Investors Individual Medical Policy -IMed
|
|
|
- Garey Richardson
- 6 years ago
- Views:
Transcription
1 Investors Individual Medical Policy -IMed Schedule of Benefits Nextcare is a specialized policy administrator on behalf of the Insurer The below table explains all the benefits in this policy and how to avail it The Policy Wording include full Benefit details, coverage definitions and exclusions All Benefits shown are per insured person, per one year coverage All limits and Co-payments are expressed in Arab Emirates Dirham Insurance coverage is only applicable for Dubai visa holders only This Schedule of benefits is not applicable for Abu Dhabi/ Al Ain policies except in case of emergency Type of Benefit DHA basic plan Annual limit 150,000 AED Geographical scope of coverage Within the Emirates of Dubai and Northern Emirates (Sharjah, Ras Al Khaimah, Ajman, Fujairah and Umn Al Quwain )for emergency : Within all emirates of the UAE Only Network Pre-existing s-existing s NEXtCARE PCP Clinics for outpatient services NEXtCARE RN3 Hospitals for inpatient and emergency services Treatment for chronic and preexisting s excluded for first 6 months of first scheme membership. After 6 months Covered to the annual policy limit subject to declaration
2 Outpatient services 20% coinsurance payable by the insured s are provided in authorized out-patient clinics of hospitals, clinics and health centers called PCP clinic Referral procedure: In respect of Essential Benefit Plan members, no costs incurred for advice, consultations or treatments provided by specialists or consultants without the insured first consulting a General Practitioner (or equivalent as designated by DHA) who is licensed by DHA or another competent UAE authority will be payable by the insurer. Laboratory test services Radiology diagnostic Physiotherapy treatment services Covered In cases of non-medical emergencies, the insurance company s prior approval is required for MRI, CT scans and endoscopies Prior approval of the insurance company is required. Maximum 6 sessions per year. 20% coinsurance payable per session inpatient services 20% coinsurance payable by the insured with a cap of 500 AED payable per encounter and an annual aggregate cap of 1000 AED.Above these caps the insurer will cover 100% of treatment. in-patient treatment at authorized hospital (RN3) The insured should first consult a general practitioner (or equivalent as designated by DHA-who is licensed by DHA or another competent UAE authority))at outpatient PCP clinic that will refer him / her to respective RN3 Hospital ( within the designated Network ) -with diagnosis- for advice,treatment provided by a specialist or consultant for inpatient treatment when medical surgical intervention is recommended. no cost will be payable for referral In-patient services will be received in rooms of two or more beds Ground transportation services in the UAE provided by an authorized party for medical emergencies Tests, diagnosis and /or treatments related to surgeries in hospitals Emergency treatment Prior approval Required from the insurance company / TPA Approval required from the insurance company within 24 hours of admission to the authorized hospital Healthcare services for emergency cases Prior approval required from the insurance company
3 (Where a pre-existing or chronic develops into an emergency within the 6-month exclusion period this must be covered up to the annual aggregate limit) Prior approval required from the insurance company Companion accommodation : The cost of accommodating a person accompanying an insured child up to the age of 16 years The cost of accommodation of a person accompanying an inpatient in the same room in cases of medical necessity at the recommendation of the treating doctor and after the prior approval of the insurance company providing coverage Maximum 100 AED per night Maximum 100 AED per night Medication Cost of drugs and medicines up to an annual limit of 1,500 AED (including coinsurance). 30% payable by the insured in respect of each and every prescription. No cover for drugs and medicines in excess of the annual limit Restricted to a list of formulary products where available Restricted to a list of formulary products where available at the physician and the pharmacist Preventive services, vaccines and immunizations Essential vaccinations and inoculations for new-borns and children as stipulated in the DHA s policies and its updates in the assigned facilities (currently the same as Federal MOH). Preventive services as stipulated by DHA to include initially diabetes screening Frequency restricted to: Diabetes: Every 3 years from age 30 High risk individuals annually from age 18 The DHA has to notify authorized insurance companies of any preventive services that will be added to the basic package at least three months in advance of the implementation date and the newly covered preventive services will be covered from that date Maternity Benefit Where any develops which becomes an emergency, the medically necessary expenses will be covered up to the annual aggregate limit- subject to declaration. Note: Where any develops which becomes an emergency, the medically necessary expenses will be covered up to the annual aggregate limit. Out-patient ante-natal services Requires prior approval from the insurance company
4 10% coinsurance payable by the insured 8 visits to PHC; All care provided by PHC obstetrician for low risk or specialist obstetrician for high risk referrals Initial investigations to include: FBC and Platelets Blood group, Rhesus status and antibodies VDRL MSU & urinalysis Rubella serology HIV Hep C offered to high risk patients GTT if high risk FBS, random s or A1c for all due to high prevalence of diabetes in UAE Visits to include reviews, checks and tests in accordance with DHA Antenatal Care Protocols 3 ante-natal ultrasound scans In-patient maternity services Requires prior approval from the insurance company or within 24 hours of emergency treatment 10% coinsurance payable by the insured Maximum benefit 7,000 AED per normal delivery, 10,000 AED for medically necessary C-section, complications and for medically necessary termination (All limits include coinsurance) New born cover Cover for 30 days from birth BCG, Hepatitis B and neo-natal screening test Excluded healthcare services ( except in cases of medical emergencies only ) Condition Diagnostic and treatment services for dental and gum treatments In case of emergency only -Subject to 20% coinsurance Hearing and vision aids, and vision correction by surgeries and laser In case of emergency only -Subject to 20% coinsurance SANCTION LIMITATION AND EXCLUSION CLAUSE No (re)insurer shall be deemed to provide cover and no (re)insurer shall be liable to pay any claim or provide any benefit hereunder to the extent that the provision of such cover, payment of such claim or provision of such benefit would expose that (re)insurer to any sanction, prohibition or restriction under United Nations resolutions or the trade or economic sanctions, laws or regulations of the European Union, United Kingdom or United States of America.
5 General exclusion list is in line with DHA mandated benefit and scope of coverage. Excluded (non basic) healthcare services: 1. Healthcare s which are not medically necessary 2. All expenses relating to dental treatment, dental prostheses, and orthodontic treatments 3. Home nursing; private nursing care; care for the sake of travelling. 4. Custodial care including Non-medical treatment services Health-related services which do not seek to improve or which do not result in a change in the medical of the patient. 5. s which do not require continuous administration by specialized medical personnel. 6. Personal comfort and convenience items (television, barber or beauty service, guest service and similar incidental services and supplies). 7. All cosmetic healthcare services and services associated with replacement of an existing breast implant. Cosmetic operations which are related to an Injury, sickness or congenital anomaly when the primary purpose is to improve physiological functioning of the involved part of the body and breast reconstruction following a mastectomy for cancer are covered. 8. Surgical and non-surgical treatment for obesity (including morbid obesity), and any other weight control programs, services, or supplies. 9. Medical services utilized for the sake of research, medically non-approved experiments and Investigations and pharmacological weight reduction regimens. 10. Healthcare s that are not performed by Authorized Healthcare Providers. 11. Healthcare services and associated expenses for the treatment of alopecia, baldness, hair falling, dandruff or wigs. 12. Health services and supplies for smoking cessation programs and the treatment of nicotine addiction. 13. Any investigations, tests or procedures carried out with the intention of ruling out any fetal anomaly. 14. Treatment and services for contraception. 15. Treatment and services for sex transformation, sterilization or intended to correct a state of sterility or infertility or sexual dysfunction. Sterilization is allowed only if medically indicated and if allowed under the Law. 16. External prosthetic devices and medical equipment. 17. Treatments and services arising as a result of hazardous activities, including but not limited to, any form of aerial flight, any kind of power-vehicle race, water sports, horse riding activities, mountaineering activities, violent sports such as judo, boxing, and wrestling, bungee jumping and any professional sports activities. 18. Growth hormone therapy. 19. Costs associated with hearing tests, vision corrections, prosthetic devices or hearing and vision aids. 20. Mental Health diseases, both out-patient and in-patient treatments, unless it is an emergency. 21. Patient treatment supplies (including for example: elastic stockings, ace bandages, gauze, syringes, diabetic test strips, and like products; non-prescription drugs and treatments,) excluding supplies required as a result of Healthcare s rendered during a Medical Emergency.
6 22. Allergy testing and desensitization (except testing for allergy towards medications and supplies used in treatment); any physical, psychiatric or psychological examinations or investigations during these examinations. 23. s rendered by any medical provider who is a relative of the patient for example the Insured person himself or first degree relatives. 24. Enteral feedings (via a tube) and other nutritional and electrolyte supplements, unless medically necessary during in-patient treatment. 25. Healthcare services for adjustment of spinal subluxation. 26. Healthcare services and treatments by acupuncture; acupressure, hypnotism, massage therapy, aromatherapy, ozone therapy, homeopathic treatments, and all forms of treatment by alternative medicine. 27. All healthcare services & treatments for in-vitro fertilization (IVF), embryo transfer; ovum and sperms transfer. 28. Elective diagnostic services and medical treatment for correction of vision 29. Nasal septum deviation and nasal concha resection. 30. All chronic s requiring haemodialysis or peritoneal dialysis, and related investigations, treatments or procedures. 31. Healthcare services, investigations and treatments related to viral hepatitis and associated complications, except for the treatment and services related to Hepatitis A. 32. Birth defects, congenital diseases and deformities. 33. Healthcare services for senile dementia and Alzheimer s disease. 34. Air or terrestrial medical evacuation and unauthorized transportation services. 35. Inpatient treatment received without prior approval from the insurance company including cases of medical emergency which were not notified within 24 hours from the date of admission. 36. Any inpatient treatment, investigations or other procedures, which can be carried out on outpatient basis without jeopardizing the Insured Person s health. 37. Any investigations or health services conducted for non-medical purposes such as investigations related to employment, travel, licensing or insurance purposes. 38. All supplies which are not considered as medical treatments including but not limited to: mouthwash, toothpaste, lozenges, antiseptics, milk formulas, food supplements, skin care products, shampoos and multivitamins (unless prescribed as replacement therapy for known vitamin deficiency s); and all equipment not primarily intended to improve a medical or injury, including but not limited to: air ers or air purifying systems, arch supports, exercise equipment and sanitary supplies. 39. More than one consultation or follow up with a medical specialist in a single day unless referred by the treating physician. 40. Health services and associated expenses for organ and tissue transplants, irrespective of whether the Insured Person is a donor or a recipient. This exclusion also applies to follow-up treatments and complications. 41. Any expenses related to immunomodulators and immunotherapy. 42. Any expenses related to the treatment of sleep related disorders. 43. s and educational programs for handicaps.
7 Healthcare services outside the scope of health insurance: 1. Injuries or illnesses suffered by the Insured Person as a result of military operations of whatever type. 2. Injuries or illnesses suffered by the Insured Person as a result of wars or acts of terror of whatever type. 3. Healthcare services for injuries and accidents arising from nuclear or chemical contamination. 4. Injuries resulting from natural disasters, including but not limited to: earthquakes, tornados and any other type of natural disaster. 5. Injuries resulting from criminal acts or resisting authority by the Insured Person. 6. Injuries resulting from a road traffic accident. 7. Healthcare services for work related illnesses and injuries as per Federal Law No. 8 of 1980 concerning the Regulation of Work Relations, its amendments, and applicable laws in this respect. 8. All cases resulting from the use of alcoholic drinks, controlled substances and drugs and hallucinating substances. Any investigation or treatment not prescribed by a doctor. 9. Injuries resulting from attempted suicide or self-inflicted injuries. 10. Diagnosis and treatment services for complications of exempted illnesses. 11. All healthcare services for internationally and/or locally recognized epidemics. 12. Healthcare services for patients suffering from (and related to the diagnosis and treatment of) HIV AIDS and its complications and all types of hepatitis except Hepatitis A For further details, on the services included in the above table / or about any other services not included Kindly contact Nextcare Call Centre at
Inactive at work Dependents & Parents
 Inactive at work Dependents & Parents Medical Takaful Plan Quotation Direct Notes for Non Abu Dhabi Plan: 1. The policy holder has the obligation of declaring the place of work stay of the insured members;
Inactive at work Dependents & Parents Medical Takaful Plan Quotation Direct Notes for Non Abu Dhabi Plan: 1. The policy holder has the obligation of declaring the place of work stay of the insured members;
Inactive at work Dependents & Parents OR Domestic Workers
 Inactive at work Dependents & Parents OR Domestic Workers Medical Takaful Plan Quotation Direct Notes for Non Abu Dhabi Plan: 1. The policy holder has the obligation of declaring the place of work stay
Inactive at work Dependents & Parents OR Domestic Workers Medical Takaful Plan Quotation Direct Notes for Non Abu Dhabi Plan: 1. The policy holder has the obligation of declaring the place of work stay
Individual Medical Insurance. Dependents & Parents Non Working
 Individual Medical Insurance Dependents & Parents Non Working 1 Our Services and Privileges: 24 hour claim services all year round Medical Network also include Sharjah & Northern Emirates Card less & Cash
Individual Medical Insurance Dependents & Parents Non Working 1 Our Services and Privileges: 24 hour claim services all year round Medical Network also include Sharjah & Northern Emirates Card less & Cash
GROUP MEDICAL INSURANCE NON BINDING AND INDICATIVE PROPOSAL
 GROUP MEDICAL INSURANCE NON BINDING AND INDICATIVE PROPOSAL Dear Sir/Madam, Thank you for considering Dar Al Takaful PJSC for your client s Medical Insurance requirements. Based on the information provided,
GROUP MEDICAL INSURANCE NON BINDING AND INDICATIVE PROPOSAL Dear Sir/Madam, Thank you for considering Dar Al Takaful PJSC for your client s Medical Insurance requirements. Based on the information provided,
SCHEDULE OF BENEFITS
 SCHEDULE OF BENEFITS Plan Benefit Limit (Including any coinsurance and/or deductible) Geographical Scope of Coverage for Basic Healthcare Services (Elective Treatment) Geographical Scope of Coverage for
SCHEDULE OF BENEFITS Plan Benefit Limit (Including any coinsurance and/or deductible) Geographical Scope of Coverage for Basic Healthcare Services (Elective Treatment) Geographical Scope of Coverage for
SCHEDULE OF BENEFITS
 SCHEDULE OF BENEFITS Plan Annual Benefit Limit (Including any coinsurance and/or deductible) Geographical Scope of Coverage for Basic Healthcare Services (Elective Treatment) Geographical Scope of Coverage
SCHEDULE OF BENEFITS Plan Annual Benefit Limit (Including any coinsurance and/or deductible) Geographical Scope of Coverage for Basic Healthcare Services (Elective Treatment) Geographical Scope of Coverage
THE ORIENTAL INSURANCE CO. LTD.
 Coverage Details UAE, Indian Sub-Continent, South East Asia. Area of Cover Geographical Territory - Extended Limit per insured per annum Third Party Administrator Eligibility of Cover IP treatments covered
Coverage Details UAE, Indian Sub-Continent, South East Asia. Area of Cover Geographical Territory - Extended Limit per insured per annum Third Party Administrator Eligibility of Cover IP treatments covered
THE ORIENTAL INSURANCE CO. LTD.
 Coverage Details UAE, Indian Sub-Continent, South East Asia and Arab countries Area of Cover Geographical Territory - Extended Limit per insured per annum Third Party Administrator Eligibility of Cover
Coverage Details UAE, Indian Sub-Continent, South East Asia and Arab countries Area of Cover Geographical Territory - Extended Limit per insured per annum Third Party Administrator Eligibility of Cover
DIC/MED/2016/KD/ rd February 2016 VIP BRONZE
 VIP BRONZE Reference is made to your query in respect of the above. We are pleased to offer you the following plan in line to meet your client s requirement. Category Family of benefits Non- HAAD Product
VIP BRONZE Reference is made to your query in respect of the above. We are pleased to offer you the following plan in line to meet your client s requirement. Category Family of benefits Non- HAAD Product
Schedule of Benefits Family Care Plan (AUH)
 Schedule of Benefits Family Care Plan (AUH) MedNet is a specialized policy administrator on behalf of the Insurer In the tables below the Benefits applicable have been summarized for each product option
Schedule of Benefits Family Care Plan (AUH) MedNet is a specialized policy administrator on behalf of the Insurer In the tables below the Benefits applicable have been summarized for each product option
Individual Medical Plan Explanatory Handbook
 Individual Medical Plan Explanatory Handbook Our Contacts Email: individualmedical@takafulemarat.com Website: www.takafulemarat.com Phone Number: 800834 For claims / pre-approvals / network queries please
Individual Medical Plan Explanatory Handbook Our Contacts Email: individualmedical@takafulemarat.com Website: www.takafulemarat.com Phone Number: 800834 For claims / pre-approvals / network queries please
Family care plan (Dubai &Abu Dhabi)
 Family care plan (Dubai &Abu Dhabi) SECTION A PREAMBLE This document is intended to describe the basic purpose of the Insurance Policy and includes a description of the General Scope of Coverage, a list
Family care plan (Dubai &Abu Dhabi) SECTION A PREAMBLE This document is intended to describe the basic purpose of the Insurance Policy and includes a description of the General Scope of Coverage, a list
جميع المعلومات التي يجب أن تعرفها ALL YOU NEED TO KNOW
 جميع المعلومات التي يجب أن تعرفها ALL YOU NEED TO KNOW IMPORTANT NOTICE The Insurance product detailed in this leaflet is a product established, maintained and controlled by National General Insurance
جميع المعلومات التي يجب أن تعرفها ALL YOU NEED TO KNOW IMPORTANT NOTICE The Insurance product detailed in this leaflet is a product established, maintained and controlled by National General Insurance
Schedule of Benefits Family Care Plan (DHA)
 Schedule of Benefits Family Care Plan (DHA) MedNet is a specialized policy administrator on behalf of the Insurer In the tables below the Benefits applicable have been summarized for each product option
Schedule of Benefits Family Care Plan (DHA) MedNet is a specialized policy administrator on behalf of the Insurer In the tables below the Benefits applicable have been summarized for each product option
ANNEXURE : 1 FLEXI - DUBAI PLANS - OPTION 1
 ANNEXURE : 1 FLEXI - DUBAI PLANS ( OPTION 1 ) Applicable only for (DXB visa holders) with Gross Salary Above AED 4,000. Preexisting & chronic conditions will be covered only for declared cases: - New membership-
ANNEXURE : 1 FLEXI - DUBAI PLANS ( OPTION 1 ) Applicable only for (DXB visa holders) with Gross Salary Above AED 4,000. Preexisting & chronic conditions will be covered only for declared cases: - New membership-
SUMMARY OF BENEFITS Fisk University Open Access Plus -BUY-UP PLAN Effective 10/1/2015 Customer Service:
 SUMMARY OF BENEFITS Fisk University Open Access Plus -BUY-UP PLAN Effective www.mycigna.com Customer Service: 866-494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
SUMMARY OF BENEFITS Fisk University Open Access Plus -BUY-UP PLAN Effective www.mycigna.com Customer Service: 866-494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
All sub-limit sums insured are the maximum per Insured Person, per Period of Insurance unless otherwise stated
 Schedule of Cover Developed by All sub-limit sums insured are the maximum per Insured Person, per unless otherwise stated Annual maximum limit per individual insured person AED 1,000,000 AED 5,000,000
Schedule of Cover Developed by All sub-limit sums insured are the maximum per Insured Person, per unless otherwise stated Annual maximum limit per individual insured person AED 1,000,000 AED 5,000,000
INDIVIDUAL & FAMILY HEALTH INSURANCE PLANS
 This is a summary of benefits applicable for each product chosen. Kindly refer to the policy wording for full benefit details and definitions. All benefit shown is per Insured Member per period of cover.
This is a summary of benefits applicable for each product chosen. Kindly refer to the policy wording for full benefit details and definitions. All benefit shown is per Insured Member per period of cover.
UnitedHealthcare Choice Plus. Standard-Plan 011 Modified
 YOUR BENEFITS UnitedHealthcare Choice Plus -Plan 011 Modified Choice Plus plan gives you the freedom to see any Physician or other health care professional from our Network, including specialists, without
YOUR BENEFITS UnitedHealthcare Choice Plus -Plan 011 Modified Choice Plus plan gives you the freedom to see any Physician or other health care professional from our Network, including specialists, without
THE ORIENTAL INSURANCE CO. LTD.
 GENERAL BENEFITS Entry Age Minimum Entry Age Maximum Cover Type OP Treatment at Hospitals OP Treatment at Clinics Eligibility & Combination DEPENDENT PARENTS Adult: 18 Years Child: 31 days Adult: Up to
GENERAL BENEFITS Entry Age Minimum Entry Age Maximum Cover Type OP Treatment at Hospitals OP Treatment at Clinics Eligibility & Combination DEPENDENT PARENTS Adult: 18 Years Child: 31 days Adult: Up to
THE ORIENTAL INSURANCE CO. LTD.
 Entry Age Minimum Entry Age Maximum Cover Type OP Treatment at Hospitals OP Treatment at Clinics Eligibility & Combination DEPENDENT PARENTS GENERAL BENEFITS Adult: 18 Years Child: 31 days Adult: Up to
Entry Age Minimum Entry Age Maximum Cover Type OP Treatment at Hospitals OP Treatment at Clinics Eligibility & Combination DEPENDENT PARENTS GENERAL BENEFITS Adult: 18 Years Child: 31 days Adult: Up to
THE ORIENTAL INSURANCE CO. LTD.
 GENERAL BENEFITS Entry Age Minimum Entry Age Maximum Cover Type OP Treatment at Hospitals OP Treatment at Clinics Eligibility & Combination DEPENDENT PARENTS Adult: 18 Years Child: 31 days Adult: Up to
GENERAL BENEFITS Entry Age Minimum Entry Age Maximum Cover Type OP Treatment at Hospitals OP Treatment at Clinics Eligibility & Combination DEPENDENT PARENTS Adult: 18 Years Child: 31 days Adult: Up to
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. RADCO Health Savings Account Open Access Plus
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. RADCO Health Savings Account Open Access Plus General Services In-Network Out-of-Network Physician office visit Primary Care Physician (PCP) Physician
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. RADCO Health Savings Account Open Access Plus General Services In-Network Out-of-Network Physician office visit Primary Care Physician (PCP) Physician
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. Cornerstone Systems, Inc. Open Access Plus
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Cornerstone Systems, Inc. Open Access Plus General Services In-network Out-of-network Primary care physician You pay $30 copay per visit Physician
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Cornerstone Systems, Inc. Open Access Plus General Services In-network Out-of-network Primary care physician You pay $30 copay per visit Physician
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co.
 SUMMARY OF BENEFITS Ohio Associated Enterprises Health Savings Account Open Access Plus www.mycigna.com Member Services: (866) 494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
SUMMARY OF BENEFITS Ohio Associated Enterprises Health Savings Account Open Access Plus www.mycigna.com Member Services: (866) 494-2111 Cigna Health and Life Insurance Co. General Services In-Network Out-of-Network
Cigna Health and Life Insurance Co.
 SUMMARY OF BENEFITS Kass Shuler, P.A. Open Access Plus - Preferred www.mycigna.com Member Services 866-494-2111 Cigna Health and Life Insurance Co. Notice of Grandfathered Plan Status This plan is being
SUMMARY OF BENEFITS Kass Shuler, P.A. Open Access Plus - Preferred www.mycigna.com Member Services 866-494-2111 Cigna Health and Life Insurance Co. Notice of Grandfathered Plan Status This plan is being
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. RADCO Open Access Plus - Plan 1
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. RADCO Open Access Plus - Plan 1 General Services In-Network Out-of-Network Physician office visit Primary Care Physician (PCP) Physician Office Visit
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. RADCO Open Access Plus - Plan 1 General Services In-Network Out-of-Network Physician office visit Primary Care Physician (PCP) Physician Office Visit
SUMMARY OF BENEFITS. Alliance Behavioral Healthcare Open Access Plus Plan Effective 7/1/12. Cigna Health and Life Insurance Co.
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Alliance Behavioral Healthcare Effective 7/1/12 Network: GWH/CIGNA Open Access Plus CIGNA has multiple networks. Your plan is paired with the GWH-CIGNA
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Alliance Behavioral Healthcare Effective 7/1/12 Network: GWH/CIGNA Open Access Plus CIGNA has multiple networks. Your plan is paired with the GWH-CIGNA
Blue Precision Platinum HMO 004 OUTLINE OF COVERAGE
 Blue Precision Platinum HMO 004 Blue Precision HMO SM Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
Blue Precision Platinum HMO 004 Blue Precision HMO SM Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
PHYSICIAN SERVICES. $30 copay 1 1 You pay 50% $40 copay. You pay 0% 1 You pay 50% INPATIENT SERVICES OUTPATIENT SERVICES
 BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
Cigna pays 50% of eligible charges Individual Out of Pocket Maximum $4,900 $12,500. Cigna pays 100% of eligible charges PHYSICIAN SERVICES
 BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
WA Bronze PPO Saver /50 (1/14)
 PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services, including member cost sharing
PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services, including member cost sharing
COMPARING HEALTH PLANS
 COMPARING HEALTH PLANS Oman Insurance Company (P.S.C.) is the local insurer and administrator in the UAE. Plans are designed and internationally administered by Bupa Global. Full details of the benefits,
COMPARING HEALTH PLANS Oman Insurance Company (P.S.C.) is the local insurer and administrator in the UAE. Plans are designed and internationally administered by Bupa Global. Full details of the benefits,
Texas Open Access Value 7500/70%
 Open Access Value 7500/70% BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional
Open Access Value 7500/70% BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional
Comprehensive benefit plan including high benefit limits and a worldwide open provider network.
 2018 Comprehensive benefit plan including high benefit limits and a worldwide open provider network. Global Freedom Plus is tailored exclusively for individuals and families residing in Latin America and
2018 Comprehensive benefit plan including high benefit limits and a worldwide open provider network. Global Freedom Plus is tailored exclusively for individuals and families residing in Latin America and
South Bay Hotel Employees, Restaurant Employees Welfare Fund Comprehensive Major Medical Plan Summary of Benefits
 PLAN FEATURES PPO PLAN BENEFIT SUMMARY In-Network Provider Non-Network Provider Deductible (per calendar year) $ 250 Individual $ 500 Individual $ 500 Family $ 1,000 Family All covered expenses, except
PLAN FEATURES PPO PLAN BENEFIT SUMMARY In-Network Provider Non-Network Provider Deductible (per calendar year) $ 250 Individual $ 500 Individual $ 500 Family $ 1,000 Family All covered expenses, except
INDIVIDUAL & FAMILY PLANS
 BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
PLAN DESIGN & BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY
 AN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $300 Individual $800 Individual $900 Family $2,400 Family All covered expenses accumulate toward the preferred or non-preferred Deductible. Unless otherwise
AN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $300 Individual $800 Individual $900 Family $2,400 Family All covered expenses accumulate toward the preferred or non-preferred Deductible. Unless otherwise
Blue Precision Silver HMO 106 Blue Precision HMO SM
 Blue Precision Silver HMO 106 Blue Precision HMO SM OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your Policy. This
Blue Precision Silver HMO 106 Blue Precision HMO SM OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your Policy. This
Changes in some state or federal law or regulations or interpretations thereof may change the terms and conditions of coverage.
 BlueCare Direct Silver SM 212 with Advocate BlueCare Direct SM OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
BlueCare Direct Silver SM 212 with Advocate BlueCare Direct SM OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
Your Summary of Benefits PPO GenRx Plans
 Your Summary of Benefits PPO GenRx Plans Small Group PPO $25 Copay GenRx Plan Effective 10/2010 In addition to dollar and percentage copays, insureds are responsible for deductibles, as described below.
Your Summary of Benefits PPO GenRx Plans Small Group PPO $25 Copay GenRx Plan Effective 10/2010 In addition to dollar and percentage copays, insureds are responsible for deductibles, as described below.
Unlimited unless otherwise indicated.
 PLAN FEATURES PARTICIPATING NON-PARTICIPATING Deductible (per calendar year) $1,000 Individual $5,000 Individual $2,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior
PLAN FEATURES PARTICIPATING NON-PARTICIPATING Deductible (per calendar year) $1,000 Individual $5,000 Individual $2,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior
Optimum Health Designs
 Designed for Individuals, Families & Employers (PCP or Specialist) Preventive Care Tests Diagnostic, Xray & Laboratory Emergency Room Surgery (Inpatient & Outpatient) Anesthesia Supplemental Accident for
Designed for Individuals, Families & Employers (PCP or Specialist) Preventive Care Tests Diagnostic, Xray & Laboratory Emergency Room Surgery (Inpatient & Outpatient) Anesthesia Supplemental Accident for
PART V SCHEDULE OF BENEFITS MEDICAL EXPENSE BENEFITS DAVIDSON COLLEGE - STUDENT PLAN INJURY AND SICKNESS BENEFITS METALLIC LEVEL:
 PART V SCHEDULE OF BENEFITS MEDICAL EXPENSE BENEFITS DAVIDSON COLLEGE - STUDENT PLAN 2014-927-1 INJURY AND SICKNESS BENEFITS METALLIC LEVEL: Maximum Benefit Deductible Coinsurance Out-of-Pocket Maximum
PART V SCHEDULE OF BENEFITS MEDICAL EXPENSE BENEFITS DAVIDSON COLLEGE - STUDENT PLAN 2014-927-1 INJURY AND SICKNESS BENEFITS METALLIC LEVEL: Maximum Benefit Deductible Coinsurance Out-of-Pocket Maximum
INTERNATIONAL PRIVATE MEDICAL INSURANCE Insurance Product Information Document
 INTERNATIONAL PRIVATE MEDICAL INSURANCE Insurance Product Information Document Company: Cigna Life Insurance Company of Europe S.A.-N.V Product: Cigna Global Silver Cigna Life Insurance Company of Europe
INTERNATIONAL PRIVATE MEDICAL INSURANCE Insurance Product Information Document Company: Cigna Life Insurance Company of Europe S.A.-N.V Product: Cigna Global Silver Cigna Life Insurance Company of Europe
Open Access Value 2500A/70%
 BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
BENEFIT IN NETWORK OUT OF NETWORK This plan is intended to comply with the federal Patient Protection and Affordable Care Act. Provisions are subject to change as additional regulatory guidance becomes
PLAN DESIGN AND BENEFITS - Tx OAMC 3000 HSA 100% 08 PREFERRED CARE
 Aetna Life Insurance Company Texas Small Group MC Open Access Plan Effective Date: 09/01/2008 PLAN FEATURES NON- Deductible (per calendar year) $3,000 Individual $6,000 Individual $6,000 Family $12,000
Aetna Life Insurance Company Texas Small Group MC Open Access Plan Effective Date: 09/01/2008 PLAN FEATURES NON- Deductible (per calendar year) $3,000 Individual $6,000 Individual $6,000 Family $12,000
Highest level of coverage with free-choice of hospitals and physicians worldwide, with the richest maternity and organ transplant benefits.
 Highest level of coverage with free-choice of hospitals and physicians worldwide, with the richest maternity and organ transplant benefits. Global Superior Plus is tailored exclusively for individuals
Highest level of coverage with free-choice of hospitals and physicians worldwide, with the richest maternity and organ transplant benefits. Global Superior Plus is tailored exclusively for individuals
Unlimited except where indicated. Unlimited except where indicated. Primary Care Physician Selection
 PLAN FEATURES Deductible (per calendar year) $500 Individual $1,250 Individual $1,000 Family $2,500 Family All covered expenses excluding prescription drugs accumulate toward both the preferred and non-preferred
PLAN FEATURES Deductible (per calendar year) $500 Individual $1,250 Individual $1,000 Family $2,500 Family All covered expenses excluding prescription drugs accumulate toward both the preferred and non-preferred
IL Small Group MC Open Access Aetna Life Insurance Company Plan Effective Date: 04/01/2009 PLAN DESIGN AND BENEFITS- MC $1,500 80/50/50 (04/09)
 PLAN FEATURES Deductible (per calendar ) $1,500 Individual $3,000 Individual $4,500 Family $9,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered
PLAN FEATURES Deductible (per calendar ) $1,500 Individual $3,000 Individual $4,500 Family $9,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered
MANAGED HEALTHCARE SYSTEM (MHS) OUTPATIENT PLAN PRIVILEGES AND CONDITIONS
 MANAGED HEALTHCARE SYSTEM (MHS) OUTPATIENT PLAN PRIVILEGES AND CONDITIONS 1. Benefits We shall pay the following benefits as specified in the schedule if incurred by the member for any outpatient medical
MANAGED HEALTHCARE SYSTEM (MHS) OUTPATIENT PLAN PRIVILEGES AND CONDITIONS 1. Benefits We shall pay the following benefits as specified in the schedule if incurred by the member for any outpatient medical
Assurant Health Access SM
 Assurant Health Access SM Health. Within Reach. Indiana, Kentucky, Maine, Minnesota, Nevada, Oregon and West Virginia Time Insurance Company Assurant Health is the brand name for products underwritten
Assurant Health Access SM Health. Within Reach. Indiana, Kentucky, Maine, Minnesota, Nevada, Oregon and West Virginia Time Insurance Company Assurant Health is the brand name for products underwritten
Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018
 Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018 Payment for Services Covered Services are reimbursed based on the Allowable Charge. Blue Cross
Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018 Payment for Services Covered Services are reimbursed based on the Allowable Charge. Blue Cross
SUBLUE AND SUORANGE: 2018 SCHEDULE OF BENEFITS -EMPLOYEE COST SHARING
 Cost Sharing Definitions Annual Deductible 1 (amounts are not cumulative across levels) $100 per individual with a maximum of $250 for a family $300 per individual with a maximum of $1,000 for a family
Cost Sharing Definitions Annual Deductible 1 (amounts are not cumulative across levels) $100 per individual with a maximum of $250 for a family $300 per individual with a maximum of $1,000 for a family
Regence Classic Plan Highlights For Groups of /1/2017
 Plan Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for In- Network providers. If a member chooses an Out-of-Network provider, the member
Plan Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for In- Network providers. If a member chooses an Out-of-Network provider, the member
PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived 30% after deductible
 PLAN FEATURES NON- Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred
PLAN FEATURES NON- Deductible (per calendar year) $1,500 Individual $1,500 Individual $3,000 Family $3,000 Family All covered expenses, including prescription drugs, accumulate toward both the preferred
Covered 100%; deductible waived 35%; after deductible
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $300 Individual $1,000 Individual $600 Family $2,000 Family All covered expenses accumulate simultaneously toward both the preferred and non-preferred
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $300 Individual $1,000 Individual $600 Family $2,000 Family All covered expenses accumulate simultaneously toward both the preferred and non-preferred
FAQs for Incoming Yale Summer Session Students
 FAQs for Incoming Yale Summer Session Students How long am I covered? A: The plan covers you for the period of international travel required by your academic plans and for which you are enrolled. What
FAQs for Incoming Yale Summer Session Students How long am I covered? A: The plan covers you for the period of international travel required by your academic plans and for which you are enrolled. What
PLAN DESIGN AND BENEFITS - Tx OAMC % 08 PREFERRED CARE
 Aetna Life Insurance Company Texas Small Group MC Open Access Plan Effective Date: 11/01/2008 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Individual $3,000 3 Individuals per $9,000
Aetna Life Insurance Company Texas Small Group MC Open Access Plan Effective Date: 11/01/2008 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Individual $3,000 3 Individuals per $9,000
Covered 100%; deductible waived 40%; after deductible
 HEALTH SAVINGS ACCOUNT Employer HSA Contribution Barnes Group Inc. $500 Individual $1,000 Family The amount reflected is on a per calendar year basis. The amount received may be prorated based on your
HEALTH SAVINGS ACCOUNT Employer HSA Contribution Barnes Group Inc. $500 Individual $1,000 Family The amount reflected is on a per calendar year basis. The amount received may be prorated based on your
Evolution Health Plan Table of benefits
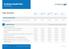 Evolution Health Plan Table of benefits Standard Standard Plus Comprehensive Premium Elite Overall maximum limit This is the maximum amount of money we will pay to, or on behalf of, each insured person
Evolution Health Plan Table of benefits Standard Standard Plus Comprehensive Premium Elite Overall maximum limit This is the maximum amount of money we will pay to, or on behalf of, each insured person
PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY - SELF FUNDED
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) None Individual $500 Individual None Family $1,000 Family Unless otherwise indicated, the deductible must be met prior to benefits
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) None Individual $500 Individual None Family $1,000 Family Unless otherwise indicated, the deductible must be met prior to benefits
PREFERRED CARE. Covered 100%; deductible waived. Covered 100%; deductible waived
 PLAN FEATURES Deductible (per calendar year) $500 Individual $500 Individual $1,500 Family $1,500 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and non-preferred
PLAN FEATURES Deductible (per calendar year) $500 Individual $500 Individual $1,500 Family $1,500 Family All covered expenses, including prescription drugs, accumulate toward both the preferred and non-preferred
Membership handbook Health Perfect and Secure Series - Abu Dhabi
 health insurance Membership handbook Health Perfect and Secure Series - Abu Dhabi what you need to know Contents Section Page No. 1. Introduction 1 2. Important note about pre-existing conditions 3 3.
health insurance Membership handbook Health Perfect and Secure Series - Abu Dhabi what you need to know Contents Section Page No. 1. Introduction 1 2. Important note about pre-existing conditions 3 3.
OUTLINE OF COVERAGE. Blue Choice PPO Bronze 005
 OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your Policy. This is not the insurance contract, and only the actual
OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your Policy. This is not the insurance contract, and only the actual
An Overview of Your Health and Dental Benefits
 An Overview of Your Health and Dental Benefits Educators Health Alliance Direct Bill Plan 2 \ EDUCATORS HEALTH ALLIANCE HEALTH AND DENTAL PLAN OPTIONS Exclusively for Educators Health Alliance Direct Bill
An Overview of Your Health and Dental Benefits Educators Health Alliance Direct Bill Plan 2 \ EDUCATORS HEALTH ALLIANCE HEALTH AND DENTAL PLAN OPTIONS Exclusively for Educators Health Alliance Direct Bill
Covered 100%; deductible waived 50%; after deductible
 HEALTH SAVINGS ACCOUNT Employer HSA Contribution Barnes Group Inc. HSA Value Plan Employee Only $250 Individual Not Applicable Family The amount reflected is on a per calendar year basis. The amount received
HEALTH SAVINGS ACCOUNT Employer HSA Contribution Barnes Group Inc. HSA Value Plan Employee Only $250 Individual Not Applicable Family The amount reflected is on a per calendar year basis. The amount received
PREFERRED CARE. Covered 100%; deductible waived Not Covered
 PLAN FEATURES NON- Deductible (per calendar year) $1,300 Individual $1,300 Individual $2,600 Family $2,600 Family All covered expenses including prescription drugs accumulate toward both the preferred
PLAN FEATURES NON- Deductible (per calendar year) $1,300 Individual $1,300 Individual $2,600 Family $2,600 Family All covered expenses including prescription drugs accumulate toward both the preferred
PRIVILEGES AND CONDITIONS
 PRIVILEGES AND CONDITIONS 1. Benefits We shall pay the benefits as specified in the schedule if a member incurs medical expenses due to illness or injury for primary care, specialist care or hospital care
PRIVILEGES AND CONDITIONS 1. Benefits We shall pay the benefits as specified in the schedule if a member incurs medical expenses due to illness or injury for primary care, specialist care or hospital care
PLAN DESIGN & BENEFITS
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) $250 Individual $500 Individual $500 Family $1,000 Family All covered expenses accumulate separately toward the preferred or non-preferred
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) $250 Individual $500 Individual $500 Family $1,000 Family All covered expenses accumulate separately toward the preferred or non-preferred
Benefit Network Non-Network * DEDUCTIBLE. Individual Not Applicable $2,000. Family Not Applicable $4,000. Individual $5,000 $15,000
 AmeriHealth POS POS $30/$50 $0/Day SEH Summary of Benefits AmeriHealth Point-of-Service lets you maintain Freedom of Choice by allowing you to select your own doctors and hospitals. You maximize your coverage
AmeriHealth POS POS $30/$50 $0/Day SEH Summary of Benefits AmeriHealth Point-of-Service lets you maintain Freedom of Choice by allowing you to select your own doctors and hospitals. You maximize your coverage
California Small Group MC Aetna Life Insurance Company NETWORK CARE
 PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
PLAN FEATURES Deductible (per calendar year) Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward the preferred and non-preferred
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING NO-REFERRAL 4.4 ($2,000 DED) $2,000 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $4,000 Individual $8,000 Family 50% $8,000 Individual $16,000 Family Amounts over the Recognized Charge, failure to pre-certification
Keller ISD - Essential Plan
 Keller ISD - Essential Plan - 2014 The Essential plan gives you the freedom to see any Physician or other health care professional from the Network, including specialists, without a referral. With this
Keller ISD - Essential Plan - 2014 The Essential plan gives you the freedom to see any Physician or other health care professional from the Network, including specialists, without a referral. With this
PLAN DESIGN AND BENEFITS - PA POS COST-SHARING 3.4 ($1,500 DED) PARTICIPATING PROVIDERS. $1,500 Individual
 Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
Plan Coinsurance * Out-of-Pocket Maximum (per calendar year, includes deductible) $3,000 Individual $6,000 Family 50% $6,000 Individual $12,000 Family Amounts over the Recognized Charge, failure to pre-certification
Unlimited/ $1,000,000 per lifetime Primary Care Physician Selection
 PLAN FEATURES Deductible (per calendar year) None Individual None Family Member Coinsurance Out-of-Pocket Maximum $1,500 $3,000 Individual (per calendar year) $3,000 $6,000 Family Member cost sharing for
PLAN FEATURES Deductible (per calendar year) None Individual None Family Member Coinsurance Out-of-Pocket Maximum $1,500 $3,000 Individual (per calendar year) $3,000 $6,000 Family Member cost sharing for
PLAN DESIGN. Customer Name: Michael Page International Inc. Proposed Effective Date: Policy Period: 12
 PLAN DESIGN Customer Name: Policy Period: 12 Data Source ID: Q3148813-4 - All Employees/357NYMCOA#2171 Option: MCOA plan alt Plan: Open POS Plus Plan Location(s): New York Specialty Networks Included:
PLAN DESIGN Customer Name: Policy Period: 12 Data Source ID: Q3148813-4 - All Employees/357NYMCOA#2171 Option: MCOA plan alt Plan: Open POS Plus Plan Location(s): New York Specialty Networks Included:
Your Summary of Benefits Premier PPO
 Your Summary of Benefits Premier PPO Small Group Premier PPO $20 Copay Plan Effective 10/2011 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about
Your Summary of Benefits Premier PPO Small Group Premier PPO $20 Copay Plan Effective 10/2011 This Summary of Benefits is a brief overview of your plan's benefits only. For more detailed information about
Regence EmployeeChoice Plan Highlights Platinum+, Platinum, Gold 500, Gold+, Gold, Gold Simple, Silver, Silver Simple For Groups of /1/2015
 Plan Features Provider choice: Member coinsurance levels are lowest for In-Network providers. If a member chooses an Out-of-Network provider, the member may be required to pay costs above the allowed amount.
Plan Features Provider choice: Member coinsurance levels are lowest for In-Network providers. If a member chooses an Out-of-Network provider, the member may be required to pay costs above the allowed amount.
PLAN DESIGN AND BENEFITS - Choice POS % - 08 PARTICIPATING PROVIDERS. $1,500 Individual $4,500 Family
 Aetna Health Inc Texas Small Group Open Access Plan Effective Date: 11/01/2008 PLAN FEATURES Deductible (per calendar year) PARTICIPATING $1,500 Individual $4,500 Family $3,000 Individual $9,000 Family
Aetna Health Inc Texas Small Group Open Access Plan Effective Date: 11/01/2008 PLAN FEATURES Deductible (per calendar year) PARTICIPATING $1,500 Individual $4,500 Family $3,000 Individual $9,000 Family
Anthem Blue Cross Effective: January 1, 2018 Your Plan: University of California UC Care Plan Your Network: UC Select and Anthem Preferred
 Anthem Blue Cross Effective: January 1, 2018 Your Plan: University of California UC Care Plan Your Network: UC Select and Anthem Preferred This summary of benefits is a brief outline of coverage, designed
Anthem Blue Cross Effective: January 1, 2018 Your Plan: University of California UC Care Plan Your Network: UC Select and Anthem Preferred This summary of benefits is a brief outline of coverage, designed
PLAN DESIGN AND BENEFITS MC Open Access Plan 1913
 PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year) $1,500 Individual $4,500 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior
PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year) $1,500 Individual $4,500 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior
FAQs FOR YALE STUDENTS TRAVELING OVERSEAS
 FOR YALE STUDENTS TRAVELING OVERSEAS How long am I covered? A: The plan covers you for the period of international travel associated with your semester or study trip abroad required by your academic plans
FOR YALE STUDENTS TRAVELING OVERSEAS How long am I covered? A: The plan covers you for the period of international travel associated with your semester or study trip abroad required by your academic plans
COMPARING BUPA GLOBAL LIFELINE PLANS
 This is intended as a summary comparison of the available benefits Full details of the benefits, limitations and exclusions for each plan in the Lifeline range can be found in the Lifeline membership guide.
This is intended as a summary comparison of the available benefits Full details of the benefits, limitations and exclusions for each plan in the Lifeline range can be found in the Lifeline membership guide.
Florida Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012
 Florida 2-100 Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOption Plan 12-2000-70 PLAN FEATURES PARTICIPATING PROVIDERS
Florida 2-100 Health Network Option (POS Open Access) Aetna Life Insurance Company Plan Effective Date: 03/01/2012 PLAN DESIGN AND BENEFITS HNOption Plan 12-2000-70 PLAN FEATURES PARTICIPATING PROVIDERS
Recommended: One baseline mammogram for females age 35-39; and one annual mammogram for females age 40 and over.
 PLAN FEATURES Deductible (per calendar year) $2,000 Individual $4,000 Family Unless otherwise indicated, the deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN FEATURES Deductible (per calendar year) $2,000 Individual $4,000 Family Unless otherwise indicated, the deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY - SELF FUNDED
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) $3,000 Individual $3,000 Individual $6,000 Family $6,000 Family All covered expenses accumulate separeately toward the preferred or
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) $3,000 Individual $3,000 Individual $6,000 Family $6,000 Family All covered expenses accumulate separeately toward the preferred or
Regence HSA Healthplan 2.0 (100%) Plan Highlights For Groups of 51+ 1/1/2015
 Plan Features The Regence HSA Healthplan 2.0 is a simple way to pay for life s medical expenses. Comprehensive health plan combined with a separate tax free savings account provides a simple way to pay
Plan Features The Regence HSA Healthplan 2.0 is a simple way to pay for life s medical expenses. Comprehensive health plan combined with a separate tax free savings account provides a simple way to pay
Covered 100%; deductible waived 50%; after deductible
 HEALTH SAVINGS ACCOUNT Employer HSA Contribution BARNES GROUP INC. HSA Value Plan Employee Only $250 Individual Not Applicable Family The amount reflected is on a per calendar year basis. The amount received
HEALTH SAVINGS ACCOUNT Employer HSA Contribution BARNES GROUP INC. HSA Value Plan Employee Only $250 Individual Not Applicable Family The amount reflected is on a per calendar year basis. The amount received
PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA HEALTH INSURANCE COMPANY - SELF-FUNDED
 PLAN FEATURES Deductible (per plan year) None Individual None Family Member Coinsurance Covered 100% Applies to all expenses unless otherwise stated. Out-of-pocket limit (per plan year) $6,350 Individual
PLAN FEATURES Deductible (per plan year) None Individual None Family Member Coinsurance Covered 100% Applies to all expenses unless otherwise stated. Out-of-pocket limit (per plan year) $6,350 Individual
I. PLAN DESCRIPTIONS. A. POS Point of Service
 I. PLAN DESCRIPTIONS A. POS Point of Service The Partnership Plan offers a single point of service plan to provide healthcare services both within and outside a defined network of Providers. No referrals
I. PLAN DESCRIPTIONS A. POS Point of Service The Partnership Plan offers a single point of service plan to provide healthcare services both within and outside a defined network of Providers. No referrals
Build your own kind of healthy Pioneer Dubai 4000 and 5000 Benefits schedule
 Build your own kind of healthy and 5000 Benefits schedule USD For plans with a start date on or after 1 January 2016 Visit www.alaininsurance.com or www.aetnainternational.com M015-178E-300816 1 Whether
Build your own kind of healthy and 5000 Benefits schedule USD For plans with a start date on or after 1 January 2016 Visit www.alaininsurance.com or www.aetnainternational.com M015-178E-300816 1 Whether
PLAN DESIGN & BENEFITS ADMINISTERED BY AETNA LIFE INSURANCE COMPANY - SELF FUNDED
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) $3000 Individual $6,000 Individual $6000 Family $12,000 Family All covered expenses accumulate separately toward the preferred or
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible (per calendar year) $3000 Individual $6,000 Individual $6000 Family $12,000 Family All covered expenses accumulate separately toward the preferred or
Hospital Expense Protection
 Available with doctor visit and laboratory benefits Hospital Expense Protection Stay one step ahead with set, cash benefits to help you pay for medical expenses in and out of the hospital National General
Available with doctor visit and laboratory benefits Hospital Expense Protection Stay one step ahead with set, cash benefits to help you pay for medical expenses in and out of the hospital National General
ARIZONA. CIGNA health savings plans. Health and Pharmacy Benefits a AZ 1/ CIGNA
 ARIZONA Individual & Family Plans CIGNA health savings plans Health and Pharmacy Benefits PLAN comparison 827693a AZ 1/10 2010 CIGNA CIGNA HealthCare plans, offered through Connecticut General Life Insurance
ARIZONA Individual & Family Plans CIGNA health savings plans Health and Pharmacy Benefits PLAN comparison 827693a AZ 1/10 2010 CIGNA CIGNA HealthCare plans, offered through Connecticut General Life Insurance
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
PLAN FEATURES Deductible (per calendar year) $5,000 Individual $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate toward
Regence Innova Plan Highlights For Groups of /1/2016
 Regence Innova Highlights Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for providers. If a member chooses a Category 3 provider, the
Regence Innova Highlights Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for providers. If a member chooses a Category 3 provider, the
ARIZONA. CIGNA health savings plans sm. Health and Pharmacy Benefits AZ 06/08
 ARIZONA Individual & Family Plans CIGNA health savings plans sm Health and Pharmacy Benefits PLAN comparison 820521 AZ 06/08 CIGNA HealthCare plans, offered through Connecticut General Life Insurance Company,
ARIZONA Individual & Family Plans CIGNA health savings plans sm Health and Pharmacy Benefits PLAN comparison 820521 AZ 06/08 CIGNA HealthCare plans, offered through Connecticut General Life Insurance Company,
Regence Classic Plan Highlights (Standard) For Groups of 51+ 1/1/2018
 Plan Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for In- Network providers. If a member chooses an Out-of-Network provider, the member
Plan Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for In- Network providers. If a member chooses an Out-of-Network provider, the member
THE MITRE CORPORATION PPO High Deductible Plan with a Health Saving Account (HSA)
 THE MITRE CORPORATION PPO High Deductible Plan with a Health Saving Account (HSA) Effective Date: 01-01-2016 PLAN FEATURES Annual Deductible $1,500 Employee $3,000 Employee $3,000 Employee + 1 Dependent
THE MITRE CORPORATION PPO High Deductible Plan with a Health Saving Account (HSA) Effective Date: 01-01-2016 PLAN FEATURES Annual Deductible $1,500 Employee $3,000 Employee $3,000 Employee + 1 Dependent
