in your plan. Some of these terms also might not have exactly the same meaning when used in your policy or plan, and in any such case, the policy or plan governs. (See your for information on how to get a copy of your policy or plan document.) Bold blue text indicates a term defined in this Glossary. See page 4 for an example showing how deductibles, co-insurance and out-of-pocket limits work together in a real life situation. Allowed Amount Maximum amount on which payment is based for covered health care services. This may be called eligible expense, payment allowance" or "negotiated rate." If your provider charges more than the allowed amount, you may have to pay the difference. (See Balance Billing.) Appeal A request for your health insurer or plan to review a decision or a grievance again. Balance Billing When a provider bills you for the difference between the provider s charge and the allowed amount. For example, if the provider s charge is $100 and the allowed amount is $70, the provider may bill you for the remaining $30. A preferred provider may not balance bill you for covered services. Co-insurance Your share of the costs of a covered health care service, calculated as a percent (for example, 20%) of the allowed amount for the service. Jane pays Her plan pays You pay co-insurance 20% 80% plus any deductibles (See page 4 for a detailed example.) you owe. For example, if the health insurance or plan s allowed amount for an office visit is $100 and you ve met your deductible, your co-insurance payment of 20% would be $20. The health insurance or plan pays the rest of the allowed amount. Co-payment A fixed amount (for example, $15) you pay for a covered health care service, usually when you receive the service. The amount can vary by the type of covered health care service. Deductible The amount you owe for health care services your health insurance or plan covers before your health insurance or plan begins to pay. For example, if your deductible is $1000, your plan won t pay anything until you ve met Jane pays 100% Her plan pays 0% (See page 4 for a detailed example.) your $1000 deductible for covered health care services subject to the deductible. The deductible may not apply to all services. Durable Medical Equipment (DME) Equipment and supplies ordered by a health care provider for everyday or extended use. Coverage for DME may include: oxygen equipment, wheelchairs, crutches or blood testing strips for diabetics. Emergency Medical Condition An illness, injury, symptom or condition so serious that a reasonable person would seek care right away to avoid severe harm. Emergency Medical Transportation Ambulance services for an emergency medical condition. Complications of Pregnancy Conditions due to pregnancy, labor and delivery that require medical care to prevent serious harm to the health of the mother or the fetus. Morning sickness and a nonemergency caesarean section aren t complications of pregnancy. Emergency Room Care Emergency services you get in an emergency room. Emergency Services Evaluation of an emergency medical condition and treatment to keep the condition from getting worse. OMB Control Numbers , , and Glossary of Health Coverage and Medical Terms Page 1 of 4
19 Excluded Services Health care services that your health insurance or plan doesn t pay for or cover. Grievance A complaint that you communicate to your health insurer or plan. Habilitation Services Health care services that help a person keep, learn or improve skills and functioning for daily living. Examples include therapy for a child who isn t walking or talking at the expected age. These services may include physical and occupational therapy, speech-language pathology and other services for people with disabilities in a variety of inpatient and/or outpatient settings. Health Insurance A contract that requires your health insurer to pay some or all of your health care costs in exchange for a premium. Home Health Care Health care services a person receives at home. Hospice Services Services to provide comfort and support for persons in the last stages of a terminal illness and their families. Hospitalization Care in a hospital that requires admission as an inpatient and usually requires an overnight stay. An overnight stay for observation could be outpatient care. Hospital Outpatient Care Care in a hospital that usually doesn t require an overnight stay. In-network Co-insurance The percent (for example, 20%) you pay of the allowed amount for covered health care services to providers who contract with your health insurance or plan. In-network co-insurance usually costs you less than out-of-network co-insurance. In-network Co-payment A fixed amount (for example, $15) you pay for covered health care services to providers who contract with your health insurance or plan. In-network co-payments usually are less than out-of-network co-payments. Medically Necessary Health care services or supplies needed to prevent, diagnose or treat an illness, injury, condition, disease or its symptoms and that meet accepted standards of medicine. Network The facilities, providers and suppliers your health insurer or plan has contracted with to provide health care services. Non-Preferred Provider A provider who doesn t have a contract with your health insurer or plan to provide services to you. You ll pay more to see a non-preferred provider. Check your policy to see if you can go to all providers who have contracted with your health insurance or plan, or if your health insurance or plan has a tiered network and you must pay extra to see some providers. Out-of-network Co-insurance The percent (for example, 40%) you pay of the allowed amount for covered health care services to providers who do not contract with your health insurance or plan. Outof-network co-insurance usually costs you more than innetwork co-insurance. Out-of-network Co-payment A fixed amount (for example, $30) you pay for covered health care services from providers who do not contract with your health insurance or plan. Out-of-network copayments usually are more than in-network co-payments. Out-of-Pocket Limit The most you pay during a policy period (usually a year) before your health insurance or plan begins to pay 100% of the allowed amount. This limit never Jane pays Her plan pays includes your premium, 0% 100% balance-billed charges or (See page 4 for a detailed example.) health care your health insurance or plan doesn t cover. Some health insurance or plans don t count all of your co-payments, deductibles, co-insurance payments, out-of-network payments or other expenses toward this limit. Physician Services Health care services a licensed medical physician (M.D. Medical Doctor or D.O. Doctor of Osteopathic Medicine) provides or coordinates. Glossary of Health Coverage and Medical Terms Page 2 of 4
20 Plan A benefit your employer, union or other group sponsor provides to you to pay for your health care services. Preauthorization A decision by your health insurer or plan that a health care service, treatment plan, prescription drug or durable medical equipment is medically necessary. Sometimes called prior authorization, prior approval or precertification. Your health insurance or plan may require preauthorization for certain services before you receive them, except in an emergency. Preauthorization isn t a promise your health insurance or plan will cover the cost. Preferred Provider A provider who has a contract with your health insurer or plan to provide services to you at a discount. Check your policy to see if you can see all preferred providers or if your health insurance or plan has a tiered network and you must pay extra to see some providers. Your health insurance or plan may have preferred providers who are also participating providers. Participating providers also contract with your health insurer or plan, but the discount may not be as great, and you may have to pay more. Premium The amount that must be paid for your health insurance or plan. You and/or your employer usually pay it monthly, quarterly or yearly. Prescription Drug Coverage Health insurance or plan that helps pay for prescription drugs and medications. Prescription Drugs Drugs and medications that by law require a prescription. Primary Care Physician A physician (M.D. Medical Doctor or D.O. Doctor of Osteopathic Medicine) who directly provides or coordinates a range of health care services for a patient. Provider A physician (M.D. Medical Doctor or D.O. Doctor of Osteopathic Medicine), health care professional or health care facility licensed, certified or accredited as required by state law. Reconstructive Surgery Surgery and follow-up treatment needed to correct or improve a part of the body because of birth defects, accidents, injuries or medical conditions. Rehabilitation Services Health care services that help a person keep, get back or improve skills and functioning for daily living that have been lost or impaired because a person was sick, hurt or disabled. These services may include physical and occupational therapy, speech-language pathology and psychiatric rehabilitation services in a variety of inpatient and/or outpatient settings. Skilled Nursing Care Services from licensed nurses in your own home or in a nursing home. Skilled care services are from technicians and therapists in your own home or in a nursing home. Specialist A physician specialist focuses on a specific area of medicine or a group of patients to diagnose, manage, prevent or treat certain types of symptoms and conditions. A non-physician specialist is a provider who has more training in a specific area of health care. UCR (Usual, Customary and Reasonable) The amount paid for a medical service in a geographic area based on what providers in the area usually charge for the same or similar medical service. The UCR amount sometimes is used to determine the allowed amount. Urgent Care Care for an illness, injury or condition serious enough that a reasonable person would seek care right away, but not so severe as to require emergency room care. Primary Care Provider A physician (M.D. Medical Doctor or D.O. Doctor of Osteopathic Medicine), nurse practitioner, clinical nurse specialist or physician assistant, as allowed under state law, who provides, coordinates or helps a patient access a range of health care services. Glossary of Health Coverage and Medical Terms Page 3 of 4
21 How You and Your Insurer Share Costs - Example Jane s Plan Deductible: $1,500 Co-insurance: 20% Out-of-Pocket Limit: $5,000 January 1 st Beginning of Coverage Period December 31 st End of Coverage Period Jane pays 100% Her plan pays 0% more costs Jane pays 20% Her plan pays 80% more costs Jane pays 0% Her plan pays 100% Jane hasn t reached her $1,500 deductible yet Her plan doesn t pay any of the costs. Office visit costs: $125 Jane pays: $125 Her plan pays: $0 Jane reaches her $1,500 deductible, co-insurance begins Jane has seen a doctor several times and paid $1,500 in total. Her plan pays some of the costs for her next visit. Office visit costs: $75 Jane pays: 20% of $75 = $15 Her plan pays: 80% of $75 = $60 Jane reaches her $5,000 out-of-pocket limit Jane has seen the doctor often and paid $5,000 in total. Her plan pays the full cost of her covered health care services for the rest of the year. Office visit costs: $200 Jane pays: $0 Her plan pays: $200 Glossary of Health Coverage and Medical Terms Page 4 of 4
Kaiser Foundation Health Plan, Inc. Northern California: High Option
 Kaiser Foundation Health Plan, Inc. Northern California: High Option 01/01/2015-12/31/2015 This is only a summary. Please read the FEHB Plan brochure (RI 73-003) that contains the complete terms of this
Kaiser Foundation Health Plan, Inc. Northern California: High Option 01/01/2015-12/31/2015 This is only a summary. Please read the FEHB Plan brochure (RI 73-003) that contains the complete terms of this
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Prev. Plus Plan This is only a summary. If you want more detail about your coverage and costs,
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Prev. Plus Plan This is only a summary. If you want more detail about your coverage and costs,
Kaiser Foundation Health Plan of the Northwest: High Option Coverage Period: 1/01/ /31/2014
 Kaiser Foundation Health Plan of the Northwest: High Option Coverage Period: 1/01/2014-12/31/2014 This is only a summary. Please read the FEHB Plan brochure (RI-73-004) that contains the complete terms
Kaiser Foundation Health Plan of the Northwest: High Option Coverage Period: 1/01/2014-12/31/2014 This is only a summary. Please read the FEHB Plan brochure (RI-73-004) that contains the complete terms
Important Questions Answers Why this Matters:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Premium Plan This is only a summary. If you want more detail about your coverage and costs, you
Some of the services this plan doesn t cover are listed on page 5. See your policy Yes plan doesn t cover?
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Network This is only a summary. If you want more detail about your coverage and costs, you can
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: Network This is only a summary. If you want more detail about your coverage and costs, you can
Employee Benefit Plan: Missoula County Public Schools Coverage Period: 01/01/ /31/2014 Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
See the chart starting on page 2 for your costs for services this plan covers.
 BlueCross BlueShield of WNY: Traditional Blue 901 Coverage Period: 10/01/2013-9/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: Indemnity
BlueCross BlueShield of WNY: Traditional Blue 901 Coverage Period: 10/01/2013-9/31/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Single/Family Plan Type: Indemnity
Important Questions Answers Why this Matters:
 Kaiser Permanente: Gwinnett County Gold HMO Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail
Kaiser Permanente: Gwinnett County Gold HMO Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail
Important Questions Answers Why this Matters:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: PPO This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: PPO This is only a summary. If you want more detail about your coverage and costs, you
Anthem Blue Cross Select HMO: B3 Coverage Period: 01/01/ /31/2015
 This is only a summary. Please read the FEHB Plan brochure (RI 73-877)) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 73-877)) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. Please read the FEHB Plan brochure (RI 73-168) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 73-168) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
$0 per covered individual up to $0 per family. What is the overall deductible?
 Kaiser Foundation Health Plan of the Northwest: High Option Coverage Period: 1/01/2016-12/31/2016 Coverage for: Self Only, Self Plus One -or- Self and Family Plan Type: HMO This is only a summary. Please
Kaiser Foundation Health Plan of the Northwest: High Option Coverage Period: 1/01/2016-12/31/2016 Coverage for: Self Only, Self Plus One -or- Self and Family Plan Type: HMO This is only a summary. Please
Coverage for: Self Only, Self Plus One, Self and Family Plan Type: HMO w/pos Kaiser Foundation Health Plan of Washington Options, Inc.
 You can view the Glossary at www.kp.org/wa/fehb-options or call 1-888-901-4636 to request a copy. Coverage Period: 01/01/2017 12/31/2017 This is only a summary. Please read the FEHB Plan brochure (RI 73-051)
You can view the Glossary at www.kp.org/wa/fehb-options or call 1-888-901-4636 to request a copy. Coverage Period: 01/01/2017 12/31/2017 This is only a summary. Please read the FEHB Plan brochure (RI 73-051)
GHI Health Plan: FEHB Standard Option Coverage Period: 1/1/ /31/2013
 This is only a summary. Please read the FEHB Plan brochure RI 73-007 that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth in
This is only a summary. Please read the FEHB Plan brochure RI 73-007 that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth in
WellCare of New York: Essential Plan 3 Coverage Period: 01/01/2017
 WellCare of New York: Essential Plan 3 Coverage Period: 01/01/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HMO This is only
WellCare of New York: Essential Plan 3 Coverage Period: 01/01/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HMO This is only
Kaiser Foundation Health Plan of the Mid-Atlantic States, Inc.: High Option
 Kaiser Foundation Health Plan of the Mid-Atlantic States, Inc.: High Option 1/01/2015-12/31/2015 This is only a summary. Please read the FEHB Plan brochure (RI 73-047) that contains the complete terms
Kaiser Foundation Health Plan of the Mid-Atlantic States, Inc.: High Option 1/01/2015-12/31/2015 This is only a summary. Please read the FEHB Plan brochure (RI 73-047) that contains the complete terms
Premera Blue Cross: WEA Select Qualified High Deductible Health Plan Coverage Period: 10/1/ /30/2013 Summary of Benefits and Coverage:
 Premera Blue Cross: WEA Select Qualified High Deductible Health Plan Coverage Period: 10/1/2012-09/30/2013 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Premera Blue Cross: WEA Select Qualified High Deductible Health Plan Coverage Period: 10/1/2012-09/30/2013 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Premera Blue Cross: WEA Select Qualified High Deductible Health Plan
 Premera Blue Cross: WEA Select Qualified High Deductible Health Plan Coverage Period: 11/1/2015-10/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage
Premera Blue Cross: WEA Select Qualified High Deductible Health Plan Coverage Period: 11/1/2015-10/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage
Highmark Blue Cross Blue Shield: HDHP Coverage Period: 04/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
MHBP Consumer Option Coverage Period: 01/01/ /31/2017
 This is only a summary. Please read the FEHB Plan brochure (RI 71-016) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 71-016) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Health Net of CA: High Option HMO 34C Coverage Period: 1/1/ /31/2013 Summary of Benefits and Coverage
 This is only a summary. Please read the FEHB Plan brochure (RI-73-159) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI-73-159) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Edgewell: Cigna: $750 PPO Preferred Network Plan Coverage Period: 1/1/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cigna.com or by calling 1-855-820-6604. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cigna.com or by calling 1-855-820-6604. Important Questions
Excellus BCBS:Simply Blue Copay
 Excellus BCBS:Simply Blue Copay A nonprofit independent licensee of the Blue Cross Blue Shield Association Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2013-12/31/2013
Excellus BCBS:Simply Blue Copay A nonprofit independent licensee of the Blue Cross Blue Shield Association Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2013-12/31/2013
Highmark Blue Cross Blue Shield: PPO Coverage Period: 04/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
Health Plan: Citrus Valley Health Partners Coverage Period: Beginning on or after 1/1/2016 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myhnas.com or by calling 1-855-323-1132. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myhnas.com or by calling 1-855-323-1132. Important Questions
You don t have to meet deductibles for specific services, but see the chart starting on page 3 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.nipponlifebenefits.com or by calling 1-800-374-1835.
HealthPartners High Option Coverage Period: 1/1/ /31/2014
 This is only a summary. Please read the FEHB Plan brochure (RI 73-009) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 73-009) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Also, members may self-refer using the Access+ Self-Refer feature.
 This is only a summary. Please read the FEHB Plan brochure (RI 73-574 ) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 73-574 ) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.aetna.com or by calling 1-855-695-3416. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.aetna.com or by calling 1-855-695-3416. Important Questions
Coverage for: Individual/Family Plan Type: HDHP
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mybenefitshome.com or by calling 1-800-652-9451. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mybenefitshome.com or by calling 1-800-652-9451. Important
Highmark Blue Cross Blue Shield: PPO Coverage Period: 04/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
Highmark Blue Cross Blue Shield: Classic Blue Coverage Period: 04/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
MHBP Standard Option Coverage Period: 01/01/ /31/2017
 This is only a summary. Please read the FEHB Plan brochure (RI 71-007) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 71-007) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
YRC Worldwide: Bronze Plan Coverage Period: 01/01/ /31/2015
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com/yrcw or by calling 1-866-686-3675. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com/yrcw or by calling 1-866-686-3675. Important
Highmark Blue Cross Blue Shield: PPO Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-299-1910. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-299-1910. Important
Waste Management: High Deductible Health Plan Coverage Period: 01/01/ /31/2015
 This is only a summary. If you want more details about your coverage and costs, you can get the complete terms in the plan document at www.mycigna.com, by calling 800-545-6534 and on www.mywmtotalrewards.com.
This is only a summary. If you want more details about your coverage and costs, you can get the complete terms in the plan document at www.mycigna.com, by calling 800-545-6534 and on www.mywmtotalrewards.com.
GHI Health Plan: FEHB Standard Option Coverage Period: 1/1/ /31/2017 Coverage for: Self Only, Self Plus One or Self and Family Plan Type: EPO
 This is only a summary. Please read the FEHB Plan brochure ([RI 73-007]) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure ([RI 73-007]) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
In-Network. Out-of-Network $6,000 Individual/$12,000 Family. What is the overall deductible? Does not apply to certain preventive care.
 Amarillo Independent School District: CDHP Plan Coverage Period: 07/01/2016 06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: ALL Plan Type: CDHP This is
Amarillo Independent School District: CDHP Plan Coverage Period: 07/01/2016 06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: ALL Plan Type: CDHP This is
Important Questions Answers Why this Matters: Network: $3,000 Individual, $6,000 Family Non-Network: $7,500 Individual, $15,000 Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-809-8663.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthscopebenefits.com or by calling 1-800-809-8663.
GHI Health Plan: FEHB High Option Coverage Period: 1/1/ /31/2017 Coverage for: Self Only, Self Plus One or Self and Family Plan Type: PPO
 This is only a summary. Please read the FEHB Plan brochure ([RI 73-007]) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure ([RI 73-007]) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Healthe Options Component Plan: Cerner Corporation Coverage Period: 01/01/ /31/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cernerhealth.com or by calling 1-877-765-1033. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cernerhealth.com or by calling 1-877-765-1033. Important
Highmark Blue Shield: PPO Coverage Period: 07/01/ /30/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkblueshield.com or by calling 1-888-745-3212.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkblueshield.com or by calling 1-888-745-3212.
Important Questions Answers Why this Matters: What is the overall deductible*? In-Network: $1,500 per person $3,000 per family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthpartners.com/3m or by calling toll free 1-877-435-7613.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthpartners.com/3m or by calling toll free 1-877-435-7613.
Health Net of Arizona: Standard Option HMO BX6 Coverage Period: 01/01/ /31/2017 Summary of Benefits and Coverage
 This is only a summary. Please read the FEHB Plan brochure (RI-73-283) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI-73-283) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Why this Matters: $ 0 See the chart starting on page 3 for your costs for services this plan covers.
 State of Illinois: State Plan Coverage Period: 07/01/2016-06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: HMO This is only
State of Illinois: State Plan Coverage Period: 07/01/2016-06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: HMO This is only
CCSD#59 HMO and Blue Advantage HMO: Blue Cross and Blue Shield of Illinois Coverage Period: 07/01/ /30/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com or by calling 1-800-892-2803. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com or by calling 1-800-892-2803. Important Questions
Some of the services this plan doesn t cover are listed in the Services Your Plan Does NOT Yes. plan doesn t cover?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mercycarehealthplans.com or by calling 1-800-895-2421.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mercycarehealthplans.com or by calling 1-800-895-2421.
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mercycarehealthplans.com or by calling 1-800-895-2421.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mercycarehealthplans.com or by calling 1-800-895-2421.
Highmark Blue Cross Blue Shield: PPO Coverage Period: 08/01/ /31/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-800-241-5704. Important
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs and for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-866-231-0847. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-866-231-0847. Important Questions
$0 See the chart starting on page 2 for your costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mercycarehealthplans.com or by calling 1-800-895-2421.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mercycarehealthplans.com or by calling 1-800-895-2421.
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
GEHA: Health Savings Advantage Coverage Period: 01/01/ /31/2016 Coverage for: Self Only, Self Plus One or Self and Family Plan Type: HDHP
 This is only a summary. Please read the FEHB Plan brochure (RI 71-014) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 71-014) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
CCSD#59 HMO and Blue Advantage HMO: Blue Cross and Blue Shield of Illinois Coverage Period: 07/01/ /30/2016 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com or by calling 1-800-892-2803. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com or by calling 1-800-892-2803. Important Questions
Highmark Blue Cross Blue Shield: Major Events Blue PPO 6600 a Community Blue Plan
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-888-510-1084. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-888-510-1084. Important
Kaiser Permanente: Walmart Northwest Low Option
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.kp.org/plandocuments or by calling 503-813-2000 or 1-800-813-2000.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.kp.org/plandocuments or by calling 503-813-2000 or 1-800-813-2000.
RPEC1807 BlueEdge HSA: Blue Cross and Blue Shield of Illinois Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com or by calling 1-800-541-2768. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com or by calling 1-800-541-2768. Important Questions
What is the overall deductible? Are there other deductibles for specific services? Yes. $500 person/$1,000 family for prescription drugs.
 Premera Blue Cross: WEA Select Basic Plan Coverage Period: 11/1/2015-10/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage Tiers Plan Type: PPO This
Premera Blue Cross: WEA Select Basic Plan Coverage Period: 11/1/2015-10/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage Tiers Plan Type: PPO This
North Kingstown Schools - # , 0002 BlueSolutions for HSA Coverage Period: 07/01/ /30/2017
 North Kingstown Schools - #1002365-0001, 0002 BlueSolutions for HSA Coverage Period: 07/01/2016-06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: See below
North Kingstown Schools - #1002365-0001, 0002 BlueSolutions for HSA Coverage Period: 07/01/2016-06/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: See below
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
GEHA: High Option Coverage Period: 01/01/ /31/2015
 This is only a summary. Please read the FEHB Plan brochure (RI 71-006) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 71-006) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
St. Charles CUSD #303 HMOI: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/ /31/2014 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.d303.org or by calling 1-331-228-4929. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.d303.org or by calling 1-331-228-4929. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.kbasolution.com or by calling 1-800-278-5488. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.kbasolution.com or by calling 1-800-278-5488. Important
$300 person/$900 family Combined for innetwork or out-of-network. Does not apply to preventive care, office visits or prescription drugs.
 Premera Blue Cross: WEA Select Plan 3 Coverage Period: 11/1/2015-10/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage Tiers Plan Type: PPO This
Premera Blue Cross: WEA Select Plan 3 Coverage Period: 11/1/2015-10/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage Tiers Plan Type: PPO This
$0 See the chart starting on page 2 for your costs for services this plan covers.
 : Blue & U Basic Select Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage Tiers Plan Type: EPO This is
: Blue & U Basic Select Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Coverage Tiers Plan Type: EPO This is
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbstx.com or by calling 1-866-295-1212. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbstx.com or by calling 1-866-295-1212. Important Questions
Midwestern Intermediate Unit #4: QHDHP Coverage Period: 01/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.miu4.k12.pa.us or by calling (724)458-6700 ext. 1202.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.miu4.k12.pa.us or by calling (724)458-6700 ext. 1202.
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthnet.com/edison or by calling 1-888-893-1572. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthnet.com/edison or by calling 1-888-893-1572. Important
: Ohio University Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. It in no way modifies your benefits as described in your plan documents. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
This is only a summary. It in no way modifies your benefits as described in your plan documents. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthyct.org or by calling 1-855-458-4928. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthyct.org or by calling 1-855-458-4928. Important
CalPERS: Sharp Performance Plus HMO Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.sharphealthplan.com/calpers or by calling 1-855-995-5004.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.sharphealthplan.com/calpers or by calling 1-855-995-5004.
$ 2,500 Individual/$5,000. Important Questions Answers Why this Matters: $2,500 Individual/$5,000
 IL QHDHP $2500 100/50 Aggregate Deductible Coverage Period: 01/01/2013-12/31/2013 Summary of Benefits and Coverage:What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: QHDHP
IL QHDHP $2500 100/50 Aggregate Deductible Coverage Period: 01/01/2013-12/31/2013 Summary of Benefits and Coverage:What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: QHDHP
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
Chevron High Deductible Health Plan (HDHP) (311)
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at hr2.chevron.com, or by calling the Chevron Human Resources
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at hr2.chevron.com, or by calling the Chevron Human Resources
Kalispell Public Schools High Deductible Plan Coverage Period: 07/01/ /30/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myfirstchoice.fchn.com or by calling 1-800-783-7312.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myfirstchoice.fchn.com or by calling 1-800-783-7312.
National Allied Workers Union Insurance Trust Fund Plan V Coverage Period: 04/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.aegisadmin.com or by calling 1-773-889-2307. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.aegisadmin.com or by calling 1-773-889-2307. Important
Kaiser Permanente: CaliforniaChoice Gold HMO B Coverage Period:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.kp.org or by calling 1-800-278-3296. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.kp.org or by calling 1-800-278-3296. Important Questions
Highmark West Virginia: SuperBlue Plus 2010 Coverage Period: 06/01/ /31/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbswv.com or by calling 1-888-809-9121. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbswv.com or by calling 1-888-809-9121. Important
Aetna Student Health: Columbia University Platinum Plan Coverage Period: Beginning on or after 8/15/2015
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at http://www.aetnastudenthealth.com/columbia or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at http://www.aetnastudenthealth.com/columbia or by calling
Nationwide Life Insurance Co.: Gold Plan - Alabama State University Coverage Period: 8/15/15-8/14/16
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
Coverage for: Single/Family Plan Type: PPO. Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbswny.com or by calling 1-888-249-2583. Important Questions
Highmark Blue Cross Blue Shield: Shared Cost Blue PPO2650 a Community Blue Plan
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-888-510-1084. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbs.com or by calling 1-888-510-1084. Important
Important Questions Answers Why this Matters: $1,500 Individual/$3,000 Family (See chart starting on page 2 for when deductible is waived.
 Kaiser Permanente: Nationwide Mutual Insurance - California Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family
Kaiser Permanente: Nationwide Mutual Insurance - California Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Covered Members Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Covered Members Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you
GEHA: Standard Option Coverage Period: 01/01/ /31/2016 Coverage for: Self Only, Self Plus One or Self and Family Plan Type: PPO
 This is only a summary. Please read the FEHB Plan brochure (RI 71-006) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
This is only a summary. Please read the FEHB Plan brochure (RI 71-006) that contains the complete terms of this plan. All benefits are subject to the definitions, limitations, and exclusions set forth
Why this Matters: $0. See chart on Page 2 for your costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.hr2.chevron.com or by calling 808-432-5955 (Oahu) or
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.hr2.chevron.com or by calling 808-432-5955 (Oahu) or
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bsneny.com or by calling 1-800-888-1238. Important Questions
Douglas County School District Health Care Plan: Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.hometownhealth.com or by calling 1-800-336-0123 Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.hometownhealth.com or by calling 1-800-336-0123 Important
Nationwide Life Insurance Co.: Gold Plan - Oregon College of Art and Craft Coverage Period: 8/29/15-8/28/16
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
$3,500 person / $7,000 family For non-preferred providers
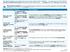 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.blueshieldca.com or by calling 888-852-5345. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.blueshieldca.com or by calling 888-852-5345. Important
BlueCross BlueShield of WNY: Gold PPO 7100
 BlueCross BlueShield of WNY: Gold PPO 7100 Coverage Beginning on or After: 01/01/2016 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the
BlueCross BlueShield of WNY: Gold PPO 7100 Coverage Beginning on or After: 01/01/2016 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the
Guide HMO 25/ / % 3600/7200 Rx1 Coverage Period: 01/01/ /31/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthalliance.org. or by calling 1-800-851-3379. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthalliance.org. or by calling 1-800-851-3379. Important
Health Alliance HMO 100 Rx28 NS1 Coverage Period: 01/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthalliance.org. or by calling 1-800-851-3379. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthalliance.org. or by calling 1-800-851-3379. Important
Important Questions Answers Why this Matters: $3,500 individual/$7,000 family in-network; $9,000 individual/$18,000 family out-ofnetwork
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.livetheorangelife.com or by calling 1-800-555-4954. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.livetheorangelife.com or by calling 1-800-555-4954. Important
Important Questions. What is the overall deductible?
 Important Questions This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.ebms.com or by calling 1-866-312-6723.
Important Questions This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.ebms.com or by calling 1-866-312-6723.
Blue Shield of CA: Shield PPO Split Deductible 20/500 Coverage Period: Beginning on or after 1/1/2013
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.blueshieldca.com or by calling 1-800-424-6521. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.blueshieldca.com or by calling 1-800-424-6521. Important
Chevron Medical HMO Plan Kaiser HI (039) Coverage Period: 01/01/ /31/2017
 Chevron Medical HMO Plan Kaiser HI (039) Coverage Period: 01/01/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: You Only You and One Adult You and
Chevron Medical HMO Plan Kaiser HI (039) Coverage Period: 01/01/2017 12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: You Only You and One Adult You and
