high deductible health plan basic
|
|
|
- Rodger Horn
- 6 years ago
- Views:
Transcription
1 high deductible health plan basic The Chevron HDHP Basic (HDHP Basic) is a new plan choice that will be offered in With this plan, you pay a low monthly premium in exchange for a high deductible. Participants enrolled in the HDHP Basic may also be eligible to open and contribute to a health savings account (HSA). This section provides more detail about the new HDHP Basic that will be offered to pre 65 eligible retirees and their pre 65 eligible dependents effective January 1, It s provided to help you make enrollment decisions and understand how this plan works. the basics You can enroll in the HDHP Basic if you re a pre 65 eligible retiree and you re eligible for Chevron retiree health and welfare benefits. You can also enroll your pre 65 eligible dependents, just as you can with Chevron s other health plans. The HDHP Basic is a preferred provider organization (PPO) health plan. You can choose to see any provider you want; however, higher benefits are paid when you go to a network provider. The HDHP Basic generally covers the same services as the Chevron High Deductible Health Plan (HDHP). The primary difference between the two plan options are your out-of-pocket costs: the premiums, deductibles and coinsurance. There are important differences in how a high deductible health plan works that will change how you pay for medical, prescription drug, mental health and substance abuse services under this plan. We ll discuss the differences later in this section. The HDHP Basic includes: Medical coverage with Anthem Blue Cross (Anthem). Prescription drug coverage with Express Scripts. Mental health substance abuse coverage with Beacon Health Options, as long as you aren t eligible for Medicare. In addition, if you enroll in the HDHP Basic, you re also automatically enrolled in the Vision Program for basic vision coverage with VSP. low monthly premium, high deductible The HDHP Basic monthly premium cost is the lowest cost plan choice offered by Chevron. If you typically choose your medical plan by monthly premium alone, be sure you understand the trade-off for a low monthly premium before you enroll: a high deductible. While most of the deductibles under all of Chevron s pre 65 retiree medical plans will increase in 2017, the HDHP Basic annual deductible is higher than all the other medical plan options Chevron provides. You have to satisfy the deductible with money out of your own pocket before the HDHP Basic begins to share the cost of covered medical services through coinsurance. Chevron will currently continue to share the monthly cost of coverage the premium with you. The HR Service Center will mail a personalized open enrollment worksheet to you under separate cover in early October. The worksheet includes the 2017 cost for coverage for pre 65 eligible participants. Chevron s company contribution to retiree medical coverage for all non-medicare medical plans for 2017 will remain the same amount as for U.S. Retiree Benefit News 24
2 how the HDHP basic is similar to other plan choices The HDHP Basic offers comprehensive coverage for the same major medical services you d expect, including office visits, emergency services, hospital care, lab services, outpatient care, pregnancy and newborn care and rehabilitative services. It also includes 100 percent coverage with no deductible for certain preventive care services, as specified by the Affordable Care Act, when you see a network provider. Additional preventive screenings and services may also be covered, depending on factors like your age and gender. If you see an out-ofnetwork provider, your visit is subject to the deductible and coinsurance will apply. If you are enrolled in the HDHP Basic, you automatically have prescription drug coverage through the Prescription Drug Program with Express Scripts. For additional summary information about the new HDHP Basic, such as benefits, deductibles, coinsurance and plan contact information, review the plan s Summary of Benefits and Coverage available on hr2.chevron.com/retiree. health savings account compatible (HSA) If you enroll in the HDHP Basic, you may also be eligible to open and contribute to a health savings account (HSA). Enrollment in the HDHP Basic gives you the keys to open an HSA, but it s your responsibility to determine if you re eligible, choose an HSA provider and then open and contribute to an account. Participation in an HSA is voluntary and is subject to strict enrollment requirements governed by the IRS. For example, you are not eligible to enroll in an HSA if you have coverage under another medical plan, including Medicare, unless it s another high deductible health plan or other permitted coverage. If you are enrolled in Medicare, you cannot open or continue to contribute to an HSA; however you can continue to use existing HSA funds to pay for qualified health care expenses. Consult your tax advisor and read about the requirements in IRS Publication 969, available at to determine if you meet the requirements to open and contribute to an HSA. The IRS limits how much you can contribute to an HSA for each year. For 2017 the IRS HSA contribution limits are: Individual: $3,400 Family: $6,750 You are allowed to make an extra $1,000 in catch-up contributions starting in the calendar year in which you turn age 55. October
3 annual combined deductible Medical, prescription drug, mental health and substance abuse services, combined The HDHP Basic has one combined deductible for medical, prescription drugs (both retail and mail-order), mental health and substance abuse services. This means you ll have to pay the full cost for covered services and supplies until you reach the deductible for the year. After you meet the deductible, coinsurance will apply. There are different deductible amounts for covered services depending on if you see a network or an out-of-network provider. Amounts paid for covered services provided by a network provider also count toward the out-of-network annual deductible. Amounts paid for covered services provided by an out-of-network provider also count toward the network annual deductible. + Coverage Category Network Out-of-Network You only $5,000 $10,000 You + One adult $10,000 $20,000 You + Child(ren) $10,000 $20,000 You + Family $10,000 $20,000 Each covered individual has a maximum deductible equal to the You only amount. annual combined out-of-pocket maximum Medical, prescription drug, mental health and substance abuse services, combined The HDHP Basic has one combined out-of-pocket maximum for medical, prescription drugs (both retail and mailorder), mental health and substance abuse services. The out-of-pocket maximum is the most you will have to pay out-of-pocket for the year for covered services and supplies. When you reach this limit, the HDHP Basic begins to pay 100 percent of the maximum allowable amounts for covered services and supplies. There are different out-ofpocket maximums depending on if you see a network provider or an out-of-network provider. Amounts paid for covered services provided by a network provider also count toward the out-of-network maximum. Amounts paid for covered services provided by an out-of-network provider also count toward the network maximum. + Coverage Category Network Out-of-Network You only $6,550 $13,100 You + One adult $13,100 $26,200 You + Child(ren) $13,100 $26,200 You + Family $13,100 $26,200 Each covered individual has an out-of-pocket maximum equal to the You only amount. U.S. Retiree Benefit News 26
4 coinsurance amounts for covered medical services The HDHP Basic has different coinsurance amounts for covered medical services depending on if you see a network or an out-of-network provider. It s your choice to use any provider you want, but it s important to know that using a network provider will save you money. The HDHP Basic will include 100 percent coverage with no copayment, coinsurance or deductible for certain preventive care services, as specified by the Affordable Care Act, when you see a network provider. If you see an out-of-network provider you ll pay 50 percent of maximum allowable amounts and the annual combined deductible will apply. If you visit a network provider, you ll pay 30 percent of maximum allowable amounts, and the plan will pay 70 percent, after you ve met your annual combined deductible, unless otherwise stated. If you visit an out-of-network provider, you ll pay 50 percent of maximum allowable amounts, and the plan will pay 50 percent, after you ve met your annual combined deductible, unless otherwise stated. You ll pay 30 percent of the cost for covered prescription drugs retail and mail-order after you ve met your annual combined deductible, unless otherwise stated. There are specific procedures and services for which you re required to notify the claims administrator in accordance with timelines identified in plan rules. Starting in 2017, if you fail to meet the HDHP Basic s notification requirements for these procedures and services, then you will pay 40 percent of maximum allowable amounts from a network provider or 50 percent of maximum allowable amounts from an out-ofnetwork provider, after you ve met your annual combined deductible, unless otherwise stated. For emergency room visits, you ll pay 30 percent of maximum allowable amounts, network or out-of-network, after you ve met your annual combined deductible, unless otherwise stated. Anthem defines a primary care provider as any of the following: Family Practice, General Practitioner, Pediatrician, Internal Medicine, OB/GYNs, GYNs, Certified Nurse Midwife, Nurse Practitioner, Physician Assistant, and Clinical/Multi Specialty Group. All other professional providers are considered specialists. If you see a network primary care provider, you ll pay 30 percent of maximum allowable amounts for the office visit, after you ve met your annual combined deductible, unless otherwise stated. If you see an out-of-network primary care provider, you ll pay 50 percent of maximum allowable amounts for the office visit, after you ve met your annual combined deductible, unless otherwise stated. If you see a network specialist, you ll pay 30 percent of maximum allowable amounts for the office visit, after you ve met your annual combined deductible, unless otherwise stated. If you see an out-of-network specialist, you ll pay 50 percent of maximum allowable amounts for the office visit, after you ve met your annual combined deductible, unless otherwise stated. October
5 prescription drug program If you are enrolled in the Medical PPO Plan, the High Deductible Health Plan (HDHP) or the new High Deductible Health Plan Basic (HDHP Basic), you automatically have prescription drug coverage through the Prescription Drug Program with Express Scripts. The Prescription Drug Program currently has prior authorization, preferred step therapy and drug quantity management programs in place, but these programs will be expanding in This is an administrative change only; you don t need to do anything as a result of this change. The Prescription Drug Program covers some drugs only if they re prescribed for certain uses (or only up to certain quantity levels). For this reason, some medications will require your prescribing doctor to provide additional clinical information so that use of the medication can be approved in advance before you can receive Prescription Drug Program benefits. This is called prior authorization. Certain drugs are covered by the Prescription Drug Program only if preferred drugs which include generics are tried first. This is called Preferred Step Therapy. If your medication is subject to Preferred Step Therapy, this means that you will be required, when clinically appropriate, to try a preferred drug before Express Scripts will authorize coverage for the use of non-preferred drugs. Drug Quantity Management is a program included in the Prescription Drug Program that s designed to make the use of prescription drugs safer and more affordable. It provides you with medicines you need for your good health and the health of your covered dependents, while making sure you receive them in the amount or quantity considered safe and most cost effective. You ll be notified by Express Scripts if your medication is subject to any of these programs in 2017, including what you need to do, if anything. Starting October 17, 2016, to find out if your prescription drug is subject to prior authorization, Preferred Step Therapy and Drug Quantity Management programs, contact Express Scripts Member Services at , or review the documents and links available from hr2.chevron.com/retiree. Click the 2017 Benefit Changes link to get started. U.S. Retiree Benefit News 14
6 Human Energy. Yours. TM Update to the Summary Plan Description Effective January 1, 2017 All changes described in this SMM are effective January 1, 2017 unless otherwise indicated. This enclosed newsletter serves as an official summary of material modification (SMM) for the plans referenced herein. Please keep this information with your other plan documents for future reference. This communication provides only certain highlights about changes of benefit provisions. It is not intended to be a complete explanation. If there are any discrepancies between this communication and the legal plan documents, the legal plan documents will prevail to the extent permitted by law. There are no vested rights with respect to Chevron health care plans or any company contributions towards the cost of such health care plans. Rather, Chevron Corporation reserves all rights, for any reason and at any time, to amend, change or terminate these plans or to change or eliminate the company contribution toward the cost of such plans. Such amendments, changes, terminations or eliminations may be applicable without regard to whether someone previously terminated employment with Chevron or previously was subject to a grandfathering provision. Some benefit plans and policies described in this document may be subject to collective bargaining and, therefore, may not apply to unionrepresented employees. You can access the summary plan descriptions for your benefits on the Internet at hr2.chevron.com/retiree or by calling the HR Service Center at ( if you re outside the U.S.), option 2. This SMM applies to the following summary plan description: January 1, 2017 High Deductible Health Plan Basic (HDHP Basic) Summary Plan Description January 1, 2017 Official Summary of Material Modification (SMM)
7 Important Correction U.S. Retiree Benefits Newsletter, Open Enrollment is Here September 2016 The High Deductible Health Plan Basic section of the newsletter/summary material modification incorrectly listed temporomandibular joint (TMJ) disorder as having a lifetime maximum under the plan. The correct statement about lifetime maximums under the plan is listed below. Lifetime Maximum This plan has a lifetime maximum for the following three services: family planning services, transportation and lodging incurred by a transplant recipient and companion(s), and nutritional counseling covered by the plan. Any amounts incurred by the plan participant that count toward the lifetime maximum while UnitedHealthcare was the claims administrator will carry over and also apply toward the lifetime maximum while Anthem Blue Cross is the claims administrator. January 1, 2017 Official Summary of Material Modification (SMM)
medical PPO plan Find a provider medical PPO option 1 no longer offered New monthly premium cost prescription drug program
 medical PPO plan Aside from the switch to a new claims administrator Anthem Blue Cross this section provides more detail about other changes to the Chevron Medical PPO Plan that will be offered to pre
medical PPO plan Aside from the switch to a new claims administrator Anthem Blue Cross this section provides more detail about other changes to the Chevron Medical PPO Plan that will be offered to pre
medical PPO plan tobacco surcharge new monthly premium cost second opinion for certain surgeries Medical PPO Plan
 medical PPO plan Aside from the switch to a new claims administrator (see Page 5) Anthem Blue Cross this section provides more detail about other changes to the Chevron Medical PPO Plan that will be offered
medical PPO plan Aside from the switch to a new claims administrator (see Page 5) Anthem Blue Cross this section provides more detail about other changes to the Chevron Medical PPO Plan that will be offered
Update to the Summary Plan Description Effective March 1, 2019
 Human Energy. Yours. TM Update to the Summary Plan Description Effective March 1, 2019 All changes described in this SMM are effective March 1, 2019. This enclosed document serves as an official summary
Human Energy. Yours. TM Update to the Summary Plan Description Effective March 1, 2019 All changes described in this SMM are effective March 1, 2019. This enclosed document serves as an official summary
Update to the Summary Plan Description Effective March 1, 2019
 Human Energy. Yours. TM Update to the Summary Plan Description Effective March 1, 2019 All changes described in this SMM are effective March 1, 2019. This enclosed document serves as an official summary
Human Energy. Yours. TM Update to the Summary Plan Description Effective March 1, 2019 All changes described in this SMM are effective March 1, 2019. This enclosed document serves as an official summary
Update to the Summary Plan Description Effective January 1, 2017
 Human Energy. Yours. TM Update to the Summary Plan Description Effective January 1, 2017 All changes described in this SMM are effective January 1, 2017 unless otherwise indicated. This enclosed newsletter
Human Energy. Yours. TM Update to the Summary Plan Description Effective January 1, 2017 All changes described in this SMM are effective January 1, 2017 unless otherwise indicated. This enclosed newsletter
mental health and substance abuse plan (MHSA) changes to your benefits that take effect january 1, 2017
 mental health and substance abuse plan (MHSA) changes to your benefits that take effect january 1, 2017 U.S. Pay and Benefit News 34 The Mental Health and Substance Abuse (MHSA) Plan, administered by Beacon
mental health and substance abuse plan (MHSA) changes to your benefits that take effect january 1, 2017 U.S. Pay and Benefit News 34 The Mental Health and Substance Abuse (MHSA) Plan, administered by Beacon
Medical and Dental HMO Summary Plan Description (SPD) Effective January 1, 2014
 Human Energy. Yours. TM Medical and Dental HMO (SPD) Effective January 1, 2014 Effective January 1, 2014 COBRA/Continuation Coverage Page 1 This document provides information about the Medical and Dental
Human Energy. Yours. TM Medical and Dental HMO (SPD) Effective January 1, 2014 Effective January 1, 2014 COBRA/Continuation Coverage Page 1 This document provides information about the Medical and Dental
2018 chevron benefit changes
 2018 chevron benefit changes This section includes information about changes to your Chevron benefits that take effect on January 1, 2018. Certain sections of this newsletter (Page 8-33) serve as an official
2018 chevron benefit changes This section includes information about changes to your Chevron benefits that take effect on January 1, 2018. Certain sections of this newsletter (Page 8-33) serve as an official
good to know health and welfare benefits when you leave chevron excerpts
 good to know health and welfare benefits when you leave chevron excerpts human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the
good to know health and welfare benefits when you leave chevron excerpts human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the
good to know health and welfare benefits when you leave chevron
 good to know health and welfare benefits when you leave chevron human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the steps you
good to know health and welfare benefits when you leave chevron human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the steps you
good to know medicare and your chevron retiree health coverage human energy. yours. TM
 good to know medicare and your chevron retiree health coverage human energy. yours. TM This information is a general overview intended to cover some but not all situations. This overview assumes you are
good to know medicare and your chevron retiree health coverage human energy. yours. TM This information is a general overview intended to cover some but not all situations. This overview assumes you are
Retiree Medical and Life Insurance
 Retiree Medical and Life Insurance Eligibility Full-time employees are eligible for retiree medical and life insurance based on their date of employment: o Before July 1, 2004. You are eligible for retiree
Retiree Medical and Life Insurance Eligibility Full-time employees are eligible for retiree medical and life insurance based on their date of employment: o Before July 1, 2004. You are eligible for retiree
UnitedHealthcare OPTIMUM CHOICE HMO PLAN with a HEALTH SAVINGS ACCOUNT
 Medical UnitedHealthcare OPTIMUM CHOICE HMO PLAN PLAN FEATURES } A referral-based plan where you work closely with your primary care physician for appropriate, cost-effective care } A strong local network
Medical UnitedHealthcare OPTIMUM CHOICE HMO PLAN PLAN FEATURES } A referral-based plan where you work closely with your primary care physician for appropriate, cost-effective care } A strong local network
good to know health and welfare benefits when you leave chevron excerpts
 good to know health and welfare benefits when you leave chevron excerpts human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the
good to know health and welfare benefits when you leave chevron excerpts human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the
Medical Plan. Comparison
 Medical Plan Comparison 2018 ATTENTION: This Medical Plan Comparison is considered a summary of material modifications (SMM) to one or more of the WHOI benefit plans. It contains a summary of important
Medical Plan Comparison 2018 ATTENTION: This Medical Plan Comparison is considered a summary of material modifications (SMM) to one or more of the WHOI benefit plans. It contains a summary of important
Your Plan: 2018 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO
 Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2018 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2018 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
Your Plan: 2017 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO
 Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2017 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
Anthem Blue Cross ACWA JPIA C00361 Your Plan: 2017 Advantage PPO Plan (1VYX) Medical benefits only plan for Retirees with Medicare A&B Your Network: Prudent Buyer PPO This summary of benefits is a brief
good to know health and welfare benefits when you leave chevron excerpts
 good to know health and welfare benefits when you leave chevron excerpts human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the
good to know health and welfare benefits when you leave chevron excerpts human energy. yours. TM This overview is provided to help you understand how your health and welfare benefits may change and the
2016 Benefit Administrators Meeting
 2016 Benefit Administrators Meeting Affordable Care Act (ACA or PPACA) and Grandfathered Plan Status The Archdiocese Plan is a self-funded Grandfathered plan and will remain Grandfathered for 2017. Grandfathered
2016 Benefit Administrators Meeting Affordable Care Act (ACA or PPACA) and Grandfathered Plan Status The Archdiocese Plan is a self-funded Grandfathered plan and will remain Grandfathered for 2017. Grandfathered
Your Plan: Lumenos HSA Embedded Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Lumenos HSA Embedded Your Network: Prudent Buyer PPO City of Chico This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Lumenos HSA Embedded Your Network: Prudent Buyer PPO City of Chico This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
EMPLOYEE BENEFIT NEWSLETTER
 EMPLOYEE BENEFIT NEWSLETTER BENEFIT INFORMATION Parkway School District s employee benefit plans renew January 1, 2014, which means it is time for the Annual Enrollment period. Our benefit package includes
EMPLOYEE BENEFIT NEWSLETTER BENEFIT INFORMATION Parkway School District s employee benefit plans renew January 1, 2014, which means it is time for the Annual Enrollment period. Our benefit package includes
Summary of Benefits. Albemarle Select KeyCare PPO
 Summary of Benefits Albemarle Select KeyCare PPO Effective October 1, 2018-December 31, 2019 Anthem KeyCare 25 PPO - Albemarle Select plan 10/01/18-12/31/19 In-Network Services Preventive Care Services
Summary of Benefits Albemarle Select KeyCare PPO Effective October 1, 2018-December 31, 2019 Anthem KeyCare 25 PPO - Albemarle Select plan 10/01/18-12/31/19 In-Network Services Preventive Care Services
You must pay all of the costs for these services up to the specific deductible amount before the plan begins to pay for these services.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-552-9159. Important Questions
OSMA Health - Health Plan HDHP Single/Family Coverage Period: 1/1/ /31/2018 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
Blue Care Elect $250 Deductible MIIA Coverage Period: on or after 07/01/2015
 Blue Care Elect $250 Deductible MIIA Coverage Period: on or after 07/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This
Blue Care Elect $250 Deductible MIIA Coverage Period: on or after 07/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This
Summary of Benefits. Albemarle Choice HDHP-HSA. (Plan uses KeyCare PPO. providers)
 Summary of Benefits Albemarle Choice HDHP-HSA (Plan uses KeyCare PPO providers) Effective October 1, 2018-December 31, 2019 Lumenos HSA-HDHP 478 Albemarle Choice plan 10/1/18-12/31/19 In-Network Services
Summary of Benefits Albemarle Choice HDHP-HSA (Plan uses KeyCare PPO providers) Effective October 1, 2018-December 31, 2019 Lumenos HSA-HDHP 478 Albemarle Choice plan 10/1/18-12/31/19 In-Network Services
Anthem Blue Cross Your Plan: PPO Plan Your Network: National PPO (BlueCard PPO)
 Anthem Blue Cross Your Plan: PPO Plan Your Network: National PPO (BlueCard PPO) This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Anthem Blue Cross Your Plan: PPO Plan Your Network: National PPO (BlueCard PPO) This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
You can see the specialist you choose without permission from this plan.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-811-3106. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-877-811-3106. Important Questions
Health Plan Shopping Guide
 Health Plan Shopping Guide Use this guide to help you choose a health insurance plan through the Massachusetts Health Connector. Step 1: Know which plans you qualify for First, you ll need to know which
Health Plan Shopping Guide Use this guide to help you choose a health insurance plan through the Massachusetts Health Connector. Step 1: Know which plans you qualify for First, you ll need to know which
Bronze LINK Coverage Period: 01/01/ /31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mhc.coop or by calling (855) 447-2900. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mhc.coop or by calling (855) 447-2900. Important Questions
Your Plan: Anthem Silver PPO 2000/35%/6850 Your Network: Prudent Buyer PPO
 Your Plan: Anthem Silver PPO 2000/35%/6850 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Your Plan: Anthem Silver PPO 2000/35%/6850 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Your Plan: Anthem Bronze PPO 6000/0%/6000 w/hsa Your Network: Prudent Buyer PPO
 Your Plan: Anthem Bronze PPO 6000/0%/6000 w/hsa Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Your Plan: Anthem Bronze PPO 6000/0%/6000 w/hsa Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
AETNA MEMBER GUIDEBOOK
 State of New Jersey AETNA MEMBER GUIDEBOOK Aetna Value HD Plan Aetna Freedom Plan Aetna Medicare Advantage PPO ESA Plan FOR EMPLOYEES AND RETIREES ENROLLED IN THE STATE HEALTH BENEFITS PROGRAM OR SCHOOL
State of New Jersey AETNA MEMBER GUIDEBOOK Aetna Value HD Plan Aetna Freedom Plan Aetna Medicare Advantage PPO ESA Plan FOR EMPLOYEES AND RETIREES ENROLLED IN THE STATE HEALTH BENEFITS PROGRAM OR SCHOOL
Regence HDHP-1 with Alternative Care Coverage Period: 01/01/ /31/2017
 Regence HDHP-1 with Alternative Care Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2017-12/31/2017 Coverage for: Individual & Eligible Family Plan Type:
Regence HDHP-1 with Alternative Care Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2017-12/31/2017 Coverage for: Individual & Eligible Family Plan Type:
2017 Open Enrollment is October 31 November 18, 2016
 Non-Union Support Staff and Local 2110 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of Non-Union Support Staff or Local 2110, you can take advantage
Non-Union Support Staff and Local 2110 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of Non-Union Support Staff or Local 2110, you can take advantage
2017 Summary of Benefits and Coverage Documents
 2017 Summary of Benefits and Coverage Documents Table of Contents Blue Plan PPO with HRA Individual Coverage 3 Green Plan PPO with HSA Individual Coverage 11 Orange Plan PPO with HSA Individual Coverage
2017 Summary of Benefits and Coverage Documents Table of Contents Blue Plan PPO with HRA Individual Coverage 3 Green Plan PPO with HSA Individual Coverage 11 Orange Plan PPO with HSA Individual Coverage
Consumer Directed Health Plan With Health Savings Account (CDHP with HSA) 2018 Frequently Asked Questions (FAQs)
 Consumer Directed Health Plan With Health Savings Account (CDHP with HSA) 2018 Frequently Asked Questions (FAQs) Q: What is the Consumer Directed Health Plan (CDHP)? A: The CDHP is one of the medical plan
Consumer Directed Health Plan With Health Savings Account (CDHP with HSA) 2018 Frequently Asked Questions (FAQs) Q: What is the Consumer Directed Health Plan (CDHP)? A: The CDHP is one of the medical plan
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
National Elevator Industry: Health Benefit Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual + Family Plan Type:
Your Benefits Connected
 Annual Enrollment 2013: November 7 through 21 Your Benefits Connected It s Time to Review Your Verizon Benefit Options BenefitsConnection www.verizon.com/benefitsconnection Annual Enrollment will begin
Annual Enrollment 2013: November 7 through 21 Your Benefits Connected It s Time to Review Your Verizon Benefit Options BenefitsConnection www.verizon.com/benefitsconnection Annual Enrollment will begin
CoventryOne Fusion 100%/50% POS Plans
 CoventryOne Fusion 100%/50% POS Plans $3,000 $5,000 In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member) $6,000,000 $6,000,000 Deductible (per benefit year) - Maximum 3 per family
CoventryOne Fusion 100%/50% POS Plans $3,000 $5,000 In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member) $6,000,000 $6,000,000 Deductible (per benefit year) - Maximum 3 per family
Your Plan: Anthem Bronze Select PPO 6350/0%/6350 w/hsa Your Network: Select PPO
 Your Plan: Anthem Bronze Select PPO 6350/0%/6350 w/hsa Your Network: Select PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Your Plan: Anthem Bronze Select PPO 6350/0%/6350 w/hsa Your Network: Select PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
2018 Medical Comparison Guide
 2018 Medical Comparison Guide This and the following pages contain a limited description of the benefit coverage available through this group plan. Coverage is governed at all times by the complete terms
2018 Medical Comparison Guide This and the following pages contain a limited description of the benefit coverage available through this group plan. Coverage is governed at all times by the complete terms
Chevron High Deductible Health Plan (HDHP) (311)
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at hr2.chevron.com, or by calling the Chevron Human Resources
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at hr2.chevron.com, or by calling the Chevron Human Resources
No. What is not included in the out of pocket limit? Even though you pay these expenses, they don t count toward the out-of-pocket limit.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan s summary plan description at www.psbenefitstrust.com or by calling (206) 441-7574,
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan s summary plan description at www.psbenefitstrust.com or by calling (206) 441-7574,
BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Value PPO
 BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Value PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at www.bridgespanhealth.com.
BridgeSpan Health Company: BridgeSpan Oregon Standard Silver Plan Value PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at www.bridgespanhealth.com.
Summary of Benefits Anthem Balanced Funding PPO / % 10/30/50/30%
 Summary of Benefits Anthem Balanced Funding PPO 3 25-1000/4000-80% 10/30/50/30% PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK CARE COVERED? 1 Yes, but the patient pays
Summary of Benefits Anthem Balanced Funding PPO 3 25-1000/4000-80% 10/30/50/30% PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred provider plan 2. OUT-OF-NETWORK CARE COVERED? 1 Yes, but the patient pays
In-network: $5,000 single / $10,000 family per calendar year. Out-of-network: $10,000 per insured per
 Regence BlueShield: Regence Direct Bronze HSA Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
Regence BlueShield: Regence Direct Bronze HSA Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
Your Plan: Anthem Silver PPO 3400/0%/3400 w/hsa Your Network: Anthem PPO
 Your Plan: Anthem Silver PPO 3400/0%/3400 w/hsa Your Network: Anthem PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Your Plan: Anthem Silver PPO 3400/0%/3400 w/hsa Your Network: Anthem PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not
Yes. Some of the services this plan doesn t cover are listed on page 4
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.centuryhealthcare/com/user/login or by calling 1-877-685-2432.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.centuryhealthcare/com/user/login or by calling 1-877-685-2432.
2017 Open Enrollment is October 31 November 18, 2016
 TWU 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of TWU, you can take advantage of a comprehensive benefits package. Now is the time to review your
TWU 2017 Open Enrollment is October 31 November 18, 2016 Your Columbia University Benefits As a member of TWU, you can take advantage of a comprehensive benefits package. Now is the time to review your
What is the overall deductible? Are there other deductibles for specific services? Is there an out-ofpocket
 Regence BlueShield: Regence Direct Silver with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers &
Regence BlueShield: Regence Direct Silver with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers &
CHOICE PLUS PLAN. UnitedHealthcare. with a HEALTH REIMBURSEMENT ACCOUNT PLAN FEATURES. Medical. You can choose any doctor or hospital you want.
 Medical UnitedHealthcare CHOICE PLUS PLAN with a HEALTH REIMBURSEMENT ACCOUNT welcometouhc.com Find a network doctor. Choose with confidence. Our UnitedHealth Premium designation program recognizes physicians
Medical UnitedHealthcare CHOICE PLUS PLAN with a HEALTH REIMBURSEMENT ACCOUNT welcometouhc.com Find a network doctor. Choose with confidence. Our UnitedHealth Premium designation program recognizes physicians
Senior Care Network: Blue Access PPO and Blue Access Choice PPO Coverage Period: 01/01/ /31/2016
 Senior Care Network: Blue Access PPO and Blue Access Choice PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
Senior Care Network: Blue Access PPO and Blue Access Choice PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual/Family
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
$5,000 person. Does not apply to preventive care. Coverage for: Individual + Family Plan Type: PPO
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
NETWORK: $4,000 single / $10,000 family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
What is the overall deductible? Are there other deductibles for specific services? Is there an out-ofpocket
 Regence BlueCross BlueShield of Oregon: Preferred Coverage Period: 12/01/2014-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible Family
Regence BlueCross BlueShield of Oregon: Preferred Coverage Period: 12/01/2014-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible Family
Montgomery County Public Schools- PPO Coverage Period: 10/01/ /30/2017
 Montgomery County Public Schools- PPO Coverage Period: 10/01/2016 09/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
Montgomery County Public Schools- PPO Coverage Period: 10/01/2016 09/30/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
CoventryOne Qualified High Deductible 100%/60% POS Plans
 CoventryOne Qualified High Deductible 100%/60% POS Plans $1,250/$2,500 $3,000/$5,500 $5,000/$10,000 In-Network Out-of-Network In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member)
CoventryOne Qualified High Deductible 100%/60% POS Plans $1,250/$2,500 $3,000/$5,500 $5,000/$10,000 In-Network Out-of-Network In-Network Out-of-Network In-Network Out-of-Network Lifetime Max (per Member)
BridgeSpan Health Company: BridgeSpan Silver HDHP 2000 MyChoice Northwest
 BridgeSpan Health Company: BridgeSpan Silver HDHP 2000 MyChoice Northwest Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Individual
BridgeSpan Health Company: BridgeSpan Silver HDHP 2000 MyChoice Northwest Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Individual
Individual & Family Plans Insured by Connecticut General Life Insurance Company. Cigna Health Savings Plans for Tennessee. medical & b 12/12
 Individual & Family Plans Insured by Connecticut General Life Insurance Company Cigna Health Savings Plans for Tennessee medical & PHARMACY INSURANCE for a VERY UNIQUE INDIVIDUAL. YOU. 858437 b 12/12 Services
Individual & Family Plans Insured by Connecticut General Life Insurance Company Cigna Health Savings Plans for Tennessee medical & PHARMACY INSURANCE for a VERY UNIQUE INDIVIDUAL. YOU. 858437 b 12/12 Services
open enrollment is here 2018 benefit changes
 your health open enrollment is here 2018 benefit changes what s inside? 04 Do I need to enroll? 06 How to enroll 07 2018 benefit changes 34 Optional benefits still available don t miss these 2018 highlights
your health open enrollment is here 2018 benefit changes what s inside? 04 Do I need to enroll? 06 How to enroll 07 2018 benefit changes 34 Optional benefits still available don t miss these 2018 highlights
Your Plan: Anthem Silver Blue Access PPO 2000/50%/6350 Your Network: Blue Access
 Your Plan: Anthem Silver Blue Access PPO 2000/50%/6350 Your Network: Blue Access This summary of benefits is a brief outline of coverage, designed to help y ou with the selection process. This summary
Your Plan: Anthem Silver Blue Access PPO 2000/50%/6350 Your Network: Blue Access This summary of benefits is a brief outline of coverage, designed to help y ou with the selection process. This summary
Anthem Blue Cross Your Plan: PPO HSA Plan Your Network: National PPO (BlueCard PPO)
 Anthem Blue Cross Your Plan: PPO HSA Plan Your Network: National PPO (BlueCard PPO) This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: PPO HSA Plan Your Network: National PPO (BlueCard PPO) This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Anthem Blue Cross Your Plan: Lumenos HSA 2000/ /40 (LHSA2153) Your Network: Prudent Buyer PPO
 Anthem Blue Cross Your Plan: Lumenos HSA 2000/4000 20/40 (LHSA2153) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
Anthem Blue Cross Your Plan: Lumenos HSA 2000/4000 20/40 (LHSA2153) Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process.
NETWORK: $500 single / $1,000 family maximum for in-network providers and $750 single / $1,500 family maximum for out-ofnetwork
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.clftpaedi.com or by calling 888-244-5096. Important Questions
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-855-333-5730. Important
HealthTrust: LUMENOS $2500 Coverage Period: 07/01/ /30/2017
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4896. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-888-224-4896. Important Questions
$2,000 single. $4,000 non-single
 Schedule of Benefits (Who Pays What) Anthem Blue Cross and Blue Shield Name of Carrier Lumenos Health Savings Account (HSA-Compatible) Plan 18 Name of Plan PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred
Schedule of Benefits (Who Pays What) Anthem Blue Cross and Blue Shield Name of Carrier Lumenos Health Savings Account (HSA-Compatible) Plan 18 Name of Plan PART A: TYPE OF COVERAGE 1. TYPE OF PLAN Preferred
Annual Notice of Changes for 2018
 BlueMedicare Choice (Regional PPO) offered by Florida Blue Annual Notice of Changes for 2018 You are currently enrolled as a member of BlueMedicare Regional PPO. Next year, there will be some changes to
BlueMedicare Choice (Regional PPO) offered by Florida Blue Annual Notice of Changes for 2018 You are currently enrolled as a member of BlueMedicare Regional PPO. Next year, there will be some changes to
Simple answers to health reform s complex issues facing every employer, and what you can do now to protect your business and your future.
 Simple answers to health reform s complex issues facing every employer, and what you can do now to protect your business and your future. If you have any questions, please contact: Health Reform: A Guide
Simple answers to health reform s complex issues facing every employer, and what you can do now to protect your business and your future. If you have any questions, please contact: Health Reform: A Guide
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Employee Benefit Plan: Missoula County Public Schools Coverage Period: 01/01/ /31/2014 Summary of Benefits and Coverage:
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Plan Type: HDHP This is only a summary. If you want more detail about your coverage and costs, you can get
Important Questions Answers Why This Matters: If took HealthQuotient:
 HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/2017-12/31/2017 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: All Tiers Plan Type: HDHP
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
Important Questions Answers Why this Matters:
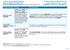 Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services? Is there an out of pocket limit on my expenses? $1,500 single / $3,000 family
2015 ANNUAL ENROLLMENT GUIDE
 2015 ANNUAL ENROLLMENT GUIDE State of Louisiana Employees and Retirees Administered by Blue Cross and Blue Shield of Louisiana Blue Cross and Blue Shield of Louisiana is incorporated as Louisiana Health
2015 ANNUAL ENROLLMENT GUIDE State of Louisiana Employees and Retirees Administered by Blue Cross and Blue Shield of Louisiana Blue Cross and Blue Shield of Louisiana is incorporated as Louisiana Health
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 CEBCO: Champaign County Plan 1a Blue Access (PPO) Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
CEBCO: Champaign County Plan 1a Blue Access (PPO) Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
2014 Side-by-side comparison between the Aetna CDHP and the Aetna PPO for Medical Coverage
 2014 Side-by-side comparison between the and the for Medical Coverage Medical Coverage Carrier Aetna Aetna Aetna Aetna Deductible Individual $1,750 $3,250 $750 $2,250 Family $3,500 $6,500 $1,500 $4,500
2014 Side-by-side comparison between the and the for Medical Coverage Medical Coverage Carrier Aetna Aetna Aetna Aetna Deductible Individual $1,750 $3,250 $750 $2,250 Family $3,500 $6,500 $1,500 $4,500
Your Options: You may choose one of the following options.
 October 17 to November 4, 2016 Benefit Information for Non Permanent Employees Working an Average of 30 Hours/Week (For employees who only qualify for Bronze Plan) The Affordable Care Act (ACA) requires
October 17 to November 4, 2016 Benefit Information for Non Permanent Employees Working an Average of 30 Hours/Week (For employees who only qualify for Bronze Plan) The Affordable Care Act (ACA) requires
Important Questions Answers Why this Matters: In-network: $2,100 person /
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mhc.coop or by calling (855) 488-0622. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mhc.coop or by calling (855) 488-0622. Important Questions
Copay Select $1,000. Coverage Period: 07/01/ /30/2016 Coverage for: Single & Family Plan Type: PPO
 Copay Select $1,000 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2015 06/30/2016 Coverage for: Single & Family Plan Type: PPO This is only a summary. If
Copay Select $1,000 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2015 06/30/2016 Coverage for: Single & Family Plan Type: PPO This is only a summary. If
$5,000 Individual/ $10,000 Family. Important Questions Answers Why this Matters: What is the overall deductible?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cvtrust.org or by calling 1-800-288-9870. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cvtrust.org or by calling 1-800-288-9870. Important Questions
Important Questions Answers Why this Matters:
 Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
Anthem BlueCross BlueShield Blue Access PPO Option 20 / Rx Option 7 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage For: Individual/Family
expenses, charges in excess of benefit maximums and
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.oetrustfunds.org or by calling 1-800-251-5014 or 1-800-532-2105.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.oetrustfunds.org or by calling 1-800-251-5014 or 1-800-532-2105.
HealthFlex: Blue Cross and Blue Shield of Illinois Coverage Period: 01/01/ /31/2015 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gbophb.org (click on HealthFlex/WebMD) or by calling
EnhancedBlue SM Gold 1000 PPO
 EnhancedBlue SM Gold 1000 PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Single & Family Plan Type: PPO This is only a
EnhancedBlue SM Gold 1000 PPO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016 12/31/2016 Coverage for: Single & Family Plan Type: PPO This is only a
HOW THE MEDICAL PLANS COMPARE
 HOW THE MEDICAL PLANS COMPARE FEATURE Cigna and UPMC High Deductible Health Plans (HDHP) Cigna Open Access Plus (OAP) UPMC Health Plan Organization (EPO) Type of Plan With a High Deductible Health Plan/Health
HOW THE MEDICAL PLANS COMPARE FEATURE Cigna and UPMC High Deductible Health Plans (HDHP) Cigna Open Access Plus (OAP) UPMC Health Plan Organization (EPO) Type of Plan With a High Deductible Health Plan/Health
2018 Retiree Choice Annual Enrollment Guide
 2018 Retiree Choice Annual Enrollment Guide October 25 through November 8, 2017 Enrolling What You Need to Do Payment Options How to Enroll What s New for 2018? Here are the benefit changes that will be
2018 Retiree Choice Annual Enrollment Guide October 25 through November 8, 2017 Enrolling What You Need to Do Payment Options How to Enroll What s New for 2018? Here are the benefit changes that will be
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mhc.coop or by calling (855) 488-0622. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.mhc.coop or by calling (855) 488-0622. Important Questions
Affinity Health Plan: Essential Plan 3 Summary of Benefits and Coverage: What this Plan Covers & W hat it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the schedule of benefits by visiting Affinityplan.org and clicking on Essential Plans or
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the schedule of benefits by visiting Affinityplan.org and clicking on Essential Plans or
$1,500 Individual/$3,000 Family for participating providers. $3,000 Individual/$6,000. Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.calcpahealth.com or by calling 1-877-480-7923. Important
You must pay all the costs up to the deductible amount before this plan. covered services after you meet the deductible.
 Secure Choice Health Savings Account Partner Coverage Period: Beginning on or after 01-01-2016 Summary of Benefits and Coverage: What this Plan covers & What it Costs Coverage for: S, S+1, and Family coverage
Secure Choice Health Savings Account Partner Coverage Period: Beginning on or after 01-01-2016 Summary of Benefits and Coverage: What this Plan covers & What it Costs Coverage for: S, S+1, and Family coverage
Regence BlueCross BlueShield of Oregon: Preferred Coverage Period: 07/01/ /31/2016
 Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
Regence BlueCross BlueShield of Oregon: Preferred Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 07/01/2016 12/31/2016 Coverage for: Individual & Eligible Family
The Guide to Your Summary of Benefits and Coverage (SBC)
 The Guide to Your Summary of Benefits and Coverage (SBC) Under the federal Affordable Care Act, health insurers and group health plans are required to provide an SBC. This regulation is intended to give
The Guide to Your Summary of Benefits and Coverage (SBC) Under the federal Affordable Care Act, health insurers and group health plans are required to provide an SBC. This regulation is intended to give
No Charge Primary care visit to treat an injury or illness. 20% Specialist care visit
 Effective: January 1, 2018 UC Medicare PPO Plan Please Note: this medical plan is a complement to your existing Medicare plan. Medicare benefits are primary and then the benefits of this plan are calculated
Effective: January 1, 2018 UC Medicare PPO Plan Please Note: this medical plan is a complement to your existing Medicare plan. Medicare benefits are primary and then the benefits of this plan are calculated
for Individuals and Families 2017
 for Individuals and Families 2017 LIVE LIFE ASSURED A great health plan that s all yours The plans in this brochure are for people who aren t on an employer plan, covered by a parent s policy, are self-employed
for Individuals and Families 2017 LIVE LIFE ASSURED A great health plan that s all yours The plans in this brochure are for people who aren t on an employer plan, covered by a parent s policy, are self-employed
East Hartford BOE (Administrators) 2014 High Deductible Health Plan Information Meeting L O C K T O N C O M P A N I E S
 East Hartford BOE (Administrators) 2014 High Deductible Health Plan Information Meeting L O C K T O N C O M P A N I E S 2014 Health & Welfare Benefits July 1, 2014 there will be no change to our current
East Hartford BOE (Administrators) 2014 High Deductible Health Plan Information Meeting L O C K T O N C O M P A N I E S 2014 Health & Welfare Benefits July 1, 2014 there will be no change to our current
Carroll County Public Schools. Flexible Benefits. Open Enrollment Guide
 Flexible Benefits Open Enrollment Guide 2019 125 North Court Street Westminster, MD 21157 Together - It's Possible! 2019 FLEXIBLE BENEFITS OPEN ENROLLMENT The Flexible Benefits Program (medical, dental,
Flexible Benefits Open Enrollment Guide 2019 125 North Court Street Westminster, MD 21157 Together - It's Possible! 2019 FLEXIBLE BENEFITS OPEN ENROLLMENT The Flexible Benefits Program (medical, dental,
$1,500 Individual/$3,000 Family for In-Network providers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-877-244-3593. HRA FUNDING
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca or by calling 1-877-244-3593. HRA FUNDING
